


Linda Van Campen, Peter Rowe and Frans Visser met at a conference. The rest, as they say, is history.
The two Dutch researchers, C. Linda van Campen and Frans Visser, and Peter Rowe from the U.S., have been on a tear recently. The Van Campen/Visser team (mostly with Peter Rowe) have published 6 ME/CFS studies thus far in 2020, one in 2019 and three in 2018. This is the second of three blogs covering their recent work.
I asked Peter Rowe how a Johns Hopkins researcher came to work so much with the two Dutch researchers. What he said pointed to how valuable in-person conferences can be.
“Frans, Linda, and I met when Sonya Chowdhury and Action for M.E. invited us all to speak on orthostatic intolerance at the UK CFS/ME Research Collaborative 2017 Conference in Bristol, England. Frans and Linda have been collecting data very carefully during tilt testing for several years in their cardiology clinic that specializes in the evaluation and treatment of ME/CFS. Their database is a gold mine of information on changes during tilt, and they are both exceptional physiologists and clinicians.
We thoroughly enjoyed the discussions at the meeting, and wanted to continue working together, so have spent an hour or so on most weekends since 2017 on Skype calls, revising papers and debating how to interpret and present the data. Linda and Frans also traveled to Baltimore for 7-10 days during each of the last two summers, allowing us to work more intensively on research questions and comparing notes on clinical management. On top of all of the scientific productivity, we have a lot of fun working together.
Many ME/CFS clinicians are relatively isolated, especially in the European setting where CBT is still treated as the optimal therapy in some circles, despite the absence of good scientific support for that position. Building this small bridge between practices has been a source of encouragement and insight on both sides of the Atlantic, and we are all pleased that the publications have brought some practical benefits for patients everywhere.”
Van Campen, Rowe and Visser made history when they pretty definitively showed that just about everyone with ME/CFS experiences reduced blood flows to the brain on a tilt table test. If they’re correct, some form of orthostatic intolerance may be as integral to this disease as post-exertional malaise (PEM).
The Brain Fog in Orthostatic Intolerance … err … ME/CFS
Cognitive Function Declines Following Orthostatic Stress in Adults With Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS). Front. Neurocience .2020 Jun 26;14:688. doi: 10.3389/fnins.2020.00688. eCollection 2020.
The group elucidated the universal orthostatic intolerance (OI) theme in another recent study which showed that virtually everyone with ME/CFS gets cognitively challenged when subjected to a tilt test.
This large (n=128) study was composed of people who met the International Consensus definition of ME and the Fukuda criteria. (No healthy controls were included.)
One might have suspected the study was slanted towards people with OI since it was composed of patients suspected of having OI, but besides assessing the usual symptoms associated with OI (dizziness, heart pounding, concentration problems, etc.) the researchers also suspected OI in people experiencing “fatigue, a feeling of weakness, intolerance of low-impact exercise, nausea, abdominal pain, facial pallor, nervousness, and shortness of breath” – which includes just about everyone with ME/CFS.
The participants were given visual N-back tests – which you can do here – just before and within five minutes following the tilt table test.
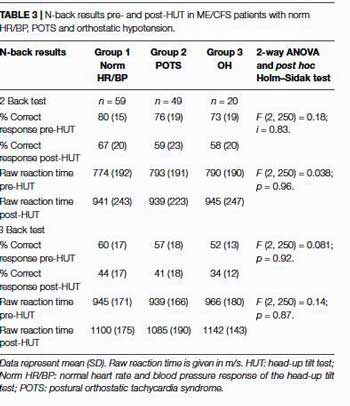
Notice how the percentage of correct answers and answer speed declined after the tilt table. (N-2 and N-3 cognitive tests were given)
After being tilted to 70 degrees for a maximum of 30 minutes (for those who could tolerate it that long), the ME/CFS group was separated into categories: those with normal heart rates/blood pressure responses, those with increased heart rates (postural orthostatic tachycardia (POTS) and those with reduced blood pressure (orthostatic hypotension). As in an earlier study the “normal group” was the largest group.
The ME/CFS group made more mistakes on the cognitive tests and took longer to do them after being tilted. (Slowed information processing is a key cognitive finding in ME/CFS.)
The ME/CFS patients with postural orthostatic tachycardia syndrome (POTS) or orthostatic hypotension (OH) didn’t do worse on the cognitive test than the ME/CFS patients without those disorders. Instead – everyone did poorly after being tilted.
The tie that appears to bind the POT and non-POTS patients together is low blood flows to the brain, and very possibly low CO2 levels as well.
Earlier studies may be illuminating what’s happening. They reveal that in the upside down world of ME/CFS/POTS, everything seems to be going in the wrong direction.
