

(In 2021, Amber outlined the ways we are failing those with very severe ME/CFS in a blog on Health Rising. In this blog, Trude Schei reports on the results of a rare survey that documented the situation they face in Norway.)
Background

The Norwegian ME Association completed a rare survey of severely ill ME patients.
In 2018, the Norwegian ME Association undertook a large survey of severely ill ME patients. We wanted to look at symptom burden and disease severity, access to help and care, and how the carers experienced their condition. The answers we received were shocking, showing both how serious the disease is, how few receive adequate care and help, and the enormous burden of care for carers. We published a large report in Norwegian in 2020, and in 2023, we published an English Language paper in the Journal of Clinical Medicine.
In this blog, I will write about this paper, a little about the larger report, and try to give some background about healthcare in Norway.

The Norwegian ME Association documented the situation facing the most vulnerable among us and their caregivers.
ME/CFS is a severe disease, even in its mildest form, but a portion of patients have a severe form of the disease. The disease greatly restricts these patients’ lives. They are largely unable to leave their homes, and they certainly do not participate in studies where patients have to travel to a clinic. For many of them, a visitor in their home would be too much.
For this reason, they are mostly invisible, and we know very little about them. If there is little research done on ME/CFS compared to disease burden and impact on quality on life, this is even more so when it comes to severe/very severe ME/CFS.
We do not know how many ME/CFS patients have severe disease. It is often claimed that 25% of ME patients have severe ME/CFS, but I have not been able to track down the source of this figure, nor do I know how “severe” was defined, or how patients were identified. It is problematic that we do not have an international consensus on how to define “severe”.
This makes it difficult to know whether different studies are talking about the same group of patients. E.g., the new NICE guidelines define “severe” as “housebound”, while the ICC criteria says “mostly bedbound”. In another Norwegian survey with 5,822 respondents, 57% said they were “mostly housebound”, 15% said they were either “mostly bedbound”, and 1% were “bedbound and in need of care”.
Since this was a Norwegian survey, we used the definition in the Norwegian guidelines for ME/CFS, which are again based on the ICC criteria. Severe is defined as “mostly bedbound” and “very severe” as “bedbound and in need of care”.
The Survey
Of the respondents, 47 were classified as “very severe”, 444 as “severe” and 95 as “severe-moderate”.
The first step in the survey was an invitation to patients and carers to tell us about areas of concern. We received more than 80 open-ended responses, and a quick summary of what they said is “everything”. However, some areas stood out, e.g., home visits from doctors, symptom relief, the role of carers, and help for children of the severely ill. Based on this pilot study, we decided to focus on disease burden, the burden of care and access to, and quality of, health care.
The resulting survey had more than 90 questions, with a special section for carers, and another section for patients with children. Since we knew we could not possibly cover all possible scenarios with structured questions, we asked respondents to give us more information in open-ended answers. In the current paper, we have only included the structured questions, but we hope to write a second paper based on the several thousand open-ended answers.
The survey was advertised through social media and emails to members. The Norwegian ME Association had a membership of around 5,000 at the time of the survey. It also hosts a number of moderated peer-to-peer support groups on Facebook, with a total membership of around 8,000, and we also used the groups to inform about the survey. The survey was online, anonymous, and limited to one answer per IP address.
The survey was open from 19 July 2018 to 1 October 2018. and we received 586 complete responses. Carers could answer on behalf of patients who were too ill. There were no time restrictions on answering, and respondents could answer one question at a time. We know that many patients used many weeks to answer, and used valuable energy to do so. We are in awe of their willingness to tell us about their experiences, and very, very grateful!
Based on questions about activities of daily living, we classified 47 as “very severe”, 444 as “severe” and 95 as “severe-moderate”. This last group has a huge symptom burden, and are very ill, but not bedbound. We retained them as a comparison group.
Responses
The responses were shocking.
Many of the respondents were young or had become ill when young. Those who had become ill as teenagers or younger were overrepresented among the very severe patients. Most patients said they were getting steadily worse or experienced great fluctuations in the disease, but very few told of improvement. The symptom burden was enormous, and the level of function very, very low. Among the 47 very severely ill, many could not turn themselves in bed or communicate. Pain, nausea, fatigue, and brain fog were constant companions. Despite this, very few received adequate help or care from the healthcare system or from local authorities.
