The Spinal Series
This is part three of a series examining spinal issues which may mimic chronic fatigue syndrome (ME/CFS) and fibromyalgia. The first two in the series involved two very ill ME/CFS patients who have recovered or are recovering following surgery to correct craniocervical instability.
- Could Craniocervical Instability Be Causing ME/CFS, Fibromyalgia & POTS? The Spinal Series – Pt. I
- Jennifer Brea’s Amazing ME/CFS Recovering Story: the Spinal Series – Pt. II
Leader in the Field
Back in 1999, Peter Rowe was way, way ahead of the curve when he was the first to explicitly link ME/CFS to Ehlers Danlos Syndrome. Twenty years ago, he concluded: “These observations suggest that a careful search for hypermobility and connective tissue abnormalities should be part of the evaluation of patients with CFS and orthostatic intolerance syndromes.”
He was the second in the scientific literature to mention POTS and neurally mediated hypotension in connection with ME/CFS. In 2014, he was the first to report that reduced range of motion in the limbs and/or spine was commonly found in ME/CFS. In 2016, he demonstrated that seemingly innocuous movements such as leg lifts were able to produce unusual amounts of neuromuscular strain and symptoms in ME/CFS. Rowe speculated that these unusual findings could result from increased strain in and reduced blood flow to the spinal cord and its associated structures, as well as from mast cell activation. In 2017, he reported on chronic fatigue in Ehlers Danlos Syndrome (EDS). Last year, he was the first to link spinal stenosis with ME/CFS.
Is there a theme to all of this? Perhaps. Rowe has been digging into and finding connective tissue and autonomic nervous system abnormalities in ME/CFS, POTS and EDS for decades.
Peter Rowe’s Spinal Stenosis Chronic Fatigue Syndrome (ME/CFS) Group
J Transl Med. 2018 Feb 2;16(1):21. doi: 10.1186/s12967-018-1397-7. Improvement of severe myalgic encephalomyelitis/chronic fatigue syndrome symptoms following surgical treatment of cervical spinal stenosis. Rowe PC, Marden CL, Heinlein S, Edwards CC 2nd.
In his 2018 report, Peter Rowe presented three cases of severe chronic fatigue syndrome (ME/CFS) which resolved after surgery for spinal stenosis (narrowing of the canal the spinal cord goes through.) Each case, interestingly, had a different kind of onset.
Patient 1
The first person’s illness started with a gastrointestinal viral illness at age 12 which produced fatigue, unrefreshing sleep, post-exertional malaise (PEM), cognitive issues, headache, muscle and joint pain, sore throat, and tender glands. She later developed dizziness upon standing and was diagnosed with POTS at age 15. (She did not respond to POTS medications.) She dropped out of high school as a sophomore. Her Beighton score did not indicate Ehlers Danlos Syndrome (EDS) was present.
With her mother having undergone two procedures to correct congenital spinal stenosis, the condition clearly ran in her family. Nevertheless – possibly because of her ME/CFS label – spinal stenosis was not considered until she developed tinnitus. At age 21 – nine years after her first symptoms appeared – an MRI clearly showed she had a congenitally narrowed cervical spinal canal at C6-C7 with spondylotic (arthritic) stenosis.
Her improvement following cervical disc replacement at C6-C7 was remarkable. By six months, this young woman – who had been disabled for over five years – was working 12 hour shifts as a horse wrangler, saddling and feeding horses, leading rides and cleaning out horse stalls. A year after the surgery, she was at University full-time while working 20 hours a week. Five years later, she remains perfectly healthy.
Patient 2
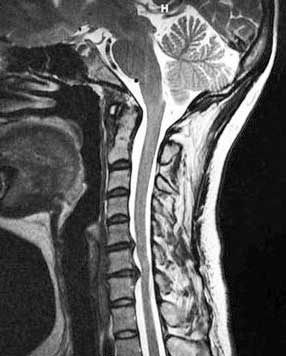
Patient 2’s discs were protruding into her spinal canal. (from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5796598/#!po=32.6923)
Patient 2 had been generally active until age 29 when, without any evidence of an inciting event, she developed profound fatigue, unrefreshing sleep, PEM, cognitive problems, headaches, and muscle and joint pains, plus an array of neurological symptoms (burning in the legs while standing, numbness in the limbs, electric shock sensations in her arms, difficulty swallowing, and clumsy gait). To top it off, she developed anxiety and depression as well.
She, too, had a family as well as a personal history of connective tissue disorders. Her sister had scoliosis and Chiari I malformation, and she had had surgery (pectus excavatum repair) to correct a sunken breastbone and early onset varicose veins, which had been treated with vein ligation and striping at age 28. As with patient one, her Beighton score was low.
An MRI of the brain and spine at age 30 revealed she had mild degenerative disc desiccation extending from C3 through C7 that the neurologist did not believe was causing her symptoms. At age 31, she tested positive for POTS, but like patient 1, did not respond to treatments. Four years later, and seven years into her illness, she was in a wheelchair with severe PEM. This time, a finding of hyper-reflexia prompted another MRI, which indicated a greatly narrowed cervical canal (7mm) at C6-C7. Her gag reflex had also disappeared and she had reduced strength in her arms, but her Hoffman’s sign was negative.
A hybrid anterior cervical disc fusion and disc replacement resulted in slow but steady improvements. By 8 months, this formerly wheelchair-bound patient was able to walk for 35 minutes a day. By 20 months, she could “exercise on an elliptical machine and recumbent bicycle, perform daily house-keeping chores, run multiple errands in a day, and paint the interior rooms of her parents’ house.” She was also able to stop 3 of her 4 antidepressant/anti-anxiety medications.
Patient Three
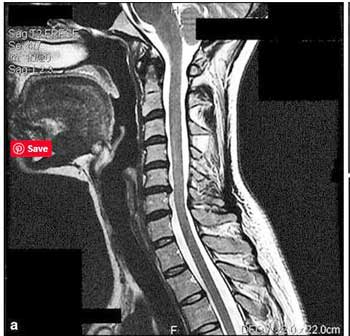
This person’s arthritis contributed to her stenosis. (from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5796598/#!po=32.6923).
In contrast to the other patients, this patient did not have a personal or family history of a connective tissue disorder. Her Beighton score, however, suggested she had Ehlers Danlos Syndrome (EDS). She was a healthy 31-year old until she developed severe fatigue following a trip overseas, and within four months had to stop working. Her symptoms were familiar to those with ME/CFS (unrefreshing sleep, post-exertional malaise, difficulty with concentration, headache, muscle and joint pains, nausea, lightheadedness, tremulousness, visual disturbances, and excessive thirst). As she got worse, anxiety and depression emerged.
She was quickly diagnosed with orthostatic intolerance (neurally mediated hypotension – severe drop in blood pressure after standing). Two years later, she developed POTS (high heart rate upon standing) as well and a positive Hoffman’s sign was present. As with the other patients in Rowe’s report, she responded poorly to POTS medications. As her symptoms progressed, she required a wheelchair for outside trips.
An MRI at age 35 indicated she had spondylosis with a canal diameter of 8.5 mm (at C5–C6). Three months after an anterior C5–C6 disc replacement, she was downhill skiing. At 7 months, she was able to exercise vigorously without provoking PEM. A year later, she reported minimal physical problems.
Another ME/CFS Patient Gets the Surgery
Esther didn’t think she had spinal stenosis, but after reading Dr. Rowe’s case report, she headed over to her orthopedist. She’d been seeing him since she woke up one morning a year and a half earlier with shoulder pain radiating down her arm and was unable to lift her arm above her head. Her orthopedist immediately ordered an MRI after reading Dr. Rowe’s report.
It wasn’t clear what her canal diameter was, but her stenosis – ranging from C4 to C7 – was much more extensive than in the three cases Dr. Rowe reported on. Her surgery occurred six weeks ago. It’s too early to tell how effective it will be, but she will keep us informed.
Dr. Rowe reported that he expected that cervical stenosis will be more common among those with more severe cases of ME/CFS.
- Check out a connection between the sympathetic nervous system and spinal problems and how treating one person’s severe scoliosis improved his energy – Chronic fatigue syndrome and your bad back
Fibromyalgia (FM)
The only large study of spinal stenosis in ME/CFS or FM was done in fibromyalgia. In 2004, Heffetz’s found cervical spinal stenosis to be quite common in his neurological and neuroradiological exams of 270 people with FM.
It should be noted that this group was probably not reflective of fibromyalgia in general. The patients were referred by rheumatologists (66%) or contacted the doctor hoping to get in a study examining the neurological basis of FM. A higher percentage than normal (59%) had also sustained some sort of usually mild head trauma, and the rate of disability appeared to be quite high. They’d seen an average of 10 different medical specialists and were taking 5 prescription drugs. Almost 70% were no longer working. They were a very ill group.
Many symptoms (neck/back pain (95%), fatigue (95%), exertional fatigue (96%), cognitive impairment (92%), instability of gait (85%), grip weakness (83%), tingling (80%), dizziness (71%) and numbness (69%) suggested spinal cord involvement. The degree of exertional fatigue (PEM) exceeded that seen in some ME/CFS studies.
The neurological exam produced other signs (upper thoracic spinothalamic sensory level (83%), hyperreflexia (64%), of the radial periosteal reflex (57%), positive Romberg sign (28%), ankle clonus (25%), positive Hoffman’s sign (26%), impaired tandem walk (23%)) suggestive of spinal cord damage or myelopathy.
Anything less than 13 mm spinal canal diameter suggests spinal canal stenosis. With their neck in extension, the average spinal canal diameter of this group at C5/6 was 10 mm. Only four of the FM patients in the study had a spinal canal diameter of 13 mm or more.
Forty of the participants in the study who later underwent surgery reported a significant improvement in their FM symptoms including pain, fatigue, and cognition, reduced depression and anxiety and improved quality of life (SF-36) .
Cervical Spinal Stenosis
Cervical spinal stenosis (from the Greek stenos – narrow) occurs when a pinching in the spinal canal compresses the spinal cord in the neck – interrupting the flow of nervous system signals. (Spinal stenosis can also occur in the mid-back and lumbar regions.) Rowe reports that a spinal canal with a less than 13 mm diameter is a strong risk factor for spinal cord damage or “myelopathy”.
The risk of spinal stenosis increases with age and often occurs when arthritis of the spinal column and discs narrows the effective space of the canal. It can also be caused by a thickening of the ligaments in the back or by bulging discs, and it can be congenital (inherited). When spinal stenosis is inherited, symptoms usually start to show up in middle age.
Symptoms
Symptoms typically start gradually and slowly get worse. (Some people with spinal stenosis, however, experience no symptoms at all. In fact, one study of elderly patients with low back stenosis found that many also had cervical (neck) and/or thoracic (mid-back) stenosis but were asymptomatic.) When moderate to severe stenosis is causing symptoms, surgery appears to be the only option.
The College of Rheumatology reports spinal stenosis can cause symptoms such as pain, cramping, weakness or numbness in the lower back and legs, neck, shoulders or arms, and WebMD has a similar symptom list (stiffness, back pain, numbness, foot drop, sciatica, problems walking, loss of bladder or bowel control (lumbar stenosis). While neck pain is often present, some people do not report neck pain.
No one looking at these symptoms would consider that spinal stenosis might be able to cause ME/CFS and fibromyalgia. Other researchers, however, have asserted that spinal cord compression can cause far more symptoms, including autonomic nervous system symptoms such as racing heart, problems standing, cognitive issues, etc.
Heffetz reported that “muscular fatigue worsened by exertion is a well-described symptom of cervical myelopathy,” and that chronic fatigue was common (but by no means universal – 57%) in Chiari I malformation. Heffetz also found that FM patients with spinal cord issues were often misdiagnosed with psychogenic illnesses like depression and anxiety (59%).
Like Jeff and Jen with their craniocervical instability, the three patients in Rowe’s survey appeared to be different from typical spinal stenosis patients. All had POTS, extreme fatigue, post-exertional malaise (PEM) and cognitive problems – and all had been diagnosed with ME/CFS; i.e., they appear to be a rather unusual ME/CFS/POTS-like spinal stenosis subset.
Diagnosing Cervical Spinal Stenosis
Dr. Rowe recommends MRI studies in individuals with abnormal findings following a careful neurological examination. Those findings include pathologically brisk reflexes, a positive Hoffman’s sign, abnormal Romberg sign, or other abnormalities suggestive of a cervical myelopathy. A family history of the disease can also support getting an MRI. Dr. Rowe emphasized that he does not obtain cervical spine MRIs in all ME/CFS patients.
