

Right now, after roughly 2 months of social distancing, cases are increasing in 17 states, about the same in 23 states, and declining in 13 states. Cases in the U.S. overall have largely plateaued at about 25,000 new cases a day. Deaths have plateaued at about 2,000 a day.
The U.S. is leading in ways it never wished to – and never thought it would. It now has about six times the number of confirmed cases (@ 1,300,000) of the next most afflicted country (Spain) and 3 times the number of deaths (@ 77,000). Our death rate per million people while significantly lower than Spain, Italy and the UK is four times that of Germany.
While the U.S. has tested more people than any other country (@ 7 million), it’s tested a far lower percentage of its population than many countries including Spain, Italy, Germany, Russia, Belgium, Portugal, Sweden, Ireland, Isreal, UAE, Austria, Qatar and others. President Trump’s statement that the U.S. has tested more than ever other country combined is not even close to being true.
As U.S. cases continue to climb (outside of New York City confirmed cases are climbing not declining) some countries (China, South Korea, Singapore, Hong Kong, New Zealand) have pretty much smothered the virus. Nobody could have expected the world’s most powerful country with all its advantages – its immense and sophisticated medical system and research apparatus – would have responded so poorly.
The economic fallout has been staggering – tens of million unemployed, trillions of dollars lost, and trillions of dollars of debt added to the national debt. By any measure, the U.S. – and many other countries to be sure – have been behind the eight-ball from the beginning; unprepared, slow to take action, the U.S. got caught from behind by a fast-moving virus and the results have been devastating.
Two months into the crisis, the testing issues remain. The fact that Congress doesn’t have enough tests to test its own members speaks volumes. Reports that infections in New York City effectively seeded infections in much of the rest of the country highlight the dramatic cost of the U.S.’s inability to quickly test for the virus. The European travel ban came at least five weeks too late.
The CDC’s port-of-entry testing regimen certainly could have detected the New York City (NYC) outbreak early, but it was shelved when the CDC failed to rapidly produce an accurate test. As countries around the world used the World Health Organization test, the FDA waited for the CDC test to appear.
By the time the first coronavirus infection in NYC was documented, models estimate that 10,000 infections had occurred. From there, New York City likely seeded many of the infections in the U.S.
A startling model provided a cautionary tale that will helpfully help us the next time a virus like this comes around. It projects that if the U.S. had issued its social distancing guidelines on March 3rd instead of March 17th, 90% of the coronavirus deaths could have been prevented. Similarly, another model suggested that 50-80% of deaths in New York could have been prevented if social distancing measures had been adopted a week or two earlier.
Models Being Redone
The controversial IHME models which so many relied on – including apparently the White House – first overstated, then understated the impact of the virus. Just three weeks ago, the model predicted zero deaths in the U.S. by June – a projection that was laughed at by experts in the field at the time.
A recent update of the model almost doubled the projected death toll. This model, interestingly enough, does not rely on epidemiological data. Instead, it assesses how the virus impacted other areas in the past to model how it will impact us now. It’s been changing dramatically over time.
Other models are being redone – not just because new information is coming in – but because most projected the epidemic fizzling out during the summer. Now, with the deaths projected to remain high for months, that’s clearly not going to happen. FiveThirtyEight reported that by the end of the month the following major models forecast the following number of deaths will occur.
Deaths as of May 5 – According to Johns Hopkins Univ. – 71,064
Deaths Forecasted for May 30
- MIT: 111K (105K—118K)
- IHME: 110K (91K—150K)
- Los Alamos: 107K (81K—173K)
- Columbia Univ.: 104K (93K—122K)
- Northeastern Univ.: 98K (89K—117K)
- Univ. of Texas: 93K (81K—160K)
No Summer Respite?
Mike Osterholm, the director of the Center for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota, gave the rather grim news: “The idea that this is going to be done soon defies microbiology.” The much ballyhooed and hoped for herd immunity is probably going to take 18-24 months to occur. Absent a vaccine, he believes the virus “is not going to stop until it infects 60 to 70 percent of people.”
Hopes that it would fade significantly in the summer have largely vanished. Historically, pandemics, Osterholm said, just don’t die out in summer. The lockdown has helped immensely but we don’t know how the reopening will go, and things could get much, much worse if a coronavirus spike in the fall and winter coincides with a nasty flu season.
National Crisis
Nobody disagrees that we’re not in a national crisis. We thought the near dismemberment of the financial industry during the 2008 recession was a once in a lifetime crisis. The Dept. of the Treasury and the Federal Reserve Board repeatedly threw out the rule book in an attempt to keep our financial system, and virtually every corporation in America, from going splat.
That was really bad, but experts are saying the financial impact of the coronavirus is “way worse” than the 2008 meltdown. Almost a month ago, when the economic effects were not as evident as they are now, Foreign Policy compared the “financial heart attack” that was the 2008 recession to the “full body seizure” that is the coronavirus.
