“We know how to treat it.” Bruce Patterson
Could Bruce Patterson M.D. be way, way ahead of the game? Patterson made news earlier this year when he reported not only did he know what was causing long COVID, but he also knew how to treat it.
Nobody was expecting that double-whammy. Plus, in more good news no new drugs were needed – they were already available. Time will tell, of course, if Patterson is right, but it’s clear that one objective is being met: long COVID is, as we’d hoped, bringing new eyes and new ideas to the study of post-infectious diseases.
ME/CFS Connection
The Gist
- Patterson has moved quickly from long COVID to ME/CFS, post-Lyme disease, and fibromyalgia.
- He believes similar processes are occurring in all these diseases. A paper charting similarities and differences in this group of diseases will be published.
- The pathogen is gone but has left behind proteins that are tweaking the immune system.
- In the case of long COVID, monocytes are being directed by CCR5 chemokines to attack the endothelial cells lining the blood vessels across the body.
- Patterson attacks this process with CCR5 antagonists that prevent the monocytes from being directed to the endothelial cells. He states that this approach is very effective.
- With his immense cohort of doctors (@150) and patients (13,000 long haulers, 1,000 post-vaccination long haulers, 500 post-Lyme, 100-200 ME/CFS, 50-100 fibromyalgia), Patterson presumably has plenty of data to dig through and plenty of patients to enroll in studies.
- Patterson appears to employ a precision medicine approach which uses a core set of CCR5 drugs plus 10-12 others that are used based on a patient’s testing results.
- Patterson also stated that he would be focused on ME/CFS/FM, and post-treatment Lyme syndrome in 2022.
- Patterson believes he is getting at the heart of post-infectious illnesses and is certainly bringing a novel approach to them.
- Patterson reported that a randomized, placebo-controlled long COVID clinical trial is underway or about to get underway. No locations have been announced.
- It’s exciting stuff, and we learned with XMRV and Rituximab to be careful. Time will tell.
Patterson related that after a friend who could not sleep came to him in the early 1990s, he used a new PCR test he’d developed for herpesviruses to determine whether a virus was active or not. (High RNA levels would apparently indicate activity). She was treated with a short course of ganciclovir and recovered. A year later they were married.
Some long-COVID groups are embracing ME/CFS, and some are turning their backs on it. Patterson, to his credit, is embracing it. He noted that the health care emergency many have speculated long COVID will bring, already exists – in the millions of people with ME/CFS, fibromyalgia, post-Lyme disease, and others – who are not being treated.
Patterson began his work with COVID, moved onto long COVID, and is now focusing on other post-infectious diseases like ME/CFS, fibromyalgia, post-Lyme disease, and post-coronavirus vaccination syndrome. The symptoms, he noted, are almost identical.
Big Network…Big Data?
He’s got quite a network (@150 doctors) and cohort going (13,000 long haulers, 1,000 post-vaccination long haulers, 500 post-Lyme, 100-200 ME/CFS, 50-100 fibromyalgia). That gives him potentially lots of data to work with.
Patterson is putting people with these diseases and conditions through the same immune tests. (I’m not sure if he’s having them go through the original 150-plus immune panel he originally put the long haulers through or through the 14 immune mediator panel. That panel was composed mostly of immune mediators produced by the innate or inflammatory immune system. IFN-y, IL-1, IL-4, Il-10, GM-CSF, CCL4, CCL3, TNF-a, IL-6, sCD40L (platelet activation), CCL5, IL-13, VEGF.)
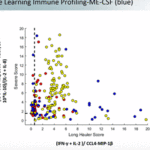
Patterson used this slide to show the ME/CFS patients (blue dots) are similar to the long-COVID and other groups.
On an Oct 19th tweet, Patterson wasn’t willing to say that people with ME/CFS had a similar immune dysregulation but did say he was using a “first of its kind proteomics instrument” to determine that. A month and a half later he was willing to go further.
