

“We have a huge problem and a major crisis on our hands.” Avindra Nath – on long COVID – at the conference
“I think the tools we’ve applied to study ME/CFS can now easily be applied to long COVID as well. And vice versa. What we’ve learned on long COVID is going to benefit us in ME/CFS,” Nath – Live Science

Avindra Nath stated one possibility is that the virus – or proteins from the virus – may still be present in the long haulers.
(This summary was taken from notes).
Dr. Avindra Nath gave the keynote talk at the 2021 IACFS/ME conference. Nath leads the clinical arm of the National Institute of Neurological Disorders and Stroke (NINDS). He’s been steeped in the central nervous system effects of post-viral disorders for decades and it shows.
The truth is – and Dr. Nath has referred to this before – that we’ve had a huge problem on our hands for quite a while. In a recent paper, Nath asserted that “Undiagnosed neuroinflammatory diseases carry a huge burden with devastating consequences”, and decried how unprepared the medical system is for a virus that affects the central nervous system. He called COVID-19 a “crisis for neurology”.
On the other hand, neurologists – perhaps the most resistant of all specialists to ME/CFS – have been something of a crisis for ME/CFS patients for a long time. It’s good to see a respected and influential neuroscientist fully embrace chronic fatigue syndrome (ME/CFS) and long COVID.
The “crisis” is not just about ME/CFS – it also concerns all the other post-infectious illnesses that have been virtually ignored by the research community for decades. The SARS-CoV-2 virus is simply demonstrating in spades what’s been known and ignored for years: that infections can, even after they’ve been “resolved”, have severe long-term consequences. Nor is it just the post-infectious aspect. I’ve been told that the NIH has put pathogen research on the back burner for years as well. Now that we’re seeing COVID-19 spin-off numerous post-infectious conditions, perhaps that will change.
Nath referred to a fascinating paper by Taquet which demonstrates: a) the many different effects infections can have; (b) how dangerous the coronavirus is; and (c) the kind of type of illuminating research that is pouring into the long-COVID field.
Taquet compared the neurological and psychiatric records of 236,000 survivors of COVID-19 to people who had come down with influenza and other respiratory diseases. The study showed that the coronavirus produces the most complications, influenza is next, and then come other respiratory infections.
The huge study validated the idea the infections, even after they are resolved, can have long-term consequences. That was eye-opening but what was really startling was how much more apt the coronavirus was to produce complications even compared to the flu. The image below compares some of the neurological complications produced by the coronavirus (red line) and influenza (blue line).
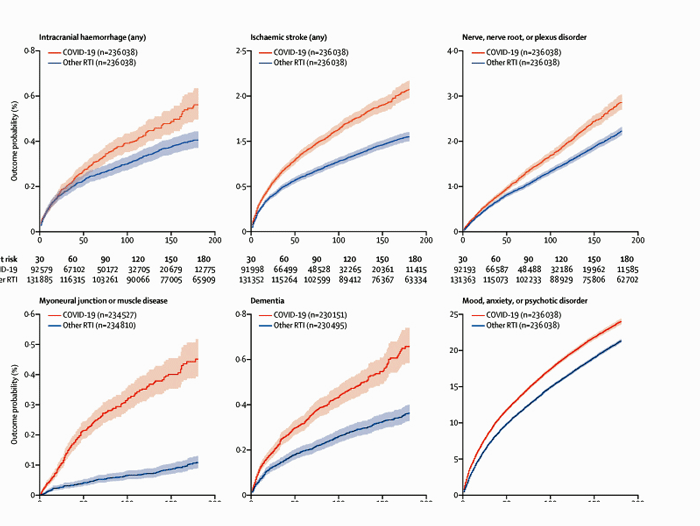
The flu can produce plenty of complications, but the coronavirus produces far more. Coronavirus – red line, flu – blue line.
Note that while the rate of psychiatric disorders is pretty similar in the COVID-19 and influenza patients, the rate of muscle disease jumps up dramatically in COVID-19 patients.
With the first tranche of the NIH-funded long-COVID studies focused on large cohorts, we should be seeing many studies like this, including those that cover more complications. We’ll be looking to see what the prevalence of ME/CFS, FM, IBS, POTS, EDS, etc. is over time, but it’ll also be fascinating to see if the rates of autoimmune disorders like multiple sclerosis, Sjogren’s Syndrome, and lupus increase as well. We should also hopefully be able to see if different infections produce different post-infectious states. All this data should be in the electronic medical records.
Nath then shared an email from the husband of a formerly healthy mother who took her life a year after long COVID left her in enormous pain and unable to sleep. It’s remarkable that in this day and age our medical system had nothing to offer her. (Hopefully, the NIH’s HEAL effort – which is designed to produce better pain drugs – will help.)
Nath believes that long COVID is probably caused by either immune activation and/or viral persistence.
The dysautonomia that’s been showing up is likely due to damage to the endothelial cells lining the blood vessels which control blood flows and inflammation, sympathetic nervous system activation, and low blood volume.
The fact that plasma exchange and steroids can really help some patients indicates the role the immune system must be playing. Nath’s description of what appears to be happening in the immune system was a highlight for me. I’ve never heard the immune situation in long COVID or ME/CFS described in the way he did, but it appears to fit both diseases.
Nath reported that a technique called “single-cell sequencing” found “extremely aggressive” monocytes in the cerebral spinal fluid of COVID-19 patients with neurological issues.
