The Breathing/Oxygen series on Health Rising continues with a rare clinical trial in chronic fatigue syndrome (ME/CFS) that’s designed to improve breathing, increase blood CO2 levels, and hopefully improve a wide number of symptoms.
The Breathing/Oxygen Series on Health Rising
- A Gas Exchange Disease? Huge CDC Exercise Study Puts New Slant on ME/CFS
- Uneasy Breaths: Strange Breathing Patterns in Long COVID May Contribute to Exercise Intolerance
- Oxygen Short? Microcirculatory Problems Could Explain Long COVID (and ME/CFS)

Heather Edgell will use her Solve M.E. Ramsay Award to improve breathing in ME/CFS and long COVID, and hopefully increase CO2 levels and improve some symptoms.
Dr. Heather Edgell seems to be in a kind of sweet spot. Interested in fainting disorders – her Ph.D. focused on the cardiovascular and autonomic aspects of fainting – she founded an autonomic and cardiorespiratory testing lab called the Women’s Cardiovascular Health Lab at York University in Toronto.
That led her to postural orthostatic tachycardia syndrome (POTS) and chronic fatigue syndrome (ME/CFS) – two diseases with a predominance in women – both of which feature orthostatic intolerance (problems standing and/or sitting upright). Now we have long COVID – another female-dominated disorder that produces similar effects.
Gender
Given the gender imbalance found in these diseases, I asked about the role female hormones might play. Dr. Edgell stated that much more work on this needs to be done and noted that estrogen is a potent vasodilator and progesterone is a respiratory stimulant. High levels of both can increase the fight/flight response.
Ramsay Award ME/CFS and Long-COVID Clinical Trial
Last year, Dr. Edgell won one of the most interesting Solve M.. Ramsay Awards in memory. Edgell’s clinical trial to assess the ability of inspiratory muscle training to improve breathing – and more importantly, increase CO2 levels, is exciting, not just because potentially provides affordable help now, but because of how much physiological research is embedded in it.
Inspiratory Muscle Training (IMT)

One of many inspiratory muscle trainers on the market. Inspiratory muscle training can instill a new, healthier breathing pattern that been shown to breathlessness and improve a host of factors.
“Inspiratory muscle training”, or IMT, is a respiratory exercise program that’s used to help people with asthma, bronchitis, emphysema, stroke, etc. breathe better. One study of people with heart failure using a cardiopulmonary exercise test (CPET) found that a home-based program improved their aerobic capacity (peak VO2) (!).
Even people in great shape can benefit from these exercises. The Training4Endurance website, for instance, has a page that demonstrates how athletes can use it to race faster and longer.
Studies have found that inspiratory muscle training can improve sleep and balance, reduce blood pressure and breathlessness, and improve functioning. The balance issue demonstrates how far the impact of weakened respiratory muscles can go. Apparently, when we encounter a soft or uneven surface, our back muscles kick in to keep us stable. Because the diaphragm supports the back muscles, a weak diaphragm keeps the back muscles from doing their job. When that happens, we turn to our ankle muscles – which results in more swaying. That’s why one inspiratory muscle study, which used the POWERbreathe® Medic Plus device, found that breathing retraining improved the participants’ balance.
Training the Respiratory Muscles
Inspiratory muscle training uses a small device that restricts the airflow in order to increase respiratory muscle strength. Edgell determines your maximum inhalation and then sets the pressure of the device at 80% of that. You then breathe through the device a certain number of times a day. She said it feels as if you were breathing through a straw.
Three times a week, the participants will do 6 sets of 6 repetitions. Each set will be separated by decreasing lengths of time over the 8 weeks, starting at a 30-second interim. All told 36 inhalations will be done 3 times a week.
It’s not called “inspiratory muscle training” for nothing. The program can actually retrain how you breathe and inculcate a new breathing pattern that sticks.
I asked if the increased amount of time many people with ME/CFS have to spend in bed could affect the muscles we use to breathe with. The answer was yes. Because we breathe more shallowly when we’re in bed, the muscles we ordinarily use when we are up and walking around can be detrained.
I asked if breathing retraining could help with the problems getting oxygen to diffuse into the small blood vessels of the lungs that two recent long-COVID studies found. She didn’t know but thought it might be able to.
