

A large CDC exercise study highlights breathing abnormalities in ME/CFS – but points a finger at the muscles.
Part one of a series on breathing and oxygenation in chronic fatigue syndrome (ME/CFS) and long COVID focuses on a large study that prompted a reassessment of what’s happening during exercise in ME/CFS.
Breathing problems – particularly shortness of breath or experiencing “air hunger” – have shown up in chronic fatigue syndrome (ME/CFS) for a long time, but only recently has breathing become a research focus. That didn’t happen because of patient complaints; it happened when exercise studies suggest that something with the breathing had gone awry during exercise.
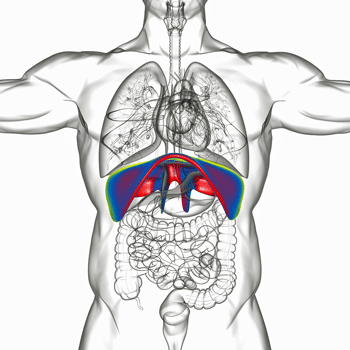
A small muscle at the bottom of the lungs is responsible for having us breathe when we’re not exercising.
In a way, that’s not a surprise at all. Breathing, after all, is inseparable from energy production. Breathing is what the body does to deliver fuel (oxygen) to the mitochondria in our cells. It is also the way our body removes the by-products of energy production (carbon dioxide) from our cells. Our breathing fluctuates depending on our energy needs. We breathe more deeply and rapidly during exercise to deliver more oxygen to our working muscles and more importantly, to remove the CO2 that’s starting to build up. Breathing is fundamental to being able to produce energy. It’s also quite a complex process.
The Signaling Process – Breathing is largely an automatic process controlled by a signaling process between chemoreceptors in the aorta in the heart and carotid arteries that supply oxygen to the head that are constantly sending information about oxygen and carbon dioxide levels to the respiratory centers in the brainstem. Increased levels of CO2 – a toxin at high levels – prompt the brainstem to increase breathing depth and/or speed in order to reduce them. On the other hand, decreased levels of CO2 prompt the brainstem to send signals that reduce breathing in order to allow them to build up to normal levels again.
The Muscles – Normal breathing is accomplished via the diaphragm – a thin kind of dome-shaped muscle – that sits between the lungs and abdomen. Its goal is simply to change the lung volume and create a pressure gradient between the inside of the lungs and the outside of them such that air rushes in to fill the void.
To cause an inhale, the diaphragm pulls downward – causing the lungs to expand – producing a drop in air pressure and the buildup of a pressure gradient between the lungs and the outside of the body. The inrushing air produces an inhale. It’s all driven by muscular activity. The phrenic nerve, which runs from the neck to the diaphragm, controls the movement of the diaphragm. When we’re active, though, the abdominal muscles help us breathe more quickly and deeply.
It’s clear that in order for the breathing process to work correctly, a number of things have to happen: the chemoreceptors have to correctly sense the gases present, and correctly send the right signals to the brainstem; the brainstem has to correctly process them, then send the correct signal to the muscles that move the lungs; which then have to correctly move them.
While exercise and breathing are intimately connected, only recently have exercise tests in ME/CFS begun to focus more on ventilation – the process of moving air through the lungs – in ME/CFS. This is partially because standard measures of ventilation haven’t been very revealing. More findings have suggested that energy production is limited, and that people with ME/CFS blow through their aerobic energy production capacity quickly and hit their anaerobic threshold. When that happens, energy production drops and symptoms increase dramatically.
Recently, though, both tilt-table and exercise stress tests suggest that a large subset of people with ME/CFS or long COVID often exhibit hypocapnia – abnormally low levels of CO2 – caused by hyperventilation (abnormally deep and/or rapid breathing). In fact, one study found that hypocapnia was far more common in ME/CFS than other forms of orthostatic intolerance such as postural orthostatic tachycardia syndrome (POTS).
Since low CO2 levels can produce many of the symptoms found in ME/CFS / long COVID it’s possible that an altered breathing pattern could play a major role in these diseases. With the hypocapnia findings, more focus has been placed on understanding how people with ME/CFS and long COVID breathe – particularly during stressful situations such as exercise, standing, or even in some cases sitting up.
Exercise Study Prompts Reassessment
A recent large study, “Cardiopulmonary, metabolic, and perceptual responses during exercise in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS): A Multi-site Clinical Assessment of ME/CFS (MCAM) sub-study,” took the breathing issue to an entirely new level.
This wasn’t just any study. It was a 403-person (!) exercise study from the CDC’s big multi-site study. Featuring patients from a bevy of ME/CFS experts, it’s the first major study to come out of the multi-site study which began long enough ago for most of us to forget it had ever happened.
Conducted by Dane Cook Ph.D.- an exercise physiologist who’s been studying exercise, pain, and brain functioning in ME/CFS, Gulf War Syndrome, and Alzheimer’s for over 20 years – it was one of the biggest cardiopulmonary exercise (CPET) studies yet done in ME/CFS, and if its authors are correct, the most rigorous.

When Cook controlled for fitness, some of the abnormalities of energy production disappeared.
Cook and friends have called into question whether past exercise studies have adequately taken into account the low fitness levels that naturally accrue to post-exertional disease.
To attempt to remedy that, the study compared people with ME/CFS to “fitness-matched healthy controls”. These were controls who exhibited near-identical peak oxygen consumption during the exercise test; i.e. at their peak, they produced the same amount of energy as did their counterparts with ME/CFS. (They tended to be in the low-normal range). They also discarded about 10% of the patients who didn’t meet their criteria for producing a maximal effort (certain heart rate level). (Having 90% of the ME/CFS patients meet the criteria for maximal effort was a good number.)
Once they matched for fitness, they found that ME/CFS patients did not hit their anaerobic threshold at lower levels of peak oxygen consumption, heart rates, lactate or work levels (watts). They suggested these are all the result of low fitness and do not reflect inherent problems in ME/CFS. Nor did they find increased rates of lactate production in ME/CFS.
(I’m not sure if I’m understanding this right but could there be a chicken and egg problem here? Did the patients who did not meet their age-adjusted expected heart rate not meet it because they had chronotropic incompetence? Some studies have concluded that problems with energy production actually preclude people with ME/CFS from reaching their expected maximal heart rate. Could the ME/CFS patients’ peak VO2 levels reflect low fitness because of their problems producing energy?
Is that kind of low fitness different from that found in healthy controls? If healthy controls have low fitness because they don’t exercise much and ME/CFS patients have low fitness because they can’t exercise – doesn’t that matter? Could Cook’s decision to treat low fitness healthy controls and low fitness ME/CFS patients the same – lead to the reintroduction of graded exercise therapy (GET) in an attempt to increase the fitness levels of ME/CFS patients? The paper does suggest CPET-guided exercise programs might be helpful – which is good – but one wonders if it’s inadvertently opened some wiggle room for other exercise prescriptions ).
At this point, the group seemed to be well on their way to erasing any idea that exercise is impacting energy functioning ME/CFS. As we’ll see, that wasn’t true at all. In the end, in fact, the authors actually arrived at a similar place as other researchers – they just came to it from a different direction.
A Gas Exchange Disease?
The big problem this big study found concerned gas exchange – the ability to perfuse oxygen into the muscles and remove carbon dioxide from the blood. The ME/CFS patients did reach their anaerobic threshold at lower levels of ventilation, at lower levels of ventilatory efficiency, and with fewer breaths – and here was the kicker – while moving more air overall. (These indices were also reduced at their peaks).