Nath reported that the T-cells appeared to be exhausted. (Impaired T-cell metabolism has been found in ME/CFS). With the adaptive arm of the immune response hurting, the immune system turned to its early appearing innate arm to help out. The problem with that is that the innate arm of the immune response is like a bludgeon compared with the fine-tuned responses (antibodies, T-cell clones). Consisting of mast cells, monocytes and macrophages, dendritic cells, the complement system, and neutrophils, the innate arm produces a ton of inflammation and is hard to turn off once it gets going.
The use of the single-cell sequencing technique highlights another benefit from the large amount of funding going into COVID research. Besides the huge studies we’re going to be seeing, we’re likely going to see a lot of cutting-edge technology being brought to bear on long COVID.
Instead of examining a variety of cells types such as PBMCs at once, single-cell sequencing involves assessing individual cells using “optimized next-generation sequencing (NGS) technologies”. A PubMed search didn’t bring up any instances of “single-cell sequencing” in ME/CFS.
Vascular injury is certainly occurring in COVID: congested blood vessels, microhemorrhages, white hyperintensities (also found in ME/CFS) all indicate the blood vessels are affected. Nath has found three different types of vascular injury in COVID, and focused on the brainstem, a brain organ that has shown up in spades in ME/CFS.
The leaky blood vessels Nath found in the brains of COVID patients. His explanation of how that occurred made a new connection. Nath’s discovery of activated blood platelets touching the endothelial cells lining the blood vessels suggested that endothelial cells had activated the platelets. That’s interesting, as Bindu Paul and colleagues proposed that mitochondrial damage to the endothelial cells plays a major role in long COVID and ME/CFS. Once those platelets are activated, they can produce inflammation and blood clotting. (Nath has yet to find virus in the central nervous system and doesn’t believe the virus is present).
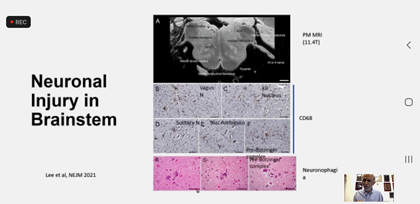
A muddled reproduction of the brainstem image Nath marveled at.
As only a neuroscientist could, Nath then marveled at a crystal-clear picture of the brainstem in COVID that had been produced. If my notes are correct, the brainstem shot suggested microglial activation was causing the loss of neurons there. Here, again, we have another potential connection between COVID and ME/CFS, as both the microglia and the brainstem are of great interest in ME/CFS.
When it came to potential treatments, Nath again veered into ME/CFS territory. After stating that antivirals might be a possibility, Nath suggested an immune treatment regimen that has been discussed (but perhaps not implemented) in ME/CFS: you knock the innate immune system down and pump the adaptive immune system (T-cells and interferon response) at the same time. One of the reasons that this treatment approach has not been taken in ME/CFS may be because of the difficulty physicians have in justifying it, but with the amount of research going into long COVID, the studies will show up that will allow that to happen in long COVID, and eventually in ME/CFS.
Nath then finished up fairly early in the session, which was good, as the lengthy question and answer period was perhaps the most interesting part of it. It was an interesting section as Nath showed no compunction about shooting down a number of sacred cows…
Q & A Period
The Gist
- Nath called long COVID “a huge problem and a major crisis”.
- A huge UK study found that COVID-19, influenza, and other respiratory infections all produced long-lasting complications in some, with COVID-19 producing more than the flu, and the flu producing more than respiratory infections. We should see many more studies of this size and ilk over time.
- Nath believes immune activation or viral persistence is likely the cause of long COVID. The coronavirus could be persisting in the stomach lining or elsewhere, and it could be pumping out proteins that are activating the immune system.
- Citing a finding of “extremely aggressive monocytes”, Nath suggested that T-cell exhaustion may be causing the immune system to compensate by jacking up the efforts of the early acting, highly inflammatory, innate immune system. It may be necessary to enhance the later-acting adaptive side of the immune system, while knocking down the innate immune system.
- Congested blood vessels, microhemorrhages, and white hyperintensities (also found in ME/CFS) all indicate that a complex problem involving the blood vessels is present. Nath believes damaged endothelial cells lining the blood vessels are activating the blood platelets, which then produce inflammation.
- While the impact on the brain can be widespread, Nath focused particular attention on the brainstem – a brain organ of interest in ME/CFS as well. Microglial activation there appears to be damaging the neurons. Nath has been unable to find evidence of virus in the brain.
- During the Q & A, Nath proposed that because of the vanishingly small amount of protein found in them, the coronavirus vaccines are far safer than the virus itself. He suggested that people who fare poorly with the vaccines would likely have done far worse with the virus.
- When asked if the glymphatic system, EBV reactivation, epigenetic alterations or autoantibodies were involved in long COVID, Nath said all of those are commonly found in central nervous system diseases. He warned about giving too much significance to EBV reactivation or the presence of autoantibodies.
- The ME/CFS Intramural Study was closed with the advent of COVID-19, and no more patients will go through the study. They are analyzing the results of the study now. The results of that study will be compared with the results of the long-COVID study, which is employing ME/CFS-like patients.
Are mast cells a major player? Dr. Peter Rowe noted that mast cells are key drivers of innate immune response and reported that he was regularly finding high histamine levels in his long-COVID patients. Nath acknowledged that he doesn’t know a lot about mast cells but agreed it is an important area.
