


Younger found a way to get to his data during the pandemic. His Neuroinflammation, Pain, and Fatigue Lab’s goal is to “end chronic pain and fatigue for millions of people across the world”.
The building is dark – the doors are locked – everything has been shut down. It’s early 2020 and the coronavirus pandemic has struck. A figure walks down the street, pauses – briefly peers into the entrance – and moves on. He turns left at the end of the building, stops at a locked door, digs into his pocket, takes out a key, and enters the building.
He’s the only one in the massive building. It’s Jarred Younger – working on his ME/CFS/FM data in his Neuroinflammation, Pain, and Fatigue Laboratory.
Brain on Fire? The Big NIH-Funded Brain Scan Study
An earlier pilot study of Younger’s revolutionary new thermography technique to assess neuroinflammation using a kind of heat mapping technique had been successful. Now Younger was in the third year of a major five-year NIH grant to determine – yes or no – whether the thermography technique was effective. Along the way, he would assess neuroinflammation in 90 ME/CFS women and 30 healthy controls. The study had all the hallmarks of a big NIH grant – it was huge, complex, and novel. It had three parts:
- Measure neuroinflammation across the brain using 4,000 assessments of gray and white matter, and cerebrospinal fluid.
- Use a good day / bad day approach in 20 women to see if the neuroinflammatory markers picked up in the brain scan were linked to symptom severity.
- Assess the efficacy of the new thermography approach using a PET scan that picked up activated microglia.
It was another example of an ME/CFS researcher pushing the medical research field further. The study could potentially validate how much and where neuroinflammation was present in ME/CFS – thus validating the disease itself and throwing it into the class of major neurological disorders.
So here he was in year 3 of the study. I asked him how it was going. He said 50 ME/CFS and 30 healthy controls had gone through the study – enough to start the interim analyses.
I remarked how exciting (terrifying?) it must be to work on something for years and have it all come down to a single statistic. Younger said that was his favorite part, though. As a scientist, that’s where the juice lies for him. It was all about the discovery. Did the technique reveal the truth?
A positive result could change the course of brain imaging. Right now, researchers use radioligands that attach to receptors on active microglia to assess neuroinflammation. The approach is controversial because the ligands can attach or dock to other receptors as well. Younger suspected that Watanabe’s 2014 ME/CFS study was correct – neuroinflammation is present in the brains of people with ME/CFS, but the ligand he had available to him (PK11195) – was messy – it could dock to a bunch of stuff.
The next-generation ligands had problems as well, and now third-generation ligands are being developed (but are not available for human research yet). We still lack access to radioligands that can distinguish between activated microglia and astrocytes. That’s an important distinction as activated microglial cells could be kicking off long-term inflammation in the astrocytes.
Determining how to treat what’s going on will require knowing where the neuroinflammation, if it’s present, is coming from. Younger is working with a group that invented one of these new markers and was hoping to test it this year with some ME/CFS and FM patients.
Because Younger’s new thermography technique is considerably cheaper and side-effect free, it had the potential to revolutionize how brain scans were done. Not only would the technique be available to more people, but it could be used to assess the effectiveness of treatments on the brain.
Younger is clearly on the cutting edge of neuroscience – in fact, that’s where he said he likes to be. I asked him about the thermography technique – are other groups picking it up? He said seizure and schizophrenia groups were picking up it at UAB (the University of Alabama at Birmingham). So far, it was working really well.
“Going Nuclear?” The Brain Invasion Study
Talk about a fascinating and potentially far-reaching study. Health Rising reported on the ME Research UK funding leukocyte infiltration study back in 2018.
Only now is the study about to actually start testing patients. The study is so novel that it took years to get through the regulatory hurdles posed by it. Younger obviously thrives on developing cutting-edge technologies, but it makes it more difficult at times as well.
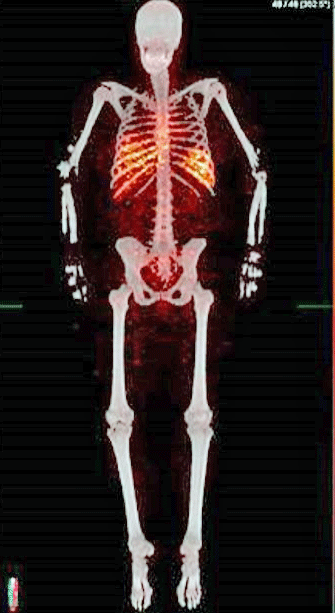
The first human leukocyte tracing image done. Note how the white blood cells (red) are concentrated in the middle of the body around the lungs and the heart, where most of the blood is.
Everything is new. First, you take out the white blood cells (leukocytes), then you separate them, put a radiotracer inside them, put them back in, and this is the tricky part – have them act as if nothing happened and have them go on about their business as usual.
The question at hand is whether white blood cells are making their way through the blood-brain barrier into the brains of ME/CFS patients. The brain has its own unique immune cells called microglial cells. White blood cells – chiefly T and B-cells from the body – on the other hand, are only pulled into the brain as a last resort. These are amongst the most powerful cells in the immune system but once they’re in the brain, they don’t know friend from foe. Like bulls in a china shop, they go on a rampage.
