
The much-anticipated long-COVID research boom – has it begun?
As so much of the future of chronic fatigue syndrome (ME/CFS), fibromyalgia (FM), and related diseases depends on the success of the long-COVID research effort, the first part of the look-ahead for 2022 focuses on long-COVID research. It should be noted that this blog probably understates the amount of ongoing long-COVID research significantly.
Has the Anticipated Boom in Long-COVID Research begun?
Despite the fact that long COVID has only been “a thing” for a year and a half, it’s garnered substantial research. A PubMed search of “chronic fatigue syndrome”, “fibromyalgia”, and “long COVID” from Nov. 2021 to Jan. 23rd, 2022 uncovered 36 ME/CFS papers, 88 fibromyalgia papers, and over 205 long-COVID papers.
It’s clear that except for the NIH – which on its own appears to have funded very few long-COVID studies – the research world has leapt at the chance of studying a new condition. With the U.S. Congress appropriating so much money for long-COVID research, many young researchers, in particular, are undoubtedly asking themselves whether the study of post-infectious diseases presents a good career path.
Of course, it’s not all about ME/CFS – several studies have already looked at the possible intersection between multiple sclerosis and long COVID – and autoimmune, inflammatory, cardiovascular, and nervous system diseases are clearly a possibility.

The Omicron variant will likely leave in its wake a tsunami of long-COVID cases. (From Wikimedia Commons).
The really good news for people with ME/CFS and related post-infectious disorders is that studies of long-COVID prevalence seem to indicate that the condition is often serious and long-lasting. That’s of course, no surprise to many, many people with ME/CFS.
We should expect and hope the lopsided ratio of long COVID to ME/CFS and fibromyalgia papers (6:1; 2.5:1) will grow and grow over time.
It’s notable that we haven’t even begun to see the effects of the almost $500 million the NIH has poured into long COVID in the paper statistics. Plus, the rapid spread of the Omicron variant, which Anthony Fauci has said may ultimately infect just about everyone, could make the tsunami of long-COVID cases predicted last summer look like a piddling beachcomber.
Long-COVID Studies Underway

Massive long-COVID studies are underway.
If all the below studies pan out, long COVID may become one of the most intensely studied conditions of all time. Consider that the studies listed below had begun over a year ago, and do not include the tens of thousands of long-COVID patients the NIH is following, the studies that started after that date, or studies that were simply missed.
- Nancy Klimas will be following 2,200 COVID-19 patients over time in a $4 million study.
- Avindra Nath is following 1,200 COVID-19 patients over time.
- Leonard Jason is tracking several hundred COVID-19 college students over time.
- A 900-person study assessing COVID-19 outcomes is slated to last through 2027.
- A 150-person observational COVID-19 Norwegian study runs through 2023.
- A 250-person Columbia study tracks COVID-19 patients over one year.
- A 250-person Johns Hopkins study will compare inflammatory/immunological, physical, pulmonary, and neuropsychological status in severely ill patients vs patients who simply received oxygen during hospitalization over 12 months.
- A 400-person French study will study sleep, exercise capacity, and respiration in COVID-19 patients for five years.
- A huge (4,000-person) European study will follow anyone with respiratory issues (such as cough, sore throat, etc.) after an infectious illness for two years.
- A 350-person New York University study will assess COVID-19 outcomes over several years in its survivorship database of coronavirus patients.
- A year-long Australian study at St. Vincent’s Hospital in Sydney is following 100 COVID-19 patients.
The Collaborative Cohort of Cohorts for COVID-19 Research (C4R) contains over 100 researchers and will reportedly follow 50,000 patients over time. This study is noteworthy not just for its scope but because it includes within it 14 already established and ongoing cohort studies. Rather remarkably, this effort appears to be largely separate from the congressionally funded long-COVID NIH project.
The Congressionally Funded NIH Project
The size, organization, funding, and scope of the Congressionally funded NIH $1.15 billion Recover long-COVID project dwarfs the other studies.