Showing hyperreflexia, clonus and a positive Hoffman’s sign
Both Rowe and Heffetz suggested that the bias associated with a chronic fatigue syndrome and fibromyalgia diagnosis may be causing some doctors to not dig deep enough when confronted with signs of spinal stenosis.
Because few doctors will think of spinal stenosis in connection with ME/CFS or FM, showing them Dr. Rowe’s case report and Dr. Heffetz’s fibromyalgia study (both of which are free (use PDF button on upper left to print)) should help. Both papers specifically note that spinal stenosis can cause the symptoms associated with ME/CFS and fibromyalgia.
Various medical websites cite a variety of tests (x-rays, MRI, CT scans) used to diagnose spinal stenosis. If spinal stenosis is being checked, though, other spinal issues sometimes associated with ME/CFS and FM such as craniocervical instability, Chiari malformation and tethered cord syndrome should be checked at the same time. CCI requires a top-of-the-line MRI. Testing with the head extended / flexed appears to be recommended for both spinal stenosis and CCI.
Jeff provides important advice for getting tested and diagnosed with CCI – including how to get your scans into the right hands. Most neurosurgeons aren’t trained to recognize craniocervical instability (CCI), and finding an imaging facility that does the right kind of scans can take time.
Prevalence
Dr. Rowe reported that it’s impossible to know how prevalent cervical spinal stenosis is in ME/CFS until “a study across a range of mild to severely affected patients is able to provide a precise estimate of its prevalence.” He stated that it appears to be present but is probably “uncommon in ME/CFS”. Several other of his ME/CFS patients – beyond those reported in the paper – have been identified with cervical spinal stenosis.
Craniocervical Instability
Dr. Rowe also noted the need to look for other spinal conditions, such as instability of the cervical spine and instability of the craniocervical junction. He reported that a small number of his adolescent patients have been diagnosed with craniocervical instability (CCI) – a known complication of joint hypermobility and Ehlers-Danlos syndrome. He noted that all of those diagnosed with CCI had described a sense of having a heavy head or a head that was not supported well. (One person’s head was so poorly supported that she was called “bobble head” by her classmates.)
His CCI/AAI patients also described increased symptoms when their necks were flexed, moved laterally or extended in positions of neck flexion, lateral rotation, or extension. Some also displayed autonomic problems and neck pain following relatively mild head trauma.
Connective Tissue Issues
Dr. Rowe, as noted earlier, has been a leader in uncovering the connective tissue issues in ME/CFS and POTS. With one of the case reports testing positive for hypermobility on the Beighton test, having pectus excavatum (sunken chest) and apparently severe varicose veins, I asked him what connective tissue issues he looked for when assessing his patients. (My sole connective tissue issue is a mild case of pectus carinatum.) After noting that the Beighton test does not cover hip and shoulder hypermobility, he stated that:
“We look for the entire range of abnormalities seen in association with hypermobility spectrum disorders, including skin hyperextensibility, easy eversion of the eyelids, Gorlin’s sign (touching the tongue to the tip of the nose), widened scars, unexpected stretch marks, piezogenic papules of the ankles, flat feet, dental crowding, and so on.”
Rowe noted that joint hypermobility can produce a number of anatomical problems that affect the nervous system, including ligament laxity at the base of the skull (cranio-cervical instability), early degenerative disc disease, cervical spine instability and kyphosis (hunchback/roundback), dynamic cervical compression, and Chiari malformation. Other possible complications include tethered cord syndrome, Tarlov Cyst Syndrome, intracranial hypertension and temporomandibular joint disease.
Conclusion
Rowe’s and Heffetz’s report indicates that not only is spinal stenosis (narrowed spinal canal) present in ME/CFS and FM, but that surgery to correct it can return some people, even some very disabled people, to health. The big question is how commonly these and other spinal conditions are actually causing or exacerbating these diseases.
Chiari malformation provides a cautionary note with regard to spinal issues. At one time considered a top possible diagnosis in FM, a large 2004 study (n=244) indicated it was no more common in FM than in healthy controls and was pretty rare to boot (2.8% of FM patients).
Dr. Heffetz’s study, because of the way it was structured, almost certainly overestimated the amount of spinal stenosis present in FM. Still, Heffetz found so much spinal stenosis (46%) in his 2004 study that even knocking that percentage down a considerable amount could still leave a substantial number of people with FM with this condition.
The 40 people in in Heffetz’s study who underwent surgery reported significant gains in significant improvement in their FM symptoms including pain, fatigue, and cognition, reduced depression and anxiety and improved quality of life (SF-36).
Unfortunately it appears impossible at this point to know if someone’s spinal stenosis is contributing to their ME/CFS/FM or not. The fact that spinal stenosis become more common as we age and does not always cause symptoms obviously complicates matters. Dr. Rowe believes that people with severe ME/CFS will be more likely to have cervical stenosis.
Dr. Rowe believes spinal stenosis (and presumably other spinal conditions such as craniocervical instability, tethered cord syndrome, Chiari malformation) are probably not common in ME/CFS, but because they can occur, and in selected cases can even be causing the disease, he strongly recommends a full neurological examination be done on everyone with ME/CFS and FM.
Health Rising’s ME/CFS and FM Spinal Series
- Could Craniocervical Instability Be Causing ME/CFS, Fibromyalgia & POTS? Pt I – The Spine Series
- Jennifer Brea’s Amazing ME/CFS Recovering Story
ME/CFS and Fibromyalgia Spinal Stenosis Survey
If you've had an X-Ray, CT scan or MRI to assess spinal stenosis please tell us what happened. (Answers are anonymous)



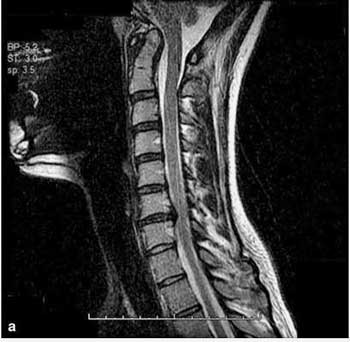




Dr Rowe wasn’t the first to suggest spinal stenosis helped people with CFS.
I was standing right next to them at the 2009 IACFS/ME conference in Reno when
Dr Peterson told him about it.
I saw his jaw drop and his eyes go wide.
“Classic CFS? HHV6A and all? Are you sure?”
Dr Peterson “Yes”
Stunned silence.
Then they walked away to talk privately.
Dr. Rowe was the first to report it in the literature but it’s no surprise that may have been Dr. Peterson – known to be a superb diagnostician – to first catch it in his practice. Thanks for sharing that.
This shows, though, how vitally important it is to get these case reports into the scientific literature. That is the only way to really spread them.
Alan Light noted that treatment trials need supporting evidence in the scientific literature and case reports provide that.
Hi Cort.
Please advis me how to go about cervical stanosis. Im in daily pain of my face neck jaw head. Im just learning of cervical stanosis and its starting to make sense.
I dont know how to persue this avenue. My c6 c7 is dameged, I have done massive dental work thinking its originating from dental issues. So far nothing was resolved. Its probably not the right place to reach out but hoping.
I’d go further than “mimic”, I’d say it was the main cause – I’ve done a blog on it here: https://goodback.co.uk/2019/01/15/chronic-fatigue-syndrome-cfs-me-and-your-bad-back/
Thanks Damien. I included a link to your blog in this blog.
A Dr. AJ Holman published a paper on positional cord compression in 2008, which talks about very similar issues related to fibromyalgia: https://www.ncbi.nlm.nih.gov/m/pubmed/18499527/
What does it mean when fatigue and other FM symptoms became far worse after ACDF surgery due to cervical spinal Stenosis with myelopathy. I’ve also since been diagnosed with Lyme and Bartonella, mast cell activation, reactivated EBV, and other conditions.
Thank you for mentioning Lyme. I am hopping that àll this great information could help Lyme patients. For instance, I have 3 discs that need to be surgically repaired.
Thank you, Cort, for this very informative article on an emerging area of interest in ME and Fibromyalgia. I have both. One small correction is that my cervical spinal stenosis and spinal compression affected C4 through C7, not C3. Believe me, a three-level surgery was more than enough for me… I’d also like to add that I am 72 years old so I would encourage seniors to not write themselves off as too old to investigate this. Seniors, we have our own ME support group to address our unique needs on FB: #MEAction Seniors Connect. You’re welcome to join us!
Hi there Esther,
I too have both ME and FM. For over 24 years now. I have become increasingly severely affected. Now totally dependent on my husband for everything and virtually housebound.
I also have spinal stenosis – diagnosed just last year, both cervical and lumbar. Only found after an MRI ordered after a visit to a pain clinic for chronic pain. My spine had fractured the year before due to osteoporosis and I’d previously been diagnosed with osteoarthritis in my spine, hips and knees. Permanent and disabling back pain has limited me even more. However, due to being so ill much of the time, my doctor advised me against having surgery.
I’m fairly ‘senior’ being 63. I would like to ask if you feel the surgery has made any improvements for you.
I’ll also look up your group on facebook!
Hi Tisha,
We’ll be glad to have you join us! I believe our group is for anyone 55 or older. I’m sorry you are suffering from so much pain. I’m sure this surgery is not for everyone. But I was told I needed it apart from ME or Fibromyalgia. And after 33 years of illness, I decided to do it sooner rather than later in hopes of getting some improvements in my condition. I am having some inklings of improvement in fatigue and my ability to stand without orthostatic problems but it is far too early for me to report anything definitive. Recovery from this surgery takes a whole year. I am using the forms Dr. Rowe used which he was kind enough to send me to try to evaluate my condition quarterly for the first year. I filled them out pre-surgery. And I will keep Cort informed about how I’m doing. I hope you find something that can offer you some relief whether it is surgery or not. I understand how terribly you are suffering.
Hi Esther,
I also have severe stenosis at C4-7. Can you tell us in which ways you’ve improved since having surgery?
Thank you!
Hi Rachel,
Please check out my response to Tisha above to see if that answers your question. I will just add that when I decided to have the surgery, I didn’t think and still do not think the data are sufficient to do what is a very difficult surgery in the hopes of an ME or Fibromyalgia improvement alone. I was told that I needed the surgery, though not as an emergency, and the possible consequences of not doing it. I was very scared at the prospect of doing such a surgery even though I’ve had many other types of surgery in the past without much fear. Something about the anterior incision felt too close to the idea of getting my throat cut and that freaked me out. But, in the end, I couldn’t bear the mental stress of waiting with no decision made, I knew I would have to do the surgery eventually anyway and, by getting the forms from Dr. Rowe, I thought I might have a chance to make a contribution to our ME community. That was what got me across the finish line. And now I’m hoping I might get to enjoy some improvement in my condition that could point the way for others. I’d be interested in hearing about your condition, if surgery is being suggested for you and what you decide to do!
Thanks for the reporting, Cort. I’ve never had a cervical MRI with my neck extended. Could a 10mm shrinkage be present and not show up on a regular MRI? Thank you, Jane.
I don’t know. My guess is, though, that it would show up as I haven’t seen any statements that particular kinds of MRI’s needed. That said, I have heard there is significant difference between newer and older MRI’s and it is probably best, if possible, to go with a newer machine.
Speaking for my own experience, spinal stenosis and CFS could coexist but not necessarily the causality to each other. My PCP exhausted all specialists, trying to find the cause of my CFS symptom and finally, strongly suggested me to take neck surgery, which was a major one. I did it, but my CFS is still there, even if not worse these days.
Yes, they must be able to co-exist. As we get older the chances of having some form of spinal stenosis go up and up – so there must be quite a few people with both FM or ME/CFS with spinal stenosis which is not causing their ME/CFS/FM. That is the dilemma isn’t it? The only way to tell if cervical stenosis might be causing ME/CFS/FM is to get the surgery!
Rowe’s patients were particularly interesting because they were younger, two had spinal issues in their family and one had EDS…They obviously didn’t have the late onset cervical stenosis that is age-related. My family does not have a history of spinal issues – I would guess that I would be a low risk (although I did have a concussion when young).
