

(Jeff Wood’s remarkable recovery following spinal surgery to correct craniocervical instability (CCI) and tethered cord shocked the ME/CFS community. It’s safe to say that almost no one saw that coming. In this piece Jeff – the former ME/CFS patient who started all this off – proposes that the pain, fatigue, etc. in ME/CFS could potentially all be explained mechanically.)
I invite you to engage with me in a thought experiment.
Connective tissue is pervasive throughout the body. Could problems with it be causing ME/CFS?
One of the central puzzles of myalgic encephalomyelitis is that multiple triggering events can lead to ME — viral infections, Fluroquinolone antibiotics, impact trauma, surgery, pregnancy, overtraining, mold exposure, and others — yet the symptoms of ME are consistent.
I have a proposal that might possibly explain this: Perhaps all these triggers lead to a failure of the body’s connective tissue, and perhaps some people’s connective tissues are more vulnerable to failure in response to these triggers.
We often associate connective tissue with ligaments and tendons, but it’s more pervasive than that. The three membranes that envelop the brain and spinal cord, for instance, are composed of connective tissues. The blood vessels, too, are composed of connective tissue.
In turn, every symptom of ME could be accounted for as a chronic, ongoing brain and spinal cord injury that occurs as a result of connective tissue failure. Exertion would result in physical trauma to those neural tissues.
A Hypothesis to Explain ME
I am proposing that ME, as defined by any current or historical criteria, is a chronic, ongoing traumatic brain injury and spinal cord injury – that often results from connective tissue damage.
More specifically:
- There is chronic, ongoing mechanical distortion of neural tissue that is further distorted by movement.
- The area impacted by the distortion can be the brainstem (including the cranial nerves), the spinal cord, or, perhaps likely, both.
- There is chronic, ongoing disturbance of blood flow and cerebral spinal fluid flow (these two concepts are together described as “craniospinal hydrodynamics”).
Let me acknowledge explicitly: I don’t have proof at this point that this hypothesis is true. My purpose here is to suggest reasons that this hypothesis might be true, and that we should follow up on the idea with research to confirm or disprove it.
Also, please understand I’m not suggesting that neurosurgery is the only solution for mechanical conditions. While a number of people with ME have corrected their underlying mechanical conditions with neurosurgery, there is an expanding universe of creative ideas for addressing mechanical conditions without neurosurgery.
Part of what I hope will come from exploring a mechanical paradigm of the disease is the development of methods less invasive, and less expensive, than neurosurgery.
Ongoing Traumatic Brain Injury: The Potential Role of Faulty Connective Tissue

Could every movement be producing a micro-traumatic brain or spinal injury? (Image by kalhh from Pixabay)
A traumatic brain injury (TBI) is traditionally thought of as a onetime occurrence: say, someone falls down, hits their head, and suffers a concussion. A spinal cord injury, too, is usually thought of as a onetime event.
I’m proposing, though, for someone with ME, these injuries aren’t “one and done” events. They are ongoing events, perpetuated by small daily micro-TBIs and spinal cord injuries that occur when we physically move.
My hypothesis is these micro-TBIs result from a failure of our connective tissue to hold our body in place. In turn, every time someone with ME engages in exertion, their neural tissue is essentially getting battered and “beaten up” and their blood and cerebral spinal fluid are being disturbed. Every time we move, we give ourselves a micro-TBI and spinal cord injury.
If that’s true, then post exertional malaise (PEM) could be considered a consequence of mechanical trauma. PEM would be the unavoidable consequence of experiencing a brain or spinal cord injury.
In the past few years, multiple people, including myself, have recovered from ME by treating craniocervical instability (CCI), and this condition illustrates one way that micro-TBIs could perpetuate one’s illness. In the case of CCI, the ligaments and joints of our skull and upper cervical vertebrae are no longer holding our skull and upper neck in place. These damaged ligaments allow excess motion at the junction of the head and neck, and this motion can mechanically beat up the brainstem, deforming it. This could explain the 1995 finding of brainstem hypoperfusion, or a lack of blood flow to the brainstem, in ME patients. (See: Brainstem perfusion is impaired in chronic fatigue syndrome).
Instability of the skull and upper neck could also explain how in people with more severe ME, even such minor exertion as talking softly while lying in bed or chewing a soft meal can exacerbate symptoms.
CCI is not the only way that mechanical problems of the craniocervical junction can cause ME symptoms. Distortions in blood or cerebrospinal fluid (CSF) through this area due to Chiari malformation, CCI, or other problems can also occur. Some problems involving craniospinal hydrodynamics include:
- Too much blood backing up in the brain due to lack of outflow.
- Too much cerebral spinal fluid, resulting in increased intracranial pressure.
- Cerebral spinal fluid leaking from a hole in the dura (connective tissue membrane), resulting in intracranial hypotension.
These are all mechanical problems — and this is just a partial listing. There are additional mechanical problems that can affect other parts of the nervous system, too.
Connective Tissue Problems With No Known Connective Tissue Disorder
Mechanical problems of this kind are better understood in Ehlers Danlos Syndrome (EDS) – a connective tissue disorder. Dr. Ron Davis has estimated 50% of people with ME meet the hypermobile hEDS criteria. However, many people who have developed ME – including myself – do not.
A surprise that’s emerged in the last few years is that some of us with ME, who don’t meet the criteria for hEDS or for any other known connective tissue disorder, nonetheless have faulty connective tissues. I believe that the criteria used to diagnose known connective tissue disorders may not capture all of us.
Until my own case, it was broadly believed that the only way anyone could develop CCI was from impact trauma (like a car accident), rheumatoid arthritis, Downs Syndrome, or through having a known connective tissue disorder. Since my case, though, we’ve seen multiple ME patients, both with and without known connective tissue disorders, recover from ME when their mechanical problems were addressed.
Many Mechanical Conditions
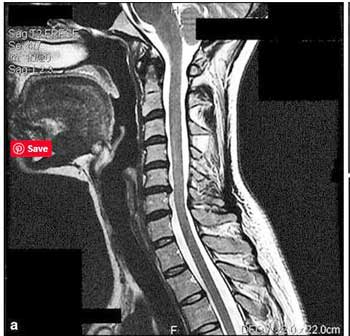
Spinal stenosis in a person with ME/CFS who recovered following surgery.
I use the term “mechanical” because it captures the nature of an ongoing, chronic traumatic brain and spinal cord injury, exacerbated by movement. While there’s been a recent focus on CCI, multiple structural neurological conditions can exist in our population, and each of these is caused by problems with the connective tissue. In addition to CCI, here are some of the mechanical problems we’ve been seeing in ME patients: Tethered cord syndrome, Chiari malformation, cervical stenosis, venous stenosis, median arcuate ligament syndrome (MALS), and Eagles syndrome.
These mechanical conditions can lead to:
- Chronic distortion of neural tissue in the brain, brainstem, cranial nerves, spinal cord, etc.
- Compression, stretching, and other mechanical forces can cause problems.
- Not enough blood getting to the brain in the proper way (cerebral hypoperfusion).
- Too much blood backing up in the brain.
- A nuanced, fluctuating combination of the above.
- An overall dysregulation of blood flow and cerebral spinal fluid, along with mechanical neural tension deranging the nervous system.
- In turn, this can activate, strain, and derange the mechanisms the body mounts to compensate, e.g., attempting to achieve functional homeostasis.
Dr. Peter Rowe believes connective tissue/nerve elongation problems are causing symptoms of pain, fatigue, brain-fog, light-headedness, nausea, sweating and flushing, headache, etc. in young people with ME/CFS when they move. Additionally, Dr. Rowe has published a case series of women who recovered from severe ME after treating cervical stenosis.
In 2020, Swedish researcher Bjorn Bragee found that 80% of ME patients had craniocervical obstructions, 83% had signs of intracranial hypertension, and 50% had hypermobility. These are all mechanical conditions, and they are all associated with connective tissue problems.
The good news is that these mechanical problems are identifiable, measurable, and treatable. Over just the last year, mechanical problems have been found to be causing, or contributing to, ME symptoms in hundreds of people. The number continues to grow as more people with ME pursue evaluation. But at this point, only a small percentage of us have been evaluated.
But, What About the ME Outbreaks?

Some mechanical problems can result in disturbed blood or spinal fluid flow.
