



Everyone comes to a disease with their own preconceptions. That fact never seemed more true than in this Canadian fibromyalgia brain study. The researchers asked a good question, got a good answer and then made an interesting interpretation.
Although the interpretation may leave something to be desired the finding was fascinating and potentially important for FM patients and possibly people with ME/CFS as well.
The Study
Clin J Pain. 2015 Sep 3. [Epub ahead of print] Basal Ganglia Perfusion in Fibromyalgia is Related to Pain Disability and Disease Impact – An Arterial Spin Labeling Study. Shokouhi M1, Davis KD, Moulin DE, Morley-Forster P, Nielson WR, Bureau Y, St Lawrence K.
The Canadian researchers wanted to know if reduced brain blood flows in FM were associated with a range of symptoms. Those symptoms included pain (visual analogue score (VAS), pain disability (Pain Disability Index – PDI), overall impact (Fibromyalgia Impact Questionnaire – FIQ), catastrophic thinking (Pain Catastrophizing Scale (PCS) and anxiety and depression (Hospital Anxiety and Depression Scale – HADS).
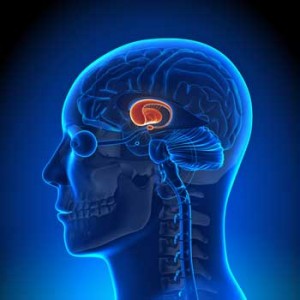
A similar basal ganglia dysfunction appears to occur in FM and ME/CFS. Attempts to explain it differ dramatically.
The study found that reduced blood flows to one part of the brain – the basal ganglia – were highly correlated with measures of disability due to pain and the overall impact of FM (FIQ). (Note that the indices of catastrophic thinking and mood were not relevant.)
Situated in the center of the brain the basal ganglia is associated with a variety of brain structures – the brainstem, thalamus and cerebral cortex – that are of great interest in both FM and ME/CFS. The basal ganglia is a center of dopamine production and is involved in such diverse functions as producing “reward” and regulating motor activity.
How to Turn a Physiological Result into a Psychological One
How were the low blood levels in the basal ganglia causing the increased disability due to pain and overall impact in FM? The authors first conclusion was that they weren’t. In fact it was the other way around. They suggested that the low blood levels in the basal ganglia reflected “maladaptive behaviors and hypervigilance”.
That was an interesting conclusion given that neither of their primary measures of maladaptive behaviors (catastrophizing or anxiety/depression) were found to be relevant in this study. How did they get beyond that problem?

The authors proposed that maladaptive behaviors were behind the low blood flows to the basal ganglia in FM.
A multiple regression analysis that found the FIQ scores were more highly correlated with anxiety and pain catastrophizing than with disability caused by pain allowed them to interpret the FIQ scores in a psychological manner. They also found a “trend” – a non-significant result – correlating the catastrophizing and anxiety scores with low blood flows in the basal ganglia.
The authors, thankfully, noted that an alternative to the maladaptive behavior explanation existed. The reduced basal ganglia activity could actually be the result of basal ganglia problems. They noted that one study suggested reduced dopamine activity in the basal ganglia was, in fact, present in FM.
They also noted that given the basal ganglia’s role in regulating movement that reduced basal ganglia activation could make it more difficult for FM patients to move and be active. They proposed that the dopamine/basal ganglia link should be investigated further.
In the conclusion section, however, the authors simply attributed the low basal ganglia blood flows they found to “fear of movement” and behavioral issues. They highlighted a fear of movement hypothesis which proposes that the degree of disability present depends on whether a patient decides to confront their symptoms or avoid them. Their sole treatment suggestion was cognitive behavioral therapy. The conclusion to their abstract simply stated
“These CBF findings may reflect differences in behavioral and psychological responses between patients.”
The idea that some sort of disease process may be impairing dopamine activity had disappeared.
How to Turn it Back Into a Physiological Result
But was it really gone? It’s true that catastrophizing and anxiety can increase pain levels but are they the sole determinant of pain in FM? The authors provided no evidence that either can impact basal ganglia functioning. Other, very different explanations for the basal ganglia dysfunction found do exist – and in a closely related disease.
Andrew Miller’s studies have found reduced basal ganglia activity in both chronic fatigue syndrome (ME/CFS) and people with hepatitis receiving interferon injections. These studies suggest that inflammatory cytokines, not maladaptive behaviors are the culprit.
Miller’s studies indicate that interferon therapy causes dramatic drops in basal ganglia functioning and dramatic increases in the fatigue, pain and other symptoms associated with “sickness behavior”. The similar basal ganglia/ dopamine findings found in ME/CFS and fatigued interferon treated hepatitis patients strongly suggests the symptoms and basal ganglia problems in ME/CFS are associated with immune activation.
This suggests the basal ganglia problems showing up in the FM study could be the result of inflammatory processes – not maladaptive behaviors.
To put it another way the trend towards maladaptive behaviors the Canadian researchers found could be the natural result of inflammatory processes; i.e. sickness behavior – in FM patients. It’s notable that the effects of dopamine reduction – reduced activity, reward, pleasure, and increased fatigue – fit sickness behavior to a T.
The Neuroinflammation- Microglia – Dopamine and Pain Connection?
A recent study neatly tied neuroinflammation – a subject of great interest in ME/CFS – to microglial activation and finally to dopamine reductions.
This study, which was described as “paradigm-shifting” found that neuroinflammation
- increased the growth rates of microglia cells which then
- inhibited the release of dopamine.
The clincher came when a drug that knocked down microglial activity – increased dopamine levels as well. The neuroinflammation – microglia – dopamine connection appears to be well-established in animal models.
The drug used was minocycline – find out more about it here: Drug Repurposing I: Antibiotics to Reduce Microglial Activation in ME/CFS and Fibromyalgia?
The Opioid Dopamine Connection
“For over 20 years, scientists have been trying to unlock the mechanisms at work that connect opioid use, pain relief, depression and addiction. Our findings represent a paradigm shift which has broad implications that are not restricted to the problem of pain and may translate to other disorders.” Catherine Cahill
Interestingly, a similar process may be occurring in people with chronic pain who unsuccessfully use opioid drugs. It turns out that opioid drugs stimulate the release of dopamine in rodents in acute pain, but fail to do that in rodents in chronic pain. For some reason the opioid – dopamine connection gets turned off in chronic pain states.
The finding suggests that the activation of dopamine – a feel good chemical – plays a major role in the effectiveness (or ineffectiveness) of opioid drugs.
