


Want to listen to the blog? Thanks to Geoff for providing a narration of it. 🙂
The multiple sclerosis drug Copaxone (glatiramer acetate) is back in the chronic fatigue syndrome (ME/CFS) news. Health Rising first reported that Copaxone helped some ME/CFS patients back in 2015, and Jarred Younger included it on his list of possible drugs for ME/CFS and fibromyalgia (FM) anti-neuroinflammation drugs way back in 2014. Ron Davis reported that Copaxone made ME/CFS patients’ cells behave normally during the nanoneedle stress test in 2019.
In “Catalytic Antibodies May Contribute to Demyelination in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome“, Copaxone has moved out of the purely anecdotal realm. We’re getting some solid data on the Copaxone multiple sclerosis/ ME/CFS connection, courtesy of Ron Davis and Michael Jensen and their colleagues at Stanford, the Open Medicine Foundation, and most importantly, the Vinod Khosla Foundation.
We still don’t know if Copaxone works in ME/CFS, but a pathway has been formed that suggests it might and could lead (one might hope!) to clinical trials at some point.
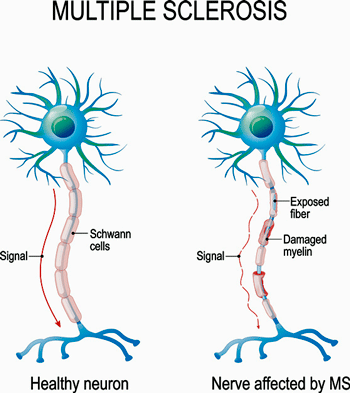
The kind of overt demyelination found in MS is not found in ME/CFS. Lower levels of demyelination are possible, however.
Multiple Sclerosis and Chronic Fatigue Syndrome (ME/CFS)
The MS ME/CFS connection has gotten even more intriguing. Both diseases feature high levels of mysterious fatigue, both can produce remitting/relapsing phases, both mostly affect women, and both are often triggered by an Epstein-Barr virus infection (ME/CFS, often immediately and MS, often decades later.)
They also differ. MS is a severe demyelinating disease where damage to the protective myelin sheath covering the nerves in the brain impedes nervous system signals. Hints that demyelination is taking place in ME/CFS have cropped up from time to time, but nothing like the overt structural changes found in MS are present in ME/CFS. Plus, one study suggested while fatigue is high in MS – perhaps even higher than that found in ME/CFS – post-exertional malaise is rare in MS.
In MS, a protein called MBP, which protects the myelin sheath, leaves the sheath and enters into what constitutes “no man’s land” for it – the bloodstream and cerebral spinal fluid – where it’s now perceived as a threat and sparks an autoimmune response. That autoimmune response then targets the myelin sheath.
Similar to the ways ships protect themselves by firing off “chaff” to attract missiles to them, Copaxone appears to act as a mimic that causes the immune system to attack it rather than the myelin sheaths of the nerves.

THE GIST
- Health Rising first reported that the multiple sclerosis drug Copaxone helped some ME/CFS patients back in 2015, and Jarred Younger included it on his list of possible drugs for ME/CFS and fibromyalgia (FM) anti-neuroinflammation drugs way back in 2014. It’s only now, though, that we have some solid evidence suggesting it might work.
- Both ME/CFS and MS feature high levels of mysterious fatigue, both can produce remitting/relapsing phases, both mostly affect women, and both are often triggered by an Epstein-Barr virus infection (ME/CFS, often immediately; and MS, often decades later.)
- They also differ. None of the overt demyelination found in MS has been found in ME/CFS. Some hints of demyelination have been found in ME/CFS, though, and microstructural damage has been found in the brains of ME/CFS and MS as well as fibromyalgia and long COVID.
- That’s intriguing as recent studies suggest that the fatigue in MS – which may be even stronger than that found in ME/CFS – is caused by microstructural problems that occur early in the illness. It’s possible, then, that similar microstructural problems could produce fatigue in ME/CFS. (Note that one study did not find evidence of post-exertional malaise in MS).
- Copaxone draws away the antibodies that attack the myelin sheaths covering the nerves in multiple sclerosis. The fact that several ME/CFS patients reported benefits from Copaxone made it of interest to Ron Davis at Stanford.
- The Stanford researchers led by Ron Davis and Michael Jensen first assessed whether higher levels of the antibodies that attack the nerves in MS were present in ME/CFS and found that they were in about half the ME/CFS patients.
- Next, they determined that the antibodies found in ME/CFS were similar to those found in MS, and that Copaxone was able to inhibit them in ME/CFS in the lab.
- They proposed that these antibodies and others known to attack proteins be further assessed in ME/CFS. Plus, Davis proposed that given the similarities between the ME/CFS and MS, other MS drugs should be trialed in ME/CFS.
- He proposed that similar pathways may be at work in ME/CFS and MS. Indeed, several MS fatigue studies directly referred to findings in ME/CFS to help explain the fatigue in MS.
- The study was limited by its small size and the emphasis on laboratory work. It suggests that Copaxone is doing the same thing in ME/CFS as it does in MS, but we won’t know that absent a clinical trial. Time will tell if this study leads to a Copaxone clinical trial in ME/CFS, but it does appear to set the stage for one.
- In the meantime, Ron Davis and Janet Dafoe would love to hear the experiences of anyone with ME/CFS who has tried Copaxone. You can email the Open Medicine Foundation or Janet at janet.dafoe@gmail.com
The Study
With some ME/CFS patients providing anecdotal evidence that Copaxone – which targets the autoimmune processes in MS – may be helpful, the search was on to see if the abzymes (antibody + enzyme) (ABS) that Copaxone targets were present in ME/CFS.
If I have it correctly, the Stanford researchers assessed the ability of the antibodies to MBP (called ABS) in the plasma of 19 ME/CFS and 19 HC patients to digest (destroy) MBP. They found that about half the ME/CFS patients’ samples damaged large amounts of MBP, while only 5% of the healthy controls did.