I should have mentioned that my spinal stenosis caused acute pain from the neck down to both shoulders and arms and balance, gait disorder … That is the main reason, plus CFS symptom, for me to take the surgery. Most, if not all, aging people have stenosis, but many of them don’t have problems/symptoms, my neurologist said. So, for patients, who have CFS symptoms only, need to consult neurologists, neurosurgeons to find out if it’s right to take spinal surgery in order to cure CFS. The surgery itself is very harsh to the body.
My spine doc says the spine and its nerves are very resilient and can adjust/adapt. I have spinal compression and whole spine has stenosis with spurs and bulging disk. It causes alot of pain. I also wonder if it’s not causing some of my neuropathy. (Stenosis with calcification and spurs, happens alot with EDS, as its trying to stabilize the spine. We also get early arthritis.)
I have a PT friend who says surgery will be her last option and she has seen it not be effective. (We both have EDS and instability.)
One Woman told me she lost her Histamine Intolerance issues, she was finally diagnosed with Systemic Nickel Allergy Syndrome & it is in numerous body items & household & food products I have numerous metal issues I react to numerous
things belt buckles, earing, wrist watch neck/wrist chains jeans buttons vitamins minerals medicines all contain meats, even so, are allergic to stainless steel Cobalt chromium the list is long some react to needles vaccines blood draws iv’s, it is
even in all cans, shaving razors, shaving creams, sodas canned foods…It is even in Sinks drains faucets baths showers even toilet flushing & door knobs, car house keys Nuts so many items also in cigarettes as well…Also, they should look at proper
CT images for Eagle Syndrome & dental Panoramics & other x-rays…I think I have both conditions my Panoramic shows 2 bones one on each side the left thicker longer, it may explain the bones pushing on the Jugular vein drops in blood
pressure even CCI Stenosis Chiari etc
Thanks Cort for providing this clear X-Ray scans. I first had to look where the problem was located (I guessed wrong where the spinal cord was:-)). When actually seeing it I had an instant strong “WOW” effect blowing my mind. Now I finally start to get the severity of the problem.
Personal experience:
I experienced the importance of the connections feet-legs-sacrum-spine-neck-brain_oxygenation and (diaphragm_)breathing-spine-neck-brain_oxygenation bit by bit. Keen senses, good intuition, good knowledge of physics and a fantastic physical therapist helped getting there.
When moving my feet or legs in a certain way, when moving my sacrum or back in a certain way and when performing a good deep-sacrum (diaphragm) breathing I can feel the near-instant effects on either hart rate or brain “freshness”.
To make clear I do not exaggerate, I had many instances I had a hard rate late night far over 160 (till that I can keep up counting it). With some of these techniques I could get the hard rate back to around 60 in often less then 10 seconds. Just to say I don’t imagine when I “sense” something is happening. I’m still in the stage of refining and making these techniques more safe, effective and reliable so it’s too soon to share.
Now these two things, stabilizing hart rate and improving “brain freshness” do not require exactly the same techniques but there is quite some overlap.
When it comes to stabilizing the hart rate I believe for now it has mainly to do with improving hart prefill a lot. Part of it is using the leg muscle pump. But it’s far from sufficient to explain the vastness and stunning speed of it’s effect: going from a longer lasting likely 200+ bpm hart rate to around 60 in sometimes as little as 5 seconds is nothing but stellar.
I believe that a significant part of the problem is that the main vein going from the legs to the hart is pushed upon by my sacrum where a denting occurs making the cross section more oval then round. With my engineering science I know this can have a very profound impact on blood flow. Now everyone has a sacrum, so something is making it dent this vein. That could be a divergent size or construction of the sacrum, but just as well a reduced length of this vital vein. Just imagine routing a garden hose around the 90 degree corner of a brick wall. When it’s long enough the bent will be loose and the hose will not be dented. When pulling strongly on both ends of the hose however, the bricks will dent it so much that flow comes to a trickle.
The topic of today is the spinal dents, so I’ll focus on that. But keep in mind the point here is that a seemingly small dent can reduce liquid flow vastly. It’s in fact a common technique in hydraulic equipment to reduce volumetric flow a lot.
Here comes the impact of a dent in the spinal fluid channel.
Each time you move your sacrum, be it by breathing or by moving your legs, you change the curvature of your back. Each time you change the curvature of your back, the tension of the tissue along your spine and the surrounding tension changes.
So each movement of the sacrum_spine combination has a double effect: it pulls less or more on the spinal cord and the tissue (like your backs muscles) around the spinal cord exerts more or less tension on the spinal cord.
This has again two effects. The varying pulling (along the length) and the varying compression (perpendicular to the spinal cords surface) of the spinal cord create a significant change in volume (of the spinal cord) available for the spinal fluid. As spinal fluid is just like water near non compressible this results in a significant flow from spinal fluid from the cord to the brains spinal fluid bag forth and back.
I can easily see a dent as seen in two out of three of those X-rays both reduce this flow a lot and create a very sharp pressure rise in the spinal cord when fluid can’t move fast enough out of it when the spinal cord is compressed.
This potential sharp rise in spinal fluid pressure when the channel is obstructed might point to a commonly observed thing in ME:
Hyperventilating *by breathing fast but shallow*. I am not referring to hyperventilating itself but rather to how we do it.
We could breath deeper but less fast and still hyperventilate. Or we could use diaphragm breathing rather then shallow chest breathing so commonly observed in ME.
Many of us with gut problem may instinctively avoid diaphragm breathing as diaphragm breathing can provoke your gut to hurt with each single breath you take as I learned. A good technique does help somewhat with this aspect.
But another thing I noticed to diaphragm breathing is that it causes much less of this “straining” of the spine and with it the spinal cord. Compared to what happens with diaphragm breathing it’s just hard to observe even if you know what to look for. Breathing shallow makes this effect near non existing.
So what has this to do with a potential blockage in the spinal fluid channel? As a “full deep diaphragm breathing” causes a large volumetric change in the spinal fluid with each breath it requires a large and unobstructed fluid channel to move the spinal fluid quick enough in order to not let spike the pressure in it very high. That easily would create massive spinal fluid leaks.
So breathing mainly with the chest and shallow *MAY* help to save the spinal channel from damaging pressure waves when this channel is obstructed (at the neck).
http://www.stayinghealthytoday.com/infection-coronary-artery-disease-plant-based-diett-stephen-fry-md/
I posted this in another comment on this thread, but here it is again. This is latest article I’ve seen from DR. FRY.
If he is right, this could be a major issue with many.
And also goes along with mold illness that Dr. SHOEMAKER talks about with CIRS. I have the bad genetics and inability to detox properly mold and biotoxins. Also had Lyme and co infections. Have that mostly under control but have to be alert and aware to new exposures.
Hi Issie,
I did stick to the older post you made as I find it way more informative and easier to get the concept then the newer one. The older one gives me info I can envision and that helps me a lot.
As to the diet:
“Whole grains, legumes, lentils, other vegetables, and fruit comprised the major portion of the diet.”
Now that is a difficult one for me. My food intolerances nearly empty that list and I did find them to be a very big factor in my disease.
Fighting them and reversing the bacterial and gut problems they caused is a difficult and really slow process that gets really high priority now. Later I might try adding more of your approach.
In the meantime I already near banned any sugar. I go very low on fructose (and carbs decomposing to fructose) as that is my worst intolerance. I try and replace some of my animal proteins to vegetarian based ones from sources I am not intolerant too.
I still eat dairy as I seem to have very few noticeable trouble with that but I try and replace yummy cheese by yogurt and milk by cream plus water in order to reduce milk protein intake. I’m not going low on fat now as I want my metabolism to switch to slow energy e.g. starch and fat and both should help reduce my gut bacterial problem.
I do increase consumption of vitamin C and vegetable with some anti-microbial properties and even use daily garlic oil while I am intolerant to garlic. But most of my intolerances seem to be triggered once a certain small amount is surpassed.
While I’m not fully buying the current concept of the blood type diet as it is, I think it makes sense that the food one can tolerate depends on ones specific immune system makeup and blood group is a significant part of that.
I hope we can both continue to improve and help make clear when, how and why to improve diet in order to improve health as much as possible. When possible I’ll try and test clues from you.
Now this continuous pulling and relaxing of the spinal cord does something else: it pulls on the spinal fluid bag. Together with the movement of spinal fluid in and out this bag (that may help mix / refresh / “sort of pump” the spinal fluid) this deforms the brains spinal bag and more importantly changes it’s pressure with each wave of it.
So with each (deep) diaphragm breath a wave of changing pressure surrounds and travels through the brain as the pressure of the brain bag modifies the entire brains pressure.
This may sound unimportant, but each time I do such strong move I feel a clear “refreshing shot of fresh oxygenated blood” flowing through my brain giving me a little feeling of bless. It lasts only a few seconds with each move. And to notice it that well I have to do movements that are unsustainable. But upon more careful observing I notice it’s effect still hold to a smaller extend when doing normal diaphragm breathing. It holds only to a small extend when chest breathing and shallow chest breathing makes it inappreciably.
This fresh shot of blood to the brain isn’t strange. According to my understanding of the brain, blood flow in the brain and it’s capillaries is heavily influenced by the cerebral fluid pressure. So a noticeable change in it does affect the flow of blood in the brain.
Now what makes such wave special? With inflammation, there often comes plenty of tiny debris and clutter in the veins and probably worse in the smallest capillaries. ME is nothing but another name for “disease with brain inflammation” so if inflammation comes with a lot of debris and wast then it’s in our brains too.
Now such waste and very small debris easily gets stuck in these small capillaries IMO. You can try and remove it by increasing blood flow but that is only a modest solution. For those ever have cleaned bottles by hand, they’ll know you have to fill them half with soapy water and shake back and forth. That’s how you remove sticky stuff from a vessels side.
Now that seems a bit like what these pressure waves are doing (although in one direction only). Apply more (cerebral fluid) pressure: reduces the blood flow in the capillaries to near zero. Reduce the pressure: create a strong pulse of blood. Doing so with every breath should be way more effective to remove clutter then having a near constant flat blood flow level IMO.
This idea aligns with what I recently wrote from a biologist. When comparing (other) primates with humans he was surprised that humans are way more active and also have a far higher metabolism rate (speed at which the cells produce and consume energy). One of his conclusions was that humans are made to move as the other primates can’t sustain such high average needed blood flow with their very relaxed way of life.
Now our brains are clearly bigger then of these primates too. So we have combined bigger brains with brain cells that have quite a higher metabolism rate. That requires special tricks to provide adequate blood flow. Coupling movement and breathing patterns to improved brain blood flow may be just one of those mechanisms.
And a dent in the spinal fluid channel could easily severally impact it if this mechanism were important, depriving our brains from proper oxygenation.
Last one before my brain falls apart.
The spinal cord also carries quite a bundle of vital nerves. These have to be quite sensitive to friction and irritation.
Now imagine how each movement of any limb and each breath you take puts a change in strain and tension on the spinal cord. Imagine that this spinal cord very likely is located in some sort of connective tissue similar to fascia.
Then each movement of any limb you do and each breath you take causes the spinal cord to move a tiny bit along the direction of its length. Now look at those sharp-ish dents on the X-rays!
Ever tried to cut a cord without a pair of scissors when outside? Just move it forth and back (OK, perpendicular works far better but still…) along the edge of a brick or stone with a sharp-ish edge and it’s done in no time (for a thin cord).
Now even a bit of movement of the spinal cord along such dents ain’t likely a good thing. And irritating and grinding into the nerves of the spinal cord ain’t likely a good thing too.
So when reading
“he demonstrated that seemingly innocuous movements such as leg lifts were able to produce unusual amounts of neuromuscular strain and symptoms in ME/CFS.”
I can’t be that surprised (for people with such neck problems). Nor can I be surprised that they would have rigid muscles and shallow chest breathing.
Both are quite good to restrict movement into a range that will far less change the curvature of the spine. It’s also in line with
“he was the first to report that reduced range of motion in the limbs and/or spine was commonly found in ME/CFS.”
In fact, spinal dents (mainly at but not limited to the neck) might be able to unite two seemingly opposite frequent subgroups of ME (and FM) patients: the stiff back and limb persons such as me on one hand and the EDS patients on the other hand.
Having stiff backs (recognize that back completely blocked feeling when at worst?) and limbs helps reduce movement of the spinal cord. The gain is not cutting it through or at least not irritating and inflaming it far too much. The downside in this hypothesis is (beyond range of motion) reduced blood flow in the brain and energy wasted in the muscles to fix their position.
