



![]()
Intro: As I’m writing this it’s already Sept and I’m on another road trip to see Dr. Peterson. Four months have gone by since the visit you are to read about below. In the interim it’s been a whirlwind – no, a tornado! – of medical activity since my last visit in May…
My treatment regimen had remained the same over the past 10 months
- IVIG (Gamunex-10%, bi-monthly)
- IV normal saline (2-3 liters/wk), IV amino acids (Aminosyn 8.5%, 2-3x’s/month)
- Valtrex (500 mg BID)
- Procrit injection (4,000 units, bi-monthly)
- Aleve (as needed for head pain)
- Meclizine (as needed for dizziness)
You can read about my previous visit here.
To summarize briefly, it centered around the fact a cervical spine MRI done in response to new neurological symptoms including an electric shock sensation down my legs when I bent my head forward, revealed an inflammatory lesion on my spinal cord. I was rushed into a second lumbar puncture but neither it nor numerous scans or laboratory tests revealed a definitive cause.
Back home I visited a neurologist in March who ruled out MS but believed I had an autoimmune disease called Neuromyelitis Optica (NMO) which he failed to inform me, can result in paraplegia and/or blindness. (I accidentally became aware of the seriousness of this illness when my nurse practitioner, during a routine exam, asked how I was getting along given my horrible diagnosis!) Sadly, he offered no further consultations, referrals or treatment options, except IV steroids which his nurse later told me ‘could kill me’. He did suggest that I remain on IVIG as that was sometimes used to treat NMO. He then sent me home simply saying “go home and research it’.
Although the blood and spinal fluid tests for NMO returned negative the neurologist stuck by his diagnosis, saying the IVIG I was taking could have masked the antibodies.
Not having a plan and not believing that I had NMO, but still in a bit of a panic, Dr. Peterson would come to the rescue, telling me to return to see him for more testing. So back I went in May for my 10th visit.
Pre-trip
“It’s amazing how you seem to pull people out of the hat when you need a ride on these long trips to see the doctor” my friend Val said to me the other day. A magic trick? Nope. I call it Divine Intervention. I just put the word out and people voluntarily appear. Angels, I call them.
This time my ‘winged’ helper is my good buddy Cort. He’s living in Denver but needs to drive to Las Vegas to get some stuff out of storage – so what’s a slight detour to Arizona and then to Lake Tahoe?
Day One (Sat ) and Day Two (Sun)
Rather than drive his truck which is not exactly comfortable, especially for someone exhibiting my symptoms (numbness, pressure and pain in my butt and legs) we take my car. The big plus is that it gets very good mileage; the big drawback is that it was recently purchased from a dealer who apparently ran the upholstery through a dry cleaners! The odor is tolerable for me, but Cort is having a tougher time. He soon realizes that the only way he’ll survive the trip is to leave the windows open the majority of the time. So, off we go, hair-a-flying, one passenger fighting nausea, the other sitting on a piece foam….Just another typical scenario for two ME/CFS patients
Even with the occasional issues, the two-day drive seems to fly by due to the good company of friends who can’t seem to shut their traps. Each day – 6 1/2 hours of driving – is filled with tons of laughs and an abundance of therapy. We thankfully arrive safely on Sunday afternoon.
Day Three (Monday)
My appointment is @ 8:15. Dr. P. orders the usual blood work and more MRI’s. (MRI’s have unfortunately become an expected addition.) He assures me that he’s relatively confident that I don’t have the dreaded NMO, multiple sclerosis or a malignancy, but he needs to get better scans of the lesion. Since the first one was done without contrast, he said I needed to repeat it, and do my brain and c-spine with and without contrast – ASAP.
With the usual juggling act, the diagnostic center in Reno was able to fit me in today – at 6:30 pm! Hey, did anyone tell them I usually call it a day by 5pm? Oh my. These visits are never easy.
After they draw enough blood to fill many vials at Labcorp next door to Dr. P’s office, I head upstairs for IV’s of amino acids and then saline – a ‘pick-me-up’ to help cope with the drastic changes in my usual schedule. Cort, meanwhile, after chatting with patients and Dr. P’s research assistant, Gunnar, heads out to Starbucks, where he can go online and get some work done.
