
Berlin Cures was targeting some of the same autoantibodies found in ME/CFS in heart failure. Then they happened upon a long-COVID patient.
As Carmen Scheibenbogen’s group was tracking down autoantibodies that affect the blood vessel functioning in chronic fatigue syndrome (ME/CFS), a small German group called Berlin Cures was using a different assay to assess the same autoantibodies in heart failure.
They had a drug called BC 007 that’s able to bind to and neutralize autoantibodies that attach to the G-protein-coupled receptors (GPCRs). Their 2016 paper claimed their new approach was easier and possibly more effective than past treatments such as immunoadsorption that have been used to mop up these autoantibodies.
Berlin Cures BC 007 Video
Several papers were then published which highlighted the new drugs’ potential usefulness in what the authors called the “functional autoantibody diseases” such as complex regional pain syndrome, postural orthostatic tachycardia syndrome, ME/CFS, and others. The papers again asserted that other means of removing these autoantibodies such as plasma exchange, immunoadsorption (which they agree can be effective), intravenous IgG treatment (IVIG), or Rituximab were either more costly, less effective, or more toxic than the BC 007 aptamer.
The BC 007 drug came to long COVID circuitously. Originally created to neutralize autoantibodies in autoimmune heart failure, the same autoantibodies were subsequently found in glaucoma, as well. When a patient with glaucoma who just happened also to have long COVID found that his long COVID symptoms cleared up after a single treatment of the BC 007 drug, the company looked deeper – and found one of the GPCR autoantibodies in long COVID.
Dr. Hohberger of the Erlangen Eye Clinic explained:
“Originally, I wanted to use it to help my glaucoma patients. When we then saw the results that arose from cooperation projects on Long COVID, it was like many small pieces of the puzzle that fit together for us. It was quite conceivable that the long COVID symptoms could also improve as a result. “
In November, Berlin Cures published a successful case report of that person. Since then, at least two more people with long COVID who have received the 75-minute infusion of the drug have reported rapid results. (All three patients were monitored in the hospital for three days after receiving the drug.)
One of them, a cross-country skier and former iron man participant (!) was clearly in superb shape before getting the whole, dreary long-COVID package. Months after the infection, he stated:
‘I was completely disoriented and unfocused, I was just trying my best to survive from one day to the next. I was a shadow of my former self, a zombie. I barely recognized myself.’
“I was no longer able to follow conversations, I couldn’t draft a presentation or carry out negotiations and my colleagues had to help me with everything. At home, tackling the smallest chores became a major challenge, and for a while, I even needed at-home help. Reading, pottering around in the garden, or taking my dog for a walk was basically all I could cope with. As if that wasn’t enough, I was plagued by financial worries, panic attacks, and what I call emotional incontinence. I was completely incapable of keeping my emotions in check.’
The week following the injection, everything – his physical and cognitive abilities and emotional balance returned.
The next long-COVID patient – also an avid exerciser – was bedridden, experienced temporary bouts of paralysis, could not follow conversations, etc. She did not experience a complete recovery but her symptoms improved markedly.
The autoantibodies in question quickly decreased after the treatment and stayed that way for the next month. The improvements seemed to stick, as well, lasting at least several months.
Small Blood Vessels in the Eyes Affected
Berlin Cures believes the drug is soaking up autoantibodies that are interfering with the microcirculation. Led by Dr. Hohberger, researchers have determined that blood flows to the eyes in COVID-19 and long COVID are diminished even in patients without any visual problems. They’ve even been able to identify the most impacted microvascular layer in the retina that’s been affected. They reported:
“These results argue for a critical impairment of retinal microcirculation after COVID-19 infection, accented in the ICP, yet affecting additional adjacent microvascular layers after even worse COVID-19 infections.”
As others have, they proposed that the SARS-CoV-2 coronavirus’s entry via the ACE-2 receptor into the endothelial cells was causing the problem – and they cited sepsis as a possible model. As the virus entered the cells, it sparked a hypercoagulation response which produced microclots. They also hypothesized that the capillary damage they’d seen in the eyes simply reflected a massive disruption of the small blood vessels across the body.
