(Dr. Baraniuk finds damage to a critical nerve pathway that connects regions of the brain involved in fatigue and pain production and autonomic nervous system regulation. The damage, which affects the integrity of the nerve axons, is unusual and suggests GWS and perhaps ME/CFS are not related to demyelinating disorders such as multiple sclerosis. His model suggests that the attention of people with GWS/ME/CFS gets pulled again and again away from the outside world and onto pain and other signals in the body, making it difficult for them to concentrate and carry out tasks).
The ME/CFS/FM Connection

Dr. Baraniuk believes a similar type of brain damage probably occurs in ME/CFS, Fibromyalgia and Gulf War Illness
As you read this blog on Baraniuk’s Gulf War Syndrome study bear in mind three things:
- Baraniuk felt his brain proteome findings of seven years ago (yes, seven) fit ME/CFS/FM/GWS patients
- all the participants in this study fit the criteria for chronic fatigue syndrome (ME/CFS) and 50% fit the criteria for fibromyalgia (FM)
- when I asked Dr. Baraniuk if ‘all roads lead to Rome’; ie if he thought GWI and ME/CFS and other disorders had similar brain issues his answer suggested he did. At one point in the paper he pointed out that similar brain structures are involved in chronic fatigue syndrome and GWI.
We won’t know until we know but it’s very possible these findings or something close to them will apply to people with chronic fatigue syndrome and fibromyalgia as well.
“Functional Neurobiology”: Looking for Fatigue and Pain in the Brain
Given that the fatigue and pain in Gulf War Syndrome tend to occur in parallel; ie., the worse the fatigue, the worse the pain that was present, Baraniuk looked for the roots of both. Noting that the orbitofrontal cortex and the prefrontal cortex both play a role in producing fatigue and pain states, Baraniuk zeroed on connecting fibers called the fronto-occipatal fasiculus (IFOF) that connect these two organs and the insula.
Think of the IFOF as a bundle of wires connecting the prefrontal cortex – the seat of decision-making center of the brain – to the insula – an autonomic nervous system regulator and the seat of the interoceptive process. Studies have shown that increased ‘connectivity’; i.e. increased activity between the prefrontal cortex and the insula plays a role in producing and maintaining chronic pain states.
The IFOF is composed of white matter, and in this study Baraniuk used diffusion tensor imaging (DTI) to see if this pathway was different in GWS patients vs healthy controls. The options were no change, a loss of white matter ‘integrity’, decreased axonal functioning (axons are the main nerve bundles), and/or demyelination and inflammation
Unusual Form of Nerve Damage Found – Demyelination Not Present
The study found option three – decreased functioning of the axons was present in the people with GWS and ME/CFS.
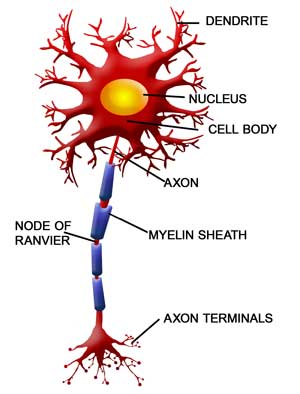
The axons which form the connection between the nerve cell body and its terminal projections appear to be weakened in a connecting circuit in the brain
This suggested that neither demyelination or neuroinflammation was occurring. Instead, something called increased axial diffusity, which refers to weakened nerve axons, was present and importantly, was associated with increased fatigue and pain; the weaker the IFOF axons were – the more pain and fatigue these patients were experiencing.
The images indicate that in GWS, these nerve bundles break down and may have trouble forming connections. This suggests that the brain circuitry, rather than any specific brain area, is disrupted in people with the condition. News Scientist
Again, these less robust axons have not been demyelinated; i.e. the myelin sheaths covering the nerves have not been attacked. Instead, they appear to be dysmyelinated, a process characterized by defective development and functioning.
“the changes appear distinct from multiple sclerosis, major depression, Alzheimer’s disease and other neurodegenerative diseases,” Rayhan, lead author of the study
The really intriguing thing is how rare this kind of nerve damage is. Baraniuk stated that hundred’s of studies have found increased demyelination but the increased axonal diffusity found in this study is rare.