Next, they took the antibodies from the ME/CFS patients’ plasma, determined if they could attack the myelin sheath, and found they could. That suggested that demyelination – a breakdown of the protective sheath covering the nerves – could be happening in ME/CFS as well.
Then, they determined whether Copaxone was able to prevent MBP from being attacked and degraded in the ME/CFS patients’ plasma – and to a significant extent (68-80%), it was. That made it clear that the same ABS antibodies are found in both MS and ME/CFS, and that the drug operated normally in ME/CFS patients.
Finding the same antibodies in ME/CFS, demonstrating that they had the potential to do the same thing in ME/CFS, and that Copaxone could stop that process in the lab, seemed to potentially set the stage for a Copaxone trial in ME/CFS.
Next Steps
The authors argued that given the broad spectrum of overlapping pathologies found in MS, other autoimmune diseases and ME/CFS and long COVID, that demyelination, particularly in ME/CFS patients experiencing nerve pain and muscle weakness, should be considered.
They recommended that studies to track the “catalytic activity” (i.e., the ability of the ABS (the antibodyzymes in question) to break down myelin in ME/CFS) should be assessed over time. Levels of ABS in the cerebral spinal fluid – typically a richer source of these antibodies – should be assessed as well, and so should other “proteolytic” antibodies – antibodies that break down proteins.
They closed the paper by stating that an assay that tracks MBP breakdown by these ABS in ME/CFS patients may help “better diagnose and treat patients in the early stages of demyelination”. From what I gathered, that test is only available in a research setting, however.
During a talk, Ron said that one next step was determining if MS treatments – not just Copaxone but other MS drugs as well – are helpful in ME/CFS.
He noted that the study suggests that some people could have an autoimmune disease like MS in addition to ME/CFS that might be treatable. Then Ron said something interesting – he thought that because ME/CFS affects major control circuits that play a role in other diseases, treatments that help other diseases might work in ME/CFS.
This makes perfect sense. While Ron noted that ME/CFS is extremely complicated, it’s not as isolated as we might think. The basal ganglia alterations in ME/CFS look like those found in hepatitis C IFN-treated patients and MS. The autonomic nervous system issues (high fight/flight) are present in many other chronic illnesses. A similar kind of exercise intolerance may be found in rheumatoid arthritis. Jarred Younger is certain that neuroinflammation is present in ME/CFS, and neuroinflammation pervades neurological diseases.
The reason really effective treatments are hard to come by in ME/CFS may have more to do with funding than because ME/CFS is some sort of untreatable, undecipherable disease. MS is no walk in the park, but it gets ample funding, and the FDA has approved over 25 drugs to treat it. Because bits and pieces of ME/CFS are found in many other diseases, drugs that affect those aspects of ME/CFS could very well help.
The study had significant limitations. It was small and because much of it was done in the lab in test tubes, we don’t know that this antibody-triggered demyelination is actually occurring in ME/CFS. It presents a nice starting point, though, and we will see how it evolves.
The Microstructural Fatigue Diseases?
The fatigue in MS is curious. It usually shows up before neurological symptoms do, is often described as the worst symptom MS patients experience, and, most intriguing of all, does not track with the degree of overt demyelination or nerve damage found. A recent study suggests that it may, however, track with microstructural changes – and here we have another potential opening for ME/CFS.
Using advanced MRI techniques, the 2024 MS study found that small microstructural changes that occurred very early in the disease process were associated with cognitive fatigue. The study reported:
“brain microstructure within normal appearing tissues is already altered in the very early stages of the disease. Moreover, additional microstructure alterations (e.g. diffuse and widespread demyelination or axonal degeneration) in pwMS may lead to disease-specific complaint of cognitive fatigue.”
Could similar microstructural changes be causing similar symptoms in ME/CFS? Microstructural changes to the brainstem, the insula, and a major communication track (superior longitudinal fasciculus) have been found in ME/CFS. Microstructural damage has also been found in fibromyalgia and several times in long COVID as well.
In fact, one long-COVID microstructural study, “Brain microstructural changes and fatigue after COVID-19”, went straight to the ME/CFS literature to explain what they’d found. They focused on the impaired “remyelination”, abnormal connectivity, reduced conduction in the brainstems, insufficient myelination of motor cortex tracts, and the basal ganglia findings in ME/CFS to explain the fatigue in both diseases.
More possible connections showed up in an MS fatigue study which proposed that the basal ganglia – a prime candidate in ME/CFS and FM – was “the fatigue center” in MS. That study also cited ME/CFS findings to support their hypothesis.
Plus, each of the four hypotheses regarding fatigue in MS from a 2015 review article has been raised for ME/CFS as well. They included:
- Compensation – The loss of signal strength between brain regions causes other parts of the brain to jump in to compensate, reducing efficiency and increasing metabolic needs – producing early fatigue.
- Brain stem damage impairs the activation of the cerebral cortex which is connected to two brain organs – the thalamus and basal ganglia involved in alertness, the autonomic nervous system and movement.
- Motor region – Lesions in the motor cortex region are associated with quick fatigability in MS during physical exercises.
- HPA Axis – Lesions in the hypothalamus in MS patients affect circadian and endocrine factors. The disruption of the circadian rhythm can impact sleep – causing fatigue, and endocrine factors regulate metabolic and immune processes.
The physical problems caused by nerve damage found in MS do not occur in ME/CFS, but it’s possible that the fatigue found in both diseases could be similar. If so, a drug like Copaxone that helps with fatigue in MS might help with the fatigue in ME/CFS.
One way problems with the microstructure of the brain could affect ME/CFS patients is by impairing the connectivity between different brain regions.
Bad Connections

Frayed wires caused by demyelination could be contributing to the connectivity findings in ME/CFS.
Demyelination could also contribute to the “connectivity” problems frequently found in ME/CFS. Connectivity problems occur when parts of the brain aren’t communicating properly with each other.