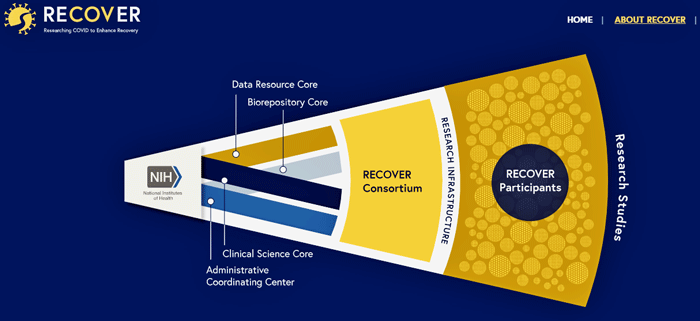
While we don’t know the details, the NIH appears to have created an impressive effort to understand long COVID.
Given Congress’s unexpected largesse, money should not be an object. The NIH has the money to study any part of the body in as much depth as it wished to, and in large cohorts to boot. If major breakthroughs in long COVID aren’t made fairly quickly, it’ll either be because the disease is impenetrable or because the NIH didn’t hire the right blend of brains, expertise, and creativity.
The NIH, for its part, has a lot at stake. In some ways, long COVID is a piece of cake. Not only is the trigger known but we know exactly when it occurred – two factors missing for most chronic diseases. The fact that researchers will be studying a clean set of otherwise healthy patients (no need to account for age, diet, comorbid illnesses, or other complicating factors) simplifies things greatly.
Plus, after two years of this virus, we also know a ton about how it works. The NIH, to its credit, is including patients who’ve been taking part in other very long-term studies in its long-COVID cohorts. That means it will already have a great deal of biological information on some long-COVID patients – giving it a considerable head start on figuring out what went wrong and to whom.
Plus, the enormous amount of money Congress gave the NIH means the NIH can devise exactly the kind of studies it wants. It can use the latest technologies, create the best data repositories, enroll the largest cohorts, build the biggest sample depositories. All the problems that have beset long-COVID’s sister diseases like ME/CFS and fibromyalgia (small study sizes, little researcher interest) were swept away once Congress gave the NIH oodles of money.
All that remains is to put the pieces together. Linking the coronavirus’s known impacts to its long-term effects should, one would think, be relatively easy so far as medical problems go. Compare trying to understand that to trying to understand Alzheimer’s disease – a neurodegenerative disease that usually occurs as a result of a process, aging, which potentially affects every system in the body. Compared to Alzheimer’s, understanding long COVID is a walk in the park.
Of course, the post-infectious field does suffer from the fact that it really hasn’t been a field. The choice of interest for just a handful of researchers (one of whom, thankfully, is Avindra Nath), the field has got pretty shaky legs to stand on. We don’t know much about how diseases like long COVID, long-EBV, long-Lyme disease, long-Giardia, long-Ebola, long SARS-CoV-1 occur.
On the bright side, the small body of knowledge about post-infectious diseases means there are no misguided paradigms to get in the way. Much of the NIH’s initial long-COVID research will, ironically – given its historical antipathy to exploratory studies – be exploratory – and that’s a good thing. (How do you stop a field from getting off the ground? Require a hypothesis before enough data has been generated to provide one.)
The NIH Research Centers
The NIH appears to have put the task of deciding who to fund or not to fund in the hands of the New York University Langone group. As of Sept. almost $500 million had been awarded to over 100 researchers and 200 research sites.
We don’t know who most of those researchers are, but we do know the 17 institutions involved. In general, most appear to be studying about 900 patients over 4 years at a cost of $15-20 million. Since these big grants will pull in many investigators from across these universities, it’s possible that some ME/CFS researchers, such as Ron Davis at Stanford and Jarred Younger at UAB, may get pulled into the grants. (Ron Davis has not yet been contacted.)
Since all we have are press releases from some of them, we just know some broad research topics. On the bright side at least two are focusing on the mitochondria. On the other hand, none mentioned dysautonomia or exercise physiology. It was disappointing, in that regard, not to see Vanderbilt, with its strong dysautonomia department, in the funded group.