Cognitive testing in healthy people results in increased blood flows to their brain but Stewart’s 2012 ME/CFS/POTS tilt table cognitive testing study found that no such increase occurred in ME/CFS patients. Instead, some patients, paradoxically, had reduced blood flows to the brain. Instead of receiving more resources to meet the cognitive challenge, the ME/CFS patient’s brains either got no additional resources or were depleted further.
Plus, the increased vasomotor tone seen in the ME/CFS patients during the tilt table test suggested that the arteries leading to their brain had narrowed reducing blood flows. Here again, the POTS/ME/CFS patients proved to be contrarians: as their arteries constricted during the tilt test, the healthy controls arteries were actually getting larger (vasodilating).
With their brains getting little help – in the form of increased blood flows – and with their blood vessels apparently clamping down as they were tilted thus reducing blood flows – it was no wonder the ME/CFS patients had more trouble doing the the cognitive test following being tilted.
Small Tilts Produce Big Effects in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
Many people with ME/CFS have problems standing. They may be overt (dizziness, fainting, severe fatigue) or they may be more subtle (increased pain, difficulty thinking and forming words). Standing isn’t the only upright posture that tasks the cardiovascular system, though. As the Bateman Horne Center “hours of upright activity” (HUA) or “feet on the floor” measure indicates, even sitting can cause orthostatic problems.
In the next study “Cerebral Blood Flow Is Reduced in Severe Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients During Mild Orthostatic Stress Testing: An Exploratory Study at 20 Degrees of Head-Up Tilt Testing” Van Campen, Rowe and Visser next showed that a 70 degree tilt table test isn’t needed to provoke plenty of symptoms and a bollixed-up orthostatic response in more severely ill patients. In the these patients simply a 20 degree tilt from a supine position will do just fine.
Low blood flows to the brain and possibly reduced CO2 levels were associated with poor performance on cognitive tests.
Being tilted to 20 degrees for 15 minutes resulted in a 27% reduction in cerebral blood flows – a similar percentage to that experienced by more well off ME/CFS patients (26%) during a 30 minute 70 degree tilt table test. A significant reduction in stroke volume index (31%) was again similar to that seen in the healthier ME/CFS group during the longer 30 minute 70 degree test.
Despite the fact that these patients were hardly being tilted up at all, four of the nineteen patients met the definition for POTS. This study makes it clear that even small changes from a supine position can bring on a raft of negative physiological changes in the severely ill.
As they did with the earlier study, the authors suggest that lowered CO2 levels could be narrowing the blood vessels – thus reducing blood flows to the brain. Lowered CO2 levels are associated with hyperventilation or “overbreathing” which refers to a rapid and deep breathing pattern that expels larger than normal amounts of CO2.
A Focus on the Breath?
The author’s one clinical suggestion was that a focus on the depth and speed of the breath could be helpful.
“When hypocapnia is observed, a focus on respiration depth and speed has the potential to be one of the therapeutic guidance options for these patients to lessen orthostatic intolerance complaints.”
The Gist
- Peter Rowe met Linda Van Campen and Frans Visser at the UK Conference. Since then they’ve worked together on many studies, including six this past year.
- The entire ME/CFS group – whether they had a diagnosis of orthostatic intolerance or not – had reduced blood flows to the brain and reduced CO2 levels upon being tilted to 70 degrees for 30 minutes.
- The entire ME/CFS group – whether they had been diagnosed with postural orthostatic tachycardia syndrome (POTS) or not – displayed markedly reduced cognitive abilities after being tilted. They got more answers wrong and took longer to complete the questions.
- The Visser group’s findings suggest that orthostatic intolerance in the form of reduced blood flows to the brain and reduced CO2 levels may be as prevalent in ME/CFS as is post-exertional malaise.
- Severely ill people with ME/CFS only needed to be tilted to 20 degrees for 15 minutes to display the same degree of reduced blood flows and drops in CO2 levels as less ill people with ME/CFS.
- An earlier cognitive study in POTS found that in contrast to the healthy controls, blood flows to the brain did not increase in the POTS patients during the cognitive stressor. Plus, the arteries of POTS patients constricted rather than dilated, as occurred with the healthy controls.
The authors suggested that a focus on breathing depth and speed could be helpful in ME/CFS. That and hyperventilation will be the focus of future blogs.
The authors found evidence of hypocapnia, it should be noted, in the broad ME/CFS group (and it was worse in POTS). Hypocapnia is associated with hyperventilation – which has a rather long and somewhat tortured history in ME/CFS dating back to the 1990’s.Hyperventilation has been found more recently several times in ME/CFS but usually in just a subset of patients. Systrom, for instance, found it in a set of patients during an invasive exercise test. Medow prevented hyperventilation and, in fact, orthostatic intolerance during a tilt table test using phenylephrine.
It’s interesting that hyperventilation is not generally associated with fatigue.
