

“It’s the first real solid attempt to come up with some biologic mechanisms for long Covid,” said Dr. Steven Deeks.
A large and complex long-COVID study was recently published. It’s one of the first major studies to follow large numbers of long-COVID patients and test the heck out of them as they become ill. This study is just the beginning – we will see many more of its ilk – but it provides a view into a different magnitude of study than we’ve seen before.

This large long COVID study had many moving parts. Even bigger ones will follow.
The ME/CFS studies that attempted to get at ME/CFS as it was being produced were limited by funding constraints. It was frustrating to see Leonard Jason, for instance, struggle to get funding from the NIH to dig into the hundreds of samples of college students who came down with ME/CFS in order to try to get at the disease at its earliest stages.
Some of the long-COVID studies coming down the pike are of another world entirely. Huge patient sets combined with ample funding will give them the opportunity to understand long COVID in a way that was impossible with ME/CFS.
For the people with chronic fatigue syndrome (ME/CFS), the biological similarities in key biological areas (exercise physiology, gut) thus far, between long COVID and ME/CFS are closer than I would have expected. This study simply adds to them, and in a new and very intriguing way, as it reaches back into some of the very first findings in ME/CFS.
The Study
The new study, “Multiple Early Factors Anticipate Post-Acute COVID-19“, involved researchers from over a dozen universities, pharmaceutical, and other companies. The fact that Gilead and Merck were amongst the funders suggested the drug companies, in a way they never have been in ME/CFS, are interested in finding treatments for long-COVID patients.
The study assessed autoantibodies, proteomics, and metabolomics in the blood and guts of 209 COVID-19 patients from infection to 2-3 months later, with 457 healthy controls. They then corroborated their findings in a group of 100 long-COVID patients.
One strike against the study for people with ME/CFS – only about 30% of the patients had not been hospitalized.
Results
Autoantibodies to the Fore
With autoantibodies appearing to contribute to long COVID in about 2/3rds of patients, autoantibodies won the prize for the biggest potential factor.
This isn’t the first-time autoantibodies took center stage in long COVID. An earlier paper suggested that a massive production of unusual autoantibodies occurred early in the infection.
This study did not survey as wide a number of autoantibodies but found that, of the 4 factors identified, autoantibodies appeared to play the biggest role in most patients. Autoantibodies – antibodies with the potential to attack or affect the body – were common both during the initial infection and when long COVID had taken hold.
The fact that the long-COVID patients tended to have mature (class-switched) autoantibodies at the onset of infection suggested the long-COVID patients’ immune systems had become activated before they were infected with COVID-19. In fact, the authors noted that a specific class of hyperactivated B-cells (AtM) was reminiscent of what’s seen in lupus – an autoimmune condition.
One wonders if a similar kind of incipient autoimmune state is present in those who later come down with ME/CFS or another post-infectious disease. The case has been made that ME/CFS, with its female prevalence, heritable component, and infectious onset, is an autoimmune disease.
A recent Japanese ME/CFS B -cell study may be suggesting something similar when it states, “B-cell responses in ME/CFS are directed against infectious agents or priming antigens induced before disease onset.”
The authors also proposed that anti-interferon a2 autoantibodies may have opened the door for long COVID by inhibiting the production of antibodies against the coronavirus – thus giving the virus more time to wreak havoc. These antibodies may have also exacerbated the illness by ramping up inflammation.
Back to the Future I: Cortisol Takes an Early Hit
It was remarkable to see two factors – cortisol and Epstein-Barr Virus (which dominated the early research efforts in ME/CFS) – show up in one of the first really large long-COVID studies.
The study found reduced cortisol levels in COVID-19 patients still suffering from viral/respiratory symptoms. The low cortisol levels were associated with steroid treatment – which suppresses inflammation – at the first two time points, but not at the third time point, suggesting that longer-term cortisol suppression was a function of the virus – not the steroid treatment.
Many studies have assessed cortisol in different ways in ME/CFS and FM (fibromyalgia) without, it should be noted, resulting in a standard treatment protocol. Interestingly, different kinds of reduced cortisol levels have been found in fibromyalgia and ME/CFS. Problems with cortisol clearance that produces higher cortisol residues in FM appears to inhibit the production of cortisol, overall. People with ME/CFS, on the other hand, tend to produce lower cortisol levels in the early morning hours.
Dr. Klimas’s modeling studies suggest the HPA axis plays a predominant role in ME/CFS and Gulf War Illness and the treatment protocol which came out of them employs a drug (mifepristone) designed to reset that system.
Let’s hope that this finding holds up in future studies and researchers finally really dig into what’s kind of been a black box for ME/CFS – the HPA (hypothalamic-pituitary-adrenal) axis. It makes total sense given its connections to the stress response, the immune system, and the metabolism that it’s involved, and many studies cite irregularities, but the field has never been able to: a) either capture and explain what’s going on in a satisfactory way; or b) provide any real treatment options.
