

(Brian Vastag comes full circle. A former employee of the NIH, Vastag’s Washington Post letter to NIH Director Francis Collins “I’m disabled. Can NIH spare a few dimes?“, in conjunction with the recently published IOM and NIH Pathways to Prevention reports, and the actions of many advocates cohered to give ME/CFS its first big boost in research funding in years.
Three ME/CFS research centers were established and an intramural study that Avindra Nath called the most intense effort he’s been involved in began. Patient #4 in that study, Brian first recently posted his experiences of the study and his thoughts on what lies ahead on a thread on the social media site Mastodon. Thanks to Brian for allowing Health Rising to share his story as we await the first publications of this potentially epochal study. Cort)
Six years ago, I returned to NIH, where I started my career as a science writer, to be a patient in an ambitious study to understand post-infectious myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
The study included 30+ researchers & substudies & was a fishing expedition to understand what goes wrong to make us so sick (like bedbound-for-years sick).
NEWS: The study’s findings have FINALLY been submitted for publication.

Avindra Nath – the leader of the study – and Brian Vastag
The study began after I wrote to then-NIH Director Francis Collins, whom I had talked to in my job as a science reporter at the Washington Post, imploring him to invest in understanding ME/CFS, which has been neglected for decades. I also knew other top administrators at NIH and so decided to use my connections to try to get some movement.
I’m disabled. Can NIH spare a few dimes?
Collins, to his credit, emailed me and said he would move fast. This was in 2015. And he kept his word. He gathered some top clinicians at NIH and told them to design an intramural study – meaning it would take place on the NIH campus in Bethesda, Md. – to try to figure out what goes so wrong in the disease. Collins chose neurovirologist Avindra Nath (pictured with me above) to be the principal investigator. Nath is the head of clinical neurology at the NIH Clinical Center.
A 2015 Institute of Medicine report “Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness” had reaffirmed that ME/CFS was a biological, not psychological, disorder, and there had been other pressures on Collins to act. So he moved responsibility for ME/CFS out of the small and under-funded Office of Women’s Health over to the National Institute of Neurological Disorders and Stroke, a more appropriate home.
While the protocol for the study was designed and approved in a month – very fast for NIH – it took almost a year to stand up the study, hire some support staff, and begin recruiting patients and healthy volunteers as controls.
As compiled by advocacy group MEAction, the first aim of the study, during visit 1 for patients, was “**To define the clinical phenotype.”** Via: History and physical examination and systemic assessment Neurological assessment Neurocognitive assessment Psychiatric evaluation Pain/headache evaluation Infectious disease and rheumatologic evaluation by specialists Neuroendocrine evaluation Fatigue testing, exercise capacity https://me-pedia.org/wiki/NIH_Post-Infectious_ME/CFS_Study
Defining the clinical phenotype – As compiled by the advocacy group MEAction, the first aim of the study, during visit 1 for patients, was “To define the clinical phenotype” via:
- History and physical examination and systemic assessment
- Neurological assessment
- Neurocognitive assessment
- Psychiatric evaluation
- Pain/headache evaluation
- Infectious disease and rheumatologic evaluation by specialists
- Neuroendocrine evaluation
- Fatigue testing, exercise capacity
Plumbing the biology of post-exertional malaise – During the second visit, patients were evaluated pre- and post-exercise, to try to plumb the biology of post-exertional malaise – the phenomenon where exertion makes us sicker, using:
- Functional MRI
- Metabolic studies
- Transcranial magnetic stimulation
- Autonomic function
- The study also added skin-punch biopsies, to evaluate small-fiber neuropathy, & muscle biopsies.
Immunology – “The third aim of this study is to conduct a detailed immunological study in blood as well as cerebrospinal fluid including a screen for autoantibodies…. We will also fully explore the gut and oral microbiome and apply proteomics and metabolomics approaches to the cerebrospinal fluid. Studies for aim 3 include:
- Cytokine & chemokine profile in cerebrospinal fluid and blood; after T cell stimulation in culture
- Flow cytometry
- B cell and T cell cloning and T cell antigen receptor sequencing
- Immunoglobulin profile
- Autoantibodies directed against brain antigens
- Cerebrospinal fluid proteomics and metabolomics
- Gut and oral microbiome
- Serum tryptase
- Viral discovery in spinal fluid
Reproducing the disease phenotype – The fourth aim was to see if the disease phenotype could be reproduced ex vivo (outside the body). NIH was to:
- Do metabolic studies on neurons made from patient blood stem cells
- Study humanized mice made from patient stem cells
- To determine if cerebrospinal fluid or antibodies injected in brains of rodents or humanized mice generated with cells from patients can lead to fatigue or behavioral abnormalities.
