



How Do I Know What’s Wrong, When I Always Have CFS?
The recent headaches started about two weeks before the stomach pain. My head seemed filled with cat litter. A woozy scratchy aching, either all over at once or in selected locations, on top, in back, in front. A bit of blurry vision.
One day the headache would be light, the next more severe. I felt a heaviness around my nose. Did I have sinus issues?
I tried Advil. No help. Alleve, but the headache persisted. Tylenol and then just aspirin, and still the pain refused to respond. Sudafed did nothing. In the drugstore, I found the big guns: MUCINEX SINUS MAX — no help.
Fifteen years ago with the onset of ME/CFS, I suffered with awful headaches that lasted months, maybe even years, as part of the spectrum of symptoms that led to the diagnosis. Back then, too, nothing helped – not medication (OTC products as well as Neurontin), not acupuncture or acupressure, not copper bracelets, not headbands, not aromatherapy or massage (honestly, I tried them all) and my depression and anxiety increased as I came to believe that headache was my default condition. In that early time, some generalized nausea accompanied the head pain.
Before ME/CFS, I’d rarely had headaches, except for one siege when I was a teenager and ran home from high school every lunch time for a week with head pain so severe I could barely see. My parents took me to a doctor who drained my sinuses with a procedure that felt like he was sucking my brains out through my nose. When that didn’t work, my mother decided I needed an enema. Guess what. No more headaches. Really. Never, until forty years later and ME/CFS.
After about ten more-or-less headache free years (I cannot remember when or why the pain stopped; probably just time reduced the severity of all my symptoms as I settled into patterns of generalized malaise accompanied by painful crashes after too much exertion), am I returning to Square One?
Two weeks after the headache onset, as I ate lunch on my porch on a beautiful Saturday, the nausea arrived. Not the run-to-puke kind, but an extreme queasiness, something like what I’d endured during the first three months of pregnancy. Suddenly my favorite combination of yogurt, blueberries, walnuts and flaxseed turned loathsome, and for the rest of the day I felt so lousy that I crawled into bed. For dinner I had tea and toast.
I woke up around 2 AM with intermittent stomach cramping in my lower abdomen for the rest of the night. Ouch and ouch and ouch until I pulled myself out of bed in the morning. Sunday brought a return of the queasy feeling but no more pain. I just didn’t feel well enough for our 51st anniversary dinner, so we canceled our reservation. (Canceling plans — routine for ME/CFS people.)
Did I have a stomach virus? Was there a connection between the stomach and head pain? Here we go again, I thought. Living with ME/CFS brings a continual struggle to FIGURE THINGS OUT. To monitor body sensations, governed usually by the ebb and flow of ME, which become familiar enough to understand and weather, except when they become unfamiliar and then uncertainty and, with me, apparently, anxiety make their grand entrances.

The questions really started to flow. Was it ME/CFS? Something else? The osteoporosis drug? A supplement? Something I ate? Lyme Disease?…WHAT is going on????
Are the worst moments of my disease returning? If so, why? Have I started any new supplements? Yes. Strontium Citrate for my osteoporosis. Could headache and/or stomach pain be a side effect? Is my ME/CFS worsening with increasing age? Am I suffering a return of Candida? Could I have Celiac Disease, even though earlier tests ruled that out? My husband was just diagnosed with Lyme Disease caused by a tick bite on one of his weekly hikes. Did the culprit tick jump off his back one night while we slept and crawl over to attack me? (Yes, sounds absurd. . .but. . .whoever knows??)
Sunday night I fell asleep around 10:30. At 12:30 AM, the stomach pain returned, this time above my navel. Strong spasms with accompanying nausea about every 15 seconds. I found a heating pad which provided some relief, and I fell back to sleep, but I awoke again at 2 AM with pain and nausea that kept intensifying until I was convinced I couldn’t make it through the night. After an hour of wicked pain and indecision, I poked my husband.
“Steve? Steve? I think we have to go to the emergency ward.” God, I was such a coward. As soon as he woke up, I wished I had waited until morning. He insisted on the ER (“I’m up now. . .”) and when the next contraction left me cringing, I slipped into my jeans and we left to drive through the dark and empty streets. I just wanted a few pills to stop the pain.
