

Both chronic fatigue syndrome (ME/CFS) and postural orthostatic tachycardia syndrome (POTS) have received far more attention than fibromyalgia regarding long COVID. Despite the large overlap between fibromyalgia (FM) and ME/CFS, and the fact that FM can be triggered by infections as well, we’ve hardly heard anything about a potential overlap between long COVID and fibromyalgia.

Are men being left out? Is the gender balance overstated in FM?
That seems strange. Fibromyalgia appears to strike the same general demographic as ME/CFS and long COVID: patients tend to be fairly young and female.
That overt female dominance in FM, though, may be due more to physician bias than anything else. A 2018 study that took physician bias out of the picture concluded that only 59% (as opposed to figures as high as 90%) of fibromyalgia patients were women. The bias, if it is there, is probably due to doctors with confirmation bias, who, believing the FM is primarily a women’s disease, find it more in women and less in men than they would otherwise.
FibroCOVID?
A recent study, “Fibromyalgia: a new facet of the post-COVID-19 syndrome spectrum?”, featured a web-based survey. Web-based surveys aren’t the most accurate surveys, but they’re being commonly used, and researchers have gotten better at creating them. An Italian group required that participants report they had had a positive COVID test, and had been diagnosed with COVID-19 by a doctor, and had gotten sick with COVID-19 at least three months prior to taking the survey. Six hundred and thirteen people completed the survey.
Given the demographics seen thus far in long COVID, it was not surprising to see that most (78%) were women, the average age was 45, and 11% had been hospitalized. Except for the 5% with inflammatory arthritis, few musculoskeletal issues were reported prior to coming down with long COVID.
While this study did find more people with long COVID and fibromyalgia in women, the disparity between women and men (57-43%) was not that great, and was similar to the proportions found in the 2018 study mentioned above. Men who ended up having FM and long COVID, in fact, tended to fare worse than women: they had higher rates of hospitalization and more often needed to be treated with oxygen.
A similar kind of bias may exist with regard to ME/CFS and FM. Since doctors are more familiar with FM than ME/CFS, they may be more likely to diagnose FM when they meet up with a patient with symptoms of pain, fatigue, cognitive and sleep problems.
Thirty-one percent of the long-COVID patients (average duration 6 months) met the criteria for FM. Several risk factors for coming down with a fibromyalgia form of long COVID were unearthed. Interestingly, given reports that most people who come down with long COVID have not been hospitalized, being sick enough to have been hospitalized and received oxygen increased the risk of being diagnosed with fibromyalgia. So did having a higher body mass index, being obese, and having high blood pressure. Experiencing cough and difficulty breathing during the infections were less significant risk factors.
Obesity has been talked about quite a bit in FM, but is it actually more prevalent in FM? Given the pain and physical limitations FM produces, perhaps one would expect it to be. A meta-analysis concluded that the overall rate of obesity in FM was 35.7%, with the rates of obesity higher in the U.S. Compare that, though, to a CDC study, which found the prevalence of obesity in all U.S. women 39.7% (aged 20–39), 43.3% (aged 40–59), and 43.3% (>60 years).
While obesity does increase one’s chances of coming down with FM after getting COVID-19, obesity doesn’t appear to be more prevalent in FM itself. The fact that obesity may increase one’s chances of getting an FM brand of long COVID is probably not surprising, as obesity probably increases the chances of all sorts of complications from COVID-19. Obesity, after all, negatively impacts many disease outcomes and may almost be as bad for your health as smoking.
The author’s ideas about why COVID-19 might be producing an FM form of long COVID were nothing new, and basically mirrored other ideas about long COVID: virus-induced damage to the endothelial cells lining the blood vessels or the neuromuscular structures, immunological changes and smouldering inflammation.
The authors believe FibroCOVID is going to lead to more work for rheumatologists.
“it is reasonable to forecast that rheumatologists will face up with a sharp rise of cases of a new entity that we defined ‘FibroCOVID’ to underline potential peculiarities and differences, such as the male involvement.”
The authors asserted that long-COVID clinics and doctors should include easy FM assessment tools, such as the Fibromyalgia Rapid Screening Tool or the London Fibromyalgia Epidemiology Study Screening Questionnaire, to determine if FM is present.
Perhaps we should, as some physicians have recommended, view ME/CFS and FM as similar diseases that occur on a continuum. That entire disease entity would affect from three to possibly over 10 million Americans. (ME/CFS: 1-2 million; FM: 2-10 million). That’s a lot of people who could benefit from insights and treatment options gathered from long-COVID research. For instance, the authors noted that immunotherapies not being used in FM will likely come into play for long COVID.
For their part, people with long COVID may be able to benefit from insights into fibromyalgia as well (see below).
