March, 2014
“Recognize your disabilities but emphasize your possibilities”~William Arthur Ward
Allow me to apologize for my tardiness. I’m sorry to be posting a blog that happened almost a year ago! But with all the visits and tests that resulted after finding the spinal cord lesion in 2013, it has taken me awhile to catch up…but I’m just about there!! Thank you for your patience. ~ Corinne
Summary of My Previous Blog

Corrine’s seen the experts, and she’s been able to eliminate some possibilities, but the way forward is still unclear
I had revisited the Mayo Clinic in Arizona, 23 years after my ME/CFS onset (when they had diagnosed me as having nothing physically wrong and sent me home, suggesting that I was depressed), to inquire about having a thoracic lymph node biopsy (mediastinoscopy). The biopsy was the suggestion of the neurologist at UCSF (Dr. P’s referral), with the hope that it might help us come up with a definitive diagnosis of neurosarcoidosis to explain the inflammatory spinal cord lesion that had been found on a cervical MRI in February 2013. With Mayo’s refusal to perform the biopsy, saying the risk was not worth the probable low yield, and my decision to not pursue further testing, I was right back where I started from when the lesion was discovered – without a cause or a treatment.
Test after test had produced non-specific answers but had ruled out some things such as MS, neuromyelitis optica (NMO) and probably malignancy, among others. Dr. G, the UCSF neurologist, has agreed to a phone consultation with Dr. P and myself to discuss treatment options. I feel this will be a pivotal trip – I plan on leaving there having made a decision on a treatment for this serious neurological issue that has become more uncomfortable and painful with each flare.
Medications: At this time all were the same as in my last blog except for the addition of a routine of daily homemade kefir, fermented veggies and kombucha which I added to my diet for their probiotic/gut health benefits.
Visit #12
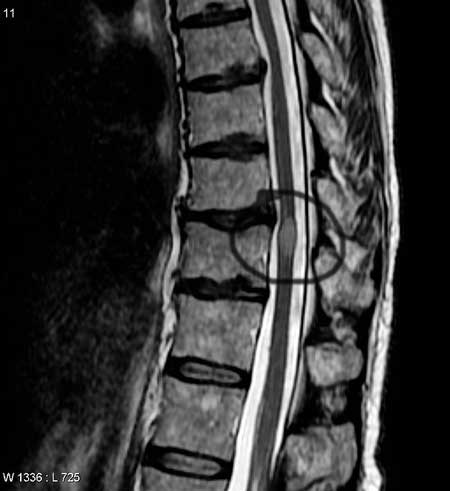
It has been six months since my last visit. The monitoring MRI’s I have every three months continue to show a stable lesion but one that remains enhanced with contrast, signifying inflammation, thus violation of the blood/brain barrier.
My original plan to have a friend drive me has fallen through, so I must fly alone instead. I am pleasantly surprised that because of compiled Rapid Rewards points from previous visits, my one way ticket will cost me a measly $12.00! Thank God for minor miracles!
My good friend and now third time Dr. P visit assistant, Cort, is meeting me there on his way back from the Stanford conference. Together, along with his inseparable canine buddies, River and Skye, we will drive back to Arizona.
Day #1 Travel (Sunday)
The usual long day from home, to airport, to Reno, to the hotel, is completed in about eight hours. I’m ready for bed as soon as I unpack. My appointment is not until 10:00 a.m. tomorrow which gives Cort plenty of time to get here from California should he come across a snag in his travel plans this afternoon. This is the last week in March and in this neck of the woods, weather is a factor that must be considered.
This particular room at the Hampton Inn has become like a second home to me – I couldn’t feel more comfortable. It isn’t long before I’m feeling drowsy – zzzzzzzzz.
Day #2 “Definitely No” (Monday)
Cort meets me for breakfast and after a quick “get acquainted” session with River and Skye, we are on our way. The plan is to meet with Dr. P this morning, have the usual labs drawn and then follow up with IV fluids for volume and hydration.
Today will be a prep for tomorrow’s discussion with Dr. G. Since Dr. P is the ME/CFS expert, I believe he and I are on a slightly different page than Dr. G, the myelitis expert. It is important that I speak to Dr. P first to get a feel as to what direction he is leaning.
