


Rachel Strohm was an active hiker, cycler and rock climber before long COVID felled her in December, 2021.
As a researcher in international development, travel vaccines for low-income countries are a typical part of my life. But I never expected that once I developed Long COVID, a travel vaccine for Japanese encephalitis might help me make a rapid recovery. Could similar vaccines hold clues to fighting Long COVID?
Long COVID: Fatigue and Frustration
My Long COVID journey began in December 2021, when I tested positive at the height of the first Omicron wave. Thanks to my previous Johnson & Johnson vaccination, it was a mild case, with the only real symptom being fatigue. After isolating for ten days, I went back to work. But I quickly found that I was struggling to re-engage.
I’d previously balanced full-time work with an active schedule of hiking, cycling, and rock climbing, but now I was pushing myself through one workday and feeling too tired to get out of bed the next. The fatigue and brain fog quickly worsened, and soon I could only stand up or focus for about an hour per day. No amount of rest, dietary changes, or supplements was helping. By March 2022, I had to go on leave from my job.
At the time, there weren’t any Long COVID specialists in Kenya, where I’ve lived since 2017. So I traveled back to Chicago to stay with my family there and enrolled at the Long COVID clinic at Northwestern Memorial Hospital. However, they couldn’t offer much for the fatigue. I left my first appointment feeling quite dejected.
The Japanese Encephalitis Vaccine
Separately from the Long COVID issue, I also needed to update some of my travel vaccines. In April 2022, I got boosters for meningitis; typhoid; tetanus, diphtheria, and pertussis (Tdap). I also got a new-to-me vaccine against the Japanese encephalitis virus (JEV), the first of a two-dose series. Despite the name, JEV is found across Asia, and I’d been planning a trip to India before I got sick. I decided to get the vaccine as long as I was at the travel clinic, just in case I ever recovered enough to travel.
Rachel received an array of vaccines – one of which was new to her.
The days after that first travel clinic appointment passed in the usual haze of fatigue and brain fog. Then I went back for my second dose of the JEV vaccine the following week. Within hours of the second dose, I felt my energy levels starting to improve. That was the first day in months that I hadn’t needed an afternoon nap.
I woke up the next day absolutely buzzing with energy. I had another appointment at Northwestern that morning, and afterwards I went across the street to an art museum and walked around for hours. I didn’t even take a nap when I got home later.
The buzzing feeling lasted for almost 10 days. I woke up early, completed my tasks for the day, started taking longer walks, and didn’t even crash the next day. I subsequently got appendicitis in late April, which killed the buzz, but I was back on my feet just days after surgery and had an easy recovery.
For ten months since then, my energy levels have consistently been about 90% of what they were pre-pandemic. I do need to rest more than I did before COVID-19, and I’ll still sometimes have a bad fatigue day if I push too hard during a workout, but thankfully this is rare. My cognition is totally back to normal, and I’m planning to finish some Ph.D. research that I’d paused earlier in the pandemic. It’s been a huge relief to be able to pick up my career again.
Vaccines and Trained Immunity
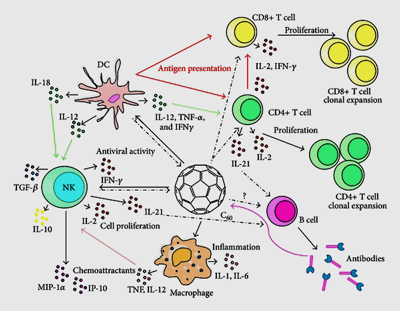
Innate immune system in action (Danijela Petrovic, Mariana Seke, Branislava Srdjenovic, Aleksandar Djordjevic, CC BY 4.0 <https://creativecommons.org/licenses/by/4.0>, via Wikimedia Commons).
Did the JEV vaccine really help me to recover from Long COVID, or was it just a quirk of timing in a recovery that I might have made anyway? I can’t make any causal claims about this from a single case study. But after reading a great deal of additional medical literature, I’ve come to believe that the vaccine may have helped my body clear viral reservoirs of SARS-CoV-2 which were likely contributing to my Long COVID fatigue (Choutka et al. 2022, Davis et al. 2022).
While this precise phenomenon has not been documented for the JEV vaccine and post-viral illnesses before, there’s a large amount of evidence showing that certain types of vaccines can help the body fight off unrelated viruses, in a process called trained immunity.
To understand trained immunity, let’s note that the human immune system is made up of two parts: the innate (general) and adaptive (specialized) immune systems. The innate immune system responds quickly to all foreign substances or germs. If the innate immune system can’t fight off a germ, this activates the adaptive immune system, which can respond to a specific bacteria or virus. The adaptive immune system may take some time to identify a new bacteria or virus, but once it has done so, it is able to remember that stimulus and respond quickly in the future.
Researchers used to believe that only the adaptive immune system had this type of immunological memory. However, recent studies have shown that the innate immune system can also improve its response to new types of viruses if it’s previously been exposed to a similar virus – often delivered through a vaccine. This is referred to as “trained immunity” of the innate immune system (Naik & Fuchs 2022, Netea et al. 2020).
In other words, getting a vaccine against one virus can help the innate immune system respond more efficiently to other viruses in the future. This may lower the risk of getting sick or reduce the severity of symptoms if one does get sick. Vaccines that can generate this type of trained immunity are also referred to as having non-specific or heterologous effects.
BCG Vaccine
One of the vaccines that have been most widely documented to generate trained immunity is the Bacillus Calmette-Guérin (BCG) vaccine. BCG is the live attenuated vaccine used against tuberculosis in many countries. Many studies have observed that children who are given this vaccine are also less likely to die of other respiratory illnesses (Aaby & Benn 2019, Arts et al. 2018, Lobo et al. 2021, Sohrabi et al. 2020). Similar effects have been found for the live attenuated measles, mumps, and rubella (MMR) vaccine and the live attenuated oral poliovirus vaccine (OPV) (Hutson 2022, Sørup et al. 2015).
