Postural orthostatic tachycardia syndrome (POTS) has always been thought to be the big deal regarding orthostatic intolerance (increased symptoms while standing or sitting) in chronic fatigue syndrome (ME/CFS).
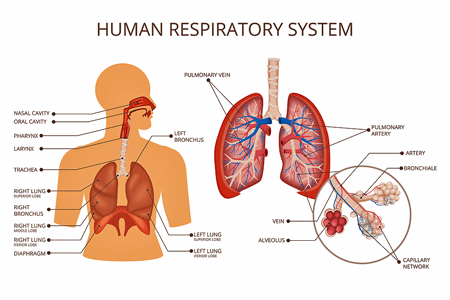
Something is definitely off in the respiratory systems of quite a few people with ME/CFS.
That may be changing with a recent study, “Physiological assessment of orthostatic intolerance in chronic fatigue syndrome“, from Dr. Benjamin Natelson MD at the Icahn School of Medicine at Mount Sinai, and Elizabeth Unger of the Centers for Disease Control and Prevention (CDC). One had the feeling that Natelson – one of the first to uncover hypocapnia in ME/CFS – has been thinking the condition (low carbon dioxide levels in the breath) has not been given its proper due. If so, he’s probably right.
It’s not that it hasn’t been popping up – it has been. Systrom has found it in his invasive exercise studies, the Visser team found it during tilt table testing, and Naschitz also found it in his exciting run of ME/CFS/FM Israeli studies fifteen years ago. (Naschitz described it as “common” in fibromyalgia.). I imagine that name recognition is pretty low, though.
Hypocapnia has never been found in everyone with ME/CFS/FM, but it appears to be present in a substantial subset. Natelson and Mancini also found it during exercise testing, and Novak found it during tilt-table testing in people with long COVID.
The Study
The Natelson/Unger study brought something new to the game: unlike the Lee-Bateman study of two years ago, it also measured the incidence of hypocapnia.
These studies findings were boosted by the fact that Natelson tested each of the 63 ME/CFS patients in the study three times over a three-year period using the NASA Lean Test.
He measured respiration, heart rate, blood pressure, and carbon dioxide levels (eTCO2) twice while the person lay supine, and then once a minute at they remained standing while leaning against the wall.
Hypocapnia was defined as having an eTCO2≤ 32 mmHg. (Since normal eTCO2 is 40mmHg, that drop – 20% – is pretty severe.) Postural orthostatic tachycardia syndrome, or POTS, was defined as a heart rate increase ≥ 30 beats per minute (BPM) during the lean, and orthostatic hypotension (OH) was defined as a drop of systolic pressure ≥ 20 mmHg from baseline levels during the lean. Tachypnea was defined as a respiratory rate of 20 or higher breaths per minute—either while lying supine or while leaning.
A Critical Test
“We recommend that all ME/CFS and Fibromyalgia patients have a NASA 10-minute Lean Test to assess for orthostatic intolerance.” The Bateman Horne Center
The NASA Lean Test constitutes a potential breakthrough for ME/CFS, FM, POTS and long-COVID patients because it provides an easy way to diagnose orthostatic intolerance – something many doctors know little about – and quickly potentially provides a biological abnormality for the doctor.
No need to somehow find a tilt table near you – at its most basic, the test simply requires an exam table, a pulse oximeter (placed on one hand), a blood pressure cuff (placed on the opposite arm), and about 20 minutes.
First, the person rests lying down for 10 minutes, then she/he stands up, and with her/his heels 6-8 inches from the wall, and shoulder blades touching it, stays there for ten minutes (or until it’s clear they have OI). All the while, heart rate, blood pressure and symptoms are recorded.
The conclusions of the Lee-Bateman NASA Lean ME/CFS study were right in line with what we knew about the incidence of orthostatic intolerance in ME/CFS: it mostly occurred in the form of postural orthostatic tachycardia syndrome (POTS) (@40% of patients).
- Check out what one person learned from their NASA Lean Test at the Bateman Horne Center
A POSH (Postural Orthostatic Syndrome of Hypocapnia) Disease
As was noted earlier, the Natelson/Unger study was different in that it measured end-tidal CO2 and looked to see if low CO2 levels (hypocapnia) were present.
About 60% of the group had at least one abnormality, and 80% of the time it was POSH. Eleven people even exhibited POSH while lying down. POSH is often associated with fast breathing (tachypnea) or fast and deep breathing (hyperventilation), but this was not the case in this study. Instead, Natelson found his patients experienced hyperpnea, or deeper than normal breathing. (Other studies have found hyperventilation.)
Hyperpnea often occurs in response to increased metabolic demand, i.e., during exercise, when our cells need more oxygen. Systrom has found that people with ME/CFS hyperventilate (breathe deeply/rapidly) during exercise —perhaps in an attempt to get more oxygen into their mitochondria.
Although the authors didn’t mention it, one wonders if an oxygen deficit in the mitochondria, even at rest, could trigger deeper breaths in some people with ME/CFS.
CO2 is often considered a toxic byproduct of energy production, but low levels of CO2 can cause problems.
The sympathetic nervous system activation we see in ME/CFS/FM and long COVID could also potentially contribute to the hyperpnea and/or hyperventilation found in ME/CFS. Conversely, because it appears that overbreathing can trigger sympathetic nervous system activation, achieving a healthier breathing pattern might help tamp down the fight/flight system.