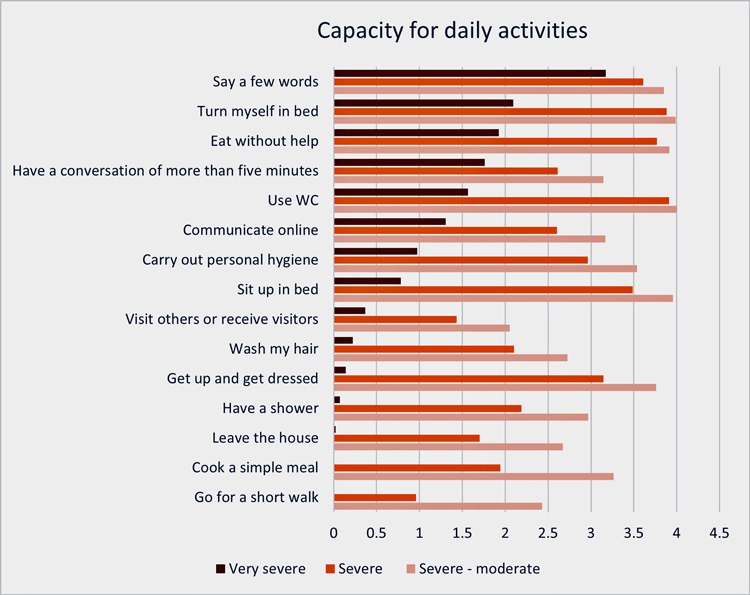
Capacity for daily activities: 0 = never, 1 = between once or twice a year, 2 = between once a week and once in two months, 3 = several times each week, and 4 = every day.
Norway has universal healthcare, and we like to pride ourselves that we have one of the best healthcare systems in the world. Local authorities have a duty to provide practical help and health care in the home when it is necessary, and we have a very good welfare system. All these institutions often failed the severely ill ME patients and their carers, though there were some instances of good care.
Many patients had chosen to say “no, thank you” to help in the home from local authorities. The nurses and other helpers who came to the patient’s home typically had no knowledge about ME/CFS, light and sound hypersensitivity, or how vulnerable the patients were. The open-ended responses told about nurses who, meaning well, tried to open curtains and start conversations. Helpers did not read instructions but came into the patient’s room to ask questions instead, wearing perfume and turning on lights. This caused a worsening of symptoms for the patients, and the “help” was actually harmful.
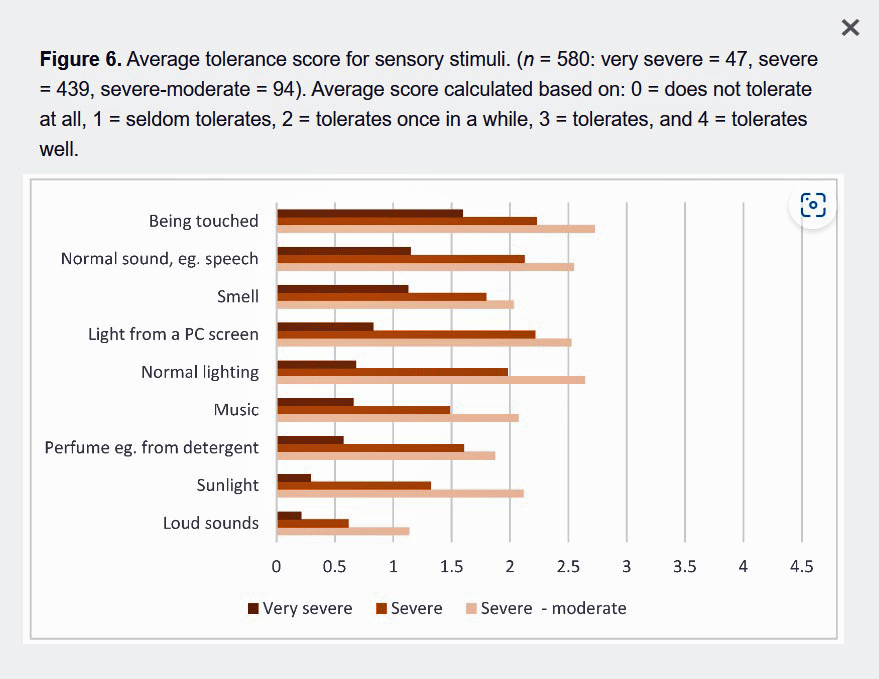
Sensory stimuli were particularly poorly tolerated by the severely ill: Among the 47 respondents with very severe ME/CFS, 36 (77%) seldom (six) or never (30) tolerated indoor lighting, 28 (60%) seldom or never tolerated the sound of normal speech, and 19 (40%) seldom or never tolerated touch.
