Alternative Medicine Meets Fibromyalgia
It was a tough group of fibromyalgia patients that a team of alternative medicine and mind/body practitioners took on. They had not responded well to other therapies and had so many co-morbid disorders (over 700 diagnoses in total) that the authors stated they would “not be presented due to their complexity and scope.” The average visual analogue pain scale scores averaged out at about 7.0 which meant they were in severe pain.
Fibromyalgia with severe forms of progression in a multidisciplinary therapy setting with emphasis on hyperthermia therapy – a prospective controlled study. Romeyke T, Scheuer HC, Stummer H. Clin Interv Aging. 2014 Dec 19;10:69-79. doi: 10.2147/CIA.S74949. eCollection 2015.
They had responded so poorly to treatments that they were picked to participate in an extended in-hospital stay where the Austrians threw the alternative medicine book at them. Over their approximately two week stay everyone received phytotherapy/mind-body therapies, hydrotherapy, lifestyle regulative therapy and movement therapies. In addition some people received detoxification, neural therapies, homeopathy and diet advice. One group received heat treatments (plus the other other therapies) while the other didn’t.
Gate Control Theory of Pain
The psychotherapy and CBT focused on providing methods of coping with pain and deflecting attention, problem solving and learning how to manage their illness better. The kind of CBT used was based on the gate-control theory of pain.
This theory posits that increasing the activity of nerves that do not relay pain signals will decrease the activity of nerves that carry pain signals. It helps explain why when you’re in pain and you consciously distract yourself your pain usually lessens. It also helps explain why people in chronic pain often experience significant placebo effects.
One of the goals of gate-control based therapies is to increase other kinds of sensory input than pain. We’ll be digging deeper into this theory later.
Heat Therapy
In addition to the other therapies half the patients were given heat therapy or hyperthermia. Many different types of heat therapy, from hot water baths to whirlpools to mud baths to steam baths exist, but in what appears to be tech speak for an infrared sauna, the study stated that the participants were given”whole-body hyperthermia with IR radiation” while they were “lying in an insulated cubicle”
For a person with fibromyalgia and/or chronic fatigue syndrome perspective both positive and negative things can happen when you heat up your body. For a start your heat rate increases to levels experienced during moderate exercise – which could be problematic for people with ME/CFS in particular. Decreased “peripheral resistance” (blood flowing more easily through the blood vessels) and increased circulation on the other hand, could be helpful. Oxygen consumption and levels of the stress hormone norepinephrine increase.

Saunaing in style – a “Geysirhöhle” by Therme Erding. Original uploader was Studi85 at de.wikipedia – Therme Erding. Licensed under CC BY-SA 3.0 de via sauna.sauna with its own geyser.
The levels of pain reducing beta-endorphins plus muscle relaxation and increased elasticity of the tendons probably contribute to the relaxed feelings many people get in saunas. Dr. Rowe’s findings of reduced tendon elasticity in adolescents with ME/CFS suggests saunas might be helpful in relieving the movement problems in ME/CFS if other aspects of the sauna are tolerated.
Hyperthermia also may be able to inhibit bacterial and viral activity. Dr. Rea in Dallas has also successfully used sauna therapy for years to detoxify people with chemical sensitivities.
Even the Mayo Clinic has some good things to say about sauna therapy
“Several studies have looked at using infrared saunas in the treatment of chronic health problems, such as high blood pressure, congestive heart failure and rheumatoid arthritis, and found some evidence of benefit. However, larger and more-rigorous studies are needed to confirm these results.”
Results
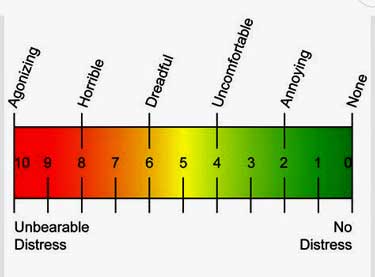
The average FM patient in the heat therapy group went from being in horrible pain to being in between being uncomfortable and being in dreadful – at least according to this scale
During their stay the hyperthermia group received, on average 5 hyperthermia treatments between 37.5 and 38.5 (100 degrees Fahrenheit) degrees in what appeared to be an infrared sauna.
The visual analogue scale (VAS) indicated that the mean level of pain on admission was 6.8 for the control group and a whopping 8.2 (very severe pain) for the group receiving hyperthermia.
