


The goal – gather different types of information into one coherent whole.
The “omics” studies (genomics, metabolomics, proteomics, transcriptomics) are all the rage. These studies are attempting to get at the molecular roots of chronic fatigue syndrome (ME/CFS), but there’s a problem. ME/CFS is probably not just a “genomics” disease, a metabolic disease, or a disease of the microbiome. It’s probably all of these.
That means we have to find some way to integrate these findings with each other and that’s what this 2020 Japanese study attempted to do. The study, “Deep phenotyping of myalgic encephalomyelitis/chronic fatigue syndrome in Japanese population“, assessed the metabolome, immunophenotype, transcriptome, and microbiome as well as standard lab tests, and gave 48 ME/CFS and 52 healthy controls questionnaires, activity measurements, simple cognitive tests, and sleep assessments.
The Gist
- In an attempt to integrate findings from several different systems together and get a more complete picture of ME/CFS a Japanese study combined metabolome, immunophenotype, transcriptome, lipidome and microbiome results as well as standard lab tests, a sleep, and basic cognitive test together.
- The metabolome, transcriptome and immune results were not particularly revealing. The lipid and microbiome results were.
- A “strong negative association” between the amount of the butyrate-producing Faecalbacterium (F. prausnitzii) and the number of sleep awakenings was particularly interesting given past studies suggesting that butyrate-producing bacteria are deficient in ME/CFS and sleep studies indicating that increased sleep awakenings are present.
- All eight of the lipid tests were abnormal in the ME/CFS group: all the inflammatory lipids were increased and all the healthy lipids were decreased – suggesting, as other studies have, that people with ME/CFS may be at increased risk of a cardiovascular disease.
- The study also suggested that the lipid and microbiome changes occur relatively early in the illness – prior to the three-year mark.
- The study had some interesting findings but was relatively primitive as well with low numbers of metabolites, immune cells, antibodies, the small laboratory panel, etc. Much, much bigger, and more comprehensive multisystemic studies are surely coming in long COVID, and at least one – the combination study from the NIH-funded ME/CFS research centers – should be as well.
Note that none of the metabolites provided much help distinguishing the ME/CFS patients from the healthy controls and only two immune cells did; instead, it was the clinical lab tests, the microbiome, and the lipoprotein levels that were most changed in the ME/CFS patients. Of the six most distinguishing markers, the microbiome and the lipoproteins stood out – taking five of the six top places.
Gut-Sleep Connection
Gut bacteria proved to have a strong effect. The authors noted there was a strong negative correlation between the abundance of bacteria from the Faecalibacterium genera abundance and the number of awakenings during sleep; that is, the more Faecalibacterium present, the fewer the awakenings, and presumably the better the sleep.
That was encouraging as sleep awakenings appear to be a particularly important aspect of sleep in both ME/CFS and fibromyalgia.
This isn’t the first time that reduced levels of Faecalibacterium have been associated with ME/CFS or with problems sleeping. Only one bacteria – F. prausnitzii – makes up the Faecalibacterium genus. F. prausnitzii is an important producer of butyrate – a gut lining protector and anti-inflammatory. Several studies suggest butyrate production is low in ME/CFS. Since inflammation has been associated with poorer sleep, an inflammatory gut could potentially interfere with sleep. Several animal studies have found that butyrate enhances sleep.
Other gut measures have been associated with sleep as well. Gut flora diversity is reduced in ME/CFS but increased gut flora diversity has been associated with increased sleep quality and efficiency and total sleep times and reduced inflammatory markers. Conversely, poor sleep may impact the gut flora: even short-term sleep deprivation was shown to alter the gut bacteria. The gut bacteria that are enhanced by poor sleep can induce fatigue.
Lipoproteins
Lipoprotein levels were also associated with reduced sleep. The choice to dig into the lipoproteins and measure eight of them was interesting and paid off. All the lipoprotein markers were “off”: the healthy low-density lipoproteins were decreased and the inflammatory high-density lipoproteins were increased. Increased levels of both triglycerides – recently highlighted in a study from the Lipkin ME/CFS group – as well as levels of the “bad” type of cholesterol, VLDL – particularly stood out.