This left a large burden of care on the patient’s family. Of the 47 very severe patients, all but one needed round-the-clock care, and most carers said they spent more than 40 hours a week on care, though this may underestimate the hours used. We were, in fact, criticized for having “40 hours” as the highest option, as many respondents wrote in the comments that they used far more time on care. We chose 40 h/week since it equals a full-time job in Norway.
The carers were worn out and desperate and felt a huge impact on their own health, financial situation, and social life. One carer described it as an “ongoing crisis”, another as “eternal vigilance, never knowing when the next crisis comes”.
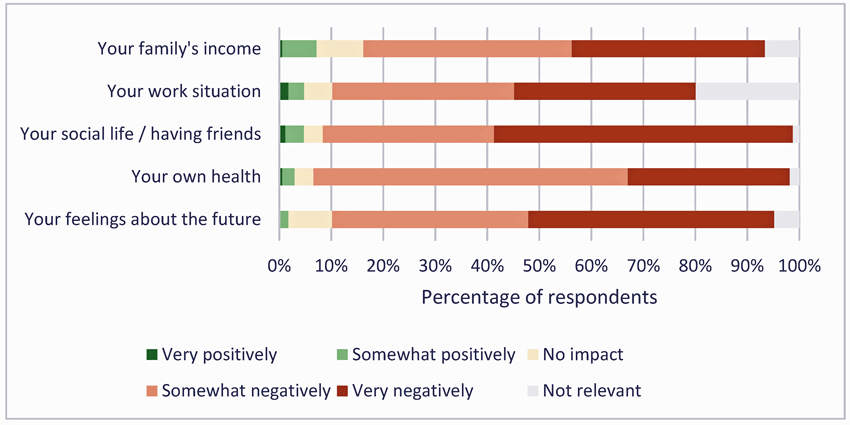
It wasn’t just the ME patients that were affected. With adequate institutional support lacking, caregivers reported being impacted in many ways.
Children of the severely ill did not receive adequate help, either. Only 27% of children had received counseling or other help, even if it is required by law. One mother wrote: “I hear the children in the living room, but I lie in the dark, too ill to see them, it is agony for a mother’s heart”.
68% of severe and 72% of very severe felt that they did not receive adequate health care. Only 1/3 felt that they got adequate help with symptoms like nausea, pain, and sleep problems. The patients were most satisfied with their general practitioner (GP/family doctor), occupational therapists, and physiotherapists, and least happy with specialized health care. We have seen the same pattern in other surveys. We believe the reason is that those who follow patients over time get a better understanding of the disease, and comprehend both how serious it is, and that it is very, very real.
Going forward

The severely ill are mostly hidden from our sight. This survey helped us see them a bit better.
We received several thousand open-ended replies, but this paper is only about the structured questions. We are hoping to write a paper about the open-ended questions, too. The responses were excruciating reading, with despair and hopelessness screaming from every line.
Many answers describe what can only be termed abuse from hospitals, doctors, and local authorities. There were patients who could not walk, but when in the hospital were not offered a wheelchair to go to the toilet, because the nurses said it was good for her to “try”.
The Gist (by Cort)
- Over almost 3 months in 2018, the Norwegian ME Association sent out a severe and very severely ill survey to its 5,000 members and 8,000 members of its Facebook page.
- The survey contained more than 90 questions and included sections focused on caregivers and the children of the severely ill.
- Based on the results of daily living questions, they classified 47 people as “very severe” (bedbound and in need of care), 444 as “severe” (mostly bedbound), and 95 as “severe-moderate” (high symptom burden but not bedbound).
- Many of the severely ill had come down with the disease while they were young, and people who had become ill as teenagers or younger were overrepresented among the very severe patients.
- Among the 47 very severely ill, many could not turn themselves in bed or communicate. Pain, nausea, fatigue, and brain fog were constant companions.
- With local health authorities sometimes causing more harm than good by not acting appropriately, many of the severely ill have chosen not to ask for their help.
- The caregivers faced an immense burden. Of the 47 very severe patients, all but one needed round-the-clock care, and most caregivers said they spent more than 40 hours a week on care. Income, work, and social life were all often significantly affected.
- Problems with sensory stimuli were particularly apparent. Only a few of the very severely ill (23%) could even withstand indoor lighting. Over half seldom or never tolerated the sound of normal speech, and 40% similarly could not tolerate touch.
