


Systrom and company came up with a way to get to Rome: i.e. to a fatigued, exercise intolerant state – in connective tissue diseases this time.
The last blog noted that many different roads may lead to Rome; i.e. to the fatigued, exertion-challenged states we see in chronic fatigue syndrome (ME/CFS), fibromyalgia (FM), long COVID, and others. Here’s another road.
It’s no surprise that David Systrom, who has specialized in uncovering interesting ways to get to ME/CFS, was the senior author of this study. This time, though, Systrom teamed up with lead author Inderjit Singh from Yale, as well as researchers hailing from Brazil and Belgium.
Singh, a younger researcher, worked with Systrom on a recent study that provided the startling suggestion that the skeletal muscles in long COVID might be similar to those found in people with heart failure.
Now in “Systemic vascular distensibility relates to exercise capacity in connective tissue disease“, Systrom and Singh take on the role connective tissue changes may play in exercise intolerance.
Connective tissue diseases (CTDs) affect the connective tissues that glue the body together. Without our connective tissue scaffolding, we’d be a jellyfish-like lump of flesh and bones.
Singh and Systrom didn’t appear to state which connective tissue diseases (CTDs) occurred in their cohort, but over 200 diseases (Ehlers Danlos Syndrome (EDS)), joint hypermobility syndrome (JHS), craniocervical instability (CCI), systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), scleroderma, polymyositis) can affect the connective tissues.
Note that Systrom and Singh were studying people with connective tissue diseases and unexplained exercise intolerance; i.e. not everyone with these diseases necessarily displays exercise intolerance.
Possible Connective Tissue Connections
Note that the diseases of the connective tissue that were the focus of this study are characterized by arterial stiffness – not joint and arterial laxity found in diseases like Ehlers Danlos Syndrome, joint hypermobility syndrome, and craniocervical instability.
People with rheumatoid arthritis – a connective tissue disease – have increased rates of fibromyalgia, and some believe that Sjogren’s Syndrome – which can also impact the connective tissues – is greatly underdiagnosed in ME/CFS as well as postural orthostatic tachycardia syndrome (POTS).
A recent study exploring the issue of exercise intolerance in RA uncovered some fascinating parallels. While ME/CFS has never been associated with RA, the two diseases share hyperactivation of the fight/flight system (sympathetic nervous system), and a similar metaboreflex profile during exercise. Another potential connection popped up when one of the authors reported that a long-COVID exercise study was showing similar results. Hooking two rather mysterious diseases like ME/CFS and long COVID up with a major, well-funded disease like RA could be very helpful.
The authors proposed that the presence of “vascular stiffening” could reduce the ability to deliver blood to the muscles and thus cause exercise intolerance in these diseases. Vascular stiffening refers to a loss of elasticity in the arteries that keeps them from dilating normally to allow greater blood flows.
The Study
Singh and Systrom put 66 connective tissue disease patients and healthy controls through the same invasive exercise tests that they’ve put ME/CFS and long-COVID patients through.
They had two goals: a) determine if connective tissue disease patients had problems exercising; and b) and if their impaired ability to exercise was associated with narrowed blood vessels and inadequate blood flows.
They used something called “multipoint systemic pressure-flow plots” to determine the “vascular distensibility” each group displayed during the workout; i.e. the degree to which their blood vessels opened in response to the need for more blood during the exercise.
Results
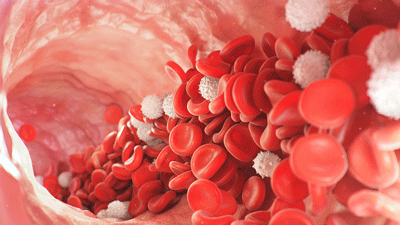
The blood vessels of the connective tissue disease patients did not dilate as much as the blood vessels of the healthy controls – thus impairing their ability to exercise.
The study found that the blood vessels of people with CTD did not dilate as much as the healthy controls. The CTD patients also displayed an “impaired stroke volume increase”. As their exercise level increased, their heart should have been pumping out ever-larger amounts of blood, but in the CTD patients, the increased blood flows ceased at an earlier timepoint.
