Research funding for chronic fatigue syndrome (ME/CFS) has been poor at best but clinical trials have elicited a wholly different degree of disappointment altogether. Few clinical trials are ever done and those often involve alternative approaches. The six active clinical trials listed in clinicaltrials.gov, for instance, include treatments like acupuncture, moxibustion, oral rehydration and CoQ10.
That makes it shocking to see a “new” drug – a drug not being used in other diseases – get a clinical trial in ME/CFS. It wasn’t supposed to happen this way. First, it’s been assumed that repurposed drugs – drugs already in use in other disease – would be tested in ME/CFS to improve symptoms – and only later, as we understood the disease better, would we get to a drug that gets at the core problems in ME/CFS. This group believes they have a drug that gets at the core of ME/CFS now, and in the first quarter of this year they expect to test that drug.
Over the next month, Health Rising will be publishing a 3 or 4-part blog series telling the story of the small group of researchers that are bringing a drug to ME/CFS they believe could get at the core of this disease.
The drug itself is highly experimental and the researchers behind it come from the biotechnology and drug development fields. They stumbled on ME/CFS by chance, but when they did, the light bulbs went on. For the past year or two, they’ve devoted their time to understanding ME/CFS and getting to the place where a clinical trial can take place.
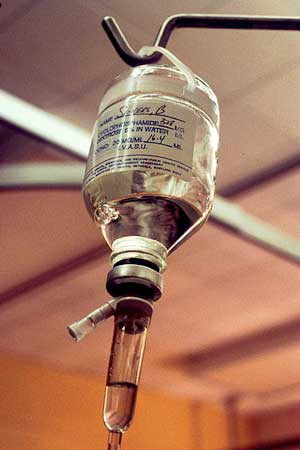
Rather shockingly, a new drug – a drug not being used in any other disease – will soon be tested in ME/CFS.
It’s important to realize that these researchers/investors – like all good researchers/investors – are essentially agnostic regarding which disease to test their drug in. They’re fully aware of the history of neglect in ME/CFS and my sense in talking to them is that that neglect, and the opportunity to provide help to such an underserved community excites them.
Their decision to spend the time, money and effort to test this drug in chronic fatigue syndrome is not because of the great need ME/CFS patients are in, but because this is the disease they believe this drug will work in. In order to come to that conclusion, they’ve explored ME/CFS very carefully.
The upshot of this very different approach (for us anyway) is that, while this drug is new, it probably enjoys a more robust theoretical foundation than any other drug that’s been tested in ME/CFS. That provides, at least for me, some reason for hope.
The group has flown under the patients’ radar but have not hid their light under a bush. Over the past year they’ve conducted an impressive outreach program – a kind of learning and enrolling tour – communicating with several major ME/CFS doctors and researchers across the country. None, they report, have been able to find any flaws in their hypothesis and all agree that their drug should be tested. The trial is expected to take place in the first quarter of this year at a well-known ME/CFS expert’s clinic. (The details of the trial will be released in the last blog.)
The upshot is that to virtually everyone’s surprise, a new and experimental drug will soon be tested in chronic fatigue syndrome (ME/CFS). It’s a fascinating story. Enjoy…
- Part I – Beginnings and the Hypothesis
- Part II – The Hypothesis Pt. II
- Part III – Treating ME/CFS and the Clinical Trial
A New Hypothesis on the Cause of ME/CFS – Part 1/3
Gerard Pereira didn’t know much about chronic fatigue syndrome (ME/CFS) but what he was hearing was setting off all sorts of bells and whistles in his head. Sometime before, he’d come across an intriguing drug (CT38) being developed by the pharmaceutical division of Proctor & Gamble. CT38 prevented muscle wasting in animals, and it had been through a Phase 1 clinical trial and tested safe in healthy humans.
Despite the promising test results, after Proctor & Gamble decided to exit the drug industry entirely, CT38 was left available for licensing.
Pereira had been tasked with finding promising new drugs and he liked this one. Despite strong animal data, though, Pereira’s employer wasn’t interested. The commercial potential, they felt, just wasn’t there. One population CT38 might help (people on mechanical ventilators) was hard to study and short in supply. A chronic disease like muscular dystrophy might fit the bill, but would require big money for long-term animal safety studies.
Pereira, though, was intrigued. CT38 targeted the stress response – a system getting a lot of attention, and it appeared to impact inflammation – a bigger and bigger concern all the time. Plus, the animal data was really good. Eventually Pereira decided to license the drug and start his own company, Cortene Inc. He and his partners (Sanjay Chanda, Hunter Gillies, Michael Corbett) would try to develop the drug themselves.
Pereira was at a cocktail party discussing his drug with a well-known Stanford doctor, who was talking about some immune findings in a strange disease called ME/CFS. Pereira had not heard of the disease before, but the immune findings, and ME/CFS in general, seemed eerily reminiscent of the data he’d seen produced for CT38.
Pereira took a deep dive into the ME/CFS literature. The more he saw, the more he liked the fit. He was particularly taken by four facets that seemed to separate ME/CFS from other diseases: the diversity of the apparent triggers, the unusual suddenness with which the disease often appeared, the gender imbalance, and the wide range and variability of symptoms – both across patients and over time. Explaining those four facets, he thought, might lead to the cause of the disease. Most of the current hypotheses couldn’t. Could he?
Take the idea that a pathogen or an immune system issue was the key culprit. Could either explain how a healthy person – often a female – could be turned into an invalid, sometimes overnight? He didn’t think so. Too many different pathogens had been connected to ME/CFS for one pathogen to do it, and pathogens usually affected both genders equally. Plus, no one had been able to definitively show a pathogen was still present and/or still responsible for the symptoms seen in the chronic phase of ME/CFS.
The immune system was certainly involved, but the patient stories he’d heard suggested that the disease happened too fast for the big guns of the immune system – which took time to get worked up – to take down a patient so suddenly. Too many people with ME/CFS caught a cold, and then were suddenly floored by the illness, for that to make sense. He didn’t think the metabolic ideas sweeping the field fit the bill either. Metabolic changes were certainly present, but a rapid metabolic breakdown that happened predominately in females was hard to explain.
Instead, he thought the initial insult (infection, stress, etc) must have caused changes in some integral system; a system able to touch the immune and autonomic nervous systems and ultimately even glucose metabolism.
An adaptation (or perhaps maladaptation) of the limbic system that determines our responses to stressors like infection, trauma, emotional distress, etc., could fit the bill. The limbic system had been considered in ME/CFS for decades, but no one had ever proposed a drug for it.
A change to the stress receptors governing those responses could happen very quickly. When it did, Pereira thought it would push the immune system in exactly the way it’s showing up in ME/CFS – and impair patients’ ability to fight off infection. That made sense given the Dubbo study reports that more severe, difficult to fight off infections, tend to trigger ME/CFS. It could also affect the autonomic nervous system, and eventually impact the glucose metabolism. The more he looked, the more he liked the idea that alterations to the stress receptors in the limbic system could explain ME/CFS. These were the same stress receptors that CT38 was designed to work on.
The HPA axis received a good deal of study in ME/CFS early on, but the results weren’t always consistent, and interest had waned somewhat over time. Still, the axis had a way of popping up. Gordon Broderick’s models suggested issues with the HPA axis could explain the gender imbalance in ME.CFS, and Dr. Bateman had proposed that ME/CFS might be an inflammatory disorder centered on the hypothalamus. Just a month ago, a study suggested an immune-neuro-endocrine interaction might be causing the fatigue in ME/CFS.
The main endocrine finding in ME/CFS was low cortisol (hypocortisolism). Hypocortisolism also occurs in chronic stress, where the initial excess of cortisol becomes low cortisol over time – and the development of something like cortisol sensitivity.
Pereira thought the HPA axis might be able to explain the gender imbalance issues as well. Women have more stress receptors than men, and another part of the hypothesis (covered in the next blog) fits women particularly well. Because the stress response is intended to take control and divert resources to/from critical/non-critical functions, it impacts most of the systems in the body. All in all, Peireira thought HPA axis issues could explain the wide range of symptoms in ME/CFS.
Long-Term Illness – Short-Term Treatment?
There was still the long-term animal safety data problem, though. CT38 had been developed initially for short-term use and gathering long-term animal safety data would be prohibitively expensive. How could a drug with short-term animal safety data be applied to a chronic, often life-long, illness like ME/CFS?
Now comes the most intriguing and exciting part of Pereira’s hypothesis. Pereira doesn’t need long-term animal safety data because he doesn’t plan on doing long-term treatments. If his hypothesis is correct, he believes CT38 will be able to reset the limbic system almost as quickly as it fell off the tracks in the first place; i.e., a couple of treatments might be enough to return the system to normal and begin the healing process.
If the idea of a more or less instantaneous reversal after decades of illness seems like some sort of fairy tale, consider that Suzanne Vernon and Gordon Broderick proposed something similar about ten years ago. Their model suggested that an HPA axis reset – by dramatically lowering cortisol levels for a short period of time – could cause the system to spontaneously reset.
This is not to say that over time other medical issues haven’t shown up in some ME/CFS patients that could complicate their situation. That’s to be expected in any decades long disease. If Pereira and Cortene are right, though, the core of this disease might be amenable to a dramatic change.
Part 2 will examine Cortene’s hypothesis in greater detail and show how it attempts to explain the many symptoms and anomalies of ME/CFS. Part 3 will explain the treatment approach and provide details on the upcoming clinical trial. (Health Rising is not affiliated with Cortene in any manner.)
To sum up – With the help of a physician, well-known within the ME/CFS community, Cortene will be conducting a small proof-of-concept trial, at a single site in the US. The details will follow, but the trial design is intended to obtain a rapid, objective assessment of their drug, and they will release the data as soon as possible. They reiterate that this is early-stage research and that caution is appropriate.
- Cortene II: A New Drug & A New Hypothesis For Chronic Fatigue Syndrome (ME/CFS)
- Cortene III – A New Drug for Chronic Fatigue Syndrome (ME/CFS): The Clinical Trial
- Cortene IV – The Cortene Chronic Fatigue Syndrome (ME/CFS) Drug Trial Begins
Health Rising is Run Almost Entirely on Donations
Please Support This Website!








Interesting. Cort. Thanks for reporting. If this resets the HPA axis, wouldn’t it work for FM also?
Good question – I haven’t talked to them about FM but I suspect so..I will try and find out.
Hi Cort, thanks for a very well researched and interesting article. It would be great to know if Cortene envisage this working for FM too. When you’ve checked will you be posting an article (which will notify us via e-alert) or will it come up on this thread?
Best wishes, Kate
Biggest problem with this approach is their mistaken belief that a short term burst of treatment with CT38 will have long term benefits. The FDA is still likely to want a 9 month canine Tox and 6 month rat tox. If those results are unfavorable, this will hamper FDA approval.
