

Ron Davis gets a win but will he ever be given the chance to bring his core disrupting technologies to ME/CFS?
An ME/CFS Moment: an indication that the ME/CFS field is moving to the next level.
An ME/CFS Moment: something unexpected happens that indicates the tide is rising for the ME/CFS field. This could include something like a big grant opportunity for the field from the NIH or an institution deciding it needs to revamp its ME/CFS program (see below).
A Possible ME/CFS Moment – something unexpected happens that may indicate the tide is rising for the ME/CFS field. This could include a new grant (see below), or an increase in a researchers or clinics workload. It might have happened anyway – but it could be a sign.
Health Rising recently highlighted two potential ME/CFS moments: Dr. Natelson’s multiple NIH grants and a very busy Bateman Horne Center. MEAction recently had the purest ME/CFS moment yet: the most respected and influential clinical care group in the U.S. – the Mayo Clinic at Rochester – reached out to MEAction to help them revamp their ME/CFS program. MEAction reported that their “detailed, respectful and frank conversations” were met with “enthusiasm and receptiveness”. When the Mayo Clinic – whose name is basically dirt in the ME/CFS community – changes its spots, ME/CFS’s star is clearly rising.
Now Ron Davis may be having one as well. If he is – it’s about time. Even having a hamstrung Ron Davis operating on a shoestring budget is a gift. Giving him the funds he needs to really dig into ME/CFS would really be something. This nice grant won’t do that but it is a start.
Davis is nothing if not an original and creative thinker. We knew that – he was called one of the most innovative creators of the 20th century, has received many awards, and is presumed to be on the shortlist for a Nobel Prize. Time and time again, outside and inside this field, he’s gone down paths all his own.
Severe ME/CFS Illness Project Pays Off

Inside and outside of ME/CFS, Ron Davis’s career has been characterized by creativity
The Open Medicine Foundation’s Severe ME/CFS data project is a good example of that. People with severe ME/CFS were being virtually ignored when Davis, citing the need to go where the disease was shining brightest, launched the deepest molecular probe into any ME/CFS patients ever – spending upwards of $100,000 per severely ill patient. It was a creative, as well as daring, “big picture” approach to studying ME/CFS.
The study findings are undergirding much of the Davis team’s work. His work on the nanoneedle, Robert Phair’s Metabolic Trap hypothesis, Phair’s itaconate pathway hypothesis, and the recent grant award all came out of the Severe Illness study, and all are novel approaches that no one in this field but Davis and his team could have come up with. So is the big Department of Defense (DOD) $1.6 million grant he and Laurel Crosby recently received.
Hair Analysis!
Davis’s almost futile attempts to get government funding (and his disdain for his reviewers) are well known. He and Mark Davis did get a big immune grant but, in truth, that one seemed almost too good a match for the NIH to fail. Otherwise, the pickings have been slim, indeed.
That makes Davis and Laurel Crosby’s recent big win all the more interesting. If one was to draw up a list of subjects that were least likely to get funded, I imagine that hair analysis – long associated with alternative health practitioners – would be near the top. I was not able to find any ME/CFS study that has employed hair analyses in order to better understand ME/CFS patients’ pathophysiology.
The hair analyses produced a surprise! Low manganese levels were commonly found. Low copper and selenium levels were also found.
Davis explained that hair analyses have always been a bit suspect because high readings can reflect anything from pollution to the ingredients in shampoo that has fallen on the hair. (One of Davis’s findings – high levels of uranium in some patients’ hair – were traced to contaminated well water.)
The major finding, though, was consistently low levels of manganese as well as low levels of copper and selenium. Those low levels must reflect something that’s going on in the body. Davis used mass spectrometry which, incidentally, is cheap and easy to do – and just never done in ME/CFS.
Manganese deficiency is nothing to play around with and has some interesting potential tie-ins with ME/CFS. Many enzymes need manganese to function. You can’t, for instance, process pyruvate – a key player in energy production – without sufficient levels of manganese. Low copper and selenium levels could also play a role in ME/CFS.
Davis clicked off a number of possibilities: the minerals are not being absorbed in the first place and the kidneys are secreting them. Balky manganese transporters may be involved. Or the mineral may just not get into the hair for some reason. It’s going to take some work to figure out. Blood work is needed to assess manganese blood levels.
Along the line, a lot of blood chemistry and genetics is going to be done – and that will have the add-on benefit of giving Davis a much clearer look at the biochemistry and genetics of ME/CFS. The patient samples – which will be sent through the mail – are going to be gathered using a new type of technology called Tasso, which allows you to draw blood without using needles.
Let’s not forget the role ME/CFS advocacy played in making this study possible. It took a lot of work over several years to get ME/CFS back into the CDMRP (Congressionally Directed Medical Research Programs) program. Our track record is still not very good there – many grants have gone in and only a few have come out funded – but we have had some successes – and every grant win increases our knowledge of ME/CFS.
An Extraordinary Run at the NIH
Davis has been very open about the shoddy treatment he believes his ME/CFS grants have received at the NIH. His upset is understandable. This study – funded by the Department of Defense, not the NIH – is the kind of long-term well-funded study that used to be a piece of cake for Davis.

Prior to focusing on ME/CFS, Davis was so successful at getting NIH grants that at times he was probably receiving more NIH funding than the entire ME/CFS field.
Outside of ME/CFS Davis has had an extraordinary run of success at the NIH. Over the past 30 years, he’s received $2 million grants 12x’s; $5 million grants 7x’s; $7 million grants 3x’s; and $8 million NIH grants 13x’s intermixed with dozens of smaller grants. Those money totals are per year by the way.
That’s well over $150 million in grants. It appears that for a good bit of the time, Davis was probably getting more NIH funding for his genetic and technology work than the NIH was providing for the entire ME/CFS field.
Contrast that track record with the one @$700,000/year NIH grant he and Mark Davis have received to study ME/CFS over the past five years and you can see why Davis is so frustrated. Davis told me that a recent grant application for an Abilify study was denied because the initial reviewer believed ME/CFS was simply depression and that was it for that.