- On the positive side, there were responses that show that it is possible to give good care and to provide carers and patients with a feeling of security. The key is to listen to the patient and to the carers and support them.
On the positive side, there were responses that show that it is possible to give good care and to provide carers and patients with a feeling of security. The key is to listen to the patient and to the carers. There is no research today on what constitutes best practice when it comes to severely ill ME/CFS patients, and in that absence, carers and patients are the experts. It is also important to provide symptom relief – but most important is respect, humility, and empathy.
However, not all patients have a family, so there is an urgent need for specially adapted care institutions. The Norwegian ME Association has cooperated with a non-profit diaconal foundation, and there are currently 12 spaces at Røysumtunet. We see that when given the right conditions, some, but not all, patients improve a little. When you are as ill as these patients are, a little is a lot, and the importance for the patient is enormous.
I have heard many presenters say how confusing ME/CFS is, and use the story of the blind, wise, men, and the elephant. How you describe the elephant depends on which part you touch. I would like to say: Talk to the elephant! It knows a lot about itself. In the absence of research, basing care on patient experience is common sense.
We are hoping that our report and the paper will contribute to shed light on the plight of the severely ill, and also to better care for this severely neglected group.
The Authors
- Kristian Sommerfelt is professor emeritus at the University in Bergen in Norway. He is a pediatrician with long experience with ME/CFS.
- Arild Angelsen is professor of economics at the University of Life Sciences in Norway. He has ME/CFS patients in his family and is a board member in the Norwegian ME Association. He has worked on several large patient surveys in Norway and internationally.
- Trude Schei is deputy CEO of the Norwegian ME Association. She is an architect by training but has had ME/CFS since 1999. She has worked on several large patient surveys in Norway and internationally.
More on the Severely Ill






Hi
I have ME/cfs
Im intressed of be in study of Me/cfs !
Im Living in Sweden 🙏
I am so extremely grateful to you for this study. I really needed the support today and in future I can use this to send to people and try to help them understand.
An excellent study by the Norwegians! I’m so glad you have collected this data & now have a paper on it – it will be very useful for other countries.
Norway continues to make excellent contributions to the ME field, as I think about the work of the wonderful DRs. Fluge and Mella.
Dr. Judy Mikovits’ research in 2009 (at UoN-Reno) discovered that “zenotropic murine leukemia virus-related virus” (XMRV) (a mouse-related virus) infected 67% of ME/CFS patients. As a virus researcher since the 1980s she was abruptly terminated and/or blackballed from receiving subsequent government research grants by the powers-that-be at the National Institute of Health. Why?? Because she insinuated that XMRV retrovirus could only become active as a result of previous inoculations. Indeed, the XMRV virus hides in B and T lymphocytes; the very immune cells that are designed to be stimulated by vaccines. Hence, the stimulation causes XMRV to become active, proliferate, and cause ME/CFS in at least two-thirds of its victims.
Indeed, to discover why a cure for ME/CFS has not been invented, one must follow “the money”* and Big Pharma/NIH/CDC politics of national immunization programs.
I entreat everyone to read Judy Mikovits’ “Plague: One Scientist’s intrepid Search for the Truth About Human Retroviruses, Chronic Fatigue Syndrome, Autism, and Other Diseases””
* $22 billion just from SARS-CoV-2 Immune-modulator innoculations
They arrested her when she went back to retrieve her notes. If she’s a “quack”, who cares what is in her notes. Like Jody Foster said in Silence of the Lambs, “UVA is no finishing school!” Dr. Judy Mikovits received her Ph.D. From UVA. She thinks outside of he box, which is what the ME/CFS patients need.
She had to retrieve her “note books” because not doing so would be a violation of her legal obligation to manage the grant program. Unfortunately, she learned the hard-way about the politics of the National Institute of Health and the politics of its research-grant protocols. Like all health agencies, not only are they regulators, but they’re also in the business of protecting their clients who are all members of Big Pharma. Why is this so? Because the agency employees are all previous employees of Big Pharma members. Dittos of Dr. Judy Mikovits
Thank you Trude. The lack of care for people with severe and very severe ME is so sad and infuriating. Recently in the UK, very distressing stories emerged about the experience of some people with very severe ME, not receiving nutritional support. A protest was organised in London, to highlight these concerns and demand better treatment, called #DontLetMEDie. It seems that the people who need the most care, often receive the least help.