Next Steps
What’s needed now is to establish that neuroinflammation is present in both ME/CFS and FM. If that’s accomplished then the dopamine link to neuroinflammation induced fatigue and pain has already been mapped out.
Are some pieces coming together? One scenario could help explain how the Lipkin/Hornig/ CFI findings of up and then down activation of the immune system works in ME/CFS.
First, an infection triggered immune upregulation sends the microglial cells humming – causing reduced dopamine release in the basal ganglia. Over time the untreated infection causes immune cell exhaustion at least in some patients. The resulting immune depletion should give the patients some relief, but Miller’s hypothesis suggests the reduced dopamine levels leave the central nervous system ultra-responsive to lower levels of inflammation. Even if the inflammation has died down the system is still reacting to it – and the disease lives on.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!




Hi cort I you can please e mail me I have some very important information for you. Thanks Jimmy jalite@comcast.net
Hello another virus to look at is shingles
I can see this as totally realistic in my case because there was no injury. As a Researchers in Holland stated there are a in their findings 4 “kinds” of Fibromyalgia. This model fits me. The type A never sick, only had an antibiotic need illness twice in my life, gets Human parvovirus B19 Spring 1990, then has aggressive fast HPV Cervical cancer January 1991. I can remember the September day 1991 driving to work feeling achy, flulike, and thinking I had just started feeling myself in June after only taking 9 rounds of chemo in February. Finishing competing my Child Development Associates, my husband had graduated seminary, we(I)had built our first new home, 2 young children 6 and 8, piano and soccer, sang in chior, did solo’s, for weddings and funerals, children’s director, Sunday Evening Adult Lecturer, Full time Family Support Worker, home made suppers every night, spotless house. My bi-vocational pastor husband only had to work and minister, I made him look wonderful. I should kick myself. I got diagnosed after threatening my doctor one day either you find out what’s wrong or I will blow you away right first then blow me away 1993 when I had to pull over because I was spasmodic too bad to drive. My husband had to interrupt his life and come get me and at 35 and few thousand tests later “even though you present symptoms typically of those with MS you have no lesions and all your tests are normal except one you have inflammation in your body of unknown origin therefore you have Fibromyalgia. They sent me to a Rheumolotologist who poked in places I yelled at the right times and I wasn’t sleeping, he concurred Fibromyalgia.
Today, as I sat and listened to two women in my Pain Management Specialist try to out whine the other on their pain scale because they had “Fibromyalgia” when one sounded like she actually had CRPS and the other a opiate problem. My
“disease” whatever it is, is beyond the scopes of the beast itself. I knew I was just going to make my PMR Dr more angry, because I was going to ask him to treat my degenerative disc without higher opiates. I refuse to go beyond hydrocodone 7.5, because I flip flop between really sensitive to drugs to normal. His Spinal blocks didn’t work last time and since insurance won’t pay like they used to, he won’t be making an extra $16,000 before Christmas. I can’t come out of pocket $4000 for maybe. Antiflammatories and special compound pharmaceuticals, one kills the kidneys the other, again $150 for 60 applications for me, but if my vet prescribe for Ziggy my 100 pound boxer, $65, same EXACT MEDICATION BY EXACT COMPANY! I live in Georgia going outside the box, my son, who when he had to choose between $100,000 year for med school or scholarship for continuing his Nurse Practitioner, said eff it, Nurse Practitioner, said smoke pot, mom. I have decided to say eff it, to. I am trying CBD. But the legal best. Not advertising the brand hear or anything. I have MS, Lupus, Fibromyalgia, and ME, symptoms but no antibodies just all the goodies. I have 2 good hours a day @ 5-6 pain level. I don’t effing whine. I walked around with a fractured spine for 3 days at 12 years old because no one believed how I hurt. We were moving, my sadistic abuser mother didn’t believe for 3 days 5 fractured vertebrates. So I learned never show your under belly. No, I didn’t come from an alcoholic at risk statistical nightmare background. Quite the stone cold, wealthy, church going opposite, just Mommy had rage problem with me, because sperm donor #1, didn’t want us, and I was the tarnish on the halo, which fits me into another Study Vagal Nerve Damage from repetitive blows to the head, good thing I have a didactic memory and high IQ.
So sorry to hear all that. I’ve had a wonderful life in comparison, but am a natural-born complainer, sad to say. Praying for you, sis!
Very interesting article and recent studies. These results suggest that acetyl tyrosine will be helpful for people with CFS/FM (dysbiosis). I have found acetyl tyrosine to be very helpful, and this recent science perhaps explains why.
Acetyl tyrosine works better in combination with methylfolate, P5P and niacin, which help to convert it into dopamine and other neurotransmitters.
How is acetyl tyrosine different from L Tyrosine? I know L Tyrosine effects dopamine and supports the thyroid. I can only take it for a number of days and then I notice myself feeling anxious…which is not something I naturally feel
Prashanti, I’m guessing that the anxiety and perhaps aggitation you feel when you supplement with L-tyrosine might be from over-excitation of the thyroid as they are the symptoms of Hyperthyroidism?
Thanks.
Dan, I find that phenylalanine makes a huge difference. It is converted to dopamine, etc.
I had read that it is converted to tyrosine and tried supplementing with tyrosine to save that one step having to take place. It didn’t work. I normally have 4 phenylalanine tablets and I tried 2 instead plus 1 tyrosine capsule. At the end of the week I had absolutely no energy. I think the problem was the tyrosine. Perhaps it was too strong for me and my body reacted to the extra amount.
Anyway, I’m sticking with the phenylalanine at this point. I’m not sure what it does that helps. This article suggests it’s the dopamine. I’m also aware that it converts to adrenaline. Both of these could help.
After a recommendation on this site a month ago, I have just had a test for all the amino acids so I can see if I am short in any others. I am awaiting the results.
Diane
Diane
I tried l-lysine which also puts dopamine back, and WOW the pain has gone. Muscle pain down 90% (I also have CFS). Every day getting more and more energy back.
Chris
Hi Chris
That’s fantastic that you have found something that works! We all seem to have different deficiencies and it’s a bit of trial and error until we find what helps. For me, the phenylalanine was the big breakthrough. The results of my amino acid testing showed my lysine levels as 16.8, when the normal range for females is less than 14 and for males is less than 12. I seem to be okay on that. However, the one that was really low was taurine at 21 (females should be 30-192 and males 38-295). I am now taking one taurine tablet a day and will discuss it on Monday with my osteopath/homeopath.