As I wait for him in the exam room, I am reminded of how the myelitis and its resulting symptoms have worsened as I find myself fidgeting in my chair trying to find a comfortable position. Because the lesion is on the posterior part of my cervical spinal cord, the symptoms are mainly those of sensation rather than motor. These sensations range from extreme numbness, hypersensitivity, achiness, a feeling of constriction or stiffness, muscle spasms and the occasional stabbing pain – anywhere from the neck down, but primarily my entire back down to my tailbone, my upper chest and rib cage, the outer one-half of both arms including the last three fingers on each hand, my buttocks, and both legs and feet.
When I experience a flare – seemingly brought on by physical and/or emotional stress in conjunction with an ME/CFS relapse – the discomfort can be unbearable, short-lived (two days), but bringing me to tears, nonetheless. Now that it has been over a year since the discovery of the lesion, one can understand why I am anxious to start a treatment regimen of some sort.
When Dr. P enters, greetings are followed by his immediate mention of the mediastinoscopy and its relative safeness. I was prepared for this so he does not get the chance to finish his sentence. “I’m not going to do it”, I state firmly.
After my visit to the Mayo Clinic and the past year of scans, lumbar punctures and biopsies, I have decided I am not going to torture myself any further. I am done with doctors “just fishing” (the exact words used by two of the doctors I saw @ Mayo).
I make it known that a mediastinoscopy is not an option. I can see that Dr. P is clear as to where I stand. “How about this?” he says, “Would you be willing to do another PET scan? It’s been awhile and we can see if those lymph nodes have changed or if there are any ‘hot’ nodes that show up in a more accessible area where a biopsy would be less invasive.” I agree to this. Other than cost and radiation exposure, of course, the PET scan is a piece of cake, far from torture. I think it is a good alternative as I’ve been interested in seeing if those thoracic lymph nodes have changed since my PET scan in July.
Dr. P and I discuss my condition further. I express how I am concerned as to how the three of us are going to get on the same page. Dr. P assures me that we all are. I politely disagree. I ask him if Dr. G understands natural killer cells, my immunosuppression and my chronic viral reactivation. “Good question”, he remarks, in a way that suggests he understands the dilemma but doesn’t want me worrying about it. I bring up the fact that he himself is not convinced that neurosarcoid is the issue here and that even if it is, he has stated that he could not in his right mind, treat me with steroids even if Dr. G believes that it is the treatment of choice. He again tries to reassure me, “Don’t worry, I’ll take care of it.”
When you have been a patient of Dr. P’s long enough, you become familiar with his pattern. The gears are turning in his head and I can see that he has a plan. I know better than to ask him what it is. I have confidence that he understands my concerns and has already figured out how to traverse this complicated maze. He departs, saying that he will see me tomorrow. That is when the conference call with Dr. G is supposed to take place. Meanwhile, I go upstairs to rehydrate with two liters of saline. While there, despite the nurse juggling schedules, the earliest I can be fit in for my PET scan is Thursday.
Cort picks me up after my infusion and we stop for take-out burritos on our way back to the hotel, both of us spent. We had talked about taking a scenic drive around the lake, checking out parts we have yet to see. Lake Tahoe is huge – the drive around it takes a good two and a half hours. We decide to pass, once again using that all too familiar phrase, “maybe next time.”
Day #3 The (Almost) Conference Call (Tuesday)
Today I return to the office for the much anticipated conference call scheduled at 11:00 a.m. I have asked Cort to join me as a form of extra assurance to help me remember what is discussed, ask what is important and, in addition, have someone as a sounding board to bounce off ideas as I attempt to decide what route to take. It feels good to know that I have a knowledgeable friend for support.
I am still feeling a bit uncertain about the three of us – Dr. P, Dr. G and myself – coming together to discuss my myelitis. I sense that my role may be that of a mediator rather than a patient. I strongly believe this attack on my spinal cord is directly connected to my 23 years of ME/CFS and immune dysfunction. I feel I can assume, though not yet directly stated, that Dr. P feels the same.
At the same time, I am a patient of Dr. G’s who has been a very helpful and concerned neurologist, but who seems to be focused directly on the lesion as a separate illness, ignoring ME/CFS and the total picture. How will I juggle the two? This could put me in an uncomfortable position and because of that, my gut tells me that the conference call will not involve the three of us. My intuition is confirmed when Cort and I get to the office. The receptionist tells me that the call between Dr. P and Dr. G has already taken place and that Dr. G will call back at the scheduled time to speak with me (I am especially glad now that I asked Cort to join me!).