Instead of being related to multiple sclerosis and other demyelinating disorders (acute disseminated encephalomyelitis, Neuromyelitis Optica, transverse myelitis, etc., GWI and perhaps ME/CFS/FM may be more related to such rare illnesses as the leukodystrophies (Pelizaeus–Merzbacher disease, Canavan disease, phenylketonuria).
According to one article low blood flows could play a role. Chronic states of low blood flow (ischemia), for instance, are associated with increased diffusity, an intriguing finding given that Baraniuk’s brain proteome study suggested brain circulatory problems play a role in ME/CFS/FM. Several studies have found reduced brain blood flows in ME/CFS, and Dr. Natelson’s study suggests that besides reduced brain blood flows, a significant number of people with ME/CFS may have increased lactate, cognitive issues, and small frontal lobe lesions.
- See: The Splitter: Researcher Asserts ‘Brain-damaged’ Subset Present in Chronic Fatigue Syndrome (ME/CFS)
While measures suggestive of demyelination were not significant we should note that a trend towards significance was present suggesting that a larger study could have shown demyelination as well. (Those measures were not correlated, however, with increased fatigue and pain.)
Broken Borders
Baraniuk isn’t interested in just displaying his results; he has a model of GWS/ME/CFS he wants to get out, and in that model the trouble starts at the top of the spinal cord, takes a turn at the prefrontal cortex, winds along the IFOF, and ends up in the insula and other related areas of the brain.
Baraniuk noted that the signals from the body entering the brain take a direct path from the dorsal horn of the spinal cord to the prefrontal cortex. That straight shot has implications; if the ‘gates’ of the dorsal horn are broken, it can slam the PFC so hard with stimuli that it will, in effect, short the PFC out leaving its pain matrix in a twitchy and over-sensitized state. This kind of out of control spinal cord-prefrontal cortex roadway has been shown to play a role in producing pain problems such as allodynia (sensitivity to touch).
Why Executives Don’t Have ME/CFS (and keep their jobs) – the Prefrontal Cortex Issue
The prefrontal cortex plays a key role in ‘executive functioning’. Having trouble planning or decision-making? How’s your attention span? Problem solving ability? Mental flexibility? Feel like you’ve lost a little mental flexibility? I sure have….
The prefrontal cortex provides a kind of ‘mental sketch pad’ we use to plan and organize our lives. Lose that mental sketch pad and you’re more or less at the whims of your environment.
Distracted Neurons: the Focus Problem in ME/CFS
“This tract of axons links cortical gray matter regions involved in fatigue, pain, emotional and reward processing. This bundle also supports activity in the ventral attention network, which searches for unexpected signals in the surrounding environment that may be inappropriately interpreted as causing pain or being dangerous. Altered function in this tract may explain the increased vigilance and distractibility observed in veterans.” lead author Rakib Rayhan
We’ve outlined problems with planning, short-term memory, etc. and there’s more. That ‘live wire’ the study indicated has taken a beating in GWS, the IFOF, also connects to a network (ventral attention network (VAN)) which is in charge of scouring our environment for unexpected threats. The study suggested that that network is on overdrive, and that spells more trouble for executive functioning and task completion.

Trouble keeping focus and tending to flit from one task to another has been a hallmark of my ME/CFS from the beginning. Consider that every time VAN switches on your attention to the task at hand is broken. In fact, increased VAN activity has been shown to be directly correlated to decreased goal focused activity (called DAN activity).
We saw this earlier with an Australian cognitive study which indicated people with ME/CFS are continuously dropping out of a task (losing focus) and then jumping back in. Think how much energy it takes to lose your way during a task and then have to scramble back in and refocus again and again and again.
The Pain of it All
“Pain and fatigue are perceptions, just like other sensory input, and Gulf War Illness could be due to extensive damage to the structures that facilitate them. Some of the veterans we studied feel pain when doing something as simple as putting on a shirt. Now we have something to tell them about why their lives have been so greatly affected.” Rayhan, lead author of study
Increased axial diffusity in the corticospinal tract suggested that the pathways descending into the spinal cord that reduce pain may be bollixed as well resulting in increased pain.
A Punishing Situation
No wonder the authors characterized the situation as ‘punishing’ .
During the onset of noxious stimuli these regions coordinate responses that provide a punishing teaching signal that leads to altered decision making based upon these painful cues…

Trying to focus with all the distractions these damaged neural networks may be producing can’t be easy..