“We hypothesize that the severity of capillary impairment after COVID-19 infection is mapped on retinal microcirculation.”
A recent review of “retinal micro-vasculopathy” (damage to the small blood vessels in the eyes) due to COVID-19 reported that despite the numerous issues found (“cotton wool spots”, microhemorrhages, and venous tortuosity), the problems found, thus far, are mostly “subclinical”; i.e. not causing impairments in vision.
Clinical Trial Soon to Get Underway
Word about the successes quickly got around prompting Berlin Cures to state that “Since our first therapeutic successes became public, we have received countless inquiries from those affected.” They stated that no further attempts to use the drug to treat long-COVID will be made until a drug trial has been completed.
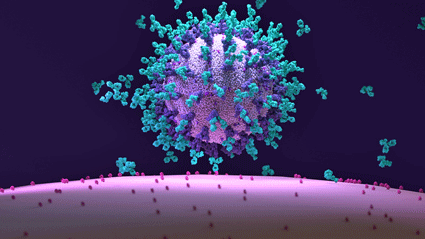
Just as antibodies can block the coronavirus from entering a cell, autoantibodies can block the receptor that opens the blood vessels from functioning properly.
Thankfully, the German government stepped in to fund a small trial of BC 007 which led the researchers to report: “we now have the opportunity to decisively advance our research in this important area.”
Three groups – The Erlangen Eye Clinic, the Max Planck Institute, the Humboldt University in Berlin and the Helmholtz Center in Munich – appear to be working together to figure out what’s what with the drug and long COVID. The clinical trial will start in 2022 and is expected to last for the next year and a half.
People with long Covid who are interested in the trial can contact Erlangen University Hospital at recover.au@uk-erlangen.de You’ll be contacted regarding trial eligibility, dates, etc.
Will the “German Miracle” Work for ME/CFS?
The Gist
- Originally developed to treat autoimmune heart failure, the BC 007 drug targets the same autoantibodies under question in ME/CFS, It also is apparently easier and cheaper to administer than the immunoadsorption technique that’s been trialed in ME/CFS.
- When one of those autoantibodies was found in a long-COVID patient with glaucoma, the drug was tried – and resulted in a long-COVID recovery. Since then, several other long-COVID patients have either rapidly recovered or significantly improved, and the recoveries appear to have stuck for at least several months.
- The drug also cleared up microvascular damage in the retina of the eyes and dramatically reduced the elevations of the autoantibodies in question. The authors believe the microcirculatory problems in the eyes may exist in the rest of the body as well.
- The microvascular problems in the eyes are intriguing as small fiber neuropathy has also been found in the eyes of ME/CFS and FM patients, and small fiber neuropathy can affect blood circulation.
- A small German clinical trial is assessing the effectiveness of BC OO7 in long COVID. German research groups are also attempting to learn how BC 007 is doing what it’s doing in long COVID.
- Other means of mopping up autoantibodies are available. Two small clinical trials suggest that immunoadsorption may be helpful in some people with ME/CFS, and a group of mostly German researchers has called for the use of apheresis in ME/CFS.
Dr. Renz-Polster suggested that increased brain blood flows may not only cause a rapid improvement of brain function but may be able to quickly “abolish the inflammatory milieu which may be at the root of the clonal B-cell expansion and the Aab (autoantibody) production.”
Alternatively, the increased blood flows may be able to reset the sympathetic nervous system -thus abolishing the immune activation it had provoked. The drug may, also, by restoring normal Ang II activity, repair cardiovascular functioning, turn off inflammation, restore brain functioning, and others. Plus, there’s more! Check them out in Dr. Renz-Polster’s paper. (Thanks to Dr Renz-Polster, Brenden, Jutta, Fritz, and others for links and information regarding BC 007.)
Deformed Red Blood Cells as Well?
An Erlangen research team from the Max Planck Institute for Physics and Medicine and the German Center for Immunotherapy has found evidence of deformed red blood cells that they believe are inhibiting oxygen supplies to the tissues in long COVID.