Overbreathing/hyperpnea/hyperventilation (all cause similar symptoms, and all produce low CO2 levels or hypocapnia) can produce symptoms such as dizziness or lightheadedness, shortness of breath, abdominal bloating and belching, fatigue, feeling weak, cognitive and sleep problems, numbness and tingling sensations, muscle spasms, chest pain, and palpitations.
Interestingly, a sudden onset of the illness, probably an infectious event, was significantly more common among the patients who demonstrated some abnormality.
Check out a 2025 Interview with Dr. Natelson
Hypocapnia
Hypocapnia refers to low CO2 levels in the breath or blood caused by overbreathing, hyperpnea (deepened breathing), tachypnea (rapid breathing), or hyperventilation (deep and rapid breathing).
Normal breathing is actually “small and light” and is barely perceptible. Compare the 10-12 breaths/min in normal breathing to the over 18 breaths/min in a person with hypocapnia. People with hypocapnia often move 2/3rds more breath in and out of their lungs than people normally do (10 L/min to 6 L/min).
Whatever the problem (hyperpnea – deeper than normal breaths; tachypnea – more rapid than normal breaths, or both) the problem is the excessive movement of air out of the body. (This is presumably why the slow and deep breathing found in some yoga practices does not appear to be a problem.)
Doctors are generally taught that hypocapnia in an otherwise healthy person is a sign of anxiety, but the Generalized Anxiety Disorder 7-item questionnaire given didn’t indicate that the patients with hypocapnia were more anxious than the patients without it.
New Forms of Orthostatic Intolerance Popping Up

Peter Novak, MD, PhD, has been making the invisible visible.
Peter Novak, a board-certified neurologist, and autonomic nervous system specialist at Brigham and Women’s Hospital in Harvard, is right in the middle of the ME/CFS/POTS/Lyme/Long-COVID soup. He’s become something of a specialist in making the invisible visible and uncovering new forms of orthostatic intolerance.
After linking hypocapnia to reduced blood flows to the brain in his own strange group of patients, he called the new condition “hypocapnic cerebral hypoperfusion”. Like his colleague David Systrom, Novak was being handed patients who just didn’t fit the mold. In Novak’s case, he was getting patients who had all the symptoms of POTS but who didn’t experience heart racing upon standing.
Novak had a long list of possible causes (baroreceptor problems interfering with “respiratory drive”, compensation for metabolic acidosis, orthostatic ventilation-perfusion mismatch, problems with the respiratory centers in the brain), and is digging deeper into this condition.
The Gist
- This is the first of a series of blogs on breathing and ME/CFS/FM and long COVID.
- Dr. Natelson did the NASA Lean Test on people with ME/CFS three times over three years. He tested heart rate, blood pressure, and CO2 levels.
- Contrary to perceived wisdom, Natelson found that hypocapnia (low CO2 levels) was the most prevalent orthostatic abnormality found. It was far more prevalent, for instance, than postural orthostatic tachycardia syndrome (POTS). Hypocapnia was even found in some people when they were lying down.
- Hypocapnia is often a result of hyperventilation, which is characterized by rapid and deep breathing. Natelson found little evidence of rapid breathing; instead, he consistently found deeper than normal breathing. Natelson et al. called the condition POSH (postural orthostatic syndrome of hypocapnia).
- We breathe more rapidly and deeply to get more oxygen to our muscles, and to remove CO2 from our blood, when we exercise. Exercise, however, was not a factor in this study.
- Normal breathing is light breathing; it’s barely perceptible.
- Other forms of orthostatic intolerance have recently been uncovered by Peter Novak MD, PhD of Harvard. Novak found hypocapnia was linked to low brain blood flows in a condition he called hypocapnic cerebral hypoperfusion.
- Novak also uncovered a condition similar to what the Visser team has found in ME/CFS. In orthostatic cerebral hypoperfusion syndrome (OCHOS), low brain blood flows are found in the absence of increased hearts rates or drops in blood pressure.
- A long list of possible causes (baroreceptor problems interfering with “respiratory drive”, compensation for metabolic acidosis, orthostatic ventilation-perfusion mismatch, problems with the respiratory centers in the brain) may be responsible for these conditions.
OCHOS occurs when someone has reduced blood flows to the brain in the absence of any other identifying characteristics; i.e. no increased heart rates (POTS), no decreases in blood pressure (orthostatic hypotension), no heart issues – just dizziness upon standing – which has surely got many of us of a psych label.
Novak’s findings seem similar to those of the Visser/Van Campen/Rowe team when they used a new, more accurate technique to assess blood flows in ME/CFS.
Novak believes that a reduction of blood flows to the brain is a core characteristic of all forms of orthostatic intolerance. Given the Visser team’s finding that everyone with ME/CFS also exhibits reduced blood flows to the brain, ME/CFS must be considered, among other things, an orthostatic intolerance disorder.
Novak also found that orthostatic intolerance, dysautonomia, and small fiber neuropathy were common in long COVID, and was the first one to identify small fiber neuropathy in post-treatment Lyme disease. In short, we’re lucky to have this skilled and respected (he’s the chief of the Division of Autonomic Neurology at Brigham) researcher focused on these areas of concern in ME/CFS/FM/POTS and long COVID.
Treatment Possibilities
Treatment Takeaways
Treatment possibilities include:
- Increasing blood volume by using oral rehydration salts, and compression hose
- Having respiratory therapists use biofeedback techniques to try to reduce the depth of breathing.
- Abdominal breathing (done slowly), breathing through pursed lips, meditation, mindfulness, relaxation exercises are recommended. We’ll check out more breathing options in this series.