- Check out a home test for hyperventilation here
Hyperpnea, which refers to deeper breathing than normal (without the increased rate of breathing found in hyperventilation), has been found in POTS.
Normal breathing, on the other hand, is often light and relaxed and comes from the diaphragm. If you’ve ever done meditation it’s astonishing how little breath the body needs – sometimes- just wisps of air effortlessly moving in and out of the nose is enough. That type of breathing is inaudible – no wheezing, panting, sighs, deep inhalations or exhalations occur.
Could changing our breathing patterns help?
- Coming Up – a Focus on the Breath


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!




I can’t wait for my dysautonomia testing results! I had the workup few days ago. This blog has perfect timing! Thanks Cort!
On the TTT, I got all wired up for HR, oxygen, and more. I noticed that at 70 degrees tilt, I felt somewhat nauseous and my feet were really sweating. Interesting that you would mention hyperpnea as I noticed I needed to take deeper and deeper breaths the longer I was on the table. I didn’t feint however.
I was also given a QSART test for how much sweat I generated on my arms and legs. I understand that it hunts for clues to see if one has small fiber poly neuropathy. They taped ampules of acetylcholine on my skin with leads to a monitor and then ran an electrical current through them. It was kind of like using a TENS machine.
Next was a test taking 9 very deep breaths in a row (supine) and slowly letting them out–rather like yogic breathing–following a lighted monitor above my head. I did this twice.
Finally, using the same lighted monitor, I had to blow into a tube and hold the force of my exhalations in a certain range for 15 seconds. I also did this twice.
I have mild symptoms of presyncope, but bad symptoms of fatigue. Although I don’t want to acquire yet another medical condition on my chart, on the other hand, it would be great if they discovered something that might be treatable.
I write this description for those of you who might have this testing in the future, and will report back on the next developments…
Thanks again Cort!
This is going to be so interesting, Nancy. Please let us know what you find out.
I had to blow into a tube once – it was an autonomic nervous system test I believe. I had never heard of these though.
Next was a test taking 9 very deep breaths in a row (supine) and slowly letting them out–rather like yogic breathing–following a lighted monitor above my head. I did this twice.
Finally, using the same lighted monitor, I had to blow into a tube and hold the force of my exhalations in a certain range for 15 seconds. I also did this twice.
Are you seeing a cardiologist or specialist in dysautonomia? I would love to hear how you got to take these interesting tests. 🙂
@ Cort; How did I get to see Stanford’s autonomic neurologist?
As you know I’m enrolled in Stanford’s Chronic Fatigue Clinic. I kept complaining about my dysautonomia symptoms and so I had to demonstrate them before I could get the referral.
I was instructed to take my BP and HR at home, first laying for 10 minutes then standing for three. I did this for about a week until I finally got a clear 30 beat difference between laying and standing. That fits the diagnostic criteria for POTS and so I was granted a referral.
Because of Covid I only had to wait a couple of weeks to get in and did have to get a Covid PCR test two days before my appointment.
The doctor’s name was Muppidi and was a very pleasant guy but unfortunately I saw him for only about 10 minutes while I was on the table. No interview questions except for the few comments I could get in before the TTT. Yes, he is very familiar with Ehlers-Danlos patients and he and the nurse usually do about 8 of these workups a day! My workup took close to 2 hours total.
I couldn’t ask questions during the tests. I guess they want you quiet so talking was not encouraged–except to describe any symptoms you are experiencing. It drives me crazy that I will have to wait until I can talk to my referring doctor to find out about the results. I guess further actions will depend on what they find…
You’re great Nancy, hacking a pathway through the undergrowth of ME/CFS healthcare!
Thank you for describing your work up, Nancy B.
And Tracey Anne, what a great description you have for her efforts: “hacking a pathway through the undergrowth of ME/CFS healthcare!”
Most of us can likely relate to this 🙂
@Nancy, to your question about seeing Stanford specialist for dysautonomia:
Try asking your primary care provider for a referral to see Dr. Mitchell Miglis, a neurologist who treats people with autonomic disorders. He is with the Stanford neurology department, and has a special interest in autonomic disorders and sleep disorders. He is familiar with both ME/CFS and POTS. My husband just started seeing him, and will be getting the autonomic testing done w/ Dr. Migilis in January. Good luck!
I would love to find out there are breathing patterns that help, especially with brain fog. I get through the day, but have relatively little time during which I can use my brain, and, as a novelist, this is a real problem.
I’m interested in that too – a blog on that will be coming up.
Would that then:
the implication being that the vessels are most likely constricting as a result of the CO2 build-up
and that adds more fuel to the fire and it is a terrible feedback mechanism that is formed.
and the breathing is wonky as a result from wonky mitochondria
– or can breathing wonkiness initiate the process?