Many ME patients — including those with a confirmed mechanical basis to their ME — have had viral onsets. At first, it might seem like viruses are unrelated to connective tissue damage. But in fact, we know that the immune molecules released to defend ourselves against viruses also damage collagen, a key ingredient in connective tissue. Whether an infection is tick born, viral, bacterial, doesn’t seem to matter. Any of those infections could initiate a breakdown of collagen.
It is not hard to imagine that the outbreaks throughout documented ME history could have a connective tissue component because of, rather than despite, the infectious component.
I suspect that some people already have vulnerable connective tissue prior to an infection. They would be more prone to connective tissue breakdown from an infection, or the infection might be the straw that broke the camel’s (connective tissue laden) back.
But viruses aren’t the only thing that lead to connective tissue damage, and that could explain how the experience of patients with viral ME onsets can be similar to those without them.
Traumatic Brain Injury: Physical and Cognitive Fatigue
A considerable body of scientific literature connects TBIs to fatigue. This literature generally discusses the TBI as a “one and done” event, resulting in a temporary aftermath of physical fatigue. But what might happen if we were experiencing a perpetual series of TBIs, made worse every time we move or exert ourselves?
What might living with ongoing micro-TBIs feel like?
It might leave us in an ongoing state of fatigue, lasting years, reliably worsened by exertion.
We can also see, in the published literature, that brain injuries result not only in physical fatigue. They can also result in cognitive fatigue. Many of us experience PEM following cognitive work. The overlap between TBI and ME symptoms is striking.
Through a Mechanical Lens: Graded Exercise Therapy (GET) and Pacing

Jeff proposes that mechanical problems could explain why graded exercise approaches fail.
Consider: Why might graded exercise therapy (GET) be harmful for many people with ME? The mechanical paradigm offers an explanation. By forcing someone with ME to move their body and exert themselves, GET could perpetuate connective tissue injury and ongoing micro-TBIs and spinal cord strain, as well as further derange cerebral spinal fluid and blood flow. This could, in turn, worsen the baseline condition of people with ME.
Also consider: Why might pacing, or intentionally limiting physical exertion, help protect people with ME from getting worse? The lack of exertion would prevent a person with ME from giving themselves micro-TBIs, spinal cord strain, and deranged cerebral spinal fluid and blood flow. Through limiting these mechanical harms, pacing would then reduce the severity of symptoms, or even maintain or increase a person’s baseline functioning.
Neuroinflammation, Immune Dysfunction, and Mast Cells
Within the ME community, among scientists and patients alike, there is an understanding that people with ME can exhibit the following: neuroinflammation, immune dysfunction, and mast cell activation.
Interestingly, traumatic brain injuries of any kind lead to neuroinflammation, immune dysfunction, and mast cell activation. Some consistencies between ME and traumatic brain injury can be seen in the article, “Mast Cell Activation, Neuroinflammation, and Tight Junction Protein Derangement in Acute Traumatic Brain Injury”:
TBI activates glial cells and immune and inflammatory cells, including mast cells in the brain associated with neuroinflammatory responses. This can, in turn, cause secondary brain damage.
TBI can cause mast cell activation, neuroinflammation, and a derangement of the tight junction proteins, and this is associated with increased [blood-brain barrier] BBB permeability.
Deeper Questions: Connective Tissue
Solutions other than neurosurgery currently exist. For example, regenerative medicine treatments can sometimes strengthen the connective tissue.
This brings us to some deeper questions: If ME can result from connective tissue failure, then what exactly is causing our connective tissues to fail? To fail badly enough that we develop ME?
What are the necessary elements to brew this terrible storm? What combination of genetics, epigenetics, environment, and specific events? How do these interact?
How do we arrest this process? How do we reverse it? How do we prevent it?
And by exactly what mechanism(s)?
I think the answers to these questions could be central to reversing, and even preventing, ME. As we live through the discovery process of finding these answers, we will learn so much more.
And how many surprising, related mysteries could we unlock along the way?
______________________________________________________

After uncovering the mechanical problems behind his severe ME/CFS, Jeff Wood completely recovered.
Jeff Wood is the creator of MechanicalBasis.org. In early 2017, after extensive research, Jeff figured out the cause of his own ME and has remained in remission since his craniocervical instability (CCI )and tethered cord surgeries. His experience has lead to a re-evaluation of both what constitutes ME/CFS and how CCI occurs as well.
Jeff developed the Mechanical Paradigm in 2018 which proposes a connection exists between ME and mechanical neurological conditions – specifically those associated with connective tissue disorders.
He has been calling for more research into these connections.
Check out blogs and other resources including Jeff’s startling story in Health Rising’s Fibromyalgia and ME/CFS Spinal Resource Center





I find many ideas I can associate with my ME. Past viruses, Salk polio vaccines in grade school. Strep that caused my brain to swell and subsequent strep infections affecting other areas. My head feeling heavy and full enough to explode. Minor exertion taing me down for several days, etc.
THE ANSWER TO YOU IS: I TREATED MANY THOUNSAND PATIENTS FOR LAST 40 YEARS. THIS IS CHRONIC NEUROINFLAMMATIONS—FOR HEADACHE –REDUCE THE INTRACRANIAL PRESSURE,FOR NEUROINFLAMMATIONS—HAVE LOW DOSE IVIG
IT WORKS LIKE MAGIC. LOOK AT THE RECENT STUDY OF COVID-19–WHICH IS ESSENTIALY THE SAME NEUROINFLAMMATION—ALL THE DOCTORS TREATE COVID-19 WITH IVIG. THEY USE IVIG FOR COVID PNEUMONIAS. DO NOT WASTE YOUR MONEY AND TIME.
Ypunused ivig for neuroinflamation? How many treatments?
How many gram/kilo bodyweight/month is low dose icig for dr Pak?
How do you reduce the intracranial pressure??
Where can I see information?
Where is the recent study?
It would be great if Cort could pull together another survey asking CFS/ME people if they’ve had certain viruses, cervical spine problems, injuries, etc and what other symptoms they may have had that relate to disautonomia, plus age of onset. I’d like to see if the results reveal patterns.
Yes, IVIG is used for neuropathy, too, which many patients with ME/CFS have. Big problems are: 1. availability of IVIG – there tend to be chronic worldwide shortages; and 2. cost. The insurance companies are very loathe to cover it.
Very interesting, my ME symptoms started after a fall from a horse resulted with a fractured skull. But that was 40 yrs ago. How do I start to get sceptical medics to look into this for me?
Hi Zita. It can be hard to be taken seriously with these conditions and concerns. Many doctors can’t be persuaded to investigate topics that are new to them. Most of us have found we need to seek specialized help to be evaluated.
Polio/DTP vaccine was my trigger also. I did suffer whiplash and had a sprained neck for 6 months undiagnosed but over come that prior to the vaccine that caused encephalitis in me. This article makes sense in the nerves being inhibited and viruses and vaccines overwhelming the system. I’ve never been tested for spinal leak..seems that should be noticeable but will research those symptoms more.
This sounds very promising. What medical test is used to discover and/or verify a chronic, ongoing brain and spinal cord injury that is exacerbated by exertion?
Jeff! I totally agree with your premise on all of this!! I can follow it through my own history right up to present. I was struck with a bad case of Mono at 15 then 13 years later I woke up and have barely been out of the bed since then. My doctor says my 51 years of illness with CFS/ME make me his oldest patient with it. I worry about the post COVID patients so. What will their lives be like down this sometimes dark road. Thank You, Jeff! I will re read your work and am grateful to have found this today! Thank you, Patte Dotson
How would you account for mental exertions in this hypothesis? Also, people have reported that heavy metal poisoning or undetected bone infection showing the same symptoms as MECFS, so they need to be accounted as well.
Any kind of CNS injury will rile up microglial cells, which also happen to be sensitive to the body inflammation. Could the common nexus be the microglia rather than CNS tissue injury?
Oops, above got posted as a reply to Patte by mistake, sorry. It’s a reply to Jeff.
I would think (from my own research) that mental exertion would happen because of central sensitization after chronic injury to the brainstem and spinal cord.
i woke with this illness almost 24yrs. ago and have been bedridden at first and now housebound and no better after all these yrs. as i am almost 70. problem is i haven’t found a dr. except dr. lerner which puts anti-virals intravenously in you. no other dr. knows anything about it so no help for me. what type of dr. understands your illness? also,i now have Parkinsons which one HAS to move whereas with ME/CFS you move you loose, right? they say epstein barr/mono causes Parkinson’s as well as cancer, MS and other illnesses.
i hope u got my post to you, patte.