Having EDS on the other hand should easily result in exaggerated changes in back curvature compared to healthy people. That would result in far large movements along the length of the spinal cord. A far smaller dent (compared to healthy people) in the spinal structure would cause irritation, inflammation and damage to the spinal cord. If the fascia where the cord is located in is low quality (connective tissue disease) then this problem could be even worse.
Note: I am not saying all ME/FM patients have spinal issues! Just that they could easily lower the threshold to getting these diseases a lot.
Your brain did a lot of work De Jurgen. I can only imagine what it was like pre-ME/CFS :). thanks for your insights. They painted a pretty vivid picture of what a problem with the spinal canal would do
“I can only imagine what it was like pre-ME/CFS :).”
I could focus soooo much deeper then I can now. And while I never was strong at structuring and organizing things, that skill seems to be almost completely gone.
When text seems structured, it’s more the result of a flow. Structuring and bundling all the separate ideas I have so far to make them more coherently available to other patients will be a major challenge.
In the future I could really use help from someone that has that skill left and some spare energy to make my ideas more accessible.
While I always had an intuitive way of thinking, that is actually stronger then before. It’s a skill I’m born with. My gradual onset ME made it necessary to learn to make better use out of it over many many years, as that is the skill last standing when having brain fog. It’s somehow a way of thinking that costs me so much less focus and energy than “classic formal thinking”.
Still, when at worst my mental skills were really poor. Remembering my own name, speaking, figgering out how to open a door… were major challenges and left my brain exhausted.
So let me take advantage of your comment to emphasis that slowly relearning skills bit by bit by breaking them down in their utmost basic components and retraining them time and again has been very useful to me, both for mental and physical tasks.
I believe doing so is an important part in ME “revalidation”: learning to do tasks again from scratch but this time adapted to your “new” body and brain. It’s quite similar to how people with brain injury have to relearn all their skills.
It’s a slow process taking plenty of willpower, just like “real” revalidation therapy is. And unlike real revalidation therapy you ain’t gonna get medical support so it’s do it yourself. Over three years I could get some select skills up and running again to a certain degree. I had to chose what to retrain first.
“thanks for your insights.”
Thanks for reading, it makes me feel like it’s not wasted effort ;-).
dejurgen, thank you for your very plausible sounding theories. Always a pleasure to read. Now they need testing! You mention, ‘With inflammation, there often comes plenty of tiny debris and clutter in the veins and probably worse in the smallest capillaries’ I wonder if this debris is what the immune system reacts to – the mysterious irritant that doesn’t turn out to be an infection, or not consistently. Could it also be cell-free DNA which Dr Myhill finds in ME/CFS patients?
I think I’ve probably got this spinal stenosis. X-rays of degenerated disks and symptoms point to it and it’s got worse. I doubt I would find a suitable specialist to find it.
“I wonder if this debris is what the immune system reacts to – the mysterious irritant that doesn’t turn out to be an infection, or not consistently. ”
If I follow your wording, I can see undigested proteins, viral DNA for example from EBV shed by infected but latent cells, misfolded proteins and cell free DNA from both destruction of our own cells and from partly digested food crossing a leaky gut fit the bill. Other miscreants exist.
Most of them do not fit what I would call debris (just a matter of what I see as debris able to clutter capillaries really effectively). I’m more thinking about nets formed through the processes of NETosis aggregating some of the above plus other clutter like cholesterol, uric acid crystalls and such attaching to them.
NETosis would be a fairly effective and (relative) low damage immune response most suited to deal with the above mentioned problems.
“Could it also be cell-free DNA which Dr Myhill finds in ME/CFS patients?”
I’m only vaguely aware of this, I’d happily take a look into it if you could provide a link to such information.
As for debris in veins etc. Look at my comment of finding in blood and organs by Dr. FRY. His findings and issues with mold/fungus causing biofilm that adhere to walls of veins and also invade organs can be a very definitive explanation for dysfunction.
Issie
Hi Issie,
I did read the pdf document you linked in the first post on https://www.healthrising.org/forums/threads/dr-stephen-fry-and-protozoa-my-life-is-greatly-improving.2122/
It’s daunting complex and makes for a very grim reading. Don’t want to have to deal with bad bio-films in my veins and organs at all. But just hoping I don’t have them won’t make them go away unfortunately :(.
I think the bio-films themselves look more like a large(r) diameter blood vessel thing. So far I can imagine it seems difficult to form them into small capillaries. But I may be wrong.
In these bigger veins (and arteries?) they do plenty of damage too however releasing toxins and potentially massively trigger the immune system. Smaller parts getting loose from a bio-film or parts broken down by the immune system or debris from the immune system fighting these may indeed well end up being part of this “debris” in the capillaries I hypothesize .
So far I try and deal with the blockage of capillaries as that impairs oxygenation and cell functioning massively, I can better understand it and can better devise potential alleviating measures then trying to break down bio-films in blood vessels and organs.
I just experience how hard and slow it is to re-balance the gut micro-biome and I can only imagine this bio-film thing inside blood vessels and organs is a lot more resilient…
Just thought about this one:
A common cause of cutting through tendons at the heel is due to a calcium spike that has grown on the bone. Such spikes are quite sharp and can cut tendons completely loose over time.
Although the causes are not entirely know, it is believed that inflammation helps growing such calcium spikes on bones. Might have something to do with changing acidity at site of inflammation, who knows. And once a small spike irritates the surrounding tissue, it will prolong the inflammation quite a bit (and it will depend on how much movement there is at that location).
Now if one were to have an infection in the neck region or have had a whiplash it might cause inflammation near one of those disks in the neck. If one were to have bad luck it might grow a sort of spike on it…
Diagnosed with Fibrositis (no fibromyalgia Dx then) age 26 by rheumatologist. Later fibromyalgia. Overall pain, spinal problems continued. Stenosis more severe with time. Posterior laminectomy and fusion C3-C7 successfully performed 7 years ago at UCLA. My condition now much, much worse. Nothing has improved, pain is more severe. I was limited before, now I’m disabled. I’m sorry I had the surgery because I believe it hastened the progression of pain and physical limitations I was told would occur w/out surgery. Now, I’m told it’s Fibromyalgia and Undifferentiated Connective Tissue Dis.
Lumbar stenosis is now severe but I will not have surgery for fear my condition will worsen.
So sorry to hear that. Please fill out the survey at the bottom.
Numerous papers Published on Systemic Nickel Allergy Syndrome (SANS) & one just recently it mentioned smoking as well, it also explains why we react to everything & Syncope is also involved as well
Does this mean that we’re throwing away all of the theories about Epstein-Barre, Enteroviruses, HHV6, mitochondrial insufficiency, and other areas of research?
What if you have severe ME and you DON’T have spinal stenosis? Right now, I’m having trouble putting faith in anyone’s research, because it’s all over the map, and no one can agree on anything.
No, I don’t think so at all. Cort wrote about just this in the blog post focusing on Jen Brea’s surgery/remission.
It seems that way but surprisingly not at all actually. Jen Brea and Jeff together had the whole package – viral reactivation, POTS, MCAS, PEM – clear up after CCI/AAI surgery and Dr. Rowe, if I remember correctly, brought in the idea of reduced blood flows and mitochondrial issues.
“Does this mean that we’re throwing away all of the theories about Epstein-Barre, Enteroviruses, HHV6”
At my late teen age I got hit by a car. The bumper of the car hit my knee. Luckily there was no clear damage as the speed of the car was low.
Two months later I got the flu. I had I think up to 40.8 degrees Centigrade fever (a lot!). After a week the flue subsided. But a small week later that knee that took a hit began swelling a lot. It was really thick and full with water. I could barely move it and at the time I considered it to be very painful. That is until I learned how much worse ME/FM pain can be :(. Fever reached up to 40 degrees again in the evening for about a week.
So the strong bout of flu had set in at my knee joint and caused very clear and strong infection and inflammation. The flu isn’t know as a classical joint infection. That knee afterwards remained sensitive to exertion and wrong movements for a few more years.
Likewise a bad healing common cold is known to be able to cause problems with the hart valves later on. And so do teeth infections.
So it seems that strong (and even less strong) infections can find week spots anywhere in the body and infect / inflame / damage them. People with an already weakened but non symptomatic neck or spine may get hit by either a strong infection or a longer lasting semi chronic inflammation up their. And that could help deteriorate the discs (see one of the lengthy posts above for a possible mechanism).
I think that a lot about ME is that a trigger like a strong infection, whiplash, mold exposure… reveals and hits on pre-existing but often hidden weak spots. That would certainly help to explain why some (seemingly healthy) people get ME after a strong infection and why some don’t.
Where do I begin? Being a person first with extreme flexibility AND stretchy skin, my geneticist declined to ‘type’ me, but most doctors say I have ‘Hypermobile/Classical-like EDS.
I also have not only spinal stenosis, (not uncommon for people with EDS), but problems with my bursa and synovial areas which supply joint lubrication (also not uncommon with EDS). When I lost feeling in my lower ‘saddle’ and legs, it was determined that I had a synovial cyst crushing my spinal cord down to a nub. The doctors were surprised I could even walk!
I can’t say this had a huge impact on my energy levels as I already had CFS symptoms in addition to dysautonomia (which no doctor wanted to investigate). The doctors recommended a spinal fusion–but I resisted.
Many EDSers have fusions and the levels above and below frequently later also need fusions. There are quite a few EDSers who have almost their entire spine fused! Since 80-90% of people with EDS also have significant fatigue, I am not so sure that these fusions have helped them. In fact, many, in addition to problems healing (common in EDS), also have exacerbated pain. So, approach fusions with caution!
As an aside, if you are developing caudia equina syndrome (numb butt and can’t control bowel movements) that is an emergency and RUN to the ER! That does require surgery! However, for people like me, time and high doses of curcumin (Cure-Pro BCM-95) actually shrank my synovial cyst and made my symptoms go away! Targeted P.T. can help with the rest. And as Cort mentioned, people with stenosis only, may or may not experience symptoms.
IMO, generally speaking, if one has instability in the cervical area (near the brain), that is more likely to produce symptoms similar to severe ME/CFS or dsyautonomia (dizziness, nausea, weakness, headaches etc.–and fatigue trying to function with it all!) In other words, I’m not so sure that this is ME/CFS proper, but a condition which produces similar symptoms. Of course, I think many people have multiple things going on and so untangling them can be tricky.
Now, a quick report about my first visit to Stanford’s CFS clinic; I had a long interview with the doctor and found parts of it frustrating because English is not his first language and I deduced that he had problems understanding some of my comments. Also I spent a lot of effort writing and documenting an ‘illness narrative’ and submitting it weeks in advance, and I also deduced that it probably wasn’t read. He kept asking me about every kind of doctor I had ever seen for all of my many medical issues. In clinic it was difficult for me to recall the dozens of specialists for everything EXCEPT ME/CFS!
In the end, he ordered a lot of labs, and those which have already come in are ‘normal.’ I got the lecture about ‘pacing’ and it was suggested I get a Fitbit. He also wanted me to get off my small Norco dose and use LDN (which I have tried and failed in the past). He recommended several supplements (turmeric, L-carnitine, Magnesium, dark chocolate and CoQ-10–all which I already take) plus a Mediterranean diet.
The final Rx was low dose liquid Abilify (aripiprazole)–but I got confusing dosing instructions. Note to others; if your insurance doesn’t provide good coverage, ask for a paper script and then try GoodRx.
I haven’t tried my first dose, but found the Stanford Facebook group and will probably log on to report my experience.
That’s the basic report! Thanks Cort!
Hadn’t heard that Ambilify helped pain. But found this:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3184588/
Interesting. Do you know of people its helped? There is also an herb that can up dopamine. Wondering if that would also help.
Issie
https://bebrainfit.com/dopamine-supplements/
Here’s a link on some dopamine enhancing supplements.
Cort, I was wondering which MRI machine would be best to diagnose/rule out all of the following: spinal stenosis, CCI, Chairi, tethered cord and possible CSF leaks? There is the upright MRI and the 3Tesla supine MRI. The 3Tesla supine machine is much closer to my home but since these tests are ultra expensive I want to do them once and get most accurate results.
I’m not an expert but from what I gathered the 3Tesla machine can do it all. The upright MRI with flexion, etc. will work for CCI. Flexion and extension is best for spinal stenosis but I don’t know if being upright helps or not.