When my infusions are done we grab a couple of burritos and head back to the hotel where I can spend a few hours resting up for my evening appointment. I savor my burrito as it will most likely be my last meal of the day as I am told not to eat two hours prior to the scan. Missing a meal is nothing new for these visits as the days are usually too hectic to give much of an opportunity to eat.
Leaving by 5:00 gives us plenty of time to take into account the Reno rush hour traffic and the fact that it’s raining. Cort’s GPS with the irritating voice that by now, after two days on the road, has gotten on my nerves, has me yelling obscenities at it. It does, however, manage to get us there easily enough. Unfortunately neither of us has a clue what is to come.
After checking in and preparing to lie in the machine, the tech says “You know you’re going to be in here awhile”. Realizing it’s beyond my control and assuming I’m better off in a state of denial I blurt out, “Don’t tell me how long. I’m ready, so let’s go”. Little did I know that two hours later at 8:30 pm, I would finally emerge from the MRI tube! A two hour MRI – definitely a record for me!
Although two (technically four) scans take time to complete, this one was lengthened by the fact that the last set of images, which the voice in my ear said would ‘take 10 minutes’, ends up taking 30 due to ‘problems’ on the other side of the glass window where the tech sits.
Understandably, I am getting a bit cranky, so when she finishes and enters the room advising me to hurry up because “there are people out there waiting and they are upset this has taken so long”, I lose it!
Regardless of her request, I cannot rush to get up as I get dizzy doing so. Taking my time, I apologize under my breath to the poor people in the waiting room.
By now it’s past my bedtime and I’m exhausted. Dressing is an effort and the short walk to the front door to meet my ride seems like a marathon. This is when it hits me- it’s dark outside!
My internal clock feels confused as I’m usually in bed when its nighttime. And, to top it off, it’s raining cats and dogs.
As we accelerate onto I-80 heading back to the hotel, neither Cort nor I can see the lines on the road. Cort doesn’t like to drive at night on the highway and he really doesn’t like to drive at night when it’s pouring. The reflection from the oncoming headlights through the rain is disconcerting and the lane dividers are difficult to distinguish. We slow down to about 35 mph and pull into the right hand lane where we’re routinely passed by cars zipping by. It’s another white-knuckle ride in Lake Tahoe (our adventure last March involved a snowstorm with no chains), but thankfully we arrive safely.
It’s 10pm before I settle in. It seems strange as I haven’t seen 10pm from any other perspective other than my bed in many years. To think I was a Disco Queen in my former life who could dance the night away. Seems like eons ago.
Day #4 (Tues)
With an 11:00 AM appt. scheduled I’m able to sleep in, but because I’m virtually starving, I’m stuffing my face at breakfast before 8 am. My neurological symptoms are acting up today. My legs feel stiff and constricted. The jabbing pain in my left mid-back is more intense. Cort drops me off at the office on his way to Starbucks.
While in the waiting area I whine to a fellow patient about my two hour MRI and am soon feeling wimpy for complaining as she tells me about the three hour scan she once endured. If I’d been given a ‘badge of courage’ for my adventure last night, I’d have immediately pinned it on her.
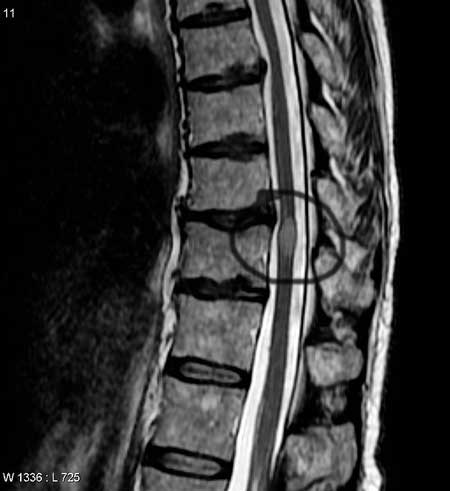
Transverse myelitis refers to a lesion or wound on the spinal cord. In this MRI the lesion appears to be in the black circle (that I drew in).
