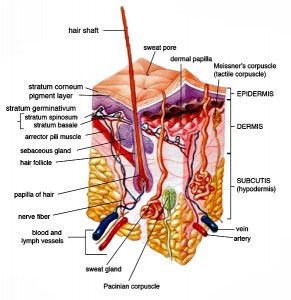
At least five studies have found significantly increased rates of small fiber neuropathy (SFN) in the skin of people with Fibromyalgia. SFN refers to the damage or destruction of the small unmyelinated sensory and/or autonomic nerve fibers. It’s believed that damage to these nerve fibers may cause symptoms such as tingling, burning sensations and pain.

A German team that had found evidence of small fiber neuropathy in FM last year thought they had the answer. They hypothesized that increased levels of pro-inflammatory cytokines were sending those remaining nerves bananas and they had good reason to think so. An earlier study of theirs found increased cytokine expression in the skin of people with SFN (who didn’t have Fibromyalgia), and a study by another group found increased gene expression of cytokines and vastly increased expression of opioid receptors in the skin of people with Fibromyalgia.
All that was needed now was a validation study and researchers could start targeting pro-inflammatory cytokines. It wouldn’t explain why the SFN was present (although pro-inflammatory cytokines could play a role) –but it could help explain why it was causing symptoms in Fibromyalgia.
The Study
Skin cytokine expression in patients with fibromyalgia syndrome is not different from controls Nurcan Üçeyler1*, Susanne Kewenig1, Waldemar Kafke1, Sarah Kittel-Schneider2 and Claudia Sommer1. BMC Neurology 2014, 14:185. http://www.biomedcentral.com/1471-2377/14/185
Using very sensitive techniques they compared gene expression of pro and anti-inflammatory cytokines and opioid receptors in the skin of 25 people with FM, 10 people with major depression and 35 healthy controls.
In a surprise finding neither the gene expression of the cytokine or the opioid receptors were increased in the FM patients relative to the other groups.
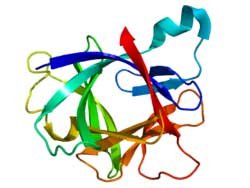
Gene expression studies suggested that increased immune activation in the form of increased cytokines in the skin was not a factor
With that finding researchers are back to square one in their efforts to translate the nerve damage seen in some Fibromyalgia patients to the pain they’re experiencing. Other possibilities increased levels of immune factors called chemokines and problems with the ion channels in the remaining nerves.
The extent of small fiber neuropathy present was measured in the FM group, and as with the past studies, a subset of patients with SFN were found. The authors did not, however, state what percentage of FM patients had SFN. They did note, though, that cytokine gene expression of was not increased in this group.
Because chemokines essentially do the same thing as pro-inflammatory cytokines do – they provoke cells to respond – high levels of chemokines could play a role.
Ion Channelopathy A Possibility
Ion channel damage is another very real possibility. Ion channels play a key role in nerve signaling and ion channel alterations have been implicated in Fibromyalgia. Dr. Martinez-Lavin’s 2012 study found that Mexican women with severe FM tended to have a particular SCN9A sodium channel gene variant and a recent review fingered sodium channel problems in several types of painful SFN. Another recent review urgently urged more research into sodium channelopathies and peripheral neuropathy and asserted that research will reveal specific subsets of sodium channelopathy patients.
Researchers have gone so far as to identify a specific ion channel (Na(v)1.7) in the dorsal root ganglia that is disturbed in several pain syndromes. Genetic mutations in this channel allow ion channels to become activated in response to weaker stimuli, or to remain open longer in response to stimulation. That, of course, is a recipe for “central sensitization”: a hyperactive-response to sensory stimuli.
Deeper Nerve Fiber Loss Found
“Small fiber neuropathies are often associated with myovascular denervation”. Dori et. al
Finally, another recent study found that in addition to small nerve fiber denervation many patients also have nerve fiber loss associated with the blood vessels. Intriguingly, some people without small nerve fiber loss in the skin , demonstrated nerve fiber loss in the myovascular region. These patients had more muscle discomfort and autonomic nervous system problems.
One of the researchers in the initial round of SFN FM studies suggested that the nerve loss in skin may extend into deeper regions. This study did not involve FM patients but suggests it may indeed, and that some FM patients without evidence of SFN in the skin could have it in other regions.