- Check out how to do an in-home test for hypocapnic hyperventilation – A Home Postural Hypocapnic Hyperventilation Test for Chronic Fatigue Syndrome and Fibromyalgia
The authors also suggested having respiratory therapists use biofeedback techniques to try to reduce the depth of breathing.
Deep breathing exercises are not suggested in hypocapnia unless done slowly (Pranayama). Otherwise, abdominal breathing, breathing through pursed lips, meditation, mindfulness, and relaxation exercises are recommended. We’ll explore more breathing exercises in this series.
- Check out how to do an in-home test for hypocapnic hyperventilation – A Home Postural Hypocapnic Hyperventilation Test for Chronic Fatigue Syndrome and Fibromyalgia
The Natelson Files:
- Dr. Natelson will be featured in the March 28th NIH Telebriefing from 3:00 – 4:00 pm ET. Preregistration is not required.
- If you’re in the New York City area check out two of Natelson’s ongoing ME/CFS studies.
- A several million-dollar, 120-person study at the Icahn School of Medicine at Mount Sinai University In New York City will include severe and non-severe ME/CFS patients, and healthy controls. IThey have funds to help participants with travel expenses and time spent (but not airfare). To find out more, call the Pain & Fatigue Study Center research staff at 212-844-6665.
- Natelson’s unique study to see if a rocking bed can improve sleep is also open. If you live in New York City and want to see if this unique kind of nap can improve your symptoms check out this study.






Cort, this is fascinating. Thank you so much for the work you’re doing.
Really interested to read your next pieces on breathing. Breathwork/vagus nerve activation (not sure if that’s the right term!) are things I’m currently looking into, in the hope they might help.
I’m looking into it for myself as well. I’m pretty darn sure that my breathing is off. I used to say I haven’t taken a deep breath in decades.
Are you aware of the Bohr effect Cort. Oxygen can only be delivered to tissue when there is enough c02 to push the oxygen off the red blood cell.
I’ve practiced buteyko for a long time. The aim is to recalibrate the co2 sensors in the neck and brain that measure levels of co2 in the blood.
What buteyko does is increase c02 in the bloodstream..till those sensors adaot to higher levels. This in turn will allow more co2 into the tissue.
You can have high oxygenation in the blood and low tissue oxygenation from iverbreathing.
The Bohr effect seems paradoxical but is well known
Interesting
Ray peat has also talked about breathing into a paper bag as one way way to raise C02
https://www.functionalps.com/blog/2012/09/26/ray-peat-phd-on-carbon-dioxide-longevity-and-regeneration/
This is very interesting and may help explain an unexpected, if subtle, theme I observed in responses to my retrospective survey on high-dose thiamine. A number of respondents reported reductions in heart rate variability and improvements in their POTS symptoms. (I hadn’t anticipated that high-dose thiamine might help with orthostatic symptoms, so didn’t specifically ask about it; these were spontaneous reports.) One potential explanation is that carbonic anhydrase inhibitors produce carbon dioxide. So if high-dose thiamine operates as a carbonic anhydrase inhibitor in vivo as predicted by in vitro studies it could potentially help to address hypocapnia and some of the related orthostatic symptoms. (Nearly 100 respondents have now respo;nded to the survey, with results that are largely consistent with my earlier write-up.) Not a panacea, but could potentially help as an adjunctive treatment along with other treatments. See https://www.healthrising.org/blog/2021/04/15/thiamine-b-1-chronic-fatigue-syndrome-fibromyalgia/ and https://www.healthrising.org/blog/2021/06/02/fibromyalgia-chronic-fatigue-syndrome-benefit-high-dose-thiamine/
I have been on the high dose thiamine track but recently realised it was a chronic cellular magnesium deficiency that was impacting as a Co-factor. I don’t think so much is needed when the magnesium issue is fixed. I was taking an oral magnesium supplement and TTFD with magnesium but the big shift was when I started utilising magnesium chloride. I think the root problem May be with the magnesium.
Thiamine greatly increases oxygenation of tissues which is why I think at high doses it works so well. I think the magnesium deficit is causing the cellular hypoxia in the first place. At least the science checked out for me and I was bedbound with OI and these breathing issues. I also had issues lying down. I was having seizures. 1 week of ionic magnesium chloride and I’m up and about again. It’s early days but the symptomatic relief has been miraculous so far.
Nat — Glad to hear of your progress! I agree that having an adequate amount of magnesium is important and that supplementation can be helpful. Under my hypothesis of the mechanism for high-dose thiamine, I also agree it is treating symptoms rather than root causes — producing CO2, which increases oxygen through Bohr effect, and reducing intracranial hypertension by reducing CSF flow. The theory of high-dose thiamine proposed by others argue it is addressing a problem with the active transport mechanism for thiamine, so they might argue it is going further upstream and directly treating a key breakdown in cellular biochemistry.
Dear Nat, may I ask what you mean by “ionic magnesium chloride”? An oral supplement, or like intravenous drip feeding? Thank you!
Quite excited about this (thank you Cort!) but also confused. I am a moderate-severe CFS person with orthostatic intolerance. I can’t sit up for more than 30 minutes without going light headed. I also take a lot of slow deep breaths after exertion as I unconsciously feel the need for more oxygen.
So does this research mean I have hypocapnia? And is the treatment to try to intervene and stop taking those deep breaths?
