

Shingles
Shingles – the word sends a chill through me. I was introduced to shingles through my grandfather’s wife, Ethel. With her Scottish brogue and her lively personality, she was a great addition to our family after my grandmother died. She and my grandfather loved to hit the dance halls – until she came down with shingles. She spent the last couple years of her life in agony in bed – telling us that she wished the lord would take her away.
 Then a couple of weeks ago, I bumped into a friend about my age who lifted up his shirt to show a dazzling array of fiery welts extending across his stomach and back. Thankfully, he’s recovered – for now.
Then a couple of weeks ago, I bumped into a friend about my age who lifted up his shirt to show a dazzling array of fiery welts extending across his stomach and back. Thankfully, he’s recovered – for now.
It seems we can literally never get away from the herpes viruses. Master evaders of the immune system, and ubiquitous in the population they’re with us from the day we get them until the day we die. The only question is whether we can keep them in check or not.
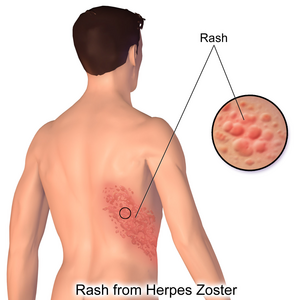
Shingles or herpes zoster is caused by the reactivation of the varicella-zoster virus (VZV), also known as human herpesvirus 3 (HHV-3, HHV3) – which also produces chickenpox in children. Virtually everyone (99%!) born on or before 1980 in the U.S. had chickenpox – whether they remember it or not – at some point.
After the initial infection with VZV (chickenpox), the virus lies dormant in a particularly touchy place – sensory nerve roots or bodies called ganglia – found in the trigeminal nerves in the face, the dorsal root ganglia outside the spine, and the nerve bodies that transmit autonomic nervous system signals.
There, the virus usually lies dormant for decades only to erupt in about 25% of people whose immune systems fail to keep it under control – usually as they age. Once reactivated, the virus migrates up the sensory nerves to the skin where it produces produce shingles or herpes zoster, and with it, the rather stunning and usually very painful rashes. For people over 85, the incidence is believed to be one in two.
Feelings of pain and tingling usually precede the appearance of the lesions that appear on the skin. The burning pain, flu-like symptoms, the feelings of depression, and motor weakness they can cause usually subside over a couple of weeks, but in about 10–15% of cases, a painful and often disabling condition called postherpetic neuralgia occurs. At this point, nerve damage has occurred and antivirals are no help. Instead, doctors turn to pain drugs, anticonvulsants, and antidepressants which have limited effectiveness.
Other complications can occur. Herpes zoster ophthalmicus (HZO) – which occurs in about 10% of herpes zoster cases – produces burning pain, extreme sensitivity to touch (allodynia), and headache along the branch of the trigeminal nerve that leads to the eye. HZO can result, particularly if left untreated, in serious eye problems, and it increases the risk of stroke.
In Ramsay-Hunt syndrome (herpes zoster oticus) different sensory neurons in the face are attacked, causing facial paralysis (palsy), ear and face pain, and sometimes hearing and balance problems. In Zoster sine herpete, skin lesions are not seen, but skin pain and motor weakness are found. Other possible outcomes include inflammation of the spinal cord (myelitis), inflammation of the brain (encephalitis), cerebellar ataxia (coordination problems), septicemia, pneumonia, and toxic shock syndrome.
An interesting 2009 hypothesis proposed that shingles, in the form of zoster sine herpete; i.e. herpes zoster without rash, might account for some cases of ME/CFS. Recently, a large study found that COVID-19 was associated with an increased risk of coming down with herpes zoster. That, of course, made sense given the continuing findings of herpes virus reactivation in long COVID. In what will probably surprise no one, as well, having herpes zoster was associated with a significant increase in coming down with ME/CFS.
Diagnosis and Treatment

The reawakened virus moves up the nerves (ouch!) to the skin where it produces its characteristic blisters.
While antibody tests can be used, they are only partially effective. PCR tests are the gold standard for diagnosis. In all cases, the effectiveness of the antiviral treatment (oral acyclovir, valacyclovir, penciclovir, famciclovir) is greatly enhanced if the reactivation is caught early – within 48-72 hours of the appearance of the rash.
Varicella zoster immune globulin (VariZIG) can be used in high-risk individuals within 10 days of the appearance of the rash.
Another Vaccine – Another Tough Question
There’s absolutely no doubt that the shingles vaccine works. The question is whether to take it or not. On the one hand, you risk the possible side effects of the vaccine, on the other a possible debilitating and painful illness. The same immune deficiencies that might end up in experiencing more side effects with the vaccine could also conceivably increase the possibility of viral reactivation and shingles.
The shingles vaccines are one of the more effective vaccines around. Prior to the introduction of the vaccination program, shingles used to be quite common in the U.S. with an average of 4 million coming down with it in the early 1990s. Since the introduction of the varicella vaccination program in 1995 in the United States, shingles “morbidity” (cases and hospitalizations) and mortality (deaths) have decreased by 93 and 95%.
Various shingles vaccines have been developed over time. An older one Zostavax (Merck) simply consisted of a one-time, larger-than-normal dose of chickenpox vaccine. While it produced fewer side effects, it is not as effective for as long a period as the double-shot Shingrix vaccine and is not suitable for people with immunosuppression or immune diseases. Merck stopped selling it in the United States in November 2020 and Australia in 2023,
The Shingrix vaccine is given in two shots two to six months apart. Not only is it more effective than Zostravax but lasts longer – at least 7 years – and possibly much longer. In adults 50 to 69 years old with healthy immune systems, Shingrix was 97% effective in preventing shingles and 91% effective in adults over 70. Even in adults with weakened immune systems, the CDC reports that the Shingrix vaccine is 68%-91% effective in preventing shingles.