Since the NIH is putting so many eggs – almost half of its long COVID funding – into their big study basket – the makeup of the research groups and the focus they take will be critical. We’ll pretty quickly find out how many have done their homework by determining how many are employing exercise stressors – a critical tool in the ME/CFS studies – to get at abnormalities that remain hidden at baseline. Below are the universities which put out press releases regarding their long-COVID funding. (See all the University Centers here.)
- Stanford University – $15 million to study 900 COVID-10 survivors over 4 years led by infectious disease specialists.
- The University of Alabama at Birmingham (UAB) is receiving about the same amount of money to do that same thing.
- The University of Health Science at San Antonio will use brain MRIs, spinal taps, and focus on metabolic issues (including the mitochondria) in its workups of about 900 COVID-19 patients.
- Icahn School of Medicine at Mt Sinai – will focus on what happened to people with severe COVID-19.
- Emory University will bring together immunologists, virologists, pharmacologists, socio-behavioral scientists, epidemiologists, data scientists, and clinical and translational researchers to follow 1000 COVID-19 patients over 4 years.
- The University of Arizona at Tucson will gather together specialists in infectious disease, immunity, inflammation, sleep, mental health, gastroenterology, pulmonary and critical care medicine, neurology, cardiovascular diseases, and virology to peer into its cohort.
- The University of Utah will focus on COVID-19’s effect on pregnant women and the health of their children.
While we don’t know what the studies will consist of, we know that the NIH spent an enormous amount of money ($120 million) finding ways to organize, coordinate, and provide access to the immense amounts of data and the samples that will be collected and concentrated in various data repositories. We also know that specialized mobile apps are being developed to track these patients, and that many tissue samples will be collected and analyzed. Some institutions will also focus on pediatric patients.
NIH-Based Efforts
The NIH, outside of its Congressionally mandated efforts, has made a few small efforts to boost long-COVID funding.
NIH Long-COVID Treatment Study Effort Fails
The NIH acted out of character when in August of 2020 it asked for treatment trials before knowing anything really about long COVID. (The NIH has repeatedly denied funding for treatment trials in ME/CFS because it says it doesn’t know enough about the disease.)
The “Urgent Request for Applications (RFA) to Repurpose Existing Drugs to Treat Long COVID” was open for six months but apparently funded only two studies. The NIH, has not, to my knowledge made any more calls for long-COVID treatment trials.
Administrative Supplement
The Dec. 7th administrative supplement for long COVID will allow those ME/CFS/FM researchers with ongoing NIH studies in applicable fields such as post-infectious diseases (i.e. ME/CFS, POTS, FM) to include long-COVID patients.
Conclusion
We’ll find out over time how many of these efforts succeed but this likely quite incomplete summary indicates that a simply staggering amount of resources have been earmarked for long-COVID research. With the NIH long-COVID research effort in its infancy we’re likely only at the beginning of the beginning of our understanding of long COVID and its connections to ME/CFS, FM, POTS, Lyme Disease, and allied diseases. This should be an exciting year indeed.
- Coming Up: 2022 ME/CFS and FM research efforts and ME/CFS, FM, and long-COVID Clinical Trials






In many countries in Europe, Long Covid -when no organ damage is found- is considered and treated as a psychosomatic disorder just like ME/CFS. Disability is not recognized by insurance doctors. History just keeps repeating itself. It makes me sad. Will those psychosomatic fairy tales never end?
It’s a difficult situation but I don’t see how it could not have turned out this way. There’s much more acceptance of ME/CFS and long COVID in the states and some people here are running into similar roadblocks. I can only imagine that it’s much worse there.
The good news is that all this research underway should end those psychosomatic fairy tales.
A patient of our community went to court in January 2022 with long covid because he was denied disability and the doctor in charge for the hearing told them: “Long Covid and ME/CFS dont exist. There is no proof for those illnesses.”
Good old Europe.
The ‘old country!” It will take more time for Europe but my hope and guess is that in a year or so he will be back and the outcome will be different. Where are you located?
