


With several technological hurdles behind them, Ron Davis’s team at the ME/CFS Collaborative Research Center at Stanford is ready to get back to full-time lab work….when Stanford University allows them.
Ron Davis’s Stanford ME/CFS Collaborative Research Center is itching to get back to full-time lab work. It’s not that Davis and his group haven’t been working. Janet Dafoe described constant Zoom calls with ME/CFS researchers, a bevy of grant applications have been completed, put some researchers – with proper social distancing – are back in the lab. The lab, though, is on the cusp of getting some long sought work done. The groundwork – some of it years in the making – has been laid for a major step forward in several areas.
The problem has been technological in nature – which is not a bad thing, as developing new technologies has kind of been Davis’s forte. The mission of his Stanford Genome Technology Center, after all, is to “develop new technologies to address important biological questions that otherwise would not be feasible”.
Davis has won numerous prizes for his work over the years, and was called one of nine top inventors that history will remember in the areas of technology, science, medicine, etc. One colleague reported that “A substantial number of the major genetic advances of the past 20 years can be traced back to Davis in some way.”
Davis’s motto seems to be: “if we don’t have the technology – we’ll just create it.”
New Nanoneedle
The really big news is a new nanoneedle. The nanoneedle was originally designed as an “ultra-sensitive, real time” biosensor designed to cheaply detect biomarkers such as proteins inside (or outside) cells at a far more sensitive level than had ever been done before.
It was then reconfigured for ME/CFS as a kind of diagnostic, drug screening and biological testing tool. That was a bit of an overwhelming load for a tool that was still being perfected. The nanoneedle’s inability to keep up with the demand meant that its full potential wasn’t nearly being reached. A dramatic upgrade was needed.
That has happened. The nanoneedle has been redesigned and sent to a manufacturer in China and one in the US to produce. Where it could test one sample and one control at a time, it can now test 100. That kind of production is essential for the nanoneedle to be able to test the wide variety of drugs Davis wants to test, and to run the multiple samples needed to try to uncover the mystery element that seems to be bollixing things up in the blood of ME/CFS patients.
Davis is waiting for the return of the new nanoneedle – and the ability to test patient samples again. Unfortunately, production has been halted due to the pandemic. Only recently, has the Chinese company that could make been reopened, but there is no set delivery date. Still, it’s on its way.
New Machine

A new “toy” will allow researchers to better understand if people with ME/CFS have gotten trapped by their own metabolism (Image by Public DomainPicturesfrom Pixabay.jpg)
Robert Phair’s Metabolic Trap hypothesis introduced numerous technological challenges, some of which have recently been resolved with the purchase of a high-pressure liquid chromatography (HPLC) instrument. Davis is confident they will make good progress assessing the hypothesis once they can start testing patient samples again. Several years after the Phair hypothesis was introduced, Davis remains hopeful that the hypothesis could explain much about ME/CFS.
New Technology
Peidong Shen, at the Stanford Genome lab, has developed a fast, inexpensive, breakthrough technology, called “multiplex targeted sequencing” that can simultaneously target and sequence small sections of DNA from any source. Targeted multiplex sequencing allows researchers to look for mutations in individual genes or the presence of a large variety of organisms that could be present.
With regards to ME/CFS, this new technique allows Stanford researchers to assess the presence of RNA viruses, such as enteroviruses. These viruses are tricky to measure because RNA gets rapidly degraded in the blood, but are responsible for several diseases such as Ebola: polio; hand, foot and mouth disease; as well as the common cold.
Enteroviruses actually have a long history in ME/CFS. Enteroviruses were amongst the first viruses thought to be associated with ME/CFS. More recently, Dr. John Chia has found enteroviruses in gut samples of ME/CFS patients and believes they may play a key role in this disease. In what Davis called a “very difficult” project, Davis’s Stanford lab is now able to simultaneously look for 17 RNA viruses in ME/CFS samples.
Davis doesn’t suspect that RNA viruses are going to pop up in high numbers in ME/CFS patients, but RNA viruses are another possibility that must be investigated, and now they will be – once they can start testing patients again. (Shen has also created a fast and cheap COVID-19 test that takes 40 minutes to process and can be used in the lab to allow them to go back to work safely.)
New Thrust
A new research thrust has emerged, courtesy of Chris Armstrong, PhD – an Australian researcher who’s been working with the Open Medicine Foundation (OMF) over the past year. Several years ago, Armstrong said he was “looking for Waldo” but wouldn’t say what Waldo was. All we knew was that something was not adding up for him in the metabolite results. That something was apparently nitrogen.
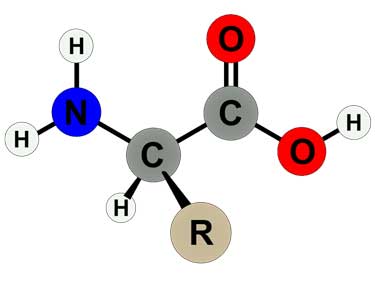
Amino acid structure -could the nitrogen that’s released from the breakdown of amino acids – be showing up in ME/CFS patients cells as ammonia?