He is not alone. Ron Tompkins also had a spectacular grant run at the NIH (10x $1 million; 9x $2 million; 2x $3 million; 5x $7 million; 6x $8 million) until he, too, ran into an ME/CFS block there. Tompkins felt his chances were so low with the NIH that he decided to direct all his grant applications to the DOD – most of which were rejected.
The loss of significant federal funding produces costs in so many ways, one of which involves continuity of staff. In a recent call, Davis talked about how hard it was to engage in long-term projects without government support. He noted that he’d lost two ME/CFS research assistants to industry in the past year.
The biggest loss, though, in that area, was surely the nanoneedle inventor, Rahim Esfandyarpour, to a University that offered him a tenure-track position. That tenure-track position came with a catch, though: Esfandyarpour would have to attract NIH funding to get it. Donations to work on the nanoneedle wouldn’t work. After the NIH – which actually funded the development of the nanoneedle for cancer – refused to fund it for ME/CFS the exciting nanoneedle work was left mostly on the back-burner.
Davis did get a new and better nanoneedle machine, but it still needs to be redesigned. Esfandyarpour is redesigning it, but given his many other responsibilities – and his lack of NIH funding – that will take time.
This rare big grant win (well, a decidedly small grant by Davis’s standards – but a big grant for this field), though, provides some hope that we’re in the midst of an ME/CFS “moment”.
The Metabolic Trap
The metabolic trap is another case of Davis striking out on his own – and a reminder that he’s on the lookout for an overarching explanation for ME/CFS. The trap hypothesis, which also came out of the severe ME/CFS patient data, emerged when Robert Phair, an engineer, biologist, and kinetic modeler, came across some data that didn’t make sense to him.
Phair was looking for something associated with an infection that could cause a system to suddenly “flip” into a new state which would be difficult to escape from, and would be able to affect multiple systems, and cause something as devastating as ME/CFS.
He found it in the ID01/ID02 enzyme system responsible for breaking down the high levels of tryptophan produced during an infection. We don’t need or want high tryptophan levels. What we want from tryptophan is the kynurenine that it gets converted into.
The ID01 enzyme steps in to break tryptophan down, but at high enough tryptophan levels the enzyme can get overwhelmed. In rides the cavalry – ID02 – and breaks the tryptophan down. What if ID02 isn’t working so well, though, and tryptophan levels continued to rise?
High tryptophan levels mean high serotonin levels in the brain – something that could potentially cause just about every symptom in ME/CFS. (The Cortene hypothesis – which showed up shortly before the Metabolic Trap hypothesis – also proposes high brain serotonin levels are causing ME/CFS). Plus, with low kynurenine levels, you lose a pretty nifty immune regulator and autoantibody controller. Both the Trap and the Cortene hypothesis have the potential to explain much.
Phair’s mathematical models indicated that high cellular tryptophan levels over time could produce a devastating situation that was almost impossible to recover from. Phair and Davis next found that the genetic requirements for the trap did appear to exist in people with ME/CFS, and a preliminary sample of ME/CFS patients’ cells suggested that the trap did exist.
Yeast!
Since then, Phair and Davis have been methodically testing the trap. They recently found that the metabolic trap can be sprung in yeast; i.e. it’s no longer a hypothetical construct – if tryptophan is allowed to rise in a cell, it can spring the trap.
When it comes to assessing basic processes yeast cells are invaluable: they have a nucleus and can easily be genetically manipulated to mimic human cells. (Frank Roberton CC – Wikimedia Commons)
You might think yeast! What does yeast have to do with humans? Well, yeast is no laughing matter in research circles. Because yeast cells share many basic biological properties with human cells, and because its genome is so well known, researchers often go to yeast to investigate very basic cellular properties and to test drugs.
It’s easy for researchers to insert human genes into yeast and then probe, test, and manipulate them – essentially mirroring in a yeast cell what happens in a human cell.
Back in the 1990s, 600 researchers from over 100 labs worked to sequence the first yeast genome. At the time, it was the largest genome ever sequenced, and yeast still occupies a prominent place in research today. In 2017, the first 3-dimensional representation of the yeast genome was produced, and yeast is now being used to develop more effective antifungal drugs (including Candida albicans), to identify longevity genes, and understand mitochondrial diseases, among many others.
Davis probably knows the yeast genome better than anyone else. He’s had many yeast grants – among them a $5 million grant to sequence the yeast genome using a new, very rapid, low-cost technique. The first thing his biochemistry page at Stanford highlights, in fact, is his yeast/genome work. It may be what he’s best known for.
First, Davis produced a yeast cell that could process tryptophan – a central element of the trap hypothesis. For a while, the yeast could handle the tryptophan buildup, but when it reached a certain level, the yeast fell into a kind of stasis state and was unable to grow. The trap had been sprung – and an ME/CFS-like state had emerged.
Davis has started to test FDA-approved drugs in his metabolic trap-engineered yeast. Not just some FDA-approved drugs – all FDA-approved drugs are being tested to see if they can unspring the metabolic trap in yeast and allow it to grow again.
The “Poster Child of Metabolic Reprogramming”: the Itaconate Pathway
Itaconate provides another example of the different thrust that Phair and Davis are taking in ME/CFS. Called the “poster child of metabolic reprogramming” itaconate is produced during the TCA (or Krebs or citric acid – take your pick) mitochondrial cycle. It was Naviaux that alerted us to the role the mitochondria play during an infection – and during an infection, the itaconate pathway gets turned on in immune cells (and probably others).
