

Hyperbaric oxygen therapy seems like an obvious choice for energy-depleted people with ME/CFS, long COVID, and fibromyalgia… But can it deliver the goods?

If oxygen provides the stuff of energy … and people with ME/CFS, FM and long COVID are energy depleted … how could HBOT not help? (Image by ChristineLMiller – Wikimedia Commons).
It seems so obvious. How could delivering massive amounts of oxygen to energy-depleted, oxygen-deprived long COVID, chronic fatigue syndrome (ME/CFS), and fibromyalgia (FM) patients not work?
Hyperbaric oxygen therapy (HBOT) potentially promises much. Studies suggest it may be able to increase the amount of oxygen being delivered to the brain, in particular, thus potentially improving metabolism, microglial cell functioning, and blood vessel functioning, promoting blood/brain integrity, reducing inflammation, and inducing neuroplasticity. Some researchers believe the ability of HBOT to revive dysfunctional brain regions (i.e., increase neuroplasticity) may be its greatest strength.
Of course, there’s also the potential impact on the mitochondria as well as HBOT’s possible ability to regenerate muscle fibers and increase muscle strength. Plus, the combination of delivering high oxygen levels in combination with hyperbaric pressure appears to trigger the activation of “regenerative processes” including stem cell proliferation and the induction of anti-inflammatory factors.
All that makes HBOT an intriguing option given the hypometabolism found in the brains of ME/CFS/FM and long-COVID patients and the low oxygen uptake David Systrom’s invasive exercise tests have consistently found in a subset of ME/CFS patients.
On the other hand, HBOT’s ability to shove oxygen seems like a blunt force kind of option that might temporarily help but not necessarily repair the problem. One would not think it would fix a shunt that’s moving blood past the muscles, nor a mitochondrial problem.
However, if ME/CFS/FM and long COVID are caused by systems that get stuck in some kind of hypoxic, inflammatory positive feedback loop (aka Martin Pall’s NO/ONOO hypothesis), then clearing up that toxic state might do the trick and flip the system back to normal. For instance, by repeatedly reducing inflammation, HBOT sessions might be able to calm the microglial cells down enough that they stop being so reactive.
Check out what we’ve learned about the efficacy of HBOT in long COVID, ME/CFS, and fibromyalgia.
Long COVID
Case Report: An Israeli case report provided an encouraging picture. Three months after a coronavirus infection had landed him in the hospital for a short stay, a formerly healthy and athletic 55-year-old was experiencing shortness of breath with exercise and cognitive problems. An MRI revealed that problems with small blood vessels in his brain were present – and apparently preventing his brain from getting the energy it needed.
He was given 60 x 90-minute sessions, 5 days per week at 2 atmospheres pressure. His improvement was rapid. After the first five sessions, he reported that his breathing was better and his muscle aches after exercise were gone. After 15 sessions, he noted less fatigue and an improvement in his previous low energy. After 20 sessions, he noticed that his breathing and ability to exercise had returned to normal and he was back to running mountain trails! His cognitive problems were gone as well.
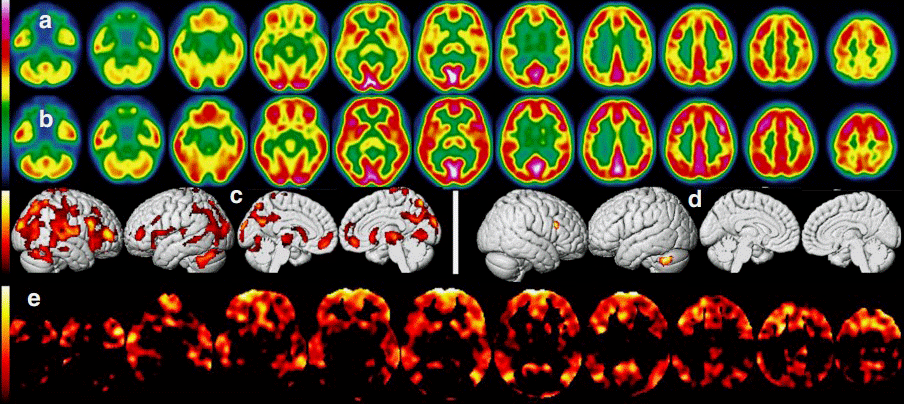
Notice the diminishing red in the white images in the C row, indicating less hypometabolism as well as the increased red in the B row, indicating increased oxygenation.
MRIs indicated that blood flows to the brain had increased. Cognitive testing validated the man’s experience when it showed he’d experienced significant improvements in global memory, executive functioning, attention, information processing speed, cognitive flexibility and multitasking.
A maximal cardiopulmonary exercise test continued the good news with a 34% increase in the VO2 max (energy production), a 34.4% improvement in the maximal METs, and a 16.9% increase in the lactic threshold. Lung functioning was improved by 44.3%, and lung perfusion by 20.2%.
It was all very good. Of course, it was possible that he might have improved on his own, but his rapid return to health upon starting HBOT suggested it was the cause.
Randomized Trial – The Israelis – who loom very big in this field – produced a bigger, more rigorous study in Hyperbaric oxygen therapy improves neurocognitive functions and symptoms of post-COVID condition: randomized controlled trial. This time, 73 long-COVID participants were divided up into HBOT (n=37) and sham HBOT (n=36) groups and given 40 sessions at 2 atmospheres pressure (five sessions a week over a two-month period). The sessions were 90 minutes, with five-minute air breaks every 20 minutes. Various symptom questionnaires including the SF-36 functional assessment questionnaire were given.
The trial required only that the long-COVID patients experience cognitive problems that affected their quality of life. With almost a quarter of the long-COVID patients (23%) not experiencing fatigue, and with over 60% of the group still working full-time, it was clear that a substantial subset would not have met the criteria for ME/CFS.
Both the sham and HBOT groups improved cognitively, but executive functioning and attention – two key areas in ME/CFS – improved only in the HBOT group. The authors proposed the increased blood flows to the frontal cortex of the brain was responsible.