Increasing CO2 Levels in ME/CFS and Long COVID
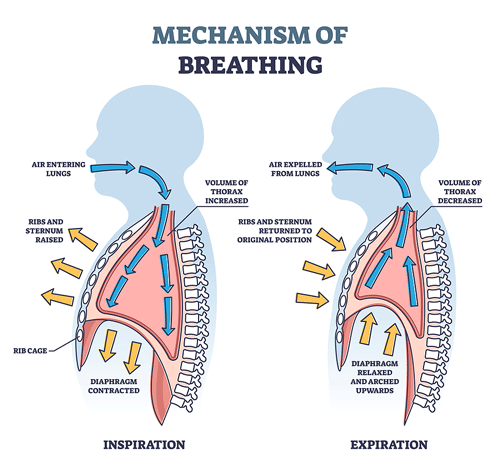
The breathing patterns in people with ME/CFS, fibromyalgia, POTS, and long COVID appear to be causing them to remove too much CO2, which may impede blood flows to the brain.
The primary goal of the retraining program is to increase the CO2 levels in ME/CFS and long-COVID patients’ blood. CO2 is a critical factor in the body that is produced during both anaerobic and aerobic energy production. Interestingly, our brainstem regulates our breathing based on our CO2 levels, not our oxygen levels.
We remove excessive CO2 in our blood by breathing. Breathing too much, though, by breathing too deeply, or too rapidly, or both, can remove too much CO2 – leading to hypocapnia, or low blood CO2 levels.
Hypocapnia can produce many symptoms including dizziness or lightheadedness, shortness of breath, bloating and belching, fatigue, feeling weak, cognitive and sleep problems, numbness and tingling sensations, muscle spasms, chest pain, and palpitations. Because low CO2 levels cause the blood vessels in the brain (as well as the lungs) to constrict, they could be impacting brain blood flows – a critical concern in ME/CFS and long COVID.
Hypocapnia Common
Hypocapnia, or low blood CO2 levels, have not been found in everyone with ME/CFS/FM, but appears to be present in a very substantial subset. Eighty percent of people with ME/CFS had POSH (postural orthostatic syndrome of hypocapnia) in a recent CDC orthostatic intolerance study. Some of them even exhibited low CO2 levels while lying down. Interestingly, a sudden onset of the illness, probably an infectious event, was significantly more common among the patients who demonstrated some abnormality.
Systrom found low CO2 levels in his invasive exercise studies, the Visser team found them during tilt table testing, and Naschitz found it in his ME/CFS/FM Israeli studies fifteen years ago. (He said it was “common” in fibromyalgia.). Natelson and Mancini also found it during exercise testing, and Novak found it during tilt-table testing in people with long COVID.
Digging Deeper
Nobody has done as thorough testing as Edgell is going to do, though. She’s going to give ME/CFS and long-COVID patients 4 tests and see what happens to their brain blood flows. They include:
- Breathing a low oxygen content (10% O2) gas or high CO2 gas (5% CO2) for 5 minutes will test the ability of “chemoreflex” to respond. The chemoreflex alters the breathing pattern in response to changes in CO2 and oxygen. It relies on chemoreceptors that track those gases in the heart and carotid arteries leading to the brainstem. If the breathing pattern in ME/CFS results in low CO2 levels and reduced brain blood flow, breathing these gases should increase CO2 and increase brain blood flow.
- Breathing at a rate of 6 breaths per minute for a total of 8 breaths (paced deep breathing). This test is to determine the activity of the rest/digest relaxation reflex (i.e., vagal activity) as compared to the opposing fight/flight stimulated reflex.
- Completing a 5-10 minute upright tilt (70 degrees head up on a tilt-table) – this test will stress the autonomic nervous system and enable the researchers to determine whether the breathing retraining has improved autonomic nervous system functioning.
- Cognitive testing done before and after will determine if any improvements in cognitive functioning have occurred.
Dr. Edgell reported that thus far, she’s seen low CO2 levels (hypocapnia) in all the ME/CFS participants in the study.
Fibromyalgia and POTS Connection
The Gist
- Heather Edgell Ph.D.’s Ramsay Grant award is a bit unusual – if successful, her inspiratory muscle clinical trial could provide a home-based, cheap and easy way to improve ME/CFS and long-COVID patients’ health.
- Inspiratory muscle training (IMT) uses a small device that restricts the airflow in order to increase respiratory muscle strength. It’s been used to improve breathing, overall functioning, sleep, athletic performance, balance, and others in many respiratory diseases, fibromyalgia, heart failure, and in seniors.
- Edgell’s study – which will also assess CO2 levels, autonomic functioning, blood flows to the brain, and cognitive performance – hopes to increase CO2 levels in her ME/CFS and long-COVID patients. Low CO2 levels are common in these diseases and can cause an extraordinary number of symptoms, including reduced blood flows to the brain.
