

“Your Blood is Black”
“Your blood is black”, said the nurse. “And thick, very thick. We see this with all our Long Covid and ME patients, their blood is very dark and thick. It is not like this with our other patients who have apheresis.”
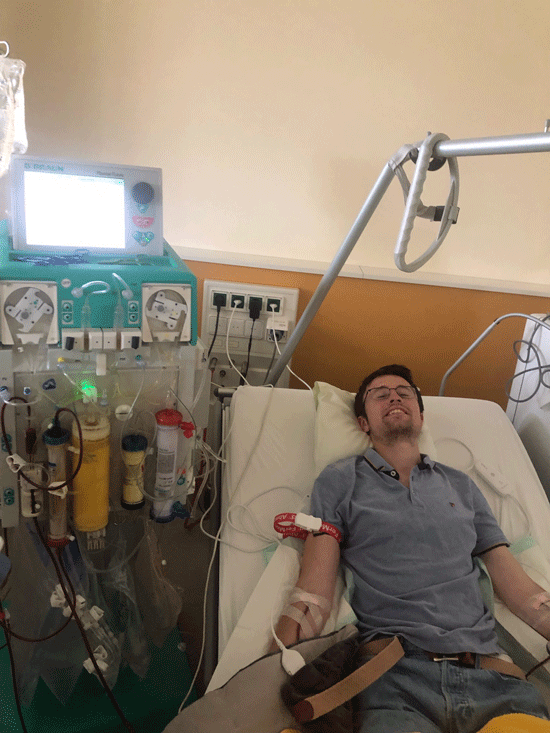
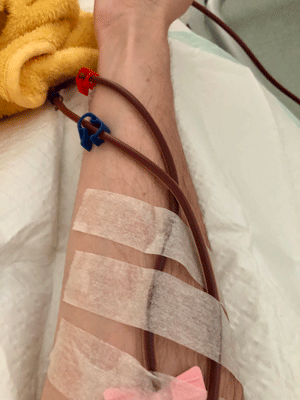
Patrick, during his first HELP apheresis session for ME/CFS.
I am now 45 minutes into my first session and my body is starting to feel waves of deeply relaxing warmth: my blood is suddenly seeping into microcirculatory spaces that have long been cut off. I also feel mild paresthesias in different parts of my body. The doctor explains to me that both of these things are signs of improving circulation.
I watch my blood as it goes out of my right arm and into the HELP filter. There, my plasma is separated out from my red blood cells (the latter are not affected by the procedure in any way). My plasma is then “washed” by coming into contact with enormous amounts of the blood-thinning agent, heparin. I say “enormous” as this truly is the case: while a typical daily oral dose of heparin might be around 20,000 units, the HELP filter makes use of a whopping 400,000 units of heparin.
Now, I’m no biochemist, but I would imagine that ingesting that much heparin at once would quickly result in an early grave. The reason that this does not happen in the case of HELP apheresis treatment is that essentially all of the heparin is reabsorbed by the filter.
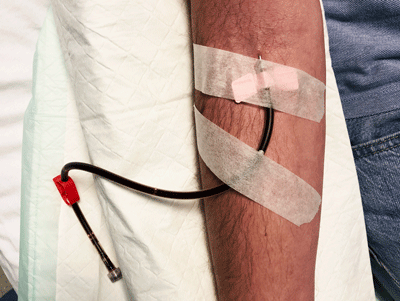
The filtered blood is then returned via my left arm. The whole procedure works in a kind of loop: out, in, out, in. 200 ml of blood is outside the body at any one time and, in total, anywhere between 2 – 4 litres of plasma volume are filtered in any given session.
In a healthy human body, there are usually around 2.8 litres of plasma but, given the hypovolemia that is so central to the illness, this amount will probably be reduced in most patients with ME/CFS. As a result, I felt that 3 litres plasma filtration was enough for me, and I stuck with this amount throughout my treatments. In total, my apheresis sessions usually lasted around 3 hours.
The Journey
I had come to the dialysis center in Bayreuth, Germany, out of a moment of desperation. I have had ME/CFS for five years. For around half of that time, I have struggled to go for a walk of even 5 minutes. During those periods, I was usually housebound, perhaps capable of one short outing. In early 2021, I was not far off from dying from ME/CFS after the most horrendous symptoms of my life (I later resolved those episodes myself through my own research and have recently published a free book that stems from that experience – you can find more details about it in my bio at the end of this article).
From there, I improved overall and, following Prof. Klimas’ recommendations for reconditioning with ME/CFS, I very slowly built up to being able to walk around 2 km (1.2 miles) on a good day, albeit slowly and with rests. It took me almost two years to get to that point. One day I did my walk when I shouldn’t have, crashed badly, and found myself stapled to the couch for the next week, struggling to sit up and lift an arm. It was then I decided I was going to take a risk and try something different.
Microclot Disease?
I had been intrigued by HELP apheresis ever since I saw it discussed in a BBC interview with Dr. Beate Jaeger, who has pioneered the use of HELP apheresis for LC/ME, and Dr. Asad Khan, an NHS lung doctor with Long Covid who has himself benefitted from apheresis. That interview introduced me to the idea that the blood in ME patients could be riddled with microclots: clots so small that they won’t give you a stroke but so numerous that they have their own significant pathological effect.
The work of Prof. Pretorius and colleagues, as she confirmed to me in correspondence, has indicated that microclots exist in ME/CFS at a significantly higher rate than in a healthy person – and this rate can be even higher in people with Long Covid. In these illnesses, these microclots – also called ‘fibrin amyloids’ – are able to attach themselves to the already-damaged endothelium lining the blood vessels, thereby interfering with the transfer of oxygen from the bloodstream into the muscles and organs.
