

Nicotine…Who Knew?
Nicotine – what a strange thing! Nicotine patches are perhaps the most surprising entrant yet in the treatment sweepstakes for long COVID, chronic fatigue syndrome (ME/CFS), fibromyalgia, and related diseases.
Nicotine, of course, is the substance in the tobacco in cigarettes which makes them so addicting – and nicotine withdrawal, we know, is no joke. Cigarettes could be viewed as profoundly efficient ways of delivering nicotine to the brain. It’s the quick hit that tobacco smoke provides, though, that makes nicotine so addicting.
Slow-release low-dose nicotine patches, gummies, lozenges, inhalers, etc., on the other hand, are used to wean cigarette smokers off their addiction. It’s the slow release that does it; when nicotine is released slowly, its addictive power apparently either completely disappears or almost disappears – allowing its beneficial properties to emerge. It certainly has some.
Indeed, a close look at what nicotine patches do brings up the question of why they didn’t show up on the radar of ME/CFS/FM patients long before the coronavirus pandemic hit…
Nicotine
“It’s fascinating to me frankly that one molecule found in nature can be so potent. It’s hard to imagine you could engineer a drug to do this.” Peter Attia MD
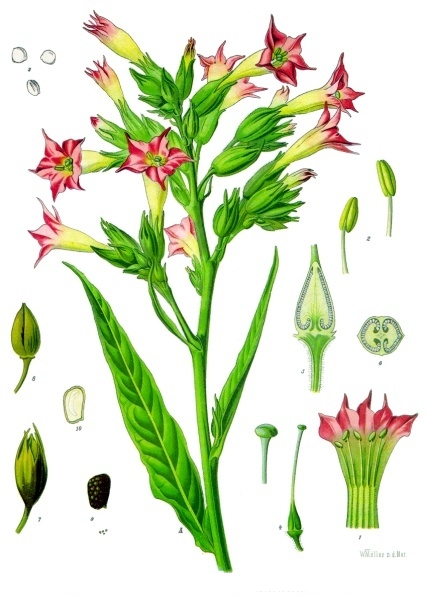
Nicotine – a protective alkaloid – is found in other plants in the Nightshade family – but saturates the tobacco plant. (Image from Wikimedia Commons)
It’s no surprise that we know a lot about nicotine. The tobacco plant – our main source of nicotine – comes from the Solanaceae family – which includes, alongside tomatoes, potatoes, eggplant, and peppers, psychoactive plants such as henbane (Hyoscyamus albus), belladonna or deadly nightshade (Atropa belladonna), jimson weed (Datura stramonium), and mandrake (Mandragora autumnalis). (Because tobacco can cause mild euphoria in some, it is also classified as a “psychoactive” plant.)
(It should be noted that nicotine does not cause the cancers caused by smoking or chewing tobacco – other parts of the plant do that.)
Feel-Good Enhancer
The fact that nicotine might make people feel better is no surprise given how many people smoked cigarettes/pipes before their dangers became apparent. By enhancing the activity of the nicotinic acetylcholine receptors (nAChRs) in the brain, nicotine increases several feel-good chemicals (mostly dopamine but also serotonin, GABA, endogenous opioids, and endorphins) that may be lacking in the brains of people with ME/CFS, FM and long COVID. Nicotine also triggers the release of acetylcholine and activates the sympathetic nervous system causing the release of epinephrine (and norepinephrine) – a stimulating neurotransmitter.
Immune Enhancer?
Immune enhancement is a total surprise, though. Nicotine also plays a key role in the cholinergic system – a system that presents fascinating possibilities for diseases like ME/CFS and fibromyalgia (FM) which feature an underactive parasympathetic nervous, or “rest and digest”, system.
The cholinergic system involves neurotransmitters (acetylcholine), receptors (AcHRs), and enzymes that activate the “cholinergic anti-inflammatory pathway“. With its direct link between the central nervous and immune systems, a dysregulated cholinergic system is believed to lead to inflammatory and autoimmune diseases. It turns out that nicotine enhances the productivity of this beaten-down system in ME/CFS/FM.
Brain-Fog Helper?
Nicotine may also help with some aspects of brain fog. A recent paper, “Nicotine’s effect on cognition, a friend or foe?”, reported that nicotine can enhance attention, and short-term and long-term memory – and nicotine has been used as a performance-enhancing drug. While warning of the dangers of smoking and high-dose nicotine use, the authors conclude that “nicotine-derived compounds could be a promising strategy to alleviate neurological disease-associated cognitive deficit“.
Indeed, an older meta-analysis of 41 double-blind, placebo-controlled studies found that nicotine or smoking “had significant positive effects on aspects of fine motor abilities, alerting and orienting attention, and episodic and working memory”. A more recent meta-analysis of 33 studies featuring nicotine patches found that they “had statistically significant positive effects on attention” but non-significant effects on memory, in healthy non-smoking adults.
Studies suggest that the nicotinic receptors involved in the cholinergic immune response play a key role in neuroinflammatory diseases such as multiple sclerosis, Alzheimer’s, and Parkinson’s disease and nicotine has produced a variety of positive effects in a multiple sclerosis mouse model.
If you follow Peter Attia, MD. in his longevity podcast, he uses nicotine at times to enhance his mental clarity.
Exercise Enhancer?
Nicotine has even received some study as an exercise enhancer. While noting that more study was needed, a 2017 meta-analysis reported that about 2/3rds of studies found that nicotine significantly increased heart rate compared to placebo or control. Given the chronotropic incompetence that appears to be happening in ME/CFS, the ability to raise the heart rate during exercise might be a help. Increased blood pressure and blood flows were also reported to be significantly increased in multiple studies. Another 2017 study found that nicotine improved anaerobic performance but a recent study did not.
Nicotine Clinical Trials
Most nicotine clinical trials are focused on smoking, but nicotine is also currently being assessed in depression, chronic pain, multiple sclerosis, improving hearing in the elderly, and improving cognition.
The COVID-19 Nicotine Saga Begins
Smoking, Nicotine and COVID-19
Nicotine increases the levels of several feel-good chemicals in the brain – particularly dopamine.
The COVID-19 nicotine saga began on a false note. Studies suggesting that smokers were at less risk from COVID-19 prompted an early 2020 paper proposing the use of nicotine as a treatment. While the limitations were noted in the first paper, the idea that smoking and/or nicotine might be protective against COVID-19 caught on in some circles. (Several years and studies later, the idea that smoking is protective has been decidedly squashed.)
Also in 2020, in “Autonomic balance determines the severity of COVID-19 courses“, Dr. Marco Leitzke and his German colleagues asserted that the more depressed the “vagal tone” was; i.e. the more depressed the parasympathetic nervous system (PNS) or rest and digest system was, the worse off people with COVID-19 were. They proposed using nicotine (as well as biofeedback and vagus nerve stimulation) to enhance the activity of that system and help patients return to health.
They based this on the hypothesis that the SARS-CoV-2 virus is binding to the nicotinic receptors called nAChRs. This hypothesis is based on close resemblance between the amino acids found in the coronavirus spike protein and a snake venom toxin that binds to nAChRs.
The idea is that by binding to the nAChRs, nicotine should be able to knock the coronavirus off of them. This is because nicotine has 30x greater affinity for these receptors than the spike protein does. Knocking the coronavirus off these receptors should allow them to operate normally, returning the immune and central nervous system to a healthy state. Whether the coronavirus spike protein is binding to the nAChRs and disrupting them is still speculative but is a possibility.
The 2023 Leitzke Paper
Leitzke’s 2023 paper, “Is the post-COVID-19 syndrome a severe impairment of acetylcholine-orchestrated neuromodulation that responds to nicotine administration”, really kicked off the nicotine interest in long COVID and ME/CFS. Leitzke cited several early studies suggesting that smoking reduced the incidence the COVID-19. He failed, though, to acknowledge later studies that had contrary findings.
Indeed, far from being helpful, a recent meta-analysis concluded that “the risk of COVID-19 progressing to more severe conditions and leading to mortality is 30–50% higher for both current and former smokers compared to individuals who have never smoked”.
(In his talk with Sophie Helbig, Leitzke acknowledged the damage smoking causes to the respiratory system and the added danger that smokers who get respiratory viruses like the coronavirus are in. He does not recommend smoking…nicotine patches and gummies, though, are a whole other ball game.)
Leitzke’s Four Case Reports
In his paper, Leitzke described four case reports of nicotine patch use. Each person was instructed to use the lowest available dosage (7.5 mg/24 h) and to administer the patch once daily in the morning.
One person with high weakness reported being weakness-free by day nine. Another reported her ability to concentrate was restored by day 4 and her fatigue and post-exertional malaise were gone by about the third week. Six months later she remained healthy.
One person who mistakenly doubled his dose – which led to horrendous vomiting and diarrhea – nevertheless saw his fatigue disappear by day 4. He too reported being well six months later. Fatigue disappeared for the last person on day six, her sleep returned to normal and her mood swings disappeared by day 5. Three months later she remained in good health.
Leitzke’s YouTube Talk
A couple of months ago, Leitzke talked with Sophie Helbig, a former fibromyalgia patient, on her “The Puzzle of Healing” channel.
THE GIST
- Nicotine – the addictive substance in tobacco smoke – may seem like a bizarre treatment option, but it appears that the addictive properties of nicotine only manifest themselves when tobacco smoke provides a quick hit to the brain.
- In fact, given its many potentially beneficial qualities, it’s a bit surprising that nicotine patches have not been tried before in diseases like ME/CFS and fibromyalgia.
- Nicotine has been shown to increase the levels of feel-good brain chemicals like dopamine, to increase mental clarity and cognition, and rebalance the immune system.
- Interestingly, nicotine enhances the activity of the parasympathetic, or “rest and digest”, branch of the autonomic nervous system/vagus nerve which appears to have taken a hit in ME/CFS, FM and long COVID.
- The long-COVID nicotine saga began when studies (falsely, it turned out) appeared to show that smoking reduced long COVID severity. That finding was bolstered by the recognition that a part of the coronavirus looked like they would bind well with nicotinic receptors that regulate the vagus nerve functioning. Doing so might throw off the immune system, brain chemicals, etc.
- Taking nicotine in the form of patches was suggested in order to knock the coronavirus off those binding sites, thus returning the subject to health.
- Indeed, the publication of four case reports by Dr. Marco Leitze reporting on the rather rapid return to health of four long-COVID patients spurred interest in the nicotine patch.
- Since then, Dr. Leitze appeared on a YouTube video talking about the use of the nicotine patch and noting that he’s seen effects ranging from no effect to complete recovery. (See blog)
- Long-COVID patient groups have created an excellent information resource on dosage, how-to’s, FAQs etc. (See blog)
- Polls from those groups suggest that the nicotine patch is not a panacea but that in some patients it can work really well, while in most people it has more moderate results when it works. That’s a not uncommon finding in our heterogeneous population for treatments that can help.
- The nicotine patch must be used correctly and can cause severe, if temporary, side effects (vomiting) if used at too high of a dose. When used correctly, while it can cause side effects at first, it appears to be pretty safe.
- Given its good (thus far) safety record and its low cost, it seems like a pretty good option for those who want to give it a go. (See the blog for more details)
Leitzke said that long-COVID patients who are not smokers can experience quite a few side effects at first. This is because Leitzke believes that when nicotine stops the coronavirus from binding to the nAChR receptors, it liberates the virus, resulting in side effects for 3-5 days until the immune system can catch up to it. All the patients he’s seen, though, pass through this stage fine.
