

Is the RECOVER Initiative listening to 30 years of experience? Time will tell.

Does the RECOVER Initiative believe that 30 years of work on post-infectious illnesses has something to offer it? Time will tell.
The RECOVER Initiative is not just a big deal for long COVID; it’s potentially a very big deal for chronic fatigue syndrome (ME/CFS), post-treatment Lyme disease syndrome, fibromyalgia, and many other diseases that are often triggered by an infection. With so much money going into the RECOVER Initiative, it’s important for every post-infectious disease that the RECOVER Initiative get it right.
More money will be spent on the Initiative over the next couple of years than has been spent on ME/CFS in 30 years, but there’s no substitute for hard-won experience. With the ME/CFS research field having a several-decade head start on studying post-infectious diseases, it can provide something of a road map – if the Initiative will listen.
Whether it’s been listening – whether it felt the small ME/CFS field had something to offer it – was a central theme in the list of questions I sent to the RECOVER Initiative several months ago. You can decide for yourself whether Initiative is or isn’t. For me, I think it will take time to know that.
The Interview
In or Out? The ME/CFS RECOVER Cohort Question
The first question was rather long-winded, but basically, it was a request to include an ME/CFS cohort in the RECOVER Initiative in order to learn about ME/CFS and inform long COVID. For the long version, see below.

Was the RECOVER Initiative willing to include an ME/CFS cohort? For the first time, I understood why it answered the way it did.
Chronic fatigue syndrome (ME/CFS) is a small research field – receiving about $15 million/year in funding from the NIH. The RECOVER Initiative, on the other hand, received $1.15 billion from Congress to study long COVID. To all indications, ME/CFS is very similar to the most prominent form of long COVID. It will be impossible, though, for the small ME/CFS field to integrate the many findings that the RECOVER Initiative and other long-COVID projects will unearth as well as the results from the numerous treatment trials. (The ME/CFS study section at the NIH does not allow for treatment trials).
There is an effective and efficient way out of this: take advantage of the infrastructure already built and enroll a cohort of people with ME/CFS into the RECOVER Initiative. The NIH would save lots of money that it would otherwise have to spend reinventing the wheel with ME/CFS, and the million-plus really long haulers in the ME/CFS community – which has been vastly underserved by the NIH over the years – would finally benefit.
My first question is – is the RECOVER Initiative or the NIH willing to add an ME/CFS cohort, and if not, why not?)
“ME/CFS is one of several conditions with symptoms that overlap significantly with Long COVID and creating cohorts for each of those conditions will decrease the rigor and statistical significance of the results. Focusing on individuals who were infected by the same virus, albeit with different variants, at the same time, increases our chances of gaining a comprehensive understanding of the recovery process for this infection. RECOVER will have data to assess the epidemiology of those who meet criteria for ME/CFS in the cohort studies and is likely to generate data applicable to understanding ME/CFS.
Researchers can also apply for NIH funding for “ancillary studies” focused on the relationship between ME/CFS (and other overlapping conditions) and Long COVID utilizing RECOVER data.”
RECOVER’S answer was a disappointing “no”, but in truth, the light bulb finally came on for me. I realized that if I was the RECOVER Initiative, I would probably concentrate my forces and exclude chronic fatigue syndrome (ME/CFS) as well (!).
Would it really hurt this enormous Initiative to plug in a couple of hundred people with ME/CFS and perhaps post-treatment Lyme disease? I don’t think so. Would it possibly help them understand the long-term effects of post-infectious illnesses? I think it would but faced with its big and uncertain task – to solve a kind of disease that the medical profession has ignored for years and has little idea what to do with – I can understand RECOVER’s answer.
Avindra Nath spoke to the benefit of focus when he proposed that if you solve one of the mystery diseases like long COVID, ME/CFS/FM, you’ll probably solve the rest of them, and the best way to do that is to have a stringent focus.
Plus, many people with long COVID who meet the criteria for ME/CFS will, of course, inevitably be in the study and be thoroughly assessed – so the long-COVID form of ME/CFS is going to be in there. If things stand as they are now with long COVID and ME/CFS so closely linked together, they will be a nice stand-in for the rest of us.