Paul Romer, a Nobel Prize-winning economist and former chief economist at the World Bank, believes the coronavirus is costing the U.S. economy something on the order of $500 billion dollars a month.
This seems like a batten down the hatches, all hands on deck, leave no stone unturned, throw the rule book out the window kind of moment.
President Trump, though, has left much of the responsibility for fighting the virus to the states. While the feds have certainly rushed much needed supplies to hot spots, and Congress and the White House have pumped trillions of dollars into the economy to stave off a collapse, the Presidential powers often used during national crises to respond have largely remained unused. This time, there has been no national strategy to produce tests, provide equipment or produce treatments.
Now we’re trying to reopen the economy. That’s understandable – the economic carnage from the coronavirus, which has exceeded everyone’s expectations – is too great not to try to find a way to reopen the economy.
The great question is how to do it. Note that maintaining safety and reopening of the economy are not necessarily contradictory processes. In fact, they may go hand in hand. Only if people feel safe will they be able to fully re-engage in society. Economies, it should be noted, started imploding across the world before they went into lockdown as people started to isolate themselves.
Will They Come?
One of the great questions facing the U.S. is: if you reopen it, will they come? How much risk are people willing to take? We’ll start finding out over the next month.
Opening the economy too soon risks a need to shut it down again, which will extend the pain and time it takes to fully reopen it. Opening it later than necessary risks causing more economic pain at a time when it’s not clear how much more economic pain the U.S. and other countries can take.
The goal is to open the economy as safely and as quickly as possible. The question is whether we’ve used the two months the lockdown has provided us to prepare to do that.
Roadmap Not Taken
Roadmaps have been produced. The American Enterprise, lead by former FDA commissioner, Scott Gottlieb, created a much cited roadmap, “National coronavirus response: A road map to reopening“, to safely re-open the economy.
The roadmap asserts that a lockdown can safely end, and people can start re-engaging with society again, when:
- A state reports a sustained reduction in cases for at least 14 days (i.e., one incubation period of the virus); and
- Local hospitals are safely able to treat all patients requiring hospitalization without resorting to crisis standards of care; and
- The capacity exists in the state to test all people with COVID-19 symptoms; and
- The state has the capacity to conduct active monitoring of all confirmed cases and their contacts.
The Great Experiment Begins
Eager to get the economy started, President Trump three weeks ago declared that 29 states could begin to reopen their economies “relatively soon”, and states are, indeed, beginning to reopen.
None of them, it should be noted, have come close to meeting the criteria cited above. Plus, after accounting for the case decline in New York City, confirmed coronavirus cases in the rest of the U.S. are growing, not declining.
The U.S. can’t remain in lockdown indefinitely, however. With 30 million people unemployed – which doesn’t count the number of employees who have been furloughed – the pain is just too great; yet testing and contact tracing is still way behind what the experts say is needed to safely reopen an economy.
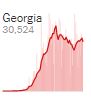
Time will tell what will happen, but in the meantime, Georgia may tell us much.
Georgia On Our Minds
Most states are moving very slowly. Georgia is moving more quickly, making it something of a test case for the nation. Georgia went first, allowing gyms, fitness centers, bowling alleys, body art studios, barbers, hair and nail salons, estheticians and massage therapists to reopen April 24th. Theaters and restaurants were allowed to reopen April 27th.
With a two-three week lag before increased infections show up, Georgia’s success or the lack of it should start to show up over the next week. Thus far, confirmed infections have been pretty stable with a small uptick.
Testing Looms as Major Issue Again
The danger with reopening an economy without sufficient testing is that a significant increase in the number of new infections wouldn’t show up for 2 or 3 weeks. An increase in deaths will show up in about 3 weeks. By that time, the contagious virus will have spread.
The two things that could presumably salve the public’s fears, allow the economy to open, and withstand the increased level of coronavirus infections that are sure to follow, are more and more testing and contact tracing – both of which are missing.
Several reports have called on the U.S. to invest in the most spectacularly aggressive testing and contact tracing regimen in history. Investing a hundred billion dollars in testing, as we face an economic crisis like none the country has seen before, seems like a no-brainer. More people have been put out of work more quickly in the past two months than has ever happened before – and it’s not close.
Given those high stakes, Romer and others are astonished that the U.S. hasn’t initiated a kind of Manhattan Project for coronavirus testing. A national testing strategy would allay fears and allow for the most rapid resumption of the economy. Testing, thus far, however, has been left largely to the states.
Despite President Trump’s assurances as far back as early March – and continuing to this day – that the testing is adequate, Governors – both Republican and Democrat – and public health experts continue to decry shortages of critical supplies such as swabs to gather nasal samples, containers to transport samples, and chemicals to test samples. The lack of a national response, which could have efficiently moved supplies to the most needed locations, has hurt – leaving some labs with some of the supplies needed, but not all. States, competing with each other, are paying through the nose to try to meet their needs.