Note that two of the three elements of a lipoprotein – the triglyceride and cholesterol center, surrounded by a phospholipid outer shell – showed up in the recent metabolomic study from the Lipkin ME/CFS research center. The same pattern prevailed: triglycerides – which can enhance oxidative stress, were high – and phospholipids – which enhance the integrity of the cell membrane, were low in that study.
This pattern as well as arterial stiffness has been found several times in ME/CFS and suggests an increased risk of cardiovascular disease is present.
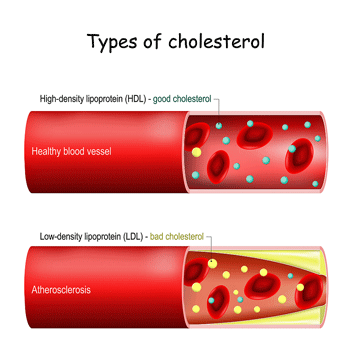
Increased levels of inflammatory lipoproteins have been found several times in ME/CFS.
Noting that statins – cholesterol-reducing drugs – have been associated with reduced sleep awakenings, the authors wondered whether they might be helpful in ME/CFS. Statins, interestingly, did not affect sleep duration and efficiency, entry to stage I sleep, or time to achieve stage I sleep but did significantly reduce sleep awakenings. Statins can produce quite a few side effects including, apparently, a reduction in CoQ10 levels, but a recent fibromyalgia study did not find evidence that statins increased symptoms in FM, and concluded that statin therapy could be helpful in people with abnormal levels of lipids such as triglycerides and cholesterol.
Increased levels of bacteria from the Coprobacillus genus were associated with an increased time required to solve a math puzzle as well.
Lastly, the study found that the increased lipoprotein levels and microbiome changes appeared to occur early in the illness (<3 years) and that the microbiome actually improved after that. Long-COVID studies suggest that a shift to an inflammatory microbiome occurs very quickly in the illness as well.
Bigger, Better Studies Coming
The study used pretty basic data. The long COVID and the NIH intramural study should assess much more comprehensive data sets.
This study came to some interesting conclusions, but it’s not the study we’re looking for. For all its complexity, it was in many ways quite basic. It measured only 40 metabolites (compared to 880 in a recent study), did what looked like a standard laboratory panel, assessed 20 of perhaps hundreds of different immune cells, just 20 antibodies (not including anti-GPCR autoantibodies), and 20 bacterial genera (no bacterial species). Plus, the sleep and cognitive assessments were pretty simple, and the cognitive test had not been validated.
Treatment Takeaways
- The authors proposed that statins might help with both the lipid profile and sleep in ME/CFS. Statin can lower CoQ10 levels and produce a number of side effects. A fibromyalgia study, though, did not find that they increased symptoms.
- The butyrate bacteria-sleep awakenings connection was intriguing and suggested that increasing these bacteria may be helpful. Check out some ways here.
These studies could include the results from a full-blown 900-metabolite analysis, large autoantibody panel, microbiome data down to the species, large immune panels, proteins from a proteome analysis, etc. combined with a sleep study, exercise, tilt table, and cognitive testing in a large number of patients.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


ME/CFS is really a disease that should be called CIRS. Chronic Inflammatory Response Syndrome. Those with the proper genetics end up with chronic low grade neuroinflammation after their system is attacked by a bio-toxin. Although one may clear the toxin, many are unable to halt the immune system’s response to the toxin. With increased neuroinflammation the brain produces less MSH (melanocytes-stimulating hormone) from the inflamed hypothalamus. MSH regulates lining permeability of the gut and blood/brain barrier. So, the answer is to decrease the neuroinflamation to knock out the fibro-fog and leaky gut. The gut flora changes are due to impaired MSH levels, and are not the primary cause of the disease. More meds like low dose Naltrexone are needed to reduce neuroinflammation.
very interesting. Long time ago my specialist find something with my MSH. He couldn’t explain it. It also have something to do with ACTH and Cortisol.