While the trained immunity generated by these vaccines does offer an important source of protection from other viral illnesses, it also has its limitations. The vaccines don’t consistently generate trained immunity for everyone (Hutson 2022). The amount of non-specific protection offered by the vaccine may depend on whether or not it’s co-administered with other vaccines, which is particularly common for children (Aaby & Benn 2019). And the protective effect wanes over time, although it can be improved by boosters which are given to adolescents or adults (Sohrabi et al. 2020).
Trained Immunity for Post-Viral Illnesses?
Getting vaccinated against a different virus may have helped Rachel fight off the coronavirus.
If some cases of Long COVID are generated by viral reservoirs of SARS-CoV-2, then it certainly seems plausible that an unrelated vaccine that generates trained immunity might help the body fight off the lingering virus. Research on the specific topic of trained immunity for post-viral illnesses is limited, but there is some intriguing evidence around BCG, JEV, and acute COVID-19 infection which suggests that this hypothesis warrants further research.
Here are some key questions and answers on the topic.
Questions
Is there any evidence that vaccines like BCG or JEV can help people recover from Long COVID, or other post-viral illnesses?
Because dysfunction of the innate immune system is implicated in many post-viral illnesses, including myalgic encephalitis/chronic fatigue syndrome (ME/CFS) (Brenu 2014), a vaccine that helped train the innate immune system might help. At present, though, there do not seem to be any studies addressing this specific question. Most of the existing research looks at whether these vaccines can help to prevent a novel infection with an unrelated virus, rather than clearing an existing infection. Therefore, the impact of trained immunity might not be the same for acute vs. post-viral illness (Hirschenberger et al. 2021).
Notarte et al. (2022) review the experimental literature on whether people with Long COVID benefit specifically from COVID-19 vaccines, but find that some people improve and others worsen after receiving the vaccine, so the results are not conclusive. And Renz-Polster (2022) summarizes some of the pathways by which the BCG vaccine might affect individuals with Long COVID or ME/CFS. Renz-Polster reports that BCG vaccination has documented anti-viral effects on human herpesviruses and that several studies have found BCG vaccination slowed or prevented progression in multiple sclerosis – a disease associated, like ME/CFS, with Epstein-Barr virus (EBV) reactivation.
Given the lack of evidence on Long COVID, do we know if vaccines like BCG or JEV offer protection from acute infection with SARS-CoV-2?
The evidence on the effects of non-COVID-19 vaccines is mixed. Two observational studies from July-August 2020 found that higher national rates of childhood BCG vaccination were associated with fewer COVID-19 deaths per million people, although it’s not clear if this finding would have held for later variants like Delta or Omicron (Berg et al. 2020, Escobar et al. 2020).
An experimental study in Greece showed that elderly people who received a BCG booster were less likely to contact COVID-19 (Tsilika et al. 2021). However, studies in the Netherlands and South Africa found BCG boosters for adults had no effect on the likelihood of contacting COVID-19 (Bonten et al. 2021, Upton et al. 2022). A number of other studies of BCG and acute COVID-19 infection are ongoing, as summarized by Lobo et al. (2021). Looking beyond BCG, a study in Qatar suggests that the flu vaccine also offers protection against acute COVID-19 infection (Tayar et al. 2022). There are no studies of the JEV vaccine and COVID-19 infection.
The Gist
- An avid cyclist, hiker, and rock climber, international development policy specialist Rachel Strohm was in excellent shape before she went toe to toe with the coronavirus.
- It began with a mild case of COVID-19 in December, 2021. Seemingly quickly recovering, she returned to work but faded quickly, and three months later, she was on leave and on a flight from her home in Kenya to Chicago to seek help.
- She didn’t get any help from doctors but did from an unexpected arena. Rachel’s job left her no stranger to getting vaccinated against all sorts of diseases. Back in Chicago, she went to a travel clinic for booster shots for meningitis; typhoid; and tetanus, diphtheria and pertussis (Tdap) as well as the first of a two vaccine shots against the Japanese encephalitis virus (JEV).
- A week later, she received a second JEV shot, and felt her energy levels start to improve within hours. She woke up the next day “absolutely buzzing with energy,” and was immediately able to return to normal activities, like a long day walking around museums without fatigue.
- The buzzing feeling lasted for 10 days, stopped only by a case of appendicitis, from which she quickly recovered. In the 10 months since then, her energy levels have been about 90% of what they were pre-long COVID, and she’s been able to pick up her career again.
- So how did a vaccine against a different virus almost totally cure Rachel’s long COVID? Her research suggests the answer may lie in something called “trained immunity”, which occurs when vaccines against one virus help to clear the body of other viruses.
- Vaccines are targeted at boosting the adaptive immune response – the immune response that kicks in several days after the infection and zeros in directly on the pathogen. In trained immunity, though, vaccines against one pathogen appear to boost the early or innate immune system’s ability to fight off an infection.
- Vaccination with the Bacillus Calmette-Guérin (BCG) vaccine as well as attenuated measles, mumps and rubella (MMR) vaccines have all been shown to enhance responses to other pathogens. The effect doesn’t show up for everyone and may be less powerful when one vaccine is administered with others. Nor has the “trained immunity” hypothesis been tested in diseases like long COVID where the virus may be lingering.
- Still, studies suggest the innate immune response in post-infectious diseases like ME/CFS is impaired, and anything that helps it work better could help clear an unresolved infection. Plus, the BCG virus does appear to help knock down herpesvirus reactivation – possibly a key factor in both ME/CFS and long COVID.
- Neither BCG nor JEV has been tested against long COVID, but BCG’s ability to impact COVID-19 is mixed with some studies saying yes, and others no. With regard to the JEV vaccine Rachel received, several mouse studies suggest it may help protect against other viruses.
- The JEV vaccine’s effect on any one person with long COVID, though, is unclear and could be impacted by a number of factors, including what viruses and vaccines they’ve been exposed to in the past, and whether the coronavirus is actually persisting in them.