Back to the Future II: Epstein-Barr Virus (EBV) Shows Up Again

Thirty-five years later Epstein-Barr virus is still being studied in ME/CFS.
Maybe you thought the coronavirus was going to be the whole show? Not at all. If any virus knows how to exploit a weakness it’s Epstein-Barr virus (EBV). EBV is one of those herpes viruses that just hangs around and around. Bruce Patterson said the coronavirus is the most complex virus he’s seen, but I suspect many pathologists would nominate EBV. This huge and complex virus has been linked to over a dozen diseases, including several cancers, and is probably the chief trigger of adolescent-associated ME/CFS. Almost 35 years after the EBV connection showed up in ME/CFS, research into it continues.
One of the authors reported that EBV reactivation appears to play a role in about a third of long-COVID patients, and was associated with the later development of fatigue and memory problems.
EBV is another factor that’s kind of shrouded in mystery. It’s too enticing a possibility to give up, and EBV ME/CFS studies, in particular, fairly regularly emerge, but there’s no consensus on the role EBV reactivation plays in this disease. Should this study’s findings hold up, a deep dive into EBV’s effects in long COVID could produce tremendous results in ME/CFS.
On the EBV note, Solve ME recently reported that a landmark study published in Science suggested that EBV may now be considered “the leading cause of multiple sclerosis” (!). Solve ME also noted that Moderna will soon begin Phase I trials of an mRNA EBV vaccine.
The Gut
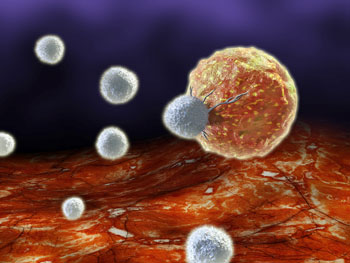
Cytotoxic T-cells in the gut got excited about something as long COVID emerged.
The study suggested that the gut gets involved early as well. The most intriguing finding was an expansion of cytotoxic (killer) T-cells that showed up – not at the infection – but months later as long COVID took root.
The authors suggested that a latter viral shedding of the coronavirus in the gut had woken up the T-cells but noted that the T-cells primed to attack the cytomegalovirus had also woken up.
The Gist
- A large study examined immune functioning in COVID-19 patients as they came down with long COVID over 2-3 months. Note, though, that only 30% had not been hospitalized.
- The study found four factors found early in the infection which appeared to push people towards having long COVID. Three of those factors have shown up in ME/CFS, and two of them dominated ME/CFS research early on.
- Having high levels of activated autoantibodies during the early stage of the infection appeared to put the most people in danger of coming down with long COVID. Most interestingly, the high levels of activated autoantibodies don’t appear to have been caused by the infection but were there before the infection started – suggesting the long COVID patients may have had an incipient autoimmune reaction going.
- Epstein-Barr virus (EBV) reactivation appeared to push about 30% of the participants toward long COVID. EBV has been studied in ME/CFS since the mid-1980’s.
- Low cortisol levels – another early avenue of study in ME/CFS – were also associated with the appearance of long COVID.
- The activation of killer T-cells in the gut as long COVID set in indicated that gut changes occur early as well.
- Four distinct pathways – all originating early in the infection – that lead to long COVID were found. The authors proposed that small immune alterations early in the illness morphed into major changes as the illness proceeded – making the origins of the ill obscure – unless it was studied in its earliest phases.
- Even though this study included 300 long COVID patients, the authors noted that bigger studies are needed. With the NIH following 900 plus long COVID cohorts across a dozen or more institutions, those studies are coming.
- Given that many things could have popped out of this study, it was remarkable to see two old ME/CFS themes (EBV reactivation, low cortisol) and one recent one (autoantibodies) quickly pop out in one of the largest longitudinal long COVID studies to date.
Bystander Activation
While the gut PASC patient had high levels of undifferentiated but activated T-cells early in the illness, other PASC patients demonstrated early specialized activation of the T-cell. All those undifferentiated but activated T-cells caused the investigators to ask if a “bystander” pathogen had become activated as well.
It turned out that cytomegalovirus (CMV)-specific T-cells had become activated as well. Somehow, the coronavirus had turned on T-cells specifically designed to take on CMV! As no actual CMV upregulation had occurred, the authors proposed that the CMV-specific T-cells were involved in the gut problems found in long COVID (PASC).
Four Roads to Long COVID
Next, the authors attempted to correlate symptoms with the gene expression of the immune cells as long COVID appeared to assert itself. They uncovered 4 quite distinct immune signatures indicating different biological types of long COVID were present:
- pro-inflammatory signatures in monocytes, cytotoxic effector signatures in CD8+ T cells and NK cells, and memory signatures in B cells.
- CD4+ T cell signatures, M2-like (anti-inflammatory) monocyte signatures, and a plasma B cell signature.
- Intermediate type.
- naïve-like T- and B-cell signatures, and resting NK cell signatures.