Long may your energy levels rise and your pain levels drop!
Diane,
Where and how did you get your amino acids tested? I started taking Lysine, inspired by Chris’ post. We’ll see how that works for me.
Update on my taking L-lysine, had a bit of a down moment when it seemed to have stopped working. So I stopped taking it for a couple of weeks. Then read somewhere that i should be taking around 4 tablets to start instead of the 1. So upped the dose and nerve pain now gone. Now I am managing to slowly increase my walking and also have a puppy! Can’t thank the article enough for making my life better after 30 years of suffering. Very sad though that everyone i tell just takes no notice. Lot of negative people around.
what drug was used in the study to lower inflammation in the basal ganglia?
I know it’s been several years but I’ll add my experience anyway: I also find that Phenylalanine is gentler than Tyrosine. Tyrosine seems too ‘raw’, too close to dopamine. I’m struggling to figure it all out as I don’t seem to tolerate serotonin enhancing supplements and drugs on the one hand, but also have a problem with anything that boosts the dopamine too forcefully. The two work in tandem in some bizarre way. Histidine helps balance things out as it’s a prominent neuromodulator, but other substances are needed also. Working it all out is hellish – it’s infinitely complex.
In my own case, as I have often said on this forum; I gradually succumbed to Fibromyalgia while very fit and pursuing an intensive daily exercise program. I was certainly not “catastrophizing” about movement and pain levels, I was pushing on in denial about my loss of energy, increase in pain and stiffness, and loss of flexibility; wanting to think I was invulnerable because of all my dedication to fitness.
I think alternative hypotheses are going to far better fit my own experience, and I am glad, Cort, that you are dedicated to offering these in your critiques of unhelpful authors like the above.
The highly-rated naturopath Gary Moller certainly argues adamantly that undiagnosed and untreated infections are how fibromyalgia starts – possibly even oral/dental ones, which he says are far too common. In my own case, the first sign of problem, preceding the fibro pain etc, was in fact excessive need to urinate, and body hydration difficulties – I could not hold fluid. This problem gradually diminished (after the medical people said their tests could find nothing the problem) but the fibro symptoms started. It certainly makes a lot of sense to me, that initially my body was desperately trying to get rid of something, then perhaps “adapted” by storing toxins in the muscle tissues…..?
It may even have been an environment-related toxin that has never been established – but years later a hair mineral analysis test showed me sky-high in cadmium, for which I can think of no explanation. Cadmium is apparently notorious for not showing up in hair mineral analysis tests until it has already reached dangerous saturation levels in the body tissues, or when the body has started to flush it out again.
The cadmium level has since diminished, but it may still require a longer period of elimination than what the HMAT results would show, but consistent with the fibro, I also have sky-high levels of calcium that never seem to come down. And low magnesium levels that never seem to come up regardless of how much of it I take as a supplement. However, I do regard my condition as significantly improving with the complex protocols I am following, so maybe a future HMAT will show a nice balancing out of minerals. I just have not got there yet, and don’t feel I have got there yet – my pain symptoms have tended to shift around and I have got new symptoms even as old ones have diminished. Interestingly, this includes excessive need to urinate, all over again around 22 years after the initial problem! So it is as if I am winding my condition backwards through the whole past process. I am trying to stay optimistic.
Of course someone who has been suffering fibro pain a long time may well have something like “catastrophism” feeding back to the brain, but this does not mean that the “catastrophism” preceded the onset of pain and caused it, does it? Any more than some prolonged torture victim is guilty of “catastrophism” regarding their torture.
Not at all!
Have you tried magnesium glycinate? Start with 50mg for 3 days, then increase the dose every 3 days by another 50mg. This form of magnesium stays in the tissues longer than others. Hope it works for you.
From my own experience, I suggest testing your urine for excess acidity and eating a more alkaline diet if necessary. Also, search your abdomen for trigger points which knot up your abdo muscles and press on your bladder. Learn what perpetuating factors keep these trigger points maintained.
Phil –
I’m mainly a lurker (although I have contributed, and I want Cort to know the discovery of this site was almost as exciting for me as I imagine discovering why I have this damn disease/syndrome might be!)
But – and I know it’s off topic for this thread, (Cort please feel fee to move it if there is a more appropriate one) I just wanted to say that I had issues with hydration for YEARS before full-blown fibro. I remember downing litre bottles of water and refilling them constantly during the day, and wondering why other people could sit through meetings or lunches without the same need I had to constantly glug through my bottle.
At the time I surmised that I’d caused the syndrome myself by simply drinking too much water and allowing my body to get used to it. (It was the early-mid 90s when Coke and Pepsi bought up all the mineral water brands and started the urban myth that we were all perennially sub-hydrated and needed ‘at least 8 glasses a day’ or whatever it was.) But reading your comment has brought up a couple of thoughts:
1) Around five years ago when the pain started and the doctors first began to throw around the “F” word, I noticed that a crash/flare was always preceded by a couple of days of SEVERE thirst which was never satiated. This slowly disappeared as the symptoms became more regular and the pain and exhaustion and waking up feeling like I was dead began to take over and become a daily occurrence.. But I still drank around 3 times as much as anybody I know and driving around Los Angeles is always a problem because I have to find a place to pee all the time.
2)BUT… I’ve been recently seeing a cardiologist, testing out a theory that came up during my most recent visit with my rheumatologist. The theory appears to be flawed, as I feared, and we’re back to square one. But for some reason we got into the hydration conversation, and he told me to drink water to which I had added salt. Holy crap! Hydration issue solved! Of course I bought the fancy salt crystals from the Himalayas or whatever but later moved on to basic cooking salt and (of course) it works just the same. When i add salt I’m no longer thirsty (takes a while to get used to the salty feeling in your mouth which can be confused with thirst) and I actually feel like I have more energy (blood volume increased hence higher levels of oxygen to organs/limbs perhaps?) And my sleep is a lot deeper. I still have mac trucks driving over me during the night, but I no longer wake up at 4am unable to get back, and I certainly don’t get up to pee 4 or 5 times during the night like I used to.
Of course apart from those thing it hasn’t changed my fibro one bit. I’m still in pain, and although not bed-ridden, I will always chose bed over getting up if I don’t have to, and take tramadol to get through most of my days. But I thought it might be food for thought – I always thought salt was the great enemy.
Thanks for sharing that! 🙂
I crave salt.