Metabolomic studies suggested that people with ME/CFS were using amino acids for fuel at a faster rate than healthy controls. That was odd – as amino acids are usually used for fuel at an elevated rate during a stress response or starvation. When you’re starving, for instance, your body will save your carbohydrates for the brain and immune system, the rest of the body will go after your fats, and only then does it begin to break down your muscles and connective tissues.
Carbohydrates and fats are made of carbon, hydrogen and oxygen, during energy production they combine with oxygen you breath to become carbon dioxide (1 carbon and 2 oxygens) and water (2 hydrogens and 1 oxygen). Amino acids can provide fuel also as they are made of carbon, hydrogen and oxygen, but doing so introduces a problem because amino acids are also made of nitrogen atoms. Because the nitrogen is not burned, it has to be eliminated – and is usually eliminated as urea.
The metabolomic studies suggest, though, that the nitrogen elimination system in ME/CFS is being overwhelmed – leaving the nitrogen to be eliminated in the form of ammonia (!) (which contains nitrogen) or nitric oxide/peroxynitrite – both of which can be highly toxic. Armstrong suspects these nitrogen byproducts of energy production could be interfering with the energy production process itself in ME/CFS. That – a situation where energy production produces something that wallops the energy production process – is, of course, the very definition of post-exertional-malaise (PEM). (By the way, if this is happening removing amino acids is not the way to go.)
Armstrong recently received a donation to assess over 10,000 molecules in biofluids and cells to track nitrogen flows through the energy production system in people with ME/CFS and healthy controls. Health Rising will devote a full blog to this hypothesis in the future.
New Problem – the Coronavirus
The Stanford ME/CFS Research Center has a lot of possibilities to explore, but the big hold-up right now is the ability to test patients. Stanford will not give Davis permission to bring patients into the lab. He tried to set something set up in the parking lot that would minimize contact, but Stanford wouldn’t go for it because they might accidentally drip blood on the asphalt! (Yes, Stanford is very conservative. There is no telling when Stanford will allow patients back in, but it will likely be some time.
Lastly, while COVID-19 has shut down much of the lab work, it has had one significant silver lining – more time to write grants, papers and analyze the multitudes of existing data. Davis’s group applied for six Congressionally Directed Research Programs (CDMRP) grants – four of which made it through the first hurdle and are moving forward.
Zoom-Zoom: New Working Group Meeting Brings in New Faces
Ron Davis organized and conducted his 4th Annual ME/CFS Working Group Meeting on the Molecular Basis of ME/CFS, this time over Zoom. The Zoom format stopped researchers from gathering in person but it also allowed Davis to greatly expand the number of researchers attending the meeting. One hundred and fifteen ME/CFS researchers “sat in” four days of talks by presenting unpublished and preliminary results. (That was an impressive number. I didn’t know we had that many researchers!). Janet Dafoe reported there was much interchange, and a focus on diagnosis, treatment, prevention and a cure.
Besides members of the Open Medicine Foundation funded research centers at Stanford, Harvard, Uppsala and Montreal, and past members of the Working Group (Neil McGregor, Mark Davis, Peidong Chen, Robert Phair, Wenzhong Xiao, Chris Armstrong, Lucinda Bateman), Davis brought in outside researchers to present.
Nancy Klimas at the Institute for Neuroimmune Medicine (INIM), Bhupresh Prusty of the Institute for Virology and Immunobiology in Germany (now working with Bob Naviaux), and Vicky Whittemore of the NIH all presented.
Plus, some newer faces gave talks. Dawei Li received a Solve ME/CFS Initiative Ramsay Award to search for genome-wide endogenous retroviruses (ERVs). Andrew Grissom, geneticist on Maureen Hanson’s team and Arnaud Germain, another Cornell researcher on Hanson’s team (who recently published a metabolomics study on ME/CFS), talked. Two-minute lightning talks were given by the developer of the nanoneedle, Rahim, Alan and Kathleen Light, Dr. Seline (T-Cells) and others.
Conclusion

Unfortunately you can’t predict breakthroughs. We don’t know what these initiatives will produce – we never do – but the ability to move forward more quickly on them is good news indeed. Davis remains convinced that a cure is possible.
Your Support Keeps Health Rising on the Web


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



Hopeful developments. Thanks Cort.
If this is Chris Armstrong (as in the article), I would like to contact you with information that supports your nitrogen/ammonia hypothesis.
Please email me if you are
Thanks
I am so grateful for the amazing people that have been able to investigate this issue. Thank you Ron Davis, I too have a sick son and knowing your working with your all helps us hang on! Susan Maik
Thank you very much Cort for researching, talking to all these people and translating their work to us! Is always a pleasure finding your newsletter in my emails. It gives me hope.
Marika from Germany
Love your work cort.
Is there something you’re not telling us?
This seems like we are still deep in research.
Hope I’m wrong tho.
No negativity here, just trying to manage expectations
Still deep in research but there are more promising possibilities than I can remember.