I get the RECOVER Initiative’s side of this, but what about the NIH? Wouldn’t the NIH benefit from the economies of scale, the RECOVER infrastructure, and the opportunity to compare the really long haulers with the shorter haulers? Shouldn’t it fund and put an ME/CFS cohort through the RECOVER Initiative? Of course, It should. The RECOVER Initiative could surely handle a 500-person ME/CFS cohort. That would be huge by our standards but would be a small blip amongst the tens of thousands of long-COVID and healthy controls that are already participating in the study.
Making a Difference: Is Forty Years of Work Enough?

RECOVER has brought in some ME/CFS experts. Time will tell how much of a difference they’ll be allowed to make.
ME/CFS may be a small field, but it’s also the only field with almost 40 years of research dedicated to understanding a post-infectious illness such as long COVID (that is – the subset of long-COVID patients with similar symptoms). The effects of exertion, for instance, have likely been explored with greater depth than in any other illnesses.
Is the RECOVER Initiative being informed by the findings from the ME/CFS field and similar fields like postural orthostatic tachycardia syndrome (POTS) and post-treatment Lyme disease, and if so – how is that happening?
“Investigators and clinicians with research expertise and clinical experience with post-infection syndromes, including ME/CFS and POTS, are contributing their expertise and knowledge to the RECOVER Initiative, participating in oversight committees and working groups that determine what assessments and tests are incorporated into the protocols, and helping design ancillary protocols to complement studies in this area.
In addition, patient representatives either affected by these conditions or advocating for research on them are contributing alongside as members of these structures. Please see the link below for a current list of post-infection illness experts. The list is likely to expand as others confirm and as the Initiative continues and will be updated periodically.
That’s an interesting list that is indeed chock-full of ME/CFS experts. Eighteen of the 28 people on the NIH’s Post-Infection Illness Expert List have experience in ME/CFS and/or POTS/dysautonomia. They include Dr. Bateman, Dr. Bonilla, Leonard Jason, David Systrom, Nancy Klimas, Peter Novak, Anthony Komaroff, Galen Marshall, Janet Mullington, Benjamin Natelson, Dane Cook, Suzanne Vernon, and others.
The expert list, though, is not part of the formal RECOVER structure; i.e. it’s not one of the committees, task forces or groups that are tasked with guiding the Initiative. In fact, so far as the page indicates, it’s not tasked with anything and only shows up in the FAQ section. Other than existing as a list, it’s not clear at all what, if anything, it does.
The Commonalities with other Post Viral Syndromes Task Force (see Pathobiology Task Forces), on the other hand, is part of the RECOVER infrastructure and contains 6 well-known ME/CFS experts (David Systrom (co-chair), Leonard Jason, Suzanne Vernon, Benjamin Natelson, Hector Bonilla, Emily Taylor). Hector Bonilla. Lucinda Bateman and Janet Mullington are also members of other committees/groups. Aside from that and the Executive Committee (see below), ME/CFS experts are sparse indeed in the Initiative. That’s probably to be expected, though, given how small the ME/CFS research field is.
Interestingly, three of the five voting members (Dr. Koroshetz, Anthony Fauci, and Joesph Breen) of the Executive Committee that directs the overall strategy are actually well acquainted with ME/CFS – so ME/CFS is actually well represented at the top.
Conclusion: ME/CFS experts are abundant in the “other post-viral syndrome” group but are rarely found in the task forces, group and committees that are guiding the Initiative. Except that is in the Executive Committee where three of the five members have considerable knowledge of ME/CFS.
To Stress or Not to Stress: That is Indeed the Question
General Question – is the RECOVER Initiative going to use exercise or other stressors to help it learn about long COVID?

Exercise stressors are ubiquitous in ME/CFS research for a reason – they work! (An ME/CFS patient at Workwell).
The ME/CFS field has found that using physical or mental stressors to provoke issues that are undetected at baseline, but which clearly affect functioning, critical to understanding the disease. For instance, exercise studies are regularly used not just to understand how the cardiovascular system or the energy production systems are functioning but also to explore the effects of physical or mental exertion on immune functioning, the brain and cognition, the gut, metabolism, protein production and others.