Is epigenetics behind long COVID? One person asked if epigenetic changes were causing long COVID? Nath agreed there probably is a host genetic component but that it’s polygenetic; i.e. it’s spread across many genes, and we need more advances in genetics to get the full picture. He also asserted that epigenetic changes are expected as epigenetics plays a role in all diseases.
Is the glymphatic system involved? Ray Perrin got a similar answer when he asked whether the glymphatic system was involved in long COVID. Nath said yes, but that glymphatic problems have shown up in every central nervous system disease.
What’s happened with the intramural ME/CFS study? I was itching to get some results from the intramural ME/CFS study, and so asked about that. Nath gave the (somewhat) disappointing, but not surprising, news. When COVID-19 came along, recruitment into the ME/CFS study stopped – permanently. Nath said that they’d put a “decent number” of patients through the study, and that the investigators were meeting weekly to analyze it. They hope to produce one large publication, followed by a series of smaller ones.
In response to an email, Nath reported that the ME/CFS intramural study is living on in the form of an intramural study of long-COVID patients with ME/CFS symptoms. The results of that study will then be compared with those of the ME/CFS study.
What about false recoveries? Some patients recover completely, and then complain of symptoms weeks later. Why is that? Nath, who had a great deal of experience with post-infectious diseases, suggested a couple of possibilities: the virus might have gotten knocked down but was still present, and was gradually building up and driving an immune system reaction… or the virus was knocked down and it took a while for autoantigens and other parts of the immune system to act up.
Are viruses present in the brain lesions? Dr. Chia wanted to know if viral RNA proteins were present in the brain lesions Nath assessed. Nath clearly tried hard – he used multiple methods to look for pathogens, and failed to find any.
Could the coronavirus be persisting in the gut? Could the virus be present in the gut lining? Nath loved this question. Absolutely the gut could be a reservoir for pathogens.
Is EBV reactivation a big deal? A doctor reported that he has 3 patients with EBV reactivation. Nath called the EBV situation complex but noted that every neuroinflammatory disease causes EBV reactivation. At least once a week he gets a notice that a spinal tap has found EBV in it. It’s very hard to sort out whether the EBV reactivation is significant or not. What we really need is a drug that blocks EBV and then see what happens.
Could virus-related proteins be causing an immune response in long COVID? Nath said this question was music to his ears. Even if HIV has been knocked down, HIV related proteins are showing up. The same is true of measles. While Nath didn’t mention it, similar hypotheses have been advanced regarding EBV, enterovirus and HHV-6 proteins.
Are autoantibodies a big deal in long COVID? Nath was not high on autoantibodies. He said you have to be very careful about autoantibodies. You find hordes of autoantibodies in all central nervous system diseases, most of which are not causing any problems.
Update: Nath recently said:


 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!



Disappointing ‘progress’…
Yes, this is actually alarming, very alarming. Is this damage permanent?
What damage are you referring to?
yes, and now me/cfs looks totally shot down, yes, only inflamatory me/cfs or if i am wrong with my brain, even only covid long haulers who develop me/cfs. feels like being throwing out the pure Me/cfs.
Nath is a neuroscientist – that’s the perspective he’s coming from. His ideas about long COVID, though, fit very well with what we know about ME/CFS – I see our understanding of ME/CFS invigorated by the work being done on long COVID.
With regard to no more people going through the intramural study I wish that wasn’t so but was not surprised. Once they starting analyzing all the data, I didn’t think they would add more people (and more data) to the study. They apparently have a huge amount of data to analyze already.
Plus, a similar ME/CFS/long COVID hospital study is underway.
ME/CFS research like most research got halted by the pandemic and now long COVID research is getting a ton of attention. In the end I’m confident that it will work out for us. Already we see so many potential similarities between the two.
Please clarify – I see lots of progress in understanding what’s going on COVID and long COVID.
may i ask, when will the intramural data from ME/cfs will be published? yes, for me, it feels like a punch in my stomach that they do no further testing and take rigourus more people with ME/cfs. ok, covid long haulers and ME/cfs but it is not the same. just like lyme or GWI is not the same as me/cfs. i mean, excact the same. but thank you for your answer!
I agree – it sucks! This and the severe ME/CFS patient study by the OMF were our really deep dives. Maybe another six months and we would have. AL lot of people went through the first phase. I don’t know how many people went through the second (more crucial) phase. Nath said that a “decent” number of patients went through the study.
Nath said that several papers would result – probably one large one and several small ones. He said five groups are analyzing the data and are meeting weekly.
I imagine that Nath and his colleagues can only do so much and that is going to the COVID and long COVID patients. That’s way it’s been for the last year and a half.
The pandemic just got in the way as it has with everything. It gives and it takes away. I’m sure it will “give” much more to ME/CFS than it will take away.
I think it will work out…I would be really surprised if the long COVID ME/CFS-like patients were dramatically different than the ME/CFS patients. These are all, I believe, people with relatively mild onset who just didn’t get better and often got worse.
We’ll see what they got from the ME/CFS group and then the long COVID group.
Thank you Cort for a great overview. I agree with you. The findings from this Covid research will have a positive ripple effect on our understanding of ME/CFS.
I am talking about CFS progress, Cort, not Covid progress. There’s no guarantee that findings are transferable.
