

You could see this study coming a mile away. Visser, Van Campen and Rowe have been busy the past couple of years doing breakthrough study after breakthrough study. It was only a matter of time – and not much time at that – before they got to long COVID.
This group researched their specialty – brain blood flows
The small study “Orthostatic Symptoms and Reductions in Cerebral Blood Flow in Long‐Haul COVID‐19 Patients: Similarities with Myalgic
Encephalomyelitis/Chronic Fatigue Syndrome” – contained 60 chronic fatigue syndrome (ME/CFS with POTS and without), and long COVID patients, and healthy controls – focused on two critically important factors: orthostatic intolerance and blood flows to the brain.
While only 10 long haulers were assessed there was no picking and choosing, no plucking out the most severe cases, no thumbs being placed on any scales – the group simply put the first 10 long haulers seen in their clinic into their study. All the patients – both the long COVID and the ME/CFS patients – in the study fulfilled the IOM criteria for chronic fatigue syndrome.
They assessed symptoms, then vaulted the participants upon a tilt table, and watched their cardiovascular systems attempt to adjust.
The symptom sets of the two groups were almost identical, with the long COVID group having a slight edge in severity. The group certainly tried to pry the groups apart but even an analysis of 21 different symptom clusters found in the Fukuda, Canadian Criteria, and IOM criteria, found no difference in symptoms between the long COVID and ME/CFS patients (with or without POTS).
Only hypersensitivity to foods and/or chemicals was more common in the ME/CFS group – perhaps suggesting that the hypersensitivity issues tend to show up later.
Double Long COVID Whammy
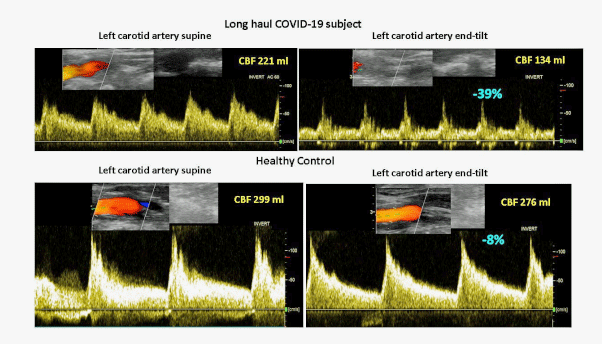
Reduced cerebral blood flows: long COVID on top and healthy control on bottom. Left is at baseline and right is when tilted.
This study found both reduced blood flows to the brain as well as high heart rates (POTS) in the long COVID patients. Given that the long COVID patients displayed both POTS and reduced blood flows to the brain, it was not surprising to find that they had even more reduced brain blood flows than the ME/CFS patients without POTS.
Talk about interrelationships between diseases. The same scenario – reduced blood flows to the brain – has been found in people with ME/CFS (without POTS and with POTS), people with POTS, and people with long COVID.
The same is true for the muscles; invasive exercise studies have found reductions in the blood flows to the muscles in long COVID and ME/CFS. With a recent large study highlighting possible endothelial cell/blood vessel problems in long COVID, the blood vessel/blood flow connection seems to be getting stronger and stronger in all these diseases.
Deconditioning Denied – Again
Deconditioning is, of course, going to rear its head in long COVID. The Van Campen/Rowe/Visser group has been instrumental in showing that even years of ME/CFS do not cause energy production problems in ME/CFS. They are there from the beginning and they are present whether someone with ME/CFS is deconditioned or not.
Now comes another slant. The long COVID patients were physically fit before becoming ill and developed the orthostatic symptoms that showed up when they stood early in the illness – before deconditioning could have kicked in – and suggested that blood flows to the brain began dropping very early in the illness.
The authors also appear to have cleared up an interesting question: why do some people with very high heart rates upon standing who fit the POTS heart rate criteria experience no symptoms while standing up? It turns out that a high heart rate is not the complete answer in POTS.