Remembering that breathing = energy, the people with ME/CFS exhausted their aerobic energy capacity with fewer breaths than did the healthy controls. The authors concluded they had “inefficient exercise ventilation”. The findings were:
- VE/VO2 – increased
- VE/CO2 (ventilatory efficiency) – increased
- VT (tidal volume) – increased
- fR (breathing frequency) – reduced.
VE/VO2 increased – VE/VO2 is the amount of ventilation or breathing done relative to the amount of oxygen consumed; i.e. the amount of energy produced. (Oxygen = energy). To put it in simpler terms, it revealed that people with ME/CFS were doing more breathing to produce energy than the fitness-matched healthy controls. Plus their breathing didn’t go as far: they entered their anaerobic threshold more quickly.
Cook explained that this breathing pattern may be an attempt to improve “alveolar ventilation”; i.e. to get the air sacs or alveoli in the lungs as filled up as possible with oxygen – in order to squeeze as much oxygen as possible into the muscles.
Cook also referred to the “Robin Hood effect” where low CO2 levels (hypocapnia) cause a paradoxical decrease in blood flows when they are most needed. This could result in vasoconstriction or narrowing of the blood vessels in the muscles that move the lungs. Noting that the respiratory muscles are always working, Staci Stevens, an exercise physiologist at Workwell Foundation, suggested some time ago that fatigued respiratory muscles could be causing problems.
High VE/CO2 (ventilatory efficiency) – Ventilatory Inefficiency Elevated – Ventilatory efficiency refers to the amount of ventilation present relative to the amount of CO2 present. The high level of ventilation relative to the amount of CO2 present suggested that the lungs of people with ME/CFS were working harder than usual to get rid of CO2.
This is often due to lung damage that results in increased levels of “dead air space”. The dead air space idea, though, appears to be a dead-end in ME/CFS and long COVID. The lungs appear to be structurally fine – they’re just working strangely. The problem more appears – as the authors noted in their paper – to be a reduction “in perfusion to active skeletal muscle”.
Whatever the situation, the authors noted that the ventilatory inefficiency found in ME/CFS has also been associated with poor exercise capacity and exercise intolerance in other diseases.
A “Unique Breathing Strategy”
Using a more fine-tuned approach than has been done before, the authors uncovered “a unique breathing strategy” in the ME/CFS group. Instead of breathing more deeply and rapidly, the ME/CFS group was breathing more deeply and slowly. As noted above the authors suggested that people with ME/CFS may be breathing this way to increase the oxygen flows to their muscles. In other words, the body is trying to compensate for a problem with energy production at the muscle level.
Interestingly, they found the same unusual – even unique – breathing pattern in people with Gulf War Illness. The fact that this same strange breathing pattern has shown up in these two symptomatically similar, but really quite different, illnesses suggests that at their heart, these two diseases share some core biological features.
Recently, a long COVID study that assessed breathing patterns during exercise found that almost 90% of long COVID patients demonstrated dysfunctional breathing patterns.
Cook has also done a lot of work on pain and also suggested that this strange breathing could also be the result of an (unconscious) but learned approach to reduce symptoms.
Dane Cook’s Presentation at the ME/CFS Stakeholders CDC Call
Or a Muscle Metabolism Disease?
Their main thrust, though, involved poor oxygen and CO2 extraction. While the authors acknowledged that problems with ventilation and heart rate exist in ME/CFS, and that much remains to be learned, they believe that they’re probably secondary to the real problem – an inability to produce sufficient amounts of energy at the muscle level.
They referred to Vermeulen’s 2014 Dutch exercise study which concluded that the exercise intolerance in ME/CFS was caused by low muscle oxygen uptake (read energy production) by the muscle cells. During the CDC talk, Cook also noted that their results are consistent with David Systrom’s group, which suggests that poor delivery of blood to muscles and poor utilization of oxygen by the muscles is present.
That suggests that the ventilation problem is actually a muscle metabolism problem; i.e. the muscles are getting pushed into anaerobic metabolism – which the body is attempting to compensate for with the strange breathing pattern. That breathing may, however, be producing low CO2 levels (hypocapnia) which may cause more symptoms. Cook did say that breathing exercises might be able to help with that. (A blog on that is coming up.)
The GIST
- It’s been underway so long that many people have probably forgotten about the CDC’s big experiment that about ten years ago began to assess hundreds of people with ME/CFS who were seeing ME/CFS experts.
- The first paper to come out of the big study was a big one indeed: hundreds of people engaged in the biggest exercise study ever done. The maximal exercise study came with a twist: it used peak energy production as a measure of fitness to match ME/CFS patients with healthy controls.
- The idea was to make sure that ME/CFS patients’ level of fitness – due to their disease or inactivity – was not skewing their findings downwards. The authors concluded that several measures of energy production (oxygen consumption, reduced heart rates) that have prominently figured in the ME/CFS literature, reflected the low fitness levels found in ME/CFS and were not inherently a part of the disease itself. (See the blog for some questions about that.)
- On the other hand, problems with breathing were found even in the fitness-matched groups. The core finding concerned problems with “gas exchange”; i.e. the ability to get oxygen into the tissues and remove carbon dioxide. This showed up in the ME/CFS patients having to breathe more to produce energy and remove carbon dioxide.
- A deeper dive into the breathing patterns found that the people with ME/CFS were breathing more deeply and more slowly during exercise than the healthy controls. Dane Cook, the leader of the group, suggested in a CDC talk last year, that the ME/CFS patients were trying to load the air sacs in their lungs with more oxygen.
- It’s also possible that hypocapnia – low levels of CO2 caused by that breathing pattern – may be vasoconstricting the blood vessels leading to the muscles moving the lungs – causing muscle fatigue and these strange breathing patterns. Another possibility concerns an attempt to avoid pain that ends up shutting down motor signals from the brain that tells the body to move and causing fatigue.
- The study results suggesting poor oxygen extraction by the muscles in ME/CFS fit with several past findings including David Systrom’s invasive exercise studies. While a variety of issues could be contributing to this including deformed red blood cells Cook appeared to be most interested in the possibility that mitochondrial issues were to blame.
Increased Perception of Effort
The biggest difference between the ME/CFS patients and the healthy controls, though, was how much more difficult the ME/CFS patients perceived the exercise to be. I wonder if anyone would disagree with the authors’ assertion:
“Based on the preponderance of data, it can be concluded that people with ME/CFS perceive exercise as requiring more effort than otherwise healthy people.”
That could be because the pain they’re experiencing basically causes the brain to shut down signals to the muscles – which makes it harder to get them to move. The authors went back to a small 1999 study which suggested that the increased perception of effort in ME/CFS was associated with a “diminution in central motor drive“; i.e. the motor centers of the brain are not giving the muscles the signals they need to move. When that happens, you have to focus and push harder to get those signals telling the muscles to move through – thus experiencing an “increased perception” of effort.
A similar scenario may be occurring with regard to mental effort. The slow information processing and poor sensory filtering processes appear to make cognitive tasks more effortful in people with ME/CFS/FM. In the same general way that ME/CFS patients’ lungs may be working harder to provide oxygen to the muscles, the brains of people with ME/CFS have to exert more effort in order to compensate for the slowed information processing and the diversion of mental resources that comes part and parcel with these diseases.