How do u deal with it
I think of the many hypotheses raised to date this is the one to bet on if you are going for rank outsiders.
Thanks. So Every time we move we give ourselves a traumatic brain injury? What about every time we think, but don’t move? What about the times when we aren’t thinking or moving at all like deep sleep or meditation? OMFG Am I giving myself a brain injury by typing this message right now? I’d better go lay down.
Also, please note that for every CCI surgery recovery story there seems to be an equal number (or greater number) of people who did not improve and/or worsened. Some considerably.
A lot depends on the type of your structural issues to say what type of moves would stress the brain or stretch the spinal cord. I attribute my semi remission of symptoms to learning which movement causes issues.
I also began treating concussion several years ago after I realized I was dealing with a spontaneous CSF leaks that started supposedly around 2011 and exacerbated in 2013. . I arranged for a lay flat work station at home and was shocked when I stopped experiencing PENE to the degree I had before. I also underwent blood patches in 2019 to treat the leaks. I spent past year in concussion rehab programs that included an osteopath, a manual therapist, a PT, a eye Dr who does visual and memory rehab. After multiple years of not being able to read a paper book I am finally able to hold a book and read it and retain what I read and not crash.
I still have significant underlying issues to address – Tethered cord syndrome. I don’t stress my cord if I bend backwards but I do if I bend forwards. Knowing this allows me to give my spinal cord rest periods and surprise,surprise my PEM/PENE is better.
I was offered surgery for it but haven’t yet pursued it. I take preparation for a neurosurgery very seriously for the same reason you mentioned. Just having surgery is not always sufficient for recovery. You have to have resources in place for some serious than work and it takes a long time.
?
Totally agreed. My catalyst was spinal csf leak, this set me on this pathway. My leak was sealed 2 years ago, now my current life is hellbent on not irritated my fickle & easily insulted neuro system.
Thanks for putting this together so clearly Jeff.
It seems quite a few people with mechanical problems will experience leaks at some point. Thanks for sharing your experience, Bec.
Doctor years ago believed a head trauma connection.
Interestingly, some EDS manifestations also get triggered by trauma https://www.ehlers-danlos.com/brain-injury-unmasking-ehlers-danlos-syndromes-after-trauma-the-fiber-print/
I also wonder what (cause or effect) the elevated hydroxyproline plays in this. Found in female patients in Naviaux study. Info on MEpedia. Yep, there’s something to this…and the vagus nerve in the neck and others that get compromised! My endometriosis got SIGNIFICANTLY worse (different from prev 12 yrs) after whiplash. My ME/CFS worsened and general health. Also, I’ve had multiple neck injuries over the yrs & have CCJ instability, CCI, & symptomatically some AAI (head popping downwards & needing to be popped upwards too often.) Pursuing answers. P.S. Jen Brea’s Medium article series would also be good to add, I think! 1 link & all parts in the series are listed at the bottom of that pg. Titled “CCI + Tethered cord series.”
How does one find Jen’s articles?
A link to her Medium blog can be found in Health Rising’s Resource page shown at the bottom of the postl
I am interested in whether Cytomegalovirus which is highly prevalent, yet disregarded as a significant illness, may be a contributor. CMV may also trigger mononucleosis.
Nice one. How would this be experimentally investigated?
If you can think of anything to do at home (within reason – no Greco-Roman wrestling), I’d give it an N = 1 crack. Like repetitive head movements to see if symptoms become worse or induce significant PEM.
Hi Jeff, thanks for your work challenging our community to think outside the box! I’m a typical story, viral and bacterial onset, severe intracranial hypertension, fibromyalgia and ME. Finally discovered I had spinal stenosis and I had the ADCF 5 6 7. But due to the injury or infection I have permanent damage of my spinal cord when it bled and tissue died. (cervical myelomiaca). I am positive I have a collagen disorder but my doctor’s just tell me there’s nothing they can do for me.
Sorry to hear about that Sara. I think Jeff’s and other’s stories will help many however. I’m just itching to find out more about the connective tissue connection. I’ll bet the DecodeME genetic study will show up something. Both my twin brother I have a connective tissue issue but only I have ME/CFS. I imagine it must be a component of it.
‘
Here’s one interesting recent study
https://www.news-medical.net/news/20200604/Study-offers-potential-targets-for-treating-people-with-Ehlers-Danlos-syndrome.aspx
I second that!
Yes! I’m 43 and have had moderate chronic lower back pain since ~age 19 due to rotated S curve scoliosis. My career was high stress and sitting behind a computer, which didn’t help my neck, but when I was 37 I got whiplash from a car hitting mine. That seemed to be the final straw to send my body into ME/CFS. I’m not sure my specialists in Seattle would know how to diagnose cranial instability.
Perhaps you can get in to see Ilene Ruhoy, MD at the Center for Healing Neurology in Seattle. She works with David Kaufman, MD the highly respected expert ME/CFS, etc physician. Apparently he is not taking new patients at present but I think she is. She definitely has experience with craniocervical Instability.
Check out the blog entry below on her clinic’s website & if you’re interested then you can find out more about the practice on the top page of the site. They don’t take insurance but if your plan has out-of-network benefits you could submit a claim.
https://www.centerforhealingneurology.com/2019/11/17/blog-cci-surgery-a-neurologists-perspective/
Hi Nancy, you are correct that Seattle is limited in educated on the subject drs. You may want to join (if you are on FB) local Ehler’s Danlos group -they deal with non traumatic CCI and maintain lists of drs who have experience and qualifications.
However with your description of pain and scoliosis I am wondering if you might be suffering from Tethered Cord Syndrome, which is the bottom of the spinal cord problem. I myself near Seattle but was diagnosed by Dr. Petra Klinge in Rhode Island. I also looked at CCI first and I have abnormal angles in that area but after I started treating the neck conservatively, with a hard nevk brace and manual therapies, my Tethered cord symptoms were exacerbated leading to the diagnosis.
I went to a Seattle chiropractor for a Digital Motion X-ray which showed damaged ligaments in my neck. However, x-rays are not sufficient to differentiate a “little” chiropractic problem with the neck and “big” neurosurgical level problem. For that you need MRIs and a neurosurgeon.
You may want to join ME/CFS + Brain and Spine group on Facebook for more resources.
Hi Jeff,
Thanks for the years of hard study under harsh conditions and for sharing so much of your results here. It’s more then just sharing: you keep engaged in working hard even after you find yourself a huge improvement. Few do such or are willing to do so.
You gave many things to think about. Personally, I do not lean towards an ME equals connective tissue disorder. I sure can see there to be a strong overlap and correlation however. Connective tissue trouble IMO should make you more prone for ME and vice versa. We for now differ in our estimation how key to ME connective tissue disorders are. I sure am willing to follow up on you, your work and other peoples work on this relation however!
Your ideas and experiences on the importance of brain stem compression or spinal cord compression played part in the development of the “the spinal cord escalator” idea by Issie and me. This idea is not opposed to yours, but offers an alternative and / or complementary view.
I first post a copy of something Irecently wrote and then add some comment on how it relates to your work.
As to viral infection possibly weakening connective tissue, I can see that. Issie and I are (also a bit) working on trying to understand that one and slowly puting it together in blog format. We have to work more on it however. Maybe I should try and see on your website again how you connected these two so far ;-).
Copy from https://www.healthrising.org/blog/2021/02/05/attention-deficit-fibromyalgia-rheumatoid-arthritis/ as I’m to tired to rewrite and adapt to fit your blog now:
”
“It turns out that the brain networks (anterior cingulate, prefrontal cortex) that process pain, and those involved in paying attention, partially overlap.”
Together with a study that glutamate injected in the brain of rats can “burn” away pheriphery nerves (Cort had a blog on that one) and widely accepted knowledge that excess glutamate can make neurons “trigger happy” or work very hard and fast (but often yield poor results by hasting too much), producing plenty of heat we come to the spinal cord escalator idea that Issie and I worked on https://www.healthrising.org/blog/2020/12/11/nucynta-opioid-small-fiber-neuropathy-fibromyalgia/.
