Health Rising’s Recovery/Recovering Stories series continues with yet another novel recovery/recovering story. Melissa’s story is the first spinal story in this series, and her recovery was unusual in its rapidity and its one-off nature. One simple, non-surgical procedure was all it took to return her ability to think, to walk, to have her energy back, and to live pain-free. While she’s not completely well, she appears to be on the road to the full health.
- Adam’s BCG Vaccination Chronic Fatigue Syndrome (ME/CFS) Recovery Story
- Can the Japanese Encephalitis Vaccine Reduce Symptoms of Long COVID?
- Lucie’s Surprisingly Simple Chronic Fatigue Syndrome (ME/CFS) Recovery Story
- Up from the Ashes: James’s Severe ME/CFS Recovery/Recovering Story – CIRS-based treatment approach
- A Rapamycin Resurgence: An MD Moves the Needle on his ME/CFS – Rapamycin
- Jason’s Eclectic Mix of Treatments Returns Him to Near Normal Health After 16 Years with ME/CFS
Persistence has been a key factor in most recovery stories thus far.
Her story was not unique, however, in how it unraveled. Except for Rachel’s lucky break with long COVID, persistence has been a key factor for everyone who’s recovered in this series. It took Melissa years of searching to finally find a doctor who would do the tests that ultimately led to her diagnosis – a cerebral spinal fluid leak. After that, it was all so easy…
She explains how it all happened below…
A Cerebrospinal Fluid Primer (from a still-recovering-cognitively non-medical professional)
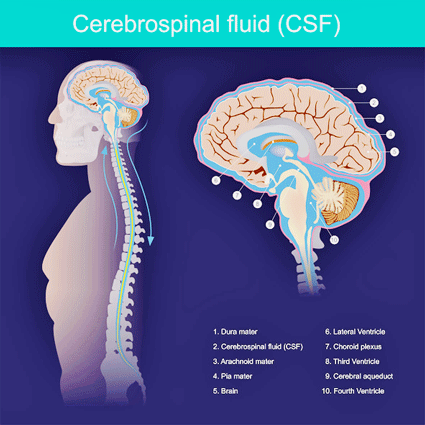
The CSF system is set up so that if cranial pressure gets too high, a leak can open to act as a relief valve. But when something goes wrong (for instance, illness, epidural, or whiplash injury), a problematic valve can be created and the dura becomes unable to seal naturally.
When the brain does not have sufficient fluid, the body compensates by making more—potentially creating a system cycling between high and low pressure. Intracranial hypertension and hypotension each have a variety of possible symptoms. In addition, connective tissue may become damaged by a leak, creating its own issues, including blood flow changes in the brain.
While cerebral spinal fluid leaks at the bottom of the spine in the lumbar region are associated with intracranial hypotension (low cerebral spinal fluid pressure), cerebral spinal fluid leaks at the base of the skull can be associated with intracranial hypertension (high cerebral spinal fluid pressure). Some studies have found high rates of intracranial hypertension in both chronic fatigue syndrome (ME/CFS) and fibromyalgia (FM).
Over time, the brain can sag from lack of fluid holding it in the proper place, affecting nerves, and putting weight/pressure on places it should not be. With the brain suddenly not supported, temperature controlled, or able to send signals properly, multisystem chaos can result – affecting the autonomic system (heart rate, breathing, etc.) and ultimately others. The worsening conditions in each system make functioning more complicated in other systems. (I suspect this may be how we get the same symptom set regardless of a post-illness or mechanical initial onset.)
Cracking Under Pressure

Pre-leak, post-leak (no one was happy but the dog).
Even as a child, I was always busy. Unable to sit idle, constantly thinking or doing or making, then crashing into bed at the end of a long day. No matter the pain or fatigue, I pushed through.
In my 20s, after several months of intermittent flu-like symptoms were followed by bone and muscle pain, I was diagnosed with rheumatic fever. Episodes of debilitating neck and back pain, fatigue, and brain fog continued over the years, all of which worsened with anything but gentle activity.
Still, I was active. I pushed through. I had no idea those symptoms were just pressure. I trusted the doctor’s advice of keeping moving, working harder, toughing it out. In 2019, just before turning 43, I jumped down from the bed of my truck after loading folding chairs for an event. A strange jarring sensation went through my spine, but it was nothing that felt serious.
By the next afternoon, I couldn’t remember what I did for a living. When asked, the information and even the ability to communicate my own confusion about it vanished as I stood staring at a new acquaintance. It was just a blip, minutes long, but that evening, my physical symptoms began to reappear.
As I write this, the connection to a spinal injury from the jump seems obvious. But what followed was a torturous succession of doctors and specialists, tests and misdiagnoses, prescriptions for medications that never had a chance to work. Tickborne illness. Narcolepsy. Postural Orthostatic Tachycardia Syndrome. The list went on. The last doctor I saw before finding my cure, said grimly, “this looks like (ME)CFS, we don’t want to see you back.” I asked about who might help me and was told there was no one. I was on my own.
I was only mildly aware of cranial pressure (IIH and CFS leaks), connective tissue disorders (EDS), and the entire world of radiology at that point, but I had been following the blog for a while. It was with a brutal preciseness that I understood what his statement meant.
It turned out I was not on my own, because the resources at Health Rising and the many patients sharing their stories online, screaming to be heard, led me to eventually discover the underlying cause of my illness. And now, after three and a half years barely functioning and a year bedbound, I’m determined to share as widely as possible in the hopes of helping others.
My symptom list may feel very familiar:
- Cognitive issues (word finding, memory, attention, complicated thinking)
- Exercise intolerance/post-exertional malaise (even minor exertions like brushing teeth, sitting up without support, chewing food)
- Orthostatic intolerance/worsening of symptoms when upright
- Severe weakness/heaviness and fatigue in limbs, worsened by even minor activity
- Near constant dull pain in mid back over rib area
- Headaches when reading or with any physical activity, worse when lying on left side, whooshing heartbeat in ear when lying on right side
- Light and noise intolerance, worsening following exertion
- Severe pain in bones of face after overdoing physical activity
- Scent sensitivity, especially smoke or chemicals
- Blurry vision, less able to see at night, eyes are irritated and appear dull, vision changes
- Occasional face pallor
- Nausea in the morning and when standing, constipation/gut issues
- Low appetite in the morning food sensitivities, gag reflex
- Ringing ears with worsening periods during each day
- Minor swelling in the abdomen, blood pooling in abdomen and limbs
- Must rest several times per day with eye mask and sound blocking headphones. No tolerance for tv, music, audio—visual or conversation quickly difficult to be around
- No tolerance for car rides or movement
- Couldn’t walk at most severe or move around much, couldn’t do physical activity even lying flat
- Disturbed sleep (initially sleeping excessively, later couldn’t stay asleep)
- Severe heat intolerance (heart rate spikes even for attempted baths, crash afterward)
- Stinging pinprick bite-like pains randomly in legs, feet, and arms, and weird electrical jolts through body that cause physical jolt
- Handwriting/fine motor control issues
- Random spots and skin peeling on palms of hands and feet, random minor swelling
- Hiccup-like spasms when upright (rarer, as is cough)
- Inability to summon enough energy to communicate when very ill, sometimes slurred words
- Face tingling, especially when lying down
- Left side neck pain since 2005, worsening in 2019, and shoulder pain and left side muscle spasms since 2005, both (wrongly) attributed to a car accident or disc issues by previous doctors
- Numbness down outside of the left arm and pinky fingers, tingling in hand and elbow, left side pain and weakness dating years prior to 2019 illness onset
- Hearing issues (trouble processing what was said)
- Symptoms improve without movement for long periods
- Intermittent positional watery/runny nose and occasional irritated throat
- Burning pain top of head when sneezing; tender, bruised-feeling scalp
- Droopy eyes, saggy and stretchy skin in places
- Temperature issues (chills, low fevers)
- Mood changes (mine was more obsessive and focused on illness research, but many have anxiety, depression, anger, impending doom, etc.).
Many of these symptoms were misleading when searching for a diagnosis, due to outdated information on the effects of cranial pressure. More on that below, but know that everyone’s individual symptoms can vary despite the same underlying issues. When I first became ill, the list was only a few symptoms long. Others have additional symptoms including seizures, spasms, gait issues, and more, leading to potential misdiagnoses of epilepsy, dementia, and many neurological or nerve disorders.
Getting Diagnosed
CSF pressure issues can be aggravated by flow problems such as stenosis, bone spurs, cysts, or many things mechanical, and made worse by connective tissue disorders (like the EDS I was unaware was in my family) or medication (like the doxycycline I was given for a tickborne illness I never had). While the majority of spinal leak cases are brought about by epidurals gone bad (and made severe when not treated in a timely manner), leaks can have many causes.
Much of the difficulty getting treatment is due to the medical community being informed by outdated material that implies an immediate headache with epidural is the chief or only cause and diagnosable symptom, and that it will heal on its own with time. Some patients do not even have headaches as a symptom. (I would note it wise to verify providers are using the safest needle type and gauge for lumbar puncture.)
Within the CSF leak patient groups, you’ll find many functioning and severe patients whose symptom profile matches those of ME/CFS exactly. Physicians unfamiliar with the true scope of leak symptoms are at a loss, risking unnecessary or harmful medications and surgeries. Brain sag has been misdiagnosed as Chiari in some cases, many MRIs return normal (as was mine), opening pressures on lumbar punctures may appear normal (as was mine), and neurologists and neurosurgeons may not take the suggestion of a leak seriously because they’re considered rare (they are not—only under reported). It is essential to find a specialist experienced in leaks and armed with the most current information.
- Please check the Spinal CSF Leak Foundation Physician Directory for doctors who have been verified to be using best practices for leak diagnosis and repair.
Clues
Pressure may be the cause of your illness, not just a symptom.
- Do you feel worse—either immediately or within days –after strenuous activity such as lifting, high-stress events, after sneezing/coughing, or bending or twisting? You may have a leak or high pressure.
- Have you had an unusual (good or bad) reaction to doxycycline, prednisone, or any medicine that affects cranial pressure? Does caffeine, salt/processed foods, or B1 affect the severity of your symptoms? (Google the medicine or food with cranial pressure to find connections.)
- Do you feel worse in the evenings or have vision or head or neck pain changes as the day progresses? Do you feel worse at different elevations or with barometric pressure swings?
- Do you find your mood shifts with your symptoms after these activities? Are your cognitive or neurological symptoms brought on by bending, lifting, twisting, jumping, straining, or Valsalva maneuver? Is some part of your pain positional?
- Do you have unusual scarring, stretchy skin, or have joint hypermobility in your family? You may have a connective tissue disorder, making leaks and pressure issues more likely.
- Do you ever feel anxious or restless when lying down? This may be high pressure urging you to get upright (to ease pressure in the skull). Do you ever find relief by lying flat? This may be low pressure returning needed fluid to your brain.
- Don’t let the incorrect notion that leaks are rare dissuade you from finding treatment. If you fit the profile and your physician dismisses the possibility, find a new one.
My Cure

A simple non-surgical procedure returned Melissa’s ability to think, her energy levels, her ability to walk, and removed her pain.
My cure was delivered by an interventional radiologist. Her team went over my illness progression, ordered a brain MRI and head CT, both of which were normal (here is where other doctors would have stopped), then moved forward with a CT myelogram which can diagnose abnormalities in the spinal cord.
The CT myelogram revealed several large leaks in the lumbar area, and I received 5 targeted fibrin and glue blood patches in a quick, non-surgical procedure. I had been severely ill and bedbound with extreme cognitive issues for a year.