Avindra Nath – who has also wondered whether these cells have gotten into the brains of ME/CFS and long-COVID patients, has said they’re like unwanted guests who never leave.
Younger been working for years for this moment. He now knows that the technique works – he can show the labeled white blood cells moving across the body and into the brain, and monitor them for almost a week (a new record) as they move across the body. Mostly they go to the muscles, where they hang out. He knows they’re safely cooped up in the brain’s blood vessels in healthy people’s brains. The next step is monitoring them in the brains of people with ME/CFS, multiple sclerosis, and other diseases.
Finding them in ME/CFS patients’ brains would be significant indeed – what Younger called a “severe pathological inflammation”. It would mean that the brain has either gone nuclear and has brought in dirty weapons to resolve something serious or that an important communication pathway has been upended and the brain is calling in strikes on itself for no good reason. It’s also possible that the blood-brain barrier has been seriously damaged in some way.
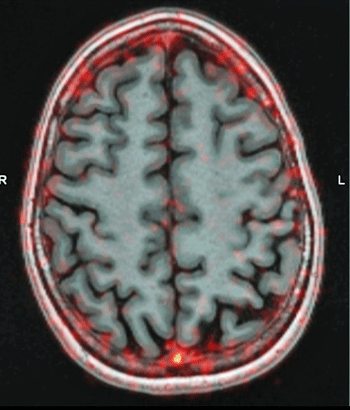
Tracing white blood cells in the brain of a healthy person. Notice how the white blood cells (red) are concentrated in the blood vessels in the brain but are not entering it. Younger should know pretty soon if ME/CFS or MS patients’ brains look different.
If Younger does find immune cell penetration he’ll do a gadolinium scan to see if the blood-brain barrier has become leaky. There are no treatments for immune cells in the brain but groups are working on that and if this technique pans out they’ll have a way to monitor it.
Noting that a leaky gut is present, and a leaky blood-brain barrier may be present, I asked if the same thing could be causing leaks in these different areas. Younger said it was possible that a similar process was occurring.
The Fibromyalgia Psilocybin Trial
Younger mentioned as an aside that the Epilepsy Division Director, Jerzy Szaflarski MD, Ph.D. is finding that cannabis works really well with epilepsy. (The UAB has one of the most advanced epilepsy research centers in the country and Alabama actually passed a law allowing cannabis to be used in the treatment of pediatric epilepsy.)
The last time I talked to Younger, he shied away from cannabis research because it was just too hard and time-consuming given all the roadblocks at the federal level, but he said, “Everything is getting easier”, and that they were a few months away from doing a psilocybin trial in fibromyalgia (!). He’d heard from enough people that it helped that he was going to give it a go. The approvals were all in – it was going to happen.
It’s going to be a small, proof-of-concept, pilot trial – just 10 people. Noting that some anecdotal evidence suggests that a full dose of psilocybin might be able to cure FM pain for several months, the study was going to involve a full dose, not a microdose. A brain scan the day before and after the drug is going to be part of the study and is going make up a Ph.D. student dissertation.

Younger expects to begin a small fibromyalgia psilocybin trial in a few months. Brain scans will be a part of it.
Clinical psychologists will meet with the participants before the trial for a couple of weeks. Someone will be in a room made up to feel calming and comfortable in the hospital the entire time. (I asked if Jimi Hendrix posters were going to be part of the décor but no). Each session (trip?) will last about six hours. The main goal on the psychologists’ part is to keep the participants calm and anxiety free.
Younger said he’d been thinking about this trial for quite a while. This arena has finally been loosening up as researchers show positive benefits. DMA, ecstasy, and LSD are all becoming available for testing. Younger celebrated the fact that if you have good scientists and good protocols, these agents are becoming available to be tested in medical trials.
Psilocybin and LSD are 5HT2A agonists (activators) that turn on that specific receptor and the serotonergic system. Exactly what it’s doing is not clear yet. Genetic evidence suggests, though, that abnormalities in this pathway exist in FM. Michigan and Daniel Clauw are starting one and there’s another one as well.
The Patient-Led Research Fund – ME/CFS and Long-COVID LDN Grant and the Next LDN? (Dextro-naltrexone)
This is going to be a decentralized trial. Interestingly, the money provided was in crypto and UAB didn’t know yet how to manage that. Younger, again, was pulling them in a new direction – albeit one he hadn’t anticipated.
I had to ask about dextro-naltrexone – a potentially more powerful form of LDN. Younger, with his Stanford studies, had basically birthed the LDN fibromyalgia movement. And I hadn’t heard of dextro-naltrexone until I heard of it from him. It’s never been used on a human before but keeps all the good parts of LDN and gets rid of the problematic parts that can cause side effects. That could mean being able to take higher doses and having much better effects.
Younger had hunted down a source, and applied for NIH funding, but was rejected. He needed about $1.2 million to get the dextro-naltrexone study going. Younger said it was on the top of his list and noted how frustrating it was that it hadn’t been tested. Talk about an opportunity, though, to potentially make a difference for a lot of people with a better and more effective form of LDN. Against that possibility, the $1.2 million seemed small, indeed. (Any donors out there?)