So, there might be a mouse made from ME running around NIH.
“If these experimental systems are able to reproduce the clinical or biological abnormalities seen in these patients, it would be a major step towards identifying the cause and the pathophysiology of the illness and for developing a variety of treatment approaches to these patients.” – Dr. Nath, principle investigator.
Patient #4

Brian Vastag was patient #4 in the NIH Intramural ME/CFS study.
I was patient #4 when I arrived in April 2017. The study was grueling. I wore an ECG cap for a sleep study (I didn’t get much sleep); had a difficult spinal tap; donated 10 million blood stem cells; had 29 vials of blood taken in one go (fun morning!); took extensive cognitive exams; spent three hours relating my entire health history to the lead clinician in the study (Brian Walitt); and on and on. I stayed as an inpatient for two weeks, with a weekend off.
Patient recruitment was slow; the aim was 40 patients in the first phase, which would be winnowed down to 20 for a second visit to NIH a year after the first. I’m not sure why recruitment was so slow. There was skepticism in the patient community due to NIH’s longtime neglect and dismissal of the illness.
Patient advocates implored Nath to speed up the study by, for instance, bringing in two patients simultaneously. Or to bring in a patient and a healthy volunteer together. They tried this but decided they didn’t have the staff bandwidth to do it. Nath and Walitt both had many other responsibilities & studies to attend to. As a senior NIH official told me about this whole thing: Everyone at NIH has a full plate. They have to push some stuff to the side to make room for new things.
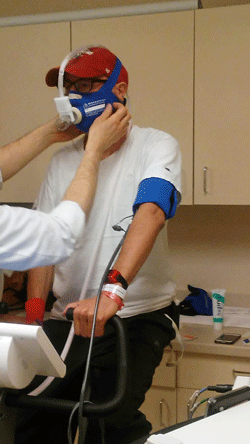
Exercise test
The study was unique in that after the extensive work-up in visit 1, five outside ME/CFS expert clinicians reviewed each case to decide if the patient fit all the published criteria for ME/CFS. This was quality control, to ensure patients really had ME/CFS. Three patients of the initial group were found to have other diagnoses – one had Parkinsonism, one had a rare (and fatal cancer), and so they were excluded from the second phase of the study.
In March of 2018, I returned to Bethesda for the second visit, having been unanimously judged to, in fact, be suffering from ME/CFS. During this visit – another 10 days inpatient – I took a cardio-pulmonary exercise test, which produces very abnormal results in ME/CFS. Exertion makes us sicker, and this test shows that objectively.
I also spent 4 nights inside a sealed metabolic chamber. Every calorie in and out is measured (I’ll spare you the scatological details). The chamber measures how much CO2 a person exhales, and these numbers together can measure metabolic rate. The chamber was loud – lots of fans – and I didn’t get much sleep. Here’s my arm sticking out of the chamber for blood work, with my friend Andreas filming for German television.

Brian’s arm sticking out of metabolic chamber for a blood draw.
Visit two was exhausting. I talked with other patients in the study who were sicker than I was, and they were absolutely annihilated by it. Some took months to recover back to their already-shitty baseline functioning. It was an ordeal, but we were all motivated to help move research forward.
The Study
From early 2017 through early 2020, the under-resourced team managed to bring in something like 18 patients for two visits, and I think they hit their target on healthy volunteers. Like we all told them, it was way too slow. But it was moving forward.
Then the #covid19pandemic hit and the clinical center closed down. The team was unable to complete full study enrollment, a few patients short. Avi Nath turned his attention to autopsy studies of early covid victims to look for signs of brain damage and viral infiltration. In early 2021, the NIH team also brought in about 10 people who developed ME/CFS-like symptoms after covid vaccination, treating some with immunoglobulin & steroids.