Note that microclots do not appear to affect the amount of oxygen in the blood (i.e. oxygen saturation) but do appear to affect the body’s capacity to transfer that oxygen to everywhere else. Could all these microclots and the inflammatory molecules that accompany them make the blood so condensed that it can turn darker, perhaps almost black, in appearance, in some patients? As has often been said of ME/CFS, there is indeed something in the blood.
Microclotting can explain, at least in large part, several significant symptoms: exercise intolerance, air hunger, pressure in the chest, breathlessness upon exertion, and feeling like blood is not getting into your skin. It can also contribute to the severity of post-exertional malaise.
Microclotting, though, is about more than just specific symptoms: it appears to create a widespread problem of tissue hypoxia (low oxygen levels) able to potentially affect the functioning of the entire body at some level.
Could microclots, though, be playing a causal role in the development of ME/CFS? That appears unlikely. Instead, it appears that the microclots are probably a consequence of other core illness processes, likely driven by an upregulation of clotting pathways.
That is not to say that heavily microclotted blood does not create a physiological disaster for someone who has it, and that correcting it might not lead to a significant improvement in health, thereby improving a person’s long-term chances of total recovery.
I’d often wondered if I’d had microclots and then came across a questionnaire that purported to determine whether they applied or not. I learned that purple fingernails could be one sign and that another could be the slow return of circulation to the fingernail after pressing hard on it for several seconds. I immediately tried pressing hard on my fingernail: instead of an instantaneous rebound, my fingernails returned to normal after 3 seconds. And to say that they were purple would be an understatement.
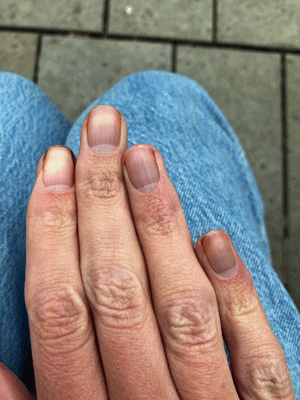
Patrick’s purplish fingernails pre-apheresis.
Results
The first apheresis session was over. I felt woozy and shaky but otherwise okay. I looked over at the filter and was amazed to see all the microclots and clotting factors (such as fibrinogen) that had been taken out of me. The residue – a kind of white, dirty sludge – sat there near the bottom of the filter. ‘How the hell was I living with all that stuff inside me?’, I thought to myself.
That question came back to me later when, in the following two treatments, the treatment produced even more residue. “This is what often happens”, Lisa, the nurse, told me. “I think it is because, in the first session, the blood is too thick for the filter to work so effectively. After it has been made a bit thinner, the filter can be even more effective.”
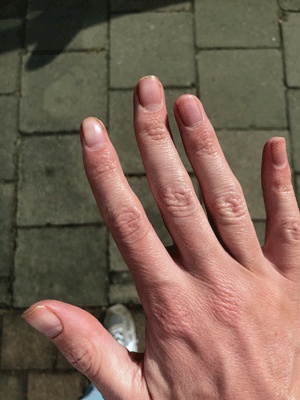
Patrick’s more normal-looking fingernails after apheresis.
I was wiped out after the first session and went into a small crash. A couple of days later, however, I noticed some changes in my body: the pressure in my chest had diminished, my arms did not instantly burn when I pushed open the heavy door of a shop and, I had no doubt, my fingernails looked noticeably lighter. These were all encouraging signs.
After my second session, my body felt much lighter. There were times that I felt like I was gliding through air on my walks (at least in comparison to my previous experience). I had some colour in my face, which had been pale for years, and my body felt sunnier. However, I still had a very bad flare-up at one point which resulted in some of my worst symptoms. Things were improving, but my illness was very much still there, ready to do its thing.
The aftermath of the third session was very challenging. I cannot emphasize enough the importance of resting, for at least two days, after an apheresis treatment. I had mistakenly thought, given my improvements, that I could still potter around the center of Bayreuth where I was staying. My body meanwhile was struggling to adapt to the massively increased oxygenation that occurred after session three. The result was that I crashed badly and was housebound for several days, struggling even to get around the apartment.
I say ‘massively increased oxygenation’ as this really was the case. I have never experienced anything like the after-effects of my third apheresis. The feeling of oxygen getting into different parts of your body is warm, wet, ‘gungy’ and intense. I felt that sensation flow over my body in powerful waves. My head throbbed with the increased blood flow to my brain. I lay still and let it pass.
The following four treatments passed more straightforwardly: each time, I felt an improvement in oxygenation. My body continued to become lighter and warmer. My fingernails also became lighter in colour. (This apparently reflected the fact that my blood was becoming less dark and was now taking on the more burgundy/maroon colour that it should be.)
In treatment six, something really encouraging happened. The nurse told me that, normally, at least with her LC/ME patients, the HELP apheresis machine requires the additional infusion of significant amounts of isotonic saline in order to help the blood flow more easily through the filter. At the beginning of my treatments, she said that my blood required the additional infusion of 1.5 litres of isotonic saline but that now the machine indicated that it required no additional infusion (beyond the standard 300ml that is used regardless). My blood was now flowing freely enough on its own.

Clots and other factors removed from the blood during the second apheresis session.
I had seven sessions of HELP apheresis in total. Coming to Germany on my own was a big risk, and on a few occasions, my health was so poor that I wished I was back home. Ultimately, however, I am very glad that I took that risk.
Now, writing almost four months after my last treatment, I would estimate that my health improved a solid 20% from the HELP sessions and that I have maintained all the gains they gave me. My circulation is still improved, my fingernails remain a normal colour and my whole body feels like it is functioning noticeably better.