Side Effects
The usual list of side effects – sore arms, and flu-like symptoms lasting a few days – are listed. One possible serious side effect concerns a very slightly increased risk of Guillain-Barré syndrome. One large study found approximately 3 excess Guillain-Barré syndrome cases per million vaccinations in senior citizens.
As with any vaccine, try to get a good night’s sleep after getting it, as this may help boost the immune response.
Vaccine Recommendations
Availability – shingles vaccines appear to be readily available – the question is whether insurance will pay for them or if you have to. The two-shot Shingrix vaccine costs about $360 U.S.
The Gist
- My personal experience with shingles – the condition caused by a herpes zoster virus reactivation – was of my grandfather’s wife – a vivacious woman who spent her last years in agony in bed because of it.
- Herpes zoster is the virus that causes chickenpox. Virtually everyone born before 1980 – whether they experienced chickenpox or not – has been exposed to the virus.
- After the initial infection, the virus lies dormant in a particularly touchy place – sensory nerve roots found in the face region or outside the spine, or elsewhere. There, the virus usually lies dormant for decades only to erupt in about 25% of people whose immune systems fail to keep it under control – usually as they age. As we get older reactivation becomes more and more likely until after the age of 85 it happens in one out of two people.
- When reactivated the virus moves up the nerves to the skin where it produces its characteristic welts, burning or stabbing pain, flu-like symptoms, etc. These symptoms usually subside over a couple of weeks, but in about 10–15% of cases, a painful and often disabling condition called postherpetic neuralgia occurs. At this point, nerve damage has occurred and antivirals are no help. Instead, doctors turn to pain drugs, anticonvulsants, and antidepressants which have limited effectiveness. Other complications can occur such as eye problems, inflammation of the spine and brain, stroke, etc.
- If a shingles rash occurs it’s critical to get it treated quickly with antivirals within 48-72 hours of the rash appearing.
- Canada reports that “The incidence and severity of both shingles and post-herpetic neuralgia increases sharply after 50 years” and that the treatment options for both have “limited effectiveness”.
- Shingles vaccines have dramatically reduced the incidence of shingles in the U.S. since the early 1990s. Since the introduction of the varicella vaccination program in 1995 in the United States, shingles “morbidity” (cases and hospitalizations) and mortality (deaths) have decreased by 93 and 95%. Even in adults with weakened immune systems, the CDC reports that the Shingrix vaccine is 68%-91% effective in preventing shingles.
- Various shingles vaccines have been developed over time. An older one Zostavax (Merck) simply consisted of a one-time, larger-than-normal dose of chickenpox vaccine. It is efficacious but is not as effective or as long-lasting as the double-shot Shingrix vaccine now in use in the U.S., Canada, Australia, and the U.K.
- Both the U.S. and Canada recommend that adults over the age of 50 get the Shingrix vaccine. Even if you’ve already had shingles, or have already received the Zostavax or the varicella (chickenpox) vaccine, the CDC still recommends that you get the Shingrix vaccine.
- The Shingrix vaccine costs approximately $360 in the U.S. but is largely covered by insurance there. Other countries provide less financial support but the vaccine appears to be available for those willing to pay for it.
- Four ME/CFS experts responded to my question about whether they recommended getting the vaccine. All recommended getting the vaccine, and two stated their patients did well with it, while one cautioned that people who had trouble with prior vaccines might want to wait until more autoimmune studies were done on it.
- Check out the Shingles poll at the bottom of the post to see how people with ME/CFS and other conditions responded to the vaccine.
Even if you’ve already had shingles, or have already received the Zostavax or the varicella (chickenpox) vaccine, the CDC still recommends that you get the Shingrix vaccine.
The Affordable Care Act and the Inflation Reduction Act of 2022 mandated that insurance companies pay for Shingrix in the U.S. and I paid nothing for mine last year.
The United Kingdom – the National Health Service reports that a shingles vaccine is available to people who are between 70 and 79. Most people will get the Zostavax vaccine, but the Shingrix vaccine is provided for those with immune issues.
Canada – the Shingrix vaccine was approved for use in Canada in 2017 and Zoxtavax is also available. Although the National Advisory Committee on Immunization recommends the Shingrix vaccine for Canadians over 50, the cost depends on a person’s drug plan and the province they live in. Ontario, for instance, provides free Shingrix shots to people 65-70 years of age.
Australia – Zostavax is being replaced by Shingrix this year in Australia as well. The Australian Immunization Handbook recommends that all adults 60 years and over, and adults aged 50 years and over who live in the same household as someone who has a weakened immune system, get the vaccine.
Support for getting the vaccine is limited, though. Only non-Indigenous individuals aged 70 years (no one younger or older – only 70-year-olds (!)), and Aboriginal and Torres Strait Islander individuals aged 50 years or older, as well as immunocompromised individuals aged 18 years or older, will have free access to the vaccine. Individuals 70-79 can get the Zostavax vaccine free until October 23rd. Everyone else has to pay for it.
ME/CFS Expert Recommendations
I asked several ME/CFS experts whether they recommended getting the Shingrix vaccine.
- Dr. Benjamin Natelson – I am a big supporter of people getting this vaccine. This one really works and shingles can be a horrible, disabling illness.
- Dr. Charles Lapp – My patients have tolerated the Shingrix vaccine well, except that the shot itself is quite uncomfortable. Two are required. I remind patients that Shingrix does not prevent shingles, but reduces the severity. For those who prefer not to have the discomfort of the two shots, I remind them that the antiviral drug Valtrex is a very effective alternative should they contract shingles.