Using new technology, the Visser group determined that POTS is a disease of sympathetic overdrive (including high heart rate) and, most importantly, reduced blood flows to the brain.
The inability to distinguish this has caused problems because it’s given doctors an opening to dismiss the high heart rate problems found in POTS and slap a psychological label on POTS patients. It’s remarkable how dangerous incomplete research can be.
Trigger

Different triggers appear to produce the same general illness. They all need to be assessed
The study also assessed a factor that’s going to become increasingly important for the ME/CFS community: disease trigger. Many people with long COVID are, understandably, desperate to get confirmation that they’ve been infected with the coronavirus to validate their illness and hopefully avoid being dismissed by the medical community.
ME/CFS has been linked to long COVID via its common post-infectious trigger, but a significant portion of people with ME/CFS either don’t have a post-infectious trigger or don’t realize they had one. This study, for instance, found that over 40% of ME/CFS patients did not report that an infection triggered their illness – yet their symptom set and, as we’ll see, their test results were apparently almost identical to those found in the postinfectious patients.
That brings up a bit of a conundrum to the long COVID/ME/CFS connection. Thus far two major hypotheses regarding long COVID require either an autoimmune response to a virus or a long-lasting inflammatory response to viral proteins. In either case, a virus is needed.
Since both of those hypotheses end up with the blood vessels there may be a nonviral path to blood vessel dysfunction which has not been uncovered. Or it may be that everyone with these diseases actually had an infectious onset but the onset didn’t always produce normal flulike symptoms – thus was hidden. An atypical form of infectious mononucleosis exists, for instance, which does not produce swollen lymph glands, fever, etc. but which produces similar immune abnormalities.
Studies that assess disease triggers, then, are going to critical in bringing non-infectious triggered patients into the broad fold of research underway.
Missed Messages
It’s important, both for people with long Covid and for people with ME/CFS, that the similarities between the two diseases are recognized. A survey, suggests, though, that the message has not been getting out to the doctors.
Despite the fact that people with long Covid often meet the criteria for ME/CFS, and that treatment protocols that can help symptomatically are readily available, the survey suggests that doctors almost never diagnose long COVID patients with either ME/CFS (3%) or postural orthostatic tachycardia syndrome (POTS) (4%).
Long COVID, then, appears largely to be seen, at least at the doctor level, as its own entity that’s inextricably linked to the coronavirus but not necessarily to other diseases – including the ones it most closely fits.
Whose Universe?
This similarity—together with the cardiac index and cerebral blood flow reduction found in both long‐haul COVID‐19 cases and ME/CFS controls—supports the view that long‐haul COVID‐19, with a symptom duration over 6 months, is a form of ME/CFS. The authors.

Should long COVID (and other post-infectious and non-post-infectious disease states) be seen as subsets of ME/CFS?
That’s problematic given a big question hovering over the field: how long COVID fits into the ME/CFS universe, and how ME/CFS fits into the long COVID universe. Long COVID is getting much more research funding than ME/CFS ever has, and given that, there will be a strong pull to define it in its own terms – leaving its sister diseases to move forward on their own.
Indeed, some people with long COVID are understandably reluctant to have it lumped in with a stigmatized disease like ME/CFS. Turning aside from the moral issue of turning one’s back on a group of long-neglected patients who appear to have essentially the same illness, there are several reasons why it would be best for all to have long COVID understood as a subset of ME/CFS.
Consider this: ME/CFS describes a kind of broad general fatiguing and exertion challenging condition under which all sorts of other conditions, post-infectious and otherwise, can be fitted. Long COVID, post-treatment Lyme syndrome, postural orthostatic tachycardia syndrome, fibromyalgia, post ICU syndrome, and probably every post-infectious syndrome known can all fit inside an ME/CFS designation.