To be clear, however: I still very much have ME/CFS. I can still experience PEM. It is a lighter experience in some ways but, in general, a crash still very much feels like it always did. I have still had some of my worst symptoms, which in my case usually come at night, although these have been overall less frequent and intense. I still have autonomic dysfunction.
Dark, blackish blood prior to apheresis.
Lighter colored blood after apheresis.
HELP apheresis has not been a magic bullet for me, but it is magical at what it does: returning the blood to its normal oxygenation capacity and flowing throughout the body as it should be. As a result, I feel lighter and can walk around more easily, I am cognitively sharper, sleep better overall and have colour in my face: my body, while still sick, feels like it is working better in a fundamental way.
Other Reports
While there are plenty of positive anecdotal reports online, such as in the Long Covid Apheresis Community Facebook group, there also exist reports of patients worsening significantly after HELP apheresis. Unfortunately, to my knowledge, we do not yet have research papers that examine the outcomes of HELP apheresis for those with LC and ME/CFS on a large scale.
However, one paper that looked at this question, albeit with a modest patient sample, was presented at the recent International Society for Apheresis conference in Berlin in early June. On page 62 of the conference booklet, there is the abstract for a talk, ‘First clinical results after apheresis treatment in Long Covid syndrome’, by Dr. Bücker from the nephrological practice in Osnabrück.
That study looked at the outcomes of 31 patients with Long Covid, who had at least two sessions of HELP apheresis (although the median number of treatments was 5). Patients were asked to evaluate symptoms on a five-tier Likert scale ranging from 1 (bad, very pronounced) to 5 (very good, asymptomatic) before and after the treatment and at a later follow-up point. From the abstract:
‘The overall rating increased from a score of 2 (range 1-3) before apheresis to 3 (1-5) after apheresis and to 4 (1.2-5) currently…. side effects were limited to 1 out of 144 treatment sessions, which resulted in a patient suffering from low blood pressure. 83 percent of the patients would recommend the treatment.’
These results are certainly encouraging but, given the cost of the treatment and the natural tendency of the desperately ill to seek improvements in their health, we urgently need larger-scale studies into the efficacy and safety of HELP apheresis for both LC and ME, in particular.
Lessons Learned
The main issues I experienced related to the intensity of the treatments, particularly the first three, which all created some kind of crash response, albeit with varying severities.
Drinking oral rehydration solution helped me greatly during those times. I wonder if ME/CFS patients risk experiencing a worsening of hypovolemia following apheresis treatment. This might be because, as previously inaccessible microcirculatory spaces suddenly become accessible again, there suddenly exists additional ‘space’ for the overall circulatory volume. The body, however, won’t have had a chance to catch up.
I normally drink 2.5 litres of Normalyte every day (indeed, I couldn’t do without it) but, after my early treatments, I found that drinking up to 3.5 litres was sometimes necessary to lessen the after-effects. I have struggled with hypovolemia throughout my illness and believe that I can sense when I experience it: a certain feeling that blood is not getting into the extremities of my body and brain.
I felt this symptom after the first few apheresis sessions and drinking extra oral rehydration solution provided relief. I wonder if some ME patients who struggle with apheresis do so because of issues related to blood volume, and whether they could tolerate the treatment better if they had a good supply of ORS. In line with this, I also wonder if microclotting might explain an additional (if much more minor) reason, alongside the renin-angiotensin-aldosterone axis downregulation, for the low blood volume that is so characteristic of this illness.
THE GIST
- In apheresis, the blood is removed from the body and then “washed” of unwanted substances such as microclots, antibodies, and pro-inflammatory factors and then returned to the body. HELP apheresis is widely used in Germany and has received more attention in ME/CFS and long COVID recently because of its ability to remove the microclots that some researchers believe are blocking blood flows to the tissues.
- Patrich Ussher traveled from France to Bayreuth, Germany where he underwent 7 apheresis sessions.
- He was told at the first session that his “blood was black” and thick – apparently a common finding in ME/CFS and long COVID.
- The first 3 sessions produced crashes of various degrees but it was also clear that Patrick’s blood was becoming more oxygenated: his color improved and his purple fingernails became lighter. He described what it felt like getting more oxygen into his system “The feeling of oxygen getting into different parts of your body is warm, wet, ‘gungy’ and intense. I felt that sensation flow over my body in powerful waves. My head throbbed with the increased blood flow to my brain.”
- The sixth session produced something of a breakthrough as it became clear that his blood was finally flowing freely and normally and had returned to a more normal color and thickness.
- Four months after his 7th and last session Patrick felt he’d improved a solid 20% and thus far had maintained all the gains he’d received. He still has PEM but is cognitively sharper, sleeps better overall, his body feels noticeably lighter and like it’s functioning better.
- While Patrick is not well his response suggests that something in his blood (microclots, antibodies, immune factors (???)) is indeed playing a role in his illness.
- He noted that while there are plenty of positive anecdotal reports online, such as in the Long Covid Apheresis Community Facebook group, there also exist reports of patients worsening significantly after HELP apheresis. One study suggested that HELP apheresis can be helpful as well (see the Health Rising blog cited in Patrick’s account)
- Drinking oral rehydration solution helped him greatly during his time there.
- Apheresis is usually not covered by insurance and costs about 1400 Euros per treatment.
- Patrick is a published author and composer. His website is www.patrickussher.com and hismost recent book is The Myth of Primary Polydipsia: Why Hypovolemic Dehydration Can Explain the Real Physiological Basis of So-Called ‘Psychogenic Water Drinking’.
