“An Outstanding study” Avindra Nath

The UK Biobank study is the first of many biobank studies we should see in COVID over time.
The UK Biobank study, “SARS-CoV-2 is associated with changes in brain structure in UK Biobank“, published in the Nature journal, no less, is the first of many of its type we are likely to see over the next couple of years, and highlights what an extraordinary opportunity the COVID-19 pandemic presents for researchers.
The study took advantage of a large number of pre-COVID MRI brain scans UK researchers had access to. This meant they could readily compare the changes in the brains from the pre-COVID state to the long-COVID state. While this kind of study won’t get at what’s happening in the brains during the time of the initial infectious event, it should give us a really good grasp of what’s happened over time. As an added benefit, it almost solely focused on people who’d had mild COVID-19.
I don’t know if we’ve had any studies like this in ME/CFS or fibromyalgia, but we should have them in spades in long COVID. The National Institutes of Health (NIH), for instance, will be scouring large databases of patients who have sometimes been followed for decades, to see what happens to them after they come down with long COVID.
The other notable thing about this study, and the studies to come, is their size. This study examined a remarkable 785 brain scans (401 people infected by the coronavirus; 384 controls) of people older than 51. Contrast that with the typical brain imaging study size in ME/CFS and fibromyalgia with 20 to 50 patients. On MEDPAGE TODAY, Avindra Nath called it an “outstanding study.”
Shrinking Brains?
The authors assessed the differences in the MRI brain scans and gave the participants some pretty rudimentary cognitive tests.

The study found that some parts of the brains of those who had been infected with the coronavirus were shrinking 7-9x faster than normal.
The findings were striking. While no one wants to hear that their brains are shrinking, in several ways, we do want to find biological abnormalities that are consistent with the cognitive problems that people with long COVID are experiencing, and the study was notable for its ability to do that. The study found, in the authors’ own words, a “significant, deleterious impact associated with (the) SARS-CoV-2 (coronavirus).”
The New York Times reported that Dr. Steven Deeks, an HIV researcher at the University of California, San Francisco, said:
“This study provides the most definitive clinical data available to date that SARS-CoV-2 directly or indirectly damages nerves and that this, in turn, can have systemic effects, including changes in the brain…It contributes to an emerging theme that nerve damage was common during the first few waves of the pandemic.”
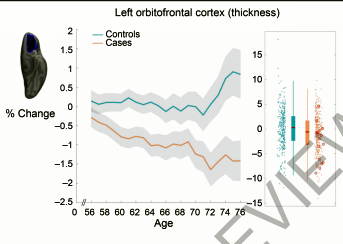
The older the person was, the greater the grey matter reductions. This was the orbitofrontal cortex (coronavirus infections – tan, non-infected-blue).
Most of the abnormalities were found in the limbic and olfactory regions. That the regions of the brain associated with smell (olfaction) were affected was no surprise. It’s not clear whether the researchers were surprised to find atrophy in some of the limbic regions of the brain, but that finding would be of no surprise to ME/CFS or fibromyalgia researchers. Many studies have found altered limbic functioning in both ME/CFS and fibromyalgia. A repetitive transcranial magnetic stimulation UCLA study is currently attempting to alter the functioning of the limbic areas of the brain in ME/CFS.
Limbic system dysfunction could contribute to everything from an activated fight/flight system, increased anxiety and fear, cognition, sleep, and autonomic nervous system, and endocrine problems.
The most prominent reductions in grey matter were found in the left parahippocampal gyrus – a part of the limbic system which encodes memory – and the lateral orbitofrontal cortex (decision-making, emotional lability). The study found reductions in four parts of the limbic system – hippocampus (short-term memory, neuroplasticity), anterior cingulate cortex (attention, motivation, pain processing, autonomic nervous system), amygdala (fear response, autonomic nervous system), and insula (homeostasis, pain processing, motor control, autonomic nervous system) – as well as the orbitofrontal cortex which has strong connections to the limbic system. A part of the cerebellum was also significantly affected.
The olfactory and limbic regions weren’t the only regions associated with grey matter loss. On a more subtle level, it appeared to be present across the entire cortex (the outermost layer of the brain.)