Not quite clear on how to use this new finding
Dr. Novak is responsible for a friend’s permanent brain damage, who he wrote off and left with no support, and what was written in his record prevented him from getting help at MGH – he was treated as a psychiatric patient and given no medical help. Neurologists elsewhere have diagnosed the damage at the hands of Dr Novak. Many other ME/CFS patients have found him to have horrible bedside manner. This was reflected in his reviews, before the bad reviews mysteriously disappeared….
so so sorry for your friend! I had and am still suffering from it also an un needed, fals treatment with specialist who they later throw out of an university hospital. It is so cruel how some specialists can severelly damage people and get away with it. And yes, here in my country it is known, but to late. but now he even works for a long time also in the US. And there noboddy knows of his history.
I have these symptoms so badly I am bedbound with OI and have seizures due to cerebral hypoperfusion. Oral and transdermal bicarbonate’s (sodium, potassium, magnesium) really work well for me in increasing co2 and reducing symptoms. I believe chronic magnesium deficiency to be the root cause (in my case at least) and supplementing has been the only time I have fixed this hypocapnic issue and felt I could breathe with zero fatigue. Its early days but so far it’s been miraculous.
Hi Nat, What products do you use and where to get them? Thank you.
Magnesium chloride orally. I buy mine from Amazon but it’s made in the U.K. so May not be available worldwide. It’s liquid so if gastric motility is an issue ( as it is for me) it’s pretty much directly absorbed. Unfortunately I picked up a virus which totally knocked me out and tanked my mg levels again and I’m still recovering/starting again. Like the thiamine I realise the trick is to try and maintain a constant level at least of ingestion. An IV would be amazing to measure/achieve this so I try to do this by putting in a litre of water and drinking it throughout the day. Like thiamine it can also make symptoms worse so it takes some time to start low and slow and build. After about a week or ten days I begin to have amazing days (where I am at around now) where my energy and breathing is much better. I’m personally now leaning towards baroreceptor dysfunction as root cause of OI sunrooms but mineral and vitamin deficiency as the cause of that, maybe magnesium. I have had chronically low blood pressure my whole life which tanks and then immediately shoots up on standing. OI symptoms didn’t become disabling until after I had my daughter.
As a side note I’m pretty sure my hypermobility is better since taking the magnesium too. I can no longer do thumb to wrist without a bit of resistance and it even hurts a bit! I noticed the other day. I think the SGB May fix the baroreceptor dysfunction but it could recurr if the deficiencies are still present. I am unable to have the Stellate Ganglion Block right now but plan to a soon as I am able. I found a study that proves it literally cures POTS, at least in the half an hour straight afterwards. Dr gall (who is supposed to be the best in the U.K.) didn’t give a s**t when I showed him though…
Hi Nat, I’m curious about your investigations which strongly resonate and/or correlate with mine. Did you give the SGB a try? Thanks
Hi Marie,
Yes the SGB was good but the physiology returned.
Bicarbonate is working again as I am pregnant and don’t feel able to use the high dose melatonin that seemed to be fixing the issue at the cellular level.
It’s an issue with co2/bohr/oxygen/hypoperfusion for sure.
There is a guy in Michigan fixing it.
Measuring end tidal co2 and using HUTT in 10 degree measurements to retrain the brain. I think biofeedback and increasing perfusion (exercise) with cellular support is the way forward. It’s totally possible to cure. I may start a social media channel to share what I’ve done and found as I do think it’s useful. I’ve just had young children and been working so hard with it myself!
hi nat, yes please, what products do you use and in wich strenght? can it be detected in a blooddraw from gp at my bed or in 24 hour urine collection how much you must take of each? My gp said even fr magnesium that it could not be detected so do not know where to start. wich kind of magnesium do you take please? I take magnesium malaat. so glad for you the 3 supplements helped you!!!
Also magnesium increases nitric oxide
Hi Nat,
I know that it has been a couple of years but I wanted to check in and see how you are doing with this approach. Do you still use transdermal bicarbonate and do you find that it works well for you?
I would like to notify health rising that I discovered the cause of my CFS as being a Caffeine sensitivity ( less than 1/4 -1/2 cup daily) which acts as an important modulator of adenosine and as a neurotransmitter and is the foundation of Adenosine Tri-Phosphate ATP which is the bodies energy store basis. It also is the chemical in your body with more control over sleep heart rate ( think O2 in and CO2 out transport while sleeping) I recommend anyone with CFS-like symptoms try a caffeine free ( or low) diet for a a few weeks as you might be surprised.
If quitting caffeine fixes you, you didn’t have ME/CFS. My kids haven’t had caffeine in their whole life and they got ME/CFS as pre-teens.
Just because your kids got ME/CFS and never used caffeine doesn’t mean that caffeine doesn’t make symptoms worse for those who have ME/CFS. Thomas is not saying that caffeine CAUSES ME/CFS, just that it makes symptoms worse.
Thanks Thomas – Going caffeine-free hasn’t helped me but congratulations on your progress.
I’ve circulating my CFS symptoms ( (I partially funded Bob Naviaux’s CFS metabolomics). I’ve been to the Mayo Clinic, John’s Hopkins, Stanford and UCSF with no luck. It really seemed like something was happening while I slept but after 3 formal sleep studies and my computer recording showed very little.Pulse Oximeter showed my hear rate was dropping into the low 40’s and high 30’s while I slept. It was so bad I used caffeine whenever I awoke 1AM-5AM) to boost mt heart rate just a little. It actually helped noticeably. But when I drank some coffee at 8AM or so, I noticed it did nothing to my heart rate. That led me to ask a UCSF muscle about caffeine and he said caffeine has many effects since its the basis of all mito energy and ATP cycles back to adenosine once its phosphate groups were removed.