Apheresis in Germany
According to the nurse, the average number of treatments is five. From looking through social media discussions, it seems that most patients have between 4-8 treatments of HELP apheresis, although there are rare reports of some patients having 12 or more treatments. Some patients may choose to take blood thinning medication in addition although, in my case, I felt this to be too risky in the absence of careful medical supervision.
Typically, patients seem to have a treatment once a week, although I chose to spread them out further, having 7 treatments over around 70 days. My guess is that the ideal natural end point of the treatment is the moment the blood turns a normal burgundy/maroon red again.
It is important to note that HELP apheresis does not just remove the microclots and clotting factors. It also removes pathogens, toxins, and LDL cholesterol. There will always be, therefore, some residue in the filter at the end of a session, even if the worst of the microclots are already long gone (although you can expect noticeably less residue at that point). Therefore, it seems to me that the color of the blood is a good indicator of the need for treatment.
HELP apheresis is a treatment with a long history in Germany and one with a proven safety track record in patients with serious heart issues and hypercholesterolemia. It has been used to treat hypercholesterolemia as well as various serious heart issues for decades. Its use for Long Covid patients was pioneered early in the pandemic by Dr. Beate Jaeger in Mulheim and her paper on its applications in this regard is well worth reading.
The treatment is offered in various dialysis centers around Germany, the full list of which can be found here (for those interested, it is believed that Dr. Jaeger, having closed her Mulheim clinic, is opening a new clinic for HELP apheresis in Bad Aibling before too long). The treatment is also offered in Switzerland and in Cyprus.
The costs of the treatment vary from clinic to clinic. In Germany, the prices appear to be the cheapest at around 1400 Euro per treatment. While this is still unfortunately very expensive, the bulk of this is simply to cover the cost of the single-use filter and, when the nursing costs are also taken into account, the clinic does not make much, if any, profit.
The cost, and lack of insurance coverage, of the treatment will sadly be a deterrent for many with ME/LC. We can only hope that, if this treatment is validated in the future, it could one day be offered to patients both on insurance and through national healthcare systems. It is certainly an exciting example of a conventional medical treatment that could improve substantially the quality of life of many ME and LC patients.
I am grateful to nurse Lisa for the excellent and warm-hearted care that she provided me throughout my treatments, and to Dr. Satanovskij for his kindness and also his patience in answering my never-ending questions. Anyone wishing to make an appointment in Bayreuth is welcome to contact Dr. Satanovskij directly.
HELP apheresis treatment can be a scary proposition, especially for a patient with an illness like ME/CFS. I doubt I have ever been more anxious than when I first saw my blood going through the line into the filter: I felt like I was going to lose consciousness.
My immediate reaction was to beg the nurse to stop the treatment. While Lisa put her hand on my shoulder, Dr. Satanovskij also came in to reassure me, telling me that HELP apheresis is a treatment of very low risk and much safer even than dialysis. He even told me that there are Sheikhs in the Middle East who have weekly sessions using their own private HELP machines.
As I looked at my blood seeping out of me in what I was pretty sure were to be my last moments on earth, I pondered with some perplexity the kinds of things that some people do for fun. But then I tried to settle myself down and decided to continue. I’m glad that I did.
Bio

His new book (published early 2025) is Understanding ME/CFS & Strategies for Healing, which explains for other patients the breakthrough ME/CFS research of Prof. Klaus Wirth and Prof. Carmen Scheibenbogen, as well as treatments which Patrick has found useful in improving his condition.
He is also a composer of music in a contemporary classical style and his music can be listened to on Spotify and Artlist. He has edited books on modern applications of Stoic philosophy and also written a book on the similarities between Buddhism and Stoicism and on neuroplasticity-based recovery for POTS. He has also worked on a new edition of his late mother’s book on living with breast cancer, Following the Pink Ribbon Path. His website is www.patrickussher.com.
Patrick is the author of The Myth of Primary Polydipsia: Why Hypovolemic Dehydration Can Explain the Real Physiological Basis of So-Called ‘Psychogenic Water Drinking’. In that book, he challenges the condition currently known as ‘psychogenic water drinking’ (aka: ‘Primary Polydipsia’), a condition in which it is currently assumed that people drink enormous quantities of water in the absence of physiological need and just because of mental illness.
The book presents an alternative hypothesis, namely that it is the excessive thirst experienced by some ME/CFS patients that has always, at least for the most part, been historically misdiagnosed as ‘psychogenic water drinking’. The book maps out a kind of polydipsia that may be specific to ME/CFS, POTS, and Long Covid and which stems from, among other things, the low blood volume that is so characteristic of those illnesses. That book is available for free download from its website.
Note from the author: Some readers of this blog might be aware that I previously wrote a book about POTS, an illness I had in 2014-2015 and from which I recovered using a brain-retraining program. My book tried to map out why that neuroplasticity program might work for POTS and related conditions.
Unfortunately, after three years of good health, I became ill again in 2018, this time with ME/CFS. This time around, brain retraining has helped but has never led me to get better beyond a certain point, as it did in 2015.
My situation has also been complicated with serious gait-related issues stemming from a car incident and knee injuries that have made it much harder to recover and which have involved a long, arduous, and still ongoing rehabilitation journey (indeed, this is what caused the return of my illness: the whole thing has been a real ‘Book of Job’ experience!).
I still believe that it is important to consider the neuroplasticity side of POTS and related illnesses and, alongside publishing various changes I would make to my book now, I decided to keep my POTS book live on Amazon, at the lowest possible price, as I believe that it can still be a helpful guide for those pursuing neuroplasticity options while also adding to the discussion around what might underlie, or at least drive in part, POTS and related illnesses.