You have been talking this researcher and others up for many years, and the delivery on research seems very slow.
Regardless of whether covid was around or not.
A European researcher will solve CFS, the Americans are asleep at the wheel.
Poor delivery relative to the size , wealth and resource of the USA.
Matthias, I understand the frustration that we’re not further along and I don’t have any idea when we will have good treatments but every year the field does grow.
Take energy production. Ten years ago we had very limited findings on energy production. Now we mitochondrial studies, exercise studies, metabolomic studies all pointing to problems with energy production.
Yes, it has not lead to a treatment but the delivery is slow for everyone with ME/CFS. The field is however, study by study, gathering evidence and moving forward. Sometimes it’s hard to see because, I suppose the final product – a treatment – has not shown up but I see researchers building on past findings and getting results. We simply need more of them and with long COVID hopefully we will.
I would be shocked if the long COVID findings aren’t transferable to ME/CFS and don’t spark new insights into it. Why wouldn’t they? We know that ME/CFS is, in part, an amalgam of post-infectious triggers. COVID is simply one more trigger.
Hi Konjin, ‘
When I asked him earlier this year he said he expected this fall – which is coming up. Let’s hope.
Witch kinds of steroids should be used if someone does get sick from the vaccine!
Good question, because I surely am having issues. One week after vax, got shingles, now bad relapse, fatigue, legs not working, what is going on here.
indeed good question because i am after more then 3 months still suffering a lot from vaccines. it was as if all my muscles disapeared and my brain (the rest of it) get shot.) still no recovering. desperate!
I was first prescribed a medrol dosepak then another and when that failed, we tried a Prednisone taper starting at 40mg decreasing by 10mg every 5 days. When that failed, we tried it again for 10 day increments. I did well on 30mg-40mg but each time I dropped to 20mg, I would face progressive worsening of symptoms. Not sure where we go from here. I was stable for 4 months prior to getting the 2nd pfizer shot.
Ugh, more random anitvax comments. Quoting Mark C’s apropos comment from a few blogs ago: “Comments like these from conspiracy theorists should really be removed. To blog readers who come here to learn more about ME/CFS, they only serve to foster the suspicion that ME/CFS patients are mentally ill.”
More to the point: thanks for the seminar summary Cort. My me/cfs symptoms prevent me from attending online. Glad I can get the gist here.
To ‘another Anne’
Your compassionate concern for your fellow PwME who are suffering is touching.
I’m confused as to why ‘another Ann’ is characterising what appears to be a perfectly rational discussion of post-vaccine symptoms – common in ME/CFS patients as Cort’s large patient survey showed – and potential treatments to alleviate them, as ‘anti-vax’ comments.
We know that for PwME, PEM and even long-term relapses can be triggered by any physical challenge, and since vaccines that often cause high immune system activation even in healthy people are clearly a physical challenge, so why can we not discuss this here, without being labelled as ‘anti-vax’?
Getting the virus itself would of course be an even worse potential relapse trigger for us, so no-one is saying ‘don’t get the vaccine’! But surely it’s wise to be prepared, and to know what treatments might be available. Dr Nath himself suggested a steroid treatment, and this discussion follows on from there.
Late to the party. Another Ann; I’m not anti vax – I’ve had both doses of Pfizer. But I’ve developed long covid symptoms since late May, approx 3 weeks after my first dose. My doctor prescribed cbt (I believe this is common for me/cfs). I had a negative covid antibody test (n-protein) at the start of august, and symptoms have been ongoing. They got much worse in early September following the cold that was going around, and I am currently unable to work (hardly able to function as a parent and husband). Being gaslit by doctors and family and friends is bad. I’d have thought someone else presumably suffering the same gaslighting would have a bit more sympathy for those finding themselves in such an awful situation. If you think it’s difficult getting a doctor to believe you have me/cfs, imagine trying to convince them that the vaccine had actually caused your condition.
Matthias,
At the IACFS/ME conference, at least 2 researchers/clinicians, I believe, said that ME and long covid “are the same thing”. What long covid researchers learn will surely extend to ME.
I am thankful for the individuals Cort has been writing about. They have been (and continue) doing research in a difficult, maligned field with very little funding. That’s the prime reason for slow results.
Another reason for slow results could simply be the problem of the disease itself. There are other major diseases – like Alzheimer’s – that have, in contrast, received a massive amount of funding , for decades, and yet still do not have significant results.
The ‘rona vax is the kill shot. It causes the creation of more spike protein everywhere that takes over your body. Look up antibody dependent enhancement (ADE). Its why the scientific studies have shown there can never be a coronavirus-family vaccine; the animals all died in the studies starting over a decade ago.
This is just ludicrous.
As Nath – head neuroscientist for NINDS at the NIH hospital said – the protein is only present in the body for a short time. I’ll take his word over yours that the spike protein is taking “over your body”.
I seem to see quite a few coronavirus vaccines that are working really well.
In the long discussion that went viral online a couple of months ago between Bret Weinstein, Robert Malone and Steve Kirsch, Steve was a firm believer in Fluvoxamine as an off-label cure for both “Long Covid” and vaccine side-effects that are similar to “Long Covid”. He stated that he was funding a randomized control trial for it. The video is more than 3 hours long but packed with informative discussion. There is a timestamp list available, Fluvoxamine comes up at 46 minutes, and then from 1 hour 49 on to about 2 hours 5 minutes, is worth long Covid sufferers listening to.