So I began looking at my more non-CFS symptom set and sure enough I found the daily cycling and sleep modulation ( like melatonin) were a good match.
So I began researching the many adenosine pathways and symptom constellations associated with it being dysregulated.
It is a major factor in heart rate control and my GI issues were all tied to adenosine via its impact on raising stomach acid. Plus there more.
So on that basis I just stopped coffee. All the symptom areas stopped within days. That was 3 months ago. So I understand not all true CFS-ME are likely due to a common cause. I found mine. I fell much better. My response was just in hopes others like me might just try quitting coffee. If there were only a few like me, quitting coffee for a week or via tapering is a pretty easy test.
I just wanted to put it out there since coffee, tea, chocolate etc… are so common and like me, maybe others just never realized. Anyway, thanks for all your efforts and if just a few people were helped, I would be happy.
Thanks for your comments. Anything is worth a try.
Ari Whitten does some online stuff about adenosine being interfered with by caffeine, and in relation to this blog he recently put out a very long post on ‘breathing’ habits/methods which seems very relevant to this article by Cort.
Where can I find this article please?
I take Magnesium Albion Glycinate 133mg. 3X a day, plus 62.5 mg. Liquid Mg. In sea minerals. Is this enough Magnesium, or do I need something different?
Hi, if you just google Ari Whitten breathing he has quite a lot of info available. Do note he does have a ‘payable’ program that he promotes but there is still a lot of good info.
Good luck.
I am excited and relieved the hypocapnic piece is finally being pinpointed. I purchased the Lumen device last year which seems to use exhaled CO2 as a proxy for ketosis. I found I was always in their highest ‘carb burning’ state no matter what I are or how I fasted UNLESS I did 3 rounds of Wim Hof breath (which increases CO2) and then I would go to their lowest/best rating of ‘fat burning.’ I believe the CO2 measure is all they use, again, as a proxy for ketosis. I tried to engage with their scientists on using this device for the ME/CFS+ community but I couldn’t get to the right person and then I got tired.
I also know that Diana Driscoll’s approach on POTS includes thiamine and magnesium as well as choline to increase our typically lowacetylcholine levels. And she has patients on Diamox. I haven’t been consistent on high does thiamine but now I will be since Diamox sounds intense. Also going to reexamine my magnesium per Nat.
I love the effect of the Wim Hof breath but I dont always want to do it.
Cort and Jeffrey – Patrick McKeown is top breathing scientist and is doing a number of small studies using the light breath plus cadence breathing (5 count in, 5count out). I would LOVE to be a part of a project that looked at simple breath tools to help ME/CFS+ community. Let me know if I could help reach out to him.
Interesting about the shift with Wim Hof. A piece on him will be part of the series on breathing. I must check out Driscoll at some point.
Ari Whitten covers a similar area of breath work to improve functionality
I’m somewhat bewildered by this notion of hypocapnia being caused by or resulting in hyperventilation. I was diagnosed with hypercapnia after blood tests at one of the old Fibro and Fatigue Clinics in 2006, but have not been tested since. In any case, I do have fairly severe and persistent OI, but I don’t have POTS. Neither my heartrate, nor my breathing seems to increase when I’ve had the stand-ins for tilt-table testing, but my blood pressure drops upon standing. I have trouble standing still for more than five minutes or so; and I have difficulty thinking unless I’m supine. Even sitting and trying to think is challenging. I’m wondering why I don’t hyperventilate to try to fix the problem of too much CO2 in my blood. I actually breathe fairly shallowly unless I attend to breathing consciously.
You could have orthostatic hypotension – a drop in blood pressure upon standing. There are treatments for that. https://www.mayoclinic.org/diseases-conditions/orthostatic-hypotension/diagnosis-treatment/drc-20352553
Yes, that’s exactly what a couple of docs have told me I have. I tried fludrocortisone, but it made my stomach upset. I’ll look into the other solutions offered by Mayo from your link. Thanks much for answering. Sorry it took me awhile to get back to the site to see it.
what is the difference between POTS & OI please? Am trying to work out which I have.
Evelyn, I’m not an expert, but my experience of OI is just that I start feeling exceptionally weak, unwell and brain-foggy if I stand up too long. I can’t think as well even sitting up, let alone standing up. I know it has to do with not having enough blood in my brain, because if I lean way over and get enough blood in my head, then the awful feeling goes away at least temporarily.
From what I gather, people with POTS have rapid heartbeat in response to their blood pressure dropping, plus, I’m sure other symptoms.
Here’s a bit abt why COPD patients go through shift of normal respiratory drive who a hypoxic drive due to chronic hypercapnia.
Could it be a similar adaptation mechanism but reversed?
“As COPD advances, these patients cannot maintain a normal respiratory exchange. COPD patients have a reduced ability to exhale carbon dioxide adequately, which leads to hypercapnia.[8][9] Over time, chronic elevation of carbon dioxide leads to acid-base disorders and a shift of normal respiratory drive to hypoxic drive.