The ME/CFS study was very much back-burnered. The pandemic was taking everyone’s attention. I talked to Brian Walitt later and asked him why the team didn’t spend the time when the Clinical Center was mostly closed to analyze the very voluminous data. I didn’t get much of a satisfactory answer, but as Nath was the PI, he was diverted to covid, and that probably is the answer.
Eventually, the NIH team formed 5 data analysis groups for the study. One for immunology, another for physiology, etc. There is so much data in this study of a small group of patients. I think the study was very ambitious, and the team was under-resourced. While 30 or so researchers were involved, most were just pitching in on very specific sub-studies. It was up to Avi and Brian to try to synthesize everything.
And finally, a few days ago – six years to the week I first entered the study – I got word that the NIH, after an extensive internal review, has FINALLY submitted their main paper from the study to a journal for publication. I suspect Avi submitted to the New England Journal of Medicine, his go-to journal, but I don’t know for sure. It took entirely too long.
And I have no idea what they’ve found, or how valuable it will be. They threw so many technologies at this illness that they must’ve found something interesting. They used a technology to look at thousands of proteins in spinal fluid, for instance. In the meantime, millions more people have developed ME/CFS after covid – an outcome obvious to all of us who have been suffering post-infectious ME/CFS pre-pandemic.
So, I don’t really know the lesson here. Yes, this is an important study, where NIH threw 30-40 different techniques and tests at a disease of unknown pathology to try to understand it. But it was seriously under-resourced for such an ambitious remit. Patients continue to suffer. We’re no closer to an effective treatment now, millions of new patients have joined our ranks due to the pandemic, and keeping a flickering flame of hope alive is challenging.
This old, 20th-century model of submitting to ‘top’ journals, waiting for peer review, then for publication, etc., does not serve patients well. It’s too slow. The pandemic showed us clinical science CAN move much faster, with preprints, online group peer-review, etc. But NIH researchers don’t have a lot of incentive to speed things along. They have good jobs for life, basically & while the team was very compassionate, they also were not in a particular hurry.
So now we patients wait again, for some journal editor somewhere to read this very large paper with tons of data in it, find peer reviewers, and then shepherd it along into publication. It could take another 6-12 months for the paper to be published. There are faster, better ways to do medical research, and I hope the field evolves to take advantage of them.
#LongCovid is, in many cases, ME/CFS. In May 2020, @Bether and I warned that this would happen in the pages of the Washington Post. The article “Researchers warn covid-19 could cause debilitating long-term illness in some patients” was extremely well-read – it was on the homepage for over 24 hours, a rarity – but it also hit the same weekend the George Floyd protests started. If not for the protests, I’m quite certain we would’ve gotten good TV and radio pick-up (broadcast people look at the top articles on WaPo and NYT and follow those stories).
I lament the lost opportunity here. If the study ends up revealing key patho-biology of ME/CFS (please g*d, I hope it does), that information could have informed the studies of #LongCovid now underway. Instead, we now have to wait for a journal to accept the article & publish it.
After the initial paper is published, there will be other papers on particular aspects of ME/CFS – substudies – that other NIH researchers will publish. Some of these papers have been finished for a year, two years, maybe longer, but Avi made the researchers hold them back until his main synthesis is published. Dr. Nath:
“However, everything cannot go into a single manuscript, so there are several other manuscripts that are going to come out. Each one of them is going to take a piece of it and describe it in more detail. So a second manuscript on muscle alone is already gone out and is under review, and there will be one on the microbiome and so on. So there are going to be a whole host of manuscripts coming out as soon as the first one gets accepted for publication…
All of this was done on 17 (not 18 as I said yesterday) patients. It is BIG SCIENCE done on a small group. The amount of data generated is mind-bogglingly incomprehensible.
The NIH also pledged that after this study finished, they would:
- Develop biomarkers
- Evaluate treatments
Last year, Dr. Nath said
“It was important to convince ourselves that there really are biological problems that are reproducible and consistent and to develop expertise to study ME/CFS, because we hadn’t looked at it before. Then we will move on to treatment studies. We have a number of different candidates [drugs] we would like to try.”
“…We’re also keen on trying to see, based on these observations, if we should try to conduct some pilot clinical studies, clinical trials, here at NIH. So those things are currently in the process of discussion.”