Study after study after study has found normal results at baseline which become quite abnormal after a stressor is added. If long COVID is similar to ME/CFS, it will likely take much longer to ferret out its secrets if these stressors are not included. Is the RECOVER Initiative: A) incorporating exercise – whether physical or mental – stressors into its studies; and B) if so – how?
Also, given how helpful adding a physical or mental stressor to a study has been in understanding diseases like ME/CFS and POTS – and how much is missed when one does not do that – and how unusual it is for other fields to employ them – has the RECOVER Initiative explicitly encouraged its investigators to include them?
“RECOVER includes patient-reported questionnaires, data extraction from electronic health records and claims data, basic clinical examinations, blood draws, and radiology studies as well as provocative testing.
The RECOVER protocol also monitors participants during testing to make sure they are able to tolerate testing with stressors. Among the various tests are:
- A 6-minute walk test
- Pulmonary function tests
- A cardiopulmonary exercise test which includes a 30 second sit-to-stand test and an active standing test.
The RECOVER protocol is online: https://recovercovid.org/protocols.”
RECOVER stated there will be provocative testing but did not state how. Three tiers of testing will occur in RECOVER.
- Tier One – Everyone will go through Tier I. PEM as a symptom is followed throughout. No exercise testing is done. A 30-second “Sit to Stand” and an “Active Standing Test” is done. These tests simply appear to be assessing the ability to stand.
- Tier Two – about 30% of the participants will go through Tier II, which includes 6-minute walk test but how its being used is not clear.
- Tier Three – about 20% of the participants will go through Tier III which includes “full cardiopulmonary exercise testing”, as well as a tilt table test. (It does not state whether the test is invasive or non-invasive. I assume it’s non-invasive). (I assume that whoever answered this question got his answer wrong and the “full cardiopulmonary exercise test” is not simply a combination of a sit-to-stand and an active stand test.)
Preliminary Conclusion: It appears that exercise tests are being used to assess a person’s ability to exercise and produce energy but it’s not clear how they are being used as a provocation as the RECOVER protocol does not clarify this. (Exercise also didn’t appear to be used as a stressor in any of the extramural studies funded by RECOVER.) Given how effective these stressors are in ME/CFS, it was surprising that RECOVER wouldn’t explicitly state they’re using them in their protocols.
I had to ask about 2-day CPET tests, which show that exercise on one day depletes the ability to engage in exercise the next day in ME/CFS.
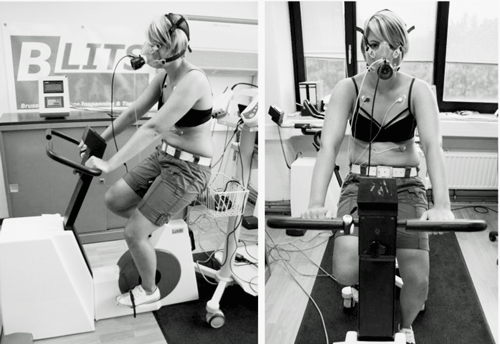
Two-day exercise tests are the only tests that have definitively shown that exercise one day reduces the amount of energy available the next. It doesn’t appear that the Initiative is going to use them.
On the subject of exercise – two-day CPET studies – one done the day after the other – have revealed an inability to reproduce energy output the next day in ME/CFS. This is apparently unheard of in the medical world. Not only has this been revealing regarding post-exertional malaise – a term created by the ME/CFS field – but they have been used many times to assist in disability claims. Will the RECOVER Initiative be using this type of test to help understand why exercise leaves people with long COVID so functionally impaired?
“The schedule for all tests, including the walking test and the cardiopulmonary exercise test are included in the RECOVER protocol Appendix: https://recovercovid.org/protocols.”
The answer again was “no” – 2-day exercise tests are not being used.
It made total sense to use exercise to understand ME/CFS given the post-exertional malaise that ME/CFS is famous for, but it still took years to get exercise installed as a standard provocation measure. Whether or not RECOVER is going to do that is unclear.
Of course, there’s much we don’t know about RECOVER. At this point, we just have access to the standard testing protocols, and there must be much, much more to the Initiative than them. My guess is that they provide the baseline data that the researchers will work off of. The studies that they produce will be a different deal. We won’t know about them and what the Initiative is actually doing until they come out.