Small Fiber Polyneuropathy Found in Long COVID
Talk about a fibromyalgia connection. Small fiber neuropathy or in the case of fibromyalgia, polyneuropathy, was first uncovered in FM in 2013. Since then, dozens of studies have validated its presence in somewhere around 40% of FM patients. It took quite a while, but recently a study confirmed that small fiber polyneuropathy (SFPN) is present in chronic fatigue syndrome (ME/CFS) as well. Now, a research group that’s assessed SFPN in fibromyalgia has moved on to long COVID.
Small fiber polyneuropathy refers to the damage and/or destruction of small, unmyelinated nerve fibers that transfer sensory and/or autonomic nervous system signals in the skin and/or eyes. FM studies have typically found narrowed small nerve fibers and lowered numbers of small nerve fibers in around 40% of patients. Symptoms associated with SFPN include tingling sensations, burning pain, pricks, electric-like sensations, heavy feeling feet, cold extremities, decreased sweating and others.
This study (“Corneal confocal microscopy identifies corneal nerve fibre loss and increased dendritic cells in patients with long COVID“) gave 40 long-COVID patients several questionnaires, including a National Institute for Health and Care Excellence (NICE) Long-COVID Questionnaire, which contains a neurological section and the Fibromyalgia Questionnaire (FM-Q) to assess the severity of muscle pain and other symptoms. The neurological section of the NICE questionnaire asked about symptoms like brain-fog, headache, sleep problems, dizziness, taste or smell problems and tingling sensation. They used a non-invasive laser scanner to assess nerve density in the cornea of the eye.
The average time after a COVID diagnosis was almost 4 months. Neurological symptoms – that were possibly caused by SFPN – were found in 55% of long-COVID patients at 4 weeks and (demonstrating that some improvement had occurred), in 45% at 8 weeks. The fact that long-COVID patients with neurological symptoms had lower corneal nerve fiber density suggested that small nerve fiber problems may have contributed to their symptoms. As has been found in fibromyalgia, the long-COVID patients with small fiber neuropathy tended to have more severe symptoms.
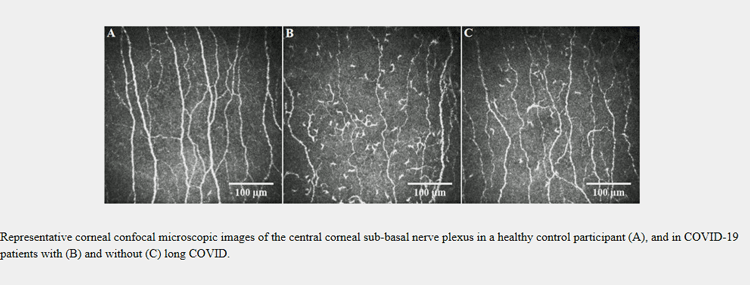
Check out the broken up small nerve fibers in the FibroCOVID patient in the middle.
Because only the skin or the corneas of the eyes have been tested, we don’t know the extent of the small nerve fiber problems in fibromyalgia, ME/CFS or long COVID. It’s been speculated that small nerve fiber problems found elsewhere could be affecting the microcirculation, contributing to orthostatic intolerance, affecting gut issues, etc. The range of possibilities is large – and quite speculative at this point. Despite several efforts, no one has been able to identify the cause of the SFPN in FM.
Echoing Dr. Nath’s assertion that a very aggressive innate immune response may be responsible for the inflammation seen in COVID-19, the authors stated that the small nerve fiber losses were “consistent with an innate immune and inflammatory process” caused by activated dendritic cells migrating into the cornea. It should be emphasized that this problem does not impair vision, and no sight problems have ever been associated with reduced small nerve fibers in the eyes of FM patients.
There was also some good news. In contrast to other nerve fibers, small nerve fibers can repair themselves, and some evidence suggested this was occurring. As noted above, some of small nerve fiber findings seen at 4 weeks began to rebound at 12 weeks.
The authors noted that COVID-19 patients diagnosed with another small nerve fiber diseases (Guillain-Barre Disease) did well with plasma exchange, which has been mentioned before in terms of long COVID. Plasma exchange or plasmapheresis involves replacing the plasma (liquid portion of the blood) with a substitute. It’s not curative but is used in a variety of autoimmune and neurological diseases to relieve symptoms.
Conclusions

Two studies suggest FibroCOVID is a real and pertinent part of long COVID.
We definitely need bigger and better studies, but these two early studies linked long COVID and fibromyalgia together in two ways: their symptom presentation and small nerve fiber damage. That made sense. Fibromyalgia has kind of been the missing disease in the long-COVID constellation of diseases, but its strong overlap with ME/CFS, and its sometimes post-infectious onset suggests that it’s going to pop up. The authors asserted that doctors should assess the presence of “FibroCOVID” in long COVID using readily available standardized questionnaires.