The idea here is: excessive glutamate and ROS in the brain (possibly produced by inflammation) can travel down the spinal cord and create (or “copy”) the same inflammatory situation that is on the nerve end at the brain side towards the nerve end on the body side.
So, a state of excessive glutamate and ROS on the tip of the spinal cord nerve in the brain can under cicumstances “travel down and leak” towards the tip of the pheriphal nerve (into the body tissues).
But, excessive glutamate and ROS on the tip of the “body part of the nerve” can copy and travel upwards and create the same state on the tip of the spinal nerve that enters the brain.
As such, an inflamed part of the brain can create and inflamed muscle or gut. And that inflamed muscle or gut can once again create or reinforce an inflamed brain. So, we have potential for a vicious circle here.
This “It turns out that the brain networks (anterior cingulate, prefrontal cortex) that process pain, and those involved in paying attention, partially overlap.” adds a new part to the idea: excess (chronic) pain would in this idea *also* be able to trigger a state of increased glutamate / ROS / inflammation at the brain (stem) part where that nerve ends up to.
That glutamate wouldn’t stay exactly there at that position. It is “interstitual” glutamate to start with, meaning it is found outside (in between) the cells. So it can leak and spread from cell to cell. It that happens long enough, glutamate would leak to nearby areas and create a combo of trigger happy neurons consuming plenty of energy, unprecise information processing and increased inflammation, temperature and ROS in that area. And the quoted info from Corts blog says those nearby (or overlapping) areas are key in paying attention…”
Most complete theory to date, fits my story to with a few variations. I’m so saving this, many thanks to the author!
Here’s a link w a fresh woman researchers theory on the genetics..
https://me-pedia.org/wiki/RCCX_Genetic_Module_Theory
Possible links to the role of many of the brain stem and spinal problems you managed to relate (and in your case improve so much) to ME:
A compressed brain stem IMO should increase brain stem inflammation. Brain tissue is IMO fairly delicate and any compression of it increases things like neuron cell wall tension and deformation.
More importantly, any mechanical compression has a big chance to mechanicaly deform near every single https://en.wikipedia.org/wiki/Chemical_synapse#Structure, picture https://en.wikipedia.org/wiki/File:Neuron_synapse.svg in some modest to bigger way.
The brain functions only thanks to each brain neuron having plenty and plenty connections per neuron to other neurons. Each such connection consists of a sort of “long wire” that is often way longer then the diameter of a neuron and at the end a neuron synapse to “connect” to the target neuron in order to pass information in a biochemical way. See https://en.wikipedia.org/wiki/File:Chemical_synapse_schema_cropped.jpg.
On the bottom right of that picture you see a cut out view of this connection. Mechanica stress can create both to not be aligned perfectly. Then, signal messenger molecules can get lost and the communication will be less effective. Less effective communication between neurons makes for a less effective brain.
Secondly, the gap between pre-synaptic neuron and post synaptic neuron, called the synaptic cleft, must be very small (distance between them) and very broad at the same time. That requires them to be very parallell too. Even a bit of mechanical stress can skew that parallellism and create plenty of opportunity for neurotransmitters “to escape”. See the anotated picture of https://en.wikipedia.org/wiki/File:Neuron_synapse.svg in the first link of this comment.
A commonly used neurotransmitter in this sort of brain communication is glutamate. If glutamate “escapes” from this narrow gap between the pre-synaptic neuron and the post synaptic neuron, then it becomes “intracellular” or in other words it “floats” in between cells. Intracellular glutamate is very excitatory (causing neurons to work very hard but often unprecise) and when it reaches too high levels it gets very inflammatory. It can create glutamate excitotoxicity or in other words even kill neurons (permanently) at high speed. Excessive ROS is but a small part in that destructive chain reaction.
So: if mechanical stress can likely deform these synaptic clefts a bit too much, you’re in for deep trouble.
As nerves use the same mechanism for their communication, they are prone to the same mechanism. Worse, nerve fibers are poorer at self repair as there are no large numbers of adjacent neurons that can take over the function easily when a connection fails (as nerves are a serial line where a single failure can be bad to catastrophic).
Add in the idea of “the spinal escalator” and any inflammatory situation (excess glutamate, ROS…) at the brain stem (with plenty and plenty of nerve endings or inflammation “injected” in the spinal cord by a vertebrea pinching it can travel up and down the spinal cord and in our idea create potential for a vicious inflammatory circle where brain (and spinal nerve) inflammation can trigger tissue end point inflammation (like in muscles) and where tissue end point inflammation can trigger brain (stem) inflammation.
To make things worse: if the spinal cord is pinched and that creates local inflammation (by pinching and by friction when moving as the spinal cord will move some with bending of the spine) then (if this local inflammation would also “spill” outside the spinal cord near the pinching vertebrea) chances for (further) calcification of the problematic vertebrea arise. Inflammation speeds up the formation of calcium spikes (sharp as knifes) on bone. This can make this vertebrea even more problematic.
My estimate is that poor connective tissue correlates “well” with more friction between the spinal cord and problematic vertebrea, further increasing irritation and inflammation…
Thanks for sharing these ideas. There’s a lot to explore.
Hi, Jeff! Thanks for your hypothesis and call for research. I’m just wondering, how would your plea get bumped up to the right decision-makers (in an urgent fashion?).
I do believe that Jeff is correct there is a mechanical basis to ME/CFS. But I don’t believe that the cause is “micro-TBIs” as he posits. His own recovery, in fact, seems to undermine this very theory.
Repeated brain injuries wreak havoc on the brain and, at a point, the brain is unable to recover. Many of those who suffer numerous concussions are left with permanent symptoms. A single TBI can leave someone permanently disabled. Sure, a “micro-TBI” is far different from a severe TBI, but if those with ME/CFS really were undergoing trauma every single movement, the cumulative effect would certainly be devastating. Is repeated “micro-TBIs” not functionally the same as football players who have their brains jostled dozens of times every game? Many of these players end up with permanent brain damage, at the extreme is CTE (chronic traumatic encephalopathy) from which it is impossible to recover.
Under Jeff’s theory, if the stimulus (the mechanical basis causing “micro-TBIs”) is removed then the disease itself is removed. This is not how the brain works; trauma once done never really goes away. Basically, if the brain really were undergoing repeated “micro-TBIs,” the disease would be inexorably progressive — but we know for a fact that is not the case.
You make an interesting insight, Ezra. I don’t quite agree though that the micro-TBI concept, as applied to ME/CFS, would inexorably lead to permanent damage. These micro-TBIs would not be necessarily analogous to repeated professional football impact trauma, as there is not the same type of impact/force.
It is also the case that some retired professional football players, having sustained multiple concussions during their careers, sill don’t have evidence of permanent CTE changes in the brain during autopsy.
See: Absence of chronic traumatic encephalopathy in retired football players with multiple concussions and neurological symptomatology.
With further research and more individual data points, we will learn more over time. Thanks for the food for thought.
Thanks for the reply, Jeff.
You make a good point. I could see it both ways. But yes, without proper research, it’s impossible to say definitively.
Either way, I’m glad that you’ve brought this theory, and the broader neck and brain theory, to my attention.
Patients with significant brain damage (stroke, TBI, etc), through physical therapy and the process of neuroplasticity, are able to grow new connections. Just because neurons die, doesn’t mean that the brain isn’t able to accommodate and regain function to the point that there are no residual symptoms from that damage.
One possibility could be that CCI just irritates rather than causing repeated TBI. When the irritation is removed, MECFS symptoms go away. Same could be the case also in Kyle McNease’s recovery: the chronic poisoning/inflammation irritates something in the brain causing MECFS-like symptoms. When the poisoning is treated, the symptoms go away.
For “real” MECFS, the brain could’ve gotten irritated after a trauma, like an infection, failed to return to previous state, and remain chronically irritated.
Some infections would change the tissues. There are so many lyme and confections suffered in the Spinal CSF leak groups as well as I personally witness my lyme friends after years of treating lyme needing a Tethered cord release surgery due to abnormal filum. In some cases when that filum is biopsied they find it being infiltrated with lymphocytes and mast cells among other inflammatory cells and it is plausible that even if the infection is gone, the inflammatory process it left behind needs to be treated surgically.