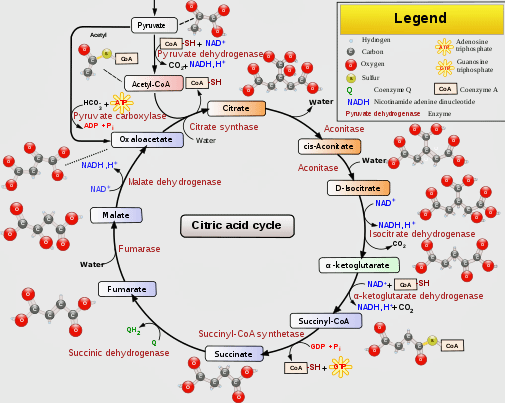
Itaconate blocks aconitate from entering the Krebs cycle (see the Krebs cycle at about two o’clock or upper right part of the circle.)
There, it produces a shunt that blocks compounds from entering the TCA cycle – thus reducing the cells’ ability to produce ATP – thus resulting in fatigued or exhausted (or hypometabolic or Dauer-like – take your pick) immune cells. Immune cell exhaustion – particularly NK and T-cells – may be present in ME/CFS, but this process could also apply to muscle cells and help explain why they get exhausted so quickly. A long-lived and hyperactive itaconate pathway could also contribute to the fat-burning problem and the strange case of the disappearing ammonia, which may exist in ME/CFS as well.
Why would a cell turn off its own energy? Perhaps to hunker down and wait out the threat (?). Perhaps to induce “sickness behavior” and get us to lie down, reduce our contact with others, and stop spreading infection.
Phair is modeling the mitochondria to see what could turn on/off this pathway and Davis said he was confident they would be able to assess the itaconate pathway in ME/CFS patients’ cells. That is, once they replace their latest loss to industry – another researcher recruited away.
BH4
The severe ME/CFS data study also prompted Davis to put in a grant to study tetrahydrobiopterin (BH4, sometimes THB). It turns out that some people had a mutation in BH4 synthesis. BH4 is a vital cofactor for numerous enzymes in the body, including those involved in the formation of nitric oxide (NO – blood vessels), and the key neurotransmitters dopamine, serotonin, and epinephrine.
A Common Thread

Davis brings a strong biochemical focus to ME/CFS research. (Image from Biochemistry Principles by Moran, Horton, etc.)
You can see a common thread emerging – biochemistry: “the study of chemical processes within and relating to living organisms”. The professor of biochemistry and genetics at Stanford Davis has a Ph.D. in biochemistry. Davis, who is superb at visualizing biochemical reactions, probably goes to sleep with visions of biochemical reactions dancing in his head.
The Gist
- Described as a “frequent provider of core disruptive technologies”, Ron Davis’s career both inside and outside of ME/CFS has been characterized by innovation and creativity.
- The Open Medicine Foundation’s Severe ME/CFS project is a typical example of Davis’s often daring approach to this disease. Upwards of $100,000 per patient allowed Davis and others to dig deeper into their molecular biology than ever before. Its findings have laid the groundwork for much of the work Davis is engaged in now.
- That includes the DOD grant Davis and Laurel Crosby just received in which they used hair analysis to uncover a common deficiency of manganese as well as copper and selenium.
- Manganese plays a critical role in many enzymatic reactions including those involved in energy production. As an added bonus the study will provide the opportunity to gather a wide range of biochemical and genetic data on a large group of ME/CFS patients.
- Davis and Phair have uncovered two unique ways (the Metabolic Trap hypothesis and itaconate pathway) which could explain how an infection could rewrite vital metabolic processes – potentially leading to ME/CFS.
- The Metabolic Trap hypothesis has evolved from its beginnings as a genetic query, to include a mathematical modeling approach, analyses of ME/CFS patients’ cells, and a duplication of the trap in yeast. Now Davis is using yeast cells to test FDA-approved drugs to see if he can “unspring” the trap.
- Davis’s focus on biochemistry brought the metabolic trap hypothesis, the itaconate pathway work, and now work on BH4 to the ME/CFS field. His technology work has brought the nanoneedle, red blood cell deformability, neutrophil flow, a sweat crash test, and other possibilities to the field.
- Bringing new and unusual possibilities to a field is nothing new for Davis who had an extraordinary run that garnered over $150 million in NIH grants prior to entering the ME/CFS field. Since then, though, he’s had difficulty getting federal funding.
- Time will tell if the DOD win constitutes a real ME/CFS moment; i.e.; a sign that ME/CFS is being accepted and recognized in places it was rejected before. Time will also tell if Davis will ever be given the opportunity to bring the “core disruptive technologies” he’s famous for to the ME/CFS field. Let’s hope he gets that chance.
His biochemical slant is one reason why his ME/CFS work is so distinct. It’s also why he’s so jazzed at the hair analysis grant – which will give him an ample opportunity to plunge into ME/CFS patients’ biochemistry.
The other thread is technology. Davis has been described as “a frequent provider of disruptive core technologies“.
Besides his genetic work that helped lay the groundwork for Genome Project Davis’s forte has been developing low-cost, effective medical devices. He’d love to develop a cheap, effective diagnostic test for ME/CFS. A number of possibilities exist.
There’s the red blood cell deformability tool that’s being developed that he believes might cost a dollar a test to produce. After finding that neutrophils are also having trouble flowing properly in ME/CFS patients’ blood a tool to measure neutrophils is a possibility as well. The idea that neutrophils – which have hardly ever been studied in this disease – might actually constitute a diagnostic test – highlights an important fact: the first diagnostic test for ME/CFS could come from a totally unforeseen corner.
Nothing demonstrates that better than the nanoneedle which uses electrical impedance to assess cellular activity. We don’t know what biological factor it’s picking up on; i.e. we don’t know what it’s telling us about ME/CFS but we do know that it produces highly consistent results. It’s invariably able to differentiate people with ME/CFS from healthy controls.
Nor do we associate ME/CFS with significant eye problems but Chris Armstrong’s early work suggests that ME/CFS patients’ eyes track movements might actually be diagnostic for this disease.