The germs of those activations stretched all the way back to the infection; i.e. the authors could chart how a person’s immune status at an infection pushed them towards a specific long-COVID endpoint. People with EBV reactivation, for instance, tended to end up in the intermediate group. Interestingly, they could not do the opposite; that is, they could not infer from end-state what the original immune state of the patients was – they needed to have that initial data to do that.
This is often what happens, though, when you perturb a very complex system. Small changes in the beginning that can produce enormous impacts over time get lost as the system evolves. One silver lining to the seemingly never-ending pandemic, though, is that researchers should have no trouble following patients from the murky beginnings of their illness’s conception.
The authors proposed it’s essential to do so, and noted how important it is for other “long” conditions such as Lyme Disease and post-ICU syndrome (but no mention of ME/CFS (???)) be exhaustively studied from their early beginnings. (That’s a very nice recommendation and let’s hope that the NIH decides to provide the funds necessary to do that.)
Most of the focus was on ways to hopefully stop long COVID in its tracks by using antivirals, boosting cortisol, and immunotherapy. Dr. Deeks, who was not part of the study, though, sounded as if they could go further.
One of the authors reported that EBV reactivation appears to play a role in about a third of long-COVID patients and was associated with the later development of fatigue and memory problems.
Dr. Deeks offered some hope for the future.
“If these pathways get confirmed, we as clinicians can actually design interventions to make people better. That is the take-home message.”
Conclusion
This large and complex study was packed with formerly hospitalized COVID-19 patients making it remarkable, indeed, to see several longstanding areas of interest in ME/CFS (cortisol, EBV reactivation), as well as some “shortstanding” ones (autoantibodies), pop out.
This is the kind of large study that we hardly ever see in chronic fatigue syndrome (ME/CFS) or fibromyalgia (FM) but even this study with its 309 long-COVID patients is going to seem like a piker compared to the NIH-funded studies that are underway. The NIH is currently funding over a dozen centers, each of which may be following as many 900 long-COVID patients over 4 years.
That’s a good thing as even this very large study, which followed over 200 patients (and then corroborated its results in another 100 patients), wasn’t, the authors said, nearly large enough. That’s apparently because the authors captured only a small part of the condition’s complexity.
These huge studies and the rigor with which they are being produced, though, means they should, as this study did, pretty quickly produce some nice, juicy leads. With the NIH sitting on about $600 million – that’s $600 million dollars – of unspent long-COVID funds, it has ample resources to build on the findings its initial studies produce.
As the last blog noted, the fact that we know the trigger and can precisely measure what happened when the gun, so to speak, when off, and that massive amounts of funding are available, suggests that long COVID – as complex as it surely is – may be a disease that’s just waiting to be solved.






Well written, Cort! This is an important development.
So many ME/CFS patients have issues with low cortisol and herpesviruses, but doctors or so reluctant to test for and treat them.
Wonder if HHV6 is also playing a role?
Insightful article! I have a question. Might the fact that high levels of activated autoantibodies appeared during the early stage of the infection indicate that a long covid patient already was suffering from an autoimmune disease before the covid infection? Does anyone knows this?
They may possibly have had tendency towards developing one.
Thank you, Cort!
My take on this study is that it is quite a disappointment for those who want to understand the “ME/CFS subtype” of Long Covid.
As you mentioned, the cohort in this study is heavily skewed toward severe cases, with 71% hospital admissions (most on ventilatory support, a lot of distinct pre-morbidities…) . Also, this study looks at a 2-3 month timepoint – we know from ME/CFS and also many LongCovid patients that this is when their problems only started to surface.
Also, the auto-antibodies they tested do not include GPCR-aabs (besides some IFN-aabs they use a lupus type panel, for whatever reason), and this is clearly a missed chance – after all, GPCR autoimmunity is one of the central hypotheses for ME/CFS inception, and other teams showed that GPCR aabs are most relevant in LongCovid, too: https://pubmed.ncbi.nlm.nih.gov/33880442/
So these results will tell us a lot about what happens to patients with preexisting chronic diseases who are admitted to a hospital for a severe viral illness. It will tell us rather little about the typical ME/CFS patient (or the ME/CFS type Long Covid patient). In other words: The few patients in their cohort that will later go on to develop ME/CFS may be too far and in between to be recognizable in this study.
(Of course: I hope I am wrong !)
Thank you Cort for starting to unpack arguably the most complex article in ME/CFS+LC history.
Agreed with Herbert; the level of relevance to many ME/CFS (and likely LC) patients is TBD.
This past week has been a whirlwind of contradictions for me:
This report with its broad range of time-sensitive predisposing factors in contrast to the Nature Communications report homing in on two robust (time-invariant) predictors — IgG3 and IgM — of who will get or did get LC.
And the Xenon lung MRI study showing respiratory exchange failure in the lung; which seems on the surface to run counter to the iCPET work (implicating peripheral oxygen extraction as the core defect) we have found so compelling.