Interestingly, microstructural improvements were found in the same area of the brain as in fibromyalgia patients who’d experienced childhood abuse. As in that fibromyalgia study, HBOT reduced symptoms of depression as well as pain and fatigue.
The physical functioning portion of the SF-36 asks how limited a person is over a range of activities – from running, to climbing several flights of stairs, to one flight of stairs, to bathing and dressing oneself – that a person experiences. They were fairly limited (60/100), but HBOT didn’t make much of a difference. People who weren’t able to climb several flights of stairs before HBOT apparently weren’t able to afterward.
The physical limitations portion, however, provided a very different picture. It asks how about your limitations regarding daily life activities such as work.
“During the past 4 weeks, have you had any of the following problems (cut down work; accomplished less, limited in the kind of work, difficulty performing work)…. as a result of your physical health?”
The participants’ initial scores (17/100) in the physical limitations questionnaire indicated that they’d had to dramatically cut down their daily activities.
HBOT didn’t remove all their limitations, but it did improve them significantly (from 17 to 51). Similarly, HBOT increased their energy scores (28-46) significantly (but not nearly to optimal health), and improved the extent to which pain interfered with their functioning (39-60).
The UK Trial – The title of a recent UK trial, “Hyperbaric oxygen therapy for the treatment of long COVID: early evaluation of a highly promising intervention“, fairly bursts with enthusiasm. This trial, done at a long-COVID clinic, was shorter – just 10 x 105-minute sessions (3 x 30-minute exposures to 100% oxygen) at 2.4 atmospheres pressure over 12 days. In the introduction, the authors noted, “in particular, HBOT has been shown to be safe and effective in the treatment of chronic fatigue syndrome.”
Instead of a mask, this study used the Midlands Diving Chamber and assessed effectiveness with the Chalder fatigue scale and a cognitive test called the NeuroTrax evaluation.
Even though the trial was small, the authors reported that the effect sizes were large – “suggesting that a substantial improvement had occurred.” Indeed, they stated that the change in the Chalder fatigue scale, information processing speed, and attention were “very large”, and global cognition, executive functioning, and verbal functioning were “large”.
Conclusion: The two HBOT long-COVID studies and the case reports all produced good results with recently ill patients. Encouragingly, even a short trial (10 sessions) produced, according to the authors, large effect sizes – suggesting that the trial produced real-life results.
Fibromyalgia
With HBOT studies stretching back 15 years, fibromyalgia easily leads the pack in HBOT studies. Way back in 2004, a Turkish study concluded that “HBO therapy has an important role in managing FMS”. It wasn’t till about 2015, though, that the FM HBOT studies really got rolling.
A Canadian group doing a metareview of chronic pain studies (including fibromyalgia) concluded:
“Early clinical research indicates HBOT may also be useful in modulating human pain; however, further studies are required to determine whether HBOT is a safe and efficacious treatment modality for chronic pain conditions.”
2016 brought the first largish, Israeli FM study. It included 60 women who received 40 sessions of 100% oxygen for 5 days/week for 90 minutes at 2 atmospheres of pressure. The goal of the study, as in most other studies, was to enhance neuroplasticity in order to tamp down the activity of the pain-enhancing brain circuits and boost the activity of pain-inhibiting circuits.
The study did just that: it decreased the hyperactivity of some regions (insula, anterior cingulate cortex, prefrontal cortex, thalamus), while increasing the activity of others. It also improved sleep, cognitive functioning, increased energy, and improved general well-being.
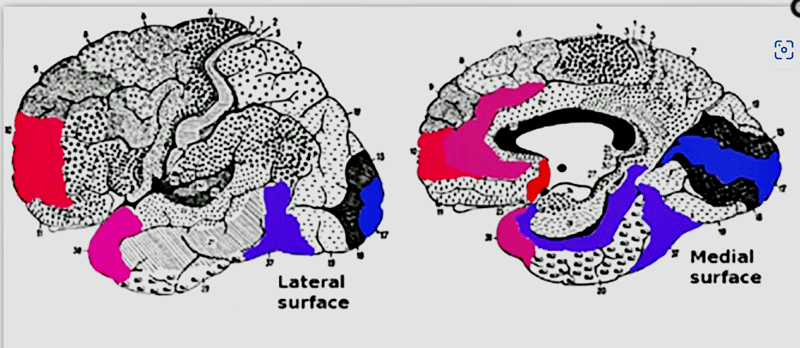
Note that highest activity increases (red) were in the prefrontal cortex while the highest activity reductions (blue) were elsewhere. (From the study)
HBOT’s impact on immune functioning was assessed in a 2016 study that included 40 90-minute sessions for 5 days/week at 2 atmospheres of pressure. The study found a “dramatic modification” of the pro-inflammatory status of FM patients but symptom severity, alas, was not dramatically affected with only pain perception showing a significant decrease.
The Gist
- Hydrogen oxygen therapy appears to promise much for energy-depleted, oxygen-deprived people with ME/CFS and long COVID. Its possibilities include taming neuroinflammation, enriching neuroplasticity, improving cognition, increasing energy, improving muscle function, etc.
- It seems like it’s made to order, but it also seems like a blunt instrument. If blood is being shunted away from the muscles, or if the mitochondria are damaged, it’s not clear how much providing extra oxygen will help. On the other hand, if an oxygen-deprived, inflammatory environment is feeding on itself, then fixing that environment could allow the system to reset itself and return to health.
- The few long-COVID HBOT case reports/studies have been small but positive, and suggest that in the right person, HBOT may even help return a person with long COVID to health.
- More fibromyalgia HBOT studies have been done than in long COVID or ME/CFS and their results – dating back over ten years – are decidedly mixed. Some studies have found little to no symptom improvements, others have found moderate improvements, and a few have found significant improvements.
- Several FM and long-COVID studies/case reports have found, though, that HBOT has been able to reverse brain abnormalities and enhance the functioning parts of the brain that have been inhibited (such as the prefrontal cortex), and also tamp down parts of the brain that have been overactivated.
