

The big National Institutes of Health (NIH) effort on long COVID is rolling. It hasn’t come easily or quickly and the NIH has a lot of catching up to do. The world has known long COVID is a serious problem since last summer, but you wouldn’t have known it by the NIH. If it weren’t for NIH Director Francis Collins’s blogs on long COVID, and one workshop, one would have wondered if the NIH even knew long COVID existed.

Congress gave the NIH $1.15 billion dollars to understand and find a cure for long COVID. Now the NIH has to make good on that investment.
No program announcements or grant efforts were created. The only thing I’ve been able to find that the NIH did was to allow add-ons for previous grant applications. A recent search on NIH’s Project Reporter site over a year after it was clear that long COVID was a real and serious condition, uncovered precious few NIH-funded long- COVID grants. For those in the chronic fatigue syndrome (ME/CFS) community, it seemed like a bad case of déjà vu. The NIH was once again ignoring a mysterious but often disabling post-infectious disease.
Then in jumped Congress. If the NIH wasn’t going to lift a finger to help long-COVID patients, Congress would, and at the end of December, President Trump signed a bill that gave the NIH a whopping $1.15 billion dollars to study long COVID over four years.
Now the NIH is on the hook for answers. You don’t provide that kind of change without an expectation that answers will be coming – and as quickly as possible. The NIH, though, is facing enormous challenges – challenges it itself helped to create. It’s dealing with a new disease entity in a field (post-infectious disorders) it’s almost completely ignored. It certainly had the opportunity to explore the field with chronic fatigue syndrome (ME/CFS) – the poster child for infectious diseases.
ME/CFS, with its high rates of disability and its horrifying impacts on functioning – significantly worse than found in heart disease, heart attack, diabetes, and multiple sclerosis – provided ample warning that a pandemic would likely leave hordes of significantly impaired people in its wake.
Given that, it was kind of hilarious to hear NIAID Director Anthony Fauci say that the idea of a pandemic kept him up at night, as he failed to provide even pitiful amounts of funding for the 1-2/12 million people with ME/CFS.

Decades neglecting post-infectious illnesses meant the NIH was almost completely unprepared for the advent of long COVID.
Those decades of neglect meant the NIH doesn’t have set protocols, a deep knowledge base, or a large bench of researchers or doctors to draw on as it tries to tackle long COVID. Virtually everyone the NIH funds will in some way be new to this game. Learning on the fly is not a great way to carry out a project like this.
Now that Congress had given the NIH funding, though, it appears to have fully embraced its mission. It could have chosen to open its coffers to all sorts of grant applications – resulting in the chaos we often see in medical research. Instead, in his February blog, “NIH launches new initiative to study Long COVID”, NIH Director Francis Collins indicated the NIH was taking a highly, organized, methodical approach to long COVID.
The groundwork for that approach was laid with three enormous infrastructure grants (48 million dollars – New York University of Medicine; $46 million – Mass General Hospital, $40 million – Mayo Clinic) that were announced in spring/summer. That meant the NIH spent almost $140 million – 12% of its total long-COVID funding – to develop the core infrastructure (Science Core, Data Resource Core, Biorepository Core, Interactive Data Portals / Robust Analytic Tools) for the massive effort.
The NIH provided short-term grants in May and June to no less than 30 institutions simply to develop the master protocols for the studies. The standardized trial designs and research methods that resulted, though, will allow researchers to speak the same language, enabling them to quickly glean insights from the studies underway. The harmonized data will go into large databases that will provide the meat for large analytical studies.
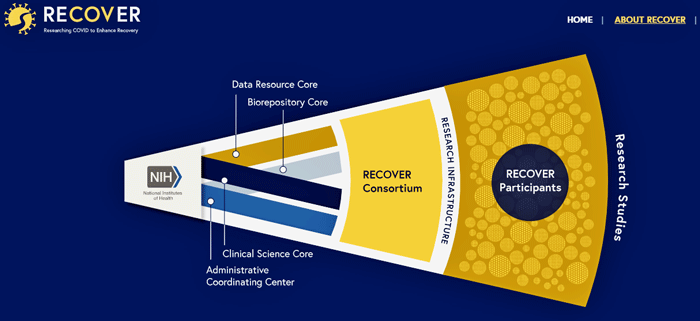
The NIH has quickly marshalled an impressive, organized effort to understand long COVID
Patient samples of all sorts of tissues will go into a central biorepository. Wearables, smartphone apps, electronic health records, and telehealth will take advantage of digital-age technologies. Large, long-running cohorts such as the Framingham study that will be integrated into the study, will help researchers understand who gets long COVID and how it’s affecting them. These studies are particularly valuable because they will be able to provide long-COVID biological data – making it easier to see how having long COVID has changed a person’s biology.