Given the infectious triggers found in many of these diseases, it would be a missed opportunity for long COVID not to be thoroughly understood and seen as being simply the most prominent of many postinfectious states. In a best-case scenario, long COVID will give birth to what will essentially be a new field of postinfectious disease research.
Long COVID, though, should also breathe life into the study of fatiguing, exertion intolerant, non-post-infectious states. As long COVID becomes more and more synonymous with ME/CFS, logic demands that non-infectious sources of exertion intolerance, fatigue, etc. found in ME/CFS be investigated as well.
The fact that ME/CFS does not require a postinfectious trigger to be present, and that it provides broad criteria focused on fatigue, exercise intolerance, and other symptoms, means that for at least right now, it makes sense it is used as a general umbrella term under which all these other diseases can be linked.
Conclusion
This study was too small to definitively show that reduced blood flows to the brain are found in long COVID but it lays out a marker that larger, better funded, researchers can use to explore long COVID. It also rebuts deconditioning claims and links long COVID, ME/CFS and POTS together in a new way which makes sense given other findings of reduced blood flows.
It also potentially adds yet another link in the long COVID – ME/CFS chain that seems to be growing ever stronger. Thus far – reduced blood flows, impaired ability to produce energy during exercise, hypercoagulation, deformed red blood cell, neuroinflammation, ACE-2 dysregulation, T-cell exhaustion, NK cell problems, gut dysbiosis, hypercatabolic state – are all possibilities.
Hopefully, the big research efforts in the US – of which we’ve heard little thus far – are checking out this study and are responding appropriately. Dysautonomia – long a focus in ME/CFS and POTS – is a recognized problem in long COVID and is getting more study. Still, the dysautonomia field is not a large one and it remains to be seen if the large U.S. studies will embrace it.
BIG (Little) Donation Drive Update
Thanks to the other over 400 people who have supported Health Rising during its yearend fundraising drive!

If that’s the kind of work that you want to hear about please support us!


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


It’s all Post viral disease, whether covid, EBV, herpes family of viruses, etc.
The fact that doctors rarely diagnose long COVID patients with M.E. shows their arrogance – It’s easier to make up a new name rather than admit we have been gaslit by many of them for decades.
Not easy to admit that you’ve been wrong for so long. It really takes something.
Post viral disease=Low blood flow in the brain= brain fog = low dopamine= feeling really bad = CFS persist= Low blood flow in the brain…
Exactly!!!!! 🤯
It can take years for people with ME/CFS to be diagnosed. My daughter had to diagnose herself after seeing many specialists. In addition, her symptoms have worsened considerably over time. It is likely that many ME/CFS sufferers are unaware of what first triggered the disorder years later when it is finally recognized, leading to the assumption that it was non-viral. It is also possible that the viral trigger for ME/CFS was a mild infection and that ME/CFS developed some time later and that the two were not recognized as being connected.
ME is caused by a virus. Period. Researchers have spent years studing its symptoms only, but not the actual disease.
Whether the virus is from Covid, CMV, EBV, etc., the virus attacks the immune system. In order for this to happen, the virus has to have found a place to reside without being identified or destroyed by the body. Secondly, since only a segment of the population becomes sick from the virus, it is clear that this it is not the virus itself, but the person’s immune reaction to it. For this to happen, the virus has to be residing in a broken or damaged immune gene which is allowing it to survive and continiously attack the body.
This is the same story repeated in the discovery of Burkett’s Lymphnoma. It was not the virus itself which caused the cancer, but the fact that the virus found its way into a broken gene which then caused the disease, later called Burkitts Lymphoma.
Researchers need to begin the monumental task of finding which broken immune gene is harboring the virus in order to eliminate it and cure this disease.
Looking forward to see who, which doctors and researchers, will be the early birds in admitting this oversight!
(If I were a betting woman I’d bet we know several of the names of the ‘early admitters’!)
