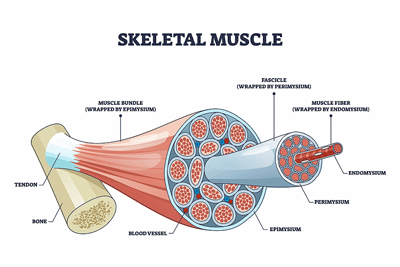
Skeletal muscles. It took a biopsy to uncover the carnitine and fatty acid problems in FM. Plasma samples would not do it.
It took a muscle biopsy to uncover it but there it was – strong evidence, apparently, of a bona fide mitochondrial deficiency in some people with fibromyalgia (FM).
Julian Ambrus, the senior author of this paper has published widely in and developed an animal model for Sjogren’s Syndrome, helped produce better diagnostic tests for the disease, is establishing a Sjogren’s Syndrome Center, and is working with drug companies to create better treatments.
Ambrus also hopes to create a center devoted to the study and treatment of metabolic diseases. Ambrus believes metabolic disorders lie at the heart of common symptoms like fatigue, exercise intolerance, gastrointestinal dysmotility, recurrent infections, and accelerated osteoarthritis.
Case Report
In 2012, he published a case report of a woman with fibromyalgia for whom the standard treatments weren’t working. She was very weak, was unable to get out of bed by herself or hold dishes in her hands to wash them.
First, a muscle biopsy demonstrated decreased levels of citric acid synthase (49% of normal), cytochrome c oxidase (53% of normal), succinate dehydrogenase (72% of normal), and nicotinamide adenine dinucleotide (NADH) dehydrogenase (73% of normal) – all signs of a defect in the mitochondrial respiratory chain.
Genome sequencing next revealed multiple polymorphisms (small changes in the DNA) (POLG1 polymorphisms (C-T polymorphism at 2254, and G-T polymorphism at 3708)) and several mitochondrial genome polymorphisms (1438 A-G, 3992 C-T, 14365 C-T, 14582 A-G, and 4042 A-G) which further cemented a mitochondrial diagnosis.
She improved significantly on a simple formula of coenzyme Q10 (ubiquinone) 200 mg, creatine 1,000 mg, carnitine 200 mg, and folic acid 1 mg taken four times a day. Each was designed to enhance a different part of the mitochondria:
- Co-Q10 transports electrons between complex I and complex III of the mitochondrial respiratory chain
- Creatine generates additional ATP through the creatine phosphate shuttle
- Carnitine enhances the transport of fatty acids – a vital substrate – into the mitochondria.
- Folic acid is necessary for several mitochondrial enzymes to work
- A-lipoic acid is a strong antioxidant.
It took several months, but the woman responded well and reported that she is able to “enjoy normal activities and more”.
Follow-up Study
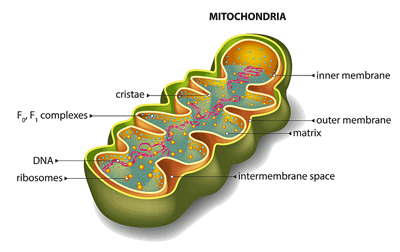
The study reported on findings indicating mitochondrial problems in 35 FM patients.
Eight years later, the Ambrus group published a follow-up, “Carnitine Palmitoyl Transferase Deficiency in a University Immunology Practice“, which described the results of metabolic workups and treatment plans for 35 patients reporting exercise intolerance and fatigue over time at a university clinic. Many of those patients had been diagnosed with fibromyalgia, most were women, and most had become ill in their 20s and 30s. Quite a few were also diagnosed with Raynaud’s Syndrome, migraine, and gut issues.
Besides fatigue and exercise intolerance, these patients commonly experienced gut problems (diarrhea, constipation, acid reflux), arthritis, headaches, frequent infections, shortness of breath, and others.
The muscle biopsies of these mostly fibromyalgia patients revealed they all had low carnitine palmitoyltransferase activity (at least a third below normal) and about a third of them had another biochemical abnormality. Note that only one patient had low plasma carnitine levels.
Treatment
All Ambrus’s patients were put on a diet low in long-chain fatty acids, which emphasized the use of medium-chain triglyceride (MCT) oil.
Patients were also given supplements known to enhance ATP generation within the mitochondria (CoQ10, carnitine, folic acid) and outside the mitochondrial (creatine) along with antioxidants (alpha-lipoic acid, and in some cases, vitamin C and/or vitamin E.