Researchers Jump on SFN Findings
While the results of this study – and it was a small one – were disappointing note how quickly researchers have jumped on the small nerve fiber findings in FM. Not only have six studies over the course of a year or so been done, but researchers are already trying to understand how they are affecting FM patients with this problem.
Testing Lab Ramps Up SFN Testing Protocols
One indication that SFN has been generating more interest is Therapath labs recent announcement that they’ve validated two more testing location on the body (between shoulder and elbow and above the wrist). Prior to this only three spots on the body, all on the legs, met the requirements for testing because it was unclear what constituted an abnormal result. That means more thorough testing for SFN is now available.
Expect to be hearing much more on the SFN problem in Fibromyalgia over the next year.







I appreciate your efforts to bring info to others. This can have an impact on so many of the illnesses we are trying to find band aids for. Some want to say that SFN is the “cause” of these illnesses. I feel SFN is another symptom of these illnesses. Ultimately, if the immune system were working properly, there wouldn’t be a SFN problem in the first place. We need to work on the cause, not the symptoms. For symptoms about the best we can do is a bandaid effect. That’s not getting to the core of the problem. Just my opinion. Why are the nerves inflamed and why are the fibers dying? What is the trigger or exposure? Why isn’t the body recognizing whatever is causing the malfunction in the first place? What would be the fix. – working on the immune system. Work on that and this may be the best we can do for ourselves.
Diet is the first thing to address. Lots of the immune system lies in the gut. Lots of foods are either inflammatory or healing. Some are known to cause autoimmune issues and others to support the immune system in a positive way. It’s the one thing we and only we can do for ourselves. But it’s the one thing people refuse to change. There is no magic pill. There are many assisting supplements. But no one thing that can fix all of this. If we get our bodies to working as optimally as possible with what will help and not hurt us, This is a good step in the right direction.
I was always lost in trying to have an answer to the question of WHY. Now I realize I don’t have to have that answer completely answered. What I need to know is; what would the answer be no matter what the reason for WHY. It comes down to supporting immune system function. So now the question is not to look for WHY the dysfunction. The question is now HOW to support the immune system so the dysfunction is minimized. Everything else is just a “bandaid”. We cover over and minimize the symptoms. We have to get to the core. Autoimmune system and Inflammation because of a faulty Immune system. Pointing back to the immune system – we’ve now come full circle.
Issie
It’s taken me nearly 15 years (& I am even a former Nurse Practitioner before having to retire on disability in 2000), but I have finally come to exactly the same conclusion, Issie! We must strengthen our immune systems by rehabilitating / maintaining the gut microbiome. That is the best thing to do for ourselves now.
Currently, I’m debating when / whether to have my genome run & analyzed in order to assist me in choosing the best advanced diet. I have no idea if I have any food sensitivities or not. I do have Hashimoto’s (autoimmune) thyroiditis / hypothyroid as well as Fibromyalgia & ME/CFS. Just learning about things like methylation pathways & the various dietary options (gluten-free, ketogenic) which may further improve things. But must determine genetics in order to make the correct choices regarding those interventions.
So far, all I’ve done is severely limit sweets, caffeine & alcohol, switch to organic (as much as possible), increase healthy fats while decreasing unhealthy fats, eliminate junk food, processed food & artificial / chemicals, maximize filtered water intake, add certain high quality supplements, & listen to my body.
Always appreciate your posts, Issie (great contributions & I’ve learned a lot) & the entire forum, Cort!
I think knowing your mutations in the methylation process could be very helpful. I did 23&me. I work on my issues with diet and supplements.
I find following Dr McDougalls diet plan to be my best medicine. I pay a lot of attention to trying to eat as organic as possible a whole food, low fat, vegan diet. He does not limit carbs as they are what gives us energy. He does however limit fat. There are some very good sites that talk about this type of eating lifestyle. Some of my favorites are: Dr McDougall, Forks over Knives, Dr McGreager, Engine 2, there are many more. Their websites keep me motivated to stick to this lifestyle. IT WORKS!!!!!
Issie
Hi Beth
I have been going through a lot of testing. I’m due to see a rheumatologist in December. I have been a nurse for 20 years and am looking into disability. The only thing that gets rid of my pain is a steaming hot shower. Do u have any suggestions for further testing and/ or pain relief? Alison
I agree with you, Issie, that the SFN is just a symptom and not the cause. However, maybe the immune system is just doing its job (which it does better on a good diet, of course.) What got my attention was when you spoke about the body recognising what is happening and what is it doing about it. I believe that despite what went wrong in the past, that the body in the present is trying to overcome the situation (for survival of the organism).