A German research team has found evidence of deformed red blood cells in long COVID
Like Ron Davis, the Erlangen research team has apparently developed their own method – called “deformation cytometry” – to assess the red blood cells in long-COVID patients. They hope to produce a “fast, reliable and inexpensive” diagnostic technique” for long COVID.
The red blood cell deformability finding suggests the blood could be blocked from reaching the tissues in multiple ways (deformed red blood cells, narrowed blood vessels) in long COVID and possibly ME/CFS. Given the degree of disability sometimes found in these diseases, the possibility that multiple harms to the blood circulation system exist doesn’t seem surprising at all. Whatever is happening is having a profound effect. One study, for instance, found that ME/CFS is significantly more functionally debilitating than heart failure, type II diabetes, or multiple sclerosis.
Whether or not the deformed red blood cells are being affected by the autoantibodies isn’t clear, but it’s possible that autoantibody-induced endothelial cell dysfunction could be creating enough inflammation and oxidative stress to cause the damage. Ron Davis has been digging deeper and deeper into the deformed red blood cell issue in ME/CFS and the Open Medicine Foundation recently announced a new grant to study them. Find out more about that work here.
Small Nerve Fiber Connection?
The microvascular retina findings bring to mind the small fiber neuropathy (small nerve fiber damage) findings also found in the eyes of people with ME/CFS and fibromyalgia. Like the microvascular issues, the small fiber neuropathy findings in the eyes don’t seem to be causing much mischief. Like the microvascular findings, though, small fiber neuropathy findings in the eyes and/or skin of fibromyalgia, ME/CFS, POTS, and long-COVID patients have been proposed to reflect systemwide issues.
For instance, Systrom has proposed that small nerve fiber damage is shunting blood away from the capillaries in the muscles. It’s possible, then, small nerve fiber damage might be associated with microcirculatory issues in these diseases. Small nerve fiber damage has been associated with microcirculatory problems in other diseases such as diabetes and chemotherapy-treated cancers.
If it’s true that small nerve damage is contributing to the microcirculatory issues in ME/CFS, FM, etc. we’ll need to know just how important those microcirculatory problems are, what’s causing the small nerve damage in the first place, and how the small nerve fiber damage in ME/CFS differs from that found in other diseases.
Other Autoantibody Treatments
Immunoadsorption
Immunoadsorption is another technique that’s been shown to mop up autoantibodies. In immunoadsorption, blood from the patient is run into a machine that filters out certain portions – such as autoantibodies – from it. A couple of small studies have produced mixed results in ME/CFS.
A small 2018 study found that a 5-day treatment regimen resulted in dramatic reductions in autoantibody issues and improved endothelial functioning. Seven of the 10 patients reported a rapid improvement of their symptoms which lasted for 6-12+ months. None of the patients recovered, however, and despite an improvement of other symptoms, five reported a worsening of fatigue towards the end of the trial.
Two years later a repeat trial in five of the responding patients was done. As in the first study, autoantibody levels dropped dramatically. Two of the patients reported a significant improvement in their fatigue, while two others reported only a small improvement in their fatigue but improvements in other symptoms. One person got worse.
Apheresis
A mostly German group of researchers has been championing the idea of using extracorporeal apheresis in ME/CFS and long COVID. In apheresis, portions of the blood are removed from the patient and then filtered.
They reported that their clinical observations suggest that extracorporeal apheresis used over either 2 or 4 days can significantly improve symptoms. ME/CFS patients with a clear-cut history of infectious onset seemed to do best, and they found elevations of autoantibodies to neurotransmitter receptors.
While apheresis is effective in reducing antibody levels, the authors also noted that because it may affect other parts of the immune system, that exactly what it’s doing is unclear.
IVIG is another possibility that will be covered in another blog.
Conclusions
Once again, we see the interest in long COVID pop out another treatment possibility for ME/CFS and related diseases.