- Few ME/CFS studies have been done, and the results have ranged from moderate to good.
- While case reports do indicate that progress can occur rapidly, in general, it seemed that more sessions (>20) worked better than fewer sessions (20 or less).
- While recoveries have been published, HBOT appears to be less of a game-changer for most than a moderate help.
- Much remains to be learned, however. We need large, placebo-controlled trials that can provide information on the optimum doses, what kinds of patients are helped, how they are helped and how long the help lasts. Unfortunately, according to clinicaltrials.gov, none of these trials appear to be underway at present.
- A recent gift of two hyperbaric oxygen chambers to Nancy Klimas’s Institute for Neuro-Immune Medicine at Nova Southeastern University in southern Florida provides the potential, though (once the infrastructure to support them has been built out) for us to learn much about the effectiveness of HBOT in ME/CFS/FM, GWI, and long COVID.
- If you’ve tried HBOT, please tell us how it went in the poll towards the bottom of the page.
The authors noted, “All of the scales in the physical component of the SF-36 significantly improved after 20 sessions (but not after 10)”. There’s nothing wrong with a 30% increase in a score, for sure, (general health status (26-35), bodily pain (21-30), and physical functioning (41-48)), but the patients hardly returned to health, either.
Another short but intriguing Italian study found that 20 sessions of HBOT at 2.4 atmospheres of pressure did not improve muscle strength or change muscle fibre content but did improve the ability of the central motor cortex to more efficiently recruit muscle fibers during exercise – potentially a very helpful thing. Yet another Italian study did not find improvement in symptoms, quality of life, or interstitial cystitis factors in FM patients with interstitial cystitis after 40 90-minute sessions of HBOT over 5 weeks at 2 atmospheres of pressure in a chamber.
A Spanish 40 sessions x 90-minute HBOT study at 1.45 atmospheres of pressure found HBOT did not improve oxygen saturation or heart rate during a six-minute walk test. The authors reported that HBOT did ‘significantly” increase the distance walked, but again, this may be misleading as the HBOT group increased from 481 to 513 meters (while the graduated exercise group increased from 508 to 558 meters). A 9% increase is apparently considered “clinically significant”, but one wonders how impressive the result was to the participants. Despite the larger number of HBOT sessions used, this study’s results were not impressive. Note, however, the significantly lower pressure used (1.45 ATA compared to 2-2.5) used in this study.
Another 40 session, 5 days per week, HBOT study at 2.0 ATA, this time in Toronto, involved 18 patients. This time the results were better, with the authors reporting that HBOT improved global functioning, reduced symptoms of anxiety and depression, and improved the quality of sleep. Notably, for the first time, a long-term follow-up assessment was done which indicated that the improvements were sustained at 3 months.
Conclusion: the results were mixed, with two studies providing moderate results, four reporting little or no symptom improvement, and two reported significant symptom improvement. The low atmospheric pressures in one study may have blunted its results. Another short study, though, did not benefit from higher pressures.
Chronic Fatigue Syndrome (ME/CFS)
A 31-year-old man, with a 1 1/2-year case of ME/CFS triggered by infectious mononucleosis that produced weakness, memory complaints, dizziness, and muscle/joint pains, received 50 sessions of HBOT over 6 weeks. (No other HBOT measures given.)
Brain PET Scans were done before and after the HBOT. The first scan generally validated what other studies have found: the man demonstrated widespread hypometabolism in the frontal cortex, and in the posterior cortical regions (precuneus, parietal, temporal, and occipital), and amygdala-hippocampal complexes, and cerebellum, which was largely reversed after HBOT.
This man’s physical and mental functioning scores of the SF36 increased by about 20 and 40 percent (from 57-70; 48-69) after HBOT. He was clearly still not well, but he experienced significant improvement in physical functioning and dramatic improvement in mental functioning.
A small (n=10) 2013 Turkish study provided 15 treatment sessions of HBOT therapy for five days over a 3-week period. It used the Visual Analog Fatigue Scale (VAFS), Fatigue Severity Scale (FSS) and Fatigue Quality of Life Score (FQLS) scaled. The HBOT therapy was well tolerated and the authors reported that the patient scores for fatigue, fatigue severity and fatigue quality of life all dramatically improved.
ME Research UK reported that in 2006, Action for ME’s survey found that some people with ME/CFS reported HBOT helped with brain fog or concentration, but others reported no lasting improvement.
Conclusions
It’s hard to draw a conclusion from these studies. The many different symptom assessment tools used and the lack of clarity about how clinically significant some “statistically significant” results are made it difficult to assess how effective many of these studies were.
The long-COVID and ME/CFS patient report suggested that HBOT can be very effective in the right patient and the long-COVID trials appeared to produce the best results. The fibromyalgia trials were not as successful, with some reporting significant benefits but others reporting few improvements in symptoms. Still, several studies showed that HBOT was able to improve brain functioning.
While one person with long COVID quickly returned to normal functioning, it appeared the studies that did more HBOT sessions had better results.
In general, it appears that when HBOT works, it’s usually less a game-changer than a moderate improver of symptoms. There is much, though, that we don’t know. We don’t know which patients HBOT works best in, nor how long the effects last. It was encouraging to see one study find the positive effects were still present 3 months later.
We clearly need large, rigorously controlled studies that have the ability not just to determine if HBOT works in long COVID, fibromyalgia, and ME/CFS but in which individuals it works, the optimum dose (length and number of sessions, atmospheric pressure) to use, how it does what it does, and most importantly, how long the effects last.
Indeed, the small (and enthusiastic) UK trial asserted, “there is an urgent need for larger-scale randomized placebo-controlled trials” as well as a registry of patients receiving HBOT for long COVID. (Both are now developed at the University Hospitals Coventry and Warwickshire NHS Trust and the Midland Chamber.)