The Botanicals Study Wins Out
Younger has basically been beating the bushes in an attempt to flush out things that can help right now with neuroinflammation. In a randomized, crossover, quadruple masked trial, he tested 9 botanicals (Boswellia serrata, Curcumin, Epimedium, Fisetin, luteolin, nettle, pycnogenol, Reishi mushroom, resveratroil) over a variety of doses in Gulf War Illness.
The Gist
- Jarred Younger – runs the Neuroinflammation, Pain, and Fatigue Laboratory at the University of Alabama at Birmingham. Its goal is to “end chronic pain and fatigue for millions of people across the world”.
- I met with him at his office. He’s in the midst of a major NIH-funded grant to measure neuroinflammation across the brain in people with ME/CFS, to determine if markers of neuroinflammation are associated with symptoms in ME/CFS, and to determine if his new thermography approach to assessing neuroinflammation works.
- Because Younger’s new thermography technique is considerably cheaper and side-effect free, it has the potential to revolutionize how brain scans were done.
- Seventy participants have been through the study and Younger will soon begin an interim analysis to determine if neuroinflammation was found.
- Younger has also developed a technique to assess if white blood cells (WBCs) from the body have entered the brain. Because the brain already contains its specialized immune cells, and WBCs don’t know friend from foe, they’re only called into the brain under the direst circumstances.
- It’s taken years to develop this new technology and get it past regulatory hurdles, but Younger will soon start testing people with ME/CFS to see if their brains have “gone nuclear” and brought in dirty weapons, so to speak, to combat something in the brain.
- If Younger finds WBCs in ME/CFS patients’ brains, he’ll begin assessing the blood-brain barrier to see if it’s developed leaks that could also explain a WBC invasion.
- Reporting that it’s become considerably easier recently to test these kinds of drugs, Younger will shortly begin a small full-dose psilocybin study to see if the drug relieves pain in fibromyalgia. He’s also beginning a low-dose naltrexone (LDN) study in long COVID and ME/CFS shortly. He has yet to get funding to study LDN’s probably more effective cousin – dextronaltrexone.
- Younger’s Gulf War Illness botanicals study found that these were helpful: curcumin, stinging nettle, and resveratrol.
- Younger’s findings suggest that the immune system is kicking in too late in fibromyalgia, and that when it does kick in, it does so with a vengeance – producing symptoms. In this scenario, people with FM and ME/CFS never get a terrible cold but are always getting whipsawed back and forth by the immune system.
- Younger’s been great at developing new technologies and getting funding but has his own supply-chain issue to deal with – post-docs. The Ph.D.’s that researchers use to write up their studies virtually disappeared for Younger and his colleagues during the pandemic. The result – about 20 papers are in the queue, waiting to be written up.
- Seven years after Younger created his Neuroinflammation, Pain and Fatigue Lab at the University of Birmingham, everything is telling him his initial hypothesis – that neuroinflammation is playing a major role in ME/CFS, fibromyalgia, and now long COVID – is correct.
Three Microglial Inhibitors That Worked
- Curcumin – Pure Encapsulations: low dose – 500 mg; high dose – 1,000 mg; – reduced pain and fatigue; note – it adds some load to the liver.
- Stinging Nettle – Nature’s Way: low dose – 400 mg; high dose – 800 mg. (Might stop a virus from replicating.)
- Resveratrol – Pure Encapsulations: low dose – 200 mg; high dose – 600 mg). WebMD reports resveratrol may be able to open the blood vessels, reduce clotting, decrease pain and help maintain proper blood sugar levels.
Pycnogenol was a possibility – it did well in the tests – but did not show a dose-response effect.
Why the Type of Pathogen Doesn’t Matter in ME/CFS (or … Why the findings in Long COVID will probably apply to ME/CFS)
Younger thinks of long COVID as a type of ME/CFS – the only thing that’s really different about it is that we know which pathogen triggered it. If Younger is right about chronic microglial activation producing the neuroinflammation (e.g. sickness behavior) that’s driving ME/CFS, the specific pathogen that triggered the microglial activation doesn’t matter. What matters is that the microglial cells (the immune cells of the brain) have become chronically activated.
The microglial cells (the immune cells of the brain) are dotted with toll-like receptors that respond to different pathogens (viruses, bacteria, mold) that turn the microglial cells on. The microglial cells have off switches – in fact, as they go into fight mode, those switches get amplified – but Younger has evidence indicating that the off switches are not working in fibromyalgia.
Younger temporarily ramped up the microglial response in FM with a bacterial toxin. As the body dealt with the toxin, a microglial inhibition response involving fractalkine should have turned the microglia off once the threat had passed. In FM, though, the microglial inhibition response (fractalkine) never kicked in, leaving the microglia activated and producing the pain hypersensitivity and flu-like symptoms associated with FM.
Younger stated that the data suggests some immune suppression in FM is giving the pathogen an extra in. The immune system does eventually kick in, but instead of dealing judiciously with the pathogen, it overreacts – causing symptoms. This happens again and again and again. You never develop a huge infection, but you’re always getting whipsawed by the immune system – and that’s potentially causing the symptoms in ME/CFS and similar diseases. That paper is under review right now.