Wayne’s is correct. This is all post-viral. For years I have had many physician friends from undergrad days tell me that ME/CFS was just a “sleep disorder”. This is what they learned in their very brief course in Immunology in Med School. They do not have a “bio-marker”, so they ramble on to the their next patient. NIH is largely responsible for this treatment disaster!
I had my cerebral blood flow measured at Dr Vissers clinic. I went there because of POTS after covid and thought they just put me in betablockers and stockings. However I also got diagnosed with ME. Now I know that when upright I have nearly 40% blood reduction to the brain, but sitting it is also greatly reduced which explains getting brain fog and not being able to watch a tv show which lasts longer than say 30 minutes.
These doctors are wonderful and have been instrumental in demonstrating there is a bio-medical origin of ME and now also Long Covid. I agree that Long Covid is ME but since ME has such a bad reputation many LC patients would prefer to think of it as a seperate disease. That was also my initial response. Would make it easier to get in disability, ME is often not tsken seriously.
I have fairly severe ME. They put me on medications that did a great job lowering my blood pressure. Last week, they took my blood pressure and it was 168/98. My Dr called out, “Bio Marker!” I am to see a cardiologist January 4th. I feel it is my left vertical is week and putting me in heart failure. If the will replace my vent rival, I will submit.
I’m on Spironolactone which reduces my blood pressure and prevents POTS, presumably from beta adrenergic effects. There was a little, positive study with it and ME/CFS. It also can inhibit Epstein Barr virus. I get POTS and steadily rising high blood pressure without it. Weird, I know, but some of us have this combination. I was also going into heart failure until I got super strict with pacing so my relapses we’re at least a month apart. That let my heart heal some, but the Spironolactone was critical. I’m on high doses. I hope something works out for you. Best Wishes, Chris
Hi Christyne. Would you mind telling us the dosing of Spironolactone that has helped you? I currently take 100mg 2X day. I can’t say that I notice any difference if I miss a dose or a day. Maybe my dosing is too low or not frequent enough? Any help would be greatly appreciated! Best Wishes, Martha
Dr. M.Hanson said in her last lecture that she believes everyone who has ME has contracted the illness after an infection, even though the person may not have realised it. They could have been asymptomatic. But, the more pressing issue is: how to treat this? Mestinon simply does not work for many ME patients, and many have side effects. Are there other options to help blood flow to the brain? Thanks Cort.
Not sure if this is ok to post here, but I just learned that a doctor in Arizona I had a tilt table test etc. with about 10 years ago has added measuring brain blood flow and electrical activity in the brain to their tilt table protocol. I think its a great thing to check and wish I had that.
https://complexneurology.com/services/diagnostic-testing/
Autonomic Testing
Autonomic testing is a complex group of procedures used to diagnose POTS and other autonomic disorders. It entails measurements of multiple parameters, to include blood pressure, heart rate, EKG, breathing and sweat function. Patients are also placed on a “tilt table.” This involves being tilted upright for 10 minutes to see how gravity affects cardiovascular and brain function. To improve the diagnostic yield of testing, the Center also employs measures of blood and flow and electrical activity of the brain. We are the only facility in Arizona which includes this testing with the tilt table.
I’ve had ME since 1977, from Giardiasis, but only diagnosed in 2013. Always icy feet, in 1998 my heels cracked to bleeding. Instead of creams I started Gingko Biloba high dose. My heels healed, I’ve been using it ever since as I feel better taking it. It expands capillaries.
Yessss!!! Ginkgo is one of the plants I think of as potential specific in ME/CFS . Along w gotu kola…. Garlic and onion… and others. Would you be willing to tell me more about it one on one just so I can learn?! Xoxo
Hi Brittany, I’m not very knowledgeable as using it has been very straightforward, and if there’s interest in the subject we ought to keep it public.
Looking it up I found that it was the first dessiduous tree to develop on our earth, maybe it’s a mother tree to all those which fed our emerging race. A beautiful thought at least.