More details here: https://www.s4me.info/threads/usa-nih-nati
So, when this study is published, the patient community needs to remind Dr. Nath, NINDS Director Walter Koroshetz, and new NIH Director Monica Bertagnolli (nominated) that their work on ME/CFS – a not uncommon illness – has just started.
The NIH held a video call for the #MEcfs & #LongCovid community. Dr. Nath confirmed that several (or many) papers are done and will be published soon after the study’s first paper is out. He also confirmed NIH is discussing treatment trials for ME/CFS. (Thanks to the folks who listened and transcribed the call).


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Thank you for this, Cort! And thank you Brian for sharing!
As a quick aside related to ME/CFS & Long COVID, did you see by chance that Minnesota Legislature just passed state funding for this patient community (they are just waiting for the Governor signature now)?
Just wanted to share here, if not.
From the Minneapolis Star Tribune: https://www.startribune.com/minnesota-lawmakers-set-to-send-mayo-friendly-health-budget-nurse-staffing-bills-to-governor/600276887/?refresh=true
‘The HHS bill includes research into long COVID and support for people suffering from the post-pandemic condition.’
The HHS bill that has passed to the Governor’s desk is providing dedicated funding measures set aside for Long COVID & related conditions, in which the language names ME/CFS, Dysautonomia & POTS in the bill.
This is the bill text (you can search ME/CFS or Long COVID): https://www.revisor.mn.gov/bills/text.php?number=SF2995&version=latest&session=ls93&session_year=2023&session_number=0
This is the budget spreadsheet: https://www.house.mn.gov/comm/docs/EuPosUxQM0mJhGZyc4gz_A.pdf?fbclid=IwAR2YrGkgfVTIkGY8fwsQZolxkwLI6z6VEnvdxEw5bjPFORZw-pOQz-z5sMo
Per the budget spreadsheet, it looks like the Minnesota Department of Health will be allotted $3.1M per year for the next 4 fiscal years to help address the laid out gaps in the bill for this patient population.
Do you know if this type of funding allocation has been given before for ME/CFS (or Long COVID) to a State Health Department? Feels like a fairly big deal / win for the community (even if not federally, but at least from a state level).
Just wanted to highlight to you if you hadn’t seen.
Whoa! How did that happen? I feel confident that nothing of that scope has been done before. I would love to know how that happened…
I know that Minnesota ME/CFS Alliance and #MEAction Minnesota have been making a lot of inroads with Minnesota legislation, meeting regularly with state leadership.
I also have heard that Kate Murray, Long COVID & Post-COVID Conditions Manager at Minnesota Department of Health was instrumental in raising to the forefront to local officials.
(Press piece that featured her work: https://www.kare11.com/article/news/local/kare11-extras/unveiling-long-covid-19-disparities-highlighted-once-again/89-518bf48c-a739-4142-bd17-7045ab6b6cdf)
May be worth amplifying to the community so other states could see as a model!
Thanks Cort.
I can’t even remember which patient selection criteria they used. I know viral onset (which is probably the right thing to do if you’re doing a very small but extremely detailed study) was necessary, but was it CCC plus other things or was it possibly not strict enough?
Study criteria were very strict: “The study was unique in that after the extensive work-up in visit 1, five outside ME/CFS expert clinicians reviewed each case to decide if the patient fit all the published criteria for ME/CFS. This was quality control, to ensure patients really had ME/CFS. Three patients of the initial group were found to have other diagnoses – one had Parkinsonism, one had a rare (and fatal cancer), and so they were excluded from the second phase of the study.”
True, thanks for unfogging me. I now remember that from your post on a different platform (possibly Twitter or Mastodon). The selection criteria indeed look very good.
Hi Brian Vastag, are you able to see what rare type of Cancer this patient was found to have? Could it have been AML or a type of stomach Cancer? thanks very much.