Found this Blog Intriguing? Please Support Health Rising and Keep the Blogs Coming


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Many ME patients have done apheresis, and many have had no response, others have had mild improvement. It means that this is not hitting at the the core of the problem. How else can one look at this? Or the apheresis is not enough and more interventions are required at the same time, but are not offered due to gaps of knowledge. Great this chap is feeling a touch better. Thank you Cort for your tireless work. Thank you.
Your comment also reminds me there are different types of apheresis, Cort also did a blog on that https://www.healthrising.org/blog/2023/05/06/apheresis-long-covid-chronic-fatigue-syndrome/.
HELP apheresis is the only one I am familiar with
for the last 7 or so years I’ve dreamt of facilities that could offer drips to infuse vitamins, saline, medications to CFS patients while there are things like cold baths, doctors on hand and some form of blood filtration ala what dialysis does for Renal patients..
peptide injections with stuff like folistatin – muscle conditioning sessions with an ME/CFS physiotherapist
even if Apheresis became part of a big set of treatments that would be amazing
This is a – very – well written article. Your style is great for understanding content, and you’ve answered questions I had without me needing to ask them. I appreciate how thoroughly your article covers the topic. The only thing that could be improved is the use of two medical terms (hypovolemia and ORS) without explanation.
I think your explanation that microclots are probably not the root cause but a secondary pathology is in line with what ME/CFS researchers like Prusty assume.
The reaction of your body to reoxygenation that you describe is in line with a reaction I’ve recently experienced when quickly filling up a Vitamin D deficiency: it resulted in an unpleasant, high-strung feeling throughout the body which was probably a wave of activation happening in the body, but petered out after some days. I also crashed some, probably due to the extra energy made available in some body pathways from that activation resulting in doing more than tolerable with ME/CFS.
I will surely be keeping out an eye for the colour of my blood next time it is drawn :-). Though based in Germany, I will not try this treatment any time soon due to cost and not being able to travel. I will try low cost treatment options like TheNicotineTest, Low Dose Naltrexone or Nattokinase before that. But it is good to know that the option still exists.
I can’t remember where I read this (Twitter?) but do I remember correctly there were some people for whom apheresis effects did not hold? I think that a question might be if in some people, there might be ongoing production of microclots resulting from an ongoing disease process (meaning effects might wane over time), while in others microclots are the remaining result of a past disease process (like Covid infection) (which should predict effects to hold).
Thank you for the kind words about my article, much appreciated.
Yes I have also seen anecdotal cases where the clots came back. And this makes sense as, as you say also, they seem to be a secondary factor and the illness can still create them. I remember Dr. Khan saying PEM, autonomic dysregulation and infections are prime factors that might drive the clotting pathways.
On the other hand, if the clotting situation can be reset powerfully enough, one can only hope that, in general, they’ll have a hard time taking hold again.
The problem with treatments like this is if you have a sequestered virus in your body driving your illness, it will come back.
This was just on the NBC news regarding a new blood test for Long Covid.
“A blood test for long Covid is possible, a study suggests”
https://www.nbcnews.com/health/health-news/long-covid-differences-blood-test-study-finds-rcna116871
This news piece discusses “dormant herpes viruses” awakening in Long Covid like they seem to do in ME/CFS.
So glad the HELP Apheresis has resulted in some improvement for you Patrick. I followed Dr Asad Khan’s experience at Mulheim, a while back. I know that the treatment doesn’t work for everyone but it makes sense that it could work for a particular cohort of patients.
Thank you for sharing your journey!
Does anyone know how you can find out if your blood is too thick using more conventional/available methods? I was diagnosed with high blood pressure, and having followed ME research I wondered if it is due to my blood being too thick, and high pressure is just the symptom of that.
My Dr had no interest in finding out the why behind my increased blood pressure, since conventional lab tests were normal. She dismissed my attempt to bring up circulatory issues, POTS, etc.. related to post viral syndromes…
Thank for anyone’s help on how to get more info on your own blood composition/thickness, and microclots as described in this posting.
Yes, I think there is a way using the standard blood test for ‘ESR rate’ (erythrocyte sedimentation rate). This measures how quickly your blood settles in a test tube. The slower it settles, the more thick it is (the thickness creates a resistance to settling). If you have a very low ESR rate, then this might be indicative of microclotting. My ESR rate, when tested a couple of years ago, was the lowest possible at 1.
I wrote to a prominent researcher involved in microclotting and he confirmed to me that a low ESR rate can be a sign of having this issue.
Hope that helps. I forgot to mention this in the article itself.
Yes, that’s correct. I forgot to mention the ESR…mine was low also – at 3.
Thanks Patrick for your well written article. I will download your book to read on ‘Psychogenic Water Drinking’ 🙂
sorry, speak dutch/german. is ERS rate sedimentation rate please? thanks!!! glad you get helped!!!
Yes, indeed ESR rate = sedimentation rate 🙂
thanks, mine is ok 🙂 but my boddy not…
Thank you! I just ordered the ESR test and will take it today. Thanks for your great article.
I know that there are different types of POTS. I have the ‘hyperadrenergic’ Pots which causes high blood pressure (I didn’t have high blood pressure before getting ME). Also, I have thick blood, I always have problems having blood drawn from me, and also tested positive for APS (Anti phospholipid syndrome) which can be caused by an underlying condition such as an autoimmune disorder….ME/CFS!
Then, on top of that, there is our low circulating blood volume. No wonder most doctors run a mile when they see us poor sick patients 🙁 I would recommend you look for another GP, one who specializes or shows an interest in this most debilitating illness we suffer from.
*As a side point at the end of this article, I too have experienced extreme thirst, even with drinking large amounts of water! This was one of the first symptoms I had with ME, though no doctors have been able to tell me why. (I didn’t have diabetes then, though I do now (type 2) thirty years later).