- Being bedbound can weaken the respiratory muscles and cause shortness of breath and other symptoms.
- The breathing retraining – which consists of taking breathes using a small device – occurs three times a week (36 inhalations each day) – and can permanently instill new and healthier breathing patterns.
- Similar breathing problems to those found in ME/CFS have also been found in fibromyalgia, postural orthostatic tachycardia syndrome (POTS), and long COVID. Two long-COVID breathing retraining clinical trials have found it helpful.
- Edgell’s study should wind up by the end of this year, and publication is expected during the first couple of months of next year.
- Breathing retraining devices are relatively cheap ($30-$60), can be purchased online without a prescription, and can be used at home. It may take a month or so to see results.
Several fibromyalgia studies found that “breathing exercises” reduced pain, improved functionality, improved sleep, reduced fatigue, etc. Just this year, 12 weeks of respiratory muscle training were found to improve respiratory efficiency and quality of life.
Inspiratory muscle training is old hat in postural orthostatic tachycardia syndrome (POTS), where a 2015 study found it improved heart rate control, and a 2022 study found that a “physiotherapy intervention involving education and breathing control” improved breathing scores. Hyperventilation has been found several times in POTS.
Long COVID
Studies have already begun to assess the effects of inspiratory muscle training in long COVID. One long-COVID study, “Outpatient Pulmonary Rehabilitation in Patients with Long COVID Improves Exercise Capacity, Functional Status, Dyspnea, Fatigue, and Quality of Life“, found that 6 weeks of respiratory training (plus individualized patient education, psychosocial counseling by a psychologist, and nutritional education by a nutritionist) improved exercise capacity, functional status, dyspnea, fatigue, and quality of life at least somewhat. Functional status went up one point on the long-COVID functional scale.
They concluded that “IMT may represent an important home-based rehabilitation strategy” for long COVID. They appeared to use the same protocol (36 inhalations a day, a couple of times a week) as Dr. Edgell’s Solve M.E.-funded clinical trial.
Another large (n=281) long-COVID study, “Inspiratory Muscle Training Enhances Recovery Post COVID-19: A Randomised Controlled Trial“, found clinically significant improvements in breathlessness, respiratory strength, and estimated aerobic fitness.
Check out how to do an in-home test for hypocapnic hyperventilation – A Home Postural Hypocapnic Hyperventilation Test for Chronic Fatigue Syndrome and Fibromyalgia.
Recommendations
As the study has not been finished, Dr. Edgell could not recommend inspiratory muscle training. She did suggest that if you find yourself hyperventilating – breathe into a paper bag for a little while – not for too long.
She should have results by December and expects papers to be out by early 2023. Recruiting people with ME/CFS has been going well but (like some other researchers) she had trouble finding people with long COVID.
Inspiratory Muscle Training at Home
One great thing about IMT is that you can do it at home. The device needed is not particularly expensive and the process is easy to learn. The Respiratory Therapy Zone recommends the following trainers. Since some of them are quite different, it might be worth reading the reviews.
- The Breather Respiratory Muscle Trainer – $49.95
- POWERbreathe Plus Resistance Breathing Exerciser Trainer – $68
- AirPhysio Sports Edition Breathing Exerciser – $69.97
- POWERbreathe Plus Fitness Breathing Muscle Trainer – $49.99
- AirPhysio Natural Breathing Lung Expansion Exerciser
- Breather Fit Respiratory Muscle Exerciser Trainer – $59.95
- Expand-A-Lung Sports Breathing Exerciser – $49.90
- Voldyne 5000 Volumetric Incentive Spirometer Exerciser
- Quest Lung Performance Peak Flow Meter – $23.47
Note that it can take a month or so to begin to see results.
(Health Rising does not receive affiliate commissions from the above links.)






I practice Buteyko Breathing, a great technique for improving co2 levels.
Me too…I have had some interesting benefits from buteyko. I promise this is true.
I had candida in my groin that no cream or even surgical solution would make go away. I started buteyko. Within two days the infection was going. It was gone in about four!!! That was a miracle to me.
I did the classical method which involves long breath holds.
The practicioner s warned me that when I got to 40 second co/ bolt score I would have a massive Herxheimer reaction.