While I was still on the procedure table, my ability to do math returned. As soon as the post-procedure restriction was up (within hours), I was walking under my own power. My pain disappeared, my energy returned, and I felt hope for the first time since I don’t know when.
Today, months later, I walked my dogs, cooked my own meals, washed my own laundry, and wrote this post. It feels unbelievable, and yet it should not—if I had broken a leg, medical care would have been available immediately. I will still need to overcome what my time bedbound wrought, the cognitive issues as my brain finds its place again, and the trauma of being so ill for so long, but I am not alone.
If you believe you have an orthostatic component to your illness, if you have any relief staying still and flat (or find you are unable to stay still and flat), please research the links below. I had no idea the restlessness of my youth was a symptom of IH, or that it would make me more susceptible to leaks.
So many of our shared symptoms can be explained by the process of CSF leaks: the post-exertional symptoms due to upright activity draining fluid from the brain, the rebound symptoms or worsening baseline due to leaks becoming worse with movement, the reading or eye movement issues due to cranial pressure and nerve involvement, and so much more. Whatever your cause, know that you are not alone. Those of us who have been through will be here, holding out a hand and screaming to be heard.
*There is a 48-hour flat test in the resource folder below from Dr. Ian Carroll. This test is helpful for discerning whether there is an orthostatic component to your symptoms, but please note longtime leakers may no longer have the expected orthostatic response—my own took about 2 weeks of flat time for symptoms to improve and they did so only slightly.
Do you feel better when you lay down and stay down? That’s a good place to start.
*A note on testing: advances in CFS leak testing and diagnosis are moving fast. While traditionally recommended imaging like upright MRIs may be useful for CCI or other conditions, they may not be clear enough to be helpful in diagnosing pressure conditions. Spinal leaks often do not show any signs in a brain MRI. Not only does the imaging required differ, but it is critical the images are read by an experienced leak specialist with a proven track record. Fortunately, several of the physicians listed in the directory below are willing to review imaging or consult with your local care provider.
Do you have an existing brain MRI? Check for SEEPS here.
Resources
- US Facebook Group—CSF LEAKS (Cerebrospinal Fluid Leak & IH)
- International Facebook group—CSF Leaks International: Cerebrospinal Leaks, SIH, Chiari, etc.
- Resource folder from Dr. Ian Carroll (Stanford)
- Directory of Imaging and CSF Leak Specialists—where to go for help
- Melissa’s new website on intracranial pressure and diseases like ME/CFS and FM.
Health Rising Cerebral Spinal Fluid Leak Blogs
Update!
Check out Melissa’s next blog which identifies why some people with ME/CFS may be more prone to getting cerebral spinal fluid leaks.






I have several things on my back, 2 i know/remember is a black disc and a cyst in cerebospinal fluid, problems with neck (was allready operated long time ago) but i am so bedridden i can not go to neurosurgeon and live in belgium so do not know good specialist for cfs leaks, would even can not go. If they allready had the knowledge and equipment to test. had several lumbar punctiors long time ago with headache, throwing , glad you are better! but for the bedbound, it is shit to not be able to go to specialists.up, etc
ps i do not know if cyst in cerebal spinal fluid schriks or not as some cysts do. schrinking, growing, schrinking, etc
If you or a caregiver has the ability, I would recommend joining the international Facebook group and searching “Belgium” or “cyst.” There may be something helpful, even if no specialist is available in your area. I am hopeful that soon more doctors will be available, as there are so many people all over the world who need both the imagining and the procedures.
If nothing else, the group may be able to offer tips you can do from home. I’m less familiar with cysts and the other types of CSF issues, but some small changes can ease symptoms. For instance certain foods or medicines may increase or decrease cerebrospinal fluid production, and certain sleeping positions may help.
I wish you the best.
Melissa this was so well written – easy for the cognitively impaired to digest – nice work. I’m slowlt recovering from a leak too, but just found ijvc from Eagles Syndrome – who knew? Wishing you well in your recovery.
Monne– Thank you. I tried very hard to make it concise, but there is SO MUCH information packed into my brain from this experience. I feel like there are a lot of comorbid conditions that really confuse and complicate diagnosis. I never even suspected my family had connective tissue disorder, but the more we looked into it, the more of us we found were making small adjustments to avoid symptoms in day to day life. I hope your recovery continues!
thanks. I should be able to go to specialists for further research and eventuel treatment but am way to bedbound, alone so no help, and in my country, when i still could go once in a while with help back then (father passed away) in wheelchair, at that time..i do not know how it is now but they even did not have an upright fmri. the equipment is here like in the stoneage and knowledge if i compare. but anyway I am so bedbound…
certain sleeping positions – which sleeping positions could you recommend for CSF leak?
The analogy often used is a nearly empty water bottle. If the cap is the head, tilting the bottle upright at all means the water slides to the bottom, leaving the cap area empty.
So if a person has a spinal leak (a low fluid level) being upright at all can cause the cerebrospinal fluid to empty into the lower areas instead of the skull. Even a pillow can lift the head enough to cause this. Sleeping totally flat with no pillow or sleeping on one’s side with a flat pillow to keep the spine straight may help. If it eases symptoms, this is a great indicator of a leak.
For someone who has high pressure issues (IH), sleeping on a wedge or incline is often recommended—to keep the fluid lower in the spine and take pressure out of the skull.
Sleeping on an incline can be a recommendation for POTS as well because it helps retain liquid, but because some leakers have POTS symptoms, leakers can be incorrectly/unintentionally recommended to sleep on an incline when it actually makes their symptoms worse.
Many people are able to tell right away if this improves or worsens symptoms but some longer-term leakers may need more time to be sure.
Hi Konjin – if someone could help you do you think you could get to a specialist?
After Melissa’s and other stories I’m thinking that everybody who can should have a full spinal check done. Easier said than done, I know but wow, to see how many symptoms these things can cause and to see Melissa recover like this – without having to do some extensive surgery – is really something.
thanks Cort! I wish i could!. I should be able to go to specialists for further research and eventuel treatment but am way to bedbound, alone so no help, and in my country, when i still could go once in a while with help back then (father passed away) in wheelchair, at that time..i do not know how it is now but they even did not have an upright fmri. the equipment is here like in the stoneage and knowledge if i compare. but anyway I am so bedbound… really wish i could go!!! it is so hard to be in need (with so many specialists) and not able to go…
may i ask, just in case, wich tests for spnal courd would all be needed. thouht that i read that this womens storry, the tests, only a few in the US could do…. thanks for the support!!!
I usually recommend only going to a doctor who specializes in leaks, but since you are very limited who you can see in your country and since you already know you have spine issues, perhaps you can call to discuss this with your current doctors. Both my tests and my blood patch to seal the leak were done by an interventional radiologist (they do imaging and minimally invasive procedures) but neurosurgeons and other doctors can do this testing as well.
They will usually do a brain MRI and CT but because you have had previous surgery and they know more about your case, they may want to start with a different test. My spinal images came from a CT Myelogram but they may do a spinal MRI instead.
Your doctors can consult with a specialist from the physician’s directory. And more on testing is also on the website with the directory:
https://spinalcsfleak.org/about-spinal-csf-leaks/diagnosis-of-spinal-csf-leak/
I hope this is helpful!
thank you for your answer. sadly enough, even if i could go laying down in pyjama, the one who operated my neck, had a heart attack and declined a lot. I even do not know if he works anymore but it would not be good to go back there. An other one i consulted when still being a bit better , with help in wheelchair, he did not even come behind his desk to “research” my boddy, reflexes, sharpnes of needle felt, standing on one foot, …the drill…he just asked me what i had because of wheelchair, i said ME. he said, oh, then you have also FM! without even examinating me. I got an laying down mri. from going there, i declined and could not go back with results. in the paper stood “ofcource with only a laying down mri), they do not have upright mri. An other specialist who found something else on my back said only, it gives you more pain and weakness in your leggs and because of ME and no nice one, she said learn to live with it, do not come back. since then , being so bedbound and in wrong position, and a fall, i have way more issues. also here, if operated for neck, they do not like to touch you anymore…not good for their name… is a CT this one (see picture) https://www.lumc.nl/over-het-lumc/afdelingen/radiologie/diagnoses-en-behandelingen/ct-scan/ Is it with contrast? so i have no docters because of being so bedridden, only gp…and am so long not coming out of the home that i do not know/hear anymore who is good. specialised in something… but really thanks!!! for the glimmer of hope!!! i must somehow go but do not know how… ps i was verry ill before the neckoperation and got a brace first and after for moths. not that i was cured, but i could dance!!! 2 weeks after the operation i was allready walking 20 minites every day and it was as if all my ME symptoms, even sleep, you name it, got milder…And i had more strenght in my leggs and arms, etc…
ps but i do not know why i declined back after a year sadly enough..
I’m so sorry you’ve gone through all this. I wish there was a way I could help but I understand how difficult (and often unhelpful) it can be to try to get to new doctors.
I wonder since you do have some images if those can be sent to someone on the leak doctor directory to see if they have any input. Perhaps if your condition improves in the future then you’d be able to find someone who could do a patch or whatever might be needed. Or maybe consider posting them in the international leak group on Facebook to see if anyone there has input. It might be helpful to know if you did have spine issues, because then you could make adjustments to how you move or lay to see if that gave you some relief.
I truly hope you can one day find help. I would love to hear that you could dance again.
thank you sweety!!! but the papers with images are in dutsh. but must look at them first/being able to find them in whole this mess here…
I felt as if , when i needed to build of my neckbrace after operation, I may be totally wrong, but as if i would have liked to keep it on for ever (what is ofcource no good). maybe therefore the decline? i really do not know… thak you verry much!!!
Cort, out of interest, which researcher has our MECFS CSF samples?
Benjamin Natelson has a nice CSF study going – https://reporter.nih.gov/search/hLn5zB6HXkyzPDTgEQ4iNg/project-details/10530012
I’m pretty sure that Avindra Nath did them in his intensive intramural study at the NIH. I wonder, though, if he did the scan that would reveal cerebral spinal leaks..That study should be out pretty soon 🙂
Dr. Peterson has loads of cerebral spinal fluid samples stored. I don’t know if they’re being used at the moment but they have been in the past.
I imagine there are other studies out there 🙂
My son was diagnosed with ME/CFS in 2017 (via an initial misdiagnosis of depression). We persevered with specialists and seeking answers because of the orthostatic component and our hypermobility as a family, and he was able to have a diagnostic – all imaging was normal – epidural blood patch in 2022. He’s gone from now being able to walk to our letterbox to being easily able to walk 12km in a day or 50+km in a week.
He is 22 now. Looking at studying for the first time.
This is amazing! I’m so happy he was able to find help! I felt like I would never convince a doctor to take me seriously and when we finally met with a leak specialist and she talked to me like the symptom list made perfect sense, both my caregiver and I burst into tears. LOL
I also wish there was more information out there about how leaks can affect mood and thinking. It’s such a huge factor.
It felt like a miracle.
He still has headaches now and then that are relatively short lived and barometric pressure seems to affect him(!?!)
Getting in front of the right specialist – in the end it was a general physician with a specialty interest in cardiovascular and autonomic function – who looked at our family as a whole and hypothesised he might have a spontaneous leak because of connective tissue issues. He referred my son to a neurosurgeon who sent him to interventional radiology.