I didn’t realize that so many were on ventilatory support and I agree that what we really want are non-hospitalized patients but how odd that this very ME/CFS-like profile showed up in them! That suggests that the post-ICU crowd or prolonged critical care group as Dominic has suggested may be quite similar to ME/CFS.
https://www.healthrising.org/blog/2019/09/05/neuroendocrine-dysfunctions-and-treatments-in-prolonged-critical-illness-relevance-for-chronic-fatigue-syndrome-me-cfs-and-fibromyalgia/
Ron Tompkins and Ron Davis have also proposed that a process similar to which occurs in severe trauma may be occurring in ME/CFS. That would all be good news as it would broaden our research possibilities greatly.
The plot thickens. We shall see:)
I read a paper from that study just recently
(Tompinks et all on trauma)
two very interesting points from it:
The way the immune system gets activated from trauma is very similar, if not the same, as in ME/CFS
A non-viral, non-parasitical, non-pathogenic event triggers the immune system just like a viral/parasitical/pathogenic one
– ain’t that interesting?!!
Doesn’t that make you wonder about the immune system?
and point number two,
What was observed in humans, was not observed in rodents AT ALL
no correlation, no correspondance.
Which also – doesn’t that make you question any study on rodents and extrapolation to humans?
Rodents are quadrupeds. I wonder how this affects their systems, to keep homeostasis blood flows/oxygen/glucose to the brain, etc
as opposed to humans
bipeds
gravity
etc
Isn’t this amazing…
“The way the immune system gets activated from trauma is very similar, if not the same, as in ME/CFS”
Tompkins certainly knew trauma after working on it for 15 years. Most people do recover from trauma but there are those who never really do – and they look just like people with ME/CFS.
Just stunning, really.
Also traumatic brian injury [TBI] and Me/CFS sooo similar… there are rehabilitation specialist that take the same approach to both.
Isn’t it interesting that the immune system is getting activated by events other than pathogens?
Does it pique your curiosity?
Perhaps there is another way to look at the immune system. It may even reframe the whole auto-immumity thing of the body getting confused and attacking itself
( I am one of the opinion that it is doctors/scientists that are confused about how the body works…)
Re: EBV – I thought this was ground already covered, by the ME/CFS researchers… another red herring.
The trauma link is indeed interesting! Also post sepsis syndrome seems to widely overlap with ME/CFS.
I may have botched something here…
The response to trauma was the same as the response to endotoxin
(which presents as flu-like symptoms, which, in ME/CFS, that is considered a later PEM symptom.. so that endotoxin leaking from the gut into the blood stream could be a component)
Easy enough – take the trauma study and compare with the long-covid studies, see if it is the same pattern of immune response etc
– – – – – – – –
Here is a paper for you:
“This study presents interferon-alpha (IFN-α)-induced persistent fatigue as a model of CFS. IFN-α, which is used in the treatment of chronic Hepatitis C Virus (HCV) infection, induces a persistent fatigue in some individuals, which does not abate post-treatment, that is, once there is no longer immune activation. This model allows for the assessment of patients before and during exposure to the immune trigger, and afterwards when the original trigger is no longer present.”
“Persistent fatigue induced by interferon-alpha: a novel, inflammation-based, proxy model of chronic fatigue syndrome”
https://www.sciencedirect.com/science/article/pii/S0306453018301963
In every infectious disease, in every trauma event, in critical care patients, in heat stress, – there is this percentage that goes on to have this response that is no longer tied to the initial insult.
What is this percentage that is constant across the board?
Unfortunate that the NIH is choosing to fund studies turning up EBV as the ‘culprit’. I would not be surprised if an EBV vaccine will turn up soon, is what I thought. Then I saw Moderna is working on one…
If everyone gets EBV – why doesn’t everyone get me/cfs / MS / the cancer associated with it etc…?
Thanks again Cort for a great article 🙂 My son was exposed to EBV and then later developed MS. I was exposed to it as a teenager. I had some mystery virus in my forties that triggered ME. Maybe West Nile, or can the flu trigger ME? Do they know which viruses are most likely to retrigger EBV? After 14 years of ME, is it worth getting tested for the most suspect viruses? Do you have a list of what they are? I’m housebound so every Dr visit can trigger a relapse. I have no idea if it is worth the risk when there isn’t a treatment approach yet as far as I can tell. Very cool article. Can’t wait to hear what comes next.
ME is caused by enteroviruses and yes, they still show up in the tissue after 14 years. A straightforward way to diagnose ME is SPECT.
Would they even know what to look for on a spect scan? I had one and have tested positive for Epstein Virus and they never put it together . The spect scan was a scam!!!! They asked me all my symptoms first rather than look at my brain scan and conclude you have xyz which we see here in your spect scan! Such a con game ! Doctors today don’t do preventative medicine but wait until your in the disease and throw big Pharma at you that rarely solves the problem . Most think your a head job when you ask questions or want to be pro-active in your health! But maybe your Spect scan nuro-doctors were different??? I’d be interested to hear. Thank you!
Maybe some of the funding for long covid research could be applied to early identification of new cases? So many people are unaware of their condition and will suffer without informed help.