SSRIs? sigh…
“Serotonin and depression
The marketing of a myth”
https://davidhealy.org/wp-content/uploads/2015/07/2015-Serotonin-and-Depression-bmj.h1771.pdf
New independent study confirms risk of weakened immune system and ADE reactions after vaccination against COVID-19. Especially Pfizer.
https://www.medrxiv.org/content/10.1101/2021.05.03.21256520v1
Preprint
Over a 1000 unvaccinated people a day are dying in the US Gijs…
Here’s the conclusion from the paper itself (rather than the abstract).
The conclusion talks about the innate immune reaction to the coronavirus…..which might be enhanced. Since it’s absolutely clear that the vaccines are protecting against hospitalization and death, it’s obvious that they aren’t harming our ability to fight it off – which makes the innate immune response question either moot – or indicates that they are helping rebalance it.
As Nath pointed out the adaptive immmune response appears to be exhausted – and the innate immune response gets exxagerated in COVID-19. It sounds like some rebalancing could help.
What is interesting is that some ME patients and some long covid patients feel normal again after vaccination. This could be explained by the reset of the immune system. But in the longer term, we still don’t know what the vaccine does.
There are authoritative virologists who fear an increase in blood clots and strokes. We shall see.
Those 1000 deaths a day in the US, how old are they on average? And were they overweight or had underlying diseases? In Israel, 95% with severe corona who are hospitalized have been fully vaccinated with Pfizer.
But it’s a rotten virus. Don’t get me wrong, I am not against vaccination, but I am critical of this new mrna vaccine. We just don’t know enough about it yet in my opinion. You are taking a risk and everyone has to weigh that up on the basis of good information.
The problem is that the information is not complete and is only really known after years. I am for vaccination but the risk if you have ME is different than if you are healthy. Choose from 2 evil. Hard choice.
Luckily, there are non-mRNA vaccines available. Nath also said the “recovers” from long COVID after the vaccinations were not sticking in his experience. They feel better for a time and then relapse. Still, it’s a clue.
Gils – re your comment about the high rate of hospitalisations of fully vaccinated people in Israel:
95% sounds like an awful lot, but am I not right in thinking that with Israel’s remarkably high rate of vaccination, the TOTAL number of hospitalisations with Covid might still be very small compared to countries where vaccine availability or uptake is relatively low?
If almost everyone there is fully vaccinated, 95% may be a tiny number of actual severe Covid cases.
With every infection outbreak you see an increase in patients who have chronic complaints. Think of Q fever and many more diseases. Because Covid-19 is an infectious disease and almost everyone will get this disease sooner or later, you will also see an increase in long covid patients with an ME-like syndrome.
Actually it is nothing new except now all eyes are on it . Finally, the doctors see this disease. Only the disability insurance companies don’t want to see it.
There are virologists who predict that covid will become a mild cold virus. let’s hope so. Because vaccination will not make covid disappear either. And vaccinated people can also get (seriously) sick.
Can someone help me out with the implications of what Nath just said. Essentially, people have permanent damage in their nervous system and will never be normal again. And therefore, ME is not reversible. What does this say to the researchers working on ME? Why are they not on all this together. I am utterly floored by this piece.
Have I missed something- didn’t see it as negative ? More that striking commonalities have been identified in LC and ME – so further research will benefit us all 🤷♂️
Agree that this is far from negative. Nath is very optimistic that they will make progress. Yes, there is damage to our nervous systems. At this moment, we don’t know how to repair that damage. Does that mean we never will? I’m quite hopeful on that one.
We’re already getting really interesting stuff on the long haulers and this is just the beginning.
Matthew Durcan,
Research will benefit, and I am eager for it. But they are coming up with some challenging things to repair. This is frightening. Even the suggestion Nath had regarding what to do with the immune system, this is no piece of cake, you know. I am alarmed. I wish he offered more in potential things to correct these problems and to treat them
Yes, it’s not a piece of cake and it’s never been a piece of cake. People with ME/CFS are well aware of that. We seem to have a proclivity for weird findings and for falling between the cracks.
But who knows what they will find? Bruce Patterson already thinks he’s figured this out. Think how many eyes are now on this problem….More money will probably be spent on long COVID this year than in 30 years in ME/CFS. That’s a lot of brain power.
I agree, and remain hopeful. Thankyou for your great work Cort
I agree – it’s nothing new – the big difference is that it’s everywhere and all eyes are on it. It does seem to be causing more complications than usual, though.
Hi Cort,
Here’s where they talk of ‘damage.’ Nath talks of dysautonomia due “damage” of the endothelial cells. B. Paul talks of ‘mitochondrial damage” to endothelial cells. And Nath is talking about various vascular injuries in the whole brain area. Certainly, lots of research is moving along. Fortunately. But this is looking very challenging if there is this kind of damage. Or am I wrong? I want to be wrong! Thanks for all your hard work. You deserve some huge rewards.
I think it will be challenging but I don’t see that as a problem. I’ve had ME/CFS for 40 years. I don’t expect to roll over and die. I think it’s going to take some work, some hard thinking, some really good studies – but I’m very hopeful that good stuff is going to come out of it.
One thing to keep in mind – they’ve never been able to find the kind of damage in the brain that they find in say MS or Parkinson’s. Also note that some of these findings came from people who died of COVID – and won’t reflect what’s happening in long COVID. I probably didn’t make that plain enough.