- Dr. Susan Levine – I think the decision of whether to give the Shingrix vaccine must be made on a case-by-case basis. We’ve had a number of cases in which vaccines have either triggered a relapse or the onset of ME/CFS, but we also know that COVID and a suppressed immune system can increase the likelihood of getting shingles, which can also cause irreversible damage. I think in an ME patient who has previously tolerated vaccines, that Shingrix should be recommended and that the patient be observed for the unlikely occurrence of Guillaume-Barré syndrome. In someone with a track record of adverse reactions to vaccines, it may be prudent to wait until there is more data collected on sequelae of Shingrix in autoimmune or immune-compromised hosts.
- Dr. Kathleen Kerr – My Shingrix vaccine experience for ME/CFS patients is in line with other vaccines. I’ve had a few patients down for a week or two but none that did not get back to baseline. If I get the chance, I generally recommend pre-loading with vitamin C and as well the mast cell stabilizers per Nancy Klimas for the Covid vaccine.
Dr. Klimas’s suggestion for mast cell stabilization while taking a vaccine”
You can mitigate the risk in a number of ways – just the way you do when you feel a relapse coming on. Before the vaccine make sure you are taking enough antioxidants, particularly NAC or glutathione and coQ10. The big mediator of post vaccination relapse and immediate reactions is mast cell activation. If it happens immediately, that is anaphylaxis, but if it happens slowly and low grade over days the mediators mast cells release can drive a classic ME/CFS relapse.”
“So, take an antihistamine before and for several days after the vaccine – the strongest one you tolerate. (Benadryl is one of the strongest, Zyrtec is another good choice). There are many mast cell stabilizers, watch Dr. Maitlands excellent lecture on our web page from the recent conference we sponsored on the subject if you want to know more: Managing the Syndrome Soup: POTS, EDS, MCAS & ME/CFS https://www.nova.edu/nim/events.html”
There are natural supplements that act to block or clear histamine and stabilize mast cells such as alpha lipoic acid, ascorbic acid, B6, diamine oxidase enzymes (DAO), luteolin, N-acetylcysteine (NAC), Omega-3’s, riboflavin, SAMe, quercetin, and natural sources of theophylline like green and black teas.
If you have been diagnosed with mast cell activation syndrome it would make sense that your risk of an immediate reaction to any vaccine should be higher, though the data on the risk to people with mast cell activation syndrome or prior vaccine allergic reactions is not yet known with the COVID vaccines.
The ME/CFS, FM and long COVID Shingles Vaccine Poll






I had the first shingles vaccine and was shocked at how sick I felt the next day. Never in my entire life (and I’m 83) have I ever experienced more than a very slight ache in my arm after ANY vaccine. This was awful and reminded me of a horrible case of the flu I had when I was about 20. However that lasted weeks and the vaccine after effects were the better part of a week with the first 2 days the worst and lessening each day afterwards.
I am scared to get another. I was diagnosed with both ME/CFS and Fibromyalgia by Dr. Lapp. I wish I could ask him his advice in getting the second shot. Aptmts at the Hunter clinic cost way more than I can afford so I’ll never know I guess. His treatment plan helped me to feel much more human after I’d been sick for 10 years before being able to be seen by him.
My reactions after first Shingrix and Moderna COVID vaccine were very noticeable. But reactions after the second doses of these 2 vaccines were much milder. Nothing like after the first time. I got them at age 57 and 59 respectively. So my reactions may be milder than someone over 80.
I’ve had every Covid vaccine and booster available. Pharmacies come to the senior facility where l live now to administer flu and Covid vaccines. I appreciate that as I no longer drive. Never had any kind of reaction after a Covid or flu vaccine thankfully.
Pat, I’ll check around and see what I can find out. I’ve been away from everyone for quite a while. I’ll get back with you.
Nancy Henson, do you live in NC, possibly near Charlotte?
I’m looking for another CFS specialty doctor to take the place of Dr Lapp, as I cannot afford appointments or treatment there either. I live in the Lake Norman area and need a specialist as soon as possible to oversee my condition.
I’m not a DR but I’d recommend not getting a second vaxx because I rarely have more than mild symptoms with any vaxx and that was the same with the 1st Shingrix. The second Shingrix was the worst vaxx I’ve ever had in my life. Everyone I’ve asked about it says the 2nd one is bad. The statement above by Dr. Charles Lapp about the anti-viral drug Valtrex should give you peace of mind.
But some doctors say you can’t take Valtrex is the shingles actually goes into your eye.
You’re in a much more complicated situation then.
Similar to what public health experts are saying now that Paxlovid doesn’t work effectively anymore.
Better never to get it than to try to fight it, IMHO. Especially if you’ve already got a debilitating chronic illness.
Interesting! I attribute alot of my recovery to getting shingles under control. I never got the vaxx because 1. I was scared of making it worse (other jabs make my shingles flare up) 2. My antibodies were through the roof already so more antibodies did not seem to be what I needed 3. I needed to be outbreak free for 12 mos and couldn’t string 12 mos together 4. Doctor hesitant bc I was not >50. I guess it’s simpler if you don’t already struggle w outbreaks? Anyway this was a good read & important discussion, thank you!
Can I ask how you were able to get your Shingles under control?
Had disseminated shingles at age 40 and fortunately was put on an antiviral right away. Even so, it was extremely uncomfortable and took about 2 weeks to subside. When I became eligible for the Shingrix vax at age 50, I jumped at it. I knew I’d be slammed with the effects of my immune system gearing up (headache, muscle aches, fever) but it was worth it. I was back to baseline in 3 days. Much better than my 5th COVID booster, which knocked me back for a month.
No problem. I’ve gone thru to read all comments so far. Its very interesting the variables in side effects.