Thank you for the reply
Thanks for this, Cort. It’s so nice to have some encouraging news in the midst of this 2020 nightmare!
This is good news! I had not thought how Ron Davis and the Stanford team were surviving through this pandemic time. It is good to know that the device that was one-sample- at- a-time and relatively slow going, has a chance of going into production, with the improvements made to it for greater usage. I hope Stanford sees its way clear to let patients in soon. That area of California has so many issues right now, between wildfires and the spreading coronavirus.
“Because the nitrogen is not burned, it has to be eliminated – and is usually eliminated as urea”.
This explains why Citrulline Matate (up to 8 grams across a day) can help:
Because it stimulates the urea cycle.
But wouldn’t citrulline malate up arginine in the system, causing further problems? Isn’t arginine contraindicated for ME/CFS?
Please see my comment at the end of this thread, re: my being prescribed the supplement L-Ornithine for elevated ammonia.
May I ask how you learned arginine is (or may be) contraindicated for ME/CFS? Your source for this may be important to share with my doctor. Thank you.
It doesn’t UP arginine. It stimulates the urea cycle, to clear out ammonia.
You are right that arginine is not suitable for people with ongoing herpes / Epstein Barr issues though.
In the sports world, smelling amonia is known to be from catabolism. The solution: up your carbs.
This worked for me.
Ultimately it was thyroid that got rid of it: you need ATP to form urea from ammonia. I had low urea for many years too. That in itself is another problem, affects the folding of proteins. Not for nothing urine therapy is a thing in some cultures.
Stimulating the urea cycle sounds like a not so good a idea if you don’t make enough ATP to begin with…
Great Article 🙂 Thanks! So interesting. Do you think videos of the working group will come out soon?
The Working Sessions have historically been private but I was told that some video’s of some of the working sessions may be available at some point.
The Hansa Center uses neutraceuticals to eliminate ammonia. Lyme disease causes a lot of ammonia toxicity and before they treat for lyme and co infections they eliminate ammonia. Otherwise treatment is rough and less effective, I believe I recall from years ago. Here is an article.
http://davidjernigan.blogspot.com/2018/05/addressing-ammonia-toxicity-lyme.html
It’s good to hear there are options. I imagine that it’s probably best to wait and see what Chris Armstrong’s study finds. A blog that digs deeper into what Chris has found is coming.
Thanks Cort, great summation and excellent news all around! I wonder why they need patients to physically come to the lab vs accessing patient samples through bio banks and other means? Was there any info on this?
Leslie, some of the tests are done using fresh blood so they have patients and controls come in at about the same time to give blood and then run those tests the same day. They also preserve some in the usual manner for other tests run later. I’m sure they will be doing what they can with the lab samples they have but they’ll need to be able to bring in patients to move forward on some of these projects.
I believe that Kirsten is right. They do have frozen samples they can run and Ron told me they set up a protected and safe place to do that. I believe only one person is allowing in that room 🙂
Makes sense, thanks Kristen and Cort
This is timely.
My daughter has very low amino acid levels.
I was about to look at supplementing them as I had read that low BCAA are also related to low iron. (Another major issue for her).
At the same time she has/had high ammonia and urea. (Not tested for some time).
Now I am not sure that providing more substate for the production of ammonia and urea is such a great idea!
Where does one start…
Iron supplementation has failed to work over a prolonged period of various forms of iron.
Every time I feel we find something that may help her…there are always so many twists in the tail!
BCAAs made me really sick. This line of research is really interesting to me. I have a genetic weakness though in mitochondria that makes me go hypoglycemic if I eat too much protein. It wasn’t a problem until I got ME/CFS too. Could eat a chicken leg before. Now can only eat three nuts in a meal. So it might just be me. I guess I would say proceed with caution if you try it. Start with very small amounts.
Thanks for that info Chris. Sorry BCAA did not help you and we will commence cautiously.
P.s. thanks Cort for the easy to understand information!
🙂
The OMF should consider if Stanford won’t let them have patients at the university, then why not get researchers like Professor Warren Tait at Otago University in New Zealand (which has no Covid 19 in the South Island and only a controlled small cluster in the North island) to do the patient testing here in New Zealand.
There’s plenty of high quality Universities in New Zealand all Covid free, and plenty of ME/CFS patients eager to help too.
New Zealand has all but eliminated Covid for the second time due to an incredibly proactive government that learn and adapt to the changing information on the pandemic.
We don’t even have to wear masks anymore and are allowed in cafes and bars as it’s so safe here. So is safe for ongoing research too!
Totally agree, NZ has had CFS outbreaks via tapanui, makes sense to test here, I’m a willing subjevt
Kind of looking like this upcoming Kynurenine trial is nothing more than a shot in the dark… It’s definitely getting annoying that Ron keeps pumping all these ideas while having little to no merit to them.
But Susan, isn’t that what exploration is all about – venturing into previously uncharted territory and mapping it?
If something is unprecedented, then nothing like it has come before to compare it to.
Yeah this article is full of mostly worthless info. I mean, what use could the nano needle possibly be? Testing numerous drugs for their potential to reduce the overreacting cells in PWMEs plasma couldn’t possibly lead to any valuable data. No, not at all…..