Hey, great post, going to talk to doc about the monocycline and also supplementing my methyl folate with the amino acids and B vitamins….also recommend n acetyl cystine which is precursor for glutathione production…..but question – I have hypertension and take meds to keep it down – but still have the orthostatic intolerance and feel dizzy or faint when I stand up or move suddenly – not sure about adding salt! But I may try the “no salt” – anyone have any success here who also is hypertensive?
I read an article about putting salt in my water a year ago, and have been making my own “electrolyte” drink ever since. IT does seem to quench my thirst much better! I just use about 1/8 t salt and 1/8 tsp “no salt” which is potassium chloride, plus a capful of cider vinegar. I don’t bother with sweetner, as I like the sour taste (maybe due to a malic acid deficiency?) The article was about how to increase your blood volume. It seems that if I drink the salt water every day I have less dizziness when I move suddenly…
Check out some more resources on Increasing Blood Volume here
You mention less dizziness. That can be a sign of low blood pressure, which I’m guessing alot of us have. Adding the salt can raise the blood pressure.
My father was in the hospital 12 times one year, They couldn’t find out what was wrong. He just got dizzy and weak very suddenly. I had taken a class on health nutrition with a recipe for a gatorade type drink for hydration. I mixed it for him when he had one of the “episodes” and within minutes he was fine. The recipe is ROUGHLY 1/3C fruit juice, pinch of salt and fill the glass with water.
Three issues seem like they may be relevant to the health puzzle. I don’t know how we could find out. Perhaps someone had there has any information on them. When I get time and energy I will start to research more. If anyone has anything to share I would so appreciate it.
1- HYDRATION.
The hydration issue is very interesting. Several people have mentioned it. I didn’t think I related to it until you mentioned the salt in the water. I CRAVE salt. It seems to have no negative effects on my body.
2-OXYGEN LEVELS.
What effect does blood oxygen level and cellular oxygen level have on chronic fatigue/ fibromyalgia? I am using a tool that is used more often in Europe than the US to increase cellular oxygen.
3-CANDIDA
For me, anyway, I think I deal off and on with candida. It can totally rob your energy. I used Candex for it and it seems to work well. Yet it still comes and goes.
Alice, I find I need quite a bit of salt. My doctor recommended that I have it for low blood pressure.
Recently my sports therapist (to whom I go for a regular massage to get rid of muscle knots because of poor posture due to weariness) told me how to mix up a sports drink. I find having this once a week is enough.
Mix half a pint (or 250ml) of fruit juice and the same quantity of water. Add in a teaspoon of salt and a teaspoon of sugar. You need both of those. The sugar supplies glucose and smooths out the salt. In the case of exercise, have some before exercising, some during, and the remainder after the exercise.
I find I don’t get nearly as many foot cramps as I used to, since taking this. I also add lots of salt to my food.
Diane
Phil,
Excessive need to urinate : This was the first sign of neurological issues for my son ( age 5/ 1986) 2 weeks following lab documented Epstein- Barr infection. All of a sudden one afternoon – peeing 30 to 40 times a day. Irritable bowel followed that, then sleep disorder, needing to eat cereal at night ( blood sugar issues ?), pain in fingers/toes, depression, the whole thing. He had been a very healthy little kid to that point, and I was a stay-at-home Mom.
This whole scenerio would improve over months ( or years), then re-occur when he caught a cold virus. Professor Don Gilden ( Colorado) is an expert on Herpes virus infections of the CNS. Just search on line – you will find the articles, symptoms,etc.
So, I am also drinking and peeing all day long – putting out 3 plus liters daily according to study results. But my issues all began with an obvious neck/pelvis injury. Did a virus invade secondarily due to altered blood-brain barrier ?
Basal ganglia : The main blood supply to the basal ganglia is the middle cerebral artery ( internet sources). If you follow that artery ‘downward’ you find that the vertebral arteries ultimately feed the middle cerebral artery. Please read about Vertebral Artery syndrome. Importantly, the vertebral arteries thread through small holes ( foramina) in the lateral protrusions of the neck vertebrae. So, any rotation of the neck vertebrae, or displacement or congenitally small foramina, could potentially influence blood flow to the basal ganglia. MR angiogram is the only way to evaluate vertebral arteries.
Rotation of neck vertebrae is very common in scoliosis. FM patients have lost the normal neck curvature. (Research by Dr. Robert Katz. MD- reported at annual rheumatology meetings, finally published? ).
Andrew J. Holman. MD. Univ. of Washington, wrote 2 important articles for Fibromyalgia Frontiers : In 2005, “Dopamine: From Parkinson’s to Fibromyalgia.” Then in 2012, ” Why You Should Be Thinking About Positional Cervical Cord Compression.” My thoughts are : Not only should we be thinking about cervical cord irritation/compression, but also blood flow through the vertebral arteries in the neck. Lying down changes the spinal curves ( neurosurgeon Shokei Yamada). I suspect that somehow stresses the neck vertebrae and interferes even more with vertebral artery blood flow.
Also, the basal ganglia appears to be adjacent to a major brain ventricle where spinal fluid circulates downward towards the neck. So, abnormal circulation/drainage of CSF may cause pressure on the basal ganglia ?? Experts please comment.
Another forum member commented that her (and her child’s CSF/ME) began with a viral infection. She and her child responded to Diamox, which reduces spinal fluid production. Eventually, they weaned off the Diamox and remained quite well. This indicates that somehow viruses can change the fluid dynamics of the brain.
Thinking about my son’s situation – by he was so vulnerable to this virus that went through his preschool : He was delivered by suction. There were many indications that they injured his neck. Long story.
My contention is now this : We will never understand this illness until we look closely at : scoliosis, vertebral differences – especially at C1/C-2, vertebral artery flow, CSF production/ drainage from the brain. Most people are able to clear the viruses that seem to absolutely devastate us. Why ??? How are we different ? Immune system, yes, but again, immune system is so interconnected with CNS function. ( Many references to that )
Important source: Scoliosis and Spinal Pain Syndrome by Valentyn Serdyuk.
I appreciate what everyone has reported here – and thanks again Cort. What you are doing is so important. Onward.
Thats really interesting about opioids, as morphine and morphine derivatives don’t work on me. Just make me feel nauseous and more tired they have no effect on pain.