The different groups appear thus far appear to exhibit a similar immune signature – with some differences. A publication is coming.
For instance, the post-vaccination cohort appears to have less VEGF, IL-6, and another – and other markers than the long haulers; they respond more quickly to treatments and very successfully;
Thus far, the 50 or so people with ME/CFS he’s tested look more like people with a post-vaccination illness (high Il-2, IFN-y, and higher long hauler indices than long haulers). The ME/CFS patients, Patterson said, don’t exhibit the vascular inflammation seen in the long haulers. Thus far, though, they respond well to CCR5 antagonists such as maraviroc and pravastatin.
That’s an interesting finding given the increasing evidence of blood vessel findings in ME/CFS and fibromyalgia. If Patterson’s findings are correct, something else (small fiber neuropathy, leaky blood vessels?) may be disturbing blood flows in ME/CFS.
Patterson is continuing to publish and will make publication a priority in the new year. One of the more controversial parts of Patterson’s hypothesis is his finding that long-lived non-classical monocytes are carrying S-1 protein from coronavirus, and are binding to fractalkine receptors on the blood vessels, causing inflammation (via IFN-y, IL-2) and possibly clotting issues.

Monocytes are the key immune player in Patterson’s long-COVID hypothesis (.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436.)
The controversial part is the idea that these monocytes that are generally pretty short-lived are hanging around much longer than expected. Patterson’s paper demonstrating this has been accepted for publication and hopefully, will be available soon.
Different Approach to Post-Infectious Diseases
“I believe we are really starting to get to the heart of what’s causing these post-pathogen conditions.” Bruce Patterson
In a breakthrough paper that landed in the Science journal in the 1990s, Patterson discovered a heretofore undetected HIV reservoir in the body. In what may be a new approach to post-infectious diseases in general, though, Patterson doesn’t believe that the problem is leftover coronaviruses at all; this time, it’s leftover coronavirus proteins.
Instead, he believes that immune cells called non-classical monocytes carrying S1 proteins from the coronavirus, are causing inflammation in the body and sometimes the brain.
Patterson envisions an approach that relies more upon technologies like proteomics that can uncover the viral proteins that have been left behind.
Treatment
CCR5 Antagonists to the Fore?
Calling them “an exciting new class of drugs that modulate the immune system”, Patterson believes that CCR5 antagonists like maraviroc, leronlimab, and statins like pravastatin are going to play a major role in treating these diseases.

CCR5 is a chemokine that Patterson believes is directing monocytes to attack endothelial cells in the blood vessels.
CCR5 is a “chemokine”- a kind of cytokine that shepherds’ immune cells toward a site of infection. CCR5 antagonists were developed in response to HIV when it was discovered that some people who were immune to the virus had a mutation that codes differently for the CCR5 receptor. Maraviroc and leronlimab are two CCR5 antagonists mentioned by Patterson, and others exist. They block the monocytes from binding to and inflaming the endothelial cells on the blood cells, thereby decreasing VEGF, TNF-a, and IL-6. Patterson stated that approach has been “very, very effective.”
Focus on Precision Medicine
Patterson kept returning to a precision medicine approach in which your treatments are predicated on the cytokine and immune mediator test results.
In his talk with Dr. Deb, a naturopathic doctor, Patterson bemoaned the one-size-fits-all approach hospitals are using with COVID. Despite his papers on COVID, it’s been very hard to get anyone to try statins – which he described as being relatively benign.
He questioned whether the widespread use of dexamethasone and the blanket immunosuppressive approach currently standard in long COVID is going to produce reservoirs of the bug in the body. It would be much better to tailor the treatment to the status of the immune system found in each patient.
While Patterson uses a core set of drugs, his treatment regimens, which include 12-14 drugs are more complex than that. Able to associate cytokine levels with specific symptoms, he appears to be using specific drugs to bring down those cytokines. High levels of VGEF (>30) – found in 85% of the long haulers – for instance, result in the appearance of peripheral neuropathy.
