

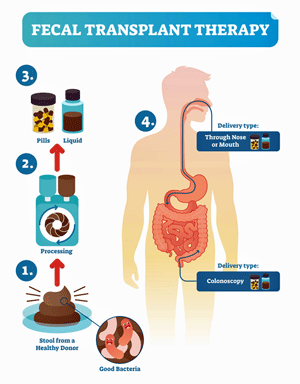
Fecal matter transplants have been a part of Chinese medicine for almost 2,000 years.
With the gut microflora (the gut-brain axis) able to affect the brain and cognition and with dysregulated gut microflora implicated in chronic fatigue syndrome (ME/CFS) and fibromyalgia (FM) – not to mention diseases like Parkinson’s and Alzheimer’s – a finding a corrective gut flora treatment might be a big deal.
So why not take up fecal matter transplants (FMT) transplants – something Chinese medicine employed almost 2,000 years ago? More recently, they’ve, after all, been successfully used to treat the very dangerous Clostridium difficile infections.
So why would they not help out ME/CFS, fibromyalgia, or irritable bowel syndrome – all disorders with gut flora issues? Laura Pace, the co-founder of the Metrodora Institute, has one reason – the difference in the flora between the bowel and the flora of the small intestine – where most of the digestion, etc. is.
Fecal matter transplants are underway, however, being tested in many diseases. Two studies have been done in ME/CFS, and a large and surprisingly comprehensive one is underway.
The Kenyon Study
They did well, though, in the first rather unorthodox ME/CFS Kenyon study, which had its participants take no less than 10 fecal transplants! It was also not placebo-controlled or methodologically rigorous, and consisted of a series of case reports.
Still, with the paper reporting that seven of the 21 treatment-resistant patients reportedly returned to full or near normal health, and six others received significant improvements in energy, the reports were encouraging indeed. One person who had been sick for decades reportedly returned to health.
It was good news, then, to hear that two more ME/CFS fecal transplant studies – a small one in Finland and a larger one in Norway – were underway.
The Finnish Study Fails
The Finnish study was small indeed – just 11 patients – and in contrast to the case series – which provided fecal matter transplants over ten days – the participants received one 30-gram treatment. Sometimes antibiotics are given to clear the bowel before treatment but not in this case.
The study was small but rigorously done. The participants had to meet the Canadian Consensus Criteria (CCC) for ME/CFS and the trial was placebo-controlled – meaning that some participants received the fecal matter while others received a placebo (a fecal matter transplant using their own feces). Plus, the fecal matter was delivered using a superior method of administration – a colonoscopy. Quality of life, visual analogue, and fatigue scales (MFI) were used to assess the effects of the treatment one month and six months later.
Unfortunately, there were no treatment effects; i.e. the patients receiving the fecal transplants were no better off after one or six months than those receiving the placebo.
Where We Are Now

With one positive and one negative study – both of which used very different treatment regimens – it’s hard to know where we are.
We have one positive and one negative treatment result. One clear difference was that the Kenyon study used the Taymount Clinic’s ten-day protocol, which includes a colon irrigation, followed by ten fecal matter transplants.
Other fecal matter transplant studies have also used different protocols. The Chinese have been doing fecal transplants for a long time and appear to use more of them. One Chinese group, for instance, reported that it’s treated over 2,000 people with fecal transplants.
A large Chinese irritable bowel study, which gave an oral antibiotic (500mg vancomycin orally twice per day) for 3 consecutive days followed by transplants for 6 days, followed the participants for five years. The study reported 50-60% efficacy rates with fatigue and mental health scores improving by roughly 30-40%, which were largely maintained over the study. Periodic (apparently yearly) fecal transplants were generally needed to maintain efficacy.
THE GIST
- With the gut microflora (the gut-brain axis) able to affect the brain and cognition, and with dysregulated gut microflora implicated in chronic fatigue syndrome (ME/CFS) and fibromyalgia (FM) – finding a corrective gut flora treatment might be a big deal.
- So why not take up fecal matter transplants (FMT) – something Chinese medicine employed almost 2,000 years ago and which are effective against the very dangerous Clostridium difficile infections.
- Laura Pace, the co-founder of the Metrodora Institute, believes the difference in the flora between the bowel and the flora of the small intestine – where most of the digestion, etc. is – is too great to make them likely helpful. They are, however, being assessed in multiple diseases.
- Two studies have been done in ME/CFS. A case series from the Kenyon study which gave no less than 10 fecal transplants to its patients, reported that seven of the 21 treatment-resistant patients returned to full or near normal health, and six others received significant improvements in energy. One person who had been sick for decades reportedly returned to health.