Maybe someone with more knowledge will chime in.
Upright posture shows a different alignment and what happens with weight bearing. Upright checks the different movements of the neck and helps see if there is a drop of the cerebral tonsils.
https://www.uprightmri.co.uk/advantages-of-upright-mri.php
3T gives better/more detail (has more signal strength than 1.5. https://info.shields.com/bid/85107/what-patients-want-to-know-about-mri-machines-1-2t-1-5t-3t-whats-the-difference) as for MRI testing. Can show stenosis and spinal compression.
https://rarediseases.org/rare-diseases/chiari-malformations/
This is a good link to Chairi.
https://www.sciencedirect.com/topics/neuroscience/spinal-stenosis
This is very long but gives good info as to stenosis and what can be done and results.
RE: Yocheved comments
I’m trying to square this with cluster outbreaks: Incline Village, (84), Lydonville, NY (85) and the long historic list of outbreaks in many countries. I got sick in 1984, and it seems as though there were a lot of sporadic case in the early 80 s as well as the two clusters.
Question: How would a hundred or more people suddenly come down with spinal generated ME/CFS at the same time in each of two different location/towns? Dr. Peterson is mentioned as someone who’s seen this, but he’s also the Dr. that followed the disease from the original outbreak in Incline Village. How does he explain cluster outbreaks with spinal issues? Very curious. I would like to hear his thoughts on this.
It may be that not everything occurs in a cluster or that the cluster outbreaks tell only part of the tale. We haven’t heard of one in years I don’t think. We also know that all sorts of pathogens can set off ME/CFS – which suggests it may be a generic reaction to infection. My guess is that there are several different flavors of “ME/CFS”. Plus there are people with other disorders – such as the congenital spinal stenosis cases Rowe reported on – which were misdiagnosed as ME/CFS. It’s also possible I suppose the initial infectin could have done different kinds of damage. Clearly symptoms aren’t enough – we need a good diagnostic test.
I was diagnosed in 2012 with fibromyalgia and cfs by my GP. I have never seen a consultant as my area does not refer to rheumatology!
My neurosurgeon did an upright X-ray with flexion and extension to supplement my Cervical Spinal MRI before my surgery. But I don’t know whether that would be sufficient to diagnose CCI and the other conditions being discussed.
After being diagnosed with Lyme disease and Chronic fatigue as a teen, I have never felt the same since. I’m now 42 and have been diagnosed since then with Chiari Malformation, scoliosis, drop foot and severe spinal stenosis. No doctor has seen a connection between these diagnoses and have only ever referred me to PT, pain management or psychiatry . Very interesting research. It gives me hope!
My daughter got mono in high school then cfs and 15 years later lyme disease. She has scoliosis and developed drop foot too. I know practioners haven’t been able to keep her atlas aligned.
ME/CFS is like the blind men looking at the elephant. Until a definitive diagnostic test is fully vetted (hopefully the nanoneedle), many conditions with similar symptoms may fall into the ME/CFS basket. I thought this was demonstrated by the new NIH study that eliminated a large percentage of the original study group because they had something else. They didn’t say what.
My field for nearly 40 years has been environmental toxins that can cause birth defects. An exposure that can cause birth defects frequently can cause health problems in adults who have been exposed.
Frequently the pattern of illness in a community or group with a particular toxic exposure can look a lot like ME/CFS.
For example, in the early 1970’s a fire retardant was accidentally mixed into the animal feed that went out to farmers all over the state of Michigan. The cows, pigs, chickens, etc. began to develop a wasting disease that looked like animal AIDs. The animals also had miscarriages and deformed offspring.
When the farm animals looked too bad to sell, the farmers ate them. Soon the farm families developed symptoms very similar to ME/CFS.
The late Dr. Irving Selikoff from Mt.Sinai’s environmental unit brought a team of specialists to Michigan and they examined and tested 1000 members of the farm families. The common finding was immune dysfunction.
This fascinating saga is documented in a book called the Poisoning of Michigan.
The flame retardant PBB is stored in body fat as are many chemicals in our environment today. The conditions that cause these toxins to come out of the body fat and circulate in the blood are stress, heat, aerobic exercise, sudden weight loss, concurrent illness, even deep tissue massage.
I could go on with other toxic exposure situations that produced symptoms quite similar to ME/CFS. Women who used cellusolve to etch on computer chips in Silicon Valley. Families exposed to TCE in Woburn, MA. Gulf War veterans. Vietnam veterans.
Many people don’t even know they have been exposed to a toxic, lipophilic chemical. Up until the early part of 2000, chlorpyrifos was approved for indoor spraying so an office or home might be treated with this highly toxic chemical.
This pesticide was widely used in the first Gulf War.
Re. the etiology of ME/CFS, clusters of cases could certainly be a common infectious agent or they could be a common toxic exposure.
The focus of studies I have seen to date has all been on an infectious etiology.
The organization I direct sponsors the National Birth Defect Registry. We collect data on structural and functional birth defects and health, genetic and exposure histories of both parents.
We currently have 481 children with a diagnosis of CFS in the registry. Eighty percent of their fathers served in Vietnam. I was surprised at this finding and am not sure what it means, but we may not be looking far enough back to determine who gets ME/CFS.
Thanks Betty. Fascinating! We really need to look into toxic exposures more… A story on that coming up.
For further information regarding the topic that Betty mentions, please read “Biological Testing Involving Human Subjects by the Department of Defense, 1977”, which put into print the testimony of witnesses brought before the US Senate Committee on Human Resources and the Subcommittee on Health and Scientific Research (95th Congress, March 8 and March 23, 1977). It will blow your mind!
Betty, I wonder if any environmental toxin other than mold was identified in Incline Village after the cluster outbreak there? Anyone know. I was at Lake Tahoe for just a weeks vacation in a friend’s cabin and got ME in the following year in 1986 so I’ve always considered myself part of that cohort. My very saavy PCP at the time asked me if I had been in Tahoe the previous year.
Do you know https://en.wikipedia.org/wiki/Legionnaires'_disease?
It’s a disease that spreads easily trough mist size water droplets and the bacteria causing it prefers warmer temperatures. The disease can occur in outbreaks.
As *Lake* Tahoe refers to a lake I looked it up. It’s located near Sacramento if I did find the correct lake, so it’s on a hotter climate.
The bacteria “L. pneumophila thrives in aquatic systems, where it is established within amoebae in a symbiotic relationship.” so the amount of it in the water can grow explosive when algae grow explosively fast.
“Sources where temperatures allow the bacteria to thrive include hot water tanks, cooling towers, and evaporative condensers of large air conditioning systems”.
->Would there be a cooling tower, electric plant or equivalent that draws water from the lake for cooling and thereby disperses it as (clouds of) evaporated mist? The increased temperature in most cooling towers would help spreading the bacteria a lot.
“Outbreaks of disease account for a minority of cases. While it can occur any time of the year, it is more common in the summer and fall.
-> When were the outbreaks?
There are different strains of the disease with different virulence. Most people exposed don’t get sick but some may die. That’s certain a strong type of infectious onset like a bad fever or worse that can trigger ME.
Symptoms are overlapping a bit with ME so in an outbrake it can be easily overlooked, especially since the Lake Tahoe outbrake is early. The first documented Legionnaires’ disease outbrake was only in 1976.
For common symptoms:
“Those with Legionnaires’ disease usually have fever, chills, and a cough, which may be dry or may produce sputum. Almost all experience fever, while around half have cough with sputum, and one-third cough up blood or bloody sputum. Some also have muscle aches, headache, tiredness, loss of appetite, loss of coordination (ataxia), chest pain, or diarrhea and vomiting.[15] Up to half of those with Legionnaires’ disease have gastrointestinal symptoms, and almost half have neurological symptoms,[14] including confusion and impaired cognition.[16] “Relative bradycardia” may also be present, which is low or low-normal heart rate despite the presence of a fever.”
Regarding under-diagnosis:
“A significant under-reporting problem occurs with legionellosis. Even in countries with effective health services and readily available diagnostic testing, about 90% of cases of Legionnaires’ disease are missed. This is partly due to the disease being a relatively rare form of pneumonia, which many clinicians may not have encountered before, thus may misdiagnose. A further issue is that people with legionellosis can present with a wide range of symptoms, some of which (such as diarrhea) may distract clinicians from making a correct diagnosis.”
Note:
in case Eric Johnson does not read this, please feel free to froward this to him. He might be well placed to compare it with the Lake Tahoe outbrake.
When looking to Margaret’s comment I saw mention too “Incline Village, (84), Lydonville, NY (85)”
The first is near Lake Tahoe, The second near a massive lake. It’s colder up there but Legionnaires’ disease can spread in such climate too but it’s supposed to occur less often.
When looking into https://me-pedia.org/wiki/1984_Incline_Village_chronic_fatigue_syndrome_outbreak I saw
“Erik Johnson, a patient who pioneered mold avoidance for CFS, theorizes that an outbreak of toxic cyanobacteria (blue green algae) on Lake Tahoe located near Incline Village, combined with other biotoxins such as toxic mold, may have created susceptibility to a viral infection and caused the outbreak.”
Just having read about “The bacteria “L. pneumophila thrives in aquatic systems, where it is established within amoebae in a symbiotic relationship.” I checked back on https://en.wikipedia.org/wiki/Amoeba to see if mold is in fact an amoeba and so can form a symbiotic relationship with this bacteria.
It appears that at the very least some types (if not all) of mold are amoeba.
Note: later reactions to mold do not have to have these bacteria on them IMO once an initial infection with mold + bacteria “L. pneumophila has triggered the immune system to dislike mold in general.
Issie, thanks for the links! Sorry for the delayed response as I needed some ‘recovery’ time from that appointment and all the labs!
In my own personal search for something that would help, I ran across Mucuna Pruriens (Velvet Bean) as a dopamine precursor, so it’s interesting that the doctor would be recommending Abilify which does similar.
I’m still waiting on the Rx (it’s not commonly asked for). The side effect list is rather scary as this is usually used for schizophrenia or extreme bi-polar at normal doses–and I’m unusually medication sensitive. Usually this drug is over $900 retail, but I am waiting for my GoodRx to come through to make it about $260–which is even cheaper than if I used my own insurance! (Damn those PBMs!)
To keep this slightly more on-topic, I do have spinal stenosis, some arthritis, plus all my EDS joint pain, so hopefully this might help my chronic pain.
New labs also showed positive past titres for EBV (not excessively high) which lends credence to the infectious onset camp. My initial onset was a rather dramatic sudden episode of almost feinting and being unable to walk in the middle of a busy district in Hong Kong after a relatively minor cold. The doctor got excited at hearing this and said he had several other people who manifested the same way. Hum, I do wonder….?
Since I do have high levels of pain, I hope this might help. I feel I am now in the zone of the ‘art’ of medicine… I’ll report more as I experience more…
Thinking maybe the herb may be worth a trial. Easy to get and less expensive.
For me and my sis, both with CFS and FMS…..it was found we have mitrochondrial dysfunction. My function worse than my sis. But I feel some of ours was triggered by vaccine and possible toxin exposure when children. But it goes back with us 4 generations now. Her kids DX with dysfunction too. We are certain my grandmother had POTS and my mom MCAS. Me with POTS, MCAS and EDS and my 19 year old nephew with POTS too. My sis and I in CFS research studies.
I also have/had Lyme and CIRS and also another fungus found in blood and organs by Dr. FRY (http://www.stayinghealthytoday.com/infection-coronary-artery-disease-plant-based-diett-stephen-fry-md/)
Findings with fungus in CFS.
https://www.sciencedirect.com/science/article/pii/S2452231718300083
This post is worth a read too. https://www.healingwell.com/community/default.aspx?f=30&m=3944646
I have Autoimmune dysfunction. Probably IF the immune system were working better, it would have fought off all these things.
I believe it all goes hand in hand. Is all connected and there is so much variation between us all. It is so complex with multiple symptoms/causes. There is no magic pill, operation, detox, etc. That will fix it. We just need our best “purple bandaid” and try to live life the best we can. Some things have helped me over the years, but no real “cure”.
Issie
It’s interesting to me that most patients who are testing positive for CCI/AAI had no other symptoms of hypermobility.
It makes me want to not put too much hope on this for myself because I have pretty extensive hypermobility since childhood and have multiple joint dislocations every day.