The results suggest that this kind of intense multi-dimensional approach to pain reduction can help. The average pain levels of those not receiving the hyperthermia treatment dropped by thirty percent (VAS = 6.8-4.8) These FM patients were definitely not out of pain – they still averaged 4.8 on the VAS, but they went from feeling somewhere between dreadful and horrible to somewhere between feeling uncomfortable and dreadful (at least according to his visual analogue scale – which is not necessarily the one they used.).
The patients receiving heat treatments plus the other treatments started off worse (VAS=8.2-6.8) and improved more (VAS = 4.0 -4.8) than the patients not receiving heat treatments. Instead of feeling “horrible” they were now simply “uncomfortable”. Their “functional capacity” was significantly increased as well.
Results Suggest Heat Treatment More Effective Than Physical Therapy
An analysis indicated that the control group ended up receiving much more physical and movement therapy than the heat treatment group. That suggested that heat treatment was more effective than physical therapy in reducing pain and improving functionality. (The amounts of phytotherapy, psychotherapy/mind/body, detoxification, neural therapies, homeopathy and diet advice received from the two groups was the same. )
The decrease in pain the FM patients received from the hyperthermia treatments and the in-hospital stay was both gratifying and sobering. It indicated that providing multiple alternative and mind/body treatments during an in hospital stay can significantly reduce pain. Whether such intense and expensive types of treatment are feasible or cost-effective is another question.
The increased functionality and greater pain reductions experienced by the patients receiving infrared heat treatments, on the other hand, was promising. If they’re accessible, heat treatments are very simple to use.
Infrared vs Traditional Heat Saunas
This study used a type of sauna – infrared saunas – that have become increasingly popular over the past ten years. Traditional saunas heat the air to sometimes astonishing temperatures (up to 180 degrees) which then heats the body from the outside in. They’ve been successfully used for detoxification and other purposes for decades.
Because the traditional sauna method of heating (convection heating) doesn’t penetrate the body as deeply as the radiant heat of infrared saunas, proponents of infrared saunas assert they are better at detoxing. Because infrared saunas operate at lower temperatures people are often are able to stay in them longer and sweat more.
Both saunas are effective at detoxification and in raising the body temperature but infrared saunas appear to be more easily tolerated.
My Experience With Sauna Therapy
I underwent sauna therapy at Dr. Rea’s practice about 30 years ago. He used exercise – to get the toxins out of the muscles and into the bloodstream, supplements and fiber – to soak up and detoxify the toxins, and sauna – to remove the toxins via sweating.
Watching multiple chemically sensitive (MCS) patients whale away at the exercise cycles made it clear that ME/CFS and MCS do not share some core problems. I quickly dropped the exercise session but I engaged in one to two sauna sessions a day for six weeks. Being in a hot traditional sauna for me is equivalent to engaging in exercise and it was a painful process. I left the program thinking it was a failure but two days later driving home I experienced feelings of wellness I hadn’t experienced for years.
I intermittently used traditional saunas since then and often experience increased clarity of thought, increased energy, etc. from them which sandwiched in between strong symptoms flares. I could never bring myself to use them regularly again.
Conclusion
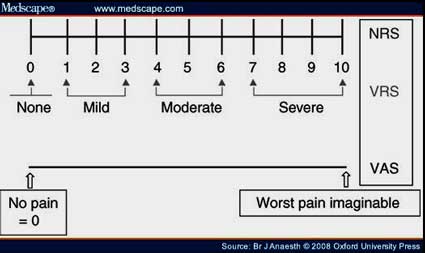
The treatment resistant patients using heat treatments and other methods went from severe to moderate pain
This study found that intensive in-hospital stays using alternative and mind/body techniques can lead to significant reductions in pain in severely ill fibromyalgia patients.
In addition infrared saunas, when used in combination with other methods, may be able to provide moderate to significant pain relief. Given their much lower temperatures infrared saunas are probably preferred for FM and ME/CFS patients.









Nothing “low-tech” was mentioned like heating pads. For many of us the “high-tech” methods are not covered by Medicare.
I know that heat always makes me feel better.
Indeed. They did mention in the study all sorts of heating devices including as a remember heating pads…
It would be nice to have an infrared sauna but they’re a bit out of reach for me. I do love sitting in a sauna…
I have a portable foldable infrared sauna that I purchases for about 150 dollars. It works great and has been very helpful in treating my chronic illness, Just go on amazon or ebay and find one. I have been using it for 5 years and has been a lifesaver for me
Cool – that’s more like it… Shoppers – please consider entering Health Rising’s Amazon.com store (right hand side of page) before you go shopping 🙂
Great, yet another study proving that what thousands of patients have done for years, actually works. It has been my experience that those who get no relief from these types of therapies have overdone it.