Similar to Cort, I’m in US but doctors didn’t tell me about shingles vaccine until it incidentally came up when I was 57 years old. At that time I started seeing a new PCP. I was telling him about my fibromyalgia. He said he didn’t know what to do with fibromyalgia. But to make sure I wasn’t having shingles or not to get it on top of fibromyalgia, he asked if I’d had shingles vaccine. That’s how I got the vaccine.
I was surprised to have very noticeable reactions after the first shot. I used to get flu vaccines in my 30’s and had no reactions. But I’d trade 2-3 days being sick for worrying about having painful blisters for weeks. Reactions after second shot were negligible.
I had had shingles 3 times, so was not interested in a fourth.
I had an interesting reaction to both the second shingles vaccine and the last Covid booster. One of the conditions that I have is POTS. When I was younger I would have 2-3 days in a row where first thing in the morning, when standing still, I would start to feel like I was going to faint. It would go away after a few days and the same thing would happen after several months, again for just a few days in a row. As I got older it just seemed to go away. I hadn’t had a near-fainting episode in years until last year. The day after I had the Covid booster I had an episode of near-fainting, and the same thing happened the day after the second Shingles vaccine.
I had shingles across my back when I was 29. I was lucky that it was caught as it was erupting because I was already hospitalized with flu, UTI and rule out stroke (they decided I had a hemiplegic basilar migraine which happily totally resolved). The antiviral worked well, I have no lingering symptoms, but three weeks of pain and knowing it could have been worse had me getting the Shingrix vaccine as soon as possible after my HMO approved it at age 60.
I read something on Twitter last week, but I haven’t sighted the study. It said the Shingles vaccine may decrease the risk of developing Alzheimer’s disease substantially.
I’ve also heard if you had severe Chicken Pox that you have a higher risk of developing a severe case of Shingles. I had a really severe case of it when I was 20. It left me with chronic hives & sinusitis for years. I’ll be getting the Shingles vaccine soon, once I turn 50 as I’m pretty sure my GP will agree that ME/CFS compromises the immune system. But I’m not sure it will work for me.
I was vaccinated for Measles as a child, yet had Measles 3 times (each time diagnosed by a doctor). I’m pretty sure I had Mumps twice as a child. My Granddad had Measles 7 times and my cousin’s son was vaccinated for Chicken Pox as a baby, but was exposed to it at Kindy, ended up with seizures, went into a coma and nearly died as a result. There’s quite a few of us in my family that vaccines haven’t worked for preventing common childhood diseases, so I suspect there’s some screwed up genetics. We rely on everyone else to be vaccinated to keep us safe.
Just to clarify I had a severe case of Chicken Pox. I’ve never had Shingles.
I had mumps several times as a kid, too, even though they kept giving me a booster MMR.
Yes! Don’t even think twice! Anyone should get the shingles vaccine.
The current one, Shingrex, requires two shots, results in a sore arm for a couple of days, and saves the consequences of a severe (or any) case of shingles.
I had the old shingles vaccine in 2009, when there was a chance I would have to be hospitalized for a severe burn, and 18 months later I got shingles. I was also under a state tax audit at the time, and it was total hell.
The pain from shingles is excruciating. The illness, which lasted almost 3 months, took me down at least one notch in functionality from my previous level, permanently. And I was lucky: I had it on my scalp and face, and was just lucky that it didn’t go into my eye, so I could take Valtrex. If it goes into your eye, you’re basically on your own.
Don’t risk it! Get the vaccine. We’re lucky we have the vaccine and shouldn’t be second guessing about whether it will make us worse or not. Our second guessing all the time will make us worse.
My mother had congestive heart failure, and the opportunistic illness which killed her was shingles.
Don’t Risk It!!!
Dr. David Kaufman told me not to get the shingles vaccine, and no flu vaccines, because of my genetic testing. I have ME/CFS, hyper-andrenergic POTS, MCAS, Fibromyalgia, etc. I had Shingles on my head when I was forty and my doctor at the time didn’t recognize it. I said, no, there’s something really wrong. Then I got the rash and a scab on my eyebrow. Luckily it stopped there.
Hi Barbara – do you remember what it was that your genetic tests showed up?
Sorry, I don’t remember. But there is something reported in my Livewello interpretation. I’ve been looking for it, but the new site stymies me. I’ll try again when I’m not so tired.
I suggest you get a second opinion. If you got shingles once, and got it on your head, thank heavens it didn’t come down onto your face and into your eye.
The unfortunate fact is that if you got it once, you will probably get it again. It cycles around. They used to think it cycled in thirty year cycles; for my mother, that was pretty much right on. My mother got shingles in her early 60s, and then it came back — when she was severely compromised by congestive heart failure — when she was 88. It was a miserable way for her to die, so I am a big advocate of the vaccine.
That is — you will likely get it around unless you get the Shingrix vaccine.
I had a shingles vaccine (the old one, just one shot) at my sister’s urging because she had shingles at around 60. She was lucky not to get it on her head, but it was still miserable.
18 months later, I came down with Shingles. Would I have if I hadn’t had the vaccine? I don’t know — but it was the old vaccine, which was known to have some shortcomings.
As soon as the Shingrix vaccine became available, my sister got it (she’s generally in good health), I got it, and as soon as she qualified (by turning 50) by niece got it. None of us wanted to die the painful death my mother did, when there was something that could prevent it.
Good luck with your decision. In general, I think vaccines are worth the sore arm, the couple days of flu-y symptoms, etc. Perhaps because I was born in the late l940s and polio was a huge scare. My parents got me all the vaccines that their cautious pediatricians advised, and I’m very grateful. I think sometimes people forget that the disease is almost always far worse than temporary side effects from the vaccine.
