

“Our present study advances a new view of FMS pain that places the pain generator and the site of pain in the same peripheral location—the painful tender muscles. Specifically, this study challenges the prevailing theory of pain in FMS.” Katz et. Al.
Studies suggest that the pressure has been building in the cerebral spinal fluid (intracranial hypertension) in both fibromyalgia (FM) and chronic fatigue syndrome (ME/CFS). That could result in all sorts of symptoms.

This study shined a light in a different direction.
But what about the muscles? Many muscle studies have been done over time yet when it comes to explaining FM they are hardly mentioned. Instead its the central sensitization paradigm that holds sway.
The painful, tight and/or constricted muscles were a defining characteristic of the disease. The term fibromyalgia came from the Latin word “fibro” (fibrosis tissue), and the Greek terms for “myo” (muscle) and “algia” (pain).
My muscles, at least, feel like they’re about to pop, they’re so tight at times. It turns out that it’s possible to measure intramuscular pressure, and that’s what this study is about.
An up-ender of perceived knowledge, Katz helped overturn the old fibromyalgia definition, reported that about 75% of people diagnosed with FM do not actually have it, and stated FM is not usually associated with a physically traumatic event.
Katz also validated fibro-fog in FM, and showed that the cognitive problems in FM thankfully do not transition into Alzheimer’s, and showed in an 11-year study that FM tends to stick around for the long term.
Now Katz is upending something again. Katz has been pretty firmly embedded in the school of FM which attributes most of its manifestations to the central nervous system. In “Intramuscular Pressure is Almost Three Times Higher in Fibromyalgia Patients: A Possible Mechanism for Understanding the Muscle Pain and Tenderness“, he challenges whether the central sensitization hypothesis can explain everything.
That’s an important question because, as Katz points out, the first-line drugs (pregabalin, duloxetine, and milnacipran) used for pain in FM (the only ones most doctors know about) attempt to reduce pain by altering central nervous system activity. Given that no one is particularly pleased with the treatment options available for FM, maybe it’s time for another slant.
The authors assessed intramuscular pressure (IMP) in FM researchers’ favorite muscle – the trapezius muscle – a big triangular muscle extending over the back and the shoulders. Thus far, trapezius muscle studies have found evidence of problems with neuromuscular control, hyperactivation, decreased collagen levels, increased levels of pyruvate and lactate (anaerobic energy metabolism), altered EMG readings, mitochondrial dysfunction and altered conduction velocity.
Intramuscular pressure was assessed using something called a Stryker pressure gauge attached to a needle through which saline was injected to a depth of about 2 cm. Muscle pressure was recorded in mmHg. Muscle tenderness was also assessed.
The study was a big one – consisting of over 100 people with FM and 30 healthy controls.
Results

High muscle pressure could be squeezing the capillaries – reducing blood flows to the muscles.
The researchers must have had an idea that they would find muscles under high pressure in FM, but I wonder if they were surprised at what they found. Stating that muscle pressure was “extremely elevated” in the FM patients, they reported that it was three times higher… The intramuscular pressures were so different in the FM patients, the authors suggested they might be a diagnostic biomarker.
Ninety-eight percent of FMS cases had a muscle pressure ≥ 23 mmHg. ( A normal resting value appears to be somewhere about 8 mmHg.) Adding weight to their already impressive findings, they found that pain and tenderness was positively associated with pressure; i.e. the more pressure the muscles were under, the more pain the FM patients were in.
Muscle pressure did not vary according to age – no matter what your age, if you have FM, it looks like you have high muscle pressure.
High (Very High) Muscle Pressure
So what does high pressure do to a muscle? The authors reported that it can compress the capillaries – the smallest blood vessels – possibly obstructing blood flows to the muscles – reducing the delivery of oxygen to them – causing the muscles to rely more on anaerobic energy metabolism, resulting in fatigue and pain.
Then they referred to a 2007 hypothesis, “The pain of fibromyalgia syndrome is due to muscle hypoperfusion induced by regional vasomotor dysregulation“, which was may have been well ahead of its time. It proposed that the muscle pain in FM was due to vasoconstricted (narrowed) blood vessels that were producing low oxygen levels in the muscles.