Getting the corona virus/”Covid” can activate EBV and cytomegalovirus,
AND
agreeing to being vaccinated with the covid shots (and the boosters) can also activate EBV and CMV. The vaccines, per a medical article that I found in one of the comments here on Health Rising, with a direct link to the article, in Covid article (THANK YOU to who posted that comment with Link!!), specifically and ESPECIALLY can reactive any toxic mold exposure that you have had in your life. This toxic mold exposure for many months made me extremely ill, thus also called “CFS” symptoms (one BIG cause of CFS!).
My doctor used this article’s reference to all of this in my Medical Exemption from getting the Vaccinations and Boosters(sss). I may or may not need this article, as the Courts are axing the “mandates” ……. for now.
Thank you for this great website, and also to the reader who posted that link in the Commends in a covid article!!
My friend agreed to be vaccinated, then changed his mind at the last minute. Is he in danger of reactivation of EBV?
Can you share the link too please?
Yes please. I would like to see the link to show to my doctor as I am significantly worse 10 months after my covid vaccines.
I too would appreciate the link. I’m in my late 70’s and have been pretty active and healthy until I had a reactivation of EBV a couple of years before the pandemic. Last winter I had a debilitating reaction to the first pfizer vaccine…increased brain fog, muscle/joint pain, fatigue/weakness; so decided to forego any additional vaccinations. Only comment from the dr. was the vax is pro inflammatory and perhaps I have an undetectable autoimmune condition….
With regards to the Covid vaccine and ebv reactivation, I had a very different experience. I physically felt better after getting the Covid vaccine. Would love to get an EBV vaccine at some point in my lifetime. Fingers crossed on that.
Any chance you can share these links? I would be as Thankful as you were.
I had read about this story few days ago, but you break it down so simply and with insight as to how it affects our community. Thank you for that Cort.
If you read Osler’s Web, the path to Chronic Fatigue Syndrome began when Dr Paul Cheney observed a striking phenomenon of reactivated EBV in a cluster of teachers at Truckee High School, not far from Incline Village.
This defied the limitations of EBV, as this is not supposed to happen in adults.
Particularly not after a flu that went from person to person with a 4-7 day lag time, as the incubation period of EBV is over a month.
Dr Cheney immediately suspected EBV was not the cause, but Chronic Epstein Barr Virus Syndrome was the leading hypothesis of the time.
He set about gathering evidence to disprove the CDC’s “EBV dominant” theory.
For this purpose, Dr Cheney assembled case studies of 19 people who fit the parameters of CEBV Syndrome, but were entirely negative on the Nichols EBV serology test, showing they (we) had never been exposed at all.
The CDC accepted this compelling evidence. Abandoned the EBV theory, and coined a replacement. Which they called “Chronic Fatigue Syndrome”
In essence, the last 35 years of thinking of EBV as “The cause of CFS” or “The trigger for CFS” belies and ignores the fact that this syndrome was coined on the basis of an illness that had no EBV at all.
Thanks for bringing this up. My kids with ME do not have any evidence of ever having an EBV infection. They match the original Tahoe group more closely, except for becoming ill as children (age 10/11).
The disparity between EBV which causes B cell proliferation and the Lake Tahoe outbreak which had such a catastrophic LOSS of B cells that they were undetectable by cell flow cytometry was explained almost immediately by the discovery of HBLV. “Human B cell Lympho-Tropic Virus” which lyses B cells: “A Cytopathic Effect”
This was the virus which scared the CDC into coining the Holmes committee and creating the new syndrome.
Just as chronic active EBV was logically called CEBV Syndrome, the new syndrome should have been named HBLV Syndrome.
This could have prevented a lot of confusion. But as we all know, the CDC was trying to disguise the Lake Tahoe outbreak so they declined to clear up the confusion.
HBLV was renamed HHV6A
Which Dr Bhupesh Prusty has recently implicated as being very effect at mitochondrial fragmentation.
If the syndrome had been named for what it was, this work could have been done long ago.
Nothing new here. Don’t forget the enteroviruses. And even more possible infections. So we have more autoimmune and reactive infections. It seems to me that there is a problem in the immune system. Kind of HIV-like illness. But more arbortive.
If these were ME/CFS studies I would probably have the same reaction – same old same old – will not lead anywhere butlong COIVD is a condition which has 1.15 billion dollars devoted to at the NIH alone. It’s a different world.
Cort, I remember you said that with “Reeves New Direction”
About 2003, wasn’t it?
Notice that every expression by Koroshetz, Fauci, Nath and others is that nothing was ever established in ME/CFS except some kind of post exertion fatigue.
Don’t you see what they are doing?
Making longcovid the “new ME/CFS” in order to put both ME and CFS behind them forever.
I have always thought ,when trying to figure out why the human response to these viruses is so varied,
That The RECEPTION COMMITTEEwhich greets the virus could be a clue .My stab is these are .
genetics
stress levels environmental allergens i.e.chemicals moulds etc.