- The recent placebo-controlled Finnish study included just 11 patients and the participants received one 30-gram treatment – but was much more methodologically rigorous. Unfortunately, there were no treatment effects; i.e. the patients receiving the fecal transplants were no better off after one or six months than those receiving the placebo.
- It’s possible that providing more fecal matter or providing it more times might have helped.
- The fecal transplant field is in flux. It’s not clear how much poop should be delivered, how it should best be delivered, or how many times it should be delivered to produce the best results.
- A 2020 review, “Current status of fecal microbiota transplantation for irritable bowel syndrome“, reported mixed results with four positive studies and three negative ones. The review concluded that larger doses (60g) were better and found that 70% of the people who did not respond to 30 grams – the dose used in the Finnish ME/CFS study – responded to 70 grams.
- The large and very comprehensive ME/CFS Norwegian Comeback study underway uses a higher dose (50-80 grams) and will periodically assess a comprehensive array of factors including the microbiome flora, leaky gut, heart rate variability, metabolomics and metagenomics analyses, and immune profiling (!).
- Containing 160 patients, the RESTORE ME placebo-controlled study – funded by Invest in ME – and begun in 2020, is even larger. It includes one transplant and will assess physical activity, and cognition and will analyze blood and fecal samples from the participants.
- According to its timeline, the last patient in the study has started the study, and the results are expected in a couple of years.
A more recent update of a 3-year IBS study, however, found that one FMT dose (30-60 grams), which was transplanted directly into the colon, was enough to allow most patients “maintain their response at 3 years”. The paper specifically noted the increase in two gut factors associated with ME/CFS – increased levels of the Faecalibacterium prausnitzii bacteria as well as butyric acid (butyrate).
While most Western studies appear to use one dose, t’s possible that the Finnish study, with its 30-gram dose, was underpowered. It’s also possible that multiple transplantations may be more effective. Doctors who employ them regularly may be finding that multiple transplants work better. That issue, however, has apparently not been well-explored in the scientific literature.
Field in Flux
With regard to ME/CFS and fecal transplants, we’re left with two widely differing results – something that’s not all that surprising given the flux the fecal transplant field is in. Questions regarding which donors are best, how much to give in each dose, the best method for transplanting the fecal matter, and the optimum number of doses pervade the field. With regard to ME/CFS, we don’t know if fecal transplants work best in people with ME/CFS and IBS or if they will also work in people with just ME/CFS, or if they work at all.
The large and quite comprehensive ME/CFS Norwegian Comeback study and the RESTORE ME studies should help. The Comeback study will using a higher dose (50-80 grams) delivered using an enema. Nowhere does the study explicitly state how many transplants are given – suggesting that it will include one dose.
The 80-person study which began in 2019 is placebo-controlled, uses validated questionnaires, follows the participants for 12 months, periodically assesses microbiome flora, leaky gut, and heart rate variability, does metabolomics and metagenomics analyses, and immune profiling (!).
This impressive study, which may be digging deeper into the physiological effects of fecal transplantation than any before it, began in 2019. Its last participant was slated to go through the study in March of this year, but the study is not expected to be complete until 2026.
Containing 160 patients, the RESTORE ME placebo-controlled study – funded by Invest in ME – is even larger. It includes one transplant and will assess physical activity, and cognition and will analyze blood and fecal samples from the participants. Since it has been underway since 2020, we should get the results sooner rather than later.
Remission Biome
The Remission Biome project with its extensive use of antibiotics, keto diet and specialized probiotics is taking a different route. It’s now attempting to put 50 people with ME/CFS on its gut protocol.
Find out more about Remission Biome check out the blog below – and if you’d like to apply to be one of the 50 – go here.






I saw once a webinar long time ago where someone of the audiance had several FMT’s but felt back again sadly enough. But maybe where the FMT’s not well done or other co-factors.so. I shurely hope that the large and quite comprehensive ME/CFS Norwegian Comeback study will be so clever to do multiple FMT’s. so sad to must wait so long for the results! 7 years over a study pff and waiting until 2026! if i could, i would go for FMT’s , safe ones.
And what about the NIH findings of gutmicribiome? are they doing anything?
It really is a superb study! I wonder, in fact, if it’s the most comprehensive FMT study ever done in any disease. Let’s hope those results come in earlier.