The Gist
- More money will be spent on the RECOVER Initiative over the next couple of years than has been spent on ME/CFS in 30 years, but there’s no substitute for hard-won experience. With the ME/CFS research field having a several-decade head start on studying post-infectious diseases, it can provide something of a road map – if the Initiative will listen. Much of this interview with the RECOVER Initiative was about that question.
- When asked about that, RECOVER pointed to a list of ME/CFS experts. It was a nice, hearty list for sure, but it appeared to be just a list; i.e. the experts weren’t tasked with doing anything and weren’t part of the leadership team for RECOVER. Several ME/CFS experts are embedded in the post-infectious disease committee, however, and several members of the Executive Committee have quite a bit of experience with it. Otherwise, the participation of ME/CFS experts is quite low.
- When asked whether the Initiative is going to include exercise or cognitive stressors, RECOVER pointed to the protocol page which indicates that cardiopulmonary exercise tests and other exercise tests will be employed at some points but does not make clear if they will be used as a provocation.
- The 2-day exercise tests that show exercise one day reduces the amount of energy available the next do not appear to be being used. Once again, though, we don’t know how the studies will proceed. Will they include these tests? Time will tell.
- RECOVER expects to launch clinical trials aimed at improving immune functioning, batting down viral persistence, and enhancing autonomic nervous system functioning, cognition, sleep and exercise tolerance over the next year. 🙂
Again on the subject of exercise. The NIH is currently in, I believe the 3rd year of its $170 “Molecular Transducers of Physical Activity Consortium” (MoTrPAC) project to understand the effects of exercise on the body. Given the exercise findings thus far in long COVID and the many exercise findings in ME/CFS, is the RECOVER project being informed in any way by the MoTrPAC findings, and if so, how?
“While there is knowledge of the potential information to be shared across the programs, there have not yet been any known formal collaborations.”
I was surprised to see only 40 funded individual grant applications. Did the NIH not get many applications? Do you expect more to be funded? Will another grant opportunity open up, and if so, do you know when?
“All applications to RECOVER for funding in response to the pathobiology NOSI and ROA, and clinical trials ROA were carefully reviewed and selected based on merit in accordance with the published review criteria. Notices for open funding opportunities and Notices of Intent to Publish a Funding Opportunity will be posted and made available on the RECOVER website: https://recovercovid.org/funding.”
Conclusion: The RECOVER Initiative is going to stick firmly to its plan of having an almost entirely in-house directed effort. Koroshetz said they wanted to avoid the kind of scattershot approach that pervades medical research which tends to produce many findings but results in few conclusions. Let’s hope they have the right crew working on this and the right plan – a lot is riding on it.
The Future
Looking forward to a year from now, what do you expect to have happened in the RECOVER Initiative?
“Within the coming year, the adult cohort will complete enrollment. There will be additional information and publications emerging from the observational RECOVER protocols. RECOVER publications will be accessible from the website.
In addition, it is expected that a number of clinical trials will have been launched focusing on possible disease mechanisms and potential treatments for key symptoms/symptom clusters, such as:
-
Viral persistence and reactivation and immune dysregulation: whether the virus stays in some people’s bodies, or if other viruses are subsequently activated, or if the immune response triggers other disorders.
-
Autonomic dysfunction: Changes in the ability to regulate heart rate, body temperature, breathing, digestion, and sensation.
-
Sleep disorders: Changes to sleep patterns or ability to sleep.
-
Neurologic/Cognitive Dysfunction: Trouble thinking clearly or brain fog.
-
Exercise intolerance/fatigue: Changes in a person’s ability to be active and/or low energy level.”
It was good to see RECOVER move quickly on treatment trials and it’ll be fascinating – and tell us much about the direction of the Initiative itself – to see what treatments they plan to test. Will they be conservative or will they be willing to assess treatments that don’t have a lot of hard data (e.g. LDN) on them but might be helpful.
Will they be daring in ways the ME/CFS field has not been? Their Paxlovid trial suggests they may be willing to try more heavy-duty immune and antiviral drugs that the ME/CFS field has had trouble getting its handle on. They may be more comfortable trying biologics, for instance, than something like oxaloacetate or dextro-naltrexone.