Hi, Cort. I have suffered with M.E. and Fibromyalgia for about 16 years now, and it is consistently life-disruptive. Last September I heard fo some doctors prescribing Trazodone along with low-dise Naltrexone to mitigate symptoms in patients with CFIDS and Fibromyalgia. I had Trazodone, and low-dose Naltrexone was available on the Internet with an RX. I decided out of desperation to try it. During the following month, all of my symptoms were significantly reduced. From what I have seen online, my experience was not uncommon with the Trazodone/Naltrexone combination. (I took 4.5 mg Naltrexone with 50 mg Trazodone.) Can your new drug possibly be used in conjunction with these others (the way Janumet is combined)? Also, I am in Northern California. Can I participate in the study for the new drug? I am 62, and I cannot afford the ongoing cost out of pocket for the Naltrexone. My insurance covers it, but I have had a hard time trying to get a doctor in my area to follow through on this.
Hi Cort, I stopped in the snow to read this! After 41 yrs of Cfs and now being 60, I am so tired of being so tired and missing half my life. I want to be a guides pig for this drug!!!!
Well in England our medical specialists say that although FM and ME/CFS have varied symptoms, they’re not sure if they are different illnesses or the same illness presenting differently. I recovered from ME/CFS years ago and now have FM and it feels not exactly the same but eerily similar. Here’s hoping for all of us!!
Lucy, I, too, became very ill with CFS/ME and slept 15 hours a day for 2 full years before I slowly improved. My symptoms are now that of Fibro. My doc thinks they are just different sets of symptoms of one disease that vary widely person to person. I would be interested in sharing more information. I had to leave work at age 59 and now am 71.
How did you recover from me what helped you can you let me know, I live in scotland and doctors here do not prescribe any treatments for this condition.
You didn’t say ‘How did you recover from ME/CFS’?
I have had it for more than 30 years.
Hej! Hur blev du bra från ME? Jag kan inte prata engelska..bara swedish..
jag är 65 år, och har fibromyalgi eller ME?
write..
I believe is same disease , it overlap 90-95% of symptoms , the same undelayinh genetic DNA changes, the difference in severity and symptoms is do to co infections and expousure.
I haven’t read any sources on the HPA axis in FM and am uninformed on its possible role in FM. Can StevefromMA or Cort please suggest a background reference to explain why this might work for FM if it works for ME by resetting the HPA axis? Thank you.
Where is the research???? Have you seen their website? Zero info/transparency. Also, there is no way to donate to or invest in this company (I spoke with the CCO). Finally, Stanford hasn’t heard of it. I’m weary.
It’s the same disease
I believe this could work, because I have seen so many occasions where environmental experiences involving my limbic system (ie emotional stuff in life) have affected my symptoms in a direct and clear pattern. I know many people are sensitive to this sort of suggestion, but basically, everything I’ve just read makes sense to me and my individual case at least…I can’t speak for the other myriad of ME/CFS presentations though…
I agree very much to this likely working for ME/CFS/fibromyalgia and maybe lyme. I’d love to be a Guinea pig for this study
I was infected with CFS/ME by taking pills!!!! Maybe people are infected people this way with out them knowing!!!!
What pills?
The end of CFS right here! I pray this drug does what they are hoping it will do. 100% I believe their hypothesis. Thanks Cort! I’ll be sitting back watching with some popcorn!
Popcorn! I love it. 🙂
How do I find the other parts of this blog? Have there been any results yet? How can I get in those trials?
No results yet, Travis….still waiting on FDA and IRB approval
Absolutely willing to participate! I am a nurse (RN) who has had ME/CFS for 3 years, short time for some, but ready to do anything to be back to me.
This sounds so good! Can you please tell us how to find out if we can participate in their study? Thanks so much!! xx
The details of the trial will be released in the final blog in about two weeks.
I can’t wait to learn how to be in this trial!
I would like to participate in this to…what I read in the hypothesis rings true for me…as I reacher cheddar a lot in the early days of me being ill and came to the same conclusion….
Having had this illness for 20 years and still looking for reasons as to what made me ill…and now they are looking at the endocrin system as to the reason I so agree….I really feel they have got it…..
I so pray this is just what is needed to reset us…
Where can we check to see if we can be part of the research individuals?
The next blog will provide ways to be considered for the study. 🙂
Ready to do anything to get better? Have you tried ozone and chelation therapy? Or Rifing? I find that lot’s of people only want to whine and complain, but are not truly interested to make the effort to take responsibility of their health and turn every stone to get better.
O, yes, I did. And stil ill. For 25 years. I tried everything you can think off. So, don’t yell if you don’t know.
Yes, I have tried both and found great benefit. However, the cost became prohibitive before I was completely well so I have fallen ill and actually became worse last year when we discovered black mold in our home. I wish Ozone therapy was affordable and available to all of us!
Really?!?!?! Are you even a patient of one of these diseases? In case you haven’t read, many people who would later get CFS/ME were very high achievers and held very demanding jobs and at the top of their profession. These posts contain more of what people have tried than posts just reaching out in hopelessness. You are ignorant and are on the wrong blog!!!
I went to Mexico in 05 for Ozone and Amino Neurotransmitter restoration for 21 days of TX. My results were very good. But did not heal me completely. I ended up buying an ozone machine and did blood transfusions for many years. The only thing that gave me some life back. Again its not a cure but it helps. The aminos definitely helped with brain clarity!
Unfortunately, many CFS/FM patients aren’t able to work and don’t have the money to pay for these out of pocket treatments and I have spoken to some who can and these modalities may help some, but they are still suffering. Please don’t judge anyone with this disease. It can be brutal.
Whine and complain huh? I’d love to meet you in person cause I’m sure you wouldn’t be talking in this manner then. You have no clue how severe it is for some of us. Have a little empathy sir.
So you criticize people here; AND you have a website selling ‘vacines’. Cort – should this person be banned? They ignorantly suggest we don’t try hard enough and take responsibility (what are we doing here?), and make a pitch for their product. Turn every stone, my ass. Go peddle your potions elsewhere. #loser
I just noticed couple of replies to my comment. I am happy to hear some of you have tried them and got some help, I salute you. And for those who got vexed I apologize for sounding insensitive, but I have had this sickness myself, so I’m not new to it. And my rather blunt expression was result of real life experience of weird hesitancy to challenge ones worldview even if it would not cost anything, but human pride(which is sometimes mightier than death).
Our western(or even global) system is so corrupted that in order to fix it we need stronger reforms(revolution?) than just appealing to it’s current perpetrators of injustice and machinations. They won’t listen us. That is what I meant by saying that whining won’t help. It was not meant to express lack of empathy for the individual.
Medical Traveling –
Please be kinder. There is only so much energy, so much financial resources, so much energy, so much failure of hope, so little energy, so much time to research, so little energy, so much fighting with doctors and insurance, so very little energy, so much lack of support or understanding, so little of everything to give of oneself to loved ones, so very very little energy…
Why would you post a comment which adds to these burdens? I am saddened.
Isn’t it strange that alot of the patients with this Malady are health care professionals> I am all for this drug and the testing format. Thank you Cort for all your research.
Is this true that many people afflicted with CFS/FM are health care workers? I am a female, nurse, who ultimately had to leave the work force
– from a stressful, demanding job.
I would be interested in participating as well bc I want to feel normal again. I too want to remain positive and really appreciate this blog and the new research!
I am a nurse and have had this for 20 years, during that time had remissions for years at a time but never 100%, this flares been the worst and visible symptoms for 6 years, just not gone this time.
Stories like these pose great challenges to those of us trying to manage a desire to stay positive and a desire to stay objective.
Yes they do don’t they! 🙂
I so agree Murph. I’m 18 years in. Bed/ housebound. The promise then disappointment is a killer.
Yes, it’s easy to lose objective and pin all one’s hope on a drug. We should never do that. As Gijs pointed out there are different types of ME/CFS – what works for one person doesn’t work for another.
My take from Peireira and Corbett is that they’re very smart people, I think they went about this in the right way – and as Ron Davis so often notes – the body is very, very complex.
Add to it that this drug is not currently being used in humans – so, we don’t have much data there – and fpr me I have very cautious optimism. We shall see.
Agreed Murph, we all can use a big dose of optimism as well…
Jay Goldstein
Yesssssss where he at?!
Yup. Limbic hypothesis.
I hope we get multiple trials for ME/CFS incl for Carotene and also Suramin with Naviaux or others, since the disease is diverse, so a single approach might work, but might need more than one approach. If even 10% are cured of ME/CFS, that would be 2 million people and still a great success then could optimize and perhaps cure more, or perhaps all.
Wow. That sounds very promising. Despite my short synacthen test returning an apparently ‘normal’ result, I can certainly relate my M.E progression to this hypothesis. Thank you for bringing this to our attention. Watching with hope & interest.
I’m wondering how affordable it will be if it is successful.
Good question. I have no idea…
I really hope this helps at least some of us. M.e. is a living hell and it would be great to have a life again!
I find comfort knowing I am not mad having so many symptoms and so hard to find a doctor that will treat it seriously. The anger that emerges when I can’t be independent is excruciating. Has anyone seen any article on symptoms of FM/CFS disappearing for the duration of pregnancy which is what I had. Hormone?
Yes I was always my best when pregnant, my over active immune system returns to normal this is usual so we can carry to term otherwise we would not be able to re produce this is how the immune system works. Normally a couple of months after having baby symptoms returns i also have over 20nknown allergies so was always going t be predisposed to cfs/me. Hope this helps.
Wow! I’m keeping everything crossed that the clinical trials are successful. Just when I was feeling that my optimism was waning, this news has really put me back in the ‘glass half full’ bracket.
By sheer fluke in 1928 Alexander Fleming discovered penicillin, and look how that changed the world. M.E. patients are well overdue for some luck, so let’s hope this is our lucky break!
Keeping hope for a brighter future keeps me going.
Fingers crossed…It would be a lucky break indeed. Time will tell.
Very interesting. This theory has been around for a while. Let’s hope it bears fruit. https://www.ncbi.nlm.nih.gov/pubmed/19165314/
So excited to see the HPA on center stage…where it belongs!
I watch with elevated hope, despite the fairytale trappings
Agree….excited to have the HPA on center stage too!
Wow Cort, this is great news but we must remain cautiously optimistic of course.Thank you so much for keeping us informed.
Yes! It’s an experimental drug. It’s not being used in other diseases – so its really very experimental but there’s hope as well. We shall see!
Is Cortene named after Cort?
:)…No. I don’t know the origin of the name but I assume it has a connection with cortisol.
V. Interesting and out of the blue. Do you know what diagnostic criteria they plan to use and are there any reported side effects from the human trial?
I don’t know but given the doctor involved and the researcher working with the doctor I don’t have any worries about the people participating in the trial. I don’t know about the side effects. All I’ve been told is that the drug was reported safe for short-term use.
Very interesting. Does he have any hypotheses about whether it will work just as effectively on new patients as on those who have been ill for 40+ years? (I’ve now had ME for almost 60 years, since Hepatitis A as a child.)