- It’s possible that Rachel caught a lucky break with the JEV vaccine. The fact that she’d never been exposed to the vaccine before and had not been ill long may have helped.
- The JEV vaccines’ rapid and striking effect on her long COVID, though, and the ready availability of other vaccines like BCG, oral polio vaccine (OPV), measles, mumps and rubella (MMR) – some of which have been shown to induce trained immunity – suggests that further investigations into whether vaccine-induced trained immunity can clear up long COVID in some people are warranted.
Of the various vaccines which can generate trained immunity, which ones might be most useful for treating acute or Long COVID?
Vaccines that can generate trained immunity have not been directly compared to each other. Generally speaking, the evidence suggests that live attenuated vaccines have a stronger protective effect than inactivated vaccines (Aaby & Benn 2019).
The JEV vaccine (Ixiaro) is inactivated. Why do you think it seemed to help you?
There’s a limited evidence base on trained immunity from the JEV vaccine. Two studies show that this vaccine can protect mice against novel viruses including Dengue and Zika (Li et al. 2016, Tarbe et al. 2020), but there’s no evidence in humans yet. A separate study shows that an inactivated vaccine made up of five types of bacteria offers protection against the flu virus in humans (Brandi et al. 2022). So there is some suggestion here that even inactivated vaccines can generate trained immunity, but much more research would be needed to document this conclusively.
Could everyone with Long COVID benefit from getting a vaccine like BCG or JEV?
While there is evidence that these types of vaccines may offer the immune system some support in clearing the SARS-CoV-2 virus, it seems unlikely that they will benefit everyone equally. Long COVID appears to affect the body through a number of underlying biological mechanisms, not just viral reservoirs (Davis et al. 2022, Koc et al. 2022).
These vaccines do not consistently generate trained immunity for everyone who receives them, given that people vary quite a lot in the number of viruses to which they’ve previously been exposed, and vaccines they’ve previously received (Sohrabi et al. 2020). Furthermore, live attenuated vaccines can pose some risk to people who are already immunocompromised (Miller & Wodi 2021), although in general, the BCG vaccine seems safe for adults recovering from acute COVID-19 (Dionato et al. 2022) and is well-tolerated in the broader population (Sohrabi et al. 2020). It may be worth discussing these vaccines with your doctor or your local travel clinic, but there’s no guarantee this is a cure for Long COVID.
Conclusions
To return to my own case for a moment, I personally feel that I caught a lucky break. By chance, I got a vaccine that appears to have generated some trained immunity and helped me recover from Long COVID. I suspect that part of this effect was due to the fact that the JEV vaccine was completely new to me, and I’ve often wondered if I would have received the same benefit from a booster for OPV or MMR, which I had already been exposed to as a child. I also had a limited range of symptoms compared to many Long COVID patients and had only been dealing with the illness for four months, so this may have facilitated a faster recovery once the viral reservoirs had been treated.
With these caveats noted, I do think that there’s huge potential in studying the use of existing vaccines to treat Long COVID. Vaccines such as BCG and OPV are safe and widely available in many countries outside the US, and the MMR and JEV vaccines are also available in the US. The lack of existing therapeutic options for Long COVID and other post-viral illnesses means that finding any accessible treatments should be a high priority.
About the Author
Rachel Strohm is the director of Social Policy Insights, a research consultancy based in Nairobi, Kenya. She holds an MA in political science from the University of California, Berkeley; an MA in international relations from Johns Hopkins University; and a BA in geography and French from Dartmouth College.
Bibliography
Aaby, P., and C.S. Benn. 2019. ‘Developing the Concept of Beneficial Non-Specific Effect of Live Vaccines with Epidemiological Studies’. Clinical Microbiology and Infection 25(12): 1459–67.
Arts, Rob J.W. et al. 2018. ‘BCG Vaccination Protects against Experimental Viral Infection in Humans through the Induction of Cytokines Associated with Trained Immunity’. Cell Host & Microbe 23(1): 89-100.e5.
Berg, Martha K. et al. 2020. ‘Mandated Bacillus Calmette-Guérin (BCG) Vaccination Predicts Flattened Curves for the Spread of COVID-19’. Science Advances 6(32): eabc1463.
Bonten, Marc, Mihai Netea, Frits Rosendaal, and Maurice van den Bosch. 2021. ‘Tuberculosis Vaccine Does Not Protect Vulnerable Elderly against COVID-19’. UMC Utrecht. https://www.umcutrecht.nl/en/over-ons/nieuws/details/jan-18-tuberculosis-vaccine-does-not-protect-vulnerable-elderly-against-covid-19 (February 7, 2023).
Brandi, Paola et al. 2022. ‘Trained Immunity Induction by the Inactivated Mucosal Vaccine MV130 Protects against Experimental Viral Respiratory Infections’. Cell Reports 38(1): 110184.
Choutka, Jan, Viraj Jansari, Mady Hornig, and Akiko Iwasaki. 2022. ‘Unexplained Post-Acute Infection Syndromes’. Nature Medicine 28(5): 911–23.
Davis, Hannah E., Lisa McCorkell, Julia Moore Vogel, and Eric J. Topol. 2023. ‘Long COVID: Major Findings, Mechanisms and Recommendations’. Nature Reviews Microbiology.
Dionato, Franciele A.V. et al. 2022. ‘BCG Vaccine Safety in COVID-19 Convalescent Adults: BATTLE a Randomized Controlled Trial’. Vaccine 40(32): 4603–8.
Escobar, Luis E., Alvaro Molina-Cruz, and Carolina Barillas-Mury. 2020. ‘BCG Vaccine Protection from Severe Coronavirus Disease 2019 (COVID-19)’. Proceedings of the National Academy of Sciences 117(30): 17720–26.
Hirschenberger, Maximilian, Victoria Hunszinger, and Konstantin Maria Johannes Sparrer. 2021. ‘Implications of Innate Immunity in Post-Acute Sequelae of Non-Persistent Viral Infections’. Cells 10(8): 2134.