Previous to this he had seen a rheumatologist (diagnosed him with central sensitisation disorder), a neurologist (diagnosed him with focal dystonia and chronic migraine), a cardiologist (diagnosed him with neurocardiogenic syncope) – all these were after he had already been “treated” by a pediatric ME/CFS specialist and children’s hospital ME/CFS clinic.
I like in your article you call it a symptom set that is similar if not identical. I still resonate very much with the ME/CFS community and will be fundraising for our Australian branch Emerge, since my younger sister is now diagnosed after contracting mosquito-borne RRV a few years ago.
I wonder if illness causes connective tissue damage and that’s how they (illness/injury/mechanical) can each lead to leaks. I know for certain my connective tissue went more lax with the severity of the leaks. By the end, I could pull my neck skin past my ear (I was not brave enough to add those photos here ha!) but as soon as I was patched, it had tightened back to nearly normal (or normal for me).
Certainly, there’s an element of high pressure. Many people in the FB group are cycling from high to low pressure, even after patching. Some have stenosis or other issues interrupting flow. There’s also the issue of Rebound High Pressure after patches (where a body overcompensates for a leak that is no longer there).
I notice mild changes with barometric pressure as well, and for me that’s a sign of high pressure. But my main trigger for high pressure after the patch is too much sodium. I’ll start to feel pressure in my head and get blurry vision with that. I’m told it should level out with time, and if it does not they can treat me for IH. You may look into the Rebound High Pressure groups on Facebook if he’s feeling changes with pressure. Sleeping on an incline, avoiding too much salt, and with some people avoiding caffeine or sugar, can really help.
Oh wow – his neurosurgeon didn’t think his headaches would be due to high pressure because of the symptom pattern but I would definitely consider that the level may still be fluctuating even 11 months post patch. He doesn’t eat processed foods and does have a low blood pressure so I don’t think he gets too much salt to be honest but I will ask him about that.
Yes! That’s why I recommended so many times in this post about making sure they are experienced with leaks or consulting someone who is. Leakers have so many stories of neurosurgeons, neurologists, and really skilled and specialized doctors who just aren’t familiar with these issues.
There is information in the folder from Dr. Ian Carroll about rebound high pressure if you’d like to look over that or provide it to your doctor. There’s also a FB group specifically for rebound high pressure–it’s not listed here but if you join the leak group you can search and ask for an invite. I hope this helps!
He may also experience headache after strenuous activity, stress, or other pressure triggers. If it is behind his eyes or the base of his neck or shoulder, feels like pressure or pulling, or is related to his activity or high sodium foods, this may be it!
There’s the story of Jennifer Brea who reported getting ME/CFS after an infection but got cured by treating cranio-cervical instability. I think she has blogged about the topic. So yes, I assume illness can affect connective tissue.
Hi Charlotte,
What a wonderful turn around for your son!
I’d like to look into leaks too as I’ve had CFS since a spinal surgery. I’m in Australia and wondered if we could connect and discuss who to consult? I really want to avoid another run around with doctors.
@Charlotte, congrats, so happy for your son’s improvement! did he have any insomnia/brain fog/cognitive impairment? if yes, did the patch help with these symptoms?
Prior to patch his symptoms met all the ICC ME/CFS criteria without exceptions. And post patch even food sensitivities and heat rashes and sleep issues are slowly resolving. He definitely has his cognition back – that’s been a remarkable improvement.
Hi Melissa! I am so happy for you reading this. I also took this post as a sign for myself. Here’s my long complex story boiled down as much as possible:
I’m 31 years old and started struggling with my health 5ish years ago. I’ve had multiple infections and got worse after each one. Chronic strep throat as a child with PANDAS. A bad case of EBV as a teen. A nasty GI bug in my early 20s. Viral pericarditis in my early 20s. Covid-19 a few months ago.
I have symptoms everywhere. I was first diagnosed with IBS-C and Endometriosis. An ER trip in 2019 serendipitously lead me to Dr. David Systrom. He diagnosed me with ME/CFS and preload failure after an iCPET. He referred me to Dr. Peter Novak who diagnosed me with POTS and Small Fiber Neuropathy. No autoimmune or autoinflammatory processes could be found. Two different geneticists then diagnosed me with hEDS. I also went on to be diagnosed with MCAS and methane dominate SIBO.
Nobody has answers for my chronic 24/7 headaches, neck/shoulder pain, and other neurological issues. It’s been blamed on POTS and migraines.
An EDS pain specialist saw me and said “I think you have a spontaneous CSF leak.” This was February 2022. My MRIs and CTs were normal. I had one of the best leak specialists in the USA do a telehealth consult with me. They said my symptoms were atypical so there was only a 10% chance I was leaking. So my fear made me decide not to pursue invasive testing. I’ve gotten worse since then and my symptoms do seem a bit more typical now…they line up almost perfectly with yours. So I have reached back out to the leak specialist to try again. However, the waitlists at these few good places is so long! Wish me luck!
Best,
Rachel
Boston, MA
Rachel! Thank you for sharing this. There are so many cases with so much going on that it seems impossible to untangle. Even with mine, I’d had a car accident, viral infections, tick bites, a bad wound infection, surgery for a massive fibroid issue, mold exposure, so many factors that I wasn’t sure where to look for help. It wasn’t until I worsened to severe that I felt sure my symptoms were positional and tied to pressure.
They’re making new discoveries and advances in this field all the time and so many of those cases have symptoms no one could imagine were caused by a leak. But the mechanisms are all there. It’s just that no one was looking.
I’m so happy to hear you’re working with a real leak specialist. It really does seem impossible to get the right help otherwise, especially when even the leak experts are still learning new causes and the best testing and treatment methods. Please feel free to reach out to me if there’s anything you have questions or concerns about. I’m also in the leak groups on Facebook. I would love to hear that this helps you!
Hi Melissa, Thanks for your response! You said it all perfectly.
I also went down the tick borne illness path with a functional medicine doctor. Lyme is a huge issue here in New England. I almost took doxycycline numerous times but a little voice in my head has kept me from taking it. Hmmm.
What’s interesting is that doxycycline can cause IH, which is problematic. However, it can also sometimes help people with hEDS! Doxycycline can alter the extracellular matrix in a positive way (it’s messed up in connective tissue diseases). It also has anti inflammatory properties. It’s been known to put some hEDS patients into remission from their POTS, MCAS, etc. But it’s a gamble on how each person will react until we learn more.
I was in the leak groups last year (among many other groups for EDS, POTS, etc.) The groups were both immensely helpful and immensely anxiety producing. I’ve taken a break from them for now. I would love to stay connected with you though! I’m hoping to have leak testing by the summer (fingers crossed).
Oh, I didn’t know this about doxycycline! I definitely had a lot of medication reactions and chemical sensitivities so skipping those as much as possible helped. But while the reaction I had to doxycycline was horrific, I personally know several people in the local area who died within days of tick bites from the bacteria common here—so I wouldn’t have *not* taken it with that risk. My symptoms at that point were less clear to me (and anyone who didn’t know about leaks).
One thing they’ve uncovered is that a lot of us fluctuate between high and low pressure while leaking. So if a medicine lowers or raises pressure, our reactions may depend partly on whether we are high or low at the time. That is to say, the same way a patch caused my POTS and sensitivities to go away could happen with artificially changing the pressure as well. And I think sharing this information is huge for figuring it all out.
I understand completely about the FB groups. It’s easier for me now that I know what was happening and have more emotional space for it, but I find that some days I want to just jump in a car, drive three states away, and deliver someone to the right doctor’s doorstep. LOL I try to pace myself with the groups and stress.
That is so interesting about fluctuating between high and low pressure, because that’s what I’ve been saying it feels like for several years!!! But my Boston doctors at top hospitals all shrug. They all think CSF leaks are rare. It makes you doubt yourself for sure!
Did you end up getting diagnosed with EDS? And how have your other symptoms been like your heat intolerance, tachycardia, constipation, and vision?
How has your headaches and other pain been?
It seems unbelievable to say, but everything bad is gone. Except for the cognitive issues (I had brain sag so I’m waiting for things to … un-sag) and the effects of being so sick for years and bedbound a full year (I get tired easier and need to build back my stamina), I would consider every single symptom leak related and resolved or resolving.
I have no pain. No numbness and tingling. No gut issues (though I have not dived back into a normal diet because I’m still avoiding salt after rebound high pressure), no tachycardia, no mood swings, just nothing bad. I mean, months ago I couldn’t walk, couldn’t eat, some days couldn’t talk. It feels unreal and I’m not sure I would believe it if I hadn’t lived through it and also saw so many people getting this same fix.
Surprisingly, even my connective tissue signs improved. My skin tightened back up very quickly (like the next day) and no one really had much explanation for that except to say that leaks cause damage to connective tissue.
Every case is different and some have dozens of leaks or more complicated repairs. Some struggle underlying with pressure issues and need to deal with that. But plugging the hole is huge. And knowing for certain the underlying cause to prevent further decline. So even when someone doesn’t have a quick fix, it’s at least an answer.
As far as the high/low—yes! This is something new even to the leak specialists. Some of them are more up on the most current findings than others, and some of them are discovering it as they help so many patients with the exact same profile. It makes it really confusing for the leakers to figure out their symptoms and almost every doctor tells them “no, only X or Y can happen with a leak” when that’s just not true.
I think they went so long with this being under reported and dismissed that a lot of doctors can’t accept it as a possibility—but there are *so many* cases that prove it.
I’m very excited/hopeful that you feel like you’ve been having pressure swings because this means you could really, truly be helped by this. I know you have a lot going on, but even if it knocked out part of your symptoms, it could make dealing with the rest so much better.
Hi Melissa, I have brain sag too in my mri had a blood patch week ago as the doctor believe I have CSF leak due to my brain sag but I still have most of the symptoms, brain fog, dizziness especially when standing or in the car, palpitations and other POTS symptoms, but headache is gone, I was wondering if your brain fog already resolve and how many blood patch did you have? how long before your brain fog resolves?
Hi Hanie,
A really important thing to remember is how blood patches work.
Some people may feel immediate improvement because the blood patch may prevent further CSF escape (and they may resume a more normal pressure). But the blood is only meant to encourage wound healing at the leak site. Over the first week, the blood that makes up the patch will dissolve (and symptoms can fluctuate), but if it’s successful, the hole will scab over and seal, and be on its way to fully healed scar tissue. It can take weeks or months for the healing to be noticeable.
This means patch restrictions should be stuck to firmly, even if you’re not sure it’s working, because you’ll want that blood to stay in place as long and possible to allow it to help heal—and because you don’t want the added pressure of being upright to fight against sealing. You’ll also not want to bend or twist, which might reopen the hole. (Think of it like a wound on your knuckle—if it’s bending or you’re bumping it, it’s going to reopen. Only it’s worse, because a spinal leak is under pressure. You’ll really want to baby it and keep your spine straight. Also, it can take up to a year for the dura to fully heal into scar tissue—which means that first year it’s easier to reopen a leak.)
So your brain fog might just be that it hasn’t fully sealed yet. Standard recommendation is 48 hours flat and 6-8 weeks of restrictions after patch. If you have a longterm leak or severe issue, many doctors will have a two week lay flat restriction, only getting up for the restroom (and the car is a big risk because it forces bending of the spine).
Some leaks are bigger or more complicated and need a couple of patches to fully seal. But the fact that your headache is gone is a huge indicator this is your answer! I hope it continues to improve and seals this time, one and done! But honestly for the first few weeks after a patch you may feel weird or symptomatic because of inflammation or while your body adjusts to the proper amount of fluid production. This doesn’t mean it didn’t work. Keep being careful for at least 2 months. Also, look into rebound high pressure just in case that comes up when the leak is good and sealed.