The improvements were not quantified. Instead, the paper stated that all the patients showed some symptomatic improvement in fatigue and exercise intolerance.
Long-Chain Fatty Acid Disorders
Fats are categorized by the length of the carbon chains they contain.
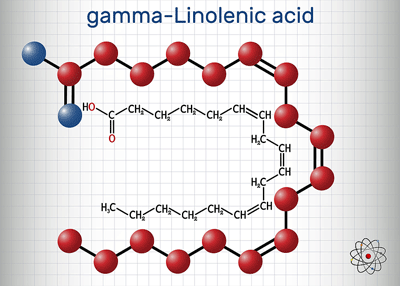
Gamma-linolenic acid with its many carbon chains is a long-chain fatty acid. Long-chain fatty acids need to be broken down to get into the mitochondria.
Short-chain fats have fewer than six carbons, medium-chain fats have between six to 12 carbons and long-chain fats have between 13–21. The shorter the carbon chain, the easier it is to break down the fat and turn it into energy. On the other hand, longer carbon chain fatty acids (such as Omega 3s) can play important roles in reducing inflammation.
While short and medium-chain fatty acids can get directly absorbed into the mitochondria, the process of preparing longer chain fatty acids for use is more complicated and takes much more work. They need to be broken down and then transported via carnitine into the mitochondria, where they need to get unloaded from carnitine. Several enzymatic reactions are required to carry out this process.
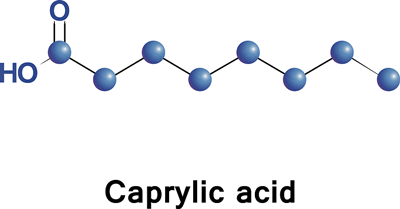
Caprylic acid is a medium-chain fatty acid. It’s carbon chains don’t need to be broken down to get into the mitochondria.
A good deal of the focus on long-chain fatty acid disorders appears to be in inborn errors of metabolism that quickly and dramatically assert themselves early in life and often result in death. These disorders affect either fatty acid transport via the carnitine pathway or mitochondrial b-oxidation (fatty acid metabolism that takes place inside the mitochondria).
They may also, though, crop up later in life and manifest themselves as rhabdomyolysis, sudden weakness, muscle pain, and kidney problems.
People with mild or moderate forms of a long-chain fatty oxidation disorder may only experience symptoms when increased β-oxidation is needed, such as during exercise or fasting, or if Ambrus is right, symptoms may be present most of the time in fatigue and exercise intolerant diseases like fibromyalgia and ME/CFS.
Long-Chain Fatty Acid-Restricted Diets

While all these foods are high in omega-3 fatty acids, they would be sparingly used in long-chain fatty acid diets.
This diet was an eye-opener for me as it’s almost opposite to my current diet, which is heavy on long-chain fatty acids (nuts and nut butter, olive oil, avocados, oily fish).
According to a 2018 paper, “Fatty acid oxidation disorders,” the treatment of long-chain fatty oxidation disorders (FAODs) – the kind found in this study – involves a long chain fat-restricted diet, supplementing with medium-chain triglyceride (MCT) oil (to support b-oxidation) and an essential fatty acid called docosahexaenoic acid (DHA – 60 mg/day for infants <20 kg; 100 mg/day for children >20 kg; and 100–200 mg/day for adults).
In severe forms of the condition, long-chain fatty acids may need to be restricted to 10% of energy and MCTs may need to make up as much as 20–30% of energy, 12% from protein, and 60-70% from carbohydrates. (A higher protein diet is now being assessed.) People with mild or moderate forms of the condition may require long-chain fatty acids to be restricted to 15–20% of energy intake. Metabolic centers will prescribe a daily limit in the number of grams of long-chain fat allowed and patients are educated about how to count grams of fat in food.
It was surprisingly hard to find much information on long-chain fatty acid levels in foods. According to one article, long or very-long-chain fats are saturated fats (mono or polyunsaturated) and are found in the following foods:
- Saturated long-chain fats – dairy fat, coconut oil, palm kernel oil, peanut oil, and other vegetable oils
- Monounsaturated long-chain fats are found in most animal and vegetable oils, but particularly macadamia, olive, canola, and safflower oil
- Polyunsaturated long-chain fats – are found in seeds, nuts (including peanuts), and some vegetable oils, avocados, meat, eggs, fish, oily fish, and marine oils.