To the administration’s credit, it has dramatically enlarged its testing capacity. The U.S. is currently testing about 200,000 people a day. (It’s also been stuck on 200,000 tests a day for about three weeks.)
Is that enough? President Trump thinks it is. On April 18th, he said the nation’s testing capacity was sufficient to open the country, and just two days ago, he said he was not a fan of expanded testing stating that “I don’t think you need that kind of testing or that much testing”.
Few others, however, believe we’re ready.
The respected “National coronavirus response: A road map to reopening” thinks it might be, but its recommendation comes with a big proviso. The roadmap calls for at least 750,000 tests a week – about half what the U.S. is currently testing – if it is paired with a massive contact tracing effort. We’re not even close to producing that kind of contact tracing effort.
The National Coronavirus Response team is on the very low end of the estimates being produced. Jeremy Konyndyk, a disaster preparedness expert, asserted: “We need to take where we are now and expand it tenfold.” A group of Harvard researchers estimates that a minimum of 500,000 people needed to be tested per day, and that the aim should be 2 million to 3 million per day.
The “Roadmap to Pandemic Resilience: Massive Scale Testing, Tracing, and Supported Isolation (TTSI) as the Path to Pandemic Resilience for a Free Society“, produced by a group of experts convened by Harvard University’s Edmond J. Safra Center for Ethics, calls for five million tests a day by early June, and up to 20 million tests per day by late July.
Last month, the Rockefeller Foundation published a road map to take the United States from about 1,000,000 tests per week to 3,000,000 tests per week by late June – enough to test everyone, they believe, with symptoms, those who came into contact with them and people at high risk of the virus. That, they believe, would allow the country to partially reopen.
That volume of testing would cost about $100 billion and would require conscripting universities and small labs to perform coronavirus tests. They also proposed that the states hire 100,000 people to do contact tracing and that a single entity be created to place bulk orders for supplies.
Even that, they don’t believe, is enough to fully reopen the economy. To do that, they believe the U.S. needs to aim for 30 million tests a week by fall.
Good News
Democrats twice blocked the latest aid package (Phase 3.5 of The Paycheck Protection Program and Health Care Enhancement Act) to force, among other things, the addition of $25 billion for coronavirus testing and a directive to the administration to prepare a national testing strategy to help states dramatically increase the number of tests available.
Of the $25 billion, $17 billion will go to the states, and $1 billion will go to the NIH to develop, validate, improve, etc, coronavirus testing. While it’s not anywhere near what some reports believe is necessary, it will clearly help.
One wonders how much better shape we would be in now, and how more ready to safely reopen the economy, if something like this had passed two months ago.
It did not appear that any funding to help the states with contact tracing was provided, leaving the states, which have been battered by dropping tax revenues, to assume the cost of that themselves. While businesses, employees, taxpayers and now hospitals have received federal support, this is the first support that the states – at the forefront of the epidemic – have received. Some have been so financially battered that Mitch McConnell suggested they declare bankruptcy.
The NIH and its Shark Tank
“We need all innovators, from the basement to the boardroom, to come together to advance diagnostic technologies, no matter where they are in development. Now is the time for that unmatched American ingenuity to bring the best and most innovative technologies forward to make testing for COVID-19 widely available.” Francis Collins, the NIH director.
It took less than a week or so, though, for the NIH to announce the creation of a $1.5 billion “Shark Tank” Initiative which it believes will result in “millions of tests per week” being available by late summer or fall of this year. Given that several groups think we should be testing millions of people per day, the NIH goal doesn’t seem that impressive, but it will certainly help.
In the “national Covid-19 testing challenge”, different groups will compete for a share of a $500 million diagnostic development pool. The NIH will then pair the winners with manufacturers and business who will assist them in rapidly scaling up the production of the tests.
This is the kind of innovative and creative approach to problem solving that the United States is known around the world for but which has taken months to muster. Again, one wonders how things would have been different if the NIH had been able to put this forward two months ago.
The Missing Blue Ribbon Panel?
“More than anything, what the United States needs right now is for the president to undertake an intellectual Manhattan Project: gather the best minds in public health, medicine, medical ethics, catastrophe preparedness and response; political leadership; and private-sector manufacturing and the pharmaceutical industry.”
Michael Osterholm, an infectious disease expert, recommended that a national strategy be developed. Osterholm envisions a panel of public health, laboratory and medical experts, ethicists, legal scholars and elected officials that would create a national roadmap for testing and contact tracing and produce a strategy for hot spot monitoring and responses to the new outbreaks that certainly will occur.
But isn’t the Coronavirus Task Force enough? There are several problems with having a wholly federal group in charge. For one, the government is a huge bureaucracy with all that implies: turf protection, defensiveness, shortsightedness, political considerations, petty rivalries, etc.