You also said that a good diet is the only thing that we can do for ourselves but there is something else we can do and that is to attend to our trigger points (knots) in our muscles. The body can only do so much in this area, the rest is up to us. I actually believe that the body creates central sensitisation to make us wake up and take notice. We have lost touch with our bodies in this brain age. We don’t listen to our body and respond to changes in tension. We live so much in our brains that we don’t notice poor posture and repetitive actions that are harming us. Normal people have trigger points but I believe that a sustained sympathetic arousal means that trigger points are a much worse problem for us. Trigger points cause blockages in blood and nerve supply to the muscle fibres and it is a known fact that they eventually spread to the skin. I believe this is what is causing the allodynia and SFN.
Enhancing the immune system with a good diet means the immune system will be doing a better job of cleaning up the resulting mess caused by blockages in the periphery. I believe this is why a nutritious diet ameliorates the intensity of the trigger points with resulting less pain. However, there are many other factors perpetuating trigger points – poor sleep, metabolic imbalances, body asymmetry, muscle abuse including poor posture and repetitive actions, infections, disease of internal organs, the weather and even psychological factors. Attending to these perpetuating factors goes a long way towards treating the trigger points but once entrenched, with ropey bands developing, they need to be manually deactivated to prevent increasing pain and as I believe, damage to the peripheral nerves.
At my worst, I suffered from severe allodynia but with attending to as many perpetuating factors as I could and manually treating my trigger points as often as possible, my allodynia is gone from most parts of my body even though I still have areas of numbness in the vicinity of my worst trigger points. I do believe, however, that due to our sustained sympathetic arousal, we will never be completely free of trigger points until the cause of the arousal and possible solution is found.
I do think we hold a lot of things in our muscles. I’ve personally experienced this myself. I once had a very skilled massage therapist who taught me about noticing how with the release of these knots comes a flood of emotion. Along with that emotion, usually there will be an event that will come to mind. It may be something very painful and we have to experience that emotion and be present with it or we will not be able to let it go. We may get it back again if something triggers a memory or emotion related to that knot. We hold pain in our bodies many times because we rather not deal with “whatever” it is that may be causing some of it. For example, we use the expression, “they are a pain in the neck”. Notice if when around that person – do you get a pain in the neck? This isn’t all the cause of these “pains” but it for sure is one cause. Our bodies are trying to tell us things but we tend to ignore its clues and warnings to us. We may be holding onto some things as a way to avoid something we either dont want to face or avoid something we don’t want to do. We have to be honest with ourselves and open ourselves up for review. It may be painful – but it may be what will help us get rid of our some of our “pains”.
Issie
Issie
Dear Issie and Tricia,
Thank you for your comments I so agree with both of you. I have got myself 80% better (I have FM), when I was about to buy an electric wheelchair and unable too work for 20 years. This has been by diet, relaxation techniques, posture, trigger point release and a type of NLP called ‘Revolution Magic’ by Olivia Roberts to release the emotions so they don’t add to my pain.
One area you don’t mention that has also been a great help to me is using the microcurrent device called the Alpha-Stim. It calms the CNS. It reduces the agitation of increased impulses going to the brain and encourages the inhibitory messages to work. It also works on modulating signals in the ion channels of nerves. Did you know that 98% of our synapses are electrical and only 2% will respond to medication!
Great article again Cort.
Linda
I find this interesting in that I have heard that massage can bring about a flood of emotions but I have never experienced it myself. Probably because I never undertake long sessions as massaging the knots pushes toxins into the system and one can only cope with a certain amount of toxins at any one time. I would even suggest that a long massage session could so overload the body as to compromise the detoxification system, changing the body pH and thus causing emotional lability. The psychological factor is only one perpetuating factor, my main ones these days are muscle overuse and inclement weather, as well as the ever present fibromyalgia which is a perpetuating factor in itself. However, I often get knots in the abdominal muscles related to emotion as one tends to tense up the abdominal muscles when emotional. I do my own massaging as I don’t need to leave the house for long weekly sessions but rather can do small amounts frequently as needed. For learning how to do this yourself, I really recommend The Trigger Point Therapy Workbook by Clair Davies.