I’m with you on the heating pad use..but..I also use Bath and Body Eucalyptus massage oil. .it is thee most effective relief potion I’ve ever used..try it!
I wonder if one of the diet therapies increased magensium in the diet, A large number of people benefit from magnesium but some can’t tolerate supplements because they can cause diarrhoea. A warm bath with epsom salts can be toerated by many people and combines heat with a known pain reliever. When I was suffering from extreme pain it was the only thing that provided immediate moderation of the pain
Yes..100% re use of MG+…it is so important for healthy muscles. .not to mention ones that accumulate lactic acid or aka trigger points. Natural Calm powder is great for many uses..all great for metabolism use.All u need to do is titrating your doses according to the diarrhea. .just cut back the dose. Magnesium is used first in tx on patients coming to the ER with heart attacks and abnl rhythms..it calms your muscles (heart too) & is first the in line when treating a threatened miscarriage or early labor..to RELAX THOSE muscles involved on the area of trouble. Google magnesiums uses and involvement in ALL our disease processes…it’s deficiency in our body are the cause of most illnesses. #1 hypertension and Diabetes! It is proposed that up to 80% of Americans are deficient in this most important mineral. GOOGLE Magnesium deficiency symptoms and you’ll see what I’m referring to. ProHealth Double strength wit ATP is my mainstay!!
I am wondering if the anti-viral potential of hyperthermia-sauna treatment would offset the increased heart rate and norepinephrine dump (leading to increase in fatigue, and possible crash) for CFS patients.
Cort off topic but….important!!!!
Have you heard how some antivirals can markedly reduce microglia activation?
This is fascinating in terms of CFS!
Could you put this to Jarred Younger?
See here re gangliclovir:
http://jem.rupress.org/content/211/2/189
wow…look at that! Thanks
any chance of raising it with Younger?
Interesting study, Cort. I’d sure love to try an infrared sauna, but I’m limited by being on Medicare. There are hand-held infrared heat devices that people can buy. Of course, they only heat locally wherever the device is held, rather than provide a full-body benefit. But if I knew that they actually provided even a small area of pain relief where my pain is the worst, I’d invest in one. Of course, when I say “invest,” I mean like under $100. If something were guaranteed to help, then I might consider going to $200. But I haven’t seen any studies or articles demonstrating the efficacy of those hand-held gizmos.
Now, I know the opposite of heat – COLD – is also supposed to lower the level of pain in FMS patients. I first read about cold therapy years ago. Immersing the body in warm water and then gradually lowering the temperature of the water over a period of time allegedly brings down pain levels. Or taking showers where you do the same thing until you’re taking cold showers regularly has the same effect. I would guess there’s a different bodily mechanism going on with cold therapy.
Thanks for this information, Cort.
I remember Dr. Rea saying that insurance companies would reimburse for people using this sauna but they would never actually pay for a patient to get a sauna -which would be much cheaper for them in the long run and much better for the patients.
Check out this from Darlene – I have a portable foldable infrared sauna that I purchases for about 150 dollars. It works great and has been very helpful in treating my chronic illness, Just go on amazon or ebay and find one. I have been using it for 5 years and has been a lifesaver for me
Whole Body Cryotherapy is a cold therapy that helps some people with fibromaylgia. It involves standing in a chamber with cold dry air at temperatures lower than 166 degrees F. (-110 C.) for 2-3 minutes. The therapy is popular with athletes as it helps them recover more quickly after working out, but it is also effective for conditions of chronic pain and inflammation. For more information read my post http://fibrofriends.typepad.com/fibro_friends/whole-body-cryotherapy/.
One thing that I think should be considered in measuring the response of CFS & Fibro patients is the number of years the patient has been ill. Many of the common at home remedies worked great for me in the earlier years of Fibro. As the years have passed, the “good days” have become further apart, the amount activity that I can handle in any given day has decreased, and how well I respond has significantly changed.
I couldn’t do without my soak in a hot bath every morning (usually a couple of hours after I get out of bed). It was a real problem when I had to have showers for 6 weeks after my back surgery. And No, a hot shower is not the same thing as immersing in a hot bath.
It gets rid of my morning stiffness and back pain 100%, but then I do have sciatic pain caused by nerve root compression from the osteophytes that formed after my 2008 lumbar disc surgery, as well as FM.
I also have severe obstructive Hypertrophic Cardiomyopathy (HCM) and my heart meds keep my heart rate very slow. I’m not aware of an increase in heart rate when I get in a hot bath at all and with my heart condition I’d be sure to notice if it did.