On the whole, these weren’t massive changes in the brain: the authors pointed out that the “structural and microstructural” changes were “modest in size”. Still, at their worst, parts of the COVID-19 patients’ brains shrank 7-9x’s more quickly than expected (our brains shrink over time.) The reductions in diffusion, along with an increase in cerebral spinal fluid, suggested that some tissue damage had occurred. It was likely due to a loss of grey matter found in the nerve bodies. (White matter refers to the sheaths covering the nerves.)
The increase in cerebrospinal volume seemed interesting given the increased cerebral spinal fluid pressure studies that have been found in both fibromyalgia and ME/CFS. (Intracranial hypertension has not been assessed yet in long COVID).
The Nose – the Key to Limbic System Dysfunction in Post-Infectious Diseases?
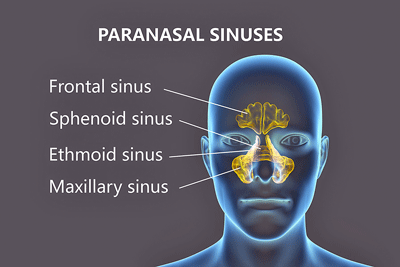
Could the nose’s connection to the limbic system lead to limbic system problems in post-infectious diseases?
The connections between the olfactory and limbic regions might be able to explain why the limbic region of the brain gets hit so hard, not just in long COVID, but in post-infectious disorders like ME/CFS.
Much of the discussion regarding the coronavirus and the olfactory regions has focused on the smell problems, but as viruses often enter the body through the nose, nearby regions of the brain might be affected in many post-infectious diseases.
In fact, reductions of grey matter in the orbitofrontal cortex and insula have been found in chronic rhinosinusitis – which the authors called a post-infectious state. (One of my doctors got her treatments and lab tests covered by using rhinosinusitis as a diagnosis). Baraniuk’s studies have shown the nose is affected in strange ways in ME/CFS.
Cognition Affected
The cognitive tests were relatively crude but did show that the COVID group had experienced reductions in information processing and attention. Given the alterations found in the parahippocampal gyrus – the seat of short-term memory – the authors questioned whether COVID-19 patients might be at increased risk of dementia further down the road. Thankfully, an international effort to answer this question is underway.
The evidence for an increased risk of dementia in diseases like ME/CFS/FM is mixed, with one fibromyalgia study suggesting not and one suggesting yes.
Without mentioning the ME/CFS connection, the study also authors noted one of the most intriguing overlaps between long COVID and ME/CFS – white matter hyperintensities. It isn’t just that microhemorrhages have been found in the brains of both long COVID and people with ME/CFS. It’s the unique pattern that they’ve taken – in both ME/CFS, with its different triggering event, and long COVID – the white matter hyperintensities seem to be spread randomly throughout the brain. Interestingly, a similar nonspecific microhemorrhage pattern also appears to crop up in “long Lyme disease” (i.e posttreatment Lyme disease syndrome), and is reportedly found in multiple sclerosis as well
The Slow Way or the Fast Way – Take Your Pick.

The ME/CFS field has much to offer long-COVID researchers and patients.
Asked to comment on the study, a Yale researcher, Dr. Spudich, stated that “this is pretty convincing evidence that something changes in brains of this overall group of people with Covid”, and then qualified her statement: “To make a conclusion that this has some long-term clinical implications for the patients I think is a stretch.”
The Gist
- A UK Biobank MRI study examined the brains of 785 people over time – about half of whom had been infected with the coronavirus. The average time after infection was about 5 months.
- The study authors found a “significant, deleterious impact associated with (the) SARS-CoV-2 (coronavirus).”
- Most of the abnormalities concerned reductions in the grey matter that makes up the nerve bodies in the limbic and olfactory regions. The reductions were “modest” but some parts of the brain shrank at 7-9x their normal rate. Smaller amounts of shrinkage were found over the entire cortex (outer covering of the brain). Older people experienced greater degrees of “shrinkage”.