Both the FDA and CDC chiefs, for instance, appear to have simply been too reluctant to take on the bureaucracies they inherited. As the testing situation got worse as worse, as the U.S. was testing hundreds of people a day while other countries were testing hundreds of thousands, they continued to rely on the advice of their top staffers. Finally, the testing situation got so bad that changes were made. By then, it was too late to control the virus without making massive changes.
A group that operates outside the bright lights, the political considerations, the turf-fighting, etc. which can give a sober, independent assessment of the best way to move forward would do three things: 1) it would provide advice from some of the best minds and most competent individuals in America; 2) it would point to innovative, effective solutions, and importantly; it would give the administration cover for the difficult decisions that need to be made.
More Good News – Vaccine Development Reportedly Goes Into Warp Drive
While the Trump administration has not embraced a national strategy for testing, or indeed much of anything, the really good news is that reports indicate the administration is putting together a kind of Manhattan Project to quickly produce a vaccine – perhaps by year’s end.
Called “Operation Warp Speed,” the program is reportedly doing what only the federal government can – pulling together private pharmaceutical companies, government agencies and the military.
It will do it, though, without one of its key members. The ouster of federal vaccine chief Dr. Richard Bright in the midst of the pandemic was surprising, to say the least. Calling Bright a “vaccine expert”, former Food and Drug Administration (FDA) Commissioner Scott Gottlieb said Bright’s ouster will “set us back” in combating the coronavirus pandemic.
Gottlieb also predicted that Bright’s sudden ouster could make businesses more wary of collaborating with the federal government than they would have been. Bright asserts he was ousted for limiting the use of hydroxychloroquine – a now discredited coronavirus treatment. His ouster followed that of Christi Grimm, a longtime inspector general who make the mistake of documenting in a report the shortages in equipment that hospitals have long been facing.
Meanwhile, Bill Gates has stepped in where the feds haven’t thus far. In another creative approach, the Gates Foundation is funding seven different vaccine factories, knowing that most of them will fail but hoping that one or two of them will work.
Let’s hope that vaccine development does indeed proceed at warp speed.
Conclusion
Outside New York City, confirmed coronavirus infections continue to grow and most models suggest that deaths from the virus will reach 100,000 people over the next month.
The U.S. and other countries are, however, slowly moving to reopen their economies. The experts say we need much more testing and more contact tracing to safely do so, but with the nation’s economic woes reaching unforeseen heights, President Trump and the governors are pushing forward. It’s a huge gamble.
To some extent, we’re running blind. If an outbreak does occur, we likely won’t have the testing and contract tracing needed to quickly squash it. Opening and then closing and then later opening the economy again, if that happens, will only extend the pain.
While COVID-19 testing in the U.S. has mostly flattened out over the past three weeks, new funding in the last aid pack should help. Plus the NIH’s COVID-19 Shark Tank contest should speed things up as well. But will it be enough? Time will tell.
And what about contact tracing? Is that really needed? (California is requiring counties show they have contact tracing in place.) And are Americans ready to re-emerge from their homes or could they lock down the economy themselves? Will the virus explode back into action as the economy reopens, or will it remain an ugly but manageable presence? And what will happen in fall when the coronavirus and the flu bump heads? Are we ready for that? Is it possible that we could have a vaccine ready by January?
So many questions remain unanswered. The great experiment continues.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!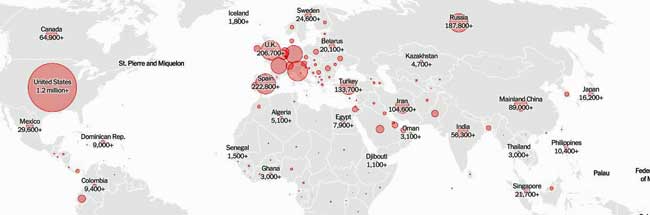








Britain is now talking about reopening – but it’s surprising (to me at least) just how anxious and risk averse some youngish people are. We are currently doing 80,000 tests a day and the government claims to be heading towards 200,000.
Personally I’m not planning to return to normal life until there is a vaccine or better treatment because I dont see myself as low risk. My OH is moderately high risk and I dont plan on killing him off just yet. However I am planning to bring forward purchases when I can to help support the economy.
In my local area businesses that have rapidly adapted – introducing home delivery services – have done well. One enterprising person started a new business delivering vegetables, they are run off their feet and constantly expanding.
People have sewn scrubs for hospitals, schools have made face visors, businesses switched to making PPE. We have an organised volunteer network to help those most at risk with shopping or just a call to reduce loneliness People are pulling together.
America needs to be adaptable, to pull together – and to learn from elsewhere what works and what doesnt. And stop regarding your President as beyond criticism.
Glad to hear. The UK has been hit pretty hard – it’s amazing what a difference a couple of weeks can make – but it was encouraging to see that the UK plans to hire 18,000 I think it was contact tracers. Good luck!