Me too! Can’t do opioids, get violently ill with nausea and just feel worse. Always wake up that way after surgery, etc. I always thought I was just sensitive and they gave me too much. Maybe something else going on. I had to scale way back on dose of naltrexone (even the standard low dose was about 4x too much for me and got so sick they took me to emergency thinking I was in cardiac distress). That is relevant because it works by affecting the opioid receptors on the immune cells……
Do you have any more details on adverse reaction to LDN ? It was very severe for me causing anaphylaxis. That was on a very low dose. Even a minor drop affected my breathing. I still wonder what the problem is.Sister takes it and it has been a miracle for her.
I have benefited significantly from fluoxetine treatment, and I’ve long thought it’s much more than treating depression.
As it happens, fluoxetine appears to dampen neuroinflammation and microglia activation:
http://www.erasmusmc.nl/erasmusjournalofmedicine/2787834/4729657/EJM07-PAG10-13_anti-infammatory-effects.pdf
Didn’t know that. Thanks Mathias…
I am so pleased that researchers are vigorously pursuing inflammation, specific causes (eg. viral load), and the affects of it’s acuity or chronicity on the brain!
An acute, sudden and severe onset flu-like episode was the onset of my journey with ME/CFS and FM. IV then oral steroids got me back to my life, but unlike the Energizer Bunny, I literally wound down over the next 3 months.
I was an active 39 yr old RN working full-time, involved in community, raising 2 tweenagers and life was wonderful. Since all specialists I’d seen had ruled out lupus, RA, CRPS, and all other sorts of auto immune issues, he said I should be happy “nothing was wrong”!
I literally had a faceoff – nose to nose, toes to toes – with my colleague and family MD before he admitted he had no clue what was at issue. Finally, an internalist diagnosed post-viral syndrome, and suggested it was likely CMV, EB, or some other retrovirus that had caused the initial “flu” and it had reactivated centrally causing the symptoms that had me bed-ridden. How wonderful to see that all these years later (>13 yrs) proper research is indicating he was on the right track.
Fortunately, I “recovered”. Unfortunately, I didn’t understand the importance of pacing or the risk of relapse. 3 bouts and 3 years later, I was diagnosed with ME/CFS, and 3 years following that, the internalist informed me that FM, not a strain, was the cause of my shoulder pain.
Unfortunately, 3 yrs ago fatigue and cognitive symptoms necessitated that I quit work. Insurers and pension companies continue to question if I am “disabled enough” to qualify for their benefits. I pray for the day a test will prove what we’ve been saying all along has a physiological basis. No one chooses ME/CFS and FM.
Like Mathias, I experienced tremendous relief of discomfort and moderate improvement of energy levels from the addition of Lyrica and duloxetine (fluoxetine’s little sister) once diagnosed with FM.
Over time the pain management stayed relatively stable, yet fatigue and cognitive issues began to worsen. At the urging of the pain specialist, I started CBD at bedtime and developed a more normal sleep/wake cycle and improved function.
Recently, sleep has become an issue again. I understand from a previously reviewed study that for us “lifers” (people that have had symptoms more than 3 yrs) that chronic inflammatory effects to the nervous system and brain are difficult to reverse. However, I have far less pain and am more able than many. I often wonder if treatment with IV steroids during the triggering illness in some way may have given me a degree of protection??
What a story Janis! I wouldn’t be surprised if the steroids did confer you some protection. If the Lipkin/Hornig study is right then immune activation early on plays a big role. I guess it depends if the immune system just got turned on or if it was protecting you from something.
What is CBD?
Cort, CBD is the “non-hallucinogenic” un-trippy cannabinoid derived from pot. THC is the trippy portion. So CBD is what I was prescribed to assist with settling, since it has a relaxing, drowsy effect without concerns for impairment.
I had to decide that it was more important to have good sleep now and quality of life since rest is so important, than be concerned about the fallout of potential effects of any of the prescribed meds on the brain. At least in my case, the gamble has been worth it in day-to-day living, although my hopes to feel well enough to work did not occur.
Thanks Janis….:)
Would be interesting to know how others have fared on fluoxetine. It took me from 50% of my former self to 90%, able to work etc etc.
I used to think I was just depressed, but now I think it acted both on depression and at a deeper physiological level at the heart of my CFS.
So, it’s just a theory, but I wonder if action on the brain / microglia is behind its benefits.
SSRIs are known to interfere with dopamine signaling in the basal ganglia and trigger EPS and movement disorders (theoretically low dopamine). I suspect that it’s dependent on genetics, also. I hope your improvement has continued.
https://www.karger.com/Article/FullText/447034
“Opioid drugs such as morphine are frequently used to relieve pain, but in patients with chronic pain they can be ineffective. The new study has now revealed why this might be the case.”
******************************
I believe many people with ME/CFS and FM are dopamine deficient. You need to restore dopamine stores in the brain that have become depleted, or dysregulated for pain drugs to have any effect. Tyrosine, protein and glucose helps the body build the neurotransmitter dopamine. To manufacture pain-killing endorphins you need a dopamine source. If you have nothing to work with (running-on-empty) to make pain-killing endorphins, all the pain medications in the world are not going to ease your pain.
Could you give us who are pretty much on our own some hints on how to increase our dopamine levels? I know chocolate helps me feel better, but I don’t need the caffeine (nor can I handle much of it), fat and sugar in it! I’m one of those super-sensitive people with multiple drug failures. They often do the opposite of what they’re supposed to, making me MORE anxious and depressed. Am having the gene testing done now to tell which psyc meds I need to avoid, instead of going by trial and error…I HATE being a guinea pig, and as I get older (am almost 60 and have had “chronic fatigue for 28 yrs) the time gets shorter…
I’m afraid I don’t know. I do remember that Miller said that dopamine enhancing anti-depressants are not necessarily the answer at all.
Like you, I found that chocolate made a huge difference to me, and for too long a period of time for it to be just the sugar rush. I was eating 150ml of chocolate a day!
Luckily I had arranged for my osteopath/naturopath to test me with all my supplements and I added in a block of chocolate. He laughed and said it would never help. He laughed even louder when he found that it did indeed make me stronger. However, it also had negative effects (sugar and dairy?) and so needed to be avoided. He then tested to discover which component of chocolate was helping me. It turned out to be phenylalanine, an amino acid that converts to tyrosine and dopamine and other things.
I now take dl-phenylalanine every morning on an empty stomach. Within less than a week I found myself smiling and even singing. I have been a different person since taking it. I would recommend that anyone who finds chocolate improves their physical state should try the phenylalanine. You will know within a couple of weeks if it is going to help. I initially took 3 tablets but now I take 4.