Well my understanding is that there are currently no biomarkers for ME/CFS, so if the nanoneedle can pick up information, previously unavailable that may then, I hope, lead to more precise, informed treatments.
I have no diagnosis of ME/CFS and that leaves me open to criticism, dismissal and zero support from the medical profession. ME/CFS needs to be regarded as the potentially debilitating condition it is, within the general medical community.
It would make a huge difference to my life, if ME/CFS was accepted as a legitimate illness, that required expert management and hopefully treatment. My life and expectations have undergone a massive change, since becoming unwell. However I think other’s perception of me is that I’m just not very motivated or competent and probably a bit lazy and a bit depressed. Nothing that couldn’t be sorted with a bit of energy, commitment and focus. Get out there and you’ll feel better, kind of approach…
When I’m feeling good I even question myself and think there’s nothing really wrong with me. But my whole life has had to be adjusted to create this better health, I can thankfully experience.
However, if I think to myself – could I just live completely freely and energetically? The answer is – No. Despite everything I do and don’t do, there still seems to be some system – something my body/brain/mind may be controlling that is debilitating and I don’t know what that is.
So, if Ron Davis’s Nanoneedle helps in the future to figure that out for me, or others who are younger than me, then I would be delighted.
One of the intriguing things about the nanoneedle is the possibility that it could provide a cheap, easy diagnostic test. There’s a long way to go before that happens – we need a lot more samples run – and other diseases need to be assessed – and it would be really good (altho I don’t know if its necessary) to understand exactly what the nanoneedle is measuring but that’s quite a possibility.
I, like everyone, wish everything would move faster but there is only so much funding. Let’s hope and work towards HR 7057 passing, let’s hope that if it does, that funding goes up and they add another research center. A Stanford one would be a nice option.
Cort feel free delete my previous post if you like/can. Pretty sarcastic response to a bit of understandable negativity. I know I get sure impatient sometimes so I shouldn’t be a smarty pants to someone expressing this.
FWIW I think the nano needle is conceptually awesome and I believe that once they get it up and running it will yield some very useful data. Even if we don’t get a treatment drug a a result, it should at least highlight some pathways and mechanisms that are ripe for investigation.
Susan, of course you’re free to share your perspective and I apologise for being a sarcastic douchebag.
Tracey Ann…don’t doubt yourself. Many have the same thoughts…if you feel slightly better on a day you begin to think…oh, I just made it all up!
Thanks LindaB, part of me can give myself quite a hard time sometimes until another part kicks in and says – No, I’m doing my best and actually managing pretty well considering…
ManShadow your second comment just makes me laugh every time I read it. And I agree with you that Susan is free to express her view too.
I have been mulling over how I will be, if I ever get to see a doctor about my possible diagnosis of ME/CFS.
It’s likely that I could end up seeing a young junior doctor, recently qualified, doing their six month stint (they change over in July and January – I’ve met them!) in (?) department.
They will probably think they’re seeing a nice, healthy looking middle aged lady, who’s feeling a bit tired and I, on the other hand (having endured years of minimising my experience) will be doing my best not to verbally eviscerate them…
I do feel very, very angry at times. But it burns up energy at an alarming rate, especially if I have no outlet!
I have another long term dispute going on with my training college (13 years) because they were practicing in a way that was extremely unethical but they say the problem is all in my head, as no one else has said they had an issue. I think the stress, at the time and subsequently, propelled me forward on a trajectory, I was possibly already on. They just made things so much worse.
Over the years I’ve had to adjust my outlook, from one of an aspiring counsellor/psychotherapist, to an ex counsellor/psychotherapist, who’s just trying to survive. I currently work part time as a home caregiver, which I generally really enjoy but I have to use all my resources just to be able to get through each morning.
Some people think care workers are obviously of a lower order of humankind but I know what we do – and many home caregivers are very decent, sensible, resourceful people.
I believe everyone with this illness has their own story and experience. For the most part I don’t really care what others think of me – my life is so far removed from anything they could envisage, their opinion doesn’t matter.
But sometimes, the whole lot piles down on top of me and I get deluged with negativity, fury, hopelessness and despair. But I have a 17 year old son and a 16 year old dog and home care clients. And yes, I know, I’m lucky I’m able to do all the things I’m able to do, so I shouldn’t whinge.
Linda B, exactly how I feel. A good day, thinking, this is great, I’m getting a handle on this. PEM kicks in, don’t sleep, feel absolutely horrendous. Two days plus to recover – it used to be weeks or longer, and still is for many, so how lucky am I – and the whole cycle starts again. This has been going on for over 15 years. Thank you Cort for all the positive news you bring us, it is what I hang on to these days.
We never know how this is all going to turn out. The Metabolic Trap hypothesis could turn out to be right or wrong. Even if its wrong that wouldn’t mean that it wasn’t a good idea – and worthy of an effort to validate it or not. For me I’m pretty happy to let Ron Davis and colleagues determine the merit of the efforts they are undergoing. Ron and his colleagues have proven themselves at the highest levels of science for many years. That’s good enough for me.