Tulane University Hypermobility Clinic & Neuro Science recently found in EDS Long COVID & ME/CFS Folate issues mutations in genetics using methyl Folate Methyl B-12 A1298C & C677T they Published in Heliyon in April 2023
Hi, I don’t know what kind of cancer the patient had.
ok thanks Brian, I was also recently diagnosed with this it has 3 names used. (PND) Paroxysmal Nocturnal Dyspnea/Orthopenia/Dyspnea. The majority actually are in heart failure or could be other things numerous ones like Myasthenia Gravis, (Anemia B-12) anxiety, etc…
I get really bad shortness of breath & mucus issues while sleeping I awaken my blood pressure goes tachycardia/bradycardia when I was in the Emergency Room a few days ago my pulse was dropping to under 50 & up to157 my oxygen is good at 99%
my ECG shows also numerous ectopic beats, a recent CT Contrast found an issue in ascending aorta a dilatation is now being watched.
They thought I was having a heart attack they called CCU right away and then did numerous blood and heart tests all were ok.
When healthy people sleep the heart controls the mucus in this it gets worse & causes congestion & suffocating feelings waking one up
Aidan, I literally just read about methyl Folate genetic mutations. Interesting take, as I also met diagnostic criteria for hEDS. Lots to learn!
Yes, very interesting findings, I also left another comment above on my heart something found a few days ago.
Also on Twitter today someone mentioned back in 2019 a team of anesthesiologists found in 23 Fibro patients they have insulin issues with the long 3-month diabetes test they have resistence they use the diabetes pills now.They published some time back in 2019 I do not have the details yet in Plos One
It is mold illness. Has ANYONE linked toxic mold aka Stachybotrys to this? Blows my mind how no one seems to understand this is an environmental illness.
Shame on the medical field for dismissing this core information.
Oralie – I’ve read a lot about mold illness, heavy metal toxins, tick-bourne illnesses, etc. but it’s published under alternative medicine docs! They are screaming at the top of their lungs, and yet the medical community dismisses it! Health insurance coverage is not existent & big pharm wants to continue the ineffective Guinea pig approach to treatment! I refuse to take another pill until someone listens!
I was cringing at the assessments the study put you through! I honestly can’t see how MECFS patients could keep up?! Did any become bedbound during the study? Then again, my norm is to hoard spoons to survive! Lol
This is a great question because the answer demonstrates just how rigorous Nath was with this study. I’ve never seen anything close to the rigor that was employed to ensure that everyone had ME/CFS. This, in fact, may be the only study in which we can be sure that everyone in it had ME/CFS.
I believe you needed to be sick a relatively short duration too. I tried to apply to the study and was told I had been sick for too long a period.
Yes, I don’t remember the timespan but it was short and your ME/CFS had to be triggered by a documented infection.
Perhaps what I call the “snowball effect”? A simple cold could turn into bronchitis, pneumonia, pleurisy, ultimately landing it the vicious cycle of what I’ve now come to know as CFS?
They only allowed post viral patients in the studyl? Has ME/CFS become a post viral illness and ended up in that ICD code?
Five years
I look forward to this study however I still have many questions. Stanford’s ME/CFS clinic had a huge proportion of people with Ehlers-Danlos. So is EDS included or excluded in any kind of ME/CFS study? I also wonder if the NIH looked at patients’ genetics; it wasn’t mentioned directly in the article.
And what was the fatal cancer of one of the subjects? Recently I got a lab that indicated an M-Spike (monoclonal antibody) in my blood–which is abnormal. About 7%, more or less, of people over 70 have these proteins which may morph into a blood or plasma cancer. Most people don’t know they have this because it is USUALLY symptomless and the test is somewhat exotic. One fatal cancer it can become is multiple myeloma. If there are symptoms, they can be very much like ME/CFS. This makes me wonder if there may be some folks unknowingly walking around with these abnormalities. The probability, after an abnormal test (depending on a lot of other factors) is about 1 to 2% per year of getting full blown myeloma. I’m not sure how long I have had this abnormality, but I do wonder if it is related to my ME/CFS fatigue.
I did not hear if any of the patients were diagnosed with EDS. If they were, they were not explicitly excluded.
I’m not sure what kind of rare cancer that one patient was diagnosed with.
Yes, they did whole genome sequencing on us. My list of tests and experiements is not exhaustive; they did so much stuff with our samples.
Thank you Brian for helping out the ME/CfS community. Hopefully these six years will bring some good information to light.
I was really struck again by how comprehensive this study was. I had forgotten about this stuff:
Do metabolic studies on neurons made from patient blood stem cells
Study humanized mice made from patient stem cells
To determine if cerebrospinal fluid or antibodies injected in brains of rodents or humanized mice generated with cells from patients can lead to fatigue or behavioral abnormalities.