It took perhaps 6 months before I gradually stopped eating chocolate. However, I have recently started on the chocolate again. This time it’s more for flavour than for effect.
I saw my osteopath again last month and he recommends calcium citrate (not carbonate) to help with the phenylalanine and make it more effective.
As a result of a recommendation on one of these blogs a month ago, I have just had a test done of all my amino acids to see if any others could perhaps make a large difference. I am awaiting the results.
wonderful information
Where and how are you getting your amino acids tested?
Prashanti, I am in the UK and I googled to find a lab. I contacted Biolab in London. They sent me a sample bottle. I had to collect my urine for a full 24 hours and measure the amount. I then mixed it and sent them a sample bottle full. They will post out results. I had to give them the name of a medical practitioner to interpret the results. (I used my osteopath/naturopath.) They offered me details of a nutritionist if I had no one of my own. It cost me £91
I first heard about the test on one of these blog posts. Here is the link to the blog. You will find the answer to may particular query right at the end. There is information there for USA and Canada.
http://www.cortjohnson.org/blog/2015/07/23/17-years-a-naturopathic-fibromyalgia-story-part-ii/?replytocom=672221#respond
Thanks so very much. I am so grateful for you taking the time to check this out. This blog/website is such a blessing
Thanx so much for sharing this! I am def going to order some phenylalanine right away! How much Ca Citrate do you take? I quit taking Ca a few yrs ago because a nutritional chiro said I didn’t need it, but I ache to the bone when I get cold (just from air conditioning!) and seem to injure easily, so I think I must need it. I was on estrogen blockers for several yrs (after having breast cancer 10 yrs ago)which weakened my bones. I take Mg Malate every day, along with Cymbalta (altho the generic they switched me to last year doesn’t work nearly as well as the name-brand did) and Mucinex which I think each help some with the aches and pains. The severe fatigue and depression plus bad mood swings are the most disabling, tho.
I haven’t yet got around to ordering calcium citrate. I am slow to do things, I’m afraid, and it was only a couple of weeks ago that the naturopath said that was the better one.
However, only yesterday in the newspapers I read that studies show that calcium does not do anything for our bones! I wonder if that is because we have been taking the wrong form of it for years (the normal calcium being simply chalk) or if it does not help.
When I get some, I will have to experiment with dosage to see what helps. At the moment I take four phenylalanine tablets a day and I would rather not increase that dose. I like the thought of something else helping it.
As for mood swings, I have been quite calm since going on the phenylalanine, until 2 weeks ago when I did far too much (showing a friend around my city) and then became terribly moody. I am still close to physical weepiness if I do a little too much in the day, though my mood is okay.
Thanx SO much for sharing, Diane! I am the same way~will have the list of supplements I need to order on my desk for weeks sometimes before I actually get it done…I abhor the brain fog, depression and fatigue that make it SO hard to get much done. I work very part-time and have loads of stuff to do on this old house, but I get frustrated SO terribly easily even tho I’m a very intelligent, capable person! I know I have to pace myself, but some days I get almost nothing done. SO frustrating! It’s encouraging to know that there are still things I can try in order to feel better. It’s SO difficult to figure out on one’s own!
I do l-lysine from Holland and Barret – 1 tablet a day, amazing. Bit sad that I have had to suffer over 30 years, and now just 1 tablet has had the most amazing impact.
What dosage is the L-Lysine? I see they make a 1000mg and 500 mg. From what I could find it looks like lysine helps increase levels of seratonin. I know it helps with cold sores which are a herpes virus. Perhaps the lysine, then is also helping with virus in the body.
In just trying to put puzzle pieces together these pieces may or may not be helpful or meaningful: I have only had a cold sore twice. Both times it was after taking azithromycin for a lung infection. A friend, who is a nurse, said she had the same thing happen after the azithromycin.
I thought this article on amino acids for CFS was helpful:
http://humanhealthspecialists.com/integrative-health-arizona-newsletter/volume-3/issue-2/amino-acids/
Hi
Cold sores may be another use for l-lysine, however I just googled what increases dopamine, and found it was l-lysine, no mention of depression though?
The findings seem to agree with “The Marshall Protocol” google it, the thought being that it is bacteria (sorry if got this incorrect but please read it for yourself).
As for the dosage 1000mg just 1 tablet a day, I have to say that last Sept 2014 I had nothing to lose and after reading that the marshall protocol suggested antibiotics to treat CFS/ME/Fibro and lyme disease. I know I was bitten by a tick when i was 15 and then followed glandular fever and meningitis. (or more likely lyme disease). Been ill since then told had ME over 30 years ago, and no fibromyalgia.
Doctor laughed when I gave him the info from the web, and said where do you think you will get the antibiotics then not from me. So I found a natural alternative, collorado silver. Massive pain in head then realised the next day brain fog gone, daft as it sounds I said it felt like blood going into part of my brain. Since then I have used Pinella again brilliant results.
Still left me with mega pain and tiredness, now l-lysine has changed all that. To be honest Prashanti, I don’t care what its for, what my illness is called, to me I had nothing to lose.
Left to my doctor I would have continued to suffer for another 20 years, now I am going to live life to the full to make up for the passed 30 years of hell.
sorry the above should read NOW fibromyalgia
Thanks so much, Chris. I like your outlook and wish you the best. I’m trying anything and everything, so I appreciate the specifics. I’ve had CFS for over 20 years…sometimes not as bad as others, but I did have to quit working twice for years at a time. The last few years have been really intense with the fatigue. It’s been a great incentive to explore the options. I’ve been on LDN for a little over a week and have noticed improvement with that too.
Interesting…I just read that opioid drugs – when they work – do so at least in part by increasing ;levels of endorphins – feel good chemicals – that basically swamp out the pain signals.
What’s the name of the drug that diminished microglial activity, and thereby increased dopamine?
“Treatment with minocycline or interfering with BDNF signaling restored chloride transport within these neurons and recovered DA-dependent reward behavior.”
http://www.jneurosci.org/content/35/22/8442.short
I believe this is the study.
I want to know, as well! Wish I could find a practitioner who knew something about ME! This is a great article, informative and helpful. Thanx, Cort.
It was minocycline – an antibiotic that has worked well in lab animals to turn down microglial activity.
I don’t know if minocycline is the best way to turn down the microglia but it can do a lot of stuff- including protect the mitochondria.