Thirty to forty thousand people will be followed long term. Hundreds of clinical research sites should be announced soon. Other post-infectious cohorts including ME/CFS, and healthy controls, will serve as control groups. Correction – Apparently the NIH will not be including people with ME/CFS in its initial grant package. The NIH specifically mentioned ME/CFS in its grant information and prominently featured the below statement featuring ME/CFS on the FAQ section of the RecoverCOVID website.
“… may also help improve our understanding of other post-viral syndromes, such as myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), and autoimmune diseases—conditions in which the body’s immune system attacks healthy cells.”
It took nine months after NIH knew it was getting funds for the NIH to announce what its major effort entailed. Was this the NIH lagging behind on long COVID? Not at all.
This is actually what the NIH on speed looks like. The NIH typically takes six to eight months to create a grant package. This time it created the long-COVID infrastructure package in two months. It usually takes months and months to review the grant applications it gets. The NIH reported though, it’s already awarded $500 million in grant awards – almost half the money provided by Congress – to over 100 researchers at more than 30 institutions. The NIH is actually moving with blazing speed. Director Collins said it would ordinarily take the NIH 2-4 years to produce something like this.
Urgent Request for Long-COVID Clinical Trials
In August, the NIH did something remarkable. It created an “Urgent” request for long-COVID clinical trial applications. This request, perhaps more than anything, demonstrates how the NIH is casting aside old behaviors as it attempts to quickly deal with long COVID
The NIH states that it will not fund clinical trials for ME/CFS because it doesn’t believe an evidence base exists that could produce positive results. Dr. Koroshetz has warned that moving too fast into clinical trials could doom later trials for ME/CFS if the early trials didn’t work out. The NIH believes the science needs to be built up first.

Even before we know anything substantive about long COVID, the NIH has put out an “urgent” call for clinical trials.
That’s clearly not the stance it’s taking with long COVID. The NIH is urgently asking for clinical trial applications long before we know anything substantive about the disease. The Request, “Urgent Request for Applications (RFA) to Repurpose Existing Drugs to Treat Long COVID”, stated: “There is an urgent public health need to find therapies to ameliorate COVID-19 disease sequelae”. The RFA will support Phase I or II clinical trials with this effort and is particularly looking for “novel” treatments.
The NIH Is willing to plow through quite a few failed trials and spend quite a bit of money, to find a few things that work. That’s completely contrary to how the NIH usually works but it’s apparently what happens when Congress hands over a billion dollars and says figure this thing out. Given the overlap we’ve seen between long COVID and ME/CFS, it would be surprising, indeed, if some of those clinical trials didn’t open opportunities for people with ME/CFS as well.
Enormous Challenge – Enormous Opportunity
While the challenges are enormous, so is the opportunity. The NIH has been given funds to bring all its resources, all its talent, and all its organizational and technological expertise to bear on a brand-new disease entity. This is its chance to show what it can do. If it works out, I imagine this effort will set the template for future others.
It’s taken 9 months to get to this point, but Collins doesn’t expect it will take years to glean important insights into long COVID – he expects they will begin showing up in the “coming months”.
“… these studies are expected to provide insights over the coming months into many important questions including the incidence and prevalence of long-term effects from SARS-CoV-2 infection, the range of symptoms, underlying causes, risk factors, outcomes, and potential strategies for treatment and prevention.”
Time will tell how this highly organized and quite impressive approach will fare. We won’t know who has been funded, what the studies are assessing, or whether ME/CFS or other post-infectious disease cohorts will be involved until the grant data has been released.
With 100 researchers funded thus far to the tune of some $250 million, it appears that the NIH has been focused on funding large studies that are running into the tens of millions of dollars. If that’s right, that kind of large study probably cuts out just about every ME/CFS researcher in the book – potentially leaving a lot of knowledge and expertise on how to understand and work with post-infectious diseases on the table. With about $650 million left, the NIH still has plenty of money to engage smaller research efforts in the fight.