The HBOT Poll for FM, ME/CFS, and Long COVID
If you’ve tried HBOT, please tell us how it went:
The Future
Few major HBOT studies, however, appear to be underway in ME/CFS, FM or long COVID. An 80-person, randomized, placebo-controlled, long-COVID Swedish study that will also investigate endothelial functioning is underway, but the study will include only 10 sessions, and those ten sessions will take place over six weeks (!) making it easily the least intensive study of any yet undertaken.
Clinicaltrials.com lists one other fibromyalgia HBOT study – a randomized but not placebo-controlled 60-session Israeli trial. No chronic fatigue syndrome trials are underwa,y but there is some exciting news from the ME/CFS front: a major ME/CFS treatment and research center has received two HBOT chambers.
The Lozick Family Foundation has donated two hyperbaric chambers to Nancy Klimas’s Institute for Neuro-Immune Medicine at Nova Southeastern University in southern Florida. Not only do these chambers provide the opportunity to get HBOT treatment in a safe environment but in a research environment as well. Dr. Klimas’s use of the chamber could tell us much about the effectiveness of this treatment option in ME/CFS, GWI, long COVID, and others.
First, the Institute needs, though, to build out the infrastructure to support the chambers before it can start using them.
Moderate improvement is nothing to sneeze at. Personally, I think it’s a lot to ask of any treatment that it be “it” for a disease like long COVID or ME/CFS. I would also bet that we won’t know the true value of HBOT until it’s used with other therapies that complement it. How about HBOT with anticoagulants? Or HBOT with mitochondrial enhancers, or antioxidants and anti-inflammatories to cool the flames down? My guess is that innovative doctors like Nancy Klimas that combine HBOT with other therapies will give us our best understanding of its value.
BIG (Little) Donation Drive Update
Thanks to the over 400 people who’ve kept Health Rising flying towards its goal.

It’s bitterly cold out there in many places, but the over 400 donors who have contributed thus far are heating things up for Health Rising! Thanks for your support!
This was a long blog, but HBOT is serious stuff now and a long blog is what it took to give its due.
Neither I nor Health Rising’s guest bloggers take the short view. We don’t rely on abstracts, for instance, but try and read the studies and puzzle these things out ourselves. That’s why, at times, we may question whether a result – even a statistically significant result – really means anything.
If you appreciate that kind of critical analysis – please support us in our year-end drive.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


I’d love to try HBOT. The problem is I have Ehlers Danlos Syndrome in addition to my history of EBV and Chronic Fatigue Syndrome.
There’s a retinal risk associated with HBOT. EDS means our tissues are flimsy, including our eyes. For that reason alone, I’d not find it worth the risk.
I have been doing hbot for 6 years now. It’s an ongoing treatment for me.
I had already suffered from Me/cfs before finding this treatment.
I started at 16.5 pressure for the first 5 years before going up to 24 pressure. I have recently been trying the 33 pressure & this has had remarkably better results. I believe the sooner you start treatment the better, especially with long Covid. There has been long Covid patients who have accessed the chamber I use & they have had amazing results. I’m fortunate enough to use hbot at the ms therapy centre near my home.
I wondered if time with the illness is a factor in how effective it is?
In my own experience I am so de conditioned after 4 years of no exercise that the work I needed to do to suck the oxygen through them mask left me feeling wrecked for a day or two. I don’t think I would have had the same problem in the first year or two.
Going to get one of those breathing trainers and try again after a couple of weeks of that
I was wondering about that as well – thus far the long COVID studies appear to be doing better…
Cort mentioned trials that included mitochondrial enhancers, anticoagulants, and antioxidants with HBOT. That’s connecting the research dots! You may only get so far physiologically with HBOT. But, throw in some biochemical support, and the improvement may be dramatic!
Hi Patricia. What ata do you find is best for me/cfs?
My hard HBOT chamber is arriving next week. Thanks 🙏
Thank you for this, Cort. My ME doc, Susan Levine, advised that HBOT does not typically bring lasting change. It’s interesting because in the hours after the first day of my two-day CPET, I felt *amazing*, better than I had in two years. I started to doubt my illness and doubt the decision to spend the money on the test plus travel/lodging/food. I really thought “maybe I’m not as sick as I thought I was.” So the next morning, day 2 of the test, I shared the thoughts with Betsy Keller at Ithaca College where I was being tested. She kind of slyly smiled and said “that’s because the exercise yesterday gave you a big old hit of oxygen. But the feeling didn’t last, did it?” No, no it did not 🙁
Still, if HBOT gave me that feeling, was close enough to home and covered by insurance, I’d definitely do it just for a few hours a day or normalcy. I’m sure I’d still have to pace though.
Interesting! That was a quick and dramatic response! I wonder what would happen if you regularly got treatment? It certainly suggests that oxygen delivery plays a key role in your illness….I really hope we get a lot more studies.
One thing this doesn’t address is the pressure of HBOT. I did about 30×45 minute sessions, and a later MRI found a Chiari Malformation (little bit of brain pushing out of my skull into my neck space). I’d done an MRI about a decade earlier for ear/sinus issues and it didn’t appear then. There’s no way to know that the HBOT caused it of course, but it’s a likely culprit. I don’t know whether it helped my CFS as I did intensive (5 days a week) IV therapy at the same time. Overall I did improve quite a lot: from severe to moderate.
Pressure! OMG I wonder if the studies used different pressures. I will check. Most of them used 2.0 ATA but one (which did not do well) used 1,.45 and some used up to 2.5.
I have had fibromyalgia (stress onset) for 2 years longer than ME/CFS (infections onset). The HBOT has been the biggest game changer for me in both pain and cognitive improvements – to the point I purchased one (oxyhealth brand Vitaeris 320) and oxygen compressor after using one at my specialists office. The LENGTH of the treatment for me matters almost more than frequency. Not only can I feel when I have sympathetic/parasympathetic shift but I have confirmed wearing my chest heart rate monitor as well – it usually occurs about 45 minutes into treatment- so I do 2 hour treatments.