Here’s a blog I did on it – http://www.cortjohnson.org/blog/2014/06/28/drug-repurposing-antibiotics-reduce-microglial-activation-mecfs-fibromyalgia/
I am not sure this is the place for this discussion, but the increased microglia cells caught my attention. I have genetically tested positive for APOE 4. It is most often discussed with Alzheimer’s. It increases microglia activity in plaques in the brain. Has anyone else been tested for this? (I am hoping Cort can tell me how to get this topic on the Forum page)
Have you heard about the studies showing that ultrasound can break up the amalyoid plaques of Alzheimers in mice? (Sorry I don’t spell the best.) It’s good to know they’re getting somewhere in treating these nasty long-term illnesses even tho it will most likely be to little too late for me…
I’ve been working on a related puzzle:
I cannot tolerate anything in the dopamine chain until it gets to norepinephrine. I get paradoxical reactions (near narcolepsy) and increased pain and general sickness from all-size doses of L-dopa (mucuna), L-tyrosine, phenylalanine, as well as receptor blockers like ritalin and nuvigil. However, I tolerate Wellbutrin (which encourages norepeniphrine) fine, and gain some short-term energy and focus from it.
Dopamine receptor up-regulators like pramipexole and sulbutiam I can only tolerate in very small doses.
Cybalta (which encourages both serotonin and norepinephrine) reduces my overall pain substantially, but does nothing to combat chronic fatigue.
Anyone have any insights into why I might have both a dopamine shortage and a dopamine intolerance? I also have autonomic neuropathy (as well as peripheral).
Wow! How did you figure that all out? Wellbutrin and several other meds made me MORE anxious (felt like screaming and/or crying all day, BP up and pulse were racing) after just one dose. Dr said, “Don’t worry about the side effects…see you in a couple months.” ! Last anti-anxiety med they tried on me made me suicidal. SCARY!
Yes, I think your reaction would be more “normal.” Norepinephrine is called noradrenaline overseas. With me, though, it just provides a couple hours of ordinary energy — less anxiety-producing than caffeine.
I don’t know why I can’t tolerate everything else related to dopamine, but I’m wondering if it has something to do with the fact that microgrial activation disrupts dopamine transmission in the same way it disrupts opioid transmission. (The study experiments with cocaine.) And, so just dumping more dopamine into the system might be worse than merely ineffective.
As you can tell, I’ve been experimenting a lot on myself, and now I’m thinking a minocycline experiment might teach me more. The study warns that they haven’t analyzed all the unwanted effects of minocycline, so at this point it might be better thought of as experimental, rather than as long-term treatment. I’ll ask my neurologist about it.
Another interesting tidbit: the study shows that a peripheral nerve injury can cause the microgrial malfunction.
I also take Wellbutrin and cymbalta and both have helped esp with pain. The wellbutrin which I take in the morning gives me a wee boost of energy. I’m worse off of it.
I do not tolerate many medications, I usually have bad side effects. I’ve only found B complex vitamins, Acetyl-L-carnitine and protein powder (either GI Sustain for leaky gut or Brown rice formula) to help with energy and weight control-I tend to lose weight rapidly at times.
I’ve never really understood my strange reactions to many meds, but as I’ve said before we are all unique in our chemical make-up, the brain is so complicated that it makes sense that one type of medication may work for some but definitely not for all.
OT, but… Do you ever deal with brain zaps with this combination? I’ve been trying to figure out the pattern of when/why I get them. At first I thought the Wellbutrin must be inhibiting the transport of serotonin, but adding extra serotonin (whether an extra Cymbalta, or l-tryptophan, or 5_HTP) can sometimes make the zaps worse — as can reducing the Wellbutrin.
I also use ALCAR, B-vitamins, plenty of fish oil, vit C, alpha lipoic, and alpha-GPC, but I think I’ve removed all the other supplements that promote dopamine.
Could explain why when I took XTC I had no PEM after a night dancing. But half an hour of too intense walking while sober would trash me for days. All dopamine
Cort, I know I’ve been a broken record on microglia for years, but recent studies have been offering some support for what I’ve been saying.
I’ve mentioned this before, a study that showed ganciclovir is a potent inhibitor of microglia. Maybe previous positive reports of this drug with CFS are more to do with microglia inhibition that anti-viral? Studies???????????????????????
http://jem.rupress.org/content/211/2/189
this study was done at Stanford, can they connect with Montoya???
Here is a link to a very interesting article about Dopamine and Fbromyalgia by By Andrew J. Holman, M.D.
Assistant Clinical Professor, University of Washington
Clinical Rheumatologist, Pacific Rheumatology Assoc.
“After centuries of disrespect and scorn, no one questions the validity of Parkinson’s disease today. It is ironic that the same neurotransmitter, dopamine, appears to play a control role in another enigma: fibromyalgia. The historic similarities are striking as evidence of dopaminergic control mechanisms begin to emerge with respect to pain, sleep, arousal and the autonomic nervous system. Each of these central nervous system functions are relevant to fibromyalgia, but hopefully FM will be sorted out and effectively treated more quickly compared to Parkinson’s disease patients.”
http://forums.prohealth.com/forums/index.php?threads/dopamine-and-fibromyalgia.189680/
Has anyone tried taurine?
GABA and dopamine agonist and neuroprotective via antagonising oxidative stress and microglial activation (apparently).
i just started taking taurine a few days ago. i notice that my brain seems more clear and i also am thinking more creatively. nice!
How much do you take? I wish I had someone who could help me make sense of all this. So thankful for you folks who give free online advise!
Cort, thanks for all the work you continue to do.
I was having severe sleep issues, not getting to sleep or waking up around 3 am with anxiety attacks – not based on any circumstances. I read that lowering cortisol levels in the afternoon/evening would help sleep. So I found that phosphytidyal serine (I cannot spell that_ would lower cortisol levels. I started taking 1 pill of PS 300 (ie 300 mg of the stuff) with my evening meal. Sleep has greatly improved. Amazing!
Have you or anyone else found this helpful?
We discovered dopamine years ago. We take mucuna capsules. It helps with sleep, brain fog, mood, and neurological pain/problems.
the dopa mucuna make me feel spacey…are there other sources?
Hi Kelly, I have been looking up these mucuna capsules and I’m completely confused! Could you tell me what type, what dosage do you take and how long did you take them before they had any effect? It seems to be marketed towards men but if it helps with my fatigue I really want to give them a go.
Many thanks,
Sharon xx
Hi, Has anyone in states that allow medical marijuana had good results with helping with fibro pain? Any any thoughts on what worked best knowing everyone is different.