The triage nurse at Robert Wood Johnson Hospital took me immediately to an emergency room bed, where nurses and doctors questioned and examined me, then went off duty, and so other doctors and nurses questioned and examined me. All asked if I had any other medical conditions, and when I said, “Chronic Fatigue Syndrome” (convinced they had never heard of Myalgic Encephalomyelitis), all gave me the same blank stares. . .and never asked me one question about it.
All the while, poor Steve sat in a little chair by my bed, his head falling onto his chest as he kept lapsing into sleep.
Gradually the stomach pains diminished, but ER protocol required I have a CAT scan, an EKG and blood work. The scan and blood tests revealed no abnormalities, but the ER doctor saw something in my EKG and wanted to admit me overnight for observation. “In women,” he said, “very often stomach pain indicates cardiac problems.” He looked at Steve. “If she were my wife, I wouldn’t let her go home.”
“You should stay,” Steve said. I guess I would have reacted similarly if he were the one lying in the hospital bed.
Shit. I just wanted a few pills. What have I gotten into?!
Steve left to get some sleep, and to bring me stuff from home later.
I tried to pass the hours until my transfer to a room (was this really going to happen?) by reading my book in spite of the continuing headache. There’s no way I could rest with all the noisy flutter of the ER. . .not to mention the groans and sporadic screams. And the loud drunken snores of the patient next to me. But I couldn’t focus on the words because of those invading fears of more severe ME/CFS symptoms.
Of course, I’d read about the awful gut issues of so many ME/CFS patients, which I’d thankfully avoided all these years. Was I now developing the IBS I’d read was linked to ME/CFS? I really didn’t believe I was having a heart attack. In fact, a part of me would rather face that than an increase in ME/CFS symptoms.
Suddenly, like ministering angels, three women in white coats appeared at my side. One looked familiar. “Oh, I’ve seen you in Dr. Hamm’s office, haven’t I?” I asked. Dr. Hamm is my internist, whose family medicine practice is associated with Robert Wood Johnson Hospital.
“That’s right,” she said. “I’m a nurse practitioner and this is Dr. Lin. We’re associates of Dr. Hamm. We’re making rounds and were notified that you’re here. Do you mind if we examine you?” The ANP explained that the third woman was an Austrian doctor there to follow the other two around to better understand American medicine. Okay. Whatever. So there were three sets of eyes.
The doctor and the ANP took over, examining me, my medical records (available through the RWJ computerized systems) and the recent test results. The third doctor watched.
About a half hour later, they filed back beside my bed. “You can go home,” said Dr. Lin. “We don’t see anything unusual on your EKG.”
“Huh?”
“We compared it to older ones, and it seems fine. The CAT scan showed excessive stool in your intestines, and that might be causing your pain. Have you been constipated?”
“Well, yes, but . . .” Constipation? I’d just submitted to the massive radiation of a CAT scan because of constipation?
Dr. Lin, an expert in Chinese medicine, provided instruction on acupressure for sinus and constipation problems. She also recommended a stool softener and laxative. I thought of my mother and her enema bag. Good grief.
Well, okay. So Steve returned and drove me home after nine hours in the ER. Hooray! No overnight stay. No heart issues. Thank you, doctors. Thank you too, Austrian stalker.
For a week until my actual appointment with Dr. Hamm, I tried the acupressure points for my headache, which responded by getting worse. I took the Colace and Miralax and my cramps and nausea persisted but in a milder form. And various explanations continued to ricochet in my brain. After 15 years, you’d think I’d be better able to ‘let it be.’
I am lucky that Dr. Hamm is empathetic and willing to help. Though not an ME/CFS expert, she listens carefully, asks good questions, and knows my history. “I’m convinced you had a virus that started with the headaches,” she explained. “Your immune system is so weak and overstressed that you couldn’t fight it, and it traveled to your stomach, probably causing the constipation and pain.” She told me to increase the Miralax to twice a day and try a Fleet enema. I left with a prescription for an antibiotic just in case I actually had a sinus infection and didn’t feel better in a week.
Well, the intestinal spasms are gone, but I’m left with constant bloating, some intermittent nausea, and vague cramps. What’s strange is that I still have my appetite, though I feel full very quickly. The headaches sort of come and go, but the intensity has dissipated. I’ve rejected the antibiotic, but have added zinc and L-Glutamine, recommended by Dr. Hamm. And I’ve returned to my normal abnormal modified life, which includes napping each day after lunch, seriously pacing my activities, drinking oceans of water and weathering unpredictable crashes.