For instance, in 2018, Staud found during a cognitive exercise test that the connections between the brain regions associated with working memory, sensory function, and motor function (there’s the motor cortex again) broke down in people with ME/CFS. Numerous brain regions demonstrated opposite patterns of connectivity in the ME/CFS patients relative to those found in the healthy controls.
- healthy controls showed increased functional connectivity to the right-lateralized middle temporal gyrus, superior lateral occipital cortex, and angular gyrus; ME/CFS patients showed decreased connectivity
- healthy controls showed increased coherence (communication) between the right-lateralized middle temporal gyrus, superior lateral occipital cortex, and angular gyrus; ME/CFS patients showed decreased coherence
- healthy controls showed increased connectivity between the hippocampus and right superior parietal lobule; ME/CFS patients showed decreased connectivity
- healthy controls showed increased connectivity to the left-lateralized pallidum, thalamus, putamen, caudate, and nucleus accumbens; ME/CFS patients showed decreased connectivity.
The authors proposed that the generally increased connectivity/coherence seen in the healthy controls reflected their brains’ ability to bring in new brain regions to help out as the fatiguing task wore on. The inability of ME/CFS patients’ brains to tap more resources, in turn produced their fatigue.
Back to Copaxone
Copaxone is one of the few drugs able to treat fatigue in MS, and anecdotal reports suggest it may be able to do the same in ME/CFS. Plus, as noted earlier, Copaxone was able to restore ME/CFS patients’ cells to normal functioning when they are put under stress using the nanoneedle.
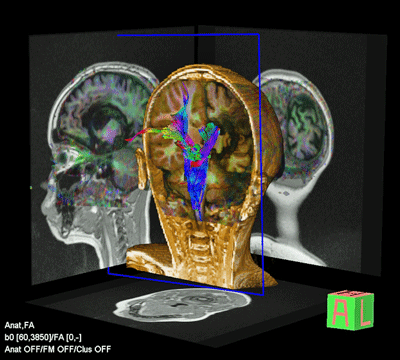
As brain imaging technology improves, we will learn much more about what’s happening in the brains of ME/CFS patients. This is from a diffusion tensor scan which can pick up microstructural changes.
As the technology to assess the microstructural integrity of the brain improves, and as it’s brought to bear on ME/CFS, FM, and long COVID, it’s going to be fascinating to see what it shows. To reiterate, none of these diseases demonstrate the kind of overt damage to the myelin sheaths found in MS – and that’s a good thing. Repairing that kind of damage may be impossible, but repairing damage to the microstructure might be another story. When asked if Copaxone could repair the damage, Davis said he didn’t know – and the best thing would be to try to avoid that.
When asked if these results would show up on a standard MRI, Davis said he wasn’t sure, but they thought that the various spots on an ME/CFS patients MRIs indicate demyelination. I looked it up, and they do. Increased white matter hyperintensities have been found at times in ME/CFS and could indicate that myelin degradation may have occurred.
Ron noted that it’s possible that the amount of antibody in ME/CFS is not as high as in MS, and therefore, not as much damage is occurring. He also poo-pooed the idea that one couldn’t have MS and ME/CFS at the same time. He also noted that the MBP antibody is not a diagnostic test for MS.
They would love to hear the experiences of anyone who has tried this approach. You can email the Open Medicine Foundation or Janet at janet.dafoe@gmail.com
Please Support Health Rising and Keep the Information Flowing


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


Interesting. Ron’s work always is. But convincing? i am not so sure. He always strikes me as incredibly intelligent, but that can sometimes be a hindrance.
The positive effect of Copaxone could be attributed to its immunomodulatory and neuroprotective effects. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9099707/
MBP antibodies are not used for an MS diagnosis, as they are not considered specific enough. There is no autoantibody diagnostic test for MS till today.
“Here we demonstrate that sera from both MS patients and healthy controls contained MBP-reactive IgM and IgG antibodies, and that the amount of these antibodies did not differ significantly between the two groups” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2753924/
The important take away would be to trial MS treatments, as several have shown positive effects.
Wow that’s fascinating! I would put my money on copaxone being beneficial for ME/CFS based on those broader immunomodulatory effects, rather than the mechanisms described in Cort’s article.
This may also explain the (small) white matter spots abnormalities found in some ME patients MRI. Professor Klimas thinks these may indicate inflammation in ME patients. But it can also be a result of reduced blood flow in the brain. So maybe you can see if they will disappeare when these patiënts use copaxone.
Wow! I was told by a neurologist 12 years ago he didn’t know what those tiny white spots were in my brain. Now I’m diagnosed with ME/cfs and fibromyalgia. I sure hope medicine figures this out. Folks are suffering.
I’m more confused than ever. Lol
How is it that me/cfs folks pull completely out of this disease by either changing to a radically new diet, moving out of one home, into a new home, moving to a different country where the air is cleaner, getting away from mold, or simply using the power of their brain and think themselves out of this disease?
I for one, will probably never be able to hold down employment, but ive made leaps and bounds considering I was once like whitney dafoe albeit its taken decades of trial and error.
It also could be that I’ve been sick for so long that I don’t know what normal feels like
There must be a lot of subsets of this illness. I for one believe and was just told by my nephrologist, that the tetracycline I took for 1.5 years straight as a teenager did this to me.im 64.
If anyone has read the copy of,now a very old print of
“The yeast connection” by dr.william crook
Wow I didn’t know about the tetracycline connection. I took a lot of it while in elementary school. (Maybe in kindergarten too without me knowing.) So much that it made my teeth yellow that can’t be whitened. But I didn’t take it continuously. I’m going to be 62 soon and I’ve been bedridden for years. I’ve no official diagnosis and consider myself having FM instead of ME. But who’s certain these two are not the same (or their subsets)?
Since there is no diagnostic test for ME, and since it seems that multiple agents can trigger the disease, and since ME patients conditions range from mild to very severe, it makes sense to me that there is no “one size fits all” answer.
Confusing? For sure. But also very disappointing when something that seems to have worked for someone else doesn’t work for “me.”
My mother, who has MS, greatly slowed down the progression of her disease by changing her diet and part of that change came from reading the Yeast Connection.