Interesting that in hEDS – the theory with POTS is lax vein tone..
> > HOWEVER < <
my EDS-versed physiotherapist
noted that while I am breathing out, my ribs are not moving back in.
I need to use cues to remind my muscles to do that (develop neuromuscular connection)
it would mean I'm not expelling out all the CO2 – I have known this is a problem for me from over a decade ago, from when I used to swim.
So then:
Could a possible model of pathology in the POTS of hEDS
be stemming
from wonky muscle patterning in the breathing apparatus?
and not 'lax vein tone' as has been proposed?
i.e. not a connective tissue problem –
a neuromuscular one?
(either at the level of the central nervous system and/or the neuromuscular junction. myelin sheath, acetylcholine or…)
– lately I have been thinking this a lot,
that the hEDS problem is not one of hypermobility
it is one of 'neuromuscularity' 😀
based on my own experiences and some of my peeps –
(I bring this up
because
ME/CFS hEDS connection)x
and also,
maybe the joint instability (NOT hypermobility necessarily) + faulty muscle patterning
from neuromuscularity
is a combo more often going unnoticed in the ME/FS pool.
I’m maxed out from researching today
https://www.ncbi.nlm.nih.gov/books/NBK53082/
Cheers!
This is a really complex subject which I don’t even partly understand.
Metabolic acidosis – a build up in lactic acid – can start the process, though. Hyperventilation is a compensatory response to an increase acid buildup in the blood.
“Hyperventilation may be a cause of respiratory alkalosis or a compensatory mechanism for metabolic acidosis. Deep sighing respiration (Kussmaul breathing) is a common feature of acidosis (hyperventilation in an attempt to remove carbon dioxide) but may take some hours to appear.
https://patient.info/doctor/acid-base-balance#:~:text=Therefore%2C%20hyperventilation%20may%20be%20a%20cause%20of%20respiratory,dioxide%29%20but%20may%20take%20some%20hours%20to%20appear.
I have no idea if that’s happening in ME/CFS.
Stewart found that low blood flows to the brain came first in POTS and were followed by reduced CO2 levels which then narrowed the arteries – impeding blood flows to the brain further..but low blood flows to the brain came first.
Then you show that in hEDS a muscle contraction problem may be present. It’s interesting that the little muscles that move the diaphragm are among the most used in the body. If there’s a problem with energy production it could show up there (Staci Stevens).
Certainly the idea of improper activation of the breathing apparatus is on the table….
There’s a person, she treats her MCAS with a sodium/potassium mix. It also helps her POTS. When I looked into trying it, I saw in Europe they sell these mixes (with magnesium and calcium added sometimes too) as basic powder. I thought that made sense, because with the energy production being off, oxidative stress – that changes the charge of the cell, right? So stabilizing PH to basic, would help with everything.
(her site has been running for a few days, I hope she gets it running again: https://www.mastcelldisease.com/my-new-all-natural-rx/)
– – – – –
What about neuroinflammation?
How do this findings start to connect with the neuroinflammation ones – are any of the researchers looking at that actively?
Sometimes it seems to me that every scientist is working on their corner of things, and in the end, their work will indicate the workings and underpinnings of the dysfunction. I wonder – is there one that is looking at the different outputs from the different teams in their totality. i.e. the bigger picture, someone who maybe can make the connections?
Is there anyone whose ‘job’ is too look at the big picture?
You have written before about these informal get-togethers organized by OMF….
😉
Wait: could someone explain how does lactic acidosis differ from POTS?
Exactly the same symptoms:
“Symptoms of lactic acidosis include rapid breathing, excessive sweating, cool and clammy skin, sweet-smelling breath, belly pain, nausea or vomiting, confusion, and coma. See whether the right amount of oxygen is reaching the body’s tissues.”
When you say that Stewart found that low blood flows came first:
then it would seem that triggers the lactic acidosis.
For some reason, this is happening when we are upright.
POTS is a case of lactic acidosis?
So then the treatment of the bicarbonate sodium and potassium would certainly be a very good way to address it, until we know why blood is not flowing to the brain.
It’s inexpensive, no medication with side effects. it also covers all your bases instead of having to take medicine for the heart plus ssris + salt + compression tights + etc
?
For reals, is it this simple?
♩ ♪ ♫ ♬
it is “strange” to read it here because i know 2 people verry severe who go to visser and van campen. 1 is at the end of her life , also severe pots, gets no treatment at all for it, the other one to.