Not a real resolution, but I’m not ready to enter another maze of more doctor hunting and testing, so for a while, I will let it be.
I do vow, however, to avoid the ER.




 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!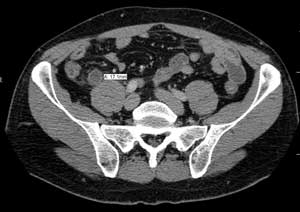





Sounds like you also have SIBO, which is a stomach condition confused IBS and usually goes along with CFS/ME/Fibro.
I deal with all the same issues you are dealing with. Unfortunately ME is a progressive disease and just continues to hit new sections of the body as time goes on. As a person with CFIDS for 32 years I can attest to this.
Sheila
Hi Carol,
Thanks for the write up.. I have had a similar thing occur without easily found explanations from a Western medical perspective. I think their diagnostic methods are sometimes unfortunately not subtle enough for our complicated systems! I have been working with an intuitive homeopath recently, who also utilizes an ETA scan method which functions via vibrational frequencies.. pretty quantum stuff! And very effective, at least in my own case. In the past, I have been severely ill to the point of requiring assistance to do pretty much everything, and have managed to recover a fair amount of function through Kundalini Yoga and figuring our how to eat. But earlier this year, I had a recurrence of symptoms, including severe muscle weakness and bone-dragging fatigue, along with a similar slew of symptoms that you mentioned. I contacted the homeopath and he ran a scan and found the resonance of a bacterial infection. He let me know that toxicity was also playing a role (and chronic constipation can really contribute to this, given how many of us are living quite sedentary lifestyles without adequate lymph flow, the natural organ “massage” action of walking, etc). Apparently, bacteria and other microbes of a certain frequency are drawn to the frequencies of certain toxins, and one can treat the often hard to treat bugs indirectly with simple, easily affordable remedies to allow the body to detoxify, which restores a naturally less hospitable frequency wherein one’s immune system is able to function as designed, and the bugs can’t thrive.
What was prescribed, and effectively did the trick for me in this case was simply organic Alfalfa tincture and liquid Choryphyll, 10 drops in water, 3 times a day. It worked very quickly, in a matter of a couple of days. You can find them in any health food store.. it may be worth a try for further improvement. If you are interested in ETA scanning, let me know I can help you get in touch with the practitioner I work with. Those who are severely ill (bedridden) may need an even gentler approach than chlorophyll and alfalfa, or perhaps a very titrated amount, because of how the detox reaction that may occur for them could impact their already severely compromised system.
Another strong point this practitioner made is for people with ME/CFS or any other serious illness should limit their time around computers and other electronic devices that emit EMF. he said this is extremely toxic to the body and for people with these kinds of challenges, it makes things a lot worse, so keep that in mind as well… This is hard for those of us who are tired and have a harder time getting out into the world as often.. I know have tended to use my computer more to compensate for the lack of ability to get out and about as much as I’d like.. I’m working on reducing this however.
Best of luck to you in your continued healing! I hope you are already feeling loads better.
All the best, Giselle
Thanks for your comments, Giselle. You’re right about how much we depend on our computers for information, connection and even entertainment, and how difficult it is to cut down significantly on technology, which is all around us. Also about the role of detoxing, and how we have to be careful not to over-stress our bodies with excessive die-off.
I will look into the alfalfa and chlorophyl supplements.
Also, with the excessive stool in your intestinal tract, I wonder if you might have some hypermobility issues as well. If not, then never mind. But, if you were called double jointed as a kid, or able to interesting things that most others could not (ie able to put your legs behind your neck, bending your thumb to your wrist) then Ehlers-Danlos type 3 might be something to look into. It causes us to be very bendy and is collagen related. I have to be very careful not to become constipated because my digestive system/intestinal tract will expand and stretch easily to accommodate extra food, or hold extra in my intestinal tract. (yah, I know, weird, but so is CFS which is something that also comes with EDS3)
I’ve been curious for a long time about the Ehlers-Dalos connection to ME. I’m pretty agile and flexible, but not excessively so. Interesting connection to intestinal troubles.