It feels like it fits me “too perfectly” so I’m scared to be hopeful.
The regular doctor (not a specialist) who wrote the report on my MRIs stated that there is “foraminal narrowing” at most of my neck vertebrae but “no stenosis.” I thought narrowing was stenosis.
But perhaps that means that the narrowing was not compressing the spinal cord. These images were taken laying down (supine T3 MRI). Also I just turned 29 (ME/CFS since 21 and POTS since 12)
One of my worst symptoms has been a constant ache at the base of my skull. It made me intolerant to light and sound and I couldn’t hold my head up so I’d always support it with my hands. I was told I was just being lazy and had bad posture.
Suddenly I stopped being able to wear contacts because my eyes were inflamed and produced abnormal tears that were as thick as jello. Also my eyes themselves felt horribly bruised and I scream if any pressure is placed on them.
I’ve been to 30 physical therapists over the years for my head/neck/ TMJ/ upper back, but nothing has helped. Although all of them have remarked that I have the worst facial, scalp, neck, and back tension they’ve ever encountered and have asked if I’d been in a car crash.
I’ve tried so many exercises, medications, etc., but the dysautonomia/ POTS/ small intestinal paresis, MCAS, and joint pain have all continued to just get worse and worse.
I’m so, so desperate to feel better that I want to cling to this CCI/ AAI possibility. But I also don’t want to set myself up for more disappointment.
What a time you’ve had! Something is causing your symptoms. If you’ve ruled other things out maybe it is CCI/AAI…Good luck!
Look into Ehlers Danlos. My nephew also just got a DX of Sjorgrins and POTS. We are pretty certain he has MCAS and EDS too.
We get this tension from trying to hold ourselves upright. Head in the hands is very common for us with EDS. Lots of us use bracing to not dislocate and/or support ourselves. Pain a definite issue.
@Glass Maybe your doctor is referring to the holes ( foramen) on the sides of the cervical vertebrae where the vertebral arteries pass through to the brain? So instability in the neck causes several problems : altered spinal fluid flow between the brain and spinal canal ( with high CSF pressure) and also possible poor blood flow through the vertebral arteries to the brain. Also problems with venous drainage. All important.
I do not have cervical spinal stenosis – must have MRI in flexion and extension of neck. But I have a small posterior fossa ( skull base), short clivus, steep angle of the tentorium – All Chiari characteristics, but no tonsillar herniation. I more recently wrote to a EDS researcher in Belgium – MD, PhD. He thinks I have a form of EDS – characterized by hypermobility in the upper neck and sacrum. I may be hypermobile in the pelvis, but have no other signs of hypermobility.
Glass, sorry to hear about all of your problems.
Probably not proper to post another blog site on Cort’s territory, but I recommend (if you haven’t already) you go to http://www.inspire.com, find the Ehlers-Danlos Community and join. Then use the search icon to look up past threads and you can find gobs of information about CCI, and all the other stuff related to the symptoms you are experiencing. The reason I encourage you to join is that much of the information won’t display unless you are registered as a ‘member.’
You may have to plow through a lot of commentary, but there are lots of ‘gems’ to be found including patient experience, doctor ratings, and alternate diagnosis ideas.
All the things that Issie mentioned (MCAS, POTS, and more) are there along with numerous links.
Certainly sounds like those may be in the ballpark along with possible spinal fluid leaks (which hasn’t been mentioned here)…
Kindest thoughts your way!
Cort, did you post the link to the report in which 40 Fibro patients improved after spinal surgery? I couldn’t find it (not that that is definitive…Ha) and would like to bring it to my Rheumatologist. Thanks, Esther
In 1998, I had a 14 hour long spine surgery to correct problems I was having after my 1975 double Herrington rod surgery. Immediately after, I was in the worse pain ever. After 2 years of this crazy pain, I was placed on Opiods. After this, my family noticed how my energy levels had decreased (but still thinking it was the surgery itself). After 7 years, I was spending half the day in bed resting. After 12 years I was housebound. For the past 10 years I am completely bed bound. Just brushing my teeth is exhausting. Interesting article connecting spinal issues with ME/CFS!
I’ve had ME for 14 years now, and 5 years ago was medically retired due to having cervical stenosis at C5/6. I was a trainer, working in the NHS, and the pain meds I was on made it unsafe for me to be at work. I’m about to have surgery to fix the stenosis. It only affects my left arm and hand, which coincidentally is affected by Poland’s Syndrome, pre birth. Or maybe it’s not a coincidence, as I have no problems with my right side.
The nerve pain was unbearable, so I’m on 300mg gabapentin x 3/day, as well as a 12mu g fentanyl patch every 3 days. I have a great deal of neck pain, despite the pain meds, as well as pain from the ME. I think I have moderate ME – up until the stenosis rearing its ugly head, I could work 3 days a week, but then would be so exhausted I couldn’t do anything else, now I’m retired, I’m able to pace myself better, but still become exhausted and need to rest lots.
I’ve filled in the questionnaire, and will repeat it in a few months following my surgery, in case I improve.
@Issie:
I’ve been reconsidering your comments again. Some things seem to come together and to forme a pattern:
If I recall well what I read in the info you linked in your comments to this blog (need time to reread and sort out things later):
* microorganisms in bio films are far far far better protected from the immune system
* the immune system must go in very high mode to break the bio film down; breaching the bio film and having the immune system inadvertently attack the arteries in full strength was suggested to be one model to explain the flare ups and subsequent relapses in MS.
* bio films can calcify over time, making the bio film even harder to break down by the immune system;
in my own opinion a calcified bio film is less active (“more death”) but hinders blood vessel functioning even more as sort of a solid wall is separating the blood from the arterial wall now.
* the vegan diet is a strongly alkali one
Add to this, IF I am correct (please clarify on these assumptions Issie, they are very important in this idea):
* you have had discovered fungal or other microorganisms “deposited” in sort of a “chuck” in (fleshy) tissue by chance during a biopsy
* you also have problems with calcium deposits around your body
* you suffer from de-calcification of the bones
* you have low calcium blood levels
* you believe the body tries to reduce blood calcium levels in order to reduce some sort of problem
Add to this following:
* inflammation is often going hand in hand with calcium deposits around the body, like calcium deposits in tendons, on bones… and irritation by those can cause further inflammation of surrounding tissue.
* calcium, as we all know from our household appliances, easy drops out of solution and deposits on surfaces
* calcium often dissolves by spraying it by an acidic solution
Add to it:
* the average Western diet (and lifestyle) makes blood far more acidic then a modest caloric diet high in vegetables and low in meat
* poor blood flow, strong exercise, stress(, and infection IMO) do locally increase acidity of the blood; anaerobic exercise or in our case a too high “background” levels of anaerobic cell functioning produces plenty of lactic acid for example
* I experienced it is *very* hard to restore my likely imbalanced gut microbiome. Just trying to kill it of and replacing by a new one does not work. These microorganisems seem to follow the “life occupies all possible places as fast as possible once conditions are favorable” rule.
=> So what if having these biofilms in our arteries is the normal? I wouldn’t have it considered as it did seem impossible challenging to sustain life like that and have the body “accept” such devastating situation. But then again, if you can survive this condition while having a very strong set of diseases weakening you, then so must healthy people be able to do so.
What if the body and the immune system have the same stance against bio films in the arteries as it has against parasites in the body? It fights them to keep their counts down. But near all people in generally healthy “undeveloped” communities carry parasites in their body. The immune system seems to prefer to keep their numbers under control over going full attack to eradicate them all.
Now if we apply this concept to bio films:
Having them causes a strong reaction of the immune system where they are. It costs plenty of effort to break them down. But then again many mircoorganisms under attack reduce replication rates so the amount of microorganisms per day that need to be destroyed could be “reasonable/feasible”.
Having calcium depositing onto the bio film however does 2 things:
* disrupt normal working (and healing) of the arteries a lot more
* cause the (local) immune reaction needed to break them down to be a few times stronger.
=> Now this “a few times stronger” could well mean the difference between a normal immune response and an immune response so strong it gets out of hand an leads to auto-immunity problems.
This strong amplification of the immune response causes a wide range of side effects like increased oxidative stress, exhaustion of the immune system, damage and leakage of blood vessels, disruption of blood flow by killing vassodilator NO by the oxidative stress, creating micro-trombi clogging up the blood vessels, extra energy consumption creating more anaerobic functioning elsewhere leading to a more acidic environment elsewhere, a more acidic environment likely at the venous side of capillaries dissolving tissue and bone calcium and allow it to deposit on the bio films in arteries creating a vicious circle…, an exhausted immune system unable to contain the expansion of bio films to a larger part of the arteries and even organs making the problem worse…
(A certain amount of )Magnesium could be deposited on such biofilms too IMO, as magnesium is about the second hardest common mineral to keep in solution.
In this vision, the biofilm problem would be separated from the capillary debris problem, but both would influence each other.
The biofilm problem would mainly be present in the (bigger) arteries. They would have quite a lot in common with arterial plaque and may even be a / the source of growing arterial plaque. Arterial plaque forms on the arteries. That is on the more alkali side. In an alkali environment calcium drops more easy out of solution.
On the venous side, lactic acid, CO2 and with it bicarbonic acid and uric acid from protein consumption make the blood more acid and that better keeps calcium into solution (or even strips it from the surrounding tissue).
They influence and reinforce each other as poorer blood flow means more acid in the venous part. More acid in the venous part means more calcium dissolved and stripped from tissue. More (“unstable”, important here) calcium in the blood means more deposit and poorer blood flow.
Women have generally a poorer blood flow and easier problems with severe bone decalcification. The later is believed to be hormonal. If so, the poorer blood flow adds to it. Both would steer women to be at higher risks for auto-immune disease.
Men may have a higher risk from uric acid formation when consuming equal amounts of (animal) protein and or alcohol. Uric acid can form crystals that can clog capillaries, deposit on tissue, trigger the immune system to destroy these uric acid crystals and will increase acidity at the venous part of the capillaries, dissolving calcium (and maybe magnesium).
I read that equal consumption of vegetarian protein compared to meat protein causes less problems with uric acid. While there are differences in amino acids between both diets, it offers not that solid an explanation as to why. The added benefit of a more alkali diet may be the biggest differentiator in the vegetarian diet.
It would help calcium drop out of solution in the arteries but it would decrease amounts of calcium dissolved in the veins a lot.
As not all calcium molecules are equally easy to dissolve, that may lead to less what I call “unstable”, easy to deposit calcium. So having calcium in the blood would not be bad, but having the easy depositable types would be. That could be another difference between meat based diets and vegan based diets: calcium in meat based diets resembles the one that gets dissolved near the veins in this theory. And that may be “unstable” calcium.
When the problem is bad like in ME, exercise likely triggers a very strong acidic local environment at the venous side of the capillaries. The poor blood flow and high ATP consumption turns the metabolism to anaerobic, creating plenty of lactic acid. When local glucose stocks drop quickly, chances are that protein consumption rates increase sharply creating plenty of ammonia waste. Part of that is converted to uric acid, which could lead to strong uric acid spikes. That would lead to a strong acidic environment (literally feeling sometimes as an acidic burning) and likely cause a peak in local tissue decalcification. Calcium in plenty of cells like muscle cells, brain cells… is essential for both good functioning and energy production (your emphasis on calcium ion channels).
Stripping it from this tissue will take time to recover (PEM). As increased amounts of calcium can drop quickly out of solution once the environment becomes alkali (when the blood passes the hart and reaches the arteries) it will quickly increase deposits on “vulnerable” surfaces like biofilms. That may likely thicken them substantially in a matter of hours. (it would not be rock hart calcium yet but softer, easier to remove slimy calcium layers on top of the harder ones). Maybe that could be sufficient to trigger an increased immune response. A delayed increased immune response is observed by researchers as part of PEM IMO and it could cause increased ME symptoms.
That brings me to a topic I was wandering about a long time now: the stinging nettle question:
Stinging nettle is renown since the Roman times as a prime medicine against Rheumatics. Flogging with it was the way to use them. Nowadays plenty of health effects are attributed to using them in for example nettle tea. But why?
For the flogging with nettles: I observed it works good to improve blood flow. That’s one part of the question.
But lately I am reluctant to use them. They contain formic acid (ant acid). That is what is supposed to increase blood flow. But it also cause a histamine release and that is often problematic in ME/FM patients…
So I dug in it deeper with these new ideas.