After the 3-day low dose period, use the 7 mg patch for 7 days, stopping it after the 10th day. This is because the nicotine receptors will become temporarily desensitized and the effects will stop. (They get re-sensitized quickly.)
Leitzke recommended not pushing too hard if you see improvement. Instead, go slowly and give your body time to heal. All sorts of compensating changes can occur in people who have been ill for a long time and they will take time to reverse.
Leitzke said he’s got a lot of feedback from patients on social media who are trying the patch. People have reported everything from nothing happening to complete recoveries.
Leitzke believes that blockage of these receptors could occur in FM and ME/CFS as well. He said he talked to “very prominent colleagues who’ve been dealing with ME/CFS for a long time”…who reported they saw “massive improvements even in ME/CFS”.
While Leitzke believes in giving nicotine patches a try, he’s being cautious about their efficacy and acknowledged that “time will tell” with them.
The ACE2 Connection
ACE2 is interesting because the coronavirus enters the cells via the ACE2 receptor and the ACE2 dysregulation may be occurring in ME/CFS and POTS as well.
A 2021 laboratory study, “Nicotine upregulates ACE2 expression and increases competence for SARS-CoV-2 in human pneumocytes“, found that nicotine increases the expression of the ACE2 (angiotensin-converting enzyme 2) receptor that the SARS-CoV-2 virus uses to enter cells. That study suggested that nicotine might enhance coronavirus replication, resulting in more serious cases of COVID-19.
Other studies, however, have found that nicotine increases ACE2 expression in some cells and downregulates in others. Plus, study evidence suggests that ACE2 expression – whether up or not – does not affect infection rates. ACE2 inhibitors, for instance, do not decrease rates of coronavirus infection. Increased rates of coronavirus infection from nicotine patch use, then, do not, at this point, appear to be a problem.
An upregulation of the ACE2 enzyme might also work in favor of postural orthostatic tachycardia (POTS) and ME/CFS patients as ACE2 activity may be reduced in POTS causing high Ang II levels, inflammation, and vasoconstriction. The case for reduced ACE2 activity in ME/CFS is less clear, but a similar downregulation of the renin-angiotensin-aldosterone system appears to be present. It should be noted, though, that the available studies are small, and better ones are needed.
Patient-Led Results
An October survey of 175 long-COVID nicotine patch users found a perhaps not surprising result. Some people (20%) felt more than 50% better, more people (36%) felt 0-50% better, others (20%) felt the same, a few (5%) felt worse, and others (17%) were still checking it out.
Those results are similar to those of a poll asking about Bruce Patterson’s treatment approach, which found that a smaller subset did really well and a larger group did somewhat to moderately well.
We’re always looking for the “answer”. When HIV hit, all sorts of treatments, including ones that seemed surefire answers, faded when exposed to clinical studies. With COVID-19, we saw some early treatments that were touted highly by some doctors (Ivermectin) fail when exposed to clinical trials.
With long COVID, we’ve seen Bruce Patterson’s long-COVID protocol, guanfacine, monoclonal antibodies, anti-coagulants, etc., and now there are nicotine patches. Until we get good well-sized, well-done studies – and many may never get good studies – we’re never going to know for sure. The results thus far suggest that the nicotine patch is not “the answer” for the vast majority of us but that it could help.
One thing we can do is apply the Arseneau test which tries to assess whether to try something or not.
Applying The Arseneau Test
The Arseneau test assesses the factors below to help decide whether or not to try a treatment:
- The credibility of the source – Leitzke is new to the ME/CFS community at least in the States, but the fact that it’s a doctor’s report helps a bit
- Quality of the evidence – entirely anecdotal – low
- The benefit, the cost, and the risk–benefit – appear to range from high to nothing; there is the risk of a short downturn; otherwise, the risk appears pretty low, and the cost is low.
While nicotine scores low on several measures, there is a possible benefit. While the ME/CFS/long-COVID population is very sensitive, the Chambers survey found few long-COVID patients who reported being worse off. Plus, the Nicotine Test Group provides an easy-does-it protocol. All in all, it seems like a pretty safe bet.
The Nicotine Test Group
The Nicotine Test Group is a patient-led Facebook group Build on Patient-led Model started by @RemissionBiome, @RenegadeResearch, @TheAcidTesters, etc., that is doing great work at providing information about using the nicotine patch.
It emphasizes that it does not deliver “medical advice” and recommends that you talk with your doctor first but appears to be the go-to place to learn about the nicotine patch, long COVID, and allied diseases. It provides protocols, tips, FAQs, information on the ingredients in various patches, ways to assess treatment effectiveness, etc. (see Files).
- Check out the Safety Guidelines and FAQs documents
Nick Chambers opened up a private Renegade Research, #The Nicotine Test Facebook group, for people with ME/CFS who are trying the patch.
Take the Nicotine Patch Poll!
Nicotine Poll
Conclusions
Nicotine is an interesting substance! Who knew? (Peter Attia had a show on it in 2021). While it’s still speculative, it’s possible that if nicotine is able to knock the coronavirus off of the nicotinic receptors (if it is indeed binding to them), it might return the immune system to homeostasis and health while improving mood and cognition. Not bad!
Aside from that, the central role nicotine plays in the vagus nerve/cholinergic/parasympathetic nervous system is intriguing indeed given findings that this area is underperforming in ME/CFS, FM, and long COVID. Nicotine appears able to increase the levels of feel-good brain chemicals and help with mental clarity and brain fog – all of which would be helpful in these diseases. Nicotine, then, could be having effects that have nothing to do with the coronavirus.
Nicotine patches are cheap and readily available, and the long-COVID/ME/CFS community has done great work in providing safety and other information. That said, the patient reports are mixed, with some people doing really well with most others reporting less positive results and a few not doing well. That’s pretty much par for the course for these heterogeneous diseases.
If you decide to try the nicotine patch, be sure to check The Nicotine Test, start slowly and please report back :). (Thanks to Tracey and Jutta for their links :))
Health Rising’s Donation Drive Update

The nicotine patch…Who knew?
Thanks to the over 150 people who have contributed to Health Rising’s BIG (little) end-of-the-year donation drive.
Who knew that nicotine patches could be so potentially helpful and well, so interesting? It took some digging but that’s what we specialize in.
If you appreciate that kind of approach, please support us in a way that works for you.


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Are there certain nicotine patches that work the best? A name brand??
That’s a great question as different patches have different ingredients. I did see a discussion on a Facebook site about staying away from patches with phthalates, I think it was. I think the Nicotine Test website has some information on that.
Cort, I think that we are “wandering in the weeds”, with treatments like nicotine patches. David Systrome is right about ME/CFS being an oxygen delivery and mitochondria metabolism problem. Pyridostigmine will trigger better venous blood return to the heart, which will permit more freshly oxygenated blood to be pushed to the periphery. This should help more patients find some relief from their “brain fog” and fatigue. I think that he is traveling down a more productive road with his Pyridostigmine/ Low Dose Naltrexone trials. If there really is a genuine problem with the peripheral parasympathetic nervous system in ME/CFS, keeping more acetylcholine in the synapse with Pyridostigmine is going to be much more efficacious than nicotine. Thanks, for all of your hard work!
Keep in mind that nicotine also increases acetylcholine.
If nicotine massively increases acetylcholine early in the sympathetic nerve pathway, that would result in much more norepinephrine at the target tissue. I do not believe that would be a good result for most ME/CFS patients. It seems like Dr. Systrom is guessing that Pyridostigmine is increasing acetylcholine more effectively in the parasympathetic nerve pathways (vagas). This improved parasympathetic stimulation would explain why his patients report improved sleep, and less gut dysbiosis.
I’m guessing it’s much more complicated. Looking at others who have tried nicotine it’s pretty much a crapshoot whether it gives him some insomnia or it helps them sleep. I for one and much more calm on nicotine than without so how just want to explain that? My point is it’s probably much more complicated.
Have you had good results from the nicotine patch? I’m considering it for fibromyalgia.
The nicotinic receptors are part of the cholinergic pathway.
Yes, but the sympathetic nerves use acetylcholine until the final target tissue synapse. There they release norepinephrine. It really is not that simple because they also minor amounts of Substance P, GABA, etc. No nerve just releases 100% of of a certain neurotransmitter.
.
Nicotine acts on Acetylcholine receptors which are part of parasympathetic nervous system (not sympathetic)
Pyridostigmine was ineffective for my ME/CVS.
I’m gonna try the nicotine patch.
For our son, 18 yrs, 2 years of Long Covid/CFS, Pyridostigmine was also ineffective.
I’m sorry. It’s shameful that we cannot get help and patients have to figure this out on our own.
It IS a shame!!! However, we are now in very experienced hands here in Germany and Pyridostigmine does seem to help some patients. So this time it was not the lack of doctoral support but the varyiing effectiveness of the drug. And yes, we started to get medical help 20 months after this started only. So I will certainly not take the blame off the system. But in this case it wasn’t their responsibility…
Did the nicotine patch worj for you? How long are you into Chronic Fatigue? Big hug and take care !!!!!!!
I couldn’t agree more. I have been severely disabled ever since I had a bad reaction to the third vaccine. Loss of balance, instability and mini muscular like seizures.
When I see my health professionals they just tell me that based on vitals that I am fine!
How does one find a study into the problem of what I believe is some type of vaccine injury!.
Thank You for taking my message. I can be contacted at Josephstorer52@gmail.com
After covid, had really sore shoulders and upper arms, even into the neck and muscles at the back of my head. When I reached for anything the pain was severe, even had trouble dressing myself. I tried the the patch for 5 days a month ago, helped a bit, but wasn’t sure, so I stopped. The pain returned, even waking me up, so I went back on the patch, finished the other 25, and I am continuing to improve, can lift my arms, though not completely and have less pain. I will finish another 30 days of the patch. I also have fibromyalgia which wasn’t too much of a bother until I got covid in November, been in pain since, though I am getting better. I expect to completely heal since I take care of myself by eating well, keeping active with chores and so on. I take vitamins daily.
It’s been 6 months since I had Covid.
Hi Pauline, May I ask what brand you use and how many mg? Where you are describing your pain is exactly like mine. I’m happy it’s helping you! I would really like to try it. I just want to make sure to use a good brand and proper dosage. I hope you continue to feel better!
Hi there.
I feel as if I wrote your post. It sounds like what I have been going thru since September of 2025. I am 77 and having such a hard time. It hurt to hold my phone and I can barely use it my thumbs to text. It started in my legs and has worked up to my upper body and like you I couldn’t raise my arms can’t hold more than a glass in my hand. Can open up a jar that even the seal is broke. And sit in the frig. Hard to cook my wrists and hands are awful. I can’t do this anymore. I must at least try something to get some relief. I had Covid four years ago and lost my smell and taste which I never got back. If you have any tips please share them with me. I’m just about ready to give up. Please help If you can.
I hope you are doing better I pray for your recovery.
If it’s working for you please let me know what patch you used and for how long on and off and if you are still using it and how much it has helped
I know it’s a lot to ask .
Hope you can help Me get back on track.