- Limbic system dysfunction has been found in ME/CFS and FM as well and could contribute to everything from an activated fight/flight system, increased anxiety and fear, cognition, sleep, and autonomic nervous system, and endocrine problems.
- The nose’s close connection to the limbic system, and the limbic system findings in ME/CFS and fibromyalgia, suggest that this area may be at risk of being damaged in post-infectious illnesses.
- Increased cerebral spinal fluid (CSF) levels suggested that damaged grey matter was being flushed into the CSF.
- Reduced brain volumes have also been found in ME/CFS.
- Studies with younger participants, which assess symptoms and which contrast long COVID with recovered coronavirus patients are needed. As this study did not differentiate long COVID from recovered patients, its findings may understate the damage found in long COVID.
- This is surely just the first of many before/after studies that will examine the brain in COVID-19 and long COVID.
Similarly, Columbia University neurologist Scott Small told the Washington Post “This paper might be the beginning of something — but they would have to do a lot more to show this is permanent or that the patients showed interesting changes in cognition.”
All are calling for more research to be done to see if the finding holds up. Of course, that research needs to be done but researchers should also feel comfortable moving forward now, trying to understand the why and how of the findings. That work, after all, has already been done in another post-infectious disease – chronic fatigue syndrome (ME/CFS).
They missed the fact that long COVID already has a potential stand-in that could help them from re-inventing the wheel and saving long-COVID patients some precious time. With similar symptoms, and exercise, blood vessel, small nerve fiber, autonomic nervous system, microbiome, brain, and brain blood flow findings, these researchers might consider taking a gander at ME/CFS research to help them better understand long COVID and the effects it has over time.
Similarly, long-COVID advocates wary at getting lumped in with a controversial disease (or any disease), or who shy away from having ME/CFS experts being involved, might worry less if they understood how embracing ME/CFS could hurry things along. With regard to cognition, for instance, more sophisticated cognitive tests show that the cognitive hit in ME/CFS, and therefore probably long COVID, is indeed lasting.
Long-COVID advocates and researchers might also want to check out the novel approaches that have been developed over time in ME/CFS that could shave years off the time needed to understand and treat long COVID.
Few diseases, for instance, use exercise stressors as a tool to understand them, but decades of work have shown them to be invaluable tools in studying ME/CFS. Tests that show little when people with ME/CFS are at rest suddenly sprout abnormalities when a researcher puts ME/CFS patients on a bike or has them stand for a while or get on a tilt table.
Similarly, compare the results of standard one-day exercise tests – which sometimes suggested people with ME/CFS were merely deconditioned – to the 2-day exercise studies that a) definitively demonstrate that exercise impairs ME/CFS patients’ ability to generate energy; and b) provide a gold standard test for disability. Those tests had been largely abandoned by the medical researchers until ME/CFS researchers resurrected them. Long-COVID researchers could move more quickly if they took these and other innovations developed by the ME/CFS field into account.
Modest But Significant Changes

“Modest” amounts of “brain damage” were found.
Dr. Douad, one of the co-authors of the study, told the New York Times that It is brain damage, but it is possible that it is reversible…it is still relatively scary because it was in mildly infected people.
Brain damage is a scary term – but seriously what did we expect? Problems with cognition, stimuli hypersensitivity, high rates of fear and anxiety, fatigue, even autonomic nervous system problems all suggest some kind of “brain damage” is present.
Let’s not overplay the damage, though. In the paper, the authors stated that the large numbers in the study would allow them to detect “subtle, but consistent spatially distributed sites of damage associated with the infection”, and relatively subtle – small but surprising changes in grey matter volume and some other findings – were what they found.
As the paper noted, more studies are needed; in particular, studies in younger patients, studies that assess symptoms, which contain better cognitive testing, etc., and, in particular, which focus on long-COVID patients. Time will tell, but it’s possible that the study’s outcomes are quite a bit understated as the study simply included everyone who’d been infected by the virus, whether they had long COVID or not.
If as suspected, the brains of people with long COVID are more affected than those who don’t develop it, we may see more alarming results in the future. The study’s short time frame (approximately 5 months after infection) also means we know nothing about the longer-term changes in the brain as well.
Please Support Health Rising!