I have a website set up now with patch info. The post patch tips are near the bottom, as well as links to the restriction recommendations. I hope it’s helpful and I hope you’re on your way to being sealed and symptom-free!
https://pressureresources.com/
Below is a link to a post patch graphic that may also be helpful. And each case is different—like with mine an MRV (to look at the veins in my skull) found I had an underlying high pressure condition that probably contributed to my leak. So if you do continue to have issues, this isn’t the end of the road—they can find out exactly what you need. But patience is an important part of sealing leaks. It may be that it just needs a bit more time for the patch to do its work.
https://csfleak.uk/resource/aftercare#set-cookie
same with me, lyme disease, injuries, accidents, mold exposure, so many things happened to me that I never suspected leaking spinal fluid and never even knew this could happen because the doctor that initially performed the procedure said it was safe. My whole life was ruined because of this procedure. I did it when I was 24 and I’m now 59 and just found out about cerebral spinal leaks because every specialist I went to over the past 30 plus years never mentioned spinal fluid leaks.
Any hypothesis lacking objective evidence needs to be very careful, and whether the treatment based on the hypothesis will bring about a strong placebo effect. In fact, this kind of thing often happens, and many CFS therapies are not found to have significant effects after strict controlled experiments.
^_^
Hi Andy. My leaks actually showed up on imaging–contrast was added so that the fluid can be seen spewing from the dura. Long-term low fluid can cause the brain to settle, as part of the fluid’s job is to float the brain in place. This can affect nerves and also put pressure on some very important areas at the base of the skull.
I absolutely did not expect my symptoms to improve so quickly, but most of them were neurological and nerve related, so the fluid being returned to the brain eased them right away. It’s proven and documented. 🙂
‘Spinal leaks often do not show any signs in a brain MRI.’
I am not sure about your specific situation, but the article explicitly mentions this sentence, which indicates that they lack confidence in the sensitivity of the diagnosis. The key is whether your success can be difficult to replicate. Because in most cases, phenomena observed on individuals cannot be successfully replicated in groups.
I’m glad to see you turning around. I wish you a speedy recovery.
It’s true it didn’t show on my MRI, but it did show on the CT Myelogram. I included the note that the MRI was normal so that readers might understand a normal MRI did not exclude leaks. I hope that anyone with an indication of potential leaks finds a specialist who’s familiar with and has experience in leak signs and the proper imaging, because DSMs and CTMs can and do find real evidence of leaks, as well as fistulas and other cerebrospinal fluid issues. 🙂
I for one , am totally confused! Unusual for
me after reading through the report twice! Could I have a cerebral/spinal leak? Only a mysterious person with highly sophisticated equipment could tell for sure!
Although the author tries to write in clear English
, there are stiill too many undefined terms for me to make any determination for myself! I have some, but not all, the symptoms she described. I am too ill to even contemplate following her arduous journey. Sincerely hoping her good health continues.
you should
e
To be honest, “only a mysterious person with highly sophisticated equipment could tell for sure” feels like a pretty good summary of what my journey felt like.
I hope that by sharing my story anyone who has or had an orthostatic component to their symptoms (if they have even one of the listed symptoms and it improves when flat) then they will look into spinal leaks, and I’ve tried to list the best places to start.
I think the message here is that more specialized testing is warranted because standard imaging such as CT or MRI miss a lot of leaks. While it is true leaks are still sometimes missed with specialized testing such as DSM and dynamic CT myelograms- both of these involve contrast injections into the thecal sac and provoked measures including saline infusions to increase pressure to better visualize a leak and/or changes in position and delayed imaging.
There are only a few locations in the US capable of doing these tests- but it’s an invaluable tool.
I will include my personal journey in the main thread.
Years ago, there was a friend who was throwing up, disorientated, head aches, light sensitivity etc. I had to give them a lift to the hospital – ambulances weren’t available where it was but it was pretty much an ambulance level emergency, at least based on symptoms. It was horrendous.
He’d had spinal surgery a week before. No one had even mentioned the potential of a CSF leak, or the symptoms to look out for. Sure enough, he had a leak. If that situation was anything to go by, I’d imagine that even the smallest leak would cause huge symptoms.
Another friend fractured their skull during rugby ruck and maul training once. CFS fluid came out of his nose and all over the ball. It stank. We had to wash it off. By contrast though, I don’t remember that he had lingering problems. Perhaps by the time the skull fracture/concussion symptoms had ceased, it had sealed back up.
It feels unbelievable but these stories are so common. Some of the spinal organizations have noted that the size of the leak doesn’t necessarily correlate with the severity, but my own symptoms did worsen as my leaks worsened.
Cranial leaks have a different symptom pattern and treatment than spinal but I believe they’re considered a little more urgent due to the risk of infection reaching the brain. I’m grateful they were both able to come away from it!
Thank you Melissa!!! I just figured out this is what I have due to 3 episodes of a prolonged, severe, gushing, “water”, runny nose over the last 3 moths. Episodes lasted 48 hours only stopping after the 2nd 24hours spent mostly in the reclining chair. Before that I had been in remission from on top of the other ME/CFS/Pots/PEM, etc symptoms for the last year, after 2 years of moderate symptoms. I’m just coming off my 4th episode which was totally different. 10 days of middle ear fullness with dizzy/lightheaded episodes bad enough I couldn’t/wouldn’t drive. Blurry vision with my glasses prescription changing,. My thyroid TSH which has been stable for several years is doing wild swings and many of the other ME/CFS symptoms are returning. So I made an urgent appt at the local Dr’s group I go to with the first DR available hoping to get an referral to someone who would recommend an MRI and (no) big surprise got totally blown off. Not a shock after dealing with Lyme/Anaplasmosis in 2015 but it still really ticks me off (see what I did there? 😉 to see how far we haven’t come. My Lyme MD is great and she got me what I needed to test the nasal discharge at the lab, if I have another gusher, a month ago. So I scheduled another appt with her today, in 2 weeks, to discuss an MRI. The info you provided here is priceless! Thank you!! There are no Drs in my state on the Spinal CSF Leak Foundation Physician Directory so looks like I’ll have to keep looking. 🙁 I pray you make a full recovery and keep sharing your story to help others,
I’m so happy you’re figuring this out! I’m less familiar with cranial issues, but I know the Facebook groups are full of helpful information–and possibly doctors that have not yet been added to the directory. If not, it’s absolutely worth traveling to connect with the right (experienced) doctors. Thank you for posting. This is exactly why I wanted to share my story. <3 It helps me feel like all that suffering wasn't wasted.
Melissa I am thrilled for you! I’m scheduled for a second targeted fibrin glue patch in 3 weeks. I had 2 dynamic CT myelograms which showed a probable leak and possible fistula- I have a full thoracic spinal fusion for severe scoliosis in 1989 and the level of artifact makes it near impossible to say anything definitively.
Rotated vertebrae, hardware, and bone matrix leaves just a 1mm space for my doctor to target. First high volume lumbar blood patch blew out after I puked and dry heaved from rebound high pressure; first targeted fibrin patch blew because I couldn’t adhere to the restrictions due to caring for my dying pit bull who has since passed😭. However, for 2 weeks post fibrin patch my HR didn’t go above 125bpm (prior to the patch my HR would spike to 150’s waking up a few steps or 180’s walking behind a power lawn mower in the heat). I was waking up and down flights of steps and my HR would often not spike over 100bpm. Also, my anxiety seemed better those 2 weeks.
Such a short time to really assess improvements but enough for me to consider a leak could be a big part of my symptoms. Fingers crossed for this next patch because it takes about 4 months to get an appointment😫
Best wishes and thank you-
elke
It is *such* a journey. I condensed years worth of twists and turns here but, absolutely, I feel you on this. My heart rate once spiked to 170 reaching for a glass of milk and I’m not going even going to count how many months I went without a shower. LOL
I’m so happy you were seeing improvement after patching! I know there are several patients who share my doctor that have more complicated situations and needed a couple of rounds of patching to get their leaks under control (one had 17 leaks) and at least some of them are through that process and nearly symptom free, so I’m hopeful that means you’ll just need another try.
I hope life doesn’t throw anything new at you before you have a chance to recover. <3 For me, it helped to call in all my favors, have food prepped and easy to grab, and everything I needed at chest level for post-patch restrictions. (I did no bending, lifting, or twisting for 8 full weeks because of connective tissue concerns.)
Thanks so much, Melissa, for giving us yet another avenue to explore. How was your patch administered? I can’t seem to find details online of how this was done. I also wonder if a person has spinal stenosis, would that render the patch useless? As you wrote, people can have many other health issues, and doctors being specialists in one studied organ can “pass the buck” to a different specialist. For example, bad allergies can also cause headaches, eye swelling and a sensation of pressure in the head, and many get no relief from allergy medicines. Ménière’s disease comes with vertigo is a person consumes salty foods (inner ear fluid retention). I have found that the biggest emotional toll is seeing doctor after doctor, without results. I don’t know how you waded through the swamp of misdiagnoses.
Exactly. My doctors were diagnosing conditions secondary to the leak, refusing to even discuss whether there was an underlying cause. It’s not natural for a person to suddenly have a half dozen different neurological issues—it definitely indicates something else is going on.
There is often something happening to create leaks. Sometimes this is stenosis, but while stenosis can slow flow and lead to intracranial hypertension that puts the system under high pressure, making people more susceptible to leaks, leaking means that every movement (or simply being upright) is gushing fluid out of that system at a rate that can’t be kept up (not to mention the escaped fluid has nowhere to go). The right imaging with doctors specialized in these cases can not only help find the leaks, but any underlying structural issues.
If illness or connective tissue disorders have weakened the dura and that led to leaks, then those may need to be managed, but the leaks still need repaired to avoid a worsening overall condition.
My blood patch was done under conscious sedation. I was face down on an imaging table and they numbed my back where they inserted image guided needles. They injected blood (over the leak without making a new puncture) and my job was to tell them if I felt pressure or pain. This part sounds a lot worse than it is because needles are scary, but for me it wasn’t. Compared to how leaking made me feel, the whole thing was cake and I was embarrassingly giddy with excitement. Once the blood is injected (and also sometimes glue to help hold it in place) then you’re supposed to stay flat for a few days to prevent reopening the hole. The patch encourages healing and if all goes well, eventually scar tissue is formed to permanently seal the hole.
You can see more about blood patches here:
https://spinalcsfleak.org/about-spinal-csf-leaks/treatment/
Thanks so much, Melissa! Is it your own blood they’re injecting?
Yes! They just took a bit out right there on the table (I forgot to mention the IV for this) and used as much as they needed. Out one needle, in another.
The tell take signs of csf leak?
I think I may have it
Can someone chime in how to identify it as the test she mentioned Myelo….. MRI isn’t available to me
An orthostatic headache is the main indicator of a leak. (Headaches when you are upright that go away or improve when you lay flat.)
However, there can be many other symptoms like those listed in the post. If you feel much worse when standing and your symptoms either go away completely or improve when you lay down, then you may have a leak.
It is also possible that people who have been leaking for a long time will lose the positional element to their symptoms and just feel bad all the time (up or down), so if your symptoms aren’t positional now, try to recall if they were when you first got sick.