@Brittany: Are you able to eat garlic and onion? Once I became ill with ME, I get sick from even the smell of it, cooked or raw.
Dear Agate Karevoll, I greatly appreciate your comment, especially since it was paired with the above study on blood flow to the brain. If I may, I would greatly appreciate knowing the size of the dose of gingko Bilbao that you use daily, if you divide your doses, and if the time of day matters when you take them. After c@–@ in 2020, and then mononucleosis this March, I have dealt with symptoms, including icy feet and painful heels.
Dear Judith, I’m taking 1200 mg equivalent concentrate, in with my other supplements at breakfast. All decent brands seem ok. If the climate here was propitious I’d grow a tree and eat a leaf every day. My icy clods feet are better now I’ve attended to thyroid and adrenal issues but I’d never consider giving up ginkgo.
https://www.frontiersin.org/articles/10.3389/fnut.2021.658630/full
I just found this study on this supplement. Thanks for mentioning, I’m going to gone it a go.
I looked up the study Mike mentioned on ginko and another substance. Looks like you have to create a custom blend, but they do give a lot of details about dosage. There was one line that I have to reprint here, it just made me laugh for some reason- maybe the juxtaposition of lived reality and scientific understatement(?). The authors wrote: “A high prevalence of nutritional supplement usage has been reported among CFS patients.”
No kidding?!!! 🙂
Are you sure its 1200mg? That’s like 10x recommended daily dosage.
What were your starting dosage? Have you increased it over time? I’ve read online that some people experience higher heart rate after taking Gingko, other lower heart rate. What’s your experience?
My wife’s doctor looked at me funny when I asked if she had cfs, paused for a bit and said “yes, it does look like symptoms that can occur after certain infections”. Later she proclaimed my wife had long covid, despite the implication that she would have had to have got covid at a time when there was no reported covid in the community within the whole country. When pressed on this she said “oh, I think covid has been under reported”. So, when you suggest doctors are dismissing long covid as being a subset of cfs, I’d say that, like my wife’s doctor, doctors might instead be preferring to diagnose patients with something that is more likely to have treatments available for, research to occur, and that can give the patient hope. Of course this won’t work for my wife if the treatment depends on the cause, which almost definitely want covid.
Very interesting.
Cameron, first, I totally agree, very, very interesting.
Meanwhile, like you I was found to have a very fatiguing flu-like garlic sensitivity or allergy. I just can’t handle garlic now, at all. This discovery came up with the first doctor to diagnose my “chronic fatigue-like” and “fibromyalgia-like” issue approx. 20 years ago. Note, I’ve known this garlic intolerance to happen to some people who have myasthenia gravis fwiw. My dad had some kind of problem from eating garlic, it fatigued him (was born in 1923). “Muscular rheumatism” – worth looking up – ran in his family, along with dairy allergies (grandmother, born 1890). My maternal grandmother (born 1893) had an anaphylactic allergy to onions. Does anyone out there know of any connections related to this stuff?
Yes, Elizabethkay I have a massive problem with onions and garlic. They’re viewed as good prebiotics, I believe, and have certain sugars in them. My Kryptonite is fructose – it’s 50% of table sugar and in so many foods. I can’t eat any fruit or higher carb veg. This developed in 2007. Took me a very long time to figure it out. Glucose tolerance tests, use glucose! I couldn’t work out why I didn’t keel over after the glucose tolerance tests. DIY investigations & eventually I worked it out. I don’t know if this sounds relevant?
I have many various brain symptoms which I think are caused by different issues. One of them I call Sediment Brain. I couldn’t work out what caused this but now I’m beginning to wonder if it’s from reduced blood flow.
When this occurs, I feel my brain has turned to sediment – like you’d find at the bottom of a pond/lake – dense, dark and heavy. My brain feels like it’s seized up and I can hardly think. (It’s NOT the same as my brain being inflamed and feeling like it’s Smouldering brain or possibly histamine resulting in a Swirly/dizzy brain or low brain blood sugar I call Droopy Brain.) If I continue to try and think, the symptoms become worse and I end up with what I call Burnt Out Exhaust Brain.