If ME/CFS was easy it would have been solved. It’s a very complex problem and while I hope for a solution soon I don’t expect any research group to come up with the answer tomorrow. (I must say, stayed tuned for an interesting blog!). Instead my best hope is for a methodical attempt by enough skilled researchers to chase down the false leads and eventually alight on the right ones. Give them enough time and I’m confident they will unpeel the onion that is ME/CFS.
Hi Cort
Do you think these kind of treatment such as Abilify could work for fibromyalgia too? I have severe fibromyalgia and it’s getting worse. I am desperately looking for a new treatment. I’ve tried pretty much every thing pain clinics can offer.
That last sentence, that Ron remains confident that a cure is possible, is what keeps me from despair. Thank you Cort. Thank you Ron and your team, and all the researchers who are putting in superhuman effort into finding a cause, a treatment and a cure. Millions of people around the world, including my son, are living in hope thanks to you.
Referring to the international consensus criteria, couldn’t a quantitative biomarker with good sensitivity and specificity for me/cfs be a tilt table test with extracranial doppler extracranico (to detect dysautonomia always present in cfs + cpet in 2 days (to exclude other pathologies with dysautonomia)?
Fatigue and unrefreshing sleep are less measurable, but not strictly needed I believe.
I hope someone will pick this idea up, it would make the diagnosis much easier, undisputable and hopefully get more attention to this devastating disease
That makes sense to me. The other forms of dysautonomia do have reduced blood flows to the brain but there is this ME/CFS group that only has reduced blood flows.
Anyone interested in diving in to kynurenine?
many mini articles at:
https://www.sciencedirect.com/topics/neuroscience/kynurenine
mentions…..
……. glutamate…..ROS……..tryptophan………..serotonin..
……….neuro / inflammation……..IDO……T-cells………COX-1…
…..COX-2…..ketamine………..galantamine
I’ve been hearing the same information for years, things are not moving. We can not wait for government money the ME organizations needs to focus on philanthropist (ideally woman) … this is the perfect time to get attentions from them ascurrently attention if being shead on ME/CFS with Covid long haulers. This is very much a sexist issue here and must be presented that way, we cannot be scare to say the truth ,,,, because it is and it will continue until we ask it stops. That is the marketing approach here enough is enough. We are dismisssed and made to feel like you we faking, it’ not real or a mental illness … this by everyone, familly, friend and doctor. So we suffer in silence. I see the key as Philanthropist, they people want to make a real difference, as many ME/CFS research project our clearly outline and started this allow quick result to their Investiment. What is that person investment was responsible to finally confirming the illness with a test. We have never been as well position to get investiment so really hoping not all the eggs are in the NIH basket. There needs to be a marketing effort toward philanthropist.
The key is trying to determine what organ, what system, what part of the body is causing the exertion intolerance. Only then, can one move forward much faster. This is the core symptom of this illness. Yes, the other symptoms are debilitating, but what is causing the body to go into PEM? What is it? This is the most bizarre of all the symptoms, and the most difficult to describe, and often the one easily dismissed by doctors who think it may be just fatigue. A huge huge thank you to our dear Cort for putting out all this info.
I have a special connection to Ron Davis’s lab because I was able to travel there (paying for my own expenses) in October of 2018 to donate blood for their research. The staff there were wonderful, and it was an amazing trip, during which I also had the opportunity to tour the Big Basin Redwood park and stick my feet in the Pacific Ocean. Of course, it took me three weeks to recover from the three-day trip, but I fully expected that. I am very grateful for their research and impressed with their progress.
Can’t help groaning, though, about Stanford’s refusal to let Davis’s team draw blood in the parking lot. They might drip blood on the asphalt? Seriously? That is so easily prevented: plastic tarps could be laid on the ground. Absorbent pads could be placed under the arm of the patient whose blood is being drawn. And the whole area could be hosed down frequently with sanitizing spray. I understand the importance of caution, but this is ridiculous.
Nevertheless, knowing how dedicated Ron Davis and his team are, they will persist, and they remain one of my greatest hopes for real answers to this disease, partly because they work in cooperation with other researchers. I was happy to hear that Dr. Nancy Klimas was included in this year’s zoom conference. I sent blood to her lab 20 years ago, and I remain one of her biggest fans.
It was great to see Nancy in there, I agree!
Hi Cort,
Sadly I was not invited once again to this meeting as a spectator. This remains very frustrating when this could easily have been arranged without cost.
Secondly, Chris Armstrong’s idea is thanks to 30 years of this very type of work by Neil McGregor, where this issue with Amino Acids has been the focus of the Newcastle/Melbourne group and has been studied for ever. It is one of the KEY unexplained phenomena that is essential to understanding MECFS metabolic energy issues.
This is of course NOT the only problem and new developments at the clinical level suggest that the progression from orthostatic intolerance to POTS MUST involve some weakness in myocardial function.
Sorry to hear that John. You always have really interesting takes on this disease. I think you should write a book actually. It would be helpful and fascinating.