I would also want the doctor who recommended against it to give you very specific reasons why
Cameron, some people have been triggered by a vaccine into a decades long or lifelong case of ME/CFS. I’m not talking about a sore arm or feeling flu-y. We are not immuno-typical. I don’t know who you are, and frankly I don’t care. You are not familiar enough with ME/CFS to insult anyone here. I’m not against vaccines, as I have clearly had the Covid vaccine.
I have had a severe case of ME/CFS for 30 years. I am quite familiar with it. I am lucky not to have suffered the psychiatric symptoms some ME/CFS patients suffer.
I am not speaking to the person who likes to hurl insults. I am speaking to rest of the tribe. We have to question our doctors – politely, but still question. We have to learn to become experts and really look at the science.
At least I hurl my insults honestly. You’re a passive aggressive insult machine.
Cameron, everybody here is different. I appreciate that you want to warn people of the horrors of Shingles, but you can’t apply your experience to everyone. We all have to weigh various risks and make our own decisions.
Fine. Good luck. But I’m not sorry I wasted the time responding to you, because maybe someone else will benefit from it.
And it doesn’t sound like you’re making a decision; it sounds like you’re afraid of vaccines and found a doctor who will second you in it.
Good luck. My immune system isn’t strong enough for me not to depend upon vaccines, whatever their short term side effects. Maybe your immune system is stronger.
Cameron, I won’t respond to you again. You try to demean me by saying I chose a doctor to agree with me because I’m “scared of vaccines.” Not true. He advised me to take all the Covid shots, because for me, Covid would be a worse risk than a vaccine reaction. I took them. He advised me not to take the shingles or flu vaccines because of genetic testing he did. A reaction to those vaccines isn’t worth the risk to me, in his opinion. He is a specialist, an expert, noted in his field. I wouldn’t do everything and anything he told me. I weigh any doctor’s advice. But I agreed with his analysis. You, Cameron, are a jerk. Please don’t interact with me any more.
Thank you Cameron you have helped me. I am Scheduled to get my first Shingrex shot tomorrow. I watched my mother in terrible excruciating pain with shingles! I have been diagnosed with chronic fatigue and fibromyalgia for almost thirty years now and I am nervous but I believe In Vaccines. Better safe than sorry…
Cort, be carefull ‘ promoting’ vaccine for every illness. Vaccine is not the answer for ME/CFS/POTS/FM/LC. I knoe some old people with shingles. It i s common. Vaccine is not a solution.
Really Gijs – I am being careful. I’m looking at the reports and studies – are you? Thus far the polls indicate that people are doing pretty well with the vaccines.
Don’t fall into the trap of publication bias Cort. I am familiar with statistics, science and publications. The positive effects are (almost) always overstated. Independent research makes something more credible (Karl Popper).
Speaking about vaccinations: wasn’t it omikron that got us out of the pandemic? And wasn’t it hygiene that prevented many infectious diseases? There are so many factors that play a role in infectious diseases. Vaccinations partly help with certain infections, but certainly not with all. Anyway, we can have a whole debate about this. I think we’re both right.
We both have our points, for sure 🙂
I received the shingles and flu vaccinations on September 4th 2013 after I had a severe respiratory infection in August. In about two weeks I couldn’t walk, autonomic dysfunction, multiple muscle myopathies, cerebral ataxia, spascity, chronic fatigue, PEM,.. etc . I started my journey with a neuro-ontologist who referred me to a movement disorders neurologist. She blew my diagnosis of Guillian Barre due to the fact I had retained hyperflexic reflexes. This caused me to miss the GBS treatments that could have shortened the severity and duration of my GBS. I presented like 2% of the patient population versus the standard presentation. Even the largest medical complex in the world can blow it. I am now 10 years post and still struggle with most issues but have learned to cope and accept. This was the day my life changed forever.
I have had shingles twice and had chronic herpes simplex my entire life. I had a standing order for acyclovir but since my GBS I have not had a single outbreak. Cure for herpes wrapped in here somewhere perhaps?
I’ve taken every vaccination offered as what more damage could be done?
I had shingles when I was 9! The doctors misdiagnosed it because I was so young. I think this was one more characteristic of my messed up immune system — going on to have an autoimmune blood disorder, then a CFS diagnosis that changed to a fibromyalgia diagnosis. I have wanted to get the shingles vaccine since it became available but insurance won’t pay for it if you are under 50 is what I was told. I encourage everyone to get it because shingles is terrible.
After the covid vaccine propaganda, ‘trust the science’ campaign and then the revelation of the ACTUAL data from the Pfizer documents that eventually got released, I will never, ever trust vaccine efficacy statistics again. All trust lost unfortunately. Unless I can see independent assessment of the raw data, I’m always going to assume a distortion of facts to sell more product. Anyone with their eyes open knows this is going on.
It is much worse. “The vast majority of drugs – more than 90 per cent – only work in 30 or 50 per cent of the people,”(…)
https://www.independent.co.uk/news/science/glaxo-chief-our-drugs-do-not-work-on-most-patients-5508670.html
A sobering fact for sure. The body is very complex and they believe that genetic factors are getting in the way. Still they do work in 30-50% of people and I’m sure those people are grateful to get some relief.
I guess my eyes aren’t open but I’m going to go with the massive drops in cases and hospitalizations from shingles since the vaccines were introduced. it’s a terrible disease if you get it.
I had the Shingrix vaccine shortly after it came out in Canada, so pre-Covid. I got it primarily because a friend had Shingles and I was shocked at how debilitating it was for her. She has permanent eye damage. It was not free, and I’d been waffling over the cost until that happened. I did not know it only lasts 7 years, so I probably will have to consider getting it again in the near future. So I answered “Probably” in the poll. Since I had no other health concerns at the time of the first vaccination, my answers to the poll may skew your results a little bit. I possibly had underlying MECFS that I was unaware of and coincidentally (?) I had a short episode—2months—of recurring MECFS-like symptoms several months after the Shingrix vaccination. I did not connect the two events, and they may well be unconnected.