When Dr. G calls, Cort and I are lead into a conference room and left to chat with him by speaker phone. He is very upbeat and relates that he and Dr. P had an excellent conversation earlier. He agrees that another PET scan is a good idea.
When talking about treatment options, Dr. G speaks mainly about steroids, emphasizing what he said before, that without any confirmed cause or diagnosis, there cannot be a targeted treatment such as Remicade – but, he would still be willing to treat me empirically with high dose oral steroids (originally he had spoken of using IV steroids), then gradually tapering off to a dose that keeps the inflammation at bay. This would take place over a period of one year. A year?! Corticosteroids for a year?! I am surprised to hear this as I was under the impression that it would be for a lesser amount of time. (I immediately picture myself puffing up like a balloon. ?)
Dr. G speaks more about the immune process of sarcoidosis (he’s still convinced that is the cause of the lesion) and answers some of my questions, although I don’t feel like I can ask him the same ones I will later ask Dr. P, i.e., what about the fact that it is well documented that long-term steroids and ME/CFS are not a good mix? It is frustrating that after all these years, this illness is still so misunderstood that I must compile a separate set of questions for my neurologist than for my ME/CFS expert. Our conversation lasts for at least 30 minutes. I thank Dr. G for his generosity with his time. My mind is a blur and my body a wet noodle, but my day is not done. I still must meet with Dr. P – the meeting after the meeting.
This meeting with Dr. P strangely feels like a secret society of the people who “get” ME/CFS – still alienated from the rest of the world. But this is where the real discussion about my treatment option begins…
Dr. P smiles as he greets me. “Did you have a good talk with Dr. G?” he asks. I tell him I did, but once again I express concern. He tries to encourage me by telling me about the wonderful conversation he had with the neurologist. “You know, it was probably the best talk I’ve ever had with a higher-up at a medical institution.” He was beaming. “He even suggested that he admired what we are doing over here.”
I feel such incredible empathy for this man. For the past 30 years this ME/CFS warrior has battled for us. Is this the only time he has felt validated by a physician from a university medical school outside the field? It is sad, yet I am “honored” to be the index patient responsible. It brings purpose to my suffering and I can find some consolation in that. Dr. P then adds, “We both agree another PET scan is a good idea so get that done and I’ll see you after the results are in to discuss what to do next.”
Off I go, barely able to think let alone walk or talk. Needless to say, our scenic drive gets put off another day.
Day #4 R&R (Wednesday)
Nothing to do today but rest. Because PET scans measure metabolic activity of cells by their glucose uptake, today I must be on a high protein, low carb diet. The frig is stocked accordingly. With some light snow falling, I’m comfy and warm spending the day in bed.
Day #5 PET-Nap (Thursday)
In order for my cells to be “starving” and able to absorb the radioactive glucose needed to expose any hypermetabolic activity, I must fast this morning. Luckily, my appointment is early. Cort and his canine sidekicks drive me to Reno for the test.
After the glucose is injected and I’m left to rest and let it “soak in,” I am then placed in the machine where I am slowly scanned, head to knees. The scanning takes about an hour during which I find myself dozing off. You know you have gotten way too used to these tests when you find yourself so relaxed that you can nap! ? Each time I awake I jerk. Worried that I am ruining the images, I express my concern to the tech, who assures me all is well.
When the PET scan is done I’m ushered to a room down the hall to complete the chest CT which almost always accompanies a PET. This test is quick but not without its issues as it involves the injection of an iodine contrast that makes you feel like you are wetting your pants – it’s very strange.
All done, it’s now lunchtime so Cort and I grab some grub before we head back to the hotel. I have reached the bottom of the energy barrel but I still have at least one more day of seeing the doctor along with a two day ride home.
I am able to relax the rest of the day but am hit with a dilemma before bedtime. Cort is going back to Reno to spend the night at a friend’s home. Because of his multiple chemical sensitivities he is having trouble tolerating his hotel room and has reached his limit. He says he will be back in the morning to get me to my 10:00 a.m. appointment. There’s just one problem: he can’t find his phone. I don’t think much of this as it has happened before. He usually ends up finding it or, on one trip here last year, my detective work uncovered it, so without much concern, off he goes.