I would hope that a drug like Mestinon, which has been around for a long time and did well in a shortie trial to improve aerobic functioning in ME/CFS, would be on their list.
It’ll be fascinating to see what they will do to improve immune functioning (IVIG, biologics) or improve autonomic functioning (hoping for Mestinon), sleep (I would bet good money we’ll see a big cognitive behavioral therapy for insomnia trial, cognitive dysfunction (stimulants, rTMS, HBOT), and finally, exercise intolerance (low dose naltrexone, Ampligen, oxaloacetate, HBOT, Mestinon).
In any case, it’s good to see the NIH will apparently shortly begin trying to address some major components of long COVID.
BIG (Little) Donation Drive Update

We’re keeping an eye on RECOVER and the other groups that make a difference in these diseases.
With as important an initiative as the RECOVER Initiative is to ME/CFS/FM and long COVID, we had to try to get some answers.
While they might not have been as forthcoming as we would want (lol), they did give us some insights into what’s going on over there – and we’re not done. We’re going to keep hawkeyed on that $1 billion-plus project.
If that’s the kind of work you want from a website, please support us in the last week of our drive. 🙂


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



Oh Cort, how disappointing. Let us hope that as the RECOVER initiative progresses, lessons from the ME field will be utilised better.
I think we really won’t know until we see the studies and what’s included in them. I have a feeling we’re getting just a very birds-eye view of the project.
While I certainly won’t do anything about it, as a decades long patient, I felt suicidal reading this. What a cruel country we live in.
I didn’t mean to leave that bleak of an impression (although I can see how I did) and I just amended the blog a bit.
I don’t think we know how the RECOVER Initiative will turn out because I think there MUST be much more to it than the protocols. Those provide the baseline – the launching point.
The studies that follow on could include anything and I assume that some will include exercise and cognitive stressors. It wsa disappointing that whoever responded to my questions didn’t state that but I would be shocked if it were otherwise.
Let’s see how this all plays out. We should know a lot more over the next year. The Initiative has a lot of promise. If they don’t take the lessons of ME/CFS on board right away they certainly will over time. They all want to succeed.
As to the decision not to include a ME/CFS cohort, I finally understand that. They’re on an uncertain quest and they don’t want to add anything to it. The NIH, however, could do add the funding for that cohort. It would make so much sense – they could fold ME/CFS right in there – it would save money – we would know how close ME/CFS and long COVID was – we could be included in treatment trials. It’s all there for the taking IMO.
I am usually the last person to agree with the NIH. But, I think Dr Nath is correct. There are some critical Biochemical, Physiological, and Molecular Biology questions that need to answered before a truly effective treatment for ME/CFS and Long Covid can be delivered. There is some extremely complicated Immunological or Biochemical breakdown that is causing these symptoms. But, isn’t that the way it is with every disease? Some dedicated Biologist will open a door, and things will begin to fall in place. There is cytological system that we either do not understand, or even realize it exists, that needs to be tackled. Long Covid is probably the best thing that happened to the ME/CFS community. Both diseases “look and walk like a duck”. NIH can no longer hide behind, “It’s a psychosomatic disease”. Throw in Gulf War Syndrome, and there are just too many patients to ignore. I think Long Covid funding will provide us with that “dedicated Biologist”. Because what we are really suggesting here, is to just keep chucking old drugs at the ME/CFS dart board. Yes, keep testing meds like Ampligen and Mestinon, but lets CURE the disease!!!!!!
Rich and Cort, I get it. But I’m in my sixties. I have Alzheimer’s on both sides of my family and I am concerned I don’t have much time left. There’s so much more I want to do and I don’t have the energy. I agree with Cort that they could include us in some small way. It would be helpful to them too
I imagine all the NIH has to do is put forth the funding to get people with ME/CFS in there…
“Yes, keep testing meds like Ampligen and Mestinon, but lets CURE the disease!!!!!!” – I like it! We obviously need more than Ampligen or Mestinon.
Yes. Testing meds to ameliorate symptoms is fine, but I don’t think they will make much difference. They won’t work for everyone and what often happens is you adapt or develop tolerance for meds. Without a cure, we will have so many more millions suffering.