Hutson, Matthew. 2022. ‘Beyond the Booster Shot | The New Yorker’. The New Yorker. https://www.newyorker.com/science/annals-of-medicine/beyond-the-booster-shot.
InformedHealth.org. 2020. InformedHealth.org [Internet] The Innate and Adaptive Immune Systems. Institute for Quality and Efficiency in Health Care (IQWiG). https://www.ncbi.nlm.nih.gov/books/NBK279396/ (February 7, 2023).
Koc, Ho Cheng et al. 2022. ‘Long COVID and Its Management’. International Journal of Biological Sciences 18(12): 4768–80.
Li, Jieqiong et al. 2016. ‘Cross-Protection Induced by Japanese Encephalitis Vaccines against Different Genotypes of Dengue Viruses in Mice’. Scientific Reports 6(1): 19953.
Lobo, Niyati et al. 2021. ‘100 Years of Bacillus Calmette–Guérin Immunotherapy: From Cattle to COVID-19’. Nature Reviews Urology 18(10): 611–22.
Naik, Shruti, and Elaine Fuchs. 2022. ‘Inflammatory Memory and Tissue Adaptation in Sickness and in Health’. Nature 607(7918): 249–55.
Netea, Mihai G. et al. 2020. ‘Defining Trained Immunity and Its Role in Health and Disease’. Nature Reviews Immunology 20(6): 375–88.
Notarte, Kin Israel et al. 2022. ‘Impact of COVID-19 Vaccination on the Risk of Developing Long-COVID and on Existing Long-COVID Symptoms: A Systematic Review’. eClinicalMedicine 53: 101624.
Okafor, Chika N., Ayesan Rewane, and Ifeanyi I. Momodu. 2022. ‘Bacillus Calmette Guerin’. In StatPearls, Treasure Island (FL): StatPearls Publishing.
Raddad, Laith Jamal Abu. ‘Effectiveness of Influenza Vaccination against SARS-CoV-2 Infection among Healthcare Workers in Qatar’.
Renz-Polster, Herbert. 2022. ‘BCG Vaccination as a Treatment Option for ME/CFS and Post Covid Syndrome?’ https://www.kinder-verstehen.de/wp-content/uploads/BCG_hypothesis_short_251222.pdf.
Sohrabi, Yahya et al. 2020. ‘Trained Immunity as a Novel Approach against COVID‐19 with a Focus on Bacillus Calmette–Guérin Vaccine: Mechanisms, Challenges and Perspectives’. Clinical & Translational Immunology 9(12).
Sørup, Signe et al. 2016. ‘Oral Polio Vaccination and Hospital Admissions With Non-Polio Infections in Denmark: Nationwide Retrospective Cohort Study’. Open Forum Infectious Diseases 3(1): ofv204.
Tarbe, Marion et al. 2020. ‘Japanese Encephalitis Virus Vaccination Elicits Cross-Reactive HLA-Class I-Restricted CD8 T Cell Response Against Zika Virus Infection’. Frontiers in Immunology 11: 577546.
Tsilika, Maria et al. 2022. ‘ACTIVATE-2: A DOUBLE-BLIND RANDOMIZED TRIAL OF BCG VACCINATION AGAINST COVID19 IN INDIVIDUALS AT RISK’. Frontiers in Immunology 13:873067.
Upton, Caryn M. et al. 2022. ‘Safety and Efficacy of BCG Re-Vaccination in Relation to COVID-19 Morbidity in Healthcare Workers: A Double-Blind, Randomised, Controlled, Phase 3 Trial’. eClinicalMedicine 48: 101414.
World Health Organization. ‘Japanese Encephalitis’. https://www.who.int/news-room/fact-sheets/detail/japanese-encephalitis (February 7, 2023).


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



I love your story and I am so glad you chose to share it. Personally I am still coasting on the huge improvement I got from the Shingrix vaccine over a month ago, with acyclovir added since I then suspected I’m in the EBV/herpesvirus reservoir MECFS cohort.
I am so hopeful for the potential for vaccines and antivirals for some of us. But it’s definitely a gamble at this stage, because when I was reading about Shingrix I saw plenty of LC and ME folks who didn’t benefit or worsened.
I wish everyone who chooses to try this path success or at least not worsening!
So interesting! It really shows how much the immune system plays in these diseases. Who knows? Maybe just a boost in the right direction is all that’s needed. I got the Shingrix vaccine and unfortunately did not receive a boost – but no ill effects either – and I’m glad I got it. We’re going to do a blog and a poll on it.
And, yes – thanks so much to Rachel for going to the effort to do the research and write the blog about what happened so that we could possibly benefit. 🙂
I’m wondering whether it was the Japanese Encephalitis Vaccine alone that made her better, or the combination of it plus all the other boosters she received?
i would like that they could reverse my decline over covid vaccines as many people have had with ME/cfs or so… So for me no vaccine anymore…
Great article. I’m going to give the JEV JEspect/Ixiaroa a go (it is endemic where I live) and report back about what it does for my ME/CFS.
I’m interested in knowing
Kevin,
It took awhile to track down supply of JEspect, but I can safely say a week and a bit after the second dose that it didn’t do anything for my ME/CFS. But I don’t have to worry about mosquito’s as much.
Good luck!
A Swedish doctor seemed to have some success with a staphylococcus vaccine about 20 years ago with ME/CFS. I don’t know if that vaccine generates ‘trained immunity’ or not.
Also, long covid is clearly linked to the covid virus. There are only hypothetical linkages to viruses in CFS, and far from any categorical proof. I know that some people like the HHV theory, I guess if that theory has veracity then potentially this ‘trained immunity’ idea has some potential merit. Maybe…
Carl-Gerhard Gottfried,he takes the vaccine every month, otherwise symptoms come back. The vaccine is not available anymore,but he stored enough vaccine for himself for the rest of his life.