I did treatment daily in the beginning and now space them out and average 2-3x/week for maintenance. I did HBOT at drs for about 6 months and have had my HBOT a little over a year. The studies with less than an hour I would expect to have not as good of results and/or take longer to show results.
I’ve been able to discontinue using both muscle relaxers and nerve agents and don’t wake up sore anymore unless I’ve let more than 4-5 days pass with treatment. I’m really hoping that as more studies are produced this will make this a more mainstream therapy so it would be covered by insurance and more people will have access to its benefits as I’ve been exceptionally privileged to be able to afford one as it’s been all out-of-pocket expense.
One hour at drs office $50/treatment – so was paying $100/wk. Owning system (largest soft sided one of this brand) with cage, mattress, bedding, and all parts, etc. $26k (US dollars). The smallest one without extras would’ve been about) $12k. The reasons for the larger one is so that I can stretch and didn’t want to feel too claustrophobic.
I unfortunately have not had a stamina increase and haven’t been able to return to work but my quality of life is greatly improved. I can even travel with it – it’s been on airlines and road trips (it’s heavy though so I’ve needed some transport assistance from friends and family).
Anyway, more treatment options that could be successful for at least some folks is better than fewer, thanks for the report!
Thanks, Rebecca! Good for you for monitoring your sympathetic nervous system response. That could reflect the HBOT enhancing your prefrontal cortex activity thus allowing it to reign in the limbic system.
I imagine that you did that with HRV (?). Clearly, we could use big enough studies that could make insurers pay for treatment.
Yes, using HRV to see nervous system response – measured with a POLAR10 monitor. We as a patient population definitely could use big HBOT studies to help determine length, frequency, atmospheres needed, etc. and get treatments mainstreamed for payment. There have been enough small studies for many years showing effectiveness (although some effects maybe temporary?) that I hope this area is further explored while there is research interest.
Insurers, especially if one is on Medicare, in my experience, are not interested in paying for this therapy. If they were, it would not be so difficult to find HBOT centers. Personally, I have continued to see insurers less and less willing to pay for expensive medications for chronic conditions: I.e, certain non-generic epilepsy drugs, non-generic somatropin Humatrope, and many others.
And many physicians,p, sadly, seem to want to be pressured to please insurers. I know several physicians leaving practice due to these pressures.
What brand? thx
HBOT? OxyHealth – style Vitaeris320
HR Monitor? Polar – style 10
I do mild HBOT through Restore Hyperwellness and find it helpful. I don’t see this mentioned in the article but I think a primary mechanism of action is that the oxygen kills gram-negative bacteria in the intestinal lumen. I find anything that reduces my microbial load in my gut is beneficial, and HBOT seems to be one way of doing that without throwing off other ecosystems.
Thanks Kira – I didn’t know that – thanks for mentioning it. It makes sense to me that HBOT could impact many systems in the body.
It’s hard to find HBOT centers that accept patients that have a condition not on the approved list . However I did find that free standing wound clinics often have a hard shell chamber and can offer it for non approved conditions.. I had a single treatment…1.5 hours at 2 atm . 400$. The recommendation is for a minimum of 15-20 dives to see any results but 40 treatments done 5 days a week is standard. I never continued because I’m to ill to make the trek and tolerate the oxidative stress it evokes. There are also a few commercial centers that have large multi place chambers that accommodate about 15 people. If it’s affordable for you I think it’s worth a try. I would have continued if I was able … I felt the Huge expense would be worth it if it gave me my life back !!!!
That’s not real HBOT though
Just an FYI. My Lyme Data study had a poll question about the effectiveness of Alternative Treatments. 347 people reported trying HBOT and of them 22% reported moderate/ very effective results. It was 13th out of 14 in effectiveness.
are there any stats on how many CFS/ME patients have tried using oxygen concentrators. i have heard anecdotally that it can make the body reliant on the concentratir
Hi Sunie
I’d also be interested in this information, as we purchased an oxygen concentrator for Covid emergencies and it’s now sitting at home. I’m wondering whether a daily hour or two of increased oxygen would be helpful or harmful to my young adult son with CFS.
I have had ME for 28 years and have been doing HBOT for the past 7 years. It is the only thing that I have tried that significantly, and consistently, helps with my ME.
I am a former biochemist and I have become quite knowledgeable about HBOT over the years. After being housebound for two years I managed to do HBOT 5 times a week for 5 weeks (before I ran out of money for it). It got me out of the house every day for 5 weeks! AND I improved at the same time.
I eventually became a volunteer at the MS Therapy Centre Lothian in Edinburgh and the centre’s boffin, eventually joining the board for three years (until the pandemic struck).
A lot of my friends with ME have tried it and it really does help
In particular, I find (as do most people) that it reduces mental fog, and improves recovery from over-exertion/crashes.
As a biochemist, I believe that it must be pushing cellular equilibrium towards anabolic processes that require energy like cell repair. As Cort’s article states, there are other benefits but this, to me, is probably the primary mechanism for helping people with energy-limiting conditions like ME.
I would love to see someone with ME have HBOT 5 times a week for a year to see what happens to them but the reality is that no one can afford that. Either financially nor the time that it would take.
In most places around the world, HBOT is rarely cheap. When I started it was £13 per session in Edinburgh. It is now £23 per session there. In North America, $150 plus per session is not uncommon. It is not a one-off therapy (it isn’t a cure) and it only helps if you go regularly.
I have experimented a lot over the years. I need to go 3 times a week after being away for a while. I can eventually cut this down gradually until I have to go only twice per week. I have never managed less than that.
Each session is an hour at pressure with about 15 minutes for pressurisation and another 15 minutes for depressurisation – so 1 hour 30 minutes in total. Plus you have to travel to and from the chamber (and this can negate any benefits gained from the HBOT).
Most people end up doing sessions at 2 ATA (atmospheres of pressure – in old parlance this is the same as a depth of 33 feet/10 metres). In my opinion, any pressure less than 1.5 ATA is worthless. There are a lot of home “chambers” sold (at great expense) that operate below this and for many reasons, that I will not go into here, are worthless to people with ME. You would be better off buying a home oxygen concentrator and using it all the time, than wasting a ton of money on one of them.. Or better yet, set up a charity and get a proper chamber for your local ME community to use as people with MS did all over the UK in the 1980s.