Once in the exam room Dr. P. enters already in mid-sentence, and I catch “MRI is back”. Already? The man truly has some influence with the radiologist. IN his hand is a stapled group of papers that appear to be a copy of an article printed off the computer. He lies it on the counter as he starts checking off numerous tests on his lab requisition pad.
Finally handing the article to me he explains that according the radiologist I probably don’t have NMO, but I might have ‘this’ instead. He suggests I read the paragraph on etiology.
The article is titled Transverse Myelitis and it lists causes such as infections caused by a list of viruses we are already so familiar with, including herpes simplex virus (HSV), Epstein-Barr virus (EBV), varicella-zoster, enteroviruses, etc., etc. I ask him if cytokines could cause this and he immediately exclaims, “Yes!”
“I want you to get another MRI (!)”
“What? After that marathon last night?”
“Oh, don’t worry, this one will be quick” (Relatively speaking, I imagine.)
He wants me to have one, with and without contrast, of the thoracic cord/spine. I totally agree since I do have a terrible pain in my mid-back.
Then Dr. P sits and meets me eye-to-eye. “Don’t take this wrong”, he says (I’m a bit leery of what’s coming next.) He proceeds to explain “So many patients show nothing visible. At least you have something concrete.” (Oh, lucky me!). With that ‘glass half-full’ comment he sends me to Labcorp to donate blood, yet again, and insists that I stop in to see Gunnar afterwards.
Transverse myelitis (TM) – refers to inflammation across the width of the spinal cord. A serious disorder, TM has been associated with numerous viral and bacterial infections including many herpesviruses and Borrelia as well as spinal cord injuries, immune activation, multiple sclerosis and reduced blood flows. One major theory proposes immune activation in response to a virus or bacteria damages the spinal cord. Because TM can co-occur with Sjogren’s Syndrome, lupus, multiple sclerosis and sarcoidosis, an autoimmune component may be present in some patients.
TM can herald further demyelinating episodes elsewhere, and the Mayo Clinic urges all patients to be assessed for multiple sclerosis and neuromyelitis optica. (Corinne’s brain scans and lab tests do not suggest she has multiple sclerosis.)
In transverse myelitis normal spinal cord functioning is lost typically causing weakness, abnormal sensations in the legs and feet and sometimes progressing to loss of bladder function and paralysis. Many people with TM experience allodynia. Acute cases of TM tend to progress rapidly and have devastating outcomes. Corrine’s onset, however, was gradual and the lesion appears to be stable at this point.
Most people who have transverse myelitis will only have one episode of it. Some recover completely and others will remain disabled.
The Mayo Clinic and other sources stress infectious causes, but suggest only corticosteroids as treatment.
I oblige. My conversation with Gunnar is quick. He tells me to prepare for the CDC study questionnaire Pt. II which will be coming my way soon. He promises that it is long – but not as long as Pt. I (last year), and can be answered on paper. (He’s aware I have problems using the computer because of dizziness.)
Out of curiosity I ask him if he knows if Dr. Lipkin has my cerebrospinal fluid for the pathogen study. “Yes, definitely”, he answers. Silently I’m wondering if Lipkin has both the 2009 and 2013 samples. I’m concerned that neither may represent what is now occurring in my central nervous system. The 2009 lumbar puncture was done pre-lesion (as far as we know)and the 2013 one may have been affected by the IVIG I was on.
In fact I wonder about the IVIG. Since the lesion seems to have progressed all the while I was on it, I guess I can assume that it was not obscuring anything or perhaps, as Dr. P suggests, whatever set off the ‘attack’ on my spinal cord could have been even worse had I not been on IVIG (?).
After our chat, ‘my driver’ (:)) picks me up and I tell him the news. It’s nice to have Cort to discuss this with. The article on transverse myelitis says the treatment is often IV steroids, but knowing my history of immune dysfunction and viral reactivation Dr. P said he would not want to give me steroids. It isn’t long before my gut tells me there is not going to be a quick fix nor an easy answer for this dilemma.
My MRI is scheduled for 2:20 so we head out on the winding highway over the mountain. As usual I pre-pop a tablet of meclizine to help prevent motion sickness. Thankfully, it’s not raining.