My trigger was contracting mono at the age of 17 (almost 20 years ago.) I did not meet the criteria for a hEDS dx, but got dxed with Hypermobility Syndrome. Dr Brock, and EDS specialist at 3 Pillars Therapeutic, told me that they’re the same thing in her opinion. She things the current criteria is too strict.
Looking back to childhood, I had signs and symptoms of Hypermobility, also I have seen it run in my family.
I was dxed severe CCI and AAi by Dr Patel and had a c0-4 fusion 6 weeks ago. I felt better, then much worse as the swelling set in from my surgery. Hoping for improvement once the swelling goes down.
I very much agree with this hypothesis. I have looked at it like, my connective tissue was already compromised, then the mono made it much worse resulting in ME, MCAS, POTS.
I also believe that exertion releases histamine, and that’s where PEM comes from.
Anyway, thanks for your article and your work Jeff. You were correct in the informal assessment you did for me last year. You gave me much hope that I had an oath to take to potentially get better.
Wait. The fusion made you much worse? And you’re thanking the author of this article for telling you you had an oath to get better and for directing you towards the very surgery that has made you much worse? This doesn’t make much sense.
6 weeks post surgery is a heavy recovery period. Most feel like crap for 3-6 months.
Interesting hypothesis. There’s multiple cases ME/CFS in my family across several generations so there’s undoubtedly something genetic occurring for us. There’s also formally diagnoses EDS so interesting to ponder if that is the underlying genetic issue…
Thanks for sharing your thoughts. There does seem to be a genetic component in many cases.
Yes it does, Jeff. So many of us have been in close contact with cats and dogs, and biting mosquitos….
From: https://www.lymedisease.org/cdc-identifies-new-species-of-bartonella/
“*Note: Bartonella has been detected in lice, ticks, fleas, sand flies, mosquitoes, wild animals and house pets. “
Gemma and Jeff, I think its important to investigate the genetic/EDS angle. But in addition, I urge you to see the work of Dr. Mozayeni and Edward Breitschwerdt, DVM. A case study is published here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5944489/
Their patient, a female veterinarian, met criteria for EDS, hypermobility type III. They treated her with antibiotics for bartonella and she improved. Please see other works by Breitschwerdt, too. The Galaxy labs website has a lot of information, since Pubmed may be too heavy reading for some. https://www.galaxydx.com/our-management-team/
I came across these guys in my search for treatment for Lyme disease. Please have a look in this direction, because both Lyme and Bartonella (and who knows what else) love to hang out in connective tissue…
Hi Infectious Onset,
Thanks for sharing this here! I’ve read that study before. I think it supports the idea of a relationship between infection and connective tissue breakdown.
Jeff, glad you are doing well and still engaged in thoughts andsharing with cfs me community.
i agree that connective tissue can play into it— and that many CT problems / hypermobility may not be diagnosed.
wonder how many cfs/me persons had strains and sprains that might show tendsncy for these problems.
While speak of tbi, i think the neuroinflammation is, in itself, a tbi. That can be isolated occurance, or, more often, ongoing and continuous.
(could call it ’nibi’ neuro inflammatory brain injury.)
There is study
https://www.sciencedirect.com/science/article/pii/S2213158220302035
showing “ sub-millimetre resolution voxels detected very significant clusters with increased T1w/T2w in ME/CFS, mostly in subcortical grey matter, but also in brainstem and projection WM tracts. ”
Hope one day qeegs and Loreta style brain imaging can progress enough to show the damage causing impairments that do not show up as easily on the general testing the majority of doctors are ‘allowed’ to use. (Also since qeeg is non-invasive.)
And could then be used for early diagnosis and to follow/correlate with medical treatments and the research/discovery/
/development of potential medicines/ treatments.
I had a look at that study Sunie and though I didn’t understand a fair bit of it, I could see that they were finding differences in the brains of people with ME/CFS and healthy controls.
that was my take-away too,
seems like more expensive tests show more…….
maybe reasons test like it and functional mri etc are not tests routinely done for cfs/me
perhaps enough cog-fog co-v patients will have them done to show the value of expensive tests that hopefully shows what damage is there from the get-go, and how it changes—and may make treatment(s) available sooner
Wouldn’t that be great – a bit overdue though…
Thanks Jeff, this is an interesting hypothesis and I hope it gets followed up with research. Last year, as an experiment, I started to wear a neck brace when being driven in the car and found that I didn’t get so fatigued by the journey. I now always wear the neck brace in the car. Although my ME started after a strange virus, I had energy issues for a while before I got ill. A few years before the virus I had whiplash from a car accident where I was hit from the side, so nothing to limit the movement of my head from the collision. I do wonder whether that had anything to do with my getting ME.
That’s interesting, Nicole, that the neck brace prevents some of your fatigue. There are several specialist MDs who use a neck brace trial to see if it improves people’s symptoms.
Thanks, Jeff. I am totally on board with this hypothesis and got very excited when I saw Peter Rowe’s speculations about spinal cord stretching, and then your post.
First, I experienced problems with any slight stress, like lifting, in my rob cage, where the joint would hurt. This would be followed by total body inflammation in subsequent days. The phenomenon was was made much worse by physio treatment which involved energetic stretching of my arms and chest, up against a wall. This was in the 1990s. As I’ve got worse with my ME almost any movement can induce PEM. The worst is any repeated arm movement while bending over, stretching the spine, as in picking things up from the floor, or wiping. Sweeping has caused my worst case of OI where I could hardly even sit up for a while.
My noticeable triggers for ME were emotional stress, chemical exposure (new office) and pneumonia, several years apart and each making things worse. but the spinal issue only became evident later. I have a dreadful spinal Xray with spurs in various places! So it all makes sense.
I haven’t managed to interest any doctor in any of this. The only thing that helps in bad moments is rolling on tennis balls, massaging the muscles on each side of the spine. That relives the pressure on the chest and back muscles somewhat.
Roll on the research into this issue!
My severe ME/CFS began almost immediately after an 11 hour spinal neuro surgery to repair damage done by 30 year old Herrington Rod surgeries. Been bedridden 14 years. Now they think I may have spinal fluid leak as I’ve had serious headaches for 4 months, drainage from ears and nose, metallic taste in mouth, profound weakness that is not my usual fatigue. Don’t know where to go for this.
Oh…and did I mention constant neck and shoulder blade pain?
I was in car accident. Have had spine pain daily for years.
My question: is the diagnosis conclusive from the spine scans?
Not always. There is currently no scan that picks up on verticle instability where the skull slides down on to the brainstem. For that there usa combination of clinical evidence, symptoms and traction trial is often needed before deciding whether to move forward with more invasive traction that is fine under fluoroscopy and you can see the brainstem angles changes and correlate that change with objective and subjective measurements.
Jeff’s site lists done neurosurgeons who specialize I. This type of neurosurgical complications. Orthopedic or spinal surgeons usually are a waste of time.
Some skilled PTs can palpate your odontoid and see if it’s too wiggly. Some chropractors can evaluate digital motion x-ray and some neurosurgeons like to look at upright MRIs with flex and extension. There are also patient driven groups where people can share imaging and brainstorm best specialists to pursue first. When I shared my imaging a couple years ago, other patients were first to recommend a Tethered cord evaluation. Sure enough two years later I got to the expert and she had no doubts about my case.
Yes, it’s so important to see a specialist who’s familiar with our population – not all docs understand these conditions.
Might explain my c-spine inflammatory lesion and it’s subsequent autoimmunity, right Cort?
Interesting hypothesis, Jeff. I had not considered that my whiplash injury could have been the original trigger and had always assumed that it was the EBV (about a year later) that was the culprit. I do have hEDS that went undiagnosed until my late 40s when I found your story & realized that I likely had spinal issues. No CCI, but cord compression due to C-spine hypermobility in flexion and extension. ACDF gave me back the ability to ride in a car without the onset of severe vertigo, but I still have very severe cognitive issues and some other symptoms. We suspect that OTC may be the culprit, but been avoiding hospital settings due to the pandemic.
Duke https://radiology.duke.edu/patient-care/specialized-services/spinal-csf-leak/
Vanderbilt https://www.vanderbilthealth.com/condition/cerebrospinal-fluid-csf-leaks
Stanford https://profiles.stanford.edu/ian-carroll#:~:text=In%202015%20Dr.,CSF%20leaks%20around%20the%20world
https://spinalcsfleak.org/about-spinal-csf-leaks/treatment/
Jeff – First of all, thank you for mentioning that ME can have a non-infectious trigger and that these patients have symptoms consistent with those who had a viral onset. These facts seem to be getting lost in most of the recent focus on ME as a post-viral illness.