The symptom study found that far more men had FibroCOVID (45%) than one would have suspected given the reports of a very strong female predominance in FM. The authors note, though, that physician bias likely plays a role in over-estimating the female predominance in FM, and believe their figures are more accurate. One wonders if better long-COVID studies will lead to a reassessment of the gender imbalance often reported in FM.
While the study did not report percentages, it did indicate that neurological symptoms were common in long COVID, and were associated with the presence of reduced small nerve fiber density/length in the corneas of the eyes. They were also associated with increased symptom severity.
On a good note, small nerve fibers can regenerate themselves, and some improvement was found in 8 weeks. The authors also reported that plasma exchange has been helpful in long-COVID patients diagnosed with another nerve fiber disease (Guillain-Barre), and noted that immune therapies not currently used in FM might prove helpful in FibroCOVID.
Check out Health Rising’s Small Fiber Neuropathy Resource Page


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Cort,
Just a little about myself. I will be 84 in Sept. & inherited my FM/CFS from my Mother.
Like most of us I went to the whole gambit of doctors who could not find anything wrong except to say, it was a woman thing, I worked too hard or the worse one, saying it was all in my head. Meaning I was mentally unbalanced. I now have cognitive dysfunction from fibrofog due to mini strokes.
My Mother verified that I as a tot I started to walk, but fell & did not walk until much later. As a little girl I complained about my legs hurting & was told it was growing pain. I never outgrew the pains as my Mother verified & she had the same problems. She also verified that I was tired all the time & had to rest, etc.
At age 20 I had to quit my first good stand up job & get a desk job with my legs elevated on a stool. I got married had two children & had to work to help with finances.
During the following years I had 3 major automobile accidents that were not my fault, but I feel these accidents really set off the FM. I received a whiplash with the first one that can still bother me.
After having FM for awhile, just to be sure I went to see Dr. Mark Pelligrino, who has FM himself, he wrote a book about auto accidents affecting FM, & other books on FM. I lived in Ohio & since he was located in Canton, OH I went to see him to be sure I had FM & the results were positive.
I am probably one of the luckiest ladies with FM, because my personal physician Dr. Christopher Cartellone, Solon, OH, who knew nothing about FM decided he would learn about it & kept me as his patient for 22 years, until I moved back to MD.
Now about the article on FM/CFS & Covid. You mentioned that there was questions about obesity & FM. I was not diagnosed with FM until 1993 after reading an article in the Arthritis Magazine. I was really in bad shape, could hardly walk & had to quit working altogether. After being diagnosed I put on 40 lbs. in no time without changing my eating habit, plus more later. So I’m stating you may not be obese before FM, but I bet many people put on weight after being diagnosed.
The other thing is whether ME/CFS is a relevant part of FM. As I stated early in my post yes, yes, the overwhelming fatigue is with me 24/7 & has been all my life. Years ago my gyn doctor took pity on me & gave diet pills just to give me energy. Again I bet others can attest to the same overwhelming fatigue.
Cort, I do not understand all the new medical terms or initials that are used to write about our illnesses as I’m in the winter of my life. Forgive me for not being that informed & thanks for letting me share just a little bit of my saga with FM/ME/CFS.
@Kay,
Have you ever been evaluated for having Ehlers-Danlos Syndrome? I don’t think fibromyalgia is something that is ‘inherited.’ Perhaps there is genetic proclivity towards developing it–but not directly inherited.
To add to the discussion, EDSers ofter have cross over fibromyalgia-like symptoms and approximately 50% have been found to have small fiber neuropathy. We are also low down on the pole for investigative studies, so that percentage is only a guess.
Also wanted to share this Japanese study on just how long does long haul Covid last; https://www.medpagetoday.com/infectiousdisease/covid19/94227?xid=nl_covidupdate_2021-08-27&eun=g1240599d0r&utm_source=Sailthru&utm_medium=email&utm_campaign=DailyUpdate_082721&utm_term=NL_Gen_Int_Daily_News_Update_active
Hint, hint, there are people still suffering after a year. Sound familiar?
Did you know Ron Davies and Whitney Dafoe have eds..not just a crossover with fibro.
I got covid early on. I recovered back to baseline. Then ever since I’ve been getting reactivations. Including a few new symptoms. Arm weakness, bones in neck hurting. Gums hurting and bleeding and a combo of itching that comes and goes and needle like insect bites that come and go.
Worsened feeling of fatigue and pem
I think it is important to make the distinction between EDS and hEDS.
hEDS most likely is not EDS… It’s the only subtype without a genetic mutation.
And by the way, there are cases of Congenital Adrenal Hyperplasia that present with joint hypermobility and EDS-like features. Its called CAH-X.
EDS specialists don’t seem to know about it. Have never seen it mentioned in the EDS Society literature or in any medical literature as a differential diagnosis.