Health Rising is almost entirely community supported!






Any brain differences pre and post vaccination, and any differences in those who had covid but were and were not vaccinated?
Nothing on that yet – hopefully we’ll see those studies. I wouldn’t be surprised.
Im interested to find out how you compared it to cov19. It was made up in a lab as they did not isolate the actual virus There’s plenty of Scientists who have been challenging this, asking for it to be produced, the actual virus ? has never been produced. Also PCR testing us so badly flawed, how can you be sure it was the virus that people had. They can’t tell anything about infection ? There are so many holes in this I’d ask who funded the study, possibly the Gates Foundation?
I doubt I’m going to persuade you Patricia but the study had many different funding sources including Parkinson’s and Alzheimer’s disease foundations. The Gates Foundation was not involved.
PCR is designed to pick up NOVEL genetic sequences that the virus has. It’s been used for decades to accurately detect pathogens such as HIV for instance. It is in fact the most accurate test for HIV infections – it can pick up an infection within hours of a person being infected and is used to test blood supplies for the virus.
THere’s a myth that the inventor of the PCR test said it should not be used to detect infectious viruses. Check that out here – https://www.reuters.com/article/uk-factcheck-pcr-idUSKBN24420X
The rapid dissemination of the genetic sequence of the coronavirus allowed vaccines to be quickly developed which numerous studies have shown to be highly effective at reducing hospitalization and death.
The guy said it cannot be used for diagnosing an illness, meaning a positive PCR test tells you nothing about your medical state. It is a qualitative test, and a very sensitive one, that will state if a sequence is present. It is not quantitative in that you can use it to determine the amount present, use comparative tests to determine an increasing or decreasing trend, or even exclude an underexposed infection that has been eliminated by the immune system. It’s the global epitome of the every thumb is a finger but not every finger is a thumb. Every ill, and/or infectious person will have a positive PCR but not every positive PCR will be from an ill or infectious person. One of the great things about PCR is its adjustable sensitivity. Inside a blood sample you will have millions of cells containing their own nucleus and genetic material. You obviously cannot just reach in and choose what you want to test. PCR is a technique that allows you to choose a desired sequence to look for and add a small volume of nucleotide bases to the sample in turn doubling the presence of the genetic sequence you are selecting for, if it is present. Each cycle is a further addition of a small volume and a doubling of your desired sequence, this is repeated until the sequence in question would be a large percentage of the samples volume. Allowing you to then test the sample and it contain an adequate number of sequences to be seen if it was in the original. The numbers involved go back to the King’s chessboard and doubling the amount of rice each consecutive square. Suffice to say they grow rapidly and there is a point at which the test will become so sensitive that positive results will come from; small, random, one off bits of genetic material that has been snipped down at some point by a restriction enzyme in an immune cell or part of the natural cell breakdown and recycling process. With enough cycles a single snippet from a different cell that encodes a even somewhat similar protein to what is being looked for can be amplified by the process to cause a positive. It is not really a “bug” but more of how powerful the process is, and for these reasons cycle limits have been established. The very need for those limits reinforces the inventor’s point that it is not a diagnostic tool, as the determining factor on your illness would simply be how many cycles had been performed.
If a PCR test can determine whether a pathogen is present or if a part of a pathogen is present (if that particular SNP is still in the body.) then it certainly IS a diagnostic tool – it diagnoses whether a pathogen is present. It’s been described as the gold standard test for pathogen prevalence by the doctors I’ve seen and is a cornerstone test for modern medicine – the amplification/cycle issue has been known since day one – meaning that the test has been adjusted for that. In short, I’m going to go with the experts.
From The National Genome Institute – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3768498/
From Medline Plus
https://blog.biocollections.com/how-accurate-are-covid-19-pcr-tests/
A study in January of 2021 found mucus PCR tests diagnosed COVID-19 correctly in 97.2% of cases.
It would not at all surprize if similar findings were observed in many of those with moderate to severe CFS. It could also help to explain why those with more chronic CFS get steadily worse as they age. With more loss of grey matter due to aging leading to worsening symptoms. My mother has had CFS for around 40 years now and now she’s in her 80s the CFS is definitely worsening.