Thanks, Leslie in Denver
Yes, high CBD helps alot with pain. I do not tolerate much THC.
Need a dispensary with alot of knowledge.
I’ve had good results with CBD, taken at bedtime. It made me more able to settle to sleep, which has been very elusive for me. Recently I required an increase dose ( fall weather and lovely flares) and had no unwanted side effects. I initially wasn’t sure how much it was helping, until forgotten meds while on a visit to my home province meant I had to do without (prescriptions of controlled substances aren’t transferable). I quickly experienced life without it and getting home was a blessing.
I can’t see good reason beyond inability to tolerate CBD for a medical professional to refuse to prescribe the medication as it provides no “high” or altered state beyond drowsiness. I hope you are successful. It’s been a boon for me!
What a revelation. I have been saying for years that Interferon ruined my brain, I was treated twice at 48 wks each. I have not been right since.
This is an important piece of research as I now have been diagnosed with Fibromyalgia and my intuition has always told me the interferon is the culprit.
Thank you so much, this will be a piece of research that will be going in my medical file.
Now there is THIS to consider:
http://www.cortjohnson.org/forums/resources/when-panic-isnt-dr-bell-on-maggies-me-cfs-and-fibromyalgia-story.237/
The “catastrophizing” may in fact be CAUSED BY the interference of blood flows.
I have been hypothesizing on this site for a long time, that at least with my experience of fibromyalgia, POTS symptoms are highly implicated. I have for a long time been “severely disabled” when it comes to some activities, such as those that involve squatting, or working with arms extended.
Maybe it is not so much a question of substances like Dopamine, as simply that a whole LOT of substances are “not getting through” to the brain and various muscles and organs, when they should be – because of problems with blood vessels. Other intersticial fluid flows may be problematic too – is there a term for the “vessels” in which these fluids flow?
Sure makes sense to me Phil….
I’ve had this feeling about blood flows for years….we shall see – the latest Fluge and Mella paper may be very constructive.
I have been wondering about the blood flow to the brain also…..sometimes just an aspirin will help with my energy level/and or brain fog….I believe asprin opens up the capillaries,etc. I was in a serious car accident a couple of years before all these health issues became apparent to me. Recently I had x-rays on my neck. There was quite a bit of damage done in my neck. That could interfere with blood flow etc to the brain.
This has me wondering… in my case, a childhood injury to the spine – a trampoline accident – may have had a role. I had not thought of this before.
The injury, however, did not stop me becoming a very fit and athletic cyclist in my twenties, after which the fibromyalgia developed, I say in conjunction with a severely stressful job that I should have quit while I was ahead.
I’m sorry, Phil. Our bodies are so resilient in many ways until something puts them over the edge. I’ve had to quit working twice…..and you know it wasn’t so bad. I’m retired now.
Good luck. We’re fortunate to have this method of communication and it feels hopeful that something will be discovered soon.
Hi
Can’t thank you enough for this article, I have suffered from CFS and now Fibromyalgia for over 30 years. After reading this I found that the supplement l-lysine (Holland and Barret) can help put dopamine back into the body.
Within a day, nerve pain went by 90%, stiffness 100%, muscle aches seem to have gone, despite my doing more. Sleeping better, more cheerful, infact day one it felt like i was high! I think of the 30 years of suffering that I went through.
2 weeks on I am slowly regaining more energy as well, I am a fighter and will try anything as I have no faith in my doctor, so have self treated as I do not tolerate drugs.
I do get the odd ache I wouldn’t say I am cured but would not like to go back to 3 weeks ago when walking a few feet would have me in agony.
Chris
That’s amazing Chris! Congratulations and thanks for passing that on…
How much l-lysine do you take? I’m desperate to feel better!
That is fantastic news, Chris! The results show that it works for you and your levels must have been low.
MK Gilbert, remember that l-lysine may not be the answer for you, but it could be worth a try. I have had a fantastic response to phenylalanine. I am now doing much more than I could previously, and I am feeling much happier in myself as a result of having more energy.
A few weeks ago, in response to one of these blogs, I had my amino acid levels tested. I now know that my l-lysine levels are slightly higher than the reference range. My aspartic acid is about double what it should be (not sure what this indicates), as is G-aminobutyric acid (but that sounds a good one to have high). However, my taurine level is 21, when the reference range for females is 30-192. I have just been out to Holland and Barrett and bought Taurine.
For anyone in the UK who is interested, the test cost me £91 and was done through Biolab UK. You have to give a medical practitioner’s name. My osteopath (who is also a naturopath) was happy to receive details for me.
I am late to the comment section but wanted to mention some ideas for thought & possible future reference & research. Iron & Iodine matter greatly to the brain & body. Example, The Substantia Nigra in the brain plays such an important role. (Ferritin levels MUST be checked along with iron to determine proper levels.) While reading one commenter’s experience drinking so much water I thought of the fluoride/thyroid dilemma. The thyroid and proper testing is greatly underestimated & misunderstood by modern medicine….hopefully this is changing.
Simply google Iron/Dopamine connection for many articles & studies.
Dr Jorge Flechas talk on iodine/Youtube will mention an amazing study & connection with FM. Dr. Mark Starr–Hypothyroidism 2 Book and/or youtube
Thanks for the ideas 🙂
hi. I found your pages years ago, and found it very helpful. Sometimes it’s a bit too advanced for me but I always read something interesting here. Anyway, I have been seeing a good pain specialist for approx 5 years. My diagnosis is currently Parkinsons, but still some doubt (severe non-motor symptoms with RBD, but still pre-motor). FM is the other possible diagnosis. The reason I am writing is to tell you about my experience using Dopamine (specifically low dose Madopar). I started in Dec 2017 when a 10 min brisk walk would result in severe PEM that worsened over the first 2-3 days and then hung around for another 2. By early 2018 I was walking 20 mine and having less severe PEM, and over a shorter period. We increased the dose during 2018 and my distances increased with lower PEM continuing. I went overseas for a month, but didn’t push it too hard in SE Asia. I was quite unwell for a few months on return in Oct 2018. A dose increase helped a bit ag again. We have not increased the dose since then, and 2019 was less healthy than 2018. Now 2020 is less healthy again with PEM returning to higher severity and duration, but not as bad as pre 2017. I’m not sure if this supports Miller’s work, but it is an example of Dopamine in action.
Interesting Greg. Thanks for passing that on and good luck!