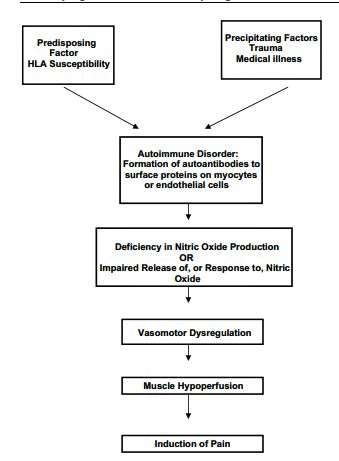
Proposed causal pathway from 2007.
Even back in 2007, plenty of evidence suggested muscle and blood vessel problems causing diminished blood flows and aerobic energy production problems were present in FM. The authors even proposed that autoantibodies were interfering with the ability of the blood vessels to dilate. Similar hypotheses are now being explored in ME/CFS and postural orthostatic tachycardia syndrome (POTS). The authors hypothesized that central sensitization was a reaction to a chronic ischemic state in the body.
They also suggested that hyperbaric oxygen therapy – which now has a couple of positive studies under its belt – could be helpful. They also noted that magnesium – a supplement commonly used in FM and chronic fatigue syndrome (ME/CFS) – can help to dilate the blood vessels by supporting nitric oxide (NO) release. (NO is produced by the blood vessels to dilate them.) They also suggested that the intravenous Myers’ Cocktail might help as well.
Except for one placebo-controlled study which did not find Myer’s cocktail more effective than placebo in FM, that was the extent of Katz’s contribution to FM. A 2018 review of FM muscle findings, however, noted that many older studies did find abnormalities indicative of hypoxia or low oxygen levels. As the central sensitization hypothesis became ascendant, though, muscle studies became less frequent.
A recent blog highlighted how an “amyloid cabal” – much to the field’s detriment – blocked research into other possibilities in Alzheimer’s for decades. The authors noted that central sensitization is happening in FM but rued the overt focus on it. It has not led to effective treatments for most patients.
Now we have a large study showing a rather prominent anomaly – greatly increased muscle pressure – which is not easily explained by central sensitization at all. The authors, unfortunately, did not attempt to explain why muscle pressure was so high in FM patients. (The FM muscle studies tend to be big on finding abnormalities but not so big on explaining them.) While the authors proposed that focusing on increased muscle pressure might open up new therapeutic treatments, they also did not say what they might be.
Still, this rather startling finding should put more emphasis on what’s happening in the muscles and the body. As an added bonus, it opened up the possibility of the first biological diagnostic test for FM.
Keep The News Flowing
Support Health Rising – A Community Supported Website


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Makes sense to me.
i tried hyperbarid oxygen for 10 days long ago and it did not help, and my muscles were a problem
I only get fibromyalgia when I’ve way overdone it, which I don’t do anymore.
I do think that the central pain sensitization model makes sense for me though. I am sensitive to much, including medications.
I also believe our conditions are multiple system, including fibromyalgia.
I agree… central sensitization is definitely part of the picture. Too many studies have shown it is present. The big question is how to fold in central sensitization and all these muscle (and small nerve fiber) findings…We should not discard the idea that central sensitization is behind it all…and we just don’t know to explain that. Perhaps the CS is causing the high muscle pressure via something to do with the autonomic nervous system…(??)
Years ago an acupuncturist told me that my muscles were tight so tight they were pushing the needles right now, she had never seen anything like it. I wonder if that’s related. I didnt /still don’t have a fibro diagnosis but it’s looking more like it.
I have been told many times that my shoulder muscles and/or my back muscles are extremely tight by my PT therapist./
I would love to understand why my upper body gets so darn tight while my lower body does not. Exercise does not make my muscles in my legs tight – it makes my upper body tight.
There are times when my calf muscles will feel very heavy and achy for no apparent reason. I totally understand the comment “they feel like they’ll pop” ! This happens with my arms as well but not as extreme. I have been taking 800mg of magnesium for about four years now.
Hi, what do you mean….you only get fibromyalgia when you’ve over done it ? Do you not mean your symptoms get worse when you’ve overdone it because fibromyalgia just doesn’t come and go, symptoms might but the condition stays you’ve just learnt your triggers. Thankfully anyway
I have always had a problem focusing on the central sensitization emphasis of FM. I have shared with you before about my experience of pushing FM into remission through a week-long juice fast. But this article reminded me of the first sign of my remission which was a softening of my muscles. My muscles used to be rock-hard and sore 24/7 but, never again following that fast. I wondered why my FM specialist gave me muscle relaxants and yet never mentioned that over-tight muscles were a symptom of FM. He was an important FM researcher pushing hard for central sensitization studies. So maybe his biases got the best of him? But, I always held to the opinion that central pain was not the only thing influencing FM. Since that time, I have a diagnosis of POTS (with hypovolemia) and I’m currently being evaluated for Myasthenia Gravis (MG). One thing important to avoid with MG is magnesium since it greatly interferes with the communication between the nerves and muscles in MG. I just learned that and went off magnesium a week ago and I’ve already seen improvement in my symptoms. Mestinon is also recommended in both MG and POTS so I hope both of those conditions will improve too. I wish you much success as you dig deeper into the connection of hypoperfusion in FM. That should help both POTS and FM patients if not many others.