Yes we’ve been hit hard – we should have shut down sooner and a lot of the deaths would have been avoided. Sensible people were already starting to physically distance before the government enforced it. Now businesses are quietly returning to work but being very careful about how they do so.
Every western country has high levels of conditions that make you more at risk from this virus. Many of these problems are not immediately obvious – like high blood pressure or diabetes. So when governments – or scientists like those in one of the links – put out messages intended to reassure many people actually see this as “I am at risk” – and that is true but what is missed is that most will still survive a virus attack.
Your comments already include one political response and one thing that clearly distinguishes America from other countries is just how politically divided you are and how much that is damaging your response. Bipartisan politics should have no place in the virus response but your President is determined to have any criticism seen as “political” and that applies even to comments from those who have no interest in your politics, only in how any people are dying as a result.
Once again, Cort, you have streamlined and communicated a vast amount of, at times, conflicting information in expert fashion. Thank you for this excellent summary.
Great summary, thanks Cort. So sad to see the poor US response…we will suffer much more because of it. The silver lining is a pause for our planet to catch its breath a bit.
This sounds a bit crazy but I see COVID-19 as possibly a lucky break; a kind of dry run that will only help when the REALLY bad virus pops up – the one that is very contagious AND has a high death rate. Instead of 70,000 dead we could have a million or more dead right now in the US and there would be nothing we could do about it.
This virus a big enough wake up call to get our attention but not something that destroys us. We might actually be lucky…
Thanks!
I concur with your assessment that this is a good wakeup call now we just have to wait till the cities are underwater to wake up from global warming. Personally, I wish a measly 1 billion dollars could be put toward ME/CFS
I might suggest reading some of Dr. Scott Atlas’ (Stanford) and Dr. Dan Erickson’s commentary and perspective where politicization is absent and facts are clearly presented. Remember; models don’t lie —but liars can model.
Here’s a link to Atlas’s ideas https://thehill.com/opinion/healthcare/495833-how-to-open-society-using-medical-science-and-logic. I imagine we will come around to them more and more simply because we must – we just can’t economically stay shut down.
A crucial factor, though, is having people feel safe enough to re-engage. I just talked to two people who’s states are opening up and they’re staying put. If many people do that the economy is going to continue to suffer.
I think the models are honest efforts. If you miss on a model everyone after all will know! It pays to be as accurate as possible – as we’ve seen, though, accuracy is not any easy thing to attain. As time goes on the models should be improving and we are seeing most consistency across them.
I imagine that the doomsayers are off and so are the optimists.
This comment is actually untrue ” And younger, healthier people have virtually zero risk of death and little risk of serious disease” .
It is true that if under 60 AND with no other conditions you are not likely to die – and even those with other conditions will probably survive – but about 20% of the infected will get an illness that is much more unpleasant than flu. Their lungs will, to quote several sufferers, “feel like they are on fire” and the damage will last at least for weeks and my yet to prove to give reduced lung capacity for life. Countries didnt lock down to protect their elderly they locked down once it was realised that younger people were suffering.
It is also divorced from the real world – a world where elderly people frequently provide childcare for children who dont get sick but can still have viral loads equal to an adults. And their teachers may well be an at risk group.
“and may yet to prove to give reduced lung capacity for life.”
That may be the huge unknown risk for young and healthy people. IF this virus would become a seasonal thing and mutate enough to negate immunity before a vaccine has been found, the many youngsters who escaped death but have severe life long lung damage WILL be risk patients by then.
While Dems block stimulus programs small businesses are failing and people’s lives are financially ruined forever. Suicide rates are also increasing.
Politics and pork projects have no place in a pandemic or medicine, IMNHO.
Yes, the Democrats did block passage of the last stimulus bill and they did it to get more aid for hospitals, funding for testing was included and a national testing strategy was included. I don’t know if that’s what you refer to as “pork”.
Check this out, though, Jorg. If you really want economic relief – then the best thing to do may be to test, test, test – and track, track, track. Until we have sufficient testing which allows us to track down people who are ill and quickly quarantine them, sending the rate of infection down, it may be impossible for the epidemic to end or the economy be able to recover. Every report I’ve seen – put together by experts in this area – asserts that more and more testing is the way to go.
https://www.newsmax.com/politics/chuck-schumer-coronavirus-testing/2020/05/05/id/966148/
I am completely baffled why we don’t have a national testing strategy and aren’t pouring a hundred billion dollars into it Besides being effective I think the public would have loved it and it would have boosted Trump’s ratings considerably. The experts are calling for it, the governors are calling for it….I’m just completely baffled. It seems like such a no-brainer for me…I must be missing something 🙂 (Can somebody clue me in???)
It’s like we’re in a trance – until it happens we’re not going to believe that its going to happen – and then it happens, and we smack ourselves in the head and wonder why we allowed that to happen again…
President Trump recently said – “We don’t need more testing”. Time will tell if he’s right. Hopefully he is but as the healthy of our economy counts on him guessing right at this point I would rather have some backup as well. Let’s hope he’s right and we can get by without all this testing.