Most doctors will start with a brain MRI but to find a spinal leak they may use a CT Myelogram. It’s very important to find a doctor who is experienced with leaks if you’re able. There’s a physician’s directory in the post you can search. Many doctors can do a blood patch, but if you’ve been leaking for a while, you want to make sure that you’re seeing one who knows how to treat the more longterm or severe issues.
So is it ME recovery story because ME is all about a yet to have been diagnosed like the CCI surgery people and this CSF leak? Or a actually u don’t have ME and we can treat you!
Are there any true ME recovery stories then? That is, not attributable to any other condition. This makes me feel very confused on what I should think about ME.
Because a cause for ME/CFS hasn’t been identified, it’s impossible to say. But whether leaks *cause* ME or leaks are *caused by* ME, great relief can be found in resolving the leak.
I’ve felt this confusion when searching for my own diagnosis, but having been misdiagnosed countless times and now knowing that many of my diagnoses were real and secondary to a leak, I think of it like this: when they one day announce a definitive cause of ME/CFS, it will not change the actual condition, only the way the medical community and the world at large refers to it.
Jerry, I tend to agree if you view MECFS as a diagnosis of exclusion rather than just a collection of symptoms. In this case, the leaky CSF necessarily excludes it from MECFS diagnosis. The underlying mechanism leading to MECFS symptoms, however, could be the same in both. Namely:
persistent intracranial pressure -> hypersensitive brain -> MECFS symptoms
one-time viral infection -> persistently hypersensitive brain -> MECFS symptoms.
At least, that is how I not get confused about MECFS and these MECFS-like cases.
I find it interesting too that an illness preceded the leak. I believe I had IH (high pressure) as a child, but it wasn’t until my 20s that the pain, fatigue, and brain fog came on–directly following an illness. I’ve always wondered if that counted toward a post viral onset, potentially damaging my connective tissue so that when I jumped from the truckbed years later, I was more easily injured (resulting in the leak).
Yeah, I guess it is possible that the head pressure was a risk factor and the illness triggered MECFS. But you recovered when the leak was plugged, so the leak/pressure must’ve been the cause of the symptoms. I can’t think of an easy way to explain having MECFS first and then recovering from it after the accident and plugging the leak years later. If that is how it worked, then that would suggest puncturing and then plugging the spine should be considered a therapy 🙂
If the illness that causes MECFS primes the spine for the leakage, then we should see prevalence of CSF leaks in long COVID patients. Or you could ask CSF patients group if their MECFS symptoms started after an illness prior to the leakage, like yours have?
I would not recommend trying a puncture to recover. haha And, yes, absolutely, all my symptoms were caused by and resolved by the leak. I just wonder about how we are identical in symptom sets and how many leakers are hiding among the ME/CFS groups.
There *is* a great deal of POTS in the long Covid group, and I wonder if that could also be connective tissue damage related. But I am not educated enough about any of those things to do more than guess.
I really forward to researchers learning how infections contribute to spinal leaks and to structural spinal issues as well such as craniocervical instability. Something to do with weakened connective tissues perhaps (?)
I also find it very interesting how in high pressure our brains encourage us to get upright and move and with low it cripples us with heavy, weak limbs and the desire to lay down anywhere and not move, compared with the way FM patients can do gentle exercise but ME/CFS can’t exert. Not that the two are directly related, just that it seems like another interesting association (IH and FM groups may feel better with gentle walking and leakers and ME/CFS groups may feel worse). I think it would benefit both groups to compare research and share tips for dealing with cranial pressure.
I think it’s best to think of ME as a symptom or collection of symptoms rather than a cause. In other words, don’t think of ME as a disease in and of itself, just a group of symptoms that can have many possible causes. The helpful thing about this website is reading the many possible causes. In the absence of doctors with free time to research our condition as we deserve, we are left to do our own research. I feel worse if I think about the lack of helpful doctors, and better if I think about my health issues as my own personal laboratory to experiment with. I prefer to think of my conditions as “quirks” rather than an incurable disease, though I don’t expect any answers or cures in this lifetime, just adaptations. I have learned through reading and “investigating” and experimenting that I will get vertigo and a full head and headache if I consume more than 400 mg of sodium in a day. I’ve discovered many other things about my body, and I realize how individual our bodies are, with their own unique sensitivities based on genetics, lifestyle, and whatever pathogens we may have been exposed to in our lives.
From what I’ve understood the statement here is that CFS leaks can cause many of the same symptoms ME/CFS does, is that correct? Do you have any idea how those people on the very severe /severe end can verify that they do not have a CFS leak? Seems like it is neither connected to a viral onset, nor are there unusual clinical findings in CSF leak research apart from brain scans?
I don’t know that the two are exclusive–perhaps damage is done to connective tissue from an earlier or unknow viral event in leakers and that causes the mechanical issues, or perhaps ME/CFS can cause leaks. Possibly ME/CFS can be triggered by either viral *or* mechanical issues. I saw more than 17 specialists during the course of my illness and I do not know that there was a single finding that might rule out ME/CFS.
I was severe and understand that getting to appointments can be devastating. I would spend several weeks before each appointment lying as still and quiet as possible in preparation and we had a series of cushions and pillows inside the vehicle to keep me relatively flat and jostle-free. My own leak specialist does her initial visit via telehealth so that patients can send over any prior imaging and their illness progression list for review beforehand. This is ideal.
Unfortunately, spinal imaging is the only way to check for leaks. The specialists may be able to suspect leaks with a great deal of accuracy, but to be certain what’s happening they need to see your brain and spine. If you have a positional element to your symptoms or can remember any positional element before you became severe, then this is absolutely suspect. For me, some indicators when I was bedbound were a worsening of symptoms when I turned my head, lifted my arms, or chewed (jaw movement), strained, or twisted at the spine–but I wasn’t really able to make that connection until after I knew I was leaking. My head felt heavy and my neck couldn’t support itself but I did not have CCI.
It’s difficult also that many leakers experience different symptoms. What was a clear trigger for me may not be for you. The Facebook group is a good place to find people with the same symptom set and look at what their imaging has told them.
I’ve gone on longer than I meant so I’ll end with: if anything is or was positional, contact a leak specialist.
Thanks a lot for your lovely and detailed response!
I have quite a lot of questions about CSF leaks as it’s the first time I’ve heard about this, even though “similar” things such as CCI, tethered cord and Chiari have received a lot of attention. From what I’ve gathered there are two kinds of CSF leaks, cranial leaks and spinal leaks. From what I’ve understood they can results in different symptoms, for example meningitis only being part of the one but not the other. How different can these symptoms be and which one did you have?
Are there strong viral connections of leakers to viral diseases, for instance the same ones as for ME/CFS being HHV-6, MERS-SARS, Covid or EBV-reactivations (and the others)?
It seems like cranial CFS leaks often lead to a high chance of contracting meningitis, which doesn’t seem to be the case for ME/CFS, can meningitis be of value as an indicator of CFS vs cranial CSF?
Are there any theories why in a minority of patients CFS leaks lead to ME/CFS-like symptoms, but normally not? Are there any theories why women seem to be more affected?
I saw that you mentioned disturbed sleep as one of the many symptoms, is unrefreshing sleep also a symptom, i.e. feeling worse waking up than going to bed?
You mention that PEM can be part of the CSF leak picture. What about exercise that is done, whilst lying in bed flat on the back, something ridiculous as having a hand-bike attached to the ceiling or lifting weights while lying flat in bed?
For the very severe patients: You mention that a good test is understanding your symptoms standing vs lying down, does the same hold true for sitting on the bed, back leaned against the wall and legs straight vs lying flat in bed?
Not necessarily for differentiation, but also to try to explain the mechanisms of ME/CFS, do CSF leakers that don’t have ME/CFS also share some of the visual symptoms of ME/CFS like Crimson crescents, Covid-toes, marble hands, white tongue and red eyes?
Thanks a lot, as you can see I have many questions 🙂
Thank you, these are GREAT questions! And they all apply so I’m glad you asked. I didn’t want to overwhelm the message of the post with side tracks because I think the most important thing I wanted to get out there was RESEARCH THIS and that only leak-specific specialists will be able to help. But I’m happy to answer anything here.
I had a spinal leak (mine were mostly in my lower lumbar area but I also had some tiny leaky spots in my cervical area and just overall not a great looking spine–scoliosis can be another factor). The symptoms of spinal leaks can be any number of items from my personal symptom list posted above but also nerve pain issues, seizures, tremors, gait issues, balance issues, vertigo, mood disorders, and the list goes on. The tricky bit here is that many leakers are functional and have only mild or limited symptoms. Some may have headache when standing and that’s all.
I know far less about cranial leaks, so I’m hesitant to give too much information here and cause someone to dismiss this as a possibility. I hope those will look up resources online. People can also have cranial and spinal leaks at the same time, so that’s a complication. But most of the cranial leakers have headaches and watery discharge from their nose or mouth. Many can have vision or hearing issues.
I’m not certain whether there’s a strong viral connection to leakers. I’ve noticed despite each group’s similar symptoms, much of the ME/CFS focus will be on viral connections while the leak groups look for physical connections first. But medical histories are complicated and something as minor as twisting the wrong way may not seem significant in the ME/CFS group because they’ve not been told to look for it. There is a strong connection to connective tissue disorders, though, and EDS is common among long-term leakers.
The majority of leaks in women will happen with epidurals during childbirth. So that’s a big factor. But aside from that, there are many different origin stories. Weightlifting, chiropractor adjustments, spine surgeries, bone spurs, falls, and countless others can cause spinal leaks. Also, injury by windows coming down on heads is oddly common–any sort of jarring of the spine. Whiplash from car accidents is a big one for cranial leakers.
Leakers can be severe or highly functional, much like the severity scale with ME/CSF. And they also have the crash after overdoing activity. Each case depends on the leak, but for me lying totally flat and doing exercise still led to PEM. I believe with mine any movement of the spine was problematic. I only felt improved if I didn’t move at all for weeks at a time, even shifting in bed. I tried various positions and activity levels but even when I was more functional, bending, lifting, reaching, and straining, or overexertion of any kind (including just standing too long) brought on symptoms. Mine tended to be delayed 1-2 days and followed a pattern with symptom type and mood. When I was very severe, even conversation going on around me could lead to a crash.
It can be harder to judge for severe cases because the positional aspect is less easy to accomplish and may diminish over time. But I did notice changes in my symptoms (often pain, numbness, heart rate, and air hunger) when I was totally flat versus being titled upright by pillows. I also had more confusion when upright, so it was much harder to focus on how being upright affected me. The main thing is that when your body is flat and head-down, cerebrospinal fluid can get to your brain. When the head is lifted, it runs out (think of a water bottle partially full on its side versus standing).
Yes, unrefreshing sleep can be a symptom and was one of mine. Initially, I had excessive sleep, then later it became disturbed sleep, but it was never refreshing.
Leakers can have bloodshot eyes, blurry vision, symptoms after eye movement, and even different sized pupils due to pressure and nerve issues. They also often have discolored hands and feet (mine were purple and splotchy, especially if I tried to shower, but sometimes red and sort of shiny, and I also had occasional face pallor). I do not know about crimson crescents but many have throat issues and mine certainly had days where it looked suspiciously red in that area.
I see a lot of CCI, EDS, tethered cord, and other conditions in the leak groups, so I believe the overlap for a lot of these conditions is substantial. But I’ve also seen brain sag misdiagnosed as Chiari so I think it’s important to find a doctor with knowledge of both.
I believe meningitis is only a risk with cranial leaks because a hole there leaves the brain exposed. I wouldn’t use it as an indictor because leakers usually try to get treated before infection.