The BC 007 drug is certainly an intriguing compound. Originally developed to treat autoimmune heart failure, the drug targets the same autoantibodies under question in ME/CFS. Apparently easier and cheaper to administer than some other options, the drug developers have had their eyes on diseases like ME/CFS and postural orthostatic tachycardia syndrome for quite some time.
When a person with both long COVID and glaucoma recovered from long COVID following getting the drug, test results revealed he had an autoantibody the drug was able to mop up.
The drug’s results in a few long-COVID patients were impressive, with some patients fully recovering. Test results showed a rapid reduction in their autoantibodies and an improvement in their retinal microcirculation. The damage found in the microvascular regions of the retina was intriguing given the findings of small fiber neuropathy in ME/CFS, and FM patients’ eyes. The German government is funding a small clinical trial in BC 007 and long COVID.
Other ways to mop up autoantibodies are available. Immunoadsorption has produced some positive results in a few small treatment trials in chronic fatigue syndrome, and apheresis is being championed by another German research group for the treatment of ME/CFS. IVIG and drugs like rituximab provide other possibilities.
BIG (little) Drive Update!
Thanks to the over 170 people who have supported Health Rising, our year-end fundraising drive is roaring along.

Health Rising is committed to unearthing treatment options for ME/CFS, FM, long COVID, and related diseases.
Health Rising is fixated on possible treatment options. Over the past six months we’ve covered six long COVID treatments that have popped up (BC 007, stellate ganglion blocks, Bruce Patterson’s statins, AXA1125, inspiritol, oxaloacetate) and they are surely just the beginning. If keeping up on emerging treatment options for long COVID, ME/CFS, FM, and others makes your autoantibodies want to squeal and run for cover, please support us.






Is there any hope of a ME/CFS trail with BC007 anytime soon? It does seem we are circling around this micro-blood clot issue, is Dr. Davis or anyone going to trial these approaches (theories) in ME/CFS in 2022?
Very likely. They’re already including ME/cfs patients in this preliminary survey: https://www.augenklinik.uk-erlangen.de/forschung-und-lehre/recover-projekt/medien/
The German government gave additional 800.000€ to include ME/CFS patients to the Phase II study.
Interesting again.
Are we all fans of James Bond ?
Have a great time in 2022 !
🙂
I’ve only just worked out your 007 remark!
I had a stroke, then a few smaller. My eyes are suffering, my fingers are losing circulation. I’m fighting constant inflammation. I’m begging to use your drug. If I don’t get help soon, I’ll have more mini strokes. Please!! My kids need me!
You seem to have gotten the principle of the Apherese not quite correctly. At least in the H.E.L.P. Apherese that’s currently being studied in terms of Long Covid here in Germany, the patient’s blood is not replaced with donor blood.
Instead it is extracorporally filtered and cleaned with the use of Heparin, which is then removed again before the blood is being fed back into the body. The Heparin binds to various inflammation inducing components in the blood plasma, maybe also to auto antibodies (afaik they’re currently specifically looking for AABs in the residue, but it’s not clear yet).
Thanks for clarifying that, Robert. At its most basic level apheresis appears to refer to the collection of different components of the blood. Yale Medicine lists three types of apheresis – only one of which, “therapeutic apheresis”, is used to treat illnesses. I used their definition of therapeutic apheresis. The German group is doing something very different.
https://www.yalemedicine.org/conditions/apheresis
Yes, the H.E.L.P. apheresis is explained in the links below, with a bit more details on the German website. It seems to be a procedure that’s mainly used in Germany (interestingly).
https://www.bbraun.com/en/products-and-therapies/extracorporeal-blood-treatment/apheresis.html#apheresis
https://www.bbraun.de/de/produkte-und-therapien/extrakorporale-blutbehandlung/help-lipoproteinapherese/help-therapie.html
Dr. Beate Jaeger is currently one of the doctors doing the research regarding apheresis here in Germany:
https://beatejaeger.com/en/research/
You’re just full of good news this week, Cort. Now that there are so many people with long Covid, I won’t be surprised if we stumble upon a couple of other drugs or therapies over the next year or so that turn out to improve long Covid symptoms while treating some other condition that the patient has. It’s encouraging to see a couple of new treatment possibilities out there. Thank you for all of the work you’ve put in to the blog this year — happy new year.