I believe H.E.L.P to be at the very least questionable. It is often mentioned as a possible cure but there is no science to back up its effectiveness and you don’t find a lot of patients either that report a breakthrough. Getting better 20% for a few months but paying 15000€ for it is a bad deal in my opinion.
I think “questionable” is maybe not the best word to describe this treatment: It is, first of all, a new treatment application. There are seldom effectiveness studies to back up new treatment applications that were invented only 2-3 yrs ago. You could say that one always has to be the first when it comes to new treatments. (I even think that 10 yrs ago there was a Doc in Germany who lost his license for treating ME/CFS with intravenous immunoglobulins (IVIG), which Scheibenbogen is seriously researching today).
But there is at least plausible scientific reasoning why HELP apheresis can help some patients by removing microclots, there are some scientists currently working on it such as Resa Pretorius; and I also remember for example some study on clotting-inducing properties of a Covid viral protein.
I think what would make it such a gamble for patients right now is that as Patrick says in the article, it does not help everyone, but the science is not yet understood enough to predict which patients will or will not be responders. Also I suppose there could be cases with ongoing microclot generation where effects might not be permanent.
I, too could not currently spend so much money on a chance.
However, 20% improvement can be a lot when it for example makes the difference between housebound and not housebound.
So what would really need to happen is for these filters to become cheaper.
What I would call questionable were if treatment providers did not inform about chances of failure, but I do not know the way they communicate.
this is overwhelming.i been struggling with CFS for over 10 years, was not in the tongues of Doctors. do take supplements, some times work and then not. but my question is: anybody tried Hydrogen Water? i ve been reading about it and makes much sense. i m looking for a affordable way to drink this. I know they have tables, not fond of that method. there are single devises, but which one. some do also convert water into alkaline. not interested that. just Hydrogen ???
I researched hydrogen generating bottles and purchased the LevelUp Way Premium Hydrogen bottle over a year ago. I’ve been pleased with it and use it daily.
thanks for your input. i looked it up , site bit confusing , talking about alkaline water? which one did you get. looks most of them kind of expensive ? thanks again. PS: what have you felt different now you are taking this. ? do you drink it right away after the process has been completed ? Do you use tap water ?
Hi Deborah,
I have used Hydrogen water. It did not have any effect for me, but we are all different and I was hoping it would help lower my A1C and any other benefit would be great. Amazon has a variety of affordable ones. In fact I just sold mine on ebay for $20 and I paid about $150
I tried tablets for Hydrogen water for one month, and didn’t notice a benefit. Good luck
thanks, then what did you try?
I tried Mercola Brand Hydrogen Tablets, if that’s what you are asking? Honestly, the one thing that has had a meaningful reduction in symptoms like pain, brain fog, fatigue, was finally sucking it up and doing the elimination diet – and then eliminating all legumes, all nightshade vegetables, and all seeds, and most all grains. Then I adopted the Wahls Protocol (for MS) but modified with the stuff I am allergic to eating.
I also think its important to eliminate things that shred mitochondria in the diet, like Glyphosate. For example, oats and beans are processed AFTER harvest with Roundup so should never be eaten unless organic.
It is nice to hear an update from Patrick. I followed his YouTube channel and read his book years ago .. I am saddened to hear his remission was not permanent. I am happy he has learned more about the illness however and wish him well. I look forward to hearing some of his music and will be popping in on his web page.
Thank you Lisa for your kind wishes for my health.
I am intersted in apharesis but from Carmen Scheibenbogen (for adults) charité university Berlin and Utha Behrends for children. They study ME/cfs etc and have “biomarkers” where they work with and are reseaching why there apharesis helps some and other not.
i can not remember where i read it, probebly on a german site. but it is not that harmlous as it seems. also the cost of it has made people poor.
when it is not payed back with insurance, there is something wrong. In germany there are many not payed back alternative things.
i am glad you feel better!
but charité university in berlin and the research around it (is is a big immunological top university) feels a lot safer for me.
sadly they only take now people from berlin and 1 place around. but in germany they want more centers for ME/cfs.
Dear Konijn, I think Scheibenbogen uses a very different type of apheresis (immune apheresis/immunoadsorption). It is an apheresis to remove autoantibodies from the blood, therefore I think does something very different than HELP apheresis which removes microclots.
I don’t think in a German context you cold say that when it is not payed back with insurance, there is automatically something wrong: Most Germans have public health insurance and in that system, there are very clear scientific evidence-based catalogues of what can be billed by doctors with public insurance. As there typically are no such scientific studies yet for a new treatment, it is consequently not paid for.
Yes, I think Scheibenbogen’s fatigue ambulance is limited to patients from Berlin and Brandenburg, and if I’m not mistaken they mainly do ME/CFS diagnosis but treatment only within the context of their scientific studies.
yes, Scheibenbogen uses a very different type of apheresis (immune apheresis/immunoadsorption). It is an apheresis to remove autoantibodies from the blood. I like with her that it is in a verry good hospital verry good researched for who it might help and for who not. There i would feel much safer if i would have immunemarkers for ME/cfs. And yes it is stil in researchcontext i though, who it may help and who not. The not payed back, i did not mean it is all bad, but if aproved, the pro’s and cons mentioned (known), etc i would feel much safer. I thought that (general) apheresis is allready long term used in germany in different places. At least i read that. I am glad he is 20% better, do not get me wrong!!! but i wait for more research and safety. Like research from scheibenbogen.
Agree 🙂 Yes, I’ve also heard apheresis is a long-term used method in Germany. Maybe in a couple of years we know more about who can be helped by what apheresis. Best wishes!
Dear Patrick Ussher,
I appreciate your honesty about the limited effect of brain retraining on your ME CFS. I think it is very important you acknowledge this.