Please let me know if I missed anything!
Did you ever have any weird taste in your mouth? I don’t have orthostatic issues (that I know of), but I do know that the base of my skull is where I feel all my pressure and sensitivities—like if I watch something for too long, say. It’s not pain, but it gets stiff. I’ve had neck issues for years, well before this, and I always wondered if there was something there. How does one get this type of imaging done? Can you just ask your PCP?
This may be related to Intracranial hypertension (IH) but I am less familiar with cranial issues. There are many in the FB groups who have similar symptoms. I have not had a weird taste but those who do sometimes have leaks or IH.
A head and neck MRI may give you information but it can be difficult to find doctors who take this seriously since most consider it rare or have outdated information. If possible, I would recommend a doctor who specializes in IH specifically or someone off the physician’s directory. And the FB groups are a great way to find information more specific to your symptoms.
This could be the same case as Jen Brea and Jeff (I forget his last name), with CCI creating intracranial pressure and causing MECFS symptoms. The treatment probably is not applicable to patients with sudden onset after viral infection (like COVID) or overtraining, but the underlying mechanism that leads to the symptoms could be the same. Researchers should look into these cases more closely to unravel MECFS.
I have long term FM with symptoms that became so much worse after having hip surgery. I had intense feeling of pressure in my head. I could feel the pressure above my eyes, and the back of my neck was extremely painful with a feeling of more pressure. I joined an IIH group on social media to learn more about the condition.
The mostly young women with this disorder suffer tremendously. It is difficult to find a competent doctor even in the US. The medicine they take like topamax often makes them feel worse. It seems to hit women of child bearing age. Many of them are very ill, and they have young children to care for and an unsympathetic partner as this is another presumed “imaginary illness.” They often end up getting a series of brain surgeries to add stents and shunts, a process that may require repeated brain surgeries.
I found my relief in taking a few supplements mentioned on this blog so I think my problem was mostly caused by a high level of neuro-inflammation instead of a spinal leak or some type of physical problem as those with IIH generally have. There are some similarities with those of us that have CFS or FM. They also suffer from POTS, and they also may develop seizures and eye problems from optic nerve inflammation.
I’m so sorry you hear you went through this. I agree, and worse, many people with IH get leaks because of the additional pressure and can end up in a cycle of repair leaks/return to high pressure/leak again. I am hopeful advances in imaging will better discover the underlying issues creating IH to avoid stents and shunts and that improved treatments are coming. I’ve heard great things about the effect of B1 on high pressure but I did take Diamox after my patch and tolerated it well (I was also able to quit taking it as soon as my body stopped overcompensating for the leak.)
But many do return to health with the proper pharmaceutical, surgical, or natural treatments and lifestyle changes–I think they just leave the groups once they recover.
Hi Karen,
I definitely have neuroinflammation and eye problems. What supplements helped you?
How did you come to suspect a CSF leak, Melissa? Did you read about it here and then follow it up yourself?
I’m so glad are feeling better.
Yes! This blog saved me. I had a friend who had a friend with ME/CFS and suggested I look into it, which was how I came here. I’d been experiencing every symptom listed for ME/CFS and took all the tests the posts offered–the at home POTS test and did the breathing in a paper bag hypoxia test, whatever I could find–then researched every aspect of the illness. It was a lot. But I couldn’t get doctors to help me.
At first I disregarded the mechanical issues because I’d been told my tingling fingers and neck pain were related to other issues and because I’d never shown signs of EDS. I’d been told my onset was a tickborne illness, but I joined the Serimmune study and discovered I’d never been exposed in the first place. Which made the reaction to the doxycycline they gave me clearer. Then I became severe when I jumped from a low porch to chase after my escaped dog. I felt off with the jump–the same as I had when jumping from the truckbed–and by the next afternoon I knew I’d made a mistake.
I began to look harder at mechanical issues and the leak just fit. I would have never seen it without the advantage of hindsight.
I cannot express how amazing it feels to come back here now and be able to post about my recovery. I want to shout at everyone to check their spines. LOL
Hi Melissa, ME/CFS is a disease that can have multiple causes. See all the different subgroups. Probably a small part has the same problem as you. I would shout it from the rooftops too if I were better. Let’s hope that a solution will also be found for all other subgroups. Good luck with your further life! Enjoy it!
I have been ill for decades with no prospect of a cure. Best wishes
I don’t mean at all to be insensitive to other subgroups, Gijs. This was a horrific experience for me overall, and I’m so grateful to be in a better place with it than last year. I feel like there are likely others like me here and I hope I can help them the way this group has helped me, but I plan to advocate for all of us.
Thank you Melissa. You’ve given me much food for thought. Doxycycline side effects, “overly mobile” and something else you said which escapes me now 😒 plus almost 100% of the other symptoms you mentioned resonate with me but I’m nowhere near as ill as you have been although lying down most of day ,homebound ,barely walking and only capable to do a little cooking nothing much else. Stay well.
I started out being much more functional as well. In the beginning I had just a handful of symptoms and on some days could almost convince myself it wasn’t that bad. But I always felt a little off, something vague but wrong-feeling. Now I can see that was my brain trying to get me down to adjust for lack of fluid. But as I kept pushing through, I injured myself further attempting to “get healthy” with things like physical therapy or bending forward too far in yoga, and continually made my leak worse. Lifting, jumping, bending were all very bad for my baseline because the damage was at my lower spine. It seems like people have a bit different symptoms and triggers when the leaks are higher, but all of us feel worse when not flat.
I hope this helps!
Melissa thank you again for the insights. Amongst other strange symptoms through life, 10 years obsessively creating a big garden, working till exhausted and till my lower back was screaming ie pushing through, and was numb was probably the ,”killer”. I will ask questions.
Very interesting. We have to be detectives sometimes to notice things, and put all the clues together.
I don’t have CFS, I have something similar to POTS, but I have learned useful things from this site. Cort does a great job!
I am absolutely sure that some people reading this will have an “Aha” moment and be lead to a CSF leak diagnosis.
Help! This is scary! That is my complete list of symptoms bar very, very few!
I doubt if I can get any help in Australia – doctors are so far behind the rest of the world.
I had a whiplash injury when I was young, and a couple of ?minor spinal injuries.
Esther, Macquarie Neurosurgery, in Sydney is named in Melissa’s information if you can look through it. Also Physicians in WA. It is a massive thing physically and financially to
undertake but if one is desperately ill there is hopefully help out there. Also long distances to travel in Australia and of course quite long waiting lists.Hope you can get some help.
Thank you, Peach Blossom. I will look into it.
I know it is far more difficult in other countries due to lack of these specialists, but if you can join the international Facebook group linked in the post, someone there might have a doctor recommendation that has not yet been added to the list. Some people also try to self heal at home by staying very flat, but with severe leakers or certain types of leaks that may not help. The leak groups can feel overwhelming at first but there is so much information available. The fact that you have a history with spinal injury may be huge—I hope you can look further into this and find someone who’s able to help!
Hi Melissa, I am so glad you were able to find a cure and successful treatment so you can return to an active, normal life.
I take issue, however, with classifying your case as ME/CFS. A collection of symptoms doesn’t prove this diagnosis.
This is where researchers and government agencies have failed us over the years. If you read Hilary Johnson’s, Osler’s Web, the seminal book on the ME/CFS epidemic, you will begin to understand what ME/CFS really is and why no official cause may ever be identified.
I do not mean to offend and in fact am less educated on the history of these conditions than I would like to be. I only want to reach any others who follow this blog who might also benefit from information on leaks. It is my hope that the sharing of our stories and resources aids all of the conditions we suffer from. But having one condition does not exclude a person from having another. Someone with the proper diagnosis of ME/CFS may also be leaking and need this help. I’ll look into the book you noted to learn more. Thank you.
Hi Melissa, Thanks for your thoughtful reply. I often think, however, that Health Rising has become too inclusive. What started out as a focus on ME/CFS has now expanded to long Covid (an illness that has a discrete origin); Ehlers Danlos Syndrome (a genetic disease with 13 variations) and now spinal fluid leaks.
If your story helps others on this expanded HR list, that is wonderful, but I do not hold out any hope that it will help a classic ME/CFS case.
Some additional notes:
Blood patches are fairly common after epidurals (the number of epidurals given each year after childbirth is staggering and a fair percentage go wrong) but those patches are administered minutes after a small needle-sized injury and have a far more likely chance to heal. It’s imperative to see a leak specialist for your patch if you’re a longtime or severe leaker. Someone not experienced could potentially make the situation worse and will not be aware of follow up care if you happen to suffer rebound high pressure (RHP is when a body that has been compensating for a leak is suddenly patched and now makes too much fluid for the sealed system. It can take days or weeks for your body to balance out so sometimes medication is used to lower pressure temporarily.)
All this to say: I wouldn’t recommend trying a random “blind” blood patch at your local doctor to see what happens. Research first, then decide.
There are also many who try to self heal at home. You can find information on that here https://spinalcsfleak.org/about-spinal-csf-leaks/treatment/ but self healing may not happen—there seems to have been something that went wrong in the process or otherwise it would have healed sooner.
I failed to mention in the post that some leakers get MCAS. There are so many potential side effects of longterm leaking.
Leaks drain the skull of fluid, leaving the brain unprotected and causing it to sag, doing damage to nerves and putting pressure where it should not be. Longterm leaking means that over time these conditions can grow worse and create physical and cognitive issues that no one wants to be permanent. If I could go back, I would ask myself to be more gentle and stay flat. I didn’t know I was leaking then, but I can look back now and see that I was struggling more than I needed while trying to keep up with daily tasks. It’s okay to let some of them go, but making things easier on yourself can actually reduce further decline. If you suspect you’re leaking, you can try keeping your chores at chest level when upright (or try staying with your head level with your spine if you’re bedbound).
Thank you for writing this important piece. I am so glad to hear you’re doing better. Your symptom list is quite familiar & extensive! There is so much symptom overlap with intracranial hypotension & other health conditions, that broader awareness of it is warranted. The imaging and diagnostics for leaks can be so tricky and I am glad you made the points about the more advanced imaging (the CT or MR myelo). I know some people who suspect leaks but are too nervous to get the myelograms and risk things like worsened leaks or arachnoiditis. Curious, did you feel the CT myelo gave you any new or worse symptoms (even if it was ultimately worth doing)?
That is a great point, thank you for bringing it up! As with any medical procedure, there is risk. Between the contrast and poking around with a needle where so many important things are, it’s definitely something to consider.
I *did* feel worse after the CT Myelogram (same symptoms, just a bit more severe with the added spot for fluid to escape). This is why it is so important to find an experienced leak specialist. They should go through a thorough medical history, then complete less invasive testing first. I’m not sure anyone should be going straight to a myelogram. But if your symptom profile fits for leaks, those more invasive tests may be the only way to find the hole, tear, fistula, or whatever is causing the leak.
Leak specialists will also be familiar with EDS and anesthesia sensitivities, so their procedures will differ. Mindful of those risks, they should use the smaller needles of the proper type and be ready for any potential reactions. Mine was done under conscious sedation and they checked with me throughout for any numbness, pain, or tingling. They can also do a quick targeted blood patch at the site of the puncture to prevent any further issue–while there are exceptions, the main problem with leaks is not so much the hole (because leaks occur and seal in a normal system) but when they are allowed to leak long-term. (If a person has EDS and is less able to heal, then this is a more serious consideration.)