The Gist
- David Systrom and his team have shown that exercise intolerance that appears to result from blood vessel problems is present in ME/CFS and long COVID.
- Now he’s moving onto a somewhat unanticipated group – people with connective tissue diseases (CTDs). (Note that the blood vessels contain connective tissues.) While connective tissue problems such as joint hypermobility and craniocervical instability have been found in ME/CFS, no one, until now, has examined how connective tissue problems might affect energy production.
- Both ME/CFS and FM, and the people with CTD in this study, appear to share a connective tissue issue: increased arterial stiffness.
- The study found that people who had a CTD and unexplained exercise intolerance displayed a similar exercise profile as people with ME/CFS and/or long COVID: an early entry into anaerobic metabolism, reduced oxygen uptake, and reduced energy production.
- This study also showed, though, that the small blood vessels were not dilating sufficiently to let normal amounts of blood through to the muscles.
- The authors speculated that excessive sympathetic nervous system activity and blunted parasympathetic activity were causing the endothelial cells lining the blood vessels to produce too many vasoconstricting substances.
- While the authors didn’t mention autoimmunity, an autoimmune process affecting the blood vessels has been proposed in ME/CFS. (Could a similar, as yet, unidentified process be occurring in some people with CTDs?)
- The finding that exercise intolerance is present in at least some people with CTDs is encouraging as it broadens the exercise intolerance field, potentially opening it up to more funding.
- Once again, the endothelial cells lining the blood vessels have popped up.
That led to lower levels of oxygen extraction in the muscles, resulting in an early entry into the anaerobic threshold (where anaerobic energy production becomes dominant), and lower levels of energy production in the CTD patients.
Except for the reduced “systemic vascular distensibility”, which has not been measured in ME/CFS, Systrom has found the same findings in ME/CFS and long COVID.
Vascular Stiffening
Arterial stiffness is most often found in diseases like diabetes, hypertension, but has popped up in both fibromyalgia and chronic fatigue syndrome (ME/CFS). A 2011 study that found increased arterial stiffness in fibromyalgia led the authors to propose endothelial cell problems were present in FM. Next, a 2017 study suggested the endothelial cells in FM may be pumping out increased levels of vasoconstricting substances.
Two studies, including one from Lynette Hodges from this year, found increased arterial stiffness in ME/CFS, as well. Hodges, a New Zealand researcher who’s been focusing on exercise intolerance, reported that chronic vascular (blood vessel) damage appeared to be impairing blood vessel vasodilation in ME/CFS as well.
In the present study, the authors proposed that sympathetic nervous system hyperactivity and parasympathetic nervous system underactivity – both of which are found in ME/CFS and FM – were causing the reduction in blood flows. Usually, the vasodilator response in the microcirculation overcomes the hold the sympathetic nervous system has on the blood vessels, but not this time.
Why this situation is happening is unclear, but the authors proposed that the CTD patients’ endothelial cells were producing too many vasoconstrictors such as endothelin (which has been implicated in fibromyalgia) and too few vasodilators, such as nitric oxide (NO). The potential problem, then, may come back down to the same endothelial cells that are receiving a lot of attention in COVID-19, long COVID, and ME/CFS.
In their ME/CFS hypothesis, Wirth and Scheibenbogen proposed that a massive vasodilator response involving bradykinin and other vasodilators attempts to overcome the tight grip the SNS has on the blood vessels. That response ultimately fails, but as it does, it produces many of the symptoms found in ME/CFS.
While the authors of this paper do not mention it, the endothelial cells are impacted in COVID-19 and long COVID by the virus’s entry via the ACE-2 receptors. Dysfunctional ACE-2 receptors. may also be present in ME/CFS and postural orthostatic tachycardia syndrome (POTS).
Autoimmunity could also play a role. Autoimmune diseases tend to gather together. Could the same autoimmune process be impacting the blood vessels in connective tissue diseases and ME/CFS? Could ME/CFS – given that the blood vessels contain connective tissue- be an autoimmune-driven connective tissue disease?
Conclusion and Review
Almost by the week, the exercise intolerance issue seems to get ever more interesting. Right on the heels of a study examining exercise intolerance in rheumatoid arthritis, we get a similar result from the Systrom/Singh team that’s been focused on ME/CFS and long COVID.