Hi Cort and everyone,
I need to apologize for my funny request to keep, as much as possible, an answer simple and short. I’m in the severe group, can concentrate for a very short time and so I don’t understand, nor can I delve deeper in order to understand (though I’ve tried many times, but finally gave up and gave in), the applications and implications of much of the terminology.
I would appreciate if someone could help me out with simplified answers to:
1. EBV reactivation – is it something that will show up in a regular blood test? Say, EBV IgG test? So that if one had pre-CFS IgG results and then a higher IgG value post-CFS onset it would indicate reactivation?
2. Is it a chronic condition? What I mean is that if someone has had CFS for years, would this reactivation appear only at the onset of CFS or all the way through?
3. Would the immune system irregularities (autoantibodies, T-cell etc.) show in a standard blood counts and/or in the serology section?
4. Are the different markers all necessary? Or is it possible to have, say, EBV reactivation but normal cortisol levels?
Many thanks!
Hi Daria
Thanks for asking your question as a physician who treats ME/CFS Long Covid and has a personal journey I can share my experience:
1. EBV YES you can order a standard blood test HOWEVER you need to know what to order and how to intepret. EBV igG will show if you have ever had it EBV in your life- ie could have had it as a kid and its positive- this is why most docs discount it. IgM is only acute or acute reactivation is shows up 2 weeks after infection and dies down after 2 months. You need to order EA-D early antigen D. This is a decent marker or chronic reactivation. NOTE; even ‘complete EBV panels do not contain EA-D must add it onto the lab order!!! Unfortunately we do not have any excellent tests widely available for chronic viral reactivation. This EBV panel plus EA-D is actually the best in my experience. CMV, HHV6 there is no way to assess reactivation outside of history and treatment. I DO test for IgM and IgG for these as a standard panel to get an idea of what a person has in their past. If there is NO IgG reaction then its not a reactivation. The Higher IgG is a subject docs debate technically the levels of IgG do not indicate reactivation HOWEVER, if the symptoms add up and the levels are increased I do not hesitate to treat ‘as if’ and see if the patient improves. “treat the patient, not the lab”
2. IS CFS and EBV chronic?? Let me know if this answers your questions or not- EBV once you have it you always have it. It lies dormant in your cells. Most people this is not big deal- we all have MANY viruses in our bodies its called a virome and this population changes based on environment just like our microbiome does. Reactivation means the EBV has had a party in your cells and is replicating like crazy and likely altering your immune system and sugar production in your mitochondria- making you feel tired. You can treat the EBV and it can go back into remission. Some people have auto remissions – most likely due to again environmental factors shifting and making it not so hospitable to EBV party-time. The EBV are super super opportunistic and will replicate when you are under stress from emotions, infections, trauma etc. I find most of us with CFS/ME who have EBV ( I do NOT believe we ALL do) have EBV flares throughout the years. Recognizing what this can feel like and how to treat it in YOUR BODY ( different folks handle different treatments) can be a HUGE key to getting your health back and CFS/ME in remission. So EBV can show flare up and down in the course of a CFS experience.
3. Auto-antibodies and T-cells: the answer is yes and no- there is not a direct auto-antibody test that I know of that is helpful for diagnosing root causes of CFS/ME or Long covid at this time. if anyone reading this does- please chime in! For T-cells there are some T-cells you can test for and these can show amounts and tendencies ie do you have enough, too much but not super specific as I think you are as asking for- not my super strong area of expertise, I have not found it to date very helpful clinically to run these panels. I know many lyme docs do. So others please add in here if you have something to chime in!.
4. Short answer: Yes, you can have EBV reactivation and normal cortisol. I personally see and treat CFS/ME as a complex condition with multiple root causes. AND altered cortisol is often but NOT always part of the picture. If it is part of the cause for you its important to address it as it will promote healing once it is in balance.
Thanks Doctor so much for helping out 🙂
This 2018 article describes polio vaccine as creating a vacuum for enteroviruses to fill and cause disease.
https://www.papolionetwork.org/uploads/9/9/7/0/99704804/poliovirus_causes_chronic_fatigue.pdf
90% of Americans get EBV before the age of 35, but once you have had it, it lives in your cells forever where anything that suppresses immunity can cause a reactivation. This is also true of a whole range of herpes family viruses: CMV, HHVa and b; HHV7; HHV1 and 2.
The famous “bubble boy” who was born with no immune system died when a bone marrow transplant from his sister infected him with EBV.
Patients undergoing antirejection treatment for transplants and/or chemotherapy can also have herpes virus reactivation.
https://hhv-6foundation.org/transplant-complications/hhv-6-is- the-predominant-reactivated-virus-other-than-cmv-in-post-transplant-cyclophosphamide-associated-infections
It is tiresome (after nearly 40 years) to read that researchers who should clearly know this are making the great discovery of “elevated EBV” in Covid patients.