Dr Resia Pretorius starts taking blood samples from ME patients in early 2022. To test for micro blood clots among other things. Dr Amy Proal is interviewing her in this video. They talk about ME towards the end.
https://www.youtube.com/watch?v=C8tzTmVwEpM
Dr Amy Proal is an American microbiologist who has a keen interest in ME as she had glandular fever/ME for a couple of years when she was a student about 20 years ago.
Thanks for explaining Berlin Cures, BC 007. I’ve often seen people mention it, support it, disagree with it but I didn’t know anything about it.
Reading this, it makes me wonder whether in the future we’ll come to the conclusion that there’s so many different elements contributing to this illness and people may have differing components to each other? Like a buffet, their plate looks different to those of other diners.
Thank you Cort for everything that you are doing. There certainly seems to be interesting studies into Long Covid so let’s hope that they eventually bring some hope to ME as well. I wish you and everyone a very happy new year and let’s all hope for a brighter future.
Thanks for another great post but can you add a reference list to the end?
(I know you have links peepered
throughout but that’s much harder for me too use plus you never know when they will take you to another post rather than the article itself or sometimes dont know which article will take you to if multiple works are cited/quoted in a paragraph). Thanks for considering it. I woukd be able to read so much more of your analyses if there was a reference section at the end.
Sorry, it’s all I can do to keep up the blogs (writing them, adding images, the GIST, email blasts) as it is.
What is the blood test to know if we can have this treatment ?
Berlin Cures does the blood test for the auto antibodies. You can find the information on their website.
Thank you for the enlightening article. A very high percentage of Multiple Sclerosis and Parkinson’s Patients have been suffering from various ME/CSF symptoms for years and decades. I hope that these patients will participate in the studies quite soon.
They already treated 3 Cfs patients. None of them got long term reliefs btw. So dont get your hope up.
Well, if you say so…
What is your source of information for that?
It’s not true @ Badpack. They only treated 4 ppl with LC, partially these ppl had ME/CFS als a result of covid. Look what they write on their website:
“In four patients treated with BC 007 under compassionate use conditions at the University of Erlangen with the intention to neutralize these autoantibodies, an enormous remission of LCS could be achieved in a short time, so that one could speak of a cure.”
They had these incredible results after only ONE infusion (75 minutes)!
After that, they stopped this experiment and prepared to do the study. The relief of the symptoms seems to last for at least several months… For me personally it would be fine to get an infusion every 3-6 months to live more or less symptom free… and the medication will be extremely cheap to produce…
Don’t take away people’s hope without at least giving sources… which does not exist for your statement but because it is defakto not true.
it sure fits all the boxes if it works doesn’t it? Cheap and effective. Let’s hope.
Do you know the name of the autoantibody referred to here? I’ve had my blood sent to Germany and they tested for 11 different autoantibodies. Only 2 of mine were in the definite positive range and another 2 were in danger.
Hey Janice, the autoantibodies for the LCS study from Berlin cures are the following:
• AT1-Receptor-Autoantibody
• MAS-Receptor-Autoantibody
• ß2-Receptor-Autoantibody
• M2-Receptor-Autoantibody
• Alpha-1-Receptor-Autoantibody
• ETA-Receptor-Autoantibody
Berlin cures use a new testing method, which seems to be much more accurate. You can read all the details on their website.
I wonder how we can test for those autoantibodies here in the US. They are listed in this document:
https://www.berlincures.com/downloads/downloads/Berlin-Cures-Consent-Form-LongCovid-EN-20211118.pdf
Labcorp seems to test for some of them, but I have no idea what I’m looking at. Here is an example:
https://www.labcorp.com/tests/163915/sub-2-sub-glycoprotein-1-antibodies-iga-igg-igm
If anyone sees an ME/CFS specialist, maybe they could ask them about it.
Those Germans. If they cure ME/CFS, I can forgive them for being bad at soccer.