More on the need for more and more testing from two senior Republicans in an op. ed piece – https://www.washingtonpost.com/opinions/2020/04/20/how-speed-up-testing-shark-tank-government/
“There is no safe path forward to combat the novel coronavirus without adequate testing. To contain covid-19 and persuade Americans to leave their homes and return to work and school, the United States will need tens of millions of diagnostic tests. Deborah Birx, the coordinator of the coronavirus task force, says there are now 1 million tests available weekly; by mid-June, there will be 2 million to 2½ million available.
That is impressive — but not nearly enough. We should squeeze every test possible out of current technologies, but we need tens of millions more to really get a handle on how far and wide this disease has spread.
We recommend spending even more to advance other research, giving money to states to buy testing equipment, improve data reporting, conduct tests and operate testing centers, and implement contact tracing to identify those who’ve come in contact with sick people so they, too, can quarantine themselves — instead of the rest of us quarantining ourselves.”
Cort,
This is what I am referring to:
$60 Million for NASA, PBS gets $75 Million, the arts get $75 Million, etc. Watch the video and get the FACTS.
What does ANY of these entities have to do with the pandemic? Why would they be included in a CARES bill that is suppose to help small Biz and individuals?
Don’t forget the people get a whopping $1200 out of this deal and true small Biz gets nothing. The SBA has noted that true small Biz provides the most jobs in the U.S. and those jobs are disappearing forever. Unemployment already exceeds 14.7%…
https://www.mrctv.org/blog/reality-check-60m-nasa-congress-new-aid-bill-struggling-americans-includes-billions-pork
https://www.mrctv.org/blog/reality-check-millions-more-americans-lose-their-jobs-left-uses-covid-19-push-their-green
What does socialism and the green agenda of the Dems have to do with starving people and financial disaster for so many small businesses?
Making everything political is wrong here or elsewhere. Believing the lies spewed by the leftist media makes people gullible and duped.
Just because you don’t support NPR or liberal arts doesn’t mean they’re aren’t legitimate businesses. Oil companies got support, gun companies got support. polluters got support, solar companies got support, the metropolitan opera got support. It has nothing to do with liberal bias.
Unfortunately the smallest businesses had a lot of trouble. Two members of my family run small busineses (less than ten employees). Fortunately both of them got help but I know many others didn’t.
Please note, though, that this was a bipartisan bill passed with overwhelming support from both parties. The responsibility for any shortcomings of the bill falls on both shoulders does it not?
The reason many small businesses didn’t get support is because of the way the bill was fashioned and the way banks lend money and their focus on their biggest customers. I don’t know the green agenda would fit into that?
Lastly maybe try getting your news from a site that doesn’t publish stories that start off saying “the liberal media”?
As to your worry about a “green agenda” consider that if you think the coronavirus is bad you ain’t seen nothing compared to global warming. As with the coronavirus the science is there – except it’s doubly/triply there. Decades of research have only solidified and worsened the original models. The same process is playing out with global warming as it did with the coronavirus – an unwillingness to accept the science – except the peril is so much greater.
Restaurants lost 70% of customers before any states or counties closed by government orders. Small businesses losing customers is not only the result of government action, but a combination of citizen behavior and government intervention.
It is a false narrative to blame the Dems, or any one politician, for the economic impacts of coronavirus.
(Stats were from the Freakonomics podcast last week…)
Thank you for this reasoned coment .
I meant this in support of Jorg
Check out another question looming before us – as the economic distress continues we may be at a make it or break it moment for the economy – https://www.nytimes.com/2020/05/09/business/as-job-losses-mount-lawmakers-face-a-make-or-break-moment.html?action=click&module=Top%20Stories&pgtype=Homepage
Thank you. I have posted additional info. above to clarify the Dem pork project…
Jorg you said that you felt politics shouldn’t get in the way. Yet you’ve interpreted aid to NPR, liberal arts, NASA as Democratic “pork projects” . Could you respond to my assertion that instead of Dem pork projects these are simply businesses getting support like any other business has been getting support.
Best comment I’ve seen about the coronavirus ” Cant help thinking the earth just sent us all to our rooms to think about what we’ve done”.
In Venice there are fish in the canals, across the world the skies are clearing and deaths from air pollution and traffic accidents are falling. Sheep play on a roundabout in Wales. We get to see what damage we have done to the planet and how soon it could shake us off.
Regarding the economic fall-out from Covid-19, 40% of those who have applied for unemployment in my state (Florida) have been determined to be ineligible. The system is impossible to navigate and some applicants spend days trying to just get an application submitted.