In Belgium it is still CFS not ME or ME/cfs. and goverment says still: a few sessions of get and cbt and you are cured. Of long haulers, i did not hear much or nothing. Maybe someone else in Belgium , maybe verry verry ocasionaly? My help(service), had Lyme together with someone she knew. My help was partially paralised, the other one also severe. Although she still has issues, she “recovered” with antibiotics. the other one not. I do not know the year she had it but she is still young. she said to me that chronic lyme desease was also not accepted for income. Like long haulers. And in ou neighbour country ME excists!!! There is even , sorry my brain, something as an european commission for was it ME or cfs research. But when i was still better and could watch what they did…. I simply can not believe anymore that if in the US something is found for say ME, it will be accepted here soon. The UK is even closer but i think that none of our politicans speak a bit of englisch 🙂 or look around in the world. And all the psychiatrists, internists with there get and cbt are not going to say fast, sorry, we where wrong and leave there seats. Even not in a year Cort! that makes me cynicly bitter laugh. And i am verry verry scared, until the proof is there, first see and then believe, what all this research in the US for long covid, will bring to ME/FM/POTS, etc It allready shows for excample ron davis not asked, nancy klimas gets much money for long haulers but where is ME, this results for her less time for ME, and all the others. If a scientist does not get money for one thing or a compagny, they switch to other things (mostly). Even Berlin cures states now although the european petition for testing on long haulers and ME/cfs, they do only long haulers, you wrote yourself no excercise testing or was it also pots, etc etc etc…first see and then believe. had over decades enough fals promises. And i can see them perfectly fine only going with long haulers further and yes, in the US, ME or so may get a verry verry little bit of it. I hope i am wrong.
Great questions, Konjin. Time will tell. We know long haulers are getting a lot of research funding. Is the NIH here going to step up to the plate and increase funding for the ME/CFS research centers? A significant increase would go a long way to being able to bring long COVID research into the ME/CFS orbit.
I imagine that it will take longer in Belgium but medical system can and have changed course and I imagine that given some definitive findings they will over time as well. I would hope that change is inevitable – what remains to be seen is how long it takes.
I can only speak of the situation in Sweden, but I feel that long covid has been accepted as a post-viral condition that isn’t a psychosomatic disorder. In fact, seperate ICD codes have been implemented to ensure adequate diagnosis. However, GPs might still go their own way on this. I also feel that long covid’s “relationship” with ME has given ME more acceptance as well. A silver lining to this horrible pandemic.
One thing that I would pay close attention to if I was a scientist and that is to what extent the omicron variant will cause long covid compared to earlier variants. Only time will tell, but if it causes far fewer cases of long covid, then there might be very important clues to uncover in comparing how the body is infected/affected by the two variants and that will then also be a clue to what causes ME as a post-viral condition. If the differentiating factor between omicron and earlier variants is, hypothetically/for example, less micro-clotting because of less viral particles entering the bloodstream, then that would be something to pay closer attention to in ME as well.
It’s a great question isn’t it? I imagine they will certainly be looking at this and if the incidence is different – what an interesting and potentially helpful clue that would be.
Here’s some good news!
https://www.theguardian.com/society/2022/jan/25/doctors-find-antibody-signature-long-covid
Nice! That’s a perfect example of the kind of thing we hope – an immune hole – they will find. This is just the beginning. Thanks for sharing that! 🙂
Yes I just read that and was about to share it, interesting work. I am getting more hopeful that studies into long covid will be meaningful for us.
Since you mentioned it in the beginning of the article, what is the research finding about MS and Long COVID?
Given the clear connection between infectious mononucleosis and MS, I imagine that the interest is intense. I’ve seen two papers on this so far: one states
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8503550/
The other this:
https://pubmed.ncbi.nlm.nih.gov/34696521/
Wow, so interesting! Thank you!
there is paper on ms in large military group being preceded in large percentage of cases by epstein barr virus.