The NIH has faults us for decades. I’m not surprised at this. I can’t help it but I’m livid. Thirty six years of wasted life because of them. I admit I’m furious.
I FEEL YOU!!! Too intensely to even begin dissecting their nonsense answers.
I intend much more direct social media hijinks and WELCOME any #PwME for collaborating on ideas to put a nice bright public light on their gaslighty antiscience foolishness. Email me! biocultural13@gmail.com
My life has not been in disarray since a severe viral infection in 1956. At 87 yrs. I am still struggling from day to day, but my will to survive keeps me going. My best wishes to Cort in his future endeavor.
Since 1956!!!!! God bless you Janet!!!
38 Years here, 39 in April. I am glad Fauci is retiring, He was in his job and refused to believe it was real, I too, am livid.
If only being livid would fix this. I hate to think I’ll never have a normal day again.
Maryann, they are going to be forced to propose more aggressive treatment protocols. But, they are going to be all the pharmaceuticals that you have read about here already: Ampligen, Rapamycin, Retuximab, Mestinon, LDN, Pridken’s antivirals, etc. Maybe, one or a combination will work for you. Someone has got to re-examine Retuximab. Watch the movie. Obvious long term ME/CFS patient runs a ten K, after treatment.
I am too angry to utter anything but expletives right now. Until I can muster more granular questions, f^*£ all the gaslighty jackasses obviously hamstringing things and not listening to Systrom and Klimas and the real ones.
With an unlubed screwdriver.
May they get sick themselves so maybe the millions of us peons might see relief sooner.
Wow. Phillips or straight-blade, Brittany?
Sadly, the people who excel in medical school tend to be sociopathic savants, and those who boot-lick their way up to management positions in public health institutions are almost guaranteed to be heartless bureaucrats. They will all get rich while we continue to suffer.
CFS researchers around the world put in their week or two of lab work each year, then spend months writing up the data so they can boast to their university admins that they published something. Their projects are poorly planned, almost never build on previous research, and never result in proof of anything. Ever. (“More research is needed…”) Why bother putting more effort into it? They get paid for shoddy work the same as they do for clever and important work.
How many more “reviews” do we need? How many more GET and CBT and yoga studies? There is a driving force that keeps PwCFS stuck in a dysfunctional state – find it!
The field needs one smart and motivated person – someone who goes into the lab for a week, analyses some of the zillions of tissue samples they’ve already collected in the last 40 years, discovers a single fact, then applies that new knowledge next week with an interventionist experiment to demonstrate its relevance: come to a conclusion; test it – right f’ing now. Repeat that process until the whole equation is spelled out. It’s unbelievable that we don’t have a single person in the field who can do that and consequently solve this in a month or two. It’s embarrassing.
At the rate it’s going, it will probably be another decade before any progress is made, and that will likely be an afterthought to some profit-making scheme cooked up by a private-sector charlatan.
I’m with you, Brittany. Actually I believe dr. Davis at univ of Calif had his son come down with this so, he’s interested now himself. I think his name is dr. Davis. There are and have been some great doctors like dr. Kamaroff at Harvard, Dr. Klimas, dr. Cheney now deceased, dr. Younger at u of ALABAMA who have tried or still trying but still nothing really. I did get covid which was a surprise as I hardly go out but I did and since then my CFS is definitely worse. Sincerely, javen
A year in, the Recover initiative is quite far from their enrollment goals. If they would include the estimated 800k-2.5M ME/CFS sufferers in the US (even as a separate but parallel category) that would broadly increase their analysis capabilities. There is no excuse for ignoring our continued suffering and our lack of ability to contribute to the economy (for those of us who are too sick to work).
I am thoroughly depressed by this. Dammit!
Cort, have you considered reaching out to the new Advanced Research Projects Agency for Health (ARPA-H) to see if they’re planning on allocating any resources to Long Covid, ME/CFS, or related conditions? Their whole premise is to seek out “high-risk/high-reward” projects and, unlike NIH, to focus more on research with near-term applications, so I think it would be unfortunate if these illnesses are not on their radar.
That’s a good idea as they appear to be pointed right at underserved diseases like us. In fact, reading about it, it seemed that they had diseases like us in mind.