The brain regions involved tell us in no uncertain fashion what to avoid and how to act. Could this damaged ‘wire’ be why every little move can sometimes seem fraught with danger or pain?
The scenario evoked doesn’t sound like fun at all; first, the dorsal horn of the spinal cord slams the prefrontal cortex with pain and sensory data weakening our ability to plan and carry out tasks. At the same time that’s happening the IFOF connection to the fatigue and pain centers is humming – further weakening our ability to focus.
With the brains alert system (VAN) on full-bore, attempts to focus on a task tend to be diverted back into monitoring the environment for something unexpected ( hyperarousal), or into the heightened pain sensations present.
This model – increased levels of pain, increased interoception and increased VAN activity – suggests the attention of people with GWS/ME/CFS gets pulled again and again away from the outside world and onto pain and other signals in the body.
Baraniuk sums the problem up in a typically understated manner….
Nociceptive stimuli can involuntarily capture attention and interfere with on-going behavior
The problem is that that ‘on-going behavior’ is what makes up most of our productive lives. he ability to plan and carry out tasks is an important part of being human. Having little or no ‘on-goingness’ could leave us at the whim of our distracted, beaten up neural networks.
If some sort of neurologically based distracting process is at the heart of ME/CFS/FM/GWI, etc., it would probably behoove us to become adept at harnessing and hopefully increasing what amount of focused attention we have. (One study suggests rates of ADHD are increased in ME/CFS and fibromyalgia.) I’ve always wondered how somebody like myself who was naturally drawn towards meditative type activities found them so difficult post ME/CFS.
It also begs the question how useful organizational or ‘anti-diversion’ tools may be in these disorders, and whether it’s possible to create new neural pathways that build up focus, create feelings of well-being (instead of pain), etc. We’re going to be looking this more in future. Johanne Starke’s blog on ways to create calm while using the internet is a first step in that direction…
When Time Heals Nothing – A Different Type of Subset Entirely
The problems in GWS may get worse, not better over time. In an interview Baraniuk said he’s found ‘three symptom areas’ (ie subsets) that correspond to what stage of the illness GWI vets are in, and that “The guys who were robust and leading the charge on this 10 years ago are now using canes.” That’s an amazing finding for an illness triggered by events that happened over 20 years ago. Time – the great healer – appears to have made things worse.
Baraniuk’s comments about chronologically based subsets is interesting given similar statements from Dr. Broderick who is finding distinct differences in young women with ME/CFS with recent onset and older women who’ve had the disorder longer.
Neglect Dogs Gulf War Illness Research
It’s not clear how many of this studies findings will apply to ME/CFS but one thing’s for sure – GWI patients have received the same, if not worse kind of neglect from the federal establishment that the ME/CFS community has endured. Six months ago Dr. Stephen Coughlin, an immunologist at the Veteran Affairs Office, resigned while accusing the VA of manipulating and hiding data and basically doing everything it could to ensure Gulf War Illness was not taken seriously. Coughlin asserted the VA did not want anything published that might prove GWI is a neurological condition.

Researchers working with the government have accused it of ignoring physiological findings and focusing on mental ones.
“If the studies produce results that do not support the [VA’s] unwritten policy, they do not release them… On the rare occasions when embarrassing study results are released, data are manipulated to make them unintelligible… Anything that supports the position that Gulf War illness is a neurological condition is unlikely to ever be published.” Dr. Stephen Coughlin
Baraniuk, as he has with ME/CFS, stepped right into the middle of the controversy, stating “If 30% of Congress got sick, or 30% of Manhattan got sick, there would have been an outcry”.
Most recently, Secretary of Veteran Affairs Shinseki’s gutting of the independent review board to research Gulf War Illness suggested the VA was trying to reverse the understanding that GWI was a physical illness. One advocate called the removal of the Chair and half the boards members ‘retaliation’ for Coughlin’s testimony.
The ME/CFS Connection
Major differences between GWI and ME/CFS do exist; in an interview the authors of the paper attributed the GWS findings to environmental factors such as exposure to Sarin gas, nerve agents, anti-nerve agent pills and the ‘industrial-strength’ bug spray the vets used copiously. It’s clear ME/CFS can be initiated or exacerbated by exposures to a variety of toxins including pesticides, formaldehyde, mold, etc., but most cases of ME/CFS appear to be triggered by infection and Dr. Klimas has found distinct differences in immune function between the two disorders.