I know that story. That was a psychiatrist who tested it himself with good results. But over time the ME/CFS came back, didn’t it? And he took the vaccine again. If I’m right… very interesting. I have also heard that a ME/CFS patient had gotten a lot better after a new infection with high fever. Sounds contradictory. It’s a strange disease. But it is clear that the immune system plays a role in some of the patients if not in all.
Regarding Gijs comment on Fever. When I did an FMT, my body basically had a feverish reaction in the form of nightsweats and chills and basically I went from 25% functional to 70% functional overnight. I have always pondered whether there was a way to induce fever as when I get sick, I never get a fever and my body temperature stays on the low side. There is a therapy called hyperthermia which does that and is used in cancer treatment and I wonder what effect it would have on ME/CFS patients. There is another therapy called extended dry-fasting (9 days without food or water) which basically does the same thing and more and has cured people Chronic Lyme, Cancer, and MS. The woman below chronicles her experiences which I find is the easiest way to start digesting this concept.
https://michelleslater.com/tag/starving-to-heal-in-siberia/
Hi Gijs, I am verry interested in FMT. May i ask in wich country you let it do? and was it before covid, how screened the FMT for to get no bad things. was it through colon or due a pilL. If you do not mind, everything I am intersted in. Long time ago, verry long time, i saw a webinar and a women with ME/cfs who had 15 FMT’s but allways declined back. So i thought at least multiple FMT’s would be necesarry. was it stool from familly wich they advise, healthy sportsmen, matched by female/male? And how was it done? thanks a lot! the fasting i do not dare because i allready have trouble eating… I am way to ill, to bedridden.
Hi Konjin, I did the FMT myself with the stool of a good friends son who was an athlete. There is a lot to consider when doing an FMT and when I did it I was very ill and barely had the energy to do the prep work. If you have trouble eating, then it even more so could be beneficial. I felt the benefit after the first one and I did several more over the next weeks. It was not cure but significantly better.
thanks so much for answering! I am also way to ill to do the prep work, over decades no contacts anymore so have no female healthy athlete friend for stool. but i feel how ill i am, declining fast, i must do something… what prepwork did you do or the son of a friend? my brain is also bad, what to consider all? i searched where i live for professional fmt but only given for colon bacteria issues. in the netherlands i found a verry preleminary 1 case study on fmt for MS. Also not for ME. Am desperate. would have tryd to go laying down. but they do it not for ME. not here, not in neighbour countrys. All only for can not remember the nae, a certain colon bacteria and so…
I wish I could come there and help you out. THe best I can do is provide you links to facebook and reddit groups on FMT. There are people who sell stool in capsules from Spain and Turkey but it is not cheap, but there are some positive reviews in the FB and reddit groups
https://www.reddit.com/r/fmt/
https://www.facebook.com/groups/1676427302597468
thank you!!! yes please. I clicked on the link you put there and also saw bad reactions, bad compagny, … It is a risk if you do not know the persons from who you get the stool. And it is not screened on anything. Or at least you do not know… would you trust capsules sold from Spain or Turkey from who knows who? Maybe i must read another time further. At least i get not more stupid from it. But the way you did it, with help from a friend son (athlete), is more reliable i guess then people asking big money for things and not knowing what you buy. But i can learn from it and hopefully find someone or especially a hospital who does it. thanks a lot!!!
The taymount clinic in UK also does FMT through capsules. In general, there would be a variety of testing for the donor beforehand. However, over time, I have come to the conclusion that most people are healthier than I am and when you are desperate and if you can find a good person who is willing to work with you for an FMT, then a general discussion about their health and stool habits could be enough. If you can find a way to advertise your need somehow (it is not easy, I know as I have tried) in local community groups then you might get lucky to find someone. Most likely, your submissions will be banned and people will feel uncomfortable discussing this, but their are people out there who want to help, its just really hard to do when you can’t leave your house.
thank you so much for all the effort of writing to me and all the info!!! yes, verry ill makes it all harder, would need to “go” lying down to UK, light, noise, sleep issues, do not know how i can manage it…. but is safer and better matched. Finding someone through community groups, etc I can imagine how hard it is and you do not know them like your friends son, the athlete, so they can tell you what they want…. Do you maybe know FMT near Belgium by coincidence? I tryd to search but could no more.. But will pick it up again but in netherlands nothing for ME.Also i do not understand the difference, pro and cons from FMT through colon and swallowing a pill. Safetywise, etc. thanks a lot!!!
i looked at the thaymount clinic and they wrote:
10 day Faecal Microbiota Transplants Programme.
Our program for FMT is 10 Transplants over 10 days at Taymount Clinic (UK) with a ‘rest weekend’ between days 5 and 6.
I do not know much of FMT, but is so many days in a row not to much? that it must be more devided over time? you are the expert… if possible please your opinion.
Personally, I think an actual healthy poop transplant through the colon is the best method. You would need to clean out your colon first. My reasons are there are other things in your gut besides bacteria (macrophages for example) and there are certain bacteria that are anaerboic (which means they die in the presence of oxygen, so any pills made from poop, these ones will have already died. Still, poop pills are commonly used for C-Diff and other illnesses and are much more convenient.
Thanks for recollecting that. A fascinating story I had forgotten about. Check out the blog
https://www.healthrising.org/blog/2015/11/21/gottfries-chronic-fatigue-syndrome-story/
FMT is not a perfect science. This is the protocol they have developed, I would suggest you ask them the questions. I would assume if you asked them, they would extend the time between sessions. I have read about people being fixed after only 1 transfusion and others who have done many and it doesn’t work. Mehgan ORourke writes in her book the Invisible Kingdom that she was herxing so bad after 5 days that she stopped. But, she later said it helped her in the long run.
https://www.amazon.com/Invisible-Kingdom-Reimagining-Chronic-Illness/dp/1594633797
pages 212-221
This old doctor is Karl (Gottries). I created my BCG protocol with his assistance. He used Staphypan but that wasn’t any more available. Thus, I had to find another vaccine. I browsed through medical literature regarding vaccines and I stumbled across BCG vaccine. I asked Karl what he thinks about using BCG for CFS. He said it was an excellent idea. I asked for his staph treatment schedule and applied the same with BCG. I needed BCG vaccine first. I drafted a petition for off label treatment and filed it to the Hungarian Drug Supervisory Agency. My petition was approved in one day under expedited procedure (under it wont hurt basis…). First results came within 3 months.