Nettle seems to contain plenty of calcium, vitamin D and vitamin K. http://www.thecurvytruth.com/calcium-vitamin-d-and-vitamin-k-for-bone-health/ and http://www.livestrong.com/article/350785-stinging-nettles-nutrition/
It is believed that this combination is important to get calcium into the wright places (by maybe dissolving wrongly deposited calcium and donate it to place where it is beneficial and needed). So that is a start. Vitamine K is often low in patients with bowel problems. Many ME patients have bowel problems. Vitamin D is often low in ME and MS patients too.
I did search further however. Would formic acid dissolve calcium and form a stable compound that stays easily in solution?
When searching for “formic acid calcium” to my surprise the first hit was en.wikipedia.org/wiki/Calcium_formate:
“Calcium formate is used within EU as an animal feed preservative. It acidifies the feed thus preventing microbe growth and increasing shelf life.”
“Calcium formate prevents the growth bacteria such as E. coli, Pseudomonas aeruginosa, Staphylococcus aureus and Enterococcus hirae in growth mediums. It also prevents the growth of fungi like Aspergillus niger and Candida albicans.”
=> Nettles are high in both calcium and formic acid so they are very likely high in calcium formate. And look at these properties! If these properties held in blood and when being near biofilms, that would be one great thing!
“Calcium formate seems to be safe as a calcium supplement for people with one time doses of 3.9 g (1200 of calcium) per day.[6] Increases in blood formate concentration have been observed with such doses, but in healthy subjects the formate does not accumulate, and is quickly metabolized.”
“Calcium formate is shown to be more readily absorbed form of calcium than calcium carbonate and calcium citrate.”
Part of what helps calcium formate to be better absorbed *could* be it dissolving better in water. *If* So, it would form less deposits on bio film in the arteries. Needs more looking into.
“No optic nerve damage has been observed with calcium formate supplementation – alongside with formaldehyde, formate is a major metabolic product of methanol, which can cause blindness upon ingestion.”
=> Now good to hear it ain’t that aggressive as formaldehyde 😉
“Ingesting liquids with high calcium formate concentrations cause severe gastrointestinal lesions.”
=> That is a reason to not go wild on it!
Some forms of calcium like en.wikipedia.org/wiki/Calcium_chloride#Food (added to food as “additives”) can bind and quickly deposit Phospor
“This description is illustrated by the fact that these solutions react with phosphate sources to give a solid precipitate of calcium phosphate”
=> Now ME patients have a shortness of (some forms of) phosphor, leading to low levels of oxidative phosphorylation and ATP.
Also the difficult to interpret http://www.jbc.org/content/124/2/437.full.pdf mentions it.
Nettles seem to have
“The urticating hair of stinging nettles contain sodium formate as well as formic acid.”
=> Very likely there will be calcium formate present as well then.
From en.wikipedia.org/wiki/Stinging_nettles:
“Human and animal waste may be responsible for elevated levels of phosphate[13] and nitrogen in the soil, providing an ideal environment for nettles. ”
=> This indicates nettles may be high in phospor too.
All of this plus the two former comments start to paint a certain possibility to me.
https://www.healthrising.org/blog/2017/02/28/biomarker-aussies-chronic-fatigue-syndrome/
Note my comments from this blog and reference to another thread. I do think there is calcium channel issues.
https://www.sciencealert.com/one-of-the-biggest-myths-about-chronic-fatigue-syndrome-just-got-destroyed
And, for more technical info on this……
https://onlinelibrary.wiley.com/doi/full/10.1111/cei.12882
FYI — I have mutations on just about every snp you can test for TRMP3.
I still find GastroCrom to be one of my best helps – it not only moderates mast cells it is a mild calcium channel blocker. Since it is so expensive, I try not to use it all the time and when I do within a short time, it helps. Also 1/4 of my RX prescribed amount of Tramadol helps. It too has mild calcium channel blocking properties. (I tried regular calcium channel blockers, and that was too much. Maybe some other properties in these two things in combination is what helps.)
https://en.m.wikipedia.org/wiki/Calcium_channel_blocker
With more narrow and potentially hardend veins, vasodilation has been helpful to me. Also if there is too thick blood as with APS or Factor 8 and Collagen Binding which are also a problem with me….not only thinning blood but increasing diameter through which it flows, seems to be helpful. But…..since I have EDS, I must be careful how much I do this or POTS becomes more of an issue. I find external compression better than internal narrowing. Binders seem helpful in certain circumstances.
Issie
@Issie:
Do you know if these Calcium channels work in two directions, e.g. they help to regulate calcium levels into the cell (when calcium levels inside the cell are to low) as well as out of the cell (when calcium levels are too high)? That could be a MAJOR question. The answer isn’t clear to me.
But I would suppose it’s possible as ALL arrows from channels in the plasma membrane (in figure 1 in the paper) point to one direction; that would either indicate the picture is missing some channels going the other way, having calcium leaking back through the cell’s membrane or some of the drawn channels to work in both directions.
Why could it be so major:
From the paper you linked:
“The current investigation showed inhibition of the ER Ca2+/ATPase pump and depletion of intracellular Ca2+ stores followed by PregS‐activated TRPM3 increased cytotoxic activity in NK cells from CFS/ME patients”
So too FEW calcium in these cells seems to be problematic in ME patients if I understand well.
Yet, you report success with several calcium channel BLOCKERS. That would REDUCE the amount of calcium getting into your cells IMO. So that doesn’t add up to me.
However, if calcium channels would allow calcium (and magnesium) to go two ways then it would make a whole lot more sense and it would be in line with my last three comments.
If you put a cell, be it an NK immune cell or an endothelial cell or almost any other cell in a strong acidic environment then their will be some sort of “potential” to extract calcium from those cells and move it out of those cells to form calcium salts. For example an environment with plenty of lactic acid (like described by me in the venous part of the capillaries) *could* extract calcium out of cells to form calcium-lactate salts. Those would be removed by the bloodstream and deposit on surfaces like bio films in the arteries and leave the cells near the capillaries in both a toxic environment full of acid and other waste AND leave them depleted from calcium (and magnesium).
IF calcium could leak out the cells this way, then using calcium blockers would make perfect sense. It probably would reduce the leak of calcium out of these cells.
It would also be in line with “The number of TRPM3 ion channels on the cell should increase when calcium stores are reduced; i.e. ME/CFS patients should have had more ion channel receptors on their NK cells- yet they had less.” from Corts blog you linked to.
Reducing the number of calcium ion channels should protect the cells better against loss of calcium *IF* a highly acidic environment existed and could extract calcium from the cells through using these channels. It’s in line with your calcium blockers experience.
=> Can you confirm that calcium levels inside cells being too low is the suspected problem at hand in ME?
=> Can you point out errors in my understanding of how calcium channels work?
Thanks 😉
As the question “But if we are low on calcium inside the cells then we should have more calcium channels then shouldn’t we?” Is a natural one I’ll write my thoughts on this one.
When I read en.wikipedia.org/wiki/Calcium_in_biology I see:
“The intracellular calcium level is kept relatively low with respect to the extracellular fluid, by an approximate magnitude of 12,000-fold.”
So obtaining an even lower level of intracellular calcium requires both ATP (energy) and calcium channels to pump it out of the channels.
IF I read correct that in ME intracellular levels are lower then in healthy people, we waste energy / ATP that we are short on to pump so much calcium out of our cells that they get dysfunctional.
Pumping so much and wasting energy till you’re sick doesn’t make sense to me. Decreasing the number of calcium channels however to make wasting energy to pump it out of the cells more difficult, reducing number of calcium channels to reduce “highways” for lactic and other acid to extract calcium from cells and using calcium channel blockers to waste fewer energy and to lose fewer calcium does however make sense.
If the assumptions in above two paragraphs are right, I’d go further and say our cells likely don’t waste ATP in order to lose too much calcium. When the cells are surrounded by a very acidic environment with acids that bind quickly to calcium then likely some calcium gets a “free ride” from the inside of the cell towards the acid.
In that point of view, it seems that opening and closing calcium channels is not only regulated by calcium levels inside the cells and that the effect of opening the calcium channels shuffles more calcium per ATP spent out of the cells then is supposed to be. The cells best reaction is to reduce the number of calcium channels in order to make it more difficult to start the action of pumping calcium out of the cells. Using calcium blockers tops on that. And so does eating a more alkali vegan diet (your approach) and trying to improve the functioning of the venous capillary blood flow or reducing blood pooling reducing acidity and exposure time (my approach).
Please feel free to correct me when I get my science wrong or where my hypothesis does not make sense.
I’m not able to comment right now and it has been awhile since I did the research…..but I love reading how your mind works and your hypothesis on all this. Science is advancing and when we find something that helps…..maybe science will sort out and tell us WHY. I have a few “purple bandaids” that help me and there are so many reasons and hypothesis as to WHY this could be. Wish I could completely sort it and have it definitely figured out.
Issie
This is a comment I made in the first referenced blog of CORTS:
I reread your blog @Cort, and noticed they first had to deplete the calcium and then work on upping the TRPM4 receptors. That would fit with what works for me. GastroCrom and Tramadol are both mild calcium channel blockers (this keeps calcium from going into the cells properly and causes a vasodilation affect) – I use those at night. Then in the a.m. use Pregnenolone which can up this action of TRPM3. This seems like this is a fine balancing act and may be something to do with receptors or autoimmune dysfunction. If we could tweak and create an epigenetic response to over ride these mutations (which is probably what I’m doing) things get better. ………Also thinning my blood with herbs (due to APS) is helping alot.
FYI, I wasn’t able to stay strict vegan. After about 4 years, I found myself getting much weaker in my muscles. I added back fish, organic meats. But not more than once a day or sometimes a few times a week. Also found that all nightshade vegetables, grains and legumes made me hurt worse. Thinking lectin is a problem with me. Finding this out made being strict vegan impossible for me. (However, when I was strict – I reversed Chronic kidney disease back to near normal.) I daily intermittent fast and have an 8 hour eating window. That has helped me alot. I dont seem to have Blood sugar issues now.
Issie
Also look into NMDA and Calcium channels. My hypothesis with POTS, is there is some connection with glutamate triggering sympathetic system and that along with calcium channel disorder may possibly be a key factor. I’ve been saying this for years hoping someone who had a lab and ability to research this would either prove me right or wrong. Thankfully it is being looked into now.
Everything is so connected and leads into other things. If there are faulty genetics and dysfunction with any of the channels – “we got a problem”. Now if we can figure a way to tweak or create expression or decrease expression (whichever way it needs to go), we may get a measure of improvement. I’ve found a few “purple bandaids” and they work for me.
I spent years learning and trying to explain WHY something worked and why certain things caused issue…….since I have found a way to be somewhat level and functional- I dont look/research much any more.
Issie
Hi Issie,
Yesterday I remembered something about ion channels only transporting electrically charged ions. That makes things entirely different.
As it’s a very difficult topic for me, please correct me where wrong.
So if I get it correct now:
* Ca++ ion channels only transport electrically charged Ca ions, not Ca salts or another form of electrically neutral salt / calcium.
* By transporting charged ions into the cell, electrical charge builds up.
* Even small amounts of charged ions increase voltage difference in the cell significantly, that helps clarifying why Ca content inside the cells can be so much lower then in the plasma and still play an important biological role.
* This small amount of charged Ca++ helps counter natural diffusion of calcium and creates a balance that can be changed by active and energy / ATP costing ion pumping.
If so that voids some of the previous reasoning. Still, my gut feeling says if you are helped by calcium channel blockers quite well and if ME patients have both too few Ca++ and fewer calcium ion channels, then Ca++ “leak” from the inside of the cell through the outside may be a factor at play. Only the mechanisms would change widely from my initial ideas.
Would you know (rough guess) how widely calcium channel blockers help ME (or FM, POTS, dysautonomy…) patients? Is there a large percentage that gets significantly worse when trying them?
I’m guessing some would get worse as not all need to vasodilate and that’s what it does. I couldn’t take a true calcium channel blocker as it was too much. But there must be other properties at play with what I take. Tramadol works on all the neurotransmitters and if glutamate is an issue, maybe that modifies that. My best meds are a very small dose of Tramadol with a Bentyl and 2 vials of GastroCrom. The combination helps.
More later…….