I developed mild ME after endoscopic sinus surgery in 2005, then progressed to moderate ME after inguinal hernia surgery in 2007. Some things I’ve observed about my illness:
* worsened progressively as I tried desperately to continue my pre-illness exercise routine
* always involved a lot of head and neck pain, which has improved somewhat with physical therapy, worsened with chiropractic treatment
* must use a contour pillow in bed, sit completely upright with back and foot support, cannot turn head more than about 45 degrees, any violation of these will result in major flair-up of head and neck pain
* spend a large portion of every day lying down with a small bag of frozen peas against each temple and cheek to treat or prevent headaches and facial pain
* can only tolerate exercise done in the supine position with head and neck immobilized
Hi Rachel, have you considered Botox injections for the facial pain? I have had TMJ Disorder for most of the time I’ve had CFS (30 years). I started having Botox injections into my mandibular (jaw) muscles every six months (about 5 years ago) and they absolutely help enormously with the jaw/facial/temple muscle pain. Fiona
Regarding the mechanical basis of problems often being overlooked: I have obstructive sleep apnea which my sleep doctor said is caused by my recessive lower jaw. I had complained for years about unrefreshing sleep but a sleep breathing disorder was overlooked, probably because my age and weight at the time did not fit their preconceived notions. The sleep doctor who ultimately diagnosed me said I have probably had OSA to some degree since birth.
Now that I am older and heavier, I have had HCPs assume my OSA is weight-related. They act shocked when I tell them I was 103 lbs. at the time of my diagnosis and that my OSA has a structural cause. I often show them my scalloped tongue (indents along the sides of the tongue from my jaw being too small) and explain that this can be a clue that a person may have OSA. One doc said, “Well, you learn something new every day!”
This makes so much sense. For me, while I have physical fatigue, for sure, mental or physical exertion creates mental fatigue.
I wasn’t done yet! Ha! The big thing for me is that in the last few months I’ve now developed this HUGE pressure in my head that for years and years I never had before. It’s gotten really bad and it’s making my cognitive symptoms and my anterograde amnesia much worse. I can’t function many days. I wonder if this can be sort of the next step in the progression of a stenosis or ligament laxity or whatever that is now manifesting in a buildup of blood or cerebral spinal fluid or whatever.
Jeff. You may be on to something. I have had ME/CFS for 3 years. It started after a 4 life traumas back to back, than I got the flu/bronchitis, was hospitalized, came home on O2 for a couple months and it took like 2 mos for bronchitis to finally subside. When it did, I was left unable to do much of anything. Everything I had been, everything I had worked so hard to accomplish, my dreams and goals were all gone. I have had every test possible from 4 different types of specialists…nothing could be found.
One thing I remember vividly was that my taste changed. I used to be a sweets fanatic. Even though I was healthy, worked out 2x a day, and was anal about everything I put in my body…every once in awhile I would crave sweets bad. After I recovered from the 2 month flu/bronchitis…I craved salty crunchy stuff. I had no interest in anything sweet. Still don’t.
That would lead me to believe that something in my brain changed. I have scoliosis and the area where my spine meets my head is very painful. I used to do 300 crunches a day. Now, I can’t even take a walk to the mailbox.
I live in a rural area in Tennessee and the Drs look at me like I’m crazy when I mention ME/CFS. Nobody treats it and most have never heard of it. I have tried unsuccessfully to move back home to Michigan for better healthcare. I can’t finish the touch ups on the remodel on my house, deep clean, stage and sell it. I’m too sick. Now with the pandemic, relocating is not an option.
I want my life back. Keep searching for answers. You may contact me if need be.
I was a rare a lucky person to be able to get an appointment in NZ with a neurosurgeon who mocked and laughed and told me my theory ( the same as Jeff’s) was completely ridiculous. It was beyond heartbreaking to do all this work to get that appointment, bring in research and she told me she wouldn’t have approved/accepted this appointment had she known about it. I don’t know many other people in New Zealand that will be able to get an appointment with a neurosurgeon, but I stayed and made her listen. But it was very clear she wasn’t interested at all. She kept telling me my bones are fine, even though I was referring to ligaments etc.
I do believe she has got it wrong and what a breakthrough it would have been in little New Zealand for her to listen.
Too much power doesn’t do any of us any good, does it? Wouldn’t it be lovely, Phillipa, if that neurosugeon had to explain their response to you, to an independent regulatory committee?
I had a horrible experience with a psychotherapist on a training course and no one would help me or support me. So I made a series of complaints and got nowhere – very demoralising and exhausting. But I have an inner Jack Russell Terrier, as in, don’t really annoy me because I won’t forget very easily ?
My last complaint was successful, even though it ended up being more about the process and less about the content – as in my initial complaint wasn’t dealt with in the correct manner – bit of a casual affair (nothing to see here, it’s all in her head). So a small victory.
There’s some great sayings here in Ireland, which I love One is: They’ve lost the run of themselves and they need some manners putting on them. These stories of medical unprofessionalism are really extraordinary. These people need to be marched to the Head Teacher’s office and a letter sent to their parents.
I think everyone with ME/CFS, needs a powerful advocate to accompany them to appointments. I had to go into the hospital a few years ago for a procedure. I wore my butterscotch, (expensive looking coat), and a velvet (very expensive looking scarf) on purpose – and I saw the change in the nurse when she saw them – she was much more respectful. Human nature.
A nurse in a long term care facility said to me that they notice when people are admitted, whether their pyjamas are ironed or not, and would I iron her dad’s pyjamas, as he was going into hospital… It all goes on behind the scenes.
A few other things. I was diagnosed with hereditary hyperhomocystienemia in 2011. I had 3 failed rotator cuff surgeries in 2012, 2014 and 2016. The 4 b2b traumas led to a nervous breakdown about 3 mos before getting the flu/brochitis and suspected ME/CFS. (Can’t find anyone to diagnose it in Athens, TN area). I was told I have scoliosis in 2014 but never had tests to diagnose it. My ortho surgeon who did my shoulders had me bend over to look at my back. He said “Wow! You’re scoliosis has gotten much worse!”. I said “I have scoliosis?!?!” He said “You didn’t know? Yeah, you have scoliosis. I’m surprised you didn’t know.” I was too!!! I was diagnosed with Barretts Esophagus in 2014 also but never had a problem with GERD. Never had indigestion. I started choking on food and water for a few months. Had endoscopy done and was diagnosed with BE. On Prilosec now. Still choking. There is a BE Treatment Center in Knoxville but they don’t take my insurance. I am on SSDi, Medicare/TNBlue Care and many specialists don’t take TN Blue Care. I am not being treated for any of the diseases I mentioned above. As I was writing this comment, I receved a call from another place that doesn’t take my insurance. I just wanted to give you a brief history of my illnesses to see if they match up with anything that you’re researching or come across in your research in the future.
Thankyou for your continued efforts to find a cause for ME/CFS.
There is bound to be some truth in Jeff’s line of thought, although I believe that with ME/CFS, many roads lead to Rome. EDS does seem to be unusually common in patients and close family members. There was also the recent finding that patients are more likely to have genetic defects in the proteins making up our mucus layers. Science also suggests that a portion of patients have autoantibodies to muscarinic receptors.
What this blurry picture looks like to me (for a possible auto-immune group) is acetylcholine action down, histamine up, adrenaline up, MMP up, mucus layers and connective tissue degraded, SIBO and leaky gut, high concentrations of lipopolysaccharides from bacteria in the bloodstream (see Shukla), oxidative stress up, mitochondrial energy production down, LPS across the blood-brain barrier, microglia chronically activated, brain wired and HPA activated. I am part of Lipkin’s 40% IBS group and I wonder if this is an auto-immune group. Although sometimes my life is very limited by this illness, I am not as sick as many and my illness waxes and wanes over time.
I agree that Jeff’s thoughts about a major hit and run causing brain stem injury or ongoing problems with faulty connective tissue deserve further investigation, especially since some patients have achieved recovery with surgery alone. Acetylcholine is the major neurotransmitter in the vagus nerve. Acetylcholine could be the overlap between subgroups.