My first thought was SIBO as well. A very easy breath test to see. After yrs of baffling fatigue, inflammation and pain, I was diagnosed with SIBO and am now convinced it’s the root of these debilitating ailments for me. As I continue to eradicate the SIBO and get my bacterial counts down, my fatigue, inflammation, cognitive function and stamina increases. Might not be Sibo for you, but a relatively easy, inexpensive test will let you know. Best wishes.
Jennifer,
I’m glad to hear that treatment has helped improve your condition. As I said to Sheila, I’m going to investigate SIBO. Thanks for the response.
Carol
Thanks, Sheila. That sounds very possible. I will talk to my doctor about treating SIBO, maybe starting Xifaxan.
Carol, thank you, as always, for sharing your experience. Always relate and am grateful to be in such good company, tho sorry you deal with all of this, too. Love your writing. Best of best wishes for feeling better soon.
Thanks for your good wishes, Tee. And thanks, also, for reading.
Carol, did you ever get a liver ultra sound??
SIBO is a possibility even if only and partial one.
I will email directly to Cort the “Route to Resolution” for SIBO
which is a protocol for resolving it. I cannot attach it to this message.
It involves and three part approach. SIBO stands for Small Intestine Bacterial Overgrowth. It occurs when the normal bacteria from one part of the gut ‘escape’ into the small intestine.
It is a three part protocol involving 1. clean out 2. re-seeding 3. feeding the good guys.
ie the usual weeding, seeding, growing process. It is very low risk and will NOT make you worse.
Okay, I’ll contact Cort. Thanks, Phillida.
Could you send me the SIBO information also, I hate to be a pain but I think I have issues that wouldn’t hurt to try the clean out , thank you! LOVE reading your stories Carol. It makes me feel like I’m not alone in this world. Sissy
I’m sending you a copy, Sissie.
Please could you email me this too please, valeriepollard48@hotmail.com Thankyou
I’m sending it to you Val 🙂
Hi the eating and feeling full thing together with the nausea and stomach cramps make me think of one of the early stages of my gallstones – I have severe m.e. which i’ve had for 29 years so i know pain and many types it are common with the illness – however this was different but it took me about a year to realise and cancel out m.e. before going to my doctor – all the while the symptoms changed every few weeks – the feeling full quickly – became an empty – always hungry pain that only went away if i ate something but within an hour came back.. after a few weeks within half an hour – and so it went on changing – until it reversed and i got horrendous pain when i ate something .. for 10 months i went through this just eating once a day cos the pain was so bad and nothing except anadin xtra could give relief – i had scans but the gallstones didn’t show up and get this the doctors believed it was just my M.E. – a first – them actually recognising the illness but i knew it wasn’t .. finally when after 10 months and the only thing that was easing the pain was apple juice and cider vinegar – i had a third scan and as they were going to stop – they saw the gallstones previously hidden.. not surprisingly with me .. anyway i’m just telling you this just incase the feeling full thing etc could be gallstones. even the headaches could be part of this as i was also rushed into a an e after a sudden massive pain in my head that just got worse and worse and had me screaming – i have had migraines all my life and this was 100 times worse however in the ambulance i was sick and the pain went…
What awful experiences you’ve had with both gallstones and migraines! I hope things have improved for you. Strange, how you can have such severe symptoms and yet scans show nothing. At least that third scan revealed the cause.
Phillida Bunkle – How can I access ‘Route To Resolution’ for SIBO?
Thanks,
Linda Gray
Speaking of gut problems, a Coursera course on the Microbiome starts on the 6th.
https://www.coursera.org/course/microbiome
I have had four really wierd trips to the ER since I have has this illness and I won’t go
Into them here, but needless to say, none of them helped and a couple of times they made me much sicker than I already was. Once I just walked out after 12 hours of being there
and completely forgotten. It is really scary to even go there. I have had gut problems and headaches from the beginning among many other of the usual strange and confusing symptoms so I sure can see where you are coming from! Just wanted to say hang in there
and I hope you will feel much better soon as I hope we all will someday. Thanks for sharing your experience with the rest of us.
Thanks for your good wishes. Sorry you had such bad experiences in the ER. It’s scary too because you always hear about the infections people pick up in hospitals.
Yes!!!!!
ME/headaches/constipation….all made supremely worse by hormone changes in menopause. Gut motility virtually non-existent. Nightmare!