(Omega-3 and omega-6 are both long-chain fatty acids. Omega-3s tend to be anti-inflammatory while high levels of omega-6s are pro-inflammatory.)
Some long-chain fat consumption is needed and should come from foods like butter, walnuts, or flaxseed oil, fatty fishes (sardines, salmon, mackerel). Lean fatty meats and non-fat milk are used as protein sources.
Since exercise places a large demand on fatty-acid produced energy, MCT (0.15–0.2 g/kg weight) is usually mixed with a glucose solution (e.g., Gatorade®) prior to exercise, and then a high carbohydrate/protein snack (3:1 carb/protein) taken afterward.
Relapses after exercise, fasting, and illness are treated by drinking carbohydrate-rich fluids and taking extra MCT every 3–4 hours. If that doesn’t work, the patient needs intravenous fluids.
Medium Chain Fatty Acid Foods – medium-chain fatty acids have shorter carbon chains (6-12) and are metabolized differently. I couldn’t find much information on medium-chain fatty acid foods either, but webpages tended to note milk, butter (particularly grass-fed), cheese, yogurt, coconut oil, goat milk, and palm kernel oil). (Some of these (butter, cheese) overlap with long-chain fatty acid foods presumably because they are rich in both). With @65% of the fatty acids in coconut oil taking the form of MCTs, coconut oil may have the highest MCT content of any food and some doctors believe coconut oil is a good choice.
MCT Oils
It appears, though, that most medium-chain intake in long-chain fatty acid-restricted diets occurs through supplementation with something like MCT oil.

Coconut oil is very high in MCTs.
The Gist
- Muscle biopsies reveal abnormalities in fatty acid metabolism in fibromyalgia. Carnitine is necessary to transport long-chain fatty acids into the mitochondria. Shorter chain fatty acids, on the other hand, are able to simply enter the mitochondria.
- Low carnitine palmitoyltransferase activity suggested that long-chain fatty acids were not being metabolized correctly – thus impeding them from entering and providing fuel for the mitochondria. About a third of the patients also had another biochemical mitochondrial abnormality.
- The authors reported that a low long-chain fatty diet plus mitochondrial supplements helped. Long-chain fatty acids are found in foods like olive oil and other vegetable oils, nuts, nut butter, oily fish, fatty meats, dairy fat, avocados.
- Medium-chain fatty acids take the place of long-chain fatty acids in the restricted long-chain fatty acid diet. These fatty acids are commonly found in coconut oil and MCT oil and some other foods. Lean meats and non-fat milk products are used for protein and carbohydrates make up from 50-70% of the diet.
- MCT oil is often used to add these fatty acids to the diet. MCT is easily absorbed and may be able to help with gut problems and inflammation. It should be taken in small amounts at first (1 tsp/day) to allow the stomach to adjust to it.
- Since exercise places a large demand on fatty-acid produced energy, MCT oil is usually mixed with a glucose solution (e.g., Gatorade®) prior to exercise, and then a high carbohydrate/protein snack (3:1 carb/protein) taken afterward.
- Relapses after exercise, fasting, and illness are treated by drinking carbohydrate-rich fluids and taking extra MCT every 3–4 hours.
One doctor warns to start MCT supplementation slowly (1 teaspoon/day and working up to 1-several tablespoons/day) as MCT oil can produce stomach problems (loose stools, diarrhea, gas, bloating, abdominal pain) if the stomach is not used to breaking it down.
Carnitine Issues in Chronic Fatigue Syndrome (ME/CFS)
Carnitine issues seem to be inherent in long-chain fatty acid disorders. While some studies have shown evidence of reduced carnitine levels in ME/CFS, others have not. The most complete study – an Australian study, “Long-chain acylcarnitine deficiency in patients with chronic fatigue syndrome. Potential involvement of altered carnitine palmitoyltransferase-I activity“, found that reductions in two carnitines: oleyl‐l‐carnitine (C18:1) and linoleyl‐l‐carnitine (C18:2), were highly correlated with fatigue levels in ME/CFS.
That suggested the CPT-1 enzyme that binds fatty acids and carnitine together for entry into the mitochondria was punking out. The authors proposed supplementing omega‐3 fatty acids in combination with l‐carnitine in order to boost CPT-1 activity. Omega 3 fatty acids can be helpful because they already exist in a form the mitochondria can use.