Gijs
Watch the you tube lectures by Dr. Anthony Heyman of George Washington Med School. This Doc is teaching other veteran Internists about CIRS (which is really ME/CFS). You will be interested in his comments on the adrenals. It is very complicated (and I even majored in Biochem at CAL!). This physician has an amazing understanding of chronic inflammation, and especially neuro-inflammation (fibro-fog !!!). Plus, he knows how to treat and heal CIRS (ME/CFS), with real results. No band aid Savella, Adderall, opioids, etc.
Interesting. To show how complex things are a 2010 study (by the same Japanese authors) found increased MSH levels.
“CFS patients with a disease duration of ≤ 5 years had significantly higher levels of α-MSH in their peripheral blood. α-MSH could be a potent biological marker for the diagnosis of CFS, at least during the first 5 years after onset of the disease.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2933583/
They couldn’t though point to what the high levels were doing.
Cort, Do you have any opinion on Dr Heyman’s work? What is your opinion on CIRS?
We’re going to have a blog out on someone who was very severely ill and improved greatly on Dr. Heyman’s work :). I’m just learning about CIRS – didn’t know anything about it until recently.
Cort,
I would love to hear the treatment details of Heyman’s patient. I just became a new patient.
Cort, you are an angel sent by God!
Blood samples and plasma samples are used to test, without any blood volume testing.
Doesn’t the blood volume influence the sample that is taken in ME/CFS patients?
An example:
Ht 0.40 L/L x 3,5 L = 1.40 total Ht : 4,5 L = 0.31 L/L Ht in reality.
Patient 1,70 cm and 70 kg. 4,5 liters normal in ME/CFS 3,5 liters?
When blood volumes are all over the place in ME/CFS should blood volume testing be a standard test when lab test with blood or plasma are used?
I have no idea about the influence of blood volume on other test results but it would sure be great if it was standard testing in ME/CFS/FM and POTS
There has to be an influence on lab tests. When a liter of blood is missing; also what’s in it is missing. That’s why ME/CFS/FM and long- covid seem “invisible” in tests.
In the example above; there is 0.40 Ht missing!
That means recalculating every lab test – % blood volume shortage.
Also in metabolites, I’m sorry Cort, for all the great work you’ve done on those studies: what’s high may be not so high and what’s low is really low.
When plasma volume is lower so are metabolites.
If only doctors and researchers would recognize that, in my view, research can really begin and be fruitful, at last.
And our health problems will be recognized as well.
Please all of you: help me think about this!
It’s a really interesting idea. I guess it depends on what’s depleted in the blood. If the blood chemistry is similar but there’s simply less blood would that be a problem? On the other hand, if a specific aspect of the blood was missing that would surely be a problem. I wish DeJurgen was around to knaw on this one.
If there’s simply less blood? That is the problem. OI, dizziness, brainfog, fatigue etc. because the brain can’t get enough blood and oxygen.
Not enough pyruvate, fatty acids and oxygen makes muscles function poorly, lots of lactate that isn’t removed soon enough and builds up in stead of being reused: FM, PEM.
And what about oxygen; less red blood cells less oxygen?
Measuring saturation on the finger while standing up, or on the earlobe?
Blood that isn’t there has no nutrients, so everything has to come up short; if only lab results were looked at IN TOTAL and not only just one liter or one kg.
I really dug in my heels and found a list of many of the foods, etc I have acquired sensitivities to. I found histamine intolerance and mentioned to my doc. Then I fell into an article. I had a frustrating reaction to a med manufacturer change that’s put me into a circle of many flares etc.