About hyperventilation, if you are so weak you even can not breath properly anymore or swollow due to muscle issues and even with trying to train your breathing muscles but it only gives you more muscle weakness from pem, i have my doubt of hyperventilation only and treatable, also knowing from the 2 that are going to visser…he does not treat neither of them for severe pots or oi
on paper, all the researck looks so good until you know them and what they do or do not… I can not speak for the us scientist! SO ,,,
Unfortunately, while I think we’re getting closer we have not moved much if any further on the treatment end. That will probably take diving deeper into what’s actually going on – finding the cause of the low CO2, the reduced brain blood flows, the energy production problems, the low blood volume, the blood vessel issues, the small nerve fiber issues. Things do seem to be cohering – I hope so at least.
Cort this is my 3rd try today to get a comment to you. Keeps coming back either name is missing-(no) e-mail is incorrect (n0).
I am now having severe dizziness and my bp is dropping to 100/40 low sometimes HR is fast when this happens sometimes slow. I have to lie down. Can’t drive. I do have CMV, CFIDS, Severe fatigue and dizziness. This is will be my last time to try and reach you today. I am worn out. I also have Athrosclerosis-where blood cannot flow to my brain as it should?I also ue a Cpap machine and an elevated bed. (head)
Darn Carole, that is rough.
Have you been able to see a dysautonomia specialist or a good cardiologist? (List here on Dysautonomia International – http://dysautonomiainternational.org/page.php?ID=14) Here’s the criteria for orthostatic hypotension (drop in blood pressure upon standing) Blood pressure drops from usual of 120/80 to 90/64 mm Hg after several minutes. You certainly meet the diastolic drop in spades and if you kept measuring I imagine you would meet the systolic.
OH can be caused by many factors. Like all kinds of OI prolonged bed rest can unfortunately exacerbate it.
One approach to OH is to increase blood volume and we have a blog coming up on that. Drugs can also be helpful including Mestinon, midodrine (Orvaten), droxidopa (Northera) and fludrocortisone.
Sometimes you have racing heartbeats as in POTS. POTS can occur alongside OH.
I hope you can see a good cardiologist or dysautonomia specialist.
C ort- Thanks you for your reply =I am getting pretty desperate at this time. I will ck with the association and org you suggested. I just hope we have someone here that is familiar with this . I live close to the CDC—but no help there so far.
Thanks again.
Carole
Carole Rushing and Cort, just wanted to say I have had great success with Mestinon.
Hi cort, do you maybe know for what kind of OI, pots, nmh, etc what treatment is? I want to “go” laying down to visser and you can lay down there to. It will give a huge crash of wich I may not recover maybe, but if i do the effort, i want at least be treated. I was yesterday so ill, with one person with verry severe pots for long time, at the end when she was tube fed, could nothing anymore, he gave mestinon a try. Alittle bit late i guess 🙁 but wanted to set that right. when i read posts from what some people in the us get all for tests and treatments, we live here 100 years behind. Wanted to go to scheibenbogen for auto-immune subset and immunesystem but she only takes people from berlin and 1 place around berlin (germany) so not for me and here are not many options…
or wich kinds of pots, oi, nmh, etc are allready found and maybe verry short the differences?
I’ve tried to send two comments + links, on my computer – (I’m usually on my phone) and they didn’t show.
Cort did a blog on HR called ‘A Mestinon Miracle: Vagus Nerve Stimulating Drug Helps Long Time ME/CFS Patient Exercise’ in 2016. Anyway I did try to do the link – it went off as usual but then didn’t appear. Same thing happened earlier today but thought I wasn’t concentrating or the links were rejected, or something. But this time I was paying attention.
So, I’ll try and send this and see what happens…
in my case, long long time ago when i could see a specialist once in a while still, several pneumologist found no low level of CO2, 1 time to low 02, peripheral and respiratoire severe muscle weakness and an abnormal reaction to the med for astma, was even worse then with my lung capacity! this one did not understood a thing from where it came and with further testing i even did not have astma.
But i know, feel, when my ribs hurt together with the rest of my many pains, i feel no strenght to speak or swollow and the weakness of my boddy and the pem more weakness and other symptoms. So it must be something else i think…
Systrom has found several subsets thus far – one of which was characterized by hyperventilation and one of which was characterized by mitochondrial problems. Each of them, if I remember correctly, had problems with oxygen utilization – but coming from different places. Maybe you are in the energy production problem boat. (???).
thank you cort! wish research was faster on all of us, we are so complex and sometimes so different in our illness.
I live in hope for a future where people with ME/CFS do not have to live a life of isolation in their own private ghetto.
Equality of access to appropriate healthcare needs to be available to all; without prejudice and misinformation creating an invisible barrier to this being achieved.
Konijn, I would be so relieved if you were able to find some sort of support with your very difficult health issues.
Tracey 🙂
Thank you for posting this Cort, I found it a fascinating read. My ME started after 6 years of chronic carbon monoxide poisoning during which time the oxygen and blood flow to my brain would have been impaired. For the past year or so I have invoked a daily diagphramic breathing practice (along side all the other things I have done over the past 8 years of having ME). I have been the most active, upright and able to stand for lengthy periods these last few months than I have been able to in all my years of having ME. Reading your write up about the study makes me believe my physical improvement coinciding with my introducing diaphragmic breathing is not mere coincidence. Once again, thank you for posting this.