Thank you,
Janine ~
Some patients like myself have viral issues that often includes EBV. LDN can trigger a “bloomig” effect on the dormant (or not so dormant as in my case) virus. There are freaks like me that respond very badly to LDN even at the lowest dose. I tried it for over a month and had such severe suicidal ideation that I almost gave into that. I am not that kind of person. I have never attempted or have been suicidal ever in my life except for the last two weeks of being on LDN and realised by some miracle that that’s what did it. After being off of it a week I was much more myself even though I was still very ill. The nicotine patches have been miraculous for me even though it took a long time to find ones that did not give me hives because I have other issues, including MCAS. It was worth it to find a patch that worked and I’m actively doing that again and today for the first time in a long while felt all 10 of my toes. Best of luck to all who struggle with chronic conditions. And remember science does not understand everything. Studies are very important but so is a large body of anecdotal evidence.
I would like to point out a misunderstanding concerning the knowledge base about nicotine knocking off spike from receptors.
There is no evidence that nicotine binds to acetylcholine receptors with an affinity 30x that of spike protein. The “30x affinity” refers to the comparison between nicotine and acetylcholine.
(Quote from Leitzkes 2023 study: “The agonist ligand nicotine shows an up to 30-fold higher affinity to nACHRs than acetylcholine (ACh)”.)
Also, please note that of the four patients in the trial, three were only 3-6 weeks post infection onset. The fourth was nine months in.
I am not against trying this treatment, I did two rounds myself (LC for 18 months), but I am concerned about inaccurate or exaggerated being passed around in the LC community.
Thanks for clarifying that – I took it from the Nicotine Test site but did not source it.
Based on Systrome’s presentations, I have a feeling that nicotine is less targeted toward the parasympathetic nervous system than Pyridostigmine. If increasing acetylcholine early in the peripheral sympathetic pathway results in an increase in norepinephrine at the blood vessel, that would not be a desirable result for many patients. Many are “wired and tired”. They have excess sympathetic tone. Nicotine might worsen that. Many ME/CFS patients take benzodiazepines to help lower their sympathetic tone, just to get some sleep.
Pyridostigmine may well work better than nicotine, but many of us don’t have a doctor who would prescribe it off label. Nicotine has the advantage of being available for all of us.
Yes, it is a shame. Many NIH Neurologists realize that Doc Systrom has an already FDA approved drug that could greatly help a subset of ME/CFS – Long Covid patients. But, they will drag their feet, as always.
Thx for ur note , I wanted to try it and I wonder if it worked for you(?)
Nicotine helps me sleep. Gives me a calm energy in the day with more mental clarity. ME/CFS for many years.
Huperzine as alternative to pyridostigmine?
As far as I remember from my first low-dose nicotine experiments, at least in my case it did not make the wired & tired worse, but had the opposite, calming effect (while also keeping me awake longer though). It definitely felt very different from the stimulating effects of coffee or being wired on adrenaline.
I still have to try Pyridostigmine or Huperzine A – did it help you with wired & tired?
Thanks for making sure things are clear and turthful, so much info to weed through.
How has nicotine worked for you?
Nicotine started to work but then I had a reaction to the chemicals in the patch. (I have chemical sensitivities).
Hi Cort
I have mcas and Mcs .did the chemical effect you
Yes, unfortunately the chemical in the patch did.
How are you doing now .I have chemicals sensitivity
Chemical sensitivity is still a factor – cannot sleep indoors – but has been slowly but steadily improving. Some people have been able to recover using the DNRS program.
Hi Cort can you help me with this please x
I agree, 4 patients with short relatively short durations of LC is hardly a study. I’m on nicotine and it does make me feel better for what it’s worth me/cfs 20 years
From what I can see all the brands have phthalates in them. If anyone knows of a brand not containing phthalates I’d be interested to hear about that.
Rugby nicotine patch does not contain phthalates
Thanks!
We talk about the patch brands in our FAQs. Near the end. It is based on the data and feedback from early testers.
Thanks!
Hi Cort can you help me with this please x
I was cured of 5 months of post covid asthma in 4 days using the patch. My doctor told me to remove it at night, so I used 1 patch for 2 days. Previously, I had been on steroids for 16 days, only to have asthma return. I had been using albuterol all throughout the day and night. I don’t need the inhaler anymore.
Wow – isn’t that something! Congratulations!
Mix nicotine with some curated dry fasting, never fails to help more. (Check it scorch protocol) The nicotine is like my antihistamine to pushing too far and getting shortness of breath.
You removed the patch at night and then put the same patch on the next day?
Hi Vanessa,
May I ask what kind of Dr. gave the ok for a nicotine patch being used to treat asthma??
I have been suffering with post Covid asthma for 4.5 years now! I am about to see my 4th pulmonologist in a few days. They keep trying to push Nucala Biologics injection to treat this as it is severe and my inhaler hardly touches it. I have been putting it off for 3.5 years now.
I am praying to God he show me which path to take because I really don’t want to inject my body with anything!
I’ve also been working with a naturopath who says long Covid is adrenal insufficiency, ME/CFS. Which now looking back I realize I have suffered with at a tolerable level before getting Covid in April 2021. After Covid my immune system tanked and I’ve been absolutely miserable since. He is helping me to slowly regulate my nervous system by doing vagal nerve exercises and guided meditation. Of course this will be slow going and isn’t an easy overnight fix. None of it is, but if I could have some help in the meantime with this asthma instead of doing an injection, I’m all for it.
I do not have FB so I don’t have access to any of this Nicotine test info either. I see from the article that it says to start at the low dose 3 mg. for 3 days and then use the 7.5 mg. patch for 7 days and stop. Then what? I wish this article had told you exactly how to use it.
I don’t know where to begin now…
Thank you for any info/advice you can share. I am desperate and have been out of work for 4 years this December. I waited 2 years to file for SSDI thinking I was going to get better and go back to work.
They denied me of course. Now I have an attorney and will face a judge this December to find out if he will rule in my favor. I’m only 44 yrs old, so of course they look at you as “too young” to be disabled! Frustrating to say the least!
Anyway, thank you!
Hello Cort, Do you know if I can find the complete nicotine patch protocol in a format other than PDF? Because I can’t translate the files. I can only translate websites with Google Chrome.
The cheapest one ($20 from Amazon) works just fine. I plan to buy 21mg for the same price the next time and cut it into 6, like Jeff does. It’s a transdermal patch that delivers nicotine, not a chemotherapy. It may deliver/wear out a bit quicker, but that could well be of advantage since you could be off the buzz by the evening.
These patches should not be cut they’re not designed to be cut it could release an undetermined amount of nicotine. One can remove only a partial portion of the backing as an alternative
Dr Ardis recommends cutting them
You may want to keep a buzz for night if small enough and you can handle it. It increases REM sleep but with it can come vivid nightmares.
Very interesting. I’ve been using nicotine patches here and there for years for brainfog and mild energy boosts. Having been a smoker pre-ME, I haven’t wanted to use them regularly to avoid addiction and the awful withdrawal process, so I would only take them a day or two at a time. I’m going to try the protocol described here and see if there are any longer-term results.
FWIW, I’ve always cut the patches, as the larger dose patches are often the same (or close) price as the lower doses. I’ve sometimes even cut them into quarters, with no perceived difference in release. I don’t understand the recommendation to put tape over the unused half instead – how is that any different than cutting them? The same amount of patch is still in contact with the skin, yes? Does cutting them somehow change the release speed or mechanism?
Interesting article, and something very easy to test. Thanks Cort!
The reason not to cut patches is that cutting them can lead to an uncontrolled release of nicotine and therefore overdosing. That is definitely true for a type of transdermal patch that contains a liquid reservoir (membrane/depot patch). It’s an interesting question if this is true also for the type of transdermal patch called “matrix patch”. For example this website https://www.sps.nhs.uk/articles/using-transdermal-patches-safely-in-healthcare-settings/ says that matrix patches can “sometimes” be cut, so I guess one can’t be sure about that unless asking the producer? May I ask what brand you cut?
Interestingly, the producer’s information for the specific brand pf matrix patch I used mentions that cutting the patch can reduce effectivity beyond just the reduction of size.
The Nicotine Test safety guidelines say not to cut any patches to avoid overdosing.
The patches I use from Amazon are single patches with a perforated line down the middle to allow you to cut them into two separate pieces. The total patch has 21mg. Cut in half gives you 1/2 of the 21mg dose. I have been using them for about a month. I do feel the positive effects so far. I have a mild form of CFS however.
Googleing “can nicotine patches be cut” also yields reasons like “Doing so can alter their release rate and may compromise their effectiveness” or “Cutting the patch interferes with the way the nicotine is released – allowing too much to be released too
quickly as well as allowing the nicotine to leak out on the skin. Cutting the patch is not recommended.”
Very interesting, thanks for that. The patches I have are Habitrol 21mg I got on Amazon (meaning perhaps chinese/fake). But I’ve always cut them, even in quarters, and haven’t noticed any perceptible difference in strength or delivery.
I can see that the dose might not be distributed evenly across the patch, causing one half (or part) to have more nicotine than the other (or even all vs. none) but it never occurred to me that the delivery rate could be different. It just appears to be a thin, flat piece of plastic (or whatever the material is). I wonder if manufacturers discourage the practice mainly to prevent users from cutting them and thereby getting a better value? I won’t stop, at least, unless I start noticing a difference.
I also would not be sure even if cutting matrix patches, if they’d give off a bit more around the cut edges?, or if the contact with air would influence the stability of nicotine in the unused pieces if not stored airtight. (Neither am I sure though if keeping one patch 4 days on the skin to use all four quarters without cutting might affect nicotine due to body temperature). I’ve found one New Zeland site that says matrix patches can be cut https://www.medicinesinformation.co.nz/bulletins/can-transdermal-patches-be-halved/, so as the matrix patch is the more modern type, I am asking myself to what extent the general warning not to cut patches might stem from a time when almost all transdermal patches were reservoir patches which would leak gel/liquid when cut. But as these two reddits about cutting patches demonstrate https://www.reddit.com/r/LifeProTips/comments/jqelce/lpt_for_those_trying_to_quit_smoking_with_the/ , https://www.reddit.com/r/LifeProTips/comments/5uycxa/lpt_when_using_nicotine_patches_to_quit_smoking/?rdt=60951, though some people cut them and one claims it’s easy to see if something leaks out when cutting, overdose emergency hospital admittance due having cut patches is also a real and dangerous thing both for nicotine and fentanyl patches, and what type of patch is available on the market might depend on the country.
So with the Nicotine Test being a worldwide project, it totally makes sense to warn against any cutting of patches for safe use.
I wonder if one could cut the patch and then tape up the cut edge so that the nicotine could still only get out the way it’s supposed to.
The patches I used are rather small, so you’d lose a lot of surface that way. But have a look at the latest guidelines by TheNicotineTest project – if I remember correctly, they mentioned somewhere that many people (including myself) have cut the matrix patch type without problems.
Since I last posted, a producer explained to me that when cutting matrix patches, the producer cannot guarantee the amount of nicotine taken up in 24 hrs from that patch anymore, because size of surface matters for how much and how fast nicotine will permeate from the patch into the skin – this osmosis process will be stronger and faster in a larger patch.
They could not make any statement on whether for cut patches, there may be either slight leakage along the cut edge, or a possibility of the patch drying out or oxydizing from air contact along the cut edge. But the matrix patches are very thin and do not seem to ooze anything when cutting, so I believe it’s negligible.