Perhaps, France has a better way. Employers are compensated to keep their employees on staff even though they cannot come in to work. This system would cut out the cost of inefficient re-employment programs and keep trained and experienced workers on staff when the economy can reopen. This is a savings to companies since hiring and furloughing workers is costly also.
https://www.french-property.com/news/french_business/covid_19_employees_wage_support/
The most frightening aspect of the Covid outbreak is its continuing mutations. It has evolved, now greatly affecting children, and has caused fatalities (several cases in metro NYC area). How can we effectively treat a disease that morphs contiually? This outbreak in children leads me to believe the virus can linger in the body much longer than originally stated. The fear of a second outbreak in the Fall is personally paralyzing. As the adage goes,”Hindsight is 20/20 Vision”. Let us proceed with health and safety as the governing factors. To all, sray well, stay safe.
With a bit of luck, this evolving of the virus should make it less deadly. That has been predicted by some virologists: it would become more like the flue, meaning both a seasonal thing and less deadly.
It sort of makes sense: people with a less aggressive variant are less likely to seek medical aid and hence are less likely to self isolate and to warn others in their neighborhood to get tested and treated too. So those strains would multiply more.
The more aggressive strains would land many people in hospital and have a checkpoint providing isolation and checking contacts every time it raises its ugly head, leaving it less chance to spread itself. That in theory could help the more benign strains out-compete the more aggressive one.
Let’s hope. That’s actually what happened with the HINI Spanish flu – it evolved into something less dangerous. First, though, it got worse! Let’s hope COVID-19 skips that step.
I heard that one country mixed samples to test against corona in order to be able to do more tests.
Say for example you test 5 people who have a low chance each of being ill. If you poor half of each sample in a common container and test if there is any virus present, then you only need 1 test to clear them all or 5+1=6 if the combined sample is flagged. On average you should save tests.
This is a simple combo and could be reworked to save more testing with a bit of optimalisation.
Cort, have you seen the paper from Germany that looks at autoimmunity and ME/CFS? Around 300 patients and 300 controls.
Of the 300 patients around two-thirds were infectious onset.
The researchers found strong link between indicators of auto-immunity and infectious onset CFS, but not in the subgroup who were not infectious onset.
Thanks for the tip! I just found it 🙂 Will do a blog on it for sure. Scheibenbogen is cranking out the work.
You are welcome.
I am an academic with access to a massive online journal database. Every now and then I search for ME/CFS journal articles, and this came up from April.
It sounds quite compelling, one of the questions raised in my head is how significant is the link to autoimmunity? Is that a secondary factor, or is it a primary factor driving disease outcomes in patients with versus without infectious onset.
Also, might it mean that rituximab might be more effective if it is tested on infectious-onset patients with auto-immunity?
Look forward to the blog!
Thanks for the ideas 🙂
Cort we all thank you for your hard work as it has been very helpful to say the least. as far as your political views I have to say they should not be in this forum. There is enough division yes based on mainstream media and libs looking for power and more votes at this time in our history. That said lets all agree that we want what is best for ourselves our country and the world. There are times when things are glaring with corruption. no doubt both parties have had there moments now and in the past. this time IN my opinion it has been on dems. Heck we had Obama in office and he knew about me/cfs and did not one thing for us!! I know if I can get word out to trump through mutual friends we can cut through red tape and put real money in this disease. I’m working on it. Lets all love each other and understand most of us want what is right but have different ways of getting to same end. Let’s try to all be brothers and sisters see from different perspectives with open unbiased minds and try to find commonality. God bless
Thanks Jimmy. I understand how easily it is for politics to enter into the discussion but I tried hard to have it be a kind of objective status report. Inevitably some concerns fell on the Trump administration but I did not mean the blog to be political.
The blog praised the rapid increase of testing while emphasizing that experts assert that we need to do much more. The blog also praised President Trump for initiating or backing the Warp speed vaccine project.
I agree that no President’s, whether Republican or Democrat, get high marks for supporting ME/CFS.
In Congress, though, we have important supporters from both parties, let’s keep adding both parties to the mix and good luck with your attempts to do so.
greg without going into any of your questions and or accusations about trump ect I will say this I’m to tired to write you back. you sound closed minded and I’ll leave it there. I assure you if you would like to discuss this on phone with me you will get off phone with a much different opinion!! that is of course assuming you are open minded and understand both the small and larger view of what has been happening in this country!! If that is the case you may e mail me and exchange numbers and I will explain in very open and honest way how to disect these issues with no prejudice but truth and love. .. Cort I understand you. I know your heart is in right place. I know you see the world from a perspective from younger days. There have been times in history where the dems have had it together and times when repubs had it together. mostly both have failed us as we know why and who enter the political establishment. I know we both want fairness , a clean planet, people to be treated fairly with love and respect!! Will keep striving and fighting for that pal!! God Bless
Jimmy, really? Cort gave a concise and factual summarry of the course the Corona Virus epidemic has taken in the US. Any implication that the handling of the crisis was inept has to be laid in the hands of the President who has relied on magical thinking while ignoring the science and abrogating the responsibility that I, as a taxpayer, expect my government to take. Stupidity is not an excuse but it explains a lot. Testing and tracing is not controversial – it is public nealth 101 (I am hearing the President speculate that it is not necessary (except in the White House?). As far as small businesses not getting enough support, true, but that is mainly due to the Treasury Dept. letting the banks decide who should get the money. Take a breath, this is not about politics but it is difficult to talk about without reconizing we are in much worse shape than we would be if the President had done a better job.