Deconditioning Hypothesis Slammed
Finally, Cook emphasized how damaging the idea that ME/CFS is a disease of low aerobic fitness (i.e. a disease of deconditioning) has been. Speaking as an exercise physiologist, Cook stated there was no scientific reason to believe that. He called it a “false narrative propagated by non-exercise scientists” which has “produced a lot of noise” and has held up the field. Ironically, Cook argued that poor aerobic fitness – not a pathophysiological problem – was responsible for the false findings of low VO2, etc. in ME/CFS. but then asserted that efforts to blame low aerobic fitness for ME/CFS were wrong.
The authors noted the limitations of CPET studies. For one, they can suggest that problems with oxygen delivery exist, but they can’t show that they do. For that, we need … invasive exercise studies – which we certainly have 🙂 – and more sophisticated tests of ventilatory and mitochondrial functioning. They also noted that the problem is probably worse than the studies show, as only the healthier people with ME/CFS tend to volunteer for exercise studies.
Conclusion
One of the strangest studies yet, this study first appeared to overturn about a decade of thought on the exercise situation in ME/CFS. Using hundreds of patients from ME/CFS experts, and healthy controls, the fitness matching of ME/CFS patients to healthy controls caused energy production problems like an inability to reach peak VO2 and to achieve normal heart rates during exercise to disappear. In place of those, though, the study found that people with ME/CFS manifested a strange breathing pattern (deep and slow) which left the lungs working overtime to get oxygen into the muscles and remove carbon dioxide from their blood.
Whether or not the fitness matching was necessary the authors were left with a similar conclusion as past studies: poor energy production at the levels of the muscles was probably driving the breathing and exercise problems in ME/CFS. The authors suggested that during exercise, people with ME/CFS were attempting to (subconsciously) compensate for the problems with gas exchange at the level of the muscles by breathing more deeply and slowly – thus driving more oxygen into their lungs. By doing that, though, at least some of them may be reducing their CO2 levels – causing symptoms similar to those found in ME/CFS. It’s also possible that fatigued respiratory muscles, poor signaling from the oxygen and CO2 receptors, or brainstem problems were playing a role.
Ultimately, though, Cook appeared to put his money on mitochondria problems – leaving him in a similar place to the other exercise physiologists who have studied ME/CFS.
Check out a clinical trial that’s trying to change how people with ME/CS and long COVID breathe in order to increase their CO2 levels.
Health Rising’s Summer Donation Drive was a Success!
Thanks to the over 200 people who contributed over $17,500 to Health Rising – allowing us to blast through our target ($15,000) – and end the donation drive early. Some more support is coming in and we’ll announce the totals when we get caught up.
Thank you so much!


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



Mitochondria keeps coming up, surely there really is something to the mitochondria and ME/CFS???
Too many smoke signals for there not to be.
EVERY disease has a mitochondrial element. It can not be any other way.
That may be true – I don’t know – but is it true that mitochondrial problems play a core role in every disease? The thing about the mitochondria, for me, is that they fits so well with the problems in energy production found. It’s such a darn good fit. I don’t if you can say that for other diseases. There are some interesting ideas about the role the mitochondria play in pain, however. And there’s Naviaux’s findings that the mitochondria play a key role in the immune response – so they do get around – that’s for sure. 🙂
I would like to be in 1 of your
Studies, it sounds like your heading for some answers!
I have been dealing with S.O.B.
For over 3 years!
I’ve been to a Cardiologist!
I’ve been to a lung specialist, they have me on on 7 different medications
I’m still having shortness of breathe !
Health Rising doesn’t actually do studies – we just report on them – but we are going to have a way for you to easily find studies in your area coming up.
The symptoms dont fit other mitochondrial diseases tbh. Take hereditary mitochondrial diseases and compare them to Cfs yourself to find out. Yes, the mitochondria are affect, No, it isnt the main problem.
I ve Been dx with pots and CFS. Breathing and chest wall fatigue is one of my worst and most consistent symptom. All I want is to breathe normally again. I also have muscle spasticity in a couple localized areas.. I hope they find a remedy.
Would Gabapentine help you? It is prescribed mostly for MS-Hug like pain.
I have spoken to Stacie Stevens at WorkWell Foundation about Chronotropic incompetence. She believes all ME/CFS patients exhibit this.
I talk about my diagnoses and very detailed mitochondrial results from Germany, Comment 210 I believe, in the recent thread about James and his recovery from CIRS. Three subjects ago or so. Definitely a huge part of this.
This study is also spot on with the deep slow breathing. I have always wondered why I did this during exercise, on stress tests to perform better even before I knew I was sick, now in daily life. Sometimes I stop a breath cycle mid stream to start a long slow breath. I remember looking at Dr. Lapp in disbelief when he told me I had reached my AT in 2:23 seconds after achieving my VO2 Max, etc. That test took far too much out of me even back then. I didn’t have a clue what was really happening. A year before that, knowing I was really unwell, but not knowing why, I achieved a 9 out of 10 Duke Treadmill Score. I breathed very slowly and deeply the entire time until the speed would no longer allow. I didn’t know that I should not have been exercising. But I kept trying. Today I am lucky to have my feet on the ground for short periods.
I don’t know what the answers are for helping us but true understanding of many facets of ME CFS are being uncovered.
The 2:23 wall is really something given that from what I understand we do start off relying on anaerobic energy, switch to aerobic, and then when that’s exhausted, switch back to anaerobic. That sounds like a very short time in aerobic energy production. I should look up my exercise test as there’s no way that I’m deconditioned. I may not be fit for sure but I’m not deconditioned.
Dr Sarah Myhill developed a mitochondrial test for CFS. If I remember rightly she found that CFS sufferers mitochondria (somehow) showed low energy compared to healthy people.
(I’m not very sciencey so I’m probably not using precise terminology!)
Does anyone have any thoughts on that test?
I recognize so well the deep and slow breathing! I do that! Always thought it was very strange: shouldn’t I be breathing quicker and shallower? I’m so looking forward to your blog on breathing! I’ve been doing Wim Hoff breathing for a while hoping I’ll help the transportation of oxygen to my mitochondria – if that is an issue…but I have no clue if I’m doing good or worsening the problem and actually doing harm. Like the time I insisted on GET and just crashed more and more until I realized how bad that was. Oh, somebody, please get the answers soon!
Thank you, Court, for your fantastic blogs and hard work for all of us!
I agree and look forward to possible breathing exercises.
Thank you for sharing your thoughts. I have the same experience as you. When I try to follow the slow breathing instructions of a guided meditation exercise, I feel like the instructor is not giving me enough time to complete a breathing cycle. I started to suspect my breathing rate is much slower than the national people. The advice to slow down breathing to overcome shortness of breath and anxiety seems don’t work for me. Yesterday, I thought, ok, I will try to do the opposite of the advice given in everywhere. I deliveratly tried to speed up my breathing rate. I was surprised to see my shortness of breath reduced very much. My chest tightness and anxiety have almost gone. I am feeling less fatigue and pain. I wonder if hyperventilation is the root of all my health issues.
Sorry I made some spelling mistakes due to faulty autocorrelation of my typing.
The word “national” will be normal. And the “hyperventilation” will be hypoventilation.
Thanks.
Would oxygen therapy be helpful at all in reducing symptoms here? Using an O2 concentrator for example- at least increasing the amount of 02 available in the system?