Like you, I had to watch a family member – my mother in law – go through shingles, however, her case was milder than your grandmother’s and she could function after a few weeks, but she never again was completely pain free.
My husband and I got the Shingrix vaccine last December, when our granddaughter was born. I am 63, and have ME/FM diagnoses, among other things. I also had a severe case of chicken pox at age 35. I definitely didn’t want a repeat of something along that line or even worse. My husband does not have ME or FM. He had almost no reaction. I felt mildly fluey with a fever of 100 to 101 for a couple of days, which I expected, as that’s what happens every time I get a Covid vaccine.
I can tell you I’d much rather give up a couple of days feeling fluey than go through what my mother in law did. Every individual is different obviously, but the research was promising enough, with enough time to get a longitudinal feel for reactions, that we definitely went for it. Thanks for the article. It validated my choices in my mind.
I have had facial/scalp shingles twice, both times under age 55. Right above my eye with close monitoring and warnings about losing sight. Severe pain, did not want it again. Diagnosed with a primary immune disorder at age 60. Now the shingles part makes sense. Immunologist highly recommended Shingrix, first dose in February, but she says wait until nearer 6 months for second dose as your immune system will respond more fully than the two month or so interval. Very sore arm, aches and pains for about 3 days. Also had the older shingles vax. With FM and a primary immune disorder, COVID shots x5. And to this point, zero covid. I believe in vaccinations.
I have multiple genetic-based autoimmune conditions, plus a history of both EBV and CMV infections (in addition to chickenpox, and both HSV1 and HSV2). I had no problems with the Zostavax vaccine, but a severe reaction to the first Shingrix shot (5 days totally incapacitated, with flu-like symptoms) – so I never got the second shot. I also had very pronounced, multi-symptom, weeks-long reactions to the mRNA covid vaccines, including very mild shingles, and I believe reactivation of either the EBV or CMV (or maybe both?) I have not had bad reactions to any other vaccines – always get my flu shot every fall, and have kept up with all “normal” vaccines, plus those recommended to various international trips. But I won’t consider EVER getting that second Shingrix shot!
Just about cleared from Shingles i developed a Month or so back.
This was triggered probably by Covid (Brother and nephew 2 houses down both tested positive and i was around there a lot) .I didnt test for it because my Covid was so mild and tbh ,hard to discern from a CFS flare up ,and only real symptom was a slightly phlegmy throat
Singles around the throat back of the head on the other hand was nasty. 4-6 Panadol a day for the pain and the Antiviral for 10 days hits pretty hard too
after a month i can finally shave my face /head again,thankfully
I had intended to get the Shingles vaccine when it was offered ,but there was a 6 month or 1 year stand down period after Covid /Covid Vaccinne , and forgot about it lol blame the brain fogs
The couple days minor flare up from a Shingles Vax seems well worth it ,compared to a Month plus of Shingles
Brother also got Shingles from Covid the year before ,which is when we learned about the Shingles Vax
This study is interesting too.
Covid-19 vaccination can induce multiple sclerosis via cross-reactive CD4+ T cells recognizing SARS-CoV-2 spike protein and myelin peptides
Qiu, Y.; Batruch, M.; Naghavian, R.; Jelcic, I.; Vlad, B.; Hilty, M.; Ineichen, B.; Wang, J.; Sospedra, M.; Martin, R..
Multiple Sclerosis Journal ; 28(3 Supplement):776, 2022.
Article in English | EMBASE | ID: covidwho-2138820
https://pesquisa.bvsalud.org/global-literature-on-novel-coronavirus-2019-ncov/resource/pt/covidwho-2138820?lang=en
I wonder Gijs if you’re applying your same skepticism to vaccine studies to results that you agree with?
This has been all over social media apparently. This is what the AP has to say:
CLAIM: The World Health Organization admitted that COVID-19 vaccines can lead to multiple sclerosis.
AP’S ASSESSMENT: False. A database on the WHO website includes an abstract for a conference presentation about research that examined two recent cases of MS. The research found there might be a potential link to COVID vaccines, but did not definitively conclude the shots triggered the neurological disease, according to the global health agency and multiple sclerosis experts. They stress the research, which is not a peer-reviewed study, is limited and more extensive studies would be needed to determine what role, if any, the inoculation plays in the onset of the disease.
I imagine we’ll learn if the rate of MS has skyrocketed over the past couple of years at some point.
The interesting thing about this study is (I assume you’ve read it) the immune system that after vaccination with the covid-19 vaccine can leads to an autoimmune response. This can also happen after an infection with covid-19. And no, on the basis of this study you cannot draw definitive conclusions. I don’t think I am writing that either.
The numbers of cardiovascular problems have increased in recent years. I don’t know the number of MS cases. Time wil tell.
I have to take acyclovir and Valtrex daily due to constant outbreaks. I also get IVIG infusions for low IGG. My Hematologist says that I don’t need the vaccine as long as I am on the daily anti-virals. My husband got the vaccine and said it hurt like crazy both times and he had a few days down (he’s “normal”) but if my Dr said to get it, I would. My father-in-law had shingles along the trigeminal nerve and lost most of his sight in one eye. It was horrible. Everyone has to make their own choices. Personally having ME/CFS has been a real struggle and I just try to follow the science. If my body reacts differently than someone else’s, then it does. I will deal with it one day at a time.
The fact that I have taken several antivirals for lengthy periods of time to treat HHV-6 and CFS in general, does that make it less likely to get shingles because I understand antivirals are the treatment for shingles?