I figure all is well but it isn’t minutes when my phone rings and it’s Dr. P’s office. The doctor wants to see me early – at 8:30 a.m.! Now what?! Just in case Cort finds his phone, I leave a message for him, but time goes on and on and no return call. I must go to bed even though I have not heard from him. My only choice is to call Skip, the local driver I hire when I am up here alone. I explain the situation to him after which he says he will pick me up at 8:00 a.m. if I don’t hear from Cort. Whew! I’m lucky to have secured a ride with so little notice even though it will be an added expense. At least I can go to bed and rest assured that my bases are covered.
Day #6 Vibrating Snow, PET Results and Treatment Plan (Friday)
I assume that Cort has not found his phone as there are no messages on mine. I go down to breakfast and return to my room to wait for Skip. A light snow fell last night and about an inch lies on the ground.
At 7:15 a.m. I am surprised to hear a knock at the door. Who could that be? Peeking through the door lens, I am shocked to see Cort – all 6’ 6” of him! ? As I let him in, he tells me he thought it would be smart to get here early just in case the weather should worsen. He has no idea my appointment is now at 8:30! Immediately I call Skip and am able to cancel. Yea, my buddy has come through again!
I sit in Cort’s SUV as he makes a final search in the hotel for his phone. Looking at the pine tree area surrounding the parking lot, I remember the last time I saw him using it – he was walking in that forested area in front of the car while letting Skye and River stretch their legs. Immediately I pull out my phone and dial his number. Exiting the vehicle, I think I hear something. As I walk toward the trees, I am positive that I hear a vibrating sound. I smile as I see the spot where the pine needles dusted with snow, are shaking. Detective Corinne does it again! What are friends for – each having done the other a favor already this morning. ?

Would the pathogens in Corinne’s system come out of the woodwork once her immune system was suppressed – or would she simply feel better?
A happy Cort, whose soggy phone surprisingly still works, drives me to Dr. P’s on clear roads. I am anxious to see the doctor and am reviewing my notes when he comes into the exam room. First we discuss the fact that the PET/CT is the same as it was when taken in July – tiny, slightly hypermetabolic lymph nodes in my chest, but nothing easier to biopsy. There is one, however, in my armpit that Dr. P says he would consider only if Dr. Lipkin had funding to study tissue at this time – “I wouldn’t put you through even that, just to have it sit in a freezer.”
Next comes the discussion regarding Dr. G’s strategy: Long term, high dose steroids. But once again, Dr. P expresses concern that he could not, in his right mind, treat me as such, fearing cancer and other havoc on an already partially immunosuppressed immune system.
Some of my labs have returned and they are sitting next to him on the counter. He turns to them saying, “The timing of this is significant. Look how high your EBV (Epstein Bar Virus) titers are. I believe you should try the antiviral, Vistide. If you can return here for two weeks, I can get you started and if you can figure out a way, you can continue it at home. You don’t need to decide right now. Think about it and let me know.”
I am overwhelmed with mixed emotions. I have asked Dr. P for over a year to put me on a stronger antiviral (I have been on Valtrex for three years), but he never seemed to want to go in that direction. Whether it was the harshness of oral Valcyte or the toxicity and difficulty with the logistics of IV Vistide, I was never really sure, but those who know Dr. P know that he has a reason for everything. His reason one month may not apply to the next. As he learns more and tries new things, his plan and strategy change. What may seem haphazard to me, makes total sense to him. Whether it’s medical science or medical intuition, I have put my trust in him but at the same time, I must make my own decisions, taking finances and other things into consideration.
He encourages me in saying that there have been a lot of people Vistide has helped. His hope would be that if we could lower the viral load enough, we could calm down the part of my immune system that is attacking my spinal cord.
The mixed emotion part is that sadly I am leaving another visit without a treatment plan.
Since the lesion was found, this is the fifth time I have left a doctor consult without immediate treatment, and we all know how difficult making these trips can be. Each one can cause a flare and worsening of my neurological symptoms, and each worsening seems to become permanent. I am saddened to think of how hard I had to push myself through this visit and hate to think of the effects the resulting crash will bring. And then to think if I decide to do Vistide, I will have to pack up and do it all again. But at least this time, I leave with a treatment option – two, in fact – even though I have put the high dose steroid one on the back burner.
I leave the office hopeful, in a way. I have a lot to think about and a lot of logistics to work out if I am to attempt to get Vistide set up at home. My medical life…..a full time job!!
It is relatively early so this time Cort and I take an alternate route back to the hotel that covers a section of the lake we’ve never seen. We get a chance to see Squaw Valley where the 1960 Winter Olympics were held – the torch’s eternal flame burning. This makes my day, I am one happy camper! ?