The Great Survey
Health Rising will have more on this later, but Younger and his Neuroinflammation, Pain, and Fatigue Laboratory have rolled out a new chronic disease survey – and it’s doozy. It’s the most comprehensive illness survey I’ve ever taken (and I’ve taken many).
It needs to be comprehensive because Younger’s group will be applying artificial intelligence and machine-learning techniques to it to better understand ME/CFS, fibromyalgia, and similar disorders. (Thankfully, it has a save and continue capability.) They’re aiming for 5,000 completed surveys.
A Dearth of Post-Docs!
Younger’s obviously done well at UAB. (Too bad for you, Stanford). He’s developed two new technologies and has been an ace at getting grants – but he has a problem. He’s sitting on a ton of data! He said he has over 20 papers waiting to be written, but one man can only do so much.
Younger’s limiting factor right now is a dearth of post-doctoral students (Ph.D.) that researchers use to write up their findings.
His big NIH-funded Daily Immune Monitoring Study, for instance, and its tens of thousands of data points are done and are waiting to be analyzed and written up. Valuable data on leptin and fractalkine – two immune factors not often discussed in these diseases but which could make a difference – are sitting there – not making much of a difference right now.
Something happened during the coronavirus pandemic that isn’t clear. Either the post-docs went to industry, or out of academia, but they are mostly gone – and not just for him but for his peers as well. Instead of rolling in post-docs, he’s having trouble finding them right now.
Neuroinflammation Man?
One of Health Rising’s first pieces on Younger called him “The Neuroinflammation Man”. Younger’s been at his Neuroinflammation, Pain, and Fatigue UAB Laboratory now for 7 years. I asked him how he feels about neuroinflammation now after all this time. Was he as confident in his hypothesis as before? He was. So far, everything he’s seen supports his hypothesis that neuroinflammation is a big player in ME/CFS and fibromyalgia.
Check out the latest from Jarred Younger – a brain stimulation device he thinks will work
BIG (Little) Drive Update

Health Rising is in the final weeks of its donation drive. If you enjoy interviews like this please support us 🙂
Thanks to the over 460 people who are making Health Rising’s end-of-the-year (beginning of next year) drive a success!
Jarred Younger is another researcher Health Rising makes every attempt to keep up with. This time that included taking a wide detour during a cross-country trip to Cape Cod to visit him. If these kinds of interviews spark your creative juices and leave you more hopeful for the future please support us.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


What about thymoquinone.
That’s a massive anti inflammatory.
Stopped my pots and PTSD feelings in it’s tracks. But it’s in black seed oil. The oil itself has too much of the wrong omegas ratio and was giving me erection problems eventually…but it had stopped my pots and fear response. I just wasn’t going to ruin my cardio for it tho. Pufas I think they call them.
Black cumin seed and thymoquinone have about 60 papers published in the last two years, according to PubMed. It’s an interesting supplement with many effects.
I wouldn’t worry about PUFA ratios, though, as the dosage from seed/oil/extract would likely be small compared to overall dietary intake.
Sorry to hear about your penis, though. Perhaps the problem is rooted elsewhere.
Nice pun there at the end.
This is a fantastic video showing his results: Dr. Jarred Younger Presents: How We Can See ME/CFS Inflammation In the Brain
https://www.youtube.com/watch?v=DU0UgWGyi0A&list=WL&index=9
It’s great to see an interview with Jarred Younger on his current research!
I always keep in mind his work on neuroinflammation with hope it will lead to treatment and an understanding of the pathophysiology of these diseases. He’s a real pioneer and I hope he gets all the resources he needs to continue his work.
i wonder if the things that worked for GWI would also work for ME/cfs or FM or so… maybe i am going to try the botanicals…
Re- curcumin – I have mentioned several times before over the last 7-8 years that I have achieved some very good results with curcumin, especially for PEM, so this does not surprise me.
Re microglia and the BBB – Mark Swain from Calgary did interesting non-ME/CFS research more than 10 years ago that showed that peripheral inflammation can initiate the infiltration of monocytes into the brain. Peripheral inflammation triggers microglia to produce CCL2, which attracts the monocytes. When CCL2 was blocked the monocytes did not enter the brain despite the ongoing peripheral inflammation. Doing so prevented sickness behaviours including fatigue.
At the time (around 2010) I corresponded with Swain as I thought this research had possible significance for ME/CFS, however there seemed little interest from his side.
Despite this, I have long maintained that it is a valid theory and have found that supplements that reduce CCL2 help with my symptoms.
Matthias, I have been paying attention and thank you for posting that this has been beneficial to you, I so appreciate people leaving good or neg feedback on the things they try.
I am also trying botanicals and was really pleased to see in summer last year that Jarred Younger intended to run a trial using botanicals. It’s great to hear that Curcumin and Resveratrol showed results for GWV and I also hope the same would apply for ME/CFS. Thanks Cort for giving us these results.
Here is a link to the UK Covid nutritional trial supplement called Phyto V, they detail the contents and the anti-inflamatory , anti-viral benefits of the product. I have only been taking these for 8 months and they are lower amounts than Jarred Younger has trialed. Not banging on about them anymore but together with my other protocols (Grateful for Dr Myhill website and book for these) I have seen improvement in my dizziness, coordination and tingling sensations in hands and feet.