The MRI only takes 40 minutes – a piece of cake! As we drive back to the hotel Cort scolds me for missing another meal. (Oops! I missed lunch again.) This ongoing theme of missing meals continues. Cort never passes on the opportunity to encourage me to put on a few pounds and this time he’s not buying my excuse that I’m too exhausted to eat. I realize in order to maintain my strength he’s probably right but it’s 5:30 and that’s my bedtime, and having to weigh food vs rest, rest is going to win out today.
Back at the hotel I’m amazed that it’s only Tuesday. It feels like I’ve been here for two weeks rather than two days! Luckily I have nothing planned for a couple of days as Dr. P will be out of town. I’m grateful for the time to catch up on some needed rest.
Day #5 Wednesday
I REST…then struggle to shower and wash my hair. That’s all I can manage for today.
Cort gets a haircut and has lunch with Annette Whittemore.
Day #6 Thursday
I REST, some more.
Looking out the window the thought enters my head that it’s a real bummer to be in such a beautiful place like Lake Tahoe and not be able to hike and enjoy the outdoors and the fresh mountain air. Had this been the pre-illness me, I’d have been lacing up my hiking boots or straddling my mountain bike for a ride with my husband on a long forest road. But the reality today is that I’m limited to experiencing nature through a hotel window.
Day #7 Friday
My appointment is at 7 a.m. and we must get a very early start as Dr. P has agreed to chat with Cort and I. The earlier the better, as we are heading home today.
The news on my T-spine MRI is good. The spinal cord appears normal so apparently the pain/pressure in my mid-back is from the inflammation on the cervical section. The only lesion on my spine and brain (other than those unidentified bright spots on the brain so many of us have) is on my posterior neck region.
Dr. P informs me that he will refer me to a neurologist at the Univ. of California San Francisco who specializes in myelitis (inflammation of the spinal cord). Knowing my history with neurologists, he adds that he’ll consult with him first to “‘feel him out and see if he’s interested” and stating “I wouldn’t want you to spend the money and energy to make that trip for nothing”. He then encourages me, “I work with these guys so they can’t ignore CFS” (but somehow I don’t entirely believe him).
He suggests that I skip a dose or two of IVIG in case the neurologist wants me off it for further testing. He would not want anything masked. “In fact”, he adds, “it may be best if you’re at your worst when you see him.”
“Oh boy, I can’t wait” I mutter, sarcastically.
Sensing that this must be a bit overwhelming, he tries to encourage me with his version of a ‘pep talk’. “You’re an index patient. This is important. You and Cort need to mention this in your blogs.” He continues to stress the importance of being an index patient without really explaining what one is. Content with the fact that it sounds good to me, I don’t question him, assuming that at some point I’ll become aware of what this title means.

Being an index patient – someone who may illuminate ME/CFS for others – was not exactly Corinne’s goal
At the same time, if running off to see specialists in another state and taking test after test, including 2-hour MRIs, is a prerequisite for ‘index patient status’, I think I might just prefer the title previously pinned on me -“The Queen of Questions”.
[The Index Patient – An Index patient appears to be a patient who follows Dr. Peterson’s protocols, is willing to do the testing he requests and participate in studies. A patient he believes is ahead in timeline and illness progression, manifesting symptoms that could be the consequence of long-term illness (a ‘canary in the coal mine’, per se) and so may be representative of other patients, and thus may hold the key to others health. The index patient’s willingness to follow Dr. Peterson’s protocols means he has a good idea of both how effective they are, and how they’re changing that patient’s physiology. Dr. Peterson has asked Corinne to participate in every possible study associated with him and she has. ]Speaking of questions we end the session with a mere handful as my labs have not returned. As in my last appointment, since we still haven’t figured out what’s causing the lesion (viral, autoimmune, malignancy, others) covering all the hypothetical’s is a waste of everyone’s time.
I do, however, get clear on a few issues, such as the affirmation to continue my treatment protocol EXCEPT for the IVIG, and the sad fact that there’s really nothing I can take to manage my new and uncomfortable symptoms. This concerns me since Dr. Peterson has referred to my condition as ‘progressive’, due to the fact that even though the repeat MRI (3 month) did not show an increase in size nor inflammation of the lesion, the symptoms themselves have worsened.