It may be we’re seeing different variations of the same disorder showing up in ME/CFS, GWS, etc.; i.e. we see evidence of a chemotherapy/radiation induced ME/CFS-like state in cancer survivors; we have the nerve agent/pesticide/toxin induced ME/CFS-like state in GWS; the infection induced subset in ME/CFS, the trauma induced subset in fibromyalgia. Only time will tell whether these disorders show up with similar neurobiological findings.
Next Baraniuk wants to analyse similar scans of people with chronic fatigue syndrome or fibromyalgia….
- Coming Up Shortly – Baraniuk’s exercise studies indicate GWS and ME/CFS brains have similar metabolic dysfunction…







Very confusing. I have much of what is written in this article. I do also have a lot of white matter also. this does not seem to fit his model or does it? Does this researcher mention the major immune system abnormalities any place in his studies? What is causing all these issues and what is his ideas about the potential cures?
I don’t if the white matter abnormalities on MRI’s are similar in origin. That would be a good question to ask him.. Baraniuk has been focusing on the brain and really doesn’t say much about the immune system, I’m afraid.
Cause? That’s a great question. I think we’ll hear more about that in his upcoming brain proteome studies and in the lactate study I’ll get to shortly.
Yes, this is a very difficult study. I probably burned out a few neurons trying to make heads or tails of it. I hope I got it right….
Yes, difficult, but I like it. I like it a lot even in it’s fledgling unfinished form. And I confess that I usually flee articles about the brain’s involvement in ME/CFIDS, terrified of the absurd and trivializing approach to ME/CFIDS as being perhaps a psychological illness. ( I am NOT imagining. this.)
I probably like it, lol, cuz it is NEW. ‘New’ is at least entertaining.
Yes, its very different. I think you’ll like the next one as well which finds high brain lactate levels after exercise in some GWS patients and connects them with cognitive problems and Dr. Baraniuks assertion that this proves GWS(ME/CFS) has a physiological basis and is not a psychological disorder.
Excellent, exciting…Ummm…wait…I am sure I have some more adjectives here somewhere, lol. But I think they were swallowed by my high brain lactate levels after I walked around the house today. YES!!! I love thisss. Long ago I quit caring about a cure as much as I care about validation, about legitimacy, and about respect from doctors, the establishment. A bit pitiful, I suppose, but I am just angry, like a child: I don’t care if it kills me anymore. I just want my tormenters to pay, lol. Eat humble pie.
Deb, it’s funny, well, not in the HAHA sense, but I am right there with you. I gave ages ago even really caring about a cure as much as I care about validation and respect from drs and others. You said it well. Nobody who doesn’t have this disease could ever really understand us when we say this. The stigma of CFS reaches so far into our psyche (Cort, help me out here, please, spelling????) that we are truly damaged here as well from the abuse we have endured for so long.
Cort, is Baranuik’s findings part of the study that you and I (and my son) were both involved in at Georgetown U?
I don’t know how you interpret all these research articles, but I sure do thank you. I printed this one out so I can sit here at my desk and try to understand it and underline what seems to be really important and interesting.
Jeanie
This one was really difficult. I guess all of Baraniuk’s are actually..He’s a deep one 🙂
Believe it or not, this was not part of that study we were involved in quite a few years ago now. Those study results have still not been published. Baraniuk did provide something of an overview of them a year and a half ago at the Ottawa Conference but nothing since then…
We’ll be looking for protein findings in the cerebral spinal fluid, some autonomic nervous system testing and I can’t remember what else. I do remember we were there for quite awhile…..:)
Hi Deb,
I can relate totally with your sentiments I also have given up looking for a cure but it is the need for validation that keeps me motivated. I like many other women with ME/CFS/FMS also have a diagnosis of severe Endometriosis and mind you things are just as bad in that field with patients having to run the gauntlet of unsympathetic medics and unsupportive general public.
My wife and I just BOTH got stigmatized in our medical records with accusations of being nuts – we both have FMS/CFS with strong chemical sensitivity. Both of us have been diagnosed with FMS/’CFS and with MCS (by a diagnostician with over 37 years as the head of a hospital department in diagnostics) & that was her SECOND independent diagnosis of MCS).