- NIH-funded studies are going to need lots of long COVID participants. Sign up to get info on the NIH effort and enroll in studies
The NIH may be the biggest medical funder in the world, but it’s certainly not the only one. Long-COVID studies are starting to pour in from countries across the globe. Those studies will be the subject of an upcoming blog.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


I wonder how your average researcher views ME/CFS with respect to Long-Covid; like the ME/CFS community certainly see these two illness as intimately related based on a shared symptomatology, but do professionals? Im no scientisist so absolutely no clue as to whether there is scientific basis (not *only* symptom-based) to lump them togther, as so many do. What im trying to imagine, with a little hope, is that researchers would require an exploration of ME/CFS research so far in order to progress in the LC research (i.e the consideration of ME/CFS would be intrinsic to the the study of LC etc..)
God knows. The NIH does feature ME/CFS pretty prominently in one part of the RecoverCOVID website and it did mention ME/CFS in the grant opportunity and long COVID certainly has elevated the prominence of ME/CFS – but do most researchers know much about it??? Another question is whether the NIH is attempting to link ME/CFS doctors with the researchers in the long COVID network? Is it pushing ME/CFS patients as a control group? It was good to see ME/CFS researchers featured in the Biology of Fatigue workshop….
Long COVID researchers could learn a ton from the exercise-based studies done in ME/CFS. Let’s hope they don’t have to reinvent that wheel. Post-exertional malaise should be front and center in the studies. Lenny Jason’s DePaul Questionnaire should be as well.
We’ll see! Looking forward to seeing what studies the NIH has actually funded with its $250 million outlay.
Don’t worry top notch researcher will read and digest all the current studies on post viral illnesses including ME/CFs. And they will do so surprisingly quickly and competently.
Do you know if they are doing any research into structural issues like tethered cord and CCI? They are pretty common in ME/CFS and more and more people with Long Covid are reporting structural symptoms and are getting diagnosed. Also, do we know if the NIH is researching connective tissue damage and MCAS in relation to Long Covid? This could provide valuable insights for ME/CFS as well.
That’s the kind of topic which someone unfamiliar with ME/CFS would completely miss. Ditto with mast cells. I wouldn’t hold my breath but we will see.
I think we can expect the immune system, the brain, the blood vessels and the muscles to get a lot of attention.
Dr. Amy Proal announced just a few days ago that PolyBio Research Foundation is going to do a study that includes structural issues. Several people replied on twitter (including me) we are willing to volunteer, but then they posted another tweet that they are using existing patients from 2 institutions that have already been confirmed to have all of the conditions they are looking at.
https://twitter.com/polybioRF/status/1438190714572128260
Cool – good to hear that a research group is embracing structural issues.
I wish, I wish, I wish, congres had done that (giving so much money to NIH) long time ago for ME/cfs. Even now. you see, if they want, they can! and they can go super fast with big study’s, trials for treatment, etc
I would have wished that many of congres had /knew persons with ME/cfs and we would be “cured” a long time ago or at least better
I am glad for the long covid haulers, but ME/cfs, FM, chronic lyme, etc we will have to wate and see and hope anxious for a small part of it.
when i read the numbers of study participants, that is how for excample breastcancer research is done. for ME/cfs i only know of the UK decode ME study who will have 20.000 or 25.000 participants for ME.
it only shows me, if they want, they can…
and how peanfull also for all the ME/cfs researchers who hardly get fundings, mostly donations or nothing and no fast aprovement for trials like for excample nancy klimas, etc
It’s a whole combination of things coming together – this huge pandemic, the many, many media stories on long COVID, the strong advocacy, and then there’s Congress providing more money for long COVID than we imagined. I’m sorry for anyone who has to go through this but it’s actually better than we thought it might.
I imagine that there are more people with post-infectious illnesses that have been diagnosed with ME/CFS, fibromyalgia, POTS, EDS, and others than there are people with long COVID but they trickled in under the radar for the most.
Now things are moving. I would just be so shocked if we didn’t find out major things that apply to ME/CFS.
i really really hope so you are right with: “I would just be so shocked if we didn’t find out major things that apply to ME/CFS.” if they then would put real money in further research for ME/cfs and other ilnesses we would get somewhere, but real money like for covid long haulers. if they do not do that, i think we still would be stuck. finding major things but no further research and no fast treatment cures. lets cross fingers!!! do you know, they have in my country even not heard of long covid!!! can you imagine that? it is like it is only in the US, UK, and maybe canada or australia…
Pretty sure its the same disease so it will apply directly or almost directly to m.e.