Hypercapnia and shift of normal respiratory drive to hypoxic drive to maintain respiratory hemostasis [10][11]: Carbon dioxide is the main stimulus for the respiratory drive in normal physiological states. An increase in carbon dioxide increases the hydrogen ions, which lowers the pH. Chemoreceptors are more sensitive to alteration in acid-base balance. An increase in arterial carbon dioxide levels indirectly stimulates central chemoreceptors (medulla oblongata) and directly stimulates peripheral chemoreceptors (carotid bodies and aortic arch). Chemoreceptors are less responsive to oxygen levels. In COPD patients, this effect is blunted as the chemoreceptors develop tolerance to chronically elevated arterial carbon dioxide levels. This is when the normal respiratory drive shifts to hypoxic drive, and the low oxygen level play a pivotal role in the stimulation of respiration through the chemoreceptors and maintain respiratory hemostasis. That is why the target pulse oximetry in these patients is 88% to 92%.”
https://www.ncbi.nlm.nih.gov/books/NBK525962/
Also, I’ve been manually firing up my diaphragm since 2015 and I had to condition myself to breathe in full breaths with a count of 3, slow releases full breath for the count of 6 to regulate my neurophysiological stress response and try contract the fight and flight response that my breathing difficulties Trigger.
I recently found out that neural cervical foraminal stenosis is impacting my diaphragm function which has been causing the diaphragmic failure and the paralysis which causes all of my dislocations.
Which is why it’s taking 18 to 24-hours a day of soft tissue therapy and neuromuscular activations to keep myself breathing and trying to take in food.
I’m actually being paralysed from the nerve roots due to structural pathologies which are common in people with pots EDS ME and fibromyalgia.
I think it’s really important that we we look at cervicogenic issues regarding actual diaphragmic failure/ cervical Angina/ or structural vagus nerve impingement impacting breathing function as well as everything that’s been considered it does all tie together.
I put this theory forward vaguely to Dr Asad Khan re the possibility of of people with ME and covid going through this hypercapnia and possible shift in hypoxic drive due to us being in chronic hypoxic States. Could this be happening due to the hypocapia environment?
https://twitter.com/agy_lena/status/1486333398998208515?t=1ZyziDKVeIqhTxPh2i23jQ&s=19
The summary was because we suffer from tissue hypoxia it wouldn’t be the same case as COPD were they suffer from arterial hypoxia.
Surely these findings explain that we suffer from arterial hypoxia too at least with cerebral hypoxia and that in itself would be enough to drive a fight or flight neurophysiological response triggering the breathing issues stated here and I highly believe its human instinct to counteract that with slow deep breaths.
I cannot exhale at the same pace or depth that I can inhale, it triggers instant physiological stress response and adrenaline surge so I really struggle with conversing or breathwork practices unless I have fired my diaphragm up, and breathing Trigger’s siezing of the diagram, same as using every other muscle, have to talk at my own pace.
When I am structurally unstable and attempt to be upright I have no cognitive function and I have to constantly remind myself it’s because Im siezing and my cerebral bloodflow isn’t circulating and I need to lie down.
I’m sure the picture will be different for everybody regarding the breathing issues and structural issues, pots phenotypes but is it not safe to assume a similar shift in hypoxic drive is happening due to the cerebral hypocapnia issues?
Hi Nat, may i ask is it normal magnesium chloride that you take and how much (because my GP says it can not be meassured and I take 400 mg magnesium malaat) or is ionic magnesium chloride something else then normal magnesium chloride? Are you still on high dose thiamine? And what is TTFD? I live in belgium, verry ill, never heard of it. Do you take that still and in wich dose please? so glad you have those symptoms relief!!! hope you improve further!!! ps do you take calcium with it because I heard there is a magnesium-calcium balance in blood?
Oral magnesium chloride. If you web search it you should find some available where you are. Mine is made in the U.K. TTFD is the form of thiamine I take. Magnesium chloride enables much higher amounts of Mg to be ingested I think so of there is a deficiency it can be addressed. It’s basically impossible to test mg levels accurately so I just go by symptoms.
My usual breathing rate at rest is 8 or 9 breaths per minute. I am a slow, deep breather, which is something I learned during meditation practice many years ago. It’s actually hard for me to speed it up at this point, and feels irritating to do so (though it’s naturally faster during exertion). However, I also have trouble holding my breath for 35 seconds. Does this imply I’m breathing too deeply and may be generating low CO levels?
According to one website slow deep breathing is OK. By slowing down your breathing you may be moving about the same amount of breath as as normal, shallower breather.
Thanks. That makes sense.
Albert Donnay reported this 30 years ago. I and many other people have done his “oxygen therapy” with good results and 30-90% improvement. His website MCSRR.org describes the state of hypoxia and how to determine if you are one of the people who will benefit from the Oxygen treatments. My condition was verified by arterial and venous blood gas tests, and the correction of the hypoxia was verified by those tests after. He calls the condition MUSES. I have a blog site that details what I personally did and show the test result: https://www.blogger.com/blog/posts/2749016591183274993?blogID=2749016591183274993&pli=1#editor/target=post;postID=1609670592977863002;onPublishedMenu=allposts;onClosedMenu=allposts;postNum=0;src=postname
It is sad to see research and information ignored and then years later someone else redoes that research – the research is not building on what has gone before. Over the 40 years I have had this illness I have seen this consistently. I wonder if all medicine is like that.
Hi Cheryl, your link is not working. Just redirects to google account login?
I’m wondering if what we perceive as ‘shallow breathing’ might actually be rapid breathing.
Worthy of note, the breathing treatment Freespira is aimed at normalizing CO2 levels and respiration rates in Panic Disorder and PTSD. While I don’t have those diagnoses, I had the opportunity to try it through my insurance.