Hi Diane, I wanted to say that you are the very first person I’ve ever met who has had ME/CFS longer than I have! Ive been housebound for decades, and first became ill 51 years ago, after I was prescribed large dose of Cipro and Bactrim for months to supposedly “ wipe out” a UTI. Those drugs destroyed my health and robbed me of my life. I simply had no energy. A cure would seem like a miracle to me now. May we all find healing. I’m sorry you’ve been ill for most of your life.
51 years! Wow.. I think that’s the longest I’ve heard. Not necessarily a record one wants to have…but glad you’ve made it through all of that.
Diane and Elaine, I am a long-time sufferer, too. I have been sick for 40 years. It is unfathomable. I was 20 years old, contracted a bad case of mono. Never regained my health.
60 years is the longest I have heard of. I have now had ME/CFS for 48 years. It emerged gradually after severe mononucleosis.The mono was sudden but recovery from it was gradual. After having a severe infection, I can’t determine if the ME was there immediately after or emerged slowly as I recovered from the initial infection
“The most common cause of mononucleosis is the Epstein-Barr virus, but other viruses can also cause this disease. Mononucleosis usually isn’t very serious.” Mayo clinic
Up to reading this post, I have not run across someone who has had it longer. I am getting all to close to a half century, something which grinds into my mind.
Wow…not exactly a record one would like to hold but I sincerely applaud you for your perseverance..
Elaine so sorry that you have suffered so much! I,m.not able to take Cipro and non can in my family!! I pray God’s hand of healing reaches out to touch your body and heart!
sorry to hear that. I wish you well and hope for more treatments for you soon. I to have had this since I was a very young child about 3 years of age and I’m 57 now. The disease has progreesed but same issues just much worse. I also had dysautonimia andnow sjogrens. Not to mention 3 cancers which is noit a doubt a result of this disease. God Bless stay faithful
I’m very positive about this trial but won’t agree about sudden disasters made by pathogens. Streptococcus is well-known as a trigger for various neurological conditions (narcolepsy , among the others). EBV infection (my ME/CFS started exactly after a very strong and debilitating IM) not only has its acute phase but also may permanently affects the immune system , and the extremely interesting recent study about subgroups of ME/CFS and CD38 expression on CD8 (which have resulted in my 1-time blood results with 55% Cd38 gene expression) as a biomarker for a subgroup shows that the idea of immune activation after a strong infection as cause of the symptoms of ME/CFS in my opinion should not be discarded. I agree that a greatly impaired responsiveness to stress is “the” issue of ME/CFS.
I have come to the conclusion that at least with me “an impaired responsiveness to stress” is a huge part of this illness. It’s not that I can’t handle any stress – I can – but little stressors have such effects on my body.
Yes, Cort, I observe the very same thing in a family member who is severely ill. This all so reminds me of Dr. Goldstein’s work.
Same for me Cort. No doubt in my mind that the way I “handled” work related stress did it. Onset was that little “flu”. In my 13th year, having quit work in 2011, I have clearly improved, however, it takes relatively little stress to relapse.
And yes, same for me Cort. Completely agree.
Indeed. I have improved a good bit over 5 years after a long series of draconian protocols, month long solitary retreats, months on end of pacing as if I were moving through molasses, seventy day elimination diets, you all know the drill. But at times something simple as a stray remark is sufficient to get me buzzing for a day and a half no matter how skilled I’ve gotten psychologically. I just can’t flex with certain stimulation.
It’s amazing how hypersensitive our stress response system. One guess is that a messed up stress response is somehow linked to our sensory systems so that small stresses can cause unusual and painful results.
This is my 1st post, so please bear with me(there is hope in this story). I’ve researched many years as a patient, Dr’s unable to diagnose. I became ill with a flu-like, temporary bedridden condition, while juggling recording studio part-time, land surveyor fulltime, musician(many other factors – story too long, circa 1993). Fast forward through a hell-ish debilitating condition, push/crash, cognitive failure with work, stress, oversensitivity to most things, the CFS symptoms we all know. By 2005 I hit rock-bottom, lost all jobs, all abilities, bedridden 5 yrs, then baby steps with “very small projects”, between crashes, leading back to playing bass at home. I was finding ways to manage and produce “simple” things, mostly from the couch, as a way forward. Low impact Yoga(stretching only) and Singing again(mildly at 1st) became huge, my 1st physical path. NOW the pay-off ! by 2014 I began 5mg of adderall daily, (dedicating 12hrs bed/12hrs out of bed), less brainfog/sensivities, and singing were slowly building stamina, well-being, and positive outlook,and progress. I researched and found “pineapple juice” for vocal hydration, a natural anti-inflammatory, many health benefits, etc.. my moderate “daily” routine developed slowly into a website of vocal sharing, increased energy over time. Managing by taking daily notes of activity/productivity vs crashes, I was making actual improvements over 2 years. I was able to rehearse and do 4 “live shows” as Frontman/Vocalist (only 1 hr each, but serious progress – using Kindle for lyrics. No more naps (stay in bed, sleeping or not, be up, whether actually up, or on the couch not sleeping). The point of all this is that there is HOPE for some of us. Pineapple Juice, Adderall, 12/12 Plan, God 1st. Easier said than done, if you have faith, is to make everything in your live a “Symphony” (noises, distractions, upsets, daily pressures, pain, etc.) The confusion becomes music if you “perceive it” all as natural occurring events. If you can’t change it, enjoy yourself within it ! From bed to: A Journey with CFS [Ronzo Effect]
I have a horrible stress response. Have had CFS and FM for 10 years now. Little stressors cause a larger response than should be expected. Awful feeling. HPA problems for sure. I’ve been on low dose cortisol (10 mg in the morning) since diagnosis. When I’ve had to go off of it for various reasons, I feel like total crap. My doctor says I have immune dysfunction as well as several autoimmune diseases. Lucky me.
Me too cort. I know it is by my bodies response to mediation – I can greatly reduce flaring symptoms by deeply meditating/switching off.
Same for me Cort. I actually have to put myself into a deep meditation/ trance state/ hypnosis as often as possible and be totally still most of the day just to survive. Strangely, I can take very small walks and that’s ok because it’s a way for me to expand and not have to encounter any stressors. But any tiny stress, even thinking about stressful things causes a huge rapid energy drain, I’ve had to become good at managing stress, and have developed all sorts of tools, and spend most of the day in a resting zone. Thats why I’m still alive. But still, this has gotten worse over the 50 plus years that I’ve had this illness. I once heard of 2 patients of Paul Cheney’s who fell into comas due to accidents or some non ME related cause. Afterwards their ME/ CFS was dramatically better, though I never knew whether it stayed that way. I could relate to why that helped. My illness was caused by huge doses of Cipro and Bactrim prescribed to me by a urologist to “wipe out” a UTI. Can’t take them now, they’re like poison. THANK YOU FOR YOUR GREAT WORK.
Thanks…really interesting about the coma patients. I know of one person who was essentially cured for a time after being under anesthesia during a long operation..
For many years, I have thought I may have a mental illness. I have always overreacted to comments or actions I consider “wrong.” I cannot stop what seems like a burning chemical reaction overtaking my body when I’m involved in an argument, etc. It happens so darn fast, I cannot control myself; like a hair trigger response. At least I’ve reached an age where I try to immediately or soon after a “blow up,” apologize to that person (mainly my partner, poor guy, but others as well). The stress and physical symptoms that follow these episodes drain me terribly. Many times I’ve thought “Gosh, am I crazy? What’s wrong with me?” My mother had similar reactions I observed as I was growing up. Now I think with CFS/ME/FMS, my system is hyper-alert and hyper-anxious. Even my meds like clonazepam (for sleep) and Cymbalta don’t help. I think Cymbalta may even worsen this behavior. If the HPA axis and low cortisol play a role as well, it would be great to be able to take something to remedy that! Here’s hoping. 🙁
Wow! I,m the Rock of Gibraltar in emergencies, but do sweat the small stuff! I can not hurry anymore! If someone is pushing and impatient, I fold! My body screams bloody murder even as I stand unmovable and then I feel paralyzed in arms and legs!
Cort, I’m so grateful to your dedication to bringing us exciting news in such a positive, ‘hopeful’ way. I really really pray this brings results for us all. Thank you.
Thanks – we shall see. We must continually remind ourselves that this is an experimental drug – it’s not being used in other diseases – it has undergone some testing in humans but we don’t know what it’s effects will be. We can hope, though, and we will see…
Hi Cort,
I have a unique combination of events: 1. Getting silicone shell saline filled breast implants that I believe caused my immune system to become so overwhelmed because I am of 25% of women that are allergic to, and/or the biotoxins of implants overloaded my detoxification pathways.
2. I became immune compromised and was infected with EBV.
2005 at 40 years old I had breast implant surgery, by 2006-2007
Slowly my energy and cognitive function began a decline that lasted until 2017, however I have never recovered any physical or mental stamina. I had explant surgery 2/17 and as you mentioned in your previous comment regarding relief of CFS/ME symptoms following coma or by receiving general anesthesia during surgery. THIS IS EXACTLY what I experienced the hours following my surgery. My surgery took place on a Tuesday, and the clarity, mood lift, physical vitality, the vim and vigor was through the roof! But by Friday all the mental malaise, physical low as if I had no serotonin came back sadly.
But I’ve been very curious as to the possibility that anesthesia has anti-inflammatory properties that mitigated the reduced nerve/vascular function in both myalgic encephalitis and CFS. Do you have any thoughts on this premise?
Thank you Cort:)
Colleen
Oh yah Colleen!
I know of one person who had a major remission after a long term surgery. A story on her is coming up. For me I always feel better after dental anesthesia – go figure!
This theory sounds great (not new, it is an old one), i believe they are on the right track but the abnormal stress respons could be an compensation reaction for low energy. Finally we can test this. But one thing is very important! WE have 2 different ME types: 1. the overdrive type (POTS etc..) and 2. the underdrive patiënt like hyper- and hypo type. I think this drug will work only for type 1 patiënts! I look forward to the results!
I actually think that this kind of treatment (manipulating any kind of receptors in the brain or elsewhere in the body) could make people potentially a lot worse in many different ways and that there is no way to tell whether you get better or worse before trying it. I think that there is a high chance that this overdriving stress response (i.e: the chronic overdrive of the sympathethic nervous system) is some kind of mechanism to keep the engine running. I believe that a specific not yet identified form of EDS is at the heart of the problem for many (not all) cfs/me sufferers. (and for many other syndromes as POTS, MCAD, …)
So, slowing down the sympathetic nervous system could be dangerous. I agree.
There was that Clonidine study in which slowing down the SNS made the adolescents with ME/CFS WORSE. That was a shocker except that when I take something that give me energy and really relaxes me I tend to fall apart. I think the increased SNS activation is there for a reason. I think it can be slowed down but it has to be done slowly.