Fascinating and hopeful story! Thanks very much. Would it be crazy to go to a travel medicine clinic and ask for the JEV and the BCG vaccines? I had the Shringrix shot a few months ago and got no help with ME/CFS. And then 3 days ago I got the second pneumonia vaccine. I’ll see if that does anything beside protect me from pneumonia.
Can’t get the BCG vaccine in the US. But the JEV is available.
Just fascinating! Thank you for writing up your story, Rachel. The fact you are a researcher is lucky for those of us with ME, etc. as you were really able to document everything so well & back up your research with great citations.
Your caveats are well taken, but if the right researcher in the ME field – or the immunology field – could only pick this up & follow the breadcrumb trail you have created…
Chris thanks for the comment on Dry Fasting. I will read up on this. Could the solution be that simple??????????
Yannick Wolfe runs a online Dryfastingclub .He talks about Covid and Cfs.
Extended Dry Fasting is not that simple or easy. You have to consider that your body is enduring a prolonged stressful event (like a surgery) and that you will need time to recover after as your immune system rebuilds and resets. I think mindset probably plays a lot into it. If you go into it thinking this is the answer, then it could be. I have a friend of my sister n law who did this and I am trying to find out how she is doing 2 months later.
The Swedish doctor Carl-Gerhard Gottfries used a vaccine against staphylococcus (Staphypan Berna) for himself and some ME-patients. I think he started way back in the 1960’s. He never managed to make another trial because the the vaccine had a mercury as preservative and it was no longer allowed. He had no money to finance the conversion of the vaccine to a non-mercury variant. Below a few links about this.
https://me-pedia.org/wiki/Carl-Gerhard_Gottfries
https://pubmed.ncbi.nlm.nih.gov/12413434/
https://pubmed.ncbi.nlm.nih.gov/10700309/
https://www.socialmedicinsktidskrift.se/index.php/smt/article/view/1455/1258
To add to this
Carl-Gerhard Gottfries: A Swedish Chronic Fatigue Syndrome Vaccine Treatment Success Story
https://www.healthrising.org/blog/2015/11/21/gottfries-chronic-fatigue-syndrome-story/
In the video below Gottfries said vaccines were used as immune a sort of immune booster in order to prevent infection in the era before antibiotics. That was one of the reasons he tried vaccines. I seems like he tested many antibiotics during three years before he tried the staphylococcus vaccine that worked. He then had to re-vaccinate every month in order not to relapse in ME. So it seems like the effect was immunomodulatory rather than eradicating a pathogen.
Maybe Japanese Encephalitis Vaccine happens to have a similar effect as the staphylococcus vaccine. Interesting.
https://youtu.be/TCF_RYCnHW4
Sharing this in case it helps anyone researching this angle.
My daughter who has POTS with MCAS went into remission for 8 months after the JnJ COVID vaccine. She had a reaction starting 9 hours after the shot that included a racing heart, chills, and a fever of 102. 36 hours later the fever broke. She felt worse POTS symptoms for a few days and rested. For 8 months afterwards she felt wonderful. She was able to exercise as she liked, eat foods that used to cause a reaction (like yogurt, tomatoes, cheese), travel, and enjoy the outside. She is back into a miserable POTS/MCAS state now.
Well if it were me I would figure out how to get that vaccine again!
For me personally, my immune system has been so crotchety since I developed ME?CFS, after glandular fever 28 years ago, that I can’t even risk basic boosters such as Tetanus anymore. Any vaccine since then has sent me into a bad relapse. Because of this, I couldn’t risk the Covid vaccinations either. But as an interesting side note to this, my husband had three Covid vaccines prior to our first shared Covid infection and we both suffered the same severity of symptoms for the same length of time: him after three vaccines, me with none. That was interesting. I’ve also had it a second time since, but it was very mild in comparison. My immune system is very bizarre and although I don’t get flu, a cold always makes me suffer a lot for at least three weeks, although I can now cut that down if I use natural anti-viral supplements at the very first hint of a symptom and throughout the illness.
Not all vaccines are created equal- namely ones with trained immunity effects- notably BCG and from a theoretical standpoint potentially JEV
BCG is definitely very good ! I got my life back 🙂 Hope to have more time to write about it.
Where can we follow to hear more about your experience Adam?
I promissed to Cort to summarize my experience with bcg. I’ll try to do it soon.
Please do! I took the BCG vaccine myself. A bit too soon to say if it’s having the intended effects. But I am extremely curious to hear your story! I’d also love to ask you some questions, if you’re up for it. My email is smithsj@gmail.com.
I’ll get in touch with you, Stephen ! The intended effect comes slowly. I perceived first effects after 3 months.
I e-mailed you from my ICloud account. You will see a hidden e-mail address bc I did not want to use the e-mail address of my office and I do not have any other.
Adam
I summarized my experiences and sent it to Cort. Hopefully, it will be published here soon.
That’s wonderful, Adam! May I ask how you were able to get the BCG vaccine? I’m in the US and it looks like I’d need to find a TB specialist who was willing to give it to me.
You do not need a TB specialist. First, you need to file for an off-label permit (an immunologist shall do it for you). Once you possess the permit, you should contact a wholesaler trading with a BCG vaccine producer. The Danish brand is very expensive. You may want to contact more than one.
Note that BCG vaccine is not in normal sale. Thus doctors cannot just order it. In addition, producers do not sell it directly.
Thanks so much for the info! 🙏
Anne, just do not give it up. It took me almost a year to obtain BCG vaccine starting from the day when I got the off-label permit. Lots of circles and hurdles…. Many e-mails without any response, rejections, offer for help but at an elevated price, finally someone who was willing to help but was not paying enough attention to the issue.. Another 3-4 months because the wholesaler forgot about me…. Right now, I always order 30 vials in advance to secure the treatment for a year.