Davis’s ideas seem to know no bounds. He’s working with a former student – now a professor at UCLA – to assess the content of sweat in hopes of developing a wearable device that could tell a person with ME/CFS that they’re pushing their limits and are going to crash if they go much further. We have no PEM warning device right now. Davis talked about a student who became bedbound with ME/CFS and wondered whether the disease was perpetuating itself by her crashes. In what must have been a very disciplined effort she made sure she didn’t crash for a year – and eventually fully recovered.
Time will tell if the “core disruptor” will be given the opportunity to unleash his creative gifts on the ME/CFS field as well. Davis did say that he put in four grant applications last year and that the comments, this time, he felt had some validity; i.e. his grant applications were being taken more seriously – a good sign.
Time will also tell if Davis is indeed having an “ME/CFS moment”; that is if the wind is finally catching his ME/CFS sails – sending more funding his way.
Given the track record he’s built over his long career, and his many interesting ideas, one would hope that would be a strong wind indeed.
Disrupt Health Rising’s Summer Donation Drive!

Thanks for blasting off Health Rising’s Summer Donation Drive.
Thanks so much to everyone who’s blasted HR off with a great start to the summer drive. With just two days into the drive, we’re already a third of the way to our goal! That’s the kind of disruption we like.
If you like the kind of well, rather lengthy – yes, but informative blogs like this one on Ron Davis – please support us!



 Health Rising’s Quickie Summer Donation Drive is On!
Health Rising’s Quickie Summer Donation Drive is On!


A few years ago, my doctor ran micronutrient testing on my blood to see whether I had any significant deficiencies. There were one or two that we tackled (eg, B12) and a small handful more that didn’t seem significant. Recently I dug up the old results and decided to try supplementing, just in case. I got everything on the list except one. Wouldn’t you know, the one I skipped was manganese!
So can one assume from this that urine analysis of these elements/minerals is not going to be the same as what shows up in hair analysis? In other words, urine levels are not a reliable read on whether or not a patient has sufficient levels of manganese, selenium, copper etc?
I have no idea. I assume = but don’t know – that this study will assess mineral levels in the hair, blood, and urine to see if they match up.
Hi Lisa, I believe you are correct, since they suggested the kidneys are flushing the nutrients vs hanging on to them, the urine would just show what is being discarded, vs what our current levels are- if I understood that all correctly:)
There is a difference between serum levels and TMA (tissue mineral analysis). The body will always try to maintain a level amount of nutrients in the blood which have the highest priority, so the body will pull out nutrients from storage sites to maintain this equilibrium.
Minerals are typically stored in storage sites which are used for reserves. Hair is thought to be a window of true stores.
I would recommend doing a test and supplementing according to the test results rather than just blindly supplementing. Trace Elements Inc is the go to lab for several reasons. And no, I have nothing to gain from this advice. I do have 30 years of using this lab for myself and others and have always been helped by the results.
Nice article. I’ve been short of manganese and supplementing has helped. Same with BH4.
Davis’ name might be on the grant for BH4, but Laurel Crosby is doing all the heavy lifting. She’s brilliant and deserves credit on her own right, not as an afterthought.
Good point. I did note this “That makes Davis and Laurel Crosby’s recent big win all the more interesting.” and added her name to the gist. To my knowledge, she’s the one that pushed for the hair analysis in the first place. That said, the blog was about Ron and his work and not so much about the genesis of the hair analysis grant – so the emphasis was on him. Thanks for acknowledging her though. She’s been working on this for years I believe.
I was so moved as I watched this brilliant man and Stanford scientist speak on the most recent Open Medicine Foundation series. He spoke about the research funding roadblocks just when he and his team, after so many years of work, were finally able to put into practice more efficient and very inexpensive measurement techniques for key metabolic parameters.
His frustration resonated with me. ME CFS at the age of 62 stole my life as I knew it, but it pales in comparison to what his young son Whitney Dafoe is living with. The question that plagues me is not why me, bad stuff happens all too regularly, but why now, as to when and why I became so utterly debilitated and chronically ill. Thank you Ron Davis for your foresight, your brilliance, and your dedication. I pray your mission proves to be possible.
Hi Learner!
Yes, Laurel has worked hard on this but in fact, she and Ron collaborate closely and talk with each other multiple times a week. they are definitely partners and in this together!
Hi Cort, verry much trouble to read/impossible. tryd it. How much are they now getting in money? was it for the manganese study alone? thanks or anyboddy who would help me!!!
Hi Konjin – sorry you’re having a rough day! I believe it was for $1.6 million dollars and the study lasts for 3 years. The manganese part is exciting but its clear that Ron and Laurel are very excited at being able get a lot of biochemistry and genetic data on a large group of ME/CFS patients. Laurel stated in a comment that they’ll be exploring “aspects of metabolism and how people with ME/CFS metabolize various sugars and amino acids”. How about that! The grant just got a lot more comprehensive! A lot of work could come out of this.
I think that’s pretty typical of big grants – they tend to open up a lot of areas.
Hi yall, I recall the day I got sick….at the age of 21(1981)…I’m now 63.i was diagnosed in 93 as moderately severe CFS.
It started with vomiting and diahrea.two weeks later I developed an ulcer which healed on its own over time but I was left with some very odd symptoms that got worse over time until, in 1993, all he’ll broke loose, I guess you could say. I had no idea a person could get this I’ll.
My 1993 trigger was an overexposure to a harmless polyurethane floor finish product. I then slept in a tent in my back yard as everytime I would enter that home, I would break out in a head to toe rash and also feel my health quickly deteriorate in seconds upon entering that home.well, winter came, I could no longer sleep in that tent. I slept in that home all winter and my health deteriorated severely….I’ve moved to several houses , some worse ,some better. I’ve been poor for decades and fear I will die of this. I look ALMOST normal.
My question is….is there a way that Ron and his team could measure this rapid decline in health upon entering that home.the rapid decline would happen in seconds!!!
It could provide a clue ,I think…if they could find a patient that was in this moment of decline…ascend/decend.i am obviously not in that ascend/decend…but if they could find someone that was????