Thanks for sharing your story, Kay. Fibromyalgia has not and continues not to get even close to the research funding that millions of people who have it deserve. In fact, fibromyalgia gets considerably less funding per patient than ME/CFS. That’s on the NIH and its hands-off, laissez-faire approach to funding disease. Now that they’ve been given lots of funds to study long COVID let’s hope that that unveils more understanding of FM. This post was written in the hopes that will happen.
Cort,
Thanks I have hoped & prayed for research about FM many years. I will be so elated when it become a disease (that’s truly what it is) instead of it being a syndrome. Kudos to you & keep up the good work.
I am sorry you have suffered and also sorry doctors at least used to be blindsided by the diagnosis and chunk it off to women and pain. Well 9 in my family have it, I pretty much know why, but some cousins I have not met, my Mom and my three sisters, along with other trailers that go with the mess. I too had a hard time with my legs growing up. I often had to opt out of gym because of them. After 9 years with Fibro, I managed to get hit with full blown ME/CFIDS and there I have suffered the most. I left the USA for the Peruvian Desert and eventually to Costa Rica where my pain level dropped to tolerable vs. severe in the USA. Skin, blood and hormones. I have it under control now but the Me/Cfids is beating me up. Eating puts me to sleep for hours each meal. I don’t like this life… can’t clean my house. I am 74 but should not be sleeping 16 hours a day. These illnesses are no piece of cake even when you can write your own book about them. Hugs.
I really hope some bureaucrats at the NIH read these stories.
Cheryl Mumford. Thanks for your post. I am sorry to hear that you went from CFS to CFIDS.
When I was finally diagnosed in 1993 with FM I set out to find all the information I could about my illness. I joined & for many years used an online group for FM/CFS from Canada. Obtained books by Dr. Devin Starlanyl & Dr. Mark Pelligrino (became his Patient for a short while, stopped seeing him because of the distance I had to travel, the trip made my FM worse). My legs were so bad I could hardly walk, used a quad cane, fell a lot & of course had all the shooting pains with terrible aches, that I believe increased my anxiety & depression. When I had to stop working I then was able to travel with my husband (a salesman) going to conventions, etc. My doctor kept telling me to stop traveling, but I kept going until 1998, by then I would get so fatigued that I’d end up eating & sleeping in our room, while my hubby continued the
night without me. I then felt badly because my hubby counted on me to be with him.
I too opted out of gym because I was not able to do the exercises, play any games like softball, etc. as they said “you run like a ruptured duck.” Instead of gym I took Spanish.
All along I had back problems with back pain & in 2000 I had surgery to connect my spine to my sacrum. My surgeon said it was like this from birth & I ended up with 4 tubes, 4 screws about two inches long with flesh taken from my buttock to make it heal.
Now my left thigh down to my knee gets numb, feels like pins & needles, is very achy with some shooting pain. My left leg also has a swelling big bulge right below the knee that acts up all the time. I keep it elevated to keep the swelling down.
I live with my son & luckily I have a friend that comes to give me a shower, wash my hair, do my laundry, clean my room, etc. I’m unable to do anything except my meals that I can
microwave. I can still walk, but not far,
with no steps & only go out to the doctor, etc.
I imagine you can related to all of my symptoms.
Just want to comment on CFIDS..I met my friend Gail online & we corresponded with phone conversations. She told me that after graduating from college she got a job, but had to quit because of CFIDS. Over the years she would tell me how she wanted to clean her bedroom but did not have the energy to do so. Her physician is the well know Dr.Lapp located in Charlotte, NC. Eventually Gail asked me not to call her. I assumed she needed to be left alone. At Christmas I sent a card to her & I received a note saying that she had passed on. She was young & suffered so much. Now I find out that the FDA considers it as CFS that you did have.
Gail told me about all the colds, viruses, allergies etc. that she could easily catch.
Cheryl, to end this if you are interested in what Dr. Lapp & his Associates have to say about CFIDs.
Check you website For Phoenix Rising & look under Dr. Lapp’s Ampligen series.
When I was just starting I used to call Phoenix Rising with my questions. They were very caring & helped me a lot. Maybe just call & they can help you.
Take care with my love!
So interesting! I too was told my aching legs as a little girl were caused by growing pains. I too inherited FM from Mom.
Diane.. Thanks for your post. I’m sitting
in my adjustable bed with my legs elevated because they are hurting so badly I could cry. Maybe I will before the remnants from hurricane IDA passes over in the next two days.
According to an earlier post FM can’t be inherited as both you & I have believed. There isn’ anything to prove it or disprove it at this time. Research is saying FM can be found clustered in families or that we might receive this through our DNA genes.
When we have bad weather of any kind my whole body changes. I usually end up in bed under a warm blanket, or with a heating pad, etc.
I certainly can relate to you & will continue to believe I inherited FM from my Mom as I saw her go through the same things I have struggled with.
Take care as you continue to struggle.