The really, really good news is that if these findings hold up – and the authors of this study noted that larger studies do need to be done – the same general process may be causing exercise intolerance in connective diseases as well. Given the authors’ mention of arterial stiffness in CTD, it’s intriguing that arterial stiffness has also been found in ME/CFS and FM.
While the degree of exercise intolerance is surely much greater in ME/CFS, a finding like that could be helpful for diseases like ME/CFS and FM that have struggled for funding.
The exercise intolerance appears to be related to an inability to get proper blood flows to the muscles. That inability results in reduced oxygen uptake at the muscle level, a collapse of the aerobic energy production system, and an increased reliance on anaerobic energy metabolism which results in early fatigability and increased levels of pain, fatigue, etc. due to the buildup of toxic byproducts.
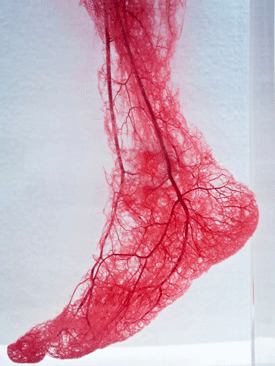
Narrowed blood vessels may not be delivering enough blood to the muscles.
This study used a different technique than past ME/CFS studies which was able to demonstrate the inability of the vasodilators to sufficiently open the blood vessels enough to allow normal amounts of blood through to the muscles.
The authors proposed that endothelial cells lining the blood vessels are emitting too many vasoconstrictors and too few vasodilators to allow the blood vessels to open enough.
Most intriguingly, this is the same general process that Wirth and Scheibenbogen proposed in their 2020 hypothesis regarding ME/CFS, with the addition that they believe that very high levels of vasodilators are responsible for many of the symptoms in ME/CFS.
The authors did not mention a potential cause of the SNS activation, but both they and Wirth and Scheibenbogen have floated the idea that an autoimmune process involving the beta-adrenergic receptors may be to blame.
BIG (little) Donation Drive Update
Thanks to the over 330 people who have propelled Health Rising to about 45% of its year-end goal.

We keep an eye on researchers we believe are producing fundamental insights in ME/CFS, FM and long COVID.
This study is not on ME/CFS, FM, or long COVID; in fact, it doesn’t even mention them. So how did a website on ME/CFS/FM and long COVID pluck this study out of the hundreds of studies that are published every day?
It was simple – we follow David Systrom. One of the greatest research gifts to the ME/CFS community of the past five years and we keep up on everything he does. When this study came out, its implications – that a similar process may be occurring in ME/CFS/FM, long COVID, and connective tissue diseases – were obvious, and we jumped on it.
If that kind of coverage gets your blood flowing, please support us!


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



Again, I think it is important that we carefully distinguish having “problems exercising” and PEM. Exercise inability is a rather common problem for cardiovascular diseases, COPD, cancer, RA, etc. PEM, on the other hand, is unique to ME/CFS. Exercise able ME/CFS patients at the mild end of the spectrum still suffer from exercise intolerance. (eg, hike 5 miles and then struggle with PEM for months). And patients at the severe/moderate end are exercise-unable because they are either severely deconditioned due to repeated PEM or in constant state of PEM from ADL.
While it may be possible to learn what’s happening during PEM by looking at other exercise-unable diseases, that still won’t answer why we get PEM at the first place, which probably is the key question for ME/CFS.
Why do you think PEM is different? I have seronegative RA and the chills, fatigue and weeks to months worth of crashes I get from physically overexcerting myself fits PEM just fine. Bedbound for 9 months in 2018. Not fun.
If that is the case, then yeah, I’d certainly agree that is PEM. But most literature I’ve seen describes RA fatigue as something like: “Exercise can feel more difficult and draining than usual if you have rheumatoid arthritis” or prescribe physical exercise as a way to reduce fatigue. Neither the NYT article nor the Brazillian study mention PEM, just the difficulty exercising caused by overactive sympathetic nerve that constricts blood vessels while exercising.