That’s a great question. The HBOT studies in fibromyalgia have had pretty good results
https://www.healthrising.org/blog/2015/06/26/new-age-fluff-or-real-treatment-fibromyalgia-hyperbaric-oxygen-therapy-study-opens-eyes/
and another study popped up in long COVID I believe.
Some French doctors are using oxygen to treat issues related to Ehlers-Danlos too! I do wonder if there is an overlap of problems.
I also wonder about ME/CFS fatigue that is not so related to exercise–like when it comes from too much brain input. I get PEM from going to doctor’s appointments and that doesn’t involve much exercise at all…
Ah – this rings some bells for me! I’ve had CFS since 1983, but after the first 3-4 years, I had recovered enough that I was able to get back into scuba diving (the primary skill for which is being able to fall overboard and sink). I refused to get a newer regulator when they came out, because I LIKED having to take long, slow breaths – it felt necessary to me. And when the industry started using Nitrox, which is 32-36% oxygen (air is 20%), I felt like a whole new world had opened up to me. As you go deeper the partial pressure of oxygen increases, and I felt totally juiced! I was stronger, had more energy, and felt considerably less tired after each dive. I joked about diving on Nitrox being hyperbaric oxygen therapy. On one weeks-long live-aboard trip, one of my fellow passengers remarked that each day, I looked younger than the day before.
Judith:
What you wriye is interesting in light of that UK doctor with long covid that recovered pretty quickly and then went on to say it is a psychological condition. He went on scuba diving trip – I wondered if that affected something…
There is also the water pressure, what that does to our veins, blood pressure, etc.
Just being in the water up to my waist, my HR comes down etc, and I can move in ways I can’t on land.
I wonder that as well. I have a prescription for oxygen during exertion and sleep, for asthma-COPD, but find I’m much more alert and active if I wear it all the time. My family noticed this shortly after I got the oxygen following a severe flare-up from flu, pneumonia, sepsis and respiratory distress. My pulse oximeter shows adequate oxygen saturation levels at rest, though it drops from about 97% to about 92% without the oxygen. I sometimes don’t notice a difference in alertness or activity—i notice more fatigue and brain fog.
My breathing problems improve drastically when I started taking LDN, I don’t know why… somebody?
Before that it was like I had to breathe “on porpoise”, like my breathing wasn’t automatic anymore ( obviously It wasn’t true, but that was my sensation)
After starting with LDN I can forget my breathing when resting, it’s automatic again and doesn’t demand anything from me
With “activity” is not so efficient
Barbara, what about other ME/CFS symptoms, like PEM for one? Do they improve with LDN? A NIH abstract says it may operate as a novel anti-inflammatory agent in the central nervous system and as a glial cell modulator, so I was wondering.
Tracey, yes, LDN had also a positive effect in my flare ups: less often, less deep and I recovered from them sooner. Flare ups were still there but everything was more stable, within the very low energy.
I speak in past tense because I have premenopause since December and now I am practically in a constant flare.
I have increased the dose of LDN (very slowly) but no improvement yet
Did you read the study? What makes you think that a lack of oxygen in the lungs is the problem in CFS?
My SpO2 is fine. I’m guessing that the SpO2 of most people-with-CFS is fine, otherwise it would have been flagged decades ago.
If anything, the question is whether the O2 you *do* have in your blood is getting into the cells, and then into mitochondria: erythrocyte > endothelium > cell wall > cytoplasm > mitochondria > electron transport chain.
There’s some evidence that cells (in PwMECFS) are not oxidizing glucose or fatty acids. Is that because of enzyme deficiency (as some researchers claimed)? Or because of oxygen deficiency? Or something else?
My oxygen level is typically fine , but it has dropped with excessive heat or exertion. The problem is most Drs don’t test your oxygen after 30 minutes of activity but rather sitting in a Dr office… Numerous people in the FB pots group have documented changes in their oxygenation. Mine can drop from 98 down to 93 on a humid day and I’ve seen it at 89 when I tried to shovel the driveway. Drs so far have refused to give me oxygen. Stating that I have to consistently go under 90 and that too much oxygen is detrimental. Ugh.
Exactly this. The body doesn’t use the O2 in your body. So you don’t create Co2. Following this, your breathing slow down bc you are in a hypocapnia State. To tell ppl now to breath faster could even prob. kill them.
I find Hyperbaric oxygen helps
I have an integrative doctor who does oxygen therapy. He says it would be very helpful but the problem is the cost.
Steve, what is a typical cost?
I’m starting a trial tomorrow. If my ears can cope I’ll have 20 sessions, 3 a week. They wanted me to do 5 straight off but I need transport to get there. Will try to remember to feed back how it goes for me.
Good article – I’ve been trying to figure out why I hit a wall so fast with aerobic exercise even though I am able to do a lot of other slower exercise.
I’ve seen 4 mitochondrial specialists after finding through treadmill metabolic testing that I am burning glucose and have lousy fatty acid oxidation. The mito specialists all agreed I have mito issues but didn’t know what to do as they can’t find a genetic problem. There are no specialists for secondary mito dysfunction, not caused by genetics.
A recent bout of intense aerobic exercise triggered atrial fibrillation. Wondering if it’s related to my POTS/ autonomic dysfunction?
Any treatment suggested?
@Learner,
I’m like you. I do awful with aerobic exercise but I can go for a long, long time doing slower exercise (like walking as opposed to running).
I have read about slow and fast twitch muscles, which are supposedly genetic and wonder if that has any thing to do with it.
People mentioning the beneficial effects of oxygen, especially Judith who mentioned Nitrox via scuba diving, really intrigue me. I wonder if this could be adapted as a treatment modality.
Today I am so frustrated. Beautiful day but I am hobbled by lack of energy. I am frustrated many days and reading about all the troubling world news doesn’t help. Doctors don’t seem to help either. I get the feeling I’m in a long line of ‘your labs were normal–next.’ Where is there help?
Me too!!!! Really can’t do intense aerobic activity, but can walk OK quite far (I recently did a two hour walk) Weird? Fairly common with this illness?
Thoughts on why this might be the case? Something to do with the muscles having to work much harder on intense aerobic activity?
Where do you find mitochondria experts?
This is very interesting and I think a useful avenue to pursue. I have definitely noticed that many of my worst crashes were initiated and reliably even perpetuated by talking, as strange as it sounds. It appears to take a lot of energy to move those breathing muscles to talk, and I have always suspected there is some kind of dysfunctional oxygen/co2 balance, etc. mechanism at work.
And again regarding deconditioning, the idea is illogical and clearly ludicrous, as exercise is precisely the thing that improves deconditioning, while it makes ME/CFS worse. When a person is crashed from ME/CFS effects, complete rest in fact is the fastest way to recovery, and the more rest the better. That’s completely the opposite of the definition of deconditioning, which states that the fatigue is caused by not having had enough exercise and the way to improve it is to exercise more. So hopefully we can finally put that old notion to rest – no pun intended.
Rick, everything you wrote is questionable.
“This is very interesting and I think a useful avenue to pursue.”
Maybe. None of it is new, really.
“I have definitely noticed that many of my worst crashes were initiated and reliably even perpetuated by talking, as strange as it sounds.”
Do yourself a favor – stop.
“I have always suspected there is some kind of dysfunctional oxygen/co2 balance, etc. mechanism at work.”
Yes, you solved CFS years ago. If only we’d all listened!