My sister, who has CIRS, has gone to drastic measures to live chemical free, mold free, organic foods, etc., etc. She also is not healed.
I have 2 friends with ME who were very gung ho about the “brain training” programs, but neither one is helped yet.
I have tried a variety of things for my own ME over the past 25 years. Some have helped more than others, and I didn’t fall into the severe category until about 7 years ago. I am super happy for the various things that are keeping me in the moderately severe range, but I haven’t been able to be out of bed for more than 20 minutes at once (on good days, usually more like 3-5 minutes) for a very long time.
All that said, I’m happy about every single possible treatment option that could help any one of us — whether just a little or quite a lot or totally healed. And I’m so happy you have experienced so much improvement.
A big thank you to everyone who researches on our behalf!
Brain Vains..
Those brain Vains…
And afcorese everything else…
Thats usually because of an incorrect diagnosis using an old criteria. Very few people with ‘Post Exertional Malaise’ PEM more than 3 years will recover. Some do, but not many. And yes there’s subgroups. I and some researchers believe ME/CFS is the result of one of several possible causes. i.e. Cell Danger Response CDR (Robert Naviaux) It’s the sickness protective state the body goes into when under threat. So will be there until the threat is gone. So if it’s viral persistence, and that gets cleared CDR will turn off. Mould intolerance will be the same. However if the threat is being caused by autoimmunity then you won’t see a recovery without that being treated. I believe that subset to be the biggest
This is a brilliant hypothesis and actually makes sense to me in a lot of ways.
Normal? No idea what that’s like either as I’m 6 decades in.
I haven’t read the Yeast Connection book but my mother had yeast allergies & so do I. Odd thing with me. In the spring & summer my ME/CFS goes into remission.
The rain sets off my symptoms. I’m bed & couch bound when it rains. On a sunny day, I could be working (a bit) in the yard or on a small hike. I’m in Seattle (of all places). It takes energy to move away. I’m all packed, but that’s another story.
Let’s all pray for answers & a cure…the clock is ticking 🙁
Somebody, send ron davis a copy of
“the yeast connection”
I suggest,Barbara,to get on vitamin d?
Have you had your levels tested?
Go get out and lie in the sun,when it’s available.
I look at vancouver and wonder to myself, “how the heck can folks live in that climate with almost zero sun for many days on end! I could never do that
Yes, Vitamin D Daily. I’m pretty much surrounded by trees at home, but IF there is even a remote chance of sun filtering through, I’m out in it. I’m ONLY here because I was born and raised. This is the absolute worst place I can live (except for Alaska!) Still looking for a little Oasis somewhere!
Rain releases a lot of mould and fungi into the air, from when it lands on plants and dirt, dead leaves and twigs etc. I bought lab grade Hepa filter, that traps mould spores. I haven’t noticed much difference. However I probably don’t have a mould issue. But I’d recommend getting a high grade filter because you are worsening when it’s raining.
Probably a bit of Mast cell activation happening when inhaling mould spores too. So maybe try an antihistamine when it starts raining
Good luck
So how did you improve, buckey? I hear lots of stories from mild to moderate patients, but I’m always interested to hear what people who’ve been truly bedbound and down the bottom end of severe to very severe have done, that they felt helped them improve. Would you share anything with us?
OK,this could be long…lol
I got sick in a motel room I was living in while going to welding community College in 1981.Come October, mice were infiltrating and I trapped them(clue #1)
Also,the water was well water(clue #2)
Prior to this at the age of 14/15 I was put on tetracycline for 1.5 years straight for severe acne on my upper back.it never put a dent in my acne one bit so my mother said to the treating dr., at intervals..”its not helping”..the dr. Just kept saying…” just keep taking it” this at a time when they handed that crap out like candy at Halloween.you need to understand the Canadian medical system.Yes free health care but everything gets billed to the govt.think now for the reason he wanted me to stay on tetracycline cha ching$$
In that motel room I got really sick ,vomiting,gushing diarrhea.just two weeks later I developed an ulcer that later healed on its own. Well,I start to develope slight weird vague symptoms but still seemed to truck along.
Fast forward to 1993 and things are getting a lot worse, so much so that I write to a gastroenteritis that it feels like something is growing inside me and that if I don’t get help soon I’m going to loose my job.
I move to a new to us home and begin to sand and roll on polyurethane hardwood floor finish.i close all the windows because a dust storm is brewing outside.the fumes from the polyurethane are now building up and I begin to get sick…really sick…but..recall that I had vague symptoms for yrs earlier. I’m now living in a tent outside because when I enter the house I now break out in a rash from head to toe and feel my health decline in litterally seconds upon going into the home.i now herniated a disc in my lower back at work.
I get a call from my neurologist asking if my back is getting any better…I stayed no.
He places me in hospital for 10 days bedrest. For whatever reason I had zero appetite so begin to fast.On the 5th day of fasting, I feel my body begin to heal.i pull out my pic line and walk out of hospital in zero pain. I arrive home and in less than a week my skin begins to bleed tiny little spots of blood all over my chest and stomach which, in about 6 days, later turn into moles. And now i feel my immune system jambed up once again.ive been stuck ever since.Just weird
Fast forward to just prior to covid I take my first dose of horse ivermectin from the farm store (12$)
I become itchy all over and tiny white crusty stuff comes out onto my skin all over my body
The directions state..” if your horse become itchy, it’s from the mosquitoe infection filaris(spelling?) I feel somewhat better ever since that one single dose of ivermectin.subsiquent doses do absolutely nothing.
I buy the book from dr Raymond Perrin and begin to do the exercises…nothing happens for many weeks but because I do the perrin point test and get a positive
SCREAM…I keep doing the skin brushing….my 2 inch lumps of my lymph system now are down to one inch…6 months later they are now I’d say less than 1/4inch and some days gone.