Back in 1997 (dying from pain induced anorexia and unwilling to take narcotics) she was told in an Oregon pain clinic that she would need pain management for the rest of her days in order to “just” survive. Since then we also found out she has Elhers Danlos Syndrome (classic type 2) as well. I was “head hunteded” for my I.T. skills when she was fully medically stable again, running her own business and taking care of our daughter.
Now both of us hate narcotics. Neither of us were willing to take them until we had to take care of our daughter as a first priority and pain made that impossible. I also had to care for my wife, especially when she was being medically abused 0- and that destroyed my own health (2 hours sleep a day does that after 3 years).
I had an artey blow from a gallbladder the size of a football and did NOT go to the hospital (I dealt with the pain myself).
Note :my wife gave birth in 97 (with a 3 layer muscle tear on no medication for pain) & has had dental surgery & other minor surgeries – regularly – with NO local because “procaine” was all the government clinics will use, and she has a bad reaction to it and it does nothing to decrease her pain. She is not a pain wimp or “drug seeking” (as all her previous docs would attest to). She also likely has a strange cytochrome P450 variant (and nobody will test her) and has lots of strange drug reactions and lack of reactions. NSAIDS do nothing but hurt her stomach & she needs massive doses of anesthesia for surgery (when she was 9 she required the same amount of “general” as her 300 pound blacksmith step father did & he was noted as strongly resistant to pain meds and anesthesia).
SO BACK TO NOW.
A few months ago the government oversight people (for Drugs of Dependence) sent us on a MANDATORY visit to yet another pain specialist (all the others said we needed what we were on, and perhaps more but would not take any more – many of them)…
Right now pain docs are under massive pressure (or they lose the right to prescribe0 to take everyone off of narcotics no matter what. It is causing many suicides. You see about 6 or 8 years back the people who had been in charge of the addiction services/methadone clinics were put in charge of the DDU & the docs got the boot. Here in South Australia where there is an active war on pain patients.
So we both have it in our government records now that we are crazy, not in need of pain medication, and must go off of everything we are on.
Now I carried my wife into the hospital (literally) for pain management in 1997 back when I was still a very healthy weight lifter with large muscles who could press 750lbs with one leg easily. She was under 95lbs at 5’8″ tall and dying from pain induced anorexia. She got 2 years of medication before our move to Australia (I was headhunted and she was medically very stable). But in 99 her meds went away. One doctor (who has a reputation in the pain patient world now for killing people) was all it took.
Then by June of 99 she was back down under 95lbs with constant pain induced vomiting (which no anti-nausea medication could stop) and dying again. By late 99 a panicked GP (who had her case dumped on him by that idiot pain doc) had sent her to another pain doc who gave her small amounts of medication. Her new pain doc told me when I asked why not just give her more if she needs it, “Of all people you should know that life is not fair” & regularly ranted about how his hands were tied. This was BEFORE the DDU was taken over by the anti-drug squad who see addicts in everyone.
Due to the real viscous cycles involved in this disease (see Dr Pall & NO/peroxynitrite ) every time she had her meds taken away thr impact made her condition far worse, raising her pain level massively and requiring far more to help her on the next pass. We have no other docs we can see (who are not scared still of the DDU) and we are far too ill to flee to another state (as many people have done).
We have so much validation of our conditions. BUT the Pain doctors here in SA are under huge legislative and bureaucratic pressure right now, to take everyone off of all pain medications that are in the least narcotic looking. They are all also STUCK in about 1988 when it comes to FMS, and will only look at information that claims that pain meds do not help with with FMS.
However – if were simply heroin junkies we could have all the drugs we want. We could even get all the free methadone we like and all the “free clean needles” we wanted. But we are not, and so we are punished for being sick.
Any sane person would have sent us on our way with statements that “they are sorry our lives are so crappy” and left us alone with our meds. After all we were also GETTING BETTER (due to Dr LPall) and removing our own narcotic pain meds as soon as we could (we prefer a bit of pain & some terrible days, to being even slightly spacy). My wife had reduced hers by 1/3 on her own. So had I.
And what was the final straw that got us as FMS patients stuck with the label of “crazy” (with over 30 years of shrinks telling docs that FMS is physical not mental)…. that straw was – we took action on our OWN LIVES and made change in our lives to make things better. We took the advice of our diagnostician and went onto alternative COX inhibitors like turmeric to reduce our dependence on narcotics, and went onto the (world acclaimed) protocol of Dr Pall. Due to chemical sensitivity we moved out to the country where we are rather isolated, but are also in a whole lot less pain and are no longer having very real anaphylactic reactions every month (and for us hospitals are more risky that the bad reactions – they make them worse). And my wifes sezure reactions from chemical exposures (you cannot fake *THAT*) is no longer as pronounced either.