The AOC1 gene has 5 SNP mutations that can result in histamine intolerance (which is a build up of histamine). Seems I have a SNP rs2052129 risk allele T (T/T) which can result in decreased DAO enzyme levels, which increases risk of histamine intolerance (and if true for me explains my weird migraines and long list of symptoms including gut issues, and that can kick out vitamin D… Would definitely explain why as young as 15 I had 2 bouts of gastritis….oodles of other stuff.
If it’s not the DAO enzyme, then maybe in the processing or another player in its role…Do doctors think about looking at this enzyme or is it the road less traveled?
I think we are slowly seeing more work on mast cell activation and we need a lot more. 🙂 I imagine in the research community it’s definitely a road less traveled but it is getting more traveled. This is the second paper if I remember correctly to link mast cell activation to IBS
https://pubmed.ncbi.nlm.nih.gov/34854984/
Microinflammation in the intestinal mucosa and symptoms of irritable bowel syndrome
Thanks Cort for the link. I also read that a vitamin A deficiency can lead to IBS. I recently dug out some childhood records from 1976/77 (I was 14/15). Seems I had a rash dx’d by a derm doc as keratosis pilaris (EDS related??) and can be caused by a vitamin A deficiency. I also have vit D deficiency as it gets kicked out, who knows why.
I have been experimenting with histamine trigger list and I definitely have more problems being wired and awake and not getting tired and causing all over restless leg/body. Not to mention I’m allergic to mold, dust mites and candida= yeast – which I read somewhere that it means you can’t eat “any breads/products.” How did I get so darn lucky? My okay to eat list has gotten extremely smaller. Maybe my next dwelling will be that bubble someone mentioned! I had to give up gardening and that really hurt!!
I’m starting to connect some more dots…..too bad there are no lemon laws on my defective genes!
We can certainly hope for such studies from the NIH—get with it! It’s great to see research coming on the metabolic, immune, and gut angles. Are you also finding studies on long-Covid brain mri’s? An early video with Dr. Nath, said that post-mortem studies of severe Covid patients showed similar abnormalities to mine: nonspecific but lots of widespread white-matter loss and atrophy. The details were similar too, but I forget them (!). Do you see long-Covid brain mri studies yet?
A couple were recently published and I think many more are to come. They have found abnormalities but not the kind you referred to. They may have been different kinds of studies, though. We’re just at the beginning of this.
I was tested at a functional doctors and my butyrate was low, so took supplements for a while, but they taste strongly like cheese but not in a good way. Got too yucky tasting for me to continue.
Also had my lipo density tested and I have the good large kind.
Dont have stomach issues or pain issues thankfully.
I take green lipped mussel oil.
Its really fantastic stuff.
You probably wouldn’t enjoy the fermented oatmeal with the sour cheesy smell it gives off. It’s really something! Good oatmeal too.
My faecalibacterum is 0.5%. Healthy micrbiome has ~13%, according to Thryve testing. That is 22x difference. Makes sense now, why i wake up 10+ times every night.
Gotta take some butyrate and check whether awaikenings will reduce.
Kefir, Xifaxan, and fiber have helped us tremendously. We can not live with out them.
I think this study is too important to wait on a relevant article to post on:
Microbiol Immunol
. 2022 Jan 31. doi: 10.1111/1348-0421.12966. Online ahead of print
A comparative study of valaciclovir, valganciclovir, and artesunate efficacy in reactivated HHV-6 and HHV-7 infections associated with chronic fatigue syndrome/myalgic encephalomyelitis
This study aimed to compare the efficacy of valaciclovir, valganciclovir, and artesunate in treating chronic reactivated human herpesvirus type 6 (HHV-6) and human herpesvirus type 7 (HHV-7) infection associated with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). From 255 patients (192 cases) with reactivated HHV-6 and HHV-7 infections (confirmed based on blood leukocyte PCR), valaciclovir, valganciclovir, or artesunate was administered at a dose of 3000, 900, and 100 mg/day, respectively, for 3 months (study group). The control group consisted of similar patients with ME/CFS (n = 63) not taking any antiviral drugs. The significance of differences was evaluated by Student’s t-test and the nonparametric criterion-the number of Z-signs. Negative PCR results in patients with HHV-6 and HHV-7 treated with valaciclovir was achieved in 26% and 23% (first month), 34%, and 28% (second month), 37% and 34% of cases (third month), respectively (P < 0.05; Z < Z0.05 ). The same results with valganciclovir were obtained in 35% and 33% (first month), 44% and 39% (second month), 48% and 45% of cases (third month), but with artesunate in 44% and 41% (first month), 57% and 53% (second month), 68% and 63% of cases (third month), respectively (P < 0.05; Z < Z0.05 ). Artesunate is more effective than valganciclovir and valacyclovir in patients with ME/CFS with reactivated HHV-6 and HHV-7 infections.