The day I got sick in the motel room I was living in for 4 months, I was drinking well water.i have high levels of uranium, nickel and antimony, from I bet ,that well water.while living in that motel in small town Saskatchewan,Canada I was also going to community College, taking a WELDING coarse.Note that Saskatchewan has very high rates of URANIUM and very high rates of MULTIPLE SCLEROSIS. I have known several people died at young that worked in the mines. I keep thinking ,there must be a connection to well water. I also spent weekends and summers at my grandparents farm and drank well water.
Hi everyone. My name is Dr. Laurel Crosby and I’m the co-investigator on this project. We sampled hair many years ago because patients were concerned about heavy metals exposure. But we found that certain trace metals appeared to be low. We don’t know if this is really a deficiency or if it’s an artifact. (That is, maybe people with ME/CFS don’t go outside as frequently or wash their hair as often as healthy counterparts. The minerals could be low in hair because the environmental exposure is lower.)
When we started to explore this question further, we realized that manganese is an important trace metal for enzymes involved in metabolism. So, we’re actually focused on aspects of metabolism and how people with ME/CFS metabolize various sugars and amino acids. If there is a clear pattern that manganese enzymes are affected, then we can speculate about why this happens. Maybe manganese content is fine in the blood, but it’s not getting into cells or into the mitochondria. These are interesting questions that we’ll pursue in our 3 year study.
Here is what you should know now: Dietary manganese comes from carbohydrate-based foods like cereal grains. There has never been a documented case of manganese deficiency because of low dietary intake. (But that was before keto diets were popular!) Calcium supplements can also bind up manganese in the gut and prevent absorption. So, there are potential ways that someone *could be* deficient, and we’ll be looking at this from many different angles.
The problem with supplementing with a trace metal like manganese is that too much can be toxic. The safest strategy is to get nutrients from whole foods. Please help us keep the ME/CFS community safe by recommending foods over supplements.
Thank you,
-Laurel
Thanks so much, Laurel and good luck with the 3-year study. Finally a nice long grant package. 🙂
Hi Dr Crosby (Laurel), thank you for the explanation.
I may have missed this in Cort’s blog post, apologies if I did. My question is,
is the research team aware the connection between Borrelia Burgdoerferi and manganese?
The Michael V Norgard Lab at UTSW published the connection between manganese, not iron, and virulence of Lyme Disease (about 2009 I think).
Interesting – I have had 3 hair mineral tests done over the years and all 3 showed extremely low manganese.
Laurel, since we know what ME is (as opposed to ME/CFS), well we do in England anyway even if you think you don’t in America, wouldn’t it be better to work on targetting drugs for the nervous system to try and reduce the various vasculitis that occurs in this disease casuing our symptoms? We have had enough quackery in ME (and ME/CFS whatever that is).
Thanks, Dr. Crosby. I am one of Dr. Bonilla’s patient who participated in an early version of the hair trial, soon after the first of Dr. Davis’ trial that included (as I recall) 9 severely ill patients, with 6 having very low selenium. My test turned up high levels of mercury and nickel and low selenium. The problem was eventually traced to an old/broken dental bridge. Removal and replacement that got rid of the mercury amalgam in the anchor teeth and eliminated the nickel in the “gold” bridge. This gave me a significant improvement in some of my ME/CFS symptoms. Good luck and thank you for all that you are doing.
Thanks for posting Laurel. My concern is that several studies show that hair mineral content doesn’t reflect dietary intake — and/or reflects the opposite. Not enough.
“These results show that high hair calcium concentration was associated with low calcium intake and low BMD. ”
https://pubmed.ncbi.nlm.nih.gov/24846904/
Dr. Crosby,
You might be interested:
I have had ME/CFS for 10-ish years and added long covid as “icing on the cake” 2 years ago. I am currently pursuing a master’s in human nutrition. Long story short, I tested Mn deficient about a year ago: Mn RBC = 7.2 ng/ml, ref range 11-23 ng/ml. A second test gave similar results. My diet has no shortage of Mn. Other micronutrients were within normal limits. (of course, no doctor found this believable due to the rarity of deficiencies-I do have a confounder of celiac disease)
I was excited to learn that Mn, Cu, and Se may be researched in further detail as I wrote a faux research proposal on the possible association of ME/CFS and Mg deficiency.
I will be following your research.
I’m curious if high serotonin levels are linked to the trap, could the use of SSRI’S be a trigger in some people?
I hope someone else can answer this. The whole serotonin question is just too complex for me.
, chez moi aussi , le taux de sérotonine est trop élevé…
Unlikely, as it’s an increase in tryptophan levels that can potentially get you into the trap, not serotonin. Tryptophan is the precursor of serotonin, so it doesn’t work in the other direction.
I wouldn’t rule out serotonin dynamics in any particular pattern just because of proven patterns with tryptophan and kynurenine. I took a pretty deep dive into the metabolic trap model equations and surrounding literature. I even simulated Dr. Robert Phair’s equations in Matlab to explore feasibility and timescales (which are actually on the order of years just to ENTER the metabolic trap state). Of note, I would point to some literature that does a good job connecting the dots between tryptophan metabolites, including this scalable mathematical model of tissue specific tryptophan metabolism (which even includes endogenous DMT): https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3843069/
While I don’t have a good idea off the top of my head how much tryptophan and kynurenine fluxes impact serotonin in a given tissue (which will inherently differ from the bloodstream or other easier to measure sources), I would recommend looking into this model for general patterns between the three (serotonin, kynurenine, and tryptophan). I might even try to take another deep dive and come back to this.
It seems possible that SSRIs could have negative effects if serotonin levels get too hight. Problem is that it’s really hard to measure and it’s in the brain that you’d want to measure it. Ability reportedly increases dopamine and decreases serotonin, which might be why it helps some people. SSSRI’s are often unhelpful for ME/CFS. It’s often prescribed by docs who think they are treating depression.