You should check out John Sarnos work, it can’t hurt. I was incredibly sceptical but its beginning to make more sense to me as time goes on.
keep an open mind , his book healing back pain is free here
http://ayurvedavignan.in/freeEbooks/Healing%20Back%20Pain.pdf
it also applies to other conditions, the important aspect is reading it and seeing if you have similar personality traits like those mentioned.
if you are a perfectionist, goodist, people pleaser and someone with low self esteem then it may have something for you
Have you ever tried just plain ginger (fresh, small pieces, chewed) for nausea? It’s been helpful for me, and also somewhat helped other digestive issues. Also eliminating all sugar in any form has helped.
Never liked the taste of ginger and can’t imagine actually chewing it fresh! Nausea is better now — but I guess I can give it a try if things get too bad. Thanks, Ellen.
Carol, that sounds awful, all the pain you endured and endured. I am very glad it was not heart trouble for you.
Getting older might make it sensible to review your diet. Not just gluten, but overall. Maybe there are foods your body cannot handle now? Just another way to look at things. I hope you do not have to endure nausea for long. And if it persists, that you can gather your resources to learn what the problem is, and with luck, fix it.
Your mother had a briliant idea all those years ago.
Carol , please email me if you feel like it. I have the same ME/CFS, FMS AND POTS. Went thru almost the exact same thing that happened with you..Found one very small helpful thing but it’s just too personal to throw it out on FB. LINDA
Carol, thank you for sharing your experience. I can relate to your mental check list of “things it might be”.
It may not be related to your situation, but for me when I’m lying in bed at night feeling aching pain in the center of my abdomen that is keeping me awake, it often turns out to be that my gall bladder is struggling to process some toxins. The solution in my case is to drink a tall glass of water with apple cider vinegar in it. (or one of those bottled apple cider vinegar drinks) It helps to get things moving through a stuck gall bladder.
I hope things will get better for you!
Thanks. Years ago I used apple cider vinegar, but these days I find it irritates my esophagus and increases heartburn. Wish ME didn’t present so many complications!
I had an email from someone who had a REALLY rough time at the ER. When I asked her if she wanted me to post it she did and added a little background. It’s incredible how some people get treated…
I would like the medical community, and the general public at large to know what can happen to someone in pain who shows up in the hospital with CFIDS/ME severe symptoms. I have a toxicology report that documents the amount of ciguatera poisoning in my blood after tests were run when I first contracted the virus. I am being poisoned by toxins from a virus that no one seems to understand yet. They found toxins in my blood that were higher than a person with cancer and hepatitis C. Yet because it’s not terminal (that we know of), it must all be “in my head”. I have been living with this since 1999.
I too recently had a visit to the error for rising blood pressure due to pinched nerve in neck (pain and muscle spasms). While I told the staff, including the doctor, it was added in as an after thought. However, after routine blood draw and urine analysis, they called my husband and son, who lived 2 hours away from my vacation home, to ask if I was suicidal.
The computer spit out all the medications I had ever been on, going back 30 years. I was told I was being moved to a different room. After I followed them thru a double door it clicked behind me. Being a social worker, I knew where I was, the psych ward.
Above my head there was a sign that reads you have the right to refuse treatment..etc”. Which I immediately explained there was nothing wrong psychologically wrong with me. 2 security guards who flanked either side of me while the attend entry explained I could not be released until the psych visited me when they came in at 9am.
I was, asked to strip in front of the female attendant who then took away all my possessions, including my cell phone where I was trying to reach my family or doctors (though it was a Friday night in august an I knew I wouldn’t be able to reach any one of my doctors. ).
I was given a gown and taken to a bare room with florescent lights and nothing but a cot with paper sheets and eye do a camera on b the wall. Now, extremely upset, anxious and still in pain, I broke down in sobs. Through some miracle of strength I managed to calm myself knowing that I was being watched.
When the doctor showed up a few hours later she looked at me and my chart and asked me why I was there. I had no reason to explain why I was thrown in psych ward. She told me to get dressed, my son was waiting for me outside. This was my experience in the er.
Next time I experience high BP spikes due to pain, I will risk a stroke or heart attack before calling an ambulance. I was all alone at the time, which is not uncommon as my husband doesn’t like the shore so I go alone.
Now I am furious and no one seems to care, including the director of the ER to which I voiced a complaint.
I can see how being temporarily thrown in a psych ward even if it was a mistake – as the doctor immediately realized it was – can be a devastating personal experience. These things can leave scars that could indeed keep someone from availing themselves of the ER when they really needed it. It’s rough.