BTW this is the reason I can’t do any exercise program, except for slow walking, and even that causes hip & R foot pain (from an old injury & ankle surgery) – the Heart Condition (which is hereditary).
I usually have a hot water bottle behind my lower back in winter while watching TV or sitting in my desk chair.
I have multiple health issues besides CFS/FM and most of them have need differing treatments, some of which are the opposite to what is recommended for one of the other health conditions (which is why it’s so difficult to go to a new Specialist – they can’t offer treatment because it usually causes an exacerbation of another of my health problems.
Since I’ve had severe episodes pain for over 30 years and other additional health problems for nearly 20 years, it’s actually easier for me to treatment myself (with the help of my GP when I have questions). Of course I have annual (or 6mthly) checkups with my Cardiologist and Endocrinologist, and my severe health problems and surgeries are in hospitals.
One can easily work out the best treatment when you have a background and knowledge of alternative therapies as I do.
The only real set-back is that living on a Disability Pension means I can’t afford my ‘perfect’ diet any more, and certain foods do cause flareups of symptoms – usually tachycardia, spikes in high BP and chronic inflammatory episodes. I also fall asleep and get very lethargic if a eat too many grains. My old diet when working was based on The Paleo Diet (which results in a complete reduction in inflammation & no IBS symptoms).
Except for when I’ve sprained an ankle etc COLD or ICE is the worst thing possible for me.
cold or ice is the worst thing for me…..
Interesting article–will go look at the study.
I don’t like infrared sauna. I do like regular sauna and particularly steamrooms, always did. I also like sweating in the hot sun. But I also like cold–and activity outside in the cold. I know of people who got better through sauna, and people who got better through cold thermogenesis. So my hypothesis is they both activate antioxidant and endorphin pathways.
I have a ceragem bed which gives out infrared heat. It feels good while I’m on it but like any other heat application for me, it’s very temporary.
I have an infrared sauna, purchased used on craigslist a couple years back after being recommended by a local chiropractor. I have to say I LOVE it. I don’t use it as much in the warmer months but during the winter and fall it is a godsend. I use it at 135 degrees and only for about 20-30 minutes at a time but after about 10 minutes in the sauna, I can do all my stretching exercises (neck and upper back) with almost no pain, much easier than without the penetrating heat. For those looking for an IR sauna, check your local craigslist. There are many. I have a small 2 person sauna that really only has room for 1 person, plugs into regular 110v outlet and sits in my unfinished basement. only takes up about 4×4 ft footprint. I do not like traditional saunas, feel like I cannot breathe properly. The IR sauna followed by a shower before bed really helps with the aches and pains of FMS.
Glad to hear – thanks for sharing your experiences 🙂
I’ve often thought about inventing a soft fleece garment that would warm the entire body. Heating pads, thermal wraps and the like don’t even begin to cover all the parts of my body that ache.
I have been using a far infared dome for the last 10 years. The dome is 180 by 14 wide. You can pull it over your body to target healing heat to wherever you need it.
I use mine in bed lying on back, stomach or side. You can set it’s timer for 15, 30, 45, or
60 minutes, and I use it day or night as needed. It’s great for releasing tight sore muscles and arthritic joint pain. I’ve had FM for 20 years and this dome has been a God sent for me, especialy after more major housecleaning or shopping. I also found it great for night leg cramps, and cold feet. Ha!
Far infrared heat helps you to detox. Drink large glass of water before and after use. This heat is comfortable and will not burn you. If my bedroom is a bit too warm, I direct a fan my way.
My dome is from HTE CO. http://www.hteamericas.com (pick your country) When I checked their website, the current price is $899. for the regular size and $999. for the larger one. I also saw that they had $100. off this month 01/15. These prices are US.
I don’t know if there are other companies selling a similar product.
Worth every penny! My husband also uses it for his aches and pains.
Thanks for passing that on Edith 🙂
FYI Coursera will soon be starting a course on chronic pain.
https://www.coursera.org/course/chronicpain
Great article, thanks for posting. I built a small but highly effective infrared sauna based on Dr. Lawrence Wilson’s design (sauna therapy) only I did a lot of modifications to make it safer and more effective. It uses 4-250w infrared bulbs. I put in a rheostat and timer and a metal light box with safety screen. I made the frame from poplar so as not to have any fumes such as cedar or pine would emit. It worked so well that I wrote a EBook on construction one. Dr Wilson’s design used a simple PVC frame with a canvas and had three lights mounted on a board. I’m sure this would work but I wanted to avoid any toxic materials. There is nothing fancy about my sauna. It is a insulated wooden frame with covered with a painters canvas (maybe not even necessary due to the insulation). Looks like a small sweat lodge.