Day #7 and Day #8 (Saturday and Sunday)
Dr. P and his research coordinator, Gunnar, want to take Cort and I to lunch so we stay an extra day. Even though I am a “dead woman walking”, this gives us a chance to say goodbye to Gunnar who will be going off to medical school in August. And, of course, Dr. P thoroughly enjoys conversing with Cort and vice versa. As for me, well let’s face it, I seldom get a chance to socialize so this is a treat.
As we eat, the snow begins to fall so we must hurry to beat the storm. If we head east we can stay ahead of it until we reach a lower elevation. We hit the road by 2:00 p.m. which only gives us three and a half hours of drive time before we must stop for the night – exhausted. This then makes for a long drive on Sunday, and I do not get home until 9:00 p.m.! I haven’t seen 9:00 p.m. in a car for 20 years! I have pushed it to the max.
As I think about how I am dearly going to pay for this, I also have to take into consideration that five years ago, before I got the chance to see Dr. P, I was bedridden seven to ten days out of the month – not nearly as functional as I am now. I could have never made a trip like this. Yes, I am struggling with this myelitis, but I have to stay positive, focusing now on the next step….Vistide?
Conclusion
No surprise – my crash was a free fall. My spinal cord flare came like it usually does, at night, my body feeling like it’s on fire from the neck down, the burning neuropathy pain that most may feel in their hands and feet, but now occurring everywhere, with nothing to do but lie there and pray. Fortunately, the worst lasted only two days but the resulting worsening of all the sensation abnormalities that make my legs feel like they are covered with cactus needles and wrapped in compression stockings remained at this new level. So the slow progression seemed to continue even though my three month MRI, once again, showed stability in the inflammatory lesion. Overall, I had two to three weeks of feeling sicker than usual.
Even when I recovered, I never fully did so neurologically. And with each flare, the same cycle continued. Having progressed to such a point I knew I had to make a choice. How far would this suffering progress? No one had told me about how bad this could get. So because the lesion had not improved, I believed I must be aggressive. I decided to pursue Vistide – giving it a shot before even thinking about high dose steroids.
I presented my case to my local doctor and thankfully, he agreed to write an order for the infusion center at the local hospital if I would go back to Dr. P’s to see if I could tolerate the potent drug and to set up my dosage. I was amazed that this could really happen – that I might be able to get Vistide at home!
By the time I got everything set into motion, it wasn’t until August when I was able to return to Dr. P’s. But this time it would be to actually try a treatment for this spinal cord lesion. Vistide, a.k.a. cidofovir…better known as “chemo” by some nurses and patients…or as others have been known to call it, “gasoline” (?)… is what I will now refer to as H-O-P-E!
(Medication changes: I began low dose naltrexone (LDN) w/ a script from my local doc in June, hoping to help with the neuroinflammation and pain. I started @ 0.5mg and slowly titrated up to 3.5mg by August, jumping up in 0.5mg increments. (I got nauseous if I increased more than 0.5mg at a time). I was told by Dr. P to cease taking Valtrex before I came up in August to begin the cidofovir).
Next blog…tackling Vistide…
‘Til next time…feel good!









What an arduous journey! Cort, so glad you could be there with so much help and support. The best of luck in treating this mix of problems!
I’ve been following your reports with interest (as yet another neurologist) and empathize with your pain (both physical and emotional) throughout your ordeal. I thought that I’d throw my 2 cents worth in, to see if there are some other options to help achieve a diagnosis to the origin of your spinal cord lesion. Do you know if you have had blood or spinal fluid tests for ‘NMO antibody’ (AKA aquaporin-4 IgG), to look for another autoimmune spinal cord disease other than M.S. and neurosarcoidosis? The other test I was wondering if had been done was an MR spectroscopy scan of the cord lesion. This uses the MRI camera to analyse the chemical composition of the cells in the lesion, and may be able to tell the difference between a lesion of inflammation/demyelination, vs. a spinal cord tumor.
Best wishes for answers and recovery!
Thank you for your suggestions.
Yes, NMO was the diagnosis I received initially from a local neurologist who then suggested I get tested using the Mayo Clinic lab which evidentally came up with the test. I tested negative for both plasma and spinal fluid. When this neurologist suggested that the IVIG I had been on may have affected the results I retested after having been off IVIG for months…I still tested negative. I also had a complete and comprehensive eye exam that scanned my optic nerve to determine if there was any inflammation and everything was (thankfully) normal. (This is all in an earlier blog in detail).