Patterson shot down some popular ideas. He doesn’t believe that monoclonal antibodies work long COVID, nor do most long-COVID patients get better after a vaccination either. If they do, the effect usually doesn’t last. He’s not in favor of apheresis either. While it may help in a small number, Patterson noted he’d had a patient who ended up in an ICU after that procedure.
If underlying chronic viral infections are present – as Patterson expects in some people with ME/CFS (but does not see much in long COVID) – antivirals are in order. Patterson wants to bring back the herpesvirus assay he developed at Stanford to test these patients.
Tracking
As Lipkin is, or is about to do, in the ME/CFS field, Patterson will be using their Imunowatch and ImmunoTrak app to track things like symptom severity, temperature, blood pressure, heart rate variability, and heart rate to assess treatment effectiveness.
Patterson acknowledged that all he has regarding treatment efficacy is anecdotal reports. Anecdotally, he said, he knows the treatment works. On the Dr. Deb show, though, Patterson (thankfully) did say the results are variable – that for some people the initial result is a return to functionality, an ability to step up your exercise, etc.
Treatment Trials Coming
He’s moving quickly. On October 9th, Patterson announced that a major (as yet unnamed) university had been enrolled. Last month, the lead investigator for the first placebo-controlled, randomized long-COVID trial using Maraviroc, a CCR5 antagonist, and a statin, atorvastatin, was announced. The study will assess symptoms, and, via InCellDx’s long hauler index, immunological changes. No study sites, that I can tell, have been published, however.
On December 6th, InCellDx announced it hired a chief operating officer as it prepared to expand into “new markets globally including the UK and EU”, and scaled its “immunology/long COVID treatment program, and advance(d) it’s biopharmaceutical development.”

Patterson appears to have a huge cohort of patients to test his ideas on. Placebo-controlled clinical trials are crucial.
Confident in his ability to treat ME/CFS/FM and post-Lyme disease, Patterson said those trials are coming as well. 2022, he said, will be focused on treating long COVID, ME/CFS/FM, post-coronavirus vaccine illness, and post-Lyme disease.
Patient recruitment can take a great deal of time in treatment trials, but with his huge network of doctors and patients (Patterson specifically mentioned the Kaplan Clinic in Virginia with regard to ME/CFS), Patterson certainly seems to have the patients he needs to quickly start trials.
Producing a treatment trial, though, can be a complicated and expensive process. No funding sources have been announced, and one wonders how Patterson and InCellDx are managing all this work: the large doctor and patient base, the trials, the research, the publications, etc.
It should be noted that Patterson’s results rest on just a few papers and have not been validated by outside groups. It should also be noted that ME/CFS researchers have, over time, produced many interesting immune results which follow-up studies have had difficulty replicating.
Take cytokines. Cytokines have been studied again and again in ME/CFS, but except for a few cytokines – most of which Patterson’s studies do not highlight – the results have mostly been too variable to be illuminating. More sophisticated cytokine analyses like the machine-learning approach Patterson is taking, do though, appear to be more effective.

Patterson’s work is innovative and exciting – but will it work? Time will tell.
What to make of all this? We have a researcher with an excellent resume who says he believes he’s found the answer to not just long COVID but possibly ME/CFS/FM, post-Lyme disease, and other post-infectious diseases.
While Patterson, in his calm, easy-going manner, exudes trustworthiness, it would be truly remarkable if these knotty problems were solved so quickly. However the Patterson saga turns out it’s clear that one goal is being achieved: long COVID is bringing new eyes and ideas to both it and ME/CFS/FM and related diseases.
He’s brought new ideas (pathogenic proteins, not pathogens are the problem) and a new treatment regimen using drugs never before used in ME/CFS to the field. He’s using machine-learning – an approach that’s rarely been used in ME/CFS. By tying his treatment regimens to his test results he’s also bringing a data-driven precision medicine approach to these diseases. Through all that he’s certainly brought quite a bit of excitement.