“And again regarding deconditioning, the idea is illogical and clearly ludicrous…”
It’s ludicrous to think that inactivity creates deconditioning? (Which is the very definition of “deconditioning” – it is a condition created by inactivity.)
“When a person is crashed from ME/CFS effects, complete rest in fact is the fastest way to recovery, and the more rest the better.”
Really? Where’s the evidence for that? Most experts recommend aerobic exercise for recovery.
“That’s completely the opposite of the definition of deconditioning, which states that the fatigue is caused by not having had enough exercise and the way to improve it is to exercise more.”
Huh? Where? Who says that?
“So hopefully we can finally put that old notion to rest – no pun intended.”
Of course, you didn’t intend it.
Steady on ‘JustTheFacts’.
There’s no need to be like that
Everything I wrote is a fact based on medical definitions of deconditioning and my own experience of living with ME for 22 years.
Furthermore, just to add to my earlier observations, many people, including myself, have acquired ME/CFS suddenly, even in a single day. Obviously a person doesn’t become “deconditioned” in a single day, and needless to say (although with someone like you it probably is needed, so I’ll say it) the idea is therefore as ludicrous as your poorly conceived and misplaced antgonistic remarks.
Your only credentials here, in fact, appear to be 22 years or more of missed psychiatric appointments. I strongly suggest you start going; in my estimation you’re unlikely to get better from your significant problems on your own. Good luck!
My impression is that someone from the CBT/GET brigade has been trolling the comment section under different names lately, pretending to be ME/CFS patients (‘JustTheFacts, in another discussion they were called ‘Martin’). Or just some other sad troll. I suggest everyone better ignore them
Wow just the facts a really harsh uncalled for reply
Who are these “most experts”? JustTheFacts, I’d like to see names. “Most” is a strong claim.
This has been eye opening for me. Never related the breathing to CFS but should have. Ive noticed I’m breathing slow and deep like yoga breathing or like Dr. Weil with his 4-7-8. Did not make me feel better at all. Ive been putting this off on severe anxiety and want to take a benzo more frequently to reduce what I think is anxiety as this state is so very uncomfortable. So, this is interesting but don’t know what to do about it. Was thinking of going to psychiatrist to discuss severe anxiety and knowing they love those SSRIs and SNRIs. They are bad for me. And to even find a psychiatrist is not like it use to be. Just pass me a benzo and give me some relief. Oh, man, this disease is so debilitating in so many ways and many still don’t believe it’s real.
What a silly post
Good observation re talking causing crashes I have the same experience. Could it be that this messes up the breathing pattern and causes extra strain?
I’m also crashing if I talk too much. I feel very strongly that I don’t have the muscle force to get the words/sound out and I feel a tightening of my chest and the air hunger. I believe breathing problems is definitely at play. Very interesting!
CO2 moves out faster through mouth than nose. I kept a strict no talking policy and I became more aware of not mouth breathing during the day or sleep.
That was definitely somethign that helped me in playing the never-crashing game. I can talk now, I still can’t sing for long.
Rick, a kind of “diaphragm energy” fatigue caused by conversational talking that I experience sounds similar to what you’ve identified. Periods of time when it would set in most rapidly when talking left no doubt about the effect.
after having CFS for 40 years and shortness of breath becoming my worst symptom about 5 years ago and tried treatment for POTS with mestinon but nothing has helped
my breathing is so bad now I can hardly walk and bend over to get my head lower when I walk
this gas exchange article sounds right to me but I am so frustrated by the lack of treatment
any suggestions for treatment are what I really wish for
There are exercises that have developed to help people who have trouble breathing to breath. A study on that funded by the Solve ME Initiative is underway and we’ll be covering that in this series.
Oh, please.
I also have the breathing issue…Sometimes I’ll b3 doing something and it feels like my lungs involuntary gasp for a deep breath on thier own.
Like I’ve been swimming underwater holding my breath?
I’ve noticed my breathing has become more abormal in pass few days. I’ve had a EMG which showed Periherial nerve and muscle damage in upper body, don’t know if it would effect my lungs? And some days I feel like I can’t command my legs to move with my brain. They usually drag slowly feeling like concrete blocks….my breath in acts up…vicious circle.
Nebulize budesonide. Every 12 hours for three months. This is going to be public soon as a major breakthrough in ME and long Covid treatment.
Great to hear! Looking forward to your article. Thanks for passing that on. Check out the article on Aaron on has long COVID. He was heading to the North and the South Poles to do an article on extreme endurance trekking when he was laid low – from the Omicron variant.
https://missoulian.com/news/local/missed-risk-long-covid-threat-extends-far-beyond-pandemic/article_70311453-1f78-5068-b1ea-02886b41741a.html
And how about the LDN Barbara mentions above? She said it helped her with her breathing.
Hi, did you try Alpha Lipoic Acid?
If you can’t breathe because of a tight chest, then maybe Gabapentine works.
Tramal also helps detightening my chest a bit.
My husband has been telling me for years that I also breathe weird when I sleep. Both shallow & deep…sometimes “aggressively” I am waiting on a referral to UF sleep clinic.
As long as I’ve had this disease, along with Small Fiber Polyneuropathy, C8 Length Depended neuropathy, and my age, I have to say that Red Blood Cells, Supplemental Oxygen, Sleep Studies, etc.. and most of the data in this study and the comments are spot on and do not surprise me since my very first diagnosis, in 1980, was a problem with my KREBS cycle. Subsequent tests medically raised my Hematocrit from 40 to 52 and hemoglobin was increased to the safe maximum of 16 or 17, and oxygen provided during numerous sleep studies showed that although overweight, I did not have obstructive sleep apnea but every test showed that diagnostically my signal to the diaphragm muscles stopped on all sleep studies concluding that I had a Central Sleep Apnea. Medically raising my hemoglobin also increases the size of the Red Blood Cells. My Pulmonary Function Tests were normal when rested and abnormal after a treadmill stress test. Deconditioning was obvious in aerobic tests but I was stronger than normal in strength tests, i.e. aerobic vs anaerobic exercises, yet the same outcome was days of rest to recuperate. The medical community is so close yet so far in the fact that they can diagnostically tell you what is wrong but can’t tell you how to treat it which I expect will be slightly different for everyone. I guess we just keep fighting and do what we feel makes for a better quality of life and not forcing the issue to do something you read about without a diagnostic test to confirm it. Confidence is high that something will pop soon!!!
I’m curious. I consistently test high in rdw, the test for variability in red blood cell size. Anyone else? Thought that could be related to the possibility of red blood cells having trouble wending their way through small blood vessels. I also have small fiber neuropathy so hmmmm.
I think we’re going to hear quite a bit more about red blood cells as we go on. Someone published a large review paper on red blood cells recently as they may pertain to long COVID. Who knows – maybe ME/CFS and long COVID is so bad because of problems with the blood vessels, deformed red blood cells, and mitochondrial issues. I don’t think it’s going to be just one thing – this disease hits functioning too hard for that -but, of course, time will tell!
Cort, thank you for all the information that you provide. Speaking of red blood cells, here’s abbreviated text from a book (referenced below) by David S. Bell, M.D., in case it’s relevant to this conversation.
“Sedimentation Rate (Sed Rate)” [Erythrocyte Sedimentation Rate/ESR; to characterize inflammation]
“This primitive test consists of letting a tube of blood sit on a counter for one hour and measuring the amount of separation between the blood cells and the fluid. ……..” [some text deleted here]
“………. I feel it is the single most useful test in diagnosis and management of CFIDS [chronic fatigue / immune dysfunction syndrome].”