And I can’t say whether the matrix patch formula contains anything that could dry out.
So, by now, I personally do not worry much about cutting matrix patches: When you’re using it outside of a scientific study, it matters less to know for sure the exact dose you’re getting from the cut patch, and more what cut size (equalling an approximate dose) is the best fit for you judging from the effects you get.
Just as a preventative measure in case anything could go bad from air exposure, I put cut pieces back into the little pocket each patch comes in and seal it with cellotape (but again, I don’t even know if that’s an issue at all). On the skin, I also put medical tape on top of the cut piece.
Everyone be safe, consult TheNicotinePatch project guidelines, and mind overdose risk is definitely an issue for reservoir type patches (if these still exist).
And anyway, that osmosis effect is not relevant because it would apply to partly applied Nicotine patches whether cut or not.
I watched a video by Dr Ardis whose premise and conclusion were that nicotine never has been and never will be addictive.
“I wonder if manufacturers discourage the practice mainly to prevent users from cutting them and thereby getting a better value?” – As the producer’s information does not explain why or how cutting matrix patches may possibly reduce effectivity of the patch beyond size reduction (and if by effectivity they mean nicotine release or sucess of quitting smoking), I unfortunately cannot verify if what you suggest may be involved too 🙂
Peter Attia describes using them for a while – ten days, I think – without problems with addiction. I’m going to give them a try – even a mental boost even now and then would be great 🙂
I saw on a Facebook site someone else cut them without problems as well.
Thanks, Cort. I’ve read that in addition to the pro-cognitive benefits, nicotine also has fairly potent anti-Parkinson’s effects, so aside from the possible cardiovascular issues everyone worries about, it seems otherwise to be a remarkably beneficial drug (when not delivered via tobacco, at least).
I wonder what nicotines role is in insulin sensitivity, I have a theory that a lot of the problems are around insulin resistance even if you have normal blood sugar levels. We know Alzheimer’s and Parkinson’s related to type 3 diabetes.. food for thought and also why fasting and specifically dry fasting reports such beneficial results.
Cort,
I felt a slight improvement after 10 days. The protocol says to stop, but is there any info out there about continuing?
Upping the dose? Taking it long term with occasions breaks?
I dont want to give up, since I’ll take a even a tiny improvement.
As I understand, you should take breaks and then resume again so that you don’t build up tolerance 🙂
If I find out nicotine has actually been helping me all this time I will be shocked! Also annoyed at all the time spent trying to quit NRT, which really is addictive. I’d warn anyone thinking of trying it that I’ve been on NRT since quitting smoking decades ago in my early 20s. I have not succeeded in stopping the NRT. In fact I often wonder if the vascular and stimulant effects of the nicotine, combined with long term exposure to the sweeteners in the lozenges, have contributed to my fibromyalgia. During a period of a few months where I was able to quit I felt healthier, and my pain got significantly worse shortly after I relapsed my addiction. Despite desperately wanting to feel better, the withdrawal is so uncomfortable for me that I always give in. Don’t take this step lightly, you might be adding an additional problem to your life rather than helping yourself.
Sarah, thank you for sharing your experience. May I ask if you use patches or lozenges, and at what dosage are you still on NRT?
From what I’ve read so far from the Nicotine Test documentation and links, patches are said to have low risk of addiction due to their constant release, which also is not coupled to behavioural habits like short term release from cigarettes or lozenges/chewing gum.
I would not be concerned about trying it for the limited time rounds (e.g. 7-10 days) as in the original study/TNT protocol. But there also seem to be people who take it for months (with some breaks now and then) and improve over time, I guess we’ll have to see what they can report about long-time use?
P.S. I am crossing my fingers and sending best wishes for your sucess in quitting if you felt healthier when quitting your nicotine replacement therapy! I’ve never been a smoker but have read many smokers are finally successful if they take enough attempts, so I am sure you’ll have success one day even if it takes several tries…
Hi JR thanks for your good wishes. I take about 8mg a day, 8 x 1mg lozenges which I break in half. I have used patches before and had the same difficulty quitting them.
I am personally quite sceptical about nicotine patches being less addictive, but would be very happy to be wrong.
Sarah, I can so relate. I quit smoking about 25 years ago, and until 6 weeks ago, I was chewing nicorette gum like a demon. I did quit once for a short period, but I went back to it. A series of synchronicities happened in my life, and I’m giving quitting another try. I started with a week to 10 days of bupropion and the largest patch. I have about 3 of the 7mg patches left, and I’m surely hoping to say goodbye to nicotine forever. I wish you the best with your fibromyalgia and grace to live with nicotine addiction, which can feel so dreadful.
The reason that the nicotine patches are less addicting than cigarettes is because it’s a slow constant release you don’t get that dopamine hit or feel good rush. If you’re using lozenges they’re going to be more addicting because it’s a quick release not a slow steady.
Hello, Thanks for your comment about your experience with NRT.
After extensive research all studies say that NRT is not addictive. You are the first person who I have seen mention this addiction.
There is also very little data on what long-term use of NRTs would be like. It is only clear that the dose is important.
What brand and dose do you use?
Where on the body do you apply the patch?
After 3 to 5 days receptors completely reset. Have you stopped for longer than 5 days to see if the “withdrawal” is still present?
Also, “withdrawal” and addiction are two different things. Would you say it is more a withdrawal feeling where the body needs time to adapt or is it actually an addiction where you get anxious for your next “hit” of nicotine?
I myself have been addicted to NRT for many years. I have also met a few people in chemists when buying saying the same thing. It’s a falsehood that NRT is not addictive… maybe not for everyone, but it certainly is for some. Obviously, it’s far better than smoking or vaping but the continued nicotine cravings are very real. I would say there is actually some shame in it and most people on NRT don’t openly admit they are still addicted to dreaded nicotine. So having said that, and having read many comments and articles on NRT for LC … it sounds interesting and potentially a game changer for some but be careful… staying on NRT for too long may get you addicted to nicotine… and I’d hate to see people have that happen to them.
Agree 100%. Nicotine is addictive in all forms. After completing a second four or so week cycle of patches, I absolutely experienced mood swings that were identical in intensity to quitting smoking cigarettes a decade prior.
Also, had zero improvement in ME/CFS symptoms, except for cognitive speed when on the patches, but the stimulators effect ended when the trial ended and did not persist.
Cort, pay attention in class! You missed the link in terms of nicotine’s benefits for neuroinflammation which I have mentioned several times. The MS study….
I have long been a proponent of nicotine in this illness. Significant improvements for me correlated with me picking up social smoking around year 3/4 of my illness.
Of course smoking is bad! So I got off it and found nicotine patches helpful
I missed neuroinflammation! Say it isn’t so! (I will look it up!). Thanks 🙂
would you be willing to connect with me regarding this Matthias? ive had terrible brain fog for some time.
I know this is about nicotine but my brain fog and almost non existent short term memory after 4 years of CFS/ME has been hugely helped by a daily dose on waking of 500mg Acetyl L-carnitine. It took about 6-8 months before I realised I was thinking a lot more clearly and my short term memory was improved. It also gives me a slight but noticeable lift in energy.
Nice! Thanks, Keith for sharing that. 🙂
When my husband quit smoking 10 years ago, he developed an inflammatory disease afterwards. In his stop smoking support group, many other members found they developed physical illnesses after they stopped smoking.
FWIW, I remember that in the 1980s, the tobacco companies considered marketing nicotine to kids with ADD.
I am so glad you were writing about this! I started on 3.5 mg just over a month ago and the improvement in my cognitive abilities is dramatic!
I was a heavy smoker for 17 years, but quit in 2004. Almost immediately, I started having ME like crashes.
I am using Sefudin patches ( Amazon brand) and cut half the plastic backing off a 7 mg patch and hold it to my skin with medical tape.
I urge everyone to check out the protocol and give this a try. It has been wonderful to have my mind working so well again.
Reading Leitzke’s Four Case Reports, I noticed 2 of the 4 patients visited the clinic within 3-4 weeks of their positive covid test. It is pretty strange for this paper and for them to consider that long covid. WHO says persistent symptoms after 3 months is qualifier. And 3 months is nothing… just saying. While the other cases have more time between positive test and nicotine treatment, the fact that the two I mentioned are included lowers the quality of evidence even more, in my opinion. But am I personally willing to try? Possibly…
Indeed, it’s absolutely horrific that a study that was the start of these nicotine experiments is so heavily flawed and methodologically quite horrendous.
There’s a tremendous amount of Longhaulers (thousands), particularly in large cities like Berlin (it’s also possible to have access to well established cohorts for example from the Charite), with a long illness duration. When 2 out of 4 patients don’t even meet the most basic LC criteria and also haven’t had a check-up for any other medical conditions or even deficiencies (3-4 weeks after a positive test means this was one of their first if not their first drs appointment post infection).
If this was a CBT/GET study we’d be rightfully heavily critising the methodology. We should be doing the same here.
I missed the fact that they were short-term long haulers and it’s true that the case reports were not top-notch – they lacked the details and thoroughness that better case reports provide. On the other hand I don’t remember case reports going to the extent of checking patients out for other diseases. I could be wrong but I don’t remember that.
In any case,the Facebook survey suggested the nicotine patches – when used correctly – were quite safe.
Though true 4 case reports do not equal a randomised controlled trial, cut that doctor some slack: Leitzke https://www.helios-gesundheit.de/kliniken/leisnig/unser-angebot/unsere-mitarbeiter/profil/person/marco-leitzke-desa/ is a doctor of anesthesiology, intensive care, pain medicine and palliative medicine, who obviously just tried something new to help the patients who presented with the outpatient clinic where he works, based on previous discussions of nicotine for other neurocognitive conditions, see e.g. 2021 German Spektrum der Wissenschaft article https://www.spektrum.de/news/kognition-nikotin-gegen-neuropsychiatrische-erkrankungen/1924141 .
His paper is not a “study” designed to test statistical significance, it is simply a hypothesis paper with 4 case reports. These sorts of case report papers can be important for scientific progress too, because they can publicise new hypotheses and treatment possibilities to other scientists, which can then lead later to larger randomized controlled trials with proper statistical methodology testing these hypotheses. For example you also often find such small case report papers for new side effects of medication, rare disease combinations etc. Many treatments start with small papers.
Therefore I don’t think it would be fair to accuse his paper of being “horrific”, “heavily flawed” and “having horrendous methodology”, because it is not a full study but simply a hypothesis/anecdotal case report paper which typically would have a small number of cases that does not allow for statistical significance.
Patient-led “The Nicotine Test” then picked the treatment up to generate larger numbers of patient experience and collects results in a survey, because if we’re being honest, a randomized controlled nicotine trial is not going to happen tomorrow.
That being said, I agree it’s important being aware that a small paper with n= 4 case reports and mixed patients (2 post-acute covid, 2 long covid) does not allow for statistically significant results, just explaining this paper is a small hypothesis/case report paper, therefore it would not be fair to expect it to be something it isn’t 🙂
I never criticised that this isn’t a RDBPC. Nor did I criticise that it was a case study. Nor did I question the sample size. Obviously one has to start somewhere (at least that was never the intention of my comment, I was alluding to the 2 out of 4 patients, I apologise if that wasn’t clear).
However, none of these things play a role when discussing the methodology I mentioned above. The problem for me is the cohort selection. This is an ever present issue in LC and ME/CFS research unsufficiently addressed which leads to an unneccesary increase in unreproducible studies. Gargabe in, gargabe out.