But the new doc says that we need shrinks, not main meds. We are to be taken off of all pain meds over time (forcibly if needed). You know – the medication that kept her from starving to death in 97, and 99 and again in 2003 when she was taken off them.
The fact that we have taught ourselves how to survive and how to manage a difficult situation, and know a lot about it, was taken as a point against us. We are apparently “obsessed” and are to be treated for depression with MEDICATION without a real diagnosis of it by a shrink(from the many shrinks who have seen us both, and who cleared us for pain medication)
learend so much about this from read medical articles (PUBMED is out friend) and that we have changed our lifestyles to not be in as much pain,. counted AGAINST us.|
|
The fact that we have taught ourselves how to survive & how to manage a difficult situation, and that we have learned far more about it than most physicians know, was taken as a point against us. We are apparently “obsessed” for doing the equivalent of not eating shrimp with a seafood allergy, or watching our diet with diabetes.
The new doc says that we need shrinks, not main meds. We are to be taken off of all pain meds over time (forcibly if needed). You know – the medication that kept her from starving to death in 97, 99 again in 2003 when she was taken off them.
What a story, Chemical refugee…Thanks for sharing.
The same war on pain relieving opiates is occurring in the US. It sounds like it’s world-wide. How effective is your alternative approach to pain? How well is it working?
I look forward to the next one about high lactate levels in the brain.
I do too!!!
It’s up!
Brain Drain Explained? Study Suggests Energy Problems May be at the Core of the Cognitive Dysfunction in ME/CFS/GW
Too tired to think straight? A recent study suggests a key energy producing process that provides the fuel for complex thought may not only be broken in people with GWS/ME/CFS but, get this, may be at its worst after exercise.
Check out the study that may explain the post-exertional brain drain in
http://www.cortjohnson.org/blog/2013/07/01/your-brain-without-energy-broken-brain-energy-loop-wipes-out-cognitive-functioning-gws-me-cfs/
Maybe you mentioned it and i missed it but how did he rule out neuroinflammation?
I can see why demyelination why discounted (as previous studies have shown in ME/CFS) but I wonder what the rationale was for ruling out inflammation?
It was the fact that one kind of ‘diffusity’ was not significantly increased in ME/CFS relative to controls but looking more closely the diffusity that was not shown is associated with a certain type of inflammation – here’s the sentence from the paper
“RD has been associated with demyelination, neuroinflammation with edema or macrophage infiltration[30]–[32]. This suggests that neurinflammation without edema has not been ruled out.
Plus there was a trend towards significance in that measure so it could be that a larger study would find that it was ‘significant’. However, AD (axial diffusity) was associated with all sorts of pain and symptom severity scores..
In the next study, interesting enough, glutamate is going to show up. It’s all very complicated…
Thanks Cort
Look forward to the next one.
So GWI gets worse with time. What about ME/CFS? There seems to be many opinions on this. Everything from “it gets better with time” to “it progresses with time”. I’ve heard David Bell and Nancy Klimas say that ME/CFS can be sent into remission and go away with time. Hopefully they are right!
Absolutely Thomas, my ME/CFS has certainly gotten much better in some ways and I think the studies indicate that most people do get better or ‘adjust better’ over time…so that they’re not so burdened. Of course, some people just get well.
That’s always refreshing to hear, Cort. I’ve been ill for 19 months (which I know is nothing compared to a lot of people) and it seems like year 2 has been more difficult that year 1 in some ways (in some ways not). But I hear that recovery (if it happens) is a bumpy road with many ups and downs. Oy vey.
Hey, Thomas – the first part was the worst for me…Oh ya…There was nothing compared to those first couple of years. Take care of yourself; don’t push too hard, don’t pull back too much :)…and I think a) you’ll adjust and stop doing things that don’t work and once you do that your body will start to heal itself a bit.