So the big question is why? What’s causing this? These studies are great but we need more on ‘the why’.
Is lack of fitness a factor, have the researchers controlled for that?
I’ve had some new symptoms show up the last few months – breathing issues. A chest x-ray showed that my lungs are hyperinflated. O2 saturation was 86 at PCP’s the other day. Don’t know if this is related to ME/CFS or something else. I get more short of breath than I used to and my lungs are congested. I feel as if I’ve become a “lazy ” breather because it takes a lot of effort. Is anyone else experiencing this?
Forgot to mention that I have a moderate pectus excavatum chest deformity which further restricts breathing.
I have a bit of the flip side of the coin – my rib cage sticks out. This is the marfanoid habitus: sometimes high arches, sometime flat feet. Sometimes chest sticks out, sometimes in.
I do have muscle patterning imbalances that my muscles do not fully activate to exhale (my ribs don’t come back in fully, I don’t get air out fully)
And also when I lay on my side, my lungs feel funny and I get coughing fits….
When I attempt to work on diaphragmatic breathing, the back of my throat hurts. It seems like I’m basically engaging all the wrong muscles, and the ones that should be active, are sleepy.
The muscle pattern imbalance = hEDS 101
Thanks Meirav. My ribcage also sticks out and I suspect I have some Marfans type issues. Am wondering if my hyperinflated lungs (don’t get air out fully) are a structural problem that has always been there, but as I age (now 65, female) it is getting worse. I was told by a PT that I need to breathe up and down and side to side. It’s difficult for me to breathe “front to back.” My ribs and chest don’t seem to want to go in that direction so unless I breathe consciously I don’t get enough air – just wondering.
Hi, I too had pectus excavatum (PE). It was surgically corrected, and my orthostatic intolerance has greatly decreased. It was the most effective intervention for my ME/CFS in 34 years. Patients with PE are incapable of breathing with the upper part of the rib cage (the thorax does not move outwards, just upwards when breathing in). Even when the deformity is corrected breathing remains somehow defective. As you age your breathing will get worse because the height of the torso is getting smaller, especially for women, due to osteoporosis and subsequent loss of bone density -and height- of vertebras. PE does not only restrict breathing, but also affects the heart per se. In my case I had a heart compression. The space between the back of my sternum and my vertebra was just 2 cm. Now it is 11 cm, and my heart is no longer squeezed. Unfortunately surgery was performed too late (at age 45) and heart failure with a right ventricle dilatation has already started.
Isa, Interesting information that you presented. I just came from the emergency room. So worn out from trouble breathing. I told the ER doc about my pectus excavatum and he told me that it didn’t have anything to do with my current breathing problems. I don’t believe that.
Anyway, that must have been a big surgery to correct a PE. I have seen pictures on the internet with rods going across the chest. Glad you are doing better. I am having multiple cardiac problems and they are always dismissed by the cardiologists. So tired of the medical community not taking our complaints seriously.
Tanja, I can relate. For years I was told my PE was just a “cosmetic problem”. I could not stand up, and apparently the solution was breast implants… I was told my heart was fine. It is only when I said I wanted, not an opinion, but a measurement of the space my heart had that the extent of the problem was noticed. Surgery was indeed very difficult. I contacted the best 4 surgeons in the world (those who have an experience with fixing PE with a Nuss procedure on patients over 40 years of age). Only one accepted; the others said it was too risky. Before surgery my maximal ventilation capacity was just 47% of what it should have been for someone of my gender, age and height (that is less than half of a normal person’s and allegedly all was ok with me!). Now it is 93%. After surgery I was amazed by the amount of air I could breathe. I never knew this was possible. My sleep pattern was also modified. Instead of sleeping 11 hours a day, I now sleep 9 hours a day. Interestingly enough this is the case with all PE patients undergoing surgery even when they do not have ME/CFS. People with PE sleep longer (probably because their oxygen intake is too low). The more recent article I read mentioned PE as a cardiopulmonary disease. So it starts being well known. This is the article about ageing and lung capacity: https://www.eurekalert.org/pub_releases/2016-12/ats-lfd120116.php
Interesting that your sleeping improved. The recent discovery of the mechanism of brain flushing during sleep, of it being dependent on the interaction of the blood pressure and the CSF pressure, seems to be again involved in “our” sleep difficulties. If the blood flow is weak, on top of the CSF hypertension, that brain flushing might well work even less efficiently than having only one of the two problems. And if a range of maladies may cause this combination, and the end result in all cases is a chronically-poor sleep, the general symptoms might end up being somewhat similar.