I’m someone who got long covid after the first covid wave in 2020, and was diagnosed officially with ME after a while as well. I wanted to hop on here to say that the ME patient and research community has been unbelievably kind and supportive of us long covid folks, and we are grateful beyond words — the reason I am not in much worse shape right now is because of the ME community who reached out to long covid folks and told us to unequivocally reject GET and gaslighting doctors, and to stop, rest, and pace. It is my fervent hope that all the research into post viral illnesses that has been kicked off by the long covid wave will benefit the broader ME community, who have suffered so long and so unjustly without attention or proper support. All my respect and solidarity to you.
Thanks so much, Zoh. I know that ME Action in the US and ME orgs in the UK, made a concerted effort to bat down graded exercise therapy for long COVID. Thanks so much for your thanks to the ME/CFS community. It means a lot. 🙂
I’m so grateful to the US. The NHS in the IK have never invested much funding into these issues. Having had fibromyalgia for over 9 years, after my first spinal surgery, it took me over 3 years to get to a sensible point of living with it. Then getting covid, I feel right back at square one again. There is no support, no groups, no offer of trials or anything in the U.K. it’s soul destroying. Anything that comes out of any trials oversees should be celebrated. Although, we will be waiting some years, to see any transference into the U.K. health system. Keep up the good work, I love reading your posts.
It’s been a rough road Marianne. It should be reiterated that on its own the NIH did very little for long COVID and that all this activity is the result of Congressional action.
We don’t know how the huge appropriation came about but we do know that advocates lead by Solve ME pounded the pavement (so to speak) and made clear that long COVID was a huge threat and that ME/CFS was a close cousin to it. and it worked. Congressional action potentially provides more bang for the buck than anything else and we need to keep expanding the resources for these diseases. In short, we need to keep up on with advocacy for fear some backsliding will occur.
It’ll be interesting to see how much funding the new research centers will get. That will give us a sense if the NIH has changed its stance on ME/CFS.
I think it’s changing even over there. From what I can tell the UK has at least to some extent embraced long COVID and several large studies are underway. Hopefully those studies will quickly change attitudes about ME/CFS. What we really need is added funding to ensure that ME/CFS researchers can quickly assess long COVID findings in this disease.
It will take longer than we wish for the findings to transfer down into the UK health system but with the quantity of research being done perhaps not as long as we think. Let’s hope!
I wonder how Emily Taylor, Solve ME, thinks things are going? I just re-read your blog from last February, featuring Emily.
Great question. She’s in the center of a lot of stuff – both ME/CFS and long COVID – right now. I hope to speak with her before lobby day and get caught up.
For years I have felt ME/CFS is the result of a viral infection. In high school, I had severe strep infections and afterward began my journey of years suffering the effects of ME/CFS. So frustrating for over 50 years being treated like a crazy hypochondriac. Shame it took a pandemic of this magnitude to have the medical community and government take it seriously.
I feel sad for the multitude of long-haul Covid patients who are joining our “club” and learning what it is like to live with this disease that is “all in our heads”. However, it is comforting to know the money is finally being allocated for serious research, now that so many are stepping forward after Covid with our same symptoms. I hope science will finally get to the bottom of this insidious disease and everyone of us can have the hope of beginning to live normal lives once again.
And, a HUGE THANK YOU, Cort, for your years of dedication in bringing and keeping this disease in the forefront, giving us hope and a sounding board. Your efforts are deeply appreciated!
Thanks! It’s exciting times 🙂
Any news on funding for the next trial of Cortene? I just feel like that research is so promising..
They are continuing to raise the funding. They have part of it…
Yes I agree with Sandy about viral infections leading to cfs/me. I live in Australia and in 2000 developed Ross River Fever after mosquito bites. This was proved to be the cause by blood tests. I lost two years of my life, able to do very little work in the garden or even less travel to “the outback”. Then the symptoms went away and normal life resumed. My wife was certain that my brerwing and drinking of Kombucha was a contributor, but of course no proof. It was well known at that time that a “trigger” could start it up again, and in 2016 I was the not-at-fault driver in a fatal accident and the well known symptoms started up, confirmed as cfs by my doctor, but naturally no treatment. My injuries were only minor. Symptoms still with me over six years later