To momentarily change the subject;
Thought I’d share the latest news on the NHS ME/CFS treatment guidelines—which have been postponed because of disputes:
https://www.bbc.com/news/health-58241864
https://www.nice.org.uk/news/article/nice-pauses-publication-of-updated-guideline-on-diagnosis-and-management-of-me-cfs
I thought the PACE study and subsequent NICE guidelines were refuted, but evidently not entirely…
Now regarding Nath’s comments; perhaps one should not think in terms of ‘damage’ but of ‘changes in function.’ The body has many interdependent systems and a great capacity of adaptability and self healing. Researchers are still not entirely sure of the underpinnings of both Covid and ME/CFS. Maybe we should be a bit more hopeful about all of this. Research WILL certainly not stop. We WILL make progress–eventually.
Anyway, think of all the man made toxins in our environment and added chemicals in what we consume. Are people getting so upset about those as much as we are about vaccines? What’s the difference between a slow death and a speedy one? I know many of us are frustrated but kindly don’t let that frustration contribute to continued fatigue.
And on a personal note, my Colchicine trial was a disaster. Third dose, 1/2 of prescribed amount, I thought I was being poisoned–horrible stomach pain, nausea and migraine. Almost went to the ER.
Hi Nancy B, in relation to the revised NICE guidelines – they were formally agreed by the NICE guidelines committee and were officially signed off. However the Royal College of Paediatrics and Child Health (RCPCH) and the Royal College of Physicians (RCS) then objected saying, apparently, that they wouldn’t implement the new guidelines. So NICE have ‘paused’ the guidelines, which goes against their own procedure. Everyone is on to it and there’s a protest on the 20th September outside NICE’s headquarters in London. NICE are looking very foolish but they haven’t made another statement as far as I know. It’s everywhere #MEAction have a petition going to NICE today, with I think around 15,000 signatures. Anyway look at any of the ME/CFS organisations – they’re all over this.
@Tracey,
Thanks for the more detailed update!
The unfortunate thing about big studies like this is they have a tendency to multiply like rabbits–even if they are wrong. And it can take a long, long time to correct mistakes. It bothers me that researchers often do not directly consult patients about how they experience the results of these (pronouncements) studies.
INFLAMMATION: Stated as the root cause of severe reaction to sars2
Overweight causes inflammation, as well as many others.
It is my belief we will all get or have already gotten this bug. There was a group study testing for sars2 and they were surprised at how many showed titters without knowing of infection.
We must do everything to strengthen our immune system and not be stressed by the buzz.
After 14 years I am STILL waiting for just one official list of ME/CFS symptoms to include “neuroinflammation”. Can’t find one so far. In the old days I wore a chemo cold cap for my poor head. I am greatly improved (by using supplements to improve my immune system) and now remember to take Aleve when a relapse comes on as the one symptom that has continued over the years is clearly neuroinflammation!!
I am looking forward to a Covid vaccine booster as I continue to believe that the Moderna vaccine has improved my ME/CFS symptoms. I use a Oura ring and can see clear improvements from April on. Second dose was April 1st.
Looking forward to studies looking into whether vaccination helps those with Long-Covid. I know about a local waitress whose long-covid symptoms of lack of taste and smell reversed after she was vaccinated.
may i ask wich supplements you take for your immune system? for me, the pfizer vaccination was a disaster. spoke to gp and she said (with other people), some things went wrong for some.
glad your moderna vaccines helped. i have an oura ring to and many measures just declined (geeting worse)
Health minister of Israël Horrowitz:
“This is simply because, in terms of its effectiveness, the vaccine is valid only for a period of five or six months,” Horowitz told Channel 13 television. “After about half a year, you have to get a third dose. Otherwise, the vaccine loses its power.”
I’m curious if vaccinated people are willing to get a third shot of Pfizer, Cort are you taking a third booster of Pfizer after a half year?
The delta variant of the coronavirus is killing almost 1300 people a day in the US and it’s causing more people to be hospitalized and die than the alpha variant and at younger ages. People with ME/CFS already had a lot of trouble with the alpha variant.
I did fine with the Pfizer shots and am looking forward to getting the protection the booster shots will provide.
Spironolactone blocks EBV. But it also has other effects which can be helpful for ME so I’m not sure how you would separate those out. I have much more trouble with POTS and relapses without it.
Thanks for the write up Cort 🙂
Dr. Nath, please don’t forget the many people including myself that you have been treating for severe COVID vaccine injuries. There are many 1000’s of us that have been injured. By ignoring these injuries, it prevents us from getting medical care, as the medical community is uneducated about these severe neurological vaccine reactions. In addition, research needs to be done to find out what is causing these reactions. Please acknowledge these vaccine reactions and educate the medical community so we can get the help that we desperately need.
Yes, we have a family member who spiralled downward after the second Pfizer. Six weeks now, and a relapse like I have never seen. It is hard to understand what has happened. One doctor proposed Ivermectin, which we are not interested in. We are in no way anti vaccines. In fact, our family member with severe ME, insisted on getting the jabs But now what do we do?
I wish you and your family the best Helena. In Europe 21000 people died after vaccination and 20 million people are sick from it. Vaccination (mRNA vaccine) isn’t the solution for COVID-19. There is comming a new vaccin for India a DNA vaccin wow… works for 66.6 percent to the Delta variant. In a report of the English government says: 2/3 of the deaths with the Delta variant are vaccinated people. So 1/3 are not.