Talk about a much needed study. Finding out what happens as people have ME/CFS for longer and longer periods of time is needed not just in ME/CFS but for long COVID as well. Solve ME’s Patient Registry will be able to help with that and we need large population studies as well.
We don’t know, for instance, if the brain hit keeps getting worse as we get older (as you note it may) or if getting hit with ME/CFS or long COVID at an older age has the greater impact.
Interesting comprehensive study, Cort. However, they do not distinguish between the different subgroups of Long-COVID. Seems like around 30% of peope are suffering from Long-COVD, but only around 1/3rd of Long-COVID are displaying ME/CFS symptoms. The other 2/3rd will be of patients affected by the SARS-CoV-2 virus itself e.g. lung damage (inflammation) primarily, but also brain and other organ damage. The lack of smell/ taste is a strong indicator of actual (permanent) brain damage, for example. So brain loss/ loss of grey matter could be related to this cohort of SARS-CoV-2 afflicted patients, as well… and yes, access to the brain via the olfactory centre/ nasal cavity makes sense (circumnavigates blood-brain-barrier). ME/CFS patients smell and taste along woith other senses are affected, but not permanently (but variably throughout relapse-recovery cycle)… Cognitive dysfunction also prevalent, here, and overlappinng with ME/CFS, which makes things complicated to tease out ME/CFS patients (the 1/3rd) with SARS-CoV-2 afflicted (2/3rds)… again, ME/CFS patients cognitive (brain-fog) difficulties NOT a permanent loss (good days, bad days throughout a relapse-recovery cycle)… they need to differentiate between the two… but definitely overlap with ME/CFS in limbic systemm being highlighted as affected… there will also be a significant segment who unfortunately for them have both i.e. SARS-CoV-2 afflicted damage and ME/CFS… so actually 3 different groups. For ME/CFS (i.e the Post-COVD-19 Fatigue Syndrome subgroup, displaying ME/CFS symptoms) they need to hone in on milder (non-hospitalized cases) displaying ME/CFS symptoms. This study does not do that – it just takes an ‘average’ across all cases…
Thanks Angus for applying your expertise to this subject. 🙂
We clearly need much more study. I guess we could all this a large but preliminary study given how much more refinement is needed with those subsets which you aptly pointed out
The infections, thankfully, were almost all mild – only 15 patients were hospitalized – I don’t think I brought that out very well – so hopefully most of the long COVID patients will fit our group. (I must say I keep forgetting about the other groups 🙂 which should ultimately include people with lung and brain damage as well as those people with milder infections who come down with autoimmune conditions over time. It’s going to be fascinating watching how all this gets untangled.
If it is about 10% of long covid patients who have ME/CFS-like symptoms, these results replicate those from the “Dubbo” study.
Right and some studies suggest it may be higher. SOme studies are also finding that the flu virus – a very tough and debilitating and even for some a deadly virus – is not creating so many “long flu” cases. Finding out why that is – if indeed its true – will be fascinating.
Patricia, if you’re a human and not a bot, go grind your axe in an appropriate forum. This is not the place.
White matter lesions are also found in many Ehlers-Danlos patients! We get brain fog too and many of the other ME/CFS symptoms.
https://pubmed.ncbi.nlm.nih.gov/27102338/
Seems as if these lesions can be triggered by trauma, infection, genetics and age. I guess that covers most of the bases!
Another interesting note, lithium use (often to treat bipolar disorder) was connected with lower Alzheimers rates. Sorry but I’m too tired to go looking for that link…
Given that the study was published last summer, I wonder if this would apply to infection with Omicron, a milder variant.
Very good question and I’m sure that we will find out how the different variants affect the risk of coming down with long COVID. Plus there’s the issue of education – I imagine that most people who get long COVID now know that the first thing they must do is rest – not that all of them follow that.