Treatment, of course, is where the rubber really meets the road. While Patterson’s results are anecdotal, he clearly believes his treatment approach is working. Most importantly, for us, Patterson promised that clinical trials in long COVID, ME/CFS/FM, and post-Lyme disease trials are coming. Hard data is what we really need.
Time will tell…
You don’t need, by the way, to have long COVID to try Patterson’s treatment approach. People with ME/CFS/FM and post-Lyme disease can start that process on Patterson’s COVID Long Haulers website.
Pros
- Good resume.
- Gets it about ME/CFS/FM and post-Lyme disease.
- Huge network/ patient, reportedly, setup.
- Taking a different slant to post-infectious illnesses.
- Focus on proteomics.
- Precision diagnostic and treatment approach.
- Confident in results.
- Moving forward quickly.
Cons
- Funding? Is he getting the funding he needs?
- Research findings rest on a few papers and have not yet been validated by other groups.
- Cytokine results don’t match those seen in ME/CFS (which are quite variable anyway).
- ME/CFS is likely a more complex disease – more infectious triggers and longer duration patients; may not fit long COVID. (Patterson did say he’s gotten excellent results in some long-duration post-Lyme disease patients.)
- Big promises – is Patterson making promises he can keep? Will we really see long-COVID, ME/CFS/FM, and post-Lyme treatment trials next year?
2021 Fundraising Drive Update
Thanks to the over 200 people who have supported Health Rising thus far!







Great summary of this fascinating subplot in the ME/CFS & long-Covid “story”. Feels almost like an early Tesla, farfetched/flawed/preposterous. And we know how that’s turned out! And I say that as someone who was a non-believer.
Regarding the machine learning approach to multi-analyte lab tests, it’s definitely being applied elsewhere. For instance: Dr. Yamamura’s team at the NCNP Neuroimmunology department in Japan has created another quite sensitive/specific machine learning classifier using B-cell subsets.
Aside from the iCPET approach that boils the pathology down to one decisive number (oxygen returning to heart), the way forward may be multivariate. Lab tests, even complex ones, are surely more scalable than exercise tests!
Cort wrote, “Patterson, of course, isn’t the first to propose that leftover proteins from a virus are tweaking the immune system. John Chia believes the same is happening with the enterovirus in ME/CFS.” I seem to recall that when I asked Dr. Chia whether my positive stomach biopsy represented current or past infection, he said current, not leftover.
It seems like each and every article has some subtle money making scheme behind it. There is a new theory and potentially treatment every few days. What happened to oxaloacetate and their $500 bottles of nonsense? That quieted down real quick! Just like the nonsense mentioned here. I wonder how much money will be made after signing up for the blood test. Will this comment get posted? I guess time will tell.
Roger,
Whilst I understand distrust in big claims and even bigger prices, having read these articles for many a year, I do not feel at all that this is a forum that proliferates snake oil marketing.
But more so than that, the same oxaloacetate blog you mentioned contained links in the comments section to a molecular biologist’s blog where oxaloacetate was thoroughly trounced (as a mitochondrial treatment). That isn’t exactly classic censorship or soft marketing in my opinion.
Roger I think you’re passing judgment too quickly. Dr. Kaufman doesn’t benefit from oxaloacetate and Dr. Patterson has a long academic record. Time will tell for all of it.
I’m curious if the ME/CFS blood he is looking at is from people like me, who have both ME/CFS and post-vaccine “long hauler” symptoms (adverse reaction to the covid vaccine) or is he evaluating blood from patients who only have ME/CFS?
I ordered his blood test precisely because I had an adverse reaction to the vaccine, and with treatment my cytokines have normalized (although I am not completely back to my pre-vaccine baseline), and I still have moderate-severe ME/CFS.