Dr. P tends to wear his emotions on his sleeves and over time I have become better adept at interpreting them. If I am right, I’m looking at:
- a man whose body language says he is concerned – concerned in a caring way
- a doctor who is a bit perplexed but interested and curious – intrigued in some ways by the challenge of figuring this out and perhaps…
- a career-long CFS expert who is excited at the possibility that perhaps, somehow, solving this mystery may expose the long sought-out connection between neuro-immune/neuro-inflammatory disease and CFS.
One of my deepest concerns as I exit his office is that he doesn’t become so stumped that he disengages and considers dropping me as a patient, or passes me off to someone else. As we all know, it wouldn’t be the first time a physician has done that to us. I pray that this doctor, who took up the fight for CFS patients 30 years ago – even when ostracized by his peers – will continue to battle for me.
Day #8 (SAT) and Day #9 (SUN)
As Cort and I head home we decide to take the scenic route along the Sierra Nevada mountain range in California. We take time to ‘stop and smell the roses’, detouring to view a few of the breathtaking lakes and vistas along the way, while snapping some photos. (We manage to do this in-between the periodic ‘cat-naps’ Cort must take :)). We both enjoy the scenery and the grandeur of Mother Nature.
For me this is cathartic as it takes my mind off my latest health crisis and, for the time being, prevents me from worrying about how in the world I’m going to make it to San Francisco. Angels…are you listening?
LABS:
(You can check out my last blog for the results of the labs from my lumbar puncture in February.)
May 2013 results:
Blood (serum/plasma):
- Elevated or positive: Coxsackie A and B-3 IgG/IgM (antibodies), EBV (EA/VCA/NA) titers, Herpes Simplex (HSV) 1 & 2 antibodies, CMV IgG (antibodies), ANA, Sjogrens SS-A & SS-B antibodies. CD4/CD8 ratio.
- Subnormal: CD3 & CD8 suppressor cells, WBC (lymphocytes low, mono and neutrophils, high). Also IgG subclass 3, and NK cell function (LU 10).
- Negative: varicella–zoster, HIV, HTLV I & II, RPR. Also toxoplasmosis, anti-sarcolemma, anti-intermyofibrillar, anti-parietal cell , RNP, Smith, Actin, mitochondrial, and anti-scleroderma antibodies
CONCLUSION
The recovery time from this trip was minimal. I actually experienced a pretty decent May overall, however I did have three or four pretty bad days in early June, a month after. Though I often exhibit my PEM in a delayed fashion, I’m not sure whether this set-back was connected to the trip. I am sure, however, that being driven to Lake Tahoe was very much easier on me than going alone by plane.
While my labs, once again, revealed elevated Sjogren’s antibodies, Dr. P reported that he did not think that particular disease had caused the myelitis. I do continue to show other auto-immune markers such as a positive ANA, a high CD4/CD8 ratio as well as WBC abnormalities (which could also suggest viral issues).
This is the first time I have exhibited CMV IgG, but Dr.P said not to ‘get too excited as it’s only antibodies, not IgM’ (current infection), however I find it interesting that I had never shown them, nor the Coxsackie A& B antibodies, in the past. My continued elevated HSV also interests me as I have never had the obvious manifestation of that virus: a cold sore on the lip. Elevated EBV titers, subnormal IgG subclass 3 and low NK cell function and numbers continue as they have since we first started testing 4 years ago.
My diagnosis of myelitis (spinal cord inflammation) remains, though the ‘transverse’ part was still in question – at least until I met with the UCSF neurologist which was scheduled in June. That adventure will be the subject of my next blog J.
My symptoms continue to go through episodes of ‘flaring and calming down’. When they flare it becomes almost unbearable. The discomfort caused by the myelitis is almost impossible to explain – numb, yet at the same time, hypersensitive and painful. During these times I am reminded that I must continue to push and pursue an answer in order to get treatment for this inflammatory lesion on my spinal cord as living with such discomfort is extremely difficult. Which brings me to another subject …coping.