I messaged Berlin Cures about trials of BC007 on CFS patients. This was the response.
“Currently no study for MECFS is in the planning. This might change in the future. We have no experience with MECFS treatment.
A multicenter, randomised trial leading to an emergency approval would certainly cost > 10 MIo EUR (ballpark figure)”
Hey Bradley,
the problem with the ME/CFS study is the funding (as usual for ME/CFS). A group of German ME/CFS activists are trying to collect the money, which is necessary to do this study (800.000 EUR). Please find the link below:
https://wir-fordern-forschung.org/en/
Feel free to share it! 110k already collected. the more the better =)
Thanks for posting that Tobias. Good luck with the fundraising
It’s exciting that further study of red blood cell deformation is finally happening. About 25 years ago I heard a presentation by a hematologist from either Australia or New Zealand. After studying RBC’s of people all over the world he had found that CFS, along with Down’s Syndrome and a few other conditions had unique RBC distribution of shapes. He also found that for acute CFS does well with B12 and that chronic CFS is helped by high doses of Evening Primrose Oil. I have been taking it for all these years. It affects the formation of the cell membrane, helping it to be more flexible when squishing through capillaries. It helped get rid of my aching legs. Since I have had Reynauds most of my life, it helps tremendously.
Sounds like there’s a lot more going on with red blood cells.
Thanks for passing the evening primrose oil idea on Gidget, I had not heard of that. 🙂
I think the clinician you’re referring to is Dr Les Simpson from New Zealand. Google him and you’ll see his theories re ME/CFS, which certainly resonate with ideas re impaired micro-circulation and cellular hypoxia. I sent Dr Simpsom a blood sample many years ago. He sent back a shot of my red cells under microscope and an explanation of their altered shape + a recommendation to take Efamol evening primrose oil 4000mg per day (8 * 500mg capsules with food in three doses through the day = 500mg 3, 2, 3). There was some mild improvement (I think) but not enough to get excited by. In any event, I know for certain that (whatever the cause) my CFS involves impaired circulation as many of the things I’ve tried in that realm have made a difference. (Especially Normalyte oral rehydration solution most recently)
Maybe in 10 years we will have treatments. Maybe…
Este fármaco ya está desarrollado, esta en fase clínica (ya pasó la fases Iniciales I y II)
Esta en fase III que se prolongara hasta mediados del 2023.
Lo siguiente es fase IV donde se analiza el comportamiento del medicamento en el mercado.
Este fármaco si todo va bien puede estar en 2024 disponible
The quarantine was also hard on both my mental health and my body. My weight has suffered a lot in the past few months, but I also lost a lot of it after getting diagnosed with Covid. After a two-week treatment with an anti-inflammatory and anti-bacterial drug called niclosamide, my body got back to normal. I mostly used capsules that I got from https://www.niclosam.com/product/niclosamide-capsules-500mg/, and I believe that they contributed a lot to the process of getting back on track. My body has suffered a lot since 2020, but I finally feel like things are getting back to normal and that I feel like myself once again.
Any idea when bc007 will be available to people in US with long covid?
Hi Tony, i was also wondering the same thing.
do you know if US citizens are allowed to be treated with BC 007?
AC Anti pf4 search ?
AC Anti gangliosides ?