In my drive to get better I ignored that and had the most horrific Herxheimer. I literally turned into a puddle. I’ve never seemed like that in my life, it was as if I was in a shower. The raised lymph node on my neck went down the same day. But I felt profoundlyly ill for six months. I stopped out of fear.
The other thing buteyko did was strengthen my collagen. I know this because I switched to wim hof and all that c02 work I’d done was ruined.
But….wim hof is great for loosening up the cardio system and getting you more in touch with your feelings. I didn’t find buteyko did that.
This makes me think I should give classical buteyko another try.
It stopped my candida infection and a raise lymph node that had been there for thirty years!!! But it’s quite a stressful practice.
The other thing I found was that because of my anxiety, my lower respiratory muscles were in total spasm…that’s the other thing I’ve been developing. I now breathe through my stomach and am redeveloping those wasted muscles.
Work in progress for sure
I too have found Buteyko breathing to be helpful for daytime and sleep. Additionally I use mouth tape at night to sleep better and it seems to help with my allergies. Given that over-breathing seems to be an issue for cfs people, I am wondering whether mouth taping during the day might also help, in addition to increasing co2.
I use a swimmer’s nose clip to limit breathing if I’m reading or watching tv.
long time ago, after seen 5 pneumologists, even 1,5 week in hospotal, everytime another diagnosos or not knowing why, from astma to no astma to copd, to no copd, to finally extreme perifere and resporatoire muscle weaknes. it began with a co incidence pre operative excamination of my lungs witch found severe diffusion disturbance. And when they tested me for astma, i needed to inhale something, my alveolair volume from my lungs even dropped further and the pneumologist could totally not understand. i had in between so many breathing excercises, it did not help a bit. i am just to weak, exhausted on a “cellular” level or i do not know where to even speak much or anything, also my boddymuscles, not only my lungs. i wished that the last specialist who said simply verry extreme perifere and respiratoire muscleweakness, would have excamined me further why??? from what does it come that severe weakness??? and that feeling i have also with this study… especially for the 25% home and.or bed bound or simply bedbound 100%. I want so tremendous know why???? and this study is not going to tell me that. you can also say, ofcource you are going to hyperventilate at some point if your muscles do not work or so… if it only was that simple…a bit of breathing excercise… i would not lay here even to exhausted to do them anymore…. and it is again a fairly cheap study…
I hope you will try this Konjin. It can help people with very impaired respiratory muscles and if you’ve been bedbound your respiratory muscles might be weakened just by virtue of you being bedbound.
I’ve never tried it but it looks to me like it consists of taking small puffs. These instruments are not expensive – and low CO2 levels just make everything worse. I think its worth a try!
I guess I’m a little afraid to try this. Every time I had physical therapy, the muscles they worked on got weaker instead of stronger. That was before I realized I had ME/CFS and started pacing though, to prevent PEM’s. Still, even my hands got weaker after hand therapy. Do you think breathing muscles are more resilient than other muscles in ME? I’ll probably wait until the study finishes.
ndeed, i have the feeling they are not looking for the cause. if i try severlly bedridden 98% some breathingexcercise, how my diafragma feels, my ribmuscles, etc they just get totally exhausted and more… and it is again an excercise studdy. when will they finally learn that we can not excercise but must pace?
This study has a lot packed into it – it’s determining, for instance, whether the low CO2 levels its finding are impeding brain blood flows and it’s trying to determine which system might be causing or contributing to them.
It’s not looking for the ultimate cause, though. It’s a clinical trial that’s trying to see if something helps.
Pacing doesn’t necessarily mean not doing any exercise. It means doing the amount of exercise you can do without producing a flare.
I wouldn’t think of this as an “exercise study”, however, in which you build up muscles to feel stronger. The “exercise” that takes place in this study is done in service of something different – increasing CO2 levels and low CO2 levels can produce a lot of symptoms. For instance, they can reduce blood flows to your brain. If it can return CO2 levels to normal it might be quite helpful. Of course, you can do it on your own at your own pace.
The exercise in this study consists of doing something that Dr. Edgell says is like drawing a breathe in from a straw.
You don’t need exercise to increase CO2 – you need to get your metabolism to oxidizing glucose.
Then your muscles will have the energy to relax.
CO2 production is at the heart of the problem. It’s a metabolic problem.
Biology 101 of all living organisms:
energy substrate in –> produces heat and CO2.
[ B1 increases CO2, uninhibits PDH, etc. ]
I wasn’t able to engage in any type of exercise, even Feldenkrais was too much, until my metabolism improved. All kinds of injuries – tendon, ligaments, muscles, joints, nerves. Physical therapy for hypertonia, which involved relaxing the muscle only weakened them more and led to nerve damage. It also led to me becoming severe and bedbound.