Unfortunately they weren’t so clever :/
Hopefully the RestoreME FMT trial will be able to get underway soon as well. I heard they were planning to finally start recruitment later this year. I believe they are using a protocol with capsules, so perhaps not as effective in terms of administration route, but would presumably be fairly easy to do multiple doses, if they choose to.
Disappointing results from Finland, but at least with a few separate studies we stand a chance of getting a reliable answer to whether this treatment is helpful or not
Thanks for your continuing great info Cort
There is actually debate about what works better. The Chinese study liked capsules because they were so easy to use. Some people think the other procedures work better but it seems like the capsules will work.
Thanks for the info on the RESTORE trial. It didn’t show up in the clinicaltrials.gov database but I’m very glad to see it and will add it to the blog. Nice to see ME/CFS researchers jumping on this.
Thanks, that’s good to know!
It’s taking place in my area so have registered interest in doing it… you never know!
The biotech company MRM Health is trying to treat Parkinson’s disease, diabetes and autoimmune diseases with a cocktail of live intestinal bacteria.
https://www.tijd.be/ondernemen/farma-biotech/belg-gaat-ziektes-bestrijden-met-levende-darmbacterien/10464956.html
From Belgium Cort 😉
I hope you can use google translate 🙂 lol
Thanks! It’s so interesting how similar gut problems have shown up in different diseases.
We agree on this 🙂
I always thought that endotoxines could cause ME/CFS.
Our symptoms are almost similar to sepsis. Almost every ME/CFS patiënt i know have intestial complaints even before the disease started.
If I remember correctly, they started years ago in Belgium with a very large-scale study of different intestinal flora in healthy and sick people, but people with ME/CFS were also included. If I can find it I’ll report it here.
Hi Gijs, did you find the study? I am verry interested, live in belgium, lay in belgium. would like also know where they do that (in a good way) because I have gotten colon issues.. thanks!
Not yet, sorry.
I will look more. I know for sure it was started some years ago.
Many people included.
You can try Yakult for your issues.
Hi Konijn, I found it 🙂
https://nieuws.kuleuven.be/nl/2016/grootste-darmflora-onderzoek-ter-wereld-onthult-verbanden-tussen-levensstijl-en-darmflora
thanks so so much! If i can and if I get answer, I will contact prof Raes with the NIH findings on gut. sadly he is a researcher and does not do FMT. but what i read, researched as much as i could, I understand that it will be taking a long time to know what a good microbiome is. I thought they stood furder with that. so I am warned…
FMT has been well known to many in the autism community for several years. Some ASD children have had remarkable positive results, but some medical professional organizations ran this method down, or even punished some of those who used it. I read ( unfortunately I can’t remember the exact source) that healthy family member donors offered the best results. Many parents used this method privately, as some medical professionals, including physicians, naturopaths etc, were at risk of losing their licences for using FMT. I’m so glad to see this ongoing research, tho’ it’s taken far too long. I’ve been following the interest and more recent burgeoning of research in this area.
The large Norwegian Comeback study has also failed, in the sense that FMT provided no improvements in people with ME/CFS or other evidence of improvement. It hasn’t been published yet, but this is information coming from trial participants. See also here https://www.reddit.com/r/cfs/comments/13c18gv/update_on_norwegian_fecal_transplant_study/.
Not keen on labelling study outcomes as failures. A negative result is not a failure if it contributes to a wider understanding of treatment options.
11 participants sounds far too small to say anything useful though. Is the placebo group included in those 11 people? “Massively underpowered study finds no treatment effects,” would be my headline.
Not a bad title! 🙂
Darn! FMT’s seem like such an easy way to get some help. I do wonder if more treatments are better. It’ll be fascinating to learn if the FMT significantly changed the gut flora in the right direction. If it did and patients didn’t get any better that would say something. Thanks for the update 🙂
I have wondered about trying this myself, because my initial
EBV infection in 1979 was not mono, but rather, it was in my gut.
I got ten fecal transplants two years ago. After the third I could walk for quite a while. Usually I am using a wheelchair for most distances outside the house. But the effect wore off over the next few weeks until it was gone. My consideration is whether the fecal transplant had been destroyed by my digestion. I have too few digestive enzyms and too few stomach acid. The digestive enzyms I substitute, but pepsin oder betain I cannot tolerate. The stomach acid is responsable for killing the bad bacterias. My conclusionis: Before a person gets a fecal transplant, not only the microbiome should bechecked, but also the digestion.