anti-neurofascine 155
Anti-contactine d’isotype IgG4
Les anticorps anti-nœud de Ranvier sont d’isotype IgG4. Ils sont dirigés contre des glycoprotéines du nœud de Ranvier, neurofascine 140/186 (Nfasc140/186), ou du paranœud, neurofascine 155 (Nfasc155), contactine 1 (CNTN1)
Vgcc
Et
Vgkc
anticorps anti-MAG et FGFR3
Anti AGO
Anticorps anti-neurones (Hu, Ri, Yo, CV2, Amphiphysine et Ma2) – sérum
Anticorps anti-CV2
Anticorps anti-Yo
Yo – anticorps anti-
Anticorps onco-neuronaux
Anticorps anti cervelet/Anticorps anti PCA2
Ri – anticorps anti-
Anticorps anti-Ri
Anticorps anti-Ma2
Anticorps anti-Hu
anticorps anti-CRMP5/CV2
Hu – anticorps anti-
Anticorps anti-Amphiphysine
anticorps anti-SOX1 sanguin
Anti gangliosides (neuronaux)
Anti amphyphisines
(Paranéoplasiques)
Anticorps anti-canaux calciques
VGCC
(Lambert Eaton etc)
Anticorps VGKC anti-canaux potassiques / Lgi1 Caspr2 –
(Paranéoplasiques)
Anti mag
Anti musk anti Rach
Anti-LRP4
Anca (vascularites)
Anti ADN / anti nucléaires
Anti thyroïde :
Anti tpo
Anti tg
Trak
Anticorps anti-cellules pariétales – estomac
CELPA
(Gastrite auto immune etc etc)
Anti digestif foie :
ANTI-MICROSOMES (de foie et de rein)
AC ANTI-TISSU
AC ANTI RETICULUM ENDOPLASMIQUE
AC ANTI-MITOCHONDRIES AC ANTI-CYTOSOL
AC ANTI LKM
TRIPLE SUBSTRAT
(Hépatites auto-immunes)
Anticorps anti-pancréas :
Anticorps anti-pancréas exocrine / PANAC.
Pancréas suite :
Autoanticorps anti-îlots de Langerhans
Autoanticorps anti-insuline
Autoanticorps antiglutamate décarboxylase, GAD
Autoanticorps antityrosine phosphatase IA2
Auto anticorps anti intestins :
Anticorps anti-endomysium et des anticorps antitransglutaminase.
Suite intestinaux :
ASCA
xANCA
Anti gangliosides (neuronaux)
Anti amphyphisines
(Paranéoplasiques)
Anticorps anti-canaux calciques
VGCC
(Lambert Eaton)
Anticorps VGKC anti-canaux potassiques / Lgi1 Caspr2 –
(Paranéoplasiques)
Anti mag
Anti musk anti Rach
Anti-LRP4
Anca (vascularites)
Anti ADN / anti nucléaires
Anti thyroïde :
Anti tpo
Anti tg
Trak
Anticorps anti-cellules pariétales – estomac
CELPA
(Gastrite auto immune etc etc)
Anti digestif foie :
ANTI-MICROSOMES (de foie et de rein)
AC ANTI-TISSU
AC ANTI RETICULUM ENDOPLASMIQUE
AC ANTI-MITOCHONDRIES AC ANTI-CYTOSOL
AC ANTI LKM
TRIPLE SUBSTRAT
(Hépatites auto-immunes)
Anticorps anti-pancréas :
Anticorps anti-pancréas exocrine / PANAC.
Pancréas suite :
Autoanticorps anti-îlots de Langerhans
Autoanticorps anti-insuline
Autoanticorps antiglutamate décarboxylase, GAD
Autoanticorps antityrosine phosphatase IA2
Auto anticorps anti intestins :
Anticorps anti-endomysium et des anticorps antitransglutaminase.
Suite intestinaux :
ASCA
xANCA
Hopefully this will help people that have the identical symptoms from vaccine injury as well.
I’m a doctor in Chicago who treats symptoms of long covid and shot injured and I appreciate what you’re doing.
Any update on this as they recruit for Phase II?
Yes, One recovered completly. Second One didnt, but probably got the Placebo.
Thank you. So…the entire Phase II trial consisted of two people?
Phase II has only just finished recruiting, and the website states there are 114 participants.
https://www.berlincures.com/en/news/sreening-completed-berlin-cures-achieves-key-milestone-in-bc-007-phase-ii-trial-for-treatment-of-long-covid
23 April 2024
That’s phase II for Long COVID.
Phase II for heart failure is a bit more advanced.
Updates from the company here:
https://www.berlincures.com/en/news
I would love to know more about where this has gone since 2022! I have had CFS/ME for over 30 years and am now severe. This could change my life! Please respond with any new info. Thank you!