Just hoping that I am getting something right and think only further time will tell. I certainly think curcumin is worth a try.
https://www.keep-healthy.com/polyphenols/
Hi Matthias, can you describe how your PEM changed with curcumin? Mine doesn’t respond to much, so maybe curcumin would help
hi Matthias, may i ask how much curcumin you take and how divided over the day if so? Or do you only take it in pem? is it with black pepper? i have often much trouble with my stomach.
i am way to ill to research and read what helps with CCL2, even do not know what it is. wich supplements and how much do you take for that?
thaks for sharing!!! for me worth a try!!!
It’s ridiculously complicated.
“Two of the molecular families closely associated with mediating communication between the brain and immune system are cytokines and the kynurenine metabolites of tryptophan. Both groups regulate neuron and glial activity in the central nervous system (CNS) and leukocyte function in the immune system, although neither group alone completely explains neuroimmune function, disease occurrence or severity. This essay suggests that the two families perform complementary functions generating an integrated network.”
An integrated cytokine and kynurenine network as the basis of neuroimmune communication – 2022
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9729788/
Hi Christyne, basically with curcumin I can do light weights ‘mini-workouts’ with much less of the muscular pain and stiffness that I used to get as key PEM symptoms. The PEM fatigue is also significantly less.
Peripheral inflammation causing neuroinflammation nicely explains PEM that typically starts 24 hours after and last 3 days. Inflammation spikes up the day after exercise and it takes full 3 days for lymphocytes to subside. It’s just that MECFS patients are so sensitive that even minute amount of peripheral inflammation from walking a short distance would be enough to trigger PEM. Likewise the low-grade inflammation caused by flu shot or alcohol.
As for curcumin, I tried a supplement some 6 years ago to no effect. (I think it was the same brand used in one of the studies that showed 15% improvement in a trial.) You may need a pure form of it though, not a supplement, to actually get to the brain and make a difference. Dopamine supposed to be another down-regulator of activated microglial cells, but dopamine supplement didn’t work either. But novelty and positive stress sure did the trick for me.
TK – I used Longvida curcumin.
Yes novelty and positive stress really helps me, must be the dopamine stimulation.
Hello, what did you take to inhibit CCL2?
Despite the fact that she believes that different things are happening in GWI and ME/CFS Nancy Klimas modeling studies suggest that the same drugs will work in it. They both work on neuroinflammation and the HPA axis – both of which disturbed in both diseases. Two different roads that lead to Rome, so to speak. I’m going to give them a try at the higher doses and with the brands Younger used.
hi Cort, verry brainfoged and ill. and it is not clear to me. younger speaks of nittle thistle, curcumin, etc. you write now about nancy klimas. (sorry brain). wich ones are you going to give a try if i may ask and at wich dose and how divided during the day? and why way higher. i thought nancy klimas had total other combo meds. i am just to diffused. sorry for asking!
ps and wich brands please?
sorry cort for my question. it is for the verry severelly ill ones often impossible to read your blog , even the summary. and in the summarry stood nothing about what you where going to take, the brands, wich botanicalls jarred younger had selected, etc I managed to read a piece until the brands of botanicalls, etc. now i understand. if possible, please put it next time also in the summary for the severelly ill ones. thank you for your blog. i hope it helps you andthat you let the world know. good lck!!!
Where’s the result of her work? There’s been an awful lot of talk from her for many years but little to show for it.
Konijn, Cort was referring to the modeling that Nancy has done, not drug trials. She believes GWS and CFS are different but that they will respond to the same treatments. In this case, Cort is going to try the 3 supplements in Younger’s trial. These 3 in the article with doses and brand names. Hope that helps
Re- the virus doesn’t matter – exactly what I have been saying for many years!!! All sorts of viruses and other stressors can initiate ME/CFS which is why I get infuriated by the studies that keep popping up looking at this potential viral cause or that. Total waste of research energy and money! And on a related note, so is the search for an antiviral ‘cure’. Viruses may be a common trigger but they do not perpetuate ME/CFS!!!!
Meant to reply to you but pressed the wrong button – please find my reply below.
Which raises the question of why there was a sharp increase in cases of ME beginning in the 1980s. I don’t buy the hypothesis that it was under diagnosed as my symptoms were incredibly dramatic when it started for me. They weren’t just vague feelings of fatigue. I’m agnostic as to whether there is a specific pathogen that causes the disease or as you’ve written just trigger pathogens that start a process that is self perpetuating.
As viruses mutate regularly, if you don’t remember anything in particular it was probably a common cold or ‘flu that was circulating at the time. As we have learned from Covid, even an asymptomatic infection can lead to chronic illness.
I absolutely agree about all sorts of viruses and other stressors initiating ME/CFS. About viruses, I don’t expect that acute (lytic, i.e. actively replicating) viruses are a major contributor to the ongoing part ME/CFS. (In my opinion, they may contribute a little to pathology in some cases simply because the whole system is off-balance, so there maybe a flare-up of infection now and then; also I’ve seen a patient report that antivirals helped a bit but were not curative. But as far as I remember, typically, many patients have no signs of active infection).