Not quite an SSRI, but I was already on an SNRI (Cymbalta / duloxetine) for major depression at the time that I caught whatever virus it was that gave me ME/CFS. The SNRI made the ME/CFS much, much worse. I was almost entirely housebound, and spent most of my time in bed.
When I was able to see my main psychiatrist again (long story but it was more than 6 months after I first crashed from the virus), he was apparently aware that the SNRI might be playing a role, and first suggested we increase the dose “to see what would happen”.
I doubled the dose as per his instructions, and within a few days my ME/CFS symptoms got so bad I could barely wake up at all most days, let alone sit up or get out of bed. This went on unabated for over a month, however my psychiatrist then didn’t feel certain this obvious worsening of my symptoms was “proof” it was the SNRI, and told me to increase the dose further!
At this point I was so, so sick and exhausted that I couldn’t stand it, and his idea seemed ridiculous. So instead I went off them completely, cold turkey. (I wouldn’t recommend this to everyone; I was just desperate.) Within about a week, most of my worst symptoms went away. Within about a month I went from being at about 20% functionality back to 80% functionality again. And I stayed at that “recovered” 80% state for at least 5 years.
That was over 10 years ago now, and other external environmental factors a few years later triggered another ME/CFS crash which I have not recovered from. But I would not go near another SNRI (or an SSRI for that matter) if you paid me a million dollars.
Thank you Cort for keeping us updated. I’ve had me/cfs since 1994. Over the years I’ve chased one red herring after the next and several years ago I gave up researching or following the latest info.
However, I recently found a functional M.D. who seems to know what he’s doing and I’m now back in the soup of following this disease.
I just rented What About ME on prime. Wow. The documentary is a few years old now but the blatant corruption involved in keeping this disease unrecognized or from getting government funding is hideous.
I see a bit more hope now that long COVID seems to mimic cfs. People believe long COVID is real so at least there may be funding for studying that, which could transfer to us.
I hope Ron can hang in there. He’ll be 81 next month. My prayers for his son and family.
Lack of progress has stemmed from NO FUNDING FOR DECADES FROM THE NIH. FRANCIS COLLINS LEFT SO MAYBE SOMEONE NEW MIGHT THINK DIFFERENTLY. RON DAVIS IS BRILLIANT AS MANY RESEARCHERS ARE AND HE HAS PRETTY GOOD RELATIONSHIP WITH NIH. BETTER THAN MOST. THREE YEARS IS SO LONG FOR ME. I HATE TO THINK ILL FEEL LIKE THIS FOR MY LIFE. ITS BEEN SINCE 1986 for me. But, as I’ve said before, I wish there could be a MANHATTAN PROJECT to figure this out. You are always on it, Cort. Any news on Dr. Ian Lipkin from Columbia University considered THE VIRUS HUNTER? He was working on CFS. He did get covid and I’ve not heard of him since. Sincerely, hipjaven@gmail.com
Lipkin is working away. I haven’t kept up with him but I heard he has a pretty interesting paper coming out on the immune system.
Very best wishes to Ron and Laurel. So glad that we have people like you fighting in our corner. Very interesting about the manganese and thank you Laurel about the warning about supplementing. I think we are in danger of doing this with other supplements out of desperation to find answers. Would just a low level in a multivitamin and mineral supplement be worth trying or could that also build up in the system to too high a level?
The best solution is to get your doc to test your levels and if low then supplement it, while doing further testing to monitor the levels. Ask your doc about multivitamin and mineral supplements. Monitoring with intermittent blood tests is a good idea. Whitney “eats” Peptamen as his only food and we supplement with several things that measure low and with a multivitamin supplement called Intramax.
Thank you so much for your reply Janet. I live in England and getting the doctors here to do anything is like asking for the holy grail! I had already been taking a multivitamin and mineral supplement on and off for a while and have just added it back in. May ask for a blood test but to get regular monitoring is going to be very unlikely and they only do the standard tests here. I tend to try things for a while and if I feel a benefit keep it in and if not stop it. Very hit and miss I know but I think it’s just that hope that one day you may stumble on something that will help. I’m not a scientist so just blunder on in my own way. Love to Whitney and I have my fingers crossed tight for him bless him.
Ron Davis is not studying ME. He is studying people with both ME and CFS. He should be studying sick people with acute onset ME. CFS is loads of fatiging illnesses that could be treatable.
Martin, I’m not sure what you mean. I was under the impression that ME and cfs were the same. ME is simply the name they gave it in England. I was diagnosed 28 years ago. I know nothing of it being treatable. Otherwise I wouldn’t be bedridden half the time.
Also, are you aware that Ron Davis’s son has been bedridden and on a feeding tube with the disease for years?
His wife is Janet Dafoe who has comments here. You might therefore want to be more sensitive in your comments.
Kira, ME is the official name that has been listed since 1969 in WHO ICD under neurological diseases at 93.3 CFS is the newer name created by a US committee headed by an NIH official in 1987 or 1988 — You can look up the date in Osler’s Web. The CFS name was first applied to the cohort of ME patients in the famous Incline Village outbreak of 1984-85, but the subsequent definitions of CFS do not comprise identical symptoms to ME, though there are overlapping elements.
I have long covid and fulfill all criteria of mecfs. One thing which popped up at the very beginning of my journey was low manganese.
Try Immunocal/ It protects the neurons and is a weigh protein which makes glutathione which is needed by the immune system.
Interesting! You know now that many people with long COVID have had it for more that six month and probably meet the criteria for ME/CFS. That means Davis can include them in his grant work.
Thanks again for your terrific reporting, Cort.
Can you provide to us any new details on the “test FDA-approved drugs in his metabolic trap-engineered yeast.” Question might include: How many drugs have been tested in yeast. How many drugs spring the trap in yeast. Are they finding commonalities in the drugs that do spring the trap. Have the drugs been tested in human cells.
So many folks are hoping this is the key that unlocks the puzzle.
Bless Drs Davis, Phair and Crosby, and their team.