I was afraid to read this article. But it obviously important. It’s hard to know how sick these people are, how the carers are exhausted and the impact on everybody around and have nothing to offer. I love « Ask the elephant » to learn how to care for a person.
My daughters have gotten the psychological help they needed as teens only as adults living in a different state, which has universal healthcare including counseling. It was so difficult for them! And me. One daughter kept saying to me that she was sure I could get up and work if I just wanted to. It was dismaying to hear this echoed initially by the psychiatrist I had to see to prove I wasn’t clinically depressed. She still thought in the end I was too focused on my health concerns, though not depressed.
That must be heartbreaking and so frustrating for you Cherie and for your daughters.
Thanks for this very important work
Two comments:
– it occurs to me that the questions used here could be converted to an excellent severity scale for the worst of us, far better than Bell or other current scales
– I find the ICC very severe = bedbound & requiring care disturbing in that it wrongly implies those of us who aren’t bedbound don’t need care. I’m merely housebound & severe-to-moderate compared to your survey responses. But I can’t cook, shop, prepare food like breakfast, do any housework (or work). If I didn’t have spouse & paid care, I would be very severe by now.
Can the M.E./CFS national nonprofit (I forget its name) — the one that gives the Ramsey awards — do a similar Quire study followed by federal + state lobbying (Include breaking down findings into US Congressional District — very effective approach for writing to & visits with Congresspersons, the proven approach that RESULTS, Inc. does.) Could you please forward this comment + this such sadly enlightening but helpful blog to them? ——————
What this survey did not address — which is what makes this all the more urgent & heartbreaking — It is the minimal income most of us have, as I do. (IF they are eligible for disability, IF they can apply. (I was too exhausted to even TALK to a Rep at first). Plus, there are the 1.5-2-year processing delays in most states. Many with this condition cite their partner leaving/divorcing them (imagine this!), with money loss likely associated. A paid caregiver, house-keeper, other non-covered needed health services + supplies & just rent that’s so high now, plus other living necessities — add up to FAR more than a SSDI payment. There was a good national article years ago citing that many have to live in a car, or even are homeless. Imagine. —————
I feel this is what is MOST needed by states & national funding, to address
— NOW! To do everything possible for these MOST suffering among us — (alongside the research for causes of & finding treatments for ME/CFS). (I speak as one who’s been about 90% bed-bound for 17 years.) Lobbying for this would bring awareness of just how extremely serious this disease for at minimum OVER HALF A MILLION CITIZENS who are most severely ill and probably deeply suffering … and likely are their children, if they have any living with them. (This number is a more conservative 20% estimate of those of us severely impacted with ME/CFS disease, than CDC’s 25%.) —————
Thank you so much for addressing this in HealthRising, Cort. Even “hot off the press,” it has already been helpful for me to share, to explain just how serious our disease is. I would like to see more coverage of the severely ill among us, including referrals to resources that could help. —————
My heartfelt best wishes and hope for ALL of us who are severely ill,
Love, Ms. Alden Lancaster (Takoma Park, MD — at edge of DC)
I couldn’t agree more & am grateful to you for making these points as it saves me from the struggle of doing so. I, too, have severe ME/CFS.
Until a direct remedy for ME/CFS is discovered, be sure to maintain a Vitamin D3 serum level of 90 to 100 ng/mL
Direct sunlight on the exposed body is the normal means to increase and maintain levels; however, in Scandinavian nations, especially on the shadow side of mountain ranges, direct sunshine is nil, especially in winter months when one is more likely to suffer D3 deficiency. The other means of obtaining sufficient D3 is the consumption of sockeye salmon and rainbow trout.
Why D3 to improve symptoms of ME/CFS ? Vitamin D3 (a hormone) provides maximum efficacy to the immune system that is tasked to immediately recognize and kill pathogens when they enter the body. Low D3 serum levels means the immune system is slow to react to and kill pathogens/antigens which will result in long-term illness. Since ME/CFS is the result of viral/retro-viral*/pathogen infection, the immune system must be enabled to discover the infected cells and mark them for death (apoptosis), and thus killing the virus in the process. Only a healthy immune system has the power to mediate symptoms. However, for a complete cure of ME/CFS, hoped-for pharmaceutical remedy is apparently necessary to assist the immune system.
* Retrovirus’ unfortunately hide in immune cells and damage their functionality, thus making a pharmaceutical remedy a difficult endeavor indeed because of the inordinate complexity of the nano- and -micro-biology of the immune system.