I hope they realize that the baseline can be a lot lower than what they think, and even what the person doing them thinks, or looks like.
I’m sure it can benefit some. There is potential to cause great harm too.
Of all the PT I did throughout my whole life, only one had good instincts to understand on the spot how to modify or stop the exercise I was going. One, because she also had similar problems. Two, she had a lot of experience working with children with all sorts of syndromes and diseases that don’t even have names, so that meant no reference to a protocol. She really had to let the patient lead, and not force herself or a set way of doing things on them.
For reference, just getting my diaphragm to relax took months of daily short session of belly breathing on the floor. At the beginning, I kept pulling all sorts of weird muscles – there is one that connects hip/spine/rib.
When I stopped pulling things, I could move on to a full session. Then twice a day, etc.
Now moving on to playing around more with the whole breathing apparatus. In sitting and standing next, etc
This has taken about… seven months.
Hi M – How did you improve your metabolism?
I have the same, very good question!
My muscles are all the same.
You can try this at your pace if you want Vanessa or you might just want to wait for the results of the study. Even if they are positive you probably want to start low and go slow and see how it goes.
The linked study is terrible, no control group and modest improvement after 6 weeks? Maybe most people just get better after 6 weeks. It’s not indicated on the study but the article here indicated they also got diet guidance and therapy, significant co-factors like that completely negate the study outcome re:breathing exercises.
I’d love to hear from anyone who has tried this gadget. I looked into it a couple of years ago, and there were so many reviews on Amazon that said it broke quickly, and that the research support was very questionable, that I didn’t try it. It’s something that intuitively appeals – like sure, why not “train our lungs”. But that doesn’t mean it actually works. So many things that have seemed to intuitively make sense with CFS turn out to be unhelpful or even harmful.
I pointed out that “the linked study” (there were actually several linked studies) was multifactorial and it was one study of several. All the other studies just employed the breathing device. I encourage you to look at those as well..
There are many devices on Amazon – I don’t know which one you are referring to – but I’m sure there are others you could check out.
“It’s something that intuitively appeals – like sure, why not “train our lungs”. But that doesn’t mean it actually works.” – Agreed – that’s why they do these studies 🙂
However, if it helps in long COVID and if it helped in fibromyalgia, I think there’s a good chance it will help some people with ME/CFS.
Hi Kathy,
I have ME after covid and I bought a breather fit. I was part of the mayo study that you are referencing. It definitely helps and you can feel a difference each week. I stopped and noticed a decline in my breathing pattern.
I also do box breathing, 4-7-8 breathing, and Wim Hof breathing. I think all breathing “training” should be thought of as relaxation. It is definitely more effective if done lying on a hard floor or other surface. It’s worth a try…..
Glad to hear it’s helped. Thanks for sharing.
I don’t know if or how this might relate to me, as I have both CFS and severe asthma with moderate COPD (“emphysema-like changes” or airway remodeling). This is obstructive lung disease; I have trouble breathing out, expiration. I have a breathing device that’s different as it gives pressure and vibration as you breathe out to help loosen excess mucus (a PEP or positive expiratory pressure device).
What I wanted to say, especially, is that these devices are quite tiring. I’m mostly homebound and until this last six months spent a lot of time in bed. I had to drastically cut down on the length of time my pulmonary doctor recommended using the device. So, if anyone wants to try an inspiration device at home I’d caution against 36 inspirations at first. Maybe try one or two sets of six first and see how that goes.
I started physical therapy again in October last year. I’m so pleased to have built up from 20 minutes total of sitting upright with 5 minutes of PT to 5-6 hours sitting up daily with 30 minutes of PT every other day. And we started with breathing exercises to strengthen my abdominal muscles…
Thanks, Cherie. You’re using a different device but that’s quite an improvement – from 20 minutes sitting up to 5-6 hours! It suggests that respiratory muscle training can make a real difference. I’m sure it helps that you’re working with a PT as well.
Good advice to start slow and build up. 🙂
i am verry glad for your improvement!!! and also that you write how tiring these “exercises” are. that you need to cut dramaticly back in it laying in bed. I need to survive with my 2% not in bed, what is in fact impossible. i am just way to weak, exchausted, ill to do this excercices. what is PT please? may i ask how you improved from being much bedbound? and what your opinion is, if you are allready 98% bedbound, need the 2% for something else like trying to eat, paying bills, etc? And decline even further? thanks and good luck!!! i hope they find better treatments for astma and copd!!! and ME ofcource!!! ps wich device do you use? i looked it up and saw 2 devices (pep).thanks!!!