Same on the IBS subgroup. Did you have IBS before you eventually developed ME/CFS? My IBS was quite severe my whole life and caused me much distress and frustration. I eventually had an acute ME/CFS onset at age 32.
Hi Tyler. I think I did start getting gut symptoms about 2-3 years before I got a virus that kicked off the ME. The gut connection is really intriguing for me. All the best to you.
@debsw:
Maybe the question is: what did trigger those gut symptoms? It seems to me those might have prepared your body to easily get ME after any sort of infection. Would you happen to know what triggered it?
Hi dejurgen. Trauma is what precipitated my gut symptoms and probably poor diet (I was a typical teenager!). The onset of an autoimmune illness can often be linked to a preceding stressful period of life and the teens is a peak time for developing autoimmunity due to hormone flux, which were both true for me.
Consider this – what if a partially blocked vagus nerve acts like a partially blocked pipe that backs up? If acetylcholine backs up in the brain and doesn’t readily get downstream where it is needed, then there will be multiple system-wide effects, with acetylcholine potentially too high in the brain and too low in the body. This could be a permanent issue until the blockage spontaneously heals or is addressed by surgery or mechanical realignment. For a potential auto-immune group with muscarinic / adrenergic receptor issues, the brain symptoms from excess acetylcholine may not be as severe (true for me), and symptoms are likely to be more variable, but low acetylcholine in the body will still cause widespread imbalance. Research has shown that choline (precursor to acetylcholine) production in the basal ganglia in the brain is upregulated and the action of acetylcholinesterase (which breaks down acetylcholine) in tissues is prolonged. Stress is a huge problem for me, in terms of managing this illness, and I think it is interesting to note that stress initially upregulates acetylcholine and then it is lower than baseline in the aftermath – PEM?
Also, when I think about the drugs sometimes used to treat ME/CFS – mestinon (blocks acetylcholinesterase thereby increasing acetylcholine), and many of the brain directed drugs like benzodiazepines are anticholinergic. For me personally, I have had some of my best success with dietary measures (particularly a gluten free diet), antibiotics and stress management, which would make sense for an auto-immune, somewhat gut driven etiology. I also benefit from supplements that help clean up the mess.
Also taking Bhupesh Prusty’s recent HPV findings into account, it is entirely possible too that a chronic viral infection drives connective tissue break down in some.
Interesting stuff. I have Scheurmann’s Kyphosis (1984) which exacerbates my (viral onset) ME symptoms tremendously but this perspective makes me wonder if it’s actually causal. Never found anyone else like me so far. Not sure where to take that here in the UK presently.
Hi Dan,
Thanks for sharing this. Some people in our community report their kyphosis was due to an underlying connective tissue disorder. Spinal problems like kyphosis and scoliosis seem fairly common in people with ME — possibly over-represented compared to the general population.
If the theory is correct, I’m wondering how much the disease might be mitigated with self-help mechanical corrections such as posture and alignment practices.
My etiology is supposedly neurological, but I also have a connective tissue disorder (not formally diagnosed as EDS, as my doctors insist a formal diagnosis would not affect my treatment).
I’ve been learning a ton about my body’s alignment in the last few years with taichi — which I had practiced casually for nearly 40 years, but which now has become critical to my daily disease management. While I have not yet seen signs of a “cure” from taichi, the practice has helped me tremendously to more fully understand the connections between my debilitation and the way I carry my body (whether actively or in rest) and, intriguingly, ways to encourage the flow of energy through the body.
I could “cheat” my taichi practice when I was young and strong by executing each move primarily with my muscles (instead of from my core). Now the only way to succeed is with near-perfect balance and posture — so that momentum and flow can lead my body to the positions with relatively little muscular effort. And, now, just walking across the house I’m constantly calling on these principles — with frequent reminders to tuck my head securely in its cradle, rather than letting it stretch out inquisitively, as was my lifelong postural habit.
It has also become clear to me that when I rest on my back — even with my trusty alignment pillow — my neck/head alignment gets subtly kinked with every breath, causing my neck muscles to engage (with tension) repeatedly, discouraging full release and relaxation. Every few breaths I have to lightly sway my head back and forth to keep re-releasing the buildup of tension. Just the slight change of weight in the head with each inhalation causes the neck to want to jump in to support the head instead of giving up the head fully to gravity. When I frequently “re-set” the head I am able to get significantly better rest.
Thank you for sharing! I too am of the belief that my efforts to maintain conscious awareness of body alignment and posture, along with Pilates has helped me significantly over the past few years, as prior to this I was deteriorating
Thanks for sharing your thoughts and your experiences with body alignment, Paw. I found this was a really interesting description,
“Just the slight change of weight in the head with each inhalation causes the neck to want to jump in to support the head instead of giving up the head fully to gravity.”
I experienced a similar sensation when I had CCI. Also, consistent with a genetic component, my dad has developed CCI now, in his 60’s. He has described a similar sensation.
I believe the hEDS diagnostic criteria (ie Beighton scale) misses a lot of connective tissue problems. In the last year, my teenage daughter, whose primary diagnosis was ME/CFS, was diagnosed with CCI. She is clearly hyper mobile, and while she scores a bit on the Beighton scale with fingers and knees, she doesn’t meet full diagnostic criteria. However, she can turn her legs around backwards at the hip joint so that her heels face forwards and her kneecaps face backwards, her right shoulder pops out of joint constantly, and her knees and ankles swivel in different directions instead of in tandem. She has the EDS-like huge stretch marks across her back, despite being 5’7″ and weighing only 100 pounds. I was diagnosed last month with CCI, and I am not outwardly hypermobile, except in my hips (and according to MRI, my cranial cervical junction). But, a few months ago, my right elbow spontaneously popped up out of the socket. It took two weeks for the pain and swelling to go down enough to accidentally pop it back into place when I turned the steering wheel. My 10 year old son was diagnosed with occult tethered cord and required surgery in September. Only his ankles appear to be hyper mobile. However, our PT, who has EDS herself, says that she is seeing more people like us, who while we don’t look hyper mobile, have interior instability within the joint. Technically, we fall under the Hypermobile Spectrum Disorder (HSD) label. But it’s all pretty much the same thing…crappy connective tissue, just expressed in different ways.
Patience, I read your comment about the stretch marks. Please do a search for “Bartonella rash” and compare images! Also regarding atypical EDS, please read this: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5944489/
I have also only localized hypermobility in my entire cervical spine with atlantoaxial instability, which I only found out after reading Jeff’s and Jennifer’s stories. However I do not score Beighton scale. I also had viral meningitis (virus not known) a year ago which I believe led to ligament degeneration. I dont think it is virus itself, but rather autoimmune reaction to it. Interestingly two days after virus onset I started to experience itchy palms and few days later I had full on neuropathy in my palms and feet, which again I can only think if as autoimune reaction.
As someone wrote, there are more roads that lead to ME / CFS / POTS. This is one of them. If the cause is known and you have been successfully operated , you do not have ME/CFS/POTS according to the criteria.
If mcas could be controlled, would collagen grow back or could stem cell therapy help?..
Also could crisper be used to sit out infections such as Epstein Barr?
Hi Oliver,
Some people have benefitted from controlling MCAS. Others have had varying success with regenerative medicine treatments, such as stem cells.
I had a stem cell procedure in my lower neck beneath my fusion, to fix some mild instability. It was successful.
Thanks for engaging. Great questions.
Thanks for the reply.
I’m amazed you as a sufferer had the wherewithal to not only creatively think about this whilst suffering but pursue action for treatment.
It also amazes me that it’s taken a sufferer and not a so called expert to draw these conclusions. Does make one wonder about orthodoxies.
I wonder if tight muscles from the mast cells causing anxiety can further worsen cranial instability and the mast cells themselves weaken the ligaments as mentioned.
When I take a benzos, my symptoms go..is this mast cells calming, muscles relaxing and not putting pressure on the cranio cervical joint and nerves..a inflammation dampening effect.
All of the above.
I think this could be solved so quickly as a concept behind chronic fatigue syndrome.
What’s holding this up in research terms..just money?
I just can’t believe we have so many working hypotheses , and ones with potential new avenue openers for medicine in many fields, and it’s neglected.
Good to hear stem cells helped by the way.
Regarding the crispr treatment..I think I’ve read the technology is there already to edit it out if being a dark player within the body.