WoW!
Isa,
From what I’m gathering, the medical literature says that only severe cases of PE affect breathing and the heart.
My guess is your doctors dismissed your case as not severe in their eyes, and hence dismissed the complications?
Do you mind if I ask if your PE presents with marfanoid habitus as well and a known connective tissue disorder?
😉
Hi Meirav,
I have an appointment later this year regarding a potential diagnosis of Ehlers-Danlos Syndrome. And you are right. The so-called reasoning is: BECAUSE pectus is cosmetic THEREFORE all cardiac symptoms are unrelated, and because those cannot be explained in any other way, well they don’t exist or are exaggerated (“she’s a woman, neurotic as all women, isn’t she?”) … The severity of pectus can only be measured by a scan. Watching a dent in a chest is useless. Eventually the vast majority of PE patients develop complications later in life (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3077846/). Unfortunately at a time when effective surgery is no longer possible.
To clarify, no doctors ever dismissed my case as not severe enough. None of them even checked whether it was severe or not. It was automatically dismissed. It was because one day I myself said I wanted a measurement of the space between the back of the sternum and the vertebra. For 10 years I asked doctors whether my pectus could explain my symptoms. I was told, “no, you don’t understand, it’s just cosmetic”. And one day I said, “I do not want an opinion, I want a measurement”.
I remember a chat with a German thoracic surgeon who told me that thoracic surgeons have been publishing studies and organising conferences for more than a decade to make cardiologists aware of the problems PE causes in many instances, but they are ignored. Cardiologists have their dogma, and they stick to it. The problem is that patients first see a cardiologist who will dismiss them. They don’t see first a surgeon.
Isa – that is so strange. I think in a different circle, doctors would quickly know that PE doesn’t present alone, that it is one trait of an underlaying condition.
What do you think about publishing a website
with the details of your story,
and information how to approach a doctor if one wanted to have this investigated?
Raise awareness.
Very often in reading medical literature, the complete list of traits in a syndrome are omitted.
So it is difficult to see oneself in those descriptions, and people and doctors may dismiss it.
It is in reading clinical case reports and other people’s stories,
that one may begin to identify and go – this sounds a lot like me.
PE is seen in a number of conditions:
Marfan – which can be a differential diagnosis for EDS.
Classical homocystinuria – which can be a differential diagnosis for Marfan.
Maybe other types of homocystinurias as well – I can’t remember off the top of my head.
Maybe other connective tissue disorders.
Hypophosphatasia also.
I posted a thread on the forums with information on that.
Do check it out.
Since hEDS is a clinical diagnosis for now,
maybe get checked out for the inherited metabolic disorders as well?
I think some of us have that at play –
either we are not being diagnosed correctly
or we have a dual diagnosis.
Or have only one copy of one defective gene and it adds up.
Very much like you told you doctors you didn’t want an option,
you want a work-up, evidence, before a diagnosis can be ruled out or confirmed.
I am of the opinion that doctors do a good job of ruling out common conditions before arriving at the clinical ones of FMS / ME/CFS / hEDS
Due diligence in ruling out rare ones is missing.
With evidence.
It’s so easy too – the tests, B6, plasma amino acids, urine organic acids.
I have been reading in a hEDS forum that some are finding certain mutations affecting fibrin. So a genetic connective tissue panel.
If you are interested, I have medical literature on all these conditions and how to go on about approaching your doctor, etc.
i find the better informed I am,
the better I do at advocating for my health.
Meirav,
Regarding my experience with the medical profession, it is not that strange really. The default mindset of the medical professional is negative even though it slightly depends on the age of the patient. Facing a teenager, the thought is “she is a nasty little brat, she needs discipline and ‘tough love’ “. With an adult in her 20s or 30s, “she wants it all, but she’s too weak to get it, so she’s malingering to cover her failures. She can’t even handle this appointment. Look at her tremor! Too ambitious for her abilities. She cannot even speak, her voice is so soft. No personality”. When you approach middle-age, “she’s neurotic, and is bored with her family life”.
So the person in front of you is not trying to identify what medical problem you may have. The cognitive bias is to find clues to comfort their gut feeling that you have nothing and you do not deserve their attention. Hence they’ll think, “nope, PE is often just cosmetic, no point to investigate, especially as there is no real treatment. Orthostatic intolerance? nope, it’s just because she is on a diet. Look at her, she’s skeletal. She just needs a good sandwich.” And I could go on and on and on…
The only advice I would give to a patient looking for help: NEVER EVER SAY YOU HAVE ME/CFS, just talk about the specific symptom you want to be helped with.