I don’t want to fuel vaccine hesitancy, but I just ran across this article about some rare neurological effects from the Covid vaccine; https://www.medpagetoday.com/neurology/generalneurology/94151?xid=nl_popmed_2021-08-27&eun=g1240599d0r&utm_source=Sailthru&utm_medium=email&utm_campaign=PopMedicine_082721&utm_term=NL_Gen_Int_PopMedicine_Active
Nancy B. Thanks for sharing about Ehlers-Danlos Syndrome. I’m not familiar with that illness. I go first to the Mayo Clinic who happens to be a good research hospital for my information, plus they treat FM patients at their hospitals. After reading the symptoms & looking at pictures I am sure that I do not have EDS.
I did not know that FM could not be inherited so I also looked up what Mayo Clinic had to say about inheriting FM from your family. It said “FM is not passed directly from parents to children, but the disorder appears to cluster within families.”
It further stated “DNA studies from family members with FM or other chronic pain syndromes have turned up a number of genes that could help explain why these disorders seem to run in families. Each of these genes plays a role in your nervous systems response to pain. Odds of developing FM are several times higher in the immediate families of people with FM than in families in which no one has FM.” I know that I’ve had FM all my life, whether inherited or passed on through genes. The most important thing to me is that I do my best to accept my illnesses with my doctors care, my faith, & the Triune God’s Help
I shared about my FM because it was my first time posting. However the only thing that I was posting about was the tests given for Coronavirus Side Effects Poll Update that Cort had posted. I never had the Coronavirus, just the two shots from Moderna. By the way I had terrible Fibrofog for 15 days a little over a month later, after my last shot. Otherwise, I was okay.
The exceptions were the obesity & the chronic fatigue that Cort talked about. Again, “I have had fatigue all my life & it has become overwhelming. I gained 40 lbs. after I was diagnosed with FM in 1993, without changing my eating habits, plus more lbs. as I became worse.” As far as I’m concerned FM has a lot to do with your weight & your fatigue.
Hi Kay, My mom has a debilitating mystery illness for at least 30 years now that consists of a long list of symptoms. She eventually read a book about yeast/candida I think it’s called the yeast connection and she still says that she has yeast bc going on the diet recommended by the author of the yeast connection helped her. Here I am now in my forties and suffering from a debilitating mystery illness consisting of a long list of symptoms that began when I was 21. There is no way I will ever believe that this isn’t connected to what is wrong with my mother. I took the fm/a fibromyalgia test and it was positive.
I’m not sure about the weight gain thing. I was slimmish when I first got ill. Although I know weight causes inflammation.
I would say eds is not full formed yet as a distinctive set of identifiable variants.
I’d also day there are a lot of overweight people without fibro
I have lost four neighbors, two friends, and have one now in the hospital for 30 days. He is only 40. We have a choice, catch covid over and over which you can, or get the vaccine and hope it will at least lower your ability to get it. And if you do, give you immunity to help fight it and an easy case if any symptoms much at all. Some have had it in hospitals but its not 100% nothing is. I have a nephew with Polio that had his shots. Some of us just have a lousy immune system. I prefer to get the shots, I don’t want to suffer the way many have survived from it, and well may have serious problems later in life. It never leaves your body like all the Herpes Zoster and Chicken pox virus… its in there waiting to cause problems. I have both vaccines now and will get a booster if it is offered. Praying I stay safe and sure don’t give it to someone else. I mask as well, its just a piece of cloth. ty
Sorry for the losses you’ve suffered.
There is much speculation in the scientific community about the efficacy of these vaccines.
They seem to offer protection for 6 months then wane.
Natural infection is speculated to give you lifetime immunity.
I know getting the infection is not ok for some.
But the idea that most people will get the infection again and again is not supported.
Indeed, the vaccinated, if we look at Israel’s data seem to be more prone to reinfection.
There is so much obsfucation that it’s hard to tell what’s going on. It’s an individual choice. That much is sure
Ughhh, Thanks for sharing. I read your post & I thought I was reading my own situation. My Mother & myself both shared many illnesses. She used to say to me “You are going to be just like me, I thought no way am I going to be like her.” I loved her with all my heart but questioned all the pills, doctors, etc. She passed away from taking too many OTC medicines as well as prescription medications due to kidney failure & never knew what was really wrong with her. The one thing I picked up on was the yeast infections. I had some type of female infection that my gyn doctor could not cure. We tried all kinds of cures with medicines, home remedies, a D&C, burning the cervic ? & finally a partial hysterectomy at age 32 that cleared it up.
I originally was diagnosed by a rheumatologist for my FM & have worked many years, getting acupuncture, special shots
supposedly to help my FM. etc. Usually every thing worked in the beginning but then stopped.
If you have tested positive for FM I suggest you try to find a doctor that has FM. They will understand what you are going through & be able to talk with you. Good luck!
It’s generation of people who have suffered because the medical system – and that means doctors and big research funders like the NIH – have turned a blind eye to them. Such a shame!