The clonidine study was a bummer indeed Cort. The activation of the SNS is a countermechanism, I think that is quite certain, the body always tries to be as economic as possible even in the worst condition, it seems to be economic to be “activated” for me/cfs sufferers – I think we have to find out why and should not try to work on the “symptoms”.
As I mentioned before in various blog posts here and elsewhere, for a certain percentage of people with cfs/me it is very unlikely that their issues do net stem from some systemic issues that are connected to some form of EDS. There are dozens (more?) of studies out there that seem to validate these connections and still there does not seem to go enough thought into it, that really puzzles me.
My personal story started when I was 20 years and I did a 24hr holter test because I wanted to get faster and more fit as a competitve runner – it turned out that I had 30.000 (!) more heartbeats a day than the average person my age. (basically I had POTS but no one told me about it).
10 years down the road I am 80% bound to bed and can´t do groceries for myself. I suffer from POTS, CCI, MCAD, ME and EDS Type 3, all of these illnesses got diagnosed by some of the best in their fields. Diagnosed but not treated, every single trip to a specialist makes me worse due to the strain of travelling.
Talking about EDS, most if not all people make the mistake to think that you have to be circus like flexible to have EDS. I am not, my brother is, my grandmother and mother are, I got a lot of different characteristics like cigarette paper scars, very thin transluscent skin, super flexible joints in my fingers and toes etc but I am not super flexible everywhere else.
What is the chance to get diagnosed with 5 different medical conditions as a 30 year old, every single condition severe enough to really fuck up your life. (sorry for the f-bomb, I am too brainfogged for something more elaborate at the moment).
Right, the chance is close to zero unless they are all interrelated and the very root cause is the same. The SNS, hormonal systems and many other systems try to come up with a plan to hold up the game while you are getting sicker because your system gets less and less effective due to some form of collagene damage (most people with this probably unidentified form of EDS get sick when they are between 25-35, so right now it is EDS Type 3, but we do not know what this actually means).
This is a life saving mechanism for sure but one that cripples you, and I think it is quite obvious why that is the case, lets look at a quite simple example that illustrates the problem: lets say your body is trying to adjust to blood pooling in your legs (your body does not want you to get unconscious) by pumping more Adrenaline in your system (that is what happens for many people with POTS and EDS), your are physically forced into a situation of severe stress, the problem is that our bodies and receptors everywhere in the body are not made for dealing with this constant stress – if this happens once in a while your receptors are not really bothered by it, but if this adrenaline response becomes the new status quo for many different bodily actions to function these receptors (many different receptors due to wide ranging ripple effect of adrenaline) get whacked over time.
So yes, you could readjust them, but in the end you are not solving the problem, for a certain subset of patients you probably make them a lot worse.
agree
Great work! Thank you!
Cure ME in 2018!!
Wow . When and where should the trial take place. And how one could sign in?
Hmmm, my understanding was that cortisol is not particularly low in ME/CFS. I got my GP to refer me for a short synthacthen test a few years ago to check my cortisol levels. The results were normal. My ME specialist said that this is usually the case in ME. He thinks that we have problems with our cortisol receptors (molecules inside cells that the cortisol binds to), rather than cortisol levels. Would that fit with their hypothesis do you know Cort?
I think your doctor is probably pretty close. The hypothesis primarily involves HPA axis receptors not cortisol – which tends to be only mildly low in the morning in people with ME/CFS.
It would be interesting to see what your doctor makes of the next blog which goes into the hypothesis in detail.
In my case particularly, my adrenal system crashed after my first 8 years with MECFS and I’ve ended up on hydrocort for life since unfortunately. I’m one I guess that the adrenals couldn’t keep up anymore and just totally burned out (the glands are OK it was perhaps the HPA). I’m pretty sure I’ll never be able to get off it though which sux.
Hi I have POTS and CFS coming up on 17 years. With each year I am progressively worse. I must say this report is the 1st that I have read where I do believe they are finally looking at the root problems. Gijs my question for you is regarding the 1st type of patient. Are you referring to Type A personalities?
2nd question to all: Does cognitive overdoing affective you? And if so, how much less than physical?
Cort,thank you once again for all your hard work and the truly EXCELLENT information you bring to us.
What is Gerard Pereira’s background? What state is this trial taking place in? And how severely ill are the patients? Do we know if any other ME researchers have been in touch with Mr Pereira?
Peireira and Corbett’s background is in drug development. Neither knew anything about ME/CFS prior to Peirara’s talk with that doctor. If I tell you the state you’ll know the doctor and the doctor would prefer that his/her name be known when the details of the trial are announced. Pereira has communicated with quite a few ME/CFS researchers and doctors.
Kudos Cort for another well-written report. Time will tell, and for those of us with this long-term condition, a modicum of hope.
Surviving chaos of re-tirement, moving to another state, husbands’ illnesses and recovery. Your website, and ProHealth are the foundation for my continued presence in this life. Ready to be more proactive in outreach and activism. Simply enduring after 27+ years is an achievement I mark, knowing that more is needed, but timing is key.
“Hope is the things with feathers that perches in the soul, and sings the tune without the words, and never stops at all…”
You provide the words; bless you for your courage and tenacity!
Will stay tuned…blog in the works “Its. M.E. & ME”…thanks for encouragement…L
Glad to hear it Linda. Looking forward to the blog and what’s next for you 🙂
Yay! Super exciting! Please keep the research coming! We are desperte for treatment!
Interesting yes, after 26 years the research is going back to exactly what some non scientists believed. I hope this is it. I am get towards old age and never will get back what was lost. The ripples mean my severe illness has also damaged close family members. But it would be so good to have a cure. So very good.
The more I research the more it is apparent to me the rise of this condition correlates to the increased density of EMF, ELF, and RF fields. I am suspicious simply because the origin labs mentioned here have consistently created toxic products, sometimes deadly. In my highest of hopes, the goodwill intent is real, and this indeed can reset our systems. The problem lies in the radically altered environment. Our DNA is being altered. We are being triggered to become ill. We are changing into a chronically ill species. If radiation is the cause, the new 5G smart grid roll-out will increase the cases exponentially. The stresses of continual ‘re-setting’ could be as bad as the exposure itself.
I dread that 5G.
I agree that the Influence of EMFs, etc… is very problematic. So is the altered food environment and the sedentary lifestyle of the vast majority of people today.
Hi Cort and Others,
I can definitely point the figure at stress. Just at the end of last year, I was doing OK and then had a stressful few days and crash I go from 50% to 20%. Then, after 3 months and 3 weeks of no stress, it was like a switch flipped again and I went from 20% to 50%. That lasted for 1 month and back down the rabbit hole to 10%. Anyway, I have been working on Dan Neuffer’s ANS Rewiring program as one avenue to work on reducing the cortisol response and I just ordered some Rhodiola and Phosphoserine (Enerphos brand) after reading about a study where Rhodiola taken 2 x 250 a day for 8 weeks helped reduce fatigue.
I am not sure I believe that is the whole picture but potentially the main one that keeps the body being unstable. You still have to then fix any other ancillary problems, but that should be easier if you have energy.
This is exciting.
Nightmares crash me all the time.
Sleeping longer can make cfs worse. If i wake before the cortisol wakening i have much less cfs next day.
The famous author in NY reverts to 2 x 4 hour sleeps to avoid cortisol wakening response
Does phosphotlyserine not work on cortisol receptors?
He is really onto something.
Hi Greg.I found your comments very interesting, as I have never read the authur/book you mentioned but have stumbled my way to his/her 2×4 sleep system. And am much better if I am able to rise before the sun. Are there any other goodies to be gleamed in this book?
If yes? Would you please give me the information necessary to get it.
Hi Greg and Susan,
When last year I was again in a strong downwards spiral after a flu vaccination I could not break it with anything I’ve learned before.
Then I gradually learned to listen better to what my body was trying to do at night. Since a child I often woke up at night and turned around in bed falling in sleep immediately after. Often I woke up with nightmares but fell wright after them back in sleep. During that strong downwards spiral, that pattern got a lot worse, up to the extreme. Yet, after each exceptionally strong nightmare I just was calm a minute or even a few seconds later, turned me around and slept again.
Later I discovered patterns in it. Just around the moment of waking up from one of those nightmares, I was often either strongly moving (like running movements to flee or boxing movements to fight of the danger) or hyperventilating very strongly. After these first observations I tried to get my mind focused on observing the moment I woke up. I had plenty of practice in improving as I woke up so much each night. The observation became stronger: nearly all instants I woke up at night I was either moving my limbs, strongly contracting my muscles or breathing really heavily.
As a result I tried to do a combination of these things (stay awake for a minute and move my legs and breath in and out deep). The unexpected happened: I started to improve. The next few months were gruesome. I spent every bit of (increasing) energy I had into my new “night routine”: each time I woke up I got out of bed, did some light exercises and breathing exercises mixed with resting in between.
The result: I was putting the axe in my sleep. Every two hours (first hours of night) to every half hour I broke my sleep for half an hour to do this routine. I should have been utterly broken. Even a healthy person would suffer from such routine. However I felt better and had a clear and continuous improvement.
This night, the first part of my sleep was for five hours uninterrupted (so without a single time waking up in between) and for the remainder of the night I woke up four to five times. I also can maintain this with shorter “nightly routine times” now: I had a half hour break the first time waking up and a few five minute breaks later on. I still continue to improve.
I do relate these original problems to my blood circulation and breathing falling below the bare minimum. I often had very cold body temperatures at night. Waking up and doing this routine “corrects” this and restarts the blood flowing well. But your point of view could be correct as well. I’ll look into this cortisol wakening response.
-> If you both could tell a bit more details on what this 2×4 routine does for you, I’d be glad to read it and see if combining our cases shines a brighter light on it. Thanks in advance, dejurgen.
This theory makes a lot of sense. I believe Dr. Klimas is trialing Mefipristone in GWI patients to re-set their “steady state.” I think she said this drug acts upon the HPA axis. Then there are the doctors that Cort mentioned and even Raymond Perrin, an Osteopath in Britain, who believes toxins in the brain are affecting the HPA. He also has a protocol to remove toxins through massage and osteopathic maneuvers. I wonder if Suramin does the same thing? Thanks as always for the great reporting Cort!
Yes, they are using mefiprestone – a fascinating drug I did a blog on once –https://www.healthrising.org/blog/2014/06/29/repurposing-ii-natural-killer-cell-drug-chronic-fatigue-syndrome/ – It makes sense that they would go after the HPA axis (and the immune system) giving their modeling findings.
After decades of being severely ill,I would allready be glad if it would help even a little bit.
thank you cort for the hope!
Hey Cort – is this new drug named after you, by any chance?!
You do such great work with this blog, always clear and understandable even for quite complex information: thank you so much.
As for this new drug – good to have some hope, but am keeping it definitely in check. Apart from anything else, even if it is proven to work, here in the UK it would probably take years to get licensed, if ever.