That was an interesting suggestion given that low omega-3 levels have been found several times in ME/CFS, including one study in which over 90% of ME/CFS patients were found to have low levels.
The Peroxisome Connection
Recently, the Lipkin metabolomic study suggested that both low carnitine levels and low peroxisome activity are present in ME/CFS. Both carnitine and peroxisomes, interestingly, are involved in the breakdown or transport of long-chain fatty acids into the mitochondria.
After the peroxisomes break down, these fatty acids carnitine transports them into the mitochondria. The breakdown of either factor could starve the mitochondria of the fuel it needs.
Given the role peroxisomes play in breaking down long chain fatty acids, it would be good to know more about fatty acid metabolism in ME/CFS.
Long-chain fatty acid oxidation disorders are just one of quite a few fatty acid metabolism disorders, and many more metabolic disorders exist. Preliminary results suggest that several inborn errors of metabolism may be more common in ME/CFS/FM than we think.
Conclusion
The authors of the carnitine polymerase transferase study in fibromyalgia, unfortunately, didn’t quantify how much their patients improved. Nor do we know how widespread the deficiency is in FM. In short, the study was hardly the epitome of rigor. It seemed like more of a “let’s get this information out into the scientific literature in hopes that someone will follow up on it” kind of study.
What we do know is that muscle biopsies did find evidence of carnitine polymerase transferase deficiency in some FM patients and that a dietary modification in combination with supplementation appeared to help. It was also clear that plasma carnitine levels missed almost all of the carnitine deficiencies found in this group.
That dietary modification presents an abrupt shift from the high-fat, moderate protein, low carbohydrate diets often prescribed for ME/CFS/FM to a lower fat, moderate protein, higher carbohydrate diet.
As exertion places strong demands on energy production a pre-exertion recipe has been developed. It includes MCT oil mixed with a glucose solution (e.g., Gatorade® (or oral rehydration solution?)) prior to exercise and then a high carbohydrate/protein snack (3:1 carb/protein) taken afterward.
Similarly, relapses after exercise, fasting, and illness are treated by drinking carbohydrate-rich fluids and taking extra MCT every 3–4 hours.






“She improved significantly on a simple formula of coenzyme Q10 (ubiquinone) 200 mg, creatine 1,000 mg, carnitine 200 mg, and folic acid 1 mg taken four times a day.”
Was this just the folic acid four times a day, or the whole formula?
Thankyou
Here’s the sentence in the paper:
“Our patient was started on a compound of coenzyme Q10 (ubiquinone) 200 mg, creatine 1000 mg, carnitine 200 mg and folic acid 1 mg to be taken four times a day.”
I assume it was everything.
When I just read this, I took it to mean that the folic acid was the only thing taken 4X day. But if you look at the use of “a compound” in the sentence, you could be right. Totally ambiguous and needs clarification, imho.
Hi Cort this is very interesting. Just as a test I took MCT oil and immediately felt better. I also took carnitine. So far so good. The dosing on the other supplements seems like a lot! Is there any way we can clarify?
I asked Dr. Ambrus about that statement and he replied: “We use creatine 4 times per day.” I don’t know about the rest of them but it sounds like you could feel comfortable trying the creatine 4x’s a day at that dose.
This is an interesting and hopefully useful approach; but I have to admit I’m weary of being recommended wholesale diet changes. This is dramatically different than my current IBS/CFS diet, and seems very difficult to maintain as well. Hopefully more research with a larger sample pool will come out; in the meanwhile I’ll wait and see for at least more anecdotal evidence.
Kathy H
I think there is going to be no substitute for whole genome sequencing of large groups, with results individually looked at, as well as subgroups.
The more ‘expensive’ a test is, the more likely it will give answers, so muscle biopsies did more than routine lab tests— and likely more than EMG etc.
There is a group using micro pore technology to check for rare muscle/nerve disorders. I think they are cutting edge, and when people such as Julian Ambrus gets the financial $$$$$$$’s to do all the testing they want, to put more pieces of puzzle together, there will be more astounding of breakthroughs. And hopefully better clarity of vision.