What would you be saying if this was a CBT/GET study? 🙂
It’s potentially garbage but not necessarily garbage. It’s possible it might be garbage but you actually don’t know either way. The patients might have a perfectly good case of long COVID.
I see where if a study is not done to standard its considered garbage. That’s not scientific either. This is kind of a fine point but in reality you don’t know if it is or not. You can’t simply reject it but you can’t rely on it either.
The CBT/GET question is kind of moot since we’ve never had CBT/GET case reports. All we’ve ever had are studies and some really large ones due to government funding. I think I would point out – as I did in this blog – that these are case reports and therefore of low quality evidence.
The fact that nicotine is cheap and safe, though, mitigates against the need for a really buttoned down study. Since the costs and risks associated with it are low I don’t need a lot to convince me to try it. If it was a dangerous drug that would be a different situation.
The quality of a study is not driven by its outcome. That is something every physicist understands, proving something is not the case is no different than that something is the case and the one isn’t more publishable than the other. Medicine and especially pharmaceutics, naturally being a positive result driven science (after all you want to treat patients) suffers from this publishing bias and as a result poor methodology drives the replication crisis in medicine.
I agree with your point about CBT/GET case reports, but my question was more of philosophical nature: What would your stance be if instead of “nicotine” the treatment was “CBT/GET”? After all the quality of research is not determined by what we believe is right or wrong or what or favourite pet theory is, but quality is quality independent of beliefs. After all the CBT/GET studies are methodologically horrendous including the horrendous scientific reasoning and evidence. I do appreciate that you pointed out that this study yields low evidence and I particularly appreciate that you pointed out that the author cites all positive Covid-19 nicotine results but fails to do so with negative results.
Cohort selection has probably been the primary driver of unreproducible results in LC research, but some significant steps have been made by subset of researchers into the right direction that have started to look at different phenotypes, after all no one should argue that PICS or organ damage are equivalent to ME/CFS.
I would argue that nothing ever mitigates the need for rigorous research. Of course patients can try out whatever makes them feel better especially if no risks are involved, but I can’t think of an instance where this has never advanced the medical field. Even though it didn’t yield positive results I am happy that we now know of the negative results of LDN in Fibromyalgia, but even more so it’s particularly important that trials with negative results are still methodologically strong enough to yield mechanistic insights, as was the case in Rituximab, where we now know that C-19 driven autoimmunity either only affects a subset of patients or autoimmunity isn’t primarily C-19 mediated.
Correction: Not sure what went on in my head, C-19 should of course be CD20.
Hey Julie I have some questions for you. Have had terrible brain fog for over 15 years and its debilitating.
I’ve got a long history with nicotine. Started smoking at 13 and my fibro symptoms started to appear in the following years. Two years go, at age 40 I finally realised I have a severe nightshade allergy that gives me joint and nerve pain. So my smoking was causing me a lot of pain for nearly 30 years.
These days I sometimes find myself puffing away on a nicotine containing vape. I take to it easily but notice how the dopamine hits start to mess with my neurochemistry within days, leading me feel worse at baseline and to crave more. After years of practice, I can get off it relatively easily, as long as I don’t keep a vape lying around
I came across the early covid nicotine promotions and actually used it as a poor excuse to take up smoking again (it was a stressful time and this was before my nightshade insight)
I’ve often wondered why I like it so much and I’m now wondering if there is some broader effects that this article highlights that I’d not previously been aware of. My fibro is pretty well managed these days through a variety of strategies but I might get me some nicotine patches and see what they do
Great article! I’m going to try the nicotine patch protocol. When I was a smoker I enjoyed the boost it gave me. I drank coffee and smoked cigarettes and felt great! (Until it didn’t). The smoke was bad.
There is the opinion out there that nicotine is actually NOT addictive, that other chemical additives in cigarettes make them addictive. I can dig up sources, if there’s interest.
Seeing some benefit from 7mg patches…
Thank you Cort. What a great article!
If anyone is interested, here’s my ME/CFS journey trialling Nicotine Patches:
https://docs.google.com/document/d/1-wZoQ0W8UmNcFlz705EBAGI43WwhfqIep_-S8rzaC9o/edit
For those of you that are visual learners, here’s a great YouTube video explaining how the nicotine might work in our system:
https://youtu.be/ZrxQD1BB-ME
I love the fact the patches have helped so many people 👏🏼
Nick, aren’t you the main guy behind the nicotine test public face? And the nicotine has not been the cure for you right?
Yes. Troy and I run the group. The patches haven’t been a cure for me, but they are a game changer and my health is 95% better. Especially if my gut biome is on par. I wear the patches 6 days a week and 10 hours a day.
No night time? And when you say 95% does that include heavy exercise? I know 99 if not 99.99 recovered long haulers don’t exercise. I know the power of nicotine to prevent or suppress flare ups but there’s also the stimulant effect that wears out the nervous system like caffeine. What about the diminishing returns? I’m surprised you wear it 6/7 consistently
I did do nighttime for the first 2 months, but then found I didn’t need to. I don’t do heavy exercise anymore. If I have energy, I socialise, do diy, spend time with my son etc. the energy is still not infinite.
Join our fb group for details on 10,000 other users. Many are different and do what works for them.
hey Nick I would love to know how to get help…had terrible brain fog for over 15 years. been hell
https://linktr.ee/thenicotinetest is where you can get more info. Or join our fb group the nicotine test.
what an extremely bad idea to test nicotine on patients. If effective, it is at most symptom treatment and most of the papers suggesting a good effect is just speculation. MOreover, while it may help smokers reducing their addiction, it will ofcourse lead to addiction with MECFS and LC patients who, because of their disease, hardly have any energetic resilience to eventually withdraw them from using nicotine.
I didn’t find anything to suggest that addiction is a real problem with nicotine patches. The highly addictive nature of nicotine apparently comes from the quick hit to the brain that occurs when it is inhaled in tobacco smoke.
Cort, do you know whether it has been thoroughly tested on non-smoking individuals?
I don’t have the studies but I know it’s been studied to assess its effects on cognition and in athletes and is being or has been studied in depression, chronic pain, MS, Parkinson’s, Alzheimer’s and other conditions. I assume they’re using non-smokers and smoking could be a big confounder.
Let’s not kid ourselves. Nicotine is a stimulant. I tried the patches twice in the last couple of years, and although it gave me an initial boost after a couple of weeks, the effect was almost gone. Could be due to building tolerance or something else. I am not sure, but no long-term effect was achieved. The side effect I suffered was insomnia. While I was using the patches, I could not achieve a good restful sleep and had to discontinue the experiment both times. Of course, we are all different, and the protocol might help some, but it certainly did not help me.
Nicotine is a bunch of things including a stimulant through its ability to upregulate norepinephrine I think it is. Some people with ME/CFS, though, actually do quite well with stimulants and they are included in the recent Mayo proceeding in managing ME/CFS. The fact that it is a stimulant is not necessarily a problem. It all depends on your body chemistry I guess.
Have a read of the research and polls. It sounds like you didn’t do the patches for long enough.
The initial side effects are a slight loss of sleep, but that disappears after 48 hours.
https://linktr.ee/thenicotinetest
@nick, why do you assume I did not do the protocol for long enough. You, like all the doctors, assume that if someone reacts differently, it’s because they have not complied. Both times I did 21 days with a break afterwards and repeated.
Sorry, I didn’t mean to cause any offence.
I hadn’t heard of people not being able to sleep after longer rounds, especially if they’re wearing the patch 24/7. The testimonials generally state sleep improves.
Also, as you had trialled the patches before a lot of our recent research and understanding, I just assumed that was the case. I’m sorry it didn’t work you. It doesn’t work for everyone unfortunately and we’re digging deeper to try and understand whether outcomes are affected by detox pathways etc.
Is our problem the parasympathetic nervous system or the sympathetic system or is it an imbalance between the two? Many of us have POTS, which, as I understand it, and from a study I was involved in, upon standing, the parasympathetic and sympathetic nervous system decreases. However, in a person without fatigue, the sympathetic SN accelerates. So, shouldn’t we rather treat the sympathetic SN?
If we stimulate the parasympathetic SN (with nicotine patches for example), what happens to the sympathetic SN? Is he also stimulated?
Sorry, it’s a bit technical, but I think it’s essential for many of us to find a good sympatho-vagal balance.
It’s very complicated and in different people it will be different. S
Because the parasympathetic nervous system reins in the sympathetic nervous if it is underperforming that could allow the SNS to ramp up – and that’s what appears to be happening in many people but there are variations.
As you note, though, the SNS is not doing well either. During exercise the SNS should drive the heart rate up but it appears to quickly poop out n this diseases. To me, the SNS seems like a system that’s been chronically activated and has become exhausted; it’s always on but when asked to pick up the pace, it can’t do it. If the PNS can calm it down maybe it can recover.
Interestingly, if I read it right, nicotine may be able to enhance both the SNS and PNS.
Some people believe that it’s not just that but that the autonomic nervous system is having trouble finding a balance and keeps jumping around.
Its been overlooked but there was a study published in Nature re small amounts of nicotine added to rats water daily. They had a marked increase in NAD+ levels..presumably through the AMPK pathway. Also, there are studies on benefits to neurodegen diseases including MS.
Ron Davis says that 25% of ME/CFS patients probably have MS..I am probably one of them. And of course the Parkinson studies. Lots more going on than just boosting acetylcholine.me thinks.
Hi Cort,
You state that “it’s a bit surprising that nicotine patches have not been tried before in diseases like ME/CFS and fibromyalgia.”
This is incorrect. Pioneering CFS doctor Jay Goldstein for one was using Nicotine patches and gum decades ago. See his book “Tuning the brain”
https://www.frontiersin.org/articles/10.3389/fphar.2020.594591/full
I have already posted this to a previous post but this gives another perspective on Tobacco as a healing agent. Give it a glance!!
Many years ago, before he retired, my doctor was Jay Goldstein. Dr. Goldstein was known for trying different modalities with his patients even though some might have seemed odd to most of the medical community. Under his direction, I tried the nicotine patch for a few days. I had to remove it due to it causing a chronic headache. It’s been over 20 years since I tried the patch and I would be willing to try it again.
Thanks for your nice comment.
It can cause headaches initially. We find a definite need to consume more fluids when starting the patch.
Do you know of any connection between the nicotine patch and carbon dioxide levels in the body? I’m seeing people with Long Covid struggle with hypocapnia…
CAUTION: This is what the AI-program “Perplexity” comes up with, when asked about the health effects of nicotene:
Nicotine negatively impacts brain development and changes brain chemistry, and its use during adolescence and young adulthood has been associated with lasting cognitive and behavioral impairments. Nicotine exposure during pregnancy harms the developing fetus and causes lasting consequences for the developing brain and lung function in newborns. Nicotine is not safe and raises blood pressure, spikes adrenaline, and increases the likelihood of having a heart attack. It also poses several health hazards, including an increased risk of cardiovascular, respiratory, and gastrointestinal disorders, decreased immune response, and ill impacts on reproductive health. Nicotine is not considered a carcinogen, but many studies have consistently demonstrated its carcinogenic potential.