From memory they have tested quite a few and I believe have uncovered some interesting candidates, that is if memory serves and that’s not wishful thinking talking :). I don’t know anything about specific drugs but I really liked the broad approach – you never know what’s out there that we’re not even thinking about that might help.
Abilify is a good example of that. Who was thinking about Abilify? Maybe just one person – the Stanford MD whose name eludes me at the moment.
Cort – that would be Dr. Bonilla, who stumbled on it with a patient who, as I recall, had been prescribed Abilify following cancer treatment.
They have now tested all FDA approved drugs from a commercial collection of about 1700 from a few years ago. They have found several that “spring the trap”. They now need to be absolutely sure this is not an artifact such as the drug activating a drug pump that pumps out tryptophan (drug pumps in yeast aren’t known to pump out amino acids, but they want to make sure). Once they are confident that it’s not an artifact, they will begin testing it in human cells. This is much more complicated than in yeast so it will take some time. The same scientists are working on other important projects and they can’t do both at the same time. With more funding they could hire more people and it would be faster. If they determine a drug stops the trap in human cells, they will investigate trying it on patients. That requires an MD and an IRB, which is time consuming.
hi Janet! thanks for the update comment. when you talk about timing, how long do you think it takes approximately? more than a year? I know it’s hard to be specific about science, but I speak roughly. Thanks for everything
Dr Myhill tests selenium in the UK and usually finds low levels in ME/CFS. I thought selenium was already a mainstay of patients’ supplement protocols.
Regarding serotonin: whenever I’ve tried supplements which deliberately or inadvertently raise serotonin – like 5-HTP – I’ve experienced a serious worsening of neuroimmune symptoms that’s taken weeks to come out of. As a word of warning, I recently tried Oxaloacetate and it had the same or a very similar deleterious effect.
So frustrating to hear of RD’s grant frustration, especially considering his obvious brilliance. But thanks for bringing news of how he and RT are persevering.
Yes! Finally! Someone looking at sweat
There are way too many substances that my body exhuded that I’m sure would have clearly showed pathology.
More or less under control now.
Tried getting a lab to analyze my sweat Covid happened.
What is the “strange case of the disappearing ammonia”?
Has anyone tried building bridges to the NIH Center for c
Complementary and Integrative Health?
https://www.nccih.nih.gov/
Interesting idea. If manganese levels are low one would hope they would be interested…:)
Very interesting, I often crave fresh pineapple, and that’s one of the foods with manganese. I eat a whole food, simple diet and find intuitive eating usually steers me in the right direction.
Researchers fundamentally dont understand how to interpret data. They see something like a Mn deficiency and think that’s the problem, the body is stupid or isn’t working right. Maybe the body is intentionally downregulating pyruvate processing or other processes requiring Mn. The CDR/Dauer state is intentional. CFS is an immune regulated protective state. From what? My money is on mold/biotoxins enhanced by chemicals used in modern society.
I agree with this
Mold/biotoxins enhanced by chemicals is where the research funding should go
I think Erik johnson presented alot of good case evidence that is being ignored by me/cfs researchers
No, Tim, they see a Mn deficiency and analyze all the pathways it is involved in, and then use science to discover what the deficiency might mean. They look at the transporters of Mn and try to determine if it is deficient in cells, or only in blood, hair or urine. They use science to determine the relationship of these findings and the possibility that it could contribute to symptoms. They note that ME/CFS patients are more likely to have this deficiency than healthy controls. It is somewhat amazing that you think these scientists don’t know how to interpret data. My money is on science and data, not conclusions that aren’t rigorously demonstrated scientifically.
You didn’t understand my comment. You are still focused on the idea that “Mn is low, must mean that something is going WRONG and we need to boost Mn.” Rather than entertaining the possibility that the body is keeping Mn low on purpose. Every bit of research on this illness has focused on the many many downstream effects of whatever the core cause is. That’s all Im saying. Im equally a fan of science and data.
Tim, I don’t see where Janet said they want to boost Mn. In fact, one of the researchers is in this thread saying not to take Mn supplements.
Completely agree. I have low manganese (and low selenium etc.) in my hair mineral analysis, but we have Parkinson in the family which means excess manganese in the brain. Doctors who have worked with hair mineral analysis for decades have well explained that the body may be holding on and storing certain trace minerals for “safety reasons”. I also have very high calcium (calcium shell is worth researching). My best approach (after trying just about everything) is sauna therapy (every single day (and taking low dose electrolytes) and supporting the hypothalamus with extracts. Yeast overgrowth was an issue for me (sauna and diet changes help).
Did the researchers work with fingernail clippings at all? With their being thicker than hair, perhaps they can be better cleaner of environmental contaminants or residues?
While all these findings are very interesting, it did not serve the patient population well for CFS researchers to subvert and suppress the very clue that started the CFS syndrome.
Much suffering could have been averted.
But this is what you wanted. Always remember that!
Oh please Erik, flip the record over. Whether you call it ME, ME/CFS, CFS, Ramsay’s disease or whatever — it “started” long before you became paranoid about mold.
Are you recovered yet? Or do you still have to avoid “the ick”?
How can I include my Very Severe, 100% bed-bound 34-year-old son in any of these studies? We live in South Carolina. I’m happy to overnight chilled hair, blood, skin cells, anything needed. Please let us help contribute to the data!!!!!
Looks like Davis has a pilot program to analyze individual bio information:
http://www.geniusdiagnostics.com/contact
I love the approach by Ron Davis: To test ALL FDA-approved drugs! 😉
And from a comment above by Cort, Davis has already found some candidate drugs! 🙂
Here’s where we see someone clearly trying to cure / improve patients!! Very grateful for his practical and goal-oriented approach, to get results and soon.
We are so lucky to have such a brilliant researcher on our side.