If you are in the UK, look for an MS Therapy Centre near you. Most help people with ME and long covid too.
If you live elsewhere, I have met many people who have travelled to the UK for affordable HBOT. As I currently have to go three times a week to get the most out of it, I cannot recommend this approach.
The USA in particular sees it as chambers as medical devices which require professional medical supervision – which makes it very expensive there (this is also why home chambers operate at such low pressures). Medical supervision is required in the UK (and many European countries) only for pressures above 2 ATA which is how the MS Therapy Centres can provide HBOT at therapeutic pressures. There is a long complicated history for all of this as hyperbaric medicine has been around for over 150 years (there was even a pressurised hospital – a WHOLE hospital – in New York for a while!).
With my name (above) I have included the website for the MS Therapy Centre in Edinburgh (now called Compass) for anyone who would like to know more about it. MS National Therapy Centres is the umbrella organisation for most of the centres in the UK. The whole thing was started by research in Dundee by a Professor James. He has written some interesting books on hyperbaric medicine (although not particularly relevant to most of us). K. K Jain has a very expensive but very interesting textbook on hyperbaric medicine that does summarise the state of the art well. It is only appropriate for people who are used to biomedical literature though.
Thanks so much for all the info and the links, K!
Hello, I’ve had much the same results as you using less atmospheric pressure. I really wish we had the studies and scientific proofing for most effective regimens- but this may be of interest to you speaking of atmospheres in treatment. (See attached blog & citations). It’s not apples to apples for ME but it’s not quite apples to oranges – I thought you may want to see the conclusions this author came to and read the articles they cite (PubMed needed) this was one of the “deep dives” (haha) I did prior to purchasing a home HBOT system and declined a more intensive higher atmospheres regimen. Interesting reads none the less but not any real new research (which is desperately needed to find out what works best). Anyhow, best wishes to you and yours in the new year – may this year bring us more optimal health and knowledge!
https://portchiro.com/blog/article/2020/5/18/hyperbaric-oxygen-therapy-1-3-atm-room-temperature-just-effective-100-oxygen-2-4-atm-evidenced-research/
Hi Rebecca,
Yes, 1.3 ATA can be beneficial for some people with 100% oxygen. Generally you have to have much longer sessions though.
However, the biggest problem is that the oxygen concentrators people use at home do not supply more than 93% oxygen (the normal range is 87% to 93%) nor do they supply enough volume for a full breath so users end up breathing a mixture of air and 93% oxygen (so more like 50% oxygen). This effectively reduces the chamber pressure further (it becomes the equivalent of a 1.15 ATA chamber with 100% oxygen). Required session times are MUCH longer at this pressure. So much so that you might as well skip the chamber part, save some money and inconvenience, and just use the home oxygen concentrator full time. A full day of that should be equivalent to an hour at 1.5 ATA with 100% oxygen.
An added issue of oxygen therapy in small chambers with nasal cannulas is that there is a build up of oxygen in the chamber. This is a fire risk that many ignore. It probably isn’t compatible with the electrical devices that people use in the chambers to pass the time.
I’ve also had decent results at 1.3 or 1.5 (not sure) ATA with a full face mask. I felt the efficacy dropped after the place switched to a nasal cannula, but they let me do some deeper dives.
Days on end of breathing 100% oxygen will destroy your lung microbiome and make you susceptible to staph infections.
Hello K McLellan, I suppose that if my ears hurt already at 3 meters below water, a 2ATA pressure will be too much?
I tried diving years ago, but couldn’t stand the pressure at 10 meters below, it was too painful…
Hi Niccon,
I have had ear equalisation issues from day one. Mainly my right ear. Although twice it has been my sinuses. It was every day for the first 6 months and then it got better. I think that I have a sticky, and perhaps narrow, eustachian tube and that the tube has probably expanded a bit with use over time.
Most people with blockage issues do improve with time. Decongestants can also help especially if mucous is being pushed into the tube during pressurisation. However, as long as the tube remains even slightly open (and unblocked by mucous), I have always been able to get air into my middle ear. I am pretty good at all the tricks!
Yawning is the best. Holding my mouth, nose and left ear closed and then blowing really hard can push air through the tube. Dropping my jaw while I do this can help (like in a closed mouth yawn – which is actually really difficult!). The biggest trick is to not let the pressure in the chamber get to high.
A pressure difference of 3m between the chamber and my ear is my absolute pain limit and by that point my tube is sealed too tightly to get air through it. So I have to get the pressure in the chamber released, sometimes by up to 2 metres, so that I can open up my eustachian tube again and get air through.
You definitely cannot do HBOT if you have blocked ears. You must be able to equalise the pressure.
I hope that this answers your question.
Thanks for the answer. I dived twice in my life and had pretty severe pain in my ears, and complications afterwards. Besides, not sure I could do HBOT where I live (Belgium). Maybe using oxygen from a tank at home might be an option instead.
I have HBOT weekly, I also have ear problems. I’ve never been able to unblock by holding my nose and blowing. My regime consists of taking ibuprofen about an hour before the dive, using a decongestant nasal spray at least 30 minutes before, sucking a menthol sweets, using earplanes plus yawning and swallowing. Sometimes it’s so painful I consider giving up but most of the time it’s ok. Unfortunately going through a bad patch right now.
The chamber I use increased the pressure more slowly for me at first. If you could a chamber that would do that and use earplanes you might possibly manage.