Also the following: Nicotine, in its pure form, has been studied for its potential beneficial effects in the medical field. It fairly specifically binds to the cholinergic nicotinic gating site on cationic ion channels, which stimulates the release of various neurotransmitters. Chronic use of nicotine has been associated with positive reinforcement, negative reinforcement, reduction of body weight, enhancement of performance, and protection against certain diseases such as Parkinson’s, Alzheimer’s, and ulcerative colitis. However, it’s important to note that nicotine also poses several health hazards, including increased risk of cardiovascular, respiratory, and gastrointestinal disorders, decreased immune response, and adverse effects on reproductive health. Therefore, while nicotine may have potential therapeutic effects, its harmful effects should be carefully considered.
And 99.9% of the studies are all about smoking not nicotine alone. Don’t believe everything you read on AI
No it’s true. There are many studies just looking at nicotine.
It’s great for reducing inflammation, brain fog, m.s. Alzheimer’s endotoxemia, but it’s definitely linked with heart disease. Nicotine itself
Patients with HIV can now live normal life spans. Why? Because the cause is known and the best research and resulting treatments follow knowing the cause.
ME/CFS will continue to be in the neverland of try anything. Tout small studies. Write about “miracle cures” promoted by people making money and designed to take advantage of desperate patients.
Patients grasping at straws to get any measure of relief will try anything. (I once had all my mercury fillings replaced because my symptoms seemed so much like mercury poisoning.)
Let’s go back to the well of “what is causing this” and remove outliers like Elhers Danlos (which is a genetic disorder) from consideration.
If researchers aren’t is working on the cause anymore, we are all in trouble.
Yes, people will try anything! There’s a long Wikipedia page on all the bizarre things that people were sure was going to treat COVID-19. It’s really something!
I was so struck by a talk where Michael Peluso said HIV treatment was at a standstill….patients were findings all sorts of ways to get drugs and get better – some of which were supposedly great (but weren’t really) and all of that changed when they found the right kind of biomarker called a surrogate biomarker that could demonstrate when patients were getting better or not – and the drugs just rolled in!
https://www.healthrising.org/blog/2022/12/22/explosion-therapeutics-long-covid-biomarker-chronic-fatigue-fibromyalgia/
Peluso said ” “we really desperately and urgently need other measurements that we can make to supplement the clinical data that people are telling us”; i.e. they need biomarkers!
Peluso compared the situation with long COVID now with the early stages of the HIV epidemic. They have some ideas about mechanistic biomarkers that can demonstrate how severe the illness is but no diagnostic, predictive, or surrogate biomarkers.
I imagine that finding a surrogate biomarker is a top goal of the RECOVER Initiative.
@Betty; not sure why you want to remove ‘outliers’ like EDSers. In Stanford’s ME/CFS clinic, before Long-Covid took over, somewhere between 1/3rd and 1/2 of their patients had EDS and also met the criteria for ME/CFS. Many people with EDS who do not have ME/CFS or Long-Covid have ‘slick’ fingertips. It was a big joke on Inspire (blog) as many EDSers couldn’t open plastic bags or use fingerprint ID and similar stuff. I have that problem. I also have had the red crescent–but that was because I had some kind of strep throat. As for the ‘thick blood’, I’m not sure about that, but I do decidedly have EDS.
It’s estimated about 80-90% of symptomatic EDSers (people with significant flexibility and other problematic related issues) have fatigue but what you may not know, it is also estimated that of all the super hypermobile people, approximately 1/2 are not symptomatic, 1/4 are somewhat symptomatic and the rest really suffer. The last group often end up at the doctor.
Personally I think that keeping EDSers in the mix may be important because we all have genes and there might be something special about EDSers which makes them more susceptible to symptoms like fatigue and PEM and disorders like ME/CFS and Long-Covid. Anyway, there seems to be many subsets of these disorders and ultimately I hope that individualized medicine will prevail.
Hi Nick, can you assuage any fears about the published data showing nicotine damages the endothelium and causes heart disease
Dear Nancy, I have to admit that our own data suggests that there is some predisposition in Elhers Danlos patients to develop ME/CFS. I am the director of the National Birth Defect Registry. We have data on nearly 10,000 cases of both structural and functional birth defects. Our registry has 42 cases of Elhers Danlos registered. These are the top related conditions reported
Top 20 Related Conditions
Joint Pain 28
Frequent Headaches 26
Allergies 25
Muscle Pain/Weakness 25
Reflux 22
Heat/Cold Sensitivity 21
Anxiety Disorder 18
Chronic Stomach Problems 17
Light Sensitivity 16
Migraines 14
Chronic Fatigue Syndrome (ME/CFS) 14
Depression 13
Scoliosis 13
Drug Reaction 13
Menstrual Problems 12
Sleep Disorder 12
Food Sensitivity 12
Chiari Malformation 12
Postural Orthostatic Tachycardia Syndrome 11
Frequent Upper Respiratory Infections 11
More than half the cases report having ME/CFS.
We collect data on maternal and paternal health, genetic and exposure data during and prior to pregnancy. 22 of the 42 Elhers Danlos cases are the children of Vietnam veterans: 3 with Vietnam veteran mothers and 20 with Vietnam veteran fathers.
Correction: more than one-third of our EH cases report ME/CFS.
Hi Betty, thank you for you long and thoughtful reply. When I read your statistics, many questions fell into my brain. First, EDS Dx is often delayed, especially in children, but also in adults. Since the characteristics of hyper mobility are on a continuum, there can be difficulty on where one draws the line. Researchers are still arguing about this. Sometimes it takes decades to get diagnosed. The medical community thinks it is rare so the Dx gets overlooked and in fact, many doctors don’t know what to look for. There also is a ‘natural history’ where certain symptoms become less or more prevalent over time. For some odd reason, fatigue often becomes worse and POTS will become better the older a person becomes. Then there is the issue of 13 different categories of EDS but in actuality these are somewhat arbitrary with overlap between types–even types with identifiable genetic markers. For myself, I fit two types but doctors almost always call me out as having Hypermobile EDS but I could as easily fit into Classical.
And then there are the uncategorized types with rarer mutations. There is more which I won’t get into. As you can see, this all gets quite complex. I hesitated to answer you because of this, but I will say that your registry is a very helpful addition to research (and activism)! I’m also on board with the suspicion that pollutants may be part of the mix. Carry on!
Betty, I just read my answer to your comment and realized that this was my oblique way of questioning EDS statistics. Hope you caught that.
Nancy, I would like to connect with you about your work and ours on EDS. My email is betty@birthdefects.org
For anyone in Sweden, there is a brand NiQuitin Clear that is available at 7mg/24h. Maybe it is available elsewhere too? I’m thinking of trying this out.
Niquitin are a reservoir patch and can initially release nicotine a little quicker than Nicotinell – which is a matrix patch. We have noticed that not all patches suit everyone and you do need to try a couple to get what works best for you.
I think nicotine also has a vasoconstricting effect, which could help those folks who need that. Wouldn’t explain people recovering from anything, of course, just a possible decrease in fatigue and brain fog while using it.
Also, off topic: bees seem to be attracted to nicotine, and get a mental boost from it. Although, it’s complicated and not necessarily good for them either.
Another thing to try! Nick Patch, in the comments, says that cigarettes contain additional chemicals which make them more addictive. This is true! I do hope that the patch is free from these.
I do have a worry about dependence because I have genetic markers which make me prone to nicotine addiction–like my mother. She couldn’t stop smoking even while getting radiation for lung cancer. She would light up, get nauseous, snub the cigarette and then try again a while later. It was so sad to see… I’m fortunate, as on the other hand, I seem to be impervious to opioid addiction.
I mention this because in my quest for pain management, I tried fentanyl patches and having Ehlers-Danlos, the patches stopped working days before they were supposed to. The expected duration is 5 to 7 days and mine stopped working at about day 3. I attribute this to my wonky connective tissue. I even tried those tricks like heating them with a hair dryer to get them to release more chemical. I mention this because of a possible similar effect with ANY patch–nicotine included.
On another topic, I discovered; pi.ai/talk, an ‘artificial personal assistant’ who I peppered with medical questions. It was fun but I think I will have to double check some of the answers…
I had been using smokeless tobacco in my lip over 20 years ago when my me/cfs hit me, so I already had nicotine running through my system pretty much 24/7. When I got hit with cfs out of the blue one of the things I noticed was that I had become very sensitive to the effects of nicotine, definitely not parasympathetic at all, quite the opposite. I had to quit back then which was really hard to do and will never touch nicotine again. It’s also mutagenic no matter how you consume it. So it definitely didn’t help me in preventing whatever virus or trigger that caused my cfs, but I definitely don’t want to get addicted again so it’s not something I would try.
Just to note that smokeless tobacco is still tobacco which means you’re still getting exposed to dozens of carcinogenic agents plus high amounts of nicotine. That’s different from the controlled slow release of nicotine (not tobacco) found in nicotine patches.
This is an interesting article cort thank you.
I used nicotine in a recent cold/ COVID/ flu type thing. It definitely helped with cognition and mood.
One thing that concerned me was the research I’ve read that nicotine is an agent that speeds up hardening of the arteries and blockages.
This is independent of the carcinogens etc found in tabacco. nicotine itself does this apparently. Did you find any evidence contrary to this
I didn’t know that! But yes it unfortunately appears to be true. While other elements in tobacco smoke also promote atherosclerosis so does nicotine and may promote endothelial dysfunction at least in animal models.
https://pubmed.ncbi.nlm.nih.gov/28549278/
A study of smokers who used nicotine replacement therapy, on the other hand, found that it “decreased CO, oxidative stress, arterial stiffness and restored endothelial glycocalyx.” So, at least in smokers, the nicotine patch improved cardiovascular functiong *you would think stopping smoking would do that) although I did come across this
https://pubmed.ncbi.nlm.nih.gov/37828134/
I couldn’t find any information on what happens to non smokers who use the patch. I imagine that Peter Attia spoke to this in his podcast.
It’s a shame. I’ve found a good deal of relief in cognition and pots using nicotine.
But I don’t wanna damage the endothelium. I’m gonna cycle it in times if need.
One thing I’ve noticed is, like abilify, you can misjudge where your body is when many of your symptoms improve and you over exert.
For me that leads to dehydration and symptoms of migraine and even mild intracranial hypertension which is spine related so make sure you rest, keep oxygenated and use b vits etc
Unfortunately, There does not appear to be much data on the use of low-dose NRT patches in humans.
Saddly, research is muddied by the erroneous mixing of cigarettes and nicotine as if they were the same thing.
As far as I can tell so far, low doses are beneficial for the cardiovascular system. Higher doses, especially over years, could have negative effects like increased angiogenesis.
An issue would probably come from the peripheral vasoconstriction which probably is not good for skin health over years of use. However, the main arteries (like those leading to the brain and organs) are actually dilated… so bloodflow increases in the brain which has been shown in studies to be hypoperfused in LC and ME.
Like anything, there will probably be some downsides to using nicotine patches for years. However, the benefits outway the downsides and hopefully people will continue the trend of feeling better after 1 to 5 months and titrating off patches. I hope this trend continues! But it is too early to know for sure and long-term ME patients might need longer. And people with ADHD will probably decide to use it long-term if they see benefits.
The repetition of the “facts” that “Nicotine is addictive,” and Tobacco contains “dozens of carcinogens” does not prove their accuracy. Tobacco is a plant, evidently used (not abused…?) by indigenous cultures for thousands of years. The carcinogens and addictive potential in cigarettes may have been added by modern Big Tobacco companies or agribusiness.