I wonder if they were able to do them? I sure hope so.
wish they had included two more sets of mice– one fed salivary extracts and one fed whole blood samples from patients, in addition to mice’s regular diet.
(and using SCIDS mice– missing immune system)
I had viral encephalitis over 56 years ago. It completely altered my life. I had COVID twice. Personally I don’t care too much what label they attach to the effects of these viruses because as a survivor I only hope for successful treatments for those patients suffering from the very similar conditions resulting from these infections. My heartfelt thanks to all the patients who participated in these grueling trials- I know- we know- what you likely experienced. And particularly you, Brian, for the leadership and courage you displayed. You are a hero. And thank you Cort for all your efforts to help this community.
Wow ! A ray of hope ! Thank you Brian for “lending” your body to the cause. That must have been a long and difficult 5 weeks.
Cort, thanks again for keeping us informed !
Even though my trigger was toxicity VS viral ,I believe there will be useful information and increased understanding of the various mechanisms involved for all .……Now we have to wait while this potentially valuable paper “slow crawls” it’s way to publication. (Silent scream)
Wow….just WOW, what a blog this is! I suffer with Long Covid, and have been diagnosed with ME/CFS and this blog rang so true for me. I never have had a positive Covid test because I was hospitalized before this country was immersed in testing and vaccinations, but I certainly fit the Long Covid profile and have been increasingly sick for over 3 years. I sincerely hope that these studies will be published as soon as humanly possible because I would love some answers to all my questions and symptoms!
Nath said the study was a success – we just don’t what that means 🙂
https://www.healthrising.org/blog/2022/05/06/nath-intramural-study-exercise/
Yes! That is my impression from this text, that they at least found something enough important despite the small, very small, cohort. Maybe that some of these studies are possible to compare to other studies also. As I understand it reproducability (darn spelling!) and comparability are two very important things right now.
At least thats what our authorities here i Sweden claims is needed to being able to establish national health care treatment recommendations. As our systems are so different from each other that was a hard translation to do, and I hope that it is translateable that way.
If science do not perform comparable and confirming/repruceable research in earnest we will still waddle around in murky waters and get nowhere.
I do so hope that long Covid and ME (all types of onset) can thrive, uhum … , from each other. At least the deconditioning is out of the question when comes to long Covid, and shear impact should also exclude patients beeing “neurotic” or malingering.
There are, though, studies within the psychiatric area that implicates, or even shows, biological changes in those diseases/illnesses. Who, today, blame autism/adhd/schizophrenia etc on parenthood?
Thanks again!
You would think deconditioning would not be a issue with long COVID but here’s the RECOVER Initiative producing an exercise clinical trial for …what reason? The only thing that I can think of is deconditioning…
Deconditioning is certainly out as a cause of ME/CFS – the exercise studies show diametrically opposed results to what deconditioning produces
https://www.healthrising.org/blog/2018/12/16/deconditioning-denied-chronic-fatigue-syndrome-deconditioning-myth/
I don’t see any reason, yet, for the ME/CFS-like subset of long COVID to be differentiated from ME/CFS. Let’s hope it stays that way and both conditions benefit from each other.
Yeah indeed! But maybe they sort of have to do that, and hopefully it will also build confidence outside ME/CFS territory to totally dismiss it finally.
Even if they find out that it is different from ME, several new concepts and methods have further developed. And alot of minds have opened up for similarities and that what we tell our doctors actually can exist.
Even I have noticed a change, even within myself, when certain facts has been revealed. I’m not crazy, I’m not lazy. What I have exists …
Brian, thank you to you and the 16 others for subjecting yourselves to such grueling testing. I view this as a sacrifice not unlike being a service member; advancing scientific understanding in some cases to your own detriment so that many millions may eventually benefit is selfless and honorable. And we know so many more of us would be willing if we weren’t so sick.
It is hard to sustain too much frustration at individual researchers within big government bureaucracy. One person may have the motivation to push themselves and their work faster, but it only takes one cog in the machinery to slow it all down, and unfortunately the government is full of cogs that can’t turn without most of the others around them. I don’t say this to excuse what we should have had years ago; just to say it’s often out of any one person’s hands. Looking forward to what these various studies will tell us. Thanks again!