He he – I wish…..Cortene and I are not related in any way other than it’s working on the disease I have. Good idea to keep the hope alive but in check – we know how difficult clinical trials are – and if this one works out it will have to be followed by much larger ones.
… and then it may be many years before it is cleared to go on the market. Hopeful 🙂 but frustrated. 😐
Cortene has said that if the FDA speeds up the approval process – which they often do do in diseases with such needs – it could take as little as 1-2 years.
The one thing that might speed things up is that the treatment protocol calls for a very quick treatment – no need to wait for months and months as with Rituximab – to determine results. If it works it will happen quickly.
If anyone should doubt the existence of CFS, they need only to look at the eagerness of those affected to try this unknown drug! The hpa axis is very much involved. When my symptoms are at their worst, my cortisol runs high. And my adrenaline response has pretty much been knocked out. FYI, I have a fairly unstressful life.
I am so incredibly excited at the possibilities!!! Especially the part about resetting the limbic system. My daughter has Complex Regional Pain Syndrome which also affects the limbic system. Can you imagine a drug that could fix both of us!!! Thanks again for your hard work and excellent reporting Cort! Made my day!
I read this article last night and when I woke up this morning I was convinced I had dreamt it! So happy to read it again this morning. Can’t wait for part II and III
I’m glad to see they are addressing stress as a cause and the HPA axis as well. Thanks Cort, for this interesting news. I’m looking forward to the next installments.
Thank you so much for this Cort. I find it hard to follow and understand the science of ME and proposed treatments. It is always a pleasure to read your well researched and well written pieces, and this one gives us all a tiny bit of (cautious) hope
Thanks. As Cortene noted caution is the word here. I love the fact, though, that this group is pouring so much time and effort into ME/CFS. We’ll see what happens.
Trying not to feel too excited or I might crash! Will follow this blog series and the trials with interest. Keeping everything crossed here in the UK.
Yes I too feel the same. Also in UK.
Now I know from past disappointments how foolish it would be to get overly positive about such news, but oh boy it’s hard to squash this rising excitement I feel reading this. I’m a believer of conscious collective energy …and it surely can’t hurt to gather up and direct that energy and positive thought towards this trial!
“The invisible fuel for this healing process is our heartfelt compassion and loving presence and the sincerity of the collective intention that we bring to it.”
-William Keepin.
Well done Cort. Can’t wait for the next instalments 🙂
We are really touched by the outpouring of response. Many of the questions and comments above will be addressed in Part 2, which explains the hypothesis in some detail. We are starting an FDA process that limits our ability to make specific comments, but we will keep you informed to the extent possible. As Cort notes, caution is appropriate for an early-stage trial such as ours.
We’re all cheering for your success.
There is an old drug called K41498, but it’s a peptide biologic, and was originally designed to be given by direct injection into the ventricles of the brain. K41498 is also called “antisauvagine-30”, or ASV for short, and it’s a 30 amino acid peptide. If this is the drug that you are testing, won’t it be very expensive, perhaps $100,000-$200,000 for a course of treatment, assuming it makes it through testing and gets FDA approval??
Rachel is it that makes you think this might be the case? Thanks
Thank you for your interest in this disease! Please keep us posted on how to be participants in the trial!
This will be year 30 for me and ME/CFS and only now are researchers looking at the right areas. I think that if this drug responds as hyped, it represents relief – and hope. Perhaps it will turn off our over-reactive responses for awhile, and allow the body’s protection systems to reset. Good luck and I hope your faith pans out.
If the trial is successful how long does it take to get through all the processes and finally deliver the drug to the market?
They would know better than me. This is what is called a proof-of-concept physician-sponsored Investigational New Drug study. I believe they would need to go through a bigger phase II trial and then an even larger phase III trial – if that’s right it would take some time.
First quarter of 2018? Wow, so many of us would like to throw ourselves at it!
Hi Cort,
Thank you for this interesting news.
I also want to that you for continuing to provide us with updates on the disease. Your writing is always clear and well researched.
Kind regards,
Alexandra Gillespie
Thanks Alexandra. It’s a continual learning process….:)
Gosh, this is interesting. One concern though – I have this fuzzy recollection of being at an ME/CFS research conference in Newcastle, England about 18 months ago when Prof Julia Newton mentioned in a Q&A that they had done a study into HPA axis abnormalities in ME patients and it had produced a null result.
Because it was a null result, she was having trouble getting the findings published, as scientific journals tend not to be so keen on publishing studies with null results.
Dr Charles Shepherd of the UK ME Association expressed surprise at the finding, since HPA axis issues have long been thought of as significant in ME. What was different about your study? – he asked Newton – why you get a null result when other similar studies have shown abnormalities?
“We controlled for depression” said Newton.
In other words, in her view (if I’m remembering and interpreting this correctly) HPA abnormalities were a product of the depression ME patients often suffer from as a result of having this debilitating disease, rather than a product of the underlying disease itself.
Newton said that she was hoping to get her findings published in PLoS One, but that was 18 months ago and I haven’t spotted anything about it there.
That’s all I can remember about this brief exchange during a Q&A panel discussion in Newcastle a while ago. Does anyone else know anything about this?
Interesting. I’m sure that they’ve controlled for depression in cortisol studies – there are have been so many of them. Controlling for depression is pretty common; I actually do not remember a single study in which controlling for it has effected the results but maybe this is a first. I’s certainly possible.
One of the interesting things about the hypothesis – which you will see in the next blog – is that what the researchers believe has gone awry in the HPA axis in ME/CFS- cannot be tested for yet.
It makes you wonder though doesn’t it? – how many other studies with null results just never see the light of day, go quite unnoticed, and thus skew our impression of what’s going on?
What happened with this research? Eight years ago.
A team led by Amos Ben-Zvi, of the University of Alberta in Edmonton, states that when the HPA axis moves from its natural homeostatic resting point, they may be unable to fully recover. When that happens, HPA axis dysfunction could become permanent, according to the study’s supporting information.
HPA axis dysfunction has been linked to disorders such as chronic fatigue syndrome, depression, post-traumatic stress disorder, and Alzheimer’s disease.
The researchers created a short-term intervention designed to help restore the normal HPA axis. This method has to do with temporarily reducing the availability of cortisol, a hormone that has to do with immune function. The reduction in cortisol levels causes the HPA axis to overcompensate and redirect to normal regulation.
This model, which must be evaluated in clinical trials, was described in an article that appears on January 23 in the journal PLoS Computational Biology.
Yes, that was actually noted in the blog. I don’t know of any clinical trials that came out of that unfortunately.
Stuart, maybe you should check out the research of Dr. Mark Demitrack. He was the first researcher to show that ME/CFS and depression are different things because they affect the HPA axis in opposite ways.
Thanks, I’ll check it out. I already have no doubt, though, that ME/CFS and depression are different things. I’m clear about that.
Lets hope this will be the breakthrough, that all M.E. sufferer’s are longing for.
I’m severely affected & already lost more than 17 years of my life.
As all the fellow patients, I’m also desperately looking forward to a treatment, but just don’t dare to get my hope high. Mr. Johnson, please ask the scientists to provide the stat with confidence level, and range of error when they release their clinic trial results.
Thank you for this update, waiting for the next one on the edge of my seat! I am curious how exercise fits in with their disease model. Is exercise just another “stressor”? Why is it a trigger for crashes? Exercise used to be a nice stress reliever for me. Now, walking more than a few blocks can trigger a 3-4 day crash. I am praying that something is available soon for our CFS community.
I think its the fact we are in anaerobic metabolism. We are not burning or using glucose properly so its like a runner doin a race way past his or her aerobic threshold. They would have PEM too. Muscles working anerobically like that.
If they could somehow stabilise glucose metabolism and aerobic cellular respiration at least we could get back some of our energy.
In research circles, especially in Australia, the pathology of this disease is increasingly understood (and has quite a bit of hard evidence behind it) as an infection caused mutation to RNA that leads to malfunction of calcium ion receptors that then leads to disorder in multiple systems, including energy transport into cells (and increased lactic acid as a side event of that), reduction in natural killer cell effectiveness, disorder of stress response and autonomic nervous system disorder. It sounds like this HPA axis hypothesis (which boils down to upregulation of stress-related receptor CRF2 in the limbic system) can be assimilated under this more widely accepted one. In other words, this change to CRF2 is “downstream” of the RNA mutation and calcium ion dysfunction. If so, this would mean this treatment would address symptoms but might not be a cure. Would you agree?
Thanks Dallas. Cortene would know better than me about how the two hypotheses integrate. I’m looking forward, though, to hearing more on the calcium ion receptor issue from down under.
How can we find out more about this compelling Australian research?
Possible 2 totally different subsets. My onset was slow without any initial infection.
HPA dysfunction does explain better than calcium ions theory why we are worse in morning…better at night….crashing under moderate stress….cant tolerate adrenaline surges or even stress from food..allergy.
I appreciate this clear overview, placing Cortene’s area for intervention in a larger context. I wonder how Davis, Naviaux, Klimas, Mella, or other researchers with a big perspective, would see this too. I am not scientifically trained, but hasn’t the old way of curing been to try to correct an illness at its source, to eliminate the incipiating factor? However, if this is not possible, or if some irreversable change has been effected, then it is necessary to try to restore health by other means. There may be other ways to restore a system to balance within its downstream effects or consequences, aren’t there? I think that Klimas’ team searches to find those potential turning points, which could not only have beneficial efffects downstream but also upstream, so to speak, as the body functions as a whole, interrelated system, on its highest level. The body systems not only reflect hierarchy but also interrelatedness, whole system features.
So maybe it is possible to change a whole system by changing something midway along, according to the hierarchical order of events—-but it has to be a particular something like a hinge which swings both ways? I am reaching for metaphors to help.
Hi, as I understand it the mutation to RNA is not reversible at this time (though gene shearing technology might help – but that’s maybe a decade away)so the only ethical and compassionate course is to treat symptoms effectively and return people to an almost normal life. Cortene looks very promising in this regard, as does a calcium channel agonist (of which there are few and, I believe, none on the market). A calcium channel agonist would work further upstream. It’s worth noting that calcium channel blockers that paradoxically improve calcium transport into cells in some systems in the body have been used with some success on people with M.E. for a while now. Nimodipine is the example that comes to mind, but it doesn’t work for everyone (research suggests about 40, maybe 50 percent of people get a some benefit from it). I am heartened by the research that has emerged over the last 3 or 4 years. It feels like we are on the edge of a major breakthrough. Long, long overdue.
Thanks Dallas. The calcium ion angle is really exciting. One doctor who wrote a book on ME/CFS used nimodipine as a central treatment. That’s the only time I’ve heard it mentioned in ME/CFS.
Dallas, I was responding to your comment in my last post and hope you’ll respond. Or anyone else with their thoughts.