I could not get the fecal transplant in the NHS but had a noticeable difference to the ME for several months just on the narrow band antibiotic for eradicating c-diff. So I think I would be a good candidate for FMT. It wasn’t a cure, but was so much better for about 4-5 months. I think if there is an overgrowth of bad bacteria it needs the antibiotics 1st then followed up with FMT. I’ve not found oral probiotic supplements, kefir and changes in diet and prebiotics are not enough. Though I’ve had an upswing recently from lactoferrin, Which someone mentioned had also settled a lot of gut issues in them. I think you are right it needs much higher dosing and changes in diet to support and pre-treatment of antibiotics to really shift things enough that it helps the ME.
From my investigations into gut dysfunction a couple decades back, here are a few points of note pertinent to this subject that I hope I remember correctly; “It is exceedingly difficult to permanently change the colonized resident bacteria of the gut”. The appendix acts as “back-up storage” of the resident bacteria – to repopulate the gut if an infection (or abx, or anything else) changes it. For these reasons, an antibiotic sterilization of the gut before a fecal transplant may be more effective, but still may not result in permanent changes. Some fecal donors tend to have more successful transplants than others. Docs who specialize in FMT’s may depend on select donors (and have greater success). The optimum gut biome likely differs somewhat between individuals (just like genetics). Science is far from fully understanding “gut microbial balance”(for optimum health), as there are still many gut microbes that we don’t even have names for yet (let alone understanding their role in a healthy gut). This makes commercial probiotics that supplement only a few known microbes have little chance of success in rebalancing the microbiome (in most people). However, fecal transplants from healthy people would transport an entire microbiome – even if we don’t know the names of all of the microbes or what constitutes microbial balance. Thus, I think this is an interesting field with promise and I applaud every new research insight. (Thx again Cort!)
Thanks Dave. I wonder if researchers should pay more attention to doctors who specialize in doing these such as the Tatamount clinic which has apparently found that doing more of them – many more – works best.
There’s also the issue – since the flora in small intestine is so different – if the wrong flora is being added. I wonder if there’s a way to bring that flora in.
Hi Cort. TY for your reply. I suspect that microbes targeting the small intestine could be administered in (acid resistant) capsules that do not dissolve until after they have entered the (high alkaline) small intestine. Whereas, microbes targeting the colon could be administered by enema.
My take: I think that a useful analogy to understand the health of our gut biome – is the ecology of prairie wool (wild prairie growth). It is a mixture of thousands of different plants (each playing a different role by taking out and giving back different essential nutrients to the soil). No one plant (or “weed”) can completely take over (to undermine the healthy balance) because the density and diversity of all of the other plants keeps the populations of all plants in check (and in balance). A healthy gut works similarly, and has a great diversity of microbes – all competing for food, space or a niche – and keeping each other in check (or in balance) by “crowding out” new pathogenic microbes and over-populations. (In fact, microbes in healthy soil may reflect an altered version of microbes in the gut, and the soil is likely the original evolutionary source of our gut microbes).
A great diversity of microbes in a gut requires a great diversity of foods to support them (which is how our ancestors supported a healthy gut). Thus, a good diet might help sustain a healthy (diverse and vibrant) microbial balance. However, getting new (previously foreign) microbes to colonize the gut walls (and become permanent residents) may be exceedingly difficult, as our immune system may perceive them as a threat and be “less than friendly or welcoming”. (In our first few months of life, our immune system is open to new microbes – as babies are born with sterilized guts – but after this window closes, the immune system in the gut wall may perceive any new microbes as “foreign” or “not us”. However, beneficial microbes that are just “passing thru” may persist for a time and have significant benefits. This might explain the need and benefit of repeated transplants. (Most of this is from a 10+ year old book that connects the health of the gut to the functioning of the brain (and the proper functioning of most body systems), called; “Gut and Psychology Syndrome” – Dr Natasha Campbell-McBride). I hope this long post might be of interest to some folks.
>Fecal transplants have nothing, though, on dramatic attempts to redo the gut in ME/CFS that are going on in the Remission Biome group, which is now attempting to put 50 people with ME/CFS on its gut protocol.
This sounds like it’s claiming that the Remission Biome protocol is more promising/dramatic, better, more complete, etc., than FMT. In my opinion, that would be pretty severe misinformation.
The key to the gut microbiome is restoring an extremely complex ecosystem. You certainly cannot do that with antibiotics. Nor can you do it with probiotics, fermented foods (https://humanmicrobiome.info/probiotic-guide), or any other currently-available supplementation. They’re all a drop in the ocean compared to FMT.