I have been prescribed high level Vit D for 4 years as I was on the low side, and lie in the open doorway during the summer months daily.
It has made absolutely no difference whatever to my severe ME/CFS syptoms, PEM etc. Just raised my vit D reading.
I’m sorry to hear, Jane
Vitamin D3 causes the immune system to discover and kill bacterial and virus infection that primarily enters the body via the respiratory system. However, retrovirus-caused ME/CFS is primarily introduced to the bloodstream directly via contaminated inoculation. Herpes retroviruses have the ability to infect T & B lymphocytes in addition to monocytes. Thus the reason that ME/CFS is so difficult to treat since the very immune cells, designed to discover and kill the retrovirus, are instead infected themselves and thus become neutralized.
If what you are saying is true, why doesn’t cure me/cfs ? Because there is no cure, stop peddling this bill shit
The cure is going to have to be an anti-viral remedy since many bio-labs throughout the world are searching for a cure. In the USA, the research only began recently because the medical establishment recognized ME/CFS since the 1934 as a psychological rather than pathological affliction. By 2009, the pathology was finally determined to be a retrovirus, the most difficult kind to treat because it embeds itself into cellular DNA in addition to B and T white cells.
In 2009, research at WTI, Nevada, the majority of ME/CFS patients were infected with Xenotropic Murine Leukemia virus-like Virus (XMRV), a retrovirus that also causes low levels of Natural Killer white cells..
The blood test tells you nothing about your vit D status – it is like thinking you know how much petrol is in a petrol station by counting the tankers going past.
Early on in my 23 years of ME we would spend 2 weeks each year in a timeshare appartment on the island of Madeira. After a few visits we noticed that within a couple of days of arriving my symptons had disappeared, and we were able to spend whole days walking in the hills, but the improvement didn’t last long when we were back in the UK. When I discovered vit D3 supplement helped reduce my symptoms I experimented with doses to recreatd the experience on Madeira. For the last 18 months I have acheived that effect by taking 200 micrograms vit D3 supplement every hour 13 times a day, with no negative effects. Recently I have increased the dose to 200 mcg every half hour, still without any negative health effects.
Hi, Alden,
This is Mohan.
Today a friend sent me a photo of Takoma Park where she was visiting her daughter. Then I remembered you, who also live in Takoma Park. So, I googled you and found this link!
How are you?
My email address is: dkmkartha@yahoo.com
Hope God’s healing is sustaining you. I see you are still helping others! How wonderful!
to broken to read, to broken to write…hope i can soon. but glad for attention on (verry) severelly ill ones.
Hi Cort,
Thanks for the go ahead with Metformin to help my FM pain! I’ll discuss it with my doctor.
I’m confused about ME/CFS & CFIDS. With my FM I have CFS & possibly ME. I have always been tired, exercise intolerant, etc. & was told that was CFS. My gyn doctor gave me diet pills, not to lose weight but to have energy to work full time & take care of my family. My cousin had Mono & I could have caught it from her. I had a cold almost continually, going to bed, loosing my voice, etc. However, we lived in the country & never had a doctor available. Therefore in reading the symptoms of ME/CFS I qualify.
I joined a forum on my PC for CFIDS to just learn about it that had another name (I don’t remember). When I stopped the forum my friend Gail asked me to call her. We had a nice relationship but she definitely was worse off than me. She graduated from college & had a good job, then she started having colds with other problems. She had to quit her job & in a short time she was basically in her bedroom. We were able to talk & although I had FM/CFS & she had CFIDS we understood each other. Dr. Lapp in Charlotte NC was her doctor. I see where Dr Lapp & you have shared information. Anyway, eventually she asked me not to call her again as she was to ill to talk. That Christmas I sent her a card & her family sent me a note saying she had passed on. It upset me that she was young & suffered so much without any help available.
I am in the UK. Our National Health Service is in a state of collapse due to government deliberate neglect and ongoing privatisation.
I hoped against hope that the new NICE guidelines would really make doctors do the right thing. For 20+ years, my condition worsened. After more than six years of mostly horrible care from agencies provided by Social Services, I quit all communication with them and now only employ one person who does a great job. Otherwise, I am mostly bed bound and can only afford a few calls a week to prepare quick meals and keep the house clean
I have no family or friends in this country.
I have had nothing but abuse, disrespect, disbelief, disinterest and neglect from every one of the dozen or more GPs I’ve seen.