I would imagine most ME/CFS patients who sent in blood did so because they had an adverse reaction to the vaccine, so I’m wondering how he will be able to determine anything about ME/CFS when we have these elevated post-vaccine cytokines in our blood.
Nina — curious what treatment helped you after the Covid vaccine? I sense that my ME/CFS was triggered by the vaccine …. Thanks
Jennifer, I was prescribed maraviroc (Selzentry) for elevated RANTES & a statin (which I was already taking). I cannot tell if the medication or if just time has helped. It is also possible the vaccines were just another “immune hit” to my already dysregulated ME/CFS immune system.
If you are in the US and haven’t done so already, please report your reaction to VAERS (patients can make reports to VAERS themselves) and make sure your physician has recorded. your adverse vaccine reaction in your medical chart.
Hi Nina — curious what treatment you used after the Covid vaccine made things worse for you? The vaccine may have triggered ME/CFS for me …. Thanks!
Hello Nina
I hope you don’t mind me asking but
I am very interested to know what adverse reaction you had to the vaccine and what treatment you consequently had which helped you to partially recover. I also reacted badly to my second vaccination and am struggling to recover. I have had me/cfs for many years. I’m finding it difficult to get my doctors to recognise that it was the vaccination that has caused my current symptoms.
Kind regards
Jill
Jill, my adverse reaction was marked worsening of all my ME/CFS symptoms–worse profound fatigue, worse daily misery, body aches, muscle weakness, muscle shaking, internal tremors, brain fog, POTS; became mostly bedbound again. Felt the same as the major crash that ended my career.
I was prescribed maraviroc (Selzentry) for elevated RANTES and a statin I was already taking. I am not certain if the medication or time has helped.
Physicians are not taught how to handle adverse vaccine reactions, unfortunately, but every symptom we have should be individually investigated as if you didn’t carry the “ME/CFS” label. If you are in the US, as a patient you can make your own report to VAERS, but you also need to ensure your physicians have recorded your adverse vaccine reaction in your medical chart as well.
Nina, curious if you ever received the Cytokine test. I’m having difficulty even getting the test setup. Still waiting on confirmation and next step.
I just want to be clear I am by no means back to the poor quality of life I had with ME/CFS before my second Covid vaccine, & unfortunately, I did not see a dramatic improvement with Patterson’s protocol.
My cytokines all normalized on his treatment but I didn’t get better. I am not as bad as I was last year after the vaccine, but I am still suffering from the adverse effects of the second covid vaccine.
Although I am far from convinced on any of a number of hypotheses circulating right now, the very fact that there are a number of them as well as connected treatment theories has to be a good thing.
Hopefully one of them comes through in the next couple of years!!
As a scientist I am very sceptical:
– Dr Patterson rolls out clinics around the globe based on an expensive treatment that has not been studied – at all (there are not even published case reports or case series)
– As it happens, this treatment is based on a drug or class of drugs that his company unsuccessfully tried to establish for treatment of cytokine storm in acute Covid 19 (https://www.ted.com/talks/bruce_patterson_m_d_translating_a_recent_scientific_discovery_about_covid_19) Here, too, Dr. Patterson gave the clear impression of overwhelming treatment success – which apparently did not materialize (even using the same catch words like precision medicine etc. that his company employs…
– While the company has apparently run > 10 000 lab tests (reportedly costing about 400 $ each) and has set up a franchise system of telemedicine MD practices around the world – appointments to be paid out of pocket by the patients – he now says that he´ll use “next year”s time to write up some scientific papers. Just makes me wonder (the results of his trial will probably be available in a few years time – how much cash changes hand in the meantime?
– I ask this question especially if I see business presentations like this: https://twitter.com/IamBreastCancer/status/1445452703564369930
– So yes, there may be something to CCR5 inhibition (some drugs in ancient Chinese Medicine contain CCR5 inhibitors) – but before you claim that you can cure a substantial part of long haulers you need to do more than just place claims – which, we should not forget – are put forth by a physician who at the same time is an owner and investor.