It certainly isn’t a cure but I do feel more stress tolerance and more calm, with less symptoms that go along with that. I could see my breathing patterns normalize and become automatic during the 5 weeks I participated. You do a 17 minute session twice per day.
YMMV – I’m also receiving IVIg and am now (subsequently) being treated for MCAS as well. But treatments like this definitely have value.
Thanks Corey. I’ll check them out
Hi.
Would breathing oxygen through a tank with a low flow rate during sleep help with this issue? I have OI as well and hypocapnia most likely because of the quality of my sleep despite medication and supplements.
What do you think?
Thank you for this very helpful information and to those who commented as well.
Is this part of THE ENDING SUFFERING PROJECT FOR ME which you wrote about 19th April, 2021? I’ve had ME/CFS/FM for 35 years and am now mostly bedbound and certainly homebound.
Thanks for the help you are giving us. We appreciate you.
I’m so happy to see this make it into the ME literature!!
I cannot do controlled breathing like in yoga, or on demand as when the doctor tells you to breath while listening to your heart, without experiencing symptoms similar to presyncope (if not actually presyncope).
Both my cardiologist and the doctor who did my pulmonary function test explained this is due to hyperventilation at the cellular level. The pulmonologist took it even further and explained this is due to brainstem dysfunction.
Thanks for the interesting article Cort. Just a word of warning about using breathing training in ME/CFS to reduce hypocapnia, based on experience of myself and my son. I have ME/CFS, teenage son has ME/CFS and POTS. We saw a breathing-specialist osteopath some months ago who measured endtidal-C02 in our breath, as in this article. (You do this using a capnometer, can buy one yourself one if you have a spare US$3500!). Results showed I have hypocapnia (C02 = 30) all the time, sitting and standing. Son has orthostatic-specific hypocapnia, i.e., normal when sitting (C02=45) but hypocapnia within a minute of standing (C02<30). We also both have terribly low breath-hold time (as predicted by your home test link). Our breathing rates were fairly normal (just slightly high) and so assumption was we were breathing too deeply.
In breathing training with the capnometer (we hired one) we were both able to successfully breathe more slowly and less deeply to make our C02 levels normal. BUT this didn't help us, it made us both worse. For son, two days of 10-15 min training per day left him crashed for 3-4 days. For me, two days of 2x30min of training left me crashed for a week.
When I went back to the training, I decided to measure my blood oxygen with finger oximeter at the same time. Result: yep, I could increase my C02 to the level of normal but ONLY by simultaneously reducing my blood oxygen levels too low (went from my normal 96/97 down to 91/92, the oximeter has alarm that goes off at 93).
So, at least for some of us, I think the overbreathing (and hypocapnia) is a RESULT of the need for more oxygen, presumably because our bodies are not extracting it properly, and reducing the overbreathing can just screw us up even more.
The idea that breathing training can fix hypocapnia and make people feel better (e.g., reduce dizziness) has good support in anxiety disorders (particularly panic disorder), but it is based on an assumption that the person has normal underlying physiology and metabolism, particularly normal oxygen extraction. And we know that commonly ain't the case in ME/CFS.
I found a capnograph for around $250 the contech ca10s on ebay/aliexpress it works good enough for monitoring co2 and has been handy figuring out what is going on with my breathing. This along with Buteyko techniques and realizing I was breath-holding a lot and paying attention to my breathing more to stop it has helped my health some.
Is there a way to get the researchers to start measuring blood glucose levels at the same time they are measuring everything else?
Lack of oxygen to the brain = hypoglycemia.
Also, in urine. Ask indiviuals to collect their urine when they can smell it of cereal milk. Or 24 urine collection. For glycosuria.
So one tactic is to make sure you are eating enough carbs, frequently through out the day. And to make sure your body is burning them for energy. I am surprised at how much glucose my body burns when under the stress response. Fruits and roots are a great source.
Also, if you are low on CO2, it would be wise to breathe out through your nose: you want to retain the little CO2 you have! Even breathing out through pursed lips might be bad advice.
I used to crash terribly from conversing, even if in supine. It would start with a feeling of my lower brain being on fire.
Same with singing. I finally figured out I was letting too much CO2 out.
B1= carbonic anhydrase inhibitor
= uninhibits PDH
If you burn glucose and not waste it to lactic acid, you produce a lot more CO2.
Think about playing the never-crashing game: keeping your HR low and not going over your anaerobic threshold, making more CO2. As you all know, our anaerobic threshold is ridiculously low.
Relaxing the hypertonicity of muscles helps too – if your diaphragm fails to relax, that affects your breathing.
Also, let’s talk about those with orthostatic hypertension. And hypertension. I think those not bedbound deal with hypertension more, together with high stress hormones. Let’s start including them too in studies and the conversations.
Ray Peat writes about all these processes, beautifully. Any one interested, he’s got books and a few articles on his website too.
All PT ever did for me was cause further injury, to muscles, connective tissue and nerves.
Working on the metabolic problems has lead me to improvements no PT ever did…
I think a lot of the early uk graded exercise therapy research used “relaxation/meditation” sessions as a control to show the supposedly superior benefits of activity and the lack of effectiveness of the “rest” more advice – ie there were negligible benefits in terms of outcomes
“You are doing x wrong. You need to follow my expensive secret protocol to slightly improve your symptoms. If my treatment doesn’t work, it is because you are doing it wrong or you aren’t trying hard enough or you don’t believe in magic.”