I have also literally felt the blood draining out of my brain, like water down the plughole. I don’t know why it suddenly does this? If this happens, I feel terrible and like I’m going to pass out. I have very extensive food sensitivies and at one point thought this might be linked to an immune reaction to having eaten something – possibly with dairy in it?
I don’t know how many people have watched Dr Nina Muirhead @DoctorswithME talk but I can see her struggling, especially as she gets more tired. That seems to be what I experience.
I’m doing much better now and I think Sediment brain kicks off when I’ve been doing too much, for too long. I am aware that reading long pieces drains me the most. There are many long articles, that really interest me but I know they’ll take too much from my brain energy supplies, so I haven’t read them yet.
Very interesting topic.
Tracy, I can so relate to all these different brain experiences. People talk (and doctors ask) about “brainfog” as if it is the/one brain symptom… when I (and I assume many of us) have such a variety of brain states/symptoms. Thanks for highlighting this 🙂
Thanks Jazz and it makes a difference as to what I need to do or not do, depending on what experience I’m having. 🙂
Tracey Anne, I would love to see a poem you’d write on that. Very evocative terms!
Thanks Cameron, I’m a useless poet but I find it easier to differentiate the various experiences I have, if I put it into easily understandable words/visual descriptions 🙂
Really well said! We also have in our household … Friday Night Brain. Which can happen actually any day or time. You get the idea.
Hi Elizabeth, are you feeling like you’re drunk? I even bought some breathalyser tests and tested myself for alcohol levels! They were negative – no alcohol.
Tracey, you have just described what happens to me when I go shopping at a department store. I will be doing fine for awhile and then my brain feels as though it is getting empty. I feel somewhat dizzy and my brain feels a little cold. I start to get nauseous and if I don’t sit down quickly enough, I might throw up. One day I did throw up even though I was already sitting. I went through this happening for years. Never knew when it would happen. My legs got weak, cold feeling brain, dizziness, and nausea. Doctors would say my blood pressure might have dropped. They said my oxygen level dropped. I tested this with Oxymeter and it never dropped. I found out that I have low B12 and take injections for it now. I have Fibromyalgia. Have had it for about 33 years. Never had those symptoms in all the years with fibro. I started feeling better after the injections, but it still happens once in a while when shopping. I am pretty sure it is all related to my brain somehow.
Hi Jane,
So sorry to hear you have those horrible symptoms. I still have the draining brain feeling and I have to be aware of it because it can happen quickly. Thankfully it doesn’t happen all the time and seems to be worse in the morning. If I can crank my system up, I seem to sort of manage to get through the rest of the day.
If you are still struggling with these symptoms, have a look at the info on orthostatic intolerance from the Bateman Horne Center (website and YouTube channel).
One thing: Bloodflow problem to the brain is not found with an MRI scan. Why? Because you lay down.
Has anyone ever isolated a virus and demonstrated its pathology?
What test was done to measure the brain blood flow? Was it a doppler ultrasound?
Extracranial doppler ultrasound
Internal carotid artery and vertebral artery Doppler flow velocity frames were ac‐
quired by one operator (FCV), using a Vivid‐I system (GE Healthcare, Hoevelaken, The
Netherlands) equipped with a 6–13 MHz linear transducer. High resolution B mode im‐
ages, color Doppler images and the Doppler velocity spectrum (pulsed‐wave mode) were
recorded in one frame. At least two consecutive series of six frames per artery were rec‐
orded. Image acquisition for all 4 vessels at each time point (supine and end‐tilt) lasted 3
(1) min. Blood flow of the internal carotid and vertebral arteries was calculated offline by
an investigator (CMCvC), who was unaware of the patient case or control status. Blood
flow in each vessel was calculated from the mean blood flow velocities x the vessel surface
Medicina 2022, 58, 28 4 of 19
area and expressed in mL/min. Vessel diameters were manually traced by CMCvC on B‐
mode images, from the intima to the opposite intima. Surface area was calculated as fol‐
lows: the peak systolic and end diastolic diameters were measured, and the mean diame‐
ter was calculated as: mean diameter = (peak systolic diameter × 1/3) + (end diastolic di‐
ameter × 2/3) [25]. Flow in the individual arteries was calculated in 3–6 cardiac cycles, and
data were averaged. Total cerebral blood flow was calculated by adding the flow of the
four arteries.