But: Lately, fascinating findings have appeared that show how viruses can sabotage the immune system and mitochondria on the cell level while not even replicating throughout the body. I am thinking of Bhupesh Prusty’s work on HHV6, but I think he said the same may apply to other viruses like EBV. It now seems to me that besides latent (dormant?) and lytic (actively replicating in large numbers) states, there is a third state which is where the virus is active/interferes with the immune system without significant replication, e.g. by sending off specific signalling molecules (microRNAs) that influence other body cells. (I am not sure what this is called but probably goes under “reactivation”).
So I don’t think it’s been ruled out that viruses could have a major role in the ongoing illness, but in more devious or clandestine way than “just” active infection, and maybe confined to specific tissues (see Prusty’s latest paper on tissue-specific HHV6 reactivation in ME/CFS brain autopsies discussing this possibility https://www.frontiersin.org/articles/10.3389/fmolb.2022.1044964/full ).
I think Prusty is working on figuring out how HHV viruses may continuously be involved in ME/CFS on the cell level and, once that mechanism has been understood, new drug targets that target the ongoing hidden activity of the virus: See this article about his previous discovery of microRNA signalling by HHV https://www.eurekalert.org/news-releases/951432 which explains that for example there may be a way to neutralize the signalling microRNAs sent out by the virus.
Thanks JR, very good points. I guess that is certainly all possible so I should remain open to it. But I still see it more likely that an initial stressor (often, but not always a virus) does ‘something’ that permanently resets the system. I personally favour an autoimmune and/or neuroimmune condition, that is not in any way affected by any kind of ongoing viral involvement. But hey, time will tell, and I don’t care as long as someone properly gets to the bottom of this illness and we can find meaningful treatments if not a cure!!!!
Yes, crossing my fingers for this!!!
My bet is currently on the complex systemic models which involve central immune system sensitisation/neuroinflammation in the brain, and what I think a guy called Steve Chalmers on Twitter called “cascade failure” in downstream/peripheral systems. The “beauty” of these models is that they are able to incorporate various triggers and various perpetuating factors, as they may all influence one central process. In such a model, you could treat a central process, but you might also treat an ongoing process such as autoimmunity that may perpetuate the central dysregulation? I am thinking of Herbert Renz Polster’s microglia review paper, and if I understood this correctly, other researchers (Amy Proal? I think; a team in Australia, etc.) have been going in a similar direction. In these models, I am thinking of what you call a system reset as a “system tipping point”, where the system tips over from a state of balance into a disregulated different state of balance. I also bet that dysregulation in ME/CFS involves a strong epigenetic component. Though this model makes me feel a bit frustrated due to complexity, it also gives hope because dysregulation does not necessarily mean permanent organic damage.
How wonderful it would be if one single pathway or central mechanism would be discovered that, if treated, could put the whole system back into balance!! That mechanism in my opinion must be able to explain PEM.
Grüße vom Main 🙂
I totally agree with what you wrote, Matthias – an initial stressor does something that permanently resets the system. It does not have to be a virus. In my case it was a severe, long-lasting intestinal candida infection.
I feel very hopeful with Jarred Youngers work in this area. I frequently feel as if my brain is on fire and that if I could turn off my brain then the rest of my body would calm down. I particularly like that he is hopeful about botanicals as I am not good with medication. LDN had a very frightening effect on me as have other medications. Fingers crossed that he gets some good results.
Hi Bobby,
My brain felt like it was smouldering too. I’ve managed to calm it down a good bit. I hope you find something that helps.
Hi Tracey Ann (Burgess),
What helped you to calm it down. Was it something botanical, meditation or a combination of things that helped.
These two, Michael VanElzakker PhD and Amy Proal PhD are well worth watching. I basically googled anti-inflammatory diet and tried to incorporate as many things as I’m able to (I have extensive food intolerances) and I try and leave out the inflammatory foods. I sprinkle turmeric and ginger on my food, which is drenched in extra virgin olive oil. I als try and work on calming my fight/flight/freeze and enhancing the rest, digest, relax and heal mode. I’m very much DIY. I’d love to try low dose naltrexone (LDN) and maybe Abilify.
https://youtu.be/UY2vwDbLlno
It appears as if the brain temperature measurements are still an evolving field. This study ((https://academic.oup.com/brain/advance-article/doi/10.1093/brain/awab466/6604351 – lay summary her: https://www.sci.news/othersciences/physiology/human-brain-temperature-10898.html )) did not find a correlation between brain temperature and brain pathology but found very variable brain temperatures even in healthy people (brain temperature ranged from 36.1 to 40.9°C ! ). They concluded that absolute brain temperature could not distinguish brain physiology from pathophysiology.
If it turned out to be true that brain temperatures can indeed vary by nearly 5 degrees Celcius even between healthy people then this technique would possibly reach some limits when comparing low numbers of patients with healthy controls. Yet, thermometry could be a valuable technique to track changes in individual patients (indeed, there is a paper from Jarred Younger´s lab that measurements are quite reproducible over time: https://www.frontiersin.org/articles/10.3389/fnhum.2020.598435/full ). Anyways, this seems to be a technique with some open questions.