I have not done a spectroscopy scan however I was told that because of the enhancement with contrast, inflammation is a given and hence it is called an ‘inflammatory lesion’. I would assume that because it has not changed in size in two years that it is not suggestive of a tumor. I have also had CSF tests done which have not supported tumor/malignancy.
The reports by the radiologists always refer to it as a lesion suggestive of demyelination.
Thank you again. I will ask about the spectroscopy at my next appointment however I do not think it will give us a cause. The idea of a biopsy of the meninges/spinal cord had come up but, of course, no one really wants to do that if not completely necessary.
Wow, I am so fascinated by this whole story! I hope I can read the next installment soon. I’m with you totally in this story, and hope and pray that this new treatment happens soon, and that it is a success.
Corinne,
You are, indeed, a warrior. Also very blessed to have such diligent and caring providers, as well as friends, in your corner. God speed with your continued journey to wholeness.
thank you! Yes, I am blessed!!
What a story Corinne – I’m so glad you’ve finally got a treatment and so hope it helps you. Thank goodness for Cort too.
i too visited the Mayo two times in the past two years with the diagnosis of CSS (as they call it there) Fibromyalgia. At the time that was the main finding except a small lesion in my brain. I had a flight back before I could get into see the neurosurgeon. I did get an RF Procedure while there in hopes it would help with the nerve pain developed from a rare herniated disk at the base of my brain stem (I have in addition 2 in my lower back and 2 lower levels of my neck, spinal stenosis, occipital neuralgia early degenerative spine disease and a few other fun things) they consider this secondary FM due to trauma to the head- the lower back pain is child’s play compared to the constant pain in my neck) When I went back to the Pain Rehabiltation clinic a few months later for a 3 week program specially geared towards CSS FM patients- they refused to allow me to see any doctors as they feared it would “disrupt” the program. They wanted us to stop the “doctor chasing” saying this is what it is- nothing more- that my neck was “essentially” stable so we needed to concentrate on how to live a better life with this disease. I understood in a way but was pissed in another being that I was there by myself – I live in Tulsa and the Mayo I visited was in Jacksonville, FL. Anywho- what I was getting to was that although my response to pain had changed in a good way and I became more active- some things seemed to get worse. Things were very stressful at home/ I was going through a divorce- him moving to a different town leaving me in a situation of taking care of my two younger boys, doing all of the shopping, cooking, cleaning, showing the house we had to sell at a moments notice, getting the boys at two places at once, then finally inspections, closing, finding s new home and having to move primarily by myself two times in 3 weeks because the houses couldn’t close at the same time- THEN moving into a house that needed to be remodeled to be proper to live in. So that was a 6 month process that I finally said enough is quite enough. After several meltdowns and massive pain / the stress involved – I guess my body just gave out. I started to lose a lot of weight- at 96 pounds I could barely function and was horribly fatigued and nauseated constantly, had a hard time swallowing, peeing, everything felt like it was breaking down. So I go to my PCP And he decided to test for EBV AND HIV. Thankfully the HIV WAS FINE BUT the EBV titers wee so high- the said they stop counting at 600 and one branch was at that level the others were in the 300’s/ also high. Also positive for CMV. The doc noted and diagnosed me with ME/CMV at that point but months later- still not an infectious doc to treat here. So interested in these meds and would love to mention to my PCP this week. Fun part is- I Had just started going on short walks and at home pilates and was really trying to get active for the first time in years- only to crash later.come to find out – the release of endorphins (exercise – good or bad excitement – sex) are not too great for us Fm peeps! Great. Meanwhile I notice a pretty Rapid weight gain began, I had sugar cravings like crazy which usually isn’t me thing, carb cravings- usually not my thing- pain started to worsen, depression really hit, couldn’t exercise anymore – besides more sweets everything was about the same yet the weight kept coming- even gained after eating only s protein bar only in a day- gained another pond. So now I have gained 21 pounds in a month and a half! I mean- 95 lbs was too thin but this is crazy. Woke up yesterday and my face was swollen up like a ballon! Is this common with the onset of ME/CFS? I mean, everything else is more important but this was the cherry on top not being able to fit into my “fat jeans” very well. I Need To get this figured out. I feel like I can’t tolerate it anymore. So
Exhausted I have a hard time working – I own my own business and am a single Mom. Any insight would be wonderful. Don’t know what to do, who to see. No specialist in that field around here I know of. Seems like it’s ALL a big question mark to the docs as they aren’t familiar with any of this. I want mention the “chemo” treatment – maybe that help
A little. Take good care- deb
Ahhhh Stress, the ME/CFS/FM killer!! I too had gone thru a ton of it when this hit. But how do you avoid life? My lesson was to just learn how to moderate my reaction to it. Though it cannot work 100% of the time, but it truly helps.