It´s good that Dr. Patterson acknowledges the suffering of ME/CFS patients –still, what we need is sound science. We´ve been down too many rabbit holes.
Thank you for that comment Herbert. We’ve had 40 years of hopes raised and hopes dashed, all coming at the expense of very ill people who can ill-afford to put what little resources (finances, energy, attention, time, etc…) they have left into yet another lost cause that doesn’t heal them. Or worse, into the pockets of the few who outright steal from them &/or harm them (GET anyone?). And toward those who divert support away from the honest practitioners who are genuinely trying to aid us.
Attention to red flags is welcome in my book. If they turn out to be distractions, that helps us deepen our trust in the end, which is ultimately a good thing. If they are legitimate, forewarned is forearmed. We’ve had far too little forewarning or forearming re: this disease.
Thank you.
Well said Anne.
Good points. Also, isn’t he a doctor rather than a researcher? I don’t know if that makes much difference, but I wouldn’t have thought full time doctors are set up as well or as practiced in the art of robust scientific research?
Herbert, totally agree and in fact this article was just released today talking about how Dr Patterson’s treatment is raising red flags and seems to be taking advantage of people and not working necessarily…
https://www.medpagetoday.com/special-reports/exclusives/96506?xid=nl_mpt_investigative2022-01-05&eun=g1854568d0r&utm_source=Sailthru&utm_medium=email&utm_campaign=InvestigativeMD_010522&utm_term=NL_Gen_Int_InvestigateMD_Active
Given the close connections between ME/CFS and FM, does anyone think these proposals would apply to MCAS as well?
Hi Cort,
I’ve visited the covidlonghaulers site and in both the contact form and the lab registration there doesn’t seem to be an option for people with ME/CFS who’ve never had Covid. (E.g. the reg asks for a covid diagnosis date and the contact form doesn’t have non-covid long hauler patient options.) I’ll, be contacting them myself, but in the meantime, can you confirm that international ME-only patients can apply? (I’m Canadian.)
Thanks
Can anyone confirm how much this costs?
$350 for the blood test and I believe $290 for a telemed consult but they say you have to have your own md/Do to work with him.
Done his full protocol. Didn’t do anything. Don’t do it. It’s really a scam. Besides he always talks about data 10000ppl but never shows them. Ask yourself why. Don’t do it. I know you are desperate like. But it’s a waste of time and money.
Badpack, sorry to hear that. Would you mind please sharing rough time period, description of protocol and approximate costs? It would be really helpful.
Other “CFS clinics” or “CFS doctors” have been touted as amazing, but when I contacted to ask, it was: No insurance accepted (okay, but what do you do there?) We run a number of tests to diagnose you (okay but I’m already diagnosed. I know I’m sick. I’m interested in treatment to improve and work toward cure. Have you cured anyone?) Well… it depends on your tests (Actually, improving or curing someone else is not dependent on my tests. Have you had anyone else improve or be cured and if so, what types of TREATMENTS do MAY you do, depending on the outcome of my tests?) Big silence. All a big, expensive scam, IMO, at one of the most touted, big name ‘clinics’ in NC, in USA, just because someone “said our illness is real.” I know it’s real, trust me. I want REAL RESEARCH AND VALID TREATMENT!!! Stop promoting snake oil. I don’t need freaking compassion or “VALIDATION.” I NEED DISCOVERY OF THE MECHANISMS CAUSING THIS DISEASE AND A WAY TO STOP IT SO I CAN LIVE WHAT’S LEFT OF MY HORRIFFICALLY AWFUL LIFE.