“The normal range of sed rate is from 10 mm per hour to about 30 mm per hour. In CFIDS the sed rate is rarely elevated above 30 (Salit 85; Buchwald 87) and in many instances is extremely low, something that few physicians have previously experienced. Because the rates are not high, doctors have been calling them normal. But the very low levels are themselves abnormal, seen in only a handful of rare illnesses. In patients with CFIDS, it is common to see a sed rate of 0, 1, or 2 mm per hour.”
David S. Bell, M.D.; “The Doctor’s Guide to Chronic Fatigue Syndrome / Understanding, Treating, and Living With CFIDS”; Da Capo Press; Copyright 1995, 1994 by David S. Bell, M.D.; page 86.
It looks like the ESR test has been replaced in the medical community by a “C-Reactive Protein” (CRP) test to characterize inflammation, the original intended testing objective, so ESR tests may not be readily available.
Best wishes to all.
Bob S.
Look at page 214 Osler’s Web
Thank you Erik!
I see also on page 226 of Osler’s Web that Dr. Bell and the late Paul Cheney M.D., Ph.D. first met and discussed each other’s work in 1987. It seems very likely that they talked about the Erythrocyte Sedimentation Rate (ESR) test as an indicator of ME/CFS.
A quick Internet search showed that ESR tests should still be available. Perhaps they are just not as widely used as they used to be (to characterize inflammation).
I just noticed that Cort Johnson and responding people already covered ESR tests as they relate to ME/CFS and fibromyalgia in a lot of detail in Health Rising – November 6, 2019 (web link below). A poll on the subject was even done.
Sorry for my repetitive posts!
https://www.healthrising.org/blog/2019/11/06/clumper-slider-esr-chronic-fatigue-fibromyalgia-poll/#:~:text=The%20ESR%20ME%2FCFS%20and%20Fibromyalgia%20Poll,-by%20Cort%20Johnson&text=It's%20the%20simplest%20of%20medical,a%20period%20of%20one%20hour.
Round and round we go ! As you say “ chicken or egg.”I put my money on hypometabolism resulting from dysfunctional / damaged mitochondria leading to low co2 production . Low cellular co2 ( I believe) would interfere with oxygen unloading at the cellular level. But looking at RBC oxygen carrying capacity seems like a good idea as well. All of this is so intertwined that finding it must be difficult to sort out. How would this tie in with the neuroglial inflammation theory that Dr.Herbert Reinz Polster proposed ? Is it chicken and egg there too ….upstream vs downstream effects ? Of course all of this is way over my head but like most desperate people I am patient researcher and trying to understand what I’m reading . Thanks for providing the research !!!!!!
There were experiments that took out mitochondria out of Cfs body cells and then underwent a high stress test. They acted normally and produced a normal amount of energy.
So yea, i kinda is a hypometabolism in vivo! but that means it isnt damaged but altered by something else in the body happening. Aka downstream effect. Like 99% else what is happening in Cfs.
No other disease has such a wide spectrum of symptoms, but ppl forget that Cfs is one of the last diseases thats completely untreated. Which means it can unfold to its fullest.
I hope so !!!!
Has anyone looked into the Root Cause Protocol by Morley Robbins? His research has indicated that the body’s improper levels of iron together with low Magnesium & copper are causing mitochondrial disfunction. rootcauseprotocol.com
Lots of words & ideas in this study, but I find it hard to take too seriously, because:
* there are numerous cases where someone went from highly fit to highly limited in a very short period, i.e. much faster than fitness can decline.
* once you have ME, exercise isn’t the sole goal in life…maximizing cognitive function within your energy envelope is a higher priority (unless you’re a pro athlete, then it’s more half and half). Stephen Hawking accomplished a lot without exercising much.
This sums up what I think is going on for me: “The slow information processing and poor sensory filtering processes appear to make cognitive tasks more effortful in people with ME/CFS/FM.”
“… the brains of people with ME/CFS have to exert more effort in order to compensate for the slowed informatiin processing and the diversion of mental resources that comes part and parcel with these diseases.”
I’ve been focusing on this recently and am aware that I can’t have too many things going on at the same time, as it uses too much brain power. My life is fairly one dimensional, most of the time and that’s very hard for others to comprehend. But I know I have to complete one task, before I start on another.
Yesterday, there was an interesting, long (!) article that I wanted to read and it took me most of the day, with breaks and a nap, to get through it. I have an ongoing list of youtube videos, articles etc., that I try and watch/read but I have to pace myself, otherwise I’ll burn up my brain energy and I can’t afford to do that.
I would like much more research on oxygen, red blood cells and respiratory problems. The problem remains: is air hunger caused by a shortage of oxygen or too much carbon dioxide? Is it compensation? Of what? lack of blood to the brain that stimulates the respiratory center? Or the shape of red blood cells? Or is the diaphragm paralyzed?
Or is it because of the mitochondria. Or the brain stem? And even more questions to answer. This all needs to be investigated. In this way we can rule out certain causes 1 by 1 and come close to the truth. All in all, this still remains the one million dollar guestion for me?
I wonder if they considered posture affecting the breathing . I try hard to stand properly but it is hard because of the pain and the fatigue as well as with POTS .
Posture is important! We’re going to have something on that.
Thanks , Cort . That would be great .
I remember the Miranda Lecture from an IAfmecfs Conf not sure which year, you reported on it Cort, I watched her presentation via the Canadian Fibro SEIDS Ladies’ Zoom Conf Nov 2020 where physio Ms Miranda put up a diagram showing a slumped seated woman and how her posture affected all her pains & fatigue, including pains around & behind the eyes.Also in your report.
Perhaps you could include a link to Miranda in your upcoming blog?
She also mentioned recumbent exercise, which can be done on a recumbent cycle, or in my case in bed to strengthen my back & core muscles, for greater strength & better posture ( & bladder control)
Will do. I thought that was a fascinating presentation!
All of this is consistent with central fatigue (which is mediated by type III/IV peripheral muscle afferents). Peripheral fatigue and central fatigue are strongly coupled in all diseases except genetic glycogen storage diseases (where the severe fatigue is due to glycogen depletion). Diseases from peripheral neuropathies to muscular dystrophies will show the same pattern if they suffer from a similar magnitude of fatigue.
The purpose of these afferents is two fold – the first is that it is the primary cause of central fatigue which decreases the excitability of the motor cortex which means force output will be lower for a given level of ventilatory drive. During a CPET, the workrate is ramped up gradually, which means higher effort will be required if there is significant central fatigue. When these afferents are blocked experimentally (in healthy people) it leads to insufficient ventilatory drive during conditions of peripheral fatigue and peripheral fatigue itself is more rapid and prolonged.
Effort is entirely centrally driven – pain can alter how people report effort during exercise – particularly the baseline levels, but that is a bias in reporting, rather than effort itself.
The second purpose of the afferents is the sensations associated with fatigue that signal to the conscious mind that performance is potentially impaired. This is critical to the survival of animals so that they can catch prey or escape predators.
The main hypotheses is
(a) impaired capillary O2 perfusion (suggestive evidence from the above study, systrom’s invasive CPET study and other 2 day CPET studies)
(b) sensitisation of these peripheral afferents – there is indirect evidence (from PMBCs rather than the nerve cells) of increased expression of receptors that would increase sensitivity post-exercise) by Alan Light and colleagues – and that team also previously showed which metabolites (by infusion in healthy people) are needed to lead to the sensations associated with fatigue.