Is there any word on what came out of the open medicine foundation annual conference Cort
There is also significant also overlap with Idiopathic intracranial hypertension. I have had FM for over thirty years. In May I had a surgery in which I was given an epidural. During the surgery my blood pressure dropped to 40/30. I actually felt better and slept better the first month post surgery. After my blood pressure was normal, I started having trouble with my left eye. I now can feel head pressure that I did not feel before the surgery. My eye calmed down when I cut my salt intake.
I also joined an IIH group on social media. to find out more about it. Several women in the group have said they also have FM. I think I am on the cusp of IIH, but I do not suffer they way many of the young women do with this disorder. I am 72, and I do not get migraines. Several of the women have had stents and shunts in their brains. If I feel that my pressure is up, I may get a bit of POTS. IIH is an orphan illness, and most neurologists have had little experience with it. I hope Covid research can help with this debilitating disorder.
Konijn, Congress gave money for CFS before 2000, a line item in the budget. The money was spent on other diseases. A whistle-blower reported this, Rep.John Porter (R, Illinois) called Congressional hearings to chastise them for ignoring what the Congress said to do. That is what happened in the past when Congress gave targeted money and we need no repeat of that story. Please do look to the future with hope, with this far larger amount of money and so many people getting ill and potentially disabled for life.
The Academy of Medicine report is a plus, and there is a lot for new researchers to read in addition to that summary of knowledge, to speed them in their way.
The one hope I have is that the British NICE group posts its new guidelines for ME/CFS and formally gives up the old ones, which are based on the notion that GET and CBT help with M.E. They almost made the big step, then chickened out, caved to pressure from the shrinks. They take up the topic again next month.
and with the centers of excellence for ME, they never really wanted
what a difference!
I’ll bet Centers of Excellence from long COVID are coming – which Emily Taylor hopes will ultimately be turned into Centers of Excellence for ME/CFS
Gosh, those who have been sicker for longer than long hauling get to queue at the end of the line?
Strange way of prioritizing and triaging people…
What’s appalling is due to the lack of funding for ME/CFS by Fauci and those in the NIH, we now have potentially millions of people with long Covid unfortunately suffering without a single therapy to help them. Therapies that could have existed prior to this pandemic if researchers been funded to investigate ME/CFS.
Let’s not forget the main reason why funding was held back, the fraudulent PACE trial run by psychiatrists, some linked to to the medical insurance industry
It’s such an appalling scandal I think it would make a jaw dropping documentary.
There’s new research from New Zealand now showing both these long term diseases are probably actually ME/CFS, as the University of Otago recently discovered the same unusual protein profiles and methylation profiles in ME/CFS patients are also showing in Long Covid patients.
Some Long Covid patients have different problems like organ damage. But as many of us have read, there’s a huge amount of people with the longest form of Long Covid with the exact same symptoms as ME/CFS.
In the audio interview link (at 6 minutes 35 seconds into this interview, the researcher admits they found the same biological profiles in both ME/CFS and Long Covid)
ME/CFS and Lond Covid
Radio NZ
https://www.rnz.co.nz/national/programmes/afternoons/audio/2018799782/our-changing-world-me-cfs-and-long-covid
Thanks Brendan. I really hope someone in the national media at some point points out that the NIH and Fauci and Collins (although I truly appreciate Collins support of ME/CFS – no other NIH Director has cared) and the NIH itself have ignored the million or so post-infectious disease patients clamoring for support for decades. ME/CFS made it clear that post-infectious illnesses may be almost uniquely functionally impairing. They really missed the boat on this issue.
I think there are multiple reasons the NIH neglected ME/CFS for so long. Here in the US the biopsychosocial approach never really took hold and the NIH has funded few studies in that vein. While that approach in Europe may have tainted things there must be other reasons.
All we really know is that the NIH never seriously stepped up. It was not long ago that it was spending $6 million a year on ME/CFS.
Some of you folks should stop your belly-aching and be grateful that they got the funds and will be studying the same type of thing as CFS. They’re going to find answers and those answers are going to help people with ME/CFS, Fibro and similar diseases.
I’ve been one of the bellyachers. The lack of support for ME/CFS really stands out more than ever now, and it’s a bit hard to let go but you’re right – this is the best news that people with ME/CFS have ever had.