Thank you Brian for going through this exhausting study for all of us!
Brian, you mentioned you had a difficult spinal tap. Can you be more specific? I’m interested as I had ME/CFS symptoms due to a spinal CSF leak. Did any of these tests measure your CSF pressure outside of a spinal tap (perhaps with ICP monitoring)? Did symptoms occur during the tap or worsen after in any way?
I have had two spinal taps in my life, the first was in 2013 at Johns Hopkins. Both were difficult for the person trying to draw fluid. I ended up having the NIH spinal tap under fluoroscopy (live Xray) and Nath said I had ‘unusual’ spinal anatomy.
I do not recall any symptom exacerbation with the spinal tap other than the lingering discomfort from the needle but I was generally pretty exhuasted for the whole visit.
I did not get CSF pressure measured.
Thanks, Brian. I find this connection more than interesting. Did your ME/CFS start or worsen within a year or so after that initial 2013 spinal tap? Over time, a slow leak can lead to brain sag which puts pressure on the brain stem (so this could potentially be a driver for a lot of your symptoms).
Either way, I would strongly recommend finding a leak specialist to do spine and *leak specific* imaging to see what’s unusual about your spine. There’s a directory of experienced specialists here: https://spinalcsfleak.org/directory/
No my symptoms did not get worse and I did not have a spinal fluid leak.
You find my story here as well, it was posted a few weeks back and titled A Patch On It.
Thank you Brian for those horrible research, must have been terrible. The unusual spinal anatomy does it look like
( a mild?) case of Scheuermann’s disease?
https://en.wikipedia.org/wiki/Scheuermann%27s_disease
Thank you to Brian and fellow ME/CFS patients who were courageous enough to submit to this array of gruelling tests knowing that they would likely impact significantly on their health. What a wonderful thing to do for our community. With this in mind I was distressed to read of the “back burnering” and other delays. When people are significantly sacrificing their quality of life for scientific benefit it is shocking that such a study can be stalled and the results still be only drip fed some 6 years later . This aspect of the project alone should be in the national press! Nevertheless all credit to Dr Nath & colleagues who took on the research and who no doubt have many demands on their time. God forbid any of them or their loved ones should comes down with this life stalling illness, it gives a whole new perspective on the need for research.
It was unfortunate, indeed, to have the study back-burnered and ultimately ended short of its intended enrollment. Then again, the pandemic did that with virtually everything. The NIH was also about to start on a strategic plan for ME/CFS and that got postponed until a couple of months ago. Thankfully, the ME/CFS study did birth Nath’s similarly intense long COVID study! In the end, I hope and think it will work out OK.
Thank you Brian for putting yourself up for what sounds like an exhausting process. This is the kind of comprehensive study I feel should be done on all sufferers. The fact that other causes were found is important in weeding out those people and hopefully with the right treatment they could be helped. Then with all who are left completely meeting the criteria it gives a more concentrated study. I wonder why the study was only open to people who had only been sick for a short time but I guess after longer period other things could be showing up. I hope though that people with longer duration of illness and severity will be studied in the future. I am excited to see the results and I hope that they keep pushing with similar studies.
Nice to see this kind of high-quality research. Unfortunately a small group. I look forward to the publications. It gives a little bit of hope. By the way, is anything known about the publication of Prusty et al? I saw his lecture in Berlin. A new biomarker was not clear to me in his presentation. Anyone?
I can’t believe how much you and the other participants went through – thank you so very much. Excited for the results!
While I am encouraged by the fact that this study was done, having only 18 participants is depressing. Many, many studies have been undertaken which say that due to a small cohort group, more follow-up studies would be required, and they die there. I’ve been ill for 31 years, and have become jaded about small studies. The fact that even the NIH has used such a small group suggests to me that there won’t be any treatments soon. I hope I am wrong. But, thanks go to Brian and Cort for sharing a glimmer of hope.
This is the great question. A much larger patient group was envisioned but the pandemic thwarted that. We’ll see how much it slows things down. The NIH could say – well we need a larger patient group and sit on their hands – or rhey could recognize that the pandemic got in the way – and say we owe these people they’ve waited long enough – and take a shot at clinical trials and fund more studies.