For people sincerely doing difficult research, whether great or misguided, thank you. For those who are riding the gravy train of desperately ill people and now see the multiplication of Long Covid, really go F*** yourselves. And I guess the jury is out on this treatment path, which is no judgment on badpack whom I believe completely. I concur this is many times I’ve seen a similar claim–but also that’s the way research goes sometimes and not every thing works for every person. Yet I have not seen explanations of failures, changes in research direction from this or other practitioners after their previous claims of breakthroughs.
notverysharpe, I would contact Dr. John Chia in Torrance, CA if it is all possible for you to get there. He does take insurance but I pay to see him out of pocket and his charges are very reasonable. He will spend as much time as needed with you and treatment plans are also not expensive. He is NOT trying to make money off of us and truly cares about finding a cure for us. I trust him and value his work.
Sir,
I would like to discuss this with you. I’m in the process of trying to get a Cytokine test done. It has been confusing and frustrating. Still waiting. Email if you are available to discuss.
Did you retest to see if the markers were changing? How many months were you on the treatment? Did you stay on treatment long enough? I have heard that it varies what is needed.
A study of the Free University of Brussels (Belgium) linked last week long covid to central nervous system hypersensibility. I remember that such link was established for the Gulf War syndrome. I don’t know if somebody has explored that. What about you?
I have that as well please let me know if you find anything out about it. im in constant fear and panic.
I just submitted a comment that didn’t post. Are comments being monitored now?
This morning I just found a recent document about a ‘multidisciplinary consensus on the treatment of long-Covid’ with a special emphasis on fatigue. I suppose it is linked to all that money appropriated for study;
https://onlinelibrary.wiley.com/doi/full/10.1002/pmrj.12684
I have to say, I am rather disappointed. It just sounds like more of the same that we have heard about dealing with ME/CFS.
It certainly isn’t new ground, but it is good to see long-Covid, ME/CFS and PEM all in the same article. Being educated about PEM early is gold in my opinion.
Adding this so it is part of the record for this discussion.
“You’re selling a test that you’ve got no good evidence works, and then you’re using it to prescribe a drug that you’ve got no good evidence works?”
https://www.motherjones.com/politics/2022/01/desperate-patients-are-shelling-out-thousands-for-a-long-covid-cure-is-it-for-real/?utm_source=STAT+Newsletters&utm_campaign=74382d6d16-MR_COPY_01&utm_medium=email&utm_term=0_8cab1d7961-74382d6d16-153285438
Just read this article and came here to post the same. So many red flags.
I will be glad if Patterson is able to help a lot of people. It’s been a few months since you published this, Cort, so I’m not sure where Patterson’s work is now, but I though of his encouraging use of statins in some patients when I read about the study below in a recent New York Times article. Epstein Barr virus reactivation is one of four things that can predispose someone to long covid should they contract covid. Going on statins was something that reactivated Epstein Barr for me in 2003 and sent me into ME, and going of of them didn’t help. In the 2010’s there were several studies that showed that statins and other TNF-alpha blockers and inhibitors can turn on herpes viruses. It was too late for me both around EBV but by 2010 also around HHV-3/herpes zoster/shingles. So if the herpes viruses are a big part of someone’s history, maybe proceed with caution with the statins. As always, one size does not fit all, and some may be quite helped by it. I would be thrilled to have the kind of immune system blood work done that is part of Patterson’s studies. Maybe he could tease out differences in statin responders.
wow I did his blood test and waited weeks for results finally got them in an email and you would think they would at least call you and tell you that. it shows im in cytokine storm but i too think i have epstein barr and shingles now ty for sharing this! also I didnt get a response on their page for longhaulers.com which is the drs on there to consult with me so i emailed and non stop kept calling the people who ran my test so finally got a reply and she said to fill out the form they send and book an appointment after that. There is no appointments available so i emailed again and she said you just have to keep checking in til you find one people cancel all the time.I looked for an opened appointment all the way to oct2023 and there is nothing.
suzette, thank you for sharing!
I’m having a similar experience. I’ve been working to get the test for about a month. This is starting to sound suspicious. Thanks for the heads up.