I do think it is more important to not include more groups, as one major problem with ME is that there are so small cohorts in ME. I believe the most important thing is, for them, to be aware of the research done in ME and investigate those things studied in ME.
Not only will similarities be studied in a large cohort, they will also have enough material to find subgroups. I believe, as somewhat knowledgeable in sciences, that it is of importance to be stringent – and patient (I kno, I know …), otherwise we will continue to be dismissed on those premisses.
I think RECOVER will bring new data with new technology, and together with ME research already done, will help in furter research on subgroups of long covid or post viral illnesses as a whole. Or, that is my hope!
Thanks for asking them the hard questions Cort. I like the ARPA H idea.
I believe results from these studies with help our community and other viral onset long haulers. I hope they study other medications along with those you mention as I’ve tried most of them (prescribed by Dr Bonilla or my rheumatologist ) and they didn’t help. Thanks for keeping us posted, great work.
Thank you for asking them these questions – which were both pointed and educational (for them)!
I think it’s important that your questions are on the record. For those individuals at the NIH who read your articles, they could potentially use these to ask their own pointed questions over there.
I also really liked Matt Mazewski’s ARPA-H idea.
We all love and appreciate cort. He’s our man. It seems this last blog has outraged some of us. Steven Strauss, Francis Collins, Fauci…none of them have helped us. They have failed us. I’m angry, I’m sad, I feel defeated, I have no wonderful life anymore. No doctor knows what to do. No one knows what to do. I think the severe stress he faced over CFS killed Dr. Cheney. He did care. One thing in particular that is so difficult for me is the haywire sympathetic nervous system. Makes mr so anxious and induces panic. No doctor knows what to do or believes it. Benzos are my only help. Just ranting, I know. I almost wish we could perform our own Bastille Day but most of us are to sick and tired. At this point, I have no suggestions. I’m upset, I’m tired to the bone, I feel so bad…just like so many of us. Happy new year. What a joke. Love to all of you. Be sure to donate to cort. He needs to pay his bills so he can continue to inform us. Sincerely, Javen
RECOVER is more of an observations project than solutions project, it seems to me. And they already know that long covid = MECFS + long covid specific damages, so there probably is no need to prove that long covid includes MECFS with 2-day CPET test, etc. They obviously are hoping to learn new insights into post-viral syndrome with RECOVER, but they are more likely to just repeat what MECFS went through for the past 30 years, or, worse, be misled by covid-specific factors by not embracing all circumstances, not just COVID19, that lead to MECFS. We know how that process will pan out: in a couple of years, vast majority of long covid patients will recover and the remaining people will be reclassified as MECFS. And we’ll repeat the process all over again for COVID29 and COVID35.
We already know enough about MECFS. What we need is a solution by testing MECFS hypotheses that already exist. And that will benefit long covid patients more than RECOVER ever would.
A big weakness in the USA seems to be it’s massive size and the massive size of its medical bureaucracy.
Size can be a strength and a weakness, with regard to Research on ME/CFS the size of the USA seems to be much more of a weakness. So much inertia.
I saw it coming…they just do not like us, have never done. otherwise we would not have been neglected for decades and got so tremendous few money for research for us. If they wanted, they could have helped us long time ago with also big money, even now, seperate from long covid…
Cort, you wrote somewhere if i am not wrong no med studys allowed in ME/cfs. I have long notices that nancy klimas, jarred younger, etc did nothing on ME/cfs. but OMF wanted to enroll in future verry smaal med studys. Are they now also not allowed to do that? And nancy klimas and others is just a no and no money?
I have no intrest anymore to read what glorious things happens for long covid. even if they would find similartys with ME/cfs, there is no intrest or money for Me/cfs.
i put my hopes in germany and UK and frace and hopefully a few other countrys.
it only hurts to read over and over again what is possible for long covid and not for ME/cfs, FM, chronic lyme, you name it… being so severelly ill for decades, so many of us, they where never interested.
and yes, they may all get ME/cfs in the severest form, FM, chronic lyme, etc all together…
i wonder what the IACF congres still has to say…to smal “bad” studys. you need in a study thousends of participants.
and Nath on if long covid is researched, cured, we can cure ME/cfs, etc… I do not believe a word. that is like saying if you can cure breastcancer (and even there people still die), you can cure kidney cancer, all cancers.. and even in breastcancer, no 2 breastcancers are the same…and how many decades, tons of money did go into that?
the only big study i know of is the uk decodeME study…
i really had it with long covid…
Thanks for this write-up, Cort.