You’d be surprised how inaccurate the descriptions of any autoimmune diseases is in the medical literature (rather like describing PEM like feeling a bit bad after exercise).
Patients with RA get POTS, nerve damage and all kinds of stange things. Yet 99% of rheumatologists have never heard about it.
The blog RA Warrior is all about how many debilitating multi-systemic symptoms doctors overlook in RA. Many of them are surprisingly similar to ME.
I have HEDS (by strict 2017 Villefranche criteria) and also had seropositive Lyme not diagnosed until after a year after the tick bite. Presumably as a result, I suffer from a lot of pain, fatigue, and very unpredictable post-exertional malaise that has made it impossible to work. I’m applying for SSDI right now and tried to get a (self-pay) appt at the Charlotte Center that does two-step exercises for CFS in order to help get SSDI. Dr. Charles Lapp wrote me back and refused to see me because he said I had HEDS and not Chronic Fatigue Syndrome, despite the debate for years as to whether PEM is a common result of several different syndromes. My docs at Duke don’t have the equipment to do it–only Charlotte, in NC, can do it–but apparently having a genetic connective tissue disease and history of late-diagnosed Lyme precludes you from getting an exercise test for my clinically well established chronic fatigue, the criteria for which I’ve met since 2012.
I wonder if I could go to Boston and get my test conducted with this physician. I used to raise tens of millions in interdisciplinary and interinstitutional research grant proposal development before I became too bedridden to work that hard, but I still have some relevant skills that I might be able to volunteer to the Harvard Team’s effort. If any of them are reading this, please respond and I’ll get in touch. My eldest lives up there so I have a place to stay.
Another question I have with Duke is, why don’t they purchase the two-step exercise stress test for their labs? With an aging population and long-COVID, it’ll be a growth industry. My cardiologist immediately had said to me, oh, we wouldn’t purchase it–wouldn’t have much need for it. Are you kidding? There are so many middle-aged workers applying for SSDI due to chronic fatigue that they’d make a gold mine out of it! But they tend not to think outside their disciplines to discern long-term trends with patients (that are evident here and at places like Inspire.)
I question the hypothesis of increased arterial stiffness in people with EDS being implicated in fatigue. Having EDS myself (and remember there are 13 major types and not all are the same), mostly people are referring to the most common, Hypermobile type.
The genetic underpinnings of hEDS are still unknown but their effects are across the structural system of the body including organs, muscles and even bones. Fatigue is prominent in EDS, especially Hypermobile EDS.
I propose that the hypothesized compromised integrity of the (stiff) vascular system stems from the connective tissue missing components which help it function. In the extracellular matrix of hEDS, there are quite a few abnormal or missing proteins. It is a complex array and all are needed for proper function.
hEDSers frequently have trouble with blood pooling in their lower extremities. As with many issues in the body, it is likely a confluence of things (heart, autonomic nervous system, etc), but EDS experts suspect that a major part of the problem is that the vessels are not working because they don’t have the tissue integrity to expand or contract optimally. It’s like they have one shape and struggle to open or close to propel the blood around the body normally. They simply don’t have the physical ability to do so. Poor blood flow equals less oxygen to the cells and tissues and that equals fatigue.
Of course this doesn’t mean the vessels don’t work at all, or else all hEDSers would be dead! Perhaps there is an autoimmune factor–or something else.
As far as RA (and other autoimmune diseases) and EDS is concerned, it is true that there is a much higher correlation between them than in the general population. But correlation is not necessarily causation…
The genetic underpinnings of hEDS and hypermobility spectrum disorders is thought to be polygenetic–along with individual variations. Like ME/CFS, EDS is also underfunded and under researched. EDS is most certainly congenital (with a few confounders). As to who has the answers, I’m still waiting… The body is very elegant and I’m sure it will be something we don’t expect.
These are fundamentals in the body. It seems very discouraging, although I’ve known for a while this is the case.
Regenerative medicine is the only way out.