Have you heard of the ” frolov device” Cort. It’s another breathing retrainerr designed to increase co2 levels
This is great information and breathing muscles get lazy just like regular muscles if you don’t exercise them. Thanks!!!!
This sounds close to GET. I have been severe for 10 years and woke up with ME/CFS overnight following a virus. Breathlessness was, and remains my worst symptom, and has no link at all to deconditioning. I have OI, poor balance, dizziness, heaviness and so on and my blood O2 reading is always normal. I’ll wait for a cause to be found. I’m hopeful, but I don’t think this gadget would do anything but use spoons I don’t have.
Breathlessness is what this device is designed to help with! And its not necessarily about deconditioning. I asked Dr. Edgell about the effects of being bedbound on breathing because a lot of people are bedbound but since people with asthma, COPD, etc. who are not bedbound benefit from this device it obviously helps people who are not bedbound or deconditioned. The two long COVID studies didn’t focus on people who were bedbound or conditioned – they focused on people like you who came down with the virus and then experienced breathlessness.
Blood 02 readings apparently don’t matter – it’s the low CO2 readings that matter and those could be contributing to the dizziness, heaviness, balance, and other problems. Again, this is not your usual “exercise program” its a program that’s designed to address a chemical imbalance that’s been documented to occur in ME/CFS and could be contributing to a bunch of symptoms. It could also inculcate a new breathing pattern that is more healthful. I think it’s worth a try.
I actually think you’re a good candidate for trying this. As I noted you fit the long COVID profile – breathlessness caused by a virus. The devices are relatively cheap and you can do it at your own pace.
Complaints about The Breather emitting high levels of VOC’s
If you have chemical sensitivities you might want to stay away from that one.
There’s also this interesting review from a COVID patient, though.
“I tested positive for COVID 19 the week before Thanksgiving. This is a very bad illness. Well, one of the symptoms shortness of breath. You can’t walk 10 feet without losing your breath. I found this on Amazon and started using it 2 days ago. I’m not totally breathing normally but I can tell a difference. This is from John Hopkins Hospital. They said you should feel a definite improvement in 6 days. I will continue using this because I don’t know what else to do for my shortness of breath. So far so good!”
https://www.amazon.com/Breather-Inspiratory-Expiratory-Respiratory-Trainer/dp/B00FE8N7Y4/ref=as_li_ss_tl?crid=FPJ0K5N1O5I6&keywords=breathing+exerciser&qid=1574439012&sprefix=breathing+ex,aps,156&sr=8-4&linkCode=sl1&tag=respiratorytherapyzone-20&linkId=a33d6c3c2b796374345b5eddbf34373d&language=en_US
I wonder how this might have similar or different effects to Wim Hof type breathing exercises? My understanding of those is that the fast breathing + holding (on empty, on exhale) is supposed to retrain the body to take in more O2 (but I could be wrong…).
@Lisa,
that is so interesting as there are so many of us who breath-hold
I’m a slight expert on breathing as I’ve tried wim hof and buteyko breathing religiously for the last 8 years.
Basically, through different methods they improve the ” affinity” between co2 and oxygen on the red blood cell.
People make the assumption that you need to breathe in lots of oxygen to saturate the tissue.
In fact, if you hyperventilate, you blow off all the carbon dioxide. Carbon dioxide is needed to push oxygen from the red blood cell into tissue. That’s why you feel light headed or faint if you hyperventilate. Lots of oxygen in the blood stream, but non in the tissue.
It’s called the Bohr effect.
If you retrain your breathing centre, the receptors in your neck respond to accepting more co2 as normal. This then means you get more oxygen into the tissue.
It takes a lot of work
I have read also that it is the poor utilisation of the CO2 that causes poor energy outcomes.
A guy called Ari Whitten is also promoting breathing techniques (on line) akin to what you are describing. He gives a technique to determine a ‘BOLT score’ (cant recall what that stands for) as a baseline before commencing the protocol so that you can judge your initial status and monitor improvements. But it also promotes the concept of effective breathing, NOT deep, and efficient utilisation of each breath.
I am not sure if this could help those who are totally bedbound but i am sure if you made contact with the Energy Blueprint website he may respond.