The one thing this study had that others have not, though, is it’s oh, so rigorously defined study group. That should help. Time will tell.
Huge thanks for your resolve and endurance. One has to hope that eventually there will be helpful outcomes for all of us who suffer these disabling life-wrecking symptoms.
I took part as a subject in the PACE trial in London UK in the 90s. This was a flawed study unfortunately, dismissed by peers and subjects.
I asked my GP why I felt so ill way back in 1960s. He said I was malingering, but did send me to a physician and then a psychiatrist for evaluation. None of them had any idea and thought I was making it up. Sadly I have not had any more positive help in the decades since, in UK, Australia or USA.
My cousin in Canada has had similar experiences, and we despair that any progress will help us after six decades of struggle.
Patient recruitment was slow because patients were mortified at the very thought of undergoing exercise tests. Just getting up to go to the bathroom is exhausting enough!
You just gave me hope!
Thank you all 🌹
Patient # 3 – Jennifer Vaughn Caldwell – commented on Facebook.
Patient #3 here. During the NIH stay, participants were administered multiple questionnaires. Based on my answers, a “vitality” score was generated. My vitality score was a 6 out of 100, which is a measure of how this disease has literally sucked the life right out of me.
As a single mom with no one to help out and no money to pay for help, it’s been incredibly hard to stay afloat with so many obstacles and devastating symptoms in my path. Like Brian, I once had a fulfilling career. I was a Clinical Research Coordinator at a university medical center for 17 years. Never once did I see a patient as debilitated as we are be dismissed, belittled and neglected until it happened to ME. I am traumatized by the way I’ve been treated by medical “professionals” over the years.
Six years since patient enrollment began, we remain incapacitated as we continue to wait for the support and treatment we desperately need and deserve. May this long awaited paper finally bring some answers and the abuse our patient community has endured to finally stop.
My daughter misses her once fun loving, spontaneous, and full of life mom. I miss her, too
Very well told story and I appreciate your efforts more than words!!! I’m new here, so please excuse while I vent…
I was already home bound and teleworking full time pre-COVID, and it was an interesting perspective to observe the world complain about COVID, the unknowns, aches/pains, serious medical effects, violation to rights to freedom (lock down), converting the antiquated FedGov to SOP online & thriving, etc. etc. I’m not exaggerating that the newly developed business practices during COVID lockdown have excessively improved my ability to telework. Oddly, I also gained a new compassion from coworkers who could not hear it’s a lonely existence and I’d much prefer to be in the office!
My point? How many people does it take to suffer in pain, experience a deteriorating quality of life and/or premature death before there is appropriate funding and focus to help? I guess a post-pandemic, Long COVID population experiencing signs of ME/CFS?! The insanity needs to stop… please!
I literally got diagnosed with everything under the sun over the past 20+ years, including Long COVID, before a CFS diagnosis this month. I’m in the severe, home bound stage! While struggling in the mild stage to keep up with life and ultimately tapping out of work at moderate stage, I was simply NOT HEARD! Worse yet, referred to therapy! Medical gaslighting is another huge problem where our society turns a blind eye! Wrapping my brain around it all is mind-boggling!
We all have our stories, and it’s beyond unethical to be continually dismissed moving forward! Any societal norm to turn a blind eye is simply evil! Perhaps we should all join hands across DC, and hope the word gets out to National News? I’m dumbfounded why we don’t matter, and pray for every single one of you suffering!
Colt, your website and articles has some of the most informative MECFS information available! I feel blessed to have found this resource and truly appreciate you!
Brian, that study sounded like absolute hell, I’d be one of them bedbound for trying! It’s beyond inspirational you stuck it out!
Rant over. I hope to read many more articles to educate myself! Again, thanks to all the like minded folks and bless ya all!!!
anesthesiaexperts.com Fibromyalgia: Is insulin resistance the missing link? I heard they use diabetic pills in patients found in 23 patients.
This was mentioned on Twitter by Christina her link is @Christina4hope.
Posted today 12:37pm June 6, 2023 this work was from 2019 and published in Plos One
Brian, I just want to say THANK YOU for your service to the ME community — not a lot of us could withstand being part of such an intensive study. I feel grateful to all of you who subjected yourselves to that. Thanks also for sharing all the valuable info, and for all of your ongoing advocacy. It really means a lot.