I would do my best to chalk it up to ignorance on the ER staff’s part. Somebody obviously made a big mistake and I hope they were roundly reprimanded for it.
OMG. I cannot imagine the psychic pain that was added to your physical pain by this terrible treatment. I imagine the hospital workers thought you were suicidal because of the high levels of toxins in your blood? Did they think you were poisoning yourself? And then running to the ER? Their whole response makes no sense and I can see so clearly why you would be furious.
I hope all this happened a while ago and that you’ve more or less come to terms with it. Also that you’ve received help with the bp problems and pain.
Hello,
I wanted to say that I also had the headaches, full too fast, stomach pain issues and for me it was a gallbladder full of sludge. It took 8 months of tests to find it and by then I had developed chronic gastritis, something I still have 18 months after gallbladder removal.I found a system that works for me to live with it, but easily the most crucial thing is to keep things moving. I do this with probiotics, digestive enzymes, kios ds, and a diet free of my particular food sensitivities, a d, 500 mg of magnesium twice a day. If I miss even a day “going”, the headaches and stomach pain send me to bed with an herbal heatpack on my belly. I also have IBS, have for years. This, when it flares, is like IBS on steroids. Mostly I wanted to say mom may have been right, keeping it all moving matters, but don’t let them ignore the pain if it could be your gallbladder. The test that finally found it for me was a hida scan. Wishing you peace.
Many responders mention gallbladder problems. That’s not something I ever considered, but. . .will certainly talk to the dr about it. Thanks.
Hi. Happy to have found this site. I’ve been searching in vain for a cause for Chronic Fatigue Syndrome and have exhausted just about every avenue of search. One possibility which surfaced in a recent search was leaky gut syndrome, which may also explain borderline IBS. I’ve read both positive and highly negative articles about effects of N-acetyl glucosamine as a treatment.
Typically I have difficulty in getting through mornings. Ten years ago I went through loss of a business, which did cause depression. Presently I’m slowly being weaned off benzodiazepines, but am on trazodone for sleep and supposed depression. My wife and psych guy state that the fatigue is due to depression, which I strongly disagree with. There might be a remnant of depression, but not more than that. Yes, I want to get into bed much of the time, but not for “escape”. It is because of genuine fatigue turned tiredness.
I’m on a regimen of other meds for maintenance after an MI and bypass surgery 14 years ago.
Any hints based upon other’s experiences would be very much appreciated. Thanks, with a wish for wellness to everyone.
Can you please email me the “Route to Resolution” for SIBO? Thank you!
Colonics
Carol,
My sympathies for your recent experience + a special thankyou for your excellent articles. For years I suffered from excruciating stomach problems + frequently required emergency care. At one point I lost 40 lbs in 3 months due to vomiting +pain. Like most of us on this site, I learned the hospital experience is a least desired option —to be avoided if possible but sometimes it is a last resort!
We all have such complicated health issues + it seems that most of us have had our share of horror stories that include gut + bowel problems.
I’ve found that extensive testing with various probiotics as well as gradually introducing vitamins +supplements one at a time plus eliminating foods that caused reactions have all helped to get me some answers. (Of course as we age, our changing body makes us jump through more + more of these medical hoops.
However, my extreme weight loss + severe anemia from all the vomiting (plus the excruciating muscle pain + flare ups from the constant emesis!…) necessitated taking an anti-emetic medication + I was trained to give myself intramuscular injections at home + this has contributed significantly to keeping me out of the emergency room. (My partner is also trained in giving me injections on days when I am too weak to do this myself. Lately, with major changes in diet, supplements/vitamins etc, I now find I rarely require the anti-emetic injection but am grateful for it’s availability when the vomiting starts.
We are all incredible survivors + you are certainly an example to us in not giving up! I wish you the best in your search for answers!
Thanks for all your kind words. As you say, ME is a devastatingly complicated disease that can force us to bounce around from one health practitioner to the next as we keep experimenting with different treatments. I’m glad that diet changes and supplements have improved that awful stomach problems for you!
I’m very glad you’re doing better! Sorry if this is duplicate information. Reactivated enteroviruses (gastrointestinal) are very common in ME/CFS. If your situation doesn’t improve, it’s something worth checking out.
Not duplicate information. Thanks for your input.