Thats the first time Ive come across this theory. However, after many years of self consideration and eventually acceptance, I feel that my own thinking, attitudes and approaches to stress are actually the root cause of my illness. In fact I subscribe to the ACE (Adverse Childhood Experience) theory, which would remove infection from my own, and it seems many others’, pathogenesis. The Cortene theory strikes a massive chord with me.
Historically, infection theory seemed much more likely to provide a cure at some point. But if chronic stress (or infection) is seemingly involved, as many commenters here would seem to recognise, this Cortene development, no matter how early, seems extremely positive. Especially as regardless of the years of trials to come, the results of this first trial might be available in a matter of months, and possibly thereby clarifying the root cause finally.
Please god!
Thank you Cort as always….
Hey Steve,
My wife is trained in a counseling method that focuses on addressing ACEs, so I was very interested to read that you concluded your CFS stems from childhood trauma. Would you mind elaborating on how you reached this conclusion? Also, are you saying that the ACEs in your life may have radically shifted your body’s stress response, and that a drug like Cortene’s (if it works) could reset it?
Thanks!
Great scoop, Cort! It was feeling to me as if you had been quiet for longer than usual so I wondered what you were working on. The longer you are quiet, the bigger it is!
Well, even if this doesn’t turn out to be a drug which can stimulate a complete reset, I think the results of these trials and research may reveal more about this illness, helping with the closing in process.
Thank you!
I’m glad to hear no more animal trials on the drug. As after 28 years of suffering I wish no one including animals to suffer.
Sadly the FDA still require the LD50 toxicity test in new drugs, where animals, including dogs, rabbits, mice, etc are given higher and higher doses of a drug until 50% of the animals die from toxic poisoning. The test can last for days on end, as the animals with no other medication to ease the suffering (due to risk the medical pain and nausea relief could cause interference) slowly are poisoned to death while fully conscious. Many researchers are now saying this toxicity test is outdated and doesn’t relate accurately to human toxicity properly (as we often see human trials fail early).
Anyway ME/CFS maybe one of the few diseases that won’t require anymore animal testing and suffering especially if this drug works in short term use.
Also if Dr Ron Davis finds an existing repurposed drug. Then at least the animal testing was a past event already done. And no more suffering has to be added to this vile illness. I guess with some of us suffering for so long makes one care more for anyone else who suffers, including innocent animals.
I know some over MECFS people won’t agree as they would do nearly anything to get well. I understand that, I’m just saying I hope it’s not at the expense of forcing the suffering onto other innocent souls.
Suffering is suffering no matter what body the being is in.
Fingers crossed they find a repurposed drug soon 🙂
Thank you, Cort, for this very well-written article; this is quite exciting on many levels, but of course, it may well not pan out. We’ll just have to wait and see.
Meanwhile, it would be very interesting to hear what Ron Davis thinks about this; if you talk with him, perhaps you can ask him?
I will. Good idea.
I am wondering whether this may help to explain what happened to me when I was prescribed pregnenolone, the precursor to most of the steroid hormones, 12 years ago, and 18 years into my illness. Instead of the hoped-for improvement, it caused me to crash dramatically. I have never recovered to anything like the level I was at prior to the treatment (which was already bad enough). Obviously flooding my system with pregnenolone was not the way to go!
Hi Fay,
Can you tell me more about your crash on Pregnenolone?
I developed ME/CFS 2.5 years ago. About 3 months in, before we knew it was ME, I was diagnosed by my primary care doctor with MS based on an MRI (white matter lesions-UBO’s) and symptoms (numbness all over, weird sensations, difficulty walking, bizarre neurological stuff).
Before getting sick I was very active (running, basketball), and with the MS diagnosis and my understanding that exercise helps I tried to do a little running thinking it could help (I only managed a short distance). At the same time I was also given 3 infusion treatments of Solu-Medrol (methylprednisolone). Instead of helping, everything got much, much worse, and I ended up in an ER. I have always wondered if it was the Solu-Medrol that made things worse, or was it the running. I now know that neither was going to help.
I only tried running twice which ended in disaster each time, but I’ve always thought that my body did not react well to the steroid. A blog post by Cort from last July described a research finding that showed “the glucocorticoid sensitivity test suggested that two types of ME/CFS exist: one subset of patients over-reacts to glucocorticoids such as cortisol, while the other reacts normally.”
Also, if anyone else has a similar experience I would be interested to hear about it.
Last week I met with my ME/CFS doctor and was asked to consider participation in a Phase 1 clinical trial for an experimental drug. I am certain that it is CT38 based upon the description. First, I want to state that there isn’t a person on this planet that I trust more with my health care than my ME/CFS doctor. I just want to make sure before starting something that I won’t have a bad reaction to it.
I suspect it is Cortene :)….That is a tough choice given your history…
I had completely forgot about that blog but that is par for the course, I’m afraid (lol)
Hi Aaron,
What in particular did you want to know about my crash? It happened over the space of about 2-3 weeks from starting on the pregnenolone. By that stage I had gone from being able to go out for a couple of hours, on average 2 days a week, and cook and fend for myself, to being totally bedridden. I stopped taking it at this point and had a phone consultation with the doctor, who then wanted to experiment with other drugs to try to undo the damage. I refused and didn’t consult with him again. He is a doctor who is highly regarded in the ME/CFS community in my country.
I just wonder how many cases there are like mine, that we never hear of. I’d tried a vast number of possible treatments over many years prior to that, none of which helped in the slightest, but neither did they make me worse, and I admit it had never crossed my mind that a treatment might do that – until it did.
This sounds very dangerous to me. A lot sufferers like myself already have very low cortisol/adrenal dysfunction and lowering cortisol even further may put you at risk of developing Addison’s disease.
High cortisol is found in some people with M.E. as well, which fits with the upregulation of stress receptors which is now fairly widely accepted as being a significant part of the disease.
Yes, a friend of mine with ME has sky-high cortisol….
Hi Dallas,
could you try to explain the actual mechanics behind “upregulation of stress receptors”?
Thank you.
See the next blog – https://www.healthrising.org/blog/2018/02/17/cortene-chronic-fatigue-syndrome-hypothesis/
Re Cortisol: When measured (by saliva) four times per day, my cortisol is lowest in the morning, hovers around bottom of range in the afternoon and evening, and is highest late at night (reversed diurnal cortisol rhythms). This makes sleep difficult and light – which is when repair and rejuvenation is supposed to take place – in the autonomic NS para-sympathetic mode. Could this trap us in a chronic sympathetic (fight or flight) stressful autonomic nervous state that could keep us exhausted and stressed (or overstimulated) by even slight stimulation? Could low or deregulated cortisol also derail thyroid function and energy (since normal thyroid function requires adequate cortisol)? Could the chronic stress affect both the HPA (adrenal)and HPT (thyroid) axes? I see many suspicious inter-related factors here.
If I understand correctly, adrenocorticotropic hormone (ACTH)is released by the pituitary to trigger cortisol release by the adrenals. I once had am ACTH challenge test to test my sdrenal cortisol release in response to an injection of ACTH. ACTH and cortisol is measured both before and after an injection of ACTH. My increase in cortisol was on the low end of normal range or “adequate”.
But at a later date, I had an ACTH EXERCISE challenge test – where my ACTH and cortisol were measured both before and immediately after 15 minutes of vigorous exercise. The stress of the exercise should make both increase. Mine both decreased. I took the results of these two tests to mean that my adrenals function at least adequately in response to the demand of ACTH, but that my ACTH production is low in response to stress – which seems to suggest that either my hypothalamus or pituitary (or both) in the HPA axis are responsible for (my) low ACTH production, as opposed to a simple adrenal impairment. However I did not know how to isolate and test my hypothalamus or pituitary function to ascertain which might be impaired. Could this new drug potentially re-regulate this axis to restore a normal reaction to stress? Here’s hoping.
Dave in Sask, I am appreciating your more comprehensive comments about cortisol testing and levels, because the slap-dash way most doctors do it, with just the level at 8 am and an ACTH challenge, can’t show what is happening either during the day with blood levels, or receptivity to the cortisol in the blood, or how normal/abnormal the regulation is on the higher level of the pituitary and hypothalamus. You went farther into the whole thing. I did too, and my testing showed a normal level at 8 am and bedtime but insufficient levels during the day. That was indicative of inadequate response at the hypothalamus and pituitary level, so I was started on a very low dose of hydrocortisone. This has definitely helped me, but it certainly didn’t restore my system to normality. I still get exhausted with exertions, etc., but the low dose hydrocortisone helps.
What Cortene is aiming for and may succeed with could be more significant and precise than what low dose cortisol can do—more of a custom job—if their clinical research succeeds, which strikes me as a very big “if”. The low level homeostasis in ME/CFS has been very “stubborn”, or persistant. I applaud their attempt and hope other researchers will also look for those points/means of reversal of this long lasting illness.
Cecelia: Years ago, I studied multiple possible stages in adrenal exhaustion. One clinician/researcher had identified 8 different stages at the time, with each having a different presentation of cortisol levels at different times of the day. In many of these stages cortisol is deregulated rather than simply deficient, except in the last most severe stage when production is always deficient. This acute deficiency is granted a disease label, and treated.
If I recall correctly, too little cortisol can cause problems (including an inadequate stress response), but too much can also cause a long list of (longer term) problems. Consider, if a healthy person was resting quietly, they would have very little stress with very little need for cortisol. But if they were then startled, a spike of cortisol would be released in response to the stress, perhaps within a fraction of a second.
Supplemented cortisol may help a general deficiency, but (as you testified) does not replace the finely tuned moment to moment fluctuations of natural regulation. Conceivably, a steady state dosed level may be providing too much during low stress times of the day, but still too little during higher stress activities or experiences. Thus, if this research succeeds in restoring normal cortisol regulation – it may offer huge benefits.
If I recall, I book that I read on the “Safe Uses of Cortisol” (by William Jeffries), generally recommended cortisol in the minimum quantity necessary to relieve symptoms, with a maximum no higher than healthy physiological levels, and with a bio-identical form of cortisol being preferable to synthetic forms, but with all of these recommendations having exceptions in some cases. But – don’t trust my memory. I don’t! (lol).
A single 8:00 am blood test for cortisol to evaluate adrenal function is woefully inadequate (IMO). Some online labs offer 4 point saliva tests (early morn, noon, late afternoon, and then at approx 10 pm). Saliva tests also avoid the stress of going to a facility for a blood sample, and the actual blood draw – which can itself elevate cortisol to much higher (unreliable) levels.
Lastly, I recall reading (perhaps 10 years ago) some claims that adrenal exhaustion could be rectified, but that it was not easy and took a long time. I never followed up to assess the validity of these claims. I lost confidence in the claims when I could find no detailed explanations of the science or methodology of the alleged recovery process, after adrenal exhaustion had commenced and derailed the homeostasis.
How do you go about trialing the new drug? Where is it been tested, when is it starting?
The trial begin I believe sometime around late April/early June. The third or fourth blog in this series will give all the details.
Thanks for the article.