I tried nicotine patches at the 7mg dose for around 9-10 days a few months after my long covid symptoms (primarily fatigue, brain fog, and exercise intolerance) started. I’ve never smoked or used nicotine in any form aside from this. It wasn’t a cure but it resulted in moderate improvement in brain fog and the benefit persisted after I stopped the patches. The only side effects I experienced were some sleep disruption when I wore the patches overnight (after a few days I switched to wearing them only during the day) and a bout of depression that hit a few days after stopping the patches but only lasted a couple days (maybe a withdrawal effect? not sure). I’d definitely say it’s worth trying.
I’m gobsmacked by the thoroughness of your article. Thank you. I have a question though. When you wrote: “After the 3-day low dose period, use the 7 mg patch for 7 days, stopping it after the 10th day. This is because the nicotine receptors will become temporarily desensitized and the effects will stop. (They get re-sensitized quickly.)” does that mean the patches should be used a TOTAL of 10 days?
Have a read of our recommendations and also the testimonials. Some people wear the patches for a week and others for two months solid.
We are recommending that everyone has a couple of days off after each ‘round’ of patches. A round usually lasts between 5 and 12 days.
https://linktr.ee/thenicotinetest
Thank you!
Dr. Paul Cheney treated thousands of ME/CFS patients, probably more than any other doctor. He found two biomarkers which have been largely ignored: missing fingerprints in nearly 1/3 of his patients and crimson crescents in their throats when they were at their sickest. The other biomarker, blood coagulation problems, was known to Berg, Davis and by my original diagnosing immunologist since I was put on an anticoagulant right away. It is interesting that blood coagulation problems are features of HIV, Covid and ME/CFS.
Just started reading this book. It looks interesting!
https://www.amazon.com/Plant-Teachers-Ayahuasca-Tobacco-Knowledge/dp/1608687732?fbclid=IwAR28aBh15CQNi65QMriH83K-Myafx4O7eugDMMqJTYq8ICC-zOaDOYraaRs
narby mentions nicotine patches in the above book
https://books.google.fr/books?id=ALc6EAAAQBAJ&pg=PA25&lpg=PA25&dq=jeremy+narby+nicotine+patches&source=bl&ots=iYPx5dAfDC&sig=ACfU3U33xEa51722MOwlPyUroMiH3O447A&hl=fr&sa=X&ved=2ahUKEwif0OHGo4KDAxXEVqQEHUJEBN0Q6AF6BAgVEAM#v=onepage&q=jeremy%20narby%20nicotine%20patches&f=false
Also he talks about Nicotine patches used for covid!!!
Yes the readers poll here is very encouraging
I must say that while we don’t have that many responses I’ve never seen such a high proportion of gamechangers. Usually we hardly get any in that category.
It should come as no surprise if, like me, you think neuroinflammation lies at the heart of this illness.
Jay Goldstein was close to the mark more than 30 years ago. Andrew Lloyd also (unfairly) got lots of stick from the patient community when he said about 15 years ago the issues were in the brain.
I think the poll results are probably skewed due to a link to this page/poll being posted in the nicotine test facebook group, where generally people are big proponents of the nicotine patch. But that’s not to say they are lying about it, I believe it is helping a lot of people, I just think it’s mostly helpful for long-covid people and not ME/CFS people nearly as much. Although it’s great that it’s working for sufferers of long-covid. Having ME/CFS myself, I have been on the patches a little over a month now, and I would say I am experiencing more fatigue than usual since starting, but less brain fog. So it’s kind of a wash. But I am only a month in, so the plan is to try it for another 2 or 3 weeks and see if anything improves. But my thoughts right now, not just from my own experience but also from reading other people’s accounts, is that the patches are not nearly as effective for ME/CFS or EBV as they are for long-covid, and the people that report major improvements are nearly all long-covid people, or cross-overs who have both long-covid and ME/CFS.
but at least I tolerate the patches well with little side effects. Sleeping was definitely harder when starting the patches, and fatigue is definitely worse when starting or coming off of a break from the patches. I’m hoping this second month on the patches will change my mind, though, and I will find some success, primarily with fatigue/energy levels, which have been worse (but not A LOT worse) since starting the patches.
When I developed POTS and started looking around on the web, I found information from Dr. Diana Driscoll and the help she got from nicotine. Later she moved from nicotine to something else for vagus support (which she is offering now).
What if you are quitting smoking using the patch? Is it recommended I stay on low dose nicotine patch after quitting this horrible addiction?
The nicotine patches, for the purpose of improving our me/cfs, need to be worn 24 hours a day for several weeks (plus breaks in between).
I think the reality is that no one wants to wear the patches more than they need to, but as many of us have seen a huge increase in our quality of life, we kinda feel happy that we’re feeling better, so it is what it is!
The most exciting thing though, when the nicotine patches gains more traction, the doctors/pharmacists in society will investigate further and hopefully come up with an alternative solution.
I have searched but not found 3 mg patches in US. Do you know where they can be found?
In Germany, 7 mg is the lowest, people remove half of the back cover and fix the patch with additional medical tape to obtain a 3.5 mg dose
I’ve had ME/CFS since I was 12.i started smoking at age 20. I think my symptoms improved while I was smoking. I stopped smoking and used nicotine gum for about 2 years between ages 30 and 33. When I quit all nicotine is when my symptoms increased and have continued to increase over the last 35 years.
I have just started LDA but once I have settled on a regular dose, will certainly give the nicotine patches a try.
I also use LDN, and found that to be a big help with brain fog
for me.
What is LDA? I am familiar with LDN.
Mary, it is low dose abilify or aripiprazole.
A question to everyone: When you used nicotine patches, did you use it on top of your usual existing medication, e.g. low dose naltrexone (LDN)?
The Nicotine Test FAQs suggest “avoiding anything “extra” while using the patch (Phase 1) that you don’t need…or are not used to. Especially anything that might interfere with the same nicotinic receptor (choline for example).”
I’m interested in trying other medications, too (like LDN, pyridostigmine, hydroxyzine).
So I’d be happy to hear from you whether you could use nicotine patches on top of your existing medication, in particular LDN? Thank you!
I also need any information on medication I can run by my pcp
It seems I could combine with low dose Trimipramine (for sleep).
Very useful
https://docs.google.com/document/d/1O_E1xvISGr3d-_Ontgfivdwhp_EVJtKrUH0ZdE_b_GI/edit?fbclid=IwAR1WPTSZ2bc_gv9adZNK-Lxh95w7lsjKNzfRpv4O28x3b3YSvlJhNUvVwGc
= summary by TheNicotineTest of first Demystifying Long Covid (LC) conference in Madrid, where TheNicotineTest held a poster presentation, thanks for posting!
If you peel back half the backing of a 7mg patch to use 3.5mg at a time, can you use the unused covered half the next day, or do you have to throw out the patch after using the first half?
I’ve been ill with ME for 8 years. In November I started using nicotine patches and it is the first time I’ve felt more normal since the ME started. I use flat matrix patches and I cut them to control the dose. My sweet spot seems to be around 5 mg. I have gone from 30% on the Bell scale to 60%, in 2 months. It’s a miracle.
There will probably never be a study about cutting the patches because it’s not an issue for smokers. This is an off label use. We aren’t smokers. A lot of us have simply cut the patches as needed.
I am 75. I had resigned myself to a limited existence and suddenly I find I don’t need to. It’s wonderful.
Which brand matrix patches do you use/cut? thanks
i use an inhalator, 8 sessions at 10 puffs a day =1 cartridge, since March ’23.
it cleared up severe depression from June ‘ 23 onwards plus anxiety and brainfog. not so much energy gain yet, but improved mental health is a life saver!
I am a former smoker. I was dealing with ME/CFS by the time I quit. This is just one person’s experience, but I do remember that my brain fog and fatigue amplified steadily after I quit smoking. When I learned that nicotine (not smoking) apparently benefitted Parkinson’s patients, that made perfect sense to me.
I had terrible chest pain. The study said results could be seen by the end of 3 months even after only one week of wearing the patch. I noticed a small decrease in pain about 3 days in but continued to see the pain recede over the three months. By the end of the three months I had negligible chest pain and it had been really really bad. I continue to have some chest tightness at times. It did not help my crashes at all. It did not help my other pain.
I began usage of 7mg nicotine patches on day 7 of my recent 2nd COVID infection and after 6 days of use, can report that my symptoms of both this current bout of COVID and those of Long COVID from my first infection in 2022 have been all but quashed. I do feel that some of the impact to my speech remains, but the alleviation of the brain fog and chronic fatigue which followed that 2022 infection has been immediate and profound in nature. With regard to side effects, the only effect I’ve experienced is vivid, active dreaming that is atypical from my norm. As it has only been a few days, I am remaining cautiously optimistic about the long term effects, but the immediate impact has been an incredible relief.
Congratulations Julie and thanks for sharing your experience. Good luck!
Same here, brainfog was gone after two weeks. Memory improved.
I had the active dreaming in the first week too. Really vivid.
Now I am fine. Used the lowest dose for about 3 weeks.
You say nicotine stimulates the sympathetic nervous system, later you say it stimulates the parasympathetic nervous system, which is it? Dopamine, epinephrine, norepinephrine, increased heart rate sound like sympathetic activation to me.
Why not both? The nerve cells release a mix of neurotransmitters including gaba. It probably has a immunomodulatory effect that lowers inflammation which helps sleep and pns
I have chronic costocondritus and fibromyalgia, I am at my wits end, do you think they can help?
No harm in giving it a try!
Sorry but I’ve missed something. What happens after the 10th day ?
Take a break – the blog should say how long.
Thanks Cort, asleep at the wheel as usual
Hi Cort,
I did look at the said blog and found what I needed to know, thanks.
Intrigued, I discovered that hippocampal subfield volumes were significantly different in ME/CFS as published in The National Library of medicine(J. Neurolsci July 2022).
Further investigation revealed that Nicotine may enhance hippocampal function(nih.gov).
So Nicotine patches may be worth a try.
Hallo, mein Sohn ist 25 Jahre alt und seit 12Jahren an Me Cfs erkrankt. Anfangs moderat, erkrankt, später so schwer, dass er das Haus kaum noch verlassen konnte, keine sozialen Kontakte pflegen konnte und starke Schmerzen hatte. Seit 3 Monaten geht es ihm besser. Wir stellten fest, dass die einzige Veränderung darin bestand, daß er begonnen hatte zu rauchen. Auf der Suche nach Nikotin und Me/cfs im Netz sind wir auf Ihren Blog gestoßen und haben nun zum Nikotinpflaster gewechselt. Danke!
Translation: Almut observed an improvement of her son’s severe ME coninciding with him starting to smoke cigarettes. Consequently, searching the web for information on nicotine and ME/CFS, they found this blog which led them to switch from cigarettes to nicotine patches.
I read some years ago that smokers are actually just self medicating for certain genetic deficiencies and that’s why countries like New Zealand are actually doing a disservice to those people.
It does help!
A quick report & warning on risk of overexertion from patches: In hindsight, patches were involved in 2 big crashes for me. They made it easier for me to overexert, and also seemingly improved tolerance of other stimulants like coffeine, which probably exascerbated the problem. If I try the patch again, I might try it on single days to try and improve an existing crash. Or if I try it again for a full week, do it at a time that allows me to rest during application, and not combine with coffeine or alcohol.