Ron Davis= Grant chaser. Not an honest researcher IMO. Loves big gated homes and researches a fatiguing illness called CFS instead of ME G93.3
Great new interview with Ron Davis by Janet Dafoe, focused on the Itaconate Pathway, hosted by the Open Medicine Foundation. It’s just over 15 mins long and Janet Dafoe, helps to interpret the research update by Ron. I thought it was very good.
‘Today, we are delighted to share the first in a series of research updates from Ronald W. Davis, PhD, Chair of OMF Scientific Advisory Board & Director of the OMF supported ME/CFS Collaborative Research Center at Stanford.’
https://www.youtube.com/watch?v=hxBIaA3YVXU
In another great interview with Janet Dafoe, ‘Ron shares details about his new Department of Defense $1.6 million grant he & Laurel Crosby received to study Manganese and its role in #MECFS.’ OMF
https://bit.ly/3N9zi3u
‘Ron Davis Updates on the Metabolic Trap Hypothesis!’ OMF
Ron Davis and Janet Dafoe discuss the progress on research into the Metabolic Trap.
https://www.youtube.com/watch?v=8drZ5eF7FI4&t=1s
‘Rob Phair, PhD, Presents on the Itaconate Shunt Hypothesis for ME/CFS’ OMF. Janet Dafoe PhD gives some very helpful explanations and asks Robert Phair to explain further, where needed. I found it complicated but I just tried to get a general idea of what’s going on.
https://www.youtube.com/watch?v=RiVDNhg4l48
Ron Davis Research Update: DNA/RNA Tech with Peidong Shen, PhD
‘Today, Ron Davis, PhD, and Janet Dafoe, PhD, sit down to discuss how DNA & RNA technology is being developed and used at Stanford to advance research into ME/CFS, Long COVID, and related multi-system chronic complex diseases (msCCD).’ OMF
https://youtu.be/MwypF_KoRDM
I’m am mostly recovered from ME/CFS at this point using Hair Tissue Mineral Analysis (htma) reports from Analytical Research Labs (ARL) in Phoenix, AZ. ARL was founded by (the late) Dr. Paul Eck who created a mineral balancing program based on the htma results. Dr. Watts was a colleague who went on to found Trace Elements Lab. The two labs are the only ones in the country that use a process that doesn’t wash out and alter the water soluble minerals (i.e. sodium & potassium) from the hair. This is essential for proper analysis.
Hair levels of minerals rarely match serum levels due to the buffering effect of the minerals in the blood. While blood levels will normally stay in a tight range, hair levels can vary by a wide range – sometimes over a 1,000%.
Most nutrition is based on a ‘replacement’ theory. If manganese is low, supplement manganese. This DOES NOT WORK! Mineral balancing (aka Nutritional Balancing) takes in account the reactions between individuals vitamins and minerals and how they effect each other – antagonistic, synergistic, etc. For example: the vast majority of ME/CFS patients will show low zinc levels. However, supplementing zinc will lower zinc cellular levels because zinc will go down in relationship to the sodium/potassium ratio and zinc lowers the sodium/potassium ratio (which is also going to be very low – mine was 20% of normal on my 1st test). It’s this knowledge of how different vitamins and minerals effect cellular mineral levels that makes metabolism malleable – metabolism can be moved to a higher state of efficiency for better energy production.
If researchers really want to make progress on ME/CFS they should start by getting up to speed on existing work and build on that knowledge. Dr. Eck’s work has been around since the 1980’s and is light years ahead of Ron Davis’s work. The lab reports are a valid, viable, and essential diagnostic report for anyhow with ME/CFS and treatment programs are already available. There are consultants that specialize in htma and mineral balancing that are available to guide patients through recovery and the cost is very reasonable.
Hi Cort – what is the “strange case of the disappearing ammonia” that you allude to in the post?
CFS is not a genetic problem. CFS is a disease symptom that occurs when the brain’s electrical brain signal production is erroneous due to electromagnetic interference, or when normal brain signals are transmitted through a neural network and damaged by electromagnetic wave disturbance. CFS is when the respiratory system, circulatory system, digestive system, muscular system, nervous system, etc. cannot function normally due to electromagnetic disturbance. ME is a disease accompanied by severe pain such as gout when uric acid concentration is high among CFS patients.
It can be easily treated by controlling the living environment in an environment where electromagnetic wave is not disturbed and tuning the brain-body control system.
CFS can be cured within 1 week, and in the case of ME, to remove uric acid after CFS treatment, it needs to be adjusted for 3-6 months.
In this method, it is only necessary to control the exposure environment such as electromagnetic waves, negative charge, static electricity, etc. and introduce B-B tuning for diseases that do not appear to have introduced antibiotics to bacterial infection.
CFS can be treated within one week and can be treated anytime, anywhere.
how did you come to this conclusion
Has Monolaurin been discussed? Does it’s antiviral and bacterial efficacy have a place in the extensive conversations regarding research? In doing some daily research, as I have a young family member bedbound with CFS/ME, I have noted a reference to its use in CFS (and of course ME). is there any discussion, that I have missed?…Thank you in advance.
Is anyone testing any EBV anti-virals, or t-cell vaccines to address EBV? What about ant-retrovirals for the possible connection between HERVs transactivating the EBV?
From what I’ve heard long COVID has triggered much more interest in EBV. Don’t know about specific trials.
What is this 2010? Antiretrovirals were proven long ago to not show any benefit. And everyone — or almost everyone — has Epstein Barr. The causes of ME/CFS are typically many, including and especially prolonged stress/stressors. That’s not going to be solved with a magic drug.
yes I have cfs from prolonged stress but maybe a medicine can be found for that too
My son has “suspected” chronic lyme desease (hard to test once in cells and tissues too long).
Mangenese plays a big role in the survival of Borrelia. Maybe all these people with a lack of manganese have lyme? Only a hypothesis.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3605662/
what happens if a healthy person without ME CfS who has a viral infection and therefore an activated innate immune system and is in total exhaustion and begins to exert himself? and what he would have discomforts exactly the same as in the ME CFS? if so, that means the cause is the same and the immune system is responsible, right?