Amen, Cort! I was diagnosed with Fibromyalgia by a Rheumatologist about 13 years ago. I am still taking the medications she prescribed. We have moved several times since, & none of the doctors I have seen know anything about Fibro. My primary cares have continued to prescribe the same Rx’s from 13 years ago.
How interesting that the decade of the 80s saw the wide adoption of TSH blood tests, its use in practice to diagnose hypothyroidism that left a large part of the population undiagnosed.
At the same time, we see the rise of ME/CFS, FMS and post-Lyme disease as diagnoses.
My guess is that autoimmune diseases, Benign Joint Hypermobility Syndrome (a.k.a. hEDS/HSD) also became more frequent diagnoses. I’d have to look into this to be sure.
And that this parallels the fragmentation of medical care to multiple specialists.
Prior to the advent of evidence-based model of medical practice, hypothyroidism was assessed using temperature, heart rate, metabolic rate (CO2), achilles tendon reflex and symptoms. Dr. Roda Barne’s book(s) is informative.
Are you aware of the rcccx theory?
For me, the story of eds is yet to be accurately defined
I follow a young eds patient and scientist sufferering from heds saying that they have found a mutation for heds at last ( 2 weeksago)
I have a friend with identical symptoms to me…he got a heds diagnosis, me a fibro, ( although m.e. suits my symptoms better these days).
I can’t really see any clear difference between heds, fibro, m.e. and maybe even lymes
Hmm..
It seems their discovery centers around Mitral Valve Prolapse.
Only a small portion of hEDSers has MVP.
Did you know that some with hEDS have been misdiagnosed? Genetic evaluation reveals a homocystinuria or hyposphatasia.
And also, there are plenty of those with adult HPP that get diagnoses of HSD, mE/CFS, FMs, autism. Etc.
It seems a shared core energy problem underlies all of them.
I have legit history and traits for non-classical CAH. It is distinct from thE mE/CFS hEDS FMS the rest of my family also has. None of them have the hormonal things for CAH. I am also the one worse off. May this be why? None understand how stress wrecks me.
I was watching a video of a woman and her Hashimotos, low cortisol, adrenal something and symptoms, i noticed her bendy hands and smooth skin. I thought to myself: had she gone to a different set of doctors, she probably would have been diagnosed with POTS, hEDS, MCAS, etc.
I think it depends on the doctor you see, who gives you what/which diagnosis.
The funniest one is when one rheumatologist wrote Bening Joint Hypermobility Syndrome FMS and EDS all as my diagnosis. What am oxymoron!
Or a male seen by the EDS doctor with a prior FMS diagnosis gets referred to the muscle disorders specialist. While females never get such referral. That’s bias at work.
I do think the endocrinological issues are more spot on, and also more helpful as to how to treat. Not that doctors know, yoi still need to out in the legwork and figure it out.
Yes, on the RCCX.
I am puzzled that Megan doesn’t mention CAH-X as a known entity in the medical world.
I think it’s important to spend time with people that have ‘x’ disease. Very little of the myriad ways it affects their lives makes it to the official medical literature.
Just look up hEDS – before the EDS Society, they would just write connective tissue and skin problems. They still do.
And so I wonder, has Megan spent time with the CAH community?
I think the energetic profile give rise to the hypermobility with instability and pain. Diet too, look at eastern cultures that have much more prevalence of hypermobility (without it beign pathological or EDS etc)
For example, someone using thyroid therapy to treat FMS, IBS, CFS, etc successfully https://newtonintegrative.com/in-tribute/
M. I’m glad that I read this small post about using thyroid treatment to treat FMS, IBS, CFS successfully. I started to answer your first post & was confused as to what you were saying, & sometimes I do get confused.
I have never heard nor know anyone who was given hypothyroidism medication to treat these other debilitating
Illnesses.
Dr. Blanchard must have waved a magic wand to treat his patients.
My hypothyroidism is definitely doing what it does & my FM/CFS, plus IBS, etc. is still the same. I take medication for all these things & have not had one day with out repercussions of some sort.
Perhaps someday it will be proven to me, but right now I don’t agree. I wonder if they have any data on how many people were cured using Dr. Blanchard treatments??
I’ll keep on praying for research for FM/CFS, etc.
M. I decided to research the connection of thyroid disease with FM because my Mom & Grandma both had hypothyroidism, they both had goiters. I don’t have a goiter. I tested positive for FM with the pain from trigger points by several different doctors. My doctor was hoping my test would show only hypothyroidism, & he would be able to treat me properly.
I researched Dr. Blanchard’s theory about thyroid diseases & how they were related to FM. This led me to Dr. John Lowe who has written a book (The Metabolic Treatment Of Fibromyalgia) & also a letter debunking what Dr. Blanchard has said.