There may also be overlap with people that have IIH. (idiopathic intracranial hypertension). I have fibromyalgia and POTS. When I started getting pain at the base of my skull and shoulders, I started to read more about IIH. Except for those with some type of structural issue, IIH generally is found in women of child bearing age. The women think there is a hormonal aspect that is generally dismissed by most of the neurologists. Like ME/CFS and FM it is difficult to find a competent doctor that can help. Lots of them suffer with incapacitating headaches and general weakness, and many of them end up getting a brain shunt or stent that may or may not work.
Personally, and I think Cort has touched on this in other studies, it’s the muscles and structure of the spine that are the problem here. So whilst you are gonna get gains strengthening your breathing muscles, there’s essentially a problem with the muscles. Is it eds, is it an energy issue a deficiency? The muscles don’t work and that’s what causes idiopathic intercranial hypotension.
Im male and have suffered from this and it’s when the muscles just spasm in exhaustion, trying to hold the skeleton together and this causes a reflex rise in pressure
Oxygen a good treatment for iih
Shortness of breath feels different from hyperventilation or air hunger. Shortness of breath feels like a lack of fitness when you climb the stairs. Usually with the feeling of physical extreme fatigue throughout the body. Air hunger feels like a lack of air while you can’t breathe properly. Hyperventilation feels like shortness of breath with too deep or too fast breathing while doing nothing. As if your body is running and you are calm. For these different types of distress you need different ways to relieve them. Before you want to use this highly-priced device, you must therefore carefully consider whether it is suitable for your type of breathing problem. A stuck or heavy diaphragm can also be caused by some kind of cramp. You often see this with chronic hyperventilation. This has nothing to do with a weakening of the muscles, but rather with cramping and exhaustion of these muscles. That requires a different approach for which this device would make little sense.
The devices range from $30 to $70 or so. I don’t know about weakening vs exhaustion of the muscles but this device is being specifically used in this ME/CFS and long COVID study to increase the low blood CO2 levels that are believed to be brought about by hyperventilation-like breathing patterns.
“That requires a different approach for which this device would make little sense.”
I just think that I trust the experts more. Dr. Edgell did her PHD on why women have more problems with fainting. She runs the The Edgell lab at York University in Canada and started a woman’s autonomic and respiratory center. She’s co-authored dozens of publications many of which she was the senior or lead author on. Given all that I trust her opinion on whether this training might be effective in this set of patients. W
I have been to respiratory specialists and learned different types of breathing techniques. It can certainly help. If you have breathing problems go to an expert en give it a try (with this divice) or other techniques.
If it is to build up more co2 in the blood and stop hyperventilation, then i agree it can help for a subgroup of patiënts. The diaphagm will be more relax. But it is totally different to shortness of breath.
And i am not impressed by ad verecundiam. Show me a RCT article N100. But the main question: what is the cause of abnormal breathing patterns?
I recommend spending the thirty odd dollars on a kindle version of Healing through Trigger Point Therapy by Devin J. Starlanyl and John Sharkey. They have a very good section on the diaphragm, including a description of how to stretch it. After all, all muscles require stretching before you can exercise them.
I’m an EDS girl who also has a collapsed nasal passage–and shortness of breath–and pain and fatigue. When I had a sleep study they told me I had hypoxia but not apnea. Because of this, insurance would not cover a C-Pap so while researching I discovered that learning to play a didgeridoo helped and sometimes cured people of their breathing problems. So I bought one. $29.
Not sure if this would be appropriate for some of you, but it has helped me immensely. I get so tired (in addition to being fatigued) of doing all kinds of dreary prescribed exercises, at this point I want to do something FUN.
So I put on a CD and toot along pretending I play better than I really do. Playing this instrument is a lot more challenging than one would realize, but it’s more about technique than strength of blowing. It takes lots of experimentation/breath control to create various sounds and rhythms.
Now I’m trying to adapt some of core my P.T. exercises to music…
Go Nancy…. a didgeridoo… brilliant.
Do continue to have fun.
Hi,
I am wondering what kind of training schedule I should follow when using a device mentioned by Dr. Edgell.
Does anyone have suggestions? I am really interested in trying breathing techniques to improve my health.
Ps. Please dont remove this post again.
One the the symptoms related to my form of CFS/ME are panic attacks.