Regarding raising awareness about pectus there used to be a site, pectus.com, with dozens of adult patients (including me) sharing via a forum their stories, sharing studies and discussing surgical techniques. Unfortunately the forum has been down for over a year now, and I’m not sure if and when it will be back. Generally speaking patients reported they had difficulties being heard by the medical profession and were often dismissed. But they have some major advantages. Firstly, pectus is visible, and secondly, those patients have more stamina to argue their point. They can go and see a specialist thousands of miles away. Thirdly, there is no mental health stigma attached to the condition. So people are not afraid to talk about it.
The PT is just garbling sounds to me, alien beings. I don’t know what use your sides and up and down and.
I have to ask her to tell me which muscle(s) i’m supposed to be using.
I can sort of figure it out from there.
Takes a few repetitions to get there.
If she uses her hands on my muscles to direct movement or cue it
it helps tons
Need tons of tactile feedback.
Marfanoid habitus is also seen in a number of conditions – hEDS and classical homocystinuria included.
I had been trying to find a physiotherapist that knows breathing well.
They can help with muscle re-patterning.
neuromuscular re-education: to engage the right muscles, and to ‘turn off’ the ones that are working when they are not supposed to.
To get the body to work as one unit, in concert.
The more you practice, the more ‘automatic’ it becomes.
It seems we need to work on that constantly, remind our muscles how to move.
That’s also what Feldenkrais does.
Have you tried it?
I like Alfons
https://www.youtube.com/c/FeldenkraiswithAlfons/videos
One-on-one sessions is good to.
You don’t have to go to the full range of motion like he does.
Even with people who are in too much pain and cannot move,
you imagine dong the movement and that already fires up the neuromuscular connection.
Minimal movement is all that is needed.
The floor provides feedback in Feldenkrais.
and Jeannie has a little something
https://youtu.be/GK8rKm9ApE0
https://www.youtube.com/watch?v=YY87e2F1yLA
(I’ve been lazy this summer… need to get back on the physical stuff)
Interesting research from Harvard linking fatigue in MS with microglia activation. Mentions CFS a few times. https://nn.neurology.org/content/7/5/e854
It makes sense for the blood vessels to squeeze while dilating for the respiratory frequency to become deeper or faster. Hyperventilation is a physical abnormal response in ME / CFS / POTS. There seems to be an opposite reaction. At rest, ME / CFS / POTS patients are running. Why?
Has anyone come across Dr Daniel Siegel before? I find him easy to listen to and entertaining too. He has all sorts of videos on You Tube on the nervous system and I’ve watched lots of them.
One I came across is ‘Dr Dan Siegel’s Hand Model of the Brain.’ It’s 8.15 mins long and I think he explains the different aspects of the brain, in terms of the nervous system, in easy to understand terms.
https://www.youtube.com/watch?v=f-m2YcdMdFw
Dr. Anthony Fauci was recently interviewed about the potential of monoclonal antibodies to treat Covid. In his comments, he said that these antibodies could be used to create any chronic virus. Have they been used in ME/CFS and if not, why not?
https://www.medpagetoday.com/podcasts/anamnesis/88367?utm_source=Sailthru&utm_medium=email&utm_campaign=Weekly%20Review%202020-09-06&utm_term=NL_DHE_Weekly_Active
Wondering how this finding relates to the recommendation that elevating the head of the bed slightly can be helpful?
The trigger point at base of skull (neck/back) (easily massaged by DaVinci Tool, finger works too but is harder, probably there is other massage tools too) leads me to have very relaxing satisfying deep breath. Afterwards less brain fog and less feelings of fatigue / not being able to stand.
Can this be in any way related to CO2 levels?
Hi – I’m making a new comment her.
Started a reply thread above – and afraid because it is nested, it will be missed.
Could someone take a look further up, towards the beginning of the comments.
It’s about lactic acidosis + POTS + OI + potassium and sodium bicarbonate as treatment.
Could it really be this simple,
ehn?
Meirav
✏️ just an idea
i wonder when inserting/nesting a reply
to an alrready long thread /discussion
if a colorful emoji could be added ?
➕ that might catch the eyes of those ? scrolling down to recent part of the thread?
♩ ♪ ♫ ♬
😉
In your linked page to a home test for hyperventilation there may be a typo:
It says
“Repeat the test but time breathe into a paper bag held across your nose and your mouth. If your symptoms appear when you are breathing into the bag you may be hyperventilating.”
Souldn´t is say disappear instead of appear?
“Repeat the test but this time breathe into a paper bag held across your nose and your mouth. If your symptoms DISappear when you are breathing into the bag you may be hyperventilating.”
Best
Herbert
I think so! Thanks
About the home test for hyperventilation: breathing into a bag will actually make you breathe more, because when you are a chronic hyperventilator you are extremely sensitive to CO2 increase in the blood. That’s also why you can’t hold your breath for long, because increase in CO2 is what triggers inhalation. A better way is to test your Control pause/BOLT score (terms from Buteyko method).