I do still have PTSD as I went on one Hellova ride when all hell broke loose in 1993, I didn’t think a human could get that sick…as I say, just like Whiteny dafoe.pain so severe and such a swollen brain that on several occasions wanted to go get the gun and end it all as so many others have done in the past
Oh I’m still tired and as springtime here in saskatchewan, Canada🇨🇦 arrives, the snow mold hits me. I never feel well until middle of June, then the heat comes on in September and down I go again, but not near to what I once was. I still don’t hold a job but. This isn’t a cure but I now have a life. I’ve seen a lot of trauma in my younger days🤷♂️. I’ve also been injected with vaccines that contain mercury🤷♂️
They tell us mercury is one of the most toxic metals, yet inject it into us🤷♂️.I failed gr. 7 and 9 and dropped out so that’s why my suspicion if the mercury🤷♂️.these vaccines are meant to cause the immune system to react, well, in 1993 I had one hellova reaction. I continue to detox
Just to add to the above…just prior to the pandemic, I call my gp/natropath/Chinese medicine guy and ask him about ivermectin,and if it’s something i should try…he states….”I have to ask if you are recording me”…I say no…he proceeds to tell me that a lady with stage 4 cancer comes and asks him to monitor her liver while on ivermectin. He says she cured her stage 4 cancer in 6 months of using ivermectin!!!
@Buckey,
Right, in the 1990s a co-workers husband had stage 4 cancer. Seattle doctors couldn’t treat him. It was too late they said.
The couple went to Mexico for treatment & by the time he got back to the United States he was cancer free.
I was very severe for seven years…and what helped me was a naturopath treating me for yeast, viruses..and tons of supplements and colonics. I was super toxic from leaky gut, and colonics twice a month for four months got me able to start walking again. Once I got rid of the load of toxins..I was able to start moving around again. I still do some colemas though to control the toxicity. I have been helped by Dr. Cheney as well..but it was the colonics, and strong nutritional program and glutathion/atp shots that got me out of bed.
The last section of our 2022 review paper on the putative role of glial cells in the pathobiology of ME/CFS sports the following heading:
“Broken Connections – May ME/CFS Be a Case of “Connectivity Hub Failure”?
It pretty much summarizes the evidence that a central problem of the ME/CFS brain is ineffective or even paradoxical communication between brain areas involved in the physiological stress response. It also refers to recent evidence that oligodendrocytes (a class of glial cells responsible for maintaining the insulating layer around the axons of nerve cells) may be dysfunctional in ME/CFS:
https://www.frontiersin.org/articles/10.3389/fncel.2022.888232/full
It is a very good idea to probe into therapies that could bear on these processes! Thank you Cort for this amazing summary!
I am 30 years severelly ill. i have followed the research since i had a computer. it is unbelievable, again such a tiny study. I would advice OMF to do a few really large studys instead of spreading the few dollars they have over so many studys. long time ago they said, can not remember who, we are the lost generation. over decades of i only read, listened to falls promises an fals hope. until i really can no more. i would say it is a typical ME/cfs study (no money). the only large study is the decodeME study, also now in i thought Finland, the US, etc (can not remember. and from the decodeME study they said on geneteics they where 10 years behind in comparison to other deseases. I am really one of the so so many lost generations.
konijin – You are not lost to us! We care about you!
We do – sending you love Konijn!
thank you, that is sweet!
thank you, that is sweet! but if the boddy can no more and the circumstances in witch i live…
On the downside it’s yet another small study; on the upside it presents more potential leads and the link to a well-studied disease is encouraging.
One reason I’ve put so much hope into the RECOVER Initiative – is that it does have money lot and it has a commitment to produce solid results and not leave things dangling. So far that hasn’t worked out so well. The RECOVER story is not over, however.
With no signs that the NIH is going to do anything more to support this disease I’m still hoping that long COVID research outside the NIH is going to produce core findings that will translate to ME/CFS. The long COVID researchers will do the work and we will try and find a way to apply it. Since pushing for more ME/CFS funding at the NIH hasn’t worked in 30 years (it still might of course) I believe we need to keep pushing for more funding for long COVID.
Despite the complexity inherent in these diseases I still believe that when you get right down to it they will have similar core issues. That’s why we have to push for an NIH Institute for postviral diseases. I don’t think we’re going to get anywhere with the NIH until that happens.
I would love to see that happen, I hope it does! Cort do you think us all signing a petition and all the ME/CFS, LC and other post-viral charities promoting the same petition would have any impact? Or is there another way? I know you may not have the answer but you have so much experience so I figured you may have the best instinct for what could work! Sometimes it’s hard to know how to have an impact since we’re all physically isolated but we’re such a strong community and our power is in how we can band together since there are so many, many millions of us!
Hi Chips. Solve ME’s advocacy week is going to focus on this and other efforts are underway. The exciting thing to me is that the ME/CFS, Post Lyme, Long COVID and other disease communities realize that this is the next necessary step for all of us. Despite the RECOVER funding Long COVID like ME/CFS still doesn’t have a home at the NIH. I will present the opportunities as I find them – and if anyone sees them please let me know.
The road to achieve this is through Congress. The NIH won’t do it on their own.
I agree, we have to unite, band together & sing…
That was a typo but I thought it humorous so I left it.
Sign, let’s sign the damn thing already.
an institute for postviral deseases? what about other infectious triggers. and what about the ME/cfs patients who had other causes of their desease. they will be left in the cold…
The proposed Institute will include ME/CFS – no strings attached that I know of. 🙂
It is time that we stop with the term long covid.
https://www.theguardian.com/society/2024/mar/15/long-covid-symptoms-flu-cold
Cort, can you bring in here the very recent article based on research in the American Assoc of the Advancement of Science from the economist I sent you – on PINS, post infectious neurological syndrome? The title is Long covid is not the only chronic condition triggered by infection
Finding similarities between post-infectious illnesses could lead to better treatments
Unfortunately I just read this blog of yours and everyone has moved on to the new one.
I fully agree.at this rate we’ll all be dead and the nameof me/cfs will have changed once or 10 times again.This illness has been going on since the beggining of time. That’s why I began trying many different things… SO TIRED OF WAITING.