Because, as you probably know, the ME CFS Patient community has been bombarded by a plethora of Body Mind therapies by their doctors and therapists. Originating from the very persistent paradigm, that ME CFS is an illness caused by the Brain’s response to various Biological, Psychological and Social triggers, rather than caused by specific (still unclear) biomedical disease processes.
This medical school of thought has caused a lot of harm and negligence to the patients, as you surely know by now.
As an example:
This research article below just came out yesterday and the ‘Scientific’ claims are actually more opinions than Science. But what is worse, it probably obstructs acceleration of Research by the medical scientific community to find real cures for our terrible illness.
https://www.tandfonline.com/doi/full/10.1080/02813432.2023.2235609
Or for a more ‘easy to digest’ article (based on the previous article):
https://kommunikasjon.ntb.no/pressemelding/18001364/oslo-chronic-fatigue-consortium-offers-a-fresh-perspective-on-chronic-fatigue-syndromes-and-post-covid-conditions?publisherId=7860342
That aside, I’m happy to hear you got improvements and hope this will continue to be so. In order to write another book with your new insights 😉
Let’s hope The Medical / Scientific/ Political community is going to shift Paradigms rapidly in order for these type of treatments to be be available in the future for all of us patients.
All the best.
Thank you, Arvi.
I agree with you. The idea that ME/CFS is ‘just’ some sort of ‘hypersensitive nervous system’ issue is very frustrating and it does a real disservice to the very sick. There are so many biomedical abnormalities going on in ME/CFS (and related illnesses).
On the other hand, there are some research-identified neurological abnormalities in ME/CFS that may respond to neuroplasticity. I hope one day that top ME/CFS researchers might devise more precise neuroplastic interventions that target these abnormalities (in rather the same way that researchers have helped devise neuroplastic interventions for brain injuries in other conditions, such as stroke). This kind of effort would be about addressing brain dysfunction and would be separate from the bio/social paradigm.
Thanks for your kind wishes for my health.
I did 2 sessions of the HELP apherisis at the St. Georg Clinic in Bad Aibling this past May & June along with extreme whole body hyperthermia & a photodynamic blood therapy. I wish that I could recommend the apherisis here, but the staff in the apherisis department was less than ideal. Very poor communication & a faulty machine during my 2nd session. I can’t say that it helped my Lyme & ME/CFS symptoms at all. Dr. Jaeger is at this clinic.
Since then, I have been made aware of a clinic in Frankfurt that does apherisis “on steroids”…includes blood hyperthermia & super oxygenation. The name of the clinic is German Health Clinic & I copied the EHP description from their website below. Hope it helps.
Therapy EHP®
The Extracorporeal Hyperthermia Perfusion – EHP® is the worldwide first method that combines process elements of hemoperfusion, hyperthermia, oxygenation and apheresis to create an independent therapy. It can be used for cancer, borreliosis, CO infections, numerous chronic diseases, autoimmune diseases or heavy metal pollution. With EHP® it is possible to treat these and more diseases effectively and at the same time optimally with few side effects.
Best wishes to you, Alan! Again, everyone please be aware there are different types of apheresis doing quite different things.
P.S. Being based in Germany, I had a Google look into this provider: Better be careful with this “German Health Clinic” – though I don’t know it, the blatant name seems to target audiences from abroad with the term “apheresis” added on in the titles in addition to hemoperfusion – possibly to catch interest – though from the description, hemoperfusion is the only type of blood wash involved.
I also would always be careful with such big fancy and partly vague words as they use to describe their “EHP therapy” like “worldwide first” or “independent therapy”, “eliminates inflammatory and other harmful molecules”, “The effectiveness increases thereby maximally” etc. and my first instinct would be to presume some fancy obfuscation and product uptalk from this.
From the description of that EHP therapy https://www.erweiterte-medizin.de/en/ehp/ (that’s an alternative brand for the same doctor and adress) it seems what they do is: do hemoperfusion https://en.wikipedia.org/wiki/Hemoperfusion (a type of e.g. charcoal filtering of the blood) which according to their description catches toxins and cytokines etc., plus warm up the blood and oxygenate it (…could be the same as oxyvenation?), plus e.g. chelate heavy metals in the blood before hemoperfusion. So this EHP seems to me rather like a combination of preexisting methods.
They state that “Our form of hemoperfusion is suitable for eliminating sepsis cases (blood poisoning), severe inflammation, cytokines and various toxins. We also use it for the treatment of Lyme disease, autoimmune diseases, cancer, at risk of multiple organ failure, liver disease, kidney disease, systemic inflammatory response syndrome (SIRS – English: systemic inflammatory response syndrome) and lung diseases such as ARDS (ARDS – English: acute respiratory distress syndrome) and much more of the blood. The effectiveness increases thereby maximally.” – as there is no further information in the method description for the mechanism of action for these diseases, I think it would be on the patient to research what hemoperfusion does and what would be the mechanisms of action how it could help their disease.
According to the websites, as a separate treatment they also offer immunoadsorption apheresis.