A note to the author and Cort, here are some publishings saying how trained immunity still resulted from inactivated vaccines
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7873984/#s3title
https://www.cell.com/cell-reports/pdfExtended/S2211-1247(21)01684-3
Thanks!
Wow, what a long journey! But well worth it, obviously. Thank you again for all the information.
Since I seem to have easy access to the Japanese Encephalitis Vaccine, I may try that one first. I’m in a crash now so am going to wait until I feel better to get it. I will update everyone here with my experience if I do end up getting it.
Rachel got Covid in Dec 2021. She had the various vaccines in April 2022, with the followup JEV vaccine a week later. Therefore, she was not sick with Long Covid for more than 5 months.
Most people who experience post-infection fatigue syndromes get better in the first year and most of those get better in the first 6 months. Recovery is the norm, not a miracle and not remarkable. That’s why most ME/CFS criteria require people to be sick for more than 6 months. Check out the Dubbo study for example.
I’m not completely ruling out vaccines helping some people get over Long Covid, (and I’m far from anti-vax), but we’ve probably seen as many people deteriorate after vaccines as improve. Pinning our hopes on the latest anecdote arising from whatever someone was doing when they recovered is often expensive and sometimes harmful. Instead, we should be demanding more funds for good quality research.
My opinion is that people who have had CFS forever become curmudgeons that shoot down anything positive and you won’t see an increase research by putting down someone’s positive experience that you yourself wish for. This article is jam packed with supporting evidence to the theory. Want to split hairs about how theres not enough data that this particular vaccine works? That’s an easy stance to take; however, right now based on the landscape we are forced into a position where we have to take calculated risks. Stories help us make those choices.
Anecdotally, I took a flu vaccine within about 6 months of the beginning of my Long Covid symptoms and it made things a whole lot worse. After that I was weary of getting any more vaccines of any sort. If there was a little more data on this subject it would be so helpful.
Agreed! It’s a crapshoot!
Looks like one can schedule the JEV vaccine online with Walgreens
I am so sorry you are suffering post vaccine and I hope you can recover soon. Not sure which covid vaccine you got but the mRNA ones are a novel technology that cause your own body to produce the spike protein, which is inflammatory. Some studies are now suggesting the spike protein circulates for much longer than originally promised.
“Generally speaking, the evidence suggests that live attenuated vaccines have a stronger protective effect than inactivated vaccines”*qouted from the article* I found this article from a google search, trying to understand how after the first dose of the typhoid vaccine (oral course of 4 pills over the a week) made me feel 1,000 % better! I was expecting to feel a little under the weather but I feel amazing. I can’t believe it and hopefully I have finally found a treatment. Oral Thyroid vaccine is a live attenuated bacteria that causes Thyroid Fever
I believe you meant to respond to Simon 😉 Also, I assume you meant Typhoid not thyroid?
Hello. Reading this 48 hrs after receiving my first dose of Shingrix. I won’t go into a whole recap of my post covid existence, except to say that two annual flu shots dramatically cleared different sets of protracted symptoms -GI microscopic colitis year one, 6-7 mos post-covid, and this fall it finally shut down what felt like meningeal irritation all summer (like water dancing on hot oil :/). Ever since covid, have basically woken up every day sensitive to light & sound, feeling like I’m perpetually hung over & living in a bell. I have new microvascular problems since covid, but appear to fall more in the netherworld of immune derangement -both under and over-responsive, which is aggravated now by having developed diabetes (pre-covid). Have never been right since contracting Mono at age 17, never testing as having persistent EB, but prone to relapses, and dancing on the edges of chronic fatigue.
It was because of the apparent mono-like breakthrough and burning sensation threatening shingles this past year that I prioritized getting my flu and shingles vaccines first before any covid updates.
The two flu shot responses have been a god-send. Covid vax mixed -neutral, possibly aggravating things last year. First two shots affected my mid-range hearing (which recovered some), aggravating pre-existing retinal degeneration I’ve had since my mod 30’s, & reactivated quiescent traumatic arthritis.
Not sure how Shingrix will affect me. Had shingles already at age 29 in grad school. Was not pleased with the breakthrough threat last year. If nothing else, my hope is the series shores my system up to prevent shingles & any attendant neuro complications. If it can give me a bump on the rest without contributing to immune overdrive, Amen. Will gladly accept any reclaimed neuro protection.
All we can do is tread carefully & thoughtfully with each vaccine. I am in no way anti-vax. But I’m not convinced the mRNA vaccine approach did not trigger damaging inflammation in my system, or my 19 yr old son’s. He suddenly lost color vision around the same time my mid-range hearing went south.
Be well & may relief find us all.
Thanks for letting us know. These are fascinating topics!
Thank you, Cort.
One thing I would like to pass on has been my ongoing success with and apparent need of olive leaf extract to tamp down the covid march 2022-present AM “hungover in a bell but I don’t drink” thing. (If only there was something to quit). I have no known current indications of sleep apnea. Ibuprofen and tylenol don’t seem to mitigate these symptoms.
Olive leaf extract has anti-viral, anti-bacterial and anti-fungal properties. It also has some impact on blood sugar and blood pressure, lowering both so there are details people should look into based on their particular needs and concerns.
Source/Brand: My preference has been either Gaia or Barlean’s capsules; both are available to me locally and have similarly high standardized concentrations of oleuropein that are working or me. When I’ve attempted to taper, use a different with a lower concentration (ie, Nature’s Way), or just plain run out, those neuro symptoms creep right back in within several days. Not all brands list oleuropein %, and the mg used to achieve that don’t match. There are variations in methods and which parts of the plant are used. Sorry, my research has been piecemeal over time and I don’t have a couple of clearly defined resources on hand. PubMed search is best – you’ll see some studies re uses for olive leaf extract with acute COVID, as well as stroke, TBI and Alzheimer’s. It has also been recommended as part of a naturopathic approach for treating Lyme Disease. Levels of evidence need a look.