Link to group article re micropore sequencing:
https://www.biospace.com/article/releases/oxford-nanopore-technologies-plc-announces-publication-nanopore-ids-50-genetic-diseases/
Thanks Sunie – I had never heard of micro-pore technology. I know the prospect of another diet sounds daunting but I am certainly going to cut back on some long-chain fatty acids and see what happens ‘
Ketogenic diets have never really done anything for me.
I’ve had a few lab tests suggesting fat malabsorption over the years – some ordered by my GI doctor and the others ordered by functional medicine practitioners. I’ve had 24 and 48 hour stool tests showing elevated fecal fat levels and 2 different urinary organic acid tests showing elevated ethylmalonic and suberic acids. Do you think these lab abnormalities could indicate a disorder like this? I’m not sure what testing to ask for at this point…
Just a comment for those who try this. You may want to buy folate rather than folic acid. Many people can’t metabolize folic acid into folate, and you wouldn’t know you couldn’t do so without a blood test. Its called methylfolate at the health food store or on Amazon. The ad may say fixate, but it’s really folic acid, so be careful
Very interesting and helpful article. My dx is Fibromyalgia, ME/CFS, and possible MS, though I could never get a definitive answer on that one and had minimal testing and eventually gave up. The MS neurologist recommended gebetic testing for inborn errors of metabolism, but apart from a few tests, the specialist wouldn’t run the full sequence as the test is very expensive and he felt that at my age, I was in my late 50s, it wouldn’t matter at this pount as my cells, etc., were deteriorating due to aging. I recently found out there is high endogamy and consanguinity in my family tree, as well as health issues showing up across generations so I now believe there is a genetic component to my health issues. I went back to my notes and hanouts from the genetic diseases specialists and started trying some of the supplements, and to my surprise I have experienced an improvement in fatigue levels. I take COQ10 daily (100mg), Vit D 1000IU, BComplex 50 but 100 gives me better results, and B12 Methylcobalamine, not the other one, which had litle egffect. Have added Omega 3. This vitamin regimen, which I’ve been on for about a year, has definitely made a difference. I wish I could try many more supplements, but I am on a disability pension, so can only incorporate one or two more things due to cost. The specialist emphasized L-Carnitine, so after reading this article, I think I will add that. Best of luck and thanks for the helpful comments.
Thank you for the folate info: as a salutary reminder of something I’d forgotten — but ignored vague misgivings about — when ordering folic acid tabs from Amazon just now. Will try to cancel hem, fortinately not too expensive if unsuccessful.
I’m heterozygous for defects in two fatty acid oxidation disorders. They didn’t bother me much before ME, except I couldn’t run 5ks without crashing badly (they use fats for energy in the second half), but I loved sprinting and other physical activity. I also had trouble with hypoglycemia here and there, so I carried a chocolate bar with me. I also crashed badly when I tried a keto diet before ME happened. I only lasted two days before my muscles were all intensely cramped and I had a screaming migraine. Apparently my muscles and brain really needed their carbs.
When I got ME, I suddenly looked like I had the full-blown FOD disorders with intolerance of dietary fat, and persistent hypoglycemia with dietary protein. Both genes impair fatty acid oxidation, and one also gives you hypoglycemia with too much dietary protein. I was diagnosed with adult-onset mitochondrial disease, which is essentially true since ME is an acquired mitochondrial disease among other things. One of my weirdest symptoms was multiple matching lipomas appeared down my spine. Lipomas are really common in FOD’s. So I am on a high carb, low fat, low protein diet. Between ME and my genetics, my fat metabolism is very slow and easily overwhelmed.
Early on in this illness I did really well on a macrobiotic diet – which is at least high carb. I just lost so much weight on it that I stopped it – but the initial response was really good – better than any other diet I’ve tried.
I’ve always noticed a craving for sweets after too much physical exertion…
any link to this macrobiotic diet? i just put back on all the weight i had lost 🙁
Would a macrobiotic diet be low in long chain fatty acids? I would like to lose weight, so it would be interesting if a high carb diet low in long chain fatty acids would do the trick. The only thing is, I possibly have MCAS and have GI issues with fermented foods like miso and kambucha – which may be part of macrobiotic diet. I am trying to wrap my head around all this. I am totally willing to try this to see if helps with my PEM, fatigue, weight, etc etc.
It was decades ago but as I remember the macrobiotic diet I tried was mostly rice and beans and stuff like that. None of those have shown up in any long fatty-chain foods that I’ve seen.