It appears Simmaron Research has forgotten their own history
was it not the NIH who ended the follow up Dubbo study for ME/cfs? if so, it shows how much they care about ME/cfs… with all long covid research, for ME/cfs, first see and then believe…. I certainly would like to see more and bigger research on ME/cfs… not that i do not care about long haulers, but they have there money and research and trials…
Further research into EBV and its relation to diseases like ME, MS and e.g. Parkinson and Lupus is certainly warranted. However, ‘ME/cfs’ is not a disease so any research into its cause or treatment is a waste. Davis c.s. already spent countless millions with nothing to show for their efforts, it is a dead end.
I find research into ME/cfs totally not a waste. there are so many subroups, no 2 patients are the same. It probebly will need personalised medicine. personalised research. big centers with big amount of people taken fully appart and tons of money for the many causes and co-morbiditys. I can not believe that 1.9 billion given for Me/cfs research would not make a huge differece. As it is now, al the small studys, you can better say that is a waste of money. And even that is not totally through but on this level, we will not get anywhere.
A recent EBV infection may have damaged the blood-brain barrier, thereby allowing other viruses to enter the brain. This is much easier in ME though than in covid because enteroviruses are tiny.
A significant presence of latent EBV plays another part in disease development because it immortalizes the B-cells that it occupies, thereby sabotaging the antibody response to new viruses. This implies a bigger task for the innate immune response, causing extensive microclotting. Hence the obstructed capillaries in ME and the thrombosis in covid-19, once again reflecting the vast difference in shape (corona viruses are a hundred times as large as enteroviruses).
CFS is not the same as ME and is by definition of unknown cause. It was intended for research only.
A disease ‘ME/CFS’ doesn’t exist, the two are unrelated.
If a third of the patients were not hospitalized, a third of the patients did not appear to have autoantibodies contributing to Long Covid, and a third of the patients had EBV reactivation, my question is: Are these the same people in these groups?
good questions Forbearance
@Cort, any answers forthcoming?
I never had an EBV-like illness and did not have EBV antibodies show up in my blood until about 20 years into ME/CFS. My trigger was toxic exposure, car accident and a lot of trauma, all in one month. I don’t see any problems with those facts, given this article. I have low cortisol in the morning, the B cell, T cell and NK cell measurements described here though.
Trauma well explains these findings. ME however is caused by a virus while CFS requires the absence of any explanation, and therefore doesn’t apply either.
The 1988 Holmes CFS doesn’t require the absence of any explanation.
It requires the exclusion of any explanation that is in the medical literature.
Dr Holmes explains the reason is to rule out anything in the literature that is known, in order to find something that is unknown.
“A possibly unique medical entity”
https://www.meresearch.org.uk/research/responses-to-ebv-antigens/
Re: the study outlined you linked –
Here is a thought:
EBV is getting ‘reactivated’ for its thyroid-peroxidase like protein
helping to convert T4 to T3
What does lactoperoxidase do, could it also be helping bring down hydrogen peroxide excess from oxidative stress?
I know nothing about this enzyme,
It says something about antimicrobial…
We have all the doctors and individuals that have found improvement with thyroid supplementation
so thyroid going wonk is part of the disease processes
Thank you Cort!
Histamine intolerance? Will they be doing any studies on this with ME/CFS/Fibro/Chronic Mono/Lyme/Long Covid/EDS??
Is histamine intolerance the same as mast cell or in the same family? The list of edibles on the histamine intolerance list matches me… an ingredient in a med that caused me tachycardia, might have been the trigger in my recent chronic mono flare. Doc got to see it 24 hours in, at the beginning of the flare. She wrote out some special paperwork, and I showed her info I found that said the med contained potato A, which potato gives me tachycardia. I inquired about histamine intolerance and she didn’t know much about it….I see her in a couple months for follow-up. She’s the one who found my chronic mono, inability cholesterol issue, and EDS….
So did possible histamine intolerance cause my chronic mono to trigger a flare? I won’t sing until I get a for sure answer. One doc I saw 6 months ago, when I told her I was dx’d with EDS, she said she had 5 other women dx’d with it around that time as well.
Histamine intolerance = food elimination/med elimination but may also have to include enzymes if deficiencies found. digestive damage? cells turned off, turned on? genetic components?
I just turned 60 and only found I have ehlers-danlos not long ago! Like all of us, I would love to earn some pain free years in the near future.
(EDS, chronic mono, fibromyalgia, chronic fatigue, etc)
Cort! I stumbled over this article. As I understan they’ve found parts of Lyme bacteria in the brain with long-lyme disease. Is this connected to what you’ve written here. Is it reactivation of EBV or residual parts/pieces of EBV?
i’ve read some by alan b macdonald a pathologist who ins involved with the Duray (foundation?)
He made probles that light up when offending infection found in brain.
Kajsa, is his work what you are referring to re lyme borreliosis?
or do you have a link for the information you are referring to that you could share?
Sunie, this is what I referred to. https://neurosciencenews.com/lyme-neuroinflammation-19976/
thanks!