I developed ME/CFS, Fibromyalgia, and Sicca Syndrome (all professionally diagnosed over a 6 year period) following traumatic brain injury 14 years ago (bike accident – triple skull fractures and base of skull fracture). I had to stop working and have subsequently tried everything natural (and supplements) I read about but nothing helps much at all. I’ve been having HBOT 33 feet / 2 atmospheres for the past 5 or 6 years (with a year + break over lockdown) but can only afford one session a week (at MS Centre). I can’t honestly say I feel any benefit, it is exhausting to travel there and to sit with mask on, yet I keep going as feel it must be doing something! I am 67 years of age, female, previously extremely healthy. I’d be happy to participate in any studies to help self and others. Blessings Healthrising and fellow contributors, may we experience breakthroughs in 2023 🙂
A lot of people with MS only go once a week for oxygen therapy. Most do not seem to get much relief from their fatigue or see any short term benefits either. For them though there is evidence that the aspect of oxygen therapy that stimulates healing (by activating stem cells) pushes their condition more towards repair of the myelin sheath and away from destruction. The result is that people with MS who go regularly for HBOT have a slower disease progression than those who do not. Some people even experience stagnation or improvement.
I have no idea if this could also apply to those of us with ME. So the question is, over the last 5 or 6 years, do you think that your ME has stabilised or deteriorated less than it was deteriorating before you started HBOT?
I don’t know what the normal long term disease progression is with ME. For me I think that my health was on a downward slope (slowly but surely) until I started HBOT. Originally, all I wanted to do was to slow down the long term decline but I got more benefit from it than just that.
I’m in the uk. I recently tried HBOT for 19 sessions (MS centre), and found it debatable whether it worked or not. Getting dressed and driving myself to the centre three times per week was challenging and probably masked any improvements. I was initially having hyperbaric sessions, but I found them exhausting compared to no pressure HBOT. I really felt like breathing out against pressure was extra tiring… plus the treatment was in sitting, and I find prolonged sitting tiring. I’d be willing to give it another go though, if there was more evidence mounting up…
Hi Hayley, the getting to and from the centre is definitely a big obstical.
You are not breathing out against pressure though as your body is at the same pressure as the rest of the chamber. This issue is normally caused by an issue in the demand regulator that supplies the oxygen to your mask. It can normally be alleviated with a touch of “free flow”. The centre that you go to should understand the problem and be able to help you with it. There are other solutions depending on the cause of the issue.
Some centres can put larger inclined chairs in their chamber to make the sitting easier but, again, it can definitely be an issue – as can be the weight of the mask and hoses (can cause neck pain and fatigue).
Hyperbaric oxygen therapy is definitely exhausting. Healthy people come out feeling tired! It seems to release stored up fatigue and forces you to deal with it right away. After a while it gives you room in your stores to hold more fatigue so that activity isn’t so limiting. The more fatigue that you have stored up, the longer it takes to release it. But the journey can be long and difficult for a lot of people and isn’t necessarily worth the costs.
I’m about to start HBOT sessions at Compass in Edinburgh shortly so this is very reassuring (and as a fellow scientist also interesting), thank you so much for this comment! I’ve been trying not to get my hopes up but it’s good to know it helps some people with ME.
I found I was more fatigued initially. The chambers can be noisy and there are temperature changes, it gets cold when you come up from the dive. I wouldnt say it has made much difference to energy levels but my husband thinks I have more energy. I continue because I was getting really bad brain fog and felt I was deteriorating. As long as I have one session a week my brain works, when I have to skip one I notice the difference. I wish I could afford to pay for more.
It took about 10 sessions for me to notice much change but my centre increases the depth gradually so that was when I switched to 10 metres. Also I couldnt cope with more than 3 a week initially, going up to 4 later, because I have ear problems.
Replying to a few comments has reminded me of the analogies that I use for the benefits of HBOT.
If you think of ME like we have corroded rechargeable batteries: they are difficult to get energy in and out of.
HBOT removes some of the crud on the batteries making them easier to charge and discharge but you also have to deal with the crud that it releases into your system right away because it is pretty nasty in its own right.
An extension of this analogy is that we also have storage tanks for fatigue. Healthy people frequently use them during the week and empty them on the weekends. For people with ME our fatigue storage capacity is full, perhaps even over full and overwhelmed. HBOT releases some of the stored up fatigue (again, we have to deal with it when it is released). If our tanks are full then releasing the fatigue gives us a bit of extra capacity and breathing space. A new fatigue storage equilibrium will eventually be reached depending on how much HBOT you do and how active you are/become.
If your fatigue storage is over full then, until the overflow is dealt with, you won’t see much benefit from HBOT – just the constant now of fatigue. I went every day for 5 weeks when I started until this phase ended (the normal protocol is 3 weeks). It could take me an hour after a session to face the 25 minute drive home (I still get hit like this from time to time).
—
HBOT does 3 main things:
1. Stimulate healing (via stem cells) especially in low oxygen tissues;
2. Reduce inflammation:
3. Pushes the equilibrium of cellular reactions towards aerobic respiration.
I have no doubt that it is the last two things that benefit people with ME the most. The reduction of inflammation is probably what helps people with Fibromyalgia the most. It is also probably what causes the immediate/short term benefits that most people get from HBOT (whether they have ME or not) as inflammation is a major feature in most of the conditions that benefit from oxygen therapy.
I have had HBOT for Long Covid – initially sitting outside the chamber and breathing in through a mask and latterly in the chamber. I have found it really helpful – to the extent that I thought it was making me completely better – so I stopped pacing. Uh oh :-(. So I’m back in a dip BUT will definitely do oxygen again. I felt markedly better and was doing markedly more activity. However I live very close to the centre – if I had to drive much more than 15 minutes for the treatment I’m not sure I could have it as regularly as I think is needed.
I am a long time CFS, FMS, sufferer. Also a DES daughter. In 2004 I chanced upon a product that provides oxygen to the bloodstream, “Cell Food”. It was created by one of the scientists that helped invent the A-Bomb! The product is based on using deuterium in a solution of purified water and seaweed. It is chemically H3O I believe. A liquid that one puts drops of in purified water or juice. After 2 weeks of use I experienced major relief to my painful hands and feet and morning grogginess, and began to feel like a version of Rip Van Winkle, re-awakening after 20 years of disability. I was able to start a regular exercise routine, and lost 35lbs over 6 months, and able to walk longer distance, swim, light weight train and even dance! I’ve been using it since then, and remain much better with much less exercise intolerance. Very rarely get brain fog, and most other symptoms minor. I wonder if this method of introducing oxygen might be more cost effective alternative to hyperbaric chamber approach. I use approximately one, one ounce bottle per month which costs $36 retail, and one can get it wholesale as a health practitioner. It was a real game changer for me! Manufactured by Lumina Health in Florida. I hope this might help someone.