Coping
Spending 26+ hours in a car together leads to the discussion of multiple subjects. One that came up repeatedly was ‘coping’. Cort asked many times what my strategies were for coping with all of this since in his estimation, I seem to handle it quite well. He suggested that I share them @ some point, with you, the readers of my blog. So here goes…

A faith in a higher power, empathy and letting negative thoughts go have helped Corinne with many years of chronic illness
First and foremost, my faith is the biggest contributor to my strength. People who know me, are well aware that I believe in a Higher Power (God) and a Higher Purpose and Plan. This always helps me put my trials as well as my tribulations in perspective. But I’m human so tears, grief, sadness and hopelessness happen. So far, I have managed to keep them the exception rather than the rule.
I have bad days, but I try not to allow them to linger. I believe I am able to do this my starting each day in a state of gratitude. I do this through prayer, focusing on what I am blessed with and grateful for. For me, this sets the tone for the day.
If I feel myself getting negative, I address it and identify what is causing it, as I believe awareness is 90% of the solution. Identifying what is making me sad or depressed, allows me to proceed – move on. If it’s something I can change, I figure out what I must do to do so. If it’s something I can’t, then it may be that I just accept it and allow myself a good cleansing cry. It also helps me to talk about it, so speaking to someone who I know will be supportive and understanding helps me to emotionally ‘move on’.
For me the key is not to dwell …not to get stuck in that place of negativity, especially when it won’t solve the issue. Sometimes it may be as simple as telling myself that ‘tomorrow will be better’…and you know what? It usually is. J
Though I still have a lot to learn, I would say I have made great strides in my emotional well-being. Looking back, it is easy to see that a good portion of the first 15 years of illness was spent being angry, oftentimes at other’s reactions to my disabilities.
I once told Dr. P about an instance in which someone dear to me had said that he didn’t like the way I had handled my illness. The good doctor responded by saying, “So what. That’s his opinion. You can’t control what anyone else thinks. All that matters is what you think!” Amen to that. Friends, family, strangers…it doesn’t matter. I will take advantage of a ‘teaching moment’ when one arises, but I no longer spend my precious energy trying to force everyone to understand my suffering.
I have hopefully replaced anger with empathy. I remind myself that everyone is struggling on the rocky road of their own rough journey called life. Empathy immediately puts me in a better place, relieving me of the energy expended with anger. I finally understand that I don’t have to always prove I am ‘right’. This frees me up to laugh and smile a lot more than I used to and I consider laughter a vital component of my ability to cope.
Am I worried right now because of this most recent and serious health crisis? At times I am, but I do my best not to focus on it. So though I have some fears regarding the diagnosis (whether it differs from ME/CFS) and the treatment options (if any), my approach is not to think too far ahead. I remind myself to try and stay in the present moment, take one day at a time and allow it to play out on it’s own terms and in it’s own time (remember, I believe in a Plan). It also truly helps to know I have a great team working on my behalf. And besides, why should I worry when I always seem able to pull those helpful and caring angels out of my hat? J
‘Til next time…Be well!
‘Sometimes the Lord calms the storm; more often he lets the storm rage and calms the child.’ ~Unknown
Next…Corinne’s Visit to a neurologist in San Francisco….



 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!




Excellent blog. I admire her courage and perseverance . Just going that far by car in the first place is huge!
Thank you Corrine and Cort for sharing a snippet of your experiences. There is
no doubt in my mind that the attributes “Perseverance”, “Stamina”, and “Appreciation” come only because of your ability to see the much bigger plan.
I came away with many pieces of medical and technical information you shared, but most importantly, I gleaned a glimpse of the “Attitude” that is necessary to overcome these challenges that are all part of this temporary life. Thank you ever-so-much 🙂
Looking forward to reading more 🙂
Corrine- Excellent Blog- Have a few questions. Where do you obtain your Gamunex IVG? I know it is RX but at the present I am using GamaSTAN IM from Telecris. It is not working as well as Immune Globulin from Bayer from a few years ago. I am wondering if they make the Gamunex for IM inj.
All of my illness started out with EBV, and CMV .
Have no idea here in Atlanta who I would see for all that you were tested for.
Good luck with your progress. Going to read more about your diagnosis.
What do they rec you change or add?
Carole
.