I have had cfs/me since 1994 I was diagnosed 1997 at john Hopkins at the same time diagnosed with syncopy,my life has been a struggle brain fog,headaches, gastritis, diffusely heterogeneous thyroid,skin problems such as eczema,lichen planus, pins and needles in skin numbness sensitivity to light,temperatures,noise the environment,massive fatigue, joint pain,glaucoma, dry mouth dry eye vertigo,constipation,diarea,the only help I’ve ever really had was from my cardiologist, after covid in 2020,2022 my symptoms got worse I have been pretty sick now for 14 months always never ending search for help I just started the nicotine patches I have noticed clearer vision if this does help I suppose it will take awhile for me I’ve been sick with cfs/me and syncopy for years I now have long covid also sleep apnea well good luck and God bless
I’m on my fourth long haul (covid 5 times starting Dec 2020) and whatever variant my kids got this time in March we are all sick two months now with unrelenting nose congestion. My 2 And 5 year old have bronchitis and developed viral asthma from it. My 10yo has unrelenting cough. I have had horrible muscle pains in shoulder neck shins and hip and loss of smell and taste and brain fog memory issues. My previous go to medicines that resolved third long haul are not working. I have been able to recover keep with combo of schisandra and reishi at night. I take phgg every day to try to protect my gut microbiome. I previously did 5 days of nicotine 7mg patch on my second long haul and it did seem to help. I am going to try 14mg this time.
My husband had PD-5 programme about 4 months ago. Tremors in his hands and jaw are gone. It doesn’t make the Parkinson’s go away but it did give him better quality of life. we got the treatment from natural herbs centre
I’m on my 3rd day. 1st day I got energy and actually was quite hyper. Hubbie noticed improvement and said I was massively more motivated. Next day not quite so good and was very tired but ok. Now on my 3rd day, I woke up and had aches and pains, including breast pain. Felt very tired. I was using 7mg and not using at night. Not sure whether to continue but will probabaly try halving the dose. Would like to know if anyone got these side effects and pushed through to improvement.
I’ve been looking for information about the relationship of someone with ME/CFS and/or Fibromyalgia using nicotine patches to quit smoking and the short Vs long-term effects of this on their condition.
I was happy to find this article, but it is the complete opposite to what I expected.
I quit smoking 61 days ago and have been using NiQuitin nicotine patches, starting with their pre-quit patches, and moving through steps 1, 2 & 3. I have also been cutting step 3 patches in half and now quarters, to help tapper myself off better instead of the abrupt 7mg to 0mg.
Personally, all I have found from using these patches, is that my fatigue levels have significantly worsened since starting the patches and as I have progressed through the stages through the last 61 days, my fatigue has worsened still.
I was hoping to find an article that would somewhat explain if this is a short term problem of nicotine withdrawl (that my body will adjust to in the coming months) Vs a long-term problem of worsened fatigue (which would suggest that smoking (roughly) 15 hand rolled cigarettes a day actually increased / maintained higher energy levels in my body).
I guess I’ll see how I feel in the next few months. I certainly don’t plan to begin smoking again, but this worsening of fatigue / significant drop in energy levels is horrible and it’s stopping me from doing almost everything now.
As an extra note, my memory / concentration has also worsened since beginning the patches.
I was recently mostly cured of burgeoning Long Covid from two days of double-dose ivermectin. I had found a study from 2020 saying that dosage worked for most people with Long Covid. (I didn’t wait for 30, or is it 60 days after my infection for the LC dx to be official, but it fit the description, was pretty bad, and was not improving). I already have long-term Lyme/CFS/fibro.
Dr. Teitelbaum’s Long Covid book also recommends ivermectin but is vague, just saying to increase the dose if the ivm helps. The FLCCC LC protocol says to do a ten-day trial of higher-dose ivm and their guidelines for dosage are higher to begin with than the typical recommended dose.
It has been over two weeks since doing it and most symptoms are still gone (at first they completely went away, but some came back). I may do another two-day double-dose ivm round, or try nic patches. I was on the typical single-dose ivm during my covid infection but not sure if it helped. I read ivm goes out of the bloodstream in a few days and out of the gut in 13 days.
Congratulations and thanks for sharing!
I was just starting my 4th bout of Long Covid when I tried the patch.
My first LC lasted 11 months the next two three months each. My wife caught covid four weeks back and then I followed days later. Naturally, I was not looking forward to three more months of LC. I was spiralling into the LC fog and darkness and had had a few very bad days. This was a week post the actual covid symptoms finished.
LC affects my brain, brain fog, exercise-induced fatigue, and light and sound sensitivity. Also conversations wore me out. anything that made my brain work. Interestingly each time the LC lifted there was a recognisable pattern of fog lift and return to normal. Once lifted it remained lifted until the next dose of the virus.
I am on day six of the patch trial now and yes it’s a game changer. the fog has lifted in the same way as in the past. I will finish the seventh patch and stop. But based on my past experiences I’m happy even now to say I have dodged a bullet. Importantly for me I was thinking that each time I got even the mildest case (3 of the 4 covid infections were very mild) I would be getting a LC response. Now I have had a great result with this, a bleek future has turned to a treatment method that can mean a short recovery period.
Great to hear! Continued good luck with it.
Yes been active and no sign of LC symptoms after a few weeks
So happy. Russell
Dr Ardis has recommended certain brands that he researched and consider “clean” or clears then the other companies.
I am new to the patch and am trying it for chronic lyme. I do believe it has helped my symptoms a lot..i had more energy from the very first day. Doing the hard chores that i had neglected for 2 years and feeling good.
After 10 days, i stopped for 2 and had a ton of pain, so i am back on it…will just see how it goes.
I was diagnosed with Covid at an Urgent Care facility in mid-February 2024. I was 87 years old and had a very bad case, with my oxygen level at 88 to 89. With a fever of 104, I was as weak as a newborn kitten. A Church member informed me where I could order Ivermectin and Hydroxxycholychloroquine over the Internet. I received my order in two days and started taking both immediately. In 24 hours my fever was gone. In three days I felt normal, although I still felt weakness and a persistent cough for another three weeks. By April all symptoms were gone, except a good deal of brain fog which I still experience. I will consider the nicotine patch. But the Ivermectin and Hydroxychoroquine worked beautifully. I took the Ivermectin for 15 days and the other for 7 days.
Congratulations on getting better. Maybe you were one of those Ivermectin worked for; maybe you would have gotten better anyway – who knows?
In the interest of providing some study data – the study which found Ivermectin helpful was retracted
https://pubmed.ncbi.nlm.nih.gov/35135310/
And other large, rigorously done studies did not find Ivermectin conferred benefit and some have found that ivermectin/hydroxychoroquinine made things worse and can produce some severe side effects.
https://pubmed.ncbi.nlm.nih.gov/39457519/
Thank you for your kind reply. I cannot comment on the data that you quote. I can only confirm that Ivermectin and Hydroxychloroquine not only worked immediately for me, but they likely saved my life. I’m so convinced of that fact that I keep a good supply of both on hand. A good number of people testified on the Dr. Mercola website that Ivermectin worked for them. BIg Pharma, with it billions, obviously has the resources to flood the Internet with negative propaganda, even from what might seem to be impressive sources. against this miracle in a pill.
Thanks for sharing your experience! That’s what it’s all about 🙂
I have had exercise intolerance and orthostatic intolerance on and off for the last 7 years and it did get much worse during covid,recently I did 2 weeks of the nicotine patch, I felt a 5x increase in energy and mental clarity, and my balance issues were 90% gone now my I tried a different company patches and my issues are mostly back, does it mean that my body got used to it? Does anyone have any ideas? Thanks!
I wonder if the formulations are different including the different compounds used to stick the patch on?
Thanks to an article I read here on Health Rising, I decided to try the nicotine patch therapy. So for the past year or so I have been wearing half of a 7mg patch (I don’t cut it, I just cut the protective covering so that only 1/2 of the patch shows at once). I cannot believe the results!
I am not cured—I didn’t expect that—and I do have days and even periods of “down time,” but that time is usually a lot less than I would have experienced had I not used the patch, and my “good days” are extremely good, not just being able to be out of bed, but actually being productive and having a social life like I used to! I also experience less crashes after a very busy day or series of days. I am just amazed at the results!
I do wonder by something in this article if I am supposed to stop wearing the patch and still see results? I’m afraid not to wear it!
Nicotine is in vegetables like peppers, celery, aubergines and others… I have never heaed of anyone being addicted to these vegetables… the addiction is not to nicotine but to the 1000 and more chemicals that the they put in cigarettes to make them addictive. Nicotine is actually beneficial and they have started to realise that… But hey, everything that is natural and beneficial gets shot down because it cannot make money …
somewhere on the phone you these will also help people who’ve lost their taste and smell.
IS THAT THRUE PLEASE???????????
I have heard that the smell does come back, but I have not tried it myself yet.
I am looking for all natural patches, I cannot find a single brand online. I did find an all natural gum 3mg, assuming that’s as good as a patch? Or is the time release a huge factor? Thanks
I have Dermatomyositis for 5 years with muscle weakness all over my body including my organs.
I want to know if the medications I take will be able to handle Nicotine patches?
I take is steroids, 3 high blood pressure, anxiety and depression, and 2 different insulins.
Of course I’ll watch my symptoms.
Nicotine is NOT ADDICTIVE . ANYBODY WHO DOES TEN MINUTES OF RESEARCH WILL DISCOVER THAT THE TABACCO INDUSTRY ADDS 2 CHEMICALS TO THE TABACCO TO MAKE IT ADDICTIVE! TALK TO AI- GOOGLE – IN BOOKS.
ALL NIGHTSHADE VEGETABLES HAVE NICOTINE IN THEM AND NOBODY IS ADDICTED TO THEM. YOU’RE ONLY FOOLING THE FEBILE MINDED
Hi Team
I was told to take
Nicotine patch – PROTOCOL-
But I don’t know where to find this one ?
Can you help me to find PROTOCOL – Nicotine Patch please
Search for “84-The-Dr-Ardis-Show-How-To-Use-Nicotine-Protocol.pdf”
Hope this helps, if you haven’t found one.
I know this is an old post, but much info has come out about a Nicotine protocol for many health issues in the past couple years, including long covid and ME/CFS.
Give this a watch for a wealth of knowledge from Dr. Ardis.
https://laban.substack.com/p/dr-bryan-ardis-the-truth-about-nicotine?r=9i22k&utm_medium=ios&utm_campaign=audio-player
Also, update your article, as Nicotine is not found to be addictive, its the 35 patented chemicals in the cigarettes that are addictive. Big tobacco did several studies, millions of pages, showing Nicotine by itself is not addictive.
Really interesting read—this is one of the more thought-provoking angles I’ve seen on nicotine beyond its traditional context. The idea that low-dose, slow-release nicotine (like patches) could potentially influence the cholinergic system and inflammation pathways is fascinating, especially given how complex conditions like long COVID and fibromyalgia are.
That said, it’s clear we’re still very early in understanding this. The anecdotal reports are encouraging, but as mentioned, larger and more controlled studies will be key before drawing firm conclusions.
From a broader perspective, it also highlights how delivery method matters—nicotine in controlled formats is very different from smoking. Definitely an area worth watching as more research develops.
Great work bringing attention to emerging ideas like this!
— Team Vapeaah (UK)