Recent attempts by my advocate with an excellent letter about the new NICE guideline and my needs resulted in the GP saying in a reply letter that we were being unfair to expect her to be the primary person to visit me at home (I ‘ve not had a single home visit for well over 4 years) and unreasonable and unfair to ask that she treat my symptoms with attention to expert advice and recommendations from experts such as the doctor who diagnosed me in 2015 and the ME Association’s resource book for health professionals and the new NICE Guidelines. Her contention was stated as based on the fact that she is not an expert, she can’t be expected to treat me according to expert guidelines such as those available for all doctors from the NHS own website!
She ended her letter with a very familiar conclusion, which I’ve received many times over the years. “If you are not satisfied with my approach, you are free to find another GP or another surgery.”
I have been to every surgery who is accepting patients in my area. They showed no respect or even an ability to listen to a carefully and clearly worded sentence from me or my ME charity advocates about my symptoms or my needs. I’ve been treated with contempt, mocked and screamed at a number of times by both GPs in my home and by Social workers. The new NICE guidelines have no effect. She wouldn’t even read them.
My condition worsens. I am 70 yrs old, cannot travel in a wheelchair taxi due to POTS, and struggled for over 6 years to get an electric tilt chair which doctors would not help me get, but finally direct communication with the wheelchair service and letter from the private charity doctor who diagnosed me was enough to have their assessment team provide the chair.
The specialist service in my area has a lead team notorious for arrogance and disregard of oatients’ concerns, and claiming to focus on “RECOVERY” with a long history of GET.
I don’t seem to have any options. When my paid care worker takes time off, I have no backup and although she provides a lot of meals ahead of any absence, I cannot manage without severe exhaustion and PEM most days. I end up increasingly exhausted and have had serious accidents/falls this year, which thankfully did not result in broken bones or severe lasting injury. Her holiday absence was 12 days long and I have not recovered to a stable baseline since then.
I feel there is no hope at all.
Kay.
Omg. That is horrible about your friend. All of these health issues. Fibromyalgia CFS ME and I have Psoriatic arthritis and it’s brutal. Lost the job I loved. So tired all day and trouble sleeping at night. Not many understand all of this.
Hi Sandy,
Thanks for your message. I have FM/CFS/ME bad enough to keep me aware of what is happening. Mine started at birth & I have battled it all my life, now I’m 85. So sorry to hear about your Psoriatic Arthritis & your battle.
Gail, my friend was diagnosed with CFIDS somewhere in the middle of her illness & that is what she had when she passed on.
My heart fell to my toes when she asked me not to call anymore because she couldn’t talk
I wonder how many people suffering with CFS/ME reach a point of not being able to talk, etc.
You take care, may God Bless.
The author has twice asked about where the 25% stat comes from and been shown all the information.
The ICC, for reasons unknown, have used a definition of severe ME not Used elsewhere which has muddied the waters. We have a group called the 25% group for the severely affected operating in the UK (despite seriously lagging now for years, the U.K. was once the leader on ME – with official validating chief medical officer report back in 2002 Etc & being one of the few countries to have a special group for the severe and more recognition consequently). This group is for anyone who is housebound, can only go out infrequently with a wheelchair and this places severe ME at that level, NOT mostly bedbound. We now have additional confusion in the UK with the NICE guidelines stating, in the few lines given to the definition, that those with severe ME are Unable to do anything for themselves , accept perhaps clean their teeth. Which again is not true (Whitney dafoe who is VERY severe cleans his own teeth afaiu) this has for some reason been added why charity reps in all official U.K. lit. since 2002.
We really have to be careful and tbh more thoughtful about how severe ME and very severe ME a defined , to give proper space to all those who are worse than moderate – ie can not go out hardly ever – but who are not in the full throws of the horror that is very severe ME. There is as many as 20% of pwME in this situation, yet literature, often written by people without severe ME experience , tends to lump people and blur lines. There is as much difference between those at the bottom of very severe ME – fully bedbound / severe pain, intolerant of any light etc and those at the upper end of severe, as there is within the mild category of those nearly recovered and those struggling to just about work but ending aLl social and active life.
I absolutely agree that we need better definitions for severity, and international consensus on how to define severity.
Since this survey was done in Norway, and we wanted to se if severity affected access to care, we used the definitions from the Norwegian guidelines for CFS/ME, which again are based on the ICC-criteria. In this definition “very severe” = bedbound and inneed of care, and “severe” = mostly bedbound.