The million dollar question:
If 90% of everyone gets EBV – why doesn’t everyone get me/cfs / MS / the cancers associated with it etc…?
where the studies being funded to answer that question?
one pretty big study
(“Taking advantage of a series of blood samples from more than 10 million military personnel”)
tried to mine data, finding EBV infection predating MS in significant numbers of people
“Study Provides Strongest Evidence Yet for the Role of Epstein-Barr Virus in Triggering Multiple Sclerosis
January 13, 2022”
found at the following link:
https://www.nationalmssociety.org/About-the-Society/News/Study-Provides-Strongest-Evidence-Yet-for-the-Role
Meirav,
relating EBV to cancer was being looked at relative to carcinogens back in 1984
“Studies on chemical carcinogen enhancement of epstein‐barr virus induced transformation of human neonatal and adult peripheral blood lymphocytes
Earl E Henderson, Gerald Fronko
International journal of cancer 33 (3), 331-338, 1984”
found at link:
https://scholar.google.com/scholar?q=related:QSr4Lhno8MYJ:scholar.google.com/&hl=en&as_sdt=0,5#d=gs_qabs&u=%23p%3DhLKFdsNrlhoJ
WHY DO SOME PEOPLE GET COVID AND OTHERS DO NOT?
[…]I appreciate the herpes simplex cure, You can contact him [[Robinsonbuc kler11]] , His name is all over google____________I believe it will helps a lot people like me …………………….
Hey Cort,
thank you so much for the great work. You are giving hope to so many people.
One question: Biontech is developing a new vaccine for EBV.
Do you know if vaccines will also help people, who are already infected with a virus?
Thanks, Mickey. I really don’t know. Since vaccines train the body to mount an immune response to a virus my guess as a laymen, though, is that they might help stop reactivation of the virus.
Great summary Cort. hopefully this study will be confirmed and they will be able to develop treatment plan
Have a look at this paper:
https://www.sciencedirect.com/science/article/pii/S1568997222000416
The autonomic aspects of the post-COVID19 syndrome
The post-COVID19 syndrome phenomenon, which the WHO had well defined, seems to involve many different organs and leads to a broad spectrum of symptoms that are difficult to attribute to a single mechanism, virus- or immune-mediated. Nevertheless, the clinical presentation of the post-COVID19 syndrome can help us better evaluate the most reasonable underlying pathophysiologic process worth exploring. In this context, many had identified overwhelming similarities between manifestations related to post-COVID19 syndrome and other disorders, such as chronic fatigue syndrome / myalgic encephalomyelitis (CFS/ME) [49], fibromyalgia [[50], [51], [52]], postural orthostatic tachycardia syndrome (POTS), [53], and manifestations associated with silicone breast implants [45]. The typical presentation of the post-COVID19 syndrome, CFS, and fibromyalgia includes chronic fatigue and widespread pain accompanied by cognitive disorders that reduce the quality of life [29,[54], [55], [56], [57], [58]] (Table 2). Interestingly, these conditions are suspected of having an underlying autoimmune dysautonomic-related disorder [[59], [60], [61]]. Furthermore, CFS and fibromyalgia are also associated with various viral infections [[62], [63], [64]].
Also from the above-mentioned paper:
It is of great importance to recognize the autoimmune manifestations of COVID-19 and post-COVID19 syndrome in order to properly cope with their outcomes in the ongoing pandemic and the long-term post-pandemic period, giving the possible autoimmune-mediated underlying mechanisms. The key to managing post-COVID19 syndrome might be concealed in our knowledge of similar presentations, such as CFS and fibromyalgia.
Thanks for this! Does anyone know if due to reactivating of EBV those with ME/CFS who started with EBV are more likely to get long covid even if their CFS has improved over the years? I guess I am wondering if we are more susceptible or is it an unlucky dip since most people have EBV dormant
I said from the being to many people that Covid is triggering EBV and is why many have not done well with Covid. It’s because the medical field DOES NOT know how to treat EBV nor do they test properly nor do they think EBV is a cause of anything? EBV is SCIENTIFICALLY LINKED to cancers and autoimmune diseases. EBV is a cause of Covid long haul symptoms yet AGAIN the medical field DOES NOT know how to treat EBV? Over 15 years ago my daughter had a young math tutor who had MS and she barely could walk and used a cane. First thing I asked her was does she have EBV, she said yes and the doctors did not say it was related to MS?? Now it’s the cause of MS and it’s the cause of so much more including cancer. In this research it’s stating EBV as a culprit and that Covid affects the gut how come doctors do not test stool for EBV, its linked to gastric cancer? How come every tumor is not tested for EBV,its the first virus tumor discovered? The medical field needs a cure/treatment for “Dormant”viruses like EBV and they should start being held responsible for Misdiagnosing patients by not Diagnosing patients with life altering viruses like EBV as a Root Cause!
My daughter and I have had Chronic EBV. What we notices was that when we got Covid and were treated with Paxlovid, the achiness and fatigue that had plagued us on and off for years, immediately stopped and (we assure) went into a state of latency or inactivity.