For me, the higher risk was *not* getting the imaging. I had progressed to a point that I was losing the ability to eat and to communicate. I would go into a sedation-like state and be unable to open my eyes, move my limbs, or speak, and I could not tolerate more than 1-2 foods and was developing swallowing issues.
It’s important to weigh the risk of the damage to the brain against the risks of testing. The team of specialists and I both felt with great certainty that my case was a leak. I’m sure there will be cases where this decision is harder.
Thank you for your excellent response! 🙂
Hi Melissa,
Thank you for your article and I am so happy that you are well on the road to recovery. My son has been sick since 2012, after we thought a viral onset. He has continued to deteriorate, and now he is not upright except for meals and a shower. I am still convinced we are missing something. We did an upright MRI a couple of years ago and a CT scan to rule out CCI and a leak, they said everything was normal. Although a number of years ago he was diagnosed as having a 9 mm Chiari Malformation but they said it wouldn’t cause his problems. I have emailed one of the specialists to at least see if they will review his case. Wish us luck!
I am so hopeful that this is your answer! I believe it’s possible that we become more likely to leak after an illness, whether from raised cranial pressure or damage to connective tissue, but I’m not sure how long it will be before science digs into that.
There are many people in the Facebook groups who were diagnosed with Chiari that was actually brain sag from longterm low fluid, and from what I understand, the upright MRIs are not as well able to show leak signs—should the doctor even know what those signs are. I’m so happy you’re seeing someone who has experience with leaks because it’s so difficult to be certain otherwise.
I’ll be pulling for you both! That’s such a very long time to suffer, but I’ve seen many who leaked longer and patching still worked!
I feel better when lying flat, but couldn’t my POTS diagnosis explain this?
Also, mestinon almost completely cured my headaches and migraines. would this indicate I probably don’t have a leak?
Spinal CFS leaks can actually cause POTS, or you can have both. There is a 48 hour flat test in the Google Drive folder linked in the post from Dr. Ian Carroll at Stanford that can help you differentiate the symptoms.
My POTS symptoms resolved with a patch, so for me they were clearly caused by the leak.
There’s also a video here that explains some of the symptoms that indicate a leak (like ringing ears) that are not present in POTS. https://youtu.be/wpdk8BS4Xf0
I do not know the effects of mestinon on leak symptoms but any medicine that affects cranial pressure, water retention, or blood flow can change the amount of pressure in your skull and affect symptoms. Sometimes medication can mask the positional aspect of the symptoms.
Anyone who has POTS and also neurological “weirdness” or any combination of ringing ears, nerve pain, numbness, vertigo, hearing issues, PEM, headaches, etc. should definitely look into leaks to be certain.
Thanks for your quick response Melissa!
So I have, or use to have, pretty much all the symptoms common to both illnesses, as highlighted in the Youtube link. But of the spinal CFS -specific symptoms, I’ve only had light and sound sensitivity, and only during really bad crashes.
Still worth pursuing? If so, any doctors close to Toronto that can be trusted to fully investigate? The directory tells me to contact Spinal Cfs Leak Canada.
So, my thing about accepting an illness without knowing the specific cause is that there is always a cause, even when we don’t know what it is. If it’s possible that a leak caused your POTS then finding out might offer a cure. That’s why I always want to check first. A lot of current medical diagnoses are diagnoses of exclusion, and when an illness is excluded based solely on the fact that it’s considered rare, then it’s no real exclusion at all.
There are a few ways to attempt separating leaks and POTS symptoms. Here is a link to the 48 hour flat test with instructions. It will give you a hint what to look for when deciding whether a symptom is POTS or not. https://drive.google.com/file/d/1ddUJJy00ew29hc1NzlVhCjwgcv6DdLiL/view?usp=share_link
And here is a questionnaire that may help sort what you’re feeling in relation to upright or downtime: https://docs.google.com/document/d/15Jv8NN1ZchapIjKnMURWO-pJA_spa3zZbeEApQ36GGo/edit?usp=share_link
It will likely become clearer if you watch for how things like sneezing, straining, bending over, etc. affect your pressure or pain, and to think about any other connections you may have (old injuries, surgeries, chiropractor visits, etc.). How do you feel when you wake in the morning vs at night, do the POTS symptoms come on as soon as you stand or after you’re up for a few minutes, that sort of thing.
If you have an existing MRI, you can also look for for signs on that using the SEEPS link in the post. If you can ask yourself these questions and be aware of when your symptoms are better or worse in relation to certain food, medicine, activity, and position, you may see a connection. Also think about your POTS onset and whether it was days or months after an injury or accident (mine was jumping down from a truck bed but I’d been sick, had surgery, and had mold exposure the year before, so I believe those may have contributed by damage to my connective tissue, so that the jump was able to do its worst).
When you have crashes, is it because you’re dehydrated or is it because you lifted something heavy? If you can sort triggers, then you should be able to categorize it.
Oh, and to find a doctor in Canada–there is a Canadian leak group on Facebook. I am not familiar with it but I have seen it discussed, as well as some in the International group mentioning their Canadian doctors consulting with Duke hospital for leak patients. Or you can email the contact in the directory–I’ve heard they’re very helpful.
It’s very much worth pointing out, that Melissa fit the classic ME/CFS ‘personality’.
As you described yourself: “Always busy. Unable to sit idle, constantly thinking or doing or making, then crashing into bed at the end of a long day. No matter the pain or fatigue, I pushed through.”
THAT’S what causes ME/CFS. That’s what led to her spinal leak(s). And if you’re newly diagnosed, or even later on in your illness, changing that fight or flight dominant state, to a rest and digest one — will be of HUGE benefit. You may need to be patched, but maybe not.
I’ve been reading Health Rising for many years – such a wonderful resource, thank you, Cort!
My son was diagnosed with ME /CFS in 1993 while at university. By 1997, he had severe fatigue and was unable to sit up or talk. After spending 10 weeks in the National Hospital of Neurology, London, he learned to speak and walk again.
By 2003 he was 50% recovered – driving, studying, teaching guitar. However, possibly because of medication give in the National, he’d developed a kind of chronic dizziness/vertigo, seeing normal objects move backwards and forwards, and feeling an inner sense of movement, which has never left him and has grown more intense over the years. This kind of vertigo doesn’t seem to be characteristic of ME.
2003- He had a fever, sore throat, swollen glands and was eventually diagnosed with Epstein Barr. Recovering from the fever, he developed an indescribable headache which has never responded to any medication. He feels very ill but doesn’t suffer from extreme fatigue, although doing things for half an hour intensifies the head and the vertigo. We pursued treatment for Epstein Barr. Dr Lerner’s protocol seemed the answer but impossible to find in the UK.
A private clinic prescribed artesunate instead of the promised valacyclovir- no response. Professor Scheibenbogen wrote that he’d unfortunately had two versions of ME but wouldn’t accept him as a patient. A bad reaction to LDN. Innumerable consultations…
He has managed to keep going until early last year, since when he’s spent most of the days lying down, feeling very ill. Recently I’ve been drawn to the research about idiopathic intracranial hypertension by Dr Nicholas Higgins, Cambridge, then reading Melissa’s excellent article, 28 April, I began to wonder if my son has something similar.
The paper, The Link between Idiopathic Intracranial Hypertension, fibromyalgia, chronic fatigue syndrome: exploration of shared physiology, 2018, referenced by Cort, among several about IIH on Health Rising, has charts showing differences and similarities between the conditions.
My son has many of them: headache, somewhat better lying down, fatigue, vestibular dysfunction-vertigo, tinnitus, rhinitis, temporomandibular disorder: paraesthesia, IBS, anxiety (naturally) muscle weakness.
I’d be glad to hear from anyone who has had lumbar punctures and felt better. (Cort described his in an early article.) Has anyone in the UK consulted Dr Higgins at Addenbrooke Hospital and been offered testing for idiopathic cranial hypertension as part of their ME treatment? I would be most grateful to hear from anybody who has had similar experiences.
Hi Susana, I would strongly caution *against* a lumbar puncture. While someone experiencing high pressure may find temporary relief by the release of that pressure, if he’s been leaking this long it may do serious damage to add another hole.
New research shows lumbar puncture to check opening pressure is ineffective in longterm leakers, as they can become trapped in a cycle of high and low pressure while their body tries to compensate for a leak. So a normal opening pressure may not be normal at all, and experts only recommend testing OP during a CT Myelogram or other test where a hole is already being opened for that. My opening pressure was normal despite leaking and I did see an increase in symptoms after my myelogram because it allowed more fluid to escape. I knew this was a risk but I felt more confident with a targeted patch, which requires knowing where the leaks are.
I’m sorry you’ve both gone through this. This is a very long time to suffer the effects of severe illness. But just from your comments here, I believe a leak specialist would be certain this needs imaging. As you said, some of these symptoms *only* appear with pressure issues and leaks.
I know it’s difficult to get into International doctors but I would recommend seeing one on the physician’s directory. When someone has leaked longterm, it takes a little more care to be certain they’re healed in the right manner—like not making new holes in the dura unless it’s absolutely necessary, using the proper type needle and gauge, adding the proper amount of blood or fibrin, and following up with care if he develops rebound high pressure (temporary high pressure caused by the sudden seal of a leak, due to the body no longer needing to produce as much fluid).
It’s my belief that illness can lead to a leak by causing damage to the connective tissue and raising cranial pressure (a system suddenly under pressure with a weak spot is more likely to burst), which could explain how many leakers have both illness and injury. But many leakers have symptoms that mirror illness (including fever and sore throat) so it’s hard to be sure which came first. Often, once a person becomes more familiar with causes and the less obvious symptoms, they’ll remember a sign of pressure issue that was present much earlier than the serious onset.
In any case, his profile, in my opinion, fits that of a leaker. I would love to see him connect with a leak specialist or, if that’s impossible, at least his doctors consulting one from the directory. I truly wish you the best of luck. <3
Hello Melissa, Thank you so much for this detailed reply.
IF this is the case, it would be far preferable not to have a lumbar puncture, I agree. When he was eight or nine, he was hit in the eye with a cricket back and spent a week in hospital to recover. I have wondered if that could have started it off. Yes, it’s along time. The constant vertigo, diagnosed as various things is the most unpleasant symptom together with the headache. I’ve started to look up specialists in this country and shall certainly keep in mind all your advice. Many, many thanks. I hope you continue to be wonderfully well Sue
Yes! Absolutely. So often with ME/CFS, connections aren’t looked for with physical injuries but it’s exactly the sort of event that triggers leaks. I would definitely mention it when you’re conferring with a leak specialist and always note the fact that he sees improvement flat. Those are two huge indicators, as well as the headache, tinnitus, and neurological issues. I’m so hopeful you’re on the right track for him! Everything, even his anxiety, may be a symptom of this pressure.
Many of the specialists on the directory will consult with other doctors if that helps. Good luck! And I’d love to hear back if they find a leak! https://spinalcsfleak.org/directory/
Good morning, Melissa,
Many thanks for your reply and your help!
It’s so generous of you to reply to everyone. I think you have a mission!
I shall follow this up now. I’ve already consulted the directory, now’s the time to show your responses to my son.