“TBr was measured via a thermistor, inserted into the brain parenchyma via a dedicated bolt placed via a burr hole (Integra Neurosciences). The bolt was placed so that the thermistor was inserted into frontal white matter at a tissue depth of around 18 mm below the dura…”
I’m not sure how they inferred a 3-D map (or 4-D, incorporating time) with a single thermistor, but I’m not going to volunteer my brain for the follow-up study.
In the Younger temperature-reproducibility study, each patient was measured only twice, 12 weeks apart, and it’s not clear if they were measured during similar time-of-day; I don’t know if the results reflect diurnal consistency (if sessions were at similar hour) or not.
Regardless, thanks for the links. This research is indeed in its infancy.
Can he objectively diagnose neuroinflammation in ME/CFS patients or not? Not at this moment, right? It’s just a hypothesis, nothing more, nothing less. At present, this theory has been rejected.
”In contrast to what was previously reported for CFS, we found no significant difference in BPND of [11C]-PK11195 when comparing patients with CFS or QFS with healthy neighborhood controls. In this small series, we were unable to find signs of neuroinflammation in patients with CFS and QFS.”
https://pubmed.ncbi.nlm.nih.gov/34815320/
It’s an evolving hypothesis. Of course, there are now 268 different evolving hypotheses 😉 And no one wants to openly reject anyone else’s hypothesis. But other groups claim to have found evidence of neuroinflammation, circa 2021.
“ME/CFS patients with varying severity of symptoms were compared with healthy controls to identify the brain regions where neuroinflammation was occurring largely in the limbic system (cingulate cortex, hippocampus, amygdala, and thalamus) a region between the brainstem and the upper regions of the brain. The nearby midbrain and pons region of the brainstem were also potentially affected. Increased binding of the radioactive tracer was ~50–200% higher than in the healthy controls, and an important part of the outcome was a correlation between the severity of the ME/CFS symptoms and the extent of activation of the microglia. While there is yet no published replication of these results the authors report in a personal communication they have successfully replicated their findings with new ligands and they have completed an expanded study that suggested neuroinflammation was occurring at some degree in the hypothalamus (28). ”
Molecular Mechanisms of Neuroinflammation in ME/CFS and Long COVID to Sustain Disease and Promote Relapses
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9174654/
An excellent paper. I recommend reading the Mark Swain paper from around 2008 on peripheral inflammation and central fatigue, and the role of CCL2. As I say above at the time I thought it could be very relevant to ME/CFS even though the research wasn’t about ME/CFS.
I also remember the infamous (in CFS patient circles) Andrew Lloyd saying many years ago that ME/CFS was all in the brain/ CNS. Lots of patients didn’t like him because he didn’t confirm the hopes of many patients that there had to be a virus perpetuating their illness.
This is a weird mindset that still exists a lot to this day – witness the ongoing belief (a very weird one, but I kind of get it given the desperate hope for ‘the cure’) and hope in ampligen.
I don’t think we can say yea or nea – we have conflicting results with more positive than negative ones. Younger’s big NIH-funded study, though, should clear that question up, I would hope.
Is the gulf war botanicals study published yet? I’d like to see the specific improvements for each one. One of the things they tested for was mood improvements and I’m struggling with depression. I guess I’ll Google curcumin, resveratrol and stinging nettle for mood. On another topic, I really hope neurologists who treat MS take up ME once Jarred’s results come in. The two diseases run together in families (like mine) and advances in either could help the other.
I couldn’t find one. He did recently publish a study showing that inflammation appears to be driving GWI, though.
https://pubmed.ncbi.nlm.nih.gov/35902364/
The preliminary results are here : https://pubmed.ncbi.nlm.nih.gov/33802272/
Here:
https://pubmed.ncbi.nlm.nih.gov/33915962/
And here:
https://pubmed.ncbi.nlm.nih.gov/33802381/
What’s fascinating is the very similar results. I also noted that reishi mushroom made people worse. My son was very sensitive to any mushrooms during his CFS. I used these findings when treating my son. He found Curcumin very effective and we used it towards the end of his Chronic phase, though he was on a lower dose than the Younger recommendation in this article.
Hi Christyne,
I have found a very healthy anti-inflammatory diet has cured my depression and anxiety and helped my ME symptoms slightly too and improved my sleep. Even though my energy limits haven’t changed much I feel more normal, more like a healthy person should feel, which is a really welcome feeling.
Scientists believe chronic inflammation can cause depression, they’ve known this for at least 15 years if I recall correctly but this knowledge hasn’t reached the public yet.
It is believed antidepressants in the future will work by reducing inflammation.
I hope this is helpful to you
I’m very grateful to Jarred Younger PhD because when I watched this 20 min YouTube video, from the Open Medicine Foundation (OMF) Symposium from around four years ago, I learnt so much.
I’d already been following many functional medicine doctors online, like Dr Mark Hyman, Dr Dale Bredesen, Dr Datis Kharrazian etc., and was particularly interested in their ideas on people with brain issues, like dementia. Back then, I had no idea who or what the OMF were but they seemed to have some fascinating ideas.