In reply to Patricia above, SARS CoV2 virions have been isolated and characterized by many different labs. A Google scholar search for this topic will reveal many papers, including this one which has characterized the virions by microscopy.
https://www.nature.com/articles/s41586-020-2665-2
In reply to the PCR testing comment above, scientists are well aware of the limitations of PCR. However, PCR or the closely related RT-PCR tests have successfully been used for years to identify Ebola, influenza, papilloma viruses, HIV, adenoviruses, etc. I just recently had a PCR test for EBV, for example.
One of the advantages of PCR testing over older methods of virus detection is that multiple sets of primers can be combined into one sample tube, thereby testing for multiple viruses simultaneously. My son, who was admitted to the hospital for appendicitis, was tested with a 4-plex panel for SARS CoV2, influenza A, influenza B, and RSV, all with one swab. There are also 16-plex panels which can provide more in-depth testing for respiratory pathogens.
In short, there is nothing mysterious about PCR tests other than that the general public had never heard of this test before Covid. It is and has been in widespread use for many pathogens, including viruses and bacteria.
Here is a link to the Biofire respiratory panel, which can detect 22 different pathogens in one sample.
https://www.biofiredx.com/products/the-filmarray-panels/filmarrayrp/
Re. changes of smell: study seems to have found mainly hyposma (loss/reduction of smell)?
As an ME/CFS patient, I have not loss of smell, but the opposite: extreme hypersensitivity to smells (in particular fragrance and many chemical inhalations – including day-to-day smells such as apples (which I used to love smelling!), clear PP document filing sleeves and aging rubber bands in clothes). It is one of my most debilitating symptoms besides Fatigue and PEM.
As far as I know, a subgroup of ME/CFS do have ME/CFS coupled with chemical sensitivites.
I wish science would find out one day what causes this: changes to the stimuli processing chain within the brain such as neuorinflammation of ganglia? Changes at olfactory receptors? Some kind of disorder to metabolizing these inhalations within the body?
Googling “hyperosmia”, I found it also occurs relating to hormone changes e.g. during pregnancy. Most interestingly, I just found there is already a body of literature on hyperosmia and hyposmia in other autoimmune diseases as well as neuodegenerative diseases. This review https://pubmed.ncbi.nlm.nih.gov/23233263/ included the sentence: “Olfactory receptor gene clusters are located in proximity to key locus of susceptibility for autoimmune diseases such as the major histocompatibility complex, suggesting not only a physic linkage, but a functional association.”
One web article https://danielcameronmd.com/whats-that-smell/ mentioned that in a small study, 50% of the patients with Lyme disease suffered from hyperosmia versus none of the controls, while hyposmia was more common with Fibromyalgia.
I sometimes thinks that for the topic of hypersensitivities in ME/CFS, researchers should compile and compare information from many related diseases and conditions, such as the abovementioned research on olfactory changes in autoimmune diseases, emerging SPS research etc.
I’m collecting all snippets of information regarding hypersensitivites so if you know about pertinent research pls. reply, thank you!
Re chemical sensitivities, check out ciin.org. They have a very extensive listing of peer reviewed published literature and other resources and nformation. I wrote research profiles for them for 20 years until they stopped their monthly publication due to illness.
Thank you Treesha!!
Maybe that’s interesting? Berlin cures announced the following on their website:
“Berlin Cures BC 007 –
Clinical Development Status Update.
Berlin Cures plans to conduct a large international study with the goal of obtaining accelerated approval of BC 007 for the treatment of Long Covid Syndrome.
A new batch of BC 007 is currently being manufactured to conduct clinical trials in the indication of Long Covid Syndrome. Berlin Cures plans to conduct a multicenter, multinational, double-blind, randomized study with the goal of achieving accelerated approval for BC 007 in Long Covid syndrome in coordination with the relevant international regulatory authorities. Our partner in conducting this study is Parexel International. The study is expected to take place at more than 15 centers in Germany, Switzerland, the Netherlands, Spain, and Finland. The study is scheduled to start in the summer of 2022.
The list of participating centers will be published in due course. Berlin Cures itself cannot select or pre-register patients for study participation. We ask all patients interested in participating in the study to contact one of the study centers.”
So we’re not talking about a small study at University Erlangen anymore. Now it’s a much bigger international multi-center study. Let’s cross our fingers, hopefully there will be promising news =)