Jonas Bergquist has been funded by the OMF to carry out a steroid study on people with ME/CFS. I haven’t seen a list of the steroids which will be included but it would be interesting to know if the study will look at hormones in the HPA axis.
A disrupted HPA axis would presumably result in alterations in HPA Hormones.
I assume that the involvement of the HPA axis would explain the greater number of women affected compared to men.
I’ve hoped to see a study on the HPT axis. However, my knowledge of HPA/HPT is very limited. Here’s hoping that this drug trial/Jonas’s steroid study turn up something positive.
Regarding the statement that something cannot be tested currently. Genetic studies, were due to see one from the OMF this year, would possibly indicate a role for the HPA axis (i.e. higher incidence of mutations affecting HPA?). Also, check out Jonas’s presentation at the OMF symposium (September 2017); there’s a fairly recent (2012?) technique which allows the detection of single molecules. So the methods for detecting small amounts of compounds are getting better.
Finally, Neil McGregor joked at the OMF symposium that his genetic findings may be “doesn’t matter”; that certainly applies to my comments!
Is ut possible for a pharmacologist in Norway to get this drug and try it out on a severly ill pasient? If monitored by hospital?
Grete… As much as we would like to support your compassionate use, please understand that we do not have sufficient safety and efficacy data to justify this.
Cortene; I understand the lack of certanty and safetyissues. Some people though, isolated and suffering for ages has nothing (litterary) to loose. while waiting for trials, are there any simular drugs that could have some of the same effect? Big doses of benzodiazepines, immunotherapy or other?
I find this hypothesis so extreemly interesting, (maybe except explaining brainfog?) and to release å very sick person of at least some symptoms would mean the world 🙂
Never recovered from mono @ age 33 – still have hi EBV decades later. What’s interesting is w/in 3-5 yrs began having thyroid recurring goiter issues and rt lobe subsequently excised as a diagnostic tool for cancer – turns out only a cold nodule & surgery was a grave & needless mistake and since then utterly brutalized & tortured by thyroid hormone therapy.
The point? Thyroid Rx – regardless if synthetic or desiccated – has caused HPA axis and cortisol dysregulation – my Dr and I conducted tests that show my cortisol levels abnormally & significantly drop w/in 3-4 hrs of taking any thyroid Rx – the more thyroid Rx taken, the more significant the drop.
ZRT Labs conducted 1.8 miilion adrenal/cortisol tests just in the 1st 10 months of 2017, most if not all were taking thyroid Rx. Thyroid Rx is a HUGE STRESSOR & disruptor of normal HPA axis function & cortisol regulation … this is inferred by thyroid Rx mfrs in their cautionary statements NOT to take thyroid Rx if you have adrenal issues (because the thyroid Rx will cause & exasperate HPA axis and cortisol dysregulation IMO). So taking thyroid Rx may be adding to the misery of those suffering from CFS.
Something seems off. It doesn’t seem like they’re done with initial animal Tox studies. Next, a first in human study with healthy volunteers is required before any sick patients may be studied. Are these investors in touch with US or EU health authorities? An IND would need to be opened for any human testing in US.
I hope that this small company has hired some seasoned regulatory affairs professionals to liaise with health authorities.
I would be happy to answer any general drug development process US regularly questions.
As the blog noted the people in the company come from the drug development field. I don’t know anything about drug development but I can only assume they are doing this correctly.
Cortene has told me this: With the help of a physician, revered within the ME/CFS community, they will be conducting a small proof-of-concept trial, at a single site in the US. The details will follow, but the trial design is intended to obtain a rapid, objective assessment of their drug, and they will release the data as soon as possible. They reiterate that this is early-stage research and that caution is appropriate.
Thank you, Cort, for such a well written article. It was so easy for me without a medical background to understand. The energy on this article feels so promising. I’m very excited.
A physical/chemical reset of the limbic system makes sense. I have tried the limbic system reset program, DNRS (Dynamic Neural Retraining System) with temporary success but nothing permanent.
Glad to hear you got some temporary success with DNRS. I expect to try that at some point. I expect that it takes quite a bit of time and effort to see results.
I’ve had success in patients with CFS/ME using DNRS and Amygdala Retraining (another limbic system resetting program), and when it is used after triggers are removed and both mitochondria and immune system balanced, I’ve seen the results be a permanent reset. The programs take 6 months, and consistent practice, but they can work.
I’m not surprised when those programs work in some people as, from I can tell, those programs reduce the load on the stress response system and presumably reduce their hypersensitivity – which is the big problem Cortene sees. Over time the systems rebalance…
You may recall Cara Tomas’s 2017 Seahorse paper on metabolism in ME/CFS. Here’s an extract from a 2013 review article which she wrote re HPA axis in ME/CFS*. I haven’t checked the comments above but this theory re HPA axis seems to have been around for a while. I found the reference to this review by doing a Google search, so possibly lots more.
*”A Review of Hypothalamic-Pituitary-Adrenal Axis Function in Chronic Fatigue Syndrome
9. Conclusion and Further Research
HPA axis dysregulation appears to be associated with CFS. A credible body of evidence suggests a mechanism by which genetic and environmental factors (and their interaction) may serve to create an endocrine milieu which may impact on immune and vascular processes and thus putatively precipitate and maintain the symptoms experienced by those with a diagnosis of CFS. Nonetheless the abnormalities are subtle, and there is marked variation in basal and challenge tests in CFS patients and a real risk that these so-called abnormalities are simply confounds or epiphenomena.”
Thanks….If I remember correctly – as we’ll see in the next blog some of the HPA axis issues the authors believe are happening cannot be measured yet. The HPA axis certainly has the potential to effect immune, vascular and other system.
How do outbreaks fit into this theory?
The hypothesis integrates pathogen attacks into it so infections – whether occurring in the form of an epidemic (because of an usually strong pathogen?) or an isolated event – fit into it.
That doesn’t quite add up to me, I’m just not seeing it myself. An infection that affects a group of people and causes a lot of them to get CFS would mean most people would be predisposed to getting it, wouldn’t it? And why would a specific infection event that cannot be identified cause CFS in a particular group? Why wouldn’t this be occurring all the time for various infectious outbreaks? Especially since it seems only certain rare outbreaks occur? I realize there are a lot of assumptions in here, but just curious how this could work.
My idea is that there are more powerful strains of pathogens and more powerful pathogens (look at the recent flu season) and one of those sweeping through an area could produce an outbreak of ME/CFS. The Dubbo studies do show that people with more severe symptoms; i.e. a more severe illness are more prone to come down with ME/CFS. I think people who get ME/CFS are more predisposed to it.
I think it’s possible that mini epidemics of ME/CFS are still occurring. I would bet good money, for instance, that instance of ME/CFS is going to go up substantially in Houston after the Hurricane with all the mold problems.
May be a good idea to add paypal
??? We have paypal ???
I have Complex Regional Pain syndrome which affects the limbic system. I have increasing levels of fatigue as the disease progresses..anything that would help would be amazing. I would go on any trial…
One question 🙂
Why arre you the only one having information about this? I try to find out more about both the CT38, the persons invoved, and ti find more Sources. This is extreemly interesting and give hopes to so many, why havent all the ME-communities (and f.eex Ron Davies at Standfors) picked up on this?
I trust both Your autencity and Your writing but would deeply love to learn more! I also Wonder if there are any medicationas available that could effect the stress receptors? To help symptomes while we wait for this miraclemedicine? Thank you so much for sharing hope and information!
Cortene has talked with quite a few researchers and doctors. One thing that should be noted is that they’re coming at this from a different angle from most researchers. Ron Davis is focusing on metabolomics and a molecular approach to ME/CFS. He’s using a very broad swath of tests to try and figure out what’s going on. Cortene, on the other hand, is coming at this from an endocrinological approach -and finding endocrinologists who are interested in ME/CFS is not easy. Cortene is taking a VERY DIFFERENT approach from Ron. If Cortene is on track I would assume that Ron’s findings would eventually support them; i.e. what they believe is happening would show up molecularly.
From what I can tell, Cortene has talked with – or attempted to talk with – most of the major figures and groups in this field. Sometimes they got a response and to be honest sometimes they didn’t.
We should remember that this is all highly experimental. They have a drug and theory and it could succeed or it could fail. As Ron so often says, the body so often throws us for a loop so it’s very possible that this drug – which looks good – could fail. In fact, Ron says if it looks too good, it is probably wrong! I thought and I’m sure Wyller thought that Clonidine was a perfect fit for ME/CFS and it made the patients worse!
I’m afraid I have no idea about medications.
For the record – Cortene has not been in touch with Naviaux!!
Hmm… I’ve had CFS for 20 years. But last year I endedcup in the hospital with what the doctors found out was extremely low cortisol. I’ve been trying to wean off hydrocortisone, but have continued testing very low, and been unable to get off the medication. There seems to be nothing wrong with my pituitary.
I’m having severe brain fog, but how would this drug affect someone like me, Cort?
Cortene’s hypothesis suggests that the low cortisol is the result of an extended high cortisol state. They’re more interested in the cortisol receptors than cortisol itself but their goal is to reset the system, if their drug works it should be bring the HPA axis and cortisol back into balance. That’s my limited understanding of this very complex system.
I have moderate/severe M.E. and fibromyalgia. I’ve been ill for 12 years, and my daughter has missed a hube part of her childhood while watching me get worse and worse.
My fear is that to do the trial I would have to go off of all my other medications. Do you know if that will be the case?
I would travel from Israel to do this trial, but at some point I would love to see you work with Tel Aviv medical researchers. We have some of the best facilites in the world.
Israel is doing and has done good work in FM/ME/CFS! I still remember all the Naschitz studies. That was an impressive string of studies..I wonder what happened to him/her.
I imagine that the first trial of Cortene will be a small one – something that will indicate that the drug is safe and effective. We’ll learn more in about two weeks.
It’s my understanding that you have to go off many of the medications that help us function. For me it would be the ones that help me go to sleep and the ones that help me function during the day. It’s the trade off.
Is the drug PG-873637?
I wondered how this theory fits in the with the ‘something in the serum’ findings?
Hi all, this seems very exciting to me. I have started a thread to track any serotonin reduction, or other therapies we feel may work if this theory is correct. I would welcome anyone’s thoughts on this. Apparently activated charcoal can reduce serotonin. Not a permanent fix, but potentially very helpful!
https://www.healthrising.org/forums/threads/cortene-study-what-to-do-in-the-meantime.5851/
Thank you Cort for your continuous advocacy and excellent reporting. This new drug and upcoming clinical trial is exciting news that glimmers a bit of hope finally. I’ve had CFS originally diagnosed as CFIDS for near 30 years, precipated by a flu like condition, with compromised t-cells and an activated EBV. I’ve had fibromyalgia for 8 years, Psoriatic Arthritis and well like everyone here- the “list” of conditions morphed into a longer list, health declined, and multiple medications were prescribed, yet proved un-effective other than to worsen my symptoms or induce worsening in the other conditions. CFS has stolen much from too many for far too long.