We’ve always wanted the NIH to move on ME/CFS because when it does it produces the kind of large, complex studies that few other institutions produces. It can do some amazing things when it moves, and it’s really moving now with the long haulers.
We still need to see what’s in those studies – and I do wonder about how ME/CFS experts and their knowledge base is going to be brought to bear – but it looks like virtually every sophisticated tool in our medical arsenal is going to be brought to bear on large long hauler studies – and the research is going to be done in an organized and effective manner.
The immune system, the brain, the cardiovascular system, the HPA axis, the muscles, genetics – major topics in ME/CFS – should be explored in scintillating detail in large, well-put-together, well-validated studies. We’ll see about the more fringe topics – the connective tissue connection, Mast Cells, spinal cord problems but in-depth studies of the major body systems seem assured.
Plus the early funding of clinical trials for repurposed drugs will surely offer up new opportunities for treatments.
Since everything suggests that the ME/CFS-like component of long COVID looks very much like ME/CFS the results should amply carry over.
Dear Cort, i can totally understand that you are as you write one of the bellyachers!!!
you have gone also such a verry long long road in desease!
and you have lost friends withh the desease!
you have seen over such long time also what hapened or did not happen with ME, the fals promises , the fals hope, etc
i certainly totally get you, i think…
first seeing and then believing i say, way to long way to ill, reading since internet came…
are: quit bellyaching.
Every voice is important. For every voice here who “bellyaches,” IMO there are thousands—— yes, THOUSANDS who wished they were well enough to even follow what is going on, much less bellyache. People who receive no support and are slowly fading from sight into the graveness of circumstances.
Some may look at it as bellyaching, but without voices sooo many would not know, and still do not know— of the problems cfs and similar diseases have faced.
Such as money line budget direction from congress miss-spent!!!!! At a crucial time that could have turned the corner on cfs / me— and how it is perceived and (mis)understood by many medical professionals and the NIH.
there is for excample study’s that GWI and ME/cfs and FM “are the same” but they differ although like immuneprofiling for excample.
I do not know what your background is, how long and severe ill you are, if you are alone, bedbound, have bad helpservice 4 hours a week, etc
I am +30 years severelly ill, totally alone, 98% bedbound, 4 hours of bad lazy help that i even can not cope with anymore, counting the seasons I survive, every week declining, etc
I should say take a look at the 25% ME group please!
I have lost everything and everyone as so many, no chance for children (lucky for them or i had to let them adopt to someone because I could not care for them.
not speaking about the 6 or 7% higher suicides, euthanasias, dying of complications-co-morbiditys that even are not looked for because you can not go to specialist, you do not tolerate light, noise, etc from hospital and even are fysical so impaired that you could not do the needed tests
and you live in a country where ME or Long covid does not excist. ME is still just cfs and the guidelines are a few sessions of GET and CBT. No intrest or knowledge from GP, even not possible to try LDN,low dose abilify, mestinon, you name it
and over decades, when there was internet, you followed all the promises of a cure, money, etc and the promises where everytime broken.
your life has simply gone away and you probebly do not even make it until here or elsewhere comes something up.
and i speak not only for me, or the 25% ME group or so, but think about ME existed long time ago, more then 30+ years and through wich hell those people have must gone and died with it.
On the 25% ME group, people disapear, it has cost for an illness that probebly excisted all the time cost so many lives. Even dr bateman her sister died of a special form of cancer linked to ME.
it is bitter sweet, more bitter then sweet. so no i am not gratefull, so no i do not trust them, so yes i am belly-aching or what ever you want.
can you imagine how my father felt dying of asbestosis and he was my only caregiver?Knowing how he must left his verry sick “child” behind!
so there is a lot more to say about belly-aching and be gratefull…
to many people have allready gone due to ME or never had the chance to get well in there lifetime or get a little bit better and how they where mistreated on top of it!
think about those please…
Agree with you, konijn
(also I had meant to say re: Instead of typo ‘are’)
Agreed! Answers are on the way!
Hi. From above: “The NIH reported though, it’s already awarded $500 million in grant awards – almost half the money provided by Congress – to over 100 researchers at more than 30 institutions.”
From the “500 million” link: “The National Institutes of Health awarded nearly $470 million… The NIH REsearching COVID to Enhance Recovery (RECOVER) Initiative made the parent award to New York University (NYU) Langone Health, New York City, which will make multiple sub-awards to more than 100 researchers at more than 30 institutions and serves as the RECOVER Clinical Science Core.”