Thanks Maureen. Why do you think the fast helped and have you been able to maintain your progress afterwards?
I think the fast pushed me into healing through ketosis, the body’s way of healing itself. I think modern society is missing something with regular feeding instead of more natural gaps of fasting and ketosis. Valter Longo’s studies are pretty conclusive about the healing power of ketosis. I just stumbled upon it accidentally. Ketosis reversed my IBS and Erythromelalgia too and it keeps my Type 2 diabetes in check. Longo’s studies focused on longevity and he extended them to diseases. I do extended fasts 4 times a year now but most people only need to do them once a year. I am fasting right now and it always amazes me how my Mast Cell Activation disappear in the midst of fasting. Too bad it doesn’t push them into full remission. Fasting doesn’t appear to address everything. But my FM symptoms, IBS and ER never returned and that remission happened in 1997.
That is so cool. I think fasts are great. I just can’t do them much -I know they can work really well. Such a pity I fall apart!
LPS in the bloodstream triggers histamine release and histamine increases vascular permeability. Possible link to the gut.
I think it is tricky to call it a fast, because of the fruit juices. Were you drinking as you felt the need? My money is on the elimination of tryptophan and the fruits juices providing fructose which is pro-metabolic. Have you looked into Ray Peat?
This seems right to me. My trapezius muscle is constantly activated, exhausted and painful.
Even taking big doses of magnesium, I’ve found the biggest problem with fibro is the muscle tension, not the pain. I can be so mentally relaxed that I care barely stay awake, but my muscles are still mega-tight. I can tolerate high muscle tension, but it leads to frequent injuries: pulled muscles, tendinitis, etc. Then the injuries keep me from being active and staying fit. Then everything hurts.
Has anyone speculated that this may tie into other existing hydrodynamic findings? Like the ME/CFS inflexible blood cells having a hard time being pumped around, or the recent vascular hardening results?
So that 22 gauge needle used for the pressure testing is the smallest regular use IV needle – and it was stuck almost an inch into the trapezius! That must have been fun – many thanks to the participants for smiling through that situation.
“That must have been fun – many thanks to the participants for smiling through that situation” They did say it was a bit trying 🙂
“Stating that muscle pressure was “extremely elevated” in the FM patients, they reported that it was three times higher…”
“The authors reported that it can compress the capillaries – the smallest blood vessels – possibly obstructing blood flows to the muscles – reducing the delivery of oxygen to them – causing the muscles to rely more on anaerobic energy metabolism, resulting in fatigue and pain.”
“Has anyone speculated that this may tie into other existing hydrodynamic findings? Like the ME/CFS inflexible blood cells having a hard time being pumped around, or the recent vascular hardening results?”
It IMO all ties in. From Wikipedia(Circulatory_system#Closed_cardiovascular_system):
“The lymphatic system… …One of its major functions is to carry the lymph, draining and returning interstitial fluid back towards the heart for return to the cardiovascular system, by emptying into the lymphatic ducts.”
Interstitial fluid is fluid in between the cells and tissue, but outside the blood circulation. This is rather important. Blood circulation is often depicted as a closed loop system, with every single drop of blood going out of the heart going through the arteries, passing by the tissue and returning through the veins to the heart again. This is not the reality. The above says that fluid *keeps* being added “back towards the heart for return to the cardiovascular system, by emptying into the lymphatic ducts.”
If nothing got lost then this “adding fluids” would keep increasing blood volume and pressure. The interstitial fluid found in between the tissue isn’t comming there through the skin. It’s getting there from the heart and being brought there by the arteries. Hence the word *return* in “back towards the heart for *return* to the cardiovascular system, by emptying into the lymphatic ducts.”
That “interstitial fluid” that got stuck in the space between cells and outside the blood circulation is brought there by the heart and arteries and needs to be returned by the lymphatic system *to the heart and blood circulation*.