I saw that Dr. Gary Gibbons fielded the ME/CFS comparator group question at the recent NIH ACD Meeting from Prof. Barbara Wold, who recommended this same sentiment that it would be a wise idea (https://videocast.nih.gov/watch=48665 – 1:04:35 mark). We’ll see what comes about from that.
On the ARPA-H note, it sounds like inaugural director Dr. Wegrzyn has publicly said that 10-20 Program Managers could start in 2023.
If you’d like your voice to be heard & hopefully represented in the PM positions that are appointed, this form is super fast & easy to complete (https://arpa-h.gov/contact/) that I’ve shared with the community.
Message example:
“I am reaching out today to express my hope that ARPA-H will prioritize Program Managers (PM) that will look for solutions with infectious-associated chronic complex diseases such as Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS), Long COVID & POTS”
Just thought I’d share to those who want to send.
I’m looking more forward to Nath publishing his findings over Recover’s work, but when will Nath publish… no one knows. Could it be this year?
If you want to understand the politics and downward research trajectory of ME/CFS, you need to read (or re-read) Osler’s Web by Hiliary Johnson, a highly accomplished writer and researcher. Yes, it is a big, dense book and will be difficult to read if you have concentration and/or visual problems. It is too bad that it was never recorded so affected patients could listen to it. Ask someone to read it to you. (A family member would be good since this will validate what has happened to you.) I think you and your reader will get a better understanding of ME/CFS and why the powers that be never want to acknowledge what has caused it.
More and more I see “reputable” institutions say on their websites something like, “ME/CFS is a misunderstood disease” AND almost always, “PEM is the hallmark of the illness.”
Seems to me then a bulk of the $billion should go to finding out whether COVID people develop PEM, and then focus on getting at the root of PEM. (Thus, Cort, your emphasis on asking about the 2-day CPET test was right on the mark).
This seems blatantly obvious to me as the priority.
Just to share here Brian, I think some patient-led data estimates that 89% of Long COVID patients are exhibiting PEM.
Right around 56% of LC patients are meeting diagnostic criteria of ME/CFS
Reference on PEM: https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(21)00299-6/fulltext
Reference on ME/CFS estimates: https://www.mdpi.com/2035-8377/15/1/1
Also, one last minor note, that I hadn’t seen until recently. Dr. Bateman is one of the 16 Voting Members on the Clinical Trials (CT) Steering Committee for RECOVER. I’m sure you saw Cort through the site, but sharing if you hadn’t.
Thanks, Dakota, I didn’t know those numbers were that high. I don’t understand why RECOVER wouldn’t put some of those people through the 2-day CPET and study all the metabolic processes before, during, after, etc., in a more thorough way than ME/CFS researchers have been able to do, and use the results as the first bread crumb on the trail of discovery.
I’m not a scientist, so maybe I should assume they know what they are doing. But I have read the word “livid” in these posts a number of times, and (justified or not) I felt similarly after reading Cort’s article.
I missed that! Thanks for pointing that out. I will update the blog 🙂
Anyone know when Systrom’s mestinon study results will be out? It sounded promising , and as someone whose major problem is PEM, symptomatic improvement for PEM would make a big difference.
Thanks
Is that this one?
https://clinicaltrials.gov/study/NCT03674541?term=systrom%20mestinon&checkSpell=false&rank=1
I think it’s impossible to say whether a focus or a broader view would be more effective until you have the benefit of hindsight. Yes, a focused question is good, but I also think of grid logic puzzles, in which answering a seemingly distanced clue can lead to the answer for a nearer question.
What if, using CFS, you can figure out that x, y and z can’t be true, and, if using long COVID, you can figure out a, b and c aren’t true. Then, if the conditions can be united in some way, you have now proved six things about post-viral-hints-of-dysautonomia-autoimmune’s-in-there-too syndromes, instead of three things about one.