Brown rice with a small amount of beans is my best option for extended energy. But I can’t have soy sauce with it. That ruins it. A big dose will put me directly into POTS, presumably from its influence on the brainstem. It also causes bad brain fog. ME patients can have an excess of free glutamate in the brain, and soy sauce is full of free glutamate. I do much better on a low glutamate diet. But if I’m trying to lose weight, the brown rice and small amount of beans is my mainstay, plus plenty of vegetables (mostly low-fat coleslaw) and fruit. It works every time. I just get bored with it.
I wonder about histamine as well and soy sauce might be full of it. I’ve always had problems with soy! Tofu would wipe me out So would soy milk (remember soy milk?) It would put me under quicker than anything. I’ve always wondered about that.
Love the coleslaw addition. 🙂
Acetyl-l-carnitine and riboflavin are critical supplements for me. They are both recommended for fatty acid oxidation disorders, although carnitine is more often recommended. I find the acetyl-l-carnitine helps my brain more, still helps my muscles, and doesn’t cause a fishy odor when I take a lot of it, whereas l-carnitine can cause the fishy odor depending on how much you take. Acetyl-l-carnitine passes the blood brain barrier more easily than l-carnitine.
How much do you take a day?
1 gm 4x day of acetyl-l-carnitine
400mg in the morning of riboflavin
Thanks for the article Cort.
How does it later effect the kidneys? We have family kidney problems. Is it specific or a range of issues that may give the doc an “a hah” moment of discovery and add it to the long list of “already” discovered conditions.
I’m afraid I don’t know. If I remember correctly, the renin-angiotensin-aldosterone axis problems in POTS and ME/CFS may be affecting the kidney.
ok. I just got dx’d with “definitely interstitial cystitis” on March 17th. Talk about feeling like having a uro-birth of a flaming hot porcupine! Ack!
I wish I could have taken the Uribel longer than 3 days. I got by with only 2 a day and maybe even 1 a day the way I magnify my meds had I taken longer. It took care of my entire body pain, everything, and even my legs warmed up and they are always cold. Even my restless leg/body, pins, needles and gnawing pain left!! I didn’t realize how much pain it got rid of until it all started piling back on. Ugh…. I’ll find out more in 4 weeks for follow-up.
I looked up my POLG1 gene…..what if I don’t have a POLG1 gene? I have a POLG gene, but my search for the POLG1 says “no genes or markers found matching “POLG1”.
Anyone have a recommendation for commercial MCT oil brands?
Jessica I recommend Nature’s Way org MCT oil
Bulletproof has a very high quality MCT (unrefined coconut) oil that I’ve been taking daily since October. Mitochondrial deficiency is one of my many MECFS problems and I’ve noticed improvement since taking this along with a Urolithin A supplement.
Costco might be a good choice. It states on the bottle that the organic MCT oil is hexane free and is probably markedly cheaper than other brands. I think I got an 40 fl oz bottle for $18.
Thanks!
MCT oil is also available in a powder which is easier on the stomach.
Man the magic q10, Creatine, Carnitine,Folic acid therapy that no one has ever heard before ! And surely no one with Cfs has taken these at any point during their disease. Hould could we overlook such an easy treatment that would cure 99% ?
…
Said no one ever.
Hmm, but has the ‘magic’ therapy been trialled concurrently with the (a major point of this article) low long chain fatty acid diet?
Amen to that!
I am new to trying these kinds of supplements . However, I have had Fibro for decades and would like to try the compound of coenzyme Q10 (ubiquinone) 200 mg, creatine 1000 mg, acetyl-l-carnitine 200 mg and methylfolate acid 1 mg -4 x’s a day.
Does anyone have any suggestions? Would you also take MCT with this?
I don’t know what has long chain fatty acids and what has short chain.
I appreciate any help and suggestions with this. Thank you all so much!~!!
Hi Jill,
I’m in my early 50’s and have had Fibro a long time too, I usually buy my supplements from amazon and also plan to buy the ones you’ve listed. I go for the products with the highest number of 5 star reviews also accounting for price, amazon’s choice is generally a safe bet.
I’m also going to try the oil and plan to make bulletproof coffee with it every morning, though I will struggle with the sweetness as I don’t normally take sugar with coffee!
I think it would be good to try the oil before any exercise too then a snack afterwords to restore energy which is two thirds carbohydrate and one third protein.
Hope this helps, good luck!