I saw better refferences before and am too tired to find one now, but IIRC roughly 95% (in a healthy person) of blood supplied by the heart through the arteries returns to the heart through the veins. That means 5% is not returned that way. Part of it will be evaporated by sweat, part will get to the bladder and part will end up between the cells near but next to the cappilaries.
The pressure at the site of blood capillaries is already a whole lot lower then the pressure at the heart side. As anybody with (leg) edema can tell, water can pile up in the legs as pressure is too few to effectively return all blood / liquid easily and efficiently to the heart through the veins.
The poorer blood circulation, the harder it is to squeeze sufficiently high amounts of blood / liquid arriving through the arteries back into the capillary veins and get it transported back to the heart.
If (IIRC) 95% of blood liquid is returned to the heart “each round it travels back and forth to the heart” in healthy people and if only 90% or less of that volume would be returned in our case, then more of it would “pile up in the interstitial fluid”. With ME/FM/… patients frequently having both stiff RBC (making blood flow slow and hampered) and low NO production (making arteries, veins and capillaries more constricted and narrow) it is easy to see that it will be hard to let return as high a percentage of the liquid provided by the heart and arteries to the veins and heart again.
The possible result of exercise? Let us assume the FM patients muscle were already tense to start with. You start to exercise. More bloods needs to be send towards the muscle. More blood arrives at the muscle capillaries. It may be less then what would happen in a healthy person (as tense muscles squeeze the arteries), but more is arriving then at rest. Lymph capillaries and vessels in the muscle however are *also* squeezed by the arteries. So they will be narrowed too. That will make the return of interstitial liquid to the heart via the muscle lymphatic system difficult. The same squeezing of the cappilary veins and veins in the muscle will make returning of the liquid in the muscle difficult too. More liquid WILL have to pile up in the muscle tissue in order to increase the local tissue / muscle pressure squeeze enough of that liquid back in the combined lymph and vein return paths. And so: increased muscle pressure.
At rest, lymph capillaries and veins still will be squeezed, so muscle pressure needs to stay high at rest in order for liquid piling up (edema) not becomming excessive. It’ll only get even worse at exercising. Then both muscle pressure rapidely will rise and blood flow still will fall short damaging muscles, creating inflammation and damaging muscle tissue, blood capillaries and plausible lymph cappilaries. In adition, poor oxygenation during exercise will create oxidative stress damaging muscle tissue, blood capillaries and plausible lymph cappilaries AND RBC making those more stiff. If that mess would take a few days to resolve after exercise, you could get close to seeing part of what is called PEM.
That problem with liquid returning to the heart could also be seen in the frequently reported poor heart preload. That is sort of saying that too few blood flows back to the first chamber of the heart. In other words, to few blood is returning easy enough to the first chamber of the heart.
There is also an ME equivallent. If returning capillaries are too constricted and RBC are stiff, return of blood from the brain to the heart will be hampered even if it has to flow downwards (when standing). When laying down, it even gets worse. More blood will flow to the head as it doesn’t have to overcome gravity to travel upwards. But it will be harder to get blood return as it no longer has the aid of gravity to flow back to the heart. Blood flowing more easily to the head, less easily returning to the heart? More liquid will pile up in the head. That very likely will increase brain pressure and be worst at night. Nights can be horrible for ME patients when it comes to recovery. With blood flow and CBF pressure IMO messed up worst at night, that does not surprise me.
Arteries, blood vessels comming from the heart, have to withstand a larger pressure then veins, blood vessels returning to the heart. This is because the blood pressure is highest near the aorta and drops along the way.
This results in arteries, including capillary arteries, being on average quite a bit more musculare and stronger build then veins. That can be found and seen in pictures of tissue cross sections that show one of each. The pictures of coarse need to compare similar capacity arteries and veins for good comparison.
One of many examples to be found is in https://s3.amazonaws.com/MagscopeScans/Histology/histology001/artery_and_vein_mammal/artery_and_vein_mammal_x10_800px.jpg.
Here you see vein on the bottom left. It is more muscular and strongly walled and smaller in diameter and cross section. The more muscular and strong structure can better withstand the higher presssure that arteries see compared to veins. The smaller diameter and cross section still allows to transport as much blood as the larger diameter and cross section of the vein as the artery has more pressure drop available to transport the blood through a smaller pipe.
The vein on the top right is thinner and less strongly walled and bigger in cross section. The structure does not need to be that strong as it is exposed to lower pressure. Its bigger cross section allows to transport comparable volumes of blood with lower pressure differences.