Thank you Wendy
I started doing mild HBOT, 1.41 ATA (6psi) 2 oxygen concentrators with a chiropractor for a genetic blistering skin disease. After 15 60-90 minute dives, my skin was remarkably better. The first 20 dives I did feel more fatigued afterwards and if I did longer then 90 minutes I felt very very fatigued for a couple of days and my skin would not heal. When I started drinking hydrogen tablets in water before and after dives I no longer had that fatigued feeling. After just short of 40 dives I have noticed that my ability to heal is faster with the skin blistering. I have also noticed my legs are stronger and am able to do stairs much easier. I have also been using Photobiomodulation since 2017. Dr Jason Sonners has some good youtubes on the many benefits of HBOT. I’m currently considering buying my own soft chamber for home since I’ve already paid $4000 out of pocket this year with the chiropractor. I do feel the regenerative benefits from mHBOT are still there even though it’s been weeks since my last dive. And if I can continue, things will improve more. I think the dose is dependent on so many factors which I can see makes it hard to study. I think if I would have done a 2ATA hard chamber first I would not have seen benefits.
An important clarification on the mechanism of action of HBOT: It was originally thought that HBOT somehow “forced” more oxygen into tissues increasing cellular respiration which somehow made cells healthier. What is now known is that HBOT works by inducing a temporary burst of oxidative stress due to the body processing high levels of oxygen it can’t actually use, which then activates cellular antioxidant mechanisms, which improves cellular healing and also helps to dilate blood vessels. This is known as a hormetic effect and interestingly many substances sold as antioxidants are in fact pro-oxidants, that work in a similar fashion. Whether or not HBOT will help someone just depends on whether these pathways are available for activation or whether they are exhausted due to age or extended illness. (a gross simplification of a very complex subject) In short, HBOT can make things better or worse, just depending of your specific physiology. Also, more is not always better with HBOT because stimulating those pathways beyond their capacity to react is directly counterproductive. For the very ill and elderly, HBOT should be applied slowly for this reason.
It’s important to understand this because most people administering or prescribing the therapy do not.
Hello Brian,
That is wonderful information, can I please ask what you comsider starting slowly with HBOT? Eg. Start with 1.3ATA a few times a week first? Or 2ATA just a few times a week?
I just started 2ATA HBOT, 60minute sessions. I just did 6 sessions in 6days and that has let to a big flare up. I’m wondering what you recommend for how many times per week to attend?
Thank you 🙏
Yeah that’s exactly the kind of uninformed irresponsible HBOT therapy that I’m talking about. Honestly, it’s been a long time since I learned this information and I gathered it from listening to a bunch of obscure medical podcasts so it’s not really fresh in my mind. And I don’t know if there are any guidelines for specific application recommendations, but I believe the person who was speaking mentioned just a couple times a week for someone who’s really sick.
Brian Schulz please can you explain how it can make you worse as I had very weak arms and legs and did 3, 1 hr sessions in a HBOT chamber at the beginning of August, two weeks later, I was in hospital unable to move my arms and legs they were that fatigued, heavy and throbbing. I had to have a hospital bed at home, which I’m still in now in November. I’ve only stood four or five times, but when I do, it just seems to make them even weaker. Been bedridden before, but I’ve never felt the heaviness that my legs have since the treatment. Pilates instructor as well as having ME I was doing very deep lateral thoracic breathing?! My arms are improving my legs aren’t whatsoever. I can’t understand what’s happened for them to lose 100% of their power and for it not to come back as yet. Strange arms getting better as I can feed myself now. I was working before I had the sessions. Only a cpl of classes a week but leg weakness wasn’t the best beforehand. Really appreciate any feedback off anybody
Hi Gail, I’m so sorry to hear what you’re going through, That sounds brutal. I can’t explain your symptoms, but what I can say is that hyperbaric oxygen therapy functions by creating an abnormally high concentration of oxygen in the blood Which leads to oxidative stress or an increased concentration of free radicals that are damaging to the body that your body needs to mop up. This in itself is a bad thing, but this also causes your body to turn on epigenetic triggers that in a moderately healthy person will improve your bodies ability to fight oxidative stress. However, if someone is really sick and your body doesn’t have that reserve capacity anymore then all you’re doing with hyperbaric oxygen therapy is just adding more oxidative stress And we know that people with MECFS are already challenged in this way. So basically, you’re just poisoning your body with too much oxidative stress Which at some point contribute over a threshold of making the illness worse, It sounds like you’re a fairly active person And I know the hell that you’re going through so if you want, I can share with you what I’ve done to recover about 50% from the illness. I don’t have time to type it out here, but if you just type my name into a search engine along with the word kayak, you will immediately find my website and my email and if you email me, I will write up what I’ve done to get better
Dear Gail, I hope you’re feeling better still by now. Your comment made me wonder if what you’re experiencing may be a lactate issue. Did they test for this at the hospital? Feels like too basic a question, but you never know with me/cfs in the hands of non-specialists. Although HBO2 helps athletes to clear lactate faster, in someone with me/cfs this may work differently. All the best.
I would love an update on this topic if there is one, I just saw a video of Bryan Johnson on YouTube doing this, his stats were quite impressive – and all on systems that indeed our bodies could benefit from. Obviously I knew about this treatment, it has been around for quite some time, but never went for it for lack of data. Bryan Johnson is kind of a special guy, of course his incentive is entirely different than ours, funnily enough he tried/takes quite a few supplements or low dose treatments that are not uncommon in our community. It gave me a reminder of this treatment option!