Betty, Dan Dantini has been shouting this from the roof top for years. Me/CFS is the result of bio -toxins like the HHVirals.
Rich, do you mean the antivirals (such as valaciclovir) are bio-toxins?
Or do you mean the Herpes viruses are/create bio-toxins? (I ask since I’m taking valaciclovir for a long time)
Thanks!
Dece,
The viral particles, mold toxins (mycotoxins), Babesia nematodes (microscopic worms), the several Lyme bacteria species, heavy metals are triggering an immune response. This is normal. Those with the right genetics are either unable to completely clear these bio-toxins, or we can not shut down the immune system once the bio- toxins are gone. The chronic inflammation leads to all the symptoms of ME,CFS,CIRS. You need to reduce the neuroinflamation, eliminate the toxins, and then repair tissue with peptides like Vaso Intestional Peptide (which is made in our pancreas, and is available at compounding pharmacies). Keep taking your antiviral!!!
Rich, do you mean the antivirals (such as valaciclovir) are bio-toxins?
Or do you mean the Herpes viruses are/create bio-toxins? (I ask since I’m taking valaciclovir for a long time)
Thanks!
I’ve read your response to my question, thanks for the explanation!
I’ll keep taking my antiviral and look in to your advice!
Thanks again!
Yes, very interesting that an herb you buy in the form of Artemesin I think it is did better than the antivirals.
You can buy artensuate on line. Dr. Cheney used this and/or wormwood (switch and spit method), but this is the first study I have seen that documented its effects. Here is a chart comparing treatment options from the HHV-6 Foundation web site. Notice the excellent profile for artensuate https://hhv-6foundation.org/clinicians/hhv-6-treatment
swish and spit method
Betty Mekdici
Why would swishing product in mouth and spitting be beneficial?
Is swish and spit just for wormwood?
My doc thinks chronic fatigue may be caused by gut inflammation directly (via proinflammatory cytokines) and indirectly via disturbed deep sleep. Microbiome changes are downstream from gut inflammation. Inflammation may be present even if the gut “looks normal” during EGD and colonoscopy and GI docs won’t take biopsies in this case, but if they did it would show inflammation. He says IBS is supposed to be a neuroligical condition and it’s diagnosed when GI symptoms are present but no inflammation is seen during colonoscopy. But if they took biopsies they would show inflammation in many cases. He did a bunch of tests on me that are normally used for diagnosing IBD and they did show inflammation (with no active infection) even though it wasn’t seen during colonoscopy. So now I’m on Mesalamine, which is a first line drug used for UC and Crohn’s, and Gastrocrom, a mast cell stabilizer. Keeping my fingers crossed.
Mast cells seem almost sure to be implicated in IBD and IBS.
Dr. Skip Pridken noticed many of his IBS patients had abnormal looking tissue when he scoped them. His present partner, a PhD Virologist at Uni of Alabama – Birmingham, are in stage three of a dual antiviral drug treatment protocol. The Virologist found active viral infections in the Intestonal tissue of Skip’s IBS patients that had ME/CFS.
https://www.google.com/search?q=heyman+cirs&ie=UTF-8&oe=UTF-8&hl=en-us&client=safari
Heyman talks on CIRS