The first thing I noted when beginning to use the sauna was it took me forever to break a sweat. The ambient temperature runs about 110′ but I could feel the heat from the bulbs penetrating my body. I’ve heard from many others with low adrenal function that they too do not sweat easily. I have to admit, as easy as this is to use, I have a hard time remembering to use it regularly. It took me several months of sporadic use before I could easily break a sweat within the first 10 minutes whereas initially it would take a half an hour. The heat feels really good and does help with muscle aches, though muscle pain is not my primary complaint.
Anyone could use a single bulb in a clip on light and get some benefit though it would most likely not induce a sweat. With this design I sit on a small stool about a foot and a half from the light box that is mounted vertically. Every few minutes I swivel around on the stool. The 4 lights are arranged in a cross pattern, 2-verticle and 2-horizontal. They are aimed and the torso from about the throat to the lower abdomen.
Thanks Dana – could you provide a link to your ebook?
I’m in heaven in a hot bath in a deep tub! I wish I could live in the tub. A heating pad in bed at night is very comforting as well. The only problem for me is when I get out of the tub, my muscles slowly contract again. I haven’t been in a sauna since I became ill, but if I get the chance, I think I should try it. Thanks for the info, Cort, all the info!
I have always loved hot spas, they seem to relax muscles and ease pain at the time, but I came to suspect that I was seizing up worse than ever once I was out of it.
Then I read something about body heat regulation being a problem in fibro sufferers, which made a lot of sense to me. I do tend to stay “hot and bothered” for hours once my temperature is increased (including from exercise). So I started trying spas again, only cooling down immediately afterwards by getting into a swimming pool – I was using the spa at the public swimming baths anyway. The swimming pool is heated, but still cools me down from what I was in the spa. If still not cool enough, I take a cool shower, stand around with fresh air on my wet skin, or even under an aircon outlet until I have cooled down some more.
Even though I cool myself down, I am sure my muscles are more flexible after having a spa and cool-down, compared to otherwise. In fact I do stretches while in the spa and they seem to be more effective that way.
I also worked on cooling down quickly after exercise.
Over the last year or so, working on numerous approaches besides this one, I have become a lot more tolerant to heat. I now love paced exercise in direct sun on a hot day, which I used to find intolerable. The heat of the sun actually soothes my muscles as I exercise. Wearing full-length compression sportswear might be helping. I actually don’t sweat as much as I used to – my clothes would become streaked with white from salt from my sweat, which no longer happens.
I am experiencing numerous changes for the better, it is really interesting. It is like a whole lot of nuisance traits in my physique and metabolism always were related to an overall condition, and are improving in unison.
But it requires dedication and quite a budget for good massage therapists etc. Infra Red saunas might be something worth adding to the list, I have never tried one and don’t even know where there are any in my area. I have found a hyperbaric oxygen chamber recently, which is the latest thing I am trying out.
I am intrigued by the possibilities that IR heat might be different in its effects on the body, compared to conventional transfer of heat into the body from water or air. Is it less inclined to leave the whole body overheated afterwards?
HI PHIL
THE INFO ON FAR INFRARED HEAT IS JUST AHEAD OF YOUR COMMENT, SENT BY EDITH.
I DO NOT FIND IT HEATS MY WHOLE BODY. I ONLY FEEL THAT THE PAIN IS GONE IN THE AREA TREATED.
I got one from http://www.HealwithHeat last year. I like that their design blocks all EMFs. I feel cold on the inside all the time and going in the sauna is the only thing that helps me warm up and relax – really helps FMS tightness. They’re willing to offer financing so it can be affordable.
Thanks for passing that on 🙂
For those that are interested in a FAR infrared Sauna, I just saw one advertised at Costco for $1,499.99. It’s a saving of $500. Sale ends 02/22/15. The shipping is included in mainland USA. You need a membership. The cost for a year in the USA is $55.00
I have a wonderful natural heat treatment most of the year. The sun, in a sheltered spot away from the wind. I just put my back to the sun, wearing a small hat, and let the heat go in. It’s wonderful, like a ray lamp. Only takes about 10-15 minutes and I feel much better. On the days when I am unable to do this I certainly notice a difference, for the worse. Also a long soak in a lovely hot bath before bed does wonders for a good nights sleep. Add a little Epsom salts and I sweat profusely (don’t do that every night though). Glad to see they are finally accepting and trialling natural treatments.
Jazel