I wish you all the best,
Susana
And certainly I shall let you know if we’ve found the right direction , at long last,
Susana
I think I had the same problem. I was 24 years old and was in a car accident. the doctor did a spinal tap. I don’t know why, but he said he was completely safe so I never gave it a second thought. When I was on the table and he was doing the spinal tap, I started shaking uncontrollably. After I got a headache, but the doctor said I would be fine and that was the end of it. However, I started having health problems. Chronic fatigue, ringing in the ears, light sensitivity, and sharp stabbbing pains in my skull. I didn’t know what to think of it and just brushed it off as I thought I would get better because the symptoms would come and go. What happened was my skull lost bone volume or collapsed, it was a slow process so I never figure it was caused by the spinal tap. I also have constant ringing in the ears and constant pain throughout my spine. I’m now 59 and after all these years of being sick, I believe I finally figured out why I was sick for almost 34 years. It was because I spinal tap I had when I was 24 yrs old because the doctor said it was completely safe and the only complications I would have was a headache for a couple of hours after.
Thank you for sharing your story, Peter. I’m so sorry this has happened to you. So many leakers are disregarded in the same ways—I’ve seen stats that as many as 98% of cases are misdiagnosed—and I find it endlessly frustrating that despite the abundance of evidence via imaging, studies, and patient cases, the majority of the medical community refuses to familiarize themselves with the current knowledge or update their outdated testing methods.
I hope that with more and more of us speaking up and finding our underlying causes, this information will spread and prevent the same from happening in future. But it’s certainly been a battle to get anyone besides leak specialists to take such a clear and sensible explanation as injury or illness causing pressure on the brainstem seriously, even with the proof.
I realize you’ve been ill for a great deal longer than I was, but I hope now that you are aware of the cause you will be able to find improvement and perhaps a good care team. I’ve been researching more now that my cognitive issues have improved and I plan to share as much as I can.
Melissa,
Thank you for sharing your journey. When i first read it back in April I almost fell over because I related to it so immensely. For the first time-someone was speaking my language, so much so, that I sent the article to my neurologist and asked could I have this?? He said my symptoms seemed very distinct and said they warranted the needed testing. He also said it is not his area of expertise but let’s get started with a brain MRI w/ contrast which we did in June. It came back “normal” and he decided he didn’t think this was a CSF issue. I fought hard, did extensive research and came back with citing research studies from Duke University and was able to help him see that the “normal” MRI doesn’t necessarily mean a whole lot especially with all these awful symptoms I’ve been enduring for 8 years now (he diagnosed me with POTS and Fibromyalgia 8 years ago and I was told we’ll never know the cause because we’ve tested for everything and nothing has shown up so now you need acceptance and coping.) I was in my absolute prime when this came on out of nowhere. I was a distance runner, working full time and living a very full, active life.
I’ve had to resign from my work and was declared disabled 7 years ago. It’s been brutal. The losses have mounted up BUT your journey lit a fire in me and I have HOPE for the first time in years. I am currently in the 2nd stage of acceptance into Duke University’s CSF program. I want to thank you from the bottom of my heart for being a voice for so many people struggling. I can’t wait to share my story in the future! Do you have any advice for me in my CSF journey? It’s so much to take in and I stay away from horror stories, only focusing on healing.
You are a blessing. God is so good.
Thank you so much for writing! I’m currently working to rebuild my life while also trying to create resources for leakers, and hearing from people who this is helping means everything!
I am so excited for you! I’m sorry about the horror stories because I feel like they’re a deterrent for a lot of people but I would caution that many of the cases that are more complicated are more likely to continually post in groups (while the majority with less complicated recovery move on and never look back). There’s a stat that says 80% respond favorably to one or more patches and I think that’s a really important figure that’s rising all the time as leak specialist learn more and more about the various causes and repairs. The reality is that a blood patch is just a syringe of blood and a few days lying flat, when many of us would do so much more to get our lives back.
My patch procedure wasn’t anything in comparison to my illness. But even now I’m still learning about pressure issues. My main tip would be to keep fighting for imaging—this is really the biggest hurdle and I’m thrilled you’re headed to Duke. Once they see the leak things become simpler and having doctors who understand that all of our seemingly unconnected symptoms stem from this one thing makes dealing with the medical system much less complicated. We don’t need ten doctors and a dozen prescriptions. We just need the leak fixed.
Secondly I think it’s really important to learn about Rebound High Pressure and about high pressure in general. I’ve discovered I had an existing high pressure issue that contributed to my leak. High pressure tends to make a person need to move and my specialist believes this is a connection that a lot of us have. We’re active and creative and push through illness because our bodies are urging us toward those things. What doctors are now learning is that high pressure when it’s too high can also create symptoms like fatigue, brain fog, POTS, and pain in the same way that leaks do. Leaks cause the brain to sag and press on the brain stem and high pressure pushes downward, also pressing on the brain stem.
When I wrote my posts I thought the few lingering cognitive issues were from being sick for so long and having brain sag. I now know that it was actually the high pressure. So when I manage that well I’m able to think clearly and write again, sometimes more efficiently than even before leaking(!).
The good news is that Duke knows about rebound high pressure and will look for underlying high pressure issues while they’re doing imaging. The bad news is that you have to navigate that on your own during recovery because there’s not a reliable way to sort high pressure from low. It’s sort of a vibe. Lol A lot of us with high pressure feel it more like a pressure sensation and less like stinging or sharp pains. Or we get the symptoms of high in one area of the head or body and low in others. I would suggest finding a pressure-buddy or the Rebound High Pressure FB group to ask when you’re post patch (I would assume you may be more likely to have rebound pressure since you’ve been dealing with this for so long and your body is accustomed to making additional fluid, but no one really knows whether or not production will adjust quickly—it’s just easier to be prepared and have low salt foods or a pressure medicine at the ready).
The rest of the tips are just practical. While you wait for your dura to heal you’re going to want to keep your spine straight and not bend, lift, twist, or strain. So set up your situation so that you don’t have to. I keep all my chores at chest level now. I have a wedge pillow for reclining (sitting at a 90 degree angle raises pressure) and a cushion for driving. Someone else is responsible for lifting all the things—it’s not worth it to risk starting the process over when it takes so long to get in to the specialists.
The two weeks post patch they’ll probably want you pretty flat (each doctor has different rules depending on your case specifics) so you may want to have a phone holder overhead and some flat foods and activities ready. Things may get weird as your pressure normalizes but don’t panic. You’ll have an amazing team to answer questions and their only real concern is usually signs of infection (high fever, neck stiffness, numbness, or bladder issues).
I’ve posted a work-in-progress website at http://www.PressureResources.com and it lists some more management and post-patch tips. I would always recommend taking notes and a symptom list with your test history with you to appointments so that you can remember to ask your questions in the shuffle (and in the upright time) and are ready with any information and already completed testing that might prevent delays. I’m sure you understand by now how much patience this whole ordeal requires but I’m SO HOPEFUL for you and I’m thrilled that you’re going for such a great team. I would also note that I’ve heard Duke will sometimes give the standard spiel that it’s less likely to be a leak if the MRI findings are normal but this isn’t the case with more than 20% of leakers (especially longtime leakers, as our bodies adapt—we’re also less likely to have clear positional symptoms). It’s hard not to have anxiety over things that are said or whether they’ll be able to find the leak but a good team will persevere. This isn’t some mystical force, it’s a very cut and dry mechanical issue that’s causing leak symptoms, and a specialist knows that. I wish you the best of luck and hope to hear more as you find your answers!
Hi could you tell me what kind of eye disturbances you had? Any eye floaters? Or trouble with focusing in large areas.
I personally had a lot of eye floaters and sometimes blurry vision. It’s important to note that this is very dependent on the case (and sometimes the cause) and that high intracranial pressure does not actually have to exhibit papilledema and low may not exhibit eye symptoms at all. I had an underlying high pressure issue with my leak, so I had both high and low symptoms. Some people have more intense vision involvement or dark spots or may black out. Current leak data suggests the most common are sensitivity to light, blurring, double vision, and visual field defects, but honestly a lot of us experience issues not listed on the data sheets.
I had my eyes tested while leaking and afterward and no signs of a pressure issue showed in those tests (this is good news, as nothing was damaged but it’s not particularly helpful for leak diagnostics).
I hope this is helpful.
Hi Melissa,
when stenosis could cause spinal leaks isn’t there a risk it will do it again after all leaks were patched?
Is there any experience if spinal leaks could close themselves, for instance if high intra cranial pressure resolved by another treatment.
Yes! It really depends on what caused the leak. For me, it was several leaks that were too large to heal by themselves—and because I didn’t realize what was happening for the first few years and made them repeatedly worse by continuing upright activity and twisting my spine. In cases where there are bone spurs or severe stenosis, surgery may be required.
It can take as long as a year for the dura to fully heal and I opened a new leak after having Covid but was able to reseal that on my own by staying flat for a few days.
Some leaks can heal if given the chance. But we have to know what’s happening in our bodies. That’s why it’s important to find a leak specialist who knows how best to deal with the various situations and to get the right imaging.
I have a website up at pressureresources.com with more info if you’d like to check it out. I hope it’s helpful!
Thank you.
Melissa-
I just want to say thank you for sharing your story. I too have had a very long journey with csf leak. It was finding your story that helped me to see that all of the random experiences and symptoms I was having were actually connected and there WAS a reason. As you know, advocating for your own health, especially feeling as bottomed out as one gets, is so immensely challenging. I’ve had 2 in office smaller blood patches and I am a week out from my second LVBP. The first being 100cc and my latest 80cc. Every patch helped me to gain a sliver of my life back. It is my greatest hope this last one will resolve my remaining symptoms so I can pick my life back up and no longer only be an observer. This has been over a 3 year process for me with debilitating pain and struggles. It is my hope that someday I too will be able to help someone through my suffering. So thank you! Thank you for “pointing me in the right direction”!
Good luck!
Thank you so much for posting, Laurie. It’s amazing when it clicks for someone that the symptoms all make sense when viewed as a leak, and I truly wish everyone could be evaluated as part of their diagnostic process. I hate that so many of us have to suffer for so long and that finding expert help isn’t quick and easy.
But I am so happy to hear you’re finding improvement! I hope you’re able to get a good, solid seal this time. After being sealed, I had a leak open with Covid and just knowing what was happening helped so much. I was able to get flat for a few days and seal at home, on my own. So I do think once the larger holes are repaired the body can catch up a bit (assuming we let it). I also saw additional improvement over the following months just as I gained back my strength and learned all the ways my underlying high pressure had been affecting me. Please feel free to reach out if there’s anything I can help with. I’ve added some post-patch and rebound high pressure tips on my website, but you may have those down by now. I will be pulling for you!
Hi,
Do you know of any other recovery stories for ME/CFS patients who have gotten better after treating a csf leak.
I get a positional headache when looking down and have been suspecting a csf leak for a while. My ME/CFS is severe so im trying to gauge whether it’s worth the risk of getting a good bit worse in case treating a leak cures me (or atleast helps).
Thanks
Hi Matthew. For me, the answer was absolutely yes, because the leak was causing pressure issues that drove every single one of my symptoms. But everyone’s case is different so until a person has the proper imaging and can figure out what’s happening, there’s always a risk.
Many people in the leak groups recover or find major improvements but the key is finding the right doctor. A lot of us waste years or worsen after the wrong care but a true, knowledgeable leak specialist is more likely to know what risks are involved in each case and how likely it is that a patch or repair can bring improvement.
I understand that it’s a legitimate concern, but my view is that the risks that come with not treating a leak are much more likely to increase disability over time. (That said, I would verify that a patch would be offered regardless of whether the leak was found before any procedure that punctured the dura.)
If you’re in any of the Facebook groups, you can search success stories to find those who it helped (though a lot of people who recover leave the groups and move on). I hope you’re able to find improvement. The Spinal CSF Foundation website has a directory of doctors who work with leaks.