They are not related to a phobia to any kind. They happen at night and they start when I’m deeply asleep. I get these dreams where, for example, the more I try to finish a task the more works get to be done; it can also be the dream where you think you have finally woken up only to find out that your are just progressing incessantly into a continuation of that same dream. It might seem innocuous but they re terrifying. When I finally manage to seemingly will my self in waking up for real, my system has worked itself up in a state of full fledge panic. And yet, I’m a rather relaxed person in my daily activities. I can always be relied upon to quietly and efficiently take charge in an emergency situation, unless I’m in one of my bed ridden episodes, of course. These nightly panic attacks started with CFS.
About 10 years ago, I went to through a week of what gave me an idea of what living in hell must feel like. I went to my local ER and didn’t get much help. The second night, after popping Ativan that turned out absolutely useless and trying all sorts of relaxing techniques that actually worsened my anxiety.
In Quebec, we have this 811 help line. I had used it before when someone in my family, or me, were in need of care. You get to talk to an experienced nurse who will ask lot of pertinent questions and either explain step by step want can be done at home and what signs to watch for if the situation worsens; or, she will recommend an OTC and direct you to a pharmacy. When she feels that doctor’s intervention is needed, she’ll say so.
So there I am, calling 811 at o’clock at night, trying, against all odds to get relief, any kind of relief. The nurse got me right away. She did give me very sound advice about medication, but mainly, she grabbed a social worker who was out the door, having finished his shift. The nurse told me he was an expert on different breathing techniques.
The man evaluates the intensity level of my anxiety and starts the breathing lesson. He spent over 45 minutes with me on the phone, practising with me. His unusual technique has served me well for over ten years. It’s not easy, though.
So, this “Breathing/Oxygen Series on Health Rising” is extremely interesting. I’m sure that more effective breathing is not a cure all, but it is certainly worth exploring. I will not buy the device yet, but I might ask my GP to refer me to a “breathing clinic”. I think we have one at our local hospital.
I’m grateful to all the members who posted here and shared their precious knowledge on this subject. And, of course, thank you Cort, for unceasingly opening new avenues to explore. 🙂
I bought a breather a few months ago and used it 3 days in a row and then forgot about it. I guess I can incorporate it back into my schedule for a few months and see what happens. I do suffer terrible shortness of breath and stiff ribs and solar plexus area.
I keep telling people to try Oxycise. 15-20 minutes a day, you don’t have to do it all at the same time. It’s deep breathing with Isometric poses, 30 positions at 4 deep breaths each.
Not selling anything, you can get the book used on Amazon.
Oxycise.com
With one of these breathing tools, do you want to have resistance on just the inhalation, or on the exhalation too?
I haven’t been able to figure it out even after a google. inspiratory muscle training suggests the inhale is important but i wanted to clarify!
This study in pwCOPD suggests resistance for both inhale and exhale is better (for that population)
https://respiratory-research.biomedcentral.com/articles/10.1186/s12931-018-0917-6
Although here it suggests that training with resistance to both at the same time is uncomfortable and actually has less benefits than training separately…
Ok google detectiving session over, if anyone has more knowledge I’d love to hear
https://www.powerbreathe.com/what-is-expiratory-muscle-strength-training/
I started using The Breather several months ago for air hunger, and I can say that it has done a fantastic job. It makes my lungs feel like they felt many years ago when I was a competitive swimmer, and I am no longer out of breath just doing regular stuff. I started with 3 sets of 10 inhalation/exhalation set/day, and have progressed to the point where I can easily use it for 10 or 15 minutes at a time, at the hardest level, if I get distracted.
Great to hear Alice – thanks for sharing that! 🙂
Carolstudier@yahoo.com
Alice, did you set both inhale and exhale to the same resistance setting? I just got mine but am confused on how to improve my CO2 specifically. Thanks. So glad it helped you. (Cory, can you delete my goof posting?! Thanks)
Hello all,
I am ‘lurking’ on Healthrising for some time now, and wanted to step in on this subject.
As a 39-year old ME CFS patient I’m very interested in this study, but I can’t seem to find home training schedules for “Inspiratory muscle training” for ME patients from dr Edgell.
Are there any generic schedules I should look out for or am I missing something? And does it matter which device I should purchase when looking into the schedules more specifically?
Cheers
I hope Dr Edgell’s results will be out soon. It seems the trial is complete but no publications yet:
https://clinicaltrials.gov/study/NCT05196529?term=heather%20edgell&rank=1#publications
Looks like the trial was completed last year, but no results have been posted:
https://clinicaltrials.gov/study/NCT05196529?term=heather%20edgell&rank=1
I could not find any publications that related to the study on PubMed:
https://pubmed.ncbi.nlm.nih.gov/?term=Edgell+H&sort=date