I’m a patient of Dr. Ambrus. I will say that his process of evaluation is far more thorough than most docs, and it was all covered by insurance. Unfortunately the lab that analyzes the muscle biopsy samples is not currently being allowed (by NY state) to do commercial work, but only Covid-related testing, so many of us are stuck waiting for our results. I had my muscle biopsy over a year ago. My sample is sitting in a freezer along with many others. It’s very frustrating, but there’s really nothing we can do. I did learn from the “ischemic forearm test” that my body produces lactic acid far sooner than is normal, but that’s it so far.
Thanks Sue! We need more doctors like Dr. Ambrus who are willing to explore this field. Good luck with getting that muscle biopsy tested!
http://raypeat.com/articles/articles/coconut-oil.shtml
How much A-lipoic acid should one take and should it be taken on an empty stomach or with a meal?
My problem started 30 years ago when I developed fibromyalgia after having right upper lobe pneumonia which flattened me for a month. I was on antibiotics for the four weeks and lost 20 pounds in four weeks. Several months after that I began to develop strange muscle pains and was eventually diagnosed with having fibromyalgia. One physician I saw for acupuncture recommended that I try L-tryptophan. Tragically I was one of the many thousands of people in the United States who were poisoned by the contaminated L-tryptophan, which was shipped from Japan even when it was known to be contaminated by the Japanese manufacturers. Then in 2006 I had spine surgery and the complication of bleeding into my spinal canal was missed by the surgeon. Not only was I left with the cauda equina syndrome but also my fibromyalgia remitted and morphed into chronic fatigue syndrome. I’ve had that ever since. I am still quite symptomatic with it with all the usual symptoms. I have been able to work part time though fortunately. Now I want to mention a few things that have helped me. The most dramatic help I got was from a product called GutMagnific, which is an FDA approved probiotic from researchers at the Swedish university of lunch. Some desperate soul with Emmy/CFS found it and tried it and got some significant benefit from it. What I noted particular for me is some increase in energy and also an improvement in my mood. The original poisoning with contaminated L-tryptophan damaged my mood areas in my brain and left me with chronic depression. It has been difficult to treat that but the GutMagnific caused a definite very positive response. More recently I have been opening one of the capsules each day and sprinkling it on my breakfast and it found that my probableSIBO remitted rapidly. I have probably hadSIBO since I was treated for a month of pneumonia with antibiotics. I have also found MiTO Q and oxaloacetate to be of some help. GutMagnific was originally designed to treat irritable bowel in people with multiple sclerosis. But anecdotal reports to the researchers have said that it can also help C diff ,SIBO, eczema and psoriasis and ulcerative colitis. GutMagnific is available online from Sweden. The company is working toward an international marketing plan now and recently won a European award for one of the best three new probiotics. If anyone tries it I would love to hear what your response to it is. I have also found that I become deficient in various surprising substances. for a couple of years I craved a product made with sesame seeds, namely halvah. And then suddenly one day I no longer wanted it at all. Then I became deficient in chromium episodically with an insatiable hunger that nothing including drinking straight from the bottle agave syrup would stop. Only large doses of chromium one. I found that I need to take vitamin B complex 3 to 4 times a day. Otherwise my nails and hair get very weak and thin and my energy drops even more. I eat a healthy diet I believe And yet I developed pellagra with rough skin on my hands and feet and numbness and weakness especially in my legs and forearms. So I would encourage everyone to take high doses of vitamins that are water soluble and look at their trace mineral levels also carefully. Thanks so much for all your help and please let me know what GutMagnific may do for you.
Really nicely written article. We have already worked out through trial and error that carnitine and MCT oil are helpful for CFS in our family, great to see some science behind that.
Regarding the 2020 article with the biopsies, I noted that many of the patient’s long list of complaints and other diagnoses could be possibly attributed to undiagnosed ME/CFS. “All of the patients presented with fatigue and exercise intolerance.” Many people first get diagnosed with fibro when they actually have ME (like myself). And some people have both.
Many of the patients had a lot of diagnoses, “including fibromyalgia”. But unless they were all screened to actually exclude ME, then these findings could also be seen as applying to ME. To attribute their findings specifically to fibromyalgia is a bit worrying and maybe misleading.
Has anyone tried rTMS (NeoRhythm headband or pad) to reduce ME/CFS symptoms? (pain, mood).