The high EBV and CMV titers do not surprise me at all. Perhaps you could start with a milder antiviral like Valtrex?? I had a increase in function and well-being when I started on that three years ago.
As far as weight…almost everyone I know with FM has had issues with weight gain. I do not have an FM diagnosis. I have always had a problem maintaining and gaining weight…I am thin and at one point, 10 pounds less than I am now. I truly had to focus on gaining weight so I didn’t look and feel like I was wasting away. I think some of it has to do with the state of dehydration most of us are always in (I gained weight with the help of IV fluids) and the fact that our bodies are working so hard to fight these reactivated viruses 24/7.
I wish you the best of luck. My prayers go out to you.
Corinne
Have you had your thiroid checked?
Yes, several times. A complete panel of T3 and 4, free T3 and 4, etc, etc.
Hi, Deb
Do you know of any doctors in Tulsa that treat or are knowledgeable of CFS/ME? Do you mind sharing who you see?
Thanks you, Sally
Hi, Deb
I’m in Tulsa too, are you able to recommend me any doctors?
I’ve been dealing with CFS for 13yrs and needing help.
Thank you,
Sally
Sally, did you find a doc in Tulsa? I’m looking too.
Sending love and a prayer your way Corinne! Sometimes the going gets rough and it can be especially hard when Dr’s don’t “get it.” We’re all in this thing together!
I’m surprised to hear that long term steroid treatment was suggested. Did the doctors go in to depth about the potential side effect of this? It can cause Cushing’s disease! The last thing she needs is to start upsetting her endocrine system.
In one of my previous blogs I mentioned that DrG said that his experience with these type of lesions is you have to ‘hit them hard and hit them long’ in order to get them to go away and stay away…otherwise they will just return. That is his experience with his myelitis/sarcoid patients.
Sending up prayers for you Corinne and for all of us battleing this disease.So nice of you Cort to be their for her and thank you Cort for all you due in keeping us all informed so well.I cannot wait to here if this Drug Vistide will help Corinne.I think i have read about Vistide in your reporting or some where else.I have a friend who works with someone in the medical field that also has ME/CFS and who is also taking Chemo here.I hope to here the outcome and i pray that it will be good news
I appreciate all of your support and especially the love and prayers. I thank you from the bottom of my heart! I promise to update you soon. 🙂
Thank you for sharing this latest visit and especially your attempt to have an equal three way conversation with two physicians.
I’m in the UK and I tend to envy the power the patient has with the US system – in that you can vote with your feet and move to another MD. However, having read this update from you, I can see that this doesn’t make any difference if none of th MDs you see are talking the same language.
We have the same system here in the UK with our quickly dissolving NHS in that I go to see a neurologist (a very bad one who has been complained about many times), the only CFS/ME referral available is to a nurse practitioner who managed to write a three page report to my GP (PCP?) after a ten minute consultation.
I wait eagerly for Cort’s updates as they come. I do believe that however bad it is in the US, it is still worse here. No research that I am aware of and I am constantly searching. BTW, I have a diagnosis of CFS from 1994 and a fibro diagnosis from around five years ago.
So felt for you around the exhaustion of travelling. I had a month in bed after just a 500 mile each way trip.
Sorry if this doesn’t make much sense, but all I am trying to say is thankyou. Prayers coming your way.
Christine
You make perfect sense… thank yous and prayers always make sense 🙂
Blessings on your journey.
Corinne
Praying the Vistide works for you Corinne! Thankful you have such great doctors and hopeful these medications will bring you healing. Sending my love and prayers to all who are suffering. xo
Corinne,
I’d like to offer suggested reading on long term steroid use. I always like to make informed decisions. Here is one link that can provide some info for you. I wish you the best with your treatment.
http://www.hss.edu/conditions_steroid-side-effects-how-to-reduce-corticosteroid-side-effects.asp#.VNytEPly5bI