Your mind will hopefully stop crazy about what’s going on as well…which can only help…
There are all sorts of trajectories but I think in the main…most people certainly improve over time…
Recovery does happen…I have many recovery stories – so sure it happens – just not as often as we’d wish…:)
Probably ill for 14 years but collapsed just 18 months ago. Feared no recovery after such a long slide down but did Gupta and some Klimas/David Smith/Bruce Campbell style pacing techniques, very severe, very curtailing, and haven’t really dipped much since.
We’ll see when the winter comes but Nancy Klimas may be onto something big with her and Connie Sol’s anaerobic threshold heart monitoring. Anyway I’m older, pushing sixty but very optimistic about recovery or great improvement. Wanted to add a small note of cheer. The other day I felt well for a brief time!
It would be hard to overstate how seriously I have had to change my nature and my impulses. I even changed my name slightly to mark the divide between the old and new me. And the trend continues. I am having to heal very deep things. I thought I could rest on my accomplishments, in theory the neurological changes are permanent after practicing six months, but this weekend my relationship with my sister presented another huge shift in my belief and approach and really it is I who am doing all of the changing.
To be well I must change, change, change. It’s hard. The point being to heal the old wounds so there is less in the mind eliciting the dysfunctional danger alerts. There is no hard line between mind and body.
An odd aside to this very interesting report perhaps, but I noticed there was no recommendation for healing this neurological anomaly. And since I am a picture post card for some of the symptoms I thought I’d throw this in to balance out the discussion to include something practical and cast my vote on the “recovery is possible” side.
I agree that it’s helpful to heal wounds so there is less in the mind eliciting dysfunctional alerts. Well said – not easy to do- but well said.
PARASITE!!! C. pulmoni aka Klapowi worm aks hidden lung worm
This is my first visit to this site so maybe this has already been addressed. Dr Larry Klapow introduced this parasite/worm in the mid 90’s and has a patent on it.
in 2011 bulletin to International Association of ME/CFS, page 176, he re-introduces the parasite/worm as a cause of ME/CFS.
Dr Klinghardt, in conversation with Dr Mercola, states that approx 80 percent of people with ME/CFS actually have this parasite.
Story is this parasite jumped from animal to human in Viet Nam when we bombed the hell out of that country. They came back to US with returning vets.
They are not contagious. They get around via food & drink. The larvae can remain in shield for up to three months before coming out.
I HAVE THIS PARASITE. I am being treated with ultraviolet light blood treatment and vit c IV. The first year + the dead worms were exiting my skin in the respiratory area, plus protein foam in urine.
The last couple of months I believe the biofilm has broken up and is not the shield it once was. The parasites are now dying more directly. They emit an enzyme (maybe toxin as well) when they die, attempting to kill the host while the host is trying to kill them. That is what I am now experiencing. My toxins level is very high. I take an rx that is supposed to clear out this toxin. It is a slow go. I also take milk thistle to clear out my kidneys. Also a slow go.
Normal labs & medicos look for parasites in urine and feces. This is not – is not – where these parasites live. They are in the respiratory area and there is no test that I know to find them. However, they did show themselves in death – coming through my skin. They are the size of a small grain of sand. I picked them up with Scotch tape.
The stage now is that they exit anus and cause itching. Also cause itching in nose, eyes, mouth area so host scratches butt, then nose, etc., and they enter body that way and go on to the respiratory area. This info is on the internet.
Barbara Lochner
Regarding axon diffusity.
Just read this on wiki about inosine, which many already take as an immune treatment.
‘It has been shown that inosine has neuroprotective properties. It has been proposed for spinal cord injury;[2] because it improves axonal rewiring, and for administration after stroke, because observation has shown that axonal re-wiring is encouraged.[3]’ Wiki- Inosine
Just an observation. I have no idea if it would be of benefit in the above model of GWI.
Cort,
Once again Thank you for another superb article. The Pain of it all fits with my illness perfectly. It is one thing to manage and accept this terrible disease, it is ten times as hard to do it in addition to chronic pain! Keep these great articles coming.
Thanks Michael 🙂 Good luck with everything.
This is a stunning finding Cort – must read through – me suspected with myelin sheath damage and brother (a Neurologist) with nerve damage – sadly as he is advised certain do not recover in the brain. So what tips at our age (70s) – surely must be viral.
Sorry to hear that, I know somebody else with myelin damage; however, her doctor has advised her that if it is viral or due to inflammation then it may be able to be reversed..Hopefully that’s true.
I rest my case with this research.