I don’t have any clear sense of why olive leaf extract is working successfully to mitigate my particular symptoms; I’m sure it is much too simplistic to suggest they involve some viral reservoir. My docs are aware I am taking it and why. We haven’t gone down the rabbit hole with extensive labs.
Truth be told, taking it has always been trial & error and a rolling AB experience for me. I figured out years ago olive leaf extract helped manage summertime skin break outs when I couldn’t afford Oracea and doxycycline was in shortage. I knew it worked on that anti-bacterial front, I tolerated it, and when I got COVID, I figured it was worth seeing if it would shore up my antiviral response. It wasn’t until I tested negative for COVID and stopped taking it that I realized it made a difference with the morning sensory sensitivity. The persistent 23 months on/off and Sx resolution upon restarting have been my guide.
I noticed yesterday that Barlean’s assistance program offers wholesale pricing (40% discount) on all of their products for folks who meet their program criteria, including active and retired military, first responders, medical providers and children with particular conditions. If ok, will include that link here for your blog readers. I have no affiliation with Barlean’s other than purchasing their products to support my own health needs.
https://www.barleans.com/pages/assistance-programs
One PubMed example… https://pubmed.ncbi.nlm.nih.gov/29149822/
🙏
Oh hey, ahem
Review Cells
. 2023 Feb 22;12(5):688. doi: 10.3390/cells12050688.
Role of SARS-CoV-2 Spike-Protein-Induced Activation of Microglia and Mast Cells in the Pathogenesis of Neuro-COVID
Theoharis C Theoharides 1 2 , Duraisamy Kempuraj 1
Affiliations expand
PMID: 36899824 PMCID: PMC10001285 DOI: 10.3390/cells12050688
Free PMC article
Abstract
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) causes coronavirus disease 2019 (COVID-19). About 45% of COVID-19 patients experience several symptoms a few months after the initial infection and develop post-acute sequelae of SARS-CoV-2 (PASC), referred to as “Long-COVID,” characterized by persistent physical and mental fatigue. However, the exact pathogenetic mechanisms affecting the brain are still not well-understood. There is increasing evidence of neurovascular inflammation in the brain. However, the precise role of the neuroinflammatory response that contributes to the disease severity of COVID-19 and long COVID pathogenesis is not clearly understood. Here, we review the reports that the SARS-CoV-2 spike protein can cause blood-brain barrier (BBB) dysfunction and damage neurons either directly, or via activation of brain mast cells and microglia and the release of various neuroinflammatory molecules. Moreover, we provide recent evidence that the novel flavanol eriodictyol is particularly suited for development as an effective treatment alone or together with oleuropein and sulforaphane (ViralProtek®), all of which have potent anti-viral and anti-inflammatory actions.
Keywords: ACE2; brain; coronavirus; cytokines; inflammation; microglia; spike protein; toll-like receptors.
https://pubmed.ncbi.nlm.nih.gov/36899824/
Oleuropein also impacts gut dysbiosis. It seems to be enjoying its 15 minutes in the research sun across a number of areas from cancer and diabetes to neuroprotection.
Not seeing references right now on any front specifically linking it to MEES. It might be worth some highly informed cross-referencing and research queries.
The following quote is from an article about a study that was published one week ago, on May 22, 2024:
Over the full 34 months of the US COVID-19 pandemic, the BCG vaccine had a significant efficacy of 54.3%. The investigators also found that the BCG-treated participants had lower rates of viral, bacterial, and fungal infections as well as COVID-19 disease itself.
The BCG vaccine confers an immunity that likely lasts decades, a clear advantage to the COVID-19 vaccine and vaccines against other infectious diseases, such as influenza, where the duration of effectiveness is only two or three months.
“The BCG vaccine offers the prospect of near-lifelong protection against every variant of COVID-19, the flu, respiratory syncytial virus, and other infectious diseases,” said Faustman.
The full article:
https://medicalxpress.com/news/2024-05-century-vaccine-diabetics-infectious-diseases.html
The full text of the study:
https://www.cell.com/iscience/fulltext/S2589-0042(24)01103-9
Whoa! Thanks Keith 🙂
You’re welcome, Cort. Here are some other vaccine studies that might interest you. The oral poliovirus vaccine (OPV) is protective against severe Covid, and likely against many other infectious diseases. OPV, a live, attenuated vaccine, hasn’t been used in the US, Canada, or Western Europe since the early 2000s, but it is still used in much of the world.
This world map shows where OPV is available:
https://www.researchgate.net/figure/Countries-using-oral-poliovirus-vaccine-OPV-in-May-2016-following-the-global-switch_fig1_318662855
OPV confers polio immunity for at least 18 years, and perhaps for life. In this study, adults aged 18-80 were given an injection of inactivated poliovirus vaccine (IPV), the kind currently used in the US, Canada, and Western Europe. Adults who had previously received OPV had much stronger and longer-lasting protection against Covid after receiving IPV than adults who received IPV, but had never received OPV.
https://www.mdpi.com/2076-393X/12/3/219
Nearly two years ago, my colon health improved significantly after taking Vivotif (Ty21a), a live, attenuated oral vaccine for typhoid. I took Vivotif after reading this study:
https://www.researchgate.net/publication/26517190_Live_Typhoid_Vaccine_for_IBD-Patients-Well_Tolerated_and_with_Possible_Therapeutic_Effect
I took it in four doses, each dose spaced two days apart. By the time I took the last dose, my colon was better than it had been in over ten years. My colon has continued to function much better since then. I took a second round of Vivotif last fall, but there was no further improvement. I recently came across this study from Finland and Sweden, which found that people who received Vivotif and Typhim Vi intramuscular (the inactivated typhoid vaccine) concomitantly had a broader and more robust immune response than people who received only one of either vaccine.
https://www.sciencedirect.com/science/article/pii/S0264410X14015692?via%3Dihub
I’m planning to get vaccinated with Typhim Vi in the next few weeks.