It’s amazing how scammers all follow the same script, decade after decade, but desperate patients will try anything, because we know we will never get any real help from the establishment medical machine.
Many thousands of wind instrument musicians around the world have been breathing deeply and frequently for centuries but don’t have disease caused by “breathing wrong”. I wonder what is their secret.
(I played saxophone in community bands for many years. Giving up my music was one of the biggest losses caused by this damn illness.)
Me too. Flute performance major. High flow low pressire breathing. The first thing to go was breath control. And I was in incredible shape. The breathing pattern supine is also outside the norm but in completely different way than when standing and a pattwrn I have nnever found in a book. . The breath is like the bow of a cello for wind instrument. If they would just listen 30 plus years ago, they would not so be so far in the dark ages. And forcing control of breath will not change the situation. I have tried experiments. The brain wants the carbon OUT.
And when entire chest area is not getting a large enough volume of blood, how is it supposed to work?
What about people like me who mostly breathe normal shallow breaths but then need to take an extra deep one every 10-15 seconds?
I’ve got a tachy heart when upright but the rate does go down just a bit while prone and a bit further when asleep. BP is normal mostly. Even then, I have events of a sudden brief rise in HR for no apparent reason. If you recall, my evaluation for POTS deemed me ‘normal’ excepting for my high heart rate. I can get a sudden sharp raise in blood pressure on occasion too (doctor’s office).
Is this a new category?
Interesting. I do have orthostatic intolerance issues, but I don’t think they’re the classic heart racing type. I guess it’s maybe also related to lack of energy supply to those muscles that hold the body upright; but there’s also slightly queasy feeling being upright that may have a different reason.
Abdominal breathing never worked for me, long slow outbreathing much better. Sometimes I do this using a beneficial type of yoga breath which constricts/slows airflow (don’t remember the name – maybe it’s Ujjayi).
Also there’s a kind of circular breathing exercise in Yoga where you breathe “up the back of your body” and then again “down the front of the body”, repeating this circle multiple times, and outbreathing can also be done using abovementioned constricted yoga breath.
I was told I had emphysema in 2009 when I was 45 years old. I smoked for 11 years, but quit smoking as soon as I was told that I had COPD. Quitting smoking was the hardest thing I ever did. But I knew I would die if I didn’t. My health was getting so bad that I needed oxygen 24/7 and was down to 92lbs. Thankfully, in 2019 I got a natural herbal prescription from a friend. It saved my life. I no longer needed oxygen and was able to climb stairs, dance, and travel the world.This is their website www multivitamincare org
So interesting. Thank you very much for sharing, Cort. Noticed if I rest all day long, I’m able to dance for an hour, without lifting my arms, wearing a N95 mask – I’ll then go through a moderate crash the next day (only morning). Without any mask, the crash will be much more severe and will last for at least two days.
Oxygen flow doesn’t seem affected by wearing the mask for what I’ve read, but the CO2 level inhaled seems to inscrease significantly. Am going to try wearing a N95 mask at home more frequently and see if it helps.
Dr Novak has found a treatment for OCHOS: calcium channel blockers. This is for those with OCHOS whose cerebral artery is paradoxically constricting when they stand. (This isn’t everyone with OCHOS.) The calcium channel blocker prevents the artery from constricting as much as it wants to, allowing a more normal blood flow.
Those patients who cannot tolerate calcium channel blockers can be tried on ACE inhibitors.
He is having some success with this treatment on the relevant subset of OCHOS patients.
He covers this (briefly) in his textbook “Autonomic Testing” in the case studies on OCHOS. Your autonomic specialist should be able to access this text through their university library. He has also mentioned it in a lecture for Dysautonomia International.
Further detail from Dr Novak:
Orthostatic cerebral hypoperfusion syndrome is associated with orthostatic intolerance and reduced orthostatic cerebral blood flow velocity without orthostatic hypotension, bradycardia, hypocapnia, or excessive tachycardia (Table 3).19
This syndrome may result from abnormal cerebral vasoconstriction or abnormal venous pooling in the upright position. Our approach to therapy is the use of calcium channel blockers or angiotensin-converting enzyme blockers for patients with hypertension or prehypertension; and volume expansion with salt, fluids, fludrocortisone, or the use of pressor medications in patients with low blood pressure.
Source: https://pubmed.ncbi.nlm.nih.gov/30308186/
Someone please send one of these doctors/researchers a blood volume measurement machine:
https://detalo-health.com/
I will do it if I win the lottery!
Some new research on this topic in regards to POTS:
Article: https://journals.physiology.org/doi/10.1152/physiol.2024.39.S1.614
Lecture: https://www.youtube.com/watch?v=j-EvLttWwpY
Very interesting. I hope someone will investigate whether the Buteyko method which increases carbon dioxide levels might be useful. CO2 is vital for proper oxygen use.
Some links:
Buteyko………… https://www.youtube.com/watch?v=fdnTvfooGn8
Shut your Mouth and Change your Life | Patrick McKeown | TEDxGalway…….
https://www.youtube.com/watch?v=mBqGS-vEIs0
Unblock Nose in Five Minutes – Buteyko Breathing Method
…. https://www.youtube.com/watch?v=tgmKIwUqhkg
http://articles.mercola.com/sites/articles/archive/2013/11/24/buteyko-breathing-method.aspx
Nose Breathing Nitric Oxide and Improved Oxygen Uptake….. https://www.youtube.com/watch?v=jJTl0VTROBc