Very true Tricia,
If you’re not used to massage it can really give a knocked out feeling, so if trying massage for the first time I suggest to my support group members to start with a very gentle 30 mins and not a full body massage.
Another good trigger point book with a bit more detail is ‘Healing through Trigger point therapy ‘ by Starlanyl and Sharkey. I use it to guide me where to place the Alpha-stim probes to relax my trigger points in a far more gentle way than massage. I also find using the ear-clips at the same time as a massage relaxes my muscles even more and helps stop the tired feeling afterwards.
Linda
Thats why you need a GOOD massage therapist. They will pay attention to you and your responses. Not only physical but mental and emotional. When you do a release the person may cry or get angry or any number of emotion. Also the body does release toxins and there can be unpleasant smells that start to come through the skin. With FMS a lot of the time only pressing trigger points is needed. But as you progress, massage with varying techniques is very good. I sure do miss the one I had. Haven’t been able to find one like her since she moved.
Issie
Hi Linda and Issie
It’s great to have this discussion on trigger points, an area much neglected when talking about pain in these illnesses of ours. I’m very happy for you, Linda, that you are doing so well now. I have heard about micro current therapy but have not been willing to take it on. The main reason being that it is very expensive and it is not guaranteed to help everyone. I’ve read that people like me who have a delayed response to anaesthetics, need to use it for much longer periods of time. I can’t imagine myself zapping my brain for 3-4 hours a day. Also, if I understand correctly, each trigger point would need 10 minutes of the probe whereas stroking massage takes only 30 seconds per trigger point. Probably OK for those with just a few new trigger points but for widespread and protracted cases, very time consuming. I’d love to hear more details of how you use it.
A question I have also is that if the micro current therapy increases alpha waves during the day, how much effect would that have on FM which I believe to be more affected by the lack of delta waves during stage 3 and 4 sleep, causing a shortage of growth hormone which perpetuates trigger points? I’ve also read that the brain can be retrained using aural tones to match the frequency of the required brain wave and and achieves results far more quickly. I’m wondering if there is a way to use this method during sleep to increase delta waves.
Linda, I do have Devin’s latest book (I have most of her books) which is very comprehensive and I also have Travell and Simons trigger point manuals which are good if you have some knowledge of anatomy and muscle mechanics (I’m an ex- nurse) but I usually recommend Clair Davies’ book as it is very concise and user- friendly for lay people just starting out. It has very accurate diagrams of where the trigger points are most likely to be found. I actually still prefer to use it myself as I’ve been doing my own therapy for 20 years now and back then Devin recommended sustained pressure which I found to be very painful. Stroking massage which I mostly do using a Theracane I find to be more effective and much less painful, especially knowing that the trigger points are unlikely to fully release or if they do, they will soon be back.
As for treating the autonomic nervous system, herbs can be helpful. I am trying with some success so far, Rhodiola Rosea which is an adrenal adaptogen and is believed to promote the parasympathetic but can be stimulating in smaller doses.
Thanks, Cort, for allowing us this input. You sure have a great blog here.
Theracane user myself. Great help for trigger points.
Issie
Interesting re: trigger points and posture, etc., but I feel like I don’t have the energy to stand up straight. Do you work on your own trigger points or receive body work?
All these research findings are so encouraging. But when can treatment protocols result from them? I recall Dr Oz saying that treatments for CFIDS & FMS have been lagging behind until more recently. I would like to hope that treatments resulting from these findings would come very soon.
Interesting, I was in the study done by Oaklander.
My nerves tingle…probably because that’s where the EBV resides.
You would like to know a natural treatment for nerve pain a natural treatment may can bring total cure for (Neuropathy) and scientifically proven,,,then visit the link that follows,,, http://www.deconero.net/health—fitness.html
Cort, FYI
Just wanted you to know that there are negative alerts on some of the information that Andre refers to. This site is apparently known for
posting “miracle cures” etc. I have received a # of alerts to claims made by the author of this web site.
( I wish there was a miracle……! )
So any discussion as the how the SFPN is being treated ? Nerve damage is a pretty significant finding in a poorly understood syndrome like FM regardless of the aetiology.