Omf needs to find and look at people that have recovered.
Looking at folks that are way too far down the rabbit hole of illness are very, very hard to turn around due to the so many changes that happen biologically.
What I see happens with science is, they start splitting hairs.its great that they can dig deep and find the damage etc. But gosh, use some common sense as well.
Easy for me to sit here and say but the people that have recovered used some pretty simple common sense approaches.
Diet changes etc
so all the people in the 25% ME group, can rot in hell? because they are to ill? if you where there, you would speak different. Anyway, the most studys are on the better patients. Luckilly there are still some scientists also including the verry severe ones who can go no where.. Even if it are only a few. And look at the decodeME questionaire results and you will see that a % gets better on its own, others not and others decline. it is such a complex heterogenous desease. if it was that simple, diet change, etc we all would be cured. and how hurtfull is this comment to Ron Davis and Janet Dafoe who’s son is so terribly ill… As if they did not try anything!
again, a verry verry severe ME/sufferer died. just wanted to mention it. If we need to wait until there comes a miracle for real monet for research for ME/cfs..it is unbelievable. we are forgotten… of what i know only the UK do 2 tests at home to include the verry severe ones. with assistence. and good studies.
All I’m saying is something has to change.
At this rate,and, if you look at how long the same research has been going on for, we’ll just keep spinning our wheels for another few decades.
By not finding answers, it gives the “all in the head” nay sayers more power.
I’ve been into this for decades as
well.financially ruined! If you look back at the history of all of this,you will see giant insurance corporations have denied claims forever, me included
I am not cured.far from it.
I was severe like whiteny, maybe worse.my brain was so inflamed and such bad fibro that I was going to go get the gun on a few occasions.A HORRIFIC ILLNESS
i could very easily fall off the wagon, into severe once again.
Researchers of today and other older research just keep redoing the same studies over and over,…keep beating a dead horse.something has to change!
I was just told a couple weeks ago by my nephrologist that tetracycline did this to me. Waiting 40 years to finally find an causual answer is cause for celebration, but REALLY, 40 years of searching,going to hundreds of appointments is a bit of a slap in the face as well.
I failed in school and dropped out, I’m sure now it was from the tetracycline.IM 64!
My illness, I believe, could have easily been unraveled if the doctors would have simply looked back at my health records and seen how many years of tetracycline i was given. I always assumed doctors were like Sherlock Holmes.maybe they did know and kept it covered up.
The book, the yeast connection was written decades ago.i took that book around to many doctors and specialists…to no avail.the book was written by one of their own. It’s one of the reasons I believe many of us have been railroaded and misled.
I believe there are many ways to have gotten me/cfs. There are lots of subsets.
With this many subsets, it’ll be years and years before this all gets sorted out.
I recall when OMF first began research.
Davis came out publicly stating …
“we will have answers in a year”
That was years ago.maybe a decade ago.
What is OMF doing now…small studies
Am I bashing OMF, I don’t think so…I’m saying….now that they have some money and clout at the very least get on with larger studies.
If you look back at my statements…I stated…”easy for me to sit here and say”
Davis seems like a very thorough investigator, like he wants to get it right the first time, I’ll give him that.
Hidden infections, why can’t they be found in the name of science. It boggles my mind that there isn’t ways to find hidden infections with the science and tools we have today.
Why did the health industry in Canada discontinue the tiny camera that patients would swallow and gastro specialists could view every inch of a person’s intestines. Brilliant tool…no longer in use.mind boggling!
A gastro specialist in Calgary,Canada invents the first artificial fecal matter transplant , has a pattent on it…DECADES AGO!…still ,it’s not in use.Mind boggling! The only way to get a FMT here in Canada is to have C.diff.
Maybe I’m just overly frustrated like many of us are as to why this is taking forever.ill just shut up now
no, you are not overfrustrated (mean in a bad way). ofcource there must be changes! like you write about artificial fecal matter transplant not in use, the health industry in Canada discontinue the tiny camera that patients would swallow and gastro specialists could view every inch of a person’s intestines no longer in use, that OMF should be doing larger studys now they have got money, etc it is all mindblowing! And the OMF promiss, you mentioned, we will have this in a year, i can not remember but if, again a false promise. The so manyest i have heard and seen…I did not write for nothing that OMF would be doing better a few really big studys isnstead of spreading the money all over for excample in such tiny studys. i do understand you! i hear you! you are also a verry long time ill. for decades! me to, time is ticking… And it indeeds feel the same as for you, why is this is taking forever! And 40 years ill to hear it where the tetracyclines as a child, who did this to you is indeed a slap in the face. I got as a child also much tetracyclines. in my ME/cfs a half year 3 kind of antibiotics , one kind was tetracycline. I want faecal transplant but also here only for C. Diff. My last hope is on the DecodeME study, now also in the US, finland and 1 or 2 other countrys and working with precisiolife (who at least subgrouped patients with the SNPS), my time is running out… They did not work together (globally), they often did not made there researchgroups bigger with there findings, it is like every researcher wants his or her’s right, etc. I really get you! Lets hope there finally changes something… how did you get better if i may ask? with that book or what?
Dietary changes,moving into a different home away from a mold home.
One dose of horse ivermectin not that long ago was a game changer for me.
Subsequent doses of ivermectin did nothing but that one dose killed something off. Perhaps a parasite or bott.🤷♂️ I’ve been around lots of animals all my life. Horses, pheasants,chickens,ducks,deer,bear,antelope,coyote,etc.etc.
And lots of nasty chemicals like lacquer paint and thinners, epoxies.
when the pandemic came, my wife and I got very sick, hospitalized.
I went onto the flccc website and did a couple of their protocols
I’ve always had cold hands and feet,allergies etc. My hands and feet are now warm. I do believe blood flow has a lot to do with all of us.also, I believe endocrine issues are a big part.
I’ve done a lot of intermittent fasting the last 3 years. I recently got in touch with a wildlife biologist that has sent me a herb that I can’t mention to you on here that seems to be doing something.