Sorry, not 20 million but 2 million have problems after vaccination.
Please provide links to your assertions. Your figure does not jive with what studies assessing the long-term effects in over 20,000 people with the Pfizer vaccine have found. The Pfizer vaccine has just been fully certified
https://news.yahoo.com/pfizers-covid-19-vaccine-just-134028656.html
Once again for everyone. The fact that 21000 people died after getting vaccinated means nothing because people are dying of all sorts of things all the time – things which have nothing at all to do with vaccinations. They are dying from heart problems, cancer, lung problems, accidents, Alzheimer’s, suicide, etc.
The real question is whether more people are dying after getting vaccinated than people who didn’t get vaccinated. The very, very large studies that have been done indicate that this is not happening and really there’s no reason to expect that it would happen because vaccines, in general, have proven to be very safe over the years and have prevented millions of deaths. We wouldn’t have 1200 people needlessly dying every day in the US if everyone had gotten vaccinated.
The NIH recently reported that 140,000 deaths in the US have been prevented by the vaccines.
https://www.nih.gov/news-events/nih-research-matters
Whether or not someone with ME/CFS decides to get vaccinated because of fears of a relapse, the idea that many people are dying from the vaccines is simply not true. It is clear, though, that many people are dying from the virus, that many people are being hospitalized, and that many more people will be coming down with long COVID.
https://www.globalresearch.ca/20595-dead-1-9-million-injured-50-serious-reported-european-union-database-adverse-drug-reactions-covid-19-shots/5751904
Not all people die from COVID, but with COVID from underlying diseases as well.
What i like to see is a good control group of unvaccinated people.
you should not downplay the consequences of vaccination. The same goes for the virus and its consequences. It just strikes me that many people act as if vaccinating is completely harmless. They have little empathy for the victims. This is called collateral damage.
Of course, vaccinations against COVID will also save lives, but how much is difficult to determine.
By the way are there previous comments deleted (in other topics)?
Thanks for providing that but it’s exactly what I mean. They’ve decided that anything that happens in the period of time after a person has been vaccinated counts as a reaction. If you have given everyone in Europe a glass of milk and assessed what happened after that you would have seen all sorts of people dying and falling ill etc.
As I’ve noted several times the vaccine trials all had large control groups – -which is precisely what that report you cited does not have. The Pfizer trial contained 43,448 people of whom 21,720 received the vaccine and 21,728 got a placebo.
https://pubmed.ncbi.nlm.nih.gov/33301246/
I am not downplaying the issue of harm. I do recognize that some people with ME/CFS are having trouble with them but I’m more responding to your assertions that many people without ME/CFS are dying or getting really sick because of the vaccines. That’s just not true.
No comments that I remember regarding the coronavirus have been deleted because of their content. We’ve only deleted a handful of comments over the years HR has been in existence.
The study you cite has limitations. You cannot make a precise calculation of how many deaths have been prevented by vaccination.
You can’t just compare the data I gave you to a glass of milk. There is a significant relationship. And the actual number may be much higher. Because much is not included in the database of side effects. There is often underreporting Whether 21,000 deaths after vaccination is a lot is up to you to decide. Even if it was half, I feel very bad for those people.
The study you give with a control group concerns the pfizer vaccine. Where safety is guaranteed for only 2 months. This is not what I mean. You would have to follow this control group for years to be able to make statements.
Unfortunately, I see in other topics that a number of substantiated comments about COVID are no longer visible. Including myself. Maybe coincidence. But disappointing.
Gijs – I looked up your comments on Health Rising. You’ve commented 493 times on HR’s blogs. That’s really good! I appreciate the interest – but not one of your comments has landed in HR’s trash or spam folders.
You’re rejecting the results of large multiple studies for your belief that something is really awry. Because we cannot precisely state the number of deaths prevented from the vaccines – that is rejected as well.
I don’t know if we’re going to get anywhere with this.
I believe you are honest but at some topics don’t see all my comments anymore -:) what went wrong? I don’t know 🙂
No problem.
you gave me studies with data just like the facts in the database I gave you. Both are subject to interpretation including your studies. That’s how it works in statistics.
They haven’t gone anywhere. You’re just mistaken. If we had been blocking people for spreading false information about the vaccines you would have been gone a long time ago! 🙂
They’re very different. One is a very large rigorously controlled trial – the other is a database that contains almost no statistics. There’s certainly no probability statistics which are the core statistics used in the drug trials. It’s simply reporting numbers – which are pretty meaningless.
Sorry Cort, maybe I didn’t look closely. I’ll look again. Apology 🙂
I don’t think our views differ that much at all. Only I look at the negative side of vaccinating with mRNA vaccines and you look at the short-term positive side of vaccination.
False information is not for me. I always substantiate my insights and opinions with data or studies as well. The latest insights show that the natural immune system works much better than vaccines. Only you must have had the disease first.
https://www.nature.com/articles/d41586-021-01442-9
https://www.news-medical.net/news/20210801/Antibody-responses-following-SARS-CoV-2-infection-more-potent-than-vaccine-elicited-ones.aspx
No one has a monopoly on wisdom. Time will tell. And let’s hope this virus goes away soon. I think so, just like the Spanish flu.