Has anyone heard of Liz Parrish. She’s relengthened her own telomeres and regained muscle mass after experimenting on herself. She needs some proper funding
Additional thought; EDSers, because of the lack of tissue strength, especially in their muscles, struggle to hold themselves together. It takes us much more energy to function and that can be draining too…
I would have thought that stiff arteries and dysfunctional ace 2 receptors would mean that we would all have high blood pressure. I have always struggled with very low blood pressure and only now have a decent one due to the large amount of pregnenolone that I take. My blood vessels are always very dilated (a tourniquet is not needed to take a blood sample) so maybe vasodilators are contributing to our symptoms. I have always believed that my PEM is caused by the fact that all my muscles are knotted up and it is known that knots interfere with the blood supply to the muscles and also interfere with the elimination of waste products from the muscles.
@Tricia, good observation! One of the hallmarks of hEDS is subluxations and dislocations. To help prevent this, the muscles do go into spasm trying to hold the body stable–and yes, as you pointed out, that can constrict blood flow!
I might add that over-use or sometimes any use of muscles can bring on pain for us. Pain can be incredibly draining as well!
Sadly I’m in the high BP brigade
Hm, I will read more later on, but first a question! Dysautonomia? Common to both CTD and ME. Is dysautonomia PEM? Or is PEM dysautonomia? Are they connected in some way? But then, what about dysautonomia and metabolic disturbancies in ME? What about overlapping syndromes, connection or misdiagnoses?
/Always confused
This could be macrophagic myofaciitis.. connective tissue solidifying at the cellular level creating the vascular restrictions.
Something to do with the mitochondrial response to viruses, restructures it’s protein structures, then macrophagic myofasciitis will set in to protect it, being in an immune defense role, that’s how connective tissue reacts on a macro level atleast, but the macrophagic myofasciitis (cellular level myofascial build up) could be what’s keeping mitochondria stuck in their viral immunity structures/roles taking away from their energy production role. Build up affects bloodflow, overlays blood vessels, capillaries, organs musculoskeletal structure leading to all the structural pathologies and subsets we see.
MMF has been heavily documented post outbreak. Stems post infection from aluminum adjuvants stored in the body. ME is commonly seen in MMF patients and MMF literature can posted the pathophysiology and symptoms pathology, encourages ME patients to be be screened for MMF. Biopsy at injection site is needed.
MMF is linked to numerous neurodegenrative and neuropsychiatric diseases.
Think about it. Deltoid nerves connect to cervical spine. The cervical pathologies we see in FM, EDS and ME.
And MMF has an effective treatment. We must stop producing vaccines with aluminum adjuvants.
I’ve tried to raise this issue for years. I specialise in reversing chronic injury pathologies and musculoskeletal pathologies using myfoascial release. Working with the connective tissue.
It takes me min 18 hrs per day to manage my own structural pathologies now, to regain and maintain basic function, keep my hands firing so I can keep my body firing. Not been investigated for MMF. Awaiting neurosurgery refferal.
Really hope this isn’t what’s what’s missing because there’s going to be millions of people requiring corrective surgery if this does unfold and go unnoticed. If it is, we can prevent it but people need to be screened / biopsiedfor MMF and treated ASAP.
For a while, I have had the idea that the joint hyperlaxity and the progressive stiffness and/or degradation of connective tissue are separate phenomena.
Perhaps different types of collagen are involved – there are 16 to 29 of them.
So while some collagen structures are lax, others can be stiff.
The hardening/deposition of connective tissue is a normal process of aging.
I tend to think of ME/CFS and hEDS as some processes of aging accelerated (early onset osteoporosis, early onset osteoarthritis, premature greying of hair, nocturia, premature orthostatic intolerance, early onset alzheimer, etc)
(High) Estrogen has a role in the process of injury to tissues, hypoxia, eventually replaced by fibrous one (collagen).
So that while I have joint hyperlaxity, I also have a stiffness overlayed that has gotten worse with age. It may be muscle, it may be fascia – who knows?
My corneas were noted to be very deprived of oxygen and also much thicker than normal. Hypoxia –> thickened connective tissue.
Same for my aorta.
So different types of collagen affected.
And that also leads me to think – is hEDS simply what is called when someone with hypermobility has ME/CFS
There are plenty of people around the world with joint hyperlaxity and no added crazyness.