Yes Chris, my change of diet and working on my Immune system has helped mine. I can feel my toes again. I have off and on symptoms now. When I was first checked, I couldn’t feel the pin pricks at all in half my feet and some parts of my ankle. Now I can. Neuropathy runs in my family and not from diabetes. My father had it in all his limbs past his knees and elbows. So trying to prevent it in the younger generations of my family is a good goal. I am on a low dose doxycycline and antimalarial herbs. I think that has helped too. Along with meds like GastroCrom and histimine blockers for MCAS. My diet is my main help though. If I have too much fat in a day, I can sure tell it. Dairy is known to trigger autoimmune problems. It is also thought FMS and SFN has an autoimmune cause. One of the latest things I’ve seen is the possibility of the immune system attacking the body worse with the introduction of any animal protein. The immune system recognizes it as a foreign protein, goes in to break that protein down, has a hard time distinguishing between animal and our own body and attacks our body too. Makes sense to me. I know I’m better since I went vegan.
Issie
I have struggled most my life with chronic pain and diagnosed with FM. More recently with EDS and considerable hypermobility. Most of my pain is expressed in neck, shoulders and jaw. When I had a particularly bad flair with TMJ, I did a variety of body work modalities such as massage, chiropractic, occupational therapy and the most helpful cranial-sacral therapy. I found a highly skilled osteopathic doctor to perform this work the best. It took me a good year or so with a combo of this work in addition to a short stint with pamelor by a pain center to get out of excruciating head pain. Deep tissue or more aggressive massage can cause pain to flair. Dry needling in trigger points (similar but not the same as acupuncture) also helpful.
Interestingly, my daughter has severe POTS/CFS which expresses a great deal of GI tract problems. Thru testing at Vanderbilt we discovered she has a 20% deficit in blood volume and severe small fiber neuropathy (operates at 5% of normal) and has major thermoregulatory problems. I suspect I would have pretty similar results. Her sister has been diagnosed with RND. We are going thru genetic testing but have only scratched the surface and finding mutations in the marfans area. I personally have found a raw foods diet to help with my symptoms and regularly take MSM which helps with the inflammation in the body. I agree getting the gut healthy is a good path to take. I think this study on SFPN will lead to some discoveries that will help many of us. Just wish they would get there sooner than later.
Im thinking about moving to a more moderate climate with stable barometric pressure. Cold and heat make the nerve pain worse. My daughter’s symptoms getting worse now that days and nights getting colder.
What an “interesting” family you have Kathy. They seem like proof that similar genetic underpinnings underlie a variety of related disorders. Good luck with your children and yours health.
I’m HyperPOTS, with EDS and MCAS. Also got a FMS DX.(lots of other stuff too). But wonder if it’s all EDS or if I have both EDS and FMS. I have problems with thermo regulation too. I just say I’m a fair weather gal.
Have not been seeing Stem cells mentioned. Any news about that?
Is there some kind of test to figure out how your microbe environment in your again tract can be figured out; and, perhaps then be corrected by taking the ones that you need. It’s a start.
One more thing, has anyone experimented with some kind of IV therapy which would include what your body needs for a boost in healing, and/ or a cleansing ingredient.
What role does yeast play in all this?
I find that the isolation these symptoms have caused me to be unbearable.
Greatly appreciate your newsletters. I have learned so much from the information you have so generously and kindly provided.
I meant investigating your microbe environment in your digestive tract.
Sorry for the wrong word “again” which was not in my line of writing the gut comment. Thank you.
Don’t they put another’s microbe GI family into another person’s GI tract. Seems to me the microbes aren’t getting to where we want them, and we are going in circles.
Ideas: suppositories? An injection of a slurry made up for that particular patient using some kind of anesthesia?
I think it is obvious the patients, no matter how much they are aware of intestinal flora, are not succeeding with trying to correct the balance. I think the upper excretions from our stomachs interfere, and break down the good guys.
Look at the success of MERSA. Think about what we have learned from direct penetration
Of the good guys.
And, it just might make the brain fed better. Leading to less suffering.
I have had the leg biopsy as well as spinal tap, which gave me the diagnosis of SFN. I have been told Fibro for so long. I have tried anything suggested. My last and first treatment of intravenous gammagobulin. The base treatment was tone 5 days, 6 hours a day. I only made two. The pressure in my head,pain, fever, nausea and vomiting. Everything slowly eased up. Not the pressure in
My head behind the eyes from tues at 6 pm until around 10:00 pm on Friday . I am dealing with a very knowledgable, and leader in this field of SFN. I am not sure what’s next.