Calling “mild” ME “mild” is a misnomer, and undercommunicates how severe even a mild form of ME is. Perhaps we even need new names.
I have tried to track down the original reference for the 25% number, in order to find out how “severe” was defined, and how they arrived at the number. I would be very grateful if you have the original reference, since I hav been unsuccessful in finding it.
According to several surveys we have done in Norway, as many as 57% of patients may be too ill to leave their homes without great difficulty – and I believe the severity of ME is grossly undercommunicated.
IN 2019 we did a survey in Norway about the course of illness, and had 5822 respondents. 25% defines themselves as “mild” (at least 50% reduction in function) 57% as “moderate” (mostly housebound) 15% as “severe” (mostly bedbound” and 1% as “very severe” (bedbound and in need of care). In 2021 we repeated this survey in all of Europe (11200 respondents) and the distribution across the different degrees of severity remained remained largely the same in all countries. In all surveys, carers could answer on behalf of patients too ill to answer themselves. Of course, there will always be a risk of bias in thes surveys, and we may not have reached the most severely ill who do not have anyone who can answer on their behalf.
Agreed. The language around a disease that is already questioned needs to be updated.
Ask a stranger what they think “MODERATE chronic fatigue syndrome” (or “MODERATE M.E.”) means, and note the gap between their best guess and a person who will never again in their life be able to work any job, experiences near-constant pain, has photophobia that limits screen time (and reading), is mostly isolated, suffers pain from social engagements of even minimal length, can’t think straight enough on most days to navigate the modern medical system bureaucracy, BUT…can run one errand on most days, or instead choose to take a shower and work in the yard for twenty minutes. That, as I understand it, qualifies as “MODERATE.”
I know this topic is covered all over Cort’s site, for many years, but what is the solution? Has one been put forward? If so, what are our marching orders?
Everyone needs to pay attention to the progress of Dr. Bruce Peterson, founder of IncellDX, a laboratory located at Hayward, California, USA.
He’s concurrently working on a remedy for ME/CFS just as he has successfully done with Long Convid Syndrome.
https://www.healthrising.org/blog/2021/07/21/patterson-cracked-long-covid/
Has anyone asked CDC how they arrived at their figure of 25% pwME/CFS being severe & bed bound?
We now know the mechanisms of SARS-CoV-2 infection. In a new paper from Nature Cell Biology, 13 months in review, with 29 (!) authors, and incorporating several follow-up studies for confirmation, the authors conclude:
“Altogether, our results indicate that SARS-CoV-2-induced DNA damage triggers a cell-intrinsic pro-inflammatory programme that, in concert with the immune response, fuels the strong inflammatory response observed in patients with COVID-19. The observed ageing phenotypes recently reported in patients with severe COVID-19 are consistent with our observations. Finally, by proposing a mechanism for the generation of DNA damage and the activation of DDR pathways and of a pro-inflammatory programme, we provide a model to improve our understanding of SARS-CoV-2-induced cellular senescence. In this regard, it will also be interesting to determine if persistent DNA damage and DDR activation, features of cellular senescence, following SARS-CoV-2 infection, contribute to the chronic manifestations of the pathology known as long COVID. ”
https://www.nature.com/articles/s41556-023-01096-x
The details are quite technical and some parts of the model rely on descriptions of newly recognized proteins in the inflammatory response and the process of cell senescence.
A researcher not involved in the study responds: “The results explain much of what is observed in COVID-19 patients, and this research will be useful in understanding long COVID. How this knowledge might lead to effective treatments of COVID-19 is not immediately clear, but a thorough understanding of the molecular and cellular derangements caused by COVID-19 will be essential. As shown in this research, the damage done by SARS-CoV-2 probably resides deep in the cell and can be severe and long lasting for that reason.”
Thankyou for this article . In every detail of these colorful charts I am “very severe” ME/CFS since 2001 .
I have had M E for 30 years it is more complicated than you think.I am lucky as know what started mine .The research is partly right but your nervous system is what’s going wrong .The more pain is from your nervous system that’s not functioning properly so it paralysis the muscles. I can tell you how nervous system works and what it does .
You should never do exercise you should concentrate on being able to move about the house .If you want to go out use a mobility scooter reserve energy at so you can build up the body .
The hardest thing for your body is walking it has to use that many nerves to function it makes you exhausted . What I eat drink and medication effects me . I have a good life now but I’m expert on what works and what doesn’t your body tells me what’s good and what’s bad for me . I have discovered many things on ME over the years too much to list .