I cannot walk after the first AZ vaccine (5 months later), nor can I concentrate (brain fog) so am not getting the second dose. Ive been advised to get the second dose regardless, but then again I was advised to do graded excercise therapy for my M.E too…
What im saying is that it’s best to ignore the noise and listen to your own body, which as someone suffering from M.E you will have plenty of experience doing. The noise surrounding these issues is tiresome, and sadly, ideological (and American.) As a European it’s clear to see from the outside that the sensitivity that surrounds asking a valid question or expressing reservation about the vaccines is a residue of their recent political upheavals ( i.e. ‘deplorables vs the rest..). Take the good stuff from American research and ignore the culture wars there if you can.
– – If you didnt react badly to the first, then get the second one, obviously. —
I hope Dr Nath hears you and does as you ask. I just watched an interview you did it sure seems these things are connected. We can only hope research interest helps us all. I have a long list of DX starting with chronic fatigue depression of course who wouldn’t … functional movement disorder, multiple chemical sensitivity(not dx with mast cell activation I did not seek the specialist as seeing doctors has become troublesome due to reactions and fatigue … several bad reactions to several drugs. As you can see we have some of the same things and your description of symptoms I could have written. Seems there is a connection. After 4 decades of this it sure is getting old. Having a doctor say they are disappointed in the medical help they get in some way makes me feel a tiny bit better. I am sure your attempts to describe your situation are much more clear than a lay person with brain fog… I am sure your description will help other doctors understand. Thank you for being willing to put it out there I think it will help us all.
How many yrs on the intramural study into ME? 20 (!) patients.
Sorry but not sorry … what have they been doing for us over there?
20 patients and now it stops bc of covid.
His remark abt Aabs. Really?
CNS GPCR Aabs may be common in neuroinflammatory diseases (ME, Alzh. …) but they DO have consequences.
A lot of them. Depending on which GPCR (s) is (are) affected.
Get the idea the ME study was more of a PR (keep them calm) thing & now Covid emerged and all of a sudden Nath is an expert?
If he was an expert he himself wld have made links with ME more clear.
Instead, you Cort, added those links in this article. Not him.
I’m sorry but Nath, NIH, NINDs etc can NEVER make up for the time they lost not investigating ME seriously.
They can act now as if they were doing good research … they weren’t.
And now it’s like “covid is being studies, move over ME”.
If they would immediately & public ally point to ‘seen this before in ME’ ok
But that’s not the case.
He doesn’t convince me at all.
Example:
“Could virus-related proteins be causing an immune response in long COVID? Nath said this question was music to his ears.
Even if HIV has been knocked down, HIV related proteins are showing up. The same is true of measles.
While Nath didn’t mention it, similar hypotheses have been advanced regarding EBV, enterovirus and HHV-6 proteins. then.”
Music to his ears?
Did he ever look at (viral) biopsies in ME patients? Viral proteins?
Knowing our immune systems have the TH2 shift. Knowing EBV & HHV6 are still candidates. Knowing NK function is off while leukocytosis (w/ etc ) & high B cells & cytokines are so often found in ME.
If this is truly his kind of ‘music’? Why not do sth about it? With 200 instead of 20 patients. Blood & biopsies. All you need to look into it further.
I don’t know what the number is but its far more than 20 patients (where did you get that number from?)
“His remark abt Aabs. Really?” – Yes, that’s his experience, and given his extensive experience in central nervous system diseases, I for one, am listening to it. He said something about physically tying the autoantibodies to the tissue in question – which is clearly beyond the pale for ME/CFS.
“If he was an expert he himself wld have made links with ME more clear.
Instead, you Cort, added those links in this article. Not him.” – That’s true, and the lack of ME/CFS was disappointing for me. It’s disappointing as well that the study proceeded so slowly. I would have thought it would have been complete by the time the pandemic struck.
I think the concentration is going to be on long COVID for quite a while to be honest but I also think, in the long run, it’s is going to open doors.
Did you see the Biology of Fatigue Workshop is hosting which has a pretty heavy ME/CFS presence? https://web.cvent.com/event/4630788d-baa2-47fb-af01-0f5b8d0d92bd/websitePage:645d57e4-75eb-4769-b2c0-f201a0bfc6ce. That’s a step forward for us and for long COVID.
I was thinking today how the NIH could make up for almost 4 decades of neglect and I concluded that they can’t. It’s not just ME/CFS – it’s FM, it’s migraine, it’s IBS, its POTS – it’s every disease with similarities with ME/CFS. It’s too much to make up for.
Let’s hope, though, that at some point, they will clearly acknowledge their mistakes. That would help.
Here here Elise. As I say higher up, I’m not convinced by Nath.
But I hope I am wrong and he comes out with some meaningful findings.
Neurologists are the absolute WORST. And it’s not hard to understand why. We know so little about the actual brain, so their defensiveness is off the charts. They’re taught they know everything, so it’s quite a blow to their ego to have to admit they actually don’t (cognitive dissonance). And when that happens, the easiest route out is to project their ignorance onto patients and blame them.
By the same token, in contrast, emergency room doctors are typically the best. They have to be, because they need to save lives, often on the spot. That’s been my experience, at least. Endocrinologists typically aren’t so great, either, unless it’s a known condition like diabetes, and as for immunologists, forget it, lol. They know about as little about the actual workings of the immune as the neurologists know about the brain.