As Jarred Younger talked about microglia and brain inflammation, I thought that sounds just like me. (My doctor had chuckled & shook their head in amusement, when I mentioned it to them) No help there then.
I embarked on a DIY attempt to lower the inflammation in my body & hopefully my brain through diet – trying to avoid the food that irritated my brain & eat what may help to calm it. Years later, I’m still focused on this & am doing fairly well. I describe myself as having Irritable Brain Syndrome (IBS).
Jarred Younger PhD has done more recent videos but this one’s shorter 🙂
https://youtu.be/8XrdSlpUQTE
Just wanted to say that the survey has been waaaaaaay too long and I have been working on it for several hours and I thought I had finished and then, even more questions popped up! Some of the questions don’t have appropriate choices of answers for my circumstances, especially when one has multiple conditions with overlapping symptoms. Yet I muddle through…not yet done. Exhausting!
I’m only doing it to help science. Anybody else taking it? Did you complete it?
I could not get though it.
I’m doing it bit by bit – it’ll take me a couple of days. I’m doing it for the science like you are. We’re going to have a blog and I’ll try to find out why it needs to be so long.
Working on it. Even with breaks it’s heavy going and I dont think some of the questions allow specific enough answers, especially when you are not in constant pain but have intermittent problems.
I could not get through the survey. Too many specific categories that are impossible to answer and no option for “don’t know/unsure” so no way to advance. How many of you know when you came down with every childhood infectious disease? How many know what exact strange infection you had when no access at the time it occurred.
I’m sure that they recognize that we’re all going by memory with the childhood illnesses and don’t expect anything more than general guesses.
They should ask something about how accurate are the general guesses, otherwise it is useless. Is it “give or take 15 years” or is it “give or take 2 years” or in my case “I have no idea” or “I have very high titters of EBV found later that were inactive but never had it actually” Given the obsessiveness and redundancy of some other sections, they could have designed this section differently. And there are many loaded questions later like “how often does this specific vary” when I never had that specific symptom and there is no N/A.
I’m rather surprised by the use of herbs powdered into a pill. Maybe it is a western idea of imitating allopathic medicine.
The use of medicinal herbs usually used decoctions, tisanes, tinctures, etc.
My Indian friend told me about how they use the black seeds: about 11 seeds, in a small glass of water overnight, you drink that in the morning. It’s possible soaking softens the shell, etc – who knows?
Meant to write:
The TRADITIONAL use…
I’ve had good luck with Resveratrol for 4 years now to help with brain fog. Still taking western meds for all the pain, though!!
I DIY through everything anti-inflammatory, diet, supplements, diaphragmatic breathing, stretches, etc. My new path is from the book The Immunity Code. Trying to heal my gut for once and for all, improve sleep and just a bunch of back to basics with some great hacks from the author.
I, also, have brain fog along with CFS and Fibromyalgia. I’m would like to try Resveratrol, but was your daily dosage?
I see that you have gut problems, which I had for over thirty years until recently. I had GERD and a lot of pain in my stomach and the pain intensified when I ate. My Gastro doctor had tried everything and nothing worked until my told me try Xifaxan (antiviral drug). For a thirty day supply, it was over $1,000. In the US there is no generic, but the rest of world, there is a generic Rifaximin. I went
pharmacychecker.com and found the generic at a Canadian pharmacy. For sixty pills, it was $55.00! My doctor gave me a prescription for Rifaximin and to take one in morning and one at night for fourteen days. Wait two months and do the same routine again. It has been over three months and no pain or GERD!!
Now, I just need to find something to take care of my fatigue and pain. I don’t know the problems you have in your gut, but you might want to talk to your doctor.
This research definitely interests me, I looked at many different theories as to what might cause CFS/ME which although im undiagnosed is the closest / only thing that accurately describes my illness, which came on suddenly although when I think carefully there were some odd issues in that year prior to it, and I was probably exercise ‘overtraining’ at the time.
I had many new problems in the past 3 years and I finally realised they seem indicative of MCAS, though I don’t get big allergic type reactions, the rashes I get are localised to my hands or forearms and doctors haven’t identified them. The biggest issue I have at the moment though is chemical sensitivity which has slowly gotten worse over 5 or 6 years, I don’t know if its just me but sometimes it spreads to include new substances or rooms and this can happen quickly over days, weeks or months. I’ve survived all the common symptoms of CFS even when ‘severe’ but this is the hardest one to deal with.
I have now noticed an association between these flare ups or shifts in sensitivity and ‘neuroinflammation’, which seems to follow some episodes of stress, exercise or prolonged exposure to known trigger chemicals. The strange thing is this does not always occur, there have been times where I exercised heavily, felt ill after but the spreading phenomena did not occur.
My question I suppose is do these ‘microglia’ have any sort of memory affected where once activated could pick out and then remember new types of everyday synthetic molecules, falsely identifying them as pathogens ?
Please think about looking into this with PANS PANDAS kids also. It would be amazing to have something tangible to show the inflammation and work out how to reduce it. This would help another set of suffering children and families.
I began the Chloe Jones survey, got over halfway through and now don’t know how to get back to it to complete it. Can anyone help me?