Since I’m not able to decipher medical things I’ll say that perhaps I could have been helped with Dr. Lowe’s advice. However, I don’t thing I’d have the energy to follow through because of CFS.
I found all this information on my iPad so I’m assume it is available to all of you.
If anyone is interested in checking further Dr. Lowe’s views are noted at;
http://www.DrLowe.com
Endocrinologist dosing to blood tests, instead of metabolic rate
(as measured by temperature and heart rate, achilles tendon reflex) and symptoms hardly get it right.
Dr Roda Barnes’ book = easy to understand
Ray Peat
Paul Robinson
https://paulrobinsonthyroid.com/
https://www.healthrising.org/blog/2019/03/07/thyroid-t3-chronic-fatigue-fibromyalgia-recovery-stories/
I think those supra-physiological doses of T3 are too much…
Dominic recently teamed up with Jonas Berquist on two papers.
Berquist spoke at the OMF open house in May and said that they are next trying out the approaches outlined in the paper – thyroid is one, so are other hormones.
https://www.frontiersin.org/articles/10.3389/fmed.2021.628029/full
https://www.frontiersin.org/articles/10.3389/fmed.2021.672370/full
– – – – – – – –
David Symstrom is checking out adrenal function in his studies.
https://endmecfs.mgh.harvard.edu/heartpreload/
(adrenal dysfunction results from the hypothyroid body trying to adapt to energy demands)
M. Thanks for all the articles, etc. concerning hypothyroidisms connection with FM/ME/CFS.
Oh, my goodness, I now have a headache trying to understand all the medical terms, etc. that I read.
I was unaware of all the research that has or is still being done to determine (if)the correct medication that is given for hypothyroidism will then aid in curing FM/ME/CFS.
Cort, I want to apologize to you because I did not know about your comments on Dominics post, etc. With my cognitive dysfunction (Fibrofog) I tend to scan most of your letters because of all the medical terms. My career while working had to do with numbers & now I count on my fingers a lot. Thanks for all you do & please continue to do. I’m sure you have had headaches too.
M. While going through Dr. Blanchard’s studies I saw a name M xxxxx who had written to the Dr. & I wondered if that could be you. This lady was one of his patients.
I tried to read all the articles you suggested & did get through quite a few. It was amazing to see
all the research that is being done. However at this point in time I would still have to have definite proof that it truly works for say 95% of the people with FM/ME/CFS. I no longer feel well enough to go through tests that may or may not work for me.
You have really researched everything about these tests & I sincerely hope you have found a plan that works for you. I admire your tenacity!
It doesn’t hurt to try
Also, substitute ME/CFS for FMS here:
https://youtu.be/K7rhZyFSkwU
And
https://www.thefibroguy.com/client-success-stories/
Is it possible to please provide a link to the second study discussed in this post, or at least the author names and publication title? I’m hoping to provide the original source to my doctor, in which the authors mention that plasma exchange has been helpful for symptom control Long Covid patients diagnosed with Guillain-Barre. I’m sorry if that information is in the post somewhere and I missed it. Thank you!
OMG – I did it again. Here it is
Corneal confocal microscopy identifies corneal nerve fibre loss and increased dendritic cells in patients with long COVID – https://pubmed.ncbi.nlm.nih.gov/34312122/
Hey Cort,
Thank you for this article, I don’t know how you do it, putting together all this scientific/medical jargon into comprehensible articles for us. Please keep up your very appreciated work. I hope more people will consider contributing to HealthRising so that you can continue.
As for the fibro, I suspect I have always have hEds, but my fibro symptoms didn’t appear until after a nasty flu. Since the emergence of long covid, I often wonder if it was a result of that flu. I try to warn family and friends that they do not want long covid if what I have is anything to go by. Sometimes, I feel like a shrill, I just wish they understood the sheer misery and life altering scope of this disease. Anyhow, tx for letting me sound off. Although I don’t comment often, I look forward to your newsletters even if I don’t read every single one. Thank you again for all your hard work.
Thanks so much Agnes!
Coincidentally just before reading this article I heard an interview with a nurse practitioner with a post covid vaccine diagnosis of severe and progressively declining SFN who is about to undergo IVIG treatments and plasmapheresis if that doesn’t work. She has since found others with similar symptoms and they have a support group going. She is desperate for help as she is barely holding on to her job and like many of us has lost the active life she once had. Very sad. Just wanted to mention that there appears this group of people too- COVID vaccinated. Not the narrative that the powers that be want to get out there but nevertheless they exist and they need help and support too and should be studied by NIH, etc.
Sorry to hear that. The vaccine studies followed tens of thousands of people and did not find consistent evidence of that happening. That’s not to say that it doesn’t happen – obviously some people are going to have strong reactions to any drug. That’s pretty clear from ME/CFS. Of course they should be supported and not left to their own devices like people with ME/CFS have been for so long. We should be the last group to turn our back on them.