(c) some other metabolic problem – this is even more speculative, despite being a popular hypothesis. We know it is definitely not due to an insufficient amount of mitochondria (there is always excess mitochondria in the muscle even at VO2Max, because motor unit recruitment is far from 100%) or glycogen depletion, but perhaps there could be other issues limiting the rate of oxygen uptake or oxidative phosphorylation.
We also know it is not due to “hypocapnia”. The Bohr effect is small at physiological pressures in humans – on the order of a few percent difference. and the VE/VCO2 figures for ME/CFS patients in Dane Cook’s study are well within the normal range and do not indicate significant hyperventilation or hypocapnia between the gas exchange threshold and the respiratory compensation threshold. I don’t know why the discussion in Systrom’s recent study also suggested this when in their previous study that discussed this possibility in more detail their reference for the Bohr effect actually showed that it was trivially small in humans and cannot necessarily explain what we see in ME/CFS patients.
Thought I’d share this article which mentions some new treatments and ideas about ME/CFS;
https://www.theguardian.com/science/2022/jun/26/can-our-mitochondria-help-to-beat-long-covid
Basically the article approaches fatigue from the mitochondrial theory and some companies are developing amino acid treatments to address this.
Also read an article where Dr. Klimas is positing on how the Supreme Court’s ruling MAY negatively influence her research, as some of the drugs she is experimenting with for Gulf War Illness and ME/CFS are also used for abortion. Sorry I’m not posting the link, but will look it up if folks here request it.
https://www.nbcnews.com/health/health-news/abortion-pill-may-treat-dozens-diseases-roe-reversal-might-upend-resea-rcna34812
If the clinical trial is successful, it could be the first step toward bringing these veterans some relief, Klimas hopes. But now that the Supreme Court has overturned the legal right to abortion established in Roe v. Wade, researchers studying mifepristone for uses outside abortion could face their own set of challenges.
“This is the only drug like it on the market,” Klimas said. “If you took this one away, it would be taking away a great big tool.”
Thank you for posting that link Cort! And thank you for all the other things you do!!!! You help keep hope alive!
All the studies which showed the impact of exercise on ME/CFS patients were 2 Day CPETs. Every. Single. One.
This was a 1 day CPET. It does not meet the conditions.
ME/CFS patients and healthy controls look the same on 1 Day CPET which is clearly written in those studies. So that ME/CFS patients and low fitness controls look the same on Day 1 — big whoop. Show me the impact of the 2nd day –because that’s where the divergence occurs.
The 2nd CPET Day is crucial to all ME/CFS exercise studies in order to draw any conclusions..
That’s the basics, which I do not think the CDC understood. Or they understood it, didn’t replicate it, but want certain outdated and harmful conclusions to be drawn anyway.
This large scale study failed to replicate the 2 Day CPET conditions, and I cannot accept any conclusions from this study.
Very sloppy, and poorly done, CDC! I think CDC failed at the basics, and that should be pointed out to them.
Running a large scale study with a low fitness group – fabulous idea. Failure to run a 2 Day CPET, but tries to make harmful conclusions against 2 Day CPET studies. NOPE. The agenda is subtle, but it’s there.
The CDC needs to enter 2 Day CPET into their protocols to be taken seriously. I don’t care how large the study is, without that 2nd day CPET, it’s a waste of money and time.
Failure to properly replicate a 2 Day CPET, means no conclusions can be drawn from this study of exercise in ME/CFS patients against 2 Day CPET studies. .
Attempting to draw those conclusions in this situation is bad science.
This study shows that the CDC still doesn’t get ME/CFS at all and that it still doesn’t have the basics down.
What a waste of time and money.
Your appraisal was too lenient, Cort.
I would have trashed this proposal, if I sat on the IRB.
It’s 2 Day CPET or bust, Unger.
We will not let the CDC slide in their harmful and dangerous ideas about exercise in ME/CFS patients because of this poorly done, sloppy study.
I generally stay out of the comments here because there’s just an exhausting amount of emotional content and misunderstanding of the science, but I couldn’t agree with your assessment more.
Just reading the comments it’s obvious that people that are commonly diagnosed with chronic fatigue syndrome are generally a collection of people with very different illnesses and likely quite a few undiagnosed inborn errors of metabolism. But if we’re talking about what seems to be the core of actual chronic fatigue syndrome (and I’m not actually sure that severely ill people have the same disease as the rest of us) then analyzing what’s happening in the body the day AFTER exercise is critical to understanding what’s going on. Also even though there’s probably certainly a lot of people with undiagnosed mitochondrial disease in various chronic fatigue cohorts, The fact that VO2 max is relatively undisturbed tells us that this isn’t a respiratory chain problem at least in the classic sense. (Although there are mitochondrial issues which still allow for the throughput of energy but produce massive amounts of oxidative stress in the process so that can’t be discounted.)
Before I got sick 15 years ago I was an athlete and I still have a very high VO2 Max (54) I feel completely fine while I exercise and I actually feel really good after I exercise and I even feel OK the next day, but once I hit that 24 hour mark I start having a literal heart failure symptoms and I feel like I’m gonna die for about a week afterwards.
Disorders of glucose metabolism, fatty acid oxidation, in mitochondrial disease does not produce this symptom pattern. What does are complex molecule diseases where the organelles responsible for cleaning up the toxic byproducts of metabolism aren’t working correctly.
Recent studies pointing to peroxisomal dysfunction are important in this regard because to my knowledge they are the first finding that has any precedent for the 24 hour delay to symptom onset.
It seems possible that as the sales become overloaded with unprocessed metabolic byproducts, they could be triggering the body to slow down respiration (I don’t mean breathing I mean the whole process of oxygen being turned into energy) until things get cleaned up and then the system slowly resets until the next metabolic push.
It’s a complicated illness because The layers upon layers of overlapping hemodynamic disruptions make it really hard to see past vascular effects on metabolism. That’s why the in vitro studies are useful as well.
Anyways I’ll probably talked long enough but as long as I’m here I just wanna clear up a couple misconceptions about oxygen and hyperbaric therapy:
If your blood oxygen levels are normal or even high, adding more oxygen is not going to help your body use oxygen better. In most cases the mechanism of action of hyperbaric therapy is to trigger a temporary spike in oxidative stress that causes the body to turn on its own antioxidant defenses which is why it can sometimes be helpful for people with mitochondrial disease where oxygen is clearly not the problem. But for a variety of reasons if the cells are stressed to a point where these mechanisms can’t be activated then hyperbaric therapy just becomes an additional source of oxidative stress in an illness that is already defined by excessive oxidative stress. So it’s probably not harmful to try but it’s worth keeping in mind that for people with serious illnesses hyperbaric therapy should be used less frequently and at lower pressure.
Gas exchange may be the exact issue. But according to a doctor I’m seeing who may have actually cracked the code on ME and fatigue syndrome variety of long Covid, the issue stems from inflammation in the bronchioles. He has me taking nebulized budesonide twice a day for three months. I personally know three people who it’s cured entirely. Doc told me it’s already worked on two people with ME/CFS (it’s a long Covid clinic, which is what I have, though I also clinically qualify for ME diagnosis). He hasn’t published anything yet but as a journalist I’m preparing to publicize.