Note: a lengthy comment on monocarboxylate transporters (MCTs) precedes this but seems to be lost; I’ll contact Cort in the hopes it’s just blocked before rewriting it.
First I’ll complete the above / missing by showing that these MCTs can not only transport neutral organic chemicals like lactic acid, but also salts:
“An acetate /ˈæsɪteɪt/ is a salt formed by the combination of acetic acid with an alkaline, earthy, metallic or nonmetallic and other base.”
The paper (on MCTs) states that these MCTs can transport acetate, and a combination of calcium and lactic acid seems to fulfill that definition.
=> MCTs very likely can remove Ca++ by the intermediate of (neutral or partly charged) calcium – lactate salts and MCTs out of the cells. This could create the observed state of too few calcium seen inside cells in ME patients. We sure are no stranger to too high lactic acid production needed for this mechanism to speed up.
Now how that relates to calcium channel blockers helping and ME patients having fewer calcium channels I have to figure out. My gut feeling says they enable leak of chemicals like C3H5O3Ca+ that have both properties that interact with MCTs and maybe with calcium ion channels. Still a crude guess.
So what mechanism might now deplete MCT levels?
* Very poor oxygenation / blood flow increase anaerobic functioning a lot.
* This increases the amount of lactic acid in the venous capillaries to very high.
* High levels of cell anaerobic functioning produce plenty of lactic acid inside the cells.
* As moving of lactic acid is helped (requires?) by MCT and strong levels of lactic acid in the capillaries make moving lactic acid from the cells towards the capillaries difficult, likely plenty of MCT is needed (“consumed, lost”) to do this.
* This creates very high levels of lactic acid inside the cells and, as explained in previous comment, this has high chances to create calcium – lactic salts that are moved out of the cells causing low intracellular calcium levels.
* Both low intracellular calcium levels and very high lactic acid levels decrease cell functioning.
* Due to the high need to shuttle lactic acid out of the cells, MCTs might be depleted.
* Depleted MCT levels further make reducing lactic acid levels inside cells difficult increasing its problem and, as explained in previous comment, MCT levels play a substantial to major role in ALL major energy producing pathways.
Now that does not sound good.
As to the role of uric acid? Maybe there is an analog calcium – uric acid mechanism. But at the very least high uric acid production from turning to proteins as a source of emergency glucose supply can create local uric acid concentrations high enough to form uric acid crystals blocking capillaries (increasing anaerobic cell functioning further) , creating massive local inflammation and may help calcium salts deposit on their crystals. Some sort of “dirt” is often used as “starter” for crystal formation.
There are different voltage gating calcium channels. We did antibody testing to see if I was having issues with these…..I wasn’t. (That was a surprise to me.) This gets pretty complex………
Note1: the internet ate this comment, this rewrite should be read before the last comment I made.
Note2: broken up into smaller parts; blocked due to length?
There are multiple reports of us ME patients producing easily increased amounts of lactic acid both in muscles and brain. It is also a common believe this happens among ME patients.
The few studies measuring it measure it by tapping blood from larger easy to access veins. I discussed elsewhere there is good reason to believe the local concentration of lactic acid is a lot bigger at the venous side of capillaries of tissue at work like muscles or brain.
The “elephant hiding in plain sight” I missed however was that this lactic acid comes mainly / near exclusively from the cells at work. Without active transport this would mean that the lactate must diffuse from the cells towards the capillaries. Diffusion happens from a higher concentration to a lower one, so if diffusion were the mechanism at work to remove the lactic acid from the cells then the concentration of lactic acid within the cells could be very very high.
In the previous comment I wrote calcium in cells is up to 12000 lower in concentration then in blood plasma. This can as the calcium is present as charged ions. A small amount of charged ions acts as a force expelling these ions out of the cells, countering the natural influx of calcium by diffusion into the cells.
Now if calcium were to react with lactate, then strongly increased lactate levels combined with really low calcium levels would help “react away” much of the calcium by forming calcium lactate salts. This would happen in both healthy people with normal lactate levels as in ME patients with strongly increased lactate levels. But the amount of calcium left in equilibrium should be significantly lower when very high levels of lactate are often present.
This leaves us to look into:
A) can calcium and lactate form salts?
B) can calcium ions and lactate form salts?
C) what are the mechanisms for transporting lactate and calcium lactate salts out off the cells?
Note: weird internet link formatting hoping to get through the spam filter.
Question A): wikipedia(Calcium_lactate)
=> yes, calcium forms salts with lactate and it has good solubility (easing the chemical reaction)
Question B): wikipedia(Calcium_lactate)
“Paradoxically, while the solubility of calcium L-lactate increases with temperature from 10 °C (4.8 g/dl) to 30 °C (8.5 g/dl), the concentration of free Ca2+
ions decreases by almost one half. This is explained as the lactate and calcium ions becoming less hydrated and forming a complex C3H5O3Ca+.
=> yes, it can form (partly charged) C3H5O3Ca+ and wikipedia explicitly states that it decreases the concentration of free Ca2+; this is important as calcium ion channels use ATP to actively try and pump Ca++ ions into the cells, this reaction with lactate reduces the amount of that Ca++
Question C): lactate appears to not be moved out of the cells by diffusion but by means of a specific transporter.
#internet link (ncbi nlm nih gov PMC2269375)
“The stereoselective transport of L-lactic acid across the plasma membrane of muscle fibres has been shown to involve a proton-linked monocarboxylate transporter (MCT) similar to that described in erythrocytes and other cells. This transporter plays an important role in the pH regulation of skeletal muscle.”
“Transport of lactate, or more accurately lactic acid, across the plasma membrane of all cells is catalysed by proton-linked monocarboxylate transporters (MCTs)”
The paper does provide another compelling bit:
“MCTs are also responsible for enabling the transport of pyruvate and the ketone bodies acetoacetate, β-hydroxybutyrate and acetate.”
=> lactate and pyruvate are essential for anaerobic glucose consumption
=> pyruvate is essential for aerobic (mytochondrial) glucose consumption
=> β-hydroxybutyrate is a key energy source in ketonic diets and is an important energy source during fasting and to some extend in the morning before breakfast is digested
=> acetoacetate en.wikipedia.org/wiki/Acetoacetic_acid
“In mammals, acetoacetate produced in the liver (along with the other two “ketone bodies”) is released into the bloodstream as an energy source during periods of fasting, exercise, or as a result of type 1 diabetes mellitus.”
“Acetoacetate is produced in the mitochondria of the liver from acetoacetyl coenzyme A (CoA).”
“The initial acetoacetate can come from the last cycle in the beta oxidation of a fatty acid, or it can be synthesized from two acetyl CoA molecules”
“First, a CoA group is enzymatically transferred to it from succinyl CoA, converting it back to acetoacetyl CoA; this is then broken into two acetyl CoA molecules by thiolase, and these then enter the citric acid cycle. Heart muscle and renal cortex prefer acetoacetate over glucose. The brain uses acetoacetate when glucose levels are low due to fasting or diabetes.”
=> Problems with these MCT transporters seem to effect/impede ALL major energy pathways by reducing their transport to places where needed!
Note that MCT (*very likely*) do not only transport these chemicals across cell membranes but also among membranes of other inner cell structures (think mytochondria as *potentially* affected; need more research)
=> acetate en.wikipedia.org/wiki/Acetate
“An acetate /ˈæsɪteɪt/ is a salt formed by the combination of acetic acid with an alkaline, earthy, metallic or nonmetallic and other base.” A salt formed of calcium and lactic acid seems to fit that definition
=> The above also means that that this readily formed C3H5O3Ca+ in the pressence of high lactic acid concentrations is moved out of cells by transport by MCTs. This depletes Ca++ levels inside the cells.
For low MCT levels, both genetic problems as well as “too high consumption” by having too high needs to remove lactic acid from the cells could deplete MCT levels and leave too few available for transport of the above mentioned fuels.
I did found one type of MCT genetic problem that is linked with energy metabolism en.wikipedia.org/wiki/Monocarboxylate_transporter_9:
“Monocarboxylate transporter 9 (MCT9, solute carrier family 16, member 9, SLC16A9) is a protein that in humans is encoded by the SLC16A9 gene…Clinical relevance…Mutations in the SLC16A9 gene have been associated with carnitine levels in blood.”
Note that carnitine plays an essential role in fat metabolism en.wikipedia.org/wiki/Carnitine
“Carnitine shuttle: Activation and transportation of fatty acids into the mitochondria”
Keep digging! Good info.
Also look up some of Remy post on TRMP3 she did some good work on that.
Issie
Dear Cort, I am thinking about doing surgery on my spinal stenosis. (I have to pay privately) Do you know anything more now about the outcome after surgery in ME/CFS patients? Thanks for your blogg!
Superb creation
This seems so positive. One symptom is feeling like your head would fall off, and I’ve often said it’s like my head is a concrete basketball sitting on a golf tee.
Are there any updates on the research into this? Is anyone actively studying it, and if not, why not?
Thanks for the kind words Alirza!
Hi Cort,
I just completed the survey, but was wondering if it a few of the questions could be modified? I am an hEDSer, diagnosed with NMH (neurally mediated hypotension instead of POTS), so since the options were only for “POTS,” I did not select. I am fused C1/C2 for AAI/CC1 and C1-T1 for spinal stenosis and myelopathy on some levels and severe instability on every level, and other issues. Somewhere in here it talked about cervical collars – I think you meant Aspen Vista maybe?
It can be very dangerous for a physical therapist or chiropractor to manually perform traction on a patient, especially if that patient has a connective tissue disorder. Would you please put a warning sign beside this question? Many EDSers (including be) do not see Dr. Bolognese (even though he is an excellent neurosurgeon) because he typically requires his patients to try traction (that he oversees.) I am glad that I did not see him because imaging showed that my vertebral artery was being impinged. Traction would have likely caused a stroke in me. Since EDSers have a higher incidence of vertebral artery ingements, physical therapists should not be doing manual traction with us, no matter how much it helps with the pain or how experienced they are. (I understand – I used to try it on myself before my neurosurgeon read me the riot act)
I just completed the survey, but I wondered if a few of the questions could be modified? I am an hEDSer, diagnosed with NMH (neurally mediated hypotension instead of POTS), so since the options were only for “POTS,” I did not select. I am fused C1/C2 for AAI/CC1 and C1-T1 for spinal stenosis and myelopathy on some levels, severe instability on every level, and other issues. It talked about cervical collars somewhere in here – I think you meant Aspen Vista maybe?
It can be very dangerous for a physical therapist or chiropractor to manually perform traction on a patient, especially if that patient has a connective tissue disorder. Would you please put a warning sign beside this question? Many EDSers (including be) do not see Dr. Bolognese (even though he is an excellent neurosurgeon) because he typically requires his patients to try traction (that he oversees.) I am glad that I did not see him because imaging showed that my vertebral artery was being impinged. Traction would have likely caused a stroke in me. Since EDSers have a higher incidence of vertebral artery impingements, physical therapists should not be doing manual traction with us, no matter how much it helps with the pain or how experienced they are. (I understand – I used to try it on myself before my neurosurgeon read me the riot act)
Although my fusions resolved many of my issues, I still have to live with hEDS, and I’m still searching for the best atypical trigeminal neuralgia treatments. These two things contribute to my fatigue, but I’m not nearly as disabled as before being diagnosed with AAI/CCI and then later with cervical stenosis, myelopathy, and instability from C2-T1.
I am 74 misdiagnosed for years just had MRI diagnosed Spondylosis bilateral pars fracture L5 for aminal stenosis of lumbosacral. Symptoms cognitive brain fog, claudification tightness in both leg calves, sciatica right leg, dysautonomia heat intolerance, nighttime incontinence, extreme fatigue, very difficult walking and depression/anxiety. Asking for similar cases, and suggested treatment, and results! Waiting on next Spinal Doctor appointment! Please help…
“It wasn’t clear what her canal diameter was, but her stenosis – ranging from C4 to C7 – was much more extensive than in the three cases Dr. Rowe reported on. Her surgery occurred six weeks ago. It’s too early to tell how effective it will be, but she will keep us informed.”
what news? thanks
Interesting that Patient 1 had a precipitating illness, Patient 2 seems to have had a sudden onset, and Patient 3 became unwell over four months.
If only we could travel back in time and scan them just before they became unwell.
Know of any doctors in Oregon who will support this? I’m in agony. My entire spine is affected.