I was very interested to see the results of the poll stating 32%/33% of people had no/mild symptoms after the second Shingrix vaxx and 65% of Zosta vaxx. Everyone I have mentioned it to or has told me they got the vaxx (healthy people) said it was the worst vaxx they ever had. Even Drs have said their patients usually are pretty sick for several days. I’d be curious to see if Drs have noticed reduced reactions, in general, to vaccines among people with ME/CSF, Fibro, etc as compared to healthy people. From my own fluctuating health during Covid it seemed that my reaction to Covid/Shingrix varied by my overall health at the time. Feeling better=worse reaction, feeling worse= less reaction. Seems to be an immune system component there somewhere?
It’s been years since I had these vaccines. Thanks to age and CFS, my memory is awful. Soif the shingles vaccinations were horrible, I’ve forgotten. That may be influencing the responses.
I’m wondering the same thing. Been on and off Valcyclovir for years for the HSV2 and have ME/CFS.
My comment was supposed to be in response to Barbara Berkeley.
I’m 74. I had both types of shingles vaccines as soon as they were available – I’ve known many people who had shingles. That’s one I’d like to skip. I have had ME/CFS for 7+ years. The first year was bad, I lived in my recliner. After that, it has moderated. I don’t do very much but I usually can live a semi-normal life. I have groceries delivered and someone cleans my house weekly.
I’m lucky that I can afford to have help, because if I try to do much, I relapse. I tried mild PT but realized I spent the days between appointments recovering from relapses. PEM is a big problem for me. I have occasionally had side effects with Covid vaccinations, but I don’t remember the shingles vaccines as being too awful. I know shingles would be disastrous for my health, as would long Covid. So far, as far as I know, I haven’t had Covid.
Have never had chicken pox, was diagnosed with ME/CFS three years ago at age 61.
Not getting the shingles vaccine and will take my chances.
The first Covid vaccine really knocked me flat, and I have not fully recovered. It took my ME/CFS from moderate to severe. Because I live in a senior’s residence, I did continue getting boosters until I’d had 4 shots, but then I decided, since I still hadn’t fully recovered, that I would wait before getting others.
With such a reaction to my first (Astra-Zenica) Covid shot, do you think it would be advisable to get Shingrex?
Just to say, this is a question I’ve been struggling with. I don’t want to get shingles, but I don’t want to decline any further.
Is there any data on whether a person who had such a reaction to A-Z might have a similar reaction to Shingrex?
Thank you so much for this blog! You have done such a good service to a community of patients vulnerable to opportunistic illnesses such as shingles. Bravo!
Thanks!
I had only a mild sore arm and a day of fatigue after the Shingrix shingles shots. So glad I got them, as I’d already had one horrible shingles attack and don’t want to risk post-herpetic neuralgia.
A recent study suggests shingles vaccines may slash dementia risk by 20%. A decreased dementia risk seems especially important for us, since we’re already dealing with brain fog. https://www.medrxiv.org/content/10.1101/2023.05.23.23290253v1
That’s good news! I had no idea – thanks for passing that on 🙂
Excellent article, as always Cort!
My son (who also has ME/CFS) got shingles as a teen, and while it is horrible, Valtrex was VERY effective and worked pretty quickly. I’m always dismayed to hear of people suffering for long periods with shingles (like your grandma) when there are multiple antivirals that work. It seems that outside of the ME/CFS world, they are not routinely prescribed.
We were careful with vaccines for our son, but he tolerated the COVID vaccines and a pre-college meningitis vax very well.
I wasn’t so lucky and became much worse for 6 months after my initial COVID vaccines, with my immune system clearly staying in over-active mode – and only finally got back to baseline thanks to Dr. Levine and my own determination to keep trying treatments. So, I’m much more cautious about vaccines.
Thanks for laying out the benefits and risks so clearly. I agree with Dr. Levine’s statement that it’s an individual decision. My son and I seem very similar in our ME/CFS symptoms and course of the disease but have very different responses to vaccines.
Sue Jackson
Live with ME/CFS
Interesting to hear your son’s experience. However, neither Valtrex nor aciclovir seemed to help with my dreadful case of shingles.
Sorry to hear that – it is a dreadful infection!
I’m usually fine with vaccines – eg., two weeks below ME/CFS baseline with most covid vaxes (Az, Pf, Mod), nothing with Novavax, and nothing with yearly flu shots especially after starting MCAS meds.
But the first Shingrix shot (age mid-50s) sent me into a serious decline in baseline. I went from nearly moderate back to 50% severe. I had to add aspirin (was already on apixaban) to stop the decline. After 6 months, I wasn’t back to baseline before the shot, although I’m slowly improving.
Possibly relevant is that I had zero evidence of ever having had chicken pox – my parents said I never (apparently) had chicken pox, I didn’t catch it when my sibling had it (or at least had no symptoms), and have never shown positive IgG for it when tested in 40s & 50s.
I first had shingles on my lower back in my 30s (around 1993). It was mild, I got anti-virals in time, and it went away in about 10 days. I got the first shingles vaccine when it came out not long after I had shingles. When Shingrix came out, I got it, too. All of that was before I developed CFS in 2018. In 2019 or 2020, I got my second case of shingles that spread rapidly from my shoulder to the back of my neck, up into my hair, down my shoulder blade, and down my arm. It was horrible! The burning, pain, itching was intense. I got anti-virals, and something to address the nerve pain (thanks brain fog. I can’t remember what it was.) It was much slower to heal, but fortunately, no post-herpetic neuralgia after several weeks. I shudder to think it could have been worse if I hadn’t had the vaccine.
I got shingles last year on my cheek and inside my mouth. Fortunately, I got on Valtrex within 72 hrs so they weren’t near as bad as they could’ve been. I do have some minor nerve sensitivity in my teeth now – nothing unbearable though.
I’m taking a daily low dose (50 mg) Valtrex to prevent both recurring herpes simplex and shingles and plan to take it for life.