Strange that people are recognizing the gas exchange issue but no one is thinking about lung inflammation. Apparently it doesn’t show up in X-rays or scans. British researchers uncovered the issue a year ago by taking MRIs of patients with xenon gas in their lungs, which revealed the issue and tipped my doctor off to this solution. Could be a game changer so many have been waiting for. Stay tuned.
Aaron, what are your ME/CFS symptoms?
Consistent PEM after physical or cognitive exertion. I’m bedridden much of the time. Unable to care for myself. Headaches. Gastro issues. Insomnia. Low blood oxygen. Erratic heart rate that spikes when standing and with low exertion levels. Brain fog.
Hi Aaron. Very much looking forward to your article. Do you have to get a prescription for that treatment? And I’d love to know what doc you are working with. I’ve had CFS for 20+ years, but Long Covid has only made things worse.
Yes, you need a prescription. The clinic is a long Covid clinic in Great Falls, Montana. Dr. Nieset. My hope is that if it works for me (still waiting on that) as it has for others, and I publicize it, that other doctors will start utilizing it and the treatment will be available in many other locations. Fingers crossed.
Thank you Aaron for sharing these interesting anecdotes. ICYMI, here’s some recent xenon lung MRI work in long Covid. This shows a significant gas exchange issue and structural defect, but doesn’t hone in on the inflammation as a factor as far as I can tell.
https://www.cbc.ca/news/canada/london/cause-of-long-covid-symptoms-revealed-by-lung-imaging-research-at-western-university-1.6504318
Thanks for this. Yes, I had seen it and have it noted in my files. It’s good to see more researchers homing in on the same issue.
Or rather, do you know what symptoms the nebulized budesonide helps with?
Apparently it clears up all of them. Some brain issues, according to this doctor, need additional treatment. He likens them to post-concussive issues. He’s not sure I need that yet, so just nebulizing for now. Today is day 24. He said someone with severe ME stood from her wheelchair after 10 days of treatment. Most people take more than a month to see improvement.
Well I certainly hope the treatment helps! At least you have found a doctor who can help you in some way. Hope you can keep us posted.
Aaron, What type of doctor is using the budesonide? Is he a pulmonologist? I am scheduled to see one on Friday for hyper-inflated lungs and breathing issues that I can’t figure out.
Hi Aaron. Is there someplace I can contact you? I’d love to learn more about this doc and treatment ASAP.
Yes, he’s a pulmonologist. He detects the issue with spirometry testing–specifically, by doing a before and after with an asthma inhaler. It showed a major difference in my testing, as it apparently does with nearly every long Covid sufferer who comes in.
Long Covid clinic in Great Falls, Montana. Dr. Nieset. Initial appointments can be done over the phone. Spirometry and other testing can be done in person in a single visit. But not everyone in the country can go there. I had to wait four months to be seen as it is. My goal, assuming it works for me, is to spread the word so the treatment becomes available everywhere.
Go to my website aaronteasdale.com for my email if you want to connect. But know that I get messages I can’t always reply to, because, well, if you have long Covid or ME you understand.
Here’s another interesting article about dogs trained to sniff out Long-Covid with an 85% accuracy; https://www.newsweek.com/detection-dogs-sniff-out-long-covid-leading-hopes-better-therapy-1719215
I wonder if they can be trained to sniff out ME/CFS? That would solve the diagnostic issue–if there were enough trained dogs to go around!
Dear editor,
As an exercise physiologist working for a long time in the field of chronic diseases, I believe it could be necessary to investigate the ventilatory and biochemical parameters, during late post-CPET recovery, nowadays.
Due to specifics of Post-Exertional Malaise (PEM) which occurs 24-72 h post-exercise and may last several days or weeks, I presume we could better understand the systemic pathophysiological processes involved in ME while focusing our observation on prolonged physiological disturbances rather on the acute phase of exercise, although rapid metabolic changes during (or shortly after) a progressive exercise test may be of great interest.
Because PEM is a major defining symptom in ME, if you want to highlight any dysfunction, you need to widen the window of your observation from the beginning of exercise testing to the end of the inappropriate long-term recovery.
GT (PhD)
Exercise Physiology in Adapted Physical Activity
Thanks, Gilles for your input. On a personal level, I couldn’t agree more as the most severe effects of too much exertion generally show up a day or more likely two later for me. It’ll be critical to learn how the damage initiated by the exertion cascades through the system to cause something like that
Is O2 being measured in the exhale?
Since less CO2 is being produced, O2 is not being taken up as it should into tissues – is it possible that it is the excess O2 slowing the exhale?
Conversely, is CO2 being measured in the inhale? Could it be trying to get more CO2 in that is slowing the inhale?
I think this may correspond to which parts of the breathing apparatus are being activated.
And yikes! There are people that just the act of sitting activates this pattern. No need for ‘exercise’. Yikes! In supine – Yikes!
At the pool [when I was able to], my breathing was confusing to me. It would take quite a while of breathing out before reaching the tipping point when the body starts to sink. But then I felt so breathless and I had to come up to the surface quickly, sometimes without even sinking first. Swimming – also confusing
Early early on in life, like 2 decades before I became severe, I lost the ability to go down to the deep end. The pressure inside my head. Intracranial hypertension? Low CO2?
I wonder if you just started pulling in random people and did this test on them, how many would show up with this pattern in seemingly ‘normal’ people?
“Whatever the situation, the authors noted that the ventilatory inefficiency found in ME/CFS has also been associated with poor exercise capacity and exercise intolerance in other diseases.”
Then the long and deep pattern might be seen in other diseases too?
I often see findings in ME/CFS turn up in studies of other disease too. Or vice-versa. Which then leaves me scratching my head – what exactly is it that makes Me/CFS, ME/CFS?
Which, from this study, it fits with the glucose issue. But why are we not burning fats efficiently either?
This long covid study is interesting, would like to see this repeated on people with ME. https://news.westernu.ca/2022/06/innovative-lung-imaging-technique-shows-cause-of-long-covid-symptoms/
“Instead of breathing more deeply and rapidly, the ME/CFS group was breathing more deeply and slowly.”
“It’s also possible that hypocapnia – low levels of CO2 caused by that breathing pattern –…”
No, breathing more slowly does NOT cause low levels of CO2! On the contrary, it causes higher levels of CO2.
It is known that hyperventilation can lead to low carbon dioxide levels in the blood (or hypocapnea), which can subsequently lead to disturbances of the acid-base balance in the blood and lower tissue oxygen levels.
Whereas low CO2 levels were found in ME/CFS the only explanation from a breathing perspective would be that given the breathing was more slowly it must be even more deeply than normal to result in relative hyperventilation needed for hypocapnea.
Has anyone measured what it is we are breathing out?
As in, what other substances asides from O2 and CO2?
Might be interesting, might have something to do with the long and deep in/exhales
Sorry I’m a bit confused, is this article implying that sufferers of CFS/ME have low levels of CO2 in the blood stream? If so is there a particular breathing exercise that we can do throughout the day to help increase the CO2 levels in our body?
A blog on that is coming up!
Many energy otc herbs/ vitamins enhance mitochondria function. There was a test to evaluate each enzyme of the Krebs cycle. Does it still exist? Would reevaluating a high concentration of any Krebs cycle enzyme before and after supplementation of all bbl vitamins and other cofactor s that are not b vitamins point to the defective Krebs step?