I also went and blood letted a few times.cant hurt to have new blood lol.
I’d share the herb if you want to try it.if you want to private massage me.ill see if I can figure out how to retrieve the pm. I’m 64 self taught on computer.lol
Also….if you’ve watched any of Realyn eangle (spelling?)YouTube videos, she barely ever mentions her extreme change in diet.
Nor do any of her guests.
The other thing i did that got almost rid of my 2 inch lymph lumps was, I started doing the exercises in the book by. Dr. Raymond Perrin.
I did his self test where you find what’s called the perrin point, you press on that perrin point and if it’s tender (I let out a scream!) That is an indication that your lymph system is not flowing and/or not flowing in the correct direction. He has book a person can purchase .I have his first book…rather small…his later books are larger and packed with lots of info. Hope this helps …someone
hello, i live in Belgium where it is still cfs, get and cbt. i live in unbareble circumstances totally alone, verry severe bedridden in the dark. only 2 hours of help a week wich is even to much for me. must be glad if i can take shakes from pharmacy for food. And my breakfurst gluten free oatmeal with lactose free milk. and once in a while a readdy meal or some fruit. certainly not the best diet but i can in no other way. i can not move because totally alone, way to bedridden,etc gp does not prescribe things you named. i have noboddy anymore. the ivermectin if they have it here, is it a medicine (can not search now anymore). what is the flccc website and wich protocols please? (sorry, i must sleep again so can not search, only typing the text to you was so hard. They would never give new blood here. not when really needed in hospital. and cfs is between the ears… i have for excample burning leggs (maybe bloodflow, i do not know ). when i was young cold hands often and feet. so many symptoms now. feeling glued to the bed in my dark room. like lead. not strenght enough to breath. diafragma, ribs almost do not work. infections or maybe auto-immune, i do not know. heart that does not want to beat fast enough, low bloodpressure, then it is high HR and better bloodpressure and i feel better. must sleep now. thanks!!!
I wish your regular doctor could help you somehow, Konijn. Cant give you blood pressure med?
I’m interested in the herb. Email is traceyellisfa@gmail.com
me too Buckey
qkcam45@att.net thank you
Please reply to Buckey’s comment, not mine, to reach him.
Congress or a new dynamic Presidency headed by someone who has a focus on the chronic health epidemic,someone such as Robert f Kennedy jr?
yes, here also a better dynamic minister of health and in the European union also someone else, both with focus on chronic health and forgotten deseases. here still even only cfs and GET and CBT.
Konijn…where do you live?
stupid Belgium…
Kennedy still believes vaccines cause autism (thoroughly debunked by large studies), that the CIA was involved in JFK’s assassination, that Prozac use is linked to mass shootings, that Covid-19 was targeted to attack Caucasians and Black people and avoid Jews, etc. Who knows what he would do with the NIH?
https://www.forbes.com/sites/saradorn/2023/10/10/rfk-jr-launches-independent-2024-run-here-are-all-the-conspiracies-he-promotes-from-vaccines-to-mass-shootings/?sh=7d6469483cef
Not so long ago, scientists thought that autism was caused by mothers who lacked empathy. Blame the mothers. Strange people, those scientists aren’t they… should we trust them blindly?
The covid vaccines for people under the 70 years was that really necessary? That is still the basic guestion.
In people younger than 70 years, infection fatality rates ranged from 0.00% to 0.31% with crude and corrected medians of 0.05%.
https://www.researchgate.net/publication/348223673_Infection_fatality_rate_of_COVID-19_inferred_from_seroprevalence_data
But that is another topic
Cort, I thought I read that those large autism studies were badly flawed.
As I stated earlier, what the heck were they thinking when they added mercury
To our childhood vaccines
We’ve been told that mercury is highly toxic and to never even have it come in contact with our skin…yet…they put it in all our childhood vaccines back in the 50s etc.
I wonder why it’s not used now?
I for one will never get another covid 19
Vaccine.my third covid 19 vaccine produced a grapefruit sized mass under my right armpit that later shrunk, but not totally gone. They can’t be good for anyone. The fact that they made it mandatory or you’ll loose your job was enough to make me wake up.follow the money train $$$
The best defence will always be already getting covid and / or having an optimal
Running immune system.
The vaccines have been proven only 25 -30%effective. Just what I’ve read
I have ME/CFS and MS. I started taking Kesimpta (ofatumumab) 2 years ago, which is a b cells depleter. It’s doing what it’s supposed to be doing really well (no ms relapse and no new brain/spinal lesion) but did absolutely nothing for my ME/CFS symptoms. I am worst than I ever was (moderate-severe) . Being immunosupressed is definitely a big problem. I don’t think the treatment per se is making me worse but the accumulation of infections over the last 18 months probably is.
Interesting you have both ME & MS. Someone I know of had both, and she had had ME/CFS for many years before developing MS. She was treated with non-myeloablative HSCT in USA for her MS (the treatment uses cyclophosphamide and an autologous stem cell transplant to basically reset the immune system and halt MS progression / puts many people into remission) and she got a full remission from her moderate-severe ME/CFS as well. She must have been a cyclophosphamide responder – not everyone with ME/CFS is according to the Fluge & Mella research. Not sure if it is something you would be interested in looking into as it definitely has risks and side effects but is an interesting treatment pathway. I’m unsure if there’s any benefits to it compared to cyclophosphamide treatment alone.
My mother had the MS, the slow one, I have the ME for 40 years. A friend has the ME and his mother had the slow MS. Just a hazard?
There’s that Epstein-Barr virus which is a trigger for many people who get ME/CFS in adolescence and early adulthood especially and which clearly plays a role in people getting MS decades later.
2020 study on Copaxone effect on EBV in MS.
EBV-specific CD8 T lymphocytes and B cells during glatiramer acetate therapy in patients with MS
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7455312/
Prof. Gavin Giovannoni March 22, 2024
Targeting Epstein–Barr virus in multiple sclerosis: when and how?