Question, please: If sub-awards aren’t yet made, how is that more than 100 researchers at more than 30 institutions has been determined? Will Langone alone decide who receives sub-awards?
Also, a search of “Conditions We Treat” at Langone Health says that they do not treat ME/CFS (or CFS or ME or PVFS/PIFS).
If Langone doesn’t treat CFS/ME/PVFS/PIFS), why would Langone be entrusted to determine who should receive sub-awards to study a specific post viral syndrome, i.e. Long Covid? And entrusted with nearly half the money awarded by Congress?
Have I misunderstood something? (Tired brain.) Should we be worried?
Thank you!
This was inevitable. It’s a case of too much money colliding with too few ME/CFS researchers and doctors.
If the NIH were going to confine its research studies to organizations that treat ME/CFS it wouldn’t be able to fund many research studies. You could probably count the number of academics centers that have both ME/CFS research efforts and ME/CFS clinics (Nancy Klimas – Nova Southeastern University, Ron Davis – Stanford) on one hand. Other than Dr. Klimas’s, I don’t know of any large ME/CFS clinics that are integrated with a research effort that is embedded at a University. (She might be one to snag one of those big grants. She’s done that before.)
Similarly, if the NIH restricted its research funding to researchers with expertise in post-infectious illnesses it would fund hardly any studies. The vast majority of people who get funded for long COVID will not have any experience in post-infectious diseases or ME/CFS or POTS or fibromyalgia. I don’t know but my guess is that the research efforts getting funded now are large studies coming out large academic centers. We don’t have a lot of those.
Besides – sometimes we forget! -this is long COVID – not ME/CFS. We will have to get used to seeing a whole bunch of researchers leading long COVID efforts that we’ve never heard of and have never done research in ME/CFS, POTS, FM, etc. or as was noted post-infectious illnesses. A new field is basically being birthed before our eyes. I imagine there will be quite a few growing pains.
As to Lagone – it’s leading the research effort and yes it will obviously be making or has made some big decisions. As to the 100 plus research efforts – either I’ve missed them so far or the NIH is just not ready to release them. It’s kind of been this way from the beginning.
Also, please, re the 48 million link above: Does the link show 448 million? Thank you!
Good catch. Yes, it does. I wondered about that as well. At first it said $48 million for the biorepository and then later $448 million. The 448 million may either be a misprint or it may refer to the fact that all the grants are being rewarded by New York Langone.
It sounds as though those of us who were unfortunate enough to get covid, may be better off in the long run. I have had ME/CFS since age 7. I think I got covid in December 2019, before it was officially recognised over here. It just makes the ME/CFS symptoms much worse, and added in shortness of breath. The second AZ vaccine made things worse again. However, I can see that when treatment comes out for Long Covid, I may be eligible for that whereas they may be slower to give the same treatment for ME/CFS. That is one silver lining to having had covid.
I suppose because Congress has granted the NIH $1.15 billion, to research Long Covid over four years,
they now have political cover to spend that money more freely, than if the NIH were spending more limited amounts of money, on the more politically fraught ME/CFS.
It’s galling to think how much money could potentially be wasted, by less experienced Long Covid researchers possibly investigating areas already covered by ME/CFS researchers. But as you say Cort, these are such large studies looking into systems and parts of the body affected by both Long Covid and ME/CFS, that new developments are bound to emerge.
We’ll just have to try and not dwell and ruminate on how frustrating this is for pwME/CFS and ME/CFS researchers, who have been begging for effective treatments and funding for decades.
I imagine there will be and already has been a lot of money wastage in getting a program of this size up and running so quickly – and in what is essentially a new field.
I don’t think the money could have made its way down to ME/CFS and similar researchers but the NIH still has a ton of money to spend. It would be crazy to ignore the hard-won gains of the past couple of decades especially in the exercise and energy field in ME/CFS. We shall see.
Seems to me that the really big grants are going to institutions on the East Coast even though we have some prime centers on the West (including the Bateman Horne Center). Hopefully some of the ‘sub-grants’ are heading to this side of the country–assuming that other post viral disorders are also included.