I totally sympathize for everyone who knows they have ME/CFS symptoms but has not gotten an ‘official diagnosis.’ I have long known that I fit the Ehlers-Danlos criteria, but it was a lengthy campaign to get it recognized and recorded by the appropriate doctor (geneticist). I fear that if a Dx isn’t listed on one’s chart, for many in the medical field, it simply doesn’t exist. I had similar problems with getting assessed for ME/CFS (which Stanford calls SEID).
But there it sits on my chart, yet there has been little help. Stanford’s perception of ME/CFS, it seems to me, is seen mostly through the lens of a virus and neuroinflammation. Their official treatment protocol has been quite limited. Since fatigue is manifest in so many disorders, ME/CFS is bound to have multiple sub-sets and or underlying mechanisms, yet they seem focused on only a few.
I am also frustrated that the director of their Chronic Fatigue Clinic seemed to not know who Ron Davis was!
On the other hand I do have some sympathy for the Clinic as they are tasked with treating patients when they have no effective therapies.
I notice, in myself, that when I have several days of ZERO activity, I experience a near normal bounce of energy, and occasionally I even have a super abundance of energy. Then with what I think of as doing the normal activities of life, with no over exertion, I have episodes of PEM, which sacks my energy and motivation. I have no idea why, except the association of a necessary zero activity ‘recharging period’ to garner additional energy. I struggle with pacing too, as there doesn’t seem to be a direct relationship with my perception of energy expended and crashes. This ‘recharging period’ seems to indicate that something in my body needs to be replenished–so what could that be?
Maybe I’m different from others, but that’s how I roll.
Sorry for the meandering thoughts, but I feel the frustration. Also the thought about Cort’s blog for making hydrogen water crossed my mind. I wonder if that could help? If there was only enough money for more studies…
I roll exactly the same Nancy. I often feel like something essential is missing and if I overdo things it takes days or weeks of doing little or nothing to replenish the stores. Then I feel comfortable again as long as I stay within my reduced limits. I too find pacing an ongoing challenge. I was interested to see nitrogen pop up again. I sometimes wonder if this illness should be called chronic poisoning rather than chronic fatigue. For me, nothing can stop a full blown crash in its tracks but b12 combined with an electrolyte solution sure helps take the edge off. B12 is a nitric oxide scavenger and that might be relevant. I also have funky things going on in my urea, methylation and trans-sulfuration cycles, including unusually low GGT which is just weird in an illness associated with high oxidative and nitrosative stress. Nitric oxide impacts vascular tone, heart rate and glutamate release in the brain and I think it is a player in this illness.
I agree with you, Nancy and debsw. Now that I’ve calmed my stress response, am getting much better sleep and have kind of sorted what I’m eating I’m left with a few things: my brain is very easily irritated or runs out of energy by what I eat or don’t eat – so I constantly have to monitor that situation.
I would think I have mast cell issues and certain foods/medications upset the rhythm of my heart, which is really not good. I was experiencing light headedness, nausea etc but that’s stopped, since I started eating the choc chip cookies. So, the other issue I have to deal with is the energy depletion. This morning, Sunday, I feel good but last Sunday morning I felt wrecked and had to have a sleep for a few hours and then I felt physically better but I also felt very annoyed that my one day off was now rapidly disappearing.
The difference was probably due to my hours worked being a bit less, this last week, due to a family member of one of my homecare clients, waiting for Covid-19 test results.
I get what you mean with the ‘chronic poisoning’. Over the years, that’s just how I felt. I think I was fine as a child but had mono/glandular fever when I was 17 and I think that may have changed something in me. I don’t see much mention of the liver and it’s role anywhere but I believe the Epstein Barr virus can affect the liver. I believe our body’s systems are very intricate and all highly interdependent and I feel that when I’m not functioning efficiently then all sorts of stuff may be building up and not getting processed.
In particular, I seem to have a difficulty if I have too much fructose in my diet and that is processed by the liver. I think when I ate more fructose than my liver could process, it then possibly had an impact on my liver to process anything else efficiently. Anyway just a thought.
I would have the same experience with the energy usage. Yesterday I was thinking that it’s a bit like driving a car when the fuel gauge is faulty. We’re just not sure when we’re going to hit the red zone or simply run out.
And I have also been trying to differentiate between feeling tired and having no energy because, for me, there is a difference. Being tired is a familiar and understandable feeling after exertion, or after a long day. Thinking about it, the only times I have previously felt no energy, is when I’ve been unwell and have the flu. In that context, only just making it to the bathroom/toilet and back to bed, to collapse in a miserable heap is not something I liked but it did make sense. I wouldn’t question it, I’d just endure it.
So, maybe feeling that energy depletion out of it’s normal context is difficult to gauge because we wouldn’t normally have to – we’d just accept it and have to rest.
Having said that, isn’t the modern culture all about suppressing the symptoms, so we can ignore them and get back to work/school/college/children etc?
Sorry to hear that John. You always have really interesting takes on this disease. I think you should write a book actually. It would be helpful and fascinating.