“EBV is the probable cause of MS and is likely to be driving MS disease activity via latent-lytic infection cycling. There is evidence that all licensed MS disease-modifying therapies target EBV, and there is a compelling case for testing other anti-EBV strategies as potential treatments for MS.”
https://pubmed.ncbi.nlm.nih.gov/38511407/
We need to join forces! I’ve read the accounts of antiretroviral self-trials for ME/CFS that have limited success, and the same occurs for MS. But there are 7 case studies of MS stopping due to Tenofovir Alafenamide (TAF), Harvard is doing a pilot study to test Truvada on EBV blood and saliva biomarkers pf EBV antibodies. Here is a 14 page doc on #EBVcausesMS. Covers all the antiviral research.
https://bit.ly/AntiviralsForMS
First, I had “glandular fever”, I stay fourth days in the ER in a teaching hospital, at 23. 17 years after, a professor (Dr Morrisset) diagnostics me with a chronically CMV active infection. Only 12 years after, I had EB infection with the reactivation of his cousin, yes, both belong to a mafia family. My GF at this time did not have EV, too. I don’t know about my mother. She had a very bad “elbow problem”, at 30s years old.
Hi Cort
What to do for those for whom nothing else has worked?
1) Take a TEST (an MRI?) for myelin degradation.
2) IF it’s positive TRY Copaxone. Since it’a already approved for MS,
I’m assuming there are no big side effects.
Does that sound reasonable to you?
I’m 81, and would like SOME time to work on my unfinished projects.
I was not clear on the followup but it seemed to me that that’s the gist – see if you fit the diagnosis for MS and try the treatment. I think doctor’s who understand Ron’s work might give you a trial of Copaxone if you score positively on MBP antibody test even if its not diagnostic for MS.
I’ve got a ton of projects I’d like to do too! 🙂
Would you mind finding out more about this Cort? I have a son with MS who is helped by copaxone, and I have ME skeptic neurologists in my area. So I’m not sure how to proceed. In particular a spinal tap could be bad for me because I’m housebound severe. Easily relapse with PEM.
How were the ME patients improved with Copaxone? What symptoms changed.
Interesting. My Ex-wife developed MS about 6 years after our marriage ended.
If anyone tries Copaxone, could you please report your experience to us? (TY).
Thx again Cort!
There was a bit of chatter around copaxone and the nanoneedle 5 or 6 years ago, so I tried it. It seemed like a reasonable thing to do based on the science, but unfortunately I felt a bit worse with it, so obviously I stopped. Trial and error is the name of the game still. I’m glad I’ve been able to try and that few of my trials have made things irrevocably worse.
Prof. Giovannoni coined #EBVcausesMS and #Antivirals4MS and has been studying this for a decade. In his new review paper below he says:
“There is evidence that all licensed MS disease-modifying therapies target EBV, and there is a compelling case for testing other anti-EBV strategies as potential treatments for MS.”
Then he explains the better approaches to treat EBV going forward.
That’s because MS drugs are only marginally effective. Copaxone was my first MS drug; it cut back the relapses but did nothing for the miserable symptoms like CFS, and progression continued, leading to a wheelchair. No relief, no cure, just slower progression and injections or infusions for life. Great for pharma revenues though, $23 billion annually for MS.
The fact that the MS drugs had even a partial effect on EBV was obscured because that would bring up the question: If MS is triggered or driven by a virus, why not treat with an antiviral like every other chronic virus is treated (HSV-1,2, Hep c, Hep-B, HIV). It was discovered by chance that people with MS who caught HIV found their MS disappeared when they started HIV antiretrovirals. These case studies were published, but it didn’t sink in until 2022 when Dr. Asherio of Harvard published the proof that EBV is the cause of MS.
Trials of antivirals and other approaches, such as restoring immune tolerance to EBV, are finally starting trials for MS. I am sharing this info with you in the hope it will alert the MS/CFS to learn from the misdirection on treatments MS patients have suffered from. The history of EBV and MS, the new treatments for it, and the effects that existing MS drugs have on EBV is documented in this paper.
https://bit.ly/AntiviralsForMS
Targeting Epstein–Barr virus in multiple sclerosis: when and how?
Prof. Gavin Giovannoni March 22, 2024
Purpose of review
Epidemiological evidence implicates Epstein–Barr virus (EBV) as the cause of multiple sclerosis (MS). However, its biological role in the pathogenesis of MS is uncertain. The article provides an overview of the role of EBV in the pathogenesis of MS and makes a case for targeting EBV as a treatment strategy for MS.
https://journals.lww.com/co-neurology/abstract/9900/targeting_epstein_barr_virus_in_multiple.152.aspx
Yes, there are multiple cases of ME patients who are initially misdiagnosed as MS – they typically receive IVIG and other MS treatments which help them tremendously. In at least one case, a patient whose diagnosis was changed from MS to ME could no longer access the treatments that had resolved her symptoms.
Where can I find the instructions for the dosages, please? I don’t know if I missed it perhaps in the article. I would like to ask my doctor if I could give it a try. Thank you
It’s interesting to read all the comments about tetracycline and “The Yeast Connection” book. I also took tetracycline for a long time (for acne) and that is when my ME/CFS started. By following the advice of the author of “The Yeast Connection” I got at least 50% improvement in my symptoms. It’s the other 50% improvement that I’m still waiting for, almost 40 years later.
I was living with MS for years before being officially diagnosed in 2021. I got annual MRIs, and I did not take any meds due to side effects. I had one flare up in 2021. My legs decided to a break and I was numb from the waist down. I decided to try MS-4. The numbness and Muscle spasms went away after a couple of weeks, but it took almost 3 months to walk properly without a cane. In June, it will be four years without incident, and I am extremely happy that I made the decision to not take any meds and went for the MS-4 formula even though my neurologist got upset and one told me to quit my job because I will be disabled. Well, I am not disabled, I still refuse to take those meds, and I am doing just fine. Believe in yourself and go with your instincts. Doctors don’t know it all. I’m surprised a lot of people with MS haven’t heard of the MS-4 protocol,