I think this is a really strong hypothesis – it will be important to research this!
I’m wondering how this hypothesis would explain such a variance in recovery stories. What about a slow, spontaneous recovery, for example? Can known connective tissue problems remit in this way?
Also, thank you, Jeff, for such an interesting and clearly written article. I wish every scientific researcher had your communication abilities.
This is from Wendy – a physiotherapist (who had trouble posting it)
Not blood, but lymphatic circulation disturbance, is what Perrin proposes. The lymphatic system is poorly understood and little attention is paid to it until there is a major problem (ie. arm lymphedema post mastectomy/lymph nodes excision). It was previously believed that there were no lymphatic vessels/circulation for the brain. This would seem illogical, as the lymphatics play such an important role throughout the rest of the body – in waste and toxin removal, and in the immune response. But the medical community thought of the brain as somewhat of a sealed system, due to the blood brain barrier. However, more recent research has revealed that there is permeability in the blood brain barrier, particularly around the hypothalamus (the control centre of the ANS) – to allow for passage of important hormonal signals from the body. In 2017, research in mice showed that there is lymphatic drainage from the brain, through the ethmoid bone (cribiform plate). I believe that disturbed mechanics in the craniocervical region can affect this drainage because of this:
https://www.drjamiedougall.com/2019/07/03/the-spheno-basilar-junction/
As a physiotherapist, I can understand how this all ties together and am pursuing treatment with both an osteopath trained in Perrin, and a manual therapy advanced practitioner PT for craniocervical issues.
As an aside, the “impaired blood perfusion” to the brain doesn’t really add up for me – there would be “hard neurological signs” if that were the case, such as we see in other conditions affecting brain perfusion. Same thing with proposing that underlying mechanisms are “strain on nervous tissues due to mechanical issues in the cervical spine” – this is what we see in degenerative cervical myelopathy, and they present very differently from CFS/ME (ie. sudden losses of balance and falls, loss of coordination in hands is what I’ve seen in these patients). But the lymphatic system disruption does make sense to me. And definitely would affect the ANS function as seen in CFS.
Grateful to find this info. It took me going through 3 PCP’s, 3 neurologists, 2 neurosurgeons, one sleep specialist (also a neurologist) bc I was sleeping 16 hrs & falling asleep and then finally 1 very good rheumatologist who looked at my whole history, asked questions, thought he knew what it was but did the touch tests anyway to confirm ME/CFS.
He wondered why no one had told me I also had degenerative disc disease. The next week my new neurologist diagnosed occipital neuralgia. I couldn’t tell what was a migraine or a headache – they never end. 7 years, $40k out of pocket in medical costs and now we are $24k backwards on mortgage forbearance. My husband and I have never been on a vacation. I couldn’t work any more after my 3rd surgery in May 2019. I tried, lasted 5 months. Paid Social Security taxes every year starting in 1986 (I was 12). But when I need the benefits? Keep ya posted, it’s been a year and a half since I applied.
Jeff,
Thank you for sending me all of this information.
How do all the triggers of CFS mentioned in the beginning of the article all correlate to CFS and the lax ligaments ( such as mold exposure)?
This is one of my favorite Health Rising articles ever. It actually encompasses many of the issues I’ve been thinking about and interconnecting them. Mold, cervical issues, stenosis etc. My head pressure feels like there is either too much of something or too little of something in my skull, along with a sense of inflammation. This would be validated by the suggestion that the blood flow out of the brain might be reduced and the spinal fluid may be increased, and potentially lead to a leak.
Thank you for this brilliant article and far bringing your experience with CCI and TC to the forefront in the CFS community.
Hello Mr. Jeff! We are many that are happy and grateful for both yours and Jennifer’s remission story, and for the extremely information you provides in those important medical subjects. However, one thing remains a mystery for us all that have followed both your stories, is the fact that both of you haven’t shared your thoughts on WHY/HOW you think your CCI surgery manage to get your POTS, CFS/ME and PEM’s to go in remission. We are hundreds of people that are wondering this and we all would really like to get your reply on that. Thank you so much in advance and we wish you both a healthy future! ❤️
Hi, lots of detailed comments here but as a non-science person (with limited energy for research) who only has access to my GP and no other specialist help, is there anything I can do either to get this looked into or to manage at home?
It resonates for me because I have a lot of neck/upper back pain, I instinctively feel like a lot of tension is situated in my spine and head, and I get a lot of mental fatigue and digestive problems. Also, my brain fog and fatigue remind me of issues my dad had after his stroke, from which he has made some significant recovery whereas my symptoms have steadily got worse!
Any layperson’s advice? X
Excellent work Jeff! Based on my condition I have been thinking along similar lines, so good to see someone has put it down in great detail for further consideration.
Hello, Sounds very plausible. Definitely want to look into this treatment. Years back, I discovered a man by the name of Garth Nicolson in an article called, Chemtrails and the New Microbes. Please read this eye opener! He says a particular Mycotoxin is found in most people with not only CFS, but several other Autoimmune illnesses stemming from the Gulf War.
I found this article when trying to figure out what was happening to me. I have had 3 left frontal lobe injuries in my life, then followed by a frontal lobe stroke 1year after last injury. Recently I’ve had a lot of issues with balance and falling and I have pink snot constantly accompanied by headache? I wound interested in hearing more and would be willing to share my story. I’m 57 and my first head injury was at 13. I survived it all but not without issues, that regular doctors can’t seem to explain to me.
I suspect PEM triggered by changes in blood brain barrier and intestinal barrier after exercise and or stress. Unclear whether there are changes to connective tissue that might also contribute to this process. During initial viral infection immune cells that do not belong in the CNS and spinal cord migrate and get triggered then perpetuate neuro inflammation. I hope that Dr Prusty’s research leads to confirmation that MECFS is also acquired mitochondrial disease. We just don’t have the tools yet to study mitochondrial function of muscle and neural tissue in vivo. Just my 2 cents.
Nice idea! 🙂
I had severe pain in my lower spine for 32 years, caused many issues eventually was diagnosed with CFS. I took an anti viral med plus vitamin c for several months to a year, pain and illness cleared up. I still get the attack’s currently both my shoulders feel like if I move they are ripping muscles, but I’m taking the medication again to see if the same result can be possible. Very terrible disease, it re activated after taking vaccine.
My hypothesis is that there is an anthropogenic class of toxins that degrade collagen. So the people to whom that happens might be the people who already have collagen problems or joint instability, and then also the people who are poor detoxers so the toxins build up in their bodies and do disproportionate amounts of damage.
These groups need not be discrete, since as we know one consequence of connective tissue disorders is issues with detox.
Me: I grew up in two mouldy houses, got chronic fatigue living in a room that was actually moldy, all across the ceiling, we just thought it was normal, managed for nearly twenty years then got ME/CFS from a CT sinus non-contrast. I think they scanned me twice at the one sitting. So the radiation would have damaged already delicate collagen in the brain and head. I think the radiation also damaged my thyroid, which added to the storm.
So: mould exposure –> failure to be able to detox random anthropogenic toxins –> fatigue from MCAS from mould exposure but also collagen damage from anthropogenic toxins, leading to permanent damage –> extreme hypersensitivity –> CT sinus non-contrast due to extreme hypersensitivity –> collagen damage from raidation (+glial activation etc) bc scanned twice but also bc now hypersensitive to radiation and unable to detox, leading to significant damage from the scan –> partial recovery after strict toxin avoidance leads to partial ability to repair the damaged collagen. Hypothetically.
Thank you for this!
My CFS started 20 years ago after a fall from a horse where I hit the ground head-first (albeit with a helmet.) How can I get evaluated for CCI/other mechanical cause?
“(Jeff Wood’s remarkable recovery following spinal surgery to correct craniocervical instability (CCI) and tethered cord shocked the ME/CFS community. It’s safe to say that almost no one saw that coming. In this piece Jeff – the former ME/CFS patient who started all this off – proposes that the pain, fatigue, etc. in ME/CFS could potentially all be explained mechanically.)”
Really, I saw it coming in 2009. Diagnosed with Chronic Fatigue Syndrome in 2001, I did not believe it, just bullsh*t. In 2009 I self-diagnosed myself with upper cervical spine instability. Confirmed by a physician in 2011. I wrote a paper (CVJinstability.org) about my journey. Joseph R. Starr