When muscles are very tense, that works against the veins more then against the arteries however. The more muscular structure of the artery can not only better withstand the higher pressure of blood, but also the higher counter pressure of tight muscles. Hence, it is logical that the veins comparatively will be squeezed more then the arteries by tense and tight muscles.
When both arteries and veins are squeezed by the muscles, but veins more due to their weaker structure, they will be squeezed comparatively more then the arteries. The flow of blood from the muscle to the heart thus will be more hampered then the flow from the heart to the muscle.
More pressure at the tissue side will be required to push the liquid / blood from the muscle back towards the heart compared to what is needed in healthy people. An equilibrium will arise where more blood liquid converts to interstitial liquid (aka a sort of edema) and a higher percentage of blood liquid will not return through the veins. That all in itself will create a rising equilibrium till there is a working balance. It will be a working balance with considerablee higher muscle pressure however.
Thanks dejurgen. What a great synopsis and proposed interconnection of those concepts/findings.
As well as the authors of this study (it seems like a bit of a family affair – I hope not too many people are sick), it is reassuring having someone like Dr David Systrom involved in ME/CFS and FM research. That is, keeping these topics on the move. I’m going to go off and watch some updates I haven’t been across.
“When laying down, it even gets worse. More blood will flow to the head as it doesn’t have to overcome gravity to travel upwards. But it will be harder to get blood return as it no longer has the aid of gravity to flow back to the heart. Blood flowing more easily to the head, less easily returning to the heart? More liquid will pile up in the head. That very likely will increase brain pressure and be worst at night. ”
I find that to be true for me. I have to raise the head of my bed and have my mattress at a slope. I still then put more pillows to raise my head. It does help with head pressure and brain drainage. Also has help my arena and breathing. (As has using mouth tape, to change breathing patterns and to keep breathing through the nose and not the mouth.) It doesn’t appear I even have apena any more. My Fitbit register my O2 to be staying pretty consistent and not in danger zone, either with breathing or heart rate while sleeping. And I don’t wake up with headaches any more. Or feelings like there is too much fluid and it will explode.
I was beginning to feel other people aren’t experiencing the tight, tight muscles since I don’t hear about that as much from people these days. It made me wonder if I had only perceived that was a common problem and I had to look for the cause. Maybe that’s because LDN is somewhat effective in treating the symptoms. My cognitive abilities seem to be declining and I question everything. I’m very discouraged and beginning to think only CRISPR or something that far out will be an effective treatment.
CRISPR provides such opportunities. Let’s hope they land on ME/CFS/FM
Cort, you should try Longo’s fasting- mimicking diet. He used low carb selections to keep you in Ketosis for 5 days. You can also ha k his diet using avocados which I do at times. Ketosis can be achieved without starvation. I get cold but never hungry when I fast. I drink a lot too.
Thanks Maureen :). I will check it out. When I could do fasts they worked wonderfully.
I have very tight painful squeezing feeling muscles in my neck and traps, one of the only things that helps is lifting heavy weights.
Searching Thyroid and Muscles I found, with low thyroid our muscles including the heart can NOT relax.
Full thyroid panel not just TSH. If only my HMO did that. There are signs, just look at my puffy face, called Mucin.
Excellent book: Hypothyroidism type 2, By Mark Starr M.D.
This makes so much sense, I have a lot of osteopathic treatments to manage my ME/CFS (or is it fibro?). Practioners often remark how tight some of my muscle groups are (shoulders, abdomen, neck and back). It’s a constant labour of love to keep everything loosened off. I know when I’m going to flare as my shoulders go super tight again.
Do you think muscle tension, vein narrowing and lower blood flow could cause higher blood pressure in fibromyalgia? I’ve had fibromyalgia for over 30 years and have been taking a beta blocker for almost three years now. I’m trying to taper off the BB now because of negative side effects. I found this article most interesting.
I’ve always been suspect that central sensitization/pain amplification theory accounts for so much of experienced pain.
This new information–excessive muscle pressure/tension–might inhibit blood flow, and if one has this problem, it could also affect blood flow to the brain–and promote ‘fog’ and impaired thinking. I wonder if Fibro Folks ever find that being relaxed (and not necessarily laying down) helps with their thought processes.
Being in the EDS camp, I do know that with flawed connective tissue, I tend to get very tight muscles in areas where my body is unbalanced as it struggles to ‘hold itself together.’ Most people have some sort of habitual misalignment and this may contribute to excessive muscle tension as well.