I am confused about using spirolonolactone for ME/CFS, and specifically POTS. It’s a diuretic and yes, it is used for heart failure, but not for (non-adrenergic) POTS. Low tech recommendations for POTS are to salt and fluid load! I got balled out for taking spirolonolactone while displaying POTSy symptoms because using it was known to make the POTS worse!
I do wonder about low blood flow to the brain in ME/CFS. I got evaluated for dysautonomia a while back and it didn’t show up on the tests. However, POTS can come and go and for me, it sometimes appears with home testing.
Cort, I think you got a negative clinical POTS test too. I also don’t have so much brain fog except with word finding. Cort, you seem to write and think very clearly as well, but I did notice some issues when you tried to film a verbal blog a while ago. So what’s with that? Clearly the brains are functioning!
However, I have PEM. Lately I notice better energy in the morning which drains away as the day progresses until my body switches to the ‘off’ position by early evening and I am unable to do much of anything. It’s like I have ‘petite crashes’ now rather than long ones that last for days.
Maybe the oxaloacetate is helping. I’m taking about 400mg. per day now.
I have noticed that historically, with every bad flu, my complete energy recovery has taken longer and longer until it morphed into the continuous ME/CFS that I have now. So maybe it is a viral onset…at least for some…
I should add that I was taking spirolonolactone off-label as an androgen blocker to help with some acne. For men it is known, at higher doses, to cause ‘moobs’ (male boobs). Just saying…
I was diagnosed 20 years back. One of so many tests was a brain X-ray with radio-opaque compound. The test showed that I had bilateral problem of blood circulation and bad peripheral circulation in both hemispheres.
In the 2000s British radiologists published few articles about ME and bad circulation in the brain. It was for me the beginning of biological markers and the end of psychiatric pathway of thinking ME.
Reduced blood circulation in the brain – fascinating! Thanks for sharing that Jean. I sincerely hope we see lots of brain imaging studies in long COVID.
Just wanted to add that low blood flow to the brain is found more generally in autonomic disorders, not just in POTS.
Research is lacking, but when Dr Peter Novak and his team at Brigham and Women’s Hospital looked at patients on the books who had symptoms of orthostatic intolerance that seemed to be caused by autonomic dysfunction but did not align with any known orthostatic syndrome, he promptly discovered two new orthostatic syndromes related to low blood flow to the brain.
OCHOS occurs without blood pressure or heart rate derangement, so in the absence of POTS, orthostatic hypotension, etc. HYCH seems a bit more complex, and seems to occur on its own or in conjunction with previously known syndromes.
Here is a press release:
https://www.brighamhealthonamission.org/2019/06/03/expanded-autonomic-testing-helps-to-pinpoint-causes-of-orthostatic-intolerance/
The research studies can be accessed if you dig a little or use Sci-Hub.
Also wanted to add that changes in cerebral blood flow can be measured fairly easily during a tilt table test using transcranial Doppler equipment. Sadly, almost nobody offers this non-invasive testing. It could make a big difference to treatment decisions and research.
Dysautonomia International offered grants this year of up to US$800,000 to institutions to purchase the equipment plus free expert help on how to use it. I wonder whether anyone took them up?
https://www.dysautonomiainternational.org/page.php?ID=37