Thanks Cort for your support and suggestions. A book is an idea, but it requires a University position to be taken seriously and why would my ideas have any greater worth than those of any other wannabe scientists? Any suggestions there would be very greatly appreciated. To be invited to participate in say the recent symposium helps with the kind of situation and there is currently very few clinicians of my caliber is such forums. This is not a complaint. It’s just an observation.
Metabalomic studies certainly present significant findings, indicating that “all is not right” with ME/CFS, but unreliable (results too variable) as a diagnostic biomarker (blood signature) for ME/CFS ti would seem… and as would seem to be the case with ‘blood biomarkers’ throughout ME/CFS history. Why? Because ME/CFS is a neurological (neuroinflammatory) disease – a disease primarily of the brain and CNS. Finding a blood biomarker for ME/CFS is akin to challenge of finding a blood biomarker for a migraine, or epilepsy or a mental disorder. Metabolic changes are therefore an “effect” of ME/CFS, not a “cause”… Dr Ron Tomkins, another neuroinflammatory proponent, aptly described the blood as being “like a sewer”. I think the changes we see in the blood are “downstream” of an inflamed brain (hypothalamus key as affects ANS/ HPA-axis). RonDavis is clealy a brilliant scientist and his highly sensitive “nanoneedle” might hopefully detect small changes in the blood of ME/CFS patients compared to healthy controls, and maybe even be develped into a much needed “blood-test” – great – but I think the root cause of ME/CFS lies within the brain:
A neuro-inflammatory model can explain the onset, symptoms and flare-ups of
myalgic encephalomyelitis/chronic fatigue syndrome (2019) https://www.publish.csiro.au/hc/pdf/HC19041
cheers
Angus
The problem with metabolic anomaly as the cause of CFS is that moderate/mild patients don’t have problem generating enough energy. It’s just that, if they do, they get into PEM state in the next day or two and become sick for days or weeks.
If the metabolic anomaly is simply a part of PEM sickness behavior, they’d be chasing a symptom, not the cause. And this is why I keep saying like a broken record that any CFS research should include moderate/mild patients rather than just severely ill ones who are in constant state of PEM with all kinds of metabolic and neurological symptoms at all times.
One might say that the research can still turn out something useful about CFS. I think chances are that it’ll turn out something useful about the anatomy of that particular symptom rather than anything specific to CFS, unless that symptom is unique to CFS. And no symptoms other than PEM — be it orthostatic intolerance, brain fog or light/sound sensitivity — has shown to be unique to CFS so far. Is metabolic anomaly unique to CFS? Not sure if they looked at other diseases. Perhaps even flu patients have similar metabolic anomaly/trap for a short duration. We won’t know till we look.
I agree that moderately ill patients should be included in almost all studies and with regards to Phair’s metabolic trap although I don’t know, my impression is that they are.
Ron Davis noted that they picked up the strongest signals and most information from the most severely ill sepsis patients – I think that guided his thinking regarding the severely ill study. That study was always meant to be a first step – the moderately ill patients were next.
Being even moderately ill with ME/CFS means a decline in functionality that few other diseases can match. Something really substantial has gone wrong. To not be able to exercise even a small amount without such payback – something major has gone really, really wrong.
That’s why ‘ve always believed that when they find out what is going on in ME/CFS it will likely stand out in everyone….
Re: AMMONIA ELEVATION, perhaps this may be useful input.
I have had ME/CFS/SEID for at least 14 years — for 14 years at a severe (95% bed bound) level. I finally began with an expert clinician (who is also an expert re: Lyme’s). He does very extensive testing.
His first round of blood testing discovered I had elevated ammonia.
It was very scary to me, as I learned that elevated ammonia is damaging to one’s brain.
He put me right away on the supplement L-Ornithine (from L-Ornithine Hydrochloride) — at a level of one 500mg tablet per day.
In my blood testing a year later, my ammonia level was normal! Thank God! : ) He is keeping me on this.
I use the product from NOW, available on Amazon. On the supplement container, it states:
“Ornithine is a non-essential amino acid that plays a central role in the urea cycle, functioning along with arginine and citrulline to rid the body of ammonia, a by-product of protein metabolism. Because ornithine is converted into arginine, it can help to maintain healthy arginine levels in the body. Ornithine can also be converted into other amino acids, such as citrulline, proline, and glutamate, as well as creatine, an important energy source.”
My doctor made clear that my ammonia elevation (“a by-product of protein metabolism” quoting above) has nothing to do with how much protein I eat … and that I should not reduce protein in my diet.
Obviously I am not suggesting anyone try using this without prior testing and consultation with her/his doctor.
…. I also want to add (to others above) my own huge appreciation for all Cort so brilliantly & caringly gives to us. THANK YOU, CORT !
Hello Alden, thank you for this information. May I ask about your symptoms with high ammonia level and then with a lower? Did it change sth?
Hi Alden. From what I understand, Newcastle uni in Australia discovered this breakdown of protein many years ago. They termed it “catabolism”. If there are not enough amino acids available, the metabolism breaks down the body’s muscle itself. I use Citrulline Matate to rid my body of metabolic waste as arginine fuels Epstein Barr virus, which is also very damaging to the body.