Thank you to the Researchers and Doctors involved in this breakthrough moment that God willing shall be the healing catalyst for the CFS/ME population.
Thanks Michelle. We’ll see what happens with Cortene. I guess we’re all crossing our fingers…
Amen I m so glad there are still some looking to help us! We are the unbelieved and the invisible. Just look at the N I H research More is spent on breast feeding and allergies! I ve had both experiences! There are choices with both those! No choices for yourself or your family, grandkids espicially, when u turn into one big blob of pain! And I m strong, a great actor! I really try to find the best in each day!
This has given me goosebumps. Yeay!!!!!!! I got ill with ME completely overnight and very suddenly. Not a single infectious agent could be found in my blood work. The only thing happening around me was sheer STRESS. I’ve always thought that years of chronic stress wiped my immune system, but more importantly they also kind of “broke” something in my brain. To me some kind of “thermostat” or some “hardware part” just broke, and all the symptoms just arise as a result of that little part “overheating”… It’s not a great analogy but I hope it illustrates my view of how I got sick… This group’s hypothesis fits like a glove, in my own particular case, of course. Fingers crossed. It will probably take years to get the drug approved in the US, and then even longer for it to trickle down (or up!) to us here in Norway. Still, this is a huge injection of much needed hope. Thanks for sharing this wonderful piece of news. 🙂
I contacted Gordon medical center in November of 2016 (right after they published their metabolome research) to get onboard with their next study. Even after all this time they have no timeline for when their study will go down, if it ever happens.
I don’t want to wait endlessly without any hope. I am an adult, I can give informed consent and I want to try cortene NOW instead of wasting away for years with this long cruel illness.
I would like to use cortene in an N of 1 clinical trial with me as the subject. How can I set this up?
I’m afraid that’s impossible. Getting into the trial might be a possibility but this is a highly experimental drug which will be tested only under the rigors of an FDA approved trial. We should know the results pretty soon (in medical time) though.
When will next pose come? And where can er read more? Why do you know do much of5 this and is Ron Davies “aboard”?
Hug from very impatiente ???
Ok, so this is one of another disease they’ve Never been able to even identify nor find any treatments, yet, this is a tease for sure. Also, why another Canine Experiment Horrors of Animals used for Cruel Lab Experiments more like Torture? Sick of knowing these have gone on for decades & decades. Animals FEEL everything. Especially Our Domestic, actually ALL. This is no more than a Tease for another Researcher & Dr’s to get some Funding, somewhere. If Animals don’t feel, then why do they USE & Torture them for so-called results that would be beneficial for Humans? Sorry, but there’s BEEN an Obvious Connection between I believe Viruses, & Immunity Issues for a very Long time, & CFS, & EBV, Are Connected, it is beyond a Common Sense conclusion. Titers are UP & yet they rarely even test for Titers anymore. This is Unfortunately all about $..Most Pharma & Medical IS. We along with those Poor Animals that have been Subjected to a Legal Form of torture & Beyond Cruelty, already suffer for over 7+ Decades in MILLS & Shelters, & backyards & basements, & yes, LABS. Sick Better realize soon, Humanity will continue to Suffer as long as there IS Less & Less Humanity towards ALL beings, including those of Animals that DO Feel EVERYTHING, including Emotions & Fear. Yes, it’s My 2 cents & I tested over 4 Decades ago with HIGH Titers, had Mono as a teen, & Tons of Stress, as all Life does, sooner or later. As for the Immunity or lack of a strong Immune System, that Goes again, as Common Sense. Some people can DO or Eat or Drink anything, & they go on, while others Live by Rules, & do everything right, & are Not overweight, have Zero Addictions, & are sick all of the time. It is genetics, & it is a lot of Viruses they’ll never be able to Keep up with, because of Modified Foods, Meds & Diseases from ALL Over the World traveling as People & Food does, shipping here & from..there, & Our Bodies are NOT able to Fight off all the Diseases & germs & Totally Modified, as in disturbing the Natural Food processes, & so it goes, we’ve done a lot of this to Ourselves, by allowing over decades & decades Our Food & the Drugs we take, to Win out over Money..Money IS what it’s all about. Even the Drug & Over Dose “situations’, that Plague Our Country as well as many others, all because of GREED one way or another, that & the Need to Self Medicate due to being sick & Not being Able to Find a Cure for ANYTHING, much less Diseases & Viruses that continue to Morph with pharma doing nothing unless they see a HUGE Profit, Period..I could go on & on, but don’t see the Point. It’s true, every bit of it, & SO much more.
All I can do is hope that is all that I have left since being struck with this DD in 1987. I lost my career, my ability to work, my life savings and most recently my husband and caregiver. I would gladly volunteer for any trials that might forward medical advancement for treatment of M.E. as the lack of progress (and acceptance) over the past 31 years has been nil. I don’t believe there will be a cure in my lifetime but certainly believe there can be more known as to the cause and treatment of this illness. There has to be this advancement before the majority of the American medical community will acknowledge this illness and thus family, friends, and employers will follow. It is interesting that the only recognition in USA is by the insurance companies who will not cover the illness that does not exist.
Can you sign up for the trial and if so where?
Some details on the trial will be coming up in the next blog.
Hi Cort,
Once again thank you for your focus and summation of a very complex world.
I am very lucky in that I am able to work and go out with my husband weekly but I must rest at all other times. I would love to be back to my normal high energy self of 13 years ago.
I am sad that so many people’s and their loved one’s lives have been negatively impacted for so many years.
I was accepted into Nova’s CF research program in October 2017. My BP drops when standing, but my heart is normal. 13 years ago I came down with a virus, slept 6 weeks and have not been able to exercise since. I used to exercise hard about 1 hour a day and was climbing 14,500 mountains easily.
Nova Rx’d Glutathione Nasal Spray 3x/day (reduce brain inflammation and gave me 25% more energy)and Low Dose Naldrexone (pulls back excessive autoimmunue reaction) 1.5mg/day and gradually increasing to 4.5mg/day. I tolerated 1.5mg ok (ears ringing, flat emotions) but could not go to 3mg/day (severe fears, anger, sad) so I stopped all. I was back to normal the next day except ear ringing continues. In a few weeks, after I recover, I am going to go back to 1.5mg/day for 3-4 months as it takes that long to see if my energy improves.
I am looking into GABA passing blood brain barrier supplements to help me sleep which helps on everything else. I have trouble going to sleep.
I only tell you this you this in the hope it may help just one person. Nova says many have been helped with Nasal Spray and Naldrexone combo. I was very disappointed that I could not take stepped up does of Naldrexone.
I too hope that Cortene works for many.
I try to not create any more inflammation in my brain!
It’s hard to do when I feel frustrated and resentful and just plain sad that I cannot go out and play when everyone around me is able.
I am always listening to the Holy Spirit for guidance because all healings come from the source of spiritual healings and bestowed by the Grace of God. Even Cortene.
What I can do every day, is to reduce all inflammation in my body through contemplation, sleep, diet and medicine.
When I sing HU (HUsong.com), a love song to God I am filled with peace and love.
May the Blessings of God Be,
Mona
I am 54 year old female whose health basically fell off cliff overnight 2 1/2 years ago after traumatic life event. I was the epitome of health, high achiever, never sick (however Bells palsy hit me in 2012, lifetime tmj issues) yet CFS has taken me down, can’t live like this, hard to accept, would like to participate in new drug trial. Please contact me regarding this.
The Bell’s palsy is a sign of Lyme disease. We’re you tested for that?
Hi Cort, Can we get info on the clinical trials? I would love to volunteer.
Hi Terri.
The change to register in the trial will be announced with the trial has received IRB and FDA approval – probably over the next two month.s
Hi Cort, I’m a little late on reading this but I had to comment.
The HPA axis link to ME/cfs has been around for many years. If you can ignore the fact that this was published in the journal of psychosomatic research, another long term issue we’ve had to contend with far too many years!
– “HPA Axis Function in Patients with CFS
Basal hypocortisolism was first reported in CFS patients in 1981”
– Adrenocortical activity and some clinical findings in acute and chronic fatigue
A Poteliakhoff
Journal of Psychosomatic Research 25 (2), 91-95, 1981
Abstract Plasma cortisol levels were significantly lower in a group of patients suffering from chronic fatigue (CF) than in a control group matched for age and sex. Social readjustment rating scores were significantly higher in the CF group, indicating their exposure to more severe and frequent stressful experiences. The incidence of rheumatic disorders was higher in the CF group and these conditions had developed after a period of CF, suggesting that CF and the associated diminished adrenocortical activity had played a part in their causation …
My official diagnosis was mid nineties and there was information relating to that then, researchers had already realised that there seemed to be a dysfunction in the HPA axis in many patients and therefore a never ending circle of symptoms because those stress hormones have never calmed down and reset. There have been many trials in regards to addressing the dysfunction in the axis, including treating the adrenal fatigue, cortisol etc the majority of which appear to have helped to a degree in some patients, whereas in others it made little difference.
Basically for me, it’s a matter of ‘been here before’ but I still remain hopeful.
i am a male 59 year old with severe cfs and fibro started 6 years ago after 2 surgeries epigenics in ucla california has a 99 percent blood test for only fibro they are going to try a old tb drug changed to help anyone heard of this i did the test and my white blood cells are 85 percent abnormal look into this and see what you guys think also i did stem cell therapy a month ago and had 3 normal days and back to this but hoping the stem cell therapy will help and hope cortene is a major breathrough hard life and loney living this way hoping and praying this year is our year for all of us JR
Where is the article published about the research ?
if you go to epegenics in ucla california or go to fm fibro facebook has alot of information on fibro and the blood test google stem cell therapy for cfs and there are many testimonies using stem cell theapy cell network has 50 clinics doing this to help let me know what you think not sure only been 5 weeks on stem cell they say takes 3 months to show much cfs is the worst for me
A warm hello to all,
Any more news (at all) on Cortene?
Has BHC released any info?..I know it’s early..Doesn’t hurt to ask?
Haven’t heard anything lately. I assume they’re still on track for a trial in the next month or so.
Here’s an update from June 13: https://cortene.wordpress.com/2018/06/
The other thing I noticed that has never been mentioned is most are slim not over weight
Anyone else noticed this
This is the first research that makes sense to me. I’ve been dealing with CFS for forty years and when I try to explain it, I can only say that it always feels like at my some point (during times of stress) a switch in my body flips off and I begin to live on adrenalin, rather than normal sources of energy, until both the Adrenalin and my body are exhausted.
I have a 28 year old daughter who has worked through many protocols with CFS Specialized practitioners with no positive changes. Actually, she is now bedridden. PLEASE advise me as to the protocols involved in getting her into the new larger trial. She is an excellent candidate, as she has exhausted other protocols and their efficacy can be used for comparative data, (should it be requested). Willing to do whatever it takes to give her the possibility of having her life back.
Thank you.