Gregf you seem to want to vent about your issues with trump to me!! It was not your conversation with me to begin with!! It was myself addressing Cort. Now I believe I was very nice when I told you I am tired and do not want to debate this or anything else political on this site. We are all sick and need to find effective treatments for our disease here.. That said your getting annoying. You have no intelligent persuasive arguments that I can not take apart. I’m not a fan of anyone but the truth!!! you seem to be bent on blaming people instead of helping people. Get over it!!! I said you may call me and speak directly. I guess your afraid to hear something that you don’t want to hear!! challenge your closed mind by trying to get real information from both sides, then debate both sides to yourself and try to find peace!! other than that I would ask you to please resist your temptation over things you have no incite about nor any life experience!!! god bless
Jimmy I’m not in your country and have no interest in your politics except when it threatens lives. Your president suggested bleach, he has recommended a drug that could prove fatal and has not been useful in clinical trials. Blind faith in him is extremely dangerous. He has made this debate political when it should be science based. Tracking and tracing is the best method to contain a virus without trashing your economy. You failed to do that – as our government did in Britain – and both countries will now pay the price and get both high deaths AND a trashed economy. Now YOU introduce politics when Cort was trying to keep to science.
To rebuild your economy people have to be able to live normally without dying as a result. Political posturing and lies wont do that but will disproportionately result in Republican deaths from the virus. Demonstrations about reopening the economy are spreading the virus to places that have not been badly hit yet. Your economy will not be rebuilt while there are mass deaths.
I know young healthy people who had corona.
After 2 months they are still very tired.
And also have other symptoms.
Looks like ME to me.
droplets suspended in air for 12 minutes:
https://www.thailandmedical.news/news/breaking-covid-research-study-confirms-that-sars-cov-2-coronavirus-can-be-spread-through-speech
mouth rinses may be of some effect:
https://www.thailandmedical.news/news/breaking-covid-19-research-medical-scientists-led-by-cardiff-university-urge-for-further-research-of-oral-rinses-to-help-combat-covid-19
China to test 15 million people
(in Wuhan?)
https://www.thailandmedical.news/news/breaking-china-covid-19-news:-china-lockdowns-jilin-city-and-more-cities-to-follow-soon
Cort
I am amused with your attempts at covering the COVID-19. First you are out of your depth- I have professional interest in this and have temerity in describing events accurately.. Second there are many states where opening up has occurred without increases- like for example Texas and Florida-there are many more. You are a victim of the liberal news monopoly. You can go on believing this stuff as it passes for accepted truth – but it looks like the real world is moving elsewhere. The liberal media are trapped in cities were their Democratic governors are causing great economic harm without justification. If you really want to understand what is happening look at the map by zip code of cases in NYC-it tells all. You could see well over a month ago that cases were clustered in immigrant communities and poor neighborhoods. If you combine incidence in poor neighborhoods with nursing homes you get over 80% of the cases. But that analysis is not politically correct. The models were and area joke – again I went through this stuff professionally. Republican states do not seem burdened by this race myopia and are moving on. But have it your way – it is acceptable by most writers.
Thanks Paul for your thoughts. As a professional I’m sure you understand that context – particularly regarding fast-moving events is critical. If you’ll cast your discerning eye over the date of the blog you’ll see that it was written just as states were opening up – too soon to tell if the infection would grow. You might also note that I reported that the one state – Georgia – which had been open for a couple of weeks – was not seeing an increase in cases.
I would be wary of using charged terms like “liberal media” (or “deep state” or “fake news”) in your posts for fear that it might undermine your status as a “professional”. Too often these simplistic devices are used as lazy excuses not to debate the facts. They are surely not appropriate in any professional setting.
I’m afraid you are missing another problem Paul – hospital transmission. You are also ignoring the excess mortality observed in Europe. While there are higher rates in our Black and minority ethnic population I can assure you there are a lot of white deaths too and not all in nursing homes. A 25 year old (white) friend of my child died recently from Covid-19 in London, he had been ill for weeks. Transmission in nursing homes usually lags infection in the wider community, you will have a lot ore deaths to come.
These articles explain why vitamin D may prove to be critical. Southern states can therefore be expected to do better than Northern states in summer https://www.sciencedaily.com/releases/2010/03/100307215534.htm and https://www.bbc.co.uk/news/health-52754280
That drug may not help unless vitamin D levels are sufficient.
If you have any care for black people, obese people or the elderly then see they know about the need to get enough vitamin D.