After a year, Stanford’s ME/CFS Clinic contacted me for a virtual appointment. I was disappointed because I had lined up a narrative with what I thought were some salient points. All that information went out the window as almost the entire 40 minutes got taken up with ‘how would you rate (this symptom)’? questions. We always tangle on this because everyday is different and it is difficult to give an ‘average.’ Even crashes can be long or short and how can you quantify those with a yes or no question and a ten point scale? Shoddy research data IMO.
I was prescribed ultra LDN to be taken with my Norco even though I had an argument with the doctor a year earlier about the research on this–me pro and he saying no such research had occurred. There was more I could comment on… Today I got a post visit survey to fill out–first time for this clinic. I am ‘licking my chops’ because there are a lot of ‘constructive comments’ I want to make!
Anyway, Tuesday I am going in for a Covid test as I have all the symptoms, even though I am fully vaccinated with Pfizer. Fortunately they are mild but I hope I don’t develop ‘double trouble.’
And as an aside, MCAS and fatigue and pain are VERY common in Ehlers-Danlos along with CCI and other connective tissue problems and I hope EDSers are included in these studies too.
The grant offering specifically mentioned ME/CFS – so the opportunity is there. Whether the researchers will take it up on that time will tell.
As your experience indicates we clearly don’t have a standardized approach to ME/CFS. With so few ME/CFS doctors available- all of the probably overworked – we don’t have the infrastructure developed that will cause that to happen. Certainly work has been done in that area but individual physicians will go their own way.
Perhaps some of that money should go to historians. It has been said, those who forget history are doomed to repeat it. Both ME/CFS and Long Covid are diseases primarily of energy deficiency. Back around the turn of the last century there was a lot of investigation of another such disease, beriberi, and a lot of debate about whether it was caused by a micro-organism or a nutritional deficiency. It turned out to be the latter. At the time there was a lot of interest in the newly discovered vitamins and their use in medical treatment. There was also a thriving snake oil industry. In 1910 the Flexner report declared that medical education in America must be based on scientific evidence – a laudable aim – and its recommendations were adopted. Unfortunately it seems it also unscientifically determined that the only acceptable basis for medicine was germ theory, and all else was deemed quackery and severely curtailed. The baby was thrown out with the bathwater. Since that time apparently, any consideration of the role of vitamins in health and disease has been virtually outlawed within the American medical establishment. Perhaps it is time for that attitude and policy to be revisited.
Here’s some info about the Flexner report:
https://en.wikipedia.org/wiki/Flexner_Report
Unfortunately, no funds have been offered for potential treatments. The disease most closely resembles MECFS. We will have tons of research trying to clarify and catalog the features of Long COVID, but no treatments are expected from these set aside funds.
Check out this
The purpose of this urgent funding opportunity announcement is to invite applications to repurpose existing therapeutic agents to treat Coronavirus Disease 2019 (COVID-19) sequelae and associated complications that result from Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) infections.
https://grants.nih.gov/grants/guide/rfa-files/RFA-TR-20-003.html
I always thought the tipping point with NIH grant money into anything with the word “fatigue” in it would come down to disability. Is it cheaper to keep people on government aid or find out why they can’t work, treat them ( or cure them?) so they can return to the work force. Unfortunately, it is far too late for many of us but late is better than never and if long covid money spills over into CFS, we all benefit. A bad taste lingers with CFS patients when the NIH or CDC is mentioned and for good reason.
I am very curious whether the scientists will find the cause of long covid with all that money. With many outbreaks such as chronic Q fever, a cause has never been found.
Everything eventually becomes psychosomatic. Same as ME. A bag of money will never solve a disease, just look at cancer.
I predict an endless search.
We shall see but Q fever has never seen a fraction of the funding that long COVID is getting.
The Myth of ‘Long COVID’
https://spectator.org/long-covid-myth/
It starts before proper research has been done by the doctors.
If we ever find out that a government knew the cause of cfs /me but for some sort of security reason……….did not ever want the trigger exposed…………….and the CDC and or NIH knew this…………………
I can sure see how conspiracy theories get started, because IMO, there is sooo much that has been done soooo poorly that it might be difficult to believe that it was not on purpose.
…….oh wait…… they did miss- spend Congress money for cfs /me on purpose.
Very promising news! BC 007 drug that helps cure Long Covid, maybe even ME/CFS ?