I received the ivGamunex from an infusion center in my local hospital. a doc with hosp privileges needs to order it.
SF blog coming out soon…stay tuned. Thank you for your well wishes! Back to you.
Your use of the word perseverance means a lot to me. I don’t think anyone else realizes what it takes to do all I’ve done…only other patients. Thank you for your encouragement and validation. I may at times sound like things are a piece of cake but they usually are not…however, I don’t always have a choice so choose to see things in a positive light. They say Attitude is everything, right?
Thanks again….San Fran blog is coming soon!
I am so thankful for your strength and willingness to share your journey with us.
I don’t know how the 2 of you made it there AND back.
Thank you Corrine and Cort.
Corinne,
You are amazing in your perseverance! I’m so sorry and belittled that you have to wait 8 months just to be seen at UCSF- what a load of C—! If you don’t know someone in that medical system you’re screwed- on top of being sick. Too bad Dr P doesn’t have some pull in the system.
My prayers go out to you that things begin to stabilize soon.
Greg
Dr P actually got me in within a week. The 8 months was the entire time from discovery, to testing, to traveling, to lumbar puncture, to local neurologist…to finally deciding I need to see a specialist @ UCSF.
Blog on that adventure coming soon!
I sure hope another angel will come along to help you get to and navigate SF Corrine and that you’ll get to the bottom of these neurological symptoms. So glad you both got some therapeutic nature time -I can so relate to wanting to lace up the hiking boots. Thanks for sharing your story – wishing you all the best.
San Fran blog is next and angels did appear!
Thanks for reading my story.
Corrine, thank you for sharing your story and your heart, and thank you Cort for being her angel when she needed you, for showing up instead of just speaking up. I pray things will begin to settle down for you Corrine and that you will continue to have the strength to trust during this journey. No one would choose to be an Index Patient, but it seems that this is the role you have been thrust into. It is encouraging to see you have wonderful caring support from Dr. Peterson and the other “angels” placed in your life when you need them the most.
There have been many times when I have found comfort in the following quote.
“When you feel like you’re drowning in life, don’t worry — your Lifeguard walks on water.” – Source Unknown
Thanks Pat, During the trip with Corinne it struck me how much better balanced she and how much better shape she was emotionally than me – even with all this distressing stuff going on.
not saying much, actually. 🙂
wonderful quote!! I love that!!
Just keep your eyes open…angels appear all the time…in disguise 🙂
Thank you for reading my story. Next one will be up soon!
Hi Cor,
Read your blog in its entirety. As I read it, I could not help but think of Robert Frost’s poem “The Road Not Taken”. Yes, you and Aud are on a road, but not one of your choosing. Nonetheless it is the one less taken and for better or worse, it too has made all the difference in your worlds. Ultimately, I think (I pray) that this road that you both are on (at least the parts you have chosen) does have an ending and that it will make all the difference in yours and a lot of other people’s lives. For your courage and persistence in going this distance, I remain hopeful and feel fortunate to be a part of your journey.
Fred
I am touched by your comment…my dear friend. Thank you and Aud for everything!
Thanks, Corinne & Cort, for bringing us this ongoing and detailed account of treatment from Dr. Peterson. I learn a lot from each installment and always look forward to the next one. Corinne, I hope your symptoms are getting better and that the spinal lesion is healing. Reading what you’ve been through, I’m especially thankful for today as I am. Thank you for sharing your journey with all of us.
Yeah, what they said. 🙂
You two are amazing!
I have a question. Since Dr Peterson doesn’t take insurance, are the MRI’s and blood work all out of pocket since they have to be ordered by someone who takes insurance or Medicare to have them paid for. I’m wondering if he has an associate who does take insurance who orders those for him. Otherwise all of this would really cost a fortune.
DrP does indeed take Medicare and other insurance…that has been one of the biggest blessings of this whole ordeal. It still hasn’t been cheap, but it makes it doable.
Glad that you see improvement in your emotional/psychological well-being in the midst of this roller coaster ride. Also that you didn’t have to pay for the trip with prolonged symptoms afterward. I appreciate all the detail you include in your accounts, along with the definitions, which help non-medical people like me follow more easily. I hope you continue to keep us posted.
Thanks,
Carol