More tension, less blood (oxygen), more tension and that could set up a pain cycle. One system out of balance–more systems out of balance…
As I run all the possible reasons for this study result and how it may contribute to treating ME/CFS and fibromyalgia, so many possible different contributing factors come to mind. Makes my head spin and good luck sorting it all out!
Thank you Cort!
@Nancy B,
“Being in the EDS camp, I do know that with flawed connective tissue, I tend to get very tight muscles in areas where my body is unbalanced as it struggles to ‘hold itself together.’”
I was looking for a place to put this very thing.
Me also with EDS and POTS and ME/CFS and FMS. I have to tense up a lot to “Hold myself together”. There is definitely blood flow issues. And that tightness and pulling things out of place because of it…..for sure causes plenty of pain. When its real bad a very mild muscle relaxer called Bentyl (usually used for IBS to relax the colon) and a 1/4 pill of a lowest dose of Tramadol is enough to relax things, settle down the autonomic nervous system and make me so much better. I don’t use it regularly as it will stop working. But its nice to have as a backup when things are really bad.
I think there is something definitely to this line of inquiry But it seems like there are far better ways to support nitric oxide production than magnesium. What about citrulline? Beets? Tadalafil?
I do believe fibromyalgia is a disease of retention and the pain and pressure can be reduced by reversing the disease process, something I have been doing for 13 years now using guaifenesin extended release and avoiding topical salicylates on my skin and in my dental products. It helps relieve intercranial pressure and tingling in my spine also. I have both fibromyalgia and CFS ME.
“They also noted that magnesium – a supplement commonly used in FM and chronic fatigue syndrome (ME/CFS) – can help to dilate the blood vessels by supporting nitric oxide (NO) release. (NO is produced by the blood vessels to dilate them.)”
You can boost NO with diet. Beet juice has been studied as a “performance enhancing drug” for sports. Top ten foods that boost NO include Arugula, rhubarb, beet greens, butter lettuce. You can buy test strips easily online.
I’ve done a smoothie with an entire raw beet every morning just for this reason.
Thanks Cort for another fantastic article!
I recently had a Covid vaccine and the woman giving me the shot had a difficult time getting the needle into the muscle in my arm.I can relate to tight muscles in the neck and upper back but was surprised at having difficulty with the shot. My arm was supported and in a relaxed position.
I think in ME/CFS or FM we should not attempt to place peripheral pathology in contrast to central pathology (here: muscle pathology against central sensitization/neuroinflammation) because muscle pathology (e.g. raised pressure) may be a reflection of perfusion problems which may easily be explained as a manifestation of central neuroinflammation and concomitant autonomous dysregulation. For me this falls into the same category as mitochondrial dysfunction: yes, it is indeed a “peripheral” manifestation but its origin plausibly is central.
It is very importent that the relationship between FM and Myofascial Pain syndrome (MPS) is beeing investigated! I have for a long time suspected that FM is a generelized version of MPS. MPS is characterized buy the presence of taut bands and trigger points. Recent studies have shown that there are microscopic contracture knots comprised of segmentally contracted sarcomeres in resting muscle of these patients.(1,2) The intramuscular pressure of the taut bands has been quantified using Magnetic Resonance Elastography, and was found to be significantly higher than in normal muscle tissue.(3) To investigate this, the pressure in FM muscle should be topographically measured, to see if the pressure is uniformely elevated or if there are regions with higher and lower pressure in the same muscle. If it is the latter the FM patients should be palpated for taut bands. If the higher pressure is restricted to the areas of taut bands, this would confirmed the hypothesis. If the pressure is uniformely distributed in the muscle this disproves the hypothesis. Also, a surface EMG devise should be used to see if the higher pressure is caused by nervsignals from CNS. If there is no increased EMG activity compared to controls, this would be compatible with the hypothesis. If there is increased EMG, this would suggest that FM patients are tense, but my hypothesis is that they are not. My hypothesis is that what has actually been measured in this study is the intramuscular pressure of taut bands.
1. Jin et al. The patophysiological nature of sarcomeres in trigger points in patients with myofascial pain syndrome: A preliminary study. Eur J Pain. 2020;24:1968-1978
2. Gerwin et al. Foci of segmentally contracted sarcomeres in trapezius muscle biopsy specimens in myalgic and nonmyalgic subjects: preliminary results. Pain Med 2020;0:1-9
3. Chen et al. Quantification of Myofascial Taut Bands. Arch Phys Med Rehabil 2016 Jan;97(1):67-73.