Antibiotics are not proven to be beneficial prior to FMT, and even FMT may not be able to reverse all the damage that antibiotics do: https://humanmicrobiome.info/fmt/#before-the-procedure. Antibiotics generally have short-term benefits and long-term detriments, and are often only beneficial for as long as you’re taking them. One mechanism is likely that they’re now having to do the job of the microbes they killed off.
If you’re thinking “similar could be said for FMT”, it’s certainly not simple to restore a complex ecosystem, and we definitely shouldn’t expect that a short-term period of FMTs, usually from very non-ideal donors, can completely restore your gut microbiome.
Donor quality is by far the most important consideration for FMT, and it’s mostly been bizarrely ignored: https://forum.humanmicrobiome.info/threads/donor-quality-and-stool-type-hypothesis-for-fmt-fecal-microbiota-trans.142/
You can see in the last link that I’ve been trying to get the donor-quality issue addressed for the past decade with little success. Thus, I’ve taken things into my own hands with humanmicrobes.org and am screening hundreds of thousands of people to try to find “super-donors”. I think it’s quite strange that antibiotic & supplement-based protocols are still being touted as more promising.
The Dove Clinic study you mentioned serves as a good example. They use Taymount’s donors, which are notoriously deficient: https://humanmicrobiome.info/where-to-get-fmt/#taymount-clinic
I pay 10x more to donors than other establishments because I want to attract the best donors. This has been effective, and virtually every donor that has been covered in the news, and every clinic’s, stool bank’s, company’s, etc., donors have applied to HMorg. The vast majority of them do not come close to qualifying.
Thanks for all the information! Yes, that was a bit of an exaggeration. Without checking I thought they were including FMT but I see they are not and will change the text. I do think Remmission is more dramatic 🙂 three-day course of Amoxiclav and a one-month course of Doxycycline taken concurrently, followed by an additional month of Minocycline, a ketosis diet, supplements and finally specialized probiotics – but I agree that the antibiotic regimen has not been proven and I remember one study which it concluded it was not helpful.
The donor issue is fascinating. Thanks for your input.
Harrop is actually correct in this regard. I have now met several donors who actually donate to stool banks and drug companies. One has type 6 stool. Another has a history of depression and PCOS.
Hopeful news for post-covid patients. Scientists at Amsterdam UMC think they have found the cause of the long-term complaints that some people are left with from a corona infection. In a laboratory, it has been possible to combat the enzyme, the possible culprit, with an experimental cancer drug.
Until now, the cause has been a mystery. But scientists at the Amsterdam UMC think they have found the culprit. “We have discovered the substance IDO-2,” says physician-researcher Brent Appelman. “That is an enzyme that causes the cells of people with post-covid to break down, and the energy factories do not work properly.”
https://www.msn.com/nl-nl/nieuws/Binnenland/kankermedicijn-hoopvol-voor-post-covidpati%C3%ABnt-grootste-doorbraak-tot-nu-toe/ar-AA1f8PEK?ocid=msedgdhp&pc=U531&cvid=1d508b385d3c4446815de6c8b29d3eb9&ei=60
That is related to the same kynurene – tryptophan pathway that is messed up in ME/CFS and is a consequence of a faulty microbiome
Very interesting. Anything in English anywhere?
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7066259/
https://www.cell.com/trends/pharmacological-sciences/fulltext/S0165-6147(23)00089-5
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7710763/
there are many articles that are all over my head
DON’T GIVE UP ON POOP!
– only some get permanent engraftment from a few FMT’s.
– many have to do it for months or even years.
– most can taper off at some point but may still need boosters from time to time
– many are living normal lives from poop.
– You can tell literally nothing from 1 or 2 FMT’s
– Some have to go through many donors to find one that helps them.
Hi Sue,
How to you establish criteria for donors? I’m thinking I want healthy infant poop?
Then how do you find the donors?
And finally, where do you get the transplant? Who is doing them, and where, and how many times?
Thanks!
You can:
– order online (expensive but good), find your own donor (own child, sibling or spouse, if healthy, is good), or travel to clinics outside north america
– you can find donors through friends, family, or posting ads online in various groups, or around town – perhaps at healthfood stores, gyms,college campuses,etc.
– if you find your own donor, you would arrange for testing, process the poop yourself and give yourself the transplants. You could either take capsules or do enemas. Some even drink the poop straight.
-Join the FMT facebook groups to learn more
Thank you for all the information. I had no idea it had become so do-able!
Was this a full colonoscopy, with bowel prep? I don’t think anyone would want one of those every day for ten days!
Being a bit facetious, but it seems like the Finnish study didn’t try hard enough to get the transplants to take, and this part of the method limited that.