I’m 72 and have had ME/CFS for 37 yrs.
I was hoping the survey would include a response option for “Shingrix improved my baseline”! Or even, “Shingrix improved my baseline ENORMOUSLY!”
As I have mentioned on here before, the first dose of Shingrix took me from bedbound 23 hours a day to walking around the flat, reaching up to high cabinets without pain, and the whole remission experience of brighter colors, euphoria and energy! It was similar to my amazing experience with the Moderna booster, but even better.
I got my second just two months later, with mpox in the middle, which took me down some, but my baseline is still MUCH higher. I’ve been back out live-drawing events, with relief from the pain in my hands and arms that was crippling me.
Once I responded to the Shingrix, I thought, maybe I’m in the herpesvirus cohort, and I started taking 400mg of Valtrex a day. I’ve been taking it since, except for short breaks around vaccinations. I plan to drop down to 100-200 at the six month mark.
Meanwhile, we got our first Novavax dose yesterday. I think the Pfizer bivalent booster last fall lowered my baseline, and I want no more MRNA for now. We hope to get four Novavax ultimately.
I’m also going to get my MMR and polio renewed, and try to get BCG as well. Hoping to get as many antibodies as I can before I inevitably do get Covid and it eats my immune system!
Obviously, my experience is just one person’s, and I believe very strongly that we know our bodies and have a sense of what is best for us. If someone feels that something won’t help them or isn’t safe for them, I’m not here to argue.
My husband has Shingles at the moment. He is 53. Diagnosed by a nurse who sent photo of swellings and rash behind his ear and back of his head. Day before, his GP had prescribed him cream for dry skin. Not happy with that, we visited Minor Injuries Clinic who diagnosed Shingles. He started on antivirals straightaway then next day, antibiotics as some blisters looked infected. He has been in lots of pain – skin on his head, his ear. Rash spread down his jawline. He has had ME/CFS for three years; sleeps 17 hours a day; severe depression. He had Hodgkins Lymphoma in 2004; 7 months of chemo. A year later, he developed RRP, which causes HPV growths on his vocal chords – he’s had 17 operations to date. Should I ask his GP for the Shingrix vaccine when his Shingles rash has disappeared or will it makes things worse for him. He had two Covid vaccines and Covid and it made all his symptoms worse; he has never recovered from this, I believe. Definitely realise his ME/CFS is virus-related – I think he has had a compromised immune system since birth – emergency caesarian as his mother had activated hpv (this is just my theory) she had emergency hysterectomy years later from this. I’ve known him 30 years, he’s had just a handful of colds in that time; Hodgkins out of the blue at 34. Is there any safe way to reduce his viral load and improve his quality of life. We have zero support from doctors (we are in the UK). He says he can’t carry on much longer.
Unfortunately no one knows how he will react to the Shingrix vaxx. (Make sure that is the one he gets!) Since he’s had shingles you’d think he would no have a huge reaction but it’s worth getting because people die from Shingles and it’s horrible when you have it. I’ve had CFS for 5+ years and have gone from mostly chair bound to functionally active 4-6 hours a day. I did it all with herbs and supplements. I keep my herpes viruses suppressed with cystus incanus tea, oregano oil, and lomatium glycerite as wellas the herbs included on this website: https://www.healthline.com/nutrition/antiviral-herbs. It’s really, really important to either find a Naturopathic DR or do a lot of research before using any supplements or herbs to make sure they are used correctly and have no interactions with any other meds or afflictions you might have! We are making good progress and finding the cause and hopefully cure for these issues so please tell your husband to hang in there!
Thank you so much for taking the time to reply. When he was diagnosed in 2020, I changed his diet to Paleo, bought numerous supplements (via Dr Myhill). Rather than improve his symptoms, it made him worse. He also tried acupuncture, again, made things worse. I know sometimes you can get die-off reactions and things might have to get worse before they get better but he is now reluctant to try anything. I do think that he is so weak and possibly has toxic overload, that his body can’t use these supplements? I bought AHCC last year but I’m too scared to ask him to take it! Years ago, for his RRP, I found the RRP association in USA that was using ART therapy (Arsunate and Artemisinin). He used this for three years and his HPV went into remission. It did have the side effect of fatigue (before he had ME/CFS). He stopped when we adopted two children. I am wondering if he should try this again.
Thank you once again.
That’s good to hear bout the ART! If it helped before it “should” help again but in his severely weakened state it would be difficult. I hope you can get lab work done because you’d definitely want to check his liver/kidney function for any adverse reactions, although it has been shown to be safe. The new recomendation from a DR I trust. ” Artemisinin 100 mg is an herbal medication. Start at 2 or 3 pills 2 times a day for 3 days on the medication, then take 11 days off. Continue this 14-day cycle. The goal is to reach 5 pills 3 times a day on the 3 days the medication is taken. I use artemisinin this way to overcome resistance. Be aware, the dose on the 3 days is quite strong. Often it causes a worsening of symptoms beginning on the second day and sometimes lasting until six days later. If a person is very medicine sensitive, I start at 1 or 2 pills 3 times a day.” Obviously you’s want to start at a much, much lower dosage and only give like 25mg and then wait until day 3 to give another 25mg if he feels ok. Then give the 25 mg on day 2 and wait until day 4 or 5 or longer if he doesn’t feel well from it. better to go very very low and slow than to make him sicker. You might never make it to the full dose but that’s ok, it’s still helping! Good luck and many prayers.
I have been unable to put full pressure on my right foot since shingrix 2 shot. I have peripheral neuropathy from that shot, which I never had before. I have Mast Cell Activation and CFIDS/ME since graduate school in Boston. That was thirty years ago. I felt worse from the Shingrix vaccine (part 2) than I did with active Covid.