* Please note *
[Bening] Joint Hypermobility Syndrome [B]JHS
has been changed to
Hypermobility Spectrum Disorders HSD + hEDS
Ooops… this got nestled under another comment by mistake!
Dysautonomia is a connective tissue problem I’d say mostly unless there’s been traumatic injury
Hmm. My pots dr is putting me on midodrine which constricts blood vessels. If this is correct, that sounds like a bad idea. He thinks that people with hEDS and pots may have floppy veins.
Midodrine definitely does work for some people with POTS. Floppy blood vessels could have the same impact as constricted ones.
I take Midodrine for my POTS, but also take Propranolol which is a Beta blocker.
This indeed points to endothelial dysfunction as a possibly unifying link. The fatigue so common in all these disorders may then possibly reflect decreased blood flow to the brain and/or blood-brain-barrier problems which could in turn trigger neuroinflammation.
As to the possible common denominator of the endothelial dysfunction / inability to vasodilate: It would be nice to know what role abnormal GPCR signaling may play in all this. Possibly the diseases are all marked by autoimmuny relalted to GPC receptors (which, btw, also play a regulatory role in the immune system and the CNS).
So, is there a problem with the contraction of the smooth muscle tissue?
The endothelial cells release substance which I believe then cause the smooth muscle tissues lining the blood vessels to relax or contract. If that’s true then the answer would be yes 🙂
Thank you Cort. Very interesting blood flow problems. And in particular the role of the autonomic nervous system. What you and I have drawn our attention to. However, this increased autonomic response can also be a compensation. But this is the road that leads to Rome . I think.
Thank you for your blog and I wish you a Merry Christmas and a Happy New Year! Also, we don’t always agree on vaccinations 🙂 But that’s a good thing. Critical thinking. I don’t own wisdom any more than anyone else.
This is a serious setback I think. I hope I’m wrong. But these are the building blocks of life our connective tissue. If the fault is there, then we’re pretty much screwed. I hope I’m wrong.
I have a friend with heds. His symptoms are exactly the same as mine. Just I saw a different eds ” specialist”
I hope you know smthg we don’t Cort. I hope doctor Davies has the ace up his sleeve cos this is a dark turn in my eyes. It’s scary
Hi Cort, if you ever write a Part 2, please look into viral hepatitis,
I was told the PEM phenomenon is often seen there but found no info about that.
I doubt if that it is the same as ME ppl experience but who knows. I have 2 relatives with RA and they have no Exercise intolerance at all. Their symptoms do not get worse after exertion or exercise.
A family friend has full blown EDS, and she is always tired, there are meds that give her energy like dramadol and Paxil. That however sounds not at all like PEM but rather fatigue.
I think its very important to research the PENE in ME-patients before we say its all the same. But it was an interesting article anyway.
Interesting! Thanks
That comment about PEM with EBV. Please do check that out. Long CoVid sufferer here. My blood tests showed “everything normal” except very high levels of ANA (300+), and EBV (750+). Chronic fatigue and PEM are my constant companions these days. But I’ve Grothe same symptoms fir nearly 25 years, about 10X milder. Plenty of testing showed “no problems”. Covid has just brought this out in its full glory.
Since having ME my blood pressure has often been low when checked. When I had my first covid vaccine (Astra) I felt fine for the first 6 hours. Then started to feel absolutely freezing and my immune system went crazy. By the 3rd day my nervous system started to feel really irritated with pounding heart and chest pain. For more than 3 months I was struggling to breath, absolutely seriously freezing despite living in an extremely warm house, and sometimes chest pain or pounding heart. My GP did blood tests for low platelets but the levels were fine. I have a history of MCS but no lung/asthma problems. Caused very poor circulation and my autonomic nervous system definitely involved.
It is very encouraging research finding that is connecting many loose ends of variety of manifests of SARS-CoV-2.
I am too tired to do much but pisses me hugely CDC does not let public or drs know how out of control lyme disease & other tick co infections are..look at data on ILADS.org and lyme disease foundation. A lot of people could also have this adding to immune exhaustion. Also passed on thru placenta. Both my kids got it. Look at new cases per year. Again example of discrimination by disease which I thought was ILLEGAL…