Results of first successful treatment confirmed with two other Long COVID patients
https://www.fau.eu/2021/08/27/news/research/further-patients-benefit-from-drug-against-long-covid/
https://www.openpetition.eu/petition/online/funding-for-bc-007-drug-against-long-covid-and-cfs-me
https://www.reddit.com/r/cfs/comments/p1ie7k/case_study_mecfs_patient_to_trial_the_drug_bc_007/
Cort, can you send this information to important ME/CFS experts? Especially professor Scheibenbogen and Fluge.
These clinical trials for BC 007 appear to have been established for me/cfs before covid came on the horizon. And in fact there are many countries where there are many more people suffering with me/cfs than there are long covid cases, such as in Canada. There are 600000 people with me/cfs in Canada who are not long covid cases.
https://clinicaltrials.gov/ct2/show/NCT04192214
https://clinicaltrials.gov/ct2/show/NCT02955420
This focus taken away from the trials for me/cfs and put on long covid feels like another slap in the face.
There is already evidence in research into long Covid that the majority of people with long Covid also have reactivated Epstein Bar Virus which became reactivated during infection with Covid. As for some recovering quickly and some taking longer is dependent on each person’s immune system. Those who push to hard to resume a normal life risk extended recovery time. ME/CFS research also finds reactivated Epstein Bar Virus one of the main causes. This is why both have the same symptoms. There are some powerful medical people who for what ever reason do not want the truth to be known about ME/CFS or long Covid. This has been shown to be true by the delay of the British NICE guidelines into ME/CFS which was about to reverse it’s guidelines on CBT and GET which they had found to be flawed research and made people worse. But just before releasing new guidelines they were threatened by powerful medical people who for what ever reason didn’t want to change with new research findings.
I recently saw a very disheartening video by Ashok Gupta on FB — actually, I only made it through 8 minutes before I had to stop watching, because I was so filled with anger and despair. It was called “ME/CFS vs. Long Covid”, so it was structured to compare the two. One of his coaches (Shonna) spoke in glowing terms about people with Long Covid — but then nothing about pwME/CFS. Ashok didn’t comment, either. One of the things she said was that pwLongCovid “were all normal, beautiful people who were just going about their lives and got struck with Covid” — and that she felt very protective of them. Again, no comment from her or from Ashok about pwME/CFS, so because of the way the talk was set up, the implication was that her positive, validating, supportive views weren’t applicable to pwME/CFS. I emailed his team to express my despair and my fear that they are selling out pwME/CFS for “the new kid on the block”. Their responses were defensive and missed the mark entirely.
I’ve been ill for decades and have tried zillions of things without success, including Ashok Gupta’s home program. Although his program didn’t work for me, I think of him as someone with integrity and compassion, and I expected more from him and his team. Maybe someone on here watched the entire video and felt that it ended up conveying a better message than the one it started out with. I just couldn’t watch any more of it to find out.
Hi Cort. I have a question for you RE some things you stated in this blog and it would be great if you could provide some clarification. RE the NIH RECOVER Initiative, you said, “Other post-infectious cohorts including ME/CFS, and healthy controls, will serve as control groups. The NIH specifically mentioned ME/CFS in its grant information and prominently featured the below statement featuring ME/CFS on the FAQ section of the RecoverCOVID website.”
Yes, I see the RECOVER FAQ: It’s estimated that millions of Americans suffer from post-viral syndromes other than PASC. Will RECOVER help them? Answer: “RECOVER may help us learn how people recover from viral infections in general. It may also help improve our understanding of other post-viral syndromes, such as myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), and autoimmune diseases—conditions in which the body’s immune system attacks healthy cells.”
But where did you see “ME/CFS” mentioned in the PASC/RECOVER grant information and see/hear that “other post-infectious cohorts, including ME/CFS, will serve as control groups”? The initial PASC/RECOVER ROAs had no mention of “ME/CFS” and we heard in the SEPT 15 NIH RECOVER Stakeholder Telebriefing that they will not be enrolling people with “other disease states” (pre-COVID) at this point in time. Thanks!
I missed that briefing – I did not know that.EVen though they say they’re want to learn about ME/CFS apparently they’re not going to provide funding to study it. Here is some of the wording I misinterpreted:
https://reporter.nih.gov/search/paV240kUGkOvdYoHTDsPhg/project-details/10177277
For example, one of the key outstanding questions is understanding the ways in which the post-acute sequelae of SARS-CoV-2 infection are similar to, and/or distinct from, other post-infectious and post-acute illness syndromes.