The results the vaccines are having with the COVID-19 pandemic are clear, though; the states with higher vaccination rates are doing fine. The states with lower vaccination rates are getting crushed. Over 2000 people a day are dying from the delta variant in the US. For the first time in recorded history Alabama had more deaths than births –
“Our state literally shrunk this year for the first time in history, even going back to World War II, when people were serving overseas; going back to the Spanish Flu epidemic, when we had the flu in our state; going back to World War I,” State Health Officer Dr. Scott Harris said Saturday. https://www.usatoday.com/story/news/health/2021/09/19/alabama-deaths-births-covid-flu-shot-coronavirus/8400102002/.
For its part, Florida accounted for one out of every 25 COVID deaths in the world last week. https://www.usatoday.com/story/news/health/2021/09/19/alabama-deaths-births-covid-flu-shot-coronavirus/8400102002/
The coronavirus has killed almost 675,000 people in the U.S. That’s pretty staggering!
It’s an oddity of human nature that we pay more attention and give more significance to individual stories than to statistics.
I have fibrocovid. My first fibro attack occurred approx 6 weeks after I had covid. I was getting out of bed in the morning and it seemed like all the muscles in my back suddenly froze and down to the floor I went. I’ve had back spasms b/f but it usually was when I was moving or twisting, not getting out of bed. I was lucky my dresser is next to my bed so I was able to pull myself up, get to the bathroom and get dressed. I told my husband I have a severe back spasm. For the next three days I treated my back spasm only for it to get worse, travel down my legs, up my back and into my arms. I remember while training as a PA-C one of my patients had fibromyalgia so I asked her what her symptoms were and she told me and it fit what I was going through. I went online to the website Earthclinic and looked to see how to treat it naturally. I drank a combination of borax and sea salt and it literally went away. I told my husband for some reason I have fibromyalgia. Since then my life has been nothing but a bunch of ups and downs, esp with blood pressure. It seems my fibromyalgia is progressing at a faster pace than other people who didn’t get theirs from Covid. I happen to be looking at different news sites online and one article on the Fox News website caught my eye. I can’t remember what the exact title was but it basically said “Treating long haul covid with a simple OTC treatment”. I read it and it made sense. We do know that FM is an overreactive nervous system usually caused from a viral infection or severe trauma. The secret is to calm down the nervous system using antihistamines. All I had in the house was Tylenol PM so I decided to give it a try figuring the Tylenol would take care of my pain while the Benadryl would calm down my nervous system. I took one and went to bed. Next day I woke up with no pain at all. I couldn’t believe it. Since then I take Tylenol PM with an extra Benadryl 25 every night and wake up feeling good with NO fibro fog at all. I could never take Benadryl b/f, it would make me sleep all night and all the next day. Now it makes me normal. This probably wouldn’t work for everyone but I remembered while sick with covid I couldn’t sleep at all, even with 50 of Benadryl…I thought that odd but Covid is a bioweapon and we’re just now seeing all the long haul problems with more being added all the time. Will there ever be a cure for fibrocovid? I don’t know I’m just thankful I’ve found a temporary treatment that works very well. Good luck to anyone who has this dreaded condition, it’s mean and nasty!
I was hospitalized for 18 days in the hospital. I have POTS, CF & Fibromyalgia, ringing in
both ears with dizziness & diabetic-2. I am allergic to Metformin… This whole package came in November 1979 as a package all together.
I was hospitalized Dec. 26, 2021. I was having bad headaches/migraines. Now, 17 months & Brain Fog worse than before Long Covid. I had a MRI but no dementia but that is what I feel like. Can’t think straight:( Ringing in the ears it’s even loader than before!! I still get some head & plus arthritis makes more pain.
Having ME/CFS,.FM. Dizziness, Ringing in the ears,& fainter-POTS since 11/1979. Now, I am 77 yrs. old.
Went to the hospital for 18 days. Dec, 26, 21. I told my son I was having migraines plus headaches every night. My dreams would continue with the same story with the same people.
So he took me to the hospital & stayed for 18 days.
It’s made my ringing Loader then before. Still get some headaches.
I had a MRI thinking I had dementia but it’s called Long Covid-19. Plus super pain & confusion & forgetfulness.
Hi everyone/fellow sufferers of fibromyalgia. I’ve discovered a new treatment that has taken my pain and exhaustion away. I use transcranial Direct Current Stimulation and it’s been a life changer. I still have fibromyalgia I just can’t feel it, SO FAR. I still stay on my diet and I still have aches and pains but they’re not from fibromyalgia. These are from advanced age and also being VERY sedentary due to severe fibromyalgia. I got fibromyalgia from Covid 19 aka FibroCOVID. I’ve posted b/f and now I’m doing this update hoping it can help anyone suffering from this mean and nasty condition. Again, good luck to everyone who has this, at times I felt it was hopeless.