P.S. The above relates to the part of this blog which says — re: the discoveries by Chris Armstrong (from Australia) who works for Ron Davis’ Open Medicine Foundation:
“The metabolomic studies suggest, though, that the nitrogen elimination system in ME/CFS is being overwhelmed – leaving the nitrogen to be eliminated in the form of ammonia (!) (which contains nitrogen) or nitric oxide/peroxynitrite – both of which can be highly toxic. Armstrong suspects these nitrogen byproducts of energy production could be interfering with the energy production process itself in ME/CFS.”
Nitrogen & ammonia goes hand in hand with Radiation Sickness which has been found in all cohorts 100% of them with Gail Kansky’s Team & also they funded a Team of top Radiobiologists on the globe in Hamilton, Ontario, Canada & they published their
findings already…Ron Davis never ever did the proper urine samples needed to diagnose radiation sickness he used on useless hair samples. The Woman involved was the first called up when the disaster happened in Japan’s nuclear plant she was
one of first inside.The radiation page of The National CFIDS foundation shows all the links & publications to date…Thank you Gail
“Armstrong recently received a donation to assess over 10,000 molecules in biofluids and cells to track nitrogen flows through the energy production system in people with ME/CFS and healthy controls. Health Rising will devote a full blog to this hypothesis over the next month or so.”
How is this going Cort?
Has it been published please?
Waiting excitedly ????
To site this article Andrej Rusin, Colin Seymour & Carmel Mothersill (2018) Chronic Fatigue & Immune Deficiency (CFIDS) RusinCFIDSionizingRad.pdf Hopefully, the truth will come out on what CFIDS really is all about
Does anyone know what became of the B12 trial described in https://www.healthrising.org/blog/2013/12/05/bringing-relief-many-chronic-fatigue-syndrome-fibromyalgia-b-12-folate-crowdfund-trial-begins/? “This hundred person, placebo-controlled, double-blinded, international trial will determine how how effective B-12/Folate is. It begins in March, 2014.” I can’t find a more recent article or progress report about it. Thank you very much.
@Cort,
is there any news from Ron Davis about his test for ME?
what about any kind of timeline to hear if test is successful?
any correlation/collaboration between Alain Morneau’s possible test and Davis’s?
anything on the CFS test that was patented by Griffith University?
https://www.google.ca/amp/s/meaustralia.net/2016/03/03/griffith-uni-claims-breakthrough-on-diagnostic-blood-test/amp/
Better start thinking outside the box.
I am a retired board certified urologist (Michigan) but practiced “alternative” medicine for 40 years. My license was revoked twice for being “unscientific” but the following are therapies that work for most chronic “untreatable” conditions
Checking sublingual intracellular magnesium & replacement with magnesium bicarb. (Plain Milk of Magnesia in seltzer water)
Salivary 24 hour cortisol profile (ZRT or Labrex Labs Portland, OR)) and consider trial of low dose hydrocortisone therapy The Safe Use of Cortisone by Jefferies
Urinary pH monitoring and raising it to 7.5-7.8 with sodium bicarb (baking soda)
Healing is Voltage by Tennant
Clinical evaluation for thyroid deficiency (Am axillary basal temps or Achilles reflex)
Hypothyroidism – Type 2 by Starr
Consider Low dose naltrexone
Hair analysis or 24 hour urine for toxic metals – Chelation Therapy
a Paleo Diet – no grain
Best wishes
Trial of regular Myer Cocktail IV’s – Vitamins & trace minerals
Ozone therapy.
I hesitate to include this, but urine therapy has done amazing things over the past 100 years Your Own Perfect Medicine by Christy
Explore http://www.earthclinic.com for other ideas.
The American Academy of Medical Preventics, and Regenerative & Functional Medicine organizations have local doctors to help with the above, except maybe not with urine therapy.
Check out
Urine therapy – see Your Own Perfect Medicine by Christy –
One could also use urea.
Like for sickle cell – the same type of red blood cell deformation is seen in many stressed states, like in ME/cFS.
I would do it low and slow, to see how the body responds.
I found I needed to up my carbs, potassium (via juice) and salt.
I have a friend that is deeply involved in all areas of CFS/Fibromyalgia for many years, he was once interviewed, several years ago, in collaboration with a Neurosurgeon form Chicago, on Good Morning America, concerning the affects of CFS and Fibromyalgia. In Dr. Davis’ son’s case I am sure imaging studies have been performed, specially MRI of the Cervical Spine to include measurements of the the base of the brain for Chiari Malformation, which affects the cerebellum. Has surgery for pressure release of this displacement be suggested? Many articles/physicians have summarized CFS and Fibromyalgia as a pseudo-disease leading to numerous consultation and unnecessary hospitalizations.
I believe it would be possible to train dogs to detect high levels of ammonia in people by smell. Just as they are now using dogs to smell for the covid virus in people.
https://www.washingtonpost.com/nation/2021/09/09/covid-sniffer-dogs/