You can find German language Google reviews for the Doctor who is managing director of German Health Clinic if you google “Dr. med. Gerhard Siebenhüner”: They have a structure of five star versus some 1 or 2 star reviews. While the glowing 5 star reviews may be authentic, it might be a possible red flag that e.g. on shopping websites this type of review structure is often seen where fake or solicited reviews are involved. You can copy the reviews from Google and enter into a translator. There is one case of a Long Covid patient who says she was “promised” to be cured but what she got was a series of expensive infusions, one of which caused an anaphylactic shock to which she (herself an emergency medicine professional) says there was a complete professional failure of reaction by both doctor and nurse. There was another patient who said they paid 10 000 EUR for 4 hrs of hemoperfusion, hyperthermia and oxygenation, felt improvement of general pain and fatigue, but the promise it would improve their neck pain had not come true, then continued to receive bills for blood works they had not agreed to, and thinks the costs are exorbitant and cost transparency lacking. There are 4 other concerning reviews regarding this practice including a severe complication during a hyperthermia treatment, or a patient stating “what we experienced here was unimaginable suffering and a lack of any support”. One of the five star reviews is: “I was diagnosed with breast cancer that had spread to my lymph nodes and bones. After the treatment here (no side effects, no hair loss, etc.) I am absolutely healthy”. Umm…
So while there would generally be patients reporting success from alternative treatments which may be the same for this clinic, I think there are a number of potential red flags.
And everyone please be aware there are different types of apheresis (blood wash) applications.
Thank you JR. Never too much information. I appreciate your reply!
Hey Patrick. We brought our son to Bayreuth in March 2023. He is 23 years old. Covid led to LC led to cfs. We adore nurse Lisa. She was wonderful with Michael for each treatment! And Dr Satinovskij is Indeed patient and smart. We interviewed 3 clinicians before going via zoom calls and he was Michaels fav doc.
Michael had 4 treatments in Bayreuth; his color improved and he felt an overall improvement if 5-10%. Very in-line with your results.
He still has cfs. It’s no magic bullet, as you mention, but he did say it felt like something lifted in his body and he felt better overall.
Great article. Continued thoughts for health for both you and our son.
Small world, Kathy!
I’m glad to hear your son had some improvement under the care of Dr. S and Lisa. One feels in good hands with them.
Thanks also for your kind wishes for my health – likewise I hope your son can move in the right direction.
Thank you!! Michael is getting through Law School which has been hard. Year 1 – and he got COVID Infection 3 recently sadly. I text Lisa yesterday that we want to bring him back! She is a really good person and that team made us feel like we were in excellent hands!
Please keep us posted on how you are doing. I will do the same about Michael with your permission!
Yes, please do let me know how Michael gets on. I hope things improve for him.
What is the protocol you are referencing?
Klimas’ recommendations for reconditioning with ME/CFS, I very slowly built up to being able to walk around 2 km (1.2 miles) on a good day, albeit slowly and with rests. It took me almost two years to get to that point.
I too am interested in the idea of virus reactivating or the cause of CFS/ME as I was diagnosed with Epstein Barr after a bout of mononucleosis in 2001. I haven’t been the same since.
Hi Beth, it is referred to near the beginning of this article: http://cfsrecoveryproject.com/how-to-benefit-from-exercise-even-if-you-have-chronic-fatigue-syndrome/
I wonder if it’s the case that the apheresis merely provided general health benefits from cleaning out the “sludge,” as it presumably would for anyone, and you were naturally benefitted by that, not by any improvement or change in the underlying causes of ME/CFS. Regardless, I’m glad you got some benefit from it, congratulations, and thanks for writing it up.
Thank you Rick for your kind words.
I’m not sure it is just a general benefit (although that might be part of it). The darker blood phenomenon seems to be specific to ME/CFS patients and this does seem to change post apheresis. The clots make the blood darker and, once the heparin removes them, the blood becomes lighter again.
Hi Cort,
My impression is that apheresis in the USA does not generally send HEPARIN back into the blood, but rather uses ALBUMIN. To replace the old and damaged proteins removed with the plasma.
Is this true, according to your knowledge?
And if so, what are the differences between the 2 styles of treatment, and which one is more effective?
What is this treatment (HELP) supposed to do? I don’t think there is any evidence of microclots in ME or LC. Seems like yet another quack remedy to me.
Hi Martin, Study by Prof. Pretorius which shows microclots in ME/CFS is linked in the article. She has also shown same in Long Covid as has Beate Jaeger (whose paper is also linked in the article). HELP removes the clots by the use of heparin as described in the blog.
Cort,
Please institute a banner at start of articles speaking of recovery.
With the banner stating, (reinforcing)that there is currently no cure.
When the machine indicated that 1.5L of saline was required, did that indicate low blood volume?
Hi Sarah. No, the machine didn’t measure blood volume. The extra isotonic saline was to help my blood flow more easily through the machine. Essentially, the requirement was there to mitigate the thickness of my blood. By the end, this was not required as my blood was no longer thick.
There’s always injecting ourselves with Heparin every day and see what happens. Seems a lot less cumbersome and risky. I’ve heard of many people feeling better and more energetic from Heparin. If I could get past my fear of needles, I’d be on it right now giving it a go. They used Heparin in the hospital to clear my port several times because of my thick, dark, nasty, clotty blood (as described here) and it made me feel noticeably better.
Patrick many thanks for sharing your journey. I found a lot of similarities with what my son is currently experiencing. Your sharing has helped shaped our plans. Any recovery is good recovery and sharing those findings helps others make their own decisions. Good luck on the continuing journey and please keep publishing.
I am hoping that this post might help Patrick. I had ME/CFS for 6 years.
I went from being very active & athletic,also working as an RN to hardly being able to get out of bed, overnight.
I visited 7 different doctors, who all told me I had to learn to live with this dreadful affliction & that I had to learn to manage it!
That was not an option for me.
I tried soooo many different remedies, until finally I stumbled on an article on Lugol’s Solution. I asked a compounding pharmicist to make it up for me.
I took one drop one day, one drop the next day , the third day I woke up feeling normal!!! I obviously was not very fit and had to ease back into my exercise regime etc, but that didn’t take too